Abstract
Phosphomannomutase-2 (PMM2) deficiency represents the most common congenital disorder of glycosylation (CDG). Currently, little is known about cell metabolic alterations occurring in these patients. Here, we quantified compounds connected to protein glycosylation (GDP-mannose, UDP-derivatives), energy metabolism (high-energy phosphates, nicotinic coenzymes, oxypurines), oxidative/nitrosative stress (GSH, nitrite, nitrate) and free amino acids in extracts of peripheral blood mononucleated cells (PBMCs), of seven PMM2-CDG patients and ten control healthy donors. Besides marked GDP-mannose decrease, PBMCs of PMM2-CDG patients had higher UDP-glucose (UDP-Glc), UDP-galactose (UDP-Gal) and UDP-Glucuronic levels, lower ATP, GTP and UTP levels, abnormal ATP/ADP, ATP/AMP and NAD+/NADH ratios, increased xanthine, uric acid and nitrite + nitrate levels, and decreased GSH and free amino acids concentrations. These results suggest a new, conceivable metabolic route leading to the increase of specific UDP-derivatives (UDP-Glc, UDP-Gal and UDP-Glucuronic), also potentially explaining the glycogen abnormalities recently found in PMM2-CDG patients. Altogether, this study highlighted various metabolic changes caused by PMM2 deficiency, illustrating the widespread effects of PMM2 mutations (beyond N-glycan biosynthesis) that may significantly vary depending on the cell line considered. Using PBMCs, as a cellular model of lower invasiveness than skin fibroblast, may advantage cell metabolism studies to investigate new therapies specifically targeted to PMM2 deficiency.
Similar content being viewed by others
Introduction
Congenital disorders of glycosylation (CDG) are a large group of inborn errors of metabolism characterized by abnormalities in the post-translational process of protein glycosylation1. CDG account for more than 190 different diseases caused by defective glycosylation sites occupancy, architecture aberrations of the oligosaccharide chain organization, defects in monosaccharide precursor transporters, or mixed errors of them2,3. Physiologically, glycosylation is a complex biochemical network of covalent modifications involving proteins and lipids, evolving from the synergism between the cytoplasm and the cellular organelles1,4. Protein glycosylation may occur either through the involvement of OH-groups of specific serine and threonine residues (O-glycosylation), or through the participation of specific asparagine (Asn) residues (N-glycosylation). The molecular mechanisms underlying this multistep-process are guaranteed by the activity of several glycosyltransferases, using activated forms of sugars and amino-sugars (such as UDP-glucose, UDP-galactose, GDP-mannose, UDP-N-acetyl-D-galactosamine, UDP-N-acetyl-D-glucosamine), recruited from the cytosol, as glycosylic donors. Particularly, the N-linked glycosylation of proteins, specific for endoplasmic reticulum (ER), starts with the assembly of a well-ordered 14-sugars oligosaccharide precursor of (N-Acetyl-glucosamine)2-(Mannose)9-(Glucose)3 attached at the dolichol bridge inserted into the ER membrane. Oligosaccharide specific transferases (OST) will then move the entire branch from dolichol to an Asn residue of the newly formed protein in the ER5, ready for subsequent remodelling. The correct formation of the oligosaccharide chain needs constant supply of GDP-mannose (GDP-Man). This compound is uniquely generated in a specific pathway, in which mannose is initially phosphorylated to mannose-6-phosphate by hexokinase. The sequential activities of Phosphomannomutase-2 (PMM2) and GDP-mannose pyrophosphorylase B (GMPPB) respectively convert mannose-6-phosphate into mannose-1-phosphate and, in a GTP-dependent reaction, mannose-1-phosphate into GDP-Man and pyrophosphate.
PMM2-CDG, the most common CDG, is an autosomal recessive disorder caused by mutations of the gene encoding for PMM2. Patients with PMM2-CDG present with prominent neurological involvement such as cerebellar atrophy6,7, neurodevelopmental delay8, hypotonia9and variable systemic involvement including, among others, hepatopathy, endocrinological and coagulation abnormalities10. PMM2 mutations cause the expression of defective PMM2 proteins with decreased enzymatic activity, provoking remarkable decrease in GDP-Man synthesis with hypoglycosylation of multiple proteins and consequent alterations of their localization and functionality1,11. Protein glycosylation defects are exploited in the laboratory diagnosis of PMM2-CDG through the analysis of serum transferrin glycoforms12, although this assay is seriously limited by serum transferrin glycosylation falling in the range of normality even in presence of CDG13,14and including PMM2-CDG15.
Notwithstanding the progress in the knowledge of PMM2 deficiency, little is currently known about the biochemical changes of cell metabolism connected to energy state, oxido-reductive state of nicotinic coenzymes, UDP-derivatives, antioxidants, nitrosative stress biomarkers and free amino acids provoked by malfunctioning of the GDP-Man production pathway. To fill this gap, recent studies provided evidences that skin fibroblasts from PMM2-CDG patients have altered levels of amino acids and acylcarnitines16, as well as significant alterations of cellular bioenergetics17,18. Additionally, it has been shown that PMM2-CDG is associated with abnormal urinary excretion of sorbitol and mannitol, probably because the accumulated mannnose-6-phosphate is isomerized to fructose-6-phosphate and glucose-6-phosphate, which are dephosphorylated and then converted to sorbitol by aldose reductase19. In the same study, treatment of skin fibroblast with an aldose-reductase inhibitor improved cellular protein N-glycosylation and, the long-term administration to one PMM2-CDG patient only, improved ataxia scores together with significant growth improvement, thus supporting the significant role of the proposed fate of excess mannose-6-phosphate in conditions of PMM2-deficiency19.
Although these studies pointed out previously unknown information of cell metabolism of PMM2-CDG patients, information on the cross-talk among GDP-Man and some of the aforementioned metabolites (i.e., the UDP-derivatives UDP-glucose, UDP-galactose, UDP-N-acetyl-D-glucosamine, UDP-N-acetyl-D-galactosamine and UDP-Glucuronic) involved in protein glycosylation has partly been evaluated in one study only, again using skin fibroblast as the cell line obtained from PMM2-CDG patients20. Importantly, previous studies on cellular metabolism in PMM2-CDG performed in skin fibroblasts might be not ethically amenable for clinical application.
In order to provide new metabolic information in a less invasive cell model, in this study we used peripheral blood mononucleated cells (PBMCs), obtained from a homogeneous cohort of compound heterozygous PMM2-CDG patients (all carrying the same c.422G>A; p.R141H mutation on one allele) and from a group of control healthy donors. We used a targeted metabolomic approach evaluating HBP-related UDP-derivatives, along with energy state metabolites, antioxidants, nitrosative stress biomarkers and free amino acids.
Results
Clinical features of PMM2-CDG patients
Table 1 summarizes the main clinical features of each of the seven PMM2 patient recruited in the study. These PMM2-CDG patients were compound heterozygous all carrying the same PMM2 mutation c.422G>A; p.R141H (100%) associated with other known PMM2 pathogenic variants (Table 1).
