Abstract
The broader clinical application of Bispecific T-cell engagers (BiTEs) is hindered by their short half-life, on-target off-tumor toxicity, and limited therapeutic effect for solid tumors. Herein, we constructed a bimetallic-enriched triple-kill nanobomb manganese/Co2+-dopamine@BiTE/HPT (MnO2/Co-DA@BiTE/HPT) based on metal-polyphenol to improve the immunosuppressive tumor microenvironment by activating innate and adaptive immunity, thereby enhancing the treatment efficacy of BiTEs (PD-L1/CD3). A hyaluronic acid-modified PD-L1 aptamer (HPT) was introduced to improve the active targeting of the nanobombs and bind with PD-L1 overexpressing colorectal cancer. Bimetallic (Mn2+/Co2+) activated the STING pathway; simultaneously, photothermal therapy (PTT) induces DNA fragmentation to cooperate with bimetallic to amplify the STING signal to “heat” the “cold” tumor microenvironment. The “hot” tumor with a large amount of T-cell infiltration facilitated BiTE recruitment of T cells to kill tumor cells. Furthermore, the efficient therapeutic potency of the triple-kill nanobombs (STING, BiTE, and PTT) was determined in subcutaneous colorectal cancer, distal, lung metastasis, and postoperative recurrence models, which indicated that MnO2/Co-DA@BiTE/HPT could improve the immune microenvironment, produce long-term immune memory, inhibit tumor growth, and prevent tumor recurrence and metastasis.
Similar content being viewed by others
Introduction
Immunotherapy, the fourth type of therapy after surgery, chemotherapy, and radiotherapy, has made revolutionary progress in cancer treatment by specifically activating the immune system against tumors.1,2 Bispecific T-cell engagers (BiTEs) are unique-targeted antibodies that recruit cytotoxic T cells against tumors by simultaneously targeting CD3 and tumor-specific antigens to promote selective T-cell killing responses.3,4 BiTE, consisting of bi-antigen specificity, can bind to two unique antigens at the same time, thus facilitating cell-to-cell interactions, which is different from antibodies that have a single antigen specificity.5 Blinatumomab, a CD3/CD19-specific antibody, was approved by the Food and Drug Administration (FDA) in 2014 for the treatment of acute lymphoblastic leukemia.6 More than 50 CD3-based T-cell BiTE antibodies, including Her2/CD3 and PSMA/CD3, are currently in clinical trials.7 However, the therapeutic effect of BiTE appears to be limited to immunogenic tumors that exhibit substantial lymphocyte infiltration and tumor-associated antigen (TAA) expression.8,9 Additionally, the clinical application of BiTE therapy in solid tumors has been limited by challenges such as short half-life, “off-target” effects, and immune tolerance. To address these issues, various nanomaterial-based delivery systems have been developed to encapsulate BiTEs, enhancing their stability, targeting capability, and safety profile. These include SiTE, PSTAGylated BiTE, S-biAb/dEGCG@NPs, and BiTEs-GSP-NCs.10,11,12,13 For instance, Gong et al. developed a supramolecular bispecific T cell engager via the infusion of the small-molecule drug amantadine, which can control the anti-tumor activity and off-tumor toxicity of bispecific antibodies.10 Fan et al. used S-biAb/dEGCG@NPs nanoparticles as a delivery vehicle for B7-H3×CD3 BiTEs to improve therapeutic outcomes in glioblastoma therapy.12 Despite these promising advances, research on efficient delivery strategies for BiTEs remains relatively limited.
