Abstract
By combining AI-assisted topic modelling and community engagement, this study aimed to advance the research landscape for Lewy body dementia (LBD). Despite being the second most common form of dementia, LBD remains under-recognized and under-researched, with greater care partner burden and poorer quality of life compared to other dementias. A multi-stage prioritization process first employed Latent Dirichlet Allocation to analyse global LBD literature (18,615 abstracts, 2006–2023), revealing an evolution from basic pathogenesis studies to advanced neuroimaging and AI applications post-2017 diagnostic guidelines. The subsequent stages involved consultation with the LBD community in Ireland through surveys, public involvement events, and consensus meetings, which identified crucial gaps in multidisciplinary approaches, prevention strategies, quality of life assessment, and palliative care. The study resulted in fifteen priority areas structured around three pillars: transdisciplinary research, lived experience, and education/information, emphasizing the development of effective diagnostic tools, quality of life frameworks, and treatment approaches.
Similar content being viewed by others
Introduction
Lewy body dementia (LBD) represents a clinical paradox – it is the second most common form of dementia worldwide1, accounting for between 15 and 30% of all dementias2,3, yet remains significantly under-recognized, mis-diagnosed and under-researched4,5. Symptoms are highly variable, resulting in significant diagnostic challenges and widespread under recognition.
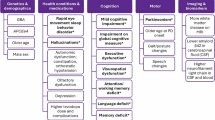
LBD refers to two related diagnoses, Parkinson’s disease dementia (PDD) and dementia with Lewy bodies (DLB)6. LBD is characterized by a complex phenotype consisting of cognitive, non-cognitive, and neurological symptoms. Core symptoms include fluctuating cognitive deficits, sleep disturbances, hallucinations, extrapyramidal symptoms6,7. With these symptoms comes greater dependence earlier in the course of the condition as well as greater care partner burden and distress8, and worse quality of life9 compared to other sub-types of dementia. Consequently, it is surprising that considerably fewer studies are conducted on LBD compared to Alzheimer’s disease (AD) or Parkinson’s (PD)4,10. Economic evidence suggests that LBD constitutes the costliest form of dementia11 compared to other neurodegenerative disorders due to its complex symptomatology and care needs.
Based on global statistics, ~7000–10,000 people are living with LBD in Ireland, with less than 5% receiving a formal diagnosis12. Recognition of LBD in Ireland remains significantly limited by both professional and public awareness, leading to delays in diagnosis and misdiagnoses. Furthermore, treatment studies for LBD in Ireland are sparse, lagging other countries, for example, the UK or US where LBD is starting to receive greater attention13.
Research prioritization studies are crucial for conditions like LBD because they inform priority setting of scarce research resources to areas where they can have the most significant impact. Furthermore, these studies foster collaboration among researchers, healthcare professionals, and patient advocacy groups, creating a more cohesive approach to addressing the unique challenges of this condition.
To date, two studies have been conducted on setting research priorities for LBD9,14. Armstrong, Gamez9 employed a semi-structured questionnaire asking people living with LBD and their care partners to select their top research priorities. Similarly, Holden, Bedenfield14 conducted a web-based survey of people with LBD and their care partners. While these two studies provide valuable insights within the US context, their applicability to other settings warrants confirmation, whether the identified priorities align with or differ from those in other global contexts. Additionally, traditional methods of priority setting, such as surveys and questionnaires, have limitations in capturing the complexity and variability of LBD symptoms. To address these limitations, we recognized the need for an innovative approach that leverages the power of emerging artificial intelligence (AI) to analyse large datasets and identify patterns that may not be apparent through traditional methods.
This study pioneers a novel approach to research priority setting, integrating AI topic modelling with Irish-focused community engagement. While grounded in the Irish healthcare context—where LBD research infrastructure is in its early stages —we aim to: (1) analyse the global LBD research landscape and its evolution since the 2017 diagnostic guideline updates, contextualizing Ireland’s position within broader scientific trends; (2) identify Ireland-specific gaps in LBD research and care through stakeholder-driven prioritization; and (3) develop a national research agenda that addresses these local priorities while offering insights for regions facing similar challenges.
Results
AI-assisted analysis of the global LBD research
A total of 18,615 research abstracts were retrieved across two periods: 9821 from 2006 to 2017 and 8794 from 2018 to 2023. After removing duplicates, the abstracts were organized into 16 topics representing common research themes, with eight topics for each period. The intertopic distance maps of topics are displayed in two-dimensional space in Fig. 1. All topics were similar in size, meaning that a similar percentage of abstracts were assigned in each topic.
a shows the intertopic distance map for the period 2006–2017, while b displays the map for 2018–2023. Each point represents a topic, and the distance between points reflects the similarity between topics; closer points indicate more similar topics.
