Abstract
CD169+ macrophages, a unique subset of macrophages that cannot be simply defined as M1 or M2 macrophages, have been reported to be associated with various autoimmune diseases. However, the role of CD169+ macrophages in autoimmune hepatitis (AIH) is largely unknown. Here we found that the infiltration of CD169+ macrophages increased in the liver of patients with AIH and strongly positively correlated with inflammation degree. In a mouse model, depletion of CD169+ macrophages ameliorated ConA-induced acute liver injury. Immune homeostasis was also improved when CD169+ macrophages were depleted, as the infiltration of monocytes, macrophages and T cells decreased. Bone marrow-derived Ly6ChiCD169+ macrophages were further identified as the crucial subset in AIH. Next, we found that CD169+ macrophages were IFNγ-responsive and IFNγ could induce the expression of CD169. In response to the IFNγ signal, CD169+ macrophages actively secrete chemokine (C–C motif) ligand (CCL12), thus recruiting CCR2+ monocytes and macrophages to exacerbate AIH. Finally, neutralizing CCL12 improved AIH. Our results suggest that bone marrow-derived CD169+ macrophages, the key subset of macrophages in AIH, actively secrete CCL12 in response to IFNγ to recruit CCR2+ monocytes and macrophages, thus exacerbating AIH. The CD169+ macrophages are a potential therapeutic target in AIH.

Similar content being viewed by others
Introduction
Autoimmune hepatitis (AIH) is an obscure inflammatory liver disease that may be caused by the interaction of individual genetic susceptibility and environmental factors1,2. It is characterized by immune-mediated destruction of hepatocytes leading to progressive necrotizing inflammation of the liver2,3,4. AIH is a disease of the hepatic parenchyma that can manifest in both acute and chronic forms. The clinical presentation often resembles acute hepatitis and may progress to liver cirrhosis and end-stage liver failure1,2. ConA-induced acute liver injury animal model is widely used to mimic clinical acute hepatitis and immune-mediated liver injury in humans4,5,6,7.
Studies have shown that macrophages in the liver play an important role in ConA-induced AIH8,9. Macrophages are the most abundant immune cells in the liver and are involved in maintaining liver immune homeostasis10,11. However, macrophages in the liver exhibit substantial heterogeneity. Kupffer cells (KCs) are the predominant macrophage population in the healthy liver, and they originate from the yolk sac12. KCs replenish relying on self-renewal under homeostatic conditions, independent of bone marrow-derived macrophages (BMDMs)13. When hepatitis occurs, KCs are activated and then inflammatory Ly6Chi monocyte-derived macrophages (MoMFs) are recruited into the liver to participate in the inflammatory response. Blocking the recruitment of MoMFs reduces hepatic inflammation and fibrosis14. Although each macrophage subset plays a distinct role in maintaining liver homeostasis, the concrete cellular and molecular mechanisms of different subsets in regulating liver immunity remain largely unknown.
CD169, also known as sialoadhesin or siglec1, is a prototype member of the siglec family of sialic acid-binding immunoglobulin-like lectin15. It is composed of 17 immunoglobin-like domains and a short cytoplasmic tail that lacks signaling motifs16. CD169 is initially reported as a marker for a macrophage subset isolated from bone marrow, lymph nodes, liver and spleen17. In recent years, CD169+ macrophages have been considered to be a distinct group of macrophages that cannot be simply defined as M1 or M2 macrophages18. For now, CD169+ macrophages have been shown to play an important role in various autoimmune diseases. It has been reported that CD169+ macrophages increased in multiple sclerosis and experimental autoimmune encephalitis19. Besides, the relative number of peripheral CD169+ monocytes is significantly and positively correlated with disease activity in rheumatoid arthritis and may even serve as a biomarker20,21. Similarly, CD14+CD169+ monocytes were significantly increased in patients with systemic lupus erythematosus22 and children with type 1 diabetes23. In addition, CD169 is highly expressed on peripheral blood monocytes in patients with primary biliary cholangitis (PBC)24. AIH and PBC are both classified as autoimmune liver diseases. However, the relationship between CD169+ macrophages and AIH is still largely unknown.
CD169-diphtheria toxin receptor (DTR) mice express DTR at the CD169 gene locus through genetic engineering techniques, enabling researchers to specifically eliminate cells expressing CD169 by injecting diphtheria toxin (DT)25.
Here, our study revealed that the number of CD169+ macrophages is positively correlated with disease severity in patients with AIH. In mice, depletion of CD169+ macrophages alleviated ConA-induced liver injury and necrosis, and improved immune homeostasis in the liver. Rather than liver-resident CD169+ macrophages, bone marrow-derived CD169+ macrophages macrophages were shown to be the key subset in AIH. Compared with CD169− macrophages, CD169+ macrophages selectively secrete CCL12 to recruit CCR2+ monocytes and macrophages to further exacerbate the acute liver injury in response to IFNγ signal.
Materials and methods
Human participants
Liver tissues from 40 patients with AIH, 21 patients with PBC, 12 patients with metabolic dysfunction-associated steatotic liver disease (MASLD) and 7 patients with chronic hepatitis B (CHB) were obtained from ultrasound-guided needle liver biopsies at diagnosis. Liver tissues of six healthy controls (HCs) were collected from donor livers before transplantation. Demographic and clinical characteristics of the study participants are presented in Supplementary Table 1. All individuals were enrolled in Shanghai Renji Hospital and provided written informed consent. The study was carried out under the principles of the Declarations of Helsinki and Istanbul and approved by the Shanghai Jiao Tong University Ethics Committee.
