Abstract
Modern maternity care lacks sufficient labor support, with nurses dedicating only 6-10% of their time to labor assistance, far below the 53% mothers expect. Given the need for continuous support, doula-trained non-clinical birth workers have gained prevalence. This scoping review examines the impact of doulas across the pregnancy care continuum, including prenatal, pregnancy, and postpartum phases. A systematic search across PubMed, Scopus, EMBASE, CINAHL, Cochrane Review, and Cochrane Central identified peer-reviewed articles (2000-2023) using Boolean search terms. A total of 23 studies met the inclusion criteria. Findings suggest that doula support improves delivery outcomes by reducing cesarean rates, preterm births, labor duration, and pain, while enhancing breastfeeding initiation. One study reported longer hospital stays, but overall, doulas appeared to lower mothers’ stress and anxiety. Expanding doula access may improve maternal and child health outcomes. Future research should explore policy integration and behavior change impacts to support evidence-based maternal healthcare.
Similar content being viewed by others
Introduction
Doulas may be an important part of assisting pregnant people throughout the pregnancy care continuum, particularly during childbirth. Doulas are non-clinical support professionals trained to provide physical, emotional, and informational support before, during, and after labor and birth. The role of the doula was revolutionized in the twentieth century as births were relocated from home to hospital settings1,2. There are various types of doulas such as prenatal doula (who assist during pregnancy), labor and birth doula (who provide support during childbirth), postpartum doula (who support individuals after delivery), antepartum doula (who help with high-risk pregnancies requiring bed rest), community-based doula (who often serve marginalized communities), abortion doula (who support individuals undergoing abortion), and a full-spectrum doulas (who provide support across a range of reproductive health experiences, including miscarriage, abortion, birth, and postpartum care).
Doulas provide more than just handholding and a soothing presence during labor; they often engage with their clients’ multiple times throughout the pregnancy care continuum (from pregnancy to postpartum)3,4. This may include emotional comfort, non-clinical physical assistance, and educational information, which may help mothers navigate through pregnancy and childbirth with greater confidence and less anxiety5,6,7. Doulas can provide constant support, advocating for individual desires, helping with non-medical pain management methods, and enhancing the overall satisfaction of the birthing process8,9. During the postpartum phase, doulas may assist with breastfeeding, facilitate physical and mental recuperation, and link families with essential resources, such as healthcare experts and support groups10,11.
Previous research has determined individuals value and benefit from having a support person with them throughout labor and delivery12,13,14. Nevertheless, many report unsatisfactory birth experience due to lack of continuous support, often described in terms of emotional distress, unmet expectations, or feelings of abandonment during childbirth. In the United States, an overwhelming 98.4% of births occur in hospitals15, leading to challenges in providing continuous labor support due to the strain on the healthcare system12. Additionally, overburdened clinical staff and limited availability of healthcare professionals such as midwives and registered nurses can hinder the provision of one-on-one care during labor. These challenges may contribute to poorer maternal and infant outcomes16. In recent years, doula care has remained an underutilized resource, suggesting a significant opportunity for further integration into standard prenatal, childbirth, and postpartum care practices17,18,19.
Research has suggested mixed results regarding the impact of doula support on pregnancy and birth outcomes, highlighting the complexity of assessing their role in maternal care. Some studies suggest that receiving support from a doula during pregnancy and after childbirth can enhance client’s confidence in managing their pregnancy and reduce stress levels, leading to improved birth outcomes1,13,20,21. However, other studies have found no significant impact of doulas on these outcomes22,23,24.
The aim of this scoping review was to identify and synthesize existing evidence regarding the roles, practices, and impact of doulas across prenatal, labor and delivery, and postpartum stages of the pregnancy care continuum. While doulas may also support people undergoing abortion or miscarriage, this review focusses specifically on birth-related and postpartum outcomes. Findings from this review seek to provide valuable insights to healthcare providers, policymakers, and expectant parents by analyzing a range of research findings and examining the effects of doula on different populations and outcomes.
Results
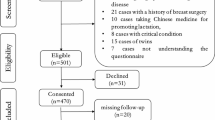
A total of 897 articles were found across six databases. A total of 130 duplicates were eliminated, resulting in a remaining count of 765 articles. Following the application of inclusion and exclusion criteria, a total of 115 articles remained after the initial screening process. In addition, when examining the complete text, 23 articles were chosen for the scoping review (Fig. 1).
From: Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group (2009). Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med 6(6): e1000097. doi:10.1371/journal.pmed1000097. For more information, visit www.prisma-statement.org. The flow diagram of the review screening process shows the number (n) of studies that were originally identified, screened, and assessed for eligibility, as well as the reasons for exclusions.
