Abstract
This study aimed to comprehensively map the patient journey and identify critical facilitators and barriers to healthcare access for patients with Atypical Hemolytic-Uremic Syndrome (aHUS) in China. A qualitative approach, guided by the Levesque framework, was used to explore aHUS patients’ experiences. Participants included aHUS patients, caregivers (when patients were unable to independently participate due to age or frailty), and specialists. Semi-structured interviews were conducted via Tencent Meeting and telephone, and the visual timeline method was used to facilitate detailed recounting of patient experiences. Thematic analysis, incorporating frequency analysis and field notes, was performed on the collected data. The study was conducted in Shandong, China, from January to August 2023. Interviews were conducted with five adult patients, four caregivers, and nine aHUS specialists. Key facilitators to healthcare access for aHUS patients included family involvement, patient autonomy, online consultations, robust public transportation, social capital, and various forms of social support. Barriers identified included low awareness of aHUS, inadequate insurance coverage, substantial non-medical burdens, gaps in professional knowledge, suboptimal diagnostic techniques, underdeveloped referral systems, and the absence of dedicated patient organizations. This study identifies key barriers and facilitators affecting aHUS patients’ healthcare access and highlights the emotional, financial, and structural challenges they face. The study advocates for enhanced public awareness of rare diseases, integrating patient autonomy into decision-making, optimizing telemedicine, expanding insurance coverage, and advancing professional expertise through training and standardized diagnostics. These findings underscore the need for equitable, patient-centered care and call for further evaluation of policy impacts in China and other middle-income settings.
Similar content being viewed by others
Introduction
Atypical Hemolytic-Uremic Syndrome (aHUS) is a rare, genetic, life-threatening condition characterized by the systemic formation of blood clots in small blood vessels, leading to microangiopathic hemolytic anemia, thrombocytopenia, and acute kidney failure(Formeck & Swiatecka-Urban, 2019; Noris & Remuzzi, 2009; Schaefer et al., 2018). The prevalence of aHUS is 4.9 cases per million people, with higher rates among children and adolescents, ranging from 2.2 to 9.4 cases per million in those under 17 years old (K. Yan, Desai, Gullapalli, Druyts, & Balijepalli, 2020). Despite advancements in treatment, particularly with complement inhibitors that have significantly improved patient outcomes(Legendre et al., 2013; Rosales, Riedl, & Zimmerhackl, 2010), aHUS patients continue to face substantial challenges in accessing healthcare services.
These challenges stem from the complex clinical nature of aHUS, the need for continuous and often expensive treatments, and the broader difficulties of navigating healthcare systems that are not fully equipped to manage rare diseases(Nga, Palma, Neto, & de Andrade, 2022; Raina et al., 2019). Understanding the facilitators and barriers to healthcare access for aHUS patients is critical for identifying gaps in care and developing targeted strategies to improve healthcare accessibility for this vulnerable population. However, most current research focuses on the biological mechanism of aHUS (Spasiano et al., 2023), with limited exploration of patients’ experiences and their healthcare journeys.
Notably, existing studies on aHUS have largely overlooked the practical challenges patients face, with only one study analyzing treatment journeys using data from social media platforms like Twitter and Facebook(Maurya et al., 2022). This gap is particularly pronounced in China where aHUS patients may encounter additional hurdles, such as limited awareness of rare diseases among healthcare providers(Li et al., 2021), unequal distribution of medical resources(Collaborators, 2018; X. Yan, He, and Dong, 2020), and challenges related to drug accessibility and affordability(D. Dong and Wang, 2016; X. Y. Zhang, Dai, Long, Chen, and Alhafi, 2024).
To address these gaps, this study adopts a qualitative method to explore the diagnostic and treatment experiences of aHUS patients in China. By mapping the patient journey, this study aims to provide a comprehensive understanding of the lived experiences, unmet needs, and healthcare challenges faced by aHUS patients. The findings will offer valuable insights to inform evidence-based recommendations for developing more patient-centered healthcare services tailored to the needs of aHUS patients.
Materials and methods
Study design
This study focuses on aHUS patients, a group facing a heavy disease burden yet underrepresented within the rare disease community. By mapping the patient journey of individuals with aHUS, the study seeks to answer a critical research question: what are the key barriers and facilitators that aHUS patients encounter when accessing healthcare services? Given the rarity of aHUS, a qualitative research design was employed to deeply explore patient experiences, uncovering the underlying reasons behind barriers and facilitators beyond mere identification. To ensure a rigorous and transparent approach, this study adhered strictly to the Standards for Reporting Qualitative Research (SRQR) (O’Brien, Harris, Beckman, Reed, and Cook, 2014).
Theoretical foundation
This study used the theoretical framework developed by Levesque et al. (Levesque, Harris, & Russell, 2013) to guide the development of interview guidelines and data analysis. The Levesque framework conceptualizes healthcare accessibility as a process, focusing on factors influencing patients’ ability to perceive, seek, reach, pay for, and engage in care, rather than merely on systemic issues(Cu, Meister, Lefebvre, & Ridde, 2021). By centering on patients’ care-seeking journeys, the framework explores the interactions between the health system (supply) and patients (demand) at different stages of care. On the supply side, it outlines five dimensions of healthcare accessibility: (1) approachability, (2) acceptability, (3) availability, and accommodation, (4) affordability, and (5) appropriateness. On the demand side, it defines five corresponding abilities of patients: the ability to perceive, seek, reach, pay, and engage. Given its widespread application in studies of healthcare accessibility (Cu et al., 2021; Henry, Beruf, & Fischer, 2020; Kourgiantakis et al., 2023; Schwarz, Schmidt, Bobek, & Ladurner, 2022), we adopted this framework in this study to explore the barriers and facilitators aHUS patients face. Interview guidelines (i.e., one for patients and the other one for specialists) were initially drafted and refined through four sessions with a panel experienced in kidney care and qualitative research methods, and two pilot interviews with a female aHUS patient and a male specialist. The interviewees have multi-disciplinary backgrounds, including nursing. All interviewers received training to conduct the interviews, and none had a prior relationship with the participants.
Sampling and recruitment
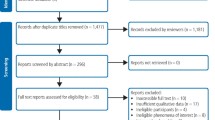
We used purposive sampling to select diverse participants across gender, age, region, urban-rural classification, and treatment methods to accurately represent aHUS patients in China. In collaboration with hospitals and rare disease organizations, we invited eligible patients who met the following criteria: (1) definitive diagnosis of aHUS; (2) provision of informed consent; and (3) fulfillment of five specified criteria (gender (male/female), geographic region (northern/southern China), place of residence (urban/rural), age group (children, young and middle-aged adults, elderly), and treatment type (hemodialysis, traditional immunomodulatory therapy, or eculizumab). Recruitment continued until thematic saturation was reached, involving a total of 10 patients. Demographic details are presented in Table 1. Due to their conditions, five children under the age of 7 and one frail 58 year-old patient were unable to participate independently, so their primary caregivers were involved to ensure comprehensive engagement. Most interviews were conducted online, with two via telephone, lasting between 30 and 72 min. For participants unfamiliar with Mandarin or primarily speaking in dialect, interviews were facilitated using a combination of spoken responses and chat box typing to ensure effective communication. Adult patients were diagnosed between the ages of 21 and 57, while pediatric patients ranged from 6 months to 7 years. The time from symptom onset to the first consultation was 1–4 days for children and 1 day to 2 months for adults. From the initial healthcare visit to diagnosis, the interval was 1–5 days for children and 20 days to 3.5 months for adults. Adults usually sought care at city-level hospitals for severe symptoms, while children with milder symptoms visited community hospitals. Most patients ultimately received care in Beijing, consulting 2 to 5 different facilities during their diagnostic journey.
For recruiting aHUS specialists, snowball sampling was employed to enhance geographical and institutional reach and ensure diverse expertise(Johnson, 2014). The recruitment process began with online searches, followed by expert recommendations until thematic saturation was achieved. A total of 9 aHUS specialists from various regions of China, including Eastern (Shanghai, Zhejiang), Western (Sichuan), Southern (Guangdong), and Northern (Beijing)areas, were invited to participate. Detailed demographic information of the specialists is provided in Table 2. All interviews were conducted online and each session lasted between 40 and 60 min.
Data collection
From January to June 2023, in-depth, semi-structured interviews were conducted using internet-based platforms (i.e., Tencent and WeChat) to ensure inclusive participation. This approach allowed for remote engagement with participants from diverse geographic regions and backgrounds. We purposively sampled two groups of interviewees: (1) aHUS specialists and (2) aHUS patients or their primary caregivers. While patients’ perspectives remained central to the analysis, caregivers were included to provide essential insights in cases where patients were too young, frail, or unable to participate in interviews independently. Additionally, specialists’ perspectives were incorporated to complement the narratives of patients and caregivers, providing a clinical lens that enriched the findings and highlighted systemic areas for improvement.