Mice
C57BL/6J mice purchased from Zhejiang Academy of Medical Sciences, aged 8–12 weeks, were used in the current study. CD169-DTR mice (C57BL/6J background) were gifted by Dr. Jiong Chen (Ningbo University, China). The animal study was approved by the Animal Care and Use Committee of the First Affiliated Hospital, Zhejiang University School of Medicine. Additional materials and methods can be found in the Supplementary Information.
Results
CD169+ macrophages were significantly increased in the livers of patients with AIH and positively correlated with disease severity
First, we confirmed that CD169+ cells in human liver are macrophages by analyzing the human liver single-cell RNA sequencing (scRNA-seq) dataset GSE124395 (Supplementary Fig. 1a–c). To clarify the association between CD169+ macrophages and AIH, we first analyzed the amount of CD169+ macrophages in the liver of HCs (n = 6) and patients with AIH (n = 40), CHB (n = 7), PBC (n = 21) and MASLD (n = 12). The immunohistochemical staining results of CD169 indicated a significant increase in the number of CD169+ macrophages in the livers of patients with AIH compared with HCs and patients with other liver diseases (Fig. 1a, b).
a Immunohistochemical staining images of CD169+ macrophages in the liver of HCs and patients with AIH, CHB, PBC and MASLD. b The number of CD169+ macrophages in the liver per HPF. c The number of CD169+ macrophages in different inflammation grades. d The correlation of the number of CD169+ macrophages and different inflammation grades. e The number of CD169+ macrophages in different fibrosis stages. f The correlation of the number of CD169+ macrophages and different fibrosis stages. g–l The correlation of the number of CD169+ macrophages and ALT (g), AST (h), ALP (i), γ-GT (j), TBIL (k) and IgG (l) levels. m Costaining immunofluorescent images of CD169 and CD68 in the liver of patients with AIH. Results are expressed as mean ± standard error. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001.
Next, we found that the numbers of CD169+ macrophages in the liver increased with the progression of inflammation grade (Fig. 1c) and had a very strong positive correlation (r = 0.8501, P < 0.0001) with liver inflammation grade (Fig. 1d). As for the fibrosis stage, no statistical significance was observed among the different fibrosis stages (Fig. 1e). A moderate correlation (r = 0.5358, P = 0.0004) was observed between the fibrosis stage and the number of CD169+ macrophages in the 40 patients with AIH enrolled in the study (Fig. 1f). To further investigate the potential clinical importance of CD169+ macrophages in AIH, we analyzed the relationship between several biochemical parameters and the number of CD169+ macrophages in AIH. Surprisingly, the number of CD169+ macrophages in AIH was significantly positively correlated with alanine aminotransferase (ALT) (r = 0.7422, P < 0.0001), aspartate transaminase (AST) (r = 0.7054, P < 0.0001), alkaline phosphatase (ALP) (r = 0.6028, P < 0.0001), γ-glutamyl transferase (γ-GT) (r = 0.7040, P < 0.0001), total bilirubin (TBIL) (r = 0.5899, P < 0.0001) and immunoglobulin G (IgG) (r = 0.6156, P < 0.0001) (Fig. 1g–l). Consistent with previous studies26,27, our results also suggest that CD169+ cells in the liver of patients with AIH are macrophages as they costain with the macrophage marker CD68 (Fig. 1m). These results together suggest that CD169+ macrophages may play an important role in AIH, especially in the progression of inflammation.
The increased CD169+ cells in the liver of mice with AIH are mainly CD11b+F4/80+Ly6C+ infiltrating macrophages
To further illustrate the relationship between CD169+ macrophages and the progression of inflammation in AIH, we conducted time gradient AIH modeling on wild-type (WT) mice. After ConA administration for 0, 6, 12 and 24 h, as liver inflammation intensifies and the necrotic area expands, the amount of CD169+ macrophages in the liver also gradually increases (Fig. 2a and Supplementary Fig. 2a). Consistent with these results, the proportion of CD169+ cells in CD45+ cells increased after 12 h of modeling and further increased at 24 h (Fig. 2b). To further investigate the phenotypes of CD169+ cells in the liver, multicolor flow cytometry staining on nonparenchymal liver cells was performed. We classified T cells, natural killer (NK) cells, natural killer T (NKT) cells, B cells, neutrophils, KCs, Ly6C+ monocytes, Ly6C+ macrophages and Ly6C− macrophages (Supplementary Fig. 2b) and then counted the proportion of CD169+ cells in each of these subgroups. In the PBS group, all macrophage populations expressed CD169, with the highest proportion of KC populations (Fig. 2c). After 12 h of ConA administration, the proportion of CD169+ cells increased in the Ly6C+ monocytes group and Ly6C+ macrophages group (Fig. 2d, e), indicating that the increased CD169+ cells were possibly MoMFs. Ly6C+ monocytes and macrophages also increased after ConA administration (Supplementary Fig. 2c). TIM4 is a marker for liver-resident KCs28,29. We observed that, after ConA administration, TIM4+CD169+ proportions decreased significantly while Ly6C+CD169+ proportions increased (Fig. 2f). Immunofluorescence results further confirmed that the increased CD169+ cells in the AIH liver are MoMFs but not KCs. As shown in Fig. 2g, h, almost all CD169 showed costaining with F4/80, whereas most CD169 did not costain with CLEC4F, another marker for KCs28.
a Macroscopic images, H&E staining images, immunofluorescent images of CD169+ macrophages, and TUNEL staining images at indicated time points after ConA administration. b Frequency of CD169+ cells in the CD45+ cells. c CD169+ proportions in various immune cells after 12 h injected with PBS. d CD169+ proportions in various immune cells after 12 h injected with 10 mg/kg ConA. e CD169+ proportions in various immune cells after 12 h injected with PBS or 10 mg/kg ConA. f Tim4+ and Ly6c+ proportions in CD45+CD3−NK1.1−B220−CD11b+Ly6G−CD169+ cell population after 12 h injected with PBS or 10 mg/kg ConA. g Costaining immunofluorescent images of F4/80 and CD169 after 12 h injected with PBS or 10 mg/kg ConA. h Costaining immunofluorescent images of CLEC4F and CD169 after 12 h injected with PBS or 10 mg/kg ConA. Results are expressed as mean ± standard error. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001.