PMM2 mutation c.422G>A; p.R141H is very common in PMM2-CDG patients and has been found to affect both folding and catalytic properties of the PMM2 protein, with consequent quite null residual activity. No homozygous patients with this mutation have been reported, probably because homozygosity is incompatible with life21. Additional associated heterozygous PMM2 mutations include c.647A >T; p.N216I, c.385G>A; p.V129M and c.667G>A; p.D223N which have been reported in association with severe phenotypes22. All patients had early presentation, with psychomotor delay, hypotonia, strabismus and dysmorphisms. Cerebellar symptoms appeared in the first years of life and cranial magnetic resonance imaging (MRI) showed severe atrophy of cerebellar hemispheres and vermis with atrophy of the brainstem. Overall disease severity measured by the NCRS was moderate to severe (Table 1). All patients had developmental disability, severe cerebellar atrophy (100%) (ataxia scoring > 20 on the BARS), inability to walk unsupported (100%), visual defects (100%), epilepsy and stroke-like episodes occurrence (28% and 42%, respectively). At the study time, patients were on free diet and they were not supplemented with oral D-galactose. Two patients were receiving anti-epileptic drugs (Phenobarbital and Levetiracetam).
Concentrations of specific compounds connected to protein glycosylation are modified in PBMCs of PMM2-CDG patients
The Panel A of Fig. 1 illustrates the concentrations of GDP-mannose detected in PBMCs from control healthy subjects and from PMM2-CDG patients.
Concentrations of GDP-mannose and UDP-derivatives in controls and PMM2-CDG PBMCs. GDP-mannose (A), UDP-Glucuronic (B), UDP-Gal (C) and UDP-Glc (D) were detected by HPLC in deproteinized extracts of PBMCs obtained from control healthy subjects and PMM2-CDG patients. Mean values and standard deviations are indicated by vertical bars. **Significantly different from controls, p < 0.001. ***Significantly different from controls, p < 0.005.
As expected, the reduced production of mannose-1-phosphate, caused by defective PMM2, resulted in a decreased formation of GDP-mannose, the concentration of which was 15.43 ± 3.03 pmol/106 cells and 8.82 ± 3.02 pmol/106 cells in controls and PMM2-CDG patients, respectively (p < 0.001).
When calculating the concentrations of UDP-Glucuronic and of the four UDP-derivatives, involved in the HBP and in the protein glycosylation process, PBMCs from controls and PMM2-CDG patients showed no changes in the levels of UDP-GalNac (24.60 ± 6.88 pmol/106 cells and 21.86 ± 9.62 pmol/106 cells in controls and PMM2-CDG patients, respectively) and UDP-GlcNac (39.81 ± 5.79 pmol/106 cells and 44.29 ± 13.43 pmol/106 cells in controls and PMM2-CDG patients, respectively). Conversely, as shown in Fig. 1, UDP-Glucuronic (B), UDP-Gal (C) and UDP-Glc (D) had significantly higher values in PBMCs from PMM2-CDG patients, compared to the values measured in PBMCs extracts of controls. Additionally, when calculating the UDP-Gal/UDP-Glc ratio in controls and PMM2-deficient PBMCs it was found that the value decreased from 0.70 ± 0.11 to 0.41 ± 0.14 (p < 0.001), thus indicating not only a change in the concentrations of these UDP-derivatives, but also an alteration in their interconversion and/or utilization.
Energy metabolism is deeply imbalanced in PBMC from PMM2-CDG patients
When analysing energy metabolism (Fig. 2A–C), we found a profound imbalance in PBMCs from PMM2-CDG patients. Indeed, the amounts of ATP, GTP and UTP were 40.0%, 37.8% and 29.4% lower, respectively, than the corresponding values recorded in controls (p < 0.01, p < 0.025 and p < 0.025, respectively;). No changes were found in the CTP levels (Fig. 2D).
Energy metabolism in PBMCs of controls and PMM2-CDG patients. Concentrations of ATP (A), GTP (B), UTP (C), CTP (D) ADP (E), and AMP (F) were detected by HPLC in deproteinized extracts of PBMCs obtained from control healthy subjects and PMM2-CDG patients. Values of the ATP/ADP (G) and ATP/AMP (H) ratios of PBMCs of controls and PMM2-CDG patients were calculated using the actual concentrations of ATP, ADP and AMP determined in each sample. Mean values and standard deviations are indicated by vertical bars. *Significantly different from controls, p < 0.01, **p < 0.001.
PBMCs of PMM2-CDG patients had significantly higher values of both ADP (1.74 times, p < 0.005, Fig. 2E) and AMP (4.47 times, p < 0.0001, Fig. 2F), with respect to the corresponding concentrations detected in PBMCs from healthy controls. The increase of these compounds, coupled with the decrease in ATP (Fig. 2A) provoked profound decrease in both ATP/ADP (−67.6%, p < 0.0001, Fig. 2G) and ATP/AMP (−87.0%, p < 0.0001, Fig. 2H) ratios in PBMCs of PMM2-CDG patients, compared to the corresponding ratios calculated in healthy controls.
The results suggesting imbalance of energy metabolism, related to mitochondrial malfunctioning in PBMCs of PMM2-CDG patients, are corroborated by the ratios of the oxidized and reduced nicotinic coenzymes and the levels of acetyl-CoA. Respect to values determined in PBMCs of controls, whilst no changes in the NADP+/NADPH ratio were observed (Fig. 3B), PMM2-CDG patients showed significant decrease in the NAD+/NADH ratio (−45%, p < 001, Fig. 3A), as well as in the concentration of acetyl-CoA (−23.1%, p < 0.02, Fig. 3C).
Nicotinic coenzyme ratios and acetyl-CoA in PBMCs of controls and PMM2-CDG patients. NAD+/NADH ratio (A), NADP+/NADPH ratio (B) and acetyl-CoA (C) determined in PBMCs obtained from control healthy subjects and PMM2-CDG patients. Values of the nicotinic coenzyme ratios of PBMCs of controls and PMM2-CDG patients were calculated using the actual concentrations of NAD+ , NADH, NADP+ and NADPH determined in each sample. Mean values and standard deviations are indicated by vertical bars. *Significantly different from controls, p < 0.01. **Significantly different from controls, p < 0.02.
Concentrations of GDP-mannose and UDP-Glc correlate with those of specific energy metabolites
In order to assess whether the metabolites involved in protein glycosylation and significantly altered in PBMCs of PMM2-CDG patients, namely, GDP-mannose, UDP-Glc and UDP-Gal, we calculated the Pearson’s regression coefficients of each of these three compounds and each of the energy-related metabolites determined in PBMCs extracts. Whilst no correlations were found in the case of UDP-Gal, the concentrations of GDP-mannose positively correlated with those of GDP (Fig. 4A). Additionally, UDP-Glc was inversely correlated with the concentrations of ATP (Fig. 4B) and of the ATP/ADP ratio (Fig. 4C), strongly suggesting a connection between the alterations of UDP-Glc levels and the imbalance in energy metabolism.
Correlations of GDP-mannose and UDP-Glc with parameters of energy metabolism. Concentrations of GDP-mannose and GDP, detected in PBMCs of PMM2-CDG patients, showed positive correlation (A), whilst UDP-Glc concentrations were negatively correlated with those of ATP (B) and of the ATP/ADP ratio (C). The Pearson’s correlation coefficients and the corresponding p values are indicated in each panel.
Purines increase, antioxidants decrease and oxidative/nitrosative stress occurrence in PBMCs from PMM2-CDG patients
As a consequence of the imbalance of energy metabolism, PBMCs from PMM2-CDG patients showed remarkable increased levels of xanthine (16.0 times, p < 0.0001, Fig. 5A) and uric acid (1.55 times, p < 0.02, Fig. 5B) compared to the corresponding values observed in controls. These data suggest an increased rate of the adenine nucleotide catabolic pathway, due to the imbalance between ATP production and consumption, causing remarkable increase of dephosphorylated products of ATP catabolism (ADP, AMP, xanthine and uric acid).
