Abstract
Over two million people are incarcerated in the United States, where they experience increased illness, injury, and barriers to medical care. Traumatic brain injury (TBI) in the incarcerated population remains underexamined, including prevalence, treatment patterns, and outcomes. We analyzed the 2021–2022 National Trauma Data Bank to identify adult patients (≥ 18 years) with TBI as defined by ICD-10 codes, and incarcerated patients were identified by injury location codes. Propensity score matching (2:1 on age, sex, and race; then with the addition of Glasgow Coma Score and Injury Severity Score) was performed to balance baseline characteristics. Subgroup analysis by TBI severity (mild, moderate, severe range) was conducted. Outcomes included hospital mortality and discharge disposition; interventions received were also recorded. Patients presenting from prison with TBI were younger, more often male, and had fewer comorbidities. They presented with distinct trauma mechanisms, specifically with more frequent assaults and less frequent motor vehicle collisions and firearm injuries. After matching, there was higher mortality among patients presenting from prison with severe TBI (30.9% vs. 25.7%, p = 0.03), corresponding with a 43% increased risk of mortality once adjusted for age, sex, race, and Injury Severity Score despite similar treatment intensity. Discharge to skilled nursing and acute rehab was significantly less frequent among survivors presenting from prison, with absolute differences of 1.7% and 5.1%, respectively (p < 0.001). These findings raise concerns about equity in care delivery and post-acute services for incarcerated individuals with TBI. Structural factors impacting discharge planning in this population warrant further investigation.
Similar content being viewed by others
Introduction
Over two million people are currently incarcerated in the United States1. The incarcerated population has an increased prevalence of medical, psychiatric, and substance use disorders relative to the non-incarcerated population, as well as an increased incidence of traumatic injury while imprisoned2. Patients experiencing incarceration have a constitutional right to healthcare delivery as ruled in Estelle vs. Gamble, a Supreme Court decision from 19733, yet a variety of barriers challenge their ability to access healthcare at the community standard.
The ramifications of these obstacles may be exacerbated in trauma, especially traumatic brain injury (TBI) where delays in care and lack of access to neurosurgical services may lead to adverse outcomes4. TBI, the consequence of blunt and penetrating force to the head resulting in intracranial bleeding and structural brain injury, exists on a spectrum of severity. Those presenting with mild injuries may experience a concussion syndrome that improves over the course of weeks to months5. In severe cases, patients may require emergent neurosurgery, prolonged intensive care stays, tracheostomy, and enteral feeding tubes; even with aggressive care, patients experience high rates of mortality, functional dependence, and disorders of consciousness that may persist for many months or years6,7. Even patients who recover functional independence experience ongoing medical morbidity8.
Among patients presenting from carceral settings to a hospital for evaluation of traumatic injuries, there are varying reports about the prevalence of TBI ranging from 1% to 30% depending on setting and study type9,10,11. In one study, evaluation and management of trauma was the most common reason for presentation to the emergency room12 and for admission13 among patients experiencing incarceration. The National Trauma Data Bank has previously been explored to describe patterns of short-term outcomes after trauma occurring at prison in a study reporting increased odds of hospital mortality compared with trauma occurring in the community after adjustment for differences in baseline characteristics14. However, there lacks description of the subgroup of patients presenting with TBI, a group with distinct clinical characteristics and disease-specific measures of illness severity and treatment intensity. In this paper, we aim to characterize the epidemiology, management, and outcomes among patients presenting from prison with TBI.
Methods
Cases of patients diagnosed with TBI were identified in the National Trauma Data Bank, a large convenience sample of cases reported by trauma centers across the United States, during years 2021 and 2022. The need to obtain ethical approval was waived by the Brown University Health Institutional Review board, and the need for consent was waived given the retrospective and anonymous nature of the study. All methods were carried out in accordance with relevant guidelines and regulations.
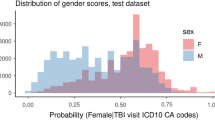
Patients presenting with TBI were identified by the ICD10 codes listed in Supplementary Table 1. Patients presenting from prison were identified by the injury location code Y92.14. Cases were included if patient age was greater than or equal to 18 years and if there was a diagnosis of TBI. Cases were excluded if missing total Glasgow Coma Score (GCS) data.