In summary, CD169+ cells increased in the liver of AIH mice, and most of the increased CD169+ cells are CD11b+F4/80+Ly6C+ infiltrating macrophages.
CD169+ macrophages were required for ConA-induced hepatic necrosis
To further elucidate the role of CD169+ macrophages in AIH, we administered DT into CD169-DTR mice to clear CD169+ macrophages25. The depletion of CD169+ macrophages was verified through flow cytometry analysis (Supplementary Fig. 3a) and immunohistochemistry staining (Supplementary Fig. 3b). An equivalent dose of DT was also injected into WT mice to control for any potential effects caused by DT injection (Fig. 3a). A lethal dose of 20 mg/kg of ConA was injected into WT and CD169-DTR mice, and the mortality of the mice was recorded. Surprisingly, 5 out of 11 WT mice died while all CD169-DTR mice survived 24 h after ConA administration (Fig. 3b). Compared with the WT ConA group, the levels of serum ALT and AST significantly reduced in the CD169-DTR ConA group (Fig. 3c). Besides, serum IFNγ and TNFα levels, the main inflammatory cytokines that cause liver necrosis and infiltration of leukocytes30, were also lower in the CD169-DTR ConA group than those in the WT ConA group (Fig. 3d). Following the depletion of CD169+ macrophages, a notable improvement in liver injury and necrosis was observed, as indicated by visual observation, hematoxylin and eosin (H&E) staining and terminal deoxynucleotidyl transferase dUTP nick-end labeling (TUNEL) staining (Fig. 3e). Notably, no hepatic necrosis was observed microscopically on H&E staining in the CD169-DTR ConA group. In addition, quantitative reverse transcription polymerase chain reaction (qRT–PCR) results showed that the expression of IFNγ, TNFα, IL6 and IL1β decreased when CD169+ macrophages were depleted, indicating alleviated liver inflammation in the CD169-DTR ConA group (Fig. 3f).
a Schematic diagram of CD169+ cell depletion and AIH modeling. b Survival curves within 24 h after 20 mg/kg ConA administration in WT or CD169-DTR mice. c Serum ALT and AST levels at 24 h after 20 mg/kg ConA administration. Serum IFNγ and TNFα levels at 24 h after 20 mg/kg ConA administration. Macroscopic images, H&E staining images and TUNEL staining images at 24 h after 20 mg/kg ConA administration. Relative IFNγ, TNFα, IL6 and IL1β mRNA levels at 24 h after 20 mg/kg ConA administration. d Schematic diagram of bone marrow transplantation and H&E staining images at 24 h after 20 mg/kg ConA administration. e H&E staining images in the bone marrow-transplanted groups at 24 h after 20 mg/kg ConA administration. f Serum ALT and AST levels in the bone marrow-transplanted groups at 24 h after 20 mg/kg ConA administration. Results are expressed as mean ± standard error. *P < 0.05, **P < 0.01, ***P < 0.001.
Taken together, our results emphasize the critical role of CD169+ macrophages in promoting ConA-induced hepatitis.
Bone marrow-derived CD169+ macrophages are a key subset in AIH progression
According to our present results, there are at least two distinct populations of CD169+ macrophages in the liver: one is yolk sac-derived CD11b+F4/80+TIM4+CD169+ KCs, and the other is bone marrow-derived CD11b+F4/80+Ly6C+CD169+ infiltrating macrophages. To clarify which origin of CD169+ macrophages plays a more critical role in AIH, we performed bone marrow transplantation (Fig. 3g). When WT bone marrow cells were transplanted into CD169-DTR mice and DT was applied, the bone marrow-derived WT CD169+ cells remained, while the liver resident CD169+ KCs of CD169-DTR mice were depleted. The efficacy of bone marrow transplantation was confirmed by genotyping (Supplementary Fig. 3c). We found that chimeric CD169-DTR mice with WT bone marrow exhibited a phenotype similar to WT mice after ConA administration, as they showed more severe liver damage and necrosis compared with CD169-DTR mice transplanted with CD169-DTR bone marrow (Fig. 3h), with higher serum ALT and AST levels (Fig. 3i).
Together, our results suggest that the bone marrow-derived CD169+ macrophages are the vital subset of macrophages in ConA-induced liver injury.
