Abstract
Cancer cachexia, a multifactorial syndrome of weight loss, muscle wasting, anorexia, and systemic inflammation, often goes unaddressed. Healthcare professionals at Uganda Cancer Institute (UCI) face substantial clinical workloads, limited resources and constrained access to guideline-based practice and limited multi-modal care, all of which adversely affect cancer cachexia recognition and management. To assess UCI professionals’ knowledge levels, practice patterns, and attitudinal barriers regarding cancer-cachexia care. A longitudinal quasi-experimental pre-post study design using mixed methods was conducted among 50 healthcare professionals. Quantitative data were collected using an ASCO/ESMO/GLIM-adapted questionnaire and analyzed with McNemar’s test, Chi-square tests, and Wilcoxon signed-rank tests (STATA-v18). In-depth interviews with 10 purposively selected participants were thematically analyzed using NVivo-v15. Participants were predominantly nurses (72%), the median age was 37 years, with 7 years of oncology experience, 64% were female. At baseline, 44% reported no prior cachexia training and assessments were largely subjective and conflated with malnutrition. Post-intervention, awareness of ASCO guidelines increased significantly to 89%, misconceptions regarding nutritional reversibility declined (p = 0.0097), and confidence in cachexia management rose by 36%. Evidence-based practices, including oral nutrition prioritization (p = 0.024), short-term corticosteroid use (p = 0.025), and anti-inflammatory therapy (p = 0.034), improved significantly. Confidence in management rose by 36% and non-assessment decreased, with modest gains in cachexia-specific assessment. Improving cachexia care in resource-limited settings requires structural integration into routine oncology practice more than individual awareness, through increased staffing, training, leadership, interdisciplinary coordination, and locally adapted guidelines.
Similar content being viewed by others
Background
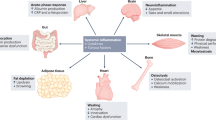
Cancer cachexia, a multifactorial syndrome of involuntary weight loss, muscle wasting, anorexia and systemic inflammation1, affects 80% with advanced malignancies2,3 and leads to 20% of cancer-related deaths4,5. Despite profound impact on prognosis, it remains underdiagnosed and undertreated even in high-resource settings, contributing to disease progression and heightened mortality rendering early detection and identification of predictive biomarkers key for improved survival6,7. Yet in many low- and middle-income countries (LMICs), care is disproportionately focused on tumor control with prioritization of curative over supportive care. In Uganda, cachexia is highly prevalent among patients with advanced cancers, with institutional data from Uganda Cancer Institute (UCI) indicating that approximately 80% of oncology patients present with some degree of cachexia. This neglect stems from complex pathophysiology, poor awareness, limited training, and absent guidelines. This high prevalence underscores the urgent need for awareness, assessment, and structured management of cachexia in this setting. While only a few specialized institutions exist with conventional cachexia care frameworks in high-income countries, most LMICs lack established standardized workflows, leaving cachexia care unaddressed until end-stage and managed through symptomatic relief8,9.
International bodies like American Society of Clinical Oncology (ASCO)10, European Society for Medical Oncology (ESMO)11, and Global Leadership Initiative on Malnutrition (GLIM)12 have outlined evidence-based guidelines. The ASCO guideline emphasizes early recognition of cachexia, symptom assessment, nutritional counseling, and interprofessional management. ESMO outlines multimodal management strategies including early nutrition, exercise, and psychosocial support, while GLIM provides standardized diagnostic criteria for malnutrition aiding early recognition of cachexia. Lim et al. (2024) emphasized effectiveness of dietary counseling, exercise programs, and psychosocial support when integrated early via interprofessional care. However, such comprehensive approaches remain rare in LMICs, where cachexia care is typically reactive, fragmented and subsumed under palliative care with absent structured education, protocols, competing healthcare demands and limited resources widening disparities13,14. In Uganda, patients face challenges to timely diagnosis, treatment, and supportive care due to strained healthcare system with workforce shortages, infrastructure deficits, and financial barriers15. Complex syndromes like cachexia often go unaddressed as observed by poor patient outcomes, lack of assessment tools and locally adapted cancer cachexia guidelines, limited inter-professional coordination, and under-prioritization of supportive care. This study aimed to identify knowledge deficits, attitudinal barriers and practice patterns to inform evidence-based strategies for integrating cachexia care into routine oncology practice.
Methods
Study design, site and population
This study employed a longitudinal quasi-experimental design using a pre- and post-intervention approach with mixed methods to assess changes in healthcare professionals’ knowledge, attitudes, and practices regarding cancer cachexia care at Uganda Cancer Institute (UCI). A leading tertiary facility located in Kampala, UCI is the national referral center for comprehensive oncology care, serving diverse patients from across the country, treating approximately 5,000 patients annually, of which 80% are cachexic. Overall, it employs approximately 170 health professionals in various departments, including nurses, oncologists, medical doctors, nutritionists, counselors, pharmacists and other allied health staff.