Characteristics of included studies
This scoping review incorporated studies from various countries. Among the included studies, 13 studies were from the United States, consisting of 6 with a retrospective cohort design, 3 used a qualitative study design, 2 employed a mixed methods study, 1 used a randomized controlled trial (RCT), and 1 with a non-experimental study design. There were 2 studies conducted in Brazil (1 mixed methods study; 1 cross-sectional study), 1 in the United Kingdom (a qualitative study), and 1 each in Canada (RCT), Mexico (retrospective cohort design), Iran (qualitative study), and Australia (mixed methods study). Further, several incorporated racially and ethnically diverse samples. For instance, multiple U.S.-based studies1,5,23,25,26,27 focused on Medicaid recipients, Black and Latina women, or women from socioeconomically disadvantaged backgrounds. Some studies also centered on incarcerated women24,28 or adolescent births29, representing vulnerable and diverse populations. The studies focused on doulas’ roles in pregnancy care continuum before pregnancy, during, and post-partum. A total of 2 studies focused on before pregnancy, 10 studies focused on during pregnancy, 1 study on post-partum, and 10 studies were a mix of both during pregnancy and post-partum. The sample participants in the scoping review ranged from 13 to 279,008 (Table 1).
Doulas-impact on mode of delivery
A total of 13 studies investigated the effect of doulas on the mode of delivery and they yielded mixed results, ranging from nine positive16,25,26,29,30,31,32,33,34 to one neutral8 to three with negative impacts22,24,35. Most studies indicated a decreased occurrence of cesarean births, thereby increasing the chances of vaginal delivery and having positive labor outcomes for both the mother and the baby16,25,26,29,30,31,32,34. This body of research highlights not only a decrease in the rate of cesarean deliveries but also an increased prevalence of non-instrumental vaginal births25,26,29,31,32,33,34. Further, a mixed-method study suggested that doulas may also empower clients and normalize the delivery process, potentially contributing to positive outcomes in promoting vaginal deliveries30. However, one study showed no significant differences in cesarean delivery rates8.
Three studies indicated a negative impact of doulas on the mode of delivery, suggesting a higher level of cesarean deliveries in their care. For example, in a study by Hodgon et al. (2017), the care group was associated with a lower rate of spontaneous vaginal delivery (61% vs 72%) and higher rates of a caesarian section (25% vs 20%) when compared to the comparison group22. Similarly, another study indicated that the doula-supported group had a higher rate of cesarean delivery compared to the standard-of-care group (27.6% vs 14.6%)24. Furthermore, Byskog et al. (2020) suggested an increased adjusted odds ratio (aOR 1.43) of cesarean delivery for specific groups of immigrants women35.
Doula-based delivery support
Several studies shed light on the role of doula support in maternal care, focusing on labor induction, pain management, and hospital stays.
Labor induction
Five studies focused on labor induction, where four studies had a positive impact23,33,34,35, and one study had a mixed impact29. The study by Kozimannil (2013b) revealed that women with doula support were more inclined to use nonmedical techniques for labor induction, with a significantly higher odds ratio (aOR 3.03)23. Additionally, Nommsen-Rivers et al. (2009) found that women under doula care often experienced shorter second stages of labor, indicating a possible efficiency in labor progression with doula support33. Moreover, research by Byrskog et al. (2020) in Sweden suggested a positive relationship between doula support and natural labor induction. In this study, community-based doula (CBD) support was defined as culturally and linguistically concordant care provided by trained lay birth workers from the same community, with a specific focus on supporting migrant women during labor and birth. For migrant nulliparous women, community-based doula support was associated with an increased odds ratio (aOR 1.38) of natural labor induction, potentially indicating doulas’ support in managing the challenges of induced labor35. A study by Trueba et al. (2000) observed a markedly lower usage of Pitocin (oxytocin) in the doula-supported group (42%) compared to the standard care group (96%). The study also suggests that the doula-supported group had a lower mean labor length than its counterpart (14 h 51 min vs 19 h 38 min)34. Also, Everson et al. (2018) reported ~43% of women gave birth without pharmacological induction or augmentation assistance, indicating a possible role for doulas in reducing reliance on medical induction procedures. On the other hand, the same study reported that a significant proportion of women (30%) relied on pharmacological methods (e.g., prostaglandins, synthetic oxytocin, misoprostol) to initiate labor, with 35% requiring augmentation via synthetic oxytocin29.