STING (stimulator of interferon genes), a signal transduction molecule involved in the virus-induced innate immune response, is currently a hot target for drug research and development.14,15 STING has rapidly expanded the field of research on immunology and tumor immunotherapy.16 The cGAS-STING pathway can sense not only exogenous danger signals from viruses and bacteria, but also endogenous danger signals from damaged mitochondria and endocytosis fragments of dead tumor cells.17,18 Activation of the STING pathway in antigen-presenting cells (APCs) may produce IFN-I to recruit and cross-prime effector T cells to overcome the “cold” tumor barrier.19,20,21 An increasing number of studies have begun to investigate the activation of the innate immune system by Mn2+.22,23,24 Mn2+, as the second cyclic GMP-AMP synthase (cGAS) activator in addition to DNA, can directly activate cGAS, which can enhance the body’s immune surveillance and immune clearance of tumors.22 The nano-STING combination with chemotherapy, radiotherapy, chimeric antigen receptor T-cell (CAR-T) therapy, checkpoint inhibitors, and other novel therapeutic methods can synergistically enhance the antitumor effect.25,26
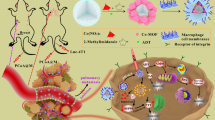
Herein, bimetallic nanobombs manganese/Co2+-dopamine (MnO2/Co-DA) with dual functions of photothermal therapy (PTT) and STING activation were formed by coordination of dopamine and Co2+ on MnO2 (Scheme 1). To enhance the ability of MnO2/Co-DA nanobombs to regulate the tumor microenvironment and overcome the off-target effects of PD-L1/CD3 BiTE, as well as the weak response of BiTE in “cold” tumors, BiTE was successfully loaded with MnO2/Co-DA by combining Co2+ with His tags in BiTE to realize the combination of the STING pathway and BiTE. Hyaluronic acid (HA)-modified PD-L1 aptamer (HPT) was introduced to prevent off-target effects and improve the active targeting of drugs. Under the self-assembly of HPT, the hierarchical loading of BiTE was realized, obtaining MnO2/Co-DA@BiTE/HPT nanobombs. The use of PTT induced DNA fragmentation to cooperate with Mn2+ and Co2+ to amplify the signal of the STING pathway, activating the innate immune system. Faced with hyaluronidase-rich tumor tissue, MnO2/Co-DA@BiTE/HPT nanobombs could rapidly depolymerize and release drugs to activate the innate and adaptive immune systems, reverse the tumor immunosuppressive microenvironment, and achieve multitarget tumor therapy.
The targeted bimetallic nanobomb (MnO2/Co-DA@BiTE/HPT) triggers the STING pathway to enhance BiTE immunotherapy
Results
Screening of metal ions
First, we successfully extracted and cultured bone marrow-derived dendritic cells (BMDCs). To investigate whether metal ions other than Mn2+ could specifically induce the secretion of IFN-β and the maturation of BMDCs. Several metal ions (Na+, Ca2+, Fe3+, Co2+) were added to incubate with BMDCs. The enzyme-linked immunosorbnent assay (ELISA) results showed that the level of interferon-β (IFN-β) was enhanced after treatment with Mn2+ and Co2+ (Fig. 1a). The phosphorylated TANK binding kinase 1 (pTBK1), phosphorylated interferon regulatory factor 3 (pIRF3), and phosphorylated STING (pSTING) proteins were analyzed to further evaluate the effects of Mn2+ and Co2+ on the STING pathway (Fig. 1b and Supplementary Fig. 1). The results showed that the addition of Mn2+ and Co2+ increased the expression levels of several phosphorylation proteins, which was consistent with a previous study. Subsequently, to evaluate whether the metal ions synergistically activate the STING pathway with MnO2, MnO2/Na-DA, MnO2/Ca-DA, MnO2/Ce-DA, and MnO2/Co-DA nanosolutions were applied to simulate BMDCs. The ELISA (Supplementary Fig. 2a) and western blot (WB) (Supplementary Figs. 2b and 3) results both indicated that MnO2/Co-DA could amplify the activation of the STING pathway owing to the synergy of Co2+ and MnO2. Therefore, the MnO2/Co-DA solution was selected as the STING activator for the subsequent experiments.
