Abstract
Acanthamoeba keratitis remains a severe complication of contact lens (CL) wear, and preventing trophozoite adhesion to the lens surface is a critical step in preventing infection. This study investigated the anti-amoebic performance and ocular safety of soft CLs embedded with nephrite, a mineral with inherent antimicrobial activity. Clear, cosmetic, and nephrite-embedded CLs were compared. We uniformly dispersed nephrite powder onto the inner mold surface and encapsulated it within the polymer network using the Flusier method, preventing direct corneal exposure while maintaining transparency. In vitro assays demonstrated that nephrite-embedded CLs had significantly fewer adherent Acanthamoeba lugdunensis trophozoites than clear (p = 0.0093) and cosmetic CLs (p = 0.0068). SEM images showed reduced pseudopodia formation and round, contracted morphology of the attached trophozoites, suggesting early encystment. Although AFM revealed greater surface roughness than clear lenses, Acanthamoeba adhesion was still markedly lower. In vivo evaluation in rabbits showed no corneal opacity, no histologic inflammatory response, and no significant differences in corneal thickness or endothelial cell density compared with other groups. These findings indicate that the nephrite-embedded CLs developed in this study effectively inhibited Acanthamoeba adhesion while maintaining corneal safety, suggesting nephrite as a promising material for CLs with anti-amoebic properties.
Similar content being viewed by others
Introduction
Acanthamoeba keratitis (AK) is an uncommon but potentially sight-threatening corneal infection characterized by severe pain, stromal inflammation, and progressive tissue destruction1,2. It is caused by Acanthamoeba species, free-living protozoa that are widely distributed in natural and domestic environments such as soil, air, and water1,2,3. Although human exposure is frequent, infection develops only under favorable conditions, typically when contaminated contact lenses serve as a vector for trophozoite attachment1,2,4,5.
Contact lens (CL) wear remains the principal risk factor for AK, accounting for more than 85–90% of reported cases worldwide6,7. The incidence has been estimated at 1–33 cases per million lens wearers annually, with increased risk due to inadequate disinfection, overnight CL wear, and exposure to tap or swimming water1,4. Despite advances in CL materials and care solutions, treatment outcomes remain suboptimal because of delayed diagnosis, poor drug penetration, and the resistance of Acanthamoeba cysts to antimicrobial agents4,5,8,9.
Pathogenesis begins when Acanthamoeba trophozoites adhere to the corneal epithelium through mannose-binding proteins that interact with epithelial glycoproteins3,10. Because adhesion is the initial step of infection, the physicochemical properties of the contact lens surface can significantly influence Acanthamoeba binding. Previous studies have shown that rough or pigment-coated lenses, such as cosmetic CLs, exhibit greater bacterial and amoebic adhesion than smooth silicone hydrogel surfaces11,12. Once attached to the lens or corneal surface, trophozoites establish close contact with epithelial cells, initiating pathogenic interactions that progress into active tissue invasion. During this process, secretion of proteases, including mannose-induced protease 133, causes epithelial lysis and stromal infiltration3. Once Acanthamoeba transform into cyst form, the organism becomes highly tolerant to dry environment and antimicrobial agents, leading to chronic, refractory infection13,14.
In recent years, several approaches have aimed to prevent contact lens-related microbial keratitis by developing new materials with antimicrobial or anti-adhesive properties15,16. Silver-based nanoparticles, tannic acid–modified compounds, and surface-active polymers have demonstrated inhibitory effects against Acanthamoeba and other pathogens15,16,17. Mineral-based biomaterials have recently drawn attention as safe and long-lasting alternatives for infection control. Among them, nephrite, a calcium–magnesium–iron silicate, has shown antimicrobial activity and can be incorporated into contact lenses without compromising optical or biological safety11,18. These properties suggest its potential as a bioactive component for contact lenses designed to resist microbial or protozoal contamination. Building upon this concept, we fabricated soft contact lenses embedded with nephrite particles to explore their anti-amoebic efficacy. We hypothesized that incorporating nephrite particles directly into the CL matrix would inhibit Acanthamoeba survival and reduce the risk of CL-related keratitis, while preserving corneal safety. This study aimed to evaluate the potential of nephrite as a functional material for contact lenses with anti-amoebic properties.
