Abstract
While patient-doctor interactions have been extensively studied, how interactions during rehabilitation influence individuals’ self-concept—particularly through the subtle reproduction of disability-related stereotypes—has received less attention. This subtle mechanism is often shaped by representations of disability framed through a biomedical or mechanistic lens (e.g., the body as a machine), which can reinforce negative assumptions and dominant discourses about clients with mobility disability. This study seeks to examine the interactional dynamics between clients and the combined entity of healthcare professionals and medical systems, emphasizing representations that contribute to the construction of clients’ experiences and self-concepts during rehabilitation. Using representation theories and Foucauldian medical discourse as our framework, we conducted in-depth interviews with 12 experienced physiotherapists, acting as intermediaries between clients and other healthcare professionals and systems. The transcripts were analyzed through a six-phased inductive thematic analysis framework. In the results, three themes were identified: (I) The Complex Medical System, But Reliable Physiotherapy Clinic; (II) A Knowledge-Language Differential in Healthcare Professionals-Clients Talks; and (III) Iconic Representations: Practical Use vs. Perceived Stigma. Each theme was supported by relevant quotes. While dominant stereotypes surrounding disability persist across the rehabilitation steps, physiotherapists’ inclusive approaches were differentiated in themes I and II. However, healthcare professionals involved in rehabilitation, including physiotherapists, still reproduce the perception of the body as a machine. The themes identified are not limited to interactions within rehabilitation settings but also extend into wider public discourse, influencing societal perceptions of mobility impairments. Future research should prioritize co-produced approaches that center lived experiences to challenge dominant representations and promote inclusive rehabilitation.
Similar content being viewed by others
Introduction
People often claim not to hold assumptions about individuals with disabilities (Lenney and Sercombe 2002), yet studies and reports show that wheelchair users continue to face societal stigma, correlating with higher levels of depression, pity, and discomfort (Human Rights Watch Council 2018; Saia et al. 2024). As negative social stereotypes still exist in social dynamics, even in developed societies that emphasize equity (Asghar et al. 2020), this raises important questions: How and where do such perceptions originate and perpetuate? Are they shaped by individuals with disabilities themselves, or do they primarily arise from societal discourse? Who holds significant influence in shaping these narratives? For instance, do healthcare professionals and systems, as the medical interpreters of health and the concept of ability, contribute to shaping their clients’ perceptions?
While a range of known factors, such as social beliefs (Galli et al. 2015), employment status, personal well-being, and income levels (Fredericks et al. 2024; Pasin and Karatekin 2024), influence an individual’s self-perception of a disability, healthcare professionals are typically the first to inform clients of their mobility-related impairments. Medical experts diagnose and label disabilities objectively, expecting clients to follow prescribed treatments. Thus, aside from the previous perceptions of disability, clients begin to understand and define their role as a disabled person for the first time during the rehabilitation process and interaction with healthcare professionals. This moment of identity negotiation is critically examined by Papadimitriou, who emphasizes how rehabilitation encounters reshape clients’ embodied self-understandings (Papadimitriou 2008). In this context, healthcare professionals may adopt one of two viewpoints: the “human view” or the medical gaze. Oliver Sacks, as discussed in Toombs (1990), highlights that the human view—which emphasizes the individual patient— uncovers insights beyond clinical data, while the medical gaze focuses on the illness itself. These contrasting approaches not only influence doctor-patient relationships (Nielsen-Bohlman et al. 2004) but also have implications for broader public perceptions toward health in both personal and public spheres (Toombs 1990). These perceptions shape and influence sociomedical discourses on health, as reflected through communication, language, and actions (Showstack et al. 2019; Federici 2022). For instance, the naming and characterization of disabilities often mirror how doctors articulate these concepts. This naming function reflects what Phelan and Gibson identify as a normative process in rehabilitation discourse, wherein deviation from bodily norms is subtly reinforced through language (Gibson and Teachman 2012; Phelan et al. 2014).
On a broader level, these perceptions affect representations in indirect interactions, social media, graphics, and public portrayals of assistive devices, which act as implicit forms of language conveying dominant discourses on disability (Krippendorff 2006; Soleimani and Hossein Halimi 2012). Such discourses may exacerbate perceptual disparities between patients and healthcare professionals, emphasizing distinct ontological perspectives on disability. For instance, for people who require mobility aids (MAs), wheelchair design—anchored in a rehabilitation-focused biomechanical perspective and often symbolizing disability—may clash with clients’ humanistic views, rooted in unique social identities. Notably, Carol Thomas’s (1999) social relational model offers a useful lens for understanding how these symbolic representations—such as those embedded in mobility aid design—intersect with societal power structures and exclusionary practices. This disconnect can influence societal perceptions of clients’ physicality and movements in ways that differ from their self-perceptions (Barbareschi et al. 2021), potentially shaping a new self-representation that may lead to psychological effects such as isolation, depression, reluctance to use aids in public, and feelings of exclusion (Barker et al. 2004; Mortenson et al. 2022). Therefore, beyond the client-doctor relationship during the rehabilitation process, it is essential to mitigate the medical objective view and promote the humanistic perspective in both direct and indirect representations.
This study, which is part of a larger project tracking the experiences of mobility aid (MA) users, specifically aims to explore physiotherapists’ perspectives regarding encounters between clients with mobility impairments and relevant sectors of the rehabilitation process, including clinics, hospitals, orthopedic services, radiology departments, etc. It examines how these interactions influence clients’ perceptions and contribute to the representation and reproduction of disability stereotypes during the rehabilitation process. This understanding helps identify and challenge stigma, enabling designs and policies that promote empowerment and social inclusion. Then, we explore the distinct perceptions between individuals with impairment affecting mobility and healthcare professionals during rehabilitation. To this end, we specifically ask: What themes illustrate the various representations surrounding the dominant discourse of mobility disability during the rehabilitation process? And accordingly, how do clients with mobility impairment perceive the body and disability differently from healthcare professionals? This study employs representation theories and a post-modernist approach to health, particularly Foucault’s medical discourse analysis, to explore themes and interpretations. Representation theory provides insight into doctor-patient interactions and differing perspectives (Street Jr. 2003), focusing on how health-related perceptions shape behaviors and decisions (Donovan et al. 2007). Rooted in French philosophy, Foucault’s approach examines the politics of knowledge and power, particularly in medicine (Ristić et al. 2021), uncovering how interactions reproduce distinct ontological views. In this study, we conducted in-depth interviews with physiotherapists, whose extensive client interactions and understanding of healthcare professionals make them ideal intermediaries in rehabilitation (World Physiotherapy, 2019). Their insights, based on experiences with diverse mobility impairments, capture valuable perspectives that may be less accessible through interviews with clients, a vulnerable group. The study’s contributions are summarized as follows:
-
By exploring the differing perspectives of clients with impairments affecting mobility and healthcare professionals, experts in disability studies and health managers can develop policies and practices to help healthcare professionals adopt new interaction and communication protocols.
-
This study contributes to the efforts of relevant experts, such as healthcare administrators, educators, and disability advocates, in developing guidelines to shape socially representative disability-related imagery.
Literature review
The academic literature has extensively explored the representations of disability in media and their significant influence on societal attitudes, emphasizing how social representations impact the lives of disabled individuals (Umar et al. 2024). Reports show that the media portrays disabilities through three archetypes: the Victim, seen as a helpless object of pity; the Hero, who overcomes challenges; and the Villain, exemplified by characters like pirates with missing limbs (Media Smart 2024). Research indicates that these representations are often inadequate, inaccurate, and predominantly negative, resulting in detrimental societal treatment of people with disabilities (Ocran 2019). For instance, a study reveals that Indonesian mass media frequently portrays individuals with disabilities using passive syntactic structures (e.g., “are given help,” “receive care”) and ableist language, which collectively reinforce stereotypes of dependency and a lack of agency, thereby perpetuating ableism (Priyanti 2018). To this end, the need for greater reassessment of strategies to combat negative attitudes toward disabled individuals is also emphasized (Derbyshire et al. 2023).
While a comparison of news media representations from 1998 to 2008 suggests a positive shift toward acknowledging the complexity of disabled identities (Devotta et al. 2013), recent research on stigma indicates that MA users frequently face public discrimination, contributing to increased depression and feelings of invisibility (Saia et al. 2024). Furthermore, numerous studies have focused on the general patient-physician relationship to address these disparities (Bensing and Dronkers 1992; Haskard Zolnierek and DiMatteo 2009; Roter et al. 1997; Suarez-Almazor 2004), particularly within Western medicine, where the relationship between patients and the healthcare system has often been subject to criticism (Matin 2021; White 2002). Building on this critique, a growing body of work in Critical Rehabilitation Studies (CRS) has emerged, challenging traditional clinical understandings of disability by foregrounding its socio-political, embodied, and relational dimensions (Mosleh 2019; Papadimitriou 2008; Teachman et al. 2020). This perspective encourages rethinking foundational assumptions in rehabilitation and promotes more reflexive and inclusive practices (Teachman et al. 2020). Recent contributions also point to the role of professional discourse in shaping patient experience and power asymmetries during care. For example, Barradell and Scholten (2024) highlight how physiotherapy continues to reflect biomedical priorities that may conflict with patients’ lived realities, reinforcing the need for critical engagement with disciplinary language and assumptions. Similarly, a recent Critical Disability Studies–informed study found that ableism persists across individual, group, and systemic levels in academic and healthcare settings, emphasizing the need for inclusive practices to confront embedded biases and enhance accessibility (Feldner et al. 2022). However, to the best of our knowledge, no studies have explored the representation and reproduction of stereotypes during rehabilitation in the orthopedic sector of healthcare, particularly in non-Western healthcare contexts. In such sociocultural contexts, holistic approaches that integrate cultural beliefs with clinical practices influence the prevailing medical discourse (Alkhaibari et al. 2023; Matin 2021). Additionally, societal attitudes toward mobility impairments play a significant role in shaping the power imbalance between clients and healthcare professionals (White 2002), influencing their (self)perceptions within clinical contexts. Our review highlights that disability representation has been widely studied in areas such as media, the workplace, and public interactions. However, no studies have examined how these representations serve as the foundation for perceptions formed during the rehabilitation process, where clients first become aware of their impairment affecting mobility.
