Abstract
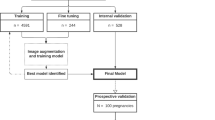
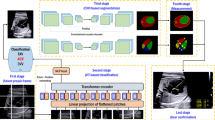
Prenatal assessment of fetal cardiac function is crucial for predicting neonatal outcomes, yet manual echocardiographic measurements are labor-intensive and subjective. We developed a fully automated artificial intelligence (AI) workflow for estimating fetal cardiac function parameters from echocardiograms. The workflow integrates a deep learning model for real-time detection and segmentation of cardiac structures, followed by quality control and geometric calculation. It was developed and validated using an internal dataset of 52,942 annotated images from 1940 normal fetal echocardiograms, with further testing on two external normal datasets (245 echocardiograms) and one internal abnormal dataset (83 echocardiograms). Performance was compared against manual and Fetal Heart Quantification (Fetal HQ) measurements, and a dynamic Z-score model referencing gestational age and fetal biometrics was established. The AI achieved accurate segmentation, with mean Dice similarity coefficients >92% and mean intersection-over-union >85% across all test datasets. It exhibited higher intraclass correction coefficients and R-values relative to experts than inter-observer variability, alongside smaller mean absolute error and limits of agreement. The mean individual equivalence coefficients of all cardiac function parameters were below zero, indicating lower variability than manual or Fetal HQ. These results demonstrate that our fully automated AI workflow enables accurate, efficient, and reproducible quantification of fetal cardiac function, supporting its potential for standardized clinical application.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available to qualified researchers on reasonable request from the corresponding authors. Please email the corresponding author Dr. Hongning Xie at xiehn@mail.sysu.edu.cn.
Code availability
The codes of the paper are available on reasonable request. Please email the corresponding author Dr. Hongning Xie at xiehn@mail.sysu.edu.cn.
References
Zimmerman, M. S. et al. Global, regional, and national burden of congenital heart disease, 1990–2017: a systematic analysis for the global burden of disease study 2017. Lancet Child Adolesce Health 4, 185–200 (2020).
Semmler, J. et al. Influence of birth weight on fetal cardiac indices at 35–37 weeks’ gestation. Ultrasound Obstet. Gynecol. 57, 266–272 (2021).
Wald, R. M. & Mertens, L. L. Hypoplastic left heart syndrome across the lifespan: clinical considerations for care of the fetus, child, and adult. Can. J. Cardiol. 38, 930–945 (2022).
Czeiger, S. et al. Umbilical–portal–systemic venous shunt and intrauterine growth restriction: an inquiry from a prospective study. Am. J. Obstet. Gynecol. 231, 340–e1 (2024).
Peixoto, A. B., Bravo-Valenzuela, N. J., Rocha, L. A. & Araujo, E. Spectral doppler, tissue doppler, and speckle-tracking echocardiography for the evaluation of fetal cardiac function: an update. Radiologia Brasileira 54, 99–106 (2021).
Nakata, M., Sakuma, J., Takano, M. & Nagasaki, S. Assessment of fetal cardiac function with echocardiography. J. Obstet. Gynaecol. Res. 46, 31–38 (2020).
DeVore, G. R., Klas, B., Satou, G. & Sklansky, M. Quantitative evaluation of fetal right and left ventricular fractional area change using speckle-tracking technology. Ultrasound Obstet. Gynecol. 53, 219–228 (2019).
DeVore, G. R., Portella, P. P., Andrade, E. H., Yeo, L. & Romero, R. Cardiac measurements of size and shape in fetuses with absent or reversed end-diastolic velocity of the umbilical artery and perinatal survival and severe growth restriction before 34 weeks’ gestation. J. Ultrasound Med. 40, 1543–1554 (2021).
DeVore, G. R., Klas, B., Satou, G. & Sklansky, M. Measuring the area of the interventricular septum in the 4-chamber view: A new technique to evaluate the fetus at risk for septal hypertrophy. J. Ultrasound Med. 41, 2939–2953 (2022).
