Abstract
Mental health apps are effective for young people, but uptake remains low, especially for minoritized youth. This scoping review of 114 studies examines youth and stakeholders’ participation and diversity, equity, and inclusion (DEI) considerations in publications on smartphone applications for youth (10 to 25 years) for depression, anxiety, and/or suicidal ideation. Our narrative synthesis reveals limited youth participation: more than half of the studies do not include youth in app development, with limited details about the extent of involvement. DEI considerations remain overlooked: factors such as cultural adaptation, literacy, disability, internet access, and privacy are each reported by less than 20% of studies. Reporting on ethnic/racial and sociodemographic characteristics was inconsistent, with an overrepresentation of university populations. Considering participation and DEI factors when designing, testing, and implementing youth mental health apps is crucial to enhance their relevance, reach, and adoption. We provide recommendations for equitable youth-tailored mental health app development and implementation.
Similar content being viewed by others
Introduction
One in five youth, aged 10 to 25, experience mental health problems, such as anxiety and depression1. Yet less than 50% of young people receive treatment2. Digital mental health (DMH), such as smartphone apps, could be key to tackling this treatment gap3. Mental health apps show promising outcomes for young people4,5,6. Yet, there is limited evidence for long-term outcomes and cost-effectiveness7. Further, use and adoption in the real-world is low--especially among minoritized youth and in low-resource settings8. As such, factors like accessibility, cost, safety, and cultural responsiveness are important for the sustainability of mental health apps beyond the implementation phase7. Therefore, to better reach marginalized youth, such as racial/ethnic minorities, LGBTQIA+, and youth from lower socioeconomic status households, inclusive design is critical to better address treatment gaps by ensuring design and delivery needs are met for these typically excluded populations9,10.
Diversity, equity, and inclusion (DEI) in DMH promotes a wide spectrum of human differences (diversity), ensures fair and impartial treatment (equity), and fosters participation and respect for all individuals (inclusion)11. Lack of attention to DEI is an important implementation barrier12. However, only 58% of mental health app evaluation frameworks consider at least one criterion related to DEI, such as access to digital tools, diverse content adapted to different cultures, languages, and literacy levels13. Related to these design gaps, culturally and linguistically diverse young people report that they do not feel represented in mental health apps14. Further, most reviews have not explored the effectiveness of DMH apps among minoritized groups generally7, and many real-world implemented apps are tested on healthy young adult samples (i.e., university students)15. In addition, co-design, defined by Kilroy and colleagues as a ‘creative approach where different stakeholders, such as end-users and clinicians, are actively involved in the development, design and implementation of intervention’16, may improve engagement with DMHs16. However, a recent review of 30 DMH co-design studies noted that these methods are inconsistently applied with varying levels of inclusion17. This suggests a lack of inclusive and equitable design practices and limited representation in DMH app academic research. Critically, to the best of our knowledge, the field lacks a systematic overview of these gaps.
Numerous academics have called for increasing attention to DEI considerations in DMH targeting youth, including co-designing with youth, reaching minoritized groups, reporting ethnicity and gender identity, and adhering to DEI principles7,12,14,18. These are seen as crucial steps to tackle the lack of fit of apps to the needs of young people from diverse backgrounds and increase uptake and engagement. Nevertheless, DEI in digital health faces significant challenges. As argued by Kamalumpundi et al. (2024), these challenges may stem from ‘deeply rooted institutional cultures, and a lack of understanding about the true meaning of DEI and its tangible benefits to society’ 19. This underscores the urgency of reviewing current research gaps to help us chart a path forward.
Considering the gap in knowledge on this topic, we conducted a scoping review to examine reporting on: (1) the participation of youth and other key players in the app design and development process; (2) DEI considerations in the development and evaluation of apps; (3) the prevalence of ethnic minoritized youth (racial/ethnic diversity), low-income youth (socioeconomic diversity), and youth with diverse gender identities, in apps. We reviewed studies describing apps for youth that target depression and anxiety disorders, which are among the leading causes of illness and disability among adolescents, and suicidal ideation, a leading cause of death (ages 15 to 29)20. This review is timely, as symptoms of depression, anxiety, and suicidal ideation spiked and remained high in young people after the onset of the COVID-19 pandemic1. We grounded this review in a framework previously developed by Ramos and colleagues (2021) for mental health app assessment, adopted from the culturally informed design framework13. Based on the results of our findings, we provide recommendations for a more equitable DMH ecosystem for youth.
Results
Included studies
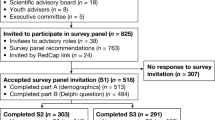
After removing duplicate articles, 5097 titles and abstracts were screened, and 264 studies underwent full-text review, with 114 studies ultimately included. No references were added by manual searching of reference lists. See Fig. 1 for the PRISMA flow diagram.
This figure shows the PRISMA flow diagram, to depict the flow of information through the different phases of a systematic review. It shows the number of publications identified, included and excluded, and the reasons for exclusions from the review.
Study characteristics
While studies published since 2009 were eligible for inclusion, most of the studies were published in 2022 through 2024 (see Fig. 2).
This figure shows the total number of included studies in the review by their year of publication.
The United States (U.S.) was the most represented (37.7%), followed by Australia (12.2%), China (7.0%), and the United Kingdom (7.0%; See Table 1 for characteristics of the included studies). The most common settings were university (28.0%), community-based (25.4%), and school-based interventions (13.1%), followed by clinical care (12.5%, e.g., outpatient mental health clinics). Two studies were conducted in a youth shelter, and four studies were recruited online, using social media recruitment. Studies targeted a range of related outcomes. A subset targeted only depression (17.5%), anxiety (14.0%), anxiety and depression simultaneously (15.7%), and suicide related outcomes (5.2%). Many studies additionally targeted other outcomes, such as rumination, stress, self-harm, and general mental well-being. Most studies used various approaches, with cognitive behavioral therapy (CBT) being the most common, either alone (24.6%) or in combination with other strategies (20.2%), such as mindfulness, self-monitoring, and behavioral activation. Most studies were randomized controlled trials (37.7%), followed by pilot trials/studies (23.7%), and development/design studies (10.5%).
Sample demographics of studies
The average age for participants was 18.3 (see Table 2). The average number of female participants across all studies was 66.7%. Most studies included more female than male participants (81.6%), and 33.3% reported participants identifying beyond the binary categories (e.g., intersex, non-binary, transgender, and gender nonconforming). In one study, non-binary participants were the majority gender identity category21. Most studies did not provide data on participants’ or their family’s income (89.5%). Immigration statuses were reported in 61% of studies (e.g., ‘born Australian’, ‘international students’, and ‘foreign nationals’).
Almost half (47.4%) did not report race/ethnicity. In 36.8% of studies, the majority identified as white (studies mainly in the US, Europe, Australia, and New Zealand). Additionally, in 6.1% of studies, participants identified primarily as Asian (conducted mainly in Japan, Korea, China), followed by 3.5% whose participants identified primarily as Black or African American (in the U.S. and Zimbabwe). Finally, participants in 3.5% primarily identified as Indigenous (conducted in Australia and New Zealand).
DEI Criteria
Most studies did not discuss any DEI criteria (52.6%; see Supplementary Table 2). The remaining studies reported one or more DEI criterion. No single criterion was reported >20% of the time (Fig. 3). Below, we describe the distribution of DEI with examples from the studies.
This figure shows the percentage of studies that reported about each Diversity, Equity, and Inclusion (DEI) Criterion.
Only 15.8% of studies mentioned measures to reduce the need for internet connectivity, such as using the apps offline, pushing data to servers once reconnected22,23,24,25,26,27,28,29, or reconfigurations for unreliable internet speeds in low resource settings23. The importance of offline use was also discussed in co-design sessions30,31. Data usage reduction strategies were mentioned in 12.3% and included offline functionality and efficient background protocols24. Some mentioned high data usage as a barriers32, or provided participants with a phone with data during the study25,33,34,35.
