Abstract
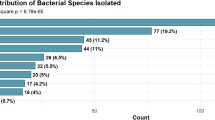
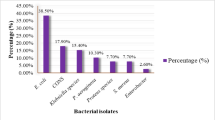
Antimicrobial resistance (AMR) is escalating especially in waterborne bacteria, feared to cause over ten-million annual global deaths by 2050. In Eastern Uganda, bacterial contamination of household drinking water containers and sources such as boreholes is increasingly reported, but data on related AMR and contamination enables are scarce, complicating redress. On 260 random water samples, conventional culture and Kirby-Bauer disk diffusion assays were applied at Makerere University. Pre-validated semi structured questionnaires aided studying the contamination enablers. Thematic synthesis, descriptive and inferential statistics (p < 0.05), were used to analyze data, with STATA version-15. Bacterial (167 isolates), representing eleven species were obtained from 41.2% of samples (mainly from jerricans), mostly Escherichia coli (N = 47, 28.1%), and Klebsiella spp (N = 34, 20.4%). Over 59 (49.2%) of isolates were resistant to at least one high-powered drug; 34% were multi-drug resistant. E. coli showed highest resistance to Cefoxitin (48%), K. pneumoniae to Ceftazidime (28%), and Salmonella spp to Nalidixic acid (70%). Contamination enablers emerged in seven themes, the largest being type of water source (N = 11), and sociodemographic (N = 7). Hence, this water is largely unsafe, and some of these bacteria are associated with persistent epidemics, including typhoid fever in Eastern Uganda, warranting concerted efforts to avert the burden.
Similar content being viewed by others
Data availability
All data generated and analyzed during this study are included in the article.
Abbreviations
- NWSC:
-
National Water and Sewerage Cooperation
- RHRW:
-
Roof-Harvested Rain Water (RHRW)
- SSA:
-
Sub-Saharan Africa
- UBOS:
-
Uganda Bureau of Statistics
- UTI:
-
Urinary Tract Infection
- VHTs:
-
Village Health Teams
- WASH:
-
Water Sanitation and Hygiene
- WHO:
-
World Health Organization
References
Getachew, Z. et al. Diarrheal disease and associated factors among children aged 6 to 59 months in Oda Bultum District, Eastern Ethiopia: a community-based cross-sectional study. BMC Infect. Dis. 24, 303 (2024).
World Health Organization (WHO). Water, Sanitation, Hygiene and Health: A Primer for Health Professionals (2020).
Malema, M. S. et al. Antibiotic-resistant pathogenic Escherichia coli isolated from rooftop rainwater-harvesting tanks in the Eastern Cape, South Africa. Int. J. Environ. Res. Public. Health. 15, 1–14 (2018).
Thomas, M. L. H., Channon, A. A., Bain, R. E. S., Nyamai, M. & Wright, J. A. Household-reported availability of drinking water in Africa: a systematic review. Water (Basel). 12, 2603 (2020).
Olatunji, A. O., Olaboye, J. A., Maha, C. C., Kolawole, T. O. & Abdul, S. Environmental microbiology and public health: advanced strategies for mitigating waterborne and airborne pathogens to prevent disease. Int. Med. Sci. Res. J. 4, 756–770 (2024).
Kristanti, R. A., Hadibarata, T., Syafrudin, M., Yılmaz, M. & Abdullah, S. Microbiological contaminants in drinking water: current status and challenges. Water Air Soil. Pollut. 233, 299 (2022).
WHO. An attempt to identify the likely sources of Escherichia coli harbouring toxin genes in rainwater tanks. Geneva (2011).
UNICEF. United Nations Children’s Fund (UNICEF); World Health Organisation (WHO). Progress on Household. United Nations Children’s Fund (2019).
Tiwari, A. et al. Strengthening pathogen and antimicrobial resistance surveillance by environmental monitoring in Sub-Saharan Africa: a stakeholder survey. Preprint 10 (2024).
Sartorius, B. et al. The burden of bacterial antimicrobial resistance in the WHO African region in 2019: a cross-country systematic analysis. Lancet Glob. Health. 12, e201–e216 (2024).
Ssekandi, N., Tlotleng, N. & Naicker, N. Sociodemographic and environmental factors associated with diarrhoeal illness in children under 5 years in Uganda, 2016: a cross-sectional study. BMC Infect. Dis. 23, 480 (2023).
