Abstract
Background
Evidence on risk factors for a complicated course of lower respiratory tract infections (LRTIs) in primary care remains limited and often consensus based. While socioeconomic status (SES) and migration background have been linked to complicated LRTIs in population-based studies, their predictive value in primary care remains unclear. Consequently, these factors are not incorporated within current guidelines, which may contribute to health inequalities. Therefore, we aimed to evaluate the added value of SES and migration background as predictive factors of a complicated course of LRTIs in primary care.
Methods
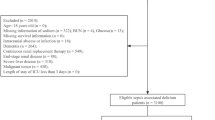
Routine care data from Dutch general practices participating in the Extramural LUMC Academic Network database (Leiden-The Hague-Zoetermeer region) from 2014 to 2023, excluding COVID-19 years, was linked to sociodemographic and hospital claims data from Statistic Netherlands. Adults presenting with LRTI complaints were included (n = 145,445). Multivariable logistic regression models were constructed to predict 30-day hospitalisation or death following LRTI. Models included conventional risk factors with SES and migration background subsequently added.
Results
In this study we show that after adjusting for conventional clinical factors, SES is a strong predictor of a complicated course of LRTI, whereas migration background is not. Patients in the lowest SES category have an adjusted odds ratio of 1.46 (95%CI: 1.31 – 1.62) for a complicated course compared to the highest.
Conclusions
SES is a strong predictor of a complicated course of LRTI in primary care, even after adjusting for conventional risk factors. The incorporation of SES into clinical decision tools and guidelines has the potential to enhance risk-stratification of patients with LRTI in daily practice of primary care, thereby supporting more equitable care.
Plain language summary
Lower respiratory tract infections, such as pneumonia, are common and sometimes lead to hospitalisation or death in severe cases. Currently, general practitioners use age and health conditions to assess risk, but social factors like socioeconomic status (SES) and migration background are not considered. This may lead to unequal differences in health outcomes. We analysed data from adults in Dutch general practices to see if these social factors improve predictions of severe outcomes within 30 days. We found that SES is an important predictor, even after accounting for other risk factors, while migration background had no significant effect. These findings suggest that including SES in future prediction tools and guidelines could help achieve a more equitable identification of patients at increased risk.
Similar content being viewed by others
Data availability
The data that support the findings of this study may be obtained from a third party and cannot be shared publicly due to the current Dutch legislation for data protection of Statistics Netherlands data. Data is stored by Statistic Netherlands. Under certain conditions, the dataset and additional microdata are accessible for statistical and scientific research and must be directly requested from Statistics Netherlands (microdata@cbs.nl). Source data for Fig. 1 and Fig. 2 are provided in Supplementary Data 1.
Code availability
All code required to reproduce the results of this study are disclosed through a repository on GitHub: https://github.com/elan-dcc/VanDokkum2648. All analyses were performed in Stata (Stata Corp 2023. Stata Statistical Software: Release 18. College Station, Texas, USA: Stata Corp LLC).
References
Volksgezondheid en Zorg. Aandoeningen op basis van ziektelast. vzinfo.nl. https://www.vzinfo.nl/ranglijsten/aandoeningen-op-basis-van-ziektelast (2024).
Santos, J. V. et al. The state of health in the European Union (EU-27) in 2019: a systematic analysis for the Global Burden of Disease study 2019. BMC Public Health 24, 1374 (2024).
Møgelmose, S., Neels, K., Beutels, P. & Hens, N. Exploring the impact of population ageing on the spread of emerging respiratory infections and the associated burden of mortality. BMC Infect. Dis. 23, 767 (2023).
Ukoaka, B. M. et al. Updated WHO list of emerging pathogens for a potential future pandemic: implications for public health and global preparedness. Infez. Med. 32, 463–477 (2024).
Government of the Netherlands. Standard health insurance. government.nl. https://www.government.nl/topics/health-insurance/standard-health-insurance (accessed 2025).
OECD & European Observatory on Health Systems and Policies. The Netherlands: Country Health Profile 2023, State of Health in the EU. World Health Organization (2023).
Bijkerk, S. et al. Socioeconomic disparities and risk of recurrent cardiovascular events and cardiovascular disease-free life expectancy in patients with established cardiovascular disease. Eur. J. Prev. Cardiol. (2025).
Kist, J. M. et al. Large health disparities in cardiovascular death in men and women, by ethnicity and socioeconomic status in an urban based population cohort. EClinicalMedicine 40, 101120 (2021).