DeVore, G. R., Satou, G. M., Afshar, Y., Harake, D. & Sklansky, M. Evaluation of fetal cardiac size and shape: a new screening tool to identify fetuses at risk for tetralogy of fallot. J. Ultrasound Med. 40, 2537–2548 (2021).
Li, S., Wang, L., Yang, H. & Fan, L. Changes in the shape and function of the fetal heart of pre-and gestational diabetes mothers. BMC pregnancy childbirth 24, 57 (2024).
Sermesant, M., Delingette, H., Cochet, H., Jaïs, P. & Ayache, N. Applications of artificial intelligence in cardiovascular imaging. Nat. Rev. Cardiol. 18, 600–609 (2021).
Castiglioni, I. et al. Ai applications to medical images: From machine learning to deep learning. Phys. Med. 83, 9–24 (2021).
Shen, Y.-T., Chen, L., Yue, W.-W. & Xu, H.-X. Artificial intelligence in ultrasound. Eur. J. Radiol. 139, 109717 (2021).
Qiao, S. et al. Flds: An intelligent feature learning detection system for visualizing medical images supporting fetal four-chamber views. IEEE J. Biomed. health Inform. 26, 4814–4825 (2021).
Ungureanu, A. et al. Learning deep architectures for the interpretation of first-trimester fetal echocardiography (life)-a study protocol for developing an automated intelligent decision support system for early fetal echocardiography. BMC Pregnancy Childbirth 23, 20 (2023).
Garcia, M. et al. Prospective evaluation of the fetal heart using fetal intelligent navigation echocardiography (fine). Ultrasound Obstet. Gynecol. 47, 450–459 (2016).
Wong, H. S., Chan, W. X., Mao, W. & Yap, C. H. 3d velocity and pressure field reconstruction in the cardiac left ventricle via physics informed neural network from echocardiography guided by 3d color doppler. Computer Methods Prog. Biomedicine 263, 108671 (2025).
Qiao, S. et al. A pseudo-siamese feature fusion generative adversarial network for synthesizing high-quality fetal four-chamber views. IEEE J. Biomed. health Inform. 27, 1193–1204 (2022).
Schlemper, J. et al. Attention gated networks: Learning to leverage salient regions in medical images. Med. image Anal. 53, 197–207 (2019).
Hu, Y. et al. Freehand ultrasound image simulation with spatially-conditioned generative adversarial networks. International Workshop on Computational Methods for Molecular Imaging 105–115 (2017).
Tang, J. et al. A multicenter study on two-stage transfer learning model for duct-dependent chds screening in fetal echocardiography. NPJ digital Med. 6, 143 (2023).
Xi, J. et al. Simultaneous segmentation of fetal hearts and lungs for medical ultrasound images via an efficient multi-scale model integrated with attention mechanism. Ultrasonic imaging 43, 308–319 (2021).
Ling, S. et al. A coarse-fine collaborative learning model for three vessel segmentation in fetal cardiac ultrasound images. IEEE J. Biomed. Health Inform. 28, 4036–4047 (2024).
Lu, Y., Li, K., Pu, B., Tan, Y. & Zhu, N. A yolox-based deep instance segmentation neural network for cardiac anatomical structures in fetal ultrasound images. IEEE/ACM Trans. Computational Biol. Bioinforma. 21, 1007–1018 (2022).
Xu, L. et al. Dw-net: A cascaded convolutional neural network for apical four-chamber view segmentation in fetal echocardiography. Computerized Med. Imaging Graph. 80, 101690 (2020).
Arnaout, R. et al. An ensemble of neural networks provides expert-level prenatal detection of complex congenital heart disease. Nat. Med. 27, 882–891 (2021).
Taksøe-Vester, C. et al. Role of artificial-intelligence-assisted automated cardiac biometrics in prenatal screening for coarctation of aorta. Ultrasound Obstet. Gynecol. 64, 36–43 (2024).
