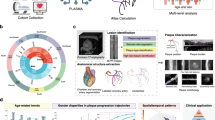
Abstract
The turnover of type I collagen plays an important role in atherogenesis and atherothrombosis. The pro-α1(I) chain of type I collagen (COL1α1) has emerged as a novel circulating biomarker associated with coronary artery disease (CAD) events. This study aimed to investigate the association between circulating COL1α1 and coronary atherosclerosis in a middle-aged general population. Participants (n = 1 078) were randomly recruited from the Linköping branch of the Swedish Cardiopulmonary Bioimage Study (SCAPIS) comprising an equal number of men and women 50–64 years old. Coronary artery calcium scores were calculated from non-contrast computed tomography (CT) while coronary stenosis, presence of plaques and segmental involvement scores were derived from coronary CT angiography. COL1α1, interleukin-6 and matrix metalloproteinase-9 were quantified in plasma. Binary logistic regression models were used. Participants with low COL1α1 levels exhibited a more unfavorable cardiovascular risk profile. There was an inverse association between COL1α1 and all measures of coronary atherosclerosis before adjustment (ORrange=0.50–0.73, p < 0.05 for all). In two multivariable models adjusting for potential confounders and CAD risk factors, an association with coronary stenosis ≥ 50% (OR = 0.61 and 0.59, respectively) and non-calcified atherosclerotic plaques (OR = 0.62 for both) remained (p < 0.05 for all). The findings shed further light on COL1α1 as a potential CAD biomarker.
Similar content being viewed by others
Introduction
Atherosclerosis can go unnoticed for decades before clinical manifestation1. As recently shown in a Swedish population-based study, around 40% of middle-aged (50–64 years) individuals had detectable coronary atherosclerosis on coronary computed tomography angiography (CCTA)2. The synthesis of collagen plays a pivotal role in the initial formation of an atherosclerotic plaque and hence also in subclinical coronary artery disease (CAD). However, this may be followed by a shift promoting collagen degradation with the ensuing risk of plaque rupture, thrombosis and CAD events3,4. Type I collagen, which constitutes around two-thirds of the plaque collagen content, is initially assembled by two pro-α1(I) chains (COL1α1) and one pro-α2(I) chain (COL1α2)4,7 . As recently reported5,6, there was an inverse relationship between plasma levels of COL1α1 and future CAD events that remained intact even after adjustments for established cardiovascular risk factors. As further shown in these studies, COL1α1 was strongly correlated to a marker of type I collagen synthesis (PRO-C1), but neither to markers of inflammation nor collagen degradation. The findings shed light on the role of collagen synthesis in atherosclerosis, possibly independent of inflammation and matrix degradation; the latter being processes that have been extensively investigated previously7,8,9,10,11,12,13.
COL1α1 may thus represent a novel biomarker for cardiovascular risk prediction. However, it is unknown whether this relationship is mediated through the development of atherosclerosis or other mechanisms, such as interaction with coagulation or myocardial vulnerability14. The major aim of the present study was to elucidate whether COL1α1 in plasma was associated with the presence and extent of coronary atherosclerosis as assessed by coronary artery calcium scores (CACS) and CCTA in a subcohort of the Swedish Cardiopulmonary Bioimage Study (SCAPIS) population. In addition, we assessed the associations between COL1α1, clinical characteristics and markers of systemic inflammation and matrix degradation.
Methods
Study population
SCAPIS has been described in detail previously2,15,16,24. In brief, SCAPIS is a nation-wide population-based prospective cohort study that randomly recruited Swedish citizens aged 50–64 (n = 30 154). The present study is based on a subcohort (“SCAPIS Leukocyte”) that randomly included 1 078 subjects (543 men and 535 women) from the Linköping site of SCAPIS (n = 5 058) with the aim of exploring coronary atherosclerosis through flow cytometry-based immune profiling and biomarker quantification. The original SCAPIS protocol had no exclusion criteria except the inability to understand written and spoken Swedish for informed consent; no additional criteria were applied for the subcohort15,17. At study inclusion, blood pressure was measured together with anthropometric measures. Data on smoking status, diabetes, and history of cardiovascular disease along with intake of anti-hypertensive and lipid-lowering medication in the last two weeks was gathered through detailed questionnaires on health and lifestyle. Venous blood samples were collected after an overnight fast for at least 8 h. Blood lipids, plasma glucose, Hemoglobin A1C (HbA1c), high-sensitivity C-reactive protein (CRP) and creatinine were analyzed immediately in the hospital’s core laboratory while plasma was stored at -80 °C for future use. Creatinine levels were used to estimate glomerular filtration rate using the revised Lund-Malmö method18. All participants signed a detailed informed consent, and the study was conducted in accordance with the Declaration of Helsinki. SCAPIS has been approved by the ethical review board in Umeå (number 2010-228-31 M) and a separate ethical application was approved for this sub-study by the ethical review board in Linköping (Dnr 2021-06248-02).