CD169+ macrophage depletion altered the immune microenvironment in AIH
Next, to further investigate the effects of CD169+ macrophage depletion on liver immune homeostasis, we performed multicolor flow cytometry to examine the alterations in various immune cells. The gating strategy is shown in Supplementary Fig. 4a. We found that, in the ConA groups, the frequency of NK cells, T cells, neutrophils and Ly6C+ monocytes decreased (Fig. 4a and Supplementary Fig. 4b), while the proportion of macrophages increased relatively after CD169+ macrophage depletion (Supplementary Fig. 4c). Similarly, immunohistochemistry results showed that, following clearing of CD169+ macrophages, the absolute numbers of T cells (identified by CD3), neutrophils (identified by MPO), monocytes (identified by LY6C) and macrophages (identified by F4/80) significantly decreased in the ConA groups, while B cells (identified by CD19) and NK cells (identified by NKp46) did not show any difference (Fig. 4b–g).
a The frequency of B cells, NK cells, T cells, neutrophils and Ly6C+ monocytes in CD45+ cells. b–g Immunohistochemical staining and quantification of CD19 (b), CD3 (c), NKp46 (d), MPO (e), Ly6C (f) and F4/80 (g) positive cells. h, The frequency of Th1, Th2, Th17, Treg and CTL. Results are expressed as mean ± standard error. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001.
Considering the importance of T cells in AIH, we further performed flow cytometry to analyze their activation (Supplementary Fig. 5a) and differentiation (Supplementary Fig. 6a). First, the proportion of CD4+ T cells decreased after depleting CD169+ macrophages, while the proportion of CD8+ T cells increased (Supplementary Fig. 5b). Our results suggest that, compared with the WT ConA group, the CD44−CD62L+ naive CD4+ T cell frequency did not change in the CD169-DTR ConA group (Supplementary Fig. 5c), while the proportion of CD25+ activated CD4+ T cells showed a minor decrease (Supplementary Fig. 5d). The proportion of naive CD8+ T cells decreased in the CD169-DTR ConA group (Supplementary Fig. 5e), while the proportion of activated CD8+ T cells remained unchanged (Supplementary Fig. 5f). As for the differentiation of T cells, CD169+ macrophage depletion inhibited the differentiation of CD4+ T cells toward Th1 (identified by IFNγ+), promoted the differentiation of Treg (identified by FOXP3 +CD25+) and had no significant effect on Th2 (identified by IL4+) and Th17 (identified by IL17A+). Besides, the proportion of IFNγ-expressing CD8+ cytotoxic T lymphocytes (CTL) significantly decreased after CD169+ macrophage depletion (Fig. 4h and Supplementary Fig. 6b–f).
Collectively, the elimination of CD169 macrophages reduced the number of various pro-inflammatory immune cells in the AIH liver and ameliorated the inflammatory state of the AIH liver.
CD169+ macrophages are IFNγ responsive
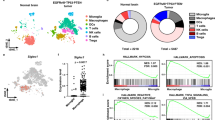
To further identify the role of CD169+ macrophages in AIH, the scRNA-seq dataset GSE201006 involving ConA-induced AIH in mice was analyzed. As expected, siglec1, the gene encoding CD169, was predominantly expressed in the macrophage population with or without ConA exposure (Fig. 5a). Also, the number of siglec1-expressing cells in the ConA group was higher than that in the WT group (Fig. 5b). To further clarify the differences between CD169+ macrophages and CD169− macrophages, we classified macrophages in the ConA group according to their siglec1 expression (Fig. 5c). Compared with CD169− macrophages, CD169+ macrophages express higher levels of Clec4b1, C1qc, Ecm1, Slc7a8, Ccl12 and so on (Fig. 5c). According to the HALLMARK enrichment analysis, CD169+ macrophages had higher expression of IFNγ-responsive genes (Fig. 5d), including Parp14, Fcgr1, Tapbp, Ccl2, Cxcl10, Oasl1, Nampt, Cmpk2, Trim26 and Lap3. These findings align with prior results demonstrating concurrent elevation of IFNγ levels and an increased proportion of CD169⁺ macrophages in AIH (Figs. 2a and 3f). Next, after neutralizing IFNγ in mice (Fig. 5e), liver necrosis was alleviated (Fig. 5f) and serum ALT and AST levels decreased (Fig. 5g). Notably, the number of CD169+ macrophages decreased after IFNγ neutralization (Fig. 5h). Next, BMDMs were induced in vitro and then stimulated with IFNγ (Fig. 5i). We observed that almost all of these BMDMs were CD169 positive (Supplementary Fig. 7a), and IFNγ stimulation increased the mean fluorescence intensity of CD169 in the CD11b+F4/80+ population (Fig. 5j). Peripheral blood mononuclear cells (PBMCs) from HCs were used for further investigation (Fig. 5k and Supplementary Fig. 7b). We found that CD14+CD169+ monocytes were significantly induced in vitro after 24 h of IFNγ stimulation (Fig. 5l, m).
a Identification of cell clusters from the GSE201006 dataset. b Expression of siglec1 in the different subsets. c Differentially expressed genes in siglec1-positive and siglec1-negative macrophages. d HALLMARK analysis of the upregulated genes enriched in the siglec1-positive macrophage subset. e Schematic diagram of IFNγ neutralization. Anti-mouse IFNγ antibody and isotype control were both used at 25 μg/g bodyweight intravenously. To induce AIH, 10 mg/kg ConA was injected into mice intravenously. f H&E staining images of the AIH mice treated with IFNγ neutralizing antibody or isotype antibody. g Serum ALT and AST levels. h Immunohistochemical staining of CD169. Arrows indicate positive staining. i Schematic diagram of mouse BMDMs stimulated by IFNγ. j Measurement of CD169 mean fluorescence intensity in the BMDMs with or without stimulation with IFNγ in vitro. k Schematic diagram of human PBMCs stimulated by IFNγ. l Representative plots of CD14+CD169+ monocytes in human PBMCs with or without stimulation with IFNγ in vitro. m The proportion of CD14+CD169+ monocytes in the total monocyte group or the total live PBMC group. Results are expressed as mean ± standard error. *P < 0.05, **P < 0.01.