Catabolites of ATP, GSH and nitric oxide metabolism in PBMCs of controls and PMM2-CDG patients. Concentrations of xanthine (A) and uric acid (B), GSH (C) and nitrite + nitrate (D) determined in PBMC obtained from control healthy subjects and PMM2-CDG patients. Mean values and standard deviations are indicated by vertical bars. N.D. = Not Detectable. *Significantly different from controls, p < 0.01. **Significantly different from controls, p < 0.001.
Thanks to the HPLC methods used to determine metabolites in cell extracts, it was possible to quantify, simultaneously to the aforementioned compounds, the concentrations of the main water-soluble intracellular antioxidants, i.e., ascorbic acid and reduced glutathione (GSH). Whilst no significant differences in the ascorbate concentrations of PBMCs from controls (415.29 ± 121.19 pmol/106 cells, not shown in the Fig. 5) and PMM2-CDG patients (453.39 ± 235.29 pmol/106 cells, not shown in the Fig. 5) were found, significantly lower GSH levels in PMM2-CDG patients (−37.6%, p < 0.0002 compared to controls, Fig. 5C) were measured. GSH decrease in PBMCs from PMM2-CDG patients was accompanied by significant increase in the sum of nitrite + nitrate (2.0 times, p < 0.0002 compared to controls, Fig. 5D), considered as stable end-products of nitric oxide formation, thereby indicating potential, dangerous conditions of nitrosative stress.
PBMCs from PMM2-CDG patients have altered concentrations of specific free amino acids
The separate HPLC analysis, dedicated to quantify the PBMCs’ content in free amino acids (FAA), revealed that PMM2-CDG patients have distinct modifications of the FAA profile. Indeed, only 7 out of 25 standard and non-standard amino acids levels quantified in PBMCs’ extracts, were significantly different in PMM2-CDG patients with respect to controls (Supplementary Fig. 1 A).
In particular, Asn, Gln, Ser and Thr levels (Supplementary Fig. 1B and 1C respectably), and His, Trp and Arg concentrations (Supplementary Fig. 2A-C) were significantly decreased in PBMCs of PMM2-CDG patients. Because of the peculiar role in cell metabolism of PBMCs, it is worth underlining the 1.92 fold lower Gln concentrations found in PMM2-deficient PBMCs (p < 0.0001 compared to control PBMCs). Additionally, the Global Arginine Bioavailability Ratio (GABR = Arg/Citrulline + Ornithine), indirectly connected to cell nitric oxide production, was significantly decreased in patients’ PBMCs (from 1.01 ± 0.31 in controls to 0.36 ± 0.14; p < 0.0001; Supplementary Fig. 2D), thus corroborating the occurrence of nitrosative stressing conditions in PMM2-deficient cells.
Pattern of metabolites in PMM2-deficient PBMCs potentially affects multiple cell metabolism pathways
In order to assess whether the metabolite pattern of PMM2-deficient PBMCs may potentially influence various cellular biochemical pathways, we performed targeted metabolomics pathway analysis. The enriched metabolic pathways demonstrated that a large number of pathways are potentially malfunctioning in PMM2-CDG patients. Figure 6 shows the top 25 most affected pathways, among which amino sugar metabolism, nucleotide metabolism, fructose and mannose metabolism and GSH metabolism are those most potentially influenced by the metabolite concentrations occurring in PMM2-deficient PBMCs.
MetaboAnalyst-based enrichment analysis of the key metabolic alterations in PMM2-deficient PBMCs. Enrichment and pathway analyses were performed using the actual concentrations of the different metabolites detected in control and PMM2-deficient PBMCs, processed through the MetaboAnalyst 6.0 platform. Specifically, the “Pathway Analysis” module within the enrichment analysis section was used to identify significantly impacted metabolic pathways. The analysis was performed using default parameters. Pathways with a p-value of less than 0.05 were considered significantly enriched, indicating potential areas of metabolic perturbation associated with the experimental conditions. Only the top 25 pathways significantly different from controls were considered in the figure.
Discussion
In the present study, using PBMCs as a cell model obtainable through moderately invasiveness procedures, we found that PMM2-CDG patients have alterations of metabolites related to the HBP, mitochondrial-dependent energy metabolism, antioxidant defences, nitrosative stress and free amino acids, some of which were to date previously unreported.
Compared to values measured in PBMCs from control healthy subjects, defective PMM2 activity in PBMCs caused, as expected, significant decrease in GDP-mannose levels and, less predictably, increase in UDP-Gal and UDP-Glc. In order to explain the increase of sorbitol and mannitol into the blood and urine of PMM2-CDG patients, previous studies performed in fibroblasts from PMM2-CDG patients, hypothesized that malfunctioning of PMM2 activity causes accumulation of mannose-6-phosphate which is isomerized into fructose-6-phosphate, subsequently dephosphorylated into fructose, and leading to its final conversion into the aforementioned poly-alcohols through the activity of aldose reductase17,19. In vitro evaluations and functional analyses in a PMM2-mutant Zebrafish corroborated this hypothesis and showed the effectiveness of an aldose-reductase inhibitor to significantly decrease polyol levels and increase GDP-mannose19.
Our data, referring to the PBMCs’ concentrations of UDP-Gal and UDP-Glc, strongly suggest the existence of an alternative metabolic fate for excessive mannose-6-phosphate, under the pathological conditions of PMM2 deficiency. Indeed, the fully reversible reaction catalyzed by MPI would cause increase of fructose-6-phosphate, through the higher isomerization rates of excessive mannose-6-phosphate. With the same mechanism, GPI would isomerize excessive fructose-6-phosphate into glucose-6-phosphate, and PGM would isomerize excessive glucose-6-phosphate into glucose-1-phosphate. The increase in substrate availability (glucose-1-phosphate) for UGP2, the enzyme catalyzing the UTP-dependent production of UDP-Glc, would ultimately produce the increase in UDP-Glc and UDP-Gal (formed by GALE in an equilibrium reaction between these UDP-derivatives). On the other hand, the equilibrium reactions transforming mannose-6-phosphate into fructose-6-phosphate, and subsequently into glucose-6-phosphate, are considered as the privileged metabolism of mannose-6-phosphate, since it was demonstrated that its isomerization by MPI transforms > 95% of the total cellular mannose-6-phosphate23,24. Therefore, increasing the intracellular levels of mannose-6-phosphate, because of PMM2 malfunctioning, will certainly lead to the increased production of the two other 6-phosphate sugars, thereby creating the favouring conditions to the increase in UDP-Glc and, in the cell lines with high biosynthetic rate of glycogen (hepatocytes), to the increase in glycogen production.
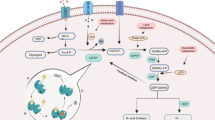
Recently, it has been found that PMM2-CDG patients have scattered hepatocytes with foci of glycogenosis25. According to what aforementioned, this phenomenon may reasonably be explained by the increased UDP-Glc availability that, when occurring in hepatocytes, may imbalance glycogen homeostasis, by increasing glycogen formation at rates higher than those of its consumption, and causing the glycogen deposits observed in liver biopsies of PMM2-CDG patients25. Schematic representation of the aforementioned reactions is depicted in Fig. 7.