Yu, L., Guo, Y., Wang, Y., Yu, J. & Chen, P. Determination of fetal left ventricular volume based on two-dimensional echocardiography. J. Healthc. Eng. 2017, 4797315 (2017).
Liang, B. et al. Automatic segmentation of 15 critical anatomical labels and measurements of cardiac axis and cardiothoracic ratio in fetal four chambers using nnu-netv2. BMC Med. Inform. Decis. Mak. 24, 128 (2024).
D’Alberti, E. et al. Artificial intelligence-enabled prenatal ultrasound for the detection of fetal cardiac abnormalities: a systematic review and meta-analysis. eClinicalMedicine (2025).
Baumgartner, C. F. et al. Sononet: real-time detection and localisation of fetal standard scan planes in freehand ultrasound. IEEE Trans. Med. imaging 36, 2204–2215 (2017).
He, J., Yang, L., Liang, B., Li, S. & Xu, C. Fetal cardiac ultrasound standard section detection model based on multitask learning and mixed attention mechanism. Neurocomputing 579, 127443 (2024).
Pu, B. et al. Hfsccd: a hybrid neural network for fetal standard cardiac cycle detection in ultrasound videos. IEEE J. Biomed. Health Inform. 28, 2943–2954 (2024).
Pu, B., Zhu, N., Li, K. & Li, S. Fetal cardiac cycle detection in multi-resource echocardiograms using hybrid classification framework. Future Gener. Computer Syst. 115, 825–836 (2021).
Pu, B. et al. Mobileunet-fpn: A semantic segmentation model for fetal ultrasound four-chamber segmentation in edge computing environments. IEEE J. Biomed. Health Inform. 26, 5540–5550 (2022).
Wang, Y., Ding, W., Lin, W., Tan, T. & Gao, Z. Fedhnr: Federated hierarchical resilient learning for echocardiogram segmentation with annotation noise. Expert Syst. Appl. 273, 126841 (2025).
Hadlock, F. P., Harrist, R., Sharman, R. S., Deter, R. L. & Park, S. K. Estimation of fetal weight with the use of head, body, and femur measurements—a prospective study. Am. J. Obstet. Gynecol. 151, 333–337 (1985).
Tuo, G. et al. Fetal aortic coarctation: A combination of third-trimester echocardiographic parameters to improve the prediction of postnatal outcome. Front. Pediatrics 10, 866994 (2022).
Dijkema, E. J., Leiner, T. & Grotenhuis, H. B. Diagnosis, imaging and clinical management of aortic coarctation. Heart 103, 1148–1155 (2017).
McGoldrick E, Stewart F, Parker R, Dalziel S. R. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane database of systematic reviews (2020).
Ramirez Zegarra, R. & Ghi, T. Use of artificial intelligence and deep learning in fetal ultrasound imaging. Ultrasound Obstet. Gynecol. 62, 185–194 (2023).
Drukker, L., Noble, J. & Papageorghiou, A. Introduction to artificial intelligence in ultrasound imaging in obstetrics and gynecology. Ultrasound Obstet. Gynecol. 56, 498–505 (2020).
Tan, Y., Peng, Y., Guo, L., Liu, D. & Luo, Y. Cost-effectiveness analysis of ai-based image quality control for perinatal ultrasound screening. BMC Med. Educ. 24, 1437 (2024).
Dan, T. et al. Deepga for automatically estimating fetal gestational age through ultrasound imaging. Artif. Intell. Med. 135, 102453 (2023).
Han, X. et al. Artificial intelligence assistance for fetal development: evaluation of an automated software for biometry measurements in the mid-trimester. BMC Pregnancy Childbirth 24, 158 (2024).
Lei, T. et al. Development and validation of an artificial intelligence assisted prenatal ultrasonography screening system for trainees. Int. J. Gynecol. Obstet. 165, 306–317 (2024).
Lei, T. et al. Enhancing trainee performance in obstetric ultrasound through an artificial intelligence system: randomized controlled trial (2024).