In summary, CD169+ macrophages are IFNγ responsive and IFNγ can induce the expression of CD169 in macrophages and monocytes in vitro.
CD169+ macrophages selectively express CCL12 in AIH
Then, Kyoto Encyclopedia of Genes and Genomes (KEGG) enrichment analysis and Gene Ontology (GO) enrichment analysis were performed to further confirm the characteristics of CD169+ macrophages. KEGG enrichment analysis suggested that the chemokine signaling pathway was upregulated in the CD169+ macrophages (Fig. 6a). GO enrichment analysis indicated that the pathways of mononuclear cell migration and lymphocyte migration were enriched in CD169+ macrophages (Fig. 6b). Chemokine genes associated with these pathways were further identified as Ccl12, Ccl2, Cxcl10 and Ccl6 (Supplementary Fig. 8a). The mRNA levels of these four chemokines increased after ConA administration and significantly decreased after the depletion of CD169+ macrophages (Fig. 6c). To further investigate the association between these chemokines and CD169+ macrophages, we sorted CD169+ macrophages in the livers of WT mice treated with ConA. Also, we reconfirmed that the sorted CD169+ cells belong to the CD11b+F4/80+ subset (Supplementary Fig. 8b). Four cell populations were isolated: R1 (CD11b+F4/80+CD169+), R2 (CD11b+F4/80+CD169−), R3 (CD11bhiF4/80lo) and R4 (CD11bneg-loF4/80−) as shown in Fig. 6d. The purity of the sorted CD169+ macrophages in the four different populations was confirmed by qRT–PCR (Supplementary Fig. 8c,d). After ConA administration, the Ccl12 expressing capacity of CD169+ macrophages in the liver was significantly enhanced (Fig. 6e). In addition, Ccl12 expression levels were significantly increased in the R1 population compared with the R2 population (6.02-fold rise on average, compared with 1.69-fold rise in Ccl2, 1.42-fold rise in Cxcl10 and 2.85-fold rise in Ccl6) (Fig. 6f). These results suggest that, compared with Ccl2, Cxcl10 and Ccl6, CD169+ macrophages are most likely to realize their primary function in AIH by secreting CCL12. A significant increase in CCL12 protein secretion was also detected in the supernatant of the R1 population (average 16.58-fold rise compared with the R2 population) (Fig. 6g). Meanwhile, CCL12 was not detected in the supernatant of R3 or R4 populations, which was consistent with scRNA-seq results (Supplementary Fig. 8e), indicating that CCL12 is expressed in macrophages. In line with our qRT–PCR results (Fig. 6c), scRNA-seq also showed an increase in Ccl12 expression after ConA administration (Supplementary Fig. 8f). We also measured CCL12 protein levels in mouse liver homogenate (Fig. 6h) and serum (Supplementary Fig. 8g) and found that CCL12 increased after ConA administration and decreased after CD169+ macrophage depletion.
a KEGG analysis of the upregulated genes enriched in the siglec1-positive macrophage subset. b GO analysis of the upregulated genes enriched in the siglec1-positive macrophage subset. c Relative mRNA levels of Ccl12, Ccl2, Cxcl10 and Ccl6. d Gating strategies for flow cytometry sorting. e Relative Ccl12, Ccl2, Cxcl10 and Ccl6 mRNA levels in the sorted CD169+ macrophages. f Relative Ccl12, Ccl2, Cxcl10 and Ccl6 mRNA levels in the sorted cells from the four gates. g Concentrations of CCL12 in the supernatants of the sorted cells from the four gates after culturing 24 h in vitro without any stimulation. h Concentrations of CCL12 in the liver homogenate. i Relative Ccl12 mRNA levels of the BMDM with or without stimulation with IFNγ in vitro. j Concentrations of CCL12 in the supernatants of the BMDM with or without stimulation with IFNγ in vitro. Results are expressed as mean ± standard error. u.d., under detection. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001.
Meanwhile, given that CD169+ macrophages are IFNγ-responsive, as mentioned above, we investigated whether IFNγ could promote CCL12 expression in CD169+ macrophages. We found that BMDMs from WT mice stimulated by IFNγ expressed higher mRNA levels of Ccl12 (Fig. 6i), and the protein levels of CCL12 in the cell supernatant was also significantly increased (Fig. 6j). In addition, the mRNA levels of the other three chemokines in these BMDMs were examined. Ccl2 and Cxcl10, known IFNγ-responsive chemokines, were upregulated following IFNγ stimulation (Supplementary Fig. 8h).
Taken together, CD169+ macrophages actively produce CCL12 in AIH in response to IFNγ stimulation.
CCL12 recruits monocytes and macrophages to exacerbate AIH
Next, we explored which types of immune cell were chemotactic by CCL12. As CCL12 has only one known receptor, chemokine (C–C motif) receptor 2 (CCR2), we examined CCR2 expression on immune cells in the AIH liver. The results of the scRNA-seq analysis indicated that CCR2 was mainly expressed in macrophages (Fig. 7a). Then, we classified CD45+ cells in the liver of AIH using flow cytometry (Supplementary Fig. 9a). After t-distributed stochastic neighbor embedding (tSNE) dimensionality reduction processing, we found that the majority of CCR2+ cells were Ly6C+ monocytes and macrophages (Fig. 7b). This is consistent with our previous results: the infiltration of Ly6C+ monocytes and macrophages in the AIH liver decreased after CD169+ macrophage depletion (Fig. 4f, g). Therefore, the migration of RAW264.7 cells (a mouse macrophage cell line) toward CCL12 was examined in vitro. We found that the chemotactic effect increased with rising CCL12 concentrations (Fig. 7c). Furthermore, we found that using CCL12 neutralizing antibodies (Fig. 7d) notably improved ConA-induced liver necrosis in mice and reduced serum ALT and AST levels (Fig. 7e, f). Both monocytes and macrophages significantly decreased after neutralizing CCL12, as demonstrated by immunohistochemistry (Fig. 7g, h).