Schematic representation of the metabolic pathways directly affected by PMM2 malfunctioning in PMM2-CDG patients. Increase in mannose-6-phosphate (Man-6-P) causes increased concentrations of fructose-6-phosphate (Fru-6-P) first, and subsequent increased concentrations of glucose-6-phosphate (Glu-6-P), because of the equilibrium reactions catalyzed by mannose phosphate isomerase (MPI) and glucose phosphate isomerase (GPI), respectively. Higher Glu-6-P availability leads to increased formation of UDP-glucose (UDP-Glc). At the same time, the increase of Fru-6-P availability also allows to maintain an adequate synthesis of UDP-GlcNac, thus ensuring a significant level, although partial, of protein glycosylation. Higher levels of UDP-Glc could be responsible for increased rate of glycogen synthesis, thus explaining the abnormal glycogen accumulation observed in the liver of PMM2-CDG patients. Arrows in red indicate the reactions occurring under these pathological conditions. Compounds in the faint yellow boxes are those undergoing significant increases.
PBMCs of our cohort of PMM2-CDG patients had higher levels of both these UDP-derivatives and a decreased value of the UDP-Gal/UDP-Glc ratio, strongly suggesting that these pathobiological mechanisms are operative, as indicated above, in the case of PMM2 deficiency. On the other hand, the occurrence of altered metabolism of UDP-derivatives may also help to explain the decreased levels of UTP in PBMCs of PMM2-CDG patients, because of a higher rate of utilization by UGP2 to form UDP-Glc. Both UDP-GlcNac and UDP-GalNac concentrations in PBMCs from PMM2-CDG patients had values similar to those measured in controls, consistent with unimpaired mucin type O-glycosylation. Interestingly, in a study analyzing fibroblast metabolism of CDG patients carrying PGM1 mutations, UDP-Gal and UDP-Glc were separately quantified, with the former showing higher levels compared to controls, and the latter being unchanged26. Our results indicate that PMM2 deficiency produces an increase in both UDP-derivatives: This difference, respect to the aforementioned study, may possibly be due to the different cell line used as well as to the different defective enzyme causing CDG. To complete the picture of the changes in UDP-derivatives in PMM2-deficient PBMCs, we found, compared to control PBMCs, higher concentrations of UDP-Glucuronic acid. Hence, it appears that part of the increased UDP-Glc is oxidized by UDP-Glc dehydrogenase, leading to increased concentrations of UDP-Glucuronic acid and the empowerment of glycosaminoglycan biosynthesis. The decision on what is the metabolic fate of the excess of UDP-Glc should mainly be dictated by the specific metabolic feature of the cell line considered, each of them having its own peculiar pattern of protein glycosylation27 and, consequently, of substrate requirement for its achievement.
Results of our study clearly showed that, together with changes of the compounds necessary for protein glycosylation, cell metabolism under conditions of PMM2 deficiency suffers from profound impairment of mitochondrial-related energy production, as indicated by the alterations of some of the key compounds of the cell energy metabolism (ATP, ADP, AMP, ATP/ADP and ATP/AMP ratios, GTP, NAD+/NADH ratio, acetyl-CoA, xanthine, uric acid). Altogether, modifications of the aforementioned molecules in PMM2-deficient PBMCs are indicative of a decreased phosphorylating capacity of mitochondria (ATP, ADP, ATP/ADP ratio), an impairment of the Krebs’ cycle (GTP, NAD+/NADH ratio and acetyl-CoA), a shift towards a more glycolytic metabolism (NAD+/NADH ratio), an activation of the degradation pathway of adenine nucleotides (ATP, AMP, ATP/AMP ratio, xanthine, uric acid). Similar patterns of energy metabolism impairment are detectable under various pathological conditions sharing, as a common metabolic feature, transient or permanent mitochondrial dysfunction28,29,30.
It is worth underlining that the negative correlations found between UDP-Glc and ATP, as well as with ATP/ADP ratio, strongly suggest that the increase in this UDP-derivatives may represent an additional negative factor significantly contributing in the overall impairment of energy metabolism of PMM2-deficient PBMCs.
Previously, decreased mitochondrial maximal ATP-linked respiration, as well as decreased complex I function of the mitochondrial ETC was detected in PMM2-CDG cultured fibroblasts and related to impaired autophagy biomarkers17. However, contrary to these results17, it has recently been reported that, in the same model of cultured fibroblasts, cells from PMM2-CDG patients had decreased glycolysis, increased activities of complexes I and II of ETC, increased levels of oxidative phosphorylation supercomplexes and unchanged mitochondrial capacity to generate ATP31. Our results clearly indicate an impairment of mitochondrial-related energy metabolism in PBMCs of PMM2-CDG patients, leading to significantly decrease in the concentrations of both purine and pyrimidine tri-phosphate nucleotides and shift of metabolism towards glycolysis. Differences compared to previous studies may possibly be due to the different cell model used17,31,32 and, consequently, to the respective metabolic cell characteristics.
It is well established that dysfunctional mitochondria are the main intracellular source of ROS formation33,34, triggering oxidative/nitrosative stress35,36. Hence, the decrease in GSH and increase in nitrite + nitrate observed in PMM2-CDG patients’ PBMCs may certainly be connected to the impairment of mitochondrial functions occurring in this glycosylation disorder. To our knowledge, no studies have previously shown that cells of PMM2-CDG patients have decreased antioxidant defences and nitrosative stress. This finding may be of utility in light of possible treatments providing recovery of GSH and preventing cell damages induced by increased RNS production.
The aforementioned hypotheses, connecting the alterations of the metabolic pattern of PMM2-deficient cells to various biochemical pathways of cell metabolism, have strongly been corroborated by the results of the enrichment pathway analysis (Fig. 6). Indeed, these results highlighted the alignment of our metabolic observations with the potential disruptions of biochemical pathways involved in amino sugar metabolism, galactose metabolism, glucuronic acid metabolism, purines and pyrimidines metabolism, energy production, fructose and mannose metabolism, glutathione metabolism, thus clearly suggesting a complex metabolic derangement occurring to cell metabolism of PMM2-CDG patients. It is highly presumable that both the extent and the consequences of these alterations may significantly vary when considering different cell lines and differentially impacting the respective cell functionality, i.e., neurons may be differently affected from hepatocytes. With this in mind, it would be possible to explain why cells of brain organoids, having modest basal glycogen biosynthetic rate37, seem to have decreased glycogen content11whilst hepatocytes are prone to increase glycogen production10. On the other hand, it is not surprising that different cell lines have differential metabolic adaptations under the same pathological condition.
In order to provide new information on the complex metabolic changes in patients carrying mutations on the PMM2 gene, one of our purposes was to quantify FAA in the PBMCs’ protein-free extracts of healthy controls and PMM2-CDG patients. A previous study, carried out in samples of skin fibroblasts, reported a general increase in FAA in PMM2-CDG patients, with the exception of Glu and Trp that showed significant decrease compared to the concentrations detected in controls16. Authors attributed this phenomenon to an increased rate of proteasomal-mediated protein degradation, producing increased release of FAA within cells. In our study, we found no increase in any FAA measured in patients’ PBMCs. Conversely, we found significant depletion in Asn, Gln, Ser, Thr, His, Trp and Arg. The significant 50% decrease of Gln is noteworthy when considering its distinctive biochemical function in PBMCs. Gln intervenes in several aspects of white blood cell metabolism, particularly serving as the primary energy source for lymphocytes during periods of significant energy demand38,39,40. Additionally, lymphocytes convert Gln into α-ketoglutarate (glutaminolytic process) which is subsequently used to fuel the Krebs’ cycle41, whereas pyruvate, the principal actor in oxidative metabolism, is split for a bimodal use to generate both lactate and acetyl-CoA.