Materials and methods
Contact lenses
Clear, cosmetic, and nephrite-embedded CLs were used in this study. All lenses were manufactured by DreamCon Co., Ltd. (Yangsan, Korea) using hydroxyethyl methacrylate (HEMA) as the base polymer with 40 ± 2% water content, oxygen permeability (Dk/t) of approximately 10 × 10¹¹ (cm × mL O₂)/(s × mL × mmHg), and a base curve/diameter of 8.6 mm/14.0 mm. The lenses were fabricated following a modified Flusier method (KR101190303B1, DreamCon Co., Korea), in which the nephrite or pigment layer is encapsulated between polymer layers to prevent direct corneal contact19. Nephrite was incorporated into the contact lenses in powder form at a concentration of 0.3 wt%. This concentration was selected because higher nephrite loading resulted in reduced powder dispersion and decreased optical transparency. The nephrite powder consisted of particles smaller than 5 μm, as confirmed by field-emission scanning electron microscopy (FE-SEM). Uniform incorporation of nephrite within the HEMA-based lens matrix was verified by FE-SEM and energy-dispersive X-ray spectroscopy (EDS). All lenses were prepared under controlled manufacturing conditions and stored under standard conditions at room temperature prior to use.
Atomic force microscopy (AFM) of lens surface
To evaluate surface roughness and morphological differences of the CLs, atomic force microscopy (AFM) was performed. Hydrated lenses were quartered and fixed to microscope slides using double-sided adhesive tape. AFM imaging was conducted in true contact mode using an NX10 AFM system (Park Systems, Suwon, Korea) equipped with a PRE75 contact-mode probe (Neuchatel, Switzerland). Images (scan area: 2,500 μm²) were analyzed using XEI 1.8.2 software (Park Systems). Surface parameters including average roughness (Ra), root-mean-square roughness (Rq), and ten-point mean height roughness (Rz) were calculated according to the international surface roughness standard ISO 4287 (JIS B 0601 equivalent).
Preparation of Acanthamoeba trophozoites
Acanthamoeba lugdunensis L3a trophozoites, the most frequently isolated type from CL storage cases in Korea, were obtained from the Department of Parasitology, Pusan National University School of Medicine. The strain was confirmed by riboprinting and 18 S rDNA sequencing. Trophozoites were cultured in peptone-yeast extract/glucose (PYG) medium (20.02 g Bacto Proteose Peptone, 1.0 g yeast extract, 950 mL distilled water, 50 mL 2 M D(+)glucose, 10 mL 0.4 M MgSO₄·7 H₂O, 8 mL 0.05 M CaCl₂, 34 mL 0.1 M sodium citrate, 10 mL 0.005 M Fe(NH4)2 (SO4)2·6 H2O, 10 mL 0.25 M NaHPO4·7 H2O, and 10 mL 0.25 M KH₂PO₄) at 25 ± 1 °C. Trophozoites were washed twice with PBS and adjusted to 2 × 10⁴ cells/mL using a hemocytometer before use.
Adhesion assay of Acanthamoeba to lenses
Each CL was placed with the concave surface facing upward in a 12-well plate containing 2 mL of PYG medium. Acanthamoeba trophozoites (2 × 10⁴/mL) were inoculated and incubated for 18 h at room temperature. After incubation, lenses were gently washed twice with PBS to remove non-adherent cells. The number of adherent trophozoites was quantified under a light microscope (×100). Sixteen randomly selected fields per CL were photographed, and the mean number of trophozoites per field was calculated. Each experiment was repeated three times with three lenses per group.
Scanning electron microscopy (SEM)
After adhesion testing, lenses were fixed in 2.5% glutaraldehyde in 100 mM sodium cacodylate buffer (pH 7.4) for 1 h at 4 °C, post-fixed with 1% osmium tetroxide, and dehydrated through graded ethanol (50–100%, 10% increment). Samples were critical point-dried with CO₂, coated with 30 nm of gold, and examined using a field-emission scanning electron microscope (SUPRA 40 VP; Carl Zeiss, Jena, Germany). The attachment morphology of Acanthamoeba were examined at magnifications ranging from ×1,000 to ×15,000.
In vivo safety test using rabbit cornea
The biocompatibility and ocular safety of all types of contact lenses were evaluated in vivo using New Zealand white rabbits (male, 2.0–2.5 kg, 8 weeks old; n = 12). All animal experiments were performed in compliance with the Association for Research in Vision and Ophthalmology (ARVO) statement, ARRIVE (Animal Research: Reporting In Vivo Experiments) guidelines, and were approved by the Institutional Animal Care and Use Committee (IACUC) of Pusan National University School of Medicine (IACUC No. PNU-2023-1721).