Phase one involved quantitative survey of interdisciplinary healthcare professionals. A sample size of 50 oncology professionals was selected based on convenience sampling of the available staff actively engaged in cancer cachexia care at outpatient department at UCI and the study aimed at exploratory assessment of their knowledge attitudes and practices in cancer cachexia rather than infer population-level estimates. Phase 2 comprised in-depth interviews with 10 of these participants purposively sampled for the qualitative component, selected to reflect diverse professional roles and perspectives, and was guided by data adequacy and thematic saturation.
Following baseline assessment, participants underwent a structured educational sensitization intervention on cancer cachexia for three months. The intervention addressed key domains including the definition and stages of cancer cachexia, diagnostic criteria (ASCO, ESMO, and GLIM guidelines), symptom assessment, body composition assessment methods, and multimodal/interdisciplinary management strategies. The intervention was delivered through interactive lectures supplemented with printed educational materials. Post-intervention assessments were conducted using the same instruments.
Data collection
Data collection was conducted from January 2024 to June 2024 by a trained nurse and clinician. Scheduling of interviews considered participant availability to avoid disruption of clinical duties.
Phase 1: participants completed a structured, interviewer-administered questionnaire developed using the ASCO/ESMO/GLIM international guidelines on cancer cachexia diagnosis and management10,11,12. The questionnaire consisted multi-dimensional aspects including: demographics, cachexia definition, pathophysiology, symptomatology, quality of life and management. Phase 2: involved in-depth interviews using a semi-structured guide informed by existing literature on healthcare professionals’ knowledge, attitude and practices in cancer cachexia16,17 and phase 1 quantitative results. It explored domains on definition, conceptual understanding, screening practices, symptomatology, management, caregiver dynamics, multi-modal approach and systemic barriers. Each of the 10 in-depth interviews lasted approximately 30 min, although actual durations varied slightly depending on participant responses. Interviews were conducted until data saturation was achieved, defined as the point at which no new themes emerged from successive interviews, confirming that the sample size was adequate for qualitative analysis.
The questionnaire and interview guide were pre-tested with 5 healthcare professionals (3 nurses and 2 medical officers) at UCI who were not part of the main study sample. The pre-test aimed to assess clarity, relevance, and comprehensibility of the questions. Minor modifications were made based on this feedback including rewording to enhance comprehension. Data from the pre-test were not included in the main study analysis.
Ethical approval
This study complies with the declaration of Helsinki on research involving human subjects. Ethical approval for the study was obtained from the Institutional Review Board of Uganda Cancer Institute (Approval No: UCI-2022-69) and Uganda National Council for Science and Technology (HS3194ES).
Consent to participate and confidentiality
All participants provided written informed consent prior to participation. The study strictly adhered to ethical principles including voluntary participation, confidentiality, anonymization of data, and the right to withdraw at any time without consequences. Identification numbers instead of names were used and data collected were treated with utmost confidentiality.
Data management and analysis
Quantitative data was entered into REDCap and exported to STATA (v18) for analysis. Objective variables including multiple-choices were classified as correct/incorrect (score = 1/0). Subjective variables were rated on a 5-point Likert scale ranging from 1 (very low) to 5 (very high). Responses were either classified as correct/wrong based on 50% cut-off or categorized using Bloom’s criteria (> 80% = good; 60–80% = moderate; <60% = poor)18. For Likert-scale, multiple responses were consolidated e.g. agree and strongly agree were merged. Symptom assessment domains were evaluated both as individual criteria and pooled data to analyze overall pattern of clinician practices and detect meaningful changes following the intervention regarding clinician engagement in cachexia assessment. Descriptive analysis included frequency distributions, percentages, medians, and interquartile ranges to summarize categorical and numerical variables. Categorical variables were further compared using McNemar’s test or Chi-square tests, as appropriate. Paired ordinal data and non-normally distributed variables were analyzed using the Wilcoxon signed-rank test. Statistical significance was defined as a p-value < 0.05.
All in-depth interviews were audio-recorded using a digital Dictaphone, transcribed verbatim, and cross-checked with audio files to ensure accuracy. Recordings were de-identified before analysis to maintain confidentiality. Qualitative data were analyzed using NVivo v15 guided by Braun and Clarke’s thematic analysis framework19. The process included: familiarization with the transcripts, generating initial codes (data reduction), searching for themes, reviewing and refining themes, defining and naming themes and producing the final report. Codes were organized into themes and representative quotes were selected to illustrate key findings. Analysis was carried out by the first author, however all authors read transcripts to enhance credibility and contributed to the analysis and final themes were selected and refined to accurately reflect the views and experiences of participants. Participant quotes are presented verbatim with respondent’s designation to preserve authenticity and highlight critical insights.