For patient interviews, the visual timeline method was employed to help patients sequentially recount their experiences, thereby enhancing clarity and detail(Hurtubise & Joslin, 2023). This method not only improves data quality but also engages participants by structuring the interview process and data analysis(Bremner, 2020). It has been widely used to document patient histories, treatment sequences, and disease progression(Pell et al., 2020). In this study, we began each session by outlining interview objectives and the expected role of interviewees when using the timeline, as shown in Supplementary Fig. 1. Tencent and WeChat allowed interviewers and participants to collaboratively complete the timeline in real-time, with one interviewer guiding the conversation and the other displaying the timeline template on a shared screen. Participants could view and contribute to the timeline simultaneously. For specialist interviews, the visual timeline was not used, as their expertise often provided a broader understanding of the disease, which did not align with the chronological data presented by visual timelines. Besides, researchers also conducted field notes and interview memos in the online videos of all interviews to document non-verbal cues, such as participants’ tone of voice, emotional expressions, pauses, and notable reactions. These contextual observations captured the nuances of participants’ responses and provided richer insights into the relative importance they attributed to various facilitators and barriers(Phillippi & Lauderdale, 2018).
Data analysis
The data analysis was conducted using MAXQDA 2020, which facilitated the systematic coding of verbatim interview transcripts, interview memos, and field notes. The initial coding framework was constructed based on the Levesque accessibility framework, focusing on the five key domains: “ability to perceive”, “ability to seek”, “ability to reach”, “ability to pay”, and “ability to engage”.
The analysis followed an iterative process, involving three rounds of coding and team discussions to ensure a comprehensive representation of the barriers and facilitators that aHUS patients encounter in accessing healthcare. To address divergent perspectives between patients, caregivers (in cases where patients were unable to participate independently due to age or frailty), and specialists, we employed a cross-referencing approach. Consensus was reached by synthesizing the issues raised by both patients and specialists, with a focus on identifying systemic factors that were relevant across all perspectives. For example, patients frequently expressed concerns about delayed diagnoses and the lack of awareness of aHUS among healthcare providers, while specialists highlighted the absence of standardized diagnostic protocols and limitations in diagnostic tools. These differing perspectives were reconciled by identifying shared systemic barriers, such as gaps in professional knowledge and diagnostic processes, which were subsequently categorized under the “ability to engage” stage in our final analysis.
To ensure the validity and applicability of our findings, the research team engaged in an iterative validation process with both patients and specialists. Given our continued, positive relationships with some of the patients, we were able to revisit the findings and interpretations with them, seeking their feedback to refine our interpretations. This validation process ensured that the findings were grounded in participants’ experiences and reflective of real-world healthcare contexts.
Ethical considerations
Ethical approval was obtained from the Ethics Committee of Centre for Health Management and Policy Research, Shandong University (No. ECSHCMSDU20211103). Participants were informed that the interviews would be audio-recorded and the data would be transcribed and anonymized to protect their privacy. All participants provided informed consent by signing a document confirming their voluntary participation from January to August 2023(Assembly, 2013), either through photographing a paper signature and sending it or by providing an electronic signature online. Furthermore, all researchers involved in processing raw interview data signed a data processing agreement to ensure data confidentiality and integrity.
Results
Overview of the patient journey of aHUS
This study mapped the care trajectories of aHUS patients through the lens of Levesque’s healthcare accessibility framework, which conceptualizes access as a multi-stage process: perceiving, seeking, reaching, paying for, and engaging with care. Drawing on interviews with patients and healthcare professionals, we identified key facilitators and barriers at each stage. In addition to thematic coding and frequency analysis, we integrated insights from interview memos and field notes to contextualize the structural dynamics shaping individual experiences.
Mapping the patient journey of aHUS
To foreground the lived experiences behind the structural themes analyzed below, we begin with two patient trajectories drawn from our interviews. These narratives were selected to illustrate key inflection points along the aHUS care continuum. These narratives are presented in Box 1 and Box 2 and were selected to reflect different points along the diagnostic and treatment spectrum. They are based on interviews with two participants (P1 and P5) whose detailed narratives offer rich trajectories along the aHUS care continuum. By centering these experiences, we aim to complement the thematic analysis with greater humanistic depth and to underscore how structural barriers are encountered and navigated in daily life.
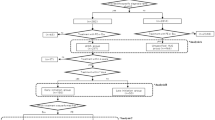
The narratives above reflect key inflection points that also recur across our broader dataset. Building on these individual trajectories, the following thematic analysis—drawing perspectives from both patient and healthcare professionals—maps common barriers and facilitators across the five stages of access. At the Perceive stage, both groups highlighted limited awareness of aHUS and fragmented recognition of available services. During the Seek stage, patient agency was viewed as essential, though often constrained by differences in education and language. At the Reach stage, challenges such as inadequate referral systems and the geographic concentration of rare disease care were partially offset by the expanding role of telemedicine. In the Pay stage, gaps in insurance coverage and significant out-of-pocket costs, including indirect expenses, were consistently noted. Finally, at the Engage stage, professional knowledge gaps and a lack of care coordination continued to impede long-term management, even when patients remained committed to treatment. To synthesize these patterns, we developed a unified patient journey map (Fig. 1). This map visually integrates the key barriers and facilitators identified across the interviews, providing a comprehensive overview of the critical touchpoints throughout the healthcare journey.
The patient medical journey from different stakeholder perspective in aHUS.
Frequency of identified facilitators and barriers
To enhance the transparency and interpretability of our findings, we incorporated a frequency table (Table 3), a widely recognized tool in qualitative research for systematically presenting data patterns and supporting visual representations(Bletzer, 2015). This table summarizes the distribution of facilitators and barriers across the stages of the patient journey, emphasizing the relative importance of these factors as reflected in the interviews. By highlighting both shared and unique priorities across groups, the table provides a structured and rigorous overview of the key facilitators and barriers identified in this study.
Barriers and facilitators at the stage of ability to perceive
The ability to perceive is a fundamental determinant of health behaviors, as highlighted in various behavioral theories. In this study, the ability to perceive refers to patients’ awareness of early aHUS symptoms, their understanding of available treatments, and their ability to make informed decisions about seeking healthcare. At this stage, healthcare-seeking behaviors were shaped by both facilitators and barriers. Key barriers included limited awareness of aHUS, inadequate recognition of available healthcare services, and the varied severity of aHUS symptoms. Family involvement emerged as a crucial facilitator, enabling patients to take symptoms seriously and seek prompt medical attention.
Limited awareness of aHUS
A lack of awareness about aHUS was the most frequently reported barrier during this stage, with 28 mentions from patients and specialists (Table 3). Patients attributed early symptoms of aHUS, such as abdominal pain, fatigue, and edema, to more common and less severe conditions, such as a cold. Patients often overlooked the further delayed recognition of these symptoms, as some patients believed severe health issues, such as hypertension, were unlikely affect younger people:
“At the very beginning, I had a slight fever and loss of appetite. I thought I was fine. that Maybe I had a cold. I didn’t want to go to the hospital.” (P3)
“I didn’t consider the possibility of having blood pressure issues. Young people don’t need to measure their blood pressure.” (P5)
Field notes revealed signs of frustration and regret (e.g., signed and paused) when patients reflected on these delays. Specialists also emphasized this issue:
“Patients who come to our hospital are typically in critical condition. This is often because they either did not pay attention to the initial symptoms or were unaware of the potential risks, only seeking medical attention when their condition has become severe.” (S4)
Inadequate recognition of available healthcare services
The inadequate recognition of available healthcare services emerged as another prominent barrier, with 16 mentions across interviews (Table 3). Patients often expressed uncertainty about service locations and doubted the quality of care available at local facilities, leading to delays in accessing specialized care:
“I feel that the hospital here may not be very good, the treatment can’t see the effect. It is only a small local hospital…In Qingdao, plasmapheresis wasn’t performed until we went to Beijing, I think the treatment was delayed.” (P1)
Specialists corroborated this issue, acknowledging their limited experience with aHUS-specific treatments, such as eculizumab. This unfamiliarity, compounded by high treatment costs and a lack of clinical guidelines, created hesitancy among healthcare providers:
“Very few people have used this drug, we have limited experience with it, and it is also quite expensive, so we tend to avoid using it.” (S5)
This limited familiarity among specialists not only delayed the introduction of effective therapies but also mirrored patients’ own uncertainties about treatment options. Both factors together exacerbated the broader issue of inadequate recognition of available healthcare services, reducing the likelihood that patients could access optimal care in a timely manner.