Particularly in PMBCs, but also in different rapidly dividing cells, Gln is a crucial substrate for energy metabolism. Its carbon skeleton and additional amino-group provide precursors for the biosynthesis not only of macromolecules, but also of nucleotides (purines, pyrimidines, and amino sugars), NADPH, antioxidants (GSH via glutamate synthesis), and many other compounds involved in the maintenance of cellular integrity and functions42. Although the reason of Gln deficiency remains unclear, it may represent a key factor to explain the general metabolic imbalance recorded in PBMCs of PMM2 patients. In this light, it should also be underlined that the low Gln levels may give a significant contribution to the immunological alterations of PMM2-deficient patients, synergistically acting with the established glycan deficiencies43.
According to our results, it is conceivable to suggest an imbalance, previously unreported in the literature, between the glycolytic and glutaminolytic axes in PBMCs from PMM2-CDG patients. Gln is also the co-substrate of glutamine:fructose-6-phosphate amidotransferase (GFAT), the key enzyme involved in UDP-GlcNac biosynthesis. It also worth mentioning that the 50% decrease in Gln found in patients’ PBMCs was not mirrored by decreased UDP-GlcNac levels. We hypothesize that the salvage pathway of UDP-GlcNac44 actively transforms part of UDP-Glc and UDP-Gal in such an amount to maintain UDP-GlcNac concentrations within a normal range, thus ensuring adequate levels of this UDP-derivative to allow functionality of protein O-glycosylation. It should also be emphasized that decrease in PBMCs Gln may also mirror metabolic dysfunctions occurring to various organs (liver, skeletal muscle, intestine) with which Gln has an active interflow. This possibility reinforces the relevance of using PBMCs as a cell model to study biochemical/metabolic changes in PMM2 deficiemcy.
It is our opinion that even the decreased availability of Ser and Thr may give significant contributions to the general energy imbalance of PBMCs in PMM2-CDG patients, because of their well-known role as gluconeogenetic amino acids. In different experimental conditions, it has been observed that decreased concentrations of Ser and Thr is detrimental for cell metabolism and contribute to energy imbalance under stressing conditions45. Additionally, Ser, Thr46and also His47are involved in the turnover of tretrahydrofolate (THF) which is essential to maintain adequate NADPH concentrations48. Therefore, the decrease in these three amino acids may contribute to the decreased concentrations of GSH measured in PBMCs of PMM2-CDG patients. Even the diminution of Trp may indirectly contribute to the GSH depletion in PBMCs of PMM2-CDG patients, in light of its role in the biosynthesis of niacin, essential to ensure correct concentrations of the nicotinic coenzyme pool. The decreased Arg concentrations caused a significant reduction in the Global Arginine Bioavailability Ratio (GABR), that is obtained by the ratio Arg/Citr + Orn. This index is directly connected to the production of nitric oxide: the higher is the value of the ratio, the lower is the quote of Arg consumed by nitric oxide synthases for NO generation49. In our cohort of PMM2-CDG patients, we found increase in the stable end-products of NO metabolism (nitrite + nitrate) and concomitant decrease in the value of GABR, strongly suggesting that PMM2-deficient PBMCs utilise Arg to form NO, via nitric oxide synthase activity.
Although PBMCs were found feasible for detecting several metabolic changes, also concurring with those observed in fibroblasts17,18,19, it should be underlined that PBMCs might not fully reflect the metabolic changes occurring in other tissues involved in PMM2-CDG, because of the peculiar metabolic characteristics and protein glycosylation needs of each specific cell line. However, it is worth underlining that these cellular peculiarities may limit any cell-based study and should be token into considerations when extrapolating the results to cell lines other than those used in the study. Lastly, we are aware that this study was performed in a limited number of patients and this may have implications when considering potential contributors to cellular metabolism such as age, gender and PMM2-mutation types.
Conclusions
Although carried out in a limited number of subjects, we here demonstrated a complex metabolic derangement in PBMCs from PMM2-CDG patients by dosing several substrates implicated in different pathways at the crossroad between glycosylation and energy metabolism, using a model to assess cell metabolism closer to the in vivo conditions than the experimental models using cultured cells from PMM2-CDG patients. This may unravel further pathobiological mechanisms of PMM2-CDG and may become relevant to monitor the effects of therapeutic approaches acting to restore metabolic disarrangement in PMM2-CDG or to replenish substrate availability for GDP-mannose synthesis50. The use of PBMCs may be useful to monitoring the effects of in vivo therapeutic approaches, including dietary interventions. Future efforts should be made to better characterize how metabolic alterations of PBMCs might contribute to immunological dysfunctions of PMM2-CDG patients. It is worth underlining that our results probably supplied the biochemical explanation of the recent evidence of glycogen homeostasis imbalance in the liver of PMM2-CDG. The interconnection of several metabolic pathways should certainly be deepened to define changes occurring to organ and tissue metabolisms, as well as to focalize potential targets for possible pharmacological interventions. In this light, due to its crucial role as a substrate for both energetic and biosynthetic purposes, it should be worth evaluating whether supplementation of Gln may ameliorate cell metabolism and immunological functions of PMM2-deficient patients.
Materials and methods
Patients’ recruitment
Seven patients from four unrelated families, with proven molecular diagnosis of PMM2-CDG, were recruited at the Department of Clinical and Experimental Medicine, Child Neurology and Psychiatry Section, University of Catania, Italy. They included 6 males and one female, with age ranging between 20 and 51 years. Blood samples and clinical information were obtained as part of the routine clinical protocol of patients with PMM2-CDG. Written informed consent was obtained from all participants and/or their relatives for enrolment in this study. The overall study on PMM2-CDG was approved by the ethic committee of the “Policlinico” Hospital of the University of Catania (approval n° 221/2020).
Isolation of PBMC population from whole blood
Human PBMCs were obtained at the Division of Hematology, AOU Policlinico – OVE, University of Catania from both healthy controls (n = 10) and PMM2-CDG patients (n = 7). After giving the informed consent, controls and PMM2-CDG patients underwent a peripheral blood withdrawal from the antecubital vein, at morning after nocturnal fasting. Briefly, blood was diluted with an equal volume of phosphate-buffered saline, pH 7.4 (PBS), layered over the Ficoll-Paque medium (Sigma-Aldrich) and centrifuged at 400 × g for 30 min, at room temperature. The PBMCs interface was carefully removed, supplemented with PBS-EDTA and centrifuged at 250 × g for 10 min. PBMCs’ pellet was subjected to hypotonic lysis (155 mM NH4Cl, 10 mM KHCO3, 0.1 mM EDTA, pH 7.4) for 10 min at room temperature with gentle mixing, to lyse contaminating red blood cells (RBC). This step was followed by a last wash with PBS-EDTA. Cell number and viability were determined using Macs Quant Analyzer 10 (Miltenyi Biotec).
Sample processing for metabolite analysis
All standards used for characterization of PBMCs’ metabolic profile, the ion coupling reagent tetrabutylammonium hydroxide, potassium dihydrogen phosphate, sodium monohydrogen phosphate, sodium acetate for buffers preparation were purchased from Sigma-Aldrich (St. Louis, MO, USA) at the highest purity available. HPLC-grade solvents (methanol, acetonitrile, chloroform, trifluoroacetic acid and tetrahydrofuran) used for sample processing and buffer preparation were obtained from J.T. Baker Inc. (Phillipsburgh, NJ, USA).
