Abstract
Background
Short-chain fatty acids are believed to mediate microbiome-host interactions. Acetic acid is the most abundant systemic short-chain fatty acid, but knowledge about its physiological functions comes mainly from rodent experiments, with limited human research particularly in the aging population.
Methods
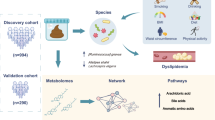
In this cross-sectional observational study, we examined the association between the gut microbiota and plasma acetic acid, specifically investigating the mediating effect of plasma acetic acid on the relationship between the gut microbiota and blood lipid profile, body composition, brain gray matter volume, and cognitive performance in older adults. The gut microbiome was profiled using full-length 16S rRNA gene sequencing to enable taxonomic classification.
Results
Here we show that specific gut microbial co-abundance group is associated with plasma acetic acid levels. Higher plasma levels of acetic acid are associated with lower plasma triglyceride levels, higher high-density lipoprotein cholesterol levels, lower body mass index, lower body fat mass, higher thalamic volume, and higher cognitive performance in certain domains. Additionally, we show that plasma acetic acid mediates the relationship between gut microbiome on these health measures.
Conclusions
This study identifies gut microbial group linked to plasma acetic acid and demonstrates its potential mediating role between the gut microbiome, blood lipid profile, brain volume and cognitive function in older adults. These insights pave the way for future research and highlight the potential of acetic acid as an intervention target for metabolic and neurological diseases, contributing to strategies that promote healthy aging.
Plain language summary
The gut microbiome plays an important role in maintaining human health, partly through producing short-chain fatty acids such as acetic acid. However, little is known about how acetic acid relates to metabolic and brain health in older adults. In this study, we examined stool and blood samples from older individuals to assess the relationship between gut bacteria, plasma acetic acid levels, and various health measures, including body composition, blood lipids, brain structure, and cognitive performance. We found that higher plasma acetic acid levels were associated with healthier metabolism, greater brain volume, and better cognitive abilities. These results suggest that acetic acid may serve as a link between gut health and metabolic health as well as brain function during aging, highlighting its potential as a target for future preventive strategies.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author, C.H.T. A decision regarding data access will be provided within four weeks of receipt of a complete request. The data are not publicly available because they contain information that could compromise research participant privacy or consent.
Code availability
The code used for data analysis in this study is not publicly available but can be provided by the corresponding author upon reasonable request.
References
Sarkar, A. et al. The microbiome in psychology and cognitive neuroscience. Trends Cogn. Sci. 22, 611–636 (2018).
Mayer, E. A., Knight, R., Mazmanian, S. K., Cryan, J. F. & Tillisch, K. Gut microbes and the brain: paradigm shift in neuroscience. J. Neurosci. 34, 15490–15496 (2014).
Fan, Y. & Pedersen, O. Gut microbiota in human metabolic health and disease. Nat. Rev. Microbiol. 19, 55–71 (2021).
Zhang, D. et al. Short-chain fatty acids in diseases. Cell Commun. Signal 21, 212 (2023).
Lynch, S. V. & Pedersen, O. The human intestinal microbiome in health and disease. N. Engl. J. Med. 375, 2369–2379 (2016).
Claesson, M. J. et al. Gut microbiota composition correlates with diet and health in the elderly. Nature 488, 178–184 (2012).
Castro-Mejia, J. L. et al. Physical fitness in community-dwelling older adults is linked to dietary intake, gut microbiota, and metabolomic signatures. Aging Cell 19, e13105 (2020).
Jackson, M. A. et al. Signatures of early frailty in the gut microbiota. Genome Med. 8, 8 (2016).
Lim, M. Y., Hong, S., Kim, J. H. & Nam, Y. D. Association between gut microbiome and frailty in the older adult population in Korea. J. Gerontol. A Biol. Sci. Med. Sci. 76, 1362–1368 (2021).
Wilmanski, T. et al. Gut microbiome pattern reflects healthy ageing and predicts survival in humans. Nat. Metab. 3, 274–286 (2021).