Varied severity of aHUS symptoms
The severity of aHUS symptoms varied among patients and had a notable influence on their perceptions and decisions regarding healthcare access (4 mentions in Table 3). For those experiencing severe symptoms, there was often a heightened urgency to seek medical care. Field notes documented a heightened emotional expression from patients when discussing severe symptom onset. In contrast, patients with milder symptoms, or their families, were more likely to delay seeking treatment, either due to an underestimation of the condition’s seriousness or uncertainty about the effectiveness of available care options:
“At that time, the child’s health condition was already very poor, and we felt that any treatment provided would always improve his situation.” (P7)
Family involvement
The involvement of caregivers or family members proved to be a crucial facilitator, with 17 mentions (Table 3). Caregivers played a vital role in recognizing early signs of the condition and prompting timely medical consultations, particularly in cases where patients were unaware of their symptoms or underestimated their severity. Field notes captured that patients often expressed gratitude or reliance on their caregivers, with subtle shifts in tone (such as softened voices or a sense of warmth), when describing the proactive role caregivers played in addressing their health concerns:
“My girlfriend noticed that my complexion is getting yellower and my face is slightly swollen, so she made an appointment with a specialist for me to go to the hospital and have a check-up.” (P3)
Barriers and facilitators at the stage of ability to seek
The ability to seek is a vital aspect of accessing appropriate care, reflecting patients’ capacity to identify, evaluate, and navigate available healthcare services. In this study, aHUS patients demonstrated this ability through their efforts to identify and choose suitable healthcare providers and make informed decisions about their treatment plans. During this stage of the patient journey, barriers such as educational limitations and language differences disrupted their ability to seek healthcare effectively. Conversely, patient autonomy emerged as a key facilitator, empowering aHUS patients to actively navigate the healthcare system and make treatment decisions aligned with their needs.
Educational level and language barriers
Educational and language barriers were significant obstacles to patients’ ability to seek care, with 12 mentions across both patients and specialists (Table 3). Participants with limited educational backgrounds faced challenges in understanding and navigating healthcare systems, making appointments, and accessing relevant health information. Additionally, language differences (e.g., dialect) further impeded communication, hindering their ability to fully engage with healthcare providers and services.
“I was young at that time, and my parents were uneducated, and I was sure that whatever was said was what it was, and I wouldn’t look for anything else.” (P4)
“Patients from other regions, especially those with lower educational levels, often do not return for follow-up visits. It is highly likely that they will only visit a local hospital for a few consultations instead.” (S2)
Patient autonomy
Patient autonomy emerged as the most frequently mentioned facilitator at the “seek” stage of the patient journey (22 mentions in Table 3), empowering patients to navigate the healthcare system and pursue specialized care. Participants reported having great autonomy in selecting hospitals, often bypassing primary healthcare institutions in favor of directly accessing secondary or tertiary care facilities that offered more advanced services:
“We took a look at the hospital environment in the provincial capital city, and we were not familiar with the specialist there. The serious patients made us feel uncomfortable. So, we thought if it was possible to go to Beijing.” (P9)
Beyond selecting hospitals, autonomy extended to treatment decisions. Patients demonstrated a proactive approach to their care, such as combining traditional Chinese medicine with Western treatments, or seeking access to therapies unavailable in their immediate region. For instance, participants described exploring alternative therapies when standard treatments were insufficient or unavailable. Field notes supported this finding by revealing that patients often conveyed confidence and determination when discussing their proactive decision-making processes:
“During the process of immunotherapy, I contracted an infectious disease. Coupled with my weakened physical condition at that time, I decided to seek traditional Chinese medicine.” (P5)
“The specialist told us to do plasmapheresis first, and I heard that this drug would soon be available in China, and then we would stop plasmapheresis as soon as the drug came, and input the eculizumab.” (P6)
Physicians also played a key role in supporting patients’ autonomy, particularly in tertiary care settings, where individuals often traveled long distances to access specialized services. Recognizing the unique needs of aHUS patients, physicians facilitated autonomy by accommodating patient preferences in treatment planning and enabling access to unavailable therapies. For example, when complement inhibitor therapies like eculizumab were not yet covered in China, physicians collaborated with patients to administer self-provided medications sourced from abroad:
“Eculizumab was not available in China at that time, but if patients purchased the medication themselves from Hong Kong or abroad, we could also administer it to them. The hospital arranges patient self-provided medications based on different circumstances.” (S8)
Barriers and facilitators at the stage of ability to reach
The ability to reach healthcare services is a crucial aspect of healthcare access, reflecting patients’ ability to overcome logistical and physical barriers to obtain timely and specialized care. In this study, the ability to reach refers to how aHUS patients physically access healthcare facilities, navigate the healthcare system, and leverage available resources to address challenges. At this stage, the underdeveloped referral system emerged as a key barrier, creating inefficiencies and placing a heavy burden on patients and their families to navigate the healthcare system independently. However, facilitators such as family and societal support, telemedicine, green channels, robust public transportation, and social capital helped alleviate these challenges and improve patients’ access to healthcare services.
Underdeveloped referral systems
Both patients and specialists emphasized the absence of formal referral channels as a major barrier to accessing appropriate care (8 mentions in Table 3). This systematic gap often necessitated reliance on personal connections within the medical community to facilitate referrals to specialized hospitals or specialists. Some patients described how these informal networks played a crucial role in navigating the fragmented healthcare system and accessing specialized care they otherwise might not have been able to reach:
“The specialist told us that he had a good relationship with a specialist from another large hospital who was skilled in treating aHUS, so we went there.” (P9)
Field notes captured specialists’ expressions of frustration and resignation when discussing the lack of a standardized referral process, as they described the necessity of relying on informal networks to help their patients:
“There are no specific referral hospitals, as our patients come from all over the country. Sometimes, I refer patients to the hospital where my familiar senior colleague works for further tests and diagnosis.” (S8)
Family and societal support
Family members played a critical role in supporting patients with limited mobility during the onset of aHUS, with 14 mentions (Table 3). They provided transportation, facilitated hospital visits, and offered emotional support, particularly for pediatric patients. Field notes documented patients’ reliance on their caregivers, often expressed in emotional tones that conveyed a deep sense of gratitude for the support provided by their family members:
“I was so weak that I was panting when I walked 50 meters. My parents had to go with me to the specialist, and my dad would drive.” (P5)
Beyond familial support, societal interventions also contributed to mitigating mobility restrictions. For instance, local government authorities provided special travel assistance during emergencies, such as offering travel permissions during the COVID-19 pandemic:
“At that time, the COVID-19 epidemic was particularly serious, so we called 12345, a convenient service hotline, to ask the government of the situation.” (P1)
Telemedicine and online consultation
Telemedicine emerged as the most frequently mentioned facilitator at this stage, cited 31 times (Table 3). It reduced the need for physical travel by enabling remote consultations with specialists in large cities like Beijing and Shanghai. Patients and caregivers emphasized its transformative role in mitigating geographic disparities and empowering them to make informed healthcare decisions. Field notes indicated that participants often expressed a sense of hope and anticipation when discussing telemedicine, though their tones also conveyed hints of hesitation and nervousness about relying on this new mode of accessing care:
“My child is too young, and the illness is severe, so it’s not practical to go to Beijing. I was registering at an online hospital and called two specialists in Beijing to inquire about their treatment plans.” (P6)
Green channels in hospitals
Green channels, special fast-track service pathways within hospitals, provided by tertiary hospitals emerged as an additional facilitator, highlighted by both patients and specialists (4 mentions in Table 3). These channels streamlined access for aHUS patients with urgent or complex medical needs by offering priority registration, expedited appointments, and direct staff assistance. Such services greatly reduced waiting times, though their availability remains limited for certain therapies, such as eculizumab, which requires in-hospital administration.
“The specialist let us register for hospitalization directly from the A&E without waiting in the outpatient queue.” (P9)
“He just called the guy who worked on the service package. The clerk set up an appointment for him. It’s like a green channel.” (S8)
Robust public transportation
China’s high-speed rail network emerged as a critical facilitator, with 17 mentions (Table 3). This infrastructure greatly reduced travel time for patients traveling from rural or remote areas to access specialized care in major cities. Field notes captured participants’ satisfaction and sense of convenience when discussing the use of high-speed railways:
“We took a high-speed train from Inner Mongolia to Beijing instead of an ambulance and saved 4 h.” (P7)
Social capital
In the absence of formal referral systems, social capital became an important facilitator for some patients, which was mentioned 11 times (Table 3). Patients frequently relied on personal or professional networks to navigate the healthcare system, secure hospital transfers, and bypass long waiting times. Field notes also documented that some participants expressed determination when describing how they leveraged their networks to overcome systemic barriers:
“The specialist told us that there was a waiting list to transfer from the ICU to the nephrology department due to limited bed availability. We tried various methods and sought help from people who could assist, and finally managed to get transferred.” (P1)
“With the help of the nurse, we skipped the queue and entered the consulting room.” (P8)
Barriers and facilitators at the stage of ability to pay
The ability to pay is a critical determinant of healthcare access, encompassing both direct medical costs, such as consultation fees and medication expenses, and non-medical costs, including travel expenses and lost income. In this study, the ability to pay reflects the financial challenges faced by aHUS patients and the resources they leveraged to address these challenges. At this stage, inadequate insurance coverage and substantial non-medical costs emerged as key barriers, placing heavy financial burden on aHUS patients and their families. However, financial support mechanisms, including charitable donations, government subsidies, and community-driven fundraising efforts, helped alleviate these challenges and reduce the overall burden.