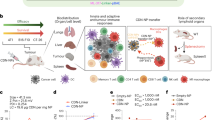
Characterization of MnO2/Co-DA@BiTE/HPT nanobombs. a IFN-β levels in culture medium after treatment with Na+, Ca2+, Fe3+, Ce3+, Mn2+, and Co2+. b WB analysis of the levels of proteins in the cGAS-STING pathway in DC2.4 cells after treatment with different concentrations of MnCl2 and CoCl2. c Diagram of PD-L1/CD3 BiTE for antitumour activity. d Binding of PD-L1×CD3 to PD-L1 on CT26 cells overexpressing PD-L1 (left) and to CD3 on CD8 T cells (right). Cells were incubated with serial dilutions of PD-L1×CD3 or mouse IgG control, followed by a fluorophore-conjugated anti-mouse IgG secondary antibody. Flow cytometry measured the specific fluorescence index (SFI) using the mean fluorescence intensity. e Transmission electron microscopy (TEM) images of MnO2/Co-DA@BiTE/HPT. f Circular dichroism of BiTE, MnO2/Co-DA@BiTE, and MnO2/Co-DA@BiTE/HPT nanobombs. g Diagram of the binding of DA to the BiTE antibody by molecular docking. h Diagram of the binding of Co2+ to the BiTE antibody by molecular docking. All data were presented as mean ± SD (n ≥ 3)
Characterization of BiTE
BiTE can bind CD3 and TAA, leading to the formation of immune synapses between T cells and tumor cells (Fig. 1c). The PD-L1/CD3 BiTE antibody with His tag was expressed by HEK293T cells (Supplementary Fig. 4). Flow cytometry was used to detect the binding affinity of PD-L1 to CT26 cells (high expression of PD-L1) and CD3 to CD8+ T cells (high expression of CD3) in BiTE structures (Supplementary Fig. 5). As shown in Fig. 1d, PD-L1/CD3 BiTE could specifically bind CT26 cells and CD8+ T cells. Compared with IgG, BiTE had a stronger binding affinity with CT26 and CD8+ T cells with increasing concentration. When T cells/CT26 cells were cultured with BiTE, the level of IFN-γ (Supplementary Fig. 6a) and the proportion of activated T cells (Supplementary Fig. 6b) increased with increasing BiTE concentration. Additionally, Supplementary Fig. 7 shows that T cells surrounded CT26 cells and lysed tumor cells after treatment with BiTE. The killing effect of T cells became more obvious with increasing BiTE concentration. However, fewer T cells attacked tumor cells without BiTE treatment, which showed that BiTE was effective in recruiting T cells to attack tumor cells.
Characterization of the MnO2/Co-DA@BiTE/HPT nanobombs
The above results inspired us to design a strategy to combine STING activators and BiTE with immune-activating therapies. First, HA-PD-L1(HPT) was synthesized by the reaction of the carboxyl group on HA and the amino-modified PD-L1 aptamer (Supplementary Fig. 8a). To verify the successful synthesis of HPT, the tetramethylrhodamine (TAM)-labeled PD-L1 aptamer was used to react with HA, and TAM-HPT was detected by agarose electrophoresis. As shown in Supplementary Fig. 8b, compared with the PD-L1 aptamer, the position of the band of HPT and TAM-HPT moved upwards, indicating that HPT was successfully synthesized.27
MnO2 nanoparticles were prepared by the potassium permanganate (KMnO4) reduction method.28 The MnO2/Co-DA nanobombs were formed by the coordination of Co2+ and DA. Due to the Co2+ in MnO2/Co-DA, BiTE could be successfully captured on the surface of MnO2/Co-DA by combining with the His tag of BiTE.29 Additionally, previous studies have reported the ability of DA to capture antibodies.30,31 Therefore, MnO2/Co-DA@BiTE nanobombs were prepared through the interaction between Co2+/DA and BiTE. Finally, MnO2/Co-DA@BiTE/HPT nanobombs were obtained via the self-assembly of HPT. The introduction of HPT could enhance the targeting ability of the nanobombs.32 The MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT nanobombs had particle sizes of ~85.7 nm and 167.2 nm, respectively (Fig. 1e and Supplementary Fig. 9). To confirm the loading of BiTE in the MnO2/Co-DA@BiTE/HPT nanobombs, we performed circular dichroism (CD) analysis using free PD-L1/CD3 BiTE as the standard, and found that BiTE was present in the MnO2/Co-DA@BiTE/HPT nanobombs (Fig. 1f). The results of molecular docking showed that DA of Co-DA structure could form hydrophobic and hydrogen bonding with amino acids of BiTE (Fig. 1g). Additionally, Co2+ of Co-DA structure formed a coordination effect with the His tags of BiTE (Fig. 1h). These results showed that BiTE molecules could bind to the Co-DA structure of MnO2/Co-DA. Supplementary Fig. 10 shows that MnO2/Co-DA@BiTE/HPT nanobombs were unstable in the PBS buffer. And MnO2/Co-DA@BiTE/HPT nanobombs displayed stability during 36 h in water and saline. The percentage of BiTE released from the MnO2/Co-DA@BiTE/HPT nanobomb was tested in PBS with different concentrations of HAase, and a high release rate was observed with increasing hyaluronidase (HAase) concentration (Supplementary Fig. 11).
