Abstract
The association of long COVID with health-related quality-of-life (HrQOL) has not been well-characterized. Participants who received blinded placebo in the ACTIV-2/A5401 outpatient COVID-19 treatment trial were included in an analysis of the association of long COVID with HrQOL (both pre-specified exploratory trial endpoints) 9 months after acute COVID-19. Long COVID was defined as presence of self-assessed COVID-19 symptoms and HrQOL was assessed with EQ-5D-5L and SF-36v2 questionnaires. Associations were evaluated by Fisher’s exact tests and Wilcoxon rank-sum tests. Of 546 participants, 13% had long COVID. Long COVID was associated with greater risk of reported problems in the EQ-5D-5L dimensions of mobility, usual activities, pain/discomfort, and anxiety/depression (risk ratios 3.45–6.00, all p < 0.001) and worse self-reported health scores (median 80 vs. 95, p < 0.001). Participants with long COVID also had worse SF-36v2 composite physical and mental component scores (both p < 0.001) and individual SF-36 domain scores (physical functioning, physical role, bodily pain, general health, vitality, social functioning, emotional role, and mental health; all p < 0.001). Associations were similar regardless of baseline (pre-COVID-19) medical history. Long COVID is associated with impaired HrQOL across multiple domains, highlighting the need to develop preventative and therapeutic interventions for this protean condition.
Similar content being viewed by others
Introduction
Long COVID is a condition involving a variety of potentially debilitating, multi-systemic symptoms following acute infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)1. Estimates of the frequency of long COVID vary across studies, with an estimated incidence of 10–35% among non-hospitalized individuals2. Clinical manifestations of long COVID span multiple organ systems, including the respiratory, cardiovascular, gastrointestinal, musculoskeletal, and neurologic systems, among others1,2,3. Given the prevalence and morbidity of this condition1, a robust understanding of the impact of long COVID on quality of life is crucial.
Health-related quality of life (HrQOL) metrics provide a multi-dimensional, person-centered perspective on an individual’s physical, emotional, and social functioning and well-being, offering valuable insight into the impact of illness on individuals’ lives not captured by traditional symptom-based tools4. A number of prior studies have reported poor HrQOL outcomes among persons with long COVID; however, most of these studies focused on persons with a history of hospitalization for COVID-19, and typically lacked a comparator group of individuals with SARS-CoV-2 infection who did not develop long COVID5,6,7,8. In this study, we compared HrQOL outcomes between individuals with vs. without long COVID among people who received blinded placebo in the ACTIV-2/A5401 outpatient COVID-19 treatment trial9, providing a rigorous, prospective evaluation of the impact of long COVID on HrQOL following predominantly mild-moderate acute infection.
Methods
Study population
This study included participants who received blinded placebo in the ACTIV-2/A5401 trial, a phase 2/3 platform trial that evaluated investigational treatments for people with mild-to-moderate COVID-19 (NCT04518410)9. Individuals eligible for inclusion in ACTIV-2/A5401 were non-hospitalized adults (≥ 18 years) who had a positive COVID-19 antigen or nucleic acid test within 10 days prior to study entry, no more than 10 days of COVID-19 symptoms at study entry, ongoing COVID-19 symptoms within one day prior to study entry, and resting peripheral oxygen saturation levels ≥ 92%, as previously described9,10. The trial was approved centrally for US sites by the institutional review board (IRB) Advarra (Pro00452666), with approval by additional local IRBs as required and local Ethics Committees for sites outside the US. All research was conducted in accordance with relevant guidelines and regulations, and in accordance with the Declaration of Helsinki. Written informed consent was obtained from all participants.
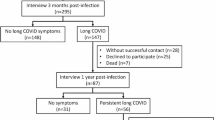
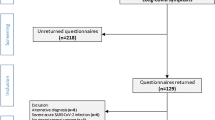
Among participants who received blinded placebo, the study population was further restricted to those who had both available study week 36 EQ-5D-5L or SF-36v2 questionnaire data and available week 36 symptom diary data. Supplementary Fig. 1 depicts a flow diagram defining the study population.