Inadequate insurance coverage
The inadequate basic medical insurance coverage emerged as the most frequently mentioned barrier at this stage. From the frequency analysis, this barrier appeared 32 times across both patients and specialists (Table 3). Nearly all participants noted that, during the study period, eculizumab was excluded from the National Medical Insurance Catalogue, requiring patients to bear the full cost of this life-saving but highly expensive medication.
“The biggest hope of our whole family and all the patients is that eculizumab can be covered by the basic medical insurance.” (P3)
Furthermore, patients also addressed that the exclusion of other necessary treatments, such as plasma exchange and complement tests, further compounded their financial strain. Field notes revealed that participants often displayed visible frustration and used emphatic language, such as “I felt a lot of financial pressure” (P1) and “all at our own expense” (P8), when discussing out-of-pocket expenses.
“We did plasmapheresis in the ICU, and had a lot of biologic infusions. These were all self-funded and not reimbursed at all, so I felt a lot of financial pressure.” (P1)
“My child’s various complement tests and H-factor tests were all at our own expense.” (P8)
Specialists also emphasized this challenge, with one noting hesitancy to recommend certain treatments, such as eculizumab due to patients’ financial constraints.
“Most drugs except eculizumab are covered by medical insurance…we would not prescribe medications that is not covered by insurance…” (S5)
Substantial non-medical burdens
Substantial non-medical expenses, such as transportation, accommodations, and income loss, were reported by participants as a major barrier to accessing healthcare, with 22 mentions in Table 3. Field notes captured expressions of exhaustion and frustration as participants recounted these struggles. Many patients or caregivers had to take extended leave or resign from their jobs to focus on care, resulting in great income loss and emotional strain. These sacrifices often created a cycle of economic instability that intensified the overall burden:
“There’s nothing we can do for so long. Because no job can or will allow you to ask for a leave so often.” (P9)
Families who relocated temporarily to access specialized care experienced additional pressures, while others were forced to reduce the frequency of medical visits due to the high costs of travel and the impact on their incomes:
“My mother and I rented a small house in Beijing to see a specialist, and only my father worked to make money.” (P5)
“We have reduced the number of visits to Beijing for medical treatment. One reason is that the cost of transportation is too expensive, and another reason is that taking leave will result in a deduction from my salary.” (P1)
Multifaceted financing sources
Various forms of financial support provided critical relief to some patients and their families, partially alleviating the financial burden associated with aHUS treatment, with 19 mentions in Table 3. These sources included charitable donations, government subsidies, and community-driven initiatives. Field notes captured participants’ mixed emotions - relief when describing successful financial assistance but also anxiety about the sustainability and accessibility of these support systems. Charitable donation programs, often administered by hospitals or foundations, were instrumental in reducing the costs of therapies such as eculizumab by offering discounted or subsidized access:
“There is currently an eculizumab donating project, which is supported by the foundation. After confirmation from the hospital, designated pharmacies, and patients, we could purchase at a discounted price.” (P5)
“When our second child also contracted the disease, at the hospital where we sought treatment, the specialist arranged for a donation within the hospital.” (P6)
Government assistance programs, including subsistence allowances and subsidies for children with severe illnesses, further provided economic relief for some families:
“Several cities in Shandong Province have implemented inclusive health insurance policies that include eculizumab as a reimbursable specialty drug under their coverage.” (P1)
Community-driven initiatives, such as online crowdfunding platforms, further supported families by raising funds from both personal and public networks:
“We previously used the Water Drop Fundraising platform, where we received donations from both strangers and friends, which helped alleviate some of the financial pressure.” (P3)
However, these support systems were not universally accessible. Eligibility criteria, institutional variations, and geographic disparities limited the reach of these programs. Field notes highlighted participants’ apprehension and uncertainty when discussing financial assistance, with some expressing concern about whether they would continue to qualify for these programs in the future.
Barriers and facilitators at the stage of ability to engage
The ability to engage represents the final and critical stage of healthcare accessibility, where patients actively participate in and benefit from healthcare services. In this study, the ability to engage encompasses patients’ adherence to treatment plans, lifestyle adjustments, and long-term management of their health conditions. At this stage, barriers such as gaps in professional knowledge, suboptimal diagnostic techniques, the absence of dedicated patient organizations, and limited reliance on healthcare professionals complicated patients’ ability to fully engage in their care. These challenges underscored the need for enhanced diagnostic tools, stronger support systems, and more collaborative interactions with healthcare providers. Conversely, facilitators such as proactive adherence to treatment and emotional support from healthcare professionals empowered patients to maintain active engagement in their care, contributing to improved disease management and better health outcomes.
Gaps in professional knowledge and the use of suboptimal diagnostic techniques
Gaps in professional knowledge and suboptimal diagnostic techniques were frequently mentioned as barriers by both patients and specialists (37 mentions in Table 3). Patients reported that limited expertise among healthcare providers impeded their ability to fully engage in their care. Many expressed frustrations over inadequate communication with specialists, who often failed to provide sufficient explanations about their condition and treatment options. Field notes further captured non-verbal cues that underscored patients’ emotional responses, such as visible hesitation, long pauses, or softer tones when recounting their diagnostic journeys or describing unhelpful interactions with healthcare providers.
“We can’t communicate much with the specialists in the hospital, they don’t explain everything to us like we are students.” (P2)
Some patients also described taking initiative to seek advice from specialists in larger hospitals when local healthcare providers lacked experience with aHUS.
“Our local hospital has never used it, all specialists didn’t use it. I contacted hospitals in Beijing to give advice to specialists here.” (P1)
Specialists highlighted additional barriers, including a lack of advanced diagnostic tools and the absence of standardized diagnostic protocols for aHUS. Field notes captured moments of visible frustration and resignation among specialists, reflecting the challenges they faced in navigating these limitations. Some expressed concerns about the impact of inadequate resources on diagnostic accuracy and patient care.
“We lack diagnostic test kits for confirmation, so we have to construct them ourselves. It is difficult for us to achieve standardization, and may not be comparable with foreign countries.” (S6)
Professionals also emphasized the need for multidisciplinary team services and proposed establishing a nationwide consultation system to improve care coordination for rare diseases like aHUS.
“There are very few patients with aHUS in China, so setting up a nationwide consultation system for special cases shouldn’t be too much trouble.” (S7)
Absence of dedicated patient organizations
Participants consistently emphasized the absence of patient organizations as a barrier to effective engagement (7 mentions in Table 3). Such organizations could provide patients and caregivers with opportunities to connect, share experiences, and access peer support. Patients noted that the lack of a formal community or professional advocacy group hindered their ability to exchange valuable insights and access critical resources that could aid in managing their conditions. This absence was particularly striking when compared with other rare diseases with well-established patient networks. Field notes captured feelings of isolation and helplessness among participants when discussing the lack of a supportive community, with some pausing or lowering their tone while expressing a desire for a shared platform:
“We currently do not have a large patient organization. When I was researching related information, I found that rare diseases like PNH have professional public accounts to organize patients, but aHUS do not.” (P5)
Limited reliance on healthcare professionals
In some cases, elderly patients relied on caregivers to make treatment adjustments, such as altering medication dosages. While this reliance provided practical support, it occasionally led to deviations from prescribed treatment plans and inconsistent adherence, posing challenges to maintaining engagement (8 mentions in Table 3).
“My mother’s blood pressure has dropped slightly, so I told her to reduce the dosage of medication and skip some unnecessary ones… She has followed my instructions on how to take them.” (P1)
Proactive adherence to treatment
Despite the challenges, most participants displayed proactive engagement by adhering to prescribed treatment regimens and attending scheduled medical appointments (12 mentions in Table 3). Many caregivers also played an active role in ensuring adherence by setting reminders and monitoring medication use. Field notes supported this finding by highlighting participants’ sense of determination and responsibility when discussing their efforts to manage their condition:
“We had to take a lot of medication every day and I would set alarms to remind my kids to take their medication. The specialist said never stop on your own, the consequences can be serious.” (P5)
From the perspective of health professionals, consistent efforts have been made to improve patient adherence and engagement by fostering interdisciplinary collaboration and providing comprehensive care tailored to the unique needs of rare disease patients. One specialist highlighted their hospital’s proactive approach in promoting awareness of aHUS and ensuring seamless coordination across departments to deliver holistic care:
“We have been consciously strengthening interdisciplinary collaboration in recent years, including training and group learning across various departments within the hospital. The interdisciplinary consultation channel enables us to provide integrated and comprehensive care for rare disease patients like aHUS.” (S9)
Discussion
This study conceptualizes healthcare access as a multi-stage process shaped by structural conditions. Drawing on the Levesque framework, we examined five interrelated dimensions (i.e., perceived need, seeking care, reaching services, paying for treatment, and care engagement) to trace how aHUS patients navigate the healthcare system. Based on interviews with patients and healthcare professionals, we argue that these “abilities” are not merely exercised at the individual level, but are shaped by deeper structural conditions embedded in socio-political and economic systems.