Data describing demographics, presentation, injury severity (as measured by the Injury Severity Score (ISS)), hospital characteristics, hospital events, and hospital outcomes were collected. ISS is a total body injury severity measure ranging from 0 to 75 and calculated by summing the squares of the Abbreviated Injury Scale (AIS) of the three most injured body regions. Comorbidities are documented in the database as present or absent; the list includes a total number of comorbidities calculated for each patient. The list of comorbidities included is provided in the Supplementary Methods. Craniotomy was identified by procedure codes listed in Supplementary Tables 1, and intracranial pressure monitoring was identified by presence of any type of monitoring device identified in the database.
Given the large sample size, skewness was calculated for each continuous variable to assess for asymmetry in its distribution. Following common practice, absolute skewness values greater than 1 were considered indicative of a highly skewed distribution. Highly skewed data are reported with median and interquartile range and compared with Mann-Whitney U test; otherwise, they are reported with mean and standard deviation and compared by t-test. Categorical variables were summarized with percentages and compared with chi-square testing. Counts of missing data points are reported but excluded from summative measures.
Demographics and presenting characteristics of cases were compared in the entire cohort and then in a propensity score-matched cohort on presentation from prison based on age, sex, and race at a 2:1 ratio. To assess outcomes, a second matched cohort was created after the addition of GCS and ISS to the propensity model. Major polytrauma was defined as an AIS greater than 2 in any organ system other than the head and neck. For matched cohorts, cases with missing data for age, sex, race, and GCS were excluded given the relatively small number of cases of patients presenting from prison. Subgroup analysis was performed based on GCS range defined as 3–8 for severe, 9–12 for moderate, and 13–15 for mild TBIs15.
Multivariable logistic regression was performed to test for association between predictors and hospital mortality, modeled with a binomial distribution and logit link. Predictors included presentation from prison, age, sex, race, body mass index, ISS, and GCS. GCS was not included in modeling for subgroup analyses in which cases were selected based on GCS range.
Analysis was performed in R (version 4.4.3). This manuscript was constructed in accordance with STROBE guidelines. The predetermined threshold for significance was a p-value < 0.05.
Results
Demographics and presentations of patients from prison and from the community
A total of 506,360 patients presenting from the community and 4,648 presenting from prison with TBI were identified. As summarized in Table 1, patients presenting from prison with TBI were younger on average than those from the community (mean 41.4 [SD 13.5] vs. 55.9 [SD 21.2] years, p < 0.001), predominantly male (95.8% vs. 64.0%, p < 0.001), and less frequently white (65.2% vs. 79.8%, p < 0.001). They had fewer comorbidities (median 1 [IQR 2] vs. 1 [IQR 3], p < 0.001) and a slightly lower body mass index (median 26.2 [IQR 6.4] vs. 26.3 [IQR 7.4], p = 0.023).
Injury severity, as measured by ISS, was lower in the prison group (median 9 [IQR 11] vs. 12 [IQR 13], p < 0.001). Patients from prison were more often treated at larger hospitals with more than 400 beds (70.0% vs. 64.1%, p < 0.001), which were less frequently for-profit (10.4% vs. 12.3%, p < 0.001), and more often had level I trauma certification (73.0% vs. 60.0%, p < 0.001). Presenting GCS was statistically higher among the prison group (median 15 [IQR 1] v. 15 [IQR 1], p < 0.001), a difference better reflected in the lesser representation of moderate (7.2% vs. 8.3%, p < 0.001) and severe (12.6% vs. 14.5%, p < 0.001) range injures. Major polytrauma was less common in the prison group (10.0% vs. 22.5%, p < 0.001).
