Abstract
Background
Over the past decade, the range of surgical options to benign prostatic obstruction (BPO) has expanded significantly with the advent of minimally invasive surgical therapies (MISTs). Nevertheless, the available evidence in the field is heterogeneous. Efficacy and safety thresholds are yet to be determined.
Objective
To evaluate perioperative and long-term complications after MISTs - including Aquablation, steam injection (Rezūm), Transperineal laser ablation of the prostate (TPLA), implantation of a prostatic urethral lift (PUL) and temporary implantable nitinol device (iTIND) - in patients with lower urinary tract symptoms due to BPO.
Evidence acquisition
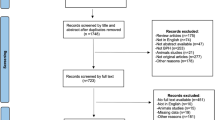
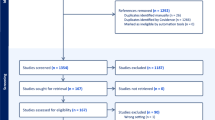
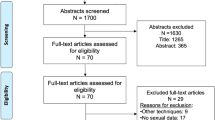
A systematic literature search was conducted in January 2024 using Medline (via PubMed), Embase (via Ovid), Scopus, and Web of Science. The search strategy used PICO criteria (Patients, Interventions, Comparisons, Outcomes) [1], focusing specifically on patients with BPH-associated LUTS who underwent MIST or other comparative treatments, aiming to assess both perioperative and long-term safety outcomes. Article selection was conducted in accordance with the PRISMA guidelines. The risk of bias and the quality of the articles included were assessed. A dedicated data extraction form was used to collect the data of interest.
Evidence synthesis
The initial electronic search identified 3660 records, of which 24 ultimately met the inclusion criteria and were included in the analysis. Overall, Aquablation was associated with a higher major complications rate of 14% (IQR 6–22), particularly in the case of patients with prostates <70 ml. PUL showed a higher early postoperative acute urinary retention rate (10.9%, IQR 9.2–12.3%), while 1.4% of patients treated with iTIND experienced major perioperative complications. Urinary tract infections were mostly reported in series assessing TPLA and Rezūm.
Conclusions
The adoption of MISTs for LUTS due to BPH is associated with a varied spectrum of perioperative and long-term complications. Our findings showed an acceptable safety profile with specific complications dependent on the type of MIST performed, highlighting the importance of individualized patient selection and procedure-specific considerations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Cumpston M, Li T, Page MJ, Chandler J, Welch VA, Higgins JP, et al. Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst Rev. 2019;10:ED000142.
McVary KT. BPH: epidemiology and comorbidities. Am J Managed Care. 2006;12:S122–8.
Anezaki H, Endo F, Swan G, Takashima K, Rojanasarot S. Cost-effectiveness analysis of minimally invasive surgical treatments for benign prostatic hyperplasia: implications for Japan’s public healthcare system. J Med Econ. 2024;27:554–65.
Sun Y, Peng B, Lei GL, Wei Q, Yang L. Study of phosphodiesterase 5 inhibitors and α-adrenoceptor antagonists used alone or in combination for the treatment of lower urinary tract symptoms due to benign prostatic hyperplasia. Ital J Urol Nephrol. 2020;72:13–21.
Zhang Y, Yuan P, Ma D, Gao X, Wei C, Liu Z, et al. Efficacy and safety of enucleation vs. resection of prostate for treatment of benign prostatic hyperplasia: a meta-analysis of randomized controlled trials. Prostate Cancer Prostatic Dis. 2019;22:493–508.
Cornu JN, Dupuis H, Gazdovich S. Hot Topics of the Past Decade: Evolutions and Revolutions in Lower Urinary Tract Symptoms. Eur Urol Focus. 2022;8:371–4.
Huang SW, Tsai CY, Tseng CS, Shih MC, Yeh YC, Chien KL, et al. Comparative efficacy and safety of new surgical treatments for benign prostatic hyperplasia: systematic review and network meta-analysis. BMJ. 2019;367:l5919.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg. 2010;8:336–41.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: A new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Bhojani N, Bidair M, Zorn KC, Trainer A, Arther A, Kramolowsky E, et al. Aquablation for Benign Prostatic Hyperplasia in Large Prostates (80-150 cc): 1-Year Results. Urology 2019;129:1–7.
Gilling P, Barber N, Bidair M, Anderson P, Sutton M, Aho T, et al. Three-year outcomes after Aquablation therapy compared to TURP: results from a blinded randomized trial. Can J Urol. 2020;27:10072–9.