Immediately after isolation, PBMCs were washed twice with ice-cold PBS and centrifuged at low speed (1860 x g) for 5 min at 4 °C. After the last washing, cell pellets were deproteinized by adding 1 ml of an ice-cold deproteinizing solution composed of CH3CN + 10 mM KH2PO4 (3:1; v: v), pH 7.40. As described elsewhere51, this procedure allows to get protein-free samples with a high recovery of hydrophilic low molecular weight compounds, with no loss of labile substances (acid sensitive and oxidizable). After vortexing for 60 s, samples underwent a high-speed centrifugation at 20,690 x g for 10 min at 4 °C. Supernatants were supplemented with large volumes of chloroform (three times the sample volume) to remove the organic solvent, centrifuged again as indicated above, and the upper aqueous phases were withdrawn and saved at −80 °C until analyzed by HPLC.
The processing method is suitable to chromatographically separate several low molecular weight metabolites including those connected to glycosylation, energy metabolism, markers of nitrosative stress, antioxidants, and the pool of FAA.
HPLC analysis of energy metabolism, UDP-derivatives and amino acids
The ThermoFisher Scientific HPLC apparatus consisted of a quaternary pump system (SpectraSystem P4000) coupled to a highly-sensitive diode array detector (UV6000LP, ThermoFisher Scientific, Rodano, Milan, Italy), equipped with 5 cm light path flow cell and set up between 200 and 350 nm wavelength. Data acquisition and analysis were performed by a PC using the ChromQuest® software package, version 5.01, provided by the HPLC manufacturer.
Separation and quantification of energy metabolites and UDP-derivatives were carried out on 100 µl of deproteinized PBMCs’ extracts using a Hypersil C-18, 250 × 4.6 mm, 5 μm particle size column, (ThermoFisher Scientific, Rodano, Milan, Italy), by applying an ion-pairing chromatographic method set up in our laboratory and described in detail elsewhere52. The method allows the simultaneous quantification of high energy phosphates (ATP, GTP, UTP, CTP, ADP, GDP, UDP, CDP, AMP, GMP, UMP, CMP, IMP), products of ATP catabolism (uric acid and xanthine), compounds related to cell energy content (acetyl-CoA), oxidized and reduced nicotinic coenzymes (NAD+, NADH, NADP+ and NADPH), protein glycosylation-related compounds (UDP-Glc, UDP-Gal, UDP-GlcNac, UDP-GalNac, GDP-man, UDP-Glucuronic), antioxidants (ascorbic acid and GSH) nitric oxide metabolites (nitrite and nitrate) in any biological sample, including PBMCs extracts. Identification and quantification of intracellular compounds were carried out at 260 nm wavelength, excluding GSH, nitrite and nitrate (206 nm wavelength), as well as NADH and NADPH (340 nm wavelength), by comparing peak areas and absorption spectra of unknown samples with those of runs of ultrapure standard mixtures with known concentrations.
The simultaneous determination of free amino acids (aspartate Asp, glutamate Glu, asparagine Asn, serine Ser, glutamine Gln, histidine His, glycine Gly, threonine Thr, citrulline Citr, arginine Arg, alanine Ala, tyrosine Tyr, valine Val, methionine Met, tryptophan Trp, phenylalanine Phe, isoleucine Ile, leucine Leu, ornithine Orn, lysine Lys), was performed using a pre-column derivatization of the sample with a mixture of ortophtalaldehyde (OPA) and 3-methylpropionic acid (MPA) in alkaline buffer (boric acid, pH 9.8)53. The chromatographic run was conducted on 25 µl sample, using the same column described above, under reversed phase chromatographic conditions and applying a proper step gradient formed with two buffers having the following composition: mobile phase A = 24 mmol/L CH3COONa + 24 mmol/L Na2HPO4 + 1% tetrahydrofuran + 0.1% trifluoroacetic acid, pH 6.5; mobile phase B = 40% CH3OH + 30% CH3CN + 30% H2O53.
Statistical analysis
Data are shown as mean ± standard deviation. GraphPad Prism program was performed for statistical analysis (GraphPad Software, release 8.01, San Diego, CA, USA). Differences between controls and PMM2-CDG patients, for each of the parameters under evaluation, were determined by the two-tailed, Student’s t-test for unpaired samples. Pearson’s coefficients were calculated to verify correlations between parameters under study in PMM2-CDG patients. Values of p< 0.05 were regarded as statistically significant. Targeted metabolomic data were analyzed using the MetaboAnalyst 6.0 platform, specifically focusing on the enrichment analysis module. Initially, raw metabolomic data of the actual concentrations of the different metabolites, underwent quality control, normalization, and transformation within MetaboAnalyst. This preprocessing included filtering out metabolites with significant missing values and applying log transformation to stabilize variance. For enrichment analysis, the “Pathway Analysis” tool, within the enrichment analysis module, was employed to identify significantly impacted metabolic pathways. This tool combines pathway topology analysis with quantitative enrichment analysis, providing comprehensive insights into the biological context of observed metabolomic changes. The analysis was performed using default parameters unless otherwise specified. Pathways with values of p < 0.05 were considered significantly enriched, indicating potential areas of metabolic perturbation associated with the experimental conditions54,55.
Data availability
Data are provided within the manuscript, supplementary information files and are available from the corresponding authors.
Abbreviations
- CDG:
-
Congenital disorders of glycosylation
- Citr:
-
Citrulline
- ER:
-
Endoplasmic reticulum
- ETC:
-
Electron transport chain
- FAA:
-
Free amino acids
- GABR:
-
Global Arginine Bioavailability Ratio
- GALE:
-
UDP-glucose 4-epimerase
- GFAT:
-
Glutamine:fructose-6-phosphate aminotransferase
- GMPPB:
-
GDP-mannose pyrophosphorylase B
- GPI:
-
Glucose-phosphate isomerase
- GSH:
-
Reduced glutathione
- HBP:
-
Hexosamine biosynthetic pathway
- MPA:
-
3-methylpropionic acid
- MPI:
-
Mannose-phosphate isomerase
- OGA:
-
O-GlcNAc-hydrolase
- OGT:
-
O-GlcNAc-transferase
- OPA:
-
Ortophtalaldehyde
- Orn:
-
Ornithine
- OST:
-
Oligosaccharide specific transferases
- PBMCs:
-
Peripheral blood mononucleated cells
- PGM:
-
Phospho-glucose mutase
- PMM2:
-
Phosphomannomutase-2
- RNS:
-
Reactive nitrogen species
- ROS:
-
Reactive oxygen species
- UDP-Gal:
-
UDP-galactose
- UDP-Glc:
-
UDP-glucose
- UDP-GalNac:
-
UDP-N-acetyl-D-galactosamine
- UDP-GlcNAc:
-
UDP-N-acetyl-D-glucosamine
- UDP-Glucuronic:
-
UDP-Glucuronic acid
- UGP2:
-
UDP-Glucose pyrophosphorylase 2
References
Schachter, H. & Freeze, H. H. Glycosylation diseases: quo vadis? Biochim. Biophys. Acta. 1792, 925–930. https://doi.org/10.1016/j.bbadis.2008.11.002 (2009).
Peanne, R. et al. Congenital disorders of glycosylation (CDG): quo vadis? Eur. J. Med. Genet. 61, 643–663. https://doi.org/10.1016/j.ejmg.2017.10.012 (2018).