Rabbits were monitored daily for any signs of distress or ocular complications. Humane endpoints were predefined and included more than 20% of the body weight loss compared with the initial body weight, persistent anorexia or dehydration, severe ocular pain unrelieved by topical anesthesia, corneal perforation, or any veterinarian-determined condition requiring discontinuation of the study. No animals reached these endpoints during the experiment.
Rabbits were anesthetized with intramuscular injections of ketamine hydrochloride (50 mg/kg) and xylazine (10 mg/kg), and topical proparacaine hydrochloride 0.5% was administered to each eye three times ten minutes before CL placement. Clear, cosmetic, and nephrite-embedded CLs were applied to the corneas for 24 h. After CL removal, the corneas were examined by slit-lamp microscopy and anterior-segment photography to assess opacity and clarity. Corneal thickness was measured using optical coherence tomography (Cirrus HD-OCT 4000, Carl Zeiss Meditec, Dublin, CA, USA), and endothelial cell counts were obtained using a non-contact specular microscope (SP-1P®, Topcon, Tokyo, Japan). Finally, the rabbits were euthanized in a CO₂ chamber (CO₂ displacement rate 50–60% of the chamber volume/min) followed by confirmation of death by absence of heartbeat and pupil reflex, in accordance with the AVMA (American Veterinary Medical Association) guidelines for the euthanasia of animals (2020). After euthanasia, corneas were excised, fixed in 4% paraformaldehyde, embedded in paraffin, sectioned, and stained with hematoxylin and eosin (H&E) for histologic examination. The presence of inflammatory cell infiltration, epithelial damage, or stromal edema was evaluated under light microscopy (Axio Scan.Z1, Carl Zeiss, Germany).
Statistical analysis
All data are expressed as mean ± standard error. Statistical analyses were conducted using IBM SPSS ver. 29 (IBM Corp., Armonk, NY, USA). Differences in Acanthamoeba adhesion counts, corneal thickness, and endothelial cell density were analyzed by unpaired Welch’s t-tests for pairwise comparisons. All experiments were repeated three times. A p-value < 0.05 was considered statistically significant.
Results
The contact lenses used in the study
Three types of lenses were used in this study: clear (Fig. 1A), cosmetic (Fig. 1B), and nephrite-embedded contact lenses (Fig. 1C). The clear and cosmetic lenses were commercially available soft contact lenses and served as control groups. The nephrite-embedded contact lens was newly developed in our laboratory using the Flusier method, in which purified nephrite powder was incorporated within the polymer matrix so that nephrite was not directly exposed to the ocular surface. To maintain optical clarity, the central visual axis was intentionally left free of nephrite to maintain transparency and normal vision. Optical transmittance of the contact lenses was evaluated according to ISO 18,369 standards by an accredited testing laboratory (Korea Testing & Research Institute). The visible light transmittance measured at the central optical zone was 99%.
Three types of contact lenses used in this study. (A) Clear contact lens, (B) Cosmetic contact lens, and (C) Nephrite-embedded contact lens.
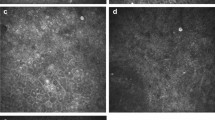
Atomic force microscopy (AFM) was used to examine the surfaces of three contact lenses. AFM analysis was performed on a 2500 μm2 area of the concave surface. The bright spots in the images indicate regions of higher surface elevation.
Atomic force microscopy (AFM) surface roughness
AFM analysis demonstrated differences in surface roughness among the three CL types (Fig. 2). The cosmetic CL showed the greatest roughness parameters (Ra, Rq, Rz), the nephrite CL exhibited intermediate values, and the clear CL presented the lowest overall roughness (Table 1).
Acanthamoeba adhesion on different contact lenses
Examination of Acanthamoeba trophozoite adhesion under light microscope (Fig. 3A and C) and quantitative analysis (Fig. 3D) demonstrated significant differences in Acanthamoeba trophozoite adhesion among the three CL types. The cosmetic CL showed the highest number of adherent trophozoites, followed by the clear CL, whereas the nephrite-embedded CL showed the fewest adherent cells (p < 0.05 for all pairwise comparisons). Compared with the cosmetic CL, the mean number of adherent trophozoites was reduced by more than 70% on the nephrite-embedded CL surface.
