Abstract
Heart rate variability (HRV) is a clinical marker used to assess autonomic function, and the application of filtering algorithms may significantly influence data quantification and interpretation. Although HRV has been extensively studied in individuals with type 2 diabetes mellitus (T2DM), the impact of artefact correction methods remains underexplored. To evaluate the effects of different artefact correction filters in Kubios software on short-term HRV parameters in individuals with T2DM. This cross-sectional, descriptive, and observational study included adults (≥ 18 years) diagnosed with T2DM. Anthropometric and metabolic data were collected, including fasting blood samples for glucose, insulin, and lipid profiles. HRV indices were analyzed across time-domain, frequency-domain, nonlinear, and global metrics. Statistical analysis was performed using ANOVA or Friedman tests according to data distribution, with significance set at p < 0.05. The sample consisted of 52 individuals (67% male, mean age 52 ± 8 years, mean BMI 29.65 ± 5.50 kg/m²). The median duration of T2DM was 3 years (IQR 1.5–10). Median metabolic parameters were insulin 12.50 µU/mL, triglycerides 141.50 mg/dL, fasting glucose 149.50 mg/dL, and HbA1c 8.65% (IQR 7.20–10.00). Application of the most restrictive artefact correction setting (“very strong”) in Kubios significantly modified overall HRV as well as time-domain, frequency-domain, and nonlinear parameters (p < 0.05), highlighting its influence on HRV quantification. This study demonstrates that artefact correction filters, particularly the “very strong” setting, substantially affect HRV analysis in individuals with T2DM. Excessively restrictive filtering may distort autonomic metrics and potentially bias interpretation. Standardization of artefact correction methods is essential to ensure accurate and reproducible HRV assessment in clinical and research settings.
Similar content being viewed by others
Introduction
Type 2 diabetes mellitus (T2DM) currently affects more than 450 million individuals worldwide, and projections estimating a rise to over 590 million by 20351 and potentially reaching 700 million by 20452. Poor long-term metabolic control after diagnosis is strongly associated with the development of micro- and macrovascular complications3. Consequently, T2DM is closely linked to a range of comorbid conditions, which remain a leading cause of mortality and morbidity in this population. This is largely attributable to shared pathophysiological mechanisms, including hypertension, obesity, and dyslipidemia3,4. Hyperglycemia is the central metabolic abnormality in T2DM, and the major contributor to the development of cardiac autonomic neuropathy (CAN), a condition characterized by progressive autonomic nervous system (ANS) dysfunction4.
Cardiac autonomic dysfunction in individuals with T2DM has been under investigation since the last century5, enabling clinicians to identify early signs of subclinical CAN, even before overt symptoms appear, since autonomic degeneration may begin in the early stages of the disease6,7. Among the available diagnostic tools, heart rate variability (HRV) has emerged as a reliable and non-invasive biomarker of autonomic function8,9,10. Its acquisition via portable heart rate monitors has demonstrated good inter- and intra-rater reliability in individuals with T2DM11. Nevertheless, technical artifacts, such as sensor misplacement or biological variability, including ectopic beats and arrhythmias, can affect HRV data. These factors can compromise signal quality and R-R intervals stationarity, that is, RR segments whose dynamics remain stable over time, preferably without abrupt shifts in mean heart rate or variability, and presenting good signal quality (i.e., absence of ectopic beats, and artifacts or noise that could influence HRV analysis), potentially leading to biased or unreliable HRV estimates.10.
To address these issues, HRV analysis software such as Kubios incorporates algorithms capable of detecting and correcting artefacts with high sensitivity and specificity. However, a lack of consensus regarding optimal filter selection has led to subjective and potentially inconsistent methodological decisions. This variability threatens both the interpretability and reproducibility of HRV research. Recent studies have highlighted the influence of different filtering strategies on HRV metrics, particularly in short-term recordings (e.g., 5-minute segments), showing that filter choice can substantially alter HRV quantification12,13,14,15,16.
Despite this growing body of evidence, no studies to date have specifically examined the impact of these artefact filters in individuals with T2DM. This gap is particularly relevant because T2DM-related autonomic dysfunction is characterized not only by reduced HRV17, but also by altered signal stationarity and a higher prevalence of ectopic beats and rhythm irregularities18, which may uniquely interact with artefact correction thresholds compared with previously studied populations13,15,19. Considering the clinical value of HRV in reflecting the cardiac autonomic modulation6, current cardiac autonomic balance20, and its established prognostic relevance, this methodological uncertainty is notable21,22,23,24. Moreover, a considerable proportion of HRV studies in diabetic populations fail to report whether or how signal correction was applied, introducing the risk of interpretative bias25,26,27,28,29,30,31,32.
Previous methodological studies indicates that certain HRV parameters, especially short-term time-domain indices, are particularly sensitive to artefacts, with even a small proportion of artefactual beats substantially altering their values33,34. This study aims to evaluate the impact of different artefact filters in Kubios software on short-term HRV parameters in individuals with T2DM. Accordingly, we hypothesize that artefact filter choice influences HRV quantification, particularly for indices reflecting short-term beat-to-beat variability in T2DM.