Participant-completed symptom diaries
Participants completed a long-term symptom diary (see Supplementary Appendix 1) at 36 weeks after study entry, as previously described11,12. The long-term diary included three global assessment questions, all completed by participant self-report. The first evaluated overall severity of COVID-19 symptoms over the previous four weeks (reported by the participant as “no symptoms,” “mild,” “moderate,” or “severe”). The second evaluated general physical health over the previous 4 weeks (reported by the participant as “excellent,” “very good,” “good,” “fair,” or “poor”). The third asked about self-assessed return to usual (pre-COVID-19) health at the time of diary completion (with options of “yes” or “no”). In addition to the three global assessment questions, participants were also asked to indicate overall severity over the previous 4 weeks of 27 individual symptoms. The 4-week assessment period in the long-term diary was selected to align with the 4-week assessment period of questions in the SF-36v2 questionnaire. The long-term diary and EQ-5D-5L and SF36-v2 questionnaires (described further below), intended to collect data on post-acute COVID-19 symptoms and functional health status, were introduced partway through the trial, and thus were only available for participants who enrolled later in the trial. All instruments (long-term diary, EQ-5D-5L, and SF36v2) were completed either on paper or electronically (Medidata eCOA platform, which linked directly to the trial Medidata Rave electronic data capture system).
Long COVID definition
Long COVID was defined as the presence of self-reported overall COVID-19 symptoms (any of mild, moderate, or severe) within the last 4 weeks at week 36, as determined by participants’ responses to the first global assessment question on the long-term symptom diary. This participant-centered definition of Long COVID has been utilized in prior ACTIV-2/A5401 analyses of post-acute COVID symptoms and is supported by published analyses supporting the internal validity of this definition11,12.
Associations of HrQOL with participant-reported non-return to health (yes versus no) at study week 36 (based on the third global assessment question in the long-term symptom diary) were explored as a supportive analysis. Previous ACTIV-2/A5401 analyses have described concordance of non-return to pre-COVID health with long COVID as defined above11,12.
Health-related quality of life questionnaires
HrQOL was assessed at study week 36 by the EQ-5D-5L (EuroQol Research Foundation, The Netherlands) and SF-36v2® Health Survey (QualityMetric, Johnson, RI, USA) questionnaires. The EQ-5D-5L13 assesses five dimensions: mobility, self-care, usual activities, pain/discomfort, and anxiety/depression. For each dimension, participants were asked to evaluate each category based on how they feel that day, choosing from five severity levels: no problems, slight problems, moderate problems, severe problems, and unable to carry out the dimension/extreme problems. The primary outcome of adverse HrQOL was defined as presence of any reported problems in each dimension (any of slight, moderate, severe, or unable to/extreme), vs. no problems. Additionally, participants were asked to rate their health that day on a vertical visual analog scale (VAS) from 0 (“worst health you can imagine”) to 100 (“best health you can imagine”).
The SF-36v214 consists of questions covering eight health domains: physical functioning, role-physical (i.e. physical health-related role limitations), bodily pain, general health, vitality (i.e. energy level and fatigue), social functioning, mental health, and role-emotional (i.e. mental health-related role limitations). Each of these domains is scored by the participant from 0 to 100, with higher scores indicating better health. Additionally, the health domain scales are used to derive two aggregate component summary measures, physical component summary and mental component summary, which are both normalized metrics with a mean score of 50 and a standard deviation of 10, with higher scores again indicating better health.
Baseline medical history categories
To explore the impact of pre-existing medical conditions at the time of SARS-CoV-2 infection on long COVID and HrQOL, baseline medical comorbidity subgroups were defined based on the presence or absence of medical conditions reported at study entry (Supplementary Table 1). Medical history events (identified by MedDRA preferred term15) were considered if their start date was prior to COVID-19 diagnosis and if they were ongoing at the time of study entry. Additionally, a select number of clinician-selected historical events with resolution dates prior to study entry (denoted with asterisks in Supplementary Table 1) were included as the events, such as acute coronary syndrome, were expected to reflect ongoing underlying disease at the time of study entry. Relevant baseline medical history events were classified into six broad subgroups (selected based on clinical relevance to Long COVID1): cardiac and vascular disorders, gastrointestinal disorders, musculoskeletal and connective tissue disorders, neurologic disorders, psychiatric disorders, and pulmonary disorders.