Results
Participant demographics
A total of 50 healthcare professionals participated baseline, with 47 completing the post-intervention assessment. Most were trained nurses (72%), medical officers (12%), others [pharmacist, nutritionist, counselor, palliative care] (10%), oncologist (4%) and resident doctor (2%). Median age was 37 years (IQR: 34–47), with 7 years’ oncology experience (IQR: 3.5–13) and 64% were females. Primary sources of information included health professionals (53.6% pre- vs. 46.7% post-intervention), media [mass media, social media, internet] (35.7% vs. 38.3%) and academic resources [publications, conference] (10.7% vs. 15%).
Theme 1: Awareness of cancer cachexia
At baseline, substantial training gaps were evident, with 44% of participants reporting no prior formal education on cancer cachexia. This lack of structured training was echoed in qualitative interviews where participants emphasized the absence of standardized diagnostic guidance and education. Prior to the intervention, interviewees largely relied on subjective assessments and lacked standardized diagnostic tools.
I don’t think there is, like, an SOP in UCI…we even don’t have any entry for BMI – Oncologist 1.
We do diagnosis, but everyone is using their own protocol. Some are using BMI. Some ask how much weight have you lost?….There is no system… No protocol for cachexia. There’s not been any formal training…what should be done – Oncologist 2.
We need to be given knowledge on how to identify… what should we look out for? – Palliative nurse.
There’s no system….it’s clinical, take the history, look at the patient – Medical Officer 1.
We do weight, BSA….used in calculating chemotherapy, so people would not mind about BMI – Medical Officer 2.
Awareness of ESMO and GLIM frameworks remained consistently low (< 50%) across both phases. Although ASCO guideline awareness increased to 89% post-intervention, participants reported minimal exposure to these frameworks underscoring the need for broader dissemination and sustained training on diagnostic criteria and multimodal management. Post-intervention, participants persistently highlighted the need for diagnostic guidance, with continued education and standard guides/tools.
We should be empowered to look out for signs… how to identify… A guide – Palliative nurse.
If I know what I’m doing, I can do it very well… I can help in my capacity and refer– Counsellor.
Despite improved ASCO guideline recognition, only one of the three diagnostic questions achieved over 50%, indicating continued theoretical gaps (Table 1). Pre-intervention, respondents loosely defined cachexia and often conflated it with malnutrition.
It involves excessive wasting. They lose muscle, weight…like over 50%, we qualify them cachexic, 15% no – Medical Officer 1.
Doctors will write in the file… severely malnourished instead – Oncologist 2.
We use terms like muscle wasting, thinness, malnutrition – Female nurse. We actually follow malnutrition classification from nutrition team. I don’t see much difference – Medical Officer 2.
Participants demonstrated high baseline knowledge regarding the clinical features and causes of cancer cachexia. Post-intervention, there was a significant reduction in the misconception that cachexia can be reversed solely with nutritional interventions (p = 0.0097), indicating the effectiveness of the educational intervention in correcting key treatment misunderstandings. Knowledge regarding pathophysiology, psychosocial impact, and differentiation from starvation-related weight loss improved in trends but did not reach statistical significance (Table 2). Symptom recognition remained consistently high in both phases, 54–92% pre- and 59–89% post-intervention, (Supplementary Table S1). Following the intervention, participants reflected a deeper, nuanced understanding of cachexia as a complex, multifactorial syndrome, highlighting areas that may require ongoing training.
Cancer cachexia is a syndrome… it causes to lose muscle, weight…characterized by poor appetite, vomiting, eating-related distress… worsened by chemotherapy – Male nurse.
Malnutrition is one part, but cachexia is more complex – Palliative nurse.
Theme 2: Approaches, attitude and confidence regarding cachexia care
Baseline attitude toward cancer cachexia care was generally positive, however the intervention resulted in significant improvements in evidence-based management perspectives. Participants demonstrated greater recognition that oral nutrition should be the first-line approach and that enteral or parenteral nutrition should not be routinely offered in patients with advanced cancer cachexia (p = 0.024). In addition, understanding of the appropriate short-term use of corticosteroids for appetite stimulation (p = 0.025) and the potential role of anti-inflammatory agents such as NSAIDs (p = 0.034) improved significantly. Participants showed significantly greater agreement that forcing patients to eat is counterproductive and may exacerbate nausea and vomiting (p = 0.0049), patient distress and caregiver strain (p = 0.0034) (Table 3). Pre-intervention interviews reflected limited emotional and professional engagement, as many viewed cachexia inevitable and caregiver burden was under-recognized.
We don’t have practice whereby let’s screen… patients don’t come here because of cachexia –Medical Officer 1.
Maybe it’s because they are all wasted… that’s their nature…they don’t gain much. They come complaining of fatigue, nausea, poor appetite… all cancer patients are naturally weak or wasted – Female nurse.
Caregivers can be informed about right way of feeding – Nutritionist.
Post-intervention, attitude shifted markedly towards empathy, hope and holistic care. Most participants endorsed caregiver support (92%), interdisciplinary care (98%) and early psychosocial interventions (100%) (Supplementary Table S2). Interviewees showed greater sensitivity to caregiver distress and patient emotional burden.