The ultraviolet-visible spectroscopy (UV‒Vis) spectrum showed that MnO2/Co-DA nanobombs had absorption peaks in the range of 600–800 nm (Supplementary Fig. 12), which should contribute to the formation of a network structure between metals and phenols, forming an absorption peak in the near infrared.33,34 In addition, the X-ray photoelectron spectroscopy (XPS) results of MnO2/Co-DA@BiTE/HPT indicated the presence of Mn and Co (Supplementary Fig. 13). Two characteristic peaks at 643 eV (Mn2p3/2) and 654.39 eV (Mn2p1/2) were attributed to MnO2 (Supplementary Fig. 14). The characteristic peaks at 782.69 eV (Co2p3/2) and 798.19 eV (Co2p1/2) were attributed to Co. Inductively coupled plasma-mass spectrometry (ICP‒MS) showed that the contents of Mn and Co were 20.83% and 14.33%, respectively. Supplementary Fig. 15 indicates that the peaks at 24°, 37°, and 67° were attributed to MnO2.35 Moreover, there was no obvious spectrum peak of MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT, indicating that the MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT nanobombs were amorphous. The MnO2/Co-DA nanobombs were irradiated by an 808 nm laser to evaluate the photothermal conversion effect. As shown in Supplementary Fig. 16, the temperature of the MnO2/Co-DA nanobombs increased gradually with increasing irradiation time. Additionally, the temperature variation of MnO2/Co-DA was positively correlated with laser power and concentration (Supplementary Fig. 17). The photothermal conversion efficiency of MnO2/Co-DA was 30.23% (Supplementary Fig. 18), and the nanobombs had great photothermal stability (Supplementary Fig. 19).
Methylene blue (MB) was used as an indicator to detect hydroxyl radical (•OH). As shown in Supplementary Fig. 20, there was no significant MB degradation in the MB and MB+H2O2 groups. In contrast, after the addition of MnO2/Co-DA, the spectrum of MB was weakened, and the intensity of the absorption spectrum became weaker with increasing incubation time (Supplementary Fig. 21). It is speculated that a Fenton-like reaction occurred between Co2+ and Mn2+. MnO2 reacted with H2O2 to form Mn2+ and O2. The bubbles are O2 (Supplementary Fig. 22a), which is produced at a faster rate as the acidity decreases. Supplementary Fig. 22b shows that the UV‒Vis spectrum intensity of MnO2 became weaker with increasing time, indicating the degradation of MnO2.
The function of BiTE in MnO2/Co-DA@BiTE/HPT in vitro
First, the expression of PD-L1 on the surface of CT26 cells was detected by immunofluorescence. As illustrated in Supplementary Fig. 23, the PD-L1 receptor was highly expressed on the surface of CT26 cells. BiTE has biological activity, which could be affected by external conditions. To evaluate the influence of BiTE binding with MnO2/Co-DA on protein biological activity, MnO2/Co-DA@BiTE/HPT nanobombs were directly treated with T/CT26 cells. When the BiTE concentration was 25 nM, the proportions of CD25+CD69+ cells in the BiTE and MnO2/Co-DA@BiTE/HPT groups were 23.54% and 21.52%, respectively (Supplementary Fig. 24a). The proportion of CD25+CD69+ cells increased with increasing concentrations of BiTE (Supplementary Fig. 24b). Furthermore, the BiTE and MnO2/Co-DA@BiTE/HPT groups exhibited increased expression of IFN-γ (Supplementary Fig. 24c). The above results indicated that the biological function of BiTE was preserved in MnO2/Co-DA@BiTE/HPT nanobombs. Additionally, the affinity of BiTE was detected by a PD-L1 ELISA kit after irradiation with an 808 nm laser. Compared with the nonlaser treatment group, ~85.09% of BiTE activity was retained after irradiation with a 0.75 W cm−2 808 nm laser (Supplementary Fig. 25), indicating that the effect of PTT on the biological activity of BiTE was negligible.