Scanning electron microscopy (SEM)
SEM imaging (Fig. 4) revealed distinct differences in CL surfaces and morphology of attached Acanthamoeba. The cosmetic CLs exhibited a more irregular and uneven surface compared with the clear CLs, while nephrite-embedded CLs showed distinct nephrite particles on their surface. On both clear and cosmetic CLs, trophozoites were firmly attached, exhibiting numerous pseudopodia. In contrast, trophozoites on the nephrite-embedded CL surface appeared round and contracted, with fewer or absent pseudopodia. These microscopic findings suggested that nephrite interfered with trophozoite attachment and induced encystment-like or stress-associated morphological changes.
Light microscopic images (original magnification×100) of Acanthamoeba attached to different types of contact lenses (CLs). Acanthamoeba attached to (A) Clear CLs, (B) Cosmetic CLs, and (C) Nephrite-embedded CLs, respectively. Acanthamoeba attached to nephrite-embedded contact lenses are indicated with arrows to distinguish them from nephrite particles. (D) Graph showing the number of Acanthamoeba attached to three types of CLs. Nephrite-embedded CLs had significantly lower number of Acanthamoeba (n = 52.3 ± 2.6) attached compared with clear CLs (n = 94.0 ± 8.6, p = 0.0093), and cosmetic CLs (n = 28.0 ± 1.6, p = 0.0068). Statistical analysis was done using unpaired Welch’s t-test.
Scanning electron microscopy (SEM) images of the surface of the contact lenses and attachedAcanthamoeba (arrows). While (A), (B), and (C) show SEM images before Acanthamoeba inoculation(original magnification×1,000), (D), (E), and (F) show images after Acanthamoeba inoculation (originalmagnification×100). The surfaces of the cosmetic CLs and nephrite-embedded CLs were rougher comparedwith that of clear CLs. More Acanthamoeba were attached to cosmetic CLs than clear and nephrite-embeddedCLs. (F) Acanthamoeba trophozoites on the nephrite-embedded CL surface exhibit reduced acanthopodiaformation, suggesting encystment-like or stress-associated morphological changes.
In vivo corneal safety
Histopathologic evaluation of rabbit eyes after 24 h of CL wear demonstrated preserved corneal integrity in all four groups (Fig. 5). None of the four groups exhibited corneal opacity (Fig. 5A). Hematoxylin–Eosin (H&E) staining revealed a well-organized corneal structure without any evidence of inflammatory cell infiltration, edema, or neovascularization (Fig. 5B). The corneal thickness was comparable among the control, clear, cosmetic, and nephrite-embedded contact CL groups (Fig. 5C), and the difference in corneal thickness was not statistically significant (Fig. 5E). Endothelial cell density was also comparable among the three groups (Fig. 5D), while the only significant difference was found between the control and cosmetic groups (p = 0.043), and no significant differences were observed among the other groups (Fig. 5F).
Safety evaluation of CLs using rabbit models. (A) Representative anterior-segment images of rabbit corneas in each group showed no corneal opacities after 24 h. (B) H&E-stained corneal sections (×100) revealed no inflammatory cell infiltration in any group. (C) Optical coherence tomography images confirmed that there were no notable differences in corneal thickness among the groups. (D) Representative images of corneal endothelial cells showed a significant difference only between the control and cosmetic CL groups. (E) Quantified analysis of corneal thickness confirmed that there were no significant differences among the groups. (F) Quantified analysis of corneal endothelial cells showed a significant difference only between the control and cosmetic CL groups (p = 0.043), whereas other comparisons were not significant. Statistical analyses were performed using an unpaired Welch’s t-test.
Discussion
Acanthamoeba keratitis (AK) remains one of the most challenging complications associated with CL wear. Preventive strategies have mainly focused on improving disinfection systems and lens-care hygiene, since contamination of the lens surface and storage case is a primary route of infection. Because the initial stage of AK involves trophozoite adhesion to the contact lens1,2, developing materials that can inherently resist microbial attachment is considered a more direct preventive approach. Nephrite, a naturally occurring mineral with known antimicrobial and anti-inflammatory properties, has recently attracted attention as a potential biomedical material.
Previous studies have demonstrated that nephrite exhibits intrinsic antimicrobial and anti-inflammatory activity by suppressing the expression of inflammatory mediators such as IL-1β, TNF-α, COX-2, and iNOS20. It is also confirmed from previous studies that nephrite inhibits microbial proliferation when incorporated into contact lens storage cases18. To apply these properties to the lens material itself, we uniformly dispersed nephrite powder onto the inner mold surface and encapsulated it within the polymer network using the Flusier method, thereby preventing any direct corneal exposure. To maintain optical transparency, nephrite was not distributed in the central visual axis on purpose. As a result, surface characterization by SEM revealed fine, homogeneously distributed nephrite particles within the lens matrix, and AFM analysis demonstrated a moderately increased surface roughness while maintaining surface uniformity.