Geresom, I. & Majwejwe, N. D. Risk factors for diarrhoeal diseases in the under fives in the rural and urban areas of mbale district: a cross sectional-comparative study. Int. J. Sci. Res. Publ. 9, 363–372 (2019).
Walusansa, A. et al. Antibiotic-resistance in medically important bacteria isolated from commercial herbal medicines in Africa from 2000 to 2021: a systematic review and meta-analysis. Antimicrob. Resist. Infect. Control. 11, 1–20 (2022).
Walusansa, A. et al. Global evidence on the potential of some Ugandan herbal medicines to mitigate antibiotic resistance: a meta-analysis across 2½ decades. J. Herb. Med. 41, 100698 (2023).
World Health Organization (WHO). Global Priority List of Antibiotic Resistant Bacteria to Guide Research, Discovery, and Development of New Antibiotics (2018).
Mpairwe, Y. & Wamala, S. Antibiotic resistance in Uganda: situation analysis and recommendations. In Uganda National Academy of Sciences, Kampala, Uganda (2015).
Onanuga, A. & Temedie, T. C. Multidrug-resistant intestinal Staphylococcus aureus among self-medicated healthy adults in Amassoma, South-South, Nigeria. J. Health Popul. Nutr. 29, 446 (2011).
Walusansa, A. et al. High prevalence of antibiotic resistant Escherichia coli serotype O157: H7 among pastoral communities in rural Uganda. Microbiol. Res. J. Int. 2020, 36–43 (2020).
Madhav, S. et al. Water pollutants: sources and impact on the environment and human health. In Sensors in Water Pollutants Monitoring: Role of Material 43–62 (2020).
Guzman-Otazo, J. et al. Conjugative transfer of multi-drug resistance IncN plasmids from environmental waterborne bacteria to Escherichia coli. Front. Microbiol. 13, 997849 (2022).
Logel, G. An investigation of environmental risk factors influencing chorela epidemic in Magale Sub-County, Manafwa District of Eastern Uganda (2017).
Gardell, L. & Behrens, I. Water quality in the Apac, Mbale & Lira districts, Uganda: a field study evaluating problems and suitable solutions. Student thesis series INES (2015).
Burleson, G. E. Integrated evaluation of drinking water purification: a mixed-method laboratory and field assessment of a biomass-powered water treatment technology (2018).
Nayebare, S. R., Wilson, L. R., Carpenter, D. O., Dziewulski, D. M. & Kannan, K. A review of potable water accessibility and sustainability issues in developing countries–case study of Uganda. Rev. Environ. Health. 29, 363–378 (2014).
Okolimong, C. et al. Association of Diarrheal Disease with Solid Waste Management Practices and Perceptions among Residents of Industrial Division in Mbale City: A Cross-Sectional Study (Springer, 2024).
Francis, O. Incidence of diarrhea and contributing factors in Nakaloke Town Council, Eastern Uganda, among children below 5 years of age. IDOSR J. Biol. Chem. Pharm. 8, 52–69 (2023).
Warsame, A. E. et al. The Malaria-Poverty Dilemma in Peri-Urban University Communities in Eastern Uganda (2021).
Cochran, W. G. Sampling Techniques (Wiley, 1977).
Fred Wambede. Mbale city profiling report. Daily mornitor (2020).
Techno. Techno Mobile Limited. Techno Mobile Limited. (2019). https://doi.org/https://www.tecno-mobile.com/ug/phones/product-list/.
Walusansa, A. et al. Medically important bacteria isolated from commercial herbal medicines in Kampala city indicate the need to enhance safety frameworks. Sci. Rep. 12, 1–19 (2022).
Cheesbrough, M. District Laboratory Practice in Tropical Countries, Part 2 (Cambridge University Press, 2006).
Vos, P. et al. Bergey’s Manual of Systematic Bacteriology: Volume 3: The Firmicutes (Springer Science & Business Media, 2011).
Lanyi, B. 1 Classical and rapid identification methods for medically important bacteria. In Methods in Microbiology, vol. 19 1–67 (Elsevier, 1988).