Theoretical framework
This study adopts representation theory, post-modernist views of the body, and Foucauldian discourse analysis to explore how the perception of disability is constructed and reproduced in the rehabilitation process. These frameworks align with our goal of examining how medical and healthcare spaces, institutional power, and professional interactions shape clients’ self-concepts and experiences, reinforcing or challenging dominant disability narratives.
Representation theory in healthcare
Representation refers to the process by which individuals construct their understanding of the world through language, symbols, images, and cultural narratives (Barthes 1978; Derrida et al. 2016). These representations shape perceptions, attitudes, and behaviors, influencing how people interpret and engage with their environment (Bandura 1977). In the context of health, extensive research has explored how illness is represented, highlighting key cognitive dimensions such as identity, cause, consequences, and control over an illness across cultures (Keller 1993; Kleinman et al. 1978; Lau et al. 1989).
In healthcare, representation plays a critical role in shaping doctor-patient interactions and perceptions of health and illness. When doctors and patients communicate, their exchanges go beyond clinical concerns and influence how both parties perceive illness and disability. In the rehabilitation context, the discourse of mobility disability is a network of interconnected ideas, attitudes, and experiences that shape the discourse and identities of both patients and healthcare professionals (Arribas-Ayllon and Walkerdine 2008). For example, a wheelchair is more than a device — it carries assumptions about dependence that shape how professionals treat clients (e.g., focusing on physical fixes) and how clients see themselves.
From a discourse theory perspective, representation is not neutral. Power dynamics heavily influence how disability is portrayed and understood, both in healthcare interactions and beyond (Hall et al. 2013). In doctor-patient relationships, these power dynamics shape how patients see themselves and their abilities. The entry of power into the semantic circle of representation involves understanding how different groups, conditions, or signs affect perceptions and meanings through power dynamics (White 2002). Representation, thus, can be inherently linked with the dynamic of differences, especially concerning the semantic perception disparities between healthcare professionals and patients (Moradi 2018). Difference, in this context, is not merely an attribute but a mechanism for creating meaning, constantly constructed and reproduced under the influence of power dynamics (Foucault 2008). Post-structuralists follow this discussion by arguing that categories like culture, identity, society, and ethnicity are not fixed but are constructed and constantly evolving through discourse shaped by power dynamics (Schrift 2018; Williams 2005). In this study, we explore how semantic differences and power dynamics in rehabilitation settings influence clients’ perceptions.
Post-Modernism and body interpretation
Modernism emphasizes objective knowledge, scientific progress, and medical intervention in disease treatment, while post-modernism challenges the notion of a universal understanding of the human body (Higgs and Scambler 1998). In the postmodern era, health is redefined beyond the absence of disease, seen instead as a dynamic, individual experience (Schrift 2018; Williams 2005). This shift prioritizes understanding how social and cultural perceptions shape health over merely controlling disease. Critics of modernist medical discourse, such as Michel Foucault and Jacques Derrida, argue against this rigid framework, instead emphasizing the subjective nature of the human body as a collection of individual experiences and interpretations (Schrift 2018; White 2002). Also, Michael Bury’s (1986) arguments about the transition from modernity to post-modernity highlight key processes such as objectification, rationalization, and subjectification, which show how medical concerns shift from disease to subjective health considerations.
In the healthcare context, therapeutic language and institutions shape perceptions of disease and life, impacting self-perception and behavior (Matin 2021). Medical language and behaviors exert control over individuals’ minds, reinforcing the authoritative role of doctors in shaping health narratives (Higgs and Scambler 1998). Subjectification is pivotal in our study, as clients undergoing rehabilitation are consistently influenced by medical language and interpretations, enforcing the subjectification on clients. Post-structuralism challenges fixed meanings in language and culture, emphasizing their construction through language, power, and social context (Fox 2016; Haghighat 2007). Language, carrying meaning, power, and knowledge, can amplify an unequal doctor-patient dynamic. Doctors use scientific language, while patients may lack linguistic agency. Michael Bury (1986) presents the main aspects of discourse in health sociology, focusing on Agency, Knowledge, and Power. In this view, the Agency emphasizes reducing human agency (e.g., doctors) in discourse systems, treating all subjects, including medicine, as open to discussion (Schrift 2018). Knowledge, according to Foucault in The Birth of the Clinic (1994), arises from doctor-patient interactions and hospital structures and is shaped by the healthcare profession’s authority in determining truth. Here, post-modernists consider both general knowledge and specialized knowledge to be the products of techniques originating from various cultural backgrounds (Higgs and Scambler 1998). Power shifted from foundational authority to disciplinary control under pastoral supervision (White 2002), manifested through therapeutic oversight, self-regulation and surveillance, normalization practices, and individualized monitoring within welfare institutions. In the welfare sector (e.g., healthcare), this shift wields significant influence over discourse, shaping both perceptions and experiences (Schrift 2018).
Foucauldian medical discourse
Foucault examined how bodies are positioned in society as subjects of social control through medical institutions. He described the power dynamics of the medical gaze and its influence on knowledge and social relations (White 2004), arguing that knowledge and power are intertwined through discourse, which allows authority figures and social actors to exercise power. Each discourse shapes its own “truth,” defining valid knowledge through exclusionary practices (Foucault 2008), with power embedded in social relations rather than possessed by individuals or groups (Foucault 1994). Furthermore, Foucault contends that discourses exist as various practices that “systematically form the object of which they speak,” shaping individuals’ actions, thoughts, and behaviors (1972, p. 49). Foucault argued that power relations are embedded within social institutions and that the gaze is one way in which power is exerted and maintained (White 2002; Schrift 2018). He believed the gaze permeated various aspects of society, such as medicine, criminal justice, and education, demonstrating how institutions and individuals wield power through observation and surveillance. He illustrates this with an interrogation room where the accused, unable to see the observers behind a glass wall, becomes the object of their scrutiny. In this dynamic, the unseen viewers hold complete control (Foucault 1995).
In The Birth of the Clinic (1994), Foucault examines the medical gaze’s role in diagnosis, reinforcing physicians’ authority and power over patients. Gaze transcends mere observation; it denotes a scrutinizing, surveillant gaze and ultimately dominates by transforming perception into a disciplinary mechanism that constructs and regulates knowledge (Flynn 1993). Gaze is important in trying to see the unthinkable matter in human seeing and to open the ways of seeing to the unseen matter (Rajchman 1988). Doctors employ the power and knowledge to investigate the patient’s body and see their body as a subject.
In Foucauldian medical discourse, another significant concept is biopower, which refers to how political power governs populations through public health, demographics, and the regulation of life. The clinic plays a pivotal role in this biopolitical system, expanding healthcare from treating individual illnesses to managing broader “techniques of health” (Foucault 2010, pp 1978–1979) that shape both individual patients and the broader population’s health and well-being (Ristić et al. 2021). Physicians assumed medico-administrative roles that addressed socio-economic factors, alongside politico-medical roles prescribing not only treatments for disease but also remedies for societal behavior to promote a healthier image (Foucault and Rabinow 1997, pp 1954–1988; Ristić et al. 2021). In The Politics of Health in the Eighteenth Century, Foucault describes how medicine rose within these emerging regulatory systems and power structures (Foucault and Rabinow 1997; White 2002).
In the following section, we used the post-modernism perspective, with a specific focus on representation theory and Foucauldian medical discourse, to analyze the perception disparities between healthcare professionals, clinics, and clients with impairments. Our aim here is to illustrate the key representational elements through which disparities are reproduced.