The results showed that nephrite-embedded contact lenses significantly inhibited Acanthamoeba adhesion compared with both clear and cosmetic CLs. SEM observations confirmed fewer adherent trophozoites with reduced acanthopodia formation on nephrite surfaces. Such morphological changes have been described during early encystment, although alternative explanations such as cellular stress or reduced viability cannot be excluded. Together, these findings suggest that embedding nephrite within the lens matrix provides anti-amoebic properties by inhibiting the adhesion of Acanthamoeba. Similar to previous reports on nephrite-containing storage cases18, the present results extend those observations to the CL itself, highlighting the potential of nephrite as a functional biomaterial for infection-resistant CLs.
AFM analysis revealed that nephrite-embedded CLs exhibited greater surface roughness than clear CLs, but paradoxically showed fewer attached trophozoites, indicating that the anti-adhesive property cannot be explained by surface roughness alone. Nephrite, a calcium–magnesium–iron silicate compounds, may play a role in influencing the electrochemical environment at the lens surface. The presence of ions such as Ca²⁺, Mg²⁺ and Fe²⁺/³⁺ could alter surface charge or local ionic gradients, which in turn might affect the adhesion of Acanthamoeba. Although direct evidence clarifying the ion-related mechanism underlying Acanthamoeba adhesion is lacking, previous studies focusing on chemical properties of CLs using ionized CL materials and silver-based contact lens solution suggest that ionized lens surfaces can influence Acanthamoeba attachment15,16. These findings suggest that the presence of nephrite within the lens matrix may influence the physicochemical environment at the lens surface and thereby affect Acanthamoeba adhesion. Although direct measurements of ion release or surface potential were not performed in this study, the observed reduction in adhesion despite increased surface roughness raises the possibility that chemical or ionic interactions, rather than surface texture alone, may contribute to the anti-adhesive effect.
In vivo evaluation using a single 24-hour exposure model showed that nephrite-embedded CLs caused no adverse ocular effects or tissue damage. No epithelial defects, stromal edema, or inflammatory infiltration were observed, and endothelial cell density remained comparable to control and clear groups. These results, although not fully representing prolonged contact lens wear, demonstrate that the incorporation of nephrite did not induce acute ocular irritation or toxicity, consistent with its previously reported biocompatibility in prior research11. This corneal safety was largely attributed to the fabrication process based on the Flusier method, in which a thin nephrite layer was applied to the inner mold surface and subsequently encapsulated within the polymer matrix during ultraviolet curing. This design completely seals the nephrite particles within the polymer matrix, effectively protecting the cornea from direct contact with nephrite while preserving ionic activity at the lens–tear film interface. This structure effectively balances two essential requirements, corneal safety and antimicrobial performance, providing a plausible explanation for the in vivo safety observed in this study. Therefore, the encapsulation of nephrite particles based on the Flusier method provides a structural basis for the favorable ocular tolerance observed under the present experimental conditions, while enabling anti-amoebic activity. These findings suggest that nephrite-embedded contact lenses may have potential as a preventive strategy against Acanthamoeba adhesion.
This study has several limitations. Firstly, the experiments used a single Acanthamoeba lugdunensis strain under controlled laboratory conditions and the results may differ among other pathogenic genotypes, including clinically prevalent T4 strains. Secondly, since the in vivo safety assessment in rabbits was performed only after 24 h of CL wear, long-term ocular safety could not be determined. Therefore, extended-wear studies involving prolonged CL application and chronic exposure will be required to fully evaluate potential late-onset inflammatory effect. Finally, the underlying reason why Acanthamoeba adhesion decreased in the nephrite-embedded CL despite the rougher surface could not be clearly identified. Further studies evaluating ion-release kinetics and surface potential induced by nephrite are needed to clarify the detailed mechanism.
In summary, nephrite-embedded CLs exhibited both anti-amoebic activity and corneal safety. The results suggest that nephrite modifies the physicochemical characteristics of the lens surface, leading to reduced Acanthamoeba adhesion. Given its favorable short-term safety profile and stable integration into the polymer network, nephrite may serve as a useful additive for developing CLs with improved resistance to Acanthamoeba adhesion.
Data availability
The data supporting this study are available from the corresponding author upon reasonable request.
