Abstract
Lewy Body dementia (LBD) is a common yet under-recognised dementia that presents distinct diagnostic and care complexities. This qualitative study explored experiences of LBD diagnosis and care through semi-structured interviews with 17 care partners and 23 healthcare professionals across urban and rural regions in Ireland. Participants described diagnostic delays and misdiagnoses linked to limited clinical awareness, alongside fragmented service provision that was frequently navigated through informal support networks. Care partners highlighted substantial emotional and financial impacts and a lack of clear guidance following diagnosis, while healthcare professionals emphasised system-level constraints and unmet training needs. Notably, both groups articulated clear, actionable priorities, including improved diagnostic pathways and more integrated, age-inclusive services. While several challenges overlapped with other dementias, participants emphasised the fluctuating symptom profile, frequent misattribution of early symptoms, and gaps in LBD-specific expertise as particularly important. Although situated in the Irish context, these findings offer transferable insights to inform service development and equity-focused reforms for non-Alzheimer’s dementias internationally.
Similar content being viewed by others
Introduction
Lewy Body dementia (LBD) is an umbrella term encompassing two closely related conditions, dementia with Lewy Bodies (DLB) and Parkinson’s Disease dementia (PDD). Both are characterised by the pathological accumulation of alpha-synuclein1,2. The clinical distinction between DLB and PDD is traditionally based on the timing of symptom onset, i.e. DLB is diagnosed when dementia precedes or coincides with parkinsonism onset, while PDD is diagnosed when motor symptoms precede dementia by at least a year. However, this distinction has been increasingly questioned, with some suggesting that the two conditions may represent points along a spectrum of Lewy body disease1,3,4.
LBD accounts for an estimated 5–25% of dementia cases globally with precise prevalence varying due to lack of formal diagnosis and underestimation being a global issue5,6. In Ireland, where approximately 65,000 people are living with dementia, it is estimated that between 7000 and 10,000 individuals may be affected by LBD7,8. While specific diagnostic data for Ireland are lacking, UK research from the DIAMOND Lewy programme suggests that clinical recognition of LBD remains low; prior to the introduction of structured assessment tools, fewer than 5% of dementia cases in secondary care were diagnosed as LBD9.
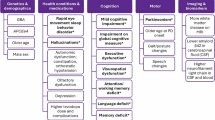
LBD presents a particularly complex diagnostic challenge due to its wide-ranging and fluctuating symptomatology. Affected individuals may experience cognitive impairment, visual hallucinations, delusions, REM sleep behaviour disorder, autonomic dysfunction, and features of parkinsonism5,10,11,12,13,14. This overlap with both psychiatric and other neurological conditions contribute to frequent misdiagnosis or delayed diagnosis15,16. Furthermore, treatment is complicated by patients’ heightened sensitivity to antipsychotics17,18, poor tolerance of antidepressants19, and the lack of established disease-modifying therapies20. Some commonly prescribed treatments for Alzheimer’s or Parkinson’s disease particularly certain antipsychotics and dopaminergic agents can exacerbate LBD symptoms. Accurate diagnosis is therefore critical to minimise potential harm and to guide appropriate, symptom-specific management2,17. As a result, individuals with LBD and their care partners may experience fragmented diagnostic, treatment, and support services, with significant implications for quality of life and clinical outcomes16,21.
In Ireland, there is currently no standardised national clinical guideline or formalised care pathway specific to LBD. While broader initiatives such as the National Dementia Strategy22 have aimed to improve dementia awareness and community-based supports, these have primarily focused on Alzheimer’s disease, leading to less emphasis on complex and less informed dementias such as LBD. This limited LBD-specific infrastructure, across diagnostic, treatment, and support services, may contributes to delayed recognition, inconsistent care experiences, and limited specialist input.
Rural-urban disparities may further exacerbate these issues, as individuals in more remote areas often have reduced access to neurology, geriatrics, or multidisciplinary teams with experience in LBD. Consequently, both care partners and clinicians may be required to must navigate fragmented pathways, often without condition-specific resources or support mechanisms7,16.
The current study seeks to understand lived experiences of care partners and healthcare professionals navigating the diagnostic and post-diagnostic journey for LBD within the Irish healthcare context. We use the term care partner to emphasise the collaborative and personal nature of support provided to people living with LBD. While caregiver can sound more clinical or imply a professional role, care partner recognises the close, ongoing relationship often shared between family members or close friends and the person they support23,24. This study builds on our earlier work, which examined the diagnostic journey from the perspective of people with LBD and Alzheimer’s disease and identified important disparities in experiences and support along the care pathway that warranted further examination25. By extending the focus to include care partners and healthcare professionals, the present study moves beyond individual experiences to capture the wider care ecosystem. Taken together, these studies offer a comprehensive, lived experince and person‑centred understanding of the diagnostic and post‑diagnostic journey for LBD in Ireland, spanning the perspectives of those living with the condition, those providing unpaid care, and those delivering formal services.
Results
A total of 40 individuals participated in this study, including 17 care partners and 23 healthcare professionals. Summary demographic details for both groups are presented in Tables 1 and 2.
Theme 1. Recognition and diagnosis
This theme captures the often complex and emotionally fraught journey individuals, and their families face in the earliest phase of the care pathway. Recognition of symptoms, navigating the diagnostic process, and receiving a formal diagnosis were central concerns raised by both care partners and healthcare professionals.
Sub-theme: overlooked or misunderstood early symptoms
Care partners described how the early signs of LBD were often subtle and misattributed to other health issues, such as infections, hearing loss, or normal aging. This misinterpretation, shared by both families and healthcare professionals, frequently led to delays in seeking or receiving a formal diagnosis. In hindsight, care partners recognised that symptoms like confusion, changes in hearing, and hallucinations were early indicators of LBD, but these were not initially identified as such. As one care partner recalled:
“He was still a bit confused… they were treating him for sepsis. That’s what they thought was happening.” (Care Partner P1)
Other instances involved symptoms being misattributed to unrelated conditions:
“We got hearing aids because I thought he was not picking up things or not following conversations was because of the deafness.” (Care Partner P2)
Several healthcare professionals also noted how early symptoms, like anxiety or hallucinations, are often misinterpreted, delaying the recognition of dementia:
“People often present with anxiety or hallucinations before dementia is suspected.” (Consultant Psychiatrist P22)
Sub-theme: diagnostic ambiguity and missteps
Both groups described how the fluctuating and complex nature of LBD symptoms can lead to delays in reaching a diagnosis. Care partners, in particular, reflected on the emotional toll and frustration of prolonged periods without answers, while healthcare professionals acknowledged that some cases likely remain undiagnosed due to the subtlety and variability of symptoms.