Figure 2 presents a bar chart illustrating the most salient words associated with Topic 1. For a comprehensive overview, details on the top 30 words for each topic, ranked by relevance, can be found in Supplementary Tables 1–4. Table 1 provides a description of all 16 topics across both time periods (2006–2017 and 2018–2023), along with the number of documents assigned to each topic. Each document was assigned to the topic with the highest probability of representing its content.
a presents a bar chart of the most salient words for λ = 0.6, and b shows the results for λ = 1. In each chart, blue bars represent the overall frequency of each term in the dataset, while red bars indicate the estimated frequency of those terms within the specific topic. When a red bar completely overlaps a blue bar, the term is almost exclusive to the selected topic.
Throughout both periods, research consistently explored the genetic factors influencing LBD, particularly mutations like GBA and LRRK, and their impact on disease progression and clinical manifestations. The role of alpha-synuclein in LBD pathogenesis remained central, with ongoing investigations into how its aggregation affects neuronal function and potential therapeutic interventions. Additionally, the relationship between LBD and comorbid conditions such as PD and AD was recurrently examined.
However, the period from 2018 to 2023 marked a shift towards integrating advanced technologies and methodologies. There was an increase in the use of imaging techniques such as MRI and EEG to study cortical connectivity and brain changes, as evidenced by the emergence of Topic 7 in the 2018–2023 period (740 documents, 9.9% of total terms) which specifically focused on ‘cortical connectivity changes in patients with DLB using MRI and EEG data’ and ‘advanced machine learning models.’ No equivalent neuroimaging-focused topic existed in the 2006–2017 period. Research also expanded to include the impact of sleep disturbances on mortality in LBD patients, analysing long-term data to establish critical risk factors and intervention points. Furthermore, studies began exploring deep brain stimulation as a treatment for apathy in LBD patients with comorbid PD, aiming to improve quality of life and cognitive function. This period also saw an emphasis on using AI and machine learning to enhance diagnostics and patient care, with Topic 5 (1147 documents, 12.1% of total terms) specifically mentioning ‘the integration of technology and artificial intelligence in patient care’ and Topic 7 (740 documents, 9.9% of total terms) highlighting ‘advanced machine learning models’ for studying brain connectivity. These AI-focused approaches were not present as distinct research themes in the 2006–2017 period.
Community engagement and priority setting
Step 1: Literature review of research priorities. The search strategy yielded 590 unique references. Of these, 106 underwent full-text review, with 16 selected for data extraction (refer to Supplementary Fig. 1), including five priority setting exercises (Table 2).
From 16 papers, a list of 39 research priority questions was derived, which was then refined through an iterative process to 19 preliminary research priority questions (refer to Supplementary Table 5).
Step 2: Prioritization survey. In total, 49 participants completed the survey, including 15 people with lived experience (people living with LBD (n = 3) or their care partners (n = 12)), 27 healthcare professionals, and seven researchers (refer to Supplementary Table 6).
The highest research priority, with 44 responses, was to develop effective tools for identifying and diagnosing LBD, such as scans or blood tests. Following closely, with 43 responses, was the need to conduct trials focused on the safety, effectiveness, and cost of new treatments for LBD. The third priority, with 40 responses, emphasized the development of non-medication treatments aimed at managing symptoms and improving quality of life through approaches like nutrition, exercise, and therapy.
Other priorities included exploring the development and causes of LBD (34 responses) and establishing key metrics for tracking treatment success and disease progression (32 responses). Additionally, there was a call to investigate potential indicators of LBD through medical tests (31 responses) and to create systems for coordinated care among healthcare professionals (31 responses). The results also indicated a desire to understand the typical progression of LBD and factors influencing it (30 responses) and to develop support resources available at the point of diagnosis (30 responses). Lastly, investigating risk factors for developing LBD, such as genetics and lifestyle, received 29 responses (refer to Supplementary Table 7).
The analysis of additional research priorities suggested by participants revealed seven topics that had not been previously identified in the literature. These priorities included exploring the connections between LBD and mental health, gaining a deeper understanding of LBD symptoms and clinical manifestations through observational studies, and comprehending the unique lived experiences of people with LBD compared to other dementia subtypes.