Cell cytotoxicity assay
MnO2/Co-DA@BiTE/HPT could trigger the release of damage-associated molecular patterns (DAMPs), tumor-derived dsDNA, and metal ions (Mn2+ and Co2+) with irradiation with an 808 nm laser, which could induce the maturation of DCs and inhibit tumors (Fig. 2a). Figure 2b shows that the cytotoxicity of MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT was concentration dependent. The activity of CT26 cells was further reduced by 808 nm laser irradiation. In addition, the RTCA system was applied to monitor the toxicity of different concentrations of MnO2/Co-DA@BiTE/HPT (Supplementary Fig. 26). Cell apoptosis was used to further analyze cytotoxicity (Supplementary Fig. 27). The BiTE group did not induce tumor cell apoptosis. MnO2 can be rapidly degraded to produce Mn2+ under high levels of H2O2 in tumor cells.36 Bimetallic Mn2+ and Co2+ could generate reactive oxygen species (ROS) via a Fenton-like reaction to induce tumor cell apoptosis. Thus, cell apoptosis was detected in the MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT groups. The apoptosis-inducing ability of the MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT groups was improved after laser irradiation. The cell cytotoxicity of MnO2/Co-DA@BiTE/HPT was superior to that of MnO2/Co-DA nanobombs. The reason is that the targeting of HPT promotes more MnO2/Co-DA@BiTE/HPT to bind to tumor cells, thus exerting a strong antitumour effect. To more directly observe the activity of MnO2/Co-DA@BiTE/HPT against CT26 cells, a live and dead kit was used to stain the cells. Supplementary Fig. 28 shows that the NS and BiTE groups displayed strong green fluorescence signals. In contrast, both green and red signals were present in the MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT groups. After laser irradiation, the red signal was significantly enhanced in the two groups, revealing that the combination of Fenton toxicity and hyperthermia amplified the tumor-killing power.
In vitro cytotoxicity of MnO2/Co-DA@BiTE/HPT nanobombs against CT26 cells and cellular immune response stimulation. a Schematic illustration of the maturation of DCs. b Cell viability of CT26 cells after treatment with various nanobombs. c Representative fluorescence images of CT26 cells treated with various treatments and then stained with γ-H2AX. d Representative fluorescence images of CT26 cells stained with anti-CRT and anti-HMGB1 antibodies. e Representative flow cytometric plots of mature BMDCs (CD80+CD86+ in CD11c+ cells) after incubation with various nanobobms. f The secretion of IFN-β in the supernatant of CT26 cells after different treatments. g Western blot analysis of p-TBK1, p-STING, and p-IRF3 in DC2.4 and RAW264.7 cells pretreated with different formulations. h Naïve T cells differentiating into CD8+ T and CD4+ T cells (gated on CD3+ T cells) with flow cytometry. i Percentage of CD8+ T cells in different groups. j Immune factor (IFN-γ) in the supernatant of the T-cell/BMDC/CT26 coincubation system. All data were presented as mean ± SD (n ≥ 3). I: NS, II: BiTE, III: MnO2/Co-DA, IV: MnO2/Co-DA+L, V: MnO2/Co-DA@BiTE/HPT, VI: MnO2/Co-DA@BiTE/HPT+L
ROS play an important role in tumor therapy, which can not only directly kill tumors, but also induce tumor cells to produce immunogenic cell death (ICD) in coordination with immunotherapy.37,38 The efficiency of the Fenton reaction was detected by an ROS probe in CT26 cells. As shown in Supplementary Fig. 29, Mn2+ and Co2+ could induce the production of •OH via a Fenton-like reaction. Therefore, the MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT groups emitted green fluorescence signals. The intensity of green signals was increased under laser irradiation, which contributed to the fact that PTT promoted rapid depolymerization of the nanobombs and released more metal ions, thus producing more •OH.
