Abstract
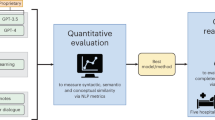
Informed consent forms are essential for protecting patient rights, but are often difficult to understand, especially in non-English settings where formal language and long, context-dependent sentences hinder comprehension. This study evaluated whether large language models (LLMs) can simplify Chinese language surgical consent forms and whether clinician revision can further improve the output. Official forms from nine hospitals were used to create three versions of each document: the original, an LLM-simplified version, and a clinician-revised version. We assessed text structure, readability, content quality, and layperson comprehension using quantitative metrics and expert ratings. The LLM version improved readability and comprehension but reduced content quality, particularly risk information. Clinician revision restored accuracy while maintaining clarity and achieved the highest comprehension scores. Linear mixed effects modeling confirmed these trends. These findings highlight both the impact of LLM-based simplification and the value of human AI collaboration in patient communication.
Similar content being viewed by others
Data availability
The data used in this study are available solely for non-commercial academic purposes and require the signing of a formal data use agreement. All academic data requests should be directed to the corresponding author at wwtdoctor02@163.com. For requests submitted by verified academic researchers, the Data Access Committee will review and respond within 1 month.
Code availability
Qualified researchers may request access to the remaining code by contacting the corresponding authors (wwtdoctor02@163.com). For requests submitted by verified academic researchers, the Data Access Committee will assess the request and grant access within one month.
References
Schenker, Y. & Meisel, A. Informed consent in clinical care: practical considerations in the effort to achieve ethical goals. JAMA 305, 1130–1131 (2011).
Perni, S. et al. Assessment of use, specificity, and readability of written clinical informed consent forms for patients with cancer undergoing radiotherapy. JAMA Oncol. 5, e190260 (2019).
Patil, A., Chawathey, S. & Malim, A. Adequacy of informed consent in elective surgical procedures: a study in a Navi Mumbai tertiary care centre. Cureus 15, e41777 (2023).
García-Álvarez, J. M. & García-Sánchez, A. Readability and comprehension of anesthesia informed consent forms in a Spanish county hospital: an observational study. Nurs. Rep. 14, 1338–1352 (2024).
Wen, G. et al. Readability and content assessment of informed consent forms for phase II-IV clinical trials in China. PLoS One 11, e0164251 (2016).
Esemen, Y., Mostofi, A., Richardson, D. & Pereira, E. Are we meeting the standards set for informed consent in spinal surgery?. Ann. R. Coll. Surg. Engl. 105, 372–377 (2023).
Shi, Q. et al. Transforming informed consent generation using large language models: mixed methods study. JMIR Med. Inf. 13, e68139 (2025).
Mirza, F. et al. Using ChatGPT to facilitate truly informed medical consent. NEJM AI 1, aics2300145 (2024).
Shah, N. H., Entwistle, D. & Pfeffer, M. A. Creation and adoption of large language models in medicine. JAMA 330, 866–869 (2023).
Wornow, M. et al. The shaky foundations of large language models and foundation models for electronic health records. NPJ Digit Med. 6, 135 (2023).
Bedi, S. et al. Testing and evaluation of health care applications of large language models: a systematic review. JAMA 333, 319–328 (2025).
Grünebaum, A., Dudenhausen, J. & Chervenak, F. A. Enhancing patient understanding in obstetrics: the role of generative AI in simplifying informed consent for labor induction with oxytocin. J. Perinat. Med. 53, 688–695 (2025).
Patel, I., Om, A., Cuzzone, D. & Garcia Nores, G. Comparing ChatGPT vs surgeon-generated informed consent documentation for plastic surgery procedures. Aesthet. Surg. J. Open Forum 6, ojae092 (2024).
Wang, Y. & Ma, Z. Ethical and legal challenges of medical AI on informed consent: China as an example. Dev. World Bioeth. 25, 46–54 (2025).
Waters, M. AI meets informed consent: a new era for clinical trial communication. JNCI Cancer Spectr. 9, https://doi.org/10.1093/jncics/pkaf028 (2025).
Feinberg, I. Z., Gajra, A., Hetherington, L. & McCarthy, K. S. Simplifying informed consent as a universal precaution. Sci. Rep. 14, 13195 (2024).
Williams, C. Y. K. et al. Use of a large language model to assess clinical acuity of adults in the emergency department. JAMA Netw. Open 7, e248895 (2024).
Cosma, C. et al. Potential role of ChatGPT in simplifying and improving informed consent forms for vaccination: a pilot study conducted in Italy. BMJ Health Care Inform. 32, e101248 (2025).
Mirza, F. N. et al. The literacy barrier in clinical trial consents: a retrospective analysis. EClinicalMedicine 75, 102814 (2024).
Mishra, V., Sarraju, A., Kalwani, N. M. & Dexter, J. P. Evaluation of prompts to simplify cardiovascular disease information generated using a large language model: cross-sectional study. J. Med. Internet Res. 26, e55388 (2024).
Meskó, B. & Topol, E. J. The imperative for regulatory oversight of large language models (or generative AI) in healthcare. NPJ Digit. Med. 6, 120 (2023).
Van Veen, D. et al. Adapted large language models can outperform medical experts in clinical text summarization. Nat. Med. 30, 1134–1142 (2024).
Omiye, J. A., Lester, J. C., Spichak, S., Rotemberg, V. & Daneshjou, R. Large language models propagate race-based medicine. NPJ Digit. Med. 6, 195 (2023).