Claesson, M. J. et al. Composition, variability, and temporal stability of the intestinal microbiota of the elderly. Proc. Natl. Acad. Sci. USA 108, 4586–4591 (2011).
Leite, G. et al. Age and the aging process significantly alter the small bowel microbiome. Cell Rep. 36, 109765 (2021).
Xu, C., Zhu, H. & Qiu, P. Aging progression of human gut microbiota. BMC Microbiol. 19, 236 (2019).
Odamaki, T. et al. Age-related changes in gut microbiota composition from newborn to centenarian: a cross-sectional study. BMC Microbiol. 16, 90 (2016).
Biagi, E. et al. Gut microbiota and extreme longevity. Curr. Biol. 26, 1480–1485 (2016).
Rampelli, S. et al. Shotgun metagenomics of gut microbiota in humans with up to extreme longevity and the increasing role of xenobiotic degradation. mSystems 5, https://doi.org/10.1128/mSystems.00124-20 (2020).
Wu, L. et al. A cross-sectional study of compositional and functional profiles of gut microbiota in Sardinian centenarians. mSystems 4, https://doi.org/10.1128/mSystems.00325-19 (2019).
Wang, N. et al. Enriched taxa were found among the gut microbiota of centenarians in East China. PLoS ONE 14, e0222763 (2019).
Kim, B. S. et al. Comparison of the gut microbiota of centenarians in longevity villages of South Korea with those of other age groups. J. Microbiol. Biotechnol. 29, 429–440 (2019).
Park, S. H. et al. Comparative analysis of gut microbiota in elderly people of urbanized towns and longevity villages. BMC Microbiol. 15, 49 (2015).
Tuikhar, N. et al. Comparative analysis of the gut microbiota in centenarians and young adults shows a common signature across genotypically non-related populations. Mech. Ageing Dev. 179, 23–35 (2019).
La-Ongkham, O., Nakphaichit, M., Nakayama, J., Keawsompong, S. & Nitisinprasert, S. Age-related changes in the gut microbiota and the core gut microbiome of healthy Thai humans. 3 Biotech 10, 276 (2020).
Ma, Y., Liu, X. & Wang, J. Small molecules in the big picture of gut microbiome-host cross-talk. EBioMedicine 81, 104085 (2022).
Rooks, M. G. & Garrett, W. S. Gut microbiota, metabolites and host immunity. Nat. Rev. Immunol. 16, 341–352 (2016).
Topping, D. L. & Clifton, P. M. Short-chain fatty acids and human colonic function: roles of resistant starch and nonstarch polysaccharides. Physiol. Rev. 81, 1031–1064 (2001).
Flint, H. J., Bayer, E. A., Rincon, M. T., Lamed, R. & White, B. A. Polysaccharide utilization by gut bacteria: potential for new insights from genomic analysis. Nat. Rev. Microbiol. 6, 121–131 (2008).
Cummings, J. H., Pomare, E. W., Branch, W. J., Naylor, C. P. & Macfarlane, G. T. Short chain fatty acids in human large intestine, portal, hepatic and venous blood. Gut 28, 1221–1227 (1987).
Martin-Gallausiaux, C., Marinelli, L., Blottiere, H. M., Larraufie, P. & Lapaque, N. SCFA: mechanisms and functional importance in the gut. Proc. Nutr. Soc. 80, 37–49 (2021).
Hron, W. T., Menahan, L. A. & Lech, J. J. Inhibition of hormonal stimulation of lipolysis in perfused rat heart by ketone bodies. J. Mol. Cell Cardiol. 10, 161–174 (1978).
Zhao, Y. et al. Structure-specific effects of short-chain fatty acids on plasma cholesterol concentration in male Syrian hamsters. J. Agric. Food Chem. 65, 10984–10992 (2017).
Sakakibara, S., Yamauchi, T., Oshima, Y., Tsukamoto, Y. & Kadowaki, T. Acetic acid activates hepatic AMPK and reduces hyperglycemia in diabetic KK-A(y) mice. Biochem. Biophys. Res. Commun. 344, 597–604 (2006).