At the “ability to perceive” stage, both patients and healthcare providers demonstrated limited awareness of aHUS, a pattern consistently reflected in interviews and supported by existing researchs(Isono, Kokado, & Kato, 2022; Vandeborne, van Overbeeke, Dooms, De Beleyr, & Huys, 2019). While knowledge gaps are commonly cited as drivers of diagnostic delay, our findings situate this deficit within broader structural dynamics. For providers, the near-invisibility of rare diseases in medical training and practice reflects not simply a lack of education, but what Farmer terms “structural violence”: the marginalization of low-prevalence conditions through institutional logics that prioritize population-level efficiency and cost containment(Farmer, Nizeye, Stulac, & Keshavjee, 2006; Li et al., 2021; Wong et al., 2015). As a result, rare diseases are consistently sidelined in medical curricula, clinical protocols, and health policy. Similarly, patients’ limited awareness of diagnostic and treatment options reflects more than a lack of individual knowledge. It stems from a broader s, driven by the concentration of expertise in urban ystemic exclusiontertiary hospitals and the insufficient integration of rare disease detection into primary care(Z. Zhang, 2024). Though reforms have aimed to strengthen primary care, it remains disconnected from rare disease referral systems(Zhao, Wang, Chen, & Zhou, 2025). In response, civil society actors (e.g., families, patient organizations, and online networks) often attempt to compensate for institutional absences(Vandeborne et al., 2019; S. Zhang, Chen, Zhang, & Zhao, 2019; Zhou, Xu, & Yang, 2022). Families, in particular, play pivotal roles in symptom recognition and care coordination, yet their efforts are reactive and individualized, signaling not empowerment but the outsourcing of state responsibility(S. Zhang et al., 2019). Addressing these entrenched disparities requires more than awareness campaigns. It calls for structural reforms, including integrating rare diseases into medical education, decentralizing diagnostic capacity, and institutionalizing access equity through sustained public investment and policy coordination(Vandeborne et al., 2019).
At the “ability to seek” stage, many aHUS patients demonstrated initiative in navigating the healthcare system and managing their care. While this appears as a form of autonomy, our findings suggest it often reflects a response to institutional gaps rather than true empowerment(Baumbusch, Mayer, & Sloan-Yip, 2018; Khan et al., 2018). Factors such as education, income, and access to information can help patients make informed choices, but these advantages are unevenly distributed(Entwistle, Carter, Cribb, & McCaffery, 2010; Feldman, 2010; Tully et al., 2022). Those with lower levels of formal education or who speak non-dominant dialects often face added difficulties, including poor communication and lack of guidance, which compound their vulnerability(Borras, 2021; Chelak & Chakole, 2023; Lor & Martinez, 2020). In such cases, autonomy becomes less a right than a responsibility, placing the burden of system navigation on individuals who are least equipped to manage it. Without supportive infrastructure, accessible health education, and inclusive service design, patient-centered care risks reinforcing inequality under the guise of choice(Agarwal & Murinson, 2012; Karamched et al., 2018; Quintal et al., 2023).
At the “ability to reach” stage, digital tools such as telemedicine and online consultation have emerged as important facilitators, offering new avenues for accessing specialized care and reducing geographic barriers(Bergier et al., 2021; Brizola et al., 2020; Severin & Dan, 2022). However, the transformative potential of these tools is often constrained by structural limitations. In many under-resourced regions, poor internet infrastructure, low levels of digital literacy, and the lack of reliable, disease-specific information limit the accessibility and effectiveness of these innovations(Chung, Ng, Jain, & Chung, 2021; X. Dong & Wang, 2024; Kruse et al., 2019; Lin et al., 2020). More fundamentally, China’s fragmented referral system remains a persistent obstacle. Despite policy support for a tiered care model, coordination between hospital levels is often weak, with unclear pathways leading to delays, duplication, and discontinuity in care(Gao, Yang, Wang, Zhang, & Lu, 2024; Lei et al., 2025). These challenges are further exacerbated by market-driven dynamics that prioritize institutional competition over collaborative care, undermining system-level integration(Jakovljevic et al., 2023). In this context, patients frequently rely on informal pathways (e.g., personal networks, social connections, or digital communities) to navigate the system. While these resources can sometimes fill institutional gaps, their effectiveness depends on unequal distributions of social capital, thereby reinforcing rather than resolving access disparities(Rodriguez-Alcalá, Qin, & Jeanetta, 2019; S. Zhang, Wu, Ma, Cheng, & Li, 2021). Although digital platforms hold promise, they cannot substitute for well-integrated care systems. Realizing their full benefit requires investment in coordinated referral pathways, equitable technological access, and support mechanisms that extend beyond digital tools. Programs like “Internet Plus” and rare disease centers are a step forward, but without structural reforms, digital solutions risk amplifying existing inequities rather than overcoming them(Paccoud, Leist, Schwaninger, van Kessel, & Klucken, 2024).
At the “ability to pay” stage, financial barriers were among the most consistently reported obstacles. Beyond affordability concerns, our findings highlight how inadequate insurance coverage functions as a structural mechanism that reproduces health inequities. As of 2023, basic insurance reimbursed roughly 63% of rare disease treatment costs, with lower rates at tertiary hospitals exacerbating burdens for aHUS patients(Kong et al., 2015; Min, Zhang, Fang, Wang, & Wang, 2019; J. Xu, Yu, Zhang, Gong, & Li, 2023). Although eculizumab was added to the National Reimbursement Drug List (NRDL) in 2024, early evidence points to continued disparities: reimbursement rates differ by region and insurance type, with patient payments ranging from several hundred yuan per dose to over ¥50,000 annually. These variations reflect deeper systemic imbalances, as China’s decentralized health financing model ties coverage generosity to local fiscal capacity, deepening regional inequities(Chen, Chen, Deng, & Ding, 2024; J. Xu et al., 2023). These pressures are further compounded by indirect costs (e.g., travel, accommodation, and wage loss) that fall outside formal reimbursement frameworks(Czech et al., 2019; Stoller, 2018). As research shows, non-medical expenses can constitute over half the economic burden of rare diseases, yet they remain largely invisible in policy design(Marshall et al., 2023). For aHUS patients in China, these unaccounted burdens translate into social exclusion, where treatment adherence depends as much on income and location as on medical access. To address these gaps, international experience offers instructive models. Singapore reduces household burden through mixed financing via the Rare Disease Fund and national insurance schemes. The European Reference Networks (ERNs) coordinate cross-border care through standardized clinical pathways(Gentilini, Neez, & Wong-Rieger, 2025). U.S. pharmaceutical assistance programs like OneSource™ and Prescription Hope support underinsured patients, while South Korea uses risk-sharing agreements to make therapies like eculizumab conditionally reimbursable(Lee et al., 2021). These models vary in design but share a recognition that equitable access requires dedicated institutional mechanisms, not just expanded insurance coverage. For China, this underscores the need for multi-level reform. Expanding rare disease funds beyond wealthy provinces, integrating regional pilots into a national financing platform, and building clinical networks modeled on ERNs could collectively enhance access and reduce geographic disparities. Such efforts must not only broaden coverage but also confront the structural conditions that marginalize patients with low-prevalence conditions.
At the “ability to engage” stage, meaningful patient participation depends not only on individual initiative, but also on institutional structures that support clinical trust, shared decision-making, and informational transparency. For aHUS patients in China, this ability is influenced by limited professional awareness, fragmented diagnostic capacity, and the absence of coordinated care pathways. These factors reflect broader structural issues, including the low policy prioritization of rare diseases, the absence of incentives for clinical specialization, and insufficient investment in diagnostic technologies such as complement testing and genetic sequencing(Jokiranta et al., 2017; Lee et al., 2021; Yang et al., 2022). Such constraints narrow the scope for active engagement, often relegating patients to passive roles in the care process. To address these issues, many health systems have introduced structural mechanisms that embed patient participation into rare disease care. For instance, multidisciplinary consultation models in Europe and North America facilitate integrated clinical decision-making(Avila, Cao, Espinosa, Manrique, & Morales, 2023; Schuermans et al., 2022), while standardized treatment guidelines and patient organizations help reduce informational asymmetries and build trust(Wada et al., 2020; S. Zhang et al., 2019). Furthermore, patient registries in the EU and U.S. enable personalized care and long-term monitoring through data-driven coordination(Dawkins et al., 2018). Although China has initiated registries for select rare conditions (e.g., hemophilia), a dedicated aHUS registry is lacking, limiting continuity of care and research potential(Gong & He, 2021). The absence of such infrastructure, along with weak referral systems and limited institutional support for patient groups, leaves many patients navigating complex care trajectories alone. This fragmentation reflects deeper institutional neglect, where rare diseases remain a low priority in national health policy. Addressing this gap requires structural investment. Expanding professional training on aHUS(Schuermans et al., 2022; S. Zhang et al., 2019), ensuring equitable access to diagnostic tools(Gong & He, 2021), enforcing national clinical guidelines(S. Zhang et al., 2019), and supporting patient-led advocacy(Merkel et al., 2016; Wada et al., 2020) are essential to promote informed and participatory care. A national aHUS registry would help institutionalize patient engagement, easing the burden on individuals and enabling more coordinated, system-level support for rare disease care(Licht et al., 2015).