Moreover, there was a strong emphasis on understanding the impact of LBD on the quality of life for both those living with the disease and their care partners. Participants highlighted the importance of recognizing early symptomatic signs to encourage timely medical consultation, exploring various care pathways, and conducting longitudinal studies. Establishing a comprehensive data cohort in Ireland was deemed essential for facilitating such longitudinal research.
Step 3: Public and Patient Involvement (PPI) event. The priorities identified by stakeholders during the PPI event closely aligned with the survey results. All attendees agreed with the established priorities and their wording. However, they collectively felt that the need for transdisciplinary research should be added to the list.
Step 4: Development of focused research agenda. A consensus emerged around three key pillars relevant to all prioritized topics: (1) transdisciplinary research, (2) lived experience, and (3) education and information. These pillars intersect with all identified priorities and collectively create a matrix that summarizes the research strategy.
Step 5: Final consensus meeting. Based on the prioritization survey, PPI feedback and consensus workshop, the final list was established, comprising 15 priorities cross-cutting three pillars of (1) transdisciplinary research, (2) lived experience, and (3) education and information (see Box 1).
Discussion
The aims of this research were to: (1) understand the global progress of LBD research and how research has evolved over a 17-year period; (2) identify research gaps through community-driven prioritization; and (3) develop a research strategy that outlines how to address these priorities moving forward.
Between 2006 and 2017, the primary research focus was on disease pathogenesis, notably α-synuclein and mechanisms to mitigate protein aggregation (Topic 1: 1798 documents, 16.7% of total terms). Studies also explored cerebrospinal fluid biomarkers and amyloid imaging using PET scans (Topic 5: 1004 documents, 12.5% of total terms). Additional research areas included the impact of co-morbid Alzheimer’s disease on phenotype and prognosis (Topic 2: 1662 documents, 13.6% of total terms), and investigations into sleep disturbances and hallucinations—excluding REM behavior sleep disorder—and their links to motor functions and treatment options (Topic 6: 639 documents, 11.3% of total terms). This period marked an exploratory phase in understanding clinical phenotypes, as opposed to what are now recognized as core symptoms. Notably absent were studies on supportive symptoms identified post-2017.
From an etiological perspective, research covered genetic mutations and cardiac imaging techniques (Topic 8: 910 documents, 9.7% of total terms), and medical comorbidities like the link between diabetes and the risk of developing DLB in older women (Topic 7: 1050 documents, 10.7% of total terms). Discussions on neuroimaging, treatment strategies, and clinical diagnosis of DLB, particularly through systematic reviews, were prevalent (Topic 3: 1581 documents, 12.8% of total terms).
Conversely, there was limited inclusion of patient and care partner perspectives in defining research priorities, as well as minimal focus on quality of life frameworks integrating psychosocial, sensory, or non-pharmacological dimensions. Notably, only Topic 5 in the 2018–2023 period (1147 documents, 12.1% of total terms) specifically addressed ‘care and intervention strategies’ and ‘the needs of people with LBD, the role of caregivers, and the impact of healthcare and support systems.’ No dedicated topics in the 2006–2017 period focused primarily on patient perspectives or quality of life measures. This limited focus on patient-centered research contrasts sharply with the predominance of biomedical topics. For example, in the 2006–2017 period, Topic 1 (alpha-synuclein pathogenesis) comprised 16.7% of total terms (1798 documents), while in 2018–2023, Topics 1 and 2 combined (molecular mechanisms and sleep-mortality associations) represented 33% of all abstracts (3451 documents). This analysis shows that patient-reported outcomes, caregiver experiences, and quality of life measures were largely absent as primary research foci until the most recent period, and even then, represented only a small fraction of the literature. This evidence strongly supports the rationale for our community-identified priorities emphasizing lived experience (Pillar 2) and the need for more patient-centered research approaches.
From 2018 to 2023, research on LBD pathogenesis remained paramount but expanded from a primary focus on α-synuclein-driven neurodegeneration to include mitochondrial dysfunction and specific mechanisms such as oxidative stress (Topic 1: 1711 documents, 16.6% of total terms). Studies also explored shared genetic traits and co-pathology with other disorders, like frontotemporal and vascular dementia, and ALS. The period saw advanced investigations into specific genetic variants like GBA and APOE as potential biomarkers (Topic 6: 464 documents, 10% of total terms), along with more sophisticated and multimodal neuroimaging techniques (Topic 7: 740 documents, 9.9% of total terms), signaling a shift from lesion-based to network-based disease conceptualization. Clinical discussions broadened to include prodromal DLB and MCI-LB, with increased mention of DLB over LBD, reflecting refined diagnostic criteria and enhanced phenotyping. However, terminology confusion persisted, such as in “PD with DLB.” In addition, research was less focused on phenotypic commonalities and differences between LBD and other types of dementia. This shift may illustrate the progress that had been previously made in clarifying the clinical phenotypes of the constituent clinical entities of LBD and their associations with other types of dementia and which underpinned the development of the refined diagnostic guidelines issued by the DLB Consortium in 2017. There was also a growing focus on therapeutic approaches, including drug treatments and deep brain stimulation for DLB with apathy (Topic 4: 952 documents, 13.3% of total terms), alongside emerging non-pharmacological strategies, though these remained in early development stages. This period also saw increased recognition and discussion of the specific ‘needs’ of people with LBD (Topic 5: 1147 documents, 12.1% of total terms).