a Expression of Ccr2 in the different clusters in AIH livers identified by the scRNA-seq dataset. b Expression of CCR2 in the different immune cells in the liver of AIH mice identified by flow cytometry. c CCL12 chemotaxis RAW264.7 cell line in vitro. d Schematic diagram of CCL12 neutralization. Anti-mouse CCL12 antibody and isotype control were both used at 1 μg/g bodyweight intravenously. To induce AIH, 10 mg/kg ConA was injected into mice intravenously. e Serum ALT and AST levels of the AIH mice treated with CCL12 neutralizing or isotype antibodies. f H&E staining of the AIH mice treated with CCL12 neutralizing antibodies or isotype control. g Immunohistochemical staining of Ly6C in the liver sections of the AIH mice treated with CCL12 neutralizing antibody or isotype control. h Immunohistochemical staining of F4/80 in the liver sections of the AIH mice treated with CCL12 neutralizing antibody or isotype control. Results are expressed as mean ± standard error. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001.
In summary, CCL12 recruited CCR2+ monocytes and macrophages, thereby exacerbating AIH in mice.
Discussion
Previous studies have extensively reported the important role of macrophages in AIH8,9, and here we identified that CD169+ macrophages are a key subset of them. Compared with the CD169− macrophages in AIH, CD169+ macrophages are more responsive to IFNγ and secrete CCL12 more actively, thus recruiting CCR2+ monocytes and macrophages as a ‘macrophage amplifier’.
Our results suggest that there are at least two different populations of CD169+ macrophages in the liver of AIH: bone marrow-derived Ly6Chi infiltrating macrophages and tissue-resident CD169+ macrophages. CD169 has previously been used as a marker of tissue-resident macrophages in many studies31,32, but in recent years, an increasing number of studies have shown that CD169+ macrophages can also be inflammatory infiltrating macrophages33,34. Our results indicated that bone marrow-derived CD169+ macrophages are the key macrophage subset in the progression of ConA, suggesting that, in addition to tissue-resident KCs, non-tissue-resident macrophages can also play an important role in acute liver injury.
After the depletion of CD169+ macrophages, not only was monocyte and macrophage infiltration in the liver reduced, but T cell infiltration was also decreased. This may be explained by the fact that CXCL10, a chemokine that recruits T cells, is expressed at higher levels in CD169+ macrophages, consistent with a previous study33. Meanwhile, previous studies have demonstrated that CD169+ macrophages can serve as antigen-presenting cells for CTL priming35 and promote the early activation of CD8+ T cells36. Our results suggest that CD169+ macrophage depletion has no significant effect on CD8+ T cell activation. These findings suggest that the interaction between CD169+ macrophages and T cells may be different under various pathological conditions, which may be related to the different expression of surface receptors on T cells under various pathological conditions. In addition, depletion of CD169+ macrophages induces a significant expansion of immunosuppressive Treg cells, which contributes to the attenuation of dysregulated autoimmune responses characteristic of AIH, thereby ameliorating the disease progression. Similar results, in which the proportion of Treg cells increased after depletion of CD169+ macrophages, have also been reported in other autoimmune diseases37, suggesting that CD169+ macrophages play an important role in immunosuppression.
CD169 was previously reported to be a type I IFN-inducible protein26. Recent studies have shown that IFNγ can induce CD169 on monocytes from patients with Graves’ disease, and the inducing effect is stronger than that of type I IFN (including IFNα and IFNβ)38. Our results suggested that CD169+ macrophages in AIH were IFNγ responsive.
CCL12, also known as monocyte chemoattractant protein (MCP) 5, has only one receptor, CCR2. In previous studies, CCL12 was found to be involved in inflammation and injury, such as participating in allergic inflammation39, promoting bone loss during acute lung injury40 and aggravating brain injury in aged mice41. In the present study, we found that the CCL12 level was elevated in AIH, suggesting that CCL12 also plays a role in ConA-induced liver injury. Moreover, our results showed that CD169+ macrophages could actively produce CCL12 in AIH, and the production of CCL12 in CD169+ macrophages could be enhanced by IFNγ in vitro, further illustrating the possible role of CCL12 in inflammatory diseases. However, in contrast to our present findings, a previous study indicated that CD169+ macrophages promote colitis by secreting CCL8 rather than CCL1234. These results suggest that the chemokine secretion profile of CD169+ macrophages can vary across diseases. The immune microenvironment varies across diseases and tissues, causing CD169+ macrophages to exhibit different responses and suggesting their flexibility or adaptability in distinct microenvironments.
We acknowledge that our study has some limitations. First, we did not explore the role of CD169+ KCs in AIH. Although bone marrow-derived CD169+ macrophages play a crucial role in AIH, it is undeniable that the depletion of CD169+ KCs may also contribute to the alleviation of acute liver injury. Second, considering that CD169 contained a short cytoplasmic tail that lacks signaling motifs, we addressed the function of CD169+ macrophages but not the role of CD169 molecule in AIH. In future studies, we plan to use CD169-specific knockout mice to investigate the function of CD169 and further characterize CD169+ macrophages. Third, considering the strong correlation between CD169+ macrophages and progression of inflammation in the AIH liver, we used a ConA model to mimic the acute inflammation of AIH and did not explore the role of CD169+ macrophages in the chronic progression of AIH, which may not reproduce all clinical characteristics of human disease. Furthermore, CD169+ macrophages also play a role in proresolving and reparative responses after an injury42. However, post-injury repair is not addressed in our study. In summary, the roles and functions of CD169+ macrophages should be further investigated for developing reliable strategies toward AIH.