Additionally, 20% of studies described app costs as a consideration. In most studies that tested an app, it was available for free, but the cost was not explicitly discussed. Some formative studies described high cost as a barrier to use36,37, or described making their app freely available for scalability, currently38, or as a future goal39. Only 3.5% of studies described methods to ensure the app runs on low-end devices, such as a mobile-friendly link to be used on any internet-accessible device40 or selecting certain platforms Table 3 because of the availability of low-cost devices41.
Language adaptations were discussed in 6% of studies. These adaptations included providing English text with Konkani or Hindi voice-over options42, a choice of multiple languages in a multi-country trial43, or English, with Aboriginal language words, given the large number of Aboriginal languages22,44. Only 9.6% discussed literacy adaptations, which included the need for a youth copy editor to ensure appropriate reading level, content for various learning styles (e.g., videos, audio)30, more images and less text45, reducing the lexicon of emotion words, emoticons, and speech-to-text functions42. Just 5.3% mentioned accommodating to disabilities such as dyslexia25,29, color-blind or visual impairments46, or learning disabilities30. Examples include adapting the font size and line spacing to accommodate dyslexic youth in consultation with a user steering group29.
Regarding identity tailoring, 14.9% of studies described features, such as customizable avatars (skin, eye, hair color, clothing)47, pronoun selection48, and character choices reflecting users’ situations30,49,50. One study allowed users to choose mentor demographics, including gender identity, LGBTQIA+ status, and racial/ethnic identity51.
Only 7.8% of studies addressed the importance of representing diverse genders, cultures, abilities, and skin tone variety in app characters (e.g., refs. 29,30), though it was often unclear if these were implemented. Some studies did not mention diverse representation explicitly, but app images showed youth with varied skin tones and gender identities (e.g., refs. 27,52).
Only 11.4% reported cultural adaptations, such as local language, colors, landscapes, and culturally relevant stories. Examples included apps using Aboriginal language and Northern Territory designs in Australia22,31, a Maori welcome song in New Zealand53, and Indigenous/LGBTQIA+ helplines for Canadian undergraduates54. Other adaptations included adding family-centered values in China55, including culturally relatable and gender-tailored stories in India42 and developing 32 app versions to tailor to different European cultures43. One U.S. study tailored content for sexual minority youth, including resources and coping strategies for negative societal views and internalized homonegativity56.
App privacy considerations were mentioned in 20% of studies. These included adherence to privacy laws (HIPAA in the US24 and EU GDPR23), encryption34,40,57, using a PIN for access39, and local phone storage24,58. Some studies mentioned easy access to privacy policies30, privacy policies in adolescent-friendly language42 and 5th-grade reading levels48, and phone security training for youth33.
Youth and stakeholder involvement
Youth involvement in design and development activities was reported in 42.9% of studies. In 12.1% of studies, youth were involved in the design (formative studies), with 2 of these involving youth after a first app version was already developed (i.e., Minimum Viable Product; the most basic version of the app that includes only the core features). In 29.9% youth were involved in both the design and evaluation. Of these, six studies included participants after a first version was developed.
See Fig. 4 for an overview of youth involvement activities used by studies.
This figure shows the variety of youth activities, such as co-creation sessions, focus groups, individual interviews, and questionnaires, across the various design stages of the included studies.
Supplementary Table 3 shows an overview of youth and other stakeholder involvement for each study. Design and Development activities with youth mainly included co-creation sessions, focus groups, individual interviews, and questionnaires. Six studies included youth advisory boards22,31,43,48,50,59, and 2 of these (in the context of the Aboriginal and Islander Mental Health Initiative for Youth) had youth researchers in the study team22,31. Overall, many studies described few details of participatory methods or activities, how the youth’s inputs influenced app design, and incomplete reports on the youth involvement.
Of note, five studies37,38,60,61,62 reported testing existing apps that were developed commercially. We could not find information on whether these were codesigned with youth (or other stakeholders), thus also coded them as no involvement. Some studies adopted multiple youth-involved activities; therefore, the total counts of activities exceed the number of studies.
Some form of stakeholder involvement was reported in 51.8% of studies, which mainly consisted of stakeholder involvement in the design and evaluation of via focus groups, interviews, co-design workshops, surveys, or prototyping (25.9% of studies). Stakeholders included mental health professionals, caregivers, social workers, designers, and developers, with clinicians most frequently involved (see Table 2).
Discussion
To the best of our knowledge, this is the first scoping review to comprehensively assess youth participation and DEI considerations in the design, evaluation, reporting, and co-design of DMH apps for youth targeting depression, anxiety, and/or suicidal ideation. Our findings from 114 studies revealed that youth are often excluded from app development. Further, few studies explicitly address equity, representation, or cultural relevance in the design or justification of their strategies, and minoritized youth are likely underrepresented.
While it is possible that some DMH were developed with more inclusive methodologies than were reported in outcome papers, over 50% of studies did not report any youth co-design processes. Further, details about the extent of youth and other stakeholder involvement were often sparse. Only a few studies employed equal partnership methods, where youth were engaged as decision-makers63. For example, only six studies used a Youth Advisory Board to inform app design. Notably, only two studies (from the same project) described instances of youth taking the lead in the research process, with dedicated youth researchers on the design team22,31. These studies involved an Indigenous Youth Advisory Group, facilitated by a youth researcher, which provided guidance on study procedures, data interpretation, and ideas for future iterations of the app. Despite calls for increasing youth involvement in DMH18,64, the current literature notes a vast absence of involvement and/or input.
In addition to limited involvement of youth in design, over half of the studies reported no DEI criteria. Critically, among the minority that did report DEI criteria, most reported only a few, and no single DEI criterion was reported more than 20% of the time. Around 10% or fewer addressed internet access, or cultural-, literacy-, and/or disability-adaptations. Privacy considerations were also often omitted, despite their importance for safeguarding young users—particularly those with minoritized identities that might not feel safe sharing their identity or behaviors65. Reporting on sociodemographic characteristics was also inconsistent (e.g., ~50% omitted race/ethnicity, 90% omitted family income). In addition to a lack of DEI criteria, there was an overrepresentation of highly educated (>30% university setting), White, female populations living in higher-income countries. This overrepresentation is problematic for multiple reasons in translating to real-world use of young people (e.g., 89% of youth live in low- and middle-income countries66). Only a few studies in our review explicitly targeted minoritized groups, such as those living in youth shelters or who identify as LGBTQIA+. What is therefore missing is the design and evaluations of these DMH interventions, which are ways to directly address concerns frequently named by racialized, Indigenous, migrant, and/or LGBTQIA+ youth. These concerns include: racialized trauma, cultural alienation, discrimination-related stress, or identity conflict. Put another way, the current findings are unfortunately in line with other recent reviews, such as Litke et al. (2023), who included 10 DMH studies67, noting that cultural inclusiveness in apps for youth are “almost nonexistent.”
To our knowledge, this is the first scoping review of DEI practices in DMH for youth with depression, anxiety, and/or suicidality. Consistent with earlier and similar reviews, the current review echoes that factors of race and ethnicity are under-researched in DMH—perhaps as a result of relying on sampling in university settings that are primarily in high-income regions7,15. Also consistent with previous reports, co-design practices in DMH are inconsistently reported17,68, and identified implementation barriers include accessibility, such as access to digital devices for low-income youth, and lack of privacy and security considerations6.