Show them other patients who’ve made it…walk them around – Palliative Nurse.
Show them love, give hope… You’re not the first…Religious leaders to give them word of their soul… because they were depressed – Female nurse.
Tell them your patient may not eat… but it’s not their fault – Male Nurse.
Support is in many ways… giving love, material support, praying for them – Counsellor.
Who is caring? What relation? …The patient feels like they are a burden, they see how hard the caregiver is working….help that person get solutions through counseling… explore options – Palliative nurse.
Confidence regarding cachexia management rose significantly from 28% to 64% post-intervention and care shifted from resignation to active engagement. This gain was mirrored by tangible increase in clinical engagement: the number of participants managing > 20 cachexia cases in the past month rose from zero to 32.
I think I’m at 75%- Female nurse.
Theme 3: Practices and interdisciplinary care
Despite gains in knowledge and attitude, translation into practical application remained suboptimal. Though the proportion of respondents using cancer cachexia-specific guidelines increased from 16% to 42.5%, generally it remained low. This was reflected in the clinical examination with pre-intervention patient assessments being sporadic, poorly structured, and often indistinguishable from general patient care, with low scores across all cancer cachexia specific assessment domains (Supplementary Table S3). Interviewees remarked overwhelming numbers and less time.
We don’t routinely assess cachexia. You can’t do all these alone….the long lines….volume of work. I don’t know who’s responsible…nurse….counselor…whoever…can just take weight…also some people are not competent to do some of these assessments - Oncologist 1.
Before they are given chemo, they are weighed. Others in outpatient… Mostly it’s the nurses… it’s a team effort…doctors can do it if we are thin on ground. No guidelines in place for everyone to know this is important or have it routine – Palliative.
The intervention was associated with a consistent reduction in non-assessment and a modest increase in cancer cachexia-specific assessment across all clinical domains (Fig. 1), demonstrating the intervention effectively improved integration of structured evaluation of cancer cachexia. Though overall, fewer than half of respondents still incorporated cachexia specific assessments or objective measures such as body mass index (BMI), muscle mass, or inflammatory markers into practice, highlighting persistent implementation gaps. With improved recognition interviewees recommended assessing as early as triage and regular visits.
We do weight monitoring per visit… to see, are we gaining, losing? At what percentage are we losing? – Male nurse.
Triage them…ask the patient when did it start… any other symptoms– Female nurse.
Patients found to be at no immediate risk of malnutrition… should be rescreened at regular intervals – Oncologist 2.
Pre-intervention, cachexia care was largely viewed as the nutritionist’s responsibility, and fragmented across teams with role ambiguity. Resource constraints, staffing shortages and lack of coordination hindered consistent practice.
Screening is done by doctor… but ideally, a nutritionist should do it….each visit according to my thinking. But because of staffing, it might be hard - Male nurse.
Nutritionist… on all wards… we use non-pharmacological methods… giving education… numbers tend to be overwhelming… it may not be realistic to have all measured, you’re having one weighing scale – Nutritionist.
Post-intervention, 90% of participants recognized the importance of interprofessional care. Referrals to nutritionists improved, with the number of respondents reporting zero referrals dropping from 54 to 26, showing a positive shift in attitude and practice. Interviewees acknowledged importance of nutritional care but also stressed the need to think beyond, by integrating palliative and psychosocial care.
We tell them about a balance diet….telling the caregiver, don’t force the patient, she should eat what she wants. Also you tell the patient not to demand, what they cannot afford, eat what is at home, as long as you have eaten from all food groups – Counsellor.
Tell the patient, before chemo, take water… eat breakfast. If the patient is vomiting, I’ll intervene… if diarrheating, I’ll rehydrate. We are taking food as medicine…eat small small… not to sit on the whole plate – Female nurse.
Proper treatment of anticipated vomiting …planned for a drug which causes less vomiting otherwise chemotherapy will lead to malnutrition - Oncologist 2.
Distress is managed through counseling, continuous education and helping them relax….let this person talk about their concerns - Palliative provider.
We have social workers, doctors… everybody has a role. – Nutritionist.
Once we have a social worker, counselor, nutritionist, doctor, nurses on ward round—it is key.…psychosocial and logistical support, engage family members, address stressors, and debunk myths – Male nurse.
Despite these improvements, a striking mismatch remained between perceived importance and actual team availability. While nurses and psychologists were widely endorsed as essential, fewer than half reported consistent access to these professionals. Interviewees emphasized severe workforce inadequacy and infrastructure constraints.
We have one nutritionist… the guy has no office… I guess he gets probably 10% of patients… We don’t have a psychologist…. We have about three social workers, but we need a bigger office… we didn’t even have them until recently - Oncologist 2.
Patients don’t get enough information…. Each should undergo counseling before treatment… more staff are needed… and work as a team. We have only two counselors… one or two nutritionists for this population… they can’t do everything - Male Nurse.