Coronary atherosclerosis
As previously reported, participants were examined by a computed tomography (CT) scan also including a CCTA protocol and systematically assessed for coronary atherosclerosis2,16. CACS was calculated according to international standards on the non-contrast images and categorized as moderate ( ≥100) and high ( ≥400). Presence of any stenosis in any of the main coronary branches (left coronary artery, left anterior descending artery or right coronary artery) was classified into stenosis below 50% or above 50%. In case the calcium content of a coronary artery segment was severe and affected the quantification of stenosis levels, it was classified as having a calcium bloom artefact. Similar to Bergström et al.2, any calcium blooming detected in a segment of the coronary branch was counted as a stenosis below 50%. The presence of coronary plaques (calcified or non-calcified) in any of the coronary segments in the 18 coronary segment model on the contrast-enhanced images were also assessed2. A segmental involvement score (SIS) was calculated as described by Bergström et al.16. SIS is a scoring system where every coronary segment affected by atherosclerosis, irrespective of stenosis degree and including calcium blooming, generates one point. For CACS, data were excluded from analysis due to CT not being performed (n = 5), previous coronary stent (n = 14), or other technical reasons (n = 9). For CCTA, apart from missing CT images, data were excluded if no CCTA-image was captured due to contrast allergy, reduced kidney function, intravenous access failure or non-consent (n = 50) or if there was a technical failure in the four most proximal coronary segments (n = 19) as described previously2.
Biomarker measurements
COL1α1 in Lithium Heparin plasma was quantified using the Magnetic Luminex® Assay (R&D Systems Inc., Minneapolis, MN, USA). Matrix metalloproteinase-9 (MMP-9) was also analyzed in the same assay as a marker of matrix degradation8. Samples were analyzed on a Flexmap 3D analyzer (Luminex corp, Hertogenbosch, Netherlands) platform using the Bioplex manager software (Biorad laboratories, California, USA). The analysis process was performed according to the manufacturer’s instructions and has been described elsewhere19. On each assay plate, 7 duplicates of the standard sample, one duplicate of the blank sample, and two different internal control plasma samples were used. No sample was outside the quantification range. Inter-assay coefficients of variability (CV%) values were 11.1%/6.3% (first control) and 16.4%/5.1% (second control) for COL1α1 and MMP-9, respectively. The Meso Scale Discovery (MSD) platform (Rockville, Maryland, USA), an electrochemiluminescence assay, was used to measure Lithium Heparin plasma concentrations of the cytokine interleukin-6 (IL-6), a marker of systemic inflammation11. The inter-assay coefficient of variation was 22.8%. The IL-6 analysis was made by SciLifeLab, a Clinical biomarkers facility in Uppsala, Sweden.
Statistical analysis
The distribution of normality was tested for continuous variables using the Kolmogorov-Smirnov analysis. Data are shown as median (interquartile range) for variables that were not normally distributed and were analyzed using the Mann-Whitney U test for group comparison of continuous variables. Data with a normal distribution are presented as mean ± standard deviation and were analyzed using Student´s t-test. For categorical variables, the Chi-squared test was used. Spearman correlation analyses were performed where a correlation coefficient > 0.2 generally considered a “poor-to-fair strength” was considered a minimum for clinical relevancy20. To assess the association between COL1α1 and coronary atherosclerosis, logistic regression models were used. Model 1 was a crude model including only COL1α1. Model 2 also included variables with correlation coefficients > 0.2, thus being potential confounders. Lastly, model 3 included established cardiovascular risk factors available in the dataset (sex, waist-hip ratio, age, smoking, use of antihypertensive and lipid-lowering medications, diabetes, HbA1c and CRP)10,13,21. Variables were included in a stepwise manner. COL1α1 levels were analyzed after being log-transformed with the base of 2 in the regression models. A 2-tailed p ≤ 0.05 was used as a cut-off for statistical significance. The SPSS Statistics software (IBM Corporation, Armonk, New York), version 29, was used for statistical analysis.