Erny, D. et al. Microbiota-derived acetate enables the metabolic fitness of the brain innate immune system during health and disease. Cell Metab. 33, 2260–2276 e2267 (2021).
Zheng, H. et al. Depletion of acetate-producing bacteria from the gut microbiota facilitates cognitive impairment through the gut-brain neural mechanism in diabetic mice. Microbiome 9, 145 (2021).
Culp, E. J. & Goodman, A. L. Cross-feeding in the gut microbiome: ecology and mechanisms. Cell Host Microbe 31, 485–499 (2023).
Rios-Covian, D., Gueimonde, M., Duncan, S. H., Flint, H. J. & de los Reyes-Gavilan, C. G. Enhanced butyrate formation by cross-feeding between Faecalibacterium prausnitzii and Bifidobacterium adolescentis. FEMS Microbiol. Lett. 362, https://doi.org/10.1093/femsle/fnv176 (2015).
den Besten, G. et al. The role of short-chain fatty acids in the interplay between diet, gut microbiota, and host energy metabolism. J. Lipid Res. 54, 2325–2340 (2013).
Deleu, S., Machiels, K., Raes, J., Verbeke, K. & Vermeire, S. Short chain fatty acids and its producing organisms: an overlooked therapy for IBD? EBioMedicine 66, 103293 (2021).
Panda, S. et al. Short-term effect of antibiotics on human gut microbiota. PLoS ONE 9, e95476 (2014).
Ramirez, J. et al. Antibiotics as major disruptors of gut microbiota. Front. Cell Infect. Microbiol. 10, 572912 (2020).
Fried, L. P. et al. Frailty in older adults: evidence for a phenotype. J. Gerontol. A Biol. Sci. Med. Sci. 56, M146–M156 (2001).
Clegg, A., Young, J., Iliffe, S., Rikkert, M. O. & Rockwood, K. Frailty in elderly people. Lancet 381, 752–762 (2013).
Iglesias, J. E. et al. A probabilistic atlas of the human thalamic nuclei combining ex vivo MRI and histology. Neuroimage 183, 314–326 (2018).
Sordillo, J. E. et al. Association of the infant gut microbiome with early childhood neurodevelopmental outcomes: an ancillary study to the VDAART randomized clinical trial. JAMA Netw. Open 2, e190905 (2019).
Sordillo, J. E. et al. Factors influencing the infant gut microbiome at age 3-6 months: findings from the ethnically diverse vitamin D antenatal asthma reduction trial (VDAART). J. Allergy Clin. Immunol. 139, 482–491.e414 (2017).
Duncan, S. H. et al. Contribution of acetate to butyrate formation by human faecal bacteria. Br. J. Nutr. 91, 915–923 (2004).
Deurenberg, P. Limitations of the bioelectrical impedance method for the assessment of body fat in severe obesity. Am. J. Clin. Nutr. 64, 449S–452S (1996).
Camargo, C. H. F., Bronzini, A., Tolentino, E. S., Medyk, C. & Schultz-Pereira, G. L. Can the CERAD neuropsychological battery be used to assess cognitive impairment in Parkinson’s disease? Arq. Neuropsiquiatr. 76, 145–149 (2018).
Haanpaa, R. M. et al. The CERAD neuropsychological battery in patients with frontotemporal lobar degeneration. Dement Geriatr. Cogn. Dis. Extra 5, 147–154 (2015).
Boets, E. et al. Systemic availability and metabolism of colonic-derived short-chain fatty acids in healthy subjects: a stable isotope study. J. Physiol. 595, 541–555 (2017).
Yamashita, H. et al. Improvement of obesity and glucose tolerance by acetate in Type 2 diabetic Otsuka Long-Evans Tokushima Fatty (OLETF) rats. Biosci. Biotechnol. Biochem. 71, 1236–1243 (2007).