In summary, we found that CD169+ macrophages infiltrate the livers of both mice and humans with AIH, and that bone marrow-derived CD169+ macrophages represent a crucial subset driving AIH progression. Depletion of CD169+ macrophages ameliorated ConA-induced AIH. In response to IFNγ signaling, CD169+ macrophages act like a macrophage amplifier to actively secrete CCL12 to recruit more CCR2+ monocytes and macrophages, further aggravating acute liver injury. In the future, targeting bone marrow-derived CD169+ macrophages may be a potential strategy for the treatment of AIH.
Data availability
The data are available from the corresponding author on reasonable request.
References
Heneghan, M. A., Yeoman, A. D., Verma, S., Smith, A. D. & Longhi, M. S. Autoimmune hepatitis. Lancet 382, 1433–1444 (2013).
Muratori, L., Lohse, A. W. & Lenzi, M. Diagnosis and management of autoimmune hepatitis. BMJ 380, e070201 (2023).
Colapietro, F. et al. Incidence and predictors of hepatocellular carcinoma in patients with autoimmune hepatitis. J. Hepatol. 80, 53–61 (2024).
He, G. W. et al. PGAM5-mediated programmed necrosis of hepatocytes drives acute liver injury. Gut 66, 716–723 (2017).
Zhao, J. et al. C/EBPα/miR-7 controls CD4+ T-cell activation and function and orchestrates experimental autoimmune hepatitis in mice. Hepatology 74, 379 (2021).
Xu, C. et al. CD36 deficiency attenuates immune-mediated hepatitis in mice by modulating the proapoptotic effects of CXC chemokine ligand 10. Hepatology 67, 1943–1955 (2018).
Lyu, Z. et al. Suppression of YTHDF2 attenuates autoimmune hepatitis by expansion of myeloid-derived suppressor cells. J. Autoimmun. 135, 102993 (2023).
Li, X. et al. zVAD alleviates experimental autoimmune hepatitis in mice by increasing the sensitivity of macrophage to TNFR1-dependent necroptosis. J. Autoimmun. 133, 102904 (2022).
Liu, Z. et al. Circadian control of ConA-induced acute liver injury and inflammatory response via Bmal1 regulation of Junb. JHEP Rep. 5, 100856 (2023).
Wen, Y., Lambrecht, J., Ju, C. & Tacke, F. Hepatic macrophages in liver homeostasis and diseases-diversity, plasticity and therapeutic opportunities. Cell Mol. Immunol. 18, 45 (2021).
Guilliams, M. & Scott, C. L. Liver macrophages in health and disease. Immunity 55, 1515–1529 (2022).
Gomez Perdiguero, E. et al. Tissue-resident macrophages originate from yolk-sac-derived erythro-myeloid progenitors. Nature 518, 547–551 (2015).
Soucie, E. L. et al. Lineage-specific enhancers activate self-renewal genes in macrophages and embryonic stem cells. Science 351, aad5510 (2016).
Baeck, C. et al. Pharmacological inhibition of the chemokine CCL2 (MCP-1) diminishes liver macrophage infiltration and steatohepatitis in chronic hepatic injury. Gut 61, 416–426 (2012).
Hartnell, A., Steel, J., Turley, H., Jones, M., Jackson, D. G. & Crocker, P. R. Characterization of human sialoadhesin, a sialic acid binding receptor expressed by resident and inflammatory macrophage populations. Blood 97, 288–296 (2001).
Martinez-Pomares, L. & Gordon, S. CD169+ macrophages at the crossroads of antigen presentation. Trends Immunol. 33, 66–70 (2012).
Crocker, P. R. & Gordon, S. Properties and distribution of a lectin-like hemagglutinin differentially expressed by murine stromal tissue macrophages. J. Exp. Med. 164, 1862–1875 (1986).
Chávez-Galán, L., Olleros, M. L., Vesin, D. & Garcia I. Much more than M1 and M2 macrophages, there are also CD169+ and TCR+ macrophages. Front. Immunol. 6, 263 (2015).
Bogie, J. F. et al. CD169 is a marker for highly pathogenic phagocytes in multiple sclerosis. Mult. Scler. J. 24, 290–300 (2018).
Eakin, A. J. et al. CD169+ monocyte and regulatory T cell subsets are associated with disease activity in rheumatoid arthritis. J. Pers. Med. 12, 1875 (2022).
Xiong, Y. S. et al. Increased expression of Siglec-1 on peripheral blood monocytes and its role in mononuclear cell reactivity to autoantigen in rheumatoid arthritis. Rheumatology 53, 250–259 (2014).
Sakumura, N. et al. CD169 expression on monocytes as a marker for assessing type I interferon status in pediatric inflammatory diseases. Clin. Immunol. 250, 109329 (2023).
Ferreira, R.C. et al. A type I interferon transcriptional signature precedes autoimmunity in children genetically at risk for type 1 diabetes. Diabetes 63, 2538–2550 (2014).
Bao, G. et al. Increased Siglec-1 expression in monocytes of patients with primary biliary cirrhosis. Immunol. Invest. 39, 645–660 (2010).
Batoon, L. et al. CD169+ macrophages are critical for osteoblast maintenance and promote intramembranous and endochondral ossification during bone repair. Biomaterials 196, 51–66 (2019).