The 2018–2023 period marked the first mention of a systematic review and included research on quality of life, introducing a multidimensional concept for the first time (Topic 5: 1147 documents, 12.1% of total terms). Despite the limited cost-effectiveness studies11, the impact of healthcare and support systems started to emerge together with the integration of new technologies like AI and machine learning (Topics 5 and 7: combined 1887 documents, 21.4% of total terms), suggesting potential for early diagnosis and targeted interventions through advanced neuroimaging and connectivity analysis. Research on “prodromal” stages remained limited, with only Topic 6 (464 documents, 10% of total terms) addressing early-onset genetic factors, and while risk factors were increasingly identified, intervention trials remained sparse during this period.
These results indicate that while the field of LBD has been evolving, it remains limited. The past and current research was predominantly clinical and biomedical, with minimal involvement from multidisciplinary teams or efforts in education and awareness. Literature from non-medical disciplines remained thin. While quality of life in LBD has been investigated using established instruments (e.g., refs. 15,16,17,18,19), there remains a paucity of methodological studies on developing or validating assessment tools specifically tailored to the unique symptomatology and caregiver dynamics of LBD. Similarly, functional ability measurements in LBD lack standardized, disease-specific frameworks. Emerging work has begun to explore sensory impairments like hyposmia in LBD (e.g., associations with CSF biomarkers20), yet research on disease staging beyond biomedical approaches—particularly in integrating patient-reported outcomes or non-pharmacological interventions—remains limited. Furthermore, there was limited research on advocacy, ethics, palliative care, or service development with only Topic 5 in the 2018–2023 period (1147 documents, 12.1% of total terms) beginning to address care systems and patient needs.
Significant gaps persist in LBD research, particularly when compared to advances in AD and PD. For instance, while large-scale AD prevention trials (e.g., the FINGER study21) have informed global brain health initiatives, analogous strategies for LBD are absent. Similarly, real-world data from PD cohorts (e.g., using smartphone-based motor monitoring22) have revolutionized personalized care, yet LBD research lags in adopting these approaches. The underutilization of RT-QuIC—a tool already refining diagnostics in prion disorders and synucleinopathies23,24—represents another missed opportunity. Despite evidence linking dysautonomia and gastrointestinal dysfunction to alpha-synuclein pathology in PD25,26, these remain understudied in LBD despite their clinical relevance. Additionally, important research on environmental and social determinants may be underrepresented in the indexed literature, as exemplified by a 2015 South American study that found associations between poor sanitary conditions and higher LBD prevalence compared to AD27, highlighting the need for more diverse, global research perspectives on LBD risk factors.
Our prioritization survey—enhanced by input from a PPI event and consensus workshop—revealed that individuals with lived experience of LBD and healthcare professionals focused on enhancing diagnostic tools, care coordination, and developing new treatments. These priorities address key challenges of LBD, including frequent misdiagnoses, poorer quality of life compared to other dementias, and a significant lack of clinical trials focused on LBD.
Notably, the research priority questions identified through the survey aligned closely with the research gaps identified through analysing the research agenda of the 17-year period research landscape: a desire for more research into risk factors, more focus on palliative care, raising awareness and providing more information to the public and healthcare professionals about LBD, more focus on pathways to care and diagnosis, and developing more peer support services in place.
The research priorities in our study show overlap with the two published US-based LBD research priority setting studies9,14. Holden, Bedenfield14 showed that people living with LBD and care partners prioritized research into disease-modifying therapies, improved disease detection and improving disease staging. Additionally, people with LBD were interested in pathophysiology and more bothered by motor symptoms while caregivers highlighted more interest in risk factors, symptomatic therapies, and neuropsychiatric symptoms. Armstrong, Gamez9 found that the top research priorities for individuals with LBD and caregivers included determining the cause of LBD, improving LBD diagnosis, investigating what to expect as the disease progresses, and improving the daily functioning of people with LBD as well as the quality of life of both people with LBD and their care partners. While overlaps between priorities identified in Ireland and those from US-based studies suggest shared challenges in high-income Anglophone contexts, they highlight—rather than resolve—the need for global prioritization efforts that center underrepresented regions.