Oh, N. et al. Large language model-assisted surgical consent forms in non-english language: content analysis and readability evaluation. J. Med. Int. Res. 27, e73222 (2025).
Aydin, S., Karabacak, M., Vlachos, V. & Margetis, K. Large language models in patient education: a scoping review of applications in medicine. Front. Med. 11, 1477898 (2024).
Picton, B. et al. Assessing AI simplification of medical texts: readability and content fidelity. Int. J. Med. Inf. 195, 105743 (2025).
Tang, L. et al. Evaluating large language models on medical evidence summarization. NPJ Digit Med 6, 158 (2023).
Ali, R. et al. Bridging the literacy gap for surgical consents: an AI-human expert collaborative approach. NPJ Digit Med. 7, 63 (2024).
Goh, E. et al. Large language model influence on diagnostic reasoning: a randomized clinical trial. JAMA Netw. Open 7, e2440969 (2024).
Tam, T. Y. C. et al. A framework for human evaluation of large language models in healthcare derived from literature review. NPJ Digit. Med. 7, 258 (2024).
Budd, S., Robinson, E. C. & Kainz, B. A survey on active learning and human-in-the-loop deep learning for medical image analysis. Med Image Anal. 71, 102062 (2021).
Decker, H. et al. Large language model-based chatbot vs surgeon-generated informed consent documentation for common procedures. JAMA Netw. Open 6, e2336997 (2023).
Teasdale, A., Mills, L. & Costello, R. Artificial intelligence-powered surgical consent: patient insights. Cureus 16, e68134 (2024).
Agar, M., Ko, D. N., Sheehan, C., Chapman, M. & Currow, D. C. Informed consent in palliative care clinical trials: challenging but possible. J. Palliat. Med. 16, 485–491 (2013).
Hager, P. et al. Evaluation and mitigation of the limitations of large language models in clinical decision-making. Nat. Med. 30, 2613–2622 (2024).
Pietrzykowski, T. & Smilowska, K. The reality of informed consent: empirical studies on patient comprehension-systematic review. Trials 22, 57 (2021).
Dennstädt, F., Hastings, J., Putora, P. M., Schmerder, M. & Cihoric, N. Implementing large language models in healthcare while balancing control, collaboration, costs and security. NPJ Digit. Med. 8, 143 (2025).
Busch, F. et al. Large language models for structured reporting in radiology: past, present, and future. Eur. Radiol. 35, 2589–2602 (2025).
Lo, L. S. The art and science of prompt engineering: a new literacy in the information age. Internet Ref. Serv. Q. 27, 203–210 (2023).
Chen, S. Y., Chang, S. S., Lin, C. C., Lou, Q. & Anderson, R. M. Psychometric evaluation of the informed consent process scale in Chinese. Nurs. Ethics 26, 2456–2466 (2019).
O’Sullivan, L., Sukumar, P., Crowley, R., McAuliffe, E. & Doran, P. Readability and understandability of clinical research patient information leaflets and consent forms in Ireland and the UK: a retrospective quantitative analysis. BMJ Open 10, e037994 (2020).
Sevey, N., Barratt, M. & Omoruyi, E. Can incoming United States pediatric interns be entrusted with the essential communication skills of informed consent?. J. Educ. Eval. Health Prof. 17, 18 (2020).
Nishimura, A. et al. Improving understanding in the research informed consent process: a systematic review of 54 interventions tested in randomized control trials. BMC Med. Ethics 14, 28 (2013).
Acknowledgements
This study received no external funding. We gratefully acknowledge Jinbang Kou and Xian Xu for their contributions as non-medical volunteers in evaluating the layperson comprehension of the informed consent texts. We also thank Xin Zhang for her valuable input and guidance in refining the statistical methodology. We further thank Che Sun from the Big Data Center for providing professional guidance on issues related to model API usage and implementation. Finally, we thank Fuzhen Dai, Nianfu Wu, Jianwei Xing, Shuqi Zhang, and Weigang Tang for kindly providing the original informed consent materials used in this study.
Author information
Authors and Affiliations
Contributions
J.L. designed the study, organized the study execution, developed the prompting strategy, collected the original informed consent documents, conducted statistical analyses, created figures and tables, and contributed to manuscript writing and revision. J.M. developed the code, performed statistical analyses, created visualizations, evaluated the layperson comprehension of all documents as a non-hepatobiliary clinician, and contributed to manuscript writing and revision. Y.Q. reviewed the LLM-generated documents as a hepatobiliary surgeon and generated the LLM+Clinician versions, performed statistical analyses, and contributed to manuscript writing and revision. T.W. assessed the content quality of all documents as a hepatobiliary surgeon and contributed to manuscript review and revision. Y.Y. assessed the content quality of all documents as a hepatobiliary surgeon and contributed to manuscript review and revision. G.Q. assessed the content quality of all documents as a hepatobiliary surgeon, contributed to the collection of original documents, and participated in manuscript review and revision. H.C. assessed the content quality of all documents as a hepatobiliary surgeon, contributed to the collection of original documents, and participated in manuscript review and revision. J.P. evaluated the layperson comprehension of all documents as a non-hepatobiliary clinician, contributed to the collection of original documents, and participated in manuscript review and revision. W.W. designed and supervised the study, oversaw the research process, contributed to manuscript review and revision, and coordinated the submission process as the corresponding author. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Luo, J., Ma, J., Qiu, Y. et al. Evaluating large language models for simplifying non-English medical consent with clinician involvement. npj Digit. Med. (2026). https://doi.org/10.1038/s41746-026-02591-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41746-026-02591-9