Liao, J. et al. Type I IFNs repolarized a CD169+ macrophage population with anti-tumor potentials in hepatocellular carcinoma. Mol. Ther. 30, 632–643 (2022).
Gupta, P. et al. Tissue-resident CD169+ macrophages form a crucial front line against Plasmodium infection. Cell Rep. 16, 1749–1761 (2016).
Barreby, E., Chen, P. & Aouadi, M. Macrophage functional diversity in NAFLD—more than inflammation. Nat. Rev. Endocrinol. 18, 461–472 (2022).
Fu, J. T. et al. Targeting EFHD2 inhibits interferon-γ signaling and ameliorates non-alcoholic steatohepatitis. J. Hepatol. 81, 389–403 (2024).
Fujita, T. et al. Hepatic stellate cells relay inflammation signaling from sinusoids to parenchyma in mouse models of immune-mediated hepatitis. Hepatology 63, 1325 (2016).
Du, X. et al. Increased Tim-3 expression alleviates liver injury by regulating macrophage activation in MCD-induced NASH mice. Cell Mol. Immunol. 16, 878–886 (2019).
Ural, B. B. et al. Identification of a nerve-associated, lung-resident interstitial macrophage subset with distinct localization and immunoregulatory properties. Sci. Immunol. 5, eaax8756 (2020).
Kim, H. J., Park, J. H., Kim, H. C., Kim, C. W., Kang, I. & Lee, H. K. Blood monocyte-derived CD169+ macrophages contribute to antitumor immunity against glioblastoma. Nat. Commun. 13, 6211 (2022).
Asano, K. et al. Intestinal CD169+ macrophages initiate mucosal inflammation by secreting CCL8 that recruits inflammatory monocytes. Nat. Commun. 6, 7802 (2015).
Bernhard, C. A., Ried, C., Kochanek, S. & Brocker, T. CD169+ macrophages are sufficient for priming of CTLs with specificities left out by cross-priming dendritic cells. Proc. Natl Acad. Sci. USA 112, 5461–5466 (2015).
Asano, K. et al. CD169-positive macrophages dominate antitumor immunity by crosspresenting dead cell-associated antigens. Immunity 34, 85–95 (2011).
Qi, W. et al. CD169+ macrophages mediate the immune response of allergic rhinitis through the Keap1/Nrf2/HO-1 axis. Adv. Sci. 11, 2309331 (2024).
Wang, D. et al. CD169+ classical monocyte as an important participant in Graves’ ophthalmopathy through CXCL12–CXCR4 axis. iScience 27, 109213 (2024).
Sarafi, M. N., Garcia-Zepeda, E. A., MacLean, J. A., Charo, I. F. & Luster, A. D. Murine monocyte chemoattractant protein (MCP)-5: a novel CC chemokine that is a structural and functional homologue of human MCP-1. J. Exp. Med. 185, 99–110 (1997).
Ma, C. et al. CCL12 induces trabecular bone loss by stimulating RANKL production in BMSCs during acute lung injury. Exp. Mol. Med. 55, 818–830 (2023).
Huang, J. et al. Age-related CCL12 aggravates intracerebral hemorrhage-induced brain injury via recruitment of macrophages and T lymphocytes. Aging Dis 11, 1103–1115 (2020).
Ismahil, M. A. et al. Splenic CD169+Tim4+ marginal metallophilic macrophages are essential for wound healing after myocardial infarction. Circulation 151, 1712–1729 (2025).
Acknowledgements
We thank Z. Gao and H. Zhao from Shanghai Universal Biotech Company for their technical assistance with flow cytometry. The graphical abstract was created with BioRender.com.
Funding
This work was supported by the National Natural Science Foundation of China (grant no. 82030019 to C.Y.; grant nos. 82130017, 81830016 and 82330018 to X.M.; grant no. 82270553 to Z.Y.; grant no. 82370573 to H. Zeng), the Key Research and Development Program of Zhejiang Province (grant no. 2022E50010 to C.Y.), the Joint Funds of the National Natural Science Foundation of China (grant no. U23A20400 to C.Y.), the Innovative Research Team of High-level Local Universities in Shanghai (grant no. SHSMU-ZDCX20210301 to X.M., and grant no. SHSMU-ZLCX20211600 to Z.Y.), and Shanghai Top-Priority Medical Center Construction Project (grant no. 2023ZZ02022 to X.M.), and Natural Science Foundation of Zhejiang Province (grant no. LQ22H030011 to J.W.).
Author information
Authors and Affiliations
Contributions
B.L.: investigation; methodology; visualization; writing—original draft. H. Zhang: investigation; methodology; writing—review and editing. P.Z.: investigation; methodology; writing—review and editing. J.C: investigation; methodology. D.L: resources; validation. J. Zhou: investigation; methodology. T.Z.: visualization; validation. Q.C.: investigation. C.T.: investigation. X.S.: investigation. H. Zeng: investigation; funding acquisition. J.W.: investigation; funding acquisition. J. Zhang: investigation. Z.Y.: conceptualization; funding acquisition; supervision; writing—review and editing. X.M.: conceptualization; funding acquisition; supervision; writing—review and editing. C.Y.: conceptualization; funding acquisition; supervision; writing—review and editing. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lin, B., Zhang, H., Zhu, P. et al. Bone marrow-derived CD169+ macrophages promote autoimmune hepatitis by recruiting CCR2+ monocytes via secreting CCL12. Exp Mol Med 57, 2930–2942 (2025). https://doi.org/10.1038/s12276-025-01607-w
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s12276-025-01607-w