Pain management
Six studies focused on doula support of pain management using natural and pharmacological interventions during labor. Four studies had a positive impact23,31,32,34 one mixed impact35 and one negative impact29. Research by Fernandes et al. (2019) found that doula support was associated with increased use of non-pharmacological pain relief methods (OR 9.68)31. Furthermore, Hans et al. (2018) suggested that those in the doula-led intervention group groups were less likely to utilize pain medication during labor (OR 0.47)32. Also, Kozhimannil et al. (2013b) found over 70% of women used nonmedical pain management23. Additionally, another study indicated that a doula-supported group received fewer epidurals compared to the control group (8% vs 32%) (Trueba et al., 2000)34. Similarly, Byrskog et al. (2020) study found that community-based doula support was linked to reduced use of pain relief methods for nulliparous women, especially in cases of epidural and bath usage (aOR 0.64, respectively). However, parous women with doula support had increased odds of labor induction (aOR 1.38)35. Further, according to the study by Everson et al. (2018), in the doula support program, approximately 50% of pregnant women received intravenous pain medications (epidural anesthesia) compared to the national average29.
Hospital stays
Only one study reported on the impact of doulas on hospital stays after childbirth. Byrskog et al. (2020) associated community-based doula support with longer hospital stays ( > 48 h) for parous women and longer post-birth hospital stays (OR 1.19) for nulliparous women35.
Doulas’ support on child outcomes
The data from various studies provide insights into several key child outcomes which include gestational period, birth weight, child mortality and morbidity, and breastfeeding initiation.
Gestational period. Five studies have shown a reduced rate of preterm birth with doula support. For several studies, approximately 5% of women gave birth before completing 37 weeks of gestation8,22,24,29. The study conducted by Kozhimannil et al. (2013a) emphasized a reduced incidence of preterm delivery, approximately 6.1%, among births who received doula support in comparison to national Medicaid participants25. Additionally, the Everson et al. (2018) study reported that 92% of neonates were full-term at birth and 3.1% were post-term in the doula support program ( > 42 weeks of gestation) compared to the national average29.
Birth weight
Four studies focused on birth weight, including three studies that had a positive effect1,8,29 and one study had a mixed impact24. According to Everson’s (2018) research, the utilization of doulas was found to be associated with a low birth weight (LBW) ( < 2500 g/<5.5pounds) rate of merely 10% among newborns, whereas approximately 7% of neonates were classified as macrocosmic ( > 4000 g;>8.8 pounds)29. Another study conducted by Gruber et al. (2013) indicated that moms who did not receive assistance from a doula were four times more prone to give birth to LBW infants, accompanied by fewer difficulties, compared to mothers who were aided by a doula1. Further, a study by Thomas et al. (2017) suggested being enrolled in the doulas-based intervention led to a lower percentage of LBW (6.5%) vs the comparison group (11.1%)8. However, one study found no significant differences in LBW between the infants born to women in prison having doula support (3.9%) when compared with the control group (5.7%)24.
Child morbidity and mortality
Out of two studies that focused on child morbidity, one also discussed the issue of mortality. Everson et al. (2018) suggested that in a national sample of doula-supported adolescent births, ~9% of the infants experienced adverse health concerns immediately after birth, and 5.6% were admitted to the neonatal intensive care unit (NICU). This study also reported a total of 10 stillbirths, resulting in a fetal fatality rate of 5.27 per 1000 births29. Another study by Shlafer et al. (2021), examined the health outcomes of infants born to incarcerated women and suggested that women who received doula services found that infants had a median APGAR (Appearance, Pulse, Grimace, Activity, and Respiration) score of 9, with approximately 6% of instances resulting in NICU hospitalization compared to a comparison group and suggested no significance differences24.
Breastfeeding initiation
Eight studies discussed breastfeeding initiation with five studies highlighting the positive impact1,28,32,33,36 and three studies with a negative impact22,30,32 of doula support on breastfeeding initiation. The Gruber et al. (2013) study, which included a sample of 248 women, suggested that approximately 90% of adult participants who received doulas support initiated breastfeeding1, compared to a lower rate in the control group. Another study by Hans et al. (2018) indicated that mothers in the doula’s intervention group were more likely to initiate breastfeeding while in the hospital (OR 1.67), but breastfeeding was not sustained over time32. Similarly, another study suggested that doula care was associated with an earlier onset of lactogenesis within 72 h of postpartum and the infant sucked well on day 3. Doula care was also associated with a high prevalence of breastfeeding at six weeks when compared with its counterpart (89% vs 40%)33. However, in a study by Hodgson et al. 2017, no significant differences were observed between the doula’s group (84%) and the control group (78%)22.
A mixed-method study conducted by Diezel et al. (2013) indicated pregnant women valued the care provided by student doulas about breastfeeding in five domains, namely physical, emotional, support person, and usefulness30. Furthermore, another mixed-method study by Shlafer et al. (2018) identified that 69% of study participants discussed breastfeeding at least one time with their doula. Women who discussed breastfeeding with their doulas were seven times more likely to initiate breastfeeding than women who did not. The qualitative inquiry identified three overarching themes from the doulas’ narratives about breastfeeding initiation among incarcerated women: breastfeeding benefits for the mother-child relationship, real or perceived barriers to breastfeeding, and the role of the doula in supporting mothers’ breastfeeding initiation28. Moreover, a qualitative study (Ganon et al., 2022) suggested that the involvement of doulas in the perinatal period would help breastfeeding initiation36.