However, the current review is novel in the literature as a demonstration of how these factors are systematically overlooked in youth DHM research: a lack of DEI. Additionally, we note that this is not a problem isolated to DMH, but broadly to digital delivery of mental and behavioral health interventions for youth. For example, a recent systematic review of 33 digital adolescent obesity prevention and management interventions69 found that most studies did not include equity criteria (as measured by a digital health equity framework that the authors adapted based Richardson70 and Crawford and Sehal71). As such, the current review is a call to action to address the lack of DEI in youth digital health design, evaluation, and implementation moving forward.
The implications of continuing to neglect this call to action and maintaining current methodologies will ultimately perpetuate the unacceptably long research-to-practice gap and waste millions of dollars invested in DMH development and research. First, if the field continues to rely on adult-only designs and neglects DEI factors in design, DMH for youth will continue to be less relevant and accessible in real-world environments. This is especially the case for minoritized groups (e.g., youth in rural areas, without access to higher education, or facing structural exclusion), who are routinely sidelined from both the design and delivery of these interventions8. Second, generalizability is diminished by the lack of diverse participant representation, from inception to implementation and continuing to rely on convenience sampling. Indeed, the current findings mirror long-standing trends in DMH research, where recruitment often occurs in academic institutions or community hubs with built-in infrastructure and digital literacy18. As a result, the perspectives of youth with unmet mental health needs are missing from much of the evidence base and it is likely DMH are poorly suited to their needs. Third, insufficient transparency in reporting undermines the replicability of research and hampers efforts to understand the mechanisms driving intervention effectiveness. For instance, when co-creation processes are poorly documented, it becomes difficult to assess the specific benefits of involving youth in the development process and to determine which participation methods are most effective72. Ultimately, the practices to date have created critical knowledge gaps regarding design requirements, privacy concerns, usability, and real-world effectiveness for diverse youth populations.
Some limitations must be noted. We assessed studies based solely on the information available in peer-reviewed academic articles. Some studies may have considered DEI criteria or sought feedback from youth and stakeholders, but may not have reported these aspects due to a lack of time or space in academic papers. We also included studies at varying stages of development (e.g., co-design, pilot testing, and RCTs), where DEI criteria may not have been equally applicable or emphasized. Furthermore, due to inconsistent reporting of co-design activities and the lack of a clear definition of “meaningful” youth involvement in the DMH field, it was sometimes difficult to determine whether youth were actively involved and to what extent their participation was substantive. Similarly, because of differences in describing racial/ethnic background, education, and income, it was challenging to code the compositions of the sample. Additionally, there is no standardized way to measure DEI in youth digital mental health. Using a different framework may have yielded different results. Despite these challenges, our findings indicate that DEI considerations, youth participation, and inclusive samples remain limited across the full spectrum of DMH development.
Based on our findings, we propose several research priorities for a more equitable youth DMH ecosystem, also shown in Table 4. First, it is essential to involve youth throughout the entire process of DMH development, including design, testing, and implementation. Scientific evidence suggests that youth engagement improves youth mental health services and may lead to better health outcomes, especially for marginalized youth73. Indeed, designing for those with the most barriers and needs improves accessibility for all. Yet, as this study highlights, the current DMH landscape continues to be developed largely without young people’s input.
Second, standards for researcher training and an increased budget for engagement are needed. The field broadly has a limited understanding of the obstacles both practitioners and young people face in co-design and testing processes in DMH apps, especially for underserved populations and youth in low-income countries74. Previous research shows that youth-engagement barriers may include a lack of researcher training, limited funding possibilities, and infrastructural challenges, such as with ethics boards and technical issues75. Some studies in our review, for instance, identified time, budget, software function constraints, and the need to use ‘best practices’ in psychology research, as barriers to incorporating all youth’s suggestions31,43. This highlights the need for standards and training for researchers (e.g., co-design methodologies, rapid qualitative analysis), adequate budgeting for youth engagement, infrastructural changes, and realistic time expectations to incorporate feedback76. Some resources for researchers to engage youth in DMH are emerging (consult for example an overview of youth engagement in general research77 and78 for digital health). User-friendly remote methods, responsive researchers, and parental support can enhance engagement with clinical youth populations79. Advancing our knowledge on how to effectively train researchers to target and enhance engagement with youth, and adapting strategies accordingly, should become a primary research priority that will require established (but modifiable) standards and funds to establish such metrics.
Third, standardizing co-design approaches, including incorporating multiple stakeholder groups, are also needed. Although co-design, user-centered, or participatory design are increasingly considered the best practice in DMH research, there is no standardized approach for applying and evaluating these methods in youth. Our review, in line with other recent work17, found that studies used a variety of terms for co-design methods and implemented them in different ways. Unfortunately, this variability was also accompanied by limited details on the process (perhaps due to space limitations for journal manuscripts). Multi-stakeholder involvement is also a crucial component of co-design that promotes equitable design80. Indeed, youth do not live in a vacuum, and their DMH use and ultimate functioning are impacted by important adults in their lives, such as parents, teachers, or health professionals. Rarely were such stakeholders mentioned in DMH design. Nonetheless, we have observed some promising examples. For instance, one study in our review, Dingwall (2023) formed an Expert Reference Group (ERG) of youth service and research professionals (4 of whom were First Nations Australians)22, which assisted in refining study procedures and interpreting and disseminating findings. While there are steps being taken, more guidance on how researchers should best use co-design, while incorporating the input of varied stakeholders, is critically needed to advance DMH for youth.
Ultimately, the current findings and call to action underscore the importance of better understanding, assessing, and implementing best practices to ensure that these methods are meaningfully integrated into research practice63. This also highlights the need for researcher guidelines or checklists to follow for reporting practices throughout their development process. Indeed, researchers, reviewers, and journals need dedicated tools, guidelines, and frameworks on DEI considerations in the context of youth digital mental health. In the current review, we used a DEI framework proposed by Ramos et al. (2021), originally designed to evaluate mental health apps. However, it remains unclear whether all DEI criteria hold the same level of importance and for which phases of the development cycle they apply. For example, diverse visual representations may not be relevant for apps that do not include pictures or images. Furthermore, there are a variety of models and methods used for cultural adaptation of digital health interventions that also involve a connection between culture and other contextual factors, such as economic conditions and social systems80. Parental consent has also emerged as a barrier to download mental health apps, specifically for marginalized youth81. It is also important to identify which DEI and personalization features matter most to diverse groups of young people. These may also include having autonomy in selecting app content, deciding what personal data to share, and accessing human support when needed.
We may need to establish new DEI criteria specifically for youth, and for each DMH development phase. Our field needs actionable guidelines to help researchers incorporate DEI in every phase of the research. Building on the recommendations of Williams et al. (2025), this may include when the inclusion or exclusion of race, ethnicity, or other sociodemographic characteristics is important for a given analysis; when the inclusion of individuals with specific identities may be necessary; or when it is important to consider social or digital determinants of health or social risk factors82. Recent digital health equity models focused on implementation and equity-focused outcomes have also emerged, which, though not specific to children and young adults, could be drawn on for tailoring to youth mental health implementation research (beyond app design)83.
New guidelines should also consider rapidly changing technologies. Artificial intelligence (AI) technologies, such as natural language processing, large language models, and machine learning algorithms, are increasingly incorporated with the goal to enhance personalization, effectiveness, and accessibility. These new technologies could make care more accessible to minoritized groups, for instance, because they could tailor their language, literacy, and cultural relevance. However, if not designed with an emphasis on equity and without youth participation, they can also present challenges, such as privacy concerns, harm to young people’s autonomy, and perpetuating harmful biases64,84. Research on AI in mental health for youth should specifically examine challenges to DEI.