Results
Participant characteristics and their associations with COL1α1 levels
Baseline characteristics in total and stratified groups according to COL1α1 levels (below or above median), are presented in Table 1. Female sex was more prevalent in the high-COL1α1 group (62% vs. 38%). In the low-COL1α1 group, participants had higher waist-hip ratio, higher systolic blood pressure, and higher levels of glucose, HbA1c and triglycerides while having lower levels of high-density lipoprotein (HDL) cholesterol. This group also used anti-hypertensive and lipid-lowering medication to a larger extent. Also, inflammatory markers (CRP and IL-6) were higher while MMP-9 was lower in the low-COL1α1 group. The glomerular filtration rate was similar between groups. Comparisons were also performed sex-stratified due to the skewness between groups. Amongst the female subjects, differences remained significant regarding waist-hip ratio, diabetes and the use of anti-hypertensive and lipid-lowering medication. The levels of triglycerides, glucose, IL-6, and CRP remained higher while HDL cholesterol and MMP-9 was lower in the low-COL1α1 group compared to the high-COL1α1 group (Supplementary table S1). In the male group, waist-hip ratio and the prevalence of diabetes differences remained between groups. The levels of triglycerides and glucose remained elevated in the low-COL1α1 group (Supplementary table S2). In correlation analysis for the whole cohort, COL1α1 was positively associated with the female sex (r = 0.31, p < 0.001) and HDL (r = 0.26, p < 0.001) while negatively associated with waist-hip ratio (r=-0.31, p < 0.001), glucose (r=-0.26, p < 0.001), and triglycerides (r=-0.22, p < 0.001). There were weak but significant, inverse correlations to the inflammatory markers CRP and IL-6 (r=-0.10, p = 0.002 and r=-0.06, p = 0.05, respectively) while MMP-9 showcased a positive correlation to COL1α1 (r = 0.08, p = 0.01), see supplementary Fig. 1–3.
Relationship between COL1α1 levels and coronary atherosclerosis
In Table 1, the prevalence of coronary atherosclerosis is presented. The low-COL1α1 group exhibited a significantly larger proportion of participants with any coronary stenosis, stenosis ≥ 50%, non-calcified plaques, SIS > 0 and SIS ≥ 4 compared to the high-COL1α1 group. In females, the difference in the prevalence of non-calcified plaques remained significant (Supplementary table S1), whereas for males, this was true for any coronary stenosis ≥ 50% (Supplementary table S2). The associations between COL1α1 levels and coronary atherosclerosis in logistic regression models are presented in in Fig. 1. Lower COL1α1 levels were significantly associated with a higher degree of coronary atherosclerosis, assessed by either CACS or CCTA, in the unadjusted model (model 1, ORrange=0.50–0.71, p < 0.05 for all). After adjusting for sex, waist-hip ratio, fasting glucose, HDL and triglycerides (model 2), COL1α1 remained significantly associated with any stenosis ≥ 50% (OR = 0.61, p = 0.03) and non-calcified plaques (OR = 0.62, p = 0.03). In model 3, the associations to high grade stenosis (OR = 0.59, p = 0.03) and non-calcified plaques (OR = 0.62, p = 0.03) remained after adjustment for cardiovascular risk factors. In both model 2 and 3, the associations were mainly attenuated by the introduction of sex as a variable in the models (supplementary table S3 and S4).
Forest plots showing odds ratios (OR) and corresponding 95% confidence intervals for the association between plasma COL1α1 levels and coronary atherosclerosis unadjusted (model 1); adjusted for sex, waist-hip ratio, fasting glucose, high density lipoprotein cholesterol, triglycerides (model 2); and for sex, waist hip ratio, age, smoking, the usage of antihypertensive and lipid-lowering medications, diabetes, HbA1c and CRP (model 3). COL1α1 levels were analyzed logarithmized with the base of 2. * Indicates remaining statistical significance (p < 0.05). CACS = coronary artery calcium score; SIS = segmental involvement score; COL1α1 = type I collagen pro-a1 chain; CRP = C-reactive protein.