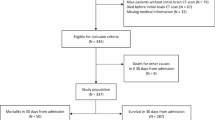
Due to removal of cases with missing covariates in the match model, 723 (15.5%) were excluded from prison group, and 60,087 (13.4%) were excluded from the community group entering the matching process. Once matched for age, sex, and race, there were 3,925 in the prison group and 7,850 in the community group in the first matched cohort. There were no differences in these demographic covariates (Supplementary Table 2), but there remained significant differences in trauma severity. Total comorbidity counts were similar (overall median 1 [IQR 2], p = 0.45), while BMI was lower among patients from prison (median 26.0 [IQR 6.3] vs. 26.5 [IQR 7.2], p < 0.001).
As shown in Table 2, the prison group had a lower mean ISS compared to the community group (median 10 (IQR 11) vs. 14 (IQR 13), p < 0.001) and a higher mean GCS score (median 15 (IQR 1) vs. 15 (IQR 3), p < 0.001); within it, there were fewer patients in the severe TBI GCS category (12.9% vs. 20.9%), and with major polytrauma (10.3% vs. 28.8%, p < 0.001). Injury patterns differed substantially: penetrating trauma was less common in the prison group (6.1% vs. 8.2%, p < 0.001), while blunt trauma predominated (93.9% vs. 91.8%, p < 0.001). Trauma intent differed, with assault accounting for the majority of prison cases (62.6% vs. 15.0%, p < 0.001), compared to mostly unintentional injuries in the community group (33.2% vs. 81.5%, p < 0.001). Self-inflicted injuries were slightly more frequent in the prison group (3.0% vs. 2.6%, p < 0.001). Mechanisms of injury also varied: the prison group was far less frequently involved in motor vehicle trauma—including occupants, pedestrians, and motorcyclists (0.2% vs. 45.4%, p < 0.001)—and firearm injuries (0.1% vs. 7.2%, p < 0.001).
After the addition of GCS and ISS to the propensity score, there were 3,925 patients in the prison group and 7,850 in the community group (Table 3). The matched covariates were not different between the groups (Supplementary Table 3). Comorbidity count remained similar between groups (median 1 [IQR 2], p = 0.37), while BMI remained minimally lower in the prison group (median 26.0 [IQR 6.3] vs. 26.5 [IQR 7.2], p < 0.001).
Treatments and outcomes
Among this GCS- and ISS-matched cohort, patients in the prison group more frequently transferred to another hospital (5.2% vs. 3.2%, p < 0.001). Use of intracranial pressure monitoring (2.7% vs. 2.3%, p = 0.237) and craniotomy/craniectomy (3.9% vs. 3.2%, p = 0.064) were not different between groups. Hospital discharge disposition varied, with decreased rates of discharge against medical advice (1.7% vs. 5.2%, p < 0.001), to acute rehabilitation facilities (ARF) (2.2% vs. 7.3%, p < 0.001) and to skilled nursing facilities (SNF) (1.7% vs. 3.4%, p < 0.001) in the prison group. This gap was more pronounced in patients over 65 years old (ARF 3.9% vs. 13.9%, SNF 3.9% vs. 14.9%, p < 0.001). Total hospital length of stay (LOS) was similar between groups (median 3 [IQR 4], p = 0.45).
In this same cohort, hospital mortality was more frequent among the prison group (5.0% vs. 3.9%, p = 0.007). Among patients with severe TBI, patients from prison exhibited significantly higher mortality compared to patients from the community (30.9% vs. 25.7%, p = 0.03). Once adjusted for age, sex, race, and ISS, presentation from prison was associated with a 43% increased risk of hospital mortality among those with severe traumatic brain injury (aOR 1.43, 95%CI [1.10, 1.86], p = 0.008). The odds of mortality did not vary between the mild (aOR 1.1, 95%CI [0.63, 1.81], p = 0.8) and moderate GCS ranges (aOR 1.77, 95%CI [0.87, 3.59], p = 0.11) based on presentation from prison (Supplementary Table 4).
Discussion
We found that TBI among patients presenting from prison is an epidemiologically distinct entity from TBI among patients presenting from the community. When matched for age, sex, and race, measures of injury severity were lower among the group from prison, and mechanisms of injury were demonstrably different. Once matched for injury severity, presentation from prison was independently associated with increased risk of hospital mortality among patients presenting with TBI, an effect driven by a 43% increased risk of mortality for patients presenting from prison in the severe TBI GCS range.