Statistical analyses
Modified Poisson regression models and Fisher’s exact tests were used to compare the frequency of any reported problems in each of the five EQ-5D-5L dimensions between participants with vs. without long COVID, as well as between participants who had vs. had not returned to pre-COVID health. Wilcoxon rank-sum tests compared scores on the EQ-5D-5L visual analog scale, SF-36v2 health domains, and SF-36v2 physical and mental component summary measures between participants with vs. without long COVID and participants who had vs. had not returned to pre-COVID health. Each analysis was performed in the overall population as well as in baseline medical history subgroups defined by presence or absence of selected medical comorbidities at baseline (described above). Tests for interaction of baseline medical comorbidities with long COVID on risk of EQ-5D-5L and SF-36v2 outcomes were also assessed with binary regression models. All P values are two-sided and confidence intervals are at the 95% level; statistical significance was set at P < 0.05. As all analyses were exploratory, adjustments for multiple comparisons were not performed. Analyses were conducted using SAS version 9.4 (SAS Institute, Cary, North Carolina).
Results
Study population
The analysis population included 546 participants who received blinded placebo treatment and were enrolled January – August 2021, who had both symptom diary data and EQ-5D-5L or SF-36v2 questionnaire data available at week 36 (Supplementary Fig. 1). Median age was 45 years, 53% were female, 82% were from the United States, 81% were white, 13% were Black, and 55% were Hispanic/Latino (Table 1). Median days from symptom onset to study entry was 5 days, 57% met protocol criteria for being at high-risk for COVID-19 progression, 17% were vaccinated, and 55% were anti-nucleocapsid or anti-spike antibody positive at study entry (Table 1). Of 413 participants with an identified SARS-CoV-2 variant (variant calling described previously16), 35% had Delta and 65% pre-Delta variant infection (Table 1).
Long COVID was present at week 36 (approximately 9 months after acute COVID-19) in 13% (69/546) of participants and non-return to pre-COVID overall health status in 21% (113/546) of participants. Baseline demographic and clinical variables were reasonably similar between groups with and without long-COVID, with the exception of sex and risk category for severe COVID-19, consistent with the literature on risk factors for long COVID17 (Table 1).
Association of long COVID with EQ-5D-5L measures
Participants with vs. without long COVID were more likely to report problems in EQ-5D-5L dimensions of mobility (36 vs. 7%, risk ratio (RR) [95% CI] 4.9 [3.2, 7.7]), usual activities (48 vs. 8%, RR 6.0 [4.1, 8.9]), pain/discomfort (72 vs. 18%, RR 4.0 [3.1, 5.0]), and anxiety/depression (48 vs. 14%, RR 3.5 [2.5, 4.8]), all p < 0.001 (Fig. 1). Problems in the self-care dimension were also significantly more common in individuals with long COVID, though the number of individuals reporting problems in self-care was extremely small (N = 21), and thus this dimension was not explored in further detail. Overall, the majority of reported problems (69–77%) were “slight” in severity. The distribution of severity levels for reported problems in EQ-5D-5L dimensions among patients with and without long COVID are shown in Supplementary Fig. 2. Additionally, participants with vs. without long COVID reported worse self-reported health scores on the EQ-5D-5L visual analogue scale (VAS) (median [IQR] 80 [70–85] vs. 95 [85–100], p < 0.001) (Supplementary Fig. 3A).
Association of long COVID with EQ-5D dimensions. Comparison of the percentage of reported problems in the EQ-5D dimensions (A) mobility, (B) usual activity, (C) pain / discomfort, and (D) anxiety / depression between participants with vs. without long COVID. Results are presented in the overall cohort (left-most plot in each panel), as well as in baseline medical history subgroups defined by the presence or absence of selected medical comorbidity categories at baseline (subsequent plots in each panel). P-values are based on Fisher’s exact tests, with ** signifying P < 0.001 and * signifying P < 0.05. GI gastrointestinal, CT connective tissue.
The association of long COVID with impaired EQ-5D outcomes persisted when examining associations among medical comorbidity subgroups defined by the presence vs. absence of specific baseline medical comorbidities at study entry prior to the onset of long COVID (Fig. 1 and Supplementary Fig. 3A). The impact of long COVID on risk for problems in EQ-5D-5L domains appeared greater among participants without baseline comorbidities than participants with baseline comorbidities (Supplementary Table 2). Interaction analyses summarized in Supplementary Table 2 demonstrate that in a number of instances, the presence vs. absence of a given baseline comorbidity and of long COVID modify each other’s association with problems in EQ-5D-5L domains (all comorbidities with pain/discomfort domains; musculoskeletal/connective tissue disorders with mobility and usual activity problems; pulmonary disorders with mobility problems; psychiatric disorders with usual activity problems; and cardiac/vascular disorders with anxiety/depression problems); however, these analyses do not adjust for multiple comparisons and may be limited by small numbers for some subgroups.