Material and methods
Establishment of the study procedure
The authors initially aimed to explore key concepts that reflect how physiotherapists perceive the perspectives of both healthcare professionals and clients with mobility impairments. A shared understanding among all authors regarding representation theory and Foucault’s conceptual framework was established. Representations and their associated meanings are trackable in the experiences of physiotherapists, who regularly engage with patients and navigate their healthcare system (Chartered Society of Physiotherapy 2022). Physiotherapists were selected as participants for both practical and ethical reasons, as direct access to clients undergoing active rehabilitation was limited by institutional protocols. Clients with mobility impairments at this stage are considered a vulnerable population who may find it difficult to discuss topics beyond their immediate care needs. However, physiotherapists, as close observers of these experiences, can signal common perceptions and make these visible for analysis. Notably, clients’ post-care experiences differ phenomenologically from their lived experiences during rehabilitation (Toombs 1990). Therefore, we do not claim to represent clients’ lived experiences directly. Rather, our focus is on how disability is represented and constructed within rehabilitation discourses, and how these constructions may influence clients’ perceptions. Physiotherapists, through their close relationships with clients and holistic understanding of the rehabilitation process, can provide meaningful insights into clients’ perceptions and experiences. Furthermore, physiotherapists’ interactions with a broad range of individuals with mobility impairments—many of whom may not be accessible for direct interviews—made them the most suitable participants for this study. Accordingly, the study conducted semi-structured in-depth interviews with physiotherapists, adhering to the Consolidated Criteria for Reporting Qualitative Research (COREQ) checklist commonly used in qualitative studies involving interviews (Tong et al. 2007).
Development of interview guidelines and questions
The questions and guidelines for this study were developed as part of a larger research project focusing on individuals who use MAs. Nine questions were intended for this specific study. To develop the interview guide, two members of the research team conducted a literature review to identify key aspects of the interview questions that could highlight representations and reproductions of disparities and dominant discourses surrounding mobility disability within the framework of Foucauldian medical discourse. To ensure contextual relevance and methodological rigor, we consulted a practicing physiotherapist during the early refinement of the interview questions. Building on this and informed by pre-interview insights, an interdisciplinary panel reviewed and revised the interview protocol. This panel included the study authors—experts in human factors, health sociology, sustainability, inclusive design, qualitative research, and cognitive biases—along with a physiotherapist and a medical anthropology expert.
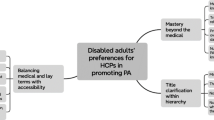
While the broader interview protocol included several components addressing a wide range of rehabilitation-related themes, the present manuscript draws exclusively on a focused subset of questions aligned with the specific aims of this study. These include participants’ perceptions of client-provider interaction, disciplinary language, and the social positioning of individuals who use MAs. Then, for interpretation, the answers to questions related to this study were reviewed (Fig. 1), serving as the basis for the current analysis. The key semi-structured interview questions, provided in English, can be found in Appendix A. To uphold the research’s validity and rigor, we engaged a physiotherapist for preliminary refinement of questions in the interview. Also, based on pre-interview insights, an interdisciplinary panel, including the authors and two external members—a physiotherapist and an expert in medical anthropology—refined the interview guidelines and questions.
Overview of the research process, comprising seven stages from identifying key concepts to interpreting responses.
Recruitment
Experienced participants were recruited based on the following inclusion criteria: (1) registered physiotherapist qualification, (2) over 5 years of experience in private practice or hospital physiotherapy wards, and (3) willingness to provide informed consent and participate voluntarily. Exclusion criteria included simultaneous participation in studies focused on medical, clinical, or medical engineering topics, as these emphasize physical interactions and could overshadow the humanistic aspects explored in the interview. Using a combination of purposive and snowball sampling, 12 physiotherapists, with extensive experience (more than 5 years) working with physical disability patients, agreed to participate in the interview. The interviewers did not have any prior familiarity with the participants. Participants’ interview characteristics are provided in Table 1.
Data collection
The interview times and locations were arranged with participants a day in advance, and detailed interviews were then conducted in Persian between March 2022 and February 2023 in private clinics and hospital physiotherapy wards in Kordkoy and Tehran, Iran. Before recording, the purpose and content of the study were briefly explained to the participants. Upon signing consent and confidentiality forms, interviews were digitally recorded, transcribed, and anonymized. All interviews were conducted by the first author, which allowed for a consistent approach in the administration of questions, tone, and interaction with participants. The interviews followed a structured guide adapted from a broader study, though this manuscript draws on a specific thematic subset focused on participants’ views on disciplinary language, professional roles, and power dynamics in MA provision. The flexible structure enabled the interviewer to adjust prompts based on participant responses, supporting deeper exploration of complex perceptual themes.
For the portion of the interview relevant to this study, ~19–58 min were specifically dedicated to exploring the selected humanistic themes. While this represents a subset of the overall interview duration—of ~50–90 min, the interactions were characterized by high participant engagement and substantial detail, demonstrating remarkable depth despite the shorter timeframe (Irvine 2011). Factors such as participant expertise, clear alignment of interview questions with study objectives, and focused discussions facilitated efficient data collection, enabling us to achieve thematic saturation within this period. Prior research confirms that interview length alone is not the sole determinant of the depth or quality of data; participant engagement levels, richness of information provided, and relevance to the study’s aims (Gilbbons 2023; Kvale 2004) collectively influence the efficacy and meaningfulness of in-depth interviews, even when conducted within comparatively shorter durations (Guest et al. 2006). The first was extended to ~58/120 min as a pilot and exploratory session that helped refine the interview approach and streamline subsequent sessions, resulting in greater consistency as reflected in Table 1.
A serene environment was upheld to ensure participants’ ease and comfort. Participants were provided a flexible time to discuss and reflect on their insights. Interviews continued until reaching saturation, which occurred at the 12th interview, when repetitive responses indicated that key ideas had been sufficiently captured.
Data analysis
Within 48 h after the interviews, the audio recordings were carefully transcribed into written text. To enhance the credibility of the analysis, the transcriptions were reviewed with participants to verify the accuracy of their ideas and responses. The interviews were translated from Persian into English and anonymously reviewed by two authors. To ensure translation accuracy, two native Persian-speaking authors, deeply familiar with the culture and metaphors, collaborated closely with a native English-speaking author throughout the translation process. Following transcription and initial verification, the interview data were analyzed using Braun and Clarke’s six-phase inductive and reflective thematic analysis framework (Braun and Clarke 2012). This method involves sequential steps, including familiarization with the data, developing preliminary codes, identifying themes, reviewing themes, defining and naming themes, and producing a report (Braun and Clarke 2006). The transcripts were entered into NVivo 12 software for data coding, and an initial codebook was created. Two coders independently performed parallel coding, followed by discussions to resolve any discrepancies in their coding decisions. The codebook was iteratively refined throughout the analysis process to ensure comprehensive coverage of the data and consistency in coding. This iterative refinement helped maintain analytical rigor and allowed emerging themes to be accurately captured. They then met regularly to discuss and resolve discrepancies, achieving consensus on the coding scheme. Following this, the authors applied both semantic (explicit) and latent (underlying) interpretation strategies to synthesize codes into broader subthemes and overarching themes (Braun and Clarke 2022). This process involved collating, sorting, and examining repetitions, similarities, differences, and gaps in the coded excerpts. Finally, relevant quotes were chosen, and the themes were reported in alignment with our research question (see Appendix B for an overview of the coding and theme development). Importantly, this thematic analysis was situated within a critical-interpretive framework, allowing us to examine not only participants’ explicit experiences but also the underlying discourses shaping those narratives (Braun and Clarke 2019). We chose this method for its flexibility (Braun and Clarke 2006), supporting descriptive insights alongside post-structural interpretation. As such, the themes were not treated as purely objective categories, but as meaning-laden constructs that reflect power relations and institutional discourses relevant to our research question (Byrne 2022).
Results
The authors initially established and agreed upon 76 codes that clustered into 8 groups. Subsequently, after further discussion, two researchers identified seven themes and five subthemes, which were later refined and consolidated into the following three themes: (I) The complex medical system, but reliable physiotherapy clinic, (II) A knowledge-language differential in healthcare professionals-clients talks, and (III) Iconic representations: practical use vs. perceived stigma.
Theme I. The complex medical system, but a reliable physiotherapy clinic
Based on this theme, physiotherapists expressed that they found there is a significant opportunity in the role of a physiotherapist to empathize with clients who sometimes share their own stories.
P2: “Sympathy, or understanding pain, is just as present in the minds of physiotherapists as it is for surgeons. However, the short interactions with orthopedics or surgeons don’t allow them [orthopedics] to express this sympathy. In contrast, for us physiotherapists, who have more time with patients, this connection naturally develops”.
Additionally, physiotherapists highlighted the intricate nature of the medical process from the perspective of clients, acknowledging its complexities and potential challenges.
P1: “Clients often view health organizations [excluding physiotherapy clinics] as the first group to blame, perceiving them as ineffective in providing adequate services”.
P1: “They often ask, Are the doctors being honest? They have many doubts about their future health in this treatment system”.
Despite this complexity, physiotherapy stood out as a beacon of trustworthiness and stability within the context of healthcare for clients. Physiotherapy clinics emphasized the importance of fostering trust and rapport with their clients, serving as pillars of support within the overwhelming maze of healthcare services.
P3: “Clients are always eager to talk if they feel the opportunity is there [clinics …They share their own personal stories if they feel comfortable with us”.
P6: “Clients are very open to the treatment process and engage with us at the physiotherapy clinics, often saying, ‘I will follow your recommendations.’…They [clients] express that our [physiotherapists] approach suits them better”.