Methodology
Study design and ethical aspects
This was a cross-sectional, descriptive, and observational study. The research was conducted at the CEUMA University – Renascença Campus, and the study was submitted to the Research Ethics Committee of the institution (protocol number: 4.179.747) and conducted according to Declaration of Helsinki. Volunteer recruitment occurred within the university community, at the outpatient clinics of the Ana Lúcia Chaves Fecury Integrated School-Clinic, and in the city of São Luís – MA through verbal communication, posters, and the internet. All volunteers included in the study signed the Informed Consent Form.
Participants
Eligible participants included adults (≥ 18 years) of both sexes, with a clinical diagnosis of T2DM. The time since diagnosis of T2DM was based on self-report from the date of medical diagnosis. The exclusion criteria included: a history of clinically proven heart disease and/or through exams, uncontrolled hypertension, myocardial infarction (within six months of the start of the study), implanted pacemaker, unstable angina, Type 1 Diabetes Mellitus, participation in a regular physical exercise program at the start of the study, neoplasms, conditions that could compromise the performance of the test, cognitive deficits, difficulty in understanding and/or adhering to study procedures, self-reported illicit drug use, and pregnancy.
Demographic, anthropometric, and self-reported comorbidities characteristics
The demographic and anthropometric variables of the participants were collected, including age, sex, body weight, height, and body mass index (BMI). Age was recorded in complete years at the time of study inclusion. Participants’ sex was categorized as male or female. Body weight was measured using a calibrated scale, and height was determined with a stadiometer, with participants standing barefoot. BMI was calculated using the formula: BMI = weight (kg)/height² (m). Participants self-reported their medical history of comorbidities, which were recorded as present or absent.
Metabolic outcomes
Blood samples were collected from the antecubital vein after a fasting period of 8–12 overnight fast. EDTA-containing tubes without anticoagulants and Vacuette separator gel (Greiner Bio-One, Kremsmünster, Austria) were used. Volunteers were allowed to consume water, but solid food and other beverages were restricted to avoid any influence on the biochemical parameters analyzed. Glycated hemoglobin (HbA1c) was assessed by high-performance liquid chromatography (Variant II, Bio-Rad, Berkeley, California), coupled with a fluorescence detector, a method certified by the National Glycohemoglobin Standardization Program. Plasma insulin was measured in micro-units per milliliter (µU/mL) using a chemiluminescence assay (UniCel DxI 800, Pasadena, California). Insulin resistance was assessed using the homeostasis model assessment (HOMA-IR), calculated by the following formula: fasting plasma glucose (mg/dL) x fasting plasma insulin (µU/mL) / 22.5. Fasting plasma glucose (FPG) was measured in milligrams per deciliter (mg/dL). Total cholesterol (total-C), LDL cholesterol, and HDL cholesterol were quantified using enzymatic methods, with values expressed in mg/dL. Triglycerides were also measured using the same enzymatic method, with values expressed in mg/dL. The VLDL (very low-density lipoprotein) concentration was calculated based on triglycerides, using a standardized formula (VLDL = triglycerides/5), with values also expressed in mg/dL. The Castelli index was calculated based on the ratio of total cholesterol to HDL cholesterol. The LDL/HDL ratio was also calculated, as it is a significant measure for determining the lipid profile. All these variables were measured in the laboratory by a single technician responsible for the procedures. The measurements were performed using the following equipment: AU 680 (Beckman Coulter, Suarlée, Belgium) for lipid and fasting plasma insulin measurement, and UniCel DxI 800 (Pasadena, California) for insulin assays.
R-R intervals recordings
HRV data acquisition adhered to international standards to minimize methodological bias8,10,35. The Polar RS800CX heart rate monitor (Polar Electro Oy Inc., Kempele, Finland) was employed to capture the HRV signal for a duration of 10–15 min at a sampling frequency of 1,000 Hz10. To this end, it was determined that all volunteers would be evaluated in the morning shift, thus avoiding physiological variations due to the circadian rhythm. Prior to the evaluation, volunteers were instructed to refrain from consuming caffeine, alcoholic beverages, and energy drinks of any kind, as well as from engaging in strenuous physical activities in the 24 h leading up to the scheduled evaluation time. Environmental conditions were controlled: the environment was air-conditioned, with a temperature ranging from 22 to 24 °C and relative humidity between 50 and 60%. At the time of evaluation, volunteers remained at rest in the supine position, breathing spontaneously, for 15 min to allow the heart rate signal to stabilize before data collection.