The Lancet Regional Health - Europe. Navigating disparities in cardiovascular disease outcomes across Europe: a call to action. Lancet Reg. Health Eur. 33, 100746 (2023).
Hojstrup, S., Thomsen, J. H. & Prescott, E. Disparities in cardiovascular disease and treatment in the Nordic countries. Lancet Reg. Health Eur. 33, 100699 (2023).
Ayorinde, A. et al. Health inequalities in infectious diseases: a systematic overview of reviews. BMJ Open 13, e067429 (2023).
Faber, M. J., Burgers, J. S. & Westert, G. P. A sustainable primary care system: lessons from the Netherlands. J. Ambul. Care Manag. 35, 174–181 (2012).
Sripa, P., Hayhoe, B., Garg, P., Majeed, A. & Greenfield, G. Impact of GP gatekeeping on quality of care, and health outcomes, use, and expenditure: a systematic review. Br. J. Gen. Pract. 69, e294–e303 (2019).
Nielen, M., Hek, K., Weesie, Y., Davids, R. & Korevaar, J. Hoe vaak hebben Nederlanders contact met de huisartsenpraktijk? Zorggebruik in de huisartsenpraktijk in 2019. NIVEL (2020).
De Bont, E. G. P. M. et al. NHG-Standaard Acuut hoesten. Nederlands Huisartsen Genootschap (2024).
Rijk, M. H. et al. Prognostic factors and prediction models for hospitalisation and all-cause mortality in adults presenting to primary care with a lower respiratory tract infection: a systematic review. BMJ Open 14, e075475 (2024).
Ramirez, J. A. et al. Adults hospitalized with pneumonia in the United States: incidence, epidemiology, and mortality. Clin. Infect. Dis. 65, 1806–1812 (2017).
Wiemken, T. L. et al. Socioeconomic position and the incidence, severity, and clinical outcomes of hospitalized patients with community-acquired pneumonia. Public Health Rep. 135, 364–371 (2020).
Sloan, C., Chandrasekhar, R., Mitchel, E., Schaffner, W. & Lindegren, M. L. Socioeconomic disparities and influenza hospitalizations, Tennessee, USA. Emerg. Infect. Dis. 21, 1602–1610 (2015).
Lawrence, H., McKeever, T. M. & Lim, W. S. Impact of social deprivation on clinical outcomes of adults hospitalised with community-acquired pneumonia in England: a retrospective cohort study. BMJ Open Respir. Res. 9, e001 (2022).
van Dokkum, E. D. et al. Health disparities in complicated lower respiratory tract infections: a population-based cohort study in The Hague, The Netherlands. BMJ Public Health 3, e002788 (2025).
Black, C. L. et al. Vital signs: influenza hospitalizations and vaccination coverage by race and ethnicity—United States, 2009–10 through 2021–22 influenza seasons. MMWR Morb. Mortal. Wkly Rep. 71, 1366–1373 (2022).
O’Halloran, A. C. et al. Rates of influenza-associated hospitalization, intensive care unit admission, and in-hospital death by race and ethnicity in the United States from 2009 to 2019. JAMA Netw. Open 4, e2121880 (2021).
Ardesch, F. H. et al. The introduction of a data-driven population health management approach in the Netherlands since 2019: the Extramural LUMC Academic Network data infrastructure. Health Policy 132, 104769 (2023).
Kist, J. M. et al. Data Resource Profile: Extramural Leiden University Medical Center Academic Network (ELAN). Int. J. Epidemiol. 53, (2024).
Hrzic, R., Clemens, T., Westra, D. & Brand, H. Comparability in cross-national health research using insurance claims data: the cases of Germany and the Netherlands. Gesundheitswesen 82, S83–S90 (2020).
Kist, J. M. et al. SCORE2 cardiovascular risk prediction models in an ethnic and socioeconomic diverse population in the Netherlands: an external validation study. EClinicalMedicine 57, 101862 (2023).
Statistics Netherlands. Microdata 2019. cbs.nl. https://www.cbs.nl/en-gb/our-services/customised-services-microdata/microdata-conducting-your-own-research/overview-of-all-datasets. (accessed 2026).
Tseng, T. E. et al. International validation of the SORG machine-learning algorithm for predicting the survival of patients with extremity metastases undergoing surgical treatment. Clin. Orthop. Relat. Res. 480, 367–378 (2022).
Burnham, K. P. & Anderson, D. R. Model Selection and Multimodel Inference: A Practical Information-Theoretic Approach. 2nd edn (Springer, 2002).