“Three years of struggling with my dad. I was horrified. I was like, what the hell? I said, and I said, do you understand? I said, what you’re after doing? I said, we’re after losing three years.” (Care Partner P18)
Healthcare professionals echoed the difficulty in reaching a timely and confident diagnosis:
“There was something different in their presentation that marked them out. But I’ve no doubt that a number have gone undiagnosed.” (General Practitioner P16)
Sub-theme: communication of diagnosis
Participants described the communication of diagnosis as a pivotal and emotionally charged moment, with the manner of delivery, clarity, empathy, and provision of follow-up support, shaping their overall experience. Experiences ranged from confusion and a lack of structured support after diagnosis to appreciation of compassionate and informative clinicians.
“It wasn’t delivered communicatively poorly, just the idea of supports. And, you know, the fact that we were sent back to Limerick again and just left, like, you know.” (Care Partner P18)
“Make sure people actually understand. And then when it’s an atypical dementia syndrome like Lewy body, you know, people don’t really know what that means.” (Geriatrician P5)
However, others described the compassion and professionalism of clinicians who helped make the diagnosis more manageable:
“She is our hero. She was wonderful and always very courteous to us and to my husband. He felt he was on a level pitch with her… able to talk to her from both a medical and personal point of view. Our meetings with her were informative and very welcomed.” (Care Partner P1)
Sub-theme: uncertainty around who to approach and when
Care partners described confusion and uncertainty about which professionals to approach, what each role entailed, and when to seek their involvement. This lack of clarity often left families feeling isolated and unsure if they were accessing the right support at the right time, with some care tasks being overlooked or delayed as a result.
“People often don’t know who to turn to - even starting the journey is hard.” (Clinical Neuropsychologist P18)
“I was frantic, you know, because the public health nurse didn’t want to call. Nobody wanted anything to do with me.” (Care Partner P4)
“Considering speech and language… I mean, really, speech and language therapist, why?” (Care Partner P17)
Theme 2. Systemic fragmentation and informal anchors
While the diagnostic phase posed challenges, participants described an even starker vacuum after receiving a formal diagnosis. This theme examines how families encountered a “cliff edge” in post-diagnostic care, marked by an absence of structured follow-up, fragmented communication between services, and heavy reliance on informal networks to manage complex and evolving needs.
Sub-theme: navigating a disjointed system
Care partners described a fragmented and confusing care system, where the lack of clear pathways and coordination left families feeling lost and unsupported. Without a clear care roadmap, care partners often took on the role of coordinator, advocate, and navigator, struggling to manage the fragmented system themselves.
“And when you’re going through it, without anybody seeming to know what to do, just made it so much worse, because I just felt lost.” (Care Partner P16)
Despite these system-level barriers, many participants emphasised the positive impact of individual healthcare professionals who went above and beyond to support families. These trusted figures often GPs, geriatric psychiatrists, or dementia nurse specialists became informal anchors in an otherwise uncertain care landscape.
“Like anything that you want, really, they’ll get you. They’re very, very helpful. They’ve been very, very good and very efficient. Yeah. I have nothing but praise for the HSE, I have to say.” (Care Partner P15)
“I didn’t feel we were being listened to until we went to [Consultant]. Because everything seemed to be based on the Lewy’s bodies dementia, but not what was happening in my home, Misidentification.” (Care Partner P16)
Sub-theme: absence of structured follow-up
Both care partners and professionals highlighted the lack of structured follow-up after diagnosis, describing how families were often left to navigate the next steps alone, with minimal guidance or support from services.
“There was no discussion about how to handle symptoms. Or I often used to go to the consultation and think, why am I bothering?” (Care Partner P8).
“He wasn’t understood, he was ignored… that’s been the most challenging” (Care Partner P18)
Some families described needing to “chase” referrals or follow up multiple times to ensure action was taken, leading to delays in receiving support.
Sub-theme: lack of communication among healthcare professionals within the care pathway
Both care partners and healthcare professionals described frequent breakdowns in communication and coordination between different parts of the healthcare system, leading to fragmented care, repeated delays, and a lack of clarity about roles and responsibilities. These gaps left both families and professionals feeling unsupported and frustrated.
“There was no real offer of understanding of places to go, networks to connect with – nothing” (Care Partner P18).
“I think that’s a big challenge. And then again, I suppose, coordination and communication really amongst the, all the teams, like with the geriatrician, the neurologist.” (Consultant of Psychiatry of Later Life P3)
There was limited continuity between hospital, primary care, and community supports. One psychiatrist noted the frustration of providing specialist input that was later disregarded, stating,
“…what’s the point in getting us involved if you’re going to undo everything we’ve done?” (Consultant of Psychiatry of Later Life P3).
“So, there isn’t that the communication between hospitals isn’t…nobody taking responsibility. So, it’s like might be changing medications and they might get a referral to somebody else. They might change, you know, so yeah, no clear pathway, I don’t think.” (Advanced Nurse Practitioner (ANP) - Memory P23)
“it’s a weakness of our system, I think, is that the public health nurses have a hugely important role to play, and they’re really well trained, and they carry a heavy workload. But the coordination is a problem, and that’s backed the way we organise our services.” (General Practitioner P16)
In contrast, some healthcare professionals brought up a promising example; an integrated online communication system used across services, which enabled real-time updates and improved coordination of referrals, appointments, and follow-up actions.
Sub-theme: reliance on informal networks
With limited formal support, families often relied on informal networks-such as neighbours, charities, and peer groups-for practical help and emotional support. While these resources were deeply valued, their necessity highlighted the inadequacy of statutory services and the patchwork nature of support available.
“But… I found that… only for the support I was getting from my next-door neighbour… I couldn’t have done a lot of things.” (Care Partner P9)
“The Alzheimer’s Society has good, really good stuff, so we tend to go through that with people and explain it and do our best from that point of view.” (Consultant Psychiatrist P17)
Theme 3. The emotional and practical burden of care
As the realities of LBD set in, both care partners and healthcare professionals described emotional and practical challenges. This theme is about the intense labour, both emotional and logistical inherent in sustaining care for someone with LBD, and the strategies participants use to cope.
Sub-theme: emotional toll on care partners
Care partners described experiencing ongoing exhaustion, burnout, and emotional strain as they managed the unpredictable and demanding nature of LBD. This constant vigilance and responsibility often led to feelings of isolation and a pressing need for additional support, as echoed by both care partners and professionals.