Physiotherapists emphasize that some clients are professional assessors of clinics and usually try several clinics in the rehabilitation process. Clients strive to validate and congregate their clinic selection through communication with other clients, both within and outside the clinic. This dialog constitutes a significant portion of daily patient interactions.
P9: “Clients comment on the clinic website or talk in private conversations, and there’s one thing they often say: they congratulate each other on choosing the clinic. They are saying, ‘I made a good choice picking this clinic, and so you [other clients] were also successful.”
P5: They focus more on psychological and behavioral aspects of the clinic, and physiotherapists than on treatment itself”.
This theme indicates that in the realm of healthcare, physiotherapy stands out as a reliable and consistent refuge. It diverges from the conventional stereotypes associated with medical clinics, presenting itself as a reliable companion for clients on their path to rehabilitation.
Theme II. A knowledge-language differential in healthcare professionals-clients talks
This theme highlights the knowledge-language disparities between involved healthcare professionals and clients, a concept central to Foucauldian medical discourse. Healthcare professionals, excluding physiotherapists, often possess extensive technical knowledge of medical terminology, treatment protocols, and rehabilitation strategies. In contrast, clients may lack familiarity with this specialized language and instead rely on their personal experiences, sensations, and vernacular to articulate their needs and concerns, potentially leading to challenges in achieving mutual understanding.
P1: “Typically, our conversations with colleagues involve technical language distinct from that used with our patients…”.
P10: “The technical terminologies are primarily used when discussing treatment procedures. In contrast, clients often express their pains and symptoms using plain language”.
P9: “While all doctors or physiotherapists may use a common medical term, the client’s interpretation of it might differ, which can mislead the patient”.
It reveals a stark contrast between the two parties, but healthcare professionals’ way of communication is often perceived as more dominant and authoritative. Here, clients are those groups who typically attempt to familiarize themselves with and use the medical term in direct communication with physiotherapists or even in social conversation.
P1: “Initially, clients often take pride in using medical terms in daily conversations, but their expressions reveal their limited knowledge and experience”.
Conversely, when physiotherapists adopt a more empathetic and inclusive approach, actively listening to and validating the lived experiences and perspectives of their clients, the disparity in knowledge-language begins to dissolve, enabling a more equitable and collaborative exchange of information.
P4: “We encourage them to describe their pain using their feelings rather than technical terms. We advise, ‘Please avoid phrases like ‘my ligament is this’ or ‘my ligament is that’ as they are often mispronounced”.
P1: “I ask them to speak simply, using their native language. For instance, if someone is Kurdish, Lor, or from the Northern region, even if his Farsi-speaking partner wants to speak, I say let them speak”.
Theme III. Icons representations: practical use vs. perceived stigma
This theme of stark contrast in perception highlights the complexity of the relationship between clients and healthcare professionals regarding the interpretation of medical devices and their implications for self-image and identity. In this theme, icons representing ability or disability are interpreted differently. Healthcare professionals, including physiotherapists, assess orthopedic products functionally and technologically, focusing on their effectiveness for mobility and rehabilitation. Whereas, clients often perceive these products as stigmatized symbols of disability, associating them with limitations and societal views of incapacity, often linking them to concepts like “destiny” or “fate”.
P3: “We [healthcare professionals and physiotherapists] view disability through the lens of technological advancements, focusing primarily on physical recovery, while disabled individuals see it in relation to aging, weakening, and the need for assistive devices in daily life”.
P2: “They sigh. They believe that this [mobility impairment] is a form of retribution and punishment for their past actions….”
Clients experience mobility limitations and a loss of social roles as a result of their reliance on assistive products. In addition, the protocols prescribed by healthcare professionals, emphasized by the use of assistive products, reinforce a deviation from the clients’ sense of ability.
P2: “Some orthotics may not suit certain clothing, creating an unflattering look or highlighting the illness, marking ‘I am a patient’ in society”.
P6: “Clients imply that their prescribed assistive devices reflect their miserable circumstances…”
In this context, clients value physiotherapists’ efforts but often express frustration, noting that healthcare professionals, including physiotherapists, cannot fully grasp the depth of their disability-related struggles since they have not experienced them firsthand. In response, physiotherapists often group clients with similar mobility levels during rehabilitation sessions, creating a sense of solidarity among those facing comparable challenges and reducing disparities.
P11: “Medical professionals view themselves as a caregiver, separate from the disability experience. Even a physiotherapist cannot fully understand their clients, as knowledge does not equate to lived experience….”
P6: “Clients often say; You’ve seen disability more than others, but you are not disabled.”
Clients’ negative emotions extend beyond clinics and are intensified in social and environmental contexts. Every instance of environmental inaccessibility reinforces their perception of disability. Consequently, in social settings, clients with impairments feel a lack of societal respect for their needs as equal citizens. This perception may arise from a dominant discourse that promotes only idealized bodies in the media. Comparing their bodies to those of able-bodied individuals, and even to their past selves, exacerbates their sense of inadequacy.
P8: “…In an unsuitable environment, mobility devices can be perceived as an insult [for clients], leading to feelings of shame and helplessness, like the sense of fear and shame after falling downstairs”.
P2: “They compare themselves to the images of bodies that the media and their financiers decide and promote unhealthy bodies…. They feel they are far from the ideal body shape [advertised in media]”.
P7: “Usually, many patients often stay in the past, leading to depression. This [depression] in all exaggerated and ironic form reaches the point where they [clients] say that when I was young, I was a judo player or when I was young, I was a basketball player…”
In this context, physiotherapists argue that the media not only misrepresents the ideal body but also showcases unrealistic body shapes. Here, feelings of inadequacy stemming from limited environmental accessibility are shaped not just by medical discourse but also by industries that leverage medicine’s perceived authority.
P1: “The media cooperate with industries and the economy and often advertise something that is not good for the health of the body.”
MAs, along with their connotations, also shape public attitudes and stereotypes. Participants noted that MAs, like wheelchairs or canes, carry symbolic meanings beyond functionality, often embodying societal stereotypes and stigma in clients’ and people’s views. This issue is not a concern for healthcare professionals. Clients with impairments affecting mobility may experience feelings of marginalization or stigma when using MAs, as these reminders of perceived differences and limitations can evoke emotional reactions such as anger and depression.
P5: “When using such products (MAs) in social situations, they [clients] feel that people treat them with pity… They [clients] feel shy and frustrated in public and therefore hesitate to use them [MAs] in public”.
Under such negative social perceptions and stigmatization, clients may resist acknowledging MAs. However, their perceptions can vary depending on factors such as personal background, social context, and the cause of their disability. To address such social representations, participants often highlighted that the design and appearance of MAs, along with technological enhancements, can enhance the credibility of assistive products and positively influence user acceptance.
P1: “Being socially perceived as a hero is different from being a fugitive or accused. Being [socially] accepted as someone whose fingers were cut off [according to religious law] for theft and someone whose finger is injured like Hans Brinker [Refers to Mary Mapes Dodge’s novel about a boy who saves Amsterdam by plugging a dike leak with his finger] is very different.”
P12: “The beauty of assistive products can influence MA users’ preference by 30–40%, which is significant for us [physiotherapists].
During coding, we highlighted the intersection of perceptions on disability between clients and healthcare professionals, rooted in their distinct ontological views, and categorized these under each thematic group (Table 2).
Discussion
In this study, our objective was to decipher the representational scenarios wherein clients’ perceptions of mobility-related disability stereotypes are reproduced during the rehabilitation process. Applying representation theories and a post-modernist perspective, particularly Foucauldian medical discourse, we analyzed interviews, identifying three themes. The interpretation of these themes shows how initial interactions with the medical system and its professionals reproduce disability stereotypes and shape clients’ perceptions within a medical discourse that contrasts with their more humanistic perspectives.
Theme I highlights the complexity of rehabilitation steps and the role of medical clinics, which becomes more evident when clients evaluate clinics in or beyond the clinical setting. However, this issue is less prominent for physiotherapy clinics, where extended sessions during rehabilitation provide clients with opportunities to share perceptions of their bodies and abilities. These interactions are often perceived as fostering empathy and patient-centered care (Rasoulivalajoozi and Touir 2023). Yet, such perceptions also need to be understood within institutional discourses that shape how clients engage, express progress, and navigate recovery. Rather than standing outside biomedical authority, physiotherapy settings may reconfigure it through more participatory forms. While participants perceived themselves and their fellow physiotherapists as offering more intimate engagement opportunities compared to other healthcare professionals, this perception may reflect professional self-positioning rather than a distinct structural difference. Physiotherapy professional identity is fluid, shaped through negotiation within professional communities and influenced by workplace and institutional structures (Hammond et al. 2016). Compared to other healthcare professionals, physiotherapists often engage in longer-term interactions, allowing for a relational approach that clients interpret as supportive (Rasoulivalajoozi et al. 2025c). The client-centered approach in these clinics enables clients to navigate the medical process more freely, reducing bureaucratic barriers and feelings of subjectification. Participants think that clients see these clinics as supportive when physiotherapists’ authority is less dominant, aligning with studies showing a recent shift in medical authority toward patient-centered care (Stivers and Timmermans, 2020). These observations also resonate with debates in disability studies: the paradox of improving function while valuing disability as diversity. The ICFFootnote 1 model offers a way to navigate this tension by framing disability at the intersection of individual ability and social context (Roush and Sharby 2011).