In conclusion, research on DMH for young people lacks an equity lens. This is due to a lack of meaningful involvement of youth and other stakeholders, particularly those from systematically excluded communities. Our review indicates that reporting on DEI criteria–such as digital access, cultural adaptation, tailoring to disability and literacy, and privacy–is limited. Youth are rarely involved in core design decisions, and the resultant research primarily represents findings from fairly homogenous populations. If this continues, researchers risk creating ineffective services that widen existing disparities and fail to meet public health objectives. Young people are among the most active users of digital technology and are significantly affected by ongoing digital transformations, including within healthcare. It is crucial to ensure that all young people have a voice in shaping digital health tools to promote equity and effectiveness. This will only happen if researchers seek out and involve all youth. As a priority for future research, we recommend focusing on how to effectively involve diverse youth populations, implementing and evaluating participation methods, and developing a youth-centered DEI framework to enhance relevance and accessibility.
Methods
The scoping review was conducted in accordance with the Joanna Briggs Institute methodology for scoping reviews85, has been registered with Open Science Framework (https://osf.io/q3cax), and was published as a protocol in BMJ Open86.
Search strategy and selection criteria
We searched Medline, Global Health, APA PsycINFO, SCOPUS, CINAHL Plus, and the Cochrane Database of Randomized Trials, using the search string shown in the Supplementary Material. We included English-language studies published between January 1, 2009, and January 1, 2025. The main aim of this scoping review was to understand the current landscape of DEI practices in academic DMH research and to inform future practice. Therefore, we restricted our scoping review to the published scientific literature.
We included peer-reviewed studies in English that focused on depression, anxiety, and/or suicidal ideation; involved human participants (clinical or non-clinical populations), aged 10–25 (or with a sample mean age >9 and ≤25); and evaluated smartphone applications, with or without additional technologies like wearables or websites. We excluded studies that used only SMS, phone calls, or non-app-based web or wearable interventions, or involved participants outside the age range. To be inclusive to non-clinical populations, we selected studies with depression, anxiety, and/or suicidal ideation as a main outcome, but studies could target other mechanisms (e.g., rumination as a risk factor for depression). We included a range of study designs (e.g., pilot, feasibility, and randomized trials).
Following the search, all citations were collated and uploaded into Covidence (www.covidence.org). Titles, abstracts, and full text were screened by two or more independent reviewers (CAF, CSS, RZ, NO, NJPF, WK, GC, KWG) for assessment against the inclusion criteria, with a training session by the lead author before screening. Disagreements were resolved through discussion or by an additional reviewer (CAF or CSS).
Data analysis
Data were extracted in duplicate in Covidence and conflicts were resolved by a third reviewer. We documented each study’s primary mental health focus, country, setting, and research design. We examined whether studies included information on youth involvement into app development using participatory methods (e.g., co-design) and the involvement of other stakeholders (e.g., guardians, clinicians), and each DEI criterion (coding as reported/not reported, see Table 5 for a description). We provide a narrative summary of the DEI criteria and youth and stakeholder involvement. The Supplementary Material shows the charting template, which we pilot tested before the extraction. If information on DEI criteria or youth/stakeholder involvement was missing in the main paper, we examined the Supplementary Material, or formative work (e.g., co-design studies), if available. If studies did not take DEI criteria into account in the development but described the need to do so in their future work, we coded this as ‘reported’.
Our original aim was to analyze the overall prevalence of racial/ethnic minoritized participants, age, education, immigration status, annual income (of parents/guardians), and gender identity. As reporting practices in the studies demonstrated high variability– with different definitions and classifications used among studies, we decided not focus on prevalence, but on identifying the majority group in the examined studies. Our categorization of race/ethnicity is shown in the Supplementary Material.
We distinguished between design and evaluation activities based on their purpose and timing in the app development process (as shown in Fig. 4). Design was defined as activities where end-users and other stakeholders generate ideas or provide feedback on early versions of an intervention. This includes approaches such as co-design workshops, focus groups, interviews, or prototyping sessions87,88. Evaluation was defined as activities that assess feasibility, usability, acceptability, or effectiveness once (a version of) an intervention is available for testing88. While design and evaluation often overlap in the iterative refining processes, we categorized activities according to their primary intent as described in the studies.
Data availability
The full data generated from this review are available from the corresponding author upon request.
References
Kauhanen, L. et al. A systematic review of the mental health changes of children and young people before and during the COVID-19 pandemic. Eur. Child Adolesc. Psychiatry 32, 995–1013 (2023).
High-income countries are failing to provide adequate mental health services for children. https://www.bmj.com/company/newsroom/high-income-countries-are-failing-to-provide-adequate-mental-health-services-for-children/ (2021).
McGorry, P. D. et al. The Lancet Psychiatry Commission on youth mental health. Lancet Psychiatry 11, 731–774 (2024).
Wright, M., Reitegger, F., Cela, H., Papst, A. & Gasteiger-Klicpera, B. Interventions with digital tools for mental health promotion among 11-18 year Olds: A Systematic Review and Meta-analysis. J. Youth Adolesc. 52, 754–779 (2023).
Chen, B. et al. Comparative effectiveness and acceptability of internet-based psychological interventions on depression in young people: a systematic review and network meta-analysis. BMC Psychiatry 25, 321 (2025).
Fernández-Batanero, J. M., Fernández-Cerero, J., Montenegro-Rueda, M. & Fernández-Cerero, D. Effectiveness of digital mental health interventions for children and adolescents. Children 12, 353 (2025).
Liverpool, S. et al. Updates on digital mental health interventions for children and young people: systematic overview of reviews. Eur. Child Adolesc. Psychiatry https://doi.org/10.1007/s00787-025-02722-9 (2025).
Bear, H. A. et al. The acceptability, engagement, and feasibility of mental health apps for marginalized and underserved young people: systematic review and qualitative study. J. Med. Internet Res. 26, e48964 (2024).
Access to Adolescent Mental Health Care, US Office of Populations Affairs Website. https://opa.hhs.gov/adolescent-health/mental-health-adolescents/access-adolescent-mental-health-care.
Schueller, S. M., Hunter, J. F., Figueroa, C. & Aguilera, A. Use of digital mental health for marginalized and underserved populations. Curr. Treat. Options Psychiatry 6, 243–255 (2019).
Corsino, L. & Fuller, A. T. Educating for diversity, equity, and inclusion: A review of commonly used educational approaches. J. Clin. Transl. Sci. 5, e169 (2021).
Adu, M. et al. Centering equity, diversity, and inclusion in youth digital mental health: findings from a research, policy, and practice knowledge exchange workshop. Front. Digit. Health 6, 1449129 (2024).
Ramos, G., Ponting, C., Labao, J. P. & Sobowale, K. Considerations of diversity, equity, and inclusion in mental health apps: A scoping review of evaluation frameworks. Behav. Res. Ther. 147, 103990 (2021).
Soubutts, E. et al. Challenges and opportunities for the design of inclusive digital mental health tools: Understanding culturally diverse young people’s experiences. in Proceedings of the CHI Conference on Human Factors in Computing Systems vol. 44 1–16 (ACM, New York, NY, USA, 2024).
Bear, H. A. et al. Determination of markers of successful implementation of mental health apps for young people: Systematic review. J. Med. Internet Res. 24, e40347 (2022).
Kilfoy, A. et al. An umbrella review on how digital health intervention co-design is conducted and described. NPJ Digit. Med. 7, 374 (2024).
McGovern, Ó., Glennon, S., Walsh, I., Gallagher, P. & McCashin, D. The use of co-design with young people for digital mental health support development: A systematic review. Internet Interv. 41, 100835 (2025).
Stiles-Shields, C., Ramos, G., Ortega, A. & Psihogios, A. M. Increasing digital mental health reach and uptake via youth partnerships. Npj Ment. Health Res 2, 1–4 (2023).