World Health Health Organisation (WHO). Guidelines for Drinking-Water Quality: Fourth Edition Incorporating the First and Second Addenda (2022).
Ministry of Health of the Republic of Uganda. National Guidelines for Management of Common Health Conditions (2023).
Clinical and Laboratory Standards Institute (CLSI). Performance Standards for Antimicrobial Susceptibility Testing (2020).
World Health Organization. Guidelines for Drinking-Water Quality: Second Addendum. Vol. 1, Recommendations (World Health Organization, 2008).
Karmela, K. J. & Lemmens, T. 7th revision of the Declaration of Helsinki: good news for the transparency of clinical trial. Croat Med. J. 50, 105 (2009).
StataCorp, L. L. C. New Stata 18 Statistical Software. Business Wire Newspaper 1–2 (2023). https://www.businesswire.com/news/home/20230426005929/en/New-Stata-18-Statistical-Software-Empowers-Researchers-to-Make-the-Most-Out-of-Their-Analyses.
Carlton, E. J. et al. Heavy rainfall events and diarrhea incidence: the role of social and environmental factors. Am. J. Epidemiol. 179, 344–352 (2014).
Marshall, K. Uganda Institutional Framework for Water Safety and Supply (2023).
Sutti, B. O., Guimarães, L. L., Borges, R. P. & de Braga, S. River flows influence on nutrients (Si, N and P) and fecal coliforms (E. coli) in two tributaries of the estuarine channel of Bertioga (Santos Estuary, São Paulo, Brazil). J. Geosci. Environ. Prot. 10, 26–46 (2022).
Pachepsky, Y. A. & Shelton, D. R. Escherichia coli and fecal coliforms in freshwater and estuarine sediments. Crit. Rev. Environ. Sci. Technol. 41, 1067–1110 (2011).
Faour-Klingbeil, D. et al. Growers’ irrigation practices, knowledge, trust, and attitudes toward wastewater reuse in Lebanon, Jordan, and Tunisia through a food safety lens. Water Pract. Technol. 18, 2619–2637 (2023).
Delair, Z. Implementation of Molecular Methods for the Detection and Characterization of Pathogenic Escherichia Coli: Industrial and Routine Monitoring Applications (University of Johannesburg, 2017).
Devane, P. M. L. Better water quality indicators for understanding microbial health risks (2016).
Hu, Y., Anes, J., Devineau, S. & Fanning, S. Klebsiella pneumoniae: prevalence, reservoirs, antimicrobial resistance, pathogenicity, and infection: a hitherto unrecognized zoonotic bacterium. Foodborne Pathog Dis. 18, 63–84 (2021).
Dweba, C. C., Zishiri, O. T. & El Zowalaty, M. E. Methicillin-resistant Staphylococcus aureus: livestock-associated, antimicrobial, and heavy metal resistance. Infect. Drug Resist. 2018, 2497–2509 (2018).
Bencardino, D., Amagliani, G. & Brandi, G. Carriage of Staphylococcus aureus among food handlers: an ongoing challenge in public health. Food Control. 130, 108362 (2021).
Nath, S. et al. Prevalence of antibiotic-resistant, toxic metal-tolerant and biofilm-forming bacteria in hospital surroundings. Environ. Anal. Health Toxicol. 35, 1452 (2020).
McNeilly, O., Mann, R., Hamidian, M. & Gunawan, C. Emerging concern for silver nanoparticle resistance in Acinetobacter baumannii and other bacteria. Front. Microbiol. 12, 652863 (2021).
Michael, H. Analyzing the connections among water access, sanitation, malaria and diarrhea outcomes in rural Central Uganda. In Undergraduate Thesis in Global Health. Duke University Durham, North Carolina (2016).
Roth, E. The ‘truth about Ebola’: Insecure epistemologies in post-outbreak Forest Guinea. Preprint at (2022).
Van Soest, M. The Political Ecology of Malaria: Emerging Dynamics of Wetland Agriculture at the Urban Fringe in Central Uganda Vol. 4 (Transcript, 2020).
Bishankha, S., Bhatta, D. R., Joshi, D. R. & Joshi, T. P. Assessment of microbial quality of chlorinated drinking tap water and susceptibility of Gram-negative bacterial isolates towards chlorine. Kathmandu Univ. J. Sci. Eng. Technol. 9, 222–229 (2013).