Xie, B. et al. Computer-aided diagnosis for fetal brain ultrasound images using deep convolutional neural networks. Int. J. computer Assist. Radiol. Surg. 15, 1303–1312 (2020).
Lin, M. et al. Deep learning system improved detection efficacy of fetal intracranial malformations in a randomized controlled trial. NPJ Digital Med. 6, 191 (2023).
Haberer, K., Fruitman, D., Power, A., Hornberger, L. & Eckersley, L. Fetal echocardiographic predictors of biventricular circulation in hypoplastic left heart complex. Ultrasound Obstet. Gynecol. 58, 405–410 (2021).
Mlodawski, J., Zmelonek-Znamirowska, A., Pawlik, L., Mlodawska, M. & Swiercz, G. Reproducibility challenges in fetal cardiac function analysis with 2d speckle-tracking echocardiography: Insights from fetalhq. J. Clin. Med. 14, 3301 (2025).
Chen, Y., Lv, X., Yang, L., Hu, D. & Ren, M. Evaluation of fetal heart size, morphology and function with fetal growth restriction using fetal hq. BMC Pregnancy Childbirth 24, 751 (2024).
Salomon, L. J. et al. Practice guidelines for performance of the routine mid-trimester fetal ultrasound scan. Ultrasound in Obstetrics & Gynecology37 (2011).
Khalil, A. et al. Isuog practice guidelines: performance of third-trimester obstetric ultrasound scan. Ultrasound Obstet. Gynecol. 63, 131–147 (2024).
Zhao, Y. et al. Detrs beat yolos on real-time object detection. Proceedings of the IEEE/CVF conference on computer vision and pattern recognition 16965–16974 (2024).
Li, F. et al. Mask dino: Towards a unified transformer-based framework for object detection and segmentation. Proceedings of the IEEE/CVF conference on computer vision and pattern recognition 3041–3050 (2023).
Otterstad, J. Measuring left ventricular volume and ejection fraction with the biplane simpson’s method. Heart 88, 559–560 (2002).
Royston, P. & Altman, D. G. Regression using fractional polynomials of continuous covariates: parsimonious parametric modelling. J. R. Stat. Soc. Ser. C: Appl. Stat. 43, 429–453 (1994).
Müller, D., Soto-Rey, I. & Kramer, F. Towards a guideline for evaluation metrics in medical image segmentation. BMC Res. Notes 15, 210 (2022).
Hauke, J. & Kossowski, T. Comparison of values of pearson’s and spearman’s correlation coefficients on the same sets of data. Quaest. geographicae 30, 87–93 (2011).
St, L. & Wold, S. Analysis of variance (anova). Chemometrics Intell. Lab. Syst. 6, 259–272 (1989).
Acknowledgements
This study was supported by research grants from the National Scientific Foundation Committee of China (82171938, 81801705), the Guangdong Provincial Basic and Applied Basic Research Fund Project (2022A1515220200), the Guangzhou Science and Technology Program (2024A04J4569).
Author information
Authors and Affiliations
Contributions
C.H.: Writing-review & editing, Writing-original draft, Visualization, Validation, Formal analysis, Investigation, Data curation, Conceptualization; L.Z.: Writing-original draft, Visualization, Formal analysis, Data curation; B.X.: Writing-review & editing, Software, Investigation, Methodology, Conceptualization; Y.J.: Visualization, Formal analysis; Y.Z. and X.L.: Resources, Data curation; T.L.: Writing-review & editing, Funding acquisition; M.H.: Visualization, Formal analysis; Y.Y. and N.W.: Software, Methodology, Resources, Investigation, Data curation; H.X.: Writing-review & editing, Funding acquisition, Supervision, Conceptualization. C.H., L.Z. and B.X. are co-first authors of this work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Huang, C., Zhang, L., Xie, B. et al. Automated interpretation of fetal cardiac function evaluation from the echocardiogram. npj Digit. Med. (2026). https://doi.org/10.1038/s41746-026-02381-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41746-026-02381-3