Data processing
HRV data were processed using Kubios HRV Standard software, version 3.5 (Kubios Ltd., Kuopio, Finland; https://www.kubios.com)36. Kubios software is an easy-to-use HRV analysis tool, including a wide variety of analysis options in overview variables, time domain, frequency domain, and nonlinear domain36. The data were analyzed within stable sessions containing 5-minute periods based on the selection of the segment with the highest signal stationarity, as visually inspected by a single experienced evaluator (> 10 years of experience in HRV signal analysis)10,37. The following criteria were adopted to select the longest stationary period: (1) no large discrepant values in the R–R interval (i.e., an R–R interval much higher or lower than the entire R–R signal, based on visual inspection of the HRV record performed by the researcher), (2) equidistance of the R–R intervals, and (3) approximately Gaussian R–R interval and heart rate distributions, assessed using the histogram tools available in Kubios10,19.
To obtain the results, all available filters in the Kubios software were used on the same 5-minute period. The beat correction algorithm based on a threshold compared each R-R interval value with a local average interval. The local average was obtained by median filtering the RR time series, and therefore, the local average was not affected by unique outliers in the RR interval time series. If an R-R interval deviated from the local average by more than a specified threshold, the interval was identified as an artifact and marked for correction. The threshold value could be selected between: (a) None (no correction was applied); (b) Very low: 0.45 s (threshold in seconds); (c) Low: 0.35 s; (d) Medium: 0.25 s; (e) Strong: 0.15 s; (f) Very strong: 0.05 s36.
Heart rate variability parameters
HRV was analyzed using overview variables, linear (time and frequency domains) and nonlinear statistical methods. The overview variables of heart rate variability (HRV) include the Parasympathetic Nervous System index (PNS index), Sympathetic Nervous System index (SNS index), and the Stress Index (SI). The PNS index reflects parasympathetic activity, with higher values indicating greater relaxation and vagal control. The SNS index represents sympathetic activity, typically increasing in alert or stressful situations. The Stress Index is an indicator of sympathetic tone, calculated from the distribution of RR intervals, and rises under conditions of higher physiological stress. Regarding linear time-domain analysis, the standard deviation of all normal NN intervals (SDNN) in ms, the root mean square of successive RR differences (RMSSD) in ms, and the number of successive NN interval differences greater than 50 ms divided by the total number of NN intervals (pNN50) in percentage were obtained. The first was representative of global HRV, while the last two reflected parasympathetic8,10,37. For frequency-domain linear analysis, spectral analysis was performed using Fast Fourier Transform, and components were reported in high frequency (HF) in absolute values (ms²) and normalized units (nu) (0.15–0.4 Hz), reflecting vagal modulation, and low frequency (LF) in absolute values (ms²) and normalized units (nu) (0.04–0.15 Hz), which had predominantly been related to high sympathetic modulation and low parasympathetic8,10,37.
The nonlinear HRV analysis was performed to obtain the standard deviation perpendicular to the identity line (SD1), standard deviation along the identity line (SD2) (representing parasympathetic and sympathetic modulation, respectively), and short-term fluctuation (α1) and long-term fluctuations (α2), where the value one (1) indicated chaotic behavior, one and a half (1.5) corresponded to regularity, and half (0.5) corresponded to randomness8,10,37.
Statistical analysis
Data were presented as mean and standard deviation, absolute values and percentages, or median and interquartile range when appropriate. To test the normality of the data, the Kolmogorov-Smirnov test was used. Because all filter conditions were applied to the same individuals and to the same selected R–R segment, comparisons across filters were treated as within-subject (repeated-measures) analyses. Accordingly, the following tests were used: (1) one-way repeated-measures ANOVA with Tukey-Kramer adjusted post-hoc comparisons when data were normally distributed; and (2) Friedman test with Dunn’s post-hoc test when data were not normally distributed. The sphericity assumption was assessed using Mauchly’s test. When sphericity was violated, degrees of freedom were corrected using the Greenhouse–Geisser method. All analyses were performed using GraphPad Prism software, version 8.0.1 for Windows (GraphPad Software, San Diego, CA, USA; https://www.graphpad.com). The probability of type 1 error occurrence was established at 5% for all tests (p < 0.05).
Results
Table 1 summarizes sociodemographic, clinical, and anthropometric characteristics of the study population. The sample consisted of 52 individuals, with a mean age of 52 ± 8 years and predominance of males (67%). The mean BMI was 29.65 ± 5.50 kg/m². The median duration of T2DM was 3 years (IQR 1.5–10 years).
Regarding metabolic outcomes, the median insulin level was 12.50 µU/mL, triglycerides 141.50 mg/dL, and fasting glucose 149.50 mg/dL. The median QUICKI index was 0.31, and HOMA was 4.38. Lipid profiles showed total cholesterol of 182 mg/dL, HDL of 42 mg/dL, LDL of 109 mg/dL, and VLDL of 27 mg/dL. The mean Castelli index was 4.53 ± 1.19, and the LDL/HDL ratio was 2.73 (IQR 2.18–3.12). HbA1c was 8.65% (IQR 7.20–10.00). Reported comorbidities included systemic arterial hypertension in 50% and dyslipidemia in 69% of the participants.
No beats were corrected under the None, Very Low, or Low filters. Minimal interpolation was observed with the Medium filter (0.03 ± 0.10%), whereas the Strong filter resulted in a small increase (0.41 ± 0.98%). In contrast, the Very Strong filter produced a markedly higher proportion of corrected beats (9.66 ± 11.41%), with values reaching up to 50% in some recordings (Table 2).