Not everyone will know what to talk about in nutrition…manpower…unavailability of the person who is specialized in that – Counselor.
Theme 4: Systemic gaps and recommendations
Participants consistently identified structural deficiencies including lack of equipment and standardized tools to assess muscle mass, BMI, weight and hand-grip strength. Advanced body composition tools like Dual-Energy X-ray Absorptiometry (DEXA) scans were not available, reflecting a key resource gap in implementing standardized assessments. These limitations hindered standardized cachexia diagnosis and monitoring. Participants called for policy and structural reforms like a nutrition unit, increased staffing, and integration of cachexia screening at all patient contact points. Early education for both patients and caregivers was emphasized to combat misinformation and improve adherence.
You’re having one weighing scale… then you’re having so so many patients – Nutritionist.
Wards should always be having weighing scales… not broken ones….we need to get standardized tools to get accurate results. Counselors should be attached to each ward, not just one for whole hospital - Female nurse.
We need to set up a functional nutritional unit….If you can screen earlier then probably we avoid that advancement - Medical officer 2.
Sensitize all health workers at whatever level. Need to integrate psychosocial screening and support in patient journey at every service point and by any health worker… teach every enrolled patient plus their caretakers, they should know what to do. Early, structured patient education can counter misinformation, reduce conflicts, and support better nutritional adherence. – Counselor.
Discussion
This study aimed to assess healthcare professionals’ knowledge, attitudes, and practices (KAP) regarding cancer cachexia care at Uganda Cancer Institute (UCI), and to explore barriers to effective care. Our findings identified gaps while also highlighting promoting strides achieved through a structured educational intervention. These results provide insights into both the challenges and potential strategies for enhancing cachexia care in resource-limited oncology settings.
Pre-intervention, cachexia was reduced to vague labels, “malnutrition” or “wasting”, with nearly 44% of providers lacking formal training contributing to blurred conceptual understanding and reliance on subjective clinical judgement resulting in missed or delayed diagnoses, patterns similarly reported in UK and southern Europe16,20,21,22,23. The absence of standardized diagnostic protocols further reinforced fragmented practice, emphasizing the urgent need for guideline dissemination and structured education24,25,26.
Post-intervention, ASCO guideline awareness jumped to 89%, however routine guideline use remained low (42.5%), undermining consistent evidence-based care, echoing implementation struggles in LMICs27 where guideline awareness does not reliably translate into practice. In 2018, only 8.1% of oncology societies had updated cachexia guidelines28,29 and awareness remained low (15%) even in high-income countries, without supportive systems to enable adoption, hampering early detection and effective practice as in our study30.
Conceptual clarity improved following the intervention, with providers increasingly distinguishing cachexia as a distinct, multifactorial syndrome involving metabolic, inflammatory, and psychosocial mechanisms rather than isolated nutritional failure31. While symptom recognition as a clinical red flag was already high at baseline, assessment remained largely subjective and inconsistent without standardized diagnostic tools echoing findings from international surveys where recognition is high but formal diagnostic criteria are rarely applied21,32.
Pre-intervention attitudes reflected therapeutic nihilism, emotional disengagement, and a perception of cachexia as inevitable, findings consistent with reports from the UK and other settings where lack of guidance and time constraints contribute to clinician disengagement17,33. Following the intervention, confidence improved markedly, accompanied by a shift toward active engagement and greater empathy toward patients and caregivers.
Care ethos shifted from viewing cachexia as inevitable17, to being recognized as modifiable and deserving of interdisciplinary, empathetic care and caregiver support34. Importantly, the intervention corrected key treatment misconceptions, including the belief that cachexia is reversible through nutrition alone, and reinforced evidence-based principles such as prioritizing oral intake, judicious use of corticosteroids, and avoidance of force-feeding. These changes align with international recommendations advocating multimodal, patient-centered care35,36. The observed rise in confidence and active case management suggests that even low-cost educational interventions can meaningfully influence clinician attitudes and perceived self-efficacy.
Pre-intervention assessments were largely ad-hoc, implicit and inconsistently applied, lacking formal frameworks with objective measures such as BMI, muscle mass, hand-grip strength or inflammatory markers rarely incorporated9,37. Although cachexia-specific assessments increased post-intervention, overall uptake remained below 50%, reflecting persistent structural and workflow barriers rather than lack of intent. Despite improvements in knowledge and attitudes, translation into practice remained persistently limited particularly in diagnostic linkage. Similar gaps between knowledge and implementation have been reported in Japan38. The intervention also prompted growing interest in triage-based and routine screening models, signaling a shift toward embedding cachexia care within standard oncology workflows.
Management knowledge boosted particularly in evidence-based non-pharmacological strategies widely adopted post-intervention and consistent with African palliative care models39. However, skepticism toward pharmacologic options persisted likely due to limited confidence and concern about side effects, reflecting global trends40. However, implementation was hindered by workforce shortages, time constraints, limited equipment and screening tools, lack of structured workflows with unclear role allocation, and prioritization of curative care over supportive measures, barriers seen in LMICs underscoring that education alone is insufficient and requires coupling of systemic-level reinforcement to produce sustainable practice change38,41.