Kamalumpundi, V. et al. Diversity, equity, and inclusion in a polarized world: Navigating challenges and opportunities in STEMM. Mol. Biol. Cell 35, vo2 (2024).
Suicide. https://www.who.int/news-room/fact-sheets/detail/suicide/.
Biernesser, C. et al. Development and codesign of flourish: A digital suicide prevention intervention for LGBTQ+ youth who have experienced online victimization. Internet Interv. 34, 100663 (2023).
Dingwall, K. M. et al. Feasibility and acceptability of the Aboriginal and Islander Mental Health Initiative for youth app: Nonrandomized pilot with First Nations young people. JMIR Hum. Factors 10, e40111 (2023).
Dambi, J. et al. A Digital Mental Health Intervention (Inuka) for Common Mental Health Disorders in Zimbabwean Adults in Response to the COVID-19 Pandemic: Feasibility and Acceptability Pilot Study. JMIR Ment. Health 9, e37968 (2022).
Silk, J. S. et al. Using a smartphone app and clinician portal to enhance brief cognitive behavioral therapy for childhood anxiety disorders. Behav. Ther. 51, 69–84 (2020).
Tighe, J. et al. Usage and acceptability of the iBobbly app: Pilot trial for suicide prevention in aboriginal and torres strait islander youth. JMIR Ment. Health 7, e14296 (2020).
Miller, I. et al. Self-Guided Digital Intervention for Depression in Adolescents: Feasibility and Preliminary Efficacy Study. JMIR Form. Res. 7, e43260 (2023).
Gonsalves, P. P. et al. Pilot randomised controlled trial of a remotely delivered online intervention for adolescent mental health problems in India: lessons learned about low acceptability and feasibility during the COVID-19 pandemic. BJPsych Open 9, e7 (2023).
Torok, M. et al. The effect of a therapeutic smartphone application on suicidal ideation in young adults: findings from a randomized controlled trial in Australia. PLoS Med. 19, e1003978 (2022).
Peuters, C. et al. A mobile healthy lifestyle intervention to promote mental health in adolescence: a mixed-methods evaluation. BMC Public Health 24, 44 (2024).
Li, S. H. et al. A cognitive behavioural therapy smartphone app for adolescent depression and anxiety: co-design of ClearlyMe. Cogn. Behav. Ther. 15, e13 (2022).
Povey, J. et al. Determining priorities in the Aboriginal and Islander Mental Health Initiative for youth app second phase participatory design project: Qualitative study and narrative literature review. JMIR Form. Res. 6, e28342 (2022).
Six, S. G., Byrne, K. A., Aly, H. & Harris, M. W. The Effect of Mental Health App Customization on Depressive Symptoms in College Students: Randomized Controlled Trial. JMIR Ment. Health 9, 1–14 (2022).
Schueller, S. M. et al. A mobile phone–based intervention to improve mental health among homeless young adults: Pilot feasibility trial. JMIR MHealth UHealth 7, e12347 (2019).
Reid, S. C. et al. A mobile phone application for the assessment and management of youth mental health problems in primary care: A randomised controlled trial. BMC Fam. Pract. 12, 131 (2011).
Kauer, S. D. et al. Self-monitoring using mobile phones in the early stages of adolescent depression: Randomized controlled trial. J. Med. Internet Res. 14, 19–35 (2012).
VanHeerwaarden, N. et al. The optimization of an eHealth solution (Thought Spot) with transition-aged youth in postsecondary settings: Participatory design research. J. Med. Internet Res. 20, e79 (2018).
Balaskas, A., Schueller, S. M., Cox, A. L., Rashleigh, C. & Doherty, G. Examining young adults daily perspectives on usage of anxiety apps: A user study. PLOS Digit. Health 2, e0000185 (2023).
Ellison, O. K. et al. Examining efficacy and potential mechanisms of mindfulness-based cognitive therapy for anxiety and stress reduction among college students in a cluster-randomized controlled trial. Int. J. Clin. Health Psychol. 24, 100514 (2024).
Cliffe, B., Moore, E., Whittle, K. & Stallard, P. Is a smartphone application (BlueIce) acceptable and safe for university students who self-harm: an open study. BMJ Open 14, e069862 (2024).
Pramana, G., Parmanto, B., Kendall, P. C. & Silk, J. S. The SmartCAT: An m-health platform for ecological momentary intervention in child anxiety treatment. Telemed. J. E. Health 20, 419–427 (2014).
Patwardhan, M. et al. Designing a Mobile Application to Support the Indicated Prevention and Early Intervention of Childhood Anxiety. https://commons.erau.edu/publication/602 (2015).
Gonsalves, P. P. et al. Design and Development of the ‘POD Adventures’ Smartphone Game: A Blended Problem-Solving Intervention for Adolescent Mental Health in India. Front. Public Health 7, 238 (2019).
Watkins, E. R. et al. Emotional competence self-help app versus cognitive behavioural self-help app versus self-monitoring app to prevent depression in young adults with elevated risk (ECoWeB PREVENT): an international, multicentre, parallel, open-label, randomised controlled. Lancet Digit. Heal. 6, e894–e903 (2024).
Serlachius, A. et al. Pilot study of a well-being app to support New Zealand young people during the COVID-19 pandemic. Internet Interv. 26, 100464 (2021).
Elledge, D. K. et al. Examining a Resilience Mental Health App in Adolescents: Acceptability and Feasibility Study. JMIR Form. Res. 7, e38042 (2023).
Cormier, M. et al. Sleep well, worry less: A co-design study for the development of the SMILE app. Digit. Health https://doi.org/10.1177/20552076241283242 (2024).
Christie, G. I. et al. Gamifying CBT to deliver emotional health treatment to young people on smartphones. Internet Interv. 18, 100286 (2019).
Prochaska, J. J. et al. Acceptability and utility of a smartphone app to support adolescent mental health (BeMe): Program evaluation study. JMIR MHealth UHealth 11, e47183 (2023).
Thabrew, H., Kumar, H. & Steadman, E. Acceptability and Feasibility of ‘Village,’ a Digital Communication App for Young People Experiencing Low Mood, Thoughts of Self-harm, and Suicidal Ideation to Obtain Support From Family and Friends: Mixed Methods Pilot Open Trial. JMIR Form. Res. 7, e41273 (2023).
Birrell, L. et al. Development of a Peer Support Mobile App and Web-Based Lesson for Adolescent Mental Health (Mind Your Mate): User-Centered Design Approach. JMIR Form. Res. 6, e36068 (2022).
Giovanelli, A. et al. The Appa Health App for Youth Mental Health: Development and Usability Study. JMIR Form. Res. 7, e49998 (2023).
Hengudomsub, P., Sudjai, P., Kangwanphanit, P., Thongkamdee, P. & Turale, S. Promoting Positive Thinking and Reducing Perceived Stress Using the Be Aware of Stress Smartphone Application among At-risk Adolescents: A Quasi-experimental Study. Pac. Rim Int. J. Nurs. Res. 28, 599–618 (2024).
Thabrew, H. et al. Well-being app to support young people during the COVID-19 pandemic: Randomised controlled trial. BMJ Open 12, e058144 (2022).
MacIsaac, A. et al. Adverse childhood experiences and building resilience with the JoyPop app: Evaluation study. JMIR MHealth UHealth 9, e25087 (2021).
Sun, Y. et al. A smartphone app for promoting mental well-being and awareness of anxious symptoms in adolescents: A pilot cluster randomized controlled trial. Games Health 11, 393–402 (2022).
Fleming, J. B., Hill, Y. N. & Burns, M. N. Usability of a culturally informed mhealth intervention for symptoms of anxiety and depression: Feedback from young sexual minority men. JMIR Hum. Factors 4, e22 (2017).