Although this study focuses on the healthcare experiences and healthcare accessibility of aHUS patients, the emotional and ethical challenges faced by rare disease families should not be overlooked. Our findings reveal that families accompany patients throughout the entire care journey, often bearing intense emotional labor and moral distress(Atkins & Padgett, 2024) as they navigate life-threatening crises, diagnostic uncertainty, and overwhelming financial burdens. In the Chinese context, where filial piety and parental sacrifice(Leung, 2020) are deeply embedded cultural values, caregiving for rare disease patients often falls heavily on close family members, especially adult children, parents or spouses(R. H. Xu, Ng, Luo, Dong, & Zhang, 2023), who must balance medical decision-making with emotional support and economic sacrifice. Additionally, gaps in communication and continuity of care across institutions, stark urban-rural disparities and inconsistent regional policies also erode medical trust(Wang et al., 2018). Recognizing and addressing these deep-seated humanistic concerns is essential for achieving truly patient- and family-centered rare disease care in China.
Implications and limitations
This study offers important insights into the multifaceted challenges faced by patients with aHUS in navigating China’s healthcare system. Using the Levesque framework, we examined healthcare access as shaped by patient abilities, drawing on the perspectives of both patients and healthcare providers. The findings carry several key implications: (1) enhancing public and professional awareness of aHUS is crucial to combat systemic invisibility and should be supported through mass media campaigns and targeted education for healthcare professionals; (2)optimizing insurance policies and diversifying funding sources, including charitable contributions, are crucial steps to alleviate the financial burden and address broader equity issues on rare patients; (3) developing specialized treatment centers, multidisciplinary care teams, and streamlined referral pathways is critical to improving both the quality and timeliness of care, particularly in low- and middle-income contexts; (4) expanding telemedicine services and strengthening patient organizations can improve access, peer support, and continuity of care.
Besides, this study has several limitations. One limitation is the small sample size, which may restrict the generalizability of the findings. Although patients were recruited from multiple centers nationwide, the referral through rare disease organizations and hospitals may introduce selection bias. Furthermore, despite employing timeline methods to minimize recall bias during interviews with patients and caregivers, some recall bias may still be present. In addition, the selection of healthcare providers primarily from high-level hospitals may have limited the inclusions of perspectives from primary healthcare providers. Future studies should aim to include a more diverse range of institutions to enhance the applicability of the findings. Conducting a quantitative study on a larger sample of aHUS population could further examine the interrelationships among identified facilitators and barriers.
Conclusion
This study identifies key facilitators and barriers to healthcare access for aHUS patients across different stages of their care journey, using Levesque’s framework. By integrating patient and specialist perspectives, along with composite narratives that humanize the emotional and existential burden, we go beyond descriptive analysis to expose deeper structural challenges, including raising awareness of aHUS, supporting patient autonomy, expanding telemedicine, improving insurance coverage, and strengthening clinical training and diagnostic protocols. The findings also highlight the emotional and ethical burdens on families, shaped by cultural norms and systemic gaps. Addressing these challenges is critical to advancing more equitable and person-centered rare disease care. Future research should assess the implementation and impact of these strategies to inform rare disease policy in China and beyond.
Data availability
All relevant qualitative data supporting the findings of this study are included within the article and the interview outlines are available in the supplementary files. The data underpinning this study consist of qualitative interview transcripts from a small and context-specific participants. Owing to the risk of participant re-identification and in accordance with our ethics approval and informed consent procedures, the raw data are not publicly available. Limited de-identified excerpts may be shared upon reasonable request to the corresponding author, contingent upon a data use agreement and, where applicable, institutional ethics approval.
References
Agarwal AK, Murinson BB (2012) New dimensions in patient-physician interaction: values, autonomy, and medical information in the patient-centered clinical encounter. Rambam Maimonides Med J 3(3):e0017. https://doi.org/10.5041/rmmj.10085
Assembly WMAG (2013) World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. Jama 310(20):2191–2194. https://doi.org/10.1001/jama.2013.281053
Atkins JC, Padgett CR (2024) Living with a rare disease: psychosocial impacts for parents and family members—a systematic review. J Child Family Stud 33(2):617–636. https://doi.org/10.1007/s10826-024-02790-6
Avila A, Cao MRD, Espinosa M, Manrique J, Morales E (2023) Recommendations for the individualised management of atypical hemolytic uremic syndrome in adults. Front Med 10:1264310. https://doi.org/10.3389/fmed.2023.1264310
Baumbusch J, Mayer S, Sloan-Yip I (2018) Alone in a crowd? parents of children with rare diseases’ experiences of navigating the healthcare system. J Genet Couns https://doi.org/10.1007/s10897-018-0294-9
Bergier H, Duron L, Sordet C, Kawka L, Schlencker A, Chasset F, Arnaud L (2021) Digital health, big data and smart technologies for the care of patients with systemic autoimmune diseases: Where do we stand?. Autoimmunity Rev 20(8):102864. https://doi.org/10.1016/j.autrev.2021.102864
Bletzer KV (2015) Visualizing the qualitative: making sense of written comments from an evaluative satisfaction survey. J Educ Eval Health Prof 12:12. https://doi.org/10.3352/jeehp.2015.12.12
Borras AM (2021) Toward an intersectional approach to health justice. Int J Health Services 51(2):206–225. https://doi.org/10.1177/0020731420981857
Bremner N (2020) Time for timelines: the take-home timeline as a tool for exploring complex life histories. Int J Qualitative Methods https://doi.org/10.1177/1609406920948978
Brizola E, Adami G, Baroncelli GI, Bedeschi MF, Berardi P, Boero S, Sangiorgi L (2020) Providing high-quality care remotely to patients with rare bone diseases during COVID-19 pandemic. Orphanet J Rare Dis 15(1):228. https://doi.org/10.1186/s13023-020-01513-6
Chelak K, Chakole S (2023) The role of social determinants of health in promoting health equality: a narrative review. Cureus 15(1):e33425. https://doi.org/10.7759/cureus.33425
Chen Y, Chen X, Deng Y, Ding J (2024) Analysis of affordability differences for rare diseases in China: a comparison across disease types and regions. Int J Equity Health 23(1):64. https://doi.org/10.1186/s12939-024-02137-z
Chung CCY, Ng YNC, Jain R, Chung BHY (2021) A thematic study: impact of COVID-19 pandemic on rare disease organisations and patients across ten jurisdictions in the Asia Pacific region. Orphanet J Rare Dis 16(1):119. https://doi.org/10.1186/s13023-021-01766-9
Collaborators GHAaQ (2018) Measuring performance on the healthcare access and quality index for 195 countries and territories and selected subnational locations: a systematic analysis from the global burden of disease study 2016. Lancet 391(10136):2236–2271. https://doi.org/10.1016/s0140-6736(18)30994-2
Cu A, Meister S, Lefebvre B, Ridde V (2021) Assessing healthcare access using the Levesque’s conceptual framework- a scoping review. Int J Equity Health 20(1):116. https://doi.org/10.1186/s12939-021-01416-3
Czech M, Baran-Kooiker A, Atikeler K, Demirtshyan M, Gaitova K, Holownia-Voloskova M, Sykut-Cegielska J (2019) A review of rare disease policies and orphan drug reimbursement systems in 12 eurasian countries. Front Public Health 7:416. https://doi.org/10.3389/fpubh.2019.00416
Dawkins HJS, Draghia-Akli R, Lasko P, Lau LPL, Jonker AH, Cutillo CM, Austin CP (2018) Progress in rare diseases research 2010-2016: an IRDiRC perspective. Clin Transl Sci 11(1):11–20. https://doi.org/10.1111/cts.12501