“I am so tired. And he’ll say, Mom, you just you know, you have to get in help, or you have to get. But it’s not help. It’s not physical help.” (Care Partner P1)
“I think I’m burnt out. I can’t take the responsibility anymore.” (Care Partner P13)
“But also, I think we need to look at the supports around family members. Yeah, we can do look at the carer burden from that aspect.” (PD Nurse Specialist P14)
Sub-theme: frustration with system limitations
Both care partners and healthcare professionals described how limited resources and time constraints within the health system led to brief, unsatisfactory consultations and a sense of frustration. These systemic limitations left families feeling unsupported and professionals unable to provide the level of care they aspired to deliver.
“I think it’s due to the fact that’s due to the fact you’re in there for five minutes. It’s not a proper consultation because the public system doesn’t have the capacity to do it” (Care Partner P8 discussing hospital resource issues caused the diagnosis delay).
“They’re trying to bypass the system… rather than having to wait for geriatrics. And I get why they do that… but it’s kind of frustrating for us because then we get looped into diagnostics when I don’t have access to a lot of stuff… We end up getting drawn into stuff we don’t have the resources for… but we’ve accepted the referral in good faith.” (Consultant Psychiatrist P3)
“And the actual resources for the team haven’t changed in about 20 years, but the demand for the service has gone way up. And so, we feel that, you know, I guess a lot of places in healthcare are feeling this way. We feel it’s inadequate for patients and for people who are referring in and for families.” (Consultant Psychiatrist P4)
These systemic barriers not only limit the support available to families but also contribute to the financial and emotional pressures described by care partners.
Sub-theme: financial and resource constraints
Participants also spoke about the financial burden that came with accessing care, including the costs associated with travelling for appointments, paying for home care, or seeking out private care options due to gaps or waiting lists in public services. Care partners commented on the problems of getting a medical card which would alleviate these stresses and streamline access to care supports:
“It was actually every doctor was writing up about that medical card… And eventually I got it…I thought you’d get what you’re entitled to and that’s that, you know… It shouldn’t be the way though.” (Care Partner P4)
“Yeah, so they refused him not on the basis of his medical needs but on his age. He was under 65” (Care Partner P2 discussing medical card) furthermore stating its impact “It went from… paying for everything and trying to manage everything independently… all of these allied professionals and Timetables and… appointments… suddenly like everything’s just like landing on your lap… Where was this when I needed it five years ago?”
“Lewy body is one of the hardest conditions to care for – carers need more than basic support.” (Consultant Geriatrician P15)
Theme 4. Inequitable access and training gaps
Theme 4 brings together two interrelated challenges: inequitable access to services and gaps in professional training. Participants’ accounts revealed that living in a rural area or being under 6526 often meant facing additional barriers to care, but these barriers were compounded when local professionals lacked the expertise to recognise or manage LBD. Thus, inequity in access was not only a matter of geography or age, but also of the knowledge and preparedness of the workforce. Addressing one without the other would be insufficient to improve the care pathway for people with LBD.
Sub-theme: rural vs. urban service disparities
Participants, especially those in rural areas, described significant barriers to accessing specialised care and community supports, often citing long travel distances, limited local services, and inconsistent availability of resources. These challenges contributed to delays in diagnosis and treatment, as well as increased emotional and practical strain for families.
“…Yeah, yeah, getting to it. It’s, it’s like, it just, you need to go out and get a bus, or pay for a taxi every week and sure, that’s it.” (Care Partner P17 discussing day centres and inability to get to it)
“Some areas are good but in others dementia isn’t prioritised in the community.” (Occupational Therapist P6).
“Community resources are patchy – some places have cafes, others have nothing.” (Advanced Nurse Practitioner (ANP) – Memory P23)
These geographic barriers are further complicated when local professionals lack specific training in LBD, making it even harder for families to access appropriate care.
Sub-theme: age related service mismatch and exclusion
Age-based criteria for certain services emerged as a significant barrier, particularly for younger individuals with LBD. Individuals with young onset LBD (under 65) were noted to experience specific challenges in accessing appropriate care. Many had difficulty finding healthcare providers who were familiar with early-onset LBD, and there was a lack of tailored resources for this age group. Spouses attending support groups also mentioned there was preconceptions that they were the child of an individual with LBD rather than a spouse as they were much younger than the general attendees.
“Everybody my age was in the support group was looking after their mother or their father who was in their 80 s. Yeah, so while the support group is good it, I was the only one that was trying to deal with the spouse and lost my job because of this and he gave up my job had to give up my business had to scale back my life.” (Care Partner P2)
“I was looking at nursing home care this is another problem nursing home care is not appropriate for young onset dementia whether it’s Alzheimer’s or LBD not appropriate” (Care Partner P13)
“Many under 65 s can’t access services – it’s much harder for them.” (Consultant Neurologist P2).
Sub-theme: limited LBD-specific expertise
Both care partners and healthcare professionals pointed to gaps in LBD-specific knowledge and training as contributing to missed or delayed diagnoses and uncertainty in care. Care partners described situations where classic symptoms were overlooked, while professionals highlighted the need for more education and awareness to improve recognition and management of LBD.
“Well, they might have been the classic symptoms, but the consultant didn’t make the diagnosis” (Care Partner P8)
“And I said, but are you not going to ask like why he fell, I mean, I didn’t push him, he wasn’t painting the wall, like why did he fall? What happened and they said, oh, no, no, no, no, our job is just to, whatever”. (Care Partner P2)
“You know, it’s just really more knowledge, more education and enabling patients and carers more, I think, and then more research as well, because I guess more research will lead to more publicity.” (Consultant Neurologist P2)
Sub-theme: inconsistent professional training
Healthcare professionals described variability in their roles and responsibilities, even among those with the same job title, which sometimes limited their ability to apply their specialist training in practice. As one consultant psychiatrist noted, this mismatch between training and real-world practice was a source of frustration, particularly when resources or support for diagnosing and managing LBD were lacking.
“But that’s frustrating… to have been trained to specialise in something and then not to be able to actually do it… when you meet somebody where they very clearly have a LBD, and you don’t really have the resources to diagnose that… you’re really just part of like an immediate problem… that’s really the way things have gone now.” (Consultant Psychiatrist P4)
Many participants highlighted the need for more LBD-specific education and training, observing that gaps in understanding among staff could make hospital admissions and ongoing care especially challenging for people with LBD.