Dietvorst, E. et al. A Smartphone Serious Game for Adolescents (Grow It! App): Development, Feasibility, and Acceptance Study. JMIR Form. Res 6, e29832 (2022).
Stallard, P., Porter, J. & Grist, R. A smartphone app (Blueice) for young people who self-harm: Open phase 1 pre-post trial. JMIR MHealth UHealth 6, e32 (2018).
Birrell, L. et al. Evaluating a Peer-Support Mobile App for Mental Health and Substance Use Among Adolescents Over 12 Months During the COVID-19 Pandemic: Randomized Controlled Trial. J. Med. Internet Res. 25, e45216 (2023).
Nicol, G., Wang, R., Graham, S., Dodd, S. & Garbutt, J. Chatbot-Delivered Cognitive Behavioral Therapy in Adolescents With Depression and Anxiety During the COVID-19 Pandemic: Feasibility and Acceptability Study. JMIR Form. Res. 6, e40242 (2022).
Muscara, F. et al. The feasibility of using smartphone apps to manage self-harm and suicidal acts in adolescents admitted to an inpatient mental health ward. Digit. Health https://doi.org/10.1177/2055207620975315 (2020).
Bantjes, J. et al. Comparative effectiveness of remote digital gamified and group CBT skills training interventions for anxiety and depression among college students: Results of a three-arm randomised controlled trial. Behav. Res. Ther. 178, 104554 (2024).
Wyatt, K. A. et al. Involvement of children and young people in the conduct of health research: A rapid umbrella review. Health Expect. 27, e14081 (2024).
Figueroa, C. A. et al. Advancing youth co-design of ethical guidelines for AI-powered digital mental health tools. Nat. Ment. Health 3, 870–878 (2025).
Cwinn, E., Cadieux, C. & Crooks, C. V. Who are we missing? The impact of requiring parental or guardian consent on research with lesbian, gay, bisexual, trans, two-spirit, queer/questioning youth. J. Adolesc. Health 68, 1204–1206 (2021).
Trask, B. Adolescents, families, and globalization in the twenty-first century. in International and Cultural Psychology 3–20 (Springer International Publishing, Cham, 2024).
Litke, S. G. et al. Mobile technologies for supporting mental health in youths: Scoping review of effectiveness, limitations, and inclusivity. JMIR Ment. Health 10, e46949 (2023).
Liverpool, S. et al. Engaging children and young people in digital mental health interventions: Systematic review of modes of delivery, facilitators, and barriers. J. Med. Internet Res. 22, e16317 (2020).
Partridge, S. R. et al. Addressing disparities: A systematic review of digital health equity for adolescent obesity prevention and management interventions. Obes. Rev. 25, e13821 (2024).
Richardson, S., Lawrence, K., Schoenthaler, A. M. & Mann, D. A framework for digital health equity. NPJ Digit Med 5, 119 (2022).
Crawford, A. & Serhal, E. Digital health equity and COVID-19: The innovation curve cannot reinforce the social gradient of health. J. Med. Internet Res. 22, e19361 (2020).
Roennfeldt, H. et al. Scoping review of co-design in mental health research: Essential elements and recommendations. OTJR 0, 15394492251367259 (2025).
Ozer, E. J. et al. Youth participatory approaches and health equity: Conceptualization and integrative review. Am. J. Community Psychol. 66, 267–278 (2020).
Gonsalves, P. P. et al. Co-designing digital mental health interventions with young people: 10 recommendations from lessons learned in low-and-middle-income countries. Health Educ. J. 84, 373–384 (2025).
Warraitch, A., Wacker, C., Buckley, E., Bourke, A. & Hadfield, K. How to address the barriers to meaningful adolescent involvement in health research: A qualitative study. J. Res. Adolesc. 34, 1626–1641 (2024).
Brotherdale, R., Berry, K., Branitsky, A. & Bucci, S. Co-producing digital mental health interventions: A systematic review. Digit. Health 10, 20552076241239172 (2024).
Bailey, K. et al. Benefits, barriers and recommendations for youth engagement in health research: combining evidence-based and youth perspectives. Res. Involv. Engagem. 10, 92 (2024).
Youth-centred digital health interventions: a framework for planning, developing and implementing solutions with and for young people. https://www.who.int/publications/i/item/9789240011717 (2021).
Bye, A., Wilson-Lemoine, E., Trevillion, K., Carter, B. & Dutta, R. Factors that affect clinical youth engagement in digital mental health research: a qualitative sub-study nested within a prospective cohort study. BMC Med. Res. Methodol. 25, 118 (2025).
Naderbagi, A. et al. Cultural and contextual adaptation of digital health interventions: Narrative review. J. Med. Internet Res. 26, e55130 (2024).
Schleider, J. L. et al. State parental consent law and treatment use among adolescents with depression. JAMA Pediatr. 179, 209–212 (2025).
Williams, J. S., Martinez, M., Dzeng, E. & Gonzalez, C. M. Promoting health equity, diversity, and inclusion in medical and scientific writing and publishing of research: A statement from the inaugural diversity, equity, and inclusion (DEI) Advocacy Team of the Journal of General Internal Medicine. J. Gen. Intern. Med. 40, 1498–1501 (2025).
Groom, L. L., Schoenthaler, A. M., Mann, D. M. & Brody, A. A. Construction of the Digital Health Equity-Focused Implementation Research conceptual model - bridging the divide between equity-focused digital health and implementation research. PLOS Digit. Health 3, e0000509 (2024).
Timmons, A. C. et al. A call to action on assessing and mitigating bias in artificial intelligence applications for mental health. Perspect. Psychol. Sci. 18, 1062–1096 (2023).
Tricco, A. C. et al. PRISMA extension for Scoping Reviews (PRISMA-ScR): Checklist and explanation. Ann. Intern. Med. 169, 467–473 (2018).
Figueroa, C. A., Pérez-Flores, N. J., Guan, K. W. & Stiles-Shields, C. Diversity, equity and inclusion considerations in mental health apps for young people: protocol for a scoping review. BMJ Open 14, e081673 (2024).
Sanders, E. B.-N. & Stappers, P. J. Co-creation and the new landscapes of design. CoDesign 4, 5–18 (2008).
ISO 9241-210:2019. ISO https://www.iso.org/standard/77520.html#lifecycle (2025).
Atik, E., Stricker, J., Schückes, M. & Pittig, A. Efficacy of a Brief Blended Cognitive Behavioral Therapy Program for the Treatment of Depression and Anxiety in University Students: Uncontrolled Intervention Study. JMIR Ment. Health 10, e44742 (2023).
Barnes, S., Prescott, J. & Adams, J. Initial evaluation of a mobile therapeutic game for adolescent anxiety disorders. Ment. Health Soc. Incl. 27, 118–132 (2023).
Bell, I. et al. A Personalized, Transdiagnostic Smartphone Intervention (Mello) Targeting Repetitive Negative Thinking in Young People With Depression and Anxiety: Pilot Randomized Controlled Trial. J. Med. Internet Res. 25, e47860 (2023).
Bendtsen, M., Müssener, U., Linderoth, C. & Thomas, K. A mobile health intervention for mental health promotion among university students: Randomized controlled trial. JMIR MHealth UHealth 8, e17208 (2020).
Biagianti, B. et al. A mobile application adjunct to augment cognitive-Behavioral Group Therapy for adolescents with Social Anxiety: Feasibility and acceptability results from the wiring adolescents with Social Anxiety via Behavioral Interventions pilot trial. J. Child Adolesc. Psychopharmacol. 33, 212–224 (2023).
Bress, J. N. et al. Efficacy of a Mobile App-Based Intervention for Young Adults With Anxiety Disorders: A Randomized Clinical Trial. JAMA Netw. Open 7, e2428372 (2024).