Dong D, Wang Y (2016) Challenges of rare diseases in China. Lancet 387(10031):1906. https://doi.org/10.1016/s0140-6736(16)30418-4
Dong X, Wang Y (2024) The geography of healthcare: Mapping patient flow and medical resource allocation in China. Econ Hum Biol 55: 101431. https://doi.org/10.1016/j.ehb.2024.101431
Emilia S, Dorica D (2022) Lack of information on the effects of COVID-19 on rare pathologies has further hampered access to healthcare services. Front. Public Health 10:852–880. https://doi.org/10.3389/fpubh.2022.852880
Entwistle VA, Carter SM, Cribb A, McCaffery K (2010) Supporting patient autonomy: the importance of clinician-patient relationships. J Gen Intern Med 25(7):741–745. https://doi.org/10.1007/s11606-010-1292-2
Farmer PE, Nizeye B, Stulac S, Keshavjee S (2006) Structural violence and clinical medicine. PLoS Med 3(10):e449. https://doi.org/10.1371/journal.pmed.0030449
Feldman MD (2010) From the editors’ desk: patient autonomy and medical decisions: getting it just right. J Gen Intern Med 25(7):639. https://doi.org/10.1007/s11606-010-1391-0
Formeck C, Swiatecka-Urban A (2019) Extra-renal manifestations of atypical hemolytic uremic syndrome. Pediatr Nephrol 34(8):1337–1348. https://doi.org/10.1007/s00467-018-4039-7
Gao Y, Yang Y, Wang S, Zhang W, Lu J (2024) Has China’s hierarchical medical system improved doctor-patient relationships?. Health Econ Rev 14(1):54. https://doi.org/10.1186/s13561-024-00520-8
Gentilini A, Neez E, Wong-Rieger D (2025) Rare disease policy in high-income countries: an overview of achievements, challenges, and solutions. Value Health 28(5):680–685. https://doi.org/10.1016/j.jval.2024.12.009
Gong L, He Q (2021) Establishing a rare diseases center: experiences from Western China. Intractable Rare Dis Res 10(1):60–61. https://doi.org/10.5582/irdr.2020.03091
Henry J, Beruf C, Fischer T (2020) Access to health care for pregnant arabic-speaking refugee women and mothers in Germany. Qual Health Res 30(3):437–447. https://doi.org/10.1177/1049732319873620
Hurtubise K, Joslin R (2023) Participant-generated timelines: a participatory tool to explore young people with chronic pain and parents’ narratives of their healthcare experiences. Qual Health Res 33(11):931–944. https://doi.org/10.1177/10497323231189388
Isono M, Kokado M, Kato K (2022) Why does it take so long for rare disease patients to get an accurate diagnosis?-a qualitative investigation of patient experiences of hereditary angioedema. PLoS ONE 17(3):e0265847. https://doi.org/10.1371/journal.pone.0265847
Jakovljevic M, Chang H, Pan J, Guo C, Hui J, Hu H, Shi L (2023) Successes and challenges of China’s health care reform: a four-decade perspective spanning 1985-2023. Cost Eff Resour Alloc 21(1):59. https://doi.org/10.1186/s12962-023-00461-9
Johnson TP (2014) Snowball Sampling: Introduction. In: Balakrishnan N, Colton T, Everitt B, Piegorsch W, Ruggeri F & Teugels LJ eds. Wiley statsRef: statistics reference online. John Wiley & Sons
Jokiranta TS, Viklicky O, Al Shorafa S, Coppo R, Gasteyger C, Macia M, Haller H (2017) Differential diagnosis of thrombotic microangiopathy in nephrology. Bmc Nephrol 18: 324. https://doi.org/10.1186/s12882-017-0727-y
Karamched KR, Hao W, Song PX, Carpenter L, Steinberg J, Baptist AP (2018) The impact of patient autonomy on older adults with asthma. Ann Allergy Asthma Immunol 121(1):65–68.e61. https://doi.org/10.1016/j.anai.2018.04.024
Khan S, Vandermorris A, Shepherd J, Begun JW, Lanham HJ, Uhl-Bien M, Berta W (2018) Embracing uncertainty, managing complexity: applying complexity thinking principles to transformation efforts in healthcare systems. BMC Health Serv Res 18(1):192. https://doi.org/10.1186/s12913-018-2994-0
Kong X, Yang Y, Gao J, Guan J, Liu Y, Wang R, Ma W (2015) Overview of the health care system in Hong Kong and its referential significance to mainland China. J Chinese Med Assoc 78(10):569–573. https://doi.org/10.1016/j.jcma.2015.02.006
Kourgiantakis T, Markoulakis R, Lee EJ, Hussain A, Lau C, Ashcroft R, Levitt A, egovia N (2023) Access to mental health and addiction services for youth and their families in Ontario: perspectives of parents, youth, and service providers. Int J Mental Health Syst 17(1):e13263. https://doi.org/10.1186/s13033-023-00572-z
Kruse C, Betancourt J, Ortiz S, Valdes Luna SM, Bamrah IK, Segovia N (2019) Barriers to the Use of Mobile Health in Improving Health Outcomes in Developing Countries: Systematic Review. J Med Internet Res 21(10):e13263. 10.2196/13263
Lee B, Bae E-Y, Bae S, Choi H-J, Son K-B, Lee Y-S, Lee T-J (2021) How can we improve patients’ access to new drugs under uncertainties? : South Korea’s experience with risk sharing arrangements. BMC Health Serv Res 21(1):967. https://doi.org/10.1186/s12913-021-06919-x
Legendre CM, Licht C, Muus P, Greenbaum LA, Babu S, Bedrosian C, Loirat C (2013) Terminal complement inhibitor eculizumab in atypical hemolytic-uremic syndrome. N Engl J Med 368(23):2169–2181. https://doi.org/10.1056/NEJMoa1208981
Lei C, Zuo Y, Kong F, Chen H, Cheng H, Song X, Zhou H (2025) Reshaping the hierarchical medical system for rare diseases: a two-tier structure and one-stop referral network. J Glob Health 15: 03005. https://doi.org/10.7189/jogh.15.03005
Leung JTY (2020) Perceived parental sacrifice, filial piety and hopelessness among Chinese adolescents: a cross-lagged panel study. J Adolesc 81:39–51. https://doi.org/10.1016/j.adolescence.2020.04.005
Levesque JF, Harris MF, Russell G (2013) Patient-centred access to health care: conceptualising access at the interface of health systems and populations. Int J Equity Health 12: 18. https://doi.org/10.1186/1475-9276-12-18
Li X, Zhang X, Zhang S, Lu Z, Zhang J, Zhou J, Ou L (2021) Rare disease awareness and perspectives of physicians in China: a questionnaire-based study. Orphanet J Rare Dis 16(1):171. https://doi.org/10.1186/s13023-021-01788-3
Licht C, Ardissino G, Ariceta G, Cohen D, Cole JA, Gasteyger C, Frémeaux-Bacchi V (2015) The global aHUS registry: methodology and initial patient characteristics. BMC Nephrol 16:207. https://doi.org/10.1186/s12882-015-0195-1
Lin J, Gong N, Cao Q, Zhou Y, Cai Y, Jin G, Zheng D (2020) What hinders congenital ectopia lentis patients’ follow-up visits? a qualitative study. BMJ Open 10(3):e030434. https://doi.org/10.1136/bmjopen-2019-030434
Lor M, Martinez GA (2020) Scoping review: definitions and outcomes of patient-provider language concordance in healthcare. Patient Educ Couns 103(10):1883–1901. https://doi.org/10.1016/j.pec.2020.05.025
Marshall DA, Gerber B, Lorenzetti DL, MacDonald KV, Bohach RJ, Currie GR (2023) Are we capturing the socioeconomic burden of rare genetic disease? A scoping review of economic evaluations and cost-of-illness studies. Pharmacoeconomics 41(12):1563–1588. https://doi.org/10.1007/s40273-023-01308-0
Maurya A, Dixit G, George A, Karki RG, Aasaithambi S, Verma H, Doherty JP (2022) Mining socialmedia to understand unmet need and treatment experience in patients with atypical hemolytic uremic syndrome (AHUS). Value in Health 25(1):S229–S229
Merkel PA, Manion M, Gopal-Srivastava R, Groft S, Jinnah HA, Robertson D, Krischer JP (2016) The partnership of patient advocacy groups and clinical investigators in the rare diseases clinical research network. Orphanet J Rare Dis 11(1):66. https://doi.org/10.1186/s13023-016-0445-8
Min R, Zhang XY, Fang PQ, Wang BY, Wang H (2019) Health service security of patients with 8 certain rare diseases: evidence from China’s national system for health service utilization of patients with healthcare insurance. Orphanet J Rare Dis 14(1):204. https://doi.org/10.1186/s13023-019-1165-7
Nga HS, Palma LMP, Neto ME, de Andrade LGM (2022) Eculizumab in low-middle income countries: how much does a life cost. J Nephrol 35(4):1255–1257. https://doi.org/10.1007/s40620-022-01282-4
Noris M, Remuzzi G (2009) Atypical hemolytic-uremic syndrome. N Engl J Med 361(17):1676–1687. https://doi.org/10.1056/NEJMra0902814
O’Brien BC, Harris IB, Beckman TJ, Reed DA, Cook DA (2014) Standards for reporting qualitative research: a synthesis of recommendations. Acad Med 89(9):1245–1251. https://doi.org/10.1097/acm.0000000000000388
Paccoud I, Leist AK, Schwaninger I, van Kessel R, Klucken J (2024) Socio-ethical challenges and opportunities for advancing diversity, equity, and inclusion in digital medicine. Digit Health 10: 20552076241277705. https://doi.org/10.1177/20552076241277705