Physiotherapists perceived that, although clients often see physiotherapy clinics as more personalized than public welfare institutions, this individualized model reflects broader socio-political values emphasizing self-management and individual responsibility. In line with previous studies, they noted that their clients appreciate empathy and genuine concern (Steenbruggen et al. 2022), which fosters mutual trust (Cucuzzella et al. 2024); however, this trust may also be shaped by professional norms that define the “ideal” patient as active, motivated, and emotionally engaged.
According to Foucauldian medical discourse, clinics operate within biopolitical frameworks that regulate bodies and populations (Ristić et al. 2021). Previous studies have shown that physiotherapists’ narratives often reflect and reproduce dominant discourses in rehabilitation, highlighting tensions between biomedical frameworks and clients’ lived experiences, as noted by Barradell and Scholten (2024). However, in this study, physiotherapists described their clinics as enacting these frameworks differently—placing greater emphasis on empowerment, engagement, self-management, and rehabilitation rather than on disciplinary control (Diener 2021). This distinguishes their approach from the more regulatory focus typical of other healthcare professions or welfare policies. This contrast mirrors cultural critiques, such as the film Patch Adams (Shadyac 1998), which challenges doctor-centric approaches and emphasizes patient engagement. We contend that strengthening autonomy and active participation reduces the dominance of clinical authority discourses. Additionally, the interior design of physiotherapy clinics reinforces this perception. Unlike traditional medical spaces featuring complex devices and instructive pictograms, physiotherapy clinics often resemble gyms with visible rehabilitation equipment. Recent studies suggest that the concealment of medical devices can alleviate fear, enhance trust, and improve patients’ mental well-being (Cucuzzella et al. 2024).
Theme II highlights the knowledge and language gaps between clients and healthcare professionals. Despite healthcare providers recognizing the value of plain language, doctors often use terms that patients struggle to understand, up to seventy times per encounter (LeBlanc et al. 2014; Pitt and Hendrickson 2020). This may result from varying medical knowledge, language proficiency (Dahm 2012), and communication skills in routine clinical interactions (Kenny et al. 2010). In addition, time constraints and management challenges in hospitals and orthopedic clinics may limit client interaction, hindering physician-patient communication (O’Reilly et al. 2022; Rasoulivalajoozi and Touir 2023). In rushed examinations, doctors often prioritize efficiency, using jargon and abbreviations that can confuse patients and discourage them from asking further questions (Tariq and Sharma 2024). Conversely, some studies suggest that advising doctors to avoid or clarify jargon may be ineffective (Dahm 2012), highlighting the need for further investigation into its role. Nevertheless, our interviews showed that physiotherapists demonstrate empathy and inclusivity by avoiding medical terms, positively impacting client integration (Rasoulivalajoozi et al. 2025b). These discrepancies in using jargon, learned through medical training (Johnsson et al. 2018; Luke 2003) and plain language by clients, not only create communication barriers (Dahm 2012) but can also reinforce a power imbalance, leading clients to perceive themselves as lower in hierarchy than doctors. Hence, as shown in Theme II, clients may feel pressured to learn medical terminology to communicate effectively, reinforcing healthcare professionals’ authority and their own passive role. This dynamic mirrors Foucault’s concept of power-knowledge, where power operates through knowledge systems, shaping social hierarchies (Foucault 2008; White 2002). In this context, while physiotherapists often appear more accessible, we interpret their narratives not as direct evidence of relational truth, but as discursive positions shaped by their institutional alignment with biomedicine (Dalboni et al. 2023). From a Foucauldian perspective, these speaking positions reproduce certain normative assumptions while also negotiating space for more inclusive representations of disability.
Theme III illustrates how disability icons, like wheelchairs, are perceived differently by healthcare professionals and users, shaping their views within and outside clinical settings. While healthcare practitioners, including physiotherapists, focus on functionality and technological advancements to aid mobility, users often perceive these icons through the lens of broader social discourse, sometimes associating them with weakness and incapacity (Papadimitriou 2008). This contrast is further emphasized by the appearance of two sides: healthcare professionals, in formal attire and stethoscopes, symbolize authority and observation (Luke 2003), while the MA used by clients serves as a symbol of disability, reinforcing stereotypes and potentially making clients feel they belong to a lower-ability class, widening the perceived gap (Nimmon and Stenfors-Hayes 2016; Rasoulivalajoozi et al. 2025a). These symbols act as tangible reminders of physical limitations, impacting clients’ psychological experiences (Taleporos and McCabe 2002), and reinforcing disability stereotypes. This also reflects a deeper issue: physiotherapy’s ‘body-as-machine’ focus limits attention to social and psychological dimensions of disability (Nicholls 2019).
This representation extends beyond the clinic into the public sphere, emerging in environmental accessibility and the symbolic perception of MA within society. For instance, each environmental inaccessibility encountered by clients can serve as a reminder of disability, reproducing stereotypes about disability (Rasoulivalajoozi et al. 2025b; Vennavally-Rao 2022). Consistent with prior research, our findings demonstrate how individuals in such unequal situations experience frustration, anger, and feelings of marginalization (Barlew et al. 2013). These feelings may intensify as clients unconsciously compare their current bodies to their past selves and societal beauty standards promoted by the media (Aparicio-Martinez et al. 2019; Jiotsa et al. 2021). Furthermore, unlike other medical accessories, MA are designed for use and independence in public settings rather than in the internal space of the clinic, influencing public judgment, perceptions, and social identities (Barlew et al. 2013; Chan et al. 2009). Therefore, the symbolic representation of assistive products, such as wheelchairs, functions as a language in social contexts (Soleimani and Hossein Halimi 2012). The design and aesthetic appeal of these assistive products can help mitigate negative stereotypes surrounding disability (Dos Santos et al. 2022; Rasoulivalajoozi 2025; Rasoulivalajoozi and Farhoudi 2025). Conventional MA designs, shaped by a mechanistic view of the body and collaborations between medical engineers and professionals, prioritize functionality over aesthetics (Faraji and Valajoozi 2014). However, this could change with a redesign of the wheelchair’s symbolic appearance to emphasize personal expression and social identity (Desmet and Hekkert 2007; Krippendorff 2006). For instance, in the X-Men movie series, Professor Charles Xavier’s wheelchair transforms him from a disabled individual into an empowered superhero (Annalee 2017). His wheelchair symbolizes strength, agency, and empowerment rather than disability, illustrating how design can challenge prevailing stereotypes and become integral to identity. While wheelchair designs have evolved, they still follow the modernist principle of ‘form follows function,’ or “functionalism” (Craven 2019). This lack of social polish reflects a mechanistic approach, prioritizing biomechanical and machinery aspects over social considerations. The human-machine perspective on the body, exemplified in series like Inspector Gadget (Chalopin et al. 1983), offers a critical view of the body as a machine (Eveleth 2018). The wheel stands out as a symbol of this mechanistic perspective in MA, like wheelchairs, prominently featured in pictograms for user identification (Dawood 2018). We believe that industrial symbols, such as the wheel, perpetuate a mechanistic view of the body in these products. Therefore, we recommend that future design studies aim to counter the dominance of purely biomechanical representations of MA by developing them to include emotional, symbolic, and socially situated dimensions, which may help challenge stigma and promote more holistic engagement.
Conclusion
Under the representation and post-modernism framework, particularly the Foucauldian medical discourse, we decoded the representations, wherein differential ontological views regarding the body and disability between healthcare professionals and clients are reproduced. The identified representations are categorized into three themes. We showed that representation in the rehabilitation steps still reproduces stereotypes and interpretations of disability, despite themes I and II highlighting some exemptions for physiotherapy clinics and physiotherapists’ approach in their communication. Indeed, within the context of Foucauldian medical discourse, although physiotherapists are part of the medical system, their approach does not fully align with the dominant discourse of medicine. Physiotherapists and their clinics adopt an inclusive approach aimed at mitigating the dominant discourse surrounding disability, allowing them to intentionally prioritize empathy and inclusivity throughout the long-term rehabilitation process. However, within all healthcare professionals engaged in the rehabilitation process, including physiotherapy, the perception of the body and the concept of disability persistently reproduce the notion of the body as a machine, identified by iconic representations (e.g., MAs).
These understandings illustrate how the concept of disability is constructed and reproduced through initial interactions within the medical system, and how this framing limits clients’ sense of empowerment and hinders social inclusion. This contrasts with the client’s perspective, which predominantly interprets the body and disability through the lens of social aspects. This doesn’t imply that clinical recovery isn’t essential to them, but it also highlights their social needs—not fully considered by healthcare professionals. All themes discussed can extend to public discourse, reinforcing the perceptions of negative stereotypes of disability. Following physiotherapists’ inclusive approach (Themes I and II), we suggest promoting inclusivity across all forms of interaction, services, and assistive product design to help alleviate negative stereotypes in movement disability discourse. Finally, the Foucauldian medical discourse provided a framework for identifying and tracking how representations of imbalances, inequities, and stereotypes surrounding disability are perpetuated.