“I think more education can only be, but yeah, I think it must be hard for people when they have to be admitted, when people with Lewy body have to be admitted and there’s no understanding there and they do have to be admitted.” (PD Nurse P1)
These accounts suggest that inconsistent professional development and limited access to targeted training contribute to difficulties in both diagnosis and ongoing management, reinforcing the need for more standardised pathways, dedicated roles, and integrated care models.
Theme 5. Call for awareness and structural change
While gaps in support services were a major concern post-diagnosis, participants also reflected on broader systemic needs sharing their hopes for a more informed, structured, and compassionate approach to LBD care in Ireland. Participants across roles shared aspirational ideas for improving care pathways. This theme captures their recommendations for systemic reforms, new roles, and models of care that could address the gaps identified in earlier stages.
Sub-theme: standardised national diagnostic pathways
Participants across both groups highlighted the need for standardised national guidelines and referral pathways for LBD. They felt that such frameworks would help reduce diagnostic uncertainty, improve consistency of care, and make support more accessible and predictable for both families and professionals. Some also noted recent improvements and ongoing efforts to address these gaps but felt that further progress is needed.
“I guess online educational supports pathways. You know, obviously, the ASI [Alzheimer’s’ Society Ireland] is good for people with dementia. And, you know, I think people have looked to maybe ASI and trying to get some information on DLB. But I think some patients have been linking a lot with the UK based supports. So, I think a dedicated Irish network would be would be very, very helpful.” (Consultant Neurologist P2)
“Once a GP wants to refer on for secondary care assessment, it’s, you know, clear guidelines as to whether it goes to the geriatricians, to neurology, to us.” (Consultant of Psychiatry of Later Life P22)
“It’s not like with like with heart patients, cancer patients. They all have follow ups in terms of, you know, if they require extra intervention, it’s made available to them, whereas I don’t know what the extra interventions are.” (Care Partner P1)
“I think the last year has improved a lot… there was a big unmet need in the under 70 s… I think we’ve done as much as we can… between the education sessions with GPs and everything else.” (Geriatrician P5)
Sub-theme: specialist and multi-disciplinary care models
Participants described the value of specialist roles and multidisciplinary teams in improving care for people with LBD. They highlighted how dedicated positions, such as nurse specialists or care coordinators, and collaborative models, like memory clinics, can enhance continuity, communication, and holistic support for both individuals with LBD and their families. These examples were seen as models for future service development.
“It’s kind of more to try and manage the carers around them, rather than the people themselves… I have quite a difficult case at the moment… a Parkinson’s related dementia, but it’s gone very like a Lewy-Body’s… It’s more to care for the person or the people living with them, rather than the person themselves.” (Advanced Nurse Practitioner (ANP) – Movement Disorders P14)
“Like similar to how in many regions, there is a Parkinson’s specialist. That is something that we’re kind of would, well, certainly I would like to have, if we were in time able to have more of a regional kind of clinic, that you would be able to upscale one person to have more of an ownership for people with Lewy body.” (Consultant Geriatrician P5)
“I did have an excellent CNS, a dementia CNS link to my clinic. She’s unfortunately moved to another post, but she was a great liaison with primary care centres, public health nurses and then community MDT as well.” (Consultant Neurologist P2)
“It’s unusual that you have two specialties that work hand in glove with regards to any condition and even with regards to memory. One of the conditions that is most appropriate for is with Lewy body.” (Consultant Geriatrician P15)
Table 3 provides a summary of the key themes identified in this study, along with the main conclusions and perspectives from both care partners and healthcare professionals.
Methods
Study setting and recruitment
Participants were recruited from healthcare settings across Ireland, including memory clinics, neurology and geriatric consultation services, as well as dementia and Parkinson’s support networks. Care partners were primarily recruited through support networks and outreach via gatekeepers in healthcare institutions such as St. James’s Hospital and Tallaght Hospital. Healthcare professionals were recruited through professional networks, institutional contacts, and online platforms, including LinkedIn and Twitter.
To ensure diversity, we specifically sought to include care partners and healthcare professionals of varying ages, genders, and professional backgrounds. We also made efforts to reach participants from both urban and rural areas by engaging with national and regional support organisations and targeting a range of healthcare disciplines to capture a wide spectrum of perspectives and experiences related to LBD care pathways in Ireland.
Care partners eligible for inclusion were individuals who were either currently providing care, as the primary carer, for someone diagnosed with LBD or who had recently done so, including those whose care role had ended due to the person’s move into long-term care or bereavement within the past two years. Consistent with our use of the term in this study, care partners encompassed spouses, children, siblings, and other close family members or friends who actively participated in care and support23,24. This focus on informal care partners was intentional, as their experiences encompass not only the practical aspects of care but also the profound emotional, social, and familial impacts of LBD, which were central to understanding the holistic care pathway from a personal perspective. Healthcare professionals were recruited from a range of disciplines, including neurologists, geriatricians, psychiatrists, clinical psychologists, neuropsychologists, social workers, occupational therapists, physiotherapists, speech and language therapists, nurses, and dietitians.
Recruitment for both care partners and healthcare professionals continued until no new significant themes emerged in later interviews, consistent with the concept of thematic saturation. However, we also considered the principle of information power27, recognising that the adequacy of our sample depended on the specificity of our aims and the diversity of our participants. This was assessed based on the richness and relevance of the data, the specificity of our research questions, and the diversity of participant backgrounds.
Data collection
A trained qualitative researcher conducted all interviews. The interviews were designed as semi-structured to capture both the practical and emotional aspects of care, including the challenges in navigating the healthcare system, the delivery of diagnosis, the services available post-diagnosis, and the emotional burden of caregiving.
The semi-structured interview schedule-one for care partners and one for healthcare professionals-was developed based on a review of relevant literature4,28,29 and informed by input from a Patient and Public Involvement (PPI) group, who provided valuable feedback on the relevance and clarity of the questions for both groups. To further refine the interview guide, practice runs were conducted with both a healthcare professional and a care partner who were not included in the main study.
Care partners were asked to reflect on their journey from the initial recognition of symptoms to the diagnosis, the communication and delivery of the diagnosis, and the post-diagnosis services they accessed. They were also encouraged to share the most difficult aspects of living with and caring for someone with LBD and provide suggestions for improving the care process.
Healthcare professionals were asked about their roles in the pathway for LBD, diagnosing if applicable and managing LBD, including their experiences with referral pathways, the availability of resources, and the level of collaboration across disciplines. They were also invited to discuss what they perceived as gaps in the care pathway and what changes they would recommend improving the pathway for individuals living with LBD and their care partners.