Self-assessed lack of return to pre-COVID health at week 36 was similarly associated with significantly worse EQ-5D-5L VAS scores (Supplementary Fig. 3B) and increased risk of reported problems in individual EQ-5D-5L dimensions (RR range 1.9–5.9; Supplementary Fig. 4), though with lower RR magnitudes compared to those for long COVID.
Association of Long COVID with SF-36v2 measures
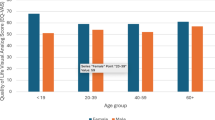
Looking at HrQOL outcomes captured by the SF-36v2 questionnaire, participants with long COVID had significantly lower (worse) SF-36v2 composite physical component scores (Fig. 2A, median (IQR) 46.8 (39.4–54.4) vs. 58.7 (56.6–59.9), p < 0.001) and composite mental component scores (Fig. 2B, median 49.0 (41.5–57.4) vs. 57.6 (51.7–60.6), p < 0.001) compared to those without long COVID. Scores were also lower for participants with long COVID in each of the individual SF-36v2 domains of general health, physical functioning, physical role, bodily pain, vitality, social functioning, emotional role, and mental health (Supplementary Fig. 5, all p < 0.001). Stratifying by presence or absence of baseline comorbidities, long COVID was associated with worse physical and mental component scores regardless of presence of specific baseline medical comorbidities (Fig. 2). Differences in physical component scores between participants with vs. without long COVID were not significant among the subgroup with baseline GI disorders, and differences in mental component scores between participants with vs. without long COVID were not significant among those with baseline neurological, GI, pulmonary, and musculoskeletal / connective tissue disorders (Fig. 2).
Association of long COVID with SF-36 physical component score and mental component score. Comparison of (A) Physical Component Scores and (B) Mental Component Scores between participants with vs. without long COVID. Results are presented in the overall cohort (left-most plot in each panel), as well as in baseline medical history subgroups defined by the presence or absence of selected medical comorbidity categories at baseline (subsequent plots in each panel). P-values are based on Wilcoxon rank-sum tests, with ** signifying P < 0.001 and * signifying P < 0.05. Abbreviations: GI: gastrointestinal, CT: connective tissue.
Self-assessed lack of return to pre-COVID health was also associated with significantly worse SF-36v2 composite physical and mental component scores (Supplementary Fig. 6) and individual SF-36v2 domain scores (Supplementary Fig. 7).
Hospitalization status and HrQOL
Among n = 557 participants who had available week 36 EQ-5D-5L or SF-36v2 data (regardless of availability of long-term symptom diary data), 44 (8%) were hospitalized prior to week 36. There was no association between hospitalization status prior to week 36 and HrQOL at week 36 by either EQ-5D-5L or SF-36v2 (with the exception of lower SF-36 physical role scores at week 36 among individuals who were hospitalized prior to week 36, p = 0.048).
Discussion
In this study, we demonstrate that long COVID is associated with impairment in HrQOL outcomes among prospectively assessed outpatients treated with blinded placebo in the ACTIV-2/A5401 COVID-19 treatment trial during the Delta and pre-Delta waves of infection. The detrimental effect of long COVID was observed to span multiple HrQOL domains, including physical, emotional, and social dimensions, highlighting that long COVID impacts numerous facets of day-to-day functioning and well-being. We also found that most associations of long COVID with impaired HrQOL outcomes were not significantly modified by the presence of pre-existing medical conditions at the time of acute COVID-19, wherein risk of impaired HrQOL with long COVID was similar or greater in persons without baseline comorbidities.