Liu, L., Fu, C. & Li, F. Acetate Affects the Process of Lipid Metabolism in Rabbit Liver, Skeletal Muscle and Adipose Tissue. Animals 9, https://doi.org/10.3390/ani9100799 (2019).
Tolhurst, G. et al. Short-chain fatty acids stimulate glucagon-like peptide-1 secretion via the G-protein-coupled receptor FFAR2. Diabetes 61, 364–371 (2012).
Xiong, Y. et al. Short-chain fatty acids stimulate leptin production in adipocytes through the G protein-coupled receptor GPR41. Proc. Natl. Acad. Sci. USA 101, 1045–1050 (2004).
Cuche, G., Cuber, J. C. & Malbert, C. H. Ileal short-chain fatty acids inhibit gastric motility by a humoral pathway. Am. J. Physiol. Gastrointest. Liver Physiol. 279, G925–G930 (2000).
Perry, R. J. et al. Acetate mediates a microbiome-brain-beta-cell axis to promote metabolic syndrome. Nature 534, 213–217 (2016).
Kondo, T., Kishi, M., Fushimi, T., Ugajin, S. & Kaga, T. Vinegar intake reduces body weight, body fat mass, and serum triglyceride levels in obese Japanese subjects. Biosci. Biotechnol. Biochem 73, 1837–1843 (2009).
Fernandes, J., Vogt, J. & Wolever, T. M. Intravenous acetate elicits a greater free fatty acid rebound in normal than hyperinsulinaemic humans. Eur. J. Clin. Nutr. 66, 1029–1034 (2012).
van der Beek, C. M. et al. Distal, not proximal, colonic acetate infusions promote fat oxidation and improve metabolic markers in overweight/obese men. Clin. Sci. 130, 2073–2082 (2016).
Li, C. et al. Gut microbiome and metabolome profiling in Framingham Heart Study reveals cholesterol-metabolizing bacteria. Cell 187, 1834–1852.e1819 (2024).
Oldendorf, W. H. Carrier-mediated blood-brain barrier transport of short-chain monocarboxylic organic acids. Am. J. Physiol. 224, 1450–1453 (1973).
Rocamora, N., Welker, E., Pascual, M. & Soriano, E. Upregulation of BDNF mRNA expression in the barrel cortex of adult mice after sensory stimulation. J. Neurosci. 16, 4411–4419 (1996).
Tanabe, J. et al. Effects of alcohol and acetate on cerebral blood flow: a pilot study. Alcohol Clin. Exp. Res. 43, 2070–2078 (2019).
Tanabe, J. et al. Effects of acetate on cerebral blood flow, systemic inflammation, and behavior in alcohol use disorder. Alcohol Clin. Exp. Res. 45, 922–933 (2021).
Forte, N. et al. The short-chain fatty acid acetate modulates orexin/hypocretin neurons: a novel mechanism in gut-brain axis regulation of energy homeostasis and feeding. Biochem. Pharm. 226, 116383 (2024).
Erny, D. et al. Host microbiota constantly control maturation and function of microglia in the CNS. Nat. Neurosci. 18, 965–977 (2015).
Rosell-Cardona, C. et al. Acute stress enhances synaptic plasticity in male mice via a microbiota-dependent mechanism. Neuropharmacology 273, 110434 (2025).
Badar-Goffer, R. S., Bachelard, H. S. & Morris, P. G. Cerebral metabolism of acetate and glucose studied by 13C-n.m.r. spectroscopy. A technique for investigating metabolic compartmentation in the brain. Biochem. J. 266, 133–139 (1990).
He, Q. et al. Acetate enables metabolic fitness and cognitive performance during sleep disruption. Cell Metab. 36, 1998–2014 e1915 (2024).
Wen, C. et al. Acetate attenuates perioperative neurocognitive disorders in aged mice. Aging 12, 3862–3879 (2020).
Govindarajan, N., Agis-Balboa, R. C., Walter, J., Sananbenesi, F. & Fischer, A. Sodium butyrate improves memory function in an Alzheimer’s disease mouse model when administered at an advanced stage of disease progression. J. Alzheimers Dis. 26, 187–197 (2011).