Discussion
The main findings of the study are that COL1α1 in plasma was inversely associated with the presence of coronary atherosclerosis and remained associated with the presence of any coronary stenosis ≥ 50% and non-calcified atherosclerotic plaques after multiple adjustments.
To our knowledge, the findings add to the previously first reported association between plasma COL1α1 and incident coronary events in another Swedish population-based cohort5. Furthermore, in line with the reported association to coronary stenosis ≥ 50%, we have previously reported a significant correlation between COL1α1 levels and prevalent angina pectoris6. In the present study, we also found an inverse and independent association between COL1α1 and non-calcified atherosclerotic plaques. Interestingly, non-calcified plaques have been linked to a higher risk of future cardiovascular events and appear more similar to histological specimens of vulnerable plaques with thin collagen-deficient fibrous caps2,22,23. Recently, a follow-up study of the national SCAPIS cohort (n = 24 791) showed that the presence of noncalcified atherosclerosis was associated with a higher risk of coronary events24.
In a large number of studies, CRP, IL-6 and MMP-9 have been linked to future coronary events8,11,12,13. Also, MMP-9 together with pro-inflammatory mediators has been shown to be abundantly present in high-risk plaques prone to rupture11,12,13,25,26. The weak associations between inflammatory markers and COL1α1 may indicate that they represent different mechanisms in terms of atherogenesis. In line with this, COL1α1 remained associated with both significant (≥ 50%) coronary stenosis and non-calcified plaques independent of CRP levels. Notably, there is an emerging role of collagen biomarkers in a wide range of cardiovascular conditions such as heart failure, aneurysmal disease and CAD7,27,28,29. Although not fully translatable to this setting, a previous study by our group showcased an association between COL1α1 and PRO-C1 (a type I collagen synthesis marker) but not with C1M (a type I collagen degradation marker). The latter has previously been associated with coronary events9,30. As such, COL1α1 builds onto the increasingly recognized role of collagen biomarkers in cardiovascular disease but might represent the less explored synthesis pathway.
When dividing the cohort into a low-COL1α1 and a high-COL1α1 group, it was apparent that COL1α1 levels below the median were associated with several characteristics aligned towards the metabolic syndrome, characterized by abdominal obesity, dyslipidemia, high blood pressure, and fasting glucose35. However, as apparent from sex-stratified analysis, some of these findings can be explained by the large COL1α1 difference between sexes. Based on the multivariable models, these factors may partly explain the relationship between circulating COL1α1 and coronary atherosclerosis with sex showing the largest attenuating effect on the associations. Nonetheless, the association with coronary stenosis ≥ 50% and non-calcified plaques remained despite adjustments for these characteristics.
Elaborating on mechanisms, it should be noted that type I collagen is the main constituent of bone tissue, making COL1α1 a plausible proxy for bone turnover7. Interestingly, bone turnover has been extensively linked to atherosclerosis, making up the basis for the bone-vascular axis concept31,32. Underlining this, one study showcased how a COL1α1 gene polymorphism implicated in osteoporosis was differentially prevalent in myocardial infarction survivors compared to controls33. Also, the relationship between insulin resistance, sex and bone health is well-established, where established bone turnover markers are decreased in diabetics and men – aligning with the relationships presented here34,35. Lastly, due to the wide flora of functions exerted by type I collagen in atherogenesis, it cannot be ruled out that circulating levels of COL1α1 have causal effects on atherosclerosis, vaguely suggested by positive studies on collagen supplementation and cardiovascular risk factors36,37.
Condensing the so far limited evidence on COL1α1 in atherosclerosis, we speculate that low COL1α1 levels could be a marker of a vulnerable plaque phenotype, possibly reflecting the inability to stabilize plaques through type I collagen synthesis3,4,27. Also, it is intriguing to speculate that the COL1α1 biomarker represents different mechanisms in the biology of atherosclerosis compared to inflammatory and matrix degradation biomarkers, possibly leading to different plaque phenotypes3,6,10. Biomarkers that are associated with non-calcified plaques have the potential to become important clinical complements to non-contrast CT that solely detects calcified plaques, the latter considered a more stable form of atherosclerosis2,22,23,26. As discussed, however, several residual confounders could be at play and the exact mechanistic framework for these findings including tissue sources of COL1α1 must be clarified.