Freeze, H. H., Jaeken, J. & Matthijs, G. CDG or not CDG. J. Inherit- Metab. Dis. 45, 383–385. https://doi.org/10.1002/jimd.12498 (2022).
Ondruskova, N., Cechova, A., Hansikova, H., Honzik, T. & Jaeken, J. Congenital disorders of glycosylation: still hot in 2020. Biochim. Biophys. Acta Gen. Subj. 1865, 129751. https://doi.org/10.1016/j.bbagen.2020.129751 (2021).
Mohorko, E., Glockshuber, R. & Aebi, M. Oligosaccharyltransferase: the central enzyme of N-linked protein glycosylation. J. Inherit. Metab. Dis. 34, 869–878. https://doi.org/10.1007/s10545-011-9337-1 (2011).
Izquierdo-Serra, M. et al. Stroke-Like episodes and cerebellar syndrome in phosphomannomutase deficiency (PMM2-CDG): evidence for Hypoglycosylation-Driven channelopathy. Int. J. Mol. Sci. 19, 619. https://doi.org/10.3390/ijms19020619 (2018).
Barone, R., Fiumara, A. & Jaeken, J. Congenital disorders of glycosylation with emphasis on cerebellar involvement. Semin Neurol. 34, 357–366. https://doi.org/10.1055/s-0034-1387197 (2014).
Muthusamy, K. et al. Neurological manifestations in PMM2-congenital disorders of glycosylation (PMM2-CDG): insights into clinico-radiological characteristics, recommendations for follow-up, and future directions. Genet. Med. 26, 101027. https://doi.org/10.1016/j.gim.2023.101027 (2023).
Monin, M. L. et al. 29 French adult patients with PMM2-congenital disorder of glycosylation: outcome of the classical pediatric phenotype and depiction of a late-onset phenotype. Orphanet J. Rare Dis. 9, 207. https://doi.org/10.1186/s13023-014-0207-4 (2014).
Lipinski, P. et al. Congenital disorders of glycosylation in children - Histopathological and ultrastructural changes in the liver. Pediatr. Neonatol. 62, 278–283. https://doi.org/10.1016/j.pedneo.2021.01.017 (2021).
Radenkovic, S. et al. Neural and metabolic dysregulation in PMM2-deficient human in vitro neural models. Cell. Rep. 43, 113883. https://doi.org/10.1016/j.celrep.2024.113883 (2024).
Sturiale, L., Barone, R. & Garozzo, D. The impact of mass spectrometry in the diagnosis of congenital disorders of glycosylation. J. Inherit. Metab. Dis. 34, 891–899. https://doi.org/10.1007/s10545-011-9306-8 (2011).
Guillard, M. et al. Plasma N-glycan profiling by mass spectrometry for congenital disorders of glycosylation type II. Clin. Chem. 57, 593–602. https://doi.org/10.1373/clinchem.2010.153635 (2011).
Wada, Y. Matrix-Assisted laser desorption/ionization mass spectrometry to detect diagnostic glycopeptide markers of congenital disorders of glycosylation. Mass. Spectrom. (Tokyo). 9, A0084. https://doi.org/10.5702/massspectrometry.A0084 (2020).
Raynor, A. et al. Hide and seek: misleading transferrin variants in PMM2-CDG complicate diagnostics. Proteom. Clin. Appl. 24, e2300040. https://doi.org/10.1002/prca.202300040 (2023).
Himmelreich, N. et al. Complex metabolic disharmony in PMM2-CDG paves the way to new therapeutic approaches. Mol. Genet. Metab. 139, 107610. https://doi.org/10.1016/j.ymgme.2023.107610 (2023).
Ligezka, A. N. et al. Interplay of impaired cellular bioenergetics and autophagy in PMM2-CDG. Genes (Basel). 14, 1585. https://doi.org/10.3390/genes14081585 (2023).
Zdrazilova, L. et al. Metabolic adaptation of human skin fibroblasts to ER stress caused by glycosylation defect in PMM2-CDG. Mol. Genet. Metab. 139, 107629. https://doi.org/10.1016/j.ymgme.2023.107629 (2023).
Ligezka, A. N. et al. Sorbitol is a severity biomarker for PMM2-CDG with therapeutic implications. Ann. Neurol. 90, 887–900. https://doi.org/10.1002/ana.26245 (2021).
Radenkovic, S. et al. Tracer metabolomics reveals the role of aldose reductase in glycosylation. Cell. Rep. Med. 4, 101056. https://doi.org/10.1016/j.xcrm.2023.101056 (2023).
Yuste-Checa, P. et al. The effects of PMM2-CDG-Causing mutations on the folding, activity, and stability of the PMM2 protein. Hum. Mutat. 36, 851–860. https://doi.org/10.1002/humu.22817 (2015).
Barone, R. et al. A nationwide survey of PMM2-CDG in Italy: high frequency of a mild neurological variant associated with the L32R mutation. J. Neurol. 262, 154–164. https://doi.org/10.1007/s00415-014-7549-7 (2015).
Sharma, V. & Freeze, H. H. Mannose efflux from the cells: a potential source of mannose in blood. J. Biol. Chem. 286, 10193–10200. https://doi.org/10.1074/jbc.M110.194241 (2011).
Sharma, V. et al. Phosphomannose isomerase inhibitors improve N-glycosylation in selected phosphomannomutase-deficient fibroblasts. J. Biol. Chem. 286, 39431–39438. https://doi.org/10.1074/jbc.M111.285502 (2011).
Starosta, R. T. et al. Liver manifestations in a cohort of 39 patients with congenital disorders of glycosylation: pin-pointing the characteristics of liver injury and proposing recommendations for follow-up. Orphanet J. Rare Dis. 16, 20. https://doi.org/10.1186/s13023-020-01630-2 (2021).
Tegtmeyer, L. C. et al. Multiple phenotypes in phosphoglucomutase 1 deficiency. N Engl. J. Med. 370, 533–542. https://doi.org/10.1056/NEJMoa1206605 (2014).
Sobral, D., Francisco, R., Duro, L., Videira, P. A. & Grosso, A. R. Concerted regulation of glycosylation factors sustains tissue identity and function. Biomedicines 10, 1805. https://doi.org/10.3390/biomedicines10081805 (2022).
Lazzarino, G. et al. Pyruvate dehydrogenase and Tricarboxylic acid cycle enzymes are sensitive targets of traumatic brain injury induced metabolic derangement. Int. J. Mol. Sci. 20, 5774. https://doi.org/10.3390/ijms20225774 (2019).
De Falco, P. et al. Hindering NAT8L expression in hepatocellular carcinoma increases cytosolic aspartate delivery that fosters Pentose phosphate pathway and purine biosynthesis promoting cell proliferation. Redox Biol. 59, 102585. https://doi.org/10.1016/j.redox.2022.102585 (2023).
Nanni, S. et al. Metabolic reprogramming by Malat1 depletion in prostate Cancer. Cancers (Basel). 13, 15. https://doi.org/10.3390/cancers13010015 (2020).
Zdrazilova, L. et al. Metabolic adaptation of human skin fibroblasts to ER stress caused by glycosylation defect in PMM2-CDG. Mol. Genet. Metab. 139, 107629. https://doi.org/10.1016/j.ymgme.2023 (2023).
Wang, Y., Li, Y., He, C., Gou, B. & Song, M. Mitochondrial regulation of cardiac aging. Biochim. Biophys. Acta Mol. Basis Dis. 1865, 1853–1864. https://doi.org/10.1016/j.bbadis.2018.12.008 (2019).