Zhang, M. et al. Viable but non-culturable state formation and resuscitation of different antibiotic-resistant Escherichia coli induced by UV/chlorine. Water Res. 2024, 122011 (2024).
Li, S. N. et al. Enhancement of chlorine-resistant bacteria inactivation via coupling Magnéli phase Ti4O7-based electrochemical oxidation and chlorination. Chem. Eng. J. 2024, 153593 (2024).
Tran, G. H., Tran, T. K., Leu, H. J., Richards, D. & Lo, S. S. An integrated system combining electrochemical oxidation and filtration processes to remove chlorine from pharmaceutical industry wastewater. Arab. J. Chem. 17, 105611 (2024).
Kapasi, Z. F. The immune system and infectious diseases and disorders. in Acute Care Physical Therapy 149–176 (Routledge, 2024).
Sehili, B. Infectious disorders. Nutraceuticals: Holist. Approach Dis. Prevent. 2024, 267 (2024).
Sahu, S. K. et al. Prevalence of acute bacterial infections and their antibiotic sensitivity pattern in children with severe acute malnutrition from a Tertiary Care Hospital of Odisha. Cureus 2024, 16 (2024).
Godwin Olaoye, H. J. Common bacteria found in drinking water distribution systems and their health implications (2024).
Zaragoza, G. et al. Community emergence of cefixime-resistant Escherichia coli belonging to ST12 with chromosomal AmpC hyperproduction. Antibiotics 13, 218 (2024).
Mithuna, R. et al. Emergence of antibiotic resistance due to the excessive use of antibiotics in medicines and feed additives: a global scenario with emphasis on the Indian perspective. Emerg. Contam. 2024, 100389 (2024).
Zhao, C., Wang, Y., Mulchandani, R. & Van Boeckel, T. P. Global surveillance of antimicrobial resistance in food animals using priority drugs maps. Nat. Commun. 15, 763 (2024).
Sharma, E., Chen, Y., Kelso, C., Sivakumar, M. & Jiang, G. Carbapenems and colistin as last-resort antibiotics: a review of challenging environmental impacts and analytical methods. Soil Environ. Health 2024, 100058 (2024).
Éric, K. I. & Papy, H. T. Beta-lactam resistance and phenotypic detection of extended-spectrum beta-lactamase in Entero bacteriaceae isolated from community-acquired urinary tract infections. South. Asian J. Res. Microbiol. 18, 15–24 (2024).
Husna, A. et al. Extended-spectrum β-lactamases (ESBL): challenges and opportunities. Biomedicines 11, 2937 (2023).
Lynch, J. P. & Zhanel, G. G. Escalation of antimicrobial resistance among MRSA part 1: focus on global spread. Expert Rev. Anti Infect. Ther. 21, 99–113 (2023).
Abebe, A. A. & Birhanu, A. G. Methicillin resistant Staphylococcus aureus: molecular mechanisms underlying drug resistance development and novel strategies to Combat. Infect. Drug Resist. 2023, 7641–7662 (2023).
Kumar, N. R., Balraj, T. A., Kempegowda, S. N. & Prashant, A. Multidrug-resistant sepsis: a critical healthcare challenge. Antibiotics 13, 46 (2024).
Lupo, A. Antibiotic resistance: the loud pandemic, dissemination and reservoirs (2023).
Christopher, S. M. Occurrence of antimicrobial pharmaceuticals and characterization of β-lactamases in Gram-negative pathogens from wastewater (2023).
Bradshaw, A. Abundance and absence: human-microbial co-evolution in the Anthropocene. Anthropocene Rev. 11, 26–48 (2024).
Ugoala, E. Antimicrobial drug resistance: a systematic review and assessment of resistant pathogen infection prevention and control (2023).
Meehan, K. et al. Exposing the myths of household water insecurity in the global north: a critical review. Wiley Interdiscipl. Rev.: Water 7, e1486 (2020).
Schaider, L. A., Swetschinski, L., Campbell, C. & Rudel, R. A. Environmental justice and drinking water quality: are there socioeconomic disparities in nitrate levels in US drinking water? Environ. Health. 18, 1–15 (2019).