Among all patients studied, those from prison were younger, more often Black, and more often male, reflecting underlying differences between the incarcerated and non-incarcerated populations1. Perhaps because of limited access to firearms and motor vehicles, related trauma involving their use was minimally represented among patients from prison. We hypothesize that the absence of these high-energy trauma mechanisms may have contributed to overall lower severity of injury among the prison group in the age-, race-, and sex-matched cohorts. The relative preponderance of self-harm as the intent of injury was also notable and is consistent with the findings of a prospectively collected multicenter cohort study in which self-injurious behavior resulted in nearly a fifth of trauma activations among incarcerated patients studied11. Patients experiencing incarceration are at elevated risk for suicidality, and it is a frequent cause of death within this group16,17.
Prior research regarding mortality after brain trauma for patients experiencing incarceration is sparse. In our study, we observed an increased frequency of hospital mortality among all TBI grades and specifically a 43% increase in adjusted odds of death associated with presentation from prison among patients with severe TBI. Shahrestani et al. reported on patients presenting with traumatic acute subdural hematoma, a subgroup of patients presenting with TBI, in the National Inpatient Sample and discovered no difference in hospital mortality based on presentation from prison; however, there was a higher proportion of patients with severe TBI in the community group,18 so differences of baseline risk might have obscured the effects of presentation from prison. Similarly, a study of patients with diverse trauma types in the 2015–2016 TQIP database did not identify a significant difference in mortality between patients presenting from prison and from the community before or after adjustment for confounders that included GCS,10 though they did not perform propensity score matching.
The causes underlying the difference in mortality seen in our study warrant further investigation. Differences in injury mechanism were not modeled and could impact outcomes through variable patterns of injury with dissimilar contributions to mortality risk despite similar ISS. While it was expected that the relative absence of the high energy motor vehicle trauma and firearm-related injuries among patients presenting from prison would confer a protective effect against mortality in this group,19 this effect was not observed or may have been countervailed by a competing harmful effect associated with presentation from prison.
While there was a preponderance of assault as a mechanism of injury among patients presenting from prison, its effect on the risk of mortality requires further study in this population. Prior studies of violence as a risk factor for short-term mortality after trauma have focused on injuries in the community. One study identified that intentional TBI produced statistically similar albeit numerically lower measures of injury severity and odds of hospital mortality20. Another study including all trauma types reported an increased risk of hospital mortality among those injured intentionally but was contaminated by high prevalence of firearm-related violence, limiting transferability to the prison population21.
Our study assessed the total, rather than direct, effects of presentation from prison, which may include effects mediated through differences in clinical course after arrival to the hospital. Although the rates of measurable TBI-specific interventions—craniotomy or ICP monitoring—did not differ significantly between groups, these metrics are limited proxies for the quality of care. The similarity in utilization does not preclude differences in timeliness or appropriateness of interventions that may be delayed by complexities in decision-making for incapacitated patients, collaboration with Department of Corrections staff, or other structural differences that alter workflows2. For example, the observation of increased hospital transfer rate raises the question of under-triage among patients presenting from prison, which could contribute to delays in definitive care. The hypothesis that unmeasured heterogeneity in clinical care contributes to worsened outcomes among the patients presenting from prison might additionally be supported by the finding of increased risk for mortality seen only among patients with severe TBI, fragile patients whose outcomes are may be more sensitive to difference in care quality and intensity. Future study should investigate variation in otherwise routine clinical care to evaluate for these effects.
Finally, discharge disposition varied greatly and meaningfully among TBI survivors with fewer patients from prison discharged to inpatient acute rehabilitation and skilled nursing facilities. Lacking data on neurological state at discharge, it is impossible to conclude that these services were as needful among patients experiencing incarceration, however it is possible that these patients had limited access to post-acute care services based on their incarceration status22. Facilities may consider incarceration status in evaluating a patient for admission, the disclosure of which may lead to decreased odds of acceptance, as was shown in a study of SNF acceptances of patients approved for compassionate release from prison in the setting of severe illness23. Additionally, patients discharged to an inpatient facility must remain accompanied by correctional officers, creating disincentive for prison systems to support this practice. Alternatively, it is possible that disposition to a post-acute care facility was less needed because some prisons and jails have on-site medical services including physical and occupational therapy routing discharging patients back to carceral facilities.