Interviews were conducted either over the phone, via video call, or in person, based on the participants’ preferences from January 2024 to March 2025. Interviews typically lasted between 60 and 90 min. All interviews were recorded with consent and transcribed verbatim.
Data analysis
We conducted a reflexive thematic analysis, following the most recent guidelines outlined by Braun and Clarke (2021)30,31. Our approach was inductive and iterative, aiming to develop a nuanced understanding of the diagnostic and care pathways for LBD in Ireland. Codes and thematic categories were managed using Microsoft Excel to organise and track coding decisions.
The analytic process began with repeated readings of the transcripts to ensure familiarisation with the data. One researcher led the initial coding, with a second team member independently reviewing a subset of transcripts to enhance the credibility and trustworthiness. Coding decisions and thematic development were discussed and refined in regular team meetings, with discrepancies resolved through collaborative dialogue and reference to relevant literature on dementia care and health systems.
Thematic categories were developed around key domains of the care experience, including recognition and diagnosis, navigation of services, post-diagnostic support, and the emotional and structural challenges described by participants.
This study adhered to the COREQ (Consolidated Criteria for Reporting Qualitative Research) 32-item checklist to support transparency and rigour in reporting32.
This study was approved by the Trinity College Health Policy Management/Centre for Global Health committee in March 2023 (for conducting interviews with care partners) and June 2024 (for conducting interviews with healthcare professionals). Informed consent was obtained from all participants, and confidentiality was maintained throughout the study by anonymising all interview data.
Discussion
The primary aim of this study was to gain an in-depth understanding of the lived experiences of care partners and healthcare professionals as they navigate the diagnostic and post-diagnostic care pathways for LBD in Ireland, complementing the perspectives of people living with LBD explored in our earlier work25. The focus was on identifying key challenges, supports, and recommendations for improvement.
This study reveals interconnected systemic issues in the diagnosis and support for LBD in Ireland. Drawing from care partner and healthcare professional perspectives, the findings point to a fragmented care system, inconsistent clinician knowledge, and limited post-diagnostic supports. Importantly, our findings show that these issues are not isolated, rather, systemic fragmentation, knowledge gaps, and informal coordination are deeply interconnected, each reinforcing the other and shaping the lived experience of LBD care in Ireland. Further, these issues are not unique to Ireland33,34, but in this context, they are exacerbated by the absence of national standardised LBD-specific frameworks and uneven resource allocation.
Participants described a health system in which families were often left to navigate the LBD care journey alone. Diagnostic pathways were unclear, service responsibilities overlapped, and follow-up was inconsistent or absent. Care partners frequently acted as de facto care coordinators, with no formal support. These findings echo the De-Stress study that found that nearly half of spousal care partners spent all their waking time providing caring, with many experiencing high levels of depression and anxiety due to inadequate professional support structures35.
Healthcare professionals similarly reported working around resource and structural constraints, gaps in LBD-specific training, relying on personal networks or informal coordination to meet patient needs. Healthcare professionals further expressed their own difficulties in delivering care within an under resourced and inconsistently structured environment. As noted in previous research this reliance on workaround strategies reflects a system struggling to meet the complex demands of dementia care36. Alongside these system-level weaknesses, younger individuals with LBD faced an additional layer of exclusion from services designed around older populations.
Care partners supporting younger individuals with LBD highlighted the unsuitability of current dementia services. Eligibility criteria based on age, inappropriate nursing home environments, and a lack of peer support created barriers that intensified the emotional and financial burden. Participants emphasised the need for care to be needs-led rather than age-restricted, particularly for conditions like LBD where young-onset is not uncommon37,38. As one participant noted, existing supports often assumed an “older age” context that failed to reflect their lived experience.
These findings align with broader research indicating that individuals with young-onset dementia frequently face systemic challenges in accessing appropriate services39,40. Studies have highlighted that services are often designed with older populations in mind, leading to environments and activities that may not resonate with younger individuals’ interests and life stages41. Additionally, restrictive eligibility criteria based on age can exclude younger individuals from accessing necessary support42. Healthcare professionals have also reported difficulties in finding suitable care placements for younger individuals, as many facilities cater predominantly to older adults43.
Irish policy acknowledges this mismatch44. The Health Service Executive (HSE) has noted that younger people with dementia face challenges in accessing appropriate services yet reforms are slow to materialise45. Despite these challenges, participants also identified key sources of support and resilience emerging from communities and informal networks.
In the absence of formal structures, community-based supports such as dementia cafés, Alzheimer’s Society initiatives, and Men’s Sheds provided vital lifelines. These grassroots efforts were frequently praised for offering both practical support and opportunities for dignity, understanding, and solidarity among peers in the face of a complex and misunderstood condition providing accessible, non-clinical supports that enhance quality of life and delay the need for more intensive interventions46. Research from Europe and the US confirms the value of peer-led interventions in dementia care, particularly in settings with stretched professional resources47,48,49,50.
For instance, peer-led support groups have been shown to provide emotional support, shared experiences, and a sense of community among caregivers of individuals with Parkinson’s disease without dementia, a condition with overlapping features to LBD47. Additionally, initiatives like the Peer Support Workers (PSW) programme in dementia care across several European countries have demonstrated the effectiveness of trained peers in providing advocacy and support, enhancing the quality of care, particularly in settings with stretched professional resources48. Evidence suggests that participation can improve self-worth, reduce loneliness, and enhance community belonging49,50.
While peer support offers vital relief, it cannot fully compensate for the lack of formal system integration and professional expertise, highlighting the interconnectedness of these challenges. A recurring theme was the limited knowledge of LBD among healthcare professionals, particularly regarding its early and atypical presentations. While the study didn’t use a formal knowledge-attitude-practice (KAP) framework, it was evident that many healthcare professionals involved in the care pathway were only partially familiar with the broader complexity of LBD. Many tended to remain within the boundaries of their own specialty, and even within the same professional role there were differing views about when and how to involve allied health services. This reflects broader training gaps and a siloed service structure, where professionals often focus on their immediate remit rather than the broader, multidisciplinary needs of those living with LBD.
These findings echo Agarwal et al. 51 and Armstrong et al. 52 who found that throughout the world LBD remains poorly understood, with many clinicians unfamiliar with its diverse symptomatology, leading to misdiagnoses and delayed treatment. Similarly, Rañola53 found that even with revised diagnostic guidelines, detection rates in routine clinical settings remain low due to poor familiarity with the condition’s diverse presentations53.