We acknowledge that our Scopus-based search strategy may have underrepresented studies from certain geographic regions or interdisciplinary research that used different terminology. While the recruitment strategy was designed to leverage established relationships within the LBD community to ensure authentic engagement from those with direct lived experience and clinical expertise. However, we acknowledge that this approach may have inadvertently excluded perspectives from healthcare professionals, researchers, or advocacy groups not connected to GBHI, Lewy Body Ireland, Dementia Trials Ireland network, or support groups like Teatime with Lewy. We acknowledge that the online survey format may have excluded individuals with limited digital literacy or internet access. Further the relatively small number of LBD diagnoses in Ireland limited our participant pool to just three individuals with LBD. While we actively engaged care partners and proxies to contribute perspectives on behalf of those unable to respond independently. These efforts aimed to balance inclusivity with pragmatic recruitment challenges, though we recognize inherent limitations in capturing all voices equitably. Efforts to include more care partners were also challenging, despite a robust turnout from healthcare professionals. Nonetheless, the priorities identified reflect a consensus among broad stakeholder groups—people with LBD, care partners, and healthcare professionals—as confirmed during our PPI event and final consensus meeting. This led to a unified list of research priorities, ensuring the research agenda is inclusive. Despite these challenges, the research’s strength lies in its collaborative approach, capturing the diverse perspectives of stakeholders and in the study of the topics of research during a 17-year long time period. Continuous validation and updating of priorities are essential as new insights and technologies emerge. Our study did not evaluate the geographic distribution of research topics or authorship. Future work should prioritize such analyses to ensure equitable representation in LBD research agendas.
Methods
Building on the principles of collaborative research and community-driven priority setting by the James Lind Alliance - a non-profit initiative that prioritizes research questions through consensus-building between patients, caregivers, and clinicians28 - we conducted a multi-stage research prioritization process. Conducted from December 2022 to March 2024, we undertook an AI-assisted topic modelling of the global LBD literature to establish a baseline understanding of the research landscape, to identify key themes and trends, and pinpoint gaps in current knowledge. This foundational stage informed subsequent development of the survey and discussions with the LBD community in Ireland.
AI-assisted topic modeling of the global LBD research
First, we applied Latent Dirichlet Allocation (LDA) to perform AI-assisted topic modelling on LBD research indexed by Scopus, spanning two-time frames: 2006–2016 (pre-2017) and 2018–2023 (post-2017). The modeling enabled us to assess evolution in LBD research, particularly in response to the 2017 DLB Consortium diagnostic guidelines6. We searched Scopus using keywords “Lewy body dementia”, “DLB”, and “PDD”, retrieving 9821 abstracts from 2006 to 2017 and 8794 abstracts from 2018 to 2023, and employing LDA to identify topics within the text documents. The percentage composition indicates the proportion of all terms in the corpus that belong to each topic, reflecting the relative research emphasis on different themes.
LDA is a statistical method that utilizes the Dirichlet distribution to uncover underlying topics within a large corpus of text documents29. It is based on two key assumptions: first, that each document is a mixture of topics, with each topic contributing to the document’s overall meaning; and second, that each topic is characterized by a distinct distribution over words, with certain words being more representative of a given topic than others.
To obtain the optimal number of topics in the collection of documents, we used a topic coherence score, which creates content vectors of words using their co-occurrences and subsequently calculates the score using normalized pointwise mutual information and the cosine similarity30. The exploration of identified topics was made based on the Salience and Relevance metrics. Salience is a metric used to identify which words are the most informative for identifying topics in all documents31. The higher the saliency value, the more helpful the term is for distinguishing the topic. Saliency is always positive and does not have a maximum value. A value of 0 indicates that a given word effectively belongs equally to all topics. Saliency is designed to look at words on a corpus-scale, as opposed to an individual topic level. Relevance is a metric used for ranking terms within topics32. It helps identify the most relevant words within a given topic and reflects the level at which a word belongs to a certain topic at the exclusion of other topics. Relevance uses a parameter λ to weight the probability of a term within a topic relative to its lift. We assumed the value of 0.6 for λ, as the optimal one, for the topic’s interpretation. The higher the relevancy metric is for a given topic, the more exclusive that term is to the given topic.