dsDNA generation and ICD induction
Excessive oxidative stress in cells can lead to the destruction of cell homeostasis, and the decline in mitochondrial membrane potential is a sign of early apoptosis of tumor cells.39 JC-1 is an ideal fluorescent dye for detecting changes in mitochondrial membrane potential. As illustrated in Supplementary Fig. 30, strong red fluorescence signals were observed in the control and BiTE groups, indicating that BiTE did not affect mitochondrial function. The fluorescence signals were weakened in the MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT groups. The red fluorescence signal disappeared under the synergistic action of PTT and metal ions. Mitochondrial stress, such as virus-induced mitochondrial stress, leads to leakage of mitochondrial DNA (mtDNA) into the cytoplasm, activating the STING pathway and promoting the production of cytokines.40 Cell apoptosis induces mitochondrial stress, and then leaks mtDNA, thus assisting Mn2+ in activating the STING pathway. In addition, ROS will damage DNA in mitochondria and the nucleus.41 Therefore, damaged dsDNA was detected by γ-H2Aχ immunofluorescence in CT26 cells after treatment with different formulations. γ-H2Aχ is a marker of double-stranded DNA (dsDNA) breakage and an important tool for studying DNA damage. γ-H2Aχ-positive staining was observed in the MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT groups in Fig. 2c, especially after laser treatment. These results showed that MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT could break dsDNA in CT26 cells with the aid of PTT. Previous studies have shown that PTT can improve antitumor immunity by inducing ICD in tumor cells, expressing calreticulin (CRT), and releasing high mobility group box 1 (HMGB1) and adenosine 5′-triphosphate (ATP). ICD acts as a bridge between tumor cells and the microenvironment by enhancing the immunogenicity of tumor cells. CRT can be transported to the surface of dying tumor cells to promote TAA uptake by APCs. A weak red fluorescence signal of CRT was observed, as well as a reduced HMGB1 signal in MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT groups. After laser treatment, the intensity of ICD was significantly increased (Fig. 2d).
Activation of the STING pathway
Mn2+ and Co2+ can activate the STING pathway of DCs to release IFN-β, thus inducing the maturation of DCs.25,42 Subsequently, different concentrations of MnO2/Co-DA nanobombs were introduced to investigate the maturation ability of BMDCs. As shown in Supplementary Fig. 31a, the proportion of mature BMDCs increased with increasing MnO2/Co-DA concentration. The level of IFN-β in the cell supernatant was also increased (Supplementary Fig. 31b), which further indicated that MnO2/Co-DA could induce the maturation of BMDCs.
A transwell system was used to study the immune response induced by MnO2/Co-DA@BiTE/HPT nanobombs in vitro (Supplementary Fig. 32). The results showed that the expression level of CD80+CD86+ on BMDCs was 32.76% in the MnO2/Co-DA@BiTE/HPT+L group, which was higher than that of the MnO2/Co-DA@BiTE/HPT group (22.39%) (Fig. 2e). MnO2/Co-DA@BiTE/HPT nanobombs could generate ROS to produce cytotoxicity, promote tumor cell death, and release TAAs. After laser irradiation, CT26 cells could release a large amount of TAAs (tumor cell debris, damaged dsDNA, etc.), which could significantly promote the maturation of BMDCs to secrete IFN-β (Fig. 2f). The expression of STING pathway-related proteins in DC2.4 and RAW264.7 cells after treatment with nanobombs. Figure 2g and Supplementary Fig. 33 show that the levels of p-TBK1, p-STING, and p-IRF3 were increased in the MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT groups. Especially after laser treatment, PTT promoted tumor cells to generate ICD, and high temperature caused the death of CT26 cells to release dsDNA, which promoted APCs to phagocytose dsDNA to cooperate with Mn2+ and Co2+ to enhance the levels of p-TBK1, p-STING, and p-IRF3.