Implications of findings
Beyond the need to identify and address contributors to increased mortality among patients presenting from prison with severe traumatic brain injuries, the size of this cohort – nearly 4,000 in a single year from this convenience sample that does not capture the entire national burden of the disease process – highlights the urgent need for clear procedures for management of patients presenting with brain injury while incarcerated. This is a population who must be managed through a specific ethical, legal, and logistical framework both while hospitalized and after discharge13,24 that may be unfamiliar to hospital staff.
Many of these patients, especially those with moderate and severe GCS range injuries, may lose decisional capacity at least transiently and require complex medical decision-making that depends heavily on individual patient preferences for and beliefs about the acceptability of treatments and specific long-term neurological outcomes. Even with an identified medical surrogate, communication may be restricted and mediated by the correctional system to the extreme of barring all visitors and communication with friends and family if deemed necessary to protect the public interest. In practice, the process of medical decision-making for incapacitated patients has been observed to be both variable and imperfectly performed24,25.
Post-hospital care is also a point of special consideration. As mentioned, there are rehabilitative resources at some prison facilities to support the recovery of patients discharging from a hospital that might divert patients from typical post-acute care facilities. Yet, these prison resources may be limited and designed with different therapeutic intent than providing rehabilitative care to patients with recent brain injuries, which could contribute to divergent long-term outcomes. Especially among the growing population of older adults who are incarcerated, this places a large financial and logistical burden26,27 on prison health resources. Recovery of function after TBI occurs over years across the spectrum from mild5 to severe7 injuries. Differential access to relevant services through this period might potentiate differential long-term outcomes.
Strengths and limitations
Strengths of this study include its large sample size drawn from many institutions, use of propensity score matching to address covariate imbalance, and stratification by severity of TBI in assessment outcomes.
Registry-based research about health outcomes among carceral populations remains a nascent field. Although injury location codes are theoretically sound with an overtly reasonable definition, their sensitivity and specificity remain to be characterized. It was assumed that patients identified as injured at prison were incarcerated, though some, presumed small, number may instead have been injured while working at or visiting a prison. Moreover, small and unique clinical populations may challenge coding conventions designed for the general population. For example, it seems improbable that approximately half of the patients from prison were discharged “home” unless “home” referred to a carceral facility which might otherwise have been coded as discharge to “law enforcement.” These limitations present opportunities for further study to elucidate the characterization of patients who are incarcerated in large registries.
Approximately 13% of all cases were excluded due to missingness of key data points, though this proportion was similar between the groups. Hospital mortality and disposition are narrow measures of outcome after TBI as most patients survive and experience recovery after hospital discharge, leaving the possibility of further divergence of outcomes based on incarceration status. The findings presented here are specific to patients presenting from prisons in the United States and may not be transferrable to patients presenting from prisons in other nations. Heterogeneity in justice systems and carceral medicine programs may precipitate measurable differences in demographics, trauma mechanisms, and clinical outcomes. Nonetheless, within the context of hypothesis-generating research, these limitations might be tolerated while awaiting confirmatory studies.
Conclusions
This study identifies a significant disparity in hospital mortality among incarcerated patients with isolated severe TBI despite similar treatment intensity after propensity score matching for baseline differences in demographics. Furthermore, disparities in discharge disposition—including lower rates of rehabilitation referrals—suggest the possibility of inequitable post-hospital care. Further research is required to elucidate the underlying causes of this disparity. Future work might investigate variation in care quality that is unmeasured in national registry datasets, differences in medical decision-making processes and outcomes, and broader structural differences in the longitudinal evaluation and management of traumatically injured patients presenting from carceral facilities.