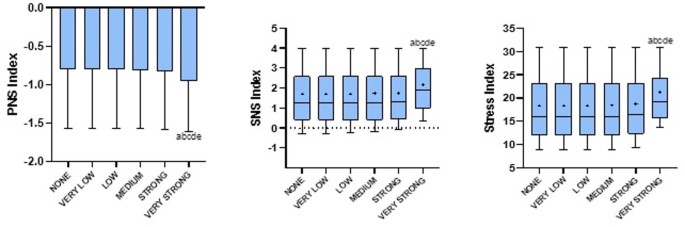
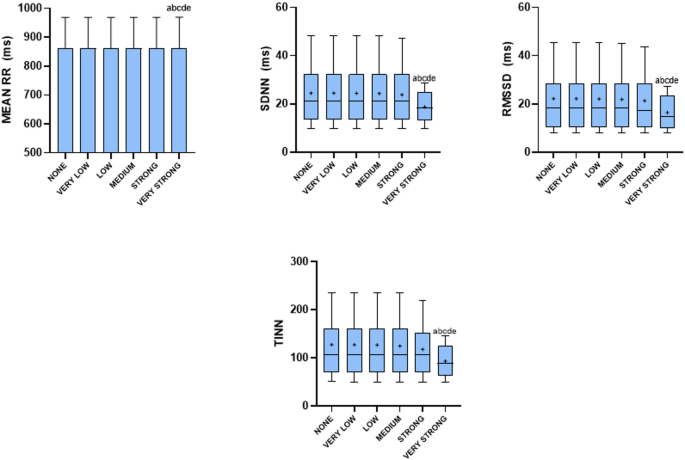
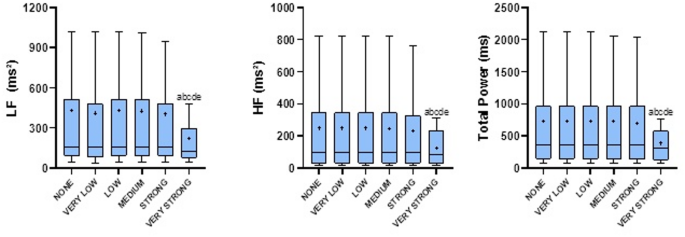
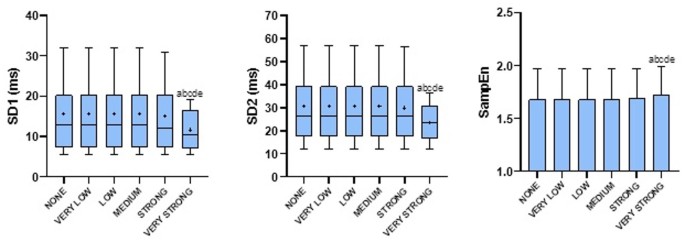
The application of the most restrictive filter of the Kubios software (very strong) resulted in statistically significant alterations in HRV parameters compared to the other filters (none, very low, low, medium, strong) across multiple analytical domains. Specifically, significant differences were observed in the overall parameters (PNS, SNS e Stress Index) p < 0.05 (Fig. 1, p < 0.05). In the time domain analysis, significant changes were found in mean RR interval (ms²), SDNN (ms), RMSSD (ms) and TINN (Fig. 2). Frequency domain parameters including LF (ms²), HF (ms²), and Total Power (ms²) were also significantly affected (Fig. 3). Additionally, in the nonlinear domain, differences were evident for SD1 (ms), SD2 (ms) and SampEn (Fig. 4). Figures for the variables that did not show statistically significant differences across filters are provided in the Supplementary Material.
Impact of corrective filters on overview heart rate variability parameters. Values are presented as mean ± SD or median and interquartile range (10th–90th percentiles). +: represents the mean. PNS: parasympathetic nervous system; sympathetic nervous system. aSignificant statistical difference compared to none; bsignificant statistical difference compared to very low; csignificant statistical difference compared to low; dsignificant statistical difference compared to medium; esignificant statistical difference compared to strong. Statistical significance (p < 0.05) for repeated-measures ANOVA (Tukey–Kramer post-hoc) or Friedman test (Dunn’s post-hoc)..
Effect of corrective filters on time-domain heart rate variability parameters. Values are presented as mean ± SD or median and interquartile range (10th–90th percentiles). +: represents the mean. Mean RR: the average interval between R-waves; ms: milliseconds; SDNN: standard deviation of all N-N normal intervals; RMSSD: square root of the mean squared differences of successive RR; TINN: baseline width of the RR interval histogram. aSignificant statistical difference compared to none; bsignificant statistical difference compared to very low; csignificant statistical difference compared to low; dsignificant statistical difference compared to medium; esignificant statistical difference compared to strong. Statistical significance (p < 0.05) for repeated-measures ANOVA (Tukey–Kramer post-hoc) or Friedman test (Dunn’s post-hoc).