Pell B, Williams D, Phillips R, Sanders J, Edwards A, Choy E, Grant A (2020) Using visual timelines in telephone interviews: reflections and lessons learned from the star family study. Int J Qualitative Methods 19:1609406920913675. https://doi.org/10.1177/1609406920913675
Phillippi J, Lauderdale J (2018) A guide to field notes for qualitative research: context and conversation. Qual Health Res 28(3):381–388. https://doi.org/10.1177/1049732317697102
Quintal A, Carreau I, Grenier AD, Hébert C, Yergeau C, Berthiaume Y, Racine E (2023) An ethics action plan for rare disease care: participatory action research approach. J Particip Med 15:e46607. https://doi.org/10.2196/46607
Raina R, Grewal MK, Radhakrishnan Y, Tatineni V, DeCoy M, Burke LLG, Bagga A (2019) Optimal management of atypical hemolytic uremic disease: challenges and solutions. Int J Nephrol Renovasc Dis 12:183–204. https://doi.org/10.2147/ijnrd.S215370
Rodriguez-Alcalá ME, Qin H, Jeanetta S (2019) The role of acculturation and social capital in access to health care: a meta-study on hispanics in the US. J Community Health 44(6):1224–1252. https://doi.org/10.1007/s10900-019-00692-z
Rosales A, Riedl M, Zimmerhackl LB (2010) Thrombotic microangiopathy: atypical HUS: current diagnostic and therapeutic approaches. Nat Rev Nephrol 6(9):504–506. https://doi.org/10.1038/nrneph.2010.98
Schaefer F, Ardissino G, Ariceta G, Fakhouri F, Scully M, Isbel N, Frémeaux-Bacchi V (2018) Clinical and genetic predictors of atypical hemolytic uremic syndrome phenotype and outcome. Kidney Int 94(2):408–418. https://doi.org/10.1016/j.kint.2018.02.029
Schuermans N, Hemelsoet D, Terryn W, Steyaert S, Van Coster R, Coucke PJ, PrOZA UD (2022) Shortcutting the diagnostic odyssey: the multidisciplinary program for undiagnosed rare diseases in adults (UD-PrOZA. Orphanet J Rare Dis 17(1):13. https://doi.org/10.1186/s13023-022-02365-y
Schwarz T, Schmidt AE, Bobek J, Ladurner J (2022) Barriers to accessing health care for people with chronic conditions: a qualitative interview study. BMC Health Serv Res 22(1):852–880. 1037. https://doi.org/10.1186/s12913-022-08426-z
Spasiano A, Palazzetti D, Dimartino L, Bruno F, Baccaro R, Pesce F, Grandaliano G (2023) Underlying genetics of aHUS: which connection with outcome and treatment discontinuation?. Int J Mol Sci 24(19):14496. https://doi.org/10.3390/ijms241914496
Stoller JK (2018) The challenge of rare diseases. Chest 153(6):1309–1314. https://doi.org/10.1016/j.chest.2017.12.018
Tully KP, Gibson AN, Pearsall MS, Umstead K, Gill C, Stuebe AM (2022) Screening and referral for social determinants of health: maternity patient and health care team perspectives. Health Equity 6(1):887–897. https://doi.org/10.1089/heq.2022.0020
Vandeborne L, van Overbeeke E, Dooms M, De Beleyr B, Huys I (2019) Information needs of physicians regarding the diagnosis of rare diseases: a questionnaire-based study in Belgium. Orphanet J Rare Dis 14(1):99. https://doi.org/10.1186/s13023-019-1075-8
Wada H, Shiraki K, Matsumoto T, Shimpo H, Yamashita Y, Shimaoka M (2020) The evaluation of a scoring system for diagnosing atypical hemolytic uremic syndrome. Thrombosis Update 1: 100012. https://doi.org/10.1016/j.tru.2020.100012
Wang X, Sun X, Birch S, Gong F, Valentijn P, Chen L, Yang H (2018) People-centred integrated care in urban China. Bull World Health Organ 96(12):843–852. https://doi.org/10.2471/blt.18.214908
Wong SH, McClaren BJ, Archibald AD, Weeks A, Langmaid T, Ryan MM, Metcalfe SA (2015) A mixed methods study of age at diagnosis and diagnostic odyssey for Duchenne muscular dystrophy. Eur J Hum Genet 23(10):1294–1300. https://doi.org/10.1038/ejhg.2014.301
Xu RH, Ng SSM, Luo N, Dong D, Zhang S (2023) Measurement of health-related quality of life in individuals with rare diseases in china: nation-wide online survey. JMIR Public Health Surveill 9:e50147. https://doi.org/10.2196/50147
Xu J, Yu MR, Zhang ZG, Gong SW, Li BQ (2023) Is sub-national healthcare social protection sufficient for protecting rare disease patients? the case of China. Front Public Health 11:1198368 https://doi.org/10.3389/fpubh.2023.1198368
Yan K, Desai K, Gullapalli L, Druyts E, Balijepalli C (2020) Epidemiology of atypical hemolytic uremic syndrome: a systematic literature review. Clin Epidemiol 12:295–305. https://doi.org/10.2147/clep.S245642
Yan X, He SJ, Dong D (2020) Determining how far an adult rare disease patient needs to travel for a definitive diagnosis: a cross-sectional examination of the 2018 national rare disease survey in China. Int J Environ Res Public Health 17(5):1757. https://doi.org/10.3390/ijerph17051757
Yang G, Cintina I, Pariser A, Oehrlein E, Sullivan J, Kennedy A (2022) The national economic burden of rare disease in the United States in 2019. Orphanet J Rare Dis 17(1):163. https://doi.org/10.1186/s13023-022-02299-5
Zhang S, Chen L, Zhang Z, Zhao Y (2019) Orphan drug development in China: progress and challenges. Lancet 394(10204):1127–1128. https://doi.org/10.1016/s0140-6736(19)32179-8
Zhang S, Wu Y, Ma W, Cheng M, Li L (2021) Seeking medical services through guanxi in China. Patient Educ Couns 104(7):1789–1795. https://doi.org/10.1016/j.pec.2020.12.004
Zhang XY, Dai LY, Long YL, Chen X, Alhafi MAK (2024) Healthcare costs for patients with rare diseases: evidence from China. Int J Health Plan Manag 39(1):48–61. https://doi.org/10.1002/hpm.3713
Zhang Z (2024) Survey and analysis on the resource situation of primary health care institutions in rural China. Front Public Health 12: 1394527. https://doi.org/10.3389/fpubh.2024.1394527
Zhao S, Wang Y, Chen Y, Zhou M (2025) Healthcare resource allocation and patient choice: evidence from rural China. Int J Equity Health 24(1):87. https://doi.org/10.1186/s12939-025-02450-1
Zhou L, Xu J, Yang J (2022) Poor education and urgent information need for emergency physicians about rare diseases in China. Orphanet J Rare Dis 17(1):211. https://doi.org/10.1186/s13023-022-02354-1
Acknowledgements
The authors thank all the patients involved in this study. This study received funding from the Beijing Novartis Pharma Co., Ltd. The funders had no role in trial design, data collection, analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Z.Y.L. and Y.N.W. contributed equally to this work. S.P.L., Z.Y.L. and Y.N.W. were involved in the conceptualization, design, and methodology of this Study. Z.Y.L. and Y.N.W. performed data analysis and drafted the manuscript. S.P.L. support the management and coordination of the planning and execution of research activities. All authors have read and approved the final version of the manuscript and consent to its publication.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests. This study received funding from the Beijing Novartis Pharma Co., Ltd (no grant no.). The funder had no influence on the design and conduct of the study; collection, management, analysis and interpretation of the data; or preparation, review or approval of the manuscript.
Ethical approval
This study was screened and approved by the Ethics Committee of Centre for Health Management and Policy Research, Shandong University (No. ECSHCMSDU20211103; approval data from 01/01/2022). This approval covered the entire study protocol. All research involving human participants was performed in strict accordance with the principles of the Declaration of Helsinki, the “Measures for Ethical Review of Biomedical Research Involving Humans”, and relevant national and institutional guidelines and regulations regarding ethical conduct in research.
Informed consent
Informed consent was obtained from all study participants, including aHUS patients, their caregivers, and medical specialists. We informed each participant of their rights, the purpose of the study and to safeguard their personal information. Informed consent was obtained from each participant on the day of their recruitment, immediately before the survey commenced. The data collection, and therefore the acquisition of consent, took place between January 13th to August 25th 2023.
Consent for publication
Patients signed informed consent regarding publishing their data.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Liu, Z., Wu, Y. & Li, S. Facilitators and barriers to healthcare services among patients with Atypical Hemolytic-Uremic Syndrome: a qualitative study. Humanit Soc Sci Commun 12, 1958 (2025). https://doi.org/10.1057/s41599-025-06257-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1057/s41599-025-06257-x