Without a clear referral process and training protocols, many healthcare professionals reported frustration at being “looped into diagnostics” without the resources to contribute meaningfully. This patchwork model of care leave families bore much of the coordination burden themselves. These findings reinforce calls for widespread healthcare professionals’ education and the establishment of mapped integrated model of care, with general practice as a supported frontline player.
One of the most consistent observations across both care partner and healthcare professional interviews was the pivotal role of general practice (GP) and primary care in initiating and sustaining the care pathway. In rural regions particularly, GPs were frequently the first, and sometimes only, consistent point of support. Despite being the initial point of contact for many families, they were often under-informed about LBD-specific symptom profiles and lacked access to timely referral pathways due to resources. This aligns with findings from Fagan (2017), which noted variability in memory service access across Ireland, particularly for non-Alzheimer’s dementias54. International studies have similarly found that primary care clinicians frequently struggle to differentiate LBD from other dementias, leading to misdiagnosis or inappropriate referrals55.
Participants in this study consistently called for clearer diagnostic guidance and better integration of primary care teams into shared-care models. While recent developments such as the Integrated Care Programme for Older Persons (ICPOP) hubs represent important steps towards improving acute care and reducing hospital admissions, participants noted that these services do not consistently provide continuous support throughout the full course of LBD. Communication between services remained uneven, and referral pathways were especially unclear for those with young-onset or atypical symptom presentations56.
Taken together, these findings illustrate a cycle in which systemic fragmentation and knowledge gaps among healthcare professionals reinforce one another, leaving care partners to fill the gaps through informal coordination and community supports. Addressing any one of these challenges in isolation is unlikely to be sufficient, rather, a coordinated, system-wide response is needed to improve the diagnostic and post-diagnostic journey for people with LBD and their families.
While many of these challenges - such as diagnostic delays, fragmented post-diagnostic support, and the significant emotional and practical burden on care partners - resonate with experiences reported across various forms of dementia57,58,59, our findings also illuminate aspects that are particularly pronounced or unique to the LBD care pathway. The fluctuating and complex symptom profile of LBD, encompassing cognitive, motor, and neuropsychiatric features, often leads to a distinct pattern of early symptom misattribution and prolonged diagnostic odysseys. For instance, the misinterpretation of visual hallucinations or fluctuations in alertness as signs of other conditions, as highlighted in our findings, appears to be a more prominent feature in LBD compared to, for example, typical Alzheimer’s disease.
Furthermore, the consistent reports of limited LBD-specific expertise and inconsistent professional training among healthcare providers suggest a particular gap in the healthcare system’s preparedness for this less common, yet highly complex, dementia subtype. This lack of specialised knowledge, coupled with the diagnostic ambiguity inherent to LBD, contributes to unique challenges in establishing clear care pathways and ensuring appropriate, timely interventions.
Compared to models in the UK, Canada, and the US, Ireland is still developing its approach to structured diagnostic and post-diagnostic support for LBD. For example, the UK’s Diagnosing Advanced Lewy Body Dementia Using a Multidisciplinary Team Approach (DIAMOND Lewy) programme and the National Institute for Health and Care Excellence (NICE) guidelines offer clinicians standardised diagnostic tools and care pathways, while Canada’s First Link and the US-based LBD Association provide coordinated follow-up, education, and advocacy33,34. Ireland’s current system is evolving, with many families and professionals often navigating care pathways without formalised frameworks, indicating an opportunity for further development.
Encouragingly, efforts to enhance LBD care in Ireland have recently gained momentum. The EMERALD Lewy project, the country’s first initiative dedicated exclusively to LBD, is now underway60. With continued support, this initiative has great potential to establish an integrated, needs-led model of LBD care in Ireland, helping to address the complexity of this condition and align national practice with international advances60,61.
This study offers rich, in-depth insights into the diagnostic and post-diagnostic experiences of both care partners and healthcare professionals involved in LBD care in Ireland. While we aimed for thematic saturation, we primarily assessed the adequacy of our sample based on the concept of information power27. The sample included participants from a range of counties and diverse professional backgrounds, which enhanced the relevance and credibility of the findings. However, some limitations remain. Geographical representation was uneven, with certain regions most notably the Midlands less well represented, which may mean that regional differences in service access or delivery were not fully captured. Additionally, there is the possibility of selection bias, as those who participated may have been more likely to share challenging or negative experiences. This does not diminish the validity of their accounts but may have influenced the overall tone of the findings. Another limitation is the absence of perspectives from social workers and public health nurses, whose roles are central to dementia care coordination in the community and limited representation of GPs. While care partners frequently identified GPs as the first point of contact, our findings regarding the GP role should be interpreted with caution, as they may not fully capture the diversity of GP perspectives and experiences. In line with recent qualitative research guidance27, we recognise that the limited GP input reduces the information power regarding this key group. Future research should seek to include a broader range of GPs to more fully explore their perspectives and contributions to the LBD care pathway.
The findings of this study highlight important opportunities to further strengthen how LBD is diagnosed and supported in Ireland. There is a clear benefit to developing a national, standardised care pathway for LBD that ensures consistency across regions, includes clear referral guidelines, and addresses both typical and young-onset presentations. Given that general practitioners are often the first point of contact for families, enhancing their role in the diagnostic process will be key. This can be supported through continued investment in targeted GP and frontline staff training, focusing on recognising the full spectrum of LBD symptoms beyond standard cognitive assessments. Strengthening the primary care response is essential to creating a more equitable and effective national care pathway, including providing primary care teams with clear protocols and access to multidisciplinary support. Efforts to reduce regional variation in access to diagnosis, follow-up, and specialist input remain important, alongside clearer role definitions within the pathway to improve coordination across sectors. Any national framework should also be age-inclusive, recognising the specific needs of younger individuals with LBD who may currently face gaps in service.
Equally important is continued investment in structured post-diagnostic supports, not only for individuals with LBD but also for their care partners. Participants described significant emotional strain, burnout, and financial challenges, often with limited formal support. Expanding access to ongoing supports such as counselling, respite services, financial guidance, and peer-led education will be critical to sustaining family-based care and reducing long-term stress. The development of dedicated roles such as LBD nurse specialists or care coordinators could further assist families in navigating complex systems with greater ease.
Irish health policy’s emphasis on ageing in place as a key goal of dementia care (Department of Health, 2024) aligns well with the needs of those living with LBD62. However, to make ageing at home sustainable, adequate clinical, emotional, and financial supports for care partners are essential. Many care partners, often older spouses or adult children, manage significant physical and emotional challenges themselves. As one participant noted, “the system just totally takes you for granted…Yeah, it should never be assumed that a person wants to do it either. Just because you’re married to somebody doesn’t mean that you want to be their 24-hour carer.” (Care Partner P8). Strengthening support for care partners will be key to making home-based care a viable and positive option for families living with LBD.