Care delivery before the intervention was siloed, with cachexia management largely delegated to overburdened nutritionists. Post-intervention, participants increasingly recognized cachexia care as a shared, interdisciplinary responsibility involving doctors, nurses, nutritionists, social workers, counselors and palliative care providers. Referral patterns improved, and the psychosocial and caregiver dimensions of cachexia were more consistently acknowledged36. However, a disconnect persisted between perceived importance and actual service availability due to fragile infrastructure, limited staffing, absent tools, and inadequate space, challenges similar to those reported in Japan, where intent to implement multimodal care outpaced capacity, highlighting that interdisciplinary care cannot be realized without institutional investment42.
The persistent gap between awareness and action observed in this study underscores a critical implementation challenge. Effective integrated cachexia care requires more than knowledge, it demands enabling systems anchored in ongoing education, leadership framework, mentorship, and institutional investment in staffing, referral pathways and workflow adaptation16,43,44. Institutional models from Australia demonstrate that structured clinician- or nurse-led programs integrated into routine oncology care can successfully operationalize multimodal cachexia management even in constrained settings through medical (BMI, muscle mass) and patient-centered (QoL, symptoms) outcome tracking via team-based delivery45,46,47.
Participants’ recommendations for institutional reforms including functional nutrition units, standardized screening tools, routine triage protocols, early patient and caregiver education, and formalized interprofessional coordination represent pragmatic, context-appropriate strategies. Without these foundational pre-requisites, gains in knowledge and attitude, risk remaining underutilized, and meaningful practice will remain suboptimal, rendering the burden of cachexia to be silently endured continuously, an experience echoed across LMICs48.
Strengths
This study is the first at the Uganda Cancer Institute (UCI) to focus on a neglected area of cancer cachexia care in LMICs addressing a significant knowledge and practice gap while providing actionable insights for improvement following a structured and tailored educational intervention. Its mixed-methods design captured measurable changes and rich contextual data. Conducted at the Ugandan national referral center, the study lends context-specific findings relevant to real-world challenges in a high-burden, low-resource African oncology center. Inclusion of diverse professional roles provided a broad holistic perspective for designing integrated, multimodal cachexia management strategies in low-resource settings. While interviewer-administered surveys reduced social desirability bias, verbatim quotes enhanced authenticity and credibility.
Limitations
The single-institution design scope may limit generalizability beyond to similar LMIC oncology settings. The quasi-experimental pre–post design lacked a control group, limiting the ability to attribute observed changes solely to the educational sensitization and precluding causal inference. The post-intervention assessment captured short-term changes in knowledge and practices and did not evaluate long-term retention or sustainability of observed improvement. The intervention did not directly address systemic constraints, which continued to limit practice improvements. Self-reported measures may have introduced potential recall and social desirability bias.
Conclusion
The findings highlight that cancer cachexia care was influenced by multiple interconnected factors including knowledge gaps, limited training, resource constraints and system-level challenges. Targeted educational intervention markedly improved knowledge and fostered nascent efforts towards a more compassionate and informed care ethos however, translating this progress into routine clinical practice remained limited by systemic barriers including underuse of diagnostic criteria and absence of standardized guidelines, fragmented workflows and staff shortages.
Meaningful shifts are possible even in resource-limited settings. Educating providers is essential but insufficient, moving forward, the challenge lies not in convincing providers what to do, but in equipping them to do it. Sustainable change will require more than individual awareness, it demands structural reforms with clinical leadership frameworks, context-specific adapted care models, locally tailored clinical guidelines and training curricula, investment in ongoing professional development, multi-disciplinary coordination and policies to embed cachexia care into routine mainstream oncology for long-lasting impact.
Pre vs. Post-intervention Assessment Practices across Symptom Domains.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Fearon, K. et al. Definition and classification of cancer cachexia: an international consensus. Lancet Oncol. 12 (5), 489–495 (2011).
von Haehling, S. & Anker, S. D. Prevalence, incidence and clinical impact of cachexia: Facts and numbers—Update 2014. J. Cachexia Sarcopenia Muscle 5(4), 261–3 (2014).
Von Haehling, S. & Anker, S. D. Cachexia as a major underestimated and unmet medical need: Facts and numbers. J. Cachexia Sarcopenia Muscle 1(1), 1–5 (2010).
Lim, S., Brown, J. L., Washington, T. A. & Greene, N. P. Development and progression of cancer cachexia: Perspectives from bench to bedside. Sports Med. Health Sci. 2(4), 177–85 (2020).
Hariyanto, T. I. & Kurniawan, A. Cachexia in Cancer Patients: Systematic Literature. (2020).
Mariean, C. R., Tiucă, O. M., Mariean, A. & Cotoi, O. S. Cancer cachexia: New insights and future directions. Cancers (Basel) https://doi.org/10.3390/cancers15235590 (2023).