De Nunzio C, Cantiello F, Fiori C, Crocerossa F, Tognoni P, Amparore D, et al. Urinary and sexual function after treatment with temporary implantable nitinol device (iTind) in men with LUTS: 6-month interim results of the MT-06-study. World J Urol. 2021;39:2037–42.
Elterman D, Shepherd S, Saadat SH, Alshak MN, Bhojani N, Zorn KC, et al. Prostatic urethral lift (UroLift) versus convective water vapor ablation (Rezum) for minimally invasive treatment of BPH: a comparison of improvements and durability in 3-year clinical outcomes. Can J Urol. 2021;28:10824–33.
Sønksen J, Barber NJ, Speakman MJ, Berges R, Wetterauer U, Greene D, et al. Prospective, randomized, multinational study of prostatic urethral lift versus transurethral resection of the prostate: 12-month results from the BPH6 study. Eur Urol. 2015;68:643–52.
Samir M, Elaal AAA, Gad KAS, Basyony MW. Two-year follow-up comparing Rezūm therapy versus bipolar transurethral resection of the prostate for treating benign prostatic hyperplasia. A prospective randomized study. Int J Urol. 2024;31:545–50.
Roehrborn CG, Gange SN, Gittelman MC, Goldberg KA, Patel K, Shore ND, et al. Convective Thermal Therapy: Durable 2-Year Results of Randomized Controlled and Prospective Crossover Studies for Treatment of Lower Urinary Tract Symptoms Due to Benign Prostatic Hyperplasia. The. J Urol. 2017;197:1507–16.
Bertolo R, Ditonno F, Veccia A, De Marco V, Migliorini F, Porcaro AB, et al. Postoperative outcomes of transperitoneal versus retroperitoneal robotic partial nephrectomy: a propensity-score matched comparison focused on patient mobilization, return to bowel function, and pain. J Robotic Surg. 2024;18:96.
Canat HL, Gurbuz C, Bozkurt M. Transurethral resection of the prostate (TURP) versus transperineal laser ablation (TPLA) due to benign prostatic hyperplasia (BPH): prospective and comparative study. Int Urol Nephrol. 2023;55:2747–52.
Gilling PJ, Barber N, Bidair M, Anderson P, Sutton M, Aho T, et al. Randomized Controlled Trial of Aquablation versus Transurethral Resection of the Prostate in Benign Prostatic Hyperplasia: One-year Outcomes. Urology 2019;125:169–73.
Labban M, Mansour M, Abdallah N, Jaafar R, Wazzan W, Bulbul M, et al. Aquablation for benign prostatic obstruction: Single center technique evolution and experience. Investigative Clin Urol. 2021;62:210–6.
Desai M, Bidair M, Bhojani N, Trainer A, Arther A, Kramolowsky E, et al. WATER II (80-150 mL) procedural outcomes. BJU Int. 2019;123:106–12.
Misrai V, Rijo E, Zorn KC, Barry-Delongchamps N, Descazeaud A. Waterjet Ablation Therapy for Treating Benign Prostatic Obstruction in Patients with Small- to Medium-size Glands: 12-month Results of the First French Aquablation Clinical Registry. Eur Urol. 2019;76:667–75.
Zorn KC, Bidair M, Trainer A, Arther A, Kramolowsky E, Desai M, et al. Aquablation therapy in large prostates (80-150 cc) for lower urinary tract symptoms due to benign prostatic hyperplasia: WATER II 3-year trial results. BJUI Compass. 2022;3:130–8.
Bach T, Gilling P, El Hajj A, Anderson P, Barber N. First Multi-Center All-Comers Study for the Aquablation Procedure. J Clin Med. 2020;9:603.
Desai M, Bidair M, Bhojani N, Trainer A, Arther A, Kramolowsky E, et al. Aquablation for benign prostatic hyperplasia in large prostates (80-150 cc): 2-year results. Can J Urol. 2020;27:10147–53.
Rukstalis D, Grier D, Stroup SP, Tutrone R, deSouza E, Freedman S, et al. Prostatic Urethral Lift (PUL) for obstructive median lobes: 12 month results of the MedLift Study. Prostate Cancer Prostatic Dis. 2019;22:411–9.
de Rienzo G, Lorusso A, Minafra P, Zingarelli M, Papapicco G, Lucarelli G, et al. Transperineal interstitial laser ablation of the prostate, a novel option for minimally invasive treatment of benign prostatic obstruction. Eur Urol. 2021;80:95–103.