Influence of corrective filters on frequency-domain heart rate variability parameters. Values are presented as mean ± SD or median and interquartile range (10th–90th percentiles). +: represents the mean. HF: high frequency band (0.15–0.40); LF: low frequency band (0.04–0.15); ms²: milliseconds square; aSignificant statistical difference compared to none; bsignificant statistical difference compared to very low; csignificant statistical difference compared to low; dsignificant statistical difference compared to medium; esignificant statistical difference compared to strong. Statistical significance (p < 0.05) for repeated-measures ANOVA (Tukey–Kramer post-hoc) or Friedman test (Dunn’s post-hoc).
Impact of corrective filters on nonlinear heart rate variability parameters. Values are presented as mean ± SD or median and interquartile range (10th–90th percentiles). +: represents the mean. HF: high frequency band (0.15–0.40); LF: low frequency band (0.04–0.15); ms²: milliseconds square; aSignificant statistical difference compared to none; bsignificant statistical difference compared to very low; csignificant statistical difference compared to low; dsignificant statistical difference compared to medium; esignificant statistical difference compared to strong. Statistical significance (p < 0.05) for repeated-measures ANOVA (Tukey–Kramer post-hoc) or Friedman test (Dunn’s post-hoc).
Discussion
The objective of this study was to assess the impact of different artifact correction filters in the Kubios software on the quantification of HRV variables in T2DM volunteers. The key finding was that the most restrictive filter, i.e., the “very strong”, produced significantly different HRV outputs compared with less restrictive settings, even when applied to a highly stationary RR segment. These results highlight the methodological sensitivity of HRV metrics to artifact correction intensity and suggest that overly restrictive filtering may substantially influence autonomic indices, potentially affecting their interpretation.
T2DM is known to adversely affect autonomic nervous system, contributing to a range of cardiovascular complications including postural hypotension38, resting tachycardia39,40, increased risk of arrhythmias41, silent myocardial ischemia39,42, decreased HRV17,43, and increased risk of sudden death39. The characteristic reduction in HRV reflects a shift toward sympathetic dominance and impaired parasympathetic modulation, which can accelerate cardiovascular disease progression in this population17. Interestingly, autonomic dysfunction often precedes clinical symptoms, underscoring the utility of HRV as an early detection tool for the subclinical diabetic autonomic neuropathy43.
However, from data acquisition to processing, HRV-based assessment of autonomic function is susceptible to a range of confounding factors, physiological, environmental, and technical, that must be rigorously controlled to ensure the accuracy of interpretations10. Beyond external factors, the selection of the stationary signal segments and the application of correction algorithms are critical steps that can significantly influence the reliability of HRV metrics, and, by extension, their clinical utility10,19. Artifacts, signal noise, and errors in R–R interval detection can distort true physiological signals. While manual review and correction algorithms help mitigate these effects, they introduce variability depending on the filtering threshold applied.
Previous studies have already confirmed the role of artifact correction in HRV analysis and highlighted the influence of filtering algorithms, especially those implemented in the Kubios software13,14,15,19. Despite this, there remains no consensus on optimal filtering strategies, and many HRV-based studies fail to report filter settings, limiting reproducibility and comparability across investigations.
In populations with comorbid conditions, such as individuals with COPD, prior evidence suggests that artifact correction filters can affect HRV outcomes across multiple domains and disease severities13. For instance, in patients with non-exacerbated COPD and exacerbated COPD (GOLD I–II), the most restrictive filters (“strong” and “very strong”) produced significant differences in SDNN and RMSSD compared with less restrictive filters, whereas pNN50% was affected mainly by the “very strong”. In non-exacerbated COPD with more severe airflow limitation (GOLD III–IV), the “very strong” filter was the only setting that differed across SDNN, RMSSD and pNN50% variables. Importantly, in exacerbated COPD (GOLD III–IV), even less restrictive filters (including “low” and “medium”) influenced SDNN and RMSSD, suggesting a broader sensitivity to preprocessing choices in that cohort13. The proportion of corrected beats also varied substantially across filter settings and subgroups, ranging from 0 to 32.00% in non-exacerbated GOLD I–II and from 0 to 39.51% in non-exacerbated GOLD III–IV, while exacerbated groups showed lower mean correction rates (0–3.42% in GOLD I–II and 0–1.12% in GOLD III–IV). A plausible physiological explanation for this difference is that COPD, particularly during exacerbations, is characterized by marked ventilatory instability44, hypoxemia-related autonomic fluctuations44, and a higher prevalence of ectopic beats45, which may increase non-stationarity and amplify the impact of even less restrictive correction settings.