After performing topic modelling, each document was assigned to the topic with the highest probability, indicating the topic that most strongly characterizes its content. This assignment enables the grouping of documents into clusters, where a cluster is defined as a set of documents that share the same dominant topic. In this context, clusters represent thematically similar documents, allowing for the organization of the corpus based on semantic structures. This analysis yields two complementary metrics: the number of documents assigned to each topic (indicating thematic prevalence) and the percentage of corpus terms belonging to each topic (indicating research emphasis by word volume).Based on the top terms belonging to each topic, the AI tool, ChatGPT, drafted summaries responding to the following prompt: “Act as a neuroscientist or clinician and give a short title and 5–10 line description of the topic that is being studied by a cluster of scientific papers on Lewy body dementia and/or DLB that are characterized by the following terms given in order of relevance.” 1)…, 2)…, 30)…” providing the top 30 most relevant terms (in order of Relevance) for each topic identified in each time period.” The AI prompt uses the technical term “cluster” to describe a set of documents that share a common dominant topic. However, for clarity and accessibility to non-expert readers, we use the term “topic” throughout the manuscript when referring to the thematic groupings identified by the LDA analysis. We use both terms interchangeably as they represent the same analytical construct in this context. Eight topics were identified for each time period based on optimal coherence scores.
Three clinicians with long experience in the field of neurocognitive disorders and old-age psychiatry (IL, JK, PA) critically reviewed and revised the summaries generated by ChatGPT so that the most common topics of each period were succinctly captured and could be compared to the priorities defined by the community of people living with LBD and their care partners.
Community engagement and priority setting
Step 1: Literature review of research priorities. To validate AI-assisted findings, we conducted a conventional review of the literature on the identified research priorities in the context of LBD. A search strategy was developed in consultation with an accredited librarian at Trinity College Dublin (refer to Supplementary Information). The search was run on 16th January 2023, applied to Embase, Medline, CINAHL, Cochrane Library, and complemented with Google Scholar Advanced Search. The inclusion criteria were intentionally broad, encompassing papers that explicitly used terms such as ‘research priorities’ or implicitly addressed gaps/unmet needs (e.g., ‘future directions,’ ‘critical challenges,’ ‘recommendations for LBD research’). Manual screening ensured contextual relevance to prioritization efforts, even if specific terminology was absent. (Table 3).
Search results were imported into EndNote X7, duplicates removed and imported into Covidence. Data was extracted from included studies using an Excel spreadsheet developed for the analysis. Extracted information included country of origin, publication year, study type, study aim, demographics, and quantitative and/or qualitative results. Two investigators subsequently analysed the data. Thematic analysis was performed using Excel to create an initial long list of themes based on the findings from both conventional and AI-assisted searches. This list was then refined into a shorter set of preliminary research priorities through an iterative process involving the steering committee convened for this project. The steering group consisted of a care partner of a person living with LBD, an advocacy group representative, two healthcare professional and three researchers specializing in LBD.
Step 2: Prioritization survey. Using the list of preliminary priorities, we developed an online cross-sectional prioritization survey to engage the LBD community, including people living with LBD, their care partners, health and social care professionals and LBD researchers in Ireland. The survey was scripted using Qualtrics and made available online from June 22 to September 27, 2023. It was disseminated through the partner networks of steering group members including the Global Brain Health Institute (GBHI), Lewy Body Ireland (LBI), and Dementia Trials Ireland (DTI) and support groups, such as “Teatime with Lewy”.
The survey comprised two sections: research prioritization and demographics. In the research prioritization section, participants were asked to list up to five topics they believed were under-researched, using open text boxes for their responses, which were referred to as “additional priorities.” Participants then selected the top ten most important topics from a refined list of research priority questions derived from the literature review. Finally, they reviewed their previously selected topics along with the additional priorities and chose the three they considered most critical. The demographics section collected information on respondents’ titles (e.g., person living with LBD, carer, health/social care provider, or other), age, gender, county of residence, and whether they lived in a rural or urban area.
The quantitative survey data were analysed descriptively, while the open-text responses were subjected to content analysis. Any ambiguities in responses were discussed and resolved by the steering committee.
To identify the top 10 most important topics, we assigned one point to each topic every time it was selected by a participant in their top 10 list, and an additional point if it was also chosen as one of the top three. This method enabled us to calculate the total score for each topic and determine the 10 topics with the highest scores. This scoring system was implemented based on feedback from the PPI, which indicated that respondents would find it challenging to rank all 19 topics, as they would likely consider each one important.