Bruehlman-Senecal, E. et al. Smartphone app to address loneliness among college students: Pilot randomized controlled trial. JMIR Ment. Health 7, e21496 (2020).
Buus, N. et al. Stakeholder perspectives on using and developing the MYPLAN suicide prevention mobile phone application: A focus group study. Arch. Suicide Res. 24, 48–63 (2020).
Deady, M. et al. The Utility of a Mental Health App in Apprentice Workers: A Pilot Study. Front. Public Health 8, 389 (2020).
Dinengsih, S. et al. Android-based smart application development for adolescent mental health. J. Angiother. 8, 1–7 (2024).
Dosovitsky, G. & Bunge, E. Development of a chatbot for depression: adolescent perceptions and recommendations. Child Adolesc. Ment. Health 28, 124–127 (2023).
Edge, D. et al. Evaluating the Effects of a Self-Help Mobile Phone App on Worry and Rumination Experienced by Young Adults: Randomized Controlled Trial. JMIR MHealth UHealth 12, e51932 (2024).
Egilsson, E., Bjarnason, R. & Njardvik, U. Usage and weekly attrition in a smartphone-based health behavior intervention for adolescents: Pilot randomized controlled trial. JMIR Form. Res. 5, e21432 (2021).
Egilsson, E., Bjarnason, R. & Njardvik, U. Usage and Daily Attrition of a Smartphone-Based Health Behavior Intervention: Randomized Controlled Trial. JMIR MHealth UHealth 11, e45414 (2023).
Ejiri, H. et al. Immediate Effects of Mobile Phone App for Depressed Mood in Young Adults with Subthreshold Depression: A Pilot Randomized Controlled Trial. Neuropsychiatr. Dis. Treat. 19, 1695–1707 (2023).
Franklin, J. C. et al. A brief mobile app reduces nonsuicidal and suicidal self-injury: Evidence from three randomized controlled trials. J. Consult. Clin. Psychol. 84, 544–557 (2016).
Gabrielli, S. et al. Engagement and effectiveness of a healthy-coping intervention via chatbot for university students during the COVID-19 pandemic: Mixed methods proof-of-concept study. JMIR MHealth UHealth 9, e27965 (2021).
Gao, Y. et al. Mobile-Delivered Mindfulness Intervention on Anxiety Level Among College Athletes: Randomized Controlled Trial. J. Med. Internet Res. 26, e40406 (2024).
He, Y. et al. Mental Health Chatbot for Young Adults With Depressive Symptoms During the COVID-19 Pandemic: Single-Blind, Three-Arm Randomized Controlled Trial. J. Med. Internet Res. 24, e40719 (2022).
Hetrick, S. E. et al. Youth Codesign of a Mobile Phone App to Facilitate Self-Monitoring and Management of Mood Symptoms in Young People With Major Depression, Suicidal Ideation, and Self-Harm. JMIR Ment. Health 5, e9 (2018).
Hilt, L. M. & Swords, C. M. Acceptability and preliminary effects of a mindfulness mobile application for ruminative adolescents. Behav. Ther. 52, 1339–1350 (2021).
Hilt, L. M., Swords, C. M. & Webb, C. A. Randomized controlled trial of a mindfulness mobile application for ruminative adolescents. J. Clin. Child Adolesc. Psychol. https://doi.org/10.1080/15374416.2022.2158840 (2023).
Hoid, D., Pan, D.-N., Liao, C. & Li, X. Effects of a Smartphone-Based, Multisession Interpretation-Bias Modification for Anxiety: Positive Intervention Effects and Low Attrition. Int. J. Environ. Res. Public Health 20, 2270 (2023).
Kageyama, K. et al. Effects of video viewing smartphone application intervention involving positive word stimulation in people with subthreshold depression: A pilot randomized controlled trial. J. Affect. Disord. 282, 74–81 (2021).
Kajitani, K. et al. Short-term effect of a smartphone application on the mental health of university students: A pilot study using a user-centered design self-monitoring application for mental health. PLoS One 15, e0239592 (2020).
Kennard, B. D. et al. As Safe as Possible (ASAP): A brief app-supported inpatient intervention to prevent postdischarge suicidal behavior in hospitalized, suicidal adolescents. Am. J. Psychiatry 175, 864–872 (2018).
Kenny, R., Dooley, B. & Fitzgerald, A. Ecological momentary assessment of adolescent problems, coping efficacy, and mood states using a mobile phone app: An exploratory study. JMIR Ment. Health 3, e51 (2016).
Kleiman, E. M. et al. A Pilot Implementation-Effectiveness Trial of a Single-Session Telehealth Workshop and Smartphone-Based Cognitive Behavioral Intervention for Managing Emotions Among College Students. Behav. Ther. 53, 1024–1036 (2022).
Ko, K. S. & Lee, W. K. A preliminary study using a mobile app as a dance/movement therapy intervention to reduce anxiety and enhance the mindfulness of adolescents in South Korea. Arts Psychother. 85, 102062 (2023).
Kulikov, V. N. et al. A CBT-based mobile intervention as an adjunct treatment for adolescents with symptoms of depression: a virtual randomized controlled feasibility trial. Front. Digit. Health 5, 1062471 (2023).
LaFreniere, L. S. & Newman, M. G. Savoring changes novel positive mindset targets of GAD treatment: Optimism, prioritizing positivity, kill-joy thinking, and worry mediation. Behav. Res. Ther. 177, 104541 (2024).
Lattie, E., Cohen, K. A., Winquist, N. & Mohr, D. C. Examining an app-based mental health self-care program, intellicare for college students: Single-arm pilot study. JMIR Ment. Health 7, e21075 (2020).
Li, A. et al. Using modern technologies for prevention of suicidal behavior among adolescents. Soc. Work Ment. Health https://doi.org/10.1080/15332985.2023.2247514 (2023).
Litvin, S. et al. The Impact of a Gamified Mobile Mental Health App (eQuoo) on Resilience and Mental Health in a Student Population: Large-Scale Randomized Controlled Trial. JMIR Ment. Health 10, e47285 (2023).
Liu, H., Peng, H., Song, X., Xu, C. & Zhang, M. Using AI chatbots to provide self-help depression interventions for university students: A randomized trial of effectiveness. Internet Inter. 27, 100495 (2022).
Martinez-Fierro, M. L. et al. Usefulness of a Mobile Application (Mentali) for Anxiety and Depression Screening in Medical Students and Description of the Associated Triggering Factors. Brain Sci. 12, 1223 (2022).
McCloud, T., Jones, R., Lewis, G., Bell, V. & Tsakanikos, E. Effectiveness of a mobile app intervention for anxiety and depression symptoms in university students: Randomized controlled trial. JMIR MHealth UHealth 8, e15418 (2020).
Miklowitz, D. J. et al. Development and open trial of a technology-enhanced family intervention for adolescents at risk for mood disorders. J. Affect. Disord. 281, 438–446 (2021).
Motter, J. N., Grinberg, A., Lieberman, D. H., Iqnaibi, W. B. & Sneed, J. R. Computerized cognitive training in young adults with depressive symptoms: Effects on mood, cognition, and everyday functioning. J. Affect. Disord. 245, 28–37 (2019).
Na, H., Jo, M., Lee, C. & Kim, D. Development and Evaluation: A Behavioral Activation Mobile Application for Self-Management of Stress for College Students. Healthc. (Switz.) 10, 1880 (2022).
Nagamitsu, S. et al. Adolescent health promotion interventions using well-care visits and a smartphone cognitive behavioral therapy app: randomized controlled trial. JMIR MHealth UHealth 10, e34154 (2021).
Neal-Barnett, A. et al. Evaluation of the effectiveness of a musical cognitive restructuring app for black inner-city girls: Survey, usage, and focus group evaluation. JMIR MHealth UHealth 7, e11310 (2019).