Doulas as maternal mental and well-being support
The assistance provided by doulas and the benefits they offer women during pregnancy and childbirth has been associated with a favorable impact on women’s mental health and maternal and child support.
Mental health
Only one study Falconi et al. (2022), found women who received doula care during pregnancy had 57.5% lower odds of postpartum depression/anxiety (OR 0.42)16.
Maternal and child support. Nine studies discussed maternal and child support which included nine with a positive impact8,27,30,32,37,38,39 and two with a mixed impact30,36.
An RCT study by Hans et al. (2018) suggested that doula-supported mothers were observed to be more likely to attend childbirth preparation classes (50% vs 10%) and more likely to utilize car seats at three weeks postpartum (97% vs 93%). Qualitative studies highlighted the critical function of doulas in caring for pregnant mothers32. Studies by Diezel et al. (2013), McGarry (2016), McLeish (2019), and Safarzadeh (2018), collectively highlighted the beneficial role of doulas in providing valuable information, fostering trust, empowerment, and enhancing self-esteem among pregnant women. These findings indicated that doula support positively influenced maternal confidence, decision-making abilities, and mental well-being30,37,38,39. Further, Kozhimannil et al. (2016) found that doulas positively influenced pregnant women’s access to healthcare services and improved the quality of care received during pregnancy and childbirth, highlighting the importance of doula support in addressing health literacy and social support needs27. Similarly, Thomas et al. (2017) demonstrated the positive impact of the By My Side Birth Support Program on women from low socioeconomic communities, with high rates of infant mortality. The program, which provided doula support, received high satisfaction rates from participants, with nearly all women expressing willingness to recommend the program or use it again in future pregnancies8.
While Gannon’s study (2022) emphasized the positive role of doulas in minimizing stigma and providing support for pregnant women with opioid use disorder, it did not explicitly address any potential challenges or limitations associated with doula support in this context36. Diezel et al. (2013) highlighted the varied abilities and positive aspects of doula support, including their contributions to interprofessional teamwork and support for vaginal deliveries. However, this study did not delve into any negative aspects or limitations of doula involvement in maternity care30.
Discussion
This scoping review aimed to assess the effects of doulas on pregnancy care by synthesizing findings from various research conducted in diverse regions. In contrast to Sobczak et al. (2023)40, which synthesized 16 studies from high-income countries on perinatal outcomes (cesarean, preterm birth, low birth weight), this review includes 23 studies and examines doula roles across the pregnancy continuum including prenatal, intrapartum, postpartum, and marginalized populations. Using qualitative, mixed-method, and international evidence, it reveals gaps in community-based and policy-driven strategies in addressing structural imbalances and emphasizes behavioral change and maternal mental health. This broader perspective informs health equity and policy.
The study examined four primary end variables, including the impact of doulas on the mode of delivery, their provision of assistance during labor and delivery, their influence on newborn outcomes, and their contribution to maternal well-being. The results exhibited discrepancies, as several investigations indicated favorable outcomes, such as higher occurrences of non-instrumental vaginal deliveries and enhanced birth outcomes. Conversely, other studies demonstrated varied or less significant effects, particularly related to cesarean rates. Doulas have been shown to fulfill a multifaceted function in facilitating labor induction and pain management in the context of childbirth, potentially mitigating the need for medical interventions. Moreover, these investigations were found to be linked with enhanced neonatal outcomes, such as an increased likelihood of full-term births and a decrease in unfavorable prenatal outcomes (e.g., Everson et al., 2018; Gruber et al., 2013; Fernandes et al., 2019)1,29,37. Qualitative research has emphasized the significant importance of doulas in delivering emotional support, mitigating the social stigma mothers may experience with pregnancy, and improving the overall well-being of mothers, especially in difficult situations. In general, doulas have been recognized as useful resources in enhancing mother and newborn outcomes, encompassing the physical and emotional dimensions of pregnancy and labor.
Various studies have indicated a positive effect with increased non-instrumental vaginal deliveries and reduced cesarean rates, while others show mixed results, including no significant differences or increased cesareans for certain groups. The variation in studies on doula’s impact on delivery mode could be due to differences in study design, diverse populations, regional practices, and client preferences. The increased cases of vaginal deliveries could be due to the involvement of enhanced prenatal education regarding childbirth expectations and a heightened sense of empowerment and autonomy throughout the birthing process1,40.