Unger, J. M., Vaidya, R., Hershman, D. L., Minasian, L. M. & Fleury, M. E. Systematic review and meta-analysis of the magnitude of structural, clinical, and physician and patient barriers to cancer clinical trial participation. JNCI. J. Natl. Cancer Inst. 111(3), 245–55 (2019).
Shankar, A. et al. Supportive care in cancer cachexia: Meeting the unmet need. Asian Pac. J. Cancer Care 7(1), 155–60 (2022).
Gaafer, O. U. & Zimmers, T. A. Nutrition challenges of cancer cachexia. JPEN. J. Parenter. Enteral Nutr. 45(S2), 16–25 (2021).
Roeland, E. J. et al. Management of cancer cachexia: ASCO guideline. J. Clin. Oncol. 38(21), 2438–53 (2020).
Arends, J. et al. Cancer cachexia in adult patients: ESMO Clinical practice guidelines☆. Esmo. Open. 6(3), 100092 (2021).
McGovern, J., Skipworth, R. J., Laird, B. J. & McMillan, D. C. Global Leadership Initiative on Malnutrition cachexia: An inflammation-first approach for the diagnosis of disease-related malnutrition. Curr. Opin. Clin. Nutr. Metab. Care. 27(5), 393–396 (2024).
Bertocchi, E. et al. Cancer cachexia: A scoping review on non-pharmacological interventions. Asia. Pac. J. Oncol. Nurs. 11(5), 100438 (2024).
Sharma, B. & Dabholkar, T. A knowledge, attitude, and practice survey on oncology healthcare professionals’ awareness of cancer cachexia diagnosis and its management: a cross-sectional study. J. Clin. Diagn. Res. https://doi.org/10.7860/JCDR/2024/65035.19184 (2024).
Nakaganda, A. et al. Challenges faced by cancer patients in Uganda: Implications for health systems strengthening in resource limited settings. J. Cancer. Policy. 27, 100263 (2021).
Scott, D., Reid, J., Hudson, P., Martin, P. & Porter, S. Health care professionals’ experience, understanding and perception of need of advanced cancer patients with cachexia and their families: The benefits of a dedicated clinic. Bmc. Palliat. Care. 15(1), 100 (2016).
Millar, C., Reid, J. & Porter, S. (eds) Healthcare professionals’ response to cachexia in advanced cancer: a qualitative study (Oncology nursing forum, 2013).
Bloom, B. S., Engelhart, M. D., Furst, E. J., Hill, W. H. & Krathwohl, D. R. Taxonomy of Educational Objectives (Longmans, Green, 1964).
Braun, V. & Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 3(2), 77–101 (2006).
Koroušić Seljak, B., Mlakar Mastnak, D., Mrevlje, Ž., Veninšek, G. & Rotovnik Kozjek, N. A multi-center survey on hospital malnutrition and cachexia in Slovenia. Eur. J. Clin. Nutr. 74 (3), 419–426 (2020).
Baracos, V. E. et al. Identification and management of cancer cachexia in patients: Assessment of healthcare providers’ knowledge and practice gaps. J. Cachexia. Sarcopenia. Muscle. 13(6), 2683–96 (2022).
Churm, D., Andrew, I. M., Holden, K., Hildreth, A. J. & Hawkins, C. A questionnaire study of the approach to the anorexia–cachexia syndrome in patients with cancer by staff in a district general hospital. Support. Care Cancer. 17 (5), 503–507 (2009).
Socratous, G., Cloconi, C., Tsatsou, I. & Charalambous, A. Nurses’ knowledge in relation to the anorexia-cachexia syndrome in cancer patients: A cross-national comparison in two European countries. SAGE Open Nurs. 7, 23779608211035208 (2021).
Kaduka, L. et al. Malnutrition and cachexia among cancer out-patients in Nairobi, Kenya. J. Nutr. Sci. 6, e63 (2017).
Meza-Valderrama, D. et al. Sarcopenia, malnutrition, and cachexia: Adapting definitions and terminology of nutritional disorders in older people with cancer. Nutrients 13(3), 761 (2021).
Wiegert, E. V. M., de Oliveira, L. C., Calixto-Lima, L., Mota e Silva Lopes, M. & Peres, W. A. F. Cancer cachexia: Comparing diagnostic criteria in patients with incurable cancer. Nutrition 79–80, 110945 (2020).
McClement, S. E. Toward a holistic understanding of cancer cachexia: Application of the human response to illness model. Asia Pac. J. Oncol. Nurs. 10, 100306 (2023).
Mauri, D. et al. Cancer cachexia: Global awareness and guideline implementation on the Web. BMJ Support. Palliat. Care. 3(2), 155–60 (2013).
Mauri, D. et al. Global coverage and consistency of guideline recommendations for cancer cachexia on the Web in 2011 and 2018. Wspolczesna Onkol. 23(2), 100–9 (2019).