Shields, K. F., Bain, R. E. S., Cronk, R., Wright, J. A. & Bartram, J. Association of supply type with fecal contamination of source water and household stored drinking water in developing countries: a bivariate meta-analysis. Environ. Health Perspect. 123, 1222–1231 (2015).
Field, K. G. & Samadpour, M. Fecal source tracking, the indicator paradigm, and managing water quality. Water Res. 41, 3517–3538 (2007).
Otchere, S. A. Environmental sanitation behaviours and attitudes of residents in Birim central municipality (2023).
Trevett, A. F., Carter, R. C. & Tyrrel, S. F. The importance of domestic water quality management in the context of faecal–oral disease transmission. J. Water Health. 3, 259–270 (2005).
Aydamo, A. A., Robele Gari, S. & Mereta, S. T. Seasonal variations in household water use, microbiological water quality, and challenges to the provision of adequate drinking water: a case of peri-urban and informal settlements of Hosanna Town, Southern Ethiopia. Environ. Health Insights. 18, 11786302241238940 (2024).
VishnuRadhan, R., Das, S., Hennion, C., Eldho, T. I. & Lonappan, A. Potable water boiling can induce havoc in the water quality management arena due to the presence of microplastics. Cleaner Water 2024, 100019 (2024).
Sürmelihindi, G. & Passchier, C. Writ in water—Unwritten histories obtained from carbonate deposits in ancient water systems. Geoarchaeology 39, 63–88 (2024).
Hardoy, J. E., Mitlin, D. & Satterthwaite, D. Environmental Problems in Third World Cities (Taylor & Francis, 2024).
Onyeaka, H. et al. Preventing chemical contaminants in food: challenges and prospects for safe and sustainable food production. Food Control. 155, 110040 (2024).
Sahoo, S. & Goswami, S. Theoretical framework for assessing the economic and environmental impact of water pollution: a detailed study on sustainable development of India. J. Future Sustain. 4, 23–34 (2024).
World Health Organization (WHO). Guidelines for Drinking-Water Quality (2011).
Food and Agriculture Organisation (FAO). Rural Water Supply and Sanitation: Wells-Pumps (2022).
Krati, S. & Shijin, R. & Nayak, S. K. Water pollution: primary sources and associated human health hazards with special emphasis on rural areas. In Water Resources Management for Rural Development 3–14 (Elsevier, 2024).
Eid, M. H. et al. New approach into human health risk assessment associated with heavy metals in surface water and groundwater using Monte Carlo Method. Sci. Rep. 14, 1008 (2024).
Uganda National Council for Science and Technology (UNCST). National Guidelines for Conduct of Research during Coronavirus Disease 2019 (Covid-19) Pandemic (2020).
Acknowledgements
We wish to thank the office of the Resident City Commissioner (RCC) of Mbale City, which authorized conducting of this study. We also thank the Village Health Teams and Village Local Council leaders who supported the research team during field data collection. We gladly acknowledge the assistance of Emmanuel Tumwebaze of Makerere University in conducting the laboratory experiments.
Funding
This study did not receive a financial grant.
Author information
Authors and Affiliations
Contributions
AW and ASE conceived the research idea, and were involved in field data collection and manuscript writing. Then JES, NN, AK, ASO, AMO, and SL were involved in data collection, data analysis and manuscript writing. HMK was the overall supervisor and administrator, and was involved in manuscript writing. All the authors proofread and approved the final draft of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This research was conducted in conformity to the national guidelines for the conduct of research in the post COVID-19 pandemic era, set by Uganda National Council for Science and Technology93. The study sought ethical approval from the Research Ethics Committee of Islamic University in Uganda (Ref. IUIUREC-2024-69). Written informed consent to participate in this study was obtained in writing from the study participants. The chairpersons of the Village Local Councils, and the Mbale District Health Officer (DHO) granted their approval for community entry and research conduct.
Consent for publication
Consent to publish the findings of this study was obtained in writing from the study participants.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Walusansa, A., Elmi, A.S., Ssenku, J.E. et al. Antimicrobial-resistance in clinically harmful bacteria contaminating household drinking water in Eastern Uganda highlights urgent need for enhanced antibiotic resistance stewardship. Sci Rep (2026). https://doi.org/10.1038/s41598-026-47699-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-47699-w