Multiple studies have illuminated the positive aspects of doula support in maternal care, with a specific focus on labor induction and augmentation, as well as its impact on pain relief during childbirth, hospital stays, and breastfeeding16,18,40,41,42. These findings indicate that women who embraced the idea of a doula empowering them to actively shape their childbirth experience, effectively handle their labor, and attain their desired positive and healthy birth outcomes. This may have also acknowledged the potential for enhancing their prenatal health and increasing the chances of a healthy birth by actively engaging in the prenatal activities offered by these programs16,18,40,41,42.
The research articles analyzed in this study generally exhibited favorable neonatal outcomes, with a predominant proportion of newborns being delivered at full term. Despite the fact that a minority of infants were born prematurely or post-term, they exhibited positive outcomes, such as elevated APGAR ratings and decreased admissions to the Neonatal Intensive Care Unit. It is worth noting that there was just one study that specifically examined neonatal mortality, a phenomenon that was shown to be exceptionally uncommon. Taken together, these findings highlight the potential advantages of doula assistance as they offer diverse forms of support to women throughout pregnancy, childbirth, the postpartum period, and other related reproductive health experiences12.
The findings from this scoping review highlight the critical role of doulas in providing emotional support, reducing stigma, and improving maternal and birth outcomes. Doulas play a multifaceted role in maternal care, providing education and emotional support by offering essential information and reassurance to women during pregnancy and postpartum periods. They act as patient advocates, ensuring that individual choices are incorporated into the delivery care plan12. In addition, doulas provide affirmation and advocacy, particularly when women have distressing symptoms that necessitate attention, making a major difference, particularly for populations experiencing marginalization in maternity care. Doulas offer invaluable assistance, helping women navigate the complex systems of social services and healthcare. This is especially helpful for women who are unfamiliar with the system or have complex medical concerns. Throughout the crucial stages of pregnancy and the postpartum period, they guarantee access to essential community resources41.
Also, the scoping review included studies on both privately hired doulas and subsidized or community-based doulas, such as those funded through Medicaid or public health initiatives. Community-based doulas, often working with marginalized populations (e.g., low-income, incarcerated, or immigrant women), provided not only culturally concordant care but also helped address structural barriers such as lack of insurance, transportation, and health literacy27,35. These doulas often serve as essential navigators of the healthcare system and social services, especially for individuals impacted by poverty, systemic racism, and limited access to prenatal education8,32. In contrast, private doulas typically serve clients with higher socioeconomic status who can afford out-of-pocket fees. This distinction underscores the class-based disparities in accessing supportive care and highlights the vital role that publicly funded community-rooted doula models play in mitigating structural inequities in maternal health42,43.
While this review primarily concentrated on short-term birth outcomes, there is a rationale to anticipate that doula support may yield long-term advantages, such as enhancing the postnatal mental health of the mother. We found only one study that had investigated this, and thus, more research is warranted. Additionally, it would be advantageous to investigate the influence of the timing of doula support, whether it occurs before labor, during childbirth, or postpartum. This approach would allow the correlation of specific doula interventions with distinct labor outcomes, further promoting and refining the training of these interventions in doula training programs. Moreover, it would provide valuable insights into the optimal timing for commencing doula support to fully harness its benefits1.
The current study demonstrates several strengths. The researchers utilized comprehensive and systematic search methods under a pre-established methodology. The process of conducting the literature search was carried out with great attention to detail and adherence to a methodical approach. Furthermore, the research underwent rigorous evaluation by two separate groups of two researchers each, ensuring that it remained within the predetermined boundaries and objectives. Furthermore, the study adhered to PRISMA guidelines and conducted a rigorous quality assessment of the studies that were included.
However, the scoping review included only studies that were published in the English language, which may have introduced a bias towards countries where English is spoken and excluded research undertaken in nations where English is not the primary language. This could limit the generalizability of the results, and the findings must be made with caution. Moreover, the inclusion of a restricted number of RCTs in this scoping review restricts the generalizability of the effectiveness of doulas on birth outcomes.
In conclusion, this scoping review has provided valuable insights into the multifaceted roles and potential impacts of doulas in the realm of pregnancy care and maternal well-being. Findings from this review suggest that public investment in community-based doula programs, including expanded Medicaid reimbursement and institutional support, may be an important strategy for addressing health disparities and improving maternal and infant health outcomes in diverse populations. Future research should prioritize rigorous studies, long-term outcome assessments, and cost-effectiveness analyses to better understand the nuanced effects and optimal integration of doulas into pregnancy care. Furthermore, there is a need to also explore the impact of doulas on health behavior change during pregnancy. This will provide a more evidence-based foundation for decision-making in maternal care.