Limitations and future studies
In this study, our access to clients’ perspectives during rehabilitation was limited due to ethical considerations. Our findings need to be read in light of the epistemic asymmetry inherent in clinicians speaking about, rather than with, clients (Freeman 2015; Wardrope and Stewart 2025). As emphasized in critical disability studies, the absence of lived voices risks reinforcing the silencing of disabled individuals (Yoshida and Shanouda 2015). Future research should establish ethical protocols to investigate clients’ thoughts more comprehensively. While physiotherapists provide valuable insights through their close interactions with MA users, future research should also incorporate the lived experiences of these users, along with perspectives from other stakeholders, to support a more holistic understanding and inform user-centered design and policy. Although physiotherapists appeared to approach certain aspects of modern medicine differently in the two themes, this may reflect their tendency to present their profession in a favorable light during interviews. Nevertheless, we attempted to analyze the data through both semantic and latent dimensions. We recommend that future studies compare the interviews of all healthcare professionals involved in the rehabilitation process. Additionally, investigating medical discourses on disability within social contexts—beyond clinical settings and rehabilitation periods—could provide valuable insights. For example, future research could use the WHO’s ICF (2002) framework to integrate medical, social, personal, and environmental factors, better capturing MA users’ experiences and promoting an enablement-focused perspective. Exploring representations in real-life scenarios and on social media platforms would enhance our understanding of how stereotypes related to the discourse of mobility disabilities are perpetuated.
Data availability
The datasets collected during this study are not publicly available due to ethical protocols and the absence of permission for data sharing.
Notes
The International Classification of Functioning, Disability, and Health (ICF) is a framework developed by the World Health Organization (WHO) to understand and describe health and health-related states.
References
Alkhaibari RA, Smith-Merry J, Forsyth R, Raymundo GM (2023) Patient-centered care in the Middle East and North African region: a systematic literature review. BMC Health Serv Res 23:135. https://doi.org/10.1186/s12913-023-09132-0
Annalee (2017) Disability, representation, and the X-Men. The Bias. https://thebias.com/2017/10/31/disability-representation-and-the-x-men/
Aparicio-Martinez P, Perea-Moreno A-J, Martinez-Jimenez MP, Redel-Macías MD, Pagliari C, Vaquero-Abellan M (2019) Social media, thin-ideal, body dissatisfaction and disordered eating attitudes: an exploratory analysis. Int J Environ Res Public Health 16(21):4177. https://doi.org/10.3390/ijerph16214177
Arribas-Ayllon M, Walkerdine V (2008) Foucauldian discourse analysis. In: Willig C & Stainton-Rogers W (eds). Sage. pp 91–108. https://orca.cardiff.ac.uk/id/eprint/24763/
Asghar S, Edward Torrens G, Iftikhar H, Welsh R, Harland R (2020) The influence of social context on the perception of assistive technology: Using a semantic differential scale to compare young adults’ views from the United Kingdom and Pakistan. Disabil Rehabil Assist Technol 15(5):563–576. https://doi.org/10.1080/17483107.2019.1646819
Bandura A (1977) Social learning theory. Englewood Cliffs, NJ: Prentice Hall
Barbareschi G, Carew MT, Johnson EA, Kopi N, Holloway C (2021) When they see a wheelchair, they’ve not even seen me”—factors shaping the experience of disability stigma and discrimination in Kenya. Int J Environ Res Public Health 18(8):4272. https://doi.org/10.3390/ijerph18084272
Barker DJ, Reid D, Cott C (2004) Acceptance and meanings of wheelchair use in senior stroke survivors. Am J Occup Ther 58(2):221–230. https://doi.org/10.5014/ajot.58.2.221
Barlew L, Secrest J, Guo Z, Fell N, Haban G (2013) The experience of being grounded: a phenomenological study of living with a wheelchair. Rehabil Nurs J 38(4):193. https://doi.org/10.1002/rnj.96
Barradell S, Scholten I (2024) How, and to what end, is the WHO-ICF framework represented in physiotherapy? Insights from a qualitative research synthesis. Physiother Theory Pract 41(4):792–809. https://doi.org/10.1080/09593985.2024.2370345
Barthes R (1978) Image-music-text (trans: Heath S). New York, NY: Hill and Wang
Bensing JM, Dronkers J (1992) Instrumental and affective aspects of physician behavior. Med Care 30(4):283–298. https://doi.org/10.1097/00005650-199204000-00001
Braun V, Clarke V (2019) Reflecting on reflexive thematic analysis. Qual Res Sport Exerc Health 11(4):589–597. https://doi.org/10.1080/2159676X.2019.1628806
Braun V, Clarke V (2006) Using thematic analysis in psychology. Qual Res Psychol 3(2):77–101. https://doi.org/10.1191/1478088706qp063oa
Braun V, Clarke V (2012) Thematic analysis. In: APA handbook of research methods in psychology, Vol 2: Research designs: quantitative, qualitative, neuropsychological, and biological. American Psychological Association. pp 57–71. https://doi.org/10.1037/13620-004
Braun V, Clarke V (2022) Conceptual and design thinking for thematic analysis. Qual Psychol 9(1):3–26. https://doi.org/10.1037/qup0000196
Bury MR (1986) Social constructionism and the development of medical sociology. Sociol Health Illn 8(2):137–169. https://doi.org/10.1111/1467-9566.ep11340129
Byrne D (2022) A worked example of Braun and Clarke’s approach to reflexive thematic analysis. Qual Quant 56(3):1391–1412. https://doi.org/10.1007/s11135-021-01182-y
Chalopin J, Heyward A, Bianchi B, Adams D, Berger H, Welker F (1983) Inspector Gadget [Animation, Action, Adventure]. https://www.imdb.com/title/tt0085033/
Chan F, Livneh H, Pruett S, Wang C-C, Zheng L (2009) Societal attitudes toward disability: concepts, measurements, and interventions. In: Understanding psychosocial adjustment to chronic illness and disability. Springer Publishing Company, New York, NY
Chartered Society of Physiotherapy (2022) Disabled, not defeated. The Chartered Society of Physiotherapy. https://www.csp.org.uk/frontline/article/disabled-not-defeated
Craven, J (2019) “Form follows function” is the most famous phrase in architecture. ThoughtCo. https://www.thoughtco.com/form-follows-function-177237
Cucuzzella C, Rasoulivalajoozi M, Farzamfar G (2024) Spatial experience of cancer inpatients in the oncology wards: a qualitative study in visual design aspects. Eur J Oncol Nurs 70:102552. https://doi.org/10.1016/j.ejon.2024.102552
Dahm M (2012) Coming to terms with medical terms – exploring insights from native and non-native English speakers in patient-physician communication. HERMES J Lang Commun Bus 49:Article 49. https://doi.org/10.7146/hjlcb.v25i49.97739
Dalboni GL, Garcêz, Regiane L, Assis, Ítalo C, Vaz DV (2023) Conceptions of disability among physiotherapists: an exploratory qualitative study. Physiother Theory Pract 39(8):1662–1671. https://doi.org/10.1080/09593985.2022.2042757
Dawood S (2018) Redesigning the wheelchair symbol to include “invisible disabilities.” Design Week. https://www.designweek.co.uk/issues/30-july-5-august-2018/why-the-wheelchair-symbol-should-be-rethought-to-include-invisible-disabilities/
Derbyshire DW, Spencer AE, Grosskopf B, Blackmore T (2023) The importance of disability representation to address implicit bias in the workplace. Front Rehabil Sci 4:1048432. https://doi.org/10.3389/fresc.2023.1048432
Derrida J, Spivak GC, Butler J (2016) Of grammatology. Johns Hopkins University Press. https://doi.org/10.56021/9781421419954
Desmet P, Hekkert P (2007) Framework of product experience. Int J Des 1(1):57–66
Devotta K, Wilton R, Yiannakoulias N (2013) Representations of disability in the Canadian news media: a decade of change? Disabil Rehabil 35(22):1859–1868. https://doi.org/10.3109/09638288.2012.760658
Diener I (2021) Physiotherapy support for self-management of persisting musculoskeletal pain disorders. South Afr J Physiother 77(1):1564. https://doi.org/10.4102/sajp.v77i1.1564
Donovan HS, Ward SE, Song MK, Heidrich SM, Gunnarsdottir, S, Phillips CM (2007) An update on the representational approach to patient education. J Nurs Scholarsh 39(3):259–265. https://doi.org/10.1111/j.1547-5069.2007.00178.x
Dos Santos ADP, Ferrari ALM, Medola FO, Sandnes FE (2022) Aesthetics and the perceived stigma of assistive technology for visual impairment. Disabil Rehabil Assist Technol 17(2):152–158. https://doi.org/10.1080/17483107.2020.1768308
Eveleth R (2018) Transhumanism is tempting—until you remember inspector gadget. WIRED. https://www.wired.com/story/what-inspector-gadget-can-teach-us-about-transhumanism/
Faraji A, Valajoozi MR (2014) Interactive foot orthosis (IFO) for people with drop foot. Appl Mech Mater 464:129–134