Antitumour assay in the simulated immune system
DCs are professional APCs that process antigens to combine with major histocompatibility complex (MHC) molecules to form a complex and bind with T-cell receptors, thus triggering the whole process of T-cell activation.43 The costimulatory molecules CD80 and CD86 on DCs bind to CD28 on the T-cell surface, thus activating T lymphocytes, stimulating the activation and proliferation of initial T cells, and initiating the immune response. Figure 2f shows that MnO2/Co-DA@BiTE/HPT could induce the maturation of BMDCs. Therefore, we investigated whether MnO2/Co-DA@BiTE/HPT promotes T-cell activation in vitro (Supplementary Fig. 34). As shown in Fig. 2h, the percentage of initial T cells activated into CD8+ T cells by BiTE was 15.20% in the T-cell/BMDC/CT26 coculture system. BiTE designed for PD-L1 could enhance T-cell function by blocking the interaction between PD-L1/PD-1. Therefore, PD-L1/CD3 BiTE could stimulate the proliferation and activation of initial T cells into CD8+ T cells. When the initial T cells were treated with MnO2/Co-DA@BiTE/HPT, the proportion of CD8+ T cells was 19.30%, which was higher than that of the BiTE and MnO2/Co-DA groups (Fig. 2i). PTT induced the death of CT26 cells to release dsDNA, which could promote the maturation of BMDCs. Mature BMDCs process TAAs released by CT26 cells and bind to T cell receptor (TCR) to further stimulate T-cell activation and proliferation. Therefore, PTT could increase the proportion of activated CD8+ T cells. Additionally, compared with NS, IFN-γ levels after treatment were increased. The level of IFN-γ in MnO2/Co-DA@BiTE/HPT+L group was significantly higher than that in the other groups (Fig. 2j).
A T-cell/BMDC/CT26 coculture system was constructed to investigate the antitumour effect of the immune system in vitro (Supplementary Fig. 35). After treatment with MnO2/Co-DA@BiTE/HPT+L, the viability of CT26 cells was 4.39%, showing a significant antitumour effect. The results demonstrated that the combination of the STING pathway, BiTE therapy, and PTT had a synergistic effect on the killing effect of tumor cells.
Pharmacokinetics and biodistribution of MnO2/Co-DA@BiTE/HPT in vivo
To obtain the pharmacokinetics of MnO2/Co-DA@BiTE/HPT in blood, CT26 tumor-bearing mice were intravenously injected with MnO2/Co-DA@BiTE/HPT. As shown in Supplementary Fig. 36, the blood circulation half-life was detected to be 4.18 h. The distribution of MnO2/Co-DA@BiTE/HPT in CT26 tumor-bearing mice was determined after systemic administration. The infrared dye Cy5.5 was used to label the nanobombs to reduce the interference of mouse fluorescence and facilitate observation. Cy5.5/MnO2/Co-DA nanobombs could effectively aggregate in tumor tissues, and the fluorescence signal could still be detected at 96 h, meaning that the nanobombs could accumulate in tumor tissues for a long time (Supplementary Fig. 37). In addition, after the introduction of HPT, the fluorescence intensity of MnO2/Co-DA@BiTE/HPT was significantly higher than that of the MnO2/Co-DA group. The reason is that the PD-L1 aptamer could enhance the specific targeting ability of the MnO2/Co-DA@BiTE/HPT nanobombs. To further confirm that the PD-L1 aptamer can specifically enhance tumor targeting, we selected a nucleic acid molecule with a similar molecular weight to the PD-L1 aptamer but without any targeting function as a control (MnO2/Co-DA@BiTE/HR). The results showed that the enrichment level of MnO2/Co-DA@BiTE/HR was lower than that of MnO2/Co-DA@BiTE/HPT group. Additionally, the major organs and the tumor tissues were collected at 96 h for ex vivo analysis (Supplementary Fig. 38). Strong fluorescence signals were observed in tumors. The fluorescence signal of MnO2/Co-DA@BiTE/HPT was higher than that of MnO2/Co-DA and MnO2/Co-DA@BiTE/HR groups. Aptamers, also known as “chemical antibodies”, can selectively bind to specific targets. Therefore, PD-L1 aptamers could target colorectal cancer with high expression of PD-L1