Xu, M. et al. Acetate attenuates inflammasome activation through GPR43-mediated Ca(2+)-dependent NLRP3 ubiquitination. Exp. Mol. Med. 51, 1–13 (2019).
Liu, J. et al. Neuroprotective effects of Clostridium butyricum against vascular dementia in mice via metabolic butyrate. Biomed. Res. Int. 2015, 412946 (2015).
Hoyles, L. et al. Regulation of blood-brain barrier integrity by microbiome-associated methylamines and cognition by trimethylamine N-oxide. Microbiome 9, 235 (2021).
Capucho, P. & Brucki, S. M. D. Judgment in mild cognitive impairment and Alzheimer’s disease. Dement. Neuropsychol. 5, 297–302 (2011).
Allaire, J. C. & Marsiske, M. Everyday cognition: age and intellectual ability correlates. Psychol. Aging 14, 627–644 (1999).
Duke, L. M. & Kaszniak, A. W. Executive control functions in degenerative dementias: a comparative review. Neuropsychol. Rev. 10, 75–99 (2000).
Baddeley, A. D. Working Memory. (Clarendon Press, Oxford University Press, 1986).
Stuss, D. T. & Benson, D. F. The Frontal Lobes. (Raven Press, 1986).
Kolb, B. & Whishaw, I. Q. Fundamentals of Human Neuropsychology. 6th edn, (Worth Publishers, 2009).
Fuster, J. M. The Prefrontal Cortex. Fifth edition. edn, (Elsevier/AP, 2015).
Yang, W., Tipparaju, S. L., Chen, G. & Li, N. Thalamus-driven functional populations in frontal cortex support decision-making. Nat. Neurosci. 25, 1339–1352 (2022).
Jovel, J. et al. Characterization of the gut microbiome using 16S or shotgun metagenomics. Front. Microbiol. 7, 459 (2016).
Ranjan, R., Rani, A., Metwally, A., McGee, H. S. & Perkins, D. L. Analysis of the microbiome: advantages of whole genome shotgun versus 16S amplicon sequencing. Biochem. Biophys. Res. Commun. 469, 967–977 (2016).
Wu, G. D. et al. Linking long-term dietary patterns with gut microbial enterotypes. Science 334, 105–108 (2011).
Vandeputte, D. et al. Stool consistency is strongly associated with gut microbiota richness and composition, enterotypes and bacterial growth rates. Gut 65, 57–62 (2016).
Acknowledgements
The phase 1 study was supported by a grant CORPG3J0371 from Chang Gung Memorial Hospital. The phase 2 study was supported by grant XMRPG3L102 from Chang Gung Memorial Hospital, sponsored by Wang Chang Gung Charity Trust. The authors acknowledge the data collection, data management, and information technology services, based on the Structured Research and Medical Informatics Cloud (SRMIC) platform system, provided by the Clinical Trial Center, Chang Gung Memorial Hospital, Linkou, Taiwan, R.O.C., with support by the Ministry of Health and Welfare under Grant No. MOHW110-TDU-B-212-124005. The funders had no role in study design, data collection and analysis, preparation of the paper, or the decision to publish.
Author information
Authors and Affiliations
Contributions
T.Y.S. and C.H.T. conceived and designed the study. T.Y.S., C.H.T., J.T.F., C.H.C., Y.M.Y., M.L.C., C.J.L., A.M.C.W., S.N.L., and C.P.L. acquired, analyzed, or interpreted data. T.Y.S. and C.H.T. drafted the manuscript. All authors critically revised the manuscript for important intellectual content. T.Y.S. and C.H.T. performed statistical analysis. J.T.F. obtained funding.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Communications Medicine thanks Theis Lange and Anja Lok for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Siow, T.Y., Wong, A.MC., Fang, JT. et al. Plasma acetic acid mediates the relationship between gut microbiome and various health measures in older adults. Commun Med (2026). https://doi.org/10.1038/s43856-026-01566-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s43856-026-01566-x