Finally, while community and voluntary organisations remain invaluable, they must complement, not substitute, statutory provision. Their contributions should be recognised and integrated within a more robust, publicly supported system of dementia care.
Data availability
Due to the sensitive nature of the interviews and privacy commitments made to participants, the data generated during this study are not publicly available.
References
Desai, U. et al. Epidemiology and economic burden of Lewy body dementia in the United States. Curr. Med. Res. Opin. 38, 1177–1188 (2022). p.
Prasad, S. et al. Recent advances in Lewy body dementia: a comprehensive review. Dis.a-Mon. 69, 101441 (2023).
Walker, Z. et al. Lewy body dementias. Lancet 386, 1683–1697 (2015). p.
McKeith, I. G. et al. Diagnosis and management of dementia with Lewy bodies. Neurology 89, 88–100 (2017).
Zhu, C. W. et al. Apathy in Lewy body disease and its effects on functional impairment over time. Front. Neurol. 15, 1339190 (2024)
Hogan, D. B. et al. The prevalence and incidence of dementia with Lewy bodies: a systematic review. Can. J. Neurol. Sci. 43, S83–S95 (2016).
Gobal Brain Health Institution. Lewy Body Ireland | Global Brain Health Institute. Available from: https://www.gbhi.org/projects/lewy-body-ireland. (2024).
The Alzheimer Society of Ireland. Dementia with Lewy Bodies. Available from: https://alzheimer.ie/dementia-with-lewy-bodies/. (2025).
Thomas, A. J. et al. Revision of assessment toolkits for improving the diagnosis of Lewy body dementia: the <scp>DIAMOND</scp> Lewy study. Int. J. Geriatr. Psychiatry 33, 1293–1304 (2018).
Bock, M. A. et al. Apathy and risk of probable incident dementia among community-dwelling older adults. Neurology 95, e3280–e3287 (2020).
Burghaus, L. et al. Hallucinations in Neurodegenerative Diseases. CNS Neurosci. Ther. 18, 149–159 (2012).
de Mendonça Lima, C. A. & Kuhne, N. Psychosocial Rehabilitation in Mental Health Care for Older Adults. In Primary Care Mental Health in Older People. 351–362, https://doi.org/10.1007/978-3-030-10814-4_25 (Springer International Publishing, 2019).
Sezgin, M. et al. Parkinson’s disease dementia and Lewy body disease. Semin. Neurol. 39, 274–282 (2019).
Bjoerke-Bertheussen, J. et al. Neuropsychiatric symptoms in mild dementia with lewy bodies and Alzheimer’s disease. Dement. Geriatr. Cogn. Disord. 34, 1–6 (2012).
Chin, K. S., Teodorczuk, A. & Watson, R. Dementia with Lewy bodies: challenges in the diagnosis and management. Aust. N.Z. J. Psychiatry 53, 291–303 (2019).
Boland, E. et al. The high cost of care and limited evidence on cost-effective strategies for Lewy body dementia: systematic review of evidence. BJPsych Open 10, e20 (2024).
McKeith, I. G. et al. Diagnosis and management of dementia with Lewy bodies. Neurology 65, 1863–1872 (2005).
Ballard, C. et al. Atypical antipsychotics for the treatment of behavioral and psychological symptoms in dementia, with a particular focus on longer term outcomes and mortality. Expert Opin. Drug Saf. 10, 35–43 (2011).
Culo, S. et al. Treating Neuropsychiatric Symptoms in Dementia With Lewy Bodies. Alzheimer Dis. Assoc. Disord. 24, 360–364 (2010).
Abdelnour, C. et al. Dementia with Lewy Bodies drug therapies in clinical trials: systematic review up to 2022. Neurol. Ther. 12, 727–749 (2023).
Livingston, G. et al. Dementia prevention, intervention, and care: 2020 report of the Lancet Commission. Lancet 396, 413–446 (2020).
Department of Health, The Irish National Dementia Strategy. Department of Health. https://www.hse.ie/eng/dementia-pathways/files/the-irish-national-dementia-strategy.pdf (2014).
National Academies of Sciences, E. & Medicine. Meeting the Challenge of Caring for Persons Living with Dementia and Their Care Partners and Caregivers: A Way Forward (eds Larson, E. B. & Stroud, C.) 228, https://doi.org/10.17226/26026 (The National Academies Press, Washington, DC, 2021).
Beatie, B. E. et al. Caregiver identity in care partners of persons living with mild cognitive impairment. Dementia 20, 2323–2339 (2021).
Conlon, J., Kinchin, I. & Leroi, I. Healthcare pathways and social experiences of Lewy body dementia and Alzheimer’s disease in Ireland. Soc. Sci. Med. 383, 118510 (2025).
Harvey, R. J. The prevalence and causes of dementia in people under the age of 65 years. J. Neurol. Neurosurg. Psychiatry 74, 1206–1209 (2003).
Malterud, K., Siersma, V. D. & Guassora, A. D. Sample size in qualitative interview studies:guided by information power. Qual. Health Res. 26, 1753–1760 (2016).
Larsson, V. et al. Living with dementia with Lewy bodies: an interpretative phenomenological analysis. BMJ Open 9, e024983 (2019).
Lee, C.-Y. et al. Quality of life in patients with dementia with Lewy Bodies. Behav. Neurol. 2018, 1–7 (2018).
Braun, V. & Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 3, 77–101 (2006).
Braun, V. & Clarke, V. One size fits all? What counts as quality practice in (reflexive) thematic analysis?Qual. Res. Psychol. 18, 328–352 (2021).
Tong, A., Sainsbury, P. & Craig, J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int. J. Qual. Health Care 19, 349–357 (2007).
Alzheimer Society of Canada. First Link®: Help for people living with dementia and care partners. Available from: https://alzheimer.ca/en/help-support/programs-services/first-link. (2025).
Thomas, S. Interactive dementia pathway toolkit. Neurology Academy. https://neurologyacademy.org/dementia-academy/projects/interactive-dementia-pathway-toolkit (2016).
Trinity College Dublin. High levels of mental health issues for spousal carers of people with dementia. 2017 [cited 2025; Available from: https://www.tcd.ie/news_events/articles/high-levels-of-mental-health-issues-for-spousal-carers-of-people-with-dementia/.
Ryan, L. Accessing community dementia care services in Ireland: Emotional barriers for caregivers. Health Soc. Care Community 29, 1980–1989 (2021).