Step 3: Public and Patient Involvement (PPI) event. A PPI event was organized to facilitate an in-depth conversation with the LBD community, offering a platform for additional feedback on the selected research priorities. This step ensured that the perspectives of those directly affected by LBD were central to shaping the research agenda.
Step 4: Development of focused research agenda. Using data gathered from the literature, survey, and the PPI event, a focused research agenda was drafted to highlight the most critical areas requiring attention, based on both empirical evidence and community feedback.
Step 5: Final consensus meeting. The process concluded in a consensus meeting where the proposed research priorities were discussed and finalized. This meeting included representatives from various stakeholder groups, including researchers, healthcare professionals, care partners, people living with LBD, and advocacy organizations, to ensure that the final set of priorities was mutually agreed upon and representative of the broad LBD community.
Data availability
The data that support the findings of this study are not publicly available but are available from the corresponding author upon reasonable request.
References
Prasad, S. et al. Recent advances in Lewy body dementia: a comprehensive review. Disease-a-Month 69, 101441 (2023).
Galvin, J. E. et al. Characterization of dementia with Lewy bodies (DLB) and mild cognitive impairment using the Lewy body dementia module (LBD-MOD). Alzheimer’s Dementia 17, 1675–1686 (2021).
Hogan, D. B. et al. The prevalence and incidence of dementia with lewy bodies: a systematic review. Can. J. Neurol. Sci. 43, S83–S95 (2016).
D’Antonio, F., et al. Dementia with Lewy bodies research consortia: a global perspective from the ISTAART Lewy body dementias professional interest area working group. Alzheimer’s Dement. Diagnosis Assess. Dis. Monit. 13, e12235 (2021).
Surendranathan, A., et al. Clinical diagnosis of Lewy body dementia. BJPsych Open 6, e61 (2020).
McKeith, I. G. et al. Diagnosis and management of dementia with Lewy bodies. Neurology 89, 88–100 (2017).
Goldman, J. G., et al. Challenges and opportunities for improving the landscape for Lewy body dementia clinical trials. Alzheimer’s Res. Ther. 12, 1–11 (2020).
Cromarty, R. A. et al. Neurophysiological biomarkers for Lewy body dementias. Clin. Neurophysiol. 127, 349–359 (2016).
Armstrong, M. J. et al. Research priorities of caregivers and individuals with dementia with Lewy bodies: an interview study. PLOS ONE 15, e0239279 (2020).
Orme, T., Guerreiro, R. & Bras, J. The genetics of dementia with lewy bodies: current understanding and future directions. Curr. Neurol. Neurosci. Rep. 18, 1–13 (2018).
Boland, E., et al. The high cost of care and limited evidence on cost-effective strategies for Lewy body dementia: systematic review of evidence. BJPsych Open, 10, e20 (2024).
Walker, Z. et al. Lewy body dementias. Lancet 386, 1683–1697 (2015).
Abdelnour, C. et al. Dementia with Lewy bodies drug therapies in clinical trials: systematic review up to 2022. Neurol. Ther 12, 727–749 (2023).
Holden, S. K. et al. Research priorities of individuals and caregivers with Lewy body dementia. Alzheimer Dis. Assoc. Disord. 37, 50–58 (2023).
Lee, C.-Y. et al. Quality of life in patients with dementia with Lewy bodies. Behav. Neurol. 2018, 8320901 (2018).
van de Beek, M. et al. Trajectories and determinants of quality of life in dementia with Lewy bodies and Alzheimer’s disease. J. Alzheimer’s Dis. 70, 389–397 (2019).
Toya, S. et al. Factors associated with quality of life in patients with dementia with Lewy bodies: additional analysis of a cross-sectional study. J. Alzheimer’s Dis. 100, 525–538 (2024).
Armstrong, M. J. et al. Patient- and proxy-reported quality of life in advanced dementia with Lewy bodies. Alzheimer’s Dement. 20, 2719–2730 (2024).
Oliveira, F. F. d., Assessing independence in activities of daily living and quality of life in patients with dementia with Lewy bodies. J. Alzheimer’s Dis. 101, 441–443 (2024).
de Oliveira, F. F. et al. Associations of neuropsychiatric features with cerebrospinal fluid biomarkers of amyloidogenesis and neurodegeneration in dementia with Lewy bodies compared with Alzheimer’s disease and cognitively healthy people. J. Alzheimer’s Dis. 81, 1295–1309 (2021).
Ngandu, T. et al. A 2 year multidomain intervention of diet, exercise, cognitive training, and vascular risk monitoring versus control to prevent cognitive decline in at-risk elderly people (FINGER): a randomised controlled trial. Lancet 385, 2255–2263 (2015).