References
Dart, J. K., G, Saw, V. P. J. & Kilvington, S. Acanthamoeba keratitis: diagnosis and treatment update 2009. Am. J. Ophthalmol. 148, 487–499 (2009).
Maycock, N. J. R. & Jayaswal, R. Update on Acanthamoeba keratitis: diagnosis, treatment, and outcomes. Cornea 35, 713–720 (2016).
Niederkorn, J. Y. The biology of Acanthamoeba keratitis. Exp. Eye Res. 202, 108365 (2021).
Fu, L. et al. Navigating the challenges of Acanthamoeba keratitis: current trends and future directions. Life (Basel). 15, 933 (2025).
Li, G. & Shekhawat, N. Acanthamoeba epitheliopathy: importance of early diagnosis. Am. J. Ophthalmol. Case Rep. 26, 101499 (2022).
Stapleton, F. & Carnt, N. Contact lens–related microbial keratitis: how have epidemiology and genetics helped Us with pathogenesis and prophylaxis? Eye (Lond). 26, 185–193 (2012).
Ting, D. S. J., Ho, C. S., Deshmukh, R., Said, D. G. & Dua, H. S. Infectious keratitis: an update on epidemiology, causative microorganisms, risk factors, and antimicrobial resistance. Eye (Lond). 35, 1084–1101 (2021).
Hay, J., Kirkness, C. M., Seal, D. V. & Wright, P. Drug resistance and Acanthamoeba keratitis: the quest for alternative antiprotozoal chemotherapy. Eye (Lond). 8, 555–563 (1994).
Ficker, L., Seal, D. & Warhurst, D. Wright P. Acanthamoeba keratitis—resistance to medical therapy. Eye (Lond). 4, 835–838 (1990).
Huth, S., Reverey, J. F., Leippe, M. & Selhuber-Unkel, C. Adhesion forces and mechanics in mannose-mediated Acanthamoeba interactions. PLoS One. 12, e0176207 (2012).
Kim, S. et al. Anti-pseudomonal effect of nephrite-impregnated contact lenses. Curr. Eye Res. 49, 914–922 (2024).
Pinto, L. F. et al. Adhesion of Acanthamoeba on scleral contact lenses according to lens shape. Invest. Ophthalmol. Vis. Sci. 65 (5), 4 (2024).
Lloyd, D. Encystment in Acanthamoeba castellanii: A review. Exp. Parasitol. 145, S20–S27 (2014).
Lorenzo-Morales, J., Khan, N. A. & Walochnik, J. An update on Acanthamoeba keratitis: diagnosis, pathogenesis and treatment. Parasite 22, 10 (2015).
Hendiger, E. B. et al. Silver nanoparticles conjugated with contact lens solutions May reduce the risk of Acanthamoeba keratitis. Pathogens 10, 583 (2021).
Padzik, M. et al. Tannic acid–modified silver nanoparticles in conjunction with contact lens solutions are useful for progress against the adhesion of Acanthamoeba spp. To contact lenses. Microorganisms 10, 1076 (2022).
Hkiri, S. et al. Silver(I)-NHC complexes as Dual-Action agents against pathogenic Acanthamoeba trophozoites: Anti-Amoebic and Anti-Adhesion activities. Int. J. Mol. Sci. 26, 9393 (2025).
Jung, J. W. et al. Amoebicidal effect of nephrite-containing contact lens storage case. J. Korean Ophthalmol. Soc. 58, 509–515 (2017).
DreamCon Co. Method for Preparing a CLs inserted coloring in lens and the contact lens prepared by the method. Korea patent. https://patents.google.com/patent/KR101190303B1/en (2012).
Yeom, M. J. et al. In vitro Inhibition of pro-inflammatory mediator mRNA expression by nephrite in lipopolysaccharide-induced mouse macrophage cells. Korean J. Orient. Physiol. Pathol. 18, 1622–1627 (2004).
Funding
This work was supported by a Junior Faculty Support Program of Pusan National University.
Author information
Authors and Affiliations
Contributions
J.H.P conducted the experiment, analyzed the results and wrote the paper. C.H.C, J.H.A, S.K, S.M.L and S.M conceived the experiment and analyzed the results. E.J.C, T.J and J.E.L conceived the experiment, analyzed the results and wrote the paper. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Park, J.H., Cho, C.H., Ahn, J.H. et al. Anti-amoebic and biocompatible properties of nephrite-embedded contact lenses. Sci Rep 16, 11114 (2026). https://doi.org/10.1038/s41598-026-38469-9
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-38469-9