Methods
Study design
A comprehensive scoping review was conducted according to the guide by the Arksey and O’Malley five-stage methodological framework44 (identifying the research questions; identifying relevant studies; study selection; charting the data; collating, summarizing, and reporting the results). In contrast to a systematic review and meta-analysis, the scoping review methodology allows for the collection of a “variety of relevant literature and research employing various methodologies”45. Using examples from empirical investigations, the framework of Arksey and O’Malley allowed flexibility to clarify ideas related to highlighting the scope of evidence on the role of doulas across the pregnancy care continuum on maternal and child health44. The aims of the current project aligned with those established for conducting scoping reviews, include a need to examine the size, span, and nature of research activity involving the impact of doulas on maternal and child health outcomes as well as the purpose of identifying gaps in the existing literature43. The review protocol was registered in the Open Science Framework registry (https://osf.io/hp6fs).
Stage 1: identifying the research question
The primary research question focuses on identifying and evaluating the evidence of doula’s impact on the pregnancy care continuum (before, during, and postpartum).
Stage 2: identify relevant studies
Article searches across the following databases were conducted including PubMed, SCOPUS, EMBASE, CINAHL, Cochrane Review, and Cochrane Central beginning on October 7th, 2022, and ending on March 15th, 2023. The search was limited to articles published in English and published literature between 2000 and 2023.
The search keywords used were a combination of “Doulas” OR “Birth Doula” OR “Postpartum Doula” OR “Antepartum Doula” OR “Abortion Doula” OR “Community-based Doula” OR “Postpartum doula” AND “Pregnancy” OR “Maternity” OR “Postpartum” OR “Prenatal” OR “Antenatal” AND “Outcome” OR “maternal health” OR (“maternal” AND “health”) OR “women’s health” AND “Child” OR “Infant.” To better narrow search results for the current review focus, database choices were limited to those from peer-reviewed sources only (grey literature was not included) and those involving human subjects’ participation46. After the initial search using these parameters, a total of 897 articles were found.
The results were reviewed by the research team to ensure the validity of the search strategy, and any disagreements were resolved by consensus with all research team members. The research team consisted of two PhD-level faculty (DD & KS) and three graduate students (PC, JP & GK) who had previous experience conducting systematic and scoping reviews as well as those specializing in maternal and child health research. Results from each database search were exported to a single library using Rayyan software(https://www.rayyan.ai/), a collaborative online research tool designed to assist with the management of systematic and scoping reviews. Duplicate articles were removed before moving toward the next steps.
Stage 3: study selection
The Preferred Reporting Item for Systematic Review and Meta-Analysis (PRISMA) framework was used to guide title and abstract screening47. Further eligibility criteria were used to ensure that the content of the included articles was relevant to the study’s goal. Abstracts were screened using the following inclusion criteria: (1) articles focusing on the role of doulas, (2) articles focusing on before, during pregnancy, and postpartum, (3) articles that include pregnancy outcomes (low birth weight, reduced cesarean births, and shortened durations of labor) and behavior change (healthy eating, physical activity, early initiation of breastfeeding, cessation of alcohol and smoking), and (4) articles published between 2000 and 2023 to access the current state of knowledge. The exclusion criteria included: (1) textbook chapters, systematic reviews, and grey literature (2) a non-English article; and (3) research articles not focused on doulas and birth outcomes. Two pairs of reviewers, the first four authors, reviewed the titles and abstracts for evidence of inclusion/exclusion criteria as well as duplications. These titles and abstract reviews were split evenly between the two pairs of reviewers (382 and 383 unique records) using the Rayyan intelligent systematic review software. If a review pair did not have consensus based on the title and abstract alone, the study was automatically included in the corpus for a full-text review.
Title and abstract screening were conducted between March 20 and April 10, 2023, followed by full-text screening from April 11 to May 5, 2023. Both pairs of reviewers assessed the full-text articles based on the criteria noted above for title and abstract reviewing. All disagreements between review pairs as well as the final decision about inclusion and exclusion of articles were discussed among all four reviewers when necessary to reach a consensus decision. The PRISMA flow chart was generated to indicate how many full-text articles were excluded and why.
Stage 4: charting the data
To capture relevant information from each study, data tables were created in an Excel spreadsheet. The final list of included studies from the full-text review was uploaded to the Excel spreadsheet by two authors (PC and GK). The extracted data included the following: (1) author, (2) title of the study, (3) publication year, (4) publication type, (5) type of study, (6) abstract screening, (7) study setting, (8) study population, (9) results or main findings and, (10) reported strength and limitations. Data extraction was conducted from May 6 to May 20, 2023.
Stage 5: collating and summarizing and reporting the results
The extracted data were summarized in a narrative report focused on the following outcomes: data capture and database system efficiency, data system utility, and influence on research, statistics, and training. These findings were discussed about the research question and the study’s overall goal. Gap detections were used to identify regions with a lack of research on good data collection procedures and a scarcity of data-on-data captures, such as countries with a scarcity of data-on-data captures.