Kuruppu, D. & Matthews, B. Young-Onset Dementia. Semin. Neurol. 33, 365–385 (2013).
Sim, J. et al. Clinical manifestations of early-onset dementia With Lewy bodies compared with late-onset dementia with Lewy bodies and early-onset Alzheimer Disease. JAMA Neurol. 79, 702 (2022).
Millenaar, J. K. et al. The care needs and experiences with the use of services of people with young-onset dementia and their caregivers: a systematic review. Int. J. Geriatr. Psychiatry 31, 1261–1276 (2016).
Rabanal, L. I. et al. Understanding the needs and experiences of people with young onset dementia: a qualitative study. BMJ Open 8, e021166 (2018).
Giebel, C. Young-onset dementia and its difficulties in diagnosis and care. Int. Psychogeriatr. 34, 315–317 (2022).
Novek, S. & Menec, V. Conceptualizing access to community-based supports from the perspectives of people living with young onset dementia, family members and providers. Dementia 22, 180–196 (2023).
Giebel, C. et al. Evaluating a young-onset dementia service from two sides of the coin: staff and service user perspectives. BMC Health Serv. Res. 20, 187 (2020).
Oireachtas Joint Committee on Health. Health Needs of Persons with Dementia and the Services Available: Discussion. [cited 2025; Available from: https://www.oireachtas.ie/en/debates/debate/joint_committee_on_health/2024-02-07/3/. (2024).
Health Service Executive. Younger Onset Dementia. Available from: https://www.hse.ie/eng/dementia-pathways/care-pathways/younger-onset-dementia/. (2020).
Begley, E., Gibb, M., Kelly, G., Keogh, F. & Timmons, S. Model of Care for Dementia in Ireland. Tullamore: National Dementia Services. https://www.hse.ie/eng/services/publications/olderpeople/model-of-care-for-dementia-in-ireland.pdf (2023).
Abendroth, M., Greenblum, C. A. & Gray, J. A. The value of peer-led support groups among caregivers of persons with Parkinson’s disease. Holist. Nurs. Pract. 28, 48–54 (2014).
Tsatali, M. et al. Peer support workers as an innovative force in advocacy in dementia care: a transnational project delivered in Norway, Greece, Italy, and Romania. J. Multidiscip. Healthc. 17, 3155–3165 (2024).
McGrath, A. et al. Sheds for life: health and wellbeing outcomes of a tailored community-based health promotion initiative for men’s sheds in Ireland. BMC Public Health 22, 1590 (2022)
Sullivan, M. P. et al. Peer support for people living with rare or young onset dementia: An integrative review. Dementia 21, 2700–2726 (2022).
Agarwal, K. et al. Lewy body dementia: overcoming barriers and identifying solutions. Alzheimer’s. Dement. 20, 2298–2308 (2024).
Armstrong, M. J. et al. Clinical care and unmet needs of individuals with dementia with lewy bodies and caregivers. Alzheimer Dis. Assoc. Disord. 35, 327–334 (2021).
Rañola, M. B. Lewy body Dementia: what are the challenges of early and accurate diagnosis?Australas. J. Neurosci. 32, 40–51 (2022).
Fagan, M. Do patients in the Republic of Ireland face a postcode lottery for dementia tests? Available from: https://www.thedetail.tv/articles/patients-in-republic-face-patchy-memory-services-and-lengthy-waits. (2017).
Taylor, J.-P. et al. New evidence on the management of Lewy body dementia. Lancet Neurol. 19, 157–169 (2020).
Health Service Executive. A Practical Guide to the Local Implementation of Integrated Care Programmes for Older Persons. https://www.hse.ie/eng/services/publications/clinical-strategy-and-programmes/a-practical-guide-to-the-local-implementation-of-integrated-care-programmes-for-older-persons.pdf (2017).
Bunn, F. et al. Psychosocial factors that shape patient and carer experiences of dementia diagnosis and treatment: a systematic review of qualitative studies. PLOS Med. 9, e1001331 (2012).
Brodaty, H. & Donkin, M. Family caregivers of people with dementia. Dialogues Clin. Neurosci. 11, 217–228 (2009).
Davies-Abbott, I. et al. The diagnostic pathway experiences of people living with rare dementia and their family caregivers: a cross-sectional mixed methods study using qualitative and economic analyses. Int. J. Environ. Res. Public Health 21, 231 (2024).
Trinity College Dublin, Hope for ‘the most common form of dementia that no-one has heard of’. https://www.tcd.ie/news_events/articles/2024/hope-for-the-most-common-form-of-dementia-that-no-one-has-heard-of/ (2024).
O’Regan, E. New hope for people with dementia as €2.5m research project to get underway at Trinity College. Irish Independent. https://www.independent.ie/irish-news/new-hope-for-people-with-dementia-as-25m-research-project-to-get-underway-at-trinity-college/a302358145.html#:~:text=Irish%20News-,New%20hope%20for%20people%20with%20dementia%20as%20%E2%82%AC2.5m,get%20underway%20at%20Trinity%20College&text=Researchers%20in%20Dublin%20have%20been,%2Done%20has%20heard%20of%22 (2024).
Department of Health. Minister for Mental Health and Older People launches national rollout of the Healthy Age Friendly Homes Programme. Available from: https://www.gov.ie/en/department-of-health/press-releases/minister-for-mental-health-and-older-people-launches-national-rollout-of-the-healthy-age-friendly-homes-programme/. (2024).
Acknowledgements
The authors would like to sincerely thank all the care partners and healthcare professionals who shared their experiences and insights for this study. We are also grateful to the individuals and organisations who supported recruitment, including the Parkinson’s Association of Ireland, TeamUp, and the broader community and clinical networks that helped connect us with participants. This research was supported by Health Research Board of Ireland Applied Programme Grants (APRO) Award (grant number 9745).
Author information
Authors and Affiliations
Contributions
J.C. conducted the interviews, analysed the data, and drafted the original manuscript. I.K. supervised the research process, served as the second coder, contributing to data analysis by reviewing and validating coding frameworks, supporting theme development, and participating in interpretive discussions to ensure reflexive rigour. I.K. also managed the revisions and undertook rewriting during the review process. IL reviewed the manuscript critically. All authors read, reviewed, and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Conlon, J., Kinchin, I. & Leroi, I. Lived experiences of Lewy body dementia diagnosis and care in Ireland. npj Dement. 2, 2 (2026). https://doi.org/10.1038/s44400-025-00050-y
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s44400-025-00050-y