Similarly, in a cohort of children, young adults, and middle-aged adults, artifact correction with very strong filters resulted in interpolation of up to 39% of data in children, 33% in young adults, and 17% in middle-aged adults. In this study significant differences were observed in time-domain HRV indices across filters in all cohorts, including SDNN, RMSSD, and pNN50 (all p < 0.001). Post-hoc Bonferroni analyses indicated that in children, even less restrictive settings (e.g., very low and low) already produced significant differences when compared with no filtering. In young adults, significant changes emerged mainly under low filtering for SDNN and RMSSD, and under medium filtering for pNN50. In contrast, in middle-aged adults, SDNN, RMSSD, and pNN50 remained largely similar across filters, except when the very strong filter was compared with the other settings, suggesting that the impact of filtering becomes more selective in older cohorts19.
Likewise, in individuals with temporomandibular dysfunction, the application of the very strong filter also showed significant differences when compared to the none filter and impacted results in all HRV domains (overview, time domain, frequency domain, and nonlinear analysis)15. In our T2DM cohort, the filter-induced changes appeared comparatively more selective and were mainly evident under the “very strong” setting, indicating an attenuated pattern relative to cohorts in which even less restrictive filters produced significant shifts in HRV indices. This pattern may be partly explained by the lower proportion of corrected beats under mild-to-moderate settings in our dataset, making differences detectable mainly when correction becomes substantial.
Although our study design does not allow the identification of an optimal filter, it does allow the identification of potentially problematic filtering choices. Our findings indicate that the primary concern is the indiscriminate use of the “very strong” setting, which produced the largest deviations in HRV outcomes. In practice, when short RR segments are highly stationary and of good signal quality, a low proportion of corrected beats is expected, and excessive correction may disproportionately influence HRV metrics. Therefore, our results support a cautious approach, favoring none/low correction whenever feasible and discouraging overly restrictive filtering, particularly in T2DM.
Given the number of HRV indices analyzed across multiple domains, the risk of type I error inflation should be considered. Although appropriate post-hoc corrections were applied within each repeated-measures comparison, no additional adjustment was performed across all HRV outcomes. No a priori sample size calculation was performed, as the study was exploratory in nature. Therefore, statistically significant differences should be interpreted with caution.
Clinically, the use of artifact correction filters, as implemented in this study, highlights the importance of methodological standardization to ensure diagnostic accuracy and prognostic reliability. However, our findings show that highly restrictive filtering can substantially influence HRV indices and, consequently, the clinical conclusions drawn. These results underscore the need for transparency and standardization in HRV preprocessing, particularly in clinical populations. Without such consistency, variability in analytical approaches may limit reproducibility and hinder the integration of HRV into clinical practice.
Conclusion
In conclusion, our study highlights the significant impact of corrective filters, particularly the ‘very strong’ filter, on HRV analysis in T2DM patients. The application of highly restrictive filters can lead to overestimation or underestimation of HRV variables, distorting HRV values and affecting the interpretation of cardiac autonomic function. Given the clinical relevance of HRV in monitoring and managing autonomic dysfunction in T2DM, careful and standardized filter selection is essential to ensure accurate, reproducible, and clinically meaningful assessments. Ultimately, standardization of preprocessing parameters including artifact correction is critical for enhancing the reliability of HRV analysis in both research and clinical settings.
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Guariguata, L. et al. Global estimates of diabetes prevalence for 2013 and projections for 2035. Diabetes Res. Clin. Pract. 103, 137–149 (2014).
Galicia-Garcia, U. et al. Pathophysiology of Type 2 Diabetes Mellitus. Int. J. Mol. Sci. 21, 1–34 (2020).
De Rosa, S. et al. Type 2 Diabetes Mellitus and Cardiovascular Disease: Genetic and Epigenetic Links. Front. Endocrinol. (Lausanne). 9, 1 (2018).
Balcıoğlu, A. S. & Müderrisoğlu, H. Diabetes and cardiac autonomic neuropathy: Clinical manifestations, cardiovascular consequences, diagnosis and treatment. World J. Diabetes. 6, 80 (2015).
Ewing, D. J., Martyn, C. N., Young, R. J. & Clarke, B. F. The Value of Cardiovascular Autonomic Function Tests: 10 Years Experience in Diabetes. Diabetes Care. 8, 491–498 (1985).
Benichou, T. et al. Heart rate variability in type 2 diabetes mellitus: A systematic review and meta–analysis. PLoS One. 13, e0195166 (2018).
Wheeler, T. & Watkins, P. J. Cardiac Denervation in Diabetes. Br. Med. J. 4, 584 (1973).
Sassi, R. et al. Advances in heart rate variability signal analysis: joint position statement by the e-Cardiology ESC Working Group and the European Heart Rhythm Association co-endorsed by the Asia Pacific Heart Rhythm Society. Europace 17, 1341–1353 (2015).
Vanderlei, L. C. M., Pastre, C. M., Hoshi, R. A., de Carvalho, T. D. & de Godoy M. F. Basic notions of heart rate variability and its clinical applicability. Rev. Bras. Cir. Cardiovasc. 24, 205–217 (2009).
Catai, A. M. et al. Heart rate variability: are you using it properly? Standardisation checklist of procedures. Brazilian J. Phys. Ther. 24, 91–102 (2020).