Nguyen-Feng, V. N., Greer, C. S. & Frazier, P. Using online interventions to deliver college student mental health resources: Evidence from randomized clinical trials. Psychol. Serv. 14, 481–489 (2017).
Nguyen-Feng, V. N., Romano, F. N. & Frazier, P. Emotional abuse moderates efficacy of an ecological momentary stress management intervention for college students. J. Couns. Psychol. 66, 461–472 (2019).
O’Brien, K. H. M., LeCloux, M., Ross, A., Gironda, C. & Wharff, E. A. A pilot study of the acceptability and usability of a smartphone application intervention for suicidal adolescents and their parents. Arch. Suicide Res. 21, 254–264 (2017).
O’Brien, K. H. M. et al. An mHealth approach to extend a brief intervention for adolescent alcohol use and suicidal behavior: Qualitative analyses of adolescent and parent feedback. J. Technol. Hum. Serv. 37, 255–285 (2019).
O’Dea, B. et al. A randomised controlled trial of a relationship-focussed mobile phone application for improving adolescents’ mental health. J. Child Psychol. Psychiatry 61, 899–913 (2020).
Park, J., Lee, J. & Noh, D. Mobile App for Improving the Mental Health of Youth in Out-of-Home Care: Development Study Using an Intervention Mapping Approach. JMIR Hum. Factors 11, e64681 (2024).
Paul, A. M. & Eubanks Fleming, C. J. Anxiety Management on Campus: An Evaluation of a Mobile Health Intervention. J. Technol. Behav. Sci. 4, 58–61 (2019).
Peake, E. et al. Preliminary Efficacy of a Digital Intervention for Adolescent Depression: Randomized Controlled Trial. J. Med. Internet Res. 26, e48467 (2024).
Peters, A. B., Kellogg, M. & Zhang, Y. Implementation of a Smartphone App to Measure and Manage Anxiety in Undergraduate Clinical Nursing Students. Nurs. Educ. Perspect. (Wolters Kluwer Health) 40, 367–369 (2019).
Raevuori, A. et al. A therapist-guided smartphone app for major depression in young adults: A randomized clinical trial. J. Affect. Disord. 286, 228–238 (2021).
Rauschenberg, C. et al. A compassion-focused ecological momentary intervention for enhancing resilience in help-seeking youth: Uncontrolled pilot study. JMIR Ment. Health 8, e25650 (2021).
Sit, H. F. et al. A Feasibility Study of the WHO Digital Mental Health Intervention Step-by-Step to Address Depression Among Chinese Young Adults. Front. Psychiatry 12, 812667 (2021).
Stallard, P. et al. Acceptability, use and safety of the BlueIce self-harm prevention app: Qualitative findings from the Beating Adolescent Self-Harm (BASH) randomised controlled trial. BMJ Ment. Health 27, e300961 (2024).
Stallard, P. et al. Clinical effectiveness and safety of adding a self-harm prevention app (BlueIce) to specialist mental health care for adolescents who repeatedly self-harm: A single blind randomised controlled trial (the BASH study). Psychiatry Res. 339, 116017 (2024).
Teng, M.-H., Hou, Y.-M., Chang, S.-H. & Cheng, H.-J. Home-delivered attention bias modification training via smartphone to improve attention control in sub-clinical generalized anxiety disorder: A randomized, controlled multi-session experiment. J. Affect. Disord. 246, 444–451 (2019).
Thomas, E. B. K. Mobile acceptance and commitment therapy with distressed first-generation college students: microrandomized trial. JMIR Ment. Health 10, e43065 (2023).
Toh, S. H. Y., Tan, J. H. Y., Kosasih, F. R. & Sündermann, O. Efficacy of the mental health app intellect to reduce stress: randomized controlled trial with a 1-month follow-up. JMIR Form. Res. 6, e40723 (2022).
Sakata M et al. Components of smartphone cognitive-behavioural therapy for subthreshold depression among 1093 university students: a factorial trial. Evid. Based. Ment. Health 25, e18–e25, (2022).
Webb, C. A., Swords, C. M., Murray, L. & Hilt, L. M. App-based mindfulness training for adolescent rumination: Predictors of immediate and cumulative benefit. Mindfulness 12, 2498–2509 (2021).
Webb, C. A., Swords, C. M., Lawrence, H. R. & Hilt, L. M. Which adolescents are well-suited to app-based mindfulness training? A randomized clinical trial and data-driven approach for personalized recommendations. J. Consult. Clin. Psychol. 90, 655–669 (2022).
Weiner, L. S. et al. Engagement, Acceptability, and Effectiveness of the Self-Care and Coach-Supported Versions of the Vira Digital Behavior Change Platform Among Young Adults at Risk for Depression and Obesity: Pilot Randomized Controlled Trial. JMIR Ment. Health 11, e51366 (2024).
Weintraub, M. J. et al. App-enhanced transdiagnostic CBT for adolescents with mood or psychotic spectrum disorders. J. Affect. Disord. 311, 319–326 (2022).
Weintraub, M. J. et al. Behavioral skill practice as a predictor of mood and family functioning in adolescents with bipolar and depressive mood disorders: Results of a 6-month randomized trial of family-focused therapy. Bipolar Disord. 26, 733–743 (2024).
Werner-Seidler, A. et al. The effects of a sleep-focused smartphone application on insomnia and depressive symptoms: A randomised controlled trial and mediation analysis. J. Child Psychol. Psychiatry 64, 1324–1335 (2023).
Whiteside, S. P. H., Ale, C. M., Vickers Douglas, K., Tiede, M. S. & Dammann, J. E. Case Examples of Enhancing Pediatric OCD Treatment with a Smartphone Application. Clin. Case Stud. 13, 80–94 (2014).
Willems, L. et al. Mental health app boost my mood (BMM) as preventive early intervention for adolescents with (sub)clinical depressive symptoms. BMC Public Health 24, 2118 (2024).
Zainal, N. H., Tan, H. H., Hong, R. Y. & Newman, M. G. Is a brief mindfulness ecological momentary intervention more efficacious than a self-monitoring app for social anxiety disorder? A randomized controlled trial. J. Anxiety Disord. 104, 102858 (2024).
Zhou, X. et al. The feasibility, acceptability and efficacy of an app-based intervention (the Coping Camp) in reducing stress among Chinese school adolescents: A cluster randomised controlled trial. PLoS One 18, e0294119 (2023).
Acknowledgements
We would like to thank G. Ramos, A. Psihogios, C. Emezue, and E. Ekuban for their advice on the interpretation of the findings. C. Figueroa and Kathleen Guan were supported through the ‘High Tech for a Sustainable Future’ capacity building programme of the 4TU Federation in the Netherlands. N. J. Perez-Flores was supported by the National Heart, Lung, and Blood Institute [under Grant T32HL130357]. C Stiles-Shields was supported in part by the National Institute of Mental Health (K08 MH125069). The content of this manuscript is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Contributions
C.A.F. was involved in conceptualizing the study. C.A.F., C.S.S., R.Z., N.O., N.J.P.F., W.K., G.C., and K.W.G. participated in abstract, full-text screening, and data extraction. C.A.F. conducted the analysis of DEI criteria, N.J.P.F. conducted the demographics analysis, G.C. and C.A.F. conducted the descriptive characteristics of studies, and R.Z. conducted the analysis on youth and stakeholder involvement. Analyses were discussed with C.A.F. and C.S.S. All authors participated in writing and editing the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Figueroa, C., Pérez-Flores, N.J., Guan, K.W. et al. Designing for all youth: a scoping review of equity and participation in mental health apps. npj Digit. Public Health 1, 8 (2026). https://doi.org/10.1038/s44482-026-00012-y
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s44482-026-00012-y