Data availability
Study data is available upon reasonable request. Contact the corresponding author for further information.
References
Buehler, E. D. & Kluckow, R. Correctional Populations in the United States, 2022 – Statistical Tables. U.S. Department of Justice; Accessed (28 Jun 2025). https://bjs.ojp.gov/document/cpus22st.pdf (2024).
Kaufman, E. J. et al. Providing equitable surgical care to patients in law enforcement custody: A review. JAMA Surgery Published Online May. 14 https://doi.org/10.1001/jamasurg.2025.1129 (2025).
Reports, U. S. & 429 U.S. Estelle v. Gamble, 97 Library of Congress, Washington, D.C. 20540 USA. Accessed (20 Feb 2024). https://www.loc.gov/item/usrep429097/ (1976).
Münch, E. et al. Management of severe traumatic brain injury by decompressive craniectomy. Neurosurgery 47 (2), 315 (2000).
Nelson, L. D. et al. Functional Recovery, Symptoms, and quality of life 1 to 5 years after traumatic brain injury: findings from the TRACK-TBI study. JAMA Netw. Open. 6 (3), e233660. https://doi.org/10.1001/jamanetworkopen.2023.3660 (2023).
McCrea, M. A. et al. Functional outcomes over the first year after moderate to severe traumatic brain injury in the Prospective, longitudinal TRACK-TBI study. JAMA Neurol. 78 (8), 982. https://doi.org/10.1001/jamaneurol.2021.2043 (2021).
Deng, H. et al. Time to follow commands in severe traumatic brain injury survivors with favorable recovery at 2 years. Neurosurgery 91 (4), 633–640. https://doi.org/10.1227/neu.0000000000002087 (2022).
Izzy, S. et al. Association of traumatic brain injury with the risk of developing chronic Cardiovascular, Endocrine, Neurological, and psychiatric disorders. JAMA Netw. Open. 5 (4), e229478. https://doi.org/10.1001/jamanetworkopen.2022.9478 (2022).
Henning, J., Frangos, S., Simon, R., Pachter, H. L. & Bholat, O. S. Patterns of traumatic injury in new York City prisoners requiring hospital admission. J. Correctional Health Care. 21 (1), 53–58. https://doi.org/10.1177/1078345814558046 (2015).
Christian, A. B. et al. Comparative outcomes for trauma patients in prison and the general population. Am. Surgeon™. 88 (8), 1954–1961. https://doi.org/10.1177/00031348221078984 (2022).
Bryant, M. K. et al. Outcomes after emergency general surgery and trauma care in incarcerated individuals: an EAST multicenter study. J. Trauma. Acute Care Surg. 93 (1), 75. https://doi.org/10.1097/TA.0000000000003614 (2022).
Maher, P. J. et al. Emergency department utilization by a jail population. Am. J. Emerg. Med. 36 (9), 1631–1634. https://doi.org/10.1016/j.ajem.2018.06.034 (2018).
Haber, L. A., Erickson, H. P., Ranji, S. R., Ortiz, G. M. & Pratt, L. A. Acute care for patients who are incarcerated: A review. JAMA Intern. Med. 179 (11), 1561. https://doi.org/10.1001/jamainternmed.2019.3881 (2019).
Newman-Plotnick, H., Byrne, J. P., Haut, E. R. & Hultman, C. S. Incarceration is associated with higher mortality after trauma: an unreported health care disparity. J. Trauma. Acute Care Surg. 98 (5), 785. https://doi.org/10.1097/TA.0000000000004512 (2025).
Brennan, P. M., Murray, G. D. & Teasdale, G. M. Simplifying the use of prognostic information in traumatic brain injury. Part 1: the GCS-Pupils score: an extended index of clinical severity. J. Neurosurg. 128 (6), 1612–1620. https://doi.org/10.3171/2017.12.jns172780 (2018).
Dixon, K. J. et al. Suicides among incarcerated persons in 18 U.S. States: findings from the National violent death reporting System, 2003–2014. J. Correctional Health Care. 26 (3), 279–291. https://doi.org/10.1177/1078345820939512 (2020).