Bont, J., Hak, E., Hoes, A. W., Schipper, M. & Verheij, T. J. A prediction rule for elderly primary-care patients with lower respiratory tract infections. Eur. Respir. J. 29, 969–975 (2007).
Moore, M. et al. Predictors of adverse outcomes in uncomplicated lower respiratory tract infections. Ann. Fam. Med. 17, 231–238 (2019).
Hak, E., Bont, J., Hoes, A. W. & Verheij, T. J. Prognostic factors for serious morbidity and mortality from community-acquired lower respiratory tract infections among the elderly in primary care. Fam. Pract. 22, 375–380 (2005).
Bruyndonckx, R. et al. Development of a prediction tool for patients presenting with acute cough in primary care: a prognostic study spanning six European countries. Br. J. Gen. Pract. 68, e342–e350 (2018).
World Health Organization. A conceptual framework for action on the social determinants of health (WHO, 2010).
Zorn, J. et al. Effects of long-term exposure to outdoor air pollution on COVID-19 incidence: a population-based cohort study accounting for SARS-CoV-2 exposure levels in the Netherlands. Environ. Res. 252, 118812 (2024).
Anekwe, C. V., Jarrell, A. R., Townsend, M. J., Gaudier, G. I. & Hiserodt, J. M. Socioeconomics of obesity. Curr. Obes. Rep. 9, 272–279 (2020).
Arpey, N. C., Gaglioti, A. H. & Rosenbaum, M. E. How socioeconomic status affects patient perceptions of health care: a qualitative study. J. Prim. Care Community Health 8, 169–175 (2017).
Hiscock, R., Bauld, L., Amos, A., Fidler, J. A. & Munafò, M. R. Socioeconomic status and smoking: a review. Ann. N. Y. Acad. Sci. 1248, 107–123 (2012).
Algren, M. H., Bak, C. K., Berg-Beckhoff, G. & Andersen, P. T. Health-risk behaviour in deprived neighbourhoods compared with non-deprived neighbourhoods: a systematic literature review of quantitative observational studies. PLoS One 10, e0139297 (2015).
Braveman, P. & Gottlieb, L. The social determinants of health: it’s time to consider the causes of the causes. Public Health Rep. 129, 19–31 (2014).
Mavus, M., van Stiphout-Kramer, B. & Bijwaard, G. Blijven of vertrekken? Een analyse van de verblijfsduur van arbeidsmigranten. Centraal Planbureau (2025).
Goorts, I. Zorg(en) voor arbeidsmigranten. Pharos (2022).
van Gaalen, R., de Vries, F., Bras, V. & Zorlu, A. Komen en gaan van arbeidsmigranten in de periode 2005–2021. Centraal Bureau voor de Statistiek (2025).
Kennedy, S., Kidd, M. P., McDonald, J. T. & Biddle, N. The healthy immigrant effect: patterns and evidence from four countries. J. Int. Migr. Integr. 16, 317–332 (2015).
Mantu, S., Berntsen, L., de Lange, T., Böcker, A. & Skowronek, N. EU migrant workers and the right to health in the Netherlands during and beyond the COVID-19 pandemic. Transfer (2025).
Winchester, C. C., Macfarlane, T. V., Thomas, M. & Price, D. Antibiotic prescribing and outcomes of lower respiratory tract infection in UK primary care. Chest 135, 1163–1172 (2009).
van Dokkum, E. D. et al. Code to accompany the article ‘Socioeconomic and migration factors as predictors of complicated lower respiratory tract infections in primary care’. GitHub (2026).
Acknowledgements
The study was not funded by a specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors contributed equally to the conceptualisation of the study. Study design and methodology: HB CvN EDvD SlC. Literature search: EDvD and NK with contributions from HB and CvN. Data curation and data analysis: EDvD and NK with substantial contributions from HB and SlC. Data interpretation: EDvD, NK, HB and CvN with substantial contributions from all authors. Visualisation of results: EDvD, NK, HB and CvN with contributions of all authors. EDvD wrote the first draft of the manuscript with inputs from NK, HB, and CvN. All authors reviewed and revised drafts of the manuscript and approved the final version. EDvD, NK, and HB have full access to and have verified all the study data provided for the analysis.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Communications Medicine Ana Clavería, Gabrial Iglesias-Caride, and the other, anonymous, reviewer for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
van Dokkum, E.D., Kraaijenbrink, N., Le Cessie, S. et al. Socioeconomic status and migration background as predictors of complicated lower respiratory tract infections in primary care. Commun Med (2026). https://doi.org/10.1038/s43856-026-01542-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s43856-026-01542-5