Cai HJ, Fang JH, Kong FL, Xu CK, Chen CH, Wang W, et al. Ultrasound-guided transperineal laser ablation for percutaneous treatment of benign prostatic hyperplasia: a new minimally invasive interventional therapy. Acta Radiol. 2022;63:553–8.
Frego N, Saita A, Casale P, Diana P, Contieri R, Avolio PP, et al. Feasibility, safety, and efficacy of ultrasound-guided transperineal laser ablation for the treatment of benign prostatic hyperplasia: a single institutional experience. World J Urol. 2021;39:3867–73.
Ghiraldi E, Higgins AM, Sterious S. Initial Experience Performing “Cautery-Free Waterjet Ablation of the Prostate”. J Endourol. 2022;36:1237–42.
El-Asmar JM, Labban M, El-Hajj A. Integration of aquablation through telemetry: an alternative to onsite proctoring? World J Urol. 2021;39:3473–9.
Elterman DS, Foller S, Ubrig B, Kugler A, Misrai V, Porreca A, et al. Focal bladder neck cautery associated with low rate of post-Aquablation bleeding. Can J Urol. 2021;28:10610–3.
McVary KT, Roehrborn CG. Three-Year Outcomes of the Prospective, Randomized Controlled Rezūm System Study: Convective Radiofrequency Thermal Therapy for Treatment of Lower Urinary Tract Symptoms Due to Benign Prostatic Hyperplasia. Urology. 2018;111:1–9.
Polverino P, Lo Re M, Saladino M, Pecoraro A, Moscardi L, Rivetti A, et al. Could transperineal interstitial laser ablation of the prostate be the right option for highly-comorbid patients with lower urinary tract symptoms due to benign prostatic obstruction? A preliminary single-center experience focusing on functional and safety outcomes. Minerva Urol Nephrol. 2024;76:646–9.
Pacella CM, Patelli G, Iapicca G, Manenti G, Perretta T, Ryan CP, et al. Transperineal laser ablation for percutaneous treatment of benign prostatic hyperplasia: a feasibility study. Results at 6 and 12 months from a retrospective multi-centric study. Prostate Cancer Prostatic Dis. 2020;23:356–63.
Minore A, Morselli S, Franzoso F, Maruzzi D, Varvello F, Toso S, et al. Is water vapor thermal therapy safe and feasible in elderly and frail men? The Italian experience. World J Urol. 2024;42:60 https://doi.org/10.1007/s00345-023-04762-9
Amparore D, Fiori C, Valerio M, Schulman C, Giannakis I, De Cillis S, et al. 3-Year results following treatment with the second generation of the temporary implantable nitinol device in men with LUTS secondary to benign prostatic obstruction. Prostate Cancer Prostatic Dis. 2021;24:349–57.
Sahakyan Y, Erman A, Bhojani N, Chughtai B, Zorn KC, Sander B, et al. Pharmacotherapy vs. minimally invasive therapies as initial therapy for moderate-to-severe benign prostatic hyperplasia: a cost-effectiveness study. Prostate Cancer Prostatic Dis. 2023;26:113–8.
Tanneru K, Jazayeri SB, Alam MU, Kumar J, Bazargani S, Kuntz G, et al. An Indirect Comparison of Newer Minimally Invasive Treatments for Benign Prostatic Hyperplasia: A Network Meta-Analysis Model. J Endourol. 2021;35:409–16.
Sibona M, Destefanis P, Vercelli E, Secco S, Gontero P, Cindolo L. Ejaculation physiology and dysfunction after BPH surgery: the role of the new MISTs. Prostate Cancer Prostatic Dis. 2023;26:475–82.
Franco JV, Jung JH, Imamura M, Borofsky M, Omar MI, Escobar Liquitay CM, et al. Minimally invasive treatments for lower urinary tract symptoms in men with benign prostatic hyperplasia: a network meta-analysis. Cochrane Database Syst Rev. 2021;7:CD013656.
Porto JG, Arbelaez MCS, Blachman-Braun R, Bhatia A, Bhatia S, Satyanarayana R, et al. Complications associated with minimally invasive surgical therapies (MIST) for surgical management of benign prostatic hyperplasia: a Manufacturer and User Facility Device Experience (MAUDE) database review. World J Urol. 2023;41:1975–82.