Carson, E. A. Mortality in State and Federal Prisons, 2001–2019 – Statistical Tables. (2021)
Shahrestani, S., Strickland, B. A., Micko, A., Brown, N. J. & Zada, G. Management of acute subdural hematoma in incarcerated patients. Clin. Neurol. Neurosurg. 201, 106441. https://doi.org/10.1016/j.clineuro.2020.106441 (2021).
Bushnik, T., Hanks, R. A., Kreutzer, J. & Rosenthal, M. Etiology of traumatic brain injury: characterization of differential outcomes up to 1 year postinjury. Arch. Phys. Med. Rehabil. 84 (2), 255–262. https://doi.org/10.1053/apmr.2003.50092 (2003).
Taylor, S., Patel, T., Desai, Y., Welsh, C. & Legome, E. Epidemiology and risk factors for intentional traumatic brain injury. Trauma. Care. 5 (1), 2. https://doi.org/10.3390/traumacare5010002 (2025).
Saif, S., Ibrahim, Y. & Bakhshayesh, P. Higher risk of mortality in intentional traumatic Injuries; A multivariate regression analysis of a trauma registry. Bull. Emerg. Trauma. 8 (2), 107–110. https://doi.org/10.30476/beat.2020.46450 (2020).
Dayanim, G., Mushero, N. & Berk, J. Access to Long-Term nursing care for Justice-Involved elderly. Health Affairs Forefront https://doi.org/10.1377/forefront.20231010.271893
Dayanim, G. et al. Nursing home availability for incarcerated persons granted compassionate release. Sci. Rep. 15 (1), 37676. https://doi.org/10.1038/s41598-025-21492-7 (2025).
Scarlet, S., DeMartino, E. S. & Siegler, M. Surrogate decision making for incarcerated patients. JAMA Intern. Med. 179 (7), 861–862. https://doi.org/10.1001/jamainternmed.2019.1386 (2019).
Batbold, S., Duke, J. D., Riggan, K. A. & DeMartino, E. S. Decision-Making for hospitalized incarcerated patients lacking decisional capacity. JAMA Intern. Med. 184 (1), 28. https://doi.org/10.1001/jamainternmed.2023.5794 (2024).
Greene, M., Ahalt, C., Stijacic-Cenzer, I., Metzger, L. & Williams, B. Older adults in jail: high rates and early onset of geriatric conditions. Health Justice. 6 (1), 3. https://doi.org/10.1186/s40352-018-0062-9 (2018).
Williams, B. A., Goodwin, J. S., Baillargeon, J., Ahalt, C. & Walter, L. C. Addressing the aging crisis in U.S. Criminal justice health care. J. Am. Geriatr. Soc. 60 (6), 1150–1156. https://doi.org/10.1111/j.1532-5415.2012.03962.x (2012).
Funding
No intra- or extramural funding directly supported this work.
Author information
Authors and Affiliations
Contributions
JF: Conceptualization, Data curation, Formal Analysis, Methodology, Writing – original draft; NS: Conceptualization, Methodology, Writing – review & editing; DC: Writing – review & editing; LH: Writing – review & editing; JB: Conceptualization, Supervision, Writing – review & editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Appendix
Appendix
Binary Comorbidity Data Included from Data Set
-
Alcohol use disorder
-
Angina pectoris
-
Bleeding disorder
-
Cerebral vascular accident
-
Chronic obstructive pulmonary disease
-
Chronic renal failure
-
Cirrhosis
-
Congenital anomalies
-
Congestive heart failure
-
Current smoker
-
Currently receiving chemotherapy for cancer
-
Dementia
-
Diabetes mellitus
-
Disseminated cancer
-
Functionally dependent health status
-
Hypertension
-
Myocardial infarction
-
Peripheral arterial disease
-
Steroid use
-
Substance use disorder
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Feler, J., Schachman, N., Cielo, D. et al. Traumatic brain injury among patients presenting from prison: a cohort study. Sci Rep 16, 13388 (2026). https://doi.org/10.1038/s41598-026-37391-4
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-37391-4