Steinert, J. R. & Amal, H. The contribution of an imbalanced redox signalling to neurological and neurodegenerative conditions. Free Radic Biol. Med. 194, 71–83. https://doi.org/10.1016/j.freeradbiomed.2022.11.035 (2023).
Chen, C. L., Zhang, L., Jin, Z., Kasumov, T. & Chen, Y. R. Mitochondrial redox regulation and myocardial ischemia-reperfusion injury. Am. J. Physiol. Cell. Physiol. 322, C12–C23. https://doi.org/10.1152/ajpcell.00131.2021 (2022).
Vrettou, S. & Wirth, B. S. -Glutathionylation and S-Nitrosylation in mitochondria: focus on homeostasis and neurodegenerative diseases. Int. J. Mol. Sci. 23, 15849. https://doi.org/10.3390/ijms232415849 (2022).
Buelna-Chontal, M., García-Niño, W. R., Silva-Palacios, A., Enríquez-Cortina, C. & Zazueta, C. Implications of oxidative and nitrosative Post-Translational modifications in therapeutic strategies against reperfusion damage. Antioxid. (Basel). 10, 749. https://doi.org/10.3390/antiox10050749 (2021).
Markussen, K. H. et al. The multifaceted roles of the brain glycogen. J. Neurochem. 168, 728–743. https://doi.org/10.1111/jnc.15926 (2024).
Curi, R., Newsholme, P. & Newsholme, E. A. Intracellular distribution of some enzymes of the glutamine utilisation pathway in rat lymphocytes. Biochem. Biophys. Res. Commun. 138, 318–322. https://doi.org/10.1016/0006-291x(86)90282-2 (1986).
Newsholme, E. A., Newsholme, P. & Curi, R. The role of the citric acid cycle in cells of the immune system and its importance in sepsis, trauma and burns. Biochem. Soc. Symp. 54, 145–162. (1987).
Mills, E. L. & Kelly, B. O’Neill, L. A. J. Mitochondria are the powerhouses of immunity. Nat. Immunol. 18, 488–498. https://doi.org/10.1038/ni.3704 (2017).
Araujo, L., Khim, P., Mkhikian, H., Mortales, C. L. & Demetriou, M. Glycolysis and Glutaminolysis cooperatively control T cell function by limiting metabolite supply to N-glycosylation. Elife 6, e21330. https://doi.org/10.7554/eLife.21330 (2017).
Wu, G. Amino acids: metabolism, functions, and nutrition. Amino Acids. 37, 1–17. https://doi.org/10.1007/s00726-009-0269-0 (2009).
Francisco, R. et al. New Insights into Immunological Involvement in Congenital Disorders of Glycosylation (CDG) from a People-Centric Approach. J. Clin. Med. 9, (2092). https://doi.org/10.3390/jcm9072092. (2020).
Nagel, A. K. & Ball, L. E. Intracellular protein O-GlcNAc modification integrates nutrient status with transcriptional and metabolic regulation. Adv. Cancer Res. 126, 137–166. https://doi.org/10.1016/bs.acr.2014.12.003 (2015).
Pan, S., Fan, M., Liu, Z., Li, X. & Wang, H. Serine, glycine and one-carbon metabolism in cancer. Int. J. Oncol. 58, 158–170. https://doi.org/10.3892/ijo.2020.5158 (2021).
Holecek, M. Histidine in health and disease: metabolism, physiological importance, and use as a supplement. Nutrients 12, 848. https://doi.org/10.3390/nu12030848 (2020).
Hennequart, M. et al. ALDH1L2 regulation of formate, formyl-methionine, and ROS controls cancer cell migration and metastasis. Cell. Rep. 42, 112562. https://doi.org/10.1016/j.celrep.2023.112562 (2023).
Chandrasekharan, U. M. et al. Elevated levels of plasma symmetric dimethylarginine and increased arginase activity as potential indicators of cardiovascular comorbidity in rheumatoid arthritis. Arthritis Res. Ther. 20, 123. https://doi.org/10.1186/s13075-018-1616-x (2018).
Budhraja, R. et al. Liposome-encapsulated mannose-1-phosphate therapy improves global N-glycosylation in different congenital disorders of glycosylation. Mol. Genet. Metab. 142, 108487. https://doi.org/10.1016/j.ymgme.2024.108487 (2024).
Giallongo, C. et al. Myeloid derived suppressor cells (MDSCs) are increased and exert immunosuppressive activity together with polymorphonuclear leukocytes (PMNs) in chronic myeloid leukemia patients. PLoS One. 9, e101848. https://doi.org/10.1371/journal.pone.0101848 (2014).
Lazzarino, G. et al. Single-sample Preparation for simultaneous cellular redox and energy state determination. Anal. Biochem. 322, 51–59. https://doi.org/10.1016/j.ab.2003.07.013 (2003).
Tavazzi, B. et al. Simultaneous high performance liquid chromatographic separation of purines, pyrimidines, N-acetylated amino acids, and Dicarboxylic acids for the chemical diagnosis of inborn errors of metabolism. Clin. Biochem. 38, 997–1008. https://doi.org/10.1016/j.clinbiochem.2005.08.002 (2005).
Amorini, A. M. et al. Severity of experimental traumatic brain injury modulates changes in concentrations of cerebral free amino acids. J. Cell. Mol. Med. 21, 530–542. https://doi.org/10.1111/jcmm.12998 (2017).
Xia, J., Psychogios, N., Young, N. & Wishart, D. S. MetaboAnalyst: a web server for metabolomic data analysis and interpretation. Nucleic Acids Res. https://doi.org/10.1093/nar/gkp356 (2009). 37(Web Server issue)W652-W660.
Pang, Z. et al. MetaboAnalyst 6.0: towards a unified platform for metabolomics data processing, analysis and interpretation. Nucleic Acids Res. 52 (W1). https://doi.org/10.1093/nar/gkae253 (2024). W398-W406.
Funding
The authors declare that no funds, grants, or other support were received to accomplish this study.
Author information
Authors and Affiliations
Contributions
Author contributions: Study conception and design: A.M.A., R.M., Gia.L. and R.B. Data curation; L.C., M.W.S., F.P., D.T., Giu.L., G.T. and A.B. Formal analysis R.M., L.C., M.W.S., F.P., A.D. S.A.L. and E.L.S; Investigation: Giu.L., G.L.V., L.L., A.P., C.G., V.D.P., A.G., and B.T. Methodology: R.M., L.C., M.W.S., A.G., B.T., and A.M.A. Software: G.L.V., L.L., A.P., C.G., V.D.P., D.T., G.T. and Giu.L. Supervision: A.M.A., Gia.L. and R.B. Validation: A.B., A.D., F.P., E.L.S., A.P., C.G., A.G. and D.T. Writing - original draft: A.M.A., Gia.L. and R.B. All authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The study was conducted within a protocol approved by the CT1 Polyclinic Local Ethics Committee entitled: “Clinical evaluation in Phosphomannomutase deficiency” (approval number 221/2020), and written informed consent was obtained from all patients, according to the Declaration of Helsinki.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Mangione, R., Cirnigliaro, L., Saab, M.W. et al. Targeted metabolomic evaluation of peripheral blood mononucleated cells from patients with PMM2-CDG. Sci Rep 15, 15929 (2025). https://doi.org/10.1038/s41598-025-98846-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-98846-8