Federici FM (ed) (2022) Language as a social determinant of health: translating and interpreting the COVID-19 pandemic. https://doi.org/10.1007/978-3-030-87817-7
Feldner HA, Evans HD, Chamblin K, Ellis LM, Harniss MK, Lee D, Woiak J (2022) Infusing disability equity within rehabilitation education and practice: a qualitative study of lived experiences of ableism, allyship, and healthcare partnership. Front Rehabil Sci 3:947592. https://doi.org/10.3389/fresc.2022.947592
Flynn TR (1993) Foucault and the eclipse of vision’. In: Levin DM (ed) Modernity and the hegemony of vision. University of California Press, Berkeley
Foucault M (1972) Archaeology of Knowledge, 2nd edn. Routledge. London, UK. https://doi.org/10.4324/9780203604168
Foucault M (1994) Birth of the clinic: an archaeology of medical perception. Vintage, New York, NY
Foucault M (1995) Discipline & Punish: the birth of the prison (trans: Sheridan A). Vintage Books, New York, NY
Foucault M (2008) Power/Knowledge. In The New Social Theory Reader, 2nd edn. Routledge, London, UK
Foucault M (2010) The birth of biopolitics: lectures at the Collège de France, 1978-1979, 1st edn. Picador, New York, NY
Foucault M, Rabinow P (1997) Essential Works of Foucault, 1954-1988 [Philosophy]. Philpapers.Org/Rec/FOUEWO. https://philpapers.org/rec/FOUEWO
Fox NJ (2016) Health sociology from post-structuralism to the new materialisms. Health 20(1):62–74. https://doi.org/10.1177/1363459315615393
Fredericks JP, Visagie S, van NL (2024) A qualitative exploration of community mobility experiences of wheelchair users. Afr J Disabil 13(1):1253. https://doi.org/10.4102/ajod.v13i0.1253
Freeman L (2015) Confronting diminished epistemic privilege and epistemic injustice in pregnancy by challenging a “panoptics of the womb. J Med Philos 40(1):44–68. https://doi.org/10.1093/jmp/jhu046
Galli G, Lenggenhager B, Scivoletto G, Molinari M, Pazzaglia M (2015) Don’t look at my wheelchair! The plasticity of longlasting prejudice. Med Educ 49(12):1239–1247. https://doi.org/10.1111/medu.12834
Gibson BE, Teachman G (2012) Critical approaches in physical therapy research: investigating the symbolic value of walking. Physiother Theory Pract 28(6):474–484. https://doi.org/10.3109/09593985.2012.676936
Gilbbons C (2023) In-depth interviews in qualitative research: Not “just a chat.” Quirkos Qualitative Research Blog. https://www.quirkos.com/blog/post/in-depth-interviews-in-qualitative-research/
Guest G, Bunce A, Johnson L (2006) How many interviews are enough?: An experiment with data saturation and variability. Field Methods 18(1):59–82. https://doi.org/10.1177/1525822X05279903
Haghighat H (2007) From structuralism to post-structuralism. Semin Univ J Methodol Soc Sci 51:91–110
Hall S, Evans J, Nixon S (2013) Representation: cultural representations and signifying practices, 2nd edn. Sage Publications, London, UK
Hammond R, Cross V, Moore A (2016) The construction of professional identity by physiotherapists: a qualitative study. Physiotherapy 102(1):71–77. https://doi.org/10.1016/j.physio.2015.04.002
Haskard Zolnierek KB, DiMatteo MR (2009) Physician communication and patient adherence to treatment: a meta-analysis. Med Care 47(8):826–834. https://doi.org/10.1097/MLR.0b013e31819a5acc
Higgs P, Scambler G (1998) Modernity, medicine and health. Routledge. https://www.routledge.com/Modernity-Medicine-and-Health/Higgs-Scambler/p/book/9780415149396
Human Rights Watch Council (2018) Iran: people with disabilities face discrimination and abuse. https://www.hrw.org/news/2018/06/26/iran-people-disabilities-face-discrimination-and-abuse
Irvine A (2011) Duration, dominance and depth in telephone and face-to-face interviews: a comparative exploration. Int J Qual Methods 10(3):202–220. https://doi.org/10.1177/160940691101000302
Jiotsa B, Naccache B, Duval M, Rocher B, Grall-Bronnec M (2021) Social media use and body image disorders: association between frequency of comparing one’s own physical appearance to that of people being followed on social media and body dissatisfaction and drive for thinness. Int J Environ Res Public Health 18(6):2880. https://doi.org/10.3390/ijerph18062880
Johnsson A, Wagman P, Boman Å, Pennbrant S (2018) What are they talking about? Content of the communication exchanges between nurses, patients and relatives in a department of medicine for older people—an ethnographic study. J Clin Nurs 27(7–8):e1651–e1659. https://doi.org/10.1111/jocn.14315
Keller ML (1993) Why don’t young adults protect themselves against sexual transmission of HIV? Possible answers to a complex question. AIDS Educ Prev 5(3):220–233
Kenny DA, Veldhuijzen W, van der Weijden T, LeBlanc A, Lockyer J, Légaré F, Campbell C (2010) Interpersonal perception in the context of doctor–patient relationships: a dyadic analysis of doctor–patient communication. Soc Sci Med 70(5):763–768. https://doi.org/10.1016/j.socscimed.2009.10.065
Kleinman A, Eisenberg L, Good B (1978) Culture, illness, and care. Ann Intern Med 88(2):251–258. https://doi.org/10.7326/0003-4819-88-2-251
Krippendorff K (2006) The semantic turn: a new foundation for design. https://www.routledge.com/The-Semantic-Turn-A-New-Foundation-for-Design/Krippendorff/p/book/9780415322201
Kvale S (2004) Interviews: an introduction to qualitative research interviewing. Sage Publications
Lau RR, Bernard TM, Hartman KA (1989) Further explorations of common-sense representations of common illnesses. Health Psychol 8(2):195–219. 10.1037//0278-6133.8.2.195
LeBlanc TW, Hesson A, Williams A, Feudtner C, Holmes-Rovner M, Williamson LD, Ubel PA (2014) Patient understanding of medical jargon: a survey study of U.S. medical students. Patient Educ Couns 95(2):238–242. https://doi.org/10.1016/j.pec.2014.01.014
Lenney M, Sercombe H (2002) Did you see that guy in the wheelchair down the pub?’—Interactions across difference in a public place. Disabil Soc 17(1):5–18. https://doi.org/10.1080/09687590120100093
Luke H (2003) Medical education and sociology of medical habitus: “it’s not about the stethoscope!”, 2003rd edn. Springer, Netherlands
Matin P (2021) Introduction of medical anthropology, 1st edn. Farhameh, Tehran, Iran
Media Smart (2024) Common portrayals of persons with disabilities | MediaSmarts [Canada’s Center for Digital Media Literacy]. Mediasmart.Ca. https://mediasmarts.ca/digital-media-literacy/media-issues/diversity-media/persons-disabilities/common-portrayals-persons-disabilities
Moradi A (2018) The concept of representation in cultural studies. Cultural Studies and Media. http://philo-media.blogfa.com/post/96#_ftnref1
Mortenson WB, Routhier F, Mahmood A, Prescott M, Labbé D, Martin Ginis KA, Miller WC (2022) Predictors of psychological distress and confidence negotiating physical and social environments among mobility device users. Am J Phys Med Rehabil 101(4):324. https://doi.org/10.1097/PHM.0000000000001816
Mosleh D (2019) Critical disability studies with rehabilitation: re-thinking the human in rehabilitation research and practice. J Humanit Rehabil. https://www.jhrehab.org/2019/11/14/making-the-case-for-critical-disability-studies-with-rehabilitation-sciences/
Nicholls DA (2019) The End of Physiotherapy. Routledge, Abingdon, Oxon
Nielsen-Bohlman L, Panzer AM, Kindig DA (2004) Health literacy: a prescription to end confusion. In: Health literacy: a prescription to end confusion. National Academies Press, US. https://www.ncbi.nlm.nih.gov/books/NBK216037/
Nimmon L, Stenfors-Hayes T (2016) The “Handling” of power in the physician-patient encounter: Perceptions from experienced physicians. BMC Med Educ 16(1):114. https://doi.org/10.1186/s12909-016-0634-0
Ocran J (2019) Disability in the media: examining stigma and identity. Disabil Soc 34(3):505–508. https://doi.org/10.1080/09687599.2018.1563987
O’Reilly OC, Shamrock AG, Rosenbaum M, Clark CR, Patterson BM (2022) Physician-patient communication in the orthopedic clinic: surgeon-identified challenges. Iowa Orthop J 42(1):275–281
Papadimitriou C (2008) Becoming en‐wheeled: the situated accomplishment of re‐embodiment as a wheelchair user after spinal cord injury. Disabil Soc 23(7):691–704. https://doi.org/10.1080/09687590802469420
Pasin T, Karatekin BD (2024) Determinants of social participation in people with disability. PLoS ONE 19(5):e0303911. https://doi.org/10.1371/journal.pone.0303911
Phelan SK, Wright, Virginia, Gibson BE (2014) Representations of disability and normality in rehabilitation technology promotional materials. Disabil Rehabil 36(24):2072–2079. https://doi.org/10.3109/09638288.2014.891055
Pitt MB, Hendrickson MA (2020) Eradicating jargon-oblivion—a proposed classification system of medical jargon. J Gen Intern Med 35(6):1861–1864. https://doi.org/10.1007/s11606-019-05526-1
Priyanti N (2018) Representations of people with disabilities in an Indonesian newspaper: a critical discourse analysis. Disabil Stud Q. https://doi.org/10.18061/dsq.v38i4.5818