Outcome measures:
In our scoping review, the following maternal and neonatal outcomes were used for measuring the impact of doulas in the pregnancy care continuum: (1) Doulas-impact on mode of delivery; (2) Doulas-based delivery support; (3) Doulas’ support on the child outcome; and (4) Doulas as maternal mental and well-being support.
Data availability
The dataset generated and analyzed during the current study is available from the corresponding author on reasonable request.
References
Gruber, K. J. et al. Impact of doulas on healthy birth outcomes. J. Perinat. Educ. 22, 49–58 (2013).
Basile, M. R. Reproductive justice and childbirth reform: doulas as agents of social change (Doctoral dissertation, University of Iowa). Iowa Research Online https://doi.org/10.17077/etd.znb7bcm0 (2012).
Dwyer, J. Continuums of reproductive choice: theorizing doula care (Doctoral dissertation, Carleton University). CURVE Repository https://doi.org/10.22215/etd/2012-06971 (2012).
Renteria-Poepsel, G. The role of doulas in enhancing patient-provider communication (Master’s dissertation, Southern Illinois University at Edwardsville). ProQuest Dissertations and Theses [https://www.proquest.com/docview/1728327221 (2015)].
Hans, S. L. et al. Promoting positive mother–infant relationships: a randomized trial of community doula support for young mothers. Infant Ment. Health J. 34, 446–457 (2013).
Breedlove, G. Perceptions of social support from pregnant and parenting teens using community-based doulas. J. Perinat. Educ. 14, 15–22 (2005).
Gilliland, A. L. After praise and encouragement: emotional support strategies used by birth doulas in the USA and Canada. Midwifery 27, 525–531 (2011).
Thomas, M. P. et al. Doula services within a healthy start program: increasing access for an underserved population. Matern. Child Health J. 21, 59–64 (2017).
Rahmati, N. An exploratory study of women’s experiences of fear about childbirth (Doctoral dissertation, University of British Columbia). UBC Theses and Dissertations https://doi.org/10.14288/1.0167295 (2014).
Gilliland, A. L. Beyond holding hands: the modern role of the professional doula. J. Obstet. Gynecol. Neonatal Nurs. 31, 762–769 (2002).
Verbiest, S. et al. Elevating mothers’ voices: recommendations for improved patient-centered postpartum. J. Behav. Med. 41, 577–590 (2018).
Bohren, M. A. et al. Continuous support for women during childbirth. Cochrane Database Syst. Rev. 7 (2017).
Hodnett, E. D. et al. Continuous support for women during childbirth. Cochrane Database Syst. Rev. 7 (2013).
Lunda, P., Minnie, C. S. & Benadé, P. Women’s experiences of continuous support during childbirth: a meta-synthesis. BMC Pregnancy Childbirth 18, 167 (2018).
MacDorman, M. F. & Declercq, E. Trends and state variations in out-of-hospital births in the United States, 2004-2017. Birth 46, 279–288 (2019).
Bohren, M. A. et al. Continuous support for women during childbirth. Cochrane Database Syst. Rev. 7, CD003766. https://doi.org/10.1002/14651858.CD003766.pub6 (2017).
Ogunwole, S. M. et al. Health equity considerations in state bills related to doula care (2015–2020). Women’s. Health Issues 32, 440–449 (2022).
Safon, C. B. et al. Doula care saves lives, improves equity, and empowers mothers. State Medicaid programs should pay for it. Health Aff. Forefront https://doi.org/10.1377/forefront.20210525.295915 (2021).
Lantz, P. M. et al. Doulas as childbirth paraprofessionals: results from a national survey. Women’s. Health Issues 15, 109–116 (2005).
Christopher, G. & Simpson, P. Improving birth outcomes requires closing the racial gap. Am. J. Public Health 104, S10–S12 (2014).
Kozhimannil, K. B. et al. Doula care, birth outcomes, and costs among Medicaid beneficiaries. Am. J. Public Health 103 (2013).
Hodgson, Z. G., Saxell, L. & Christians, J. K. An evaluation of interprofessional group antenatal care: a prospective comparative study. BMC Pregnancy Childbirth 17, 297 (2017).
Kozhimannil, K. B. et al. Use of nonmedical methods of labor induction and pain management among US women. Birth 40, 227–236 (2013b).
Shlafer, R. et al. Maternal and neonatal outcomes among incarcerated women who gave birth in custody. Birth 48, 122–131 (2021).
Kozhimannil, K. B. et al. Doula care, birth outcomes, and costs among Medicaid beneficiaries. Am. J. Public Health 103, e113–e121 (2013).
Kozhimannil, K. B. et al. Potential benefits of increased access to doula support during childbirth. Am. J. Manag. Care 20, e340 (2014).