One evident limitation of the present study is that it is not possible to link the findings to future events nor infer any causal relationships using a cross-sectional design. Also, being an explorative study with limited statistical power due to few cases with certain coronary characteristics such as high-grade stenosis and non-calcified plaques, we did not correct our analyses for multiple comparisons, increasing the risk for type I errors. The limited prevalence of coronary characteristics also prevented more in-depth exploration using sex-stratified analysis for example. Moreover, data on IL-6 should be interpreted with caution due to high inter-assay coefficients of variation which are probably explained by low concentrations in plasma. The study was conducted in a particular age group in Sweden, making the generalizability to other populations limited.
Conclusion
Low levels of COL1α1 in plasma, possibly reflecting an impaired type I collagen synthesis, were associated with coronary atherosclerosis, in particular coronary stenosis ≥ 50% and non-calcified atherosclerotic plaques, in a population-based Swedish cohort. These findings suggest that COL1α1 has the potential to be used as a biomarker of coronary atherosclerosis, however, this warrants future studies, ideally involving larger cohorts with higher prevalence of atherosclerotic plaques.
Data availability
The data underlying this article are available in the article and raw data can be provided upon reasonable request.
References
Sanchis-Gomar, F., Perez-Quilis, C., Leischik, R. & Lucia, A. Epidemiology of coronary heart disease and acute coronary syndrome. Ann. Transl Med. 4, 256. https://doi.org/10.21037/atm.2016.06.33 (2016).
Bergström, G. et al. Prevalence of Subclinical Coronary Artery Atherosclerosis in the General Population. Circulation 144, 916–929. https://doi.org/10.1161/circulationaha.121.055340 (2021).
Bentzon, J. F., Otsuka, F., Virmani, R. & Falk, E. Mechanisms of plaque formation and rupture. Circ. Res. 114, 1852–1866. https://doi.org/10.1161/CIRCRESAHA.114.302721 (2014).
Rekhter, M. D. Collagen synthesis in atherosclerosis: too much and not enough. Cardiovasc. Res. 41, 376–384. https://doi.org/10.1016/s0008-6363(98)00321-6 (1999).
Ong, K. L. et al. Usefulness of Certain Protein Biomarkers for Prediction of Coronary Heart Disease. Am. J. Cardiol. 125, 542–548. https://doi.org/10.1016/j.amjcard.2019.11.016 (2020).
Hammaréus, F. et al. Plasma type I collagen α1 chain in relation to coronary artery disease: findings from a prospective population-based cohort and an acute myocardial infarction prospective cohort in Sweden. BMJ Open. 13, e073561. https://doi.org/10.1136/bmjopen-2023-073561 (2023).
Martin, E. M., Chang, J., González, A. & Genovese, F. Circulating collagen type I fragments as specific biomarkers of cardiovascular outcome risk: Where are the opportunities? Matrix Biol. https://doi.org/10.1016/j.matbio.2025.03.001 (2025).
Garvin, P., Jonasson, L., Nilsson, L., Falk, M. & Kristenson, M. Plasma Matrix Metalloproteinase-9 Levels Predict First-Time Coronary Heart Disease: An 8-Year Follow-Up of a Community-Based Middle Aged Population. PLoS One. 10, e0138290. https://doi.org/10.1371/journal.pone.0138290 (2015).
Holm Nielsen, S. et al. A biomarker of collagen type I degradation is associated with cardiovascular events and mortality in patients with atherosclerosis. J. Intern. Med. 285, 118–123. https://doi.org/10.1111/joim.12819 (2019).
Libby, P., Ridker, P. M. & Hansson, G. K. Progress and challenges in translating the biology of atherosclerosis. Nature 473, 317–325. https://doi.org/10.1038/nature10146 (2011).
Kaptoge, S. et al. Inflammatory cytokines and risk of coronary heart disease: new prospective study and updated meta-analysis. Eur. Heart J. 35, 578–589. https://doi.org/10.1093/eurheartj/eht367 (2014).