Zhan, A. et al. Using smartphones and machine learning to quantify parkinson disease severity: the mobile Parkinson disease score. JAMA Neurol. 75, 876–880 (2018).
Rossi, M. et al. Ultrasensitive RT-QuIC assay with high sensitivity and specificity for Lewy body-associated synucleinopathies. Acta Neuropathol. 140, 49–62 (2020).
Sano, K. et al. Prion-like seeding of misfolded α-Synuclein in the brains of dementia with Lewy body patients in RT-QUIC. Mol. Neurobiol. 55, 3916–3930 (2018).
Cersosimo, M. G. & Benarroch, E. E. Autonomic involvement in Parkinson’s disease: pathology, pathophysiology, clinical features and possible peripheral biomarkers. J. Neurol. Sci. 313, 57–63 (2012).
Kim, S. et al. Transneuronal propagation of pathologic α-Synuclein from the gut to the brain models Parkinson’s disease. Neuron. 103, 627–641.e7 (2019).
Oliveira, F. et al. Contrasts between patients with Lewy body dementia syndromes and APOE-ε3/ε3 patients with late-onset Alzheimer disease dementia. Neurologist. 20, 35–41 (2015).
Kelly, S. et al. Dementia priority setting partnership with the James Lind Alliance: using patient and public involvement and the evidence base to inform the research agenda. Age Ageing. 44, 985–993 (2015).
Blei, D., Ng, A. & Jordan, M. Latent dirichlet allocation. J. Machine Learn. Res. 3, 993–1022 (2003).
Syed, S. & Spruit, M. Full-text or abstract? Examining topic coherence scores using latent dirichlet allocation. In Proc. 2017 IEEE International Conference on Data Science and Advanced Analytics (DSAA) (IEEE, 2017).
Chuang, J., Manning, C.D. & Heer, J. Termite: visualization techniques for assessing textual topic models. In Proc. International Working Conference on Advanced Visual Interfaces (ACM, 2012).
Sievert, C. & Shirley, K. LDAvis: A method for visualizing and interpreting topics. In Proc. Workshop on Interactive Language Learning, Visualization, and Interfaces. 63–70 https://aclanthology.org/W14-3110/ (Baltimore, Maryland, USA. Association for Computational Linguistics, 2014).
Acknowledgements
This project was funded by Dementia Trials Ireland awarded to Irina Kinchin. While working on this paper, Irina Kinchin was supported by the Health Research Board (HRB) Fellowship ‘Applying Research into Policy and Practice (ARPP)’ (ARPP-2020-011). She is currently supported by the HRB Applied Programme Grants (APRO) Award (Reference 9745). The funding sources had no involvement in the study design; in the collection, analysis, and interpretation of data; in the writing of the report; or in the decision to submit the article for publication. We wish to express our gratitude to all the participants who dedicated their time and shared their insights throughout this study. Special thank you to the care partners and healthcare professionals whose invaluable contributions have enriched our understanding of Lewy Body Dementia. Our thanks extend to the Global Brain Health Institute (GBHI), Lewy Body Ireland, and Dementia Trials Ireland for their assistance in disseminating the survey and engaging the community. Additionally, we acknowledge the efforts of our steering group members, who provided oversight and direction, ensuring the study remained focused and impactful. Their expertise and commitment have been fundamental to the success of this project. Lastly, we thank the Public and Patient Involvement groups, especially those involved in the 'Teatime with Lewy' sessions, for their active participation and for providing a platform for further discussion and validation of our research findings.
Author information
Authors and Affiliations
Contributions
Irina Kinchin – Conceptualization, Methodology, Writing - Original Draft, Writing - Review & Editing, Supervision, Funding acquisition Rachel L. Fitzpatrick – Investigation, Writing - Original Draft Grigorios Papageorgiou – Software, Writing - Review & Editing Joseph Kane – Review & Editing Panagiotis Alexopoulos – Software, Review & Editing Polychronis Economou – Software, Review & Editing Jayne Conlon - Review & Editing Petya Grigorova – Review & Editing Iracema Leroi – Conceptualization, Methodology, Review & Editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
Ethics approval was obtained from the Centre for Health Policy and Management Research Ethics Committee at Trinity College Dublin.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kinchin, I., Fitzpatrick, R.L., Papageorgiou, G. et al. From data to dialogue in setting research priorities for Lewy body dementia. npj Dement. 1, 19 (2025). https://doi.org/10.1038/s44400-025-00019-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s44400-025-00019-x