Our results provide a rigorous evaluation of how long COVID following primarily mild-moderate acute infection influences HrQOL, strengthening evidence from prior literature documenting poor HrQOL in individuals with long COVID. A meta-analysis on long COVID and HrQOL by Malik et al. that included 12 studies predominantly encompassing previously hospitalized populations reported poor quality of life by EQ-5D-5L metrics, with pooled prevalence of problems in each EQ-5D-5L domain and pooled EQ-VAS generally similar to that observed among individuals with long COVID in our study5. The existing literature evaluating the impact of long COVID on HrQOL among outpatients following mild-moderate COVID-19 is more limited. In three cross-sectional, observational studies evaluating HrQOL among individuals with long COVID following mild-moderate COVID-197,8,18, the observed HrQOL outcomes were generally worse than those observed among participants with long COVID in our study, with lower EQ-5D-5L VAS scores (mean / median scores 51–64, as opposed to a median score of 80 in our study) and increased prevalence of problems in most EQ-5D-5L domains. This difference may be because the participants in these studies were drawn from populations seeking care at hospital-associated long COVID clinics, in the case of two of the studies, or from individuals participating in long COVID patient support groups, in the case of the third study, which may represent populations with more severe long COVID manifestations than in our study. In a small prospective cohort of individuals with non-severe COVID-19 in Sweden, individuals who had persistent symptoms > 8 weeks had a more pronounced drop in their EQ-5D-VAS from their pre-COVID levels than those without persistent symptoms19. Our findings extend on previously reported findings and corroborate the significant influence of long COVID on HrQOL in a large, prospective cohort of outpatients within a clinical trial with diversity in terms of geography, demographics, and medical history. The systematic assessment of participants who were blinded to treatment and followed from documented acute COVID-19 until a pre-specified post-acute COVID time point allowed characterization of long COVID and the spectrum of HrQOL effects in a general population with reduced bias.
There are several limitations to our study. Our study was conducted in 2021 prior to widespread vaccination or modern variants, which may limit generalizability to the present setting. The observational nature of this study also precludes establishing causality between long COVID and the observed HrQOL deficits. Additionally, both the presence of Long COVID and the HrQOL outcomes were evaluated by participant self-report. This raises the possibility of common methods bias (i.e. bias introduced when both the independent and dependent variables in an analysis are collected via the same methods, for instance the same individual providing self-reported responses), which is a common limitation in questionnaire-based research and could lead to over-estimation of the association between long COVID and HrQOL. Furthermore, we employed standard HrQOL questionnaires (EQ-5D-5L and SF-36v2), which are used widely in quality-of-life literature but not validated for COVID-19-related or long COVID-specific quality-of-life assessment. Other limitations include unmeasured confounders, the lack of pre-COVID HrQOL data for comparison, missing HrQOL questionnaires and symptom diaries, and the absence of adjustment for multiple comparisons in statistical analyses.
Ultimately, our study provides evidence for reduced HrQOL in the setting of long COVID, a finding with important implications for long COVID management considerations and research priorities. Our observation that long COVID influences various dimensions of quality-of-life, including physical, mental, and social well-being, suggests that attention should be given to each of these elements when caring for individuals with long COVID in the clinic. Additionally, the prominence of diminished HrQOL with long COVID suggests that as new therapeutic interventions for this condition are developed and evaluated, the ability of these interventions to improve HrQOL should be evaluated as a key study endpoint. Various recent studies of novel interventions for long COVID have analyzed change in HrQOL measures as study outcomes, including recent trials of outpatient pulmonary rehabilitation20, vortioxetine21, and group physical and mental rehabilitation programs22. Change in HrQOL outcomes should continue to be emphasized in future trials of long COVID therapeutic interventions. Finally, given the significant HrQOL morbidity of long COVID and the infancy of effective therapeutic options, our study underscores the crucial importance of developing effective preventative strategies for long COVID.
Data availability
Data are available under restricted access. Access to the data is governed by ACTG policy. Access can be requested by submitting a data request at https://submit.mis.s-3.net/ and will require the written agreement of ACTG. Requests will be addressed as per ACTG standard operating procedures. Completion of an ACTG Data Use Agreement may be required.
References
Davis, H. E., McCorkell, L., Vogel, J. M. & Topol, E. J. Long COVID: major findings, mechanisms and recommendations. Nat. Rev. Microbiol. 21, 133–146 (2023).
Hope, A. A. & Evering, T. H. Postacute sequelae of severe acute respiratory syndrome coronavirus 2 infection. Infect. Dis. Clin. North Am. 36, 379–395 (2022).
Groff, D. et al. Short-term and long-term rates of postacute sequelae of SARS-CoV-2 infection: A systematic review. JAMA Netw. Open 4, e2128568 (2021).
Testa, M. A. & Simonson, D. C. Assessment of quality-of-life outcomes. N Engl. J. Med. 334, 835–840 (1996).
Malik, P. et al. Post-acute COVID-19 syndrome (PCS) and health-related quality of life (HRQoL)-A systematic review and meta-analysis. J Med. Virol. 94, 253–262 (2022).
Poudel, A. N. et al. Impact of Covid-19 on health-related quality of life of patients: A structured review. PLoS ONE 16, e0259164 (2021).