Sarwar, N. et al. Interleukin-6 receptor pathways in coronary heart disease: a collaborative meta-analysis of 82 studies. Lancet 379, 1205–1213. https://doi.org/10.1016/s0140-6736(11)61931-4 (2012).
Cederström, S. et al. Association between high-sensitivity C-reactive protein and coronary atherosclerosis in a general middle-aged population. Sci. Rep. 13, 12171. https://doi.org/10.1038/s41598-023-39051-3 (2023).
Naghavi, M. et al. From vulnerable plaque to vulnerable patient: a call for new definitions and risk assessment strategies: Part I. Circulation 108, 1664–1672. https://doi.org/10.1161/01.Cir.0000087480.94275.97 (2003).
Bergstrom, G. et al. The Swedish CArdioPulmonary BioImage Study: objectives and design. J. Intern. Med. 278, 645–659. https://doi.org/10.1111/joim.12384 (2015).
Bergström, G. et al. Body weight at age 20 and in midlife is more important than weight gain for coronary atherosclerosis: Results from SCAPIS. Atherosclerosis 373, 46–54. https://doi.org/10.1016/j.atherosclerosis.2023.01.024 (2023).
Sandstedt, M. et al. Complete fatty degeneration of thymus associates with male sex, obesity and loss of circulating naïve CD8(+) T cells in a Swedish middle-aged population. Immun. Ageing. 20, 45. https://doi.org/10.1186/s12979-023-00371-7 (2023).
Björk, J. et al. A novel method for creatinine adjustment makes the revised Lund-Malmö GFR estimating equation applicable in children. Scand. J. Clin. Lab. Invest. 80, 456–463. https://doi.org/10.1080/00365513.2020.1774641 (2020).
Zhang, Y., Li, X. & Di, Y. P. Fast and Efficient Measurement of Clinical and Biological Samples Using Immunoassay-Based Multiplexing Systems. Methods Mol. Biol. 2102, 129–147. https://doi.org/10.1007/978-1-0716-0223-2_6 (2020).
Chan, Y. H. Biostatistics 104: correlational analysis. Singap. Med. J. 44, 614–619 (2003).
Yusuf, S. et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet 364, 937–952. https://doi.org/10.1016/s0140-6736(04)17018-9 (2004).
Kral, B. G. et al. Noncalcified coronary plaque volumes in healthy people with a family history of early onset coronary artery disease. Circ. Cardiovasc. Imaging. 7, 446–453. https://doi.org/10.1161/circimaging.113.000980 (2014).
Williams, M. C. et al. Low-Attenuation Noncalcified Plaque on Coronary Computed Tomography Angiography Predicts Myocardial Infarction: Results From the Multicenter SCOT-HEART Trial (Scottish Computed Tomography of the HEART). Circulation 141, 1452–1462. https://doi.org/10.1161/circulationaha.119.044720 (2020).
Bergström, G. et al. Coronary Computed Tomography Angiography in Prediction of First Coronary Events. Jama 335, 245–254. https://doi.org/10.1001/jama.2025.21077 (2026).
Galis, Z. S., Sukhova, G. K., Lark, M. W. & Libby, P. Increased expression of matrix metalloproteinases and matrix degrading activity in vulnerable regions of human atherosclerotic plaques. J. Clin. Invest. 94, 2493–2503. https://doi.org/10.1172/jci117619 (1994).
26 Suzuki, K. et al. Higher Noncalcified Plaque Volume Is Associated With Increased Plaque Vulnerability and Vascular Inflammation. Circ. Cardiovasc. Imaging. 17, e015769. https://doi.org/10.1161/circimaging.123.015769 (2024).
Holm Nielsen, S. et al. Exploring the role of extracellular matrix proteins to develop biomarkers of plaque vulnerability and outcome. J. Intern. Med. 287, 493–513. https://doi.org/10.1111/joim.13034 (2020).
Chirinos, J. A. et al. Endotrophin, a Collagen VI Formation-Derived Peptide, in Heart Failure. NEJM Evid. 1 https://doi.org/10.1056/evidoa2200091 (2022).
Black, K. M. et al. Preliminary biomarkers for identification of human ascending thoracic aortic aneurysm. J. Am. Heart Assoc. 2, e000138. https://doi.org/10.1161/JAHA.113.000138 (2013).