Rajchman J (1988) Foucault’s art of seeing. October 44:88. https://doi.org/10.2307/778976
Rasoulivalajoozi M (2025) Pedestrians’ social empathy and interaction with wheelchair users: the impact of user gestures and mobility aid design in a pilot study. Int J Ind Ergon 109:103793. https://doi.org/10.1016/j.ergon.2025.103793
Rasoulivalajoozi M, Cucuzzella C, Farhoudi M (2025a) Domains of wheelchair users’ socio-emotional experiences: Design insights from a scoping review. Disabil Health J. https://doi.org/10.1016/j.dhjo.2025.101829
Rasoulivalajoozi M, Cucuzzella C, Farhoudi M (2025b) Perceived inclusivity in mobility aids use: a qualitative study in Iran. Disabilities 5(1):15. https://doi.org/10.3390/disabilities5010015
Rasoulivalajoozi M, Cucuzzella C, Farhoudi M (2025c) The dynamics of affective experiences with wheelchair use during rehabilitation: a qualitative study through physiotherapists’ perspectives. Acta Psychol 256:105022. https://doi.org/10.1016/j.actpsy.2025.105022
Rasoulivalajoozi M, Farhoudi M (2025) Advancing eHMI for powered wheelchairs beyond safety and communication: a pilot study on enriching social interaction through a co-design approach. Transp Res Part F Traffic Psychol Behav 114:200–215. https://doi.org/10.1016/j.trf.2025.05.036
Rasoulivalajoozi M, Touir G (2023) Spinal fusion surgery for high-risk patients: a review of hospitals information. Soc Determ Health 9:1–12. https://doi.org/10.22037/sdh.v9i1.39958
Ristić AJ, Zaharijević A, Miličić N (2021) Foucault’s concept of clinical gaze today. Health Care Anal 29(2):99–112. https://doi.org/10.1007/s10728-020-00402-0
Roter DL, Stewart M, Putnam SM, Lipkin M, Stiles W, Inui TS (1997) Communication patterns of primary care physicians. JAMA 277(4):350–356
Roush SE, Sharby N (2011) Disability reconsidered: the paradox of physical therapy. Phys Ther 91(12):1715–1727. https://doi.org/10.2522/ptj.20100389
Saia T, Vogel E, Salazar S (2024) We need a world we can operate in”: exploring the relationship between societal stigma and depression among wheelchair users. Disabil Health J 17(3):101624. https://doi.org/10.1016/j.dhjo.2024.101624
Schrift AD (2018) Foucault and poststructuralism. In: A companion to literary theory. John Wiley & Sons, Ltd. pp 176–187. https://doi.org/10.1002/9781118958933.ch14
Shadyac T (Director) (1998) Patch Adams [Biography, Comedy, Drama]. Universal Pictures, Blue Wolf Productions, Farrell/Minoff
Showstack R, Santos M, Feuerherm E, Jacobson H, Martínez G (2019) Language as a social determinant of health: an applied linguistics perspective on health equity. AAALetter. https://www.aaal.org/news/aaaletter
Soleimani B, Hossein Halimi M (2012) Aesthetic approaches to product design and development. Baghe Nazar 8(16):72–92
Steenbruggen RA, Dolleman G, van Heusden-Scholtalbers LA, Maas M, Hoogeboom TJ, Brand P, van der Wees P (2022) Quality aspects of hospital-based physiotherapy from the perspective of key stakeholders: a qualitative study. BMJ Open Qual 11(2):e001843. https://doi.org/10.1136/bmjoq-2022-001843
Stivers T, Timmermans S (2020) Medical authority under siege: how clinicians transform patient resistance into acceptance. J Health Soc Behav 61(1):60–78. https://doi.org/10.1177/0022146520902740
Street RL Jr (2003) Communication in medical encounters: an ecological perspective. In: Handbook of health communication. Lawrence Erlbaum Associates Publishers. pp 63–89, Mahwah, New Jersey
Suarez-Almazor ME (2004) Patient-physician communication. Curr Opin Rheumatol 16(2):91–95. https://doi.org/10.1097/00002281-200403000-00003
Taleporos G, McCabe MP (2002) Body image and physical disability—personal perspectives. Soc Sci Med 54(6):971–980. https://doi.org/10.1016/S0277-9536(01)00069-7
Tariq RA, Sharma S (2024) Inappropriate medical abbreviations. In StatPearls. StatPearls Publishing. http://www.ncbi.nlm.nih.gov/books/NBK519006/
Teachman G, McDonough P, Macarthur C, Gibson BE (2020) Interrogating inclusion with youths who use augmentative and alternative communication. Sociol Health Illn 42(5):1108–1122. https://doi.org/10.1111/1467-9566.13087
Thomas C (with Internet Archive) (1999) Female forms: experiencing and understanding disability. Open University Press, Buckingham. http://archive.org/details/femaleformsexper0000thom
Tong A, Sainsbury P, Craig J (2007) Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care 19(6):349–357. https://doi.org/10.1093/intqhc/mzm042
Toombs SK (1990) The meaning of illness: a phenomenological approach to the patient-physician relationship. Thesis, Rice University. https://scholarship.rice.edu/handle/1911/16399
Umar U, Lestari Natalia D, Franciska Ullyana Y (2024) Book review: disability, media, and representations (other bodies). Disabil Soc 39(10):2747–2749. https://doi.org/10.1080/09687599.2024.2355780
Vennavally-Rao J (2022) Some airline passengers with wheelchairs say they’re treated like second-class citizens. CTVNews. https://www.ctvnews.ca/canada/some-airline-passengers-with-wheelchairs-say-they-re-treated-like-second-class-citizens-1.6136609
Wardrope A, Stewart H (2025) Epistemic privilege, phenomenology and symptomatology in functional/dissociative seizures. Soc Epistemol 39(2):134–149. https://doi.org/10.1080/02691728.2024.2400066
White CA (2004) Meaning and its measurement in psychosocial oncology. Psychooncology 13(7):468–481. https://doi.org/10.1002/pon.815
White K (2002) An introduction to the sociology of health and illness. SAGE Publications, London, UK
WHO (2002) Towards a common language for functioning, disability and health ICF. World Health Organization. https://cdn.who.int/media/docs/default-source/classification/icf/icfbeginnersguide.pdf?sfvrsn=eead63d3_4&download=true
Williams J (2005) Introduction: what is poststructuralism? (Chapter 1). In: Understanding poststructuralism. Acumen Publishing. pp 1–24 https://www.cambridge.org/core/books/abs/understanding-poststructuralism/introduction-what-is-poststructuralism/56B4129DF3B18481D8FDD586E8369EA4
World Physiotherapy (2019) Description of physical therapy policy statement. World Physiotherapy. https://world.physio/sites/default/files/2020-07/PS-2019-Description-of-physical-therapy.pdf,
Yoshida KK, Shanouda F (2015) A culture of silence: modes of objectification and the silencing of disabled bodies. Disabil Soc 30(3):432–444. https://doi.org/10.1080/09687599.2015.1019042
Acknowledgements
We would like to thank the Mani Physiotherapy Center, Novin Physiotherapy Clinic, and all participants for their invaluable assistance during participant interviews. This research was funded by the Social Science and Humanities Research Council- May 2020–April 2024, grant number 390-2018-0025.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study. Author 1 was responsible for data curation, formal analysis, methodology, and visualization, and contributed to both the drafting and critical revision of the manuscript. Author 2 contributed to supervising the research process, validation, and drafting and revising the manuscript. Author 3 was involved in the investigation, visualization, critical revision, and ensured validation. Author 4 contributed to the methodology and critical revision of the manuscript. All authors read and approved the final draft.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical statement
Ethical approval for this study was obtained from the Human Research Ethics Committee of Concordia University, Montreal, Canada (Certification Number: 30016116). The study was reviewed and approved on February 18, 2022, prior to data collection. All research procedures involving human participants were conducted in accordance with the ethical standards of the institutional research committee. The approval covered all procedures related to participant recruitment, data collection, storage, and analysis.
Informed consent
Written informed consent was obtained from all participants prior to their inclusion in the study. Participants were informed about the purpose of the research, the voluntary nature of their participation, their right to withdraw at any time without penalty, and the confidentiality of their responses. Consent covered participation in the study, use of anonymized data for analysis, and permission to publish aggregated findings. All consent procedures were carried out by the principal investigator from February 2022 to January 2023, following Concordia University’s ethical guidelines.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Rasoulivalajoozi, M., Cucuzzella, C., Farhoudi, M. et al. Intersecting perceptions: a Foucauldian study of mobility disability representations in clinical encounters from physiotherapists’ perspectives. Humanit Soc Sci Commun 12, 1829 (2025). https://doi.org/10.1057/s41599-025-06109-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1057/s41599-025-06109-8