Ellis, J. et al. Health care professionals’ experiences of dealing with cancer cachexia. Int. J. Clin. Oncol. 28(4), 592–602 (2023).
Donohoe, C. L., Ryan, A. M. & Reynolds, J. V. Cancer cachexia: Mechanisms and clinical implications. Gastroenterol. Res. Pract. 2011, 601434 (2011).
Del Fabbro, E. et al. Health professionals’ attitudes toward the detection and management of cancer-related anorexia-cachexia syndrome, and a proposal for standardized assessment. J. Community. Support. Oncol. 13(5), 181–7 (2015).
Spiro, A., Baldwin, C., Patterson, A., Thomas, J. & Andreyev, H. The views and practice of oncologists towards nutritional support in patients receiving chemotherapy. Br. J. Cancer. 95 (4), 431–434 (2006).
Sanni, Q. A. et al. Cancer multidisciplinary teams in Africa: A narrative review of their role and availability. Cureus https://doi.org/10.7759/cureus.84553 (2025).
Carriero, M. C. et al. Attitudes, knowledge and clinical practice of health professionals towards psychological disorders in cancer patients: An observational study. Diseases 12(7), 141 (2024).
Agarwal, A. et al. Caregiver challenges seen from the perspective of certified home hospice medical directors. Am. J. Hosp. Palliat. Care 39(9), 1023–1028 (2022).
Bianchini, C., Bonomo, P., Bossi, P., Caccialanza, R. & Fabi, A. Bridging gaps in cancer cachexia care: Current insights and future perspectives. Cancer. Treat. Rev. 125, 102717 (2024).
Sato, R., Hayashi, N., Nakayama, N. & Okimura, A. Factors affecting the assessment of cancer cachexia by nurses caring for patients with advanced cancer undergoing chemotherapy: A cross-sectional survey. Asia. Pac. J. Oncol. Nurs. 9(9), 100075 (2022).
Fraser, B. A. et al. Palliative care development in Africa: lessons from Uganda and Kenya. J. Global Oncol. 4, 1–10 (2017).
Zhang, L. & Bonomi, P. D. Treating Cancer Cachexia Should Be Essential in Cancer Care (2024).
Sato, R., Naito, T. & Hayashi, N. Barriers in nursing practice in cancer cachexia: A scoping review. Asia-Pac. J. Oncol. Nurs. 8(5), 498–507 (2021).
Amano, K. et al. Factors associated with practice of multimodal care for cancer cachexia among physicians and nurses engaging in cancer care. JCO Oncol. Pract. 19(8), 602–9 (2023).
Amano, K. et al. Perspectives of health care professionals on multimodal interventions for cancer cachexia. Palliat. Med. Rep. 3(1), 244–54 (2022).
Senesse, P. et al. Management of cancer cachexia and guidelines implementation in a comprehensive cancer center: A physician-led cancer nutrition program adapted to the practices of a country. J. Pain Symptom Manage. 54(3), 387–93.e3 (2017).
Granda-Cameron, C. & Lynch, M. P. Clinical framework for quality improvement of cancer cachexia. Asia-Pac. J. Oncol. Nurs. 5(4), 369–376 (2018).
Naito, T. Nursing management of cancer cachexia: A new frontier. Asia-Pac. J. Oncol. Nurs. 8(5), 442–444 (2021).
Baba, M. R. & Buch, S. A. Revisiting cancer cachexia: Pathogenesis, diagnosis, and current treatment approaches. Asia-Pac. J. Oncol. Nurs. 8(5), 508–18 (2021).
Naito, T. et al. The barriers to interprofessional care for cancer cachexia among Japanese healthcare providers: A nationwide survey. J. Cachexia Sarcopenia Muscle 15(1), 387–400 (2024).
Acknowledgements
We would like to thank the healthcare professionals who participated in this study and shared their valuable time and insights. We also appreciate the support of the research team for facilitating data collection and providing a conducive environment for this work. Finally, we acknowledge the funder and institutional support that made this research possible.
Funding
This research was supported by Pfizer Inc. USA (Grant number: 75890805). The funder had no role in the study design, data collection, analysis, interpretation, or manuscript writing.
Author information
Authors and Affiliations
Contributions
DD: conceptualized the study, designed the study, performed data analysis and interpretation, wrote the first draft, edited and reviewed subsequent drafts.SS: conceptualized the study, designed the study, edited and reviewed subsequent drafts.CK: coordinated the study, supervised data collection, and reviewed subsequent drafts.AB: performed data management, data analysis and interpretation, edited and reviewed subsequent drafts.EA: managed the project and reviewed subsequent drafts.NN: designed the study, data interpretation, supervised the project, edited and reviewed subsequent drafts.All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Darshit, D., Srikant, S., Komukama, C. et al. Addressing gaps in cancer cachexia care among healthcare professionals at Uganda Cancer Institute. Sci Rep 16, 10871 (2026). https://doi.org/10.1038/s41598-026-45419-y
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-45419-y