Malesevic, S. et al. Impaired health-related quality of life in long-COVID syndrome after mild to moderate COVID-19. Sci. Rep. 13, 7717 (2023).
Tabacof, L. et al. Post-acute COVID-19 syndrome negatively impacts physical function, cognitive function, health-related quality of life, and participation. Am. J. Phys. Med. Rehabil. 101, 48–52 (2022).
Currier, J. S. et al. ACTIV-2: a platform trial for the evaluation of novel therapeutics for the treatment of early COVID-19 in outpatients. J. Infect. Dis. 228, S77–S82 (2023).
Chew, K. W. et al. Antiviral and clinical activity of bamlanivimab in a randomized trial of non-hospitalized adults with COVID-19. Nat. Commun. 13, 4931 (2022).
Evering, T. H. et al. Long COVID after Bamlanivimab treatment. J. Infect. Dis. 228, S126–S135 (2023).
Evering, T. H. et al. Post-acute COVID-19 outcomes including participant-reported long COVID: amubarvimab/romlusevimab versus placebo in the ACTIV-2 trial. EClinicalMedicine 75, 102787 (2024).
EuroQol Research Foundation. EQ-5D-5L User Guide, https://euroqol.org/publications/user-guides. (2019).
Maruish, M. E. E. User’s manual for the SF-36v2 Health Survey 3rd edn. (QualityMetric Incorporated, 2011).
Welcome to MedDRA. Medical Dictionary for Regulatory Activities. https://www.meddra.org.
Evering, T. H. et al. Safety and efficacy of combination SARS-CoV-2 neutralizing monoclonal antibodies Amubarvimab plus Romlusevimab in nonhospitalized patients with COVID-19. Ann. Intern. Med. 176, 658–666 (2023).
Long COVID Basics. (accessed 20 March 2025); https://www.cdc.gov/covid/long-term-effects/index.html.
Meys, R. et al. Generic and Respiratory-specific quality of life in non-hospitalized patients with COVID-19. J. Clin. Med. 9, 3993 (2020).
Lofstrom, E. et al. Health-related quality of life and long-term symptoms among patients with non-severe covid-19 - a prospective cohort study. Infect. Dis. (Lond.) 55, 272–281 (2023).
Nopp, S. et al. Outpatient pulmonary rehabilitation in patients with long COVID improves exercise capacity, functional status, dyspnea, fatigue, and quality of life. Respiration 101, 593–601 (2022).
McIntyre, R. S. et al. Vortioxetine for the treatment of post-COVID-19 condition: a randomized controlled trial. Brain 147, 849–857 (2024).
McGregor, G. et al. Clinical effectiveness of an online supervised group physical and mental health rehabilitation programme for adults with post-covid-19 condition (REGAIN study): multicentre randomised controlled trial. BMJ 384, e076506 (2024).
Acknowledgements
We thank the study participants, site staff, site investigators, and the entire ACTIV-2/A5401 study team; the ACTIV-2 Community Advisory Board; the ACTG, including Lara Hosey, Jhoanna Roa, and Nilam Patel; the University of Washington Virology Specialty Laboratory; the ACTG Laboratory Center; Frontier Science; Harvard Center for Biostatistics in AIDS Research and ACTG Statistical and Data Analysis Center, the National Institute of Allergy and Infectious Diseases/Division of AIDS; the Foundation for the National Institutes of Health and the ACTIV partnership; and the PPD clinical research business of Thermo Fisher Scientific.
Funding
This work was supported by the National Institute of Allergy and Infectious Diseases of the National Institutes of Health under Award Numbers UM1AI068636, UM1AI068634, UM1AI106701, and P30AI152501. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Consortia
Contributions
KWC, THE, CM, and MDH conceived and designed the present study. CM, JSC, JJE, ESD, DAW, WF, US, MDH, DMS, THE, and KWC were involved with parent study design and implementation. CM, JR, and MDH conducted statistical analyses. MMG, CM, JR, MDH, and KWC interpreted the data. MMG and KWC drafted the manuscript. All authors reviewed, edited, and approved the manuscript.
Corresponding authors
Ethics declarations
Competing interests
DMS has consulted for the following companies: Model Medicines and Hyundai Biosciences. The remaining authors have no conflicts of interest relevant to this publication.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Gandhi, M.M., Moser, C., Currier, J.S. et al. Association of long COVID with health-related quality-of-life outcomes. Sci Rep 16, 14229 (2026). https://doi.org/10.1038/s41598-026-36189-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-36189-8