Bertelsen, D. M. et al. Matrix Metalloproteinase Mediated Type I Collagen Degradation is an Independent Predictor of Increased Risk of Acute Myocardial Infarction in Postmenopausal Women. Sci. Rep. 8, 5371. https://doi.org/10.1038/s41598-018-23458-4 (2018).
31 Thompson, B. & Towler, D. A. Arterial calcification and bone physiology: role of the bone-vascular axis. Nat. Rev. Endocrinol. 8, 529–543. https://doi.org/10.1038/nrendo.2012.36 (2012).
Ye, C. et al. Decreased Bone Mineral Density Is an Independent Predictor for the Development of Atherosclerosis: A Systematic Review and Meta-Analysis. PLoS One. 11, e0154740. https://doi.org/10.1371/journal.pone.0154740 (2016).
Speer, G. et al. Myocardial infarction is associated with Spl binding site polymorphism of collagen type 1A1 gene. Acta Cardiol. 61, 321–325. https://doi.org/10.2143/AC.61.3.2014835 (2006).
Szulc, P., Naylor, K., Hoyle, N. R., Eastell, R. & Leary, E. T. Use of CTX-I and PINP as bone turnover markers: National Bone Health Alliance recommendations to standardize sample handling and patient preparation to reduce pre-analytical variability. Osteoporos. Int. 28, 2541–2556. https://doi.org/10.1007/s00198-017-4082-4 (2017).
Biamonte, E., Bendotti, G., Nigro, G., Cavigiolo, B. & Gallo, M. Bone Health in Metabolic Syndrome-Is It a Neglected Aspect of Dysmetabolic-Related Diseases? J. Clin. Med. 14 https://doi.org/10.3390/jcm14165785 (2025).
Adiguzel, E., Ahmad, P. J., Franco, C. & Bendeck, M. P. Collagens in the progression and complications of atherosclerosis. Vasc Med. 14, 73–89. https://doi.org/10.1177/1358863x08094801 (2009).
Jalili, Z. et al. Effects of collagen peptide supplementation on cardiovascular markers: a systematic review and meta-analysis of randomised, placebo-controlled trials. Br. J. Nutr. 129, 779–794. https://doi.org/10.1017/s0007114522001301 (2023).
Acknowledgements
We would like to acknowledge statistician Mats Fredrikson, assistant professor at Forum Ostergotland, Faculty of Medicine and Health Sciences, Linkoping University for his significant statistical support. The authors would also like to acknowledge support of Affinity Proteomics Uppsala at SciLifeLab Sweden and Anna K Lundberg at Linköping university Sweden for providing assistance in protein analyses. Further, we acknowledge the support from Linköping University.
Funding
Open access funding provided by Linköping University. The Swedish SCAPIS trial was mainly funded by the Swedish Heart-Lung Foundation and had considerable support from Knut and Alice Wallenbergs Foundation, Vinnova, the Swedish Research Council and the participating Universities (Uppsala, Umea, Linkoping, Lund, Gothenburg and Karolinska Institute, Stockholm) and University Hospitals (Uppsala Umea, Linkoping, Skane, Sahlgrenska and Karolinska). SCAPIS Linkoping received additional funding from FORSS (the Medical Research Council of Southeast Sweden). For the present study, research support was provided by Academy of Health Care, County Council of Jönköping (Futurum). For this study, the funders had no direct involvement in study design, collection, analysis and interpretation of data, writing of the report or decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
F.H – conception, design of the study; acquisition, analysis, visualization and interpretation of data; drafted the manuscript. L.N - design of the study; interpretation of data; revised the manuscript. R.W.S.C - conception, design of the study; acquisition and interpretation of data; revised the manuscript. F.H.N - conception, design of the study; interpretation of data; revised the manuscript. C.J.Ö - conception, design of the study; acquisition and interpretation of data; revised the manuscript. L.J - conception, design of the study; acquisition, analysis, and interpretation of data; revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hammaréus, F., Nilsson, L., Chung, R.W. et al. Circulating type I collagen pro-α1 chain is inversely associated with the presence of coronary atherosclerosis in a Swedish middle-aged population. Sci Rep 16, 9965 (2026). https://doi.org/10.1038/s41598-026-45736-2
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-45736-2