Bassi, D. et al. Inter and intra-rater reliability of short-term measurement of heart rate variability on rest in diabetic type 2 patients. J Med. Syst 42 (12):236 (2018).
Alcantara, J. M. A. et al. Impact of using different levels of threshold-based artefact correction on the quantification of heart rate variability in three independent human cohorts. J Clin. Med 9 (2):325 (2020).
Santos-de-Araújo, A. D. et al. Impact of different corrective filters on heart rate variability in chronic obstructive pulmonary disease: conclusions and recommendations for future research. Res. Biomed. Eng. https://doi.org/10.1007/S42600-024-00368-1/FIGURES/3 (2024).
Aranda, C., de la Cruz, B. & Naranjo, J. Effects of different automatic filters on the analysis of heart rate variability with Kubios HRV software. Arch. Med. Deport. 34, 196–200 (2017).
Cutrim, R. C. et al. Impact of applying different levels of threshold-based artifact correction on the processing of heart rate variability data in individuals with temporomandibular disorder. Sci. Rep. 2024. 141 (14), 1–9 (2024).
Ribeiro, G. et al. Can RR intervals editing and selection techniques interfere with the analysis of heart rate variability? Brazilian J. Phys. Ther. 22, 383–390 (2018).
Benichou, T. et al. Heart rate variability in type 2 diabetes mellitus: A systematic review and meta–analysis. PLoS One 13 (4):e0195166 (2018).
Li, A. Q. & Zhang, F. Blood glucose variability impacts heart rate dynamics in older type 2 diabetic and coronary heart disease patients. World J. Diabetes. 16, 110722 (2025).
Alcantara, J. M. A. et al. Impact of using different levels of threshold-based artefact correction on the quantification of heart rate variability in three independent human cohorts. J Clin. Med 9 (2):325 (2020).
Sucharita, S., Bantwal, G., Idiculla, J., Ayyar, V. & Vaz, M. Autonomic nervous system function in type 2 diabetes using conventional clinical autonomic tests, heart rate and blood pressure variability measures. Indian J. Endocrinol. Metab. 15, 198 (2011).
Da Silva, A. K. F., De Rezende Barbosa, D. C., Vanderlei, M. P., Christofaro, F. M., Vanderlei, L. & D. G. D. & C. M. Application of Heart Rate Variability in Diagnosis and Prognosis of Individuals with Diabetes Mellitus: Systematic Review. Ann. Noninvasive Electrocardiol. 21, 223–235 (2016).
Silva, A. K. F., da, Christofaro, D. G. D., Bernardo, A. F. B., Vanderlei, F. M. & Vanderlei, L. C. M. Sensitivity, Specificity and Predictive Value of Heart RateVariability Indices in Type 1 Diabetes Mellitus. Arq. Bras. Cardiol. 108, 255 (2017).
Moraes, D. N. et al. Prognostic Value of Resting Heart Rate and Heart Rate Variability in the 12-lead Electrocardiogram: Mortality Data from the CODE Database. Am. J. Cardiol. 248, 23–31 (2025).
Han, Z. et al. Prognostic value of admission heart rate in patients with ST-segment elevation myocardial infarction: Role of Type 2 diabetes mellitus. BMC Cardiovasc. Disord. 12, 104 (2012).
Lai, Y. R. et al. Feasibility of combining heart rate variability and electrochemical skin conductance as screening and severity evaluation of cardiovascular autonomic neuropathy in type 2 diabetes. J. Diabetes Investig. 12, 1671 (2021).
Monzer, N. et al. The cardiac autonomic response to acute psychological stress in type 2 diabetes. PLoS One 17 (3):e0265234 (2022).
Silva, A. K. F., da, Christofaro, D. G. D., Bernardo, A. F. B., Vanderlei, F. M. & Vanderlei, L. C. M. Sensitivity, Specificity and Predictive Value of Heart Rate Variability Indices in Type 1 Diabetes Mellitus. Arq. Bras. Cardiol. 108, 255–262 (2017).
Da Silva, A. K. F., De Rezende Barbosa, D. C., Vanderlei, M. P., Christofaro, F. M., Vanderlei, L. & D. G. D. & C. M. Application of Heart Rate Variability in Diagnosis and Prognosis of Individuals with Diabetes Mellitus: Systematic Review. Ann. Noninvasive Electrocardiol. 21, 223 (2016).
Silva-E-Oliveira, J., Amélio, P. M., Abranches, I. L. L., Damasceno, D. D. & Furtado, F. Heart rate variability based on risk stratification for type 2 diabetes mellitus. Einstein (São Paulo) 15, 141–147 (2017).
Tuttolomondo, A. et al. Assessment of heart rate variability (HRV) in subjects with type 2 diabetes mellitus with and without diabetic foot: correlations with endothelial dysfunction indices and markers of adipo-inflammatory dysfunction. Cardiovasc. Diabetol. 20, 1–12 (2021).
Wang, K. et al. Heart Rate Variability and Incident Type 2 Diabetes in General Population. J. Clin. Endocrinol. Metab. 108, 2510 (2023).