Zhu M, Babar M, Hawks-Ladds N, Tawfik MM, Loloi J, Labagnara K, et al. Real-world four-year functional and surgical outcomes of Rezum therapy in younger versus elderly men. Prostate Cancer Prostatic Dis. 2024;27:109–15.
Bertolo R, Iacovelli V, Cipriani C, Carilli M, Vittori M, Antonucci M, et al. Ejaculatory function following transperineal laser ablation vs TURP for benign prostatic obstruction: a randomized trial. BJU Int. 2023;132:100–8.
Kim J, Polchert M, Chacko B, Tannenbaum J, Raheem O. Do Minimally Invasive Benign Prostatic Hyperplasia Treatments Preserve Sexual Function? A Contemporary Review of the Literature. Curr Urol Rep. 2021;22:56.
Elterman D, Gao B, Lu S, Bhojani N, Zorn KC, Chughtai B. New Technologies for Treatment of Benign Prostatic Hyperplasia. The. Urologic Clin North Am. 2022;49:11–22.
Sun F, Yao H, Bao X, Wang X, Wang D, Zhang D, et al. The Efficacy and Safety of HoLEP for Benign Prostatic Hyperplasia With Large Volume: A Systematic Review and Meta-Analysis. Am J Mens Health. 2022;16:15579883221113204.
Nguyen DD, Li T, Ferreira R, Baker Berjaoui M, Nguyen ALV, Chughtai B, et al. Ablative minimally invasive surgical therapies for benign prostatic hyperplasia: A review of Aquablation, Rezum, and transperineal laser prostate ablation. Prostate Cancer Prostatic Dis. 2024;27:22–8.
Siena G, Sessa F, Cindolo L. Use of a Schelin Catheter for analgesia during Rezum treatment of the prostate. Prostate Cancer Prostatic Dis. 2024;27:147–9.
Roehrborn CG, Chin PT, Woo HH. The UroLift implant: mechanism behind rapid and durable relief from prostatic obstruction. Prostate Cancer Prostatic Dis. 2022;25:79–85.
Tafuri A, Panunzio A, De Carlo F, Luperto E, Di Cosmo F, Cavaliere A, et al. Transperineal Laser Ablation for Benign Prostatic Enlargement: A Systematic Review and Pooled Analysis of Pilot Studies. J Clin Med. 2023;12:1860.
Destefanis P, Sibona M, Vitiello F, Vercelli E, Micai L, Montefusco G, et al. Trans - Perineal laser ablation of the prostate in high surgical risk patients affected by severe lower urinary tract symptoms related to benign prostatic obstruction. Prostate Cancer Prostatic Dis. 2023 https://doi.org/10.1038/s41391-023-00736-5 Epub ahead of print.
Author information
Authors and Affiliations
Contributions
LL: Conceptualization, data analysis, original draft preparation. AS, SC, DP: Data collection, Data Analysis; AC: Data collection and curation; PDO, SP, FDM, AAG, DA, RB, RC, RL, MF, BR, GV, AA, CDN: Manuscript revision and editing; AM, AM: Supervision, original draft preparation, conceptualization.
Corresponding author
Ethics declarations
Competing interests
CDN, Editor in Chief of prostate Cancer and Prostatic Disease.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lambertini, L., Sandulli, A., Coco, S. et al. Complication rate across the minimally invasive surgical treatments (MISTs): where do we stand? A systematic review of the literature. Prostate Cancer Prostatic Dis 28, 639–651 (2025). https://doi.org/10.1038/s41391-024-00900-5
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41391-024-00900-5
This article is cited by
-
MISTs for benign prostatic hyperplasia as first line interventional treatment: Alea iacta est?
Prostate Cancer and Prostatic Diseases (2026)
-
Best of 2024 in Prostate Cancer and Prostatic diseases
Prostate Cancer and Prostatic Diseases (2025)
-
Short term results after minimally invasive treatments for benign prostatic enlargement: the first randomized trial comparing transperineal laser ablation and water vapor ablation
Prostate Cancer and Prostatic Diseases (2025)
-
Transperineal laser ablation in the management of benign prostatic hyperplasia: an updated systematic review and pooled analysis
Prostate Cancer and Prostatic Diseases (2025)
-
Thulium laser incision of prostate with selective median lobe vaporesection versus water vapor thermal therapy in the treatment of benign prostatic obstruction with ejaculation-sparing intent: a retrospective, comparative analysis from two institutions
International Urology and Nephrology (2025)