Kozhimannil, K. B. et al. Disrupting the pathways of social determinants of health: doula support during pregnancy and childbirth. J. Am. Board Fam. Med. 29, 308–317 (2016).
Shlafer, R. J. et al. Intention and initiation of breastfeeding among women who are incarcerated. Nurs. Women’s. Health 22, 64–78 (2018).
Everson, C. L., Cheyney, M. & Bovbjerg, M. L. Outcomes of care for 1,892 doula-supported adolescent births in the United States: The DONA international data project, 2000 to 2013. J. Perinat. Educ. 27, 135–147 (2018).
Diezel, H. et al. The value of care provided by student doulas: An examination of the perceptions of women in their care. J. Perinat. Educ. 22, 39 (2013).
Fernandes, L. M., Mishkin, K. E. & Lansky, S. Doula support among Brazilian women who attended the Senses of Birth health education intervention–a cross-sectional analysis. BMC Pregnancy Childbirth 22, 765 (2022).
Hans, S. L., Edwards, R. C. & Zhang, Y. Randomized controlled trial of doula-home-visiting services: impact on maternal and infant health. Matern. Child Health J. 22, 105–113 (2018).
Nommsen-Rivers, L. A. et al. Doula care, early breastfeeding outcomes, and breastfeeding status at 6 weeks postpartum among low-income primiparae. J. Obstet. Gynecol. Neonatal Nurs. 38, 157–173 (2009).
Trueba, G. et al. Alternative strategy to decrease cesarean section: support by doulas during labor. J. Perinat. Educ. 9, 8–13 (2000).
Byrskog, U., Small, R. & Schytt, E. Community-based bilingual doulas for migrant women in labour and birth–findings from a Swedish register-based cohort study. BMC Pregnancy Childbirth 20, 721 (2020).
Gannon, M. et al. Doula engagement and maternal opioid use disorder (OUD): experiences of women in OUD recovery during the perinatal period. Midwifery 106, 103243 (2022).
McGarry, A., Stenfert Kroese, B. & Cox, R. How do women with an intellectual disability experience the support of a doula during their pregnancy, childbirth and after the birth of their child?. J. Appl. Res. Intellect. Disabil. 29, 21–33 (2016).
McLeish, J. & Redshaw, M. “Being the best person that they can be and the best mum”: a qualitative study of community volunteer doula support for disadvantaged mothers before and after birth in England. BMC Pregnancy Childbirth 19, 21 (2019).
Safarzadeh, A., Shafipour, V. & Salar, A. Expectant mothers’ experiences with lay doulas in maternity units of hospitals in impoverished areas of Iran: a qualitative study. Iran. J. Nurs. Midwifery Res. 23, 43 (2018).
Sobczak, A. et al. The effect of doulas on maternal and birth outcomes: a scoping review. Cureus 15, 5 (2023).
Knocke, K. et al. Doula care and maternal health: an evidence review (Issue Brief No. HP-2022-24). Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health Human Services [https://aspe.hhs.gov/reports/doula-care (2022)].
Safon, C. B. et al. Medicaid reimbursement for doula care: policy considerations from a scoping review. Med. Care Res. Rev. 81, 311–326 (2024).
Daudt, H. M., van Mossel, C. & Scott, S. J. Enhancing the scoping study methodology: a large, inter-professional team’s experience with Arksey and O’Malley’s framework. BMC Med. Res. Methodol. 13, 48 (2013).
Arksey, H. & O’Malley, L. Scoping studies: towards a methodological framework. Int. J. Soc. Res. Methodol. 8, 19–32 (2005).
Peterson, J. et al. Understanding scoping reviews: definition, purpose, and process. J. Am. Assoc. Nurse Pract. 29, 12–16 (2017).
Adams, J. et al. Searching and synthesising ‘grey literature’ and ‘grey information’ in public health: critical reflections on three case studies. Syst. Rev. 5, 164 (2016).
Moher, D. et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int. J. Surg. 8, 336–341 (2010).
Acknowledgements
We would like to thank Monica Maher (librarian) for her help and support in conducting the scoping review search.
Author information
Authors and Affiliations
Contributions
This study was conceptualized and designed by P.C. The literature search and study selection were conducted by P.C., J.P. and G.K., with oversight from D.D. and K.S. Data extraction and charting were performed by P.C. and G.K. The synthesis and interpretation of findings were led by P.C., J.P. and G.K., with input from D.D. and K.S. The manuscript was drafted by P.C. and G.K., while D.D., K.S., P.C., J.P. and G.K. reviewed, revised, and approved the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Chaudhary, P., Rech, J.P., Kumar, G. et al. Role of doulas across the pregnancy care continuum on maternal and child health: a scoping review. npj Womens Health 3, 63 (2025). https://doi.org/10.1038/s44294-025-00109-4
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s44294-025-00109-4