Veiga, T. P. et al. Braden scale has low reliability in different patients under care in intensive care unit. Rev Assoc. Med. Bras 68 (9):1221-1227 (2022).
Stapelberg, N. J. C., Neumann, D. L., Shum, D. H. K. & McConnell, H. Hamilton-Craig, I. The sensitivity of 38 heart rate variability measures to the addition of artifact in human and artificial 24-hr cardiac recordings. Ann. Noninvasive Electrocardiol. 23, e12483 (2017).
Bourdillon, N., Yazdani, S., Vesin, J. M., Schmitt, L. & Millet, G. P. RMSSD Is More Sensitive to Artifacts Than Frequency-Domain Parameters: Implication in Athletes’ Monitoring. J. Sports Sci. Med. 21, 260 (2022).
Task Force of the European. Society of Cardiology and the North American Society of Pacing and Electrophysiology. Circulation 93, 1043–1065 (1996).
Tarvainen, M. P., Niskanen, J. P., Lipponen, J. A., Ranta-aho, P. O. & Karjalainen, P. A. Kubios HRV - Heart rate variability analysis software. Comput. Methods Programs Biomed. 113, 210–220 (2014).
Shaffer, F. & Ginsberg, J. P. An Overview of Heart Rate Variability Metrics and Norms. Front. Public. Heal. 5, 258 (2017).
D’Ippolito, I., Carlucci, M. A., D’Amato, C., Lauro, D. & Spallone, V. Determinants of Orthostatic Hypotension in Type 2 Diabetes: Is Cardiac Autonomic Neuropathy the Main Factor? Endocr. Pract. 30, 802–809 (2024).
Vinik, A. I., Erbas, T. & Casellini, C. M. Diabetic cardiac autonomic neuropathy, inflammation and cardiovascular disease. J. Diabetes Investig. 4, 4 (2013).
Ewing, D. J., Campbell, I. W. & Clarke, B. F. Assessment of cardiovascular effects in diabetic autonomic neuropathy and prognostic implications. Ann. Intern. Med. 92, 308–311 (1980).
Grisanti, L. A. Diabetes and Arrhythmias: Pathophysiology, Mechanisms and Therapeutic Outcomes. Front. Physiol. 9, 1669 (2018).
Kaze, A. D., Fonarow, G. C. & Echouffo-Tcheugui, J. B. Cardiac Autonomic Dysfunction and Risk of Silent Myocardial Infarction Among Adults With Type 2 Diabetes. J. Am. Hear. Assoc. Cardiovasc. Cerebrovasc. Dis. 12, e029814 (2023).
Wang, K. et al. Heart Rate Variability and Incident Type 2 Diabetes in General Population. J. Clin. Endocrinol. Metab. 108, 2510 (2023).
Wedzicha, J. A. & Seemungal, T. A. COPD exacerbations: defining their cause and prevention. Lancet (London England). 370, 786 (2007).
Rusinowicz, T., Zielonka, T. M. & Zycinska, K. Cardiac Arrhythmias in Patients with Exacerbation of COPD. Adv. Exp. Med. Biol. 1022, 53–62 (2017).
Acknowledgements
To the Foundation to Support Research and Scientific Development and Maranhão Technology (FAPEMA), Coordination for the Improvement of Higher Education Personnel (CAPES), and the National Council for Scientific and Technological Development (CNPq) for their support and commitment to maintaining postgraduate programs in Brazil. Professor Ph.D. Audrey Borghi-Silva is CNPq Research Productivity Scholarship - Level 1B. Professor Ph.D. Daniela Bassi-Dibai is FAPEMA Research Productivity Scholarship.
Funding
This study was funded by a research productivity grant granted by the Foundation to Support Research and Scientific Development and Maranhão Technology (FAPEMA) (process number BEPP-02544/23), and National Council for Scientific and Technological Development (CNPq) (process number: 402329/2023-6).
Author information
Authors and Affiliations
Contributions
Conceptualization: DB, ADS, AB; Data curation: ADS, DB, AB; Formal Analysis: ADS, DB, DSR, LVA, JKF, LARG, MRFD, VPF, MCM, PMS, AB; Validation: ADS, DB, AB; Visualization: ADS, DB, DSR, LVA, JKF, LARG, MRFD, VPF, MCM, PMS, AB; Writing – original draft: ADS, DB; Writing – review & editing: ADS, DB, DSR, LVA, JKF, LARG, MRFD, VPF, MCM, PMS, AB.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval and consent to participate
Approval by the Research Ethics Committee of the Ceuma University (protocol number 4.179.747), and conducted according to Declaration of Helsinki. All participants who voluntarily agreed to participate signed a consent form.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Bassi-Dibai, D., Santos-de-Araújo, A.D., Rocha, D.S. et al. Threshold-based artefact correction methods influence heart rate variability measurements in individuals with type 2 diabetes mellitus. Sci Rep 16, 11341 (2026). https://doi.org/10.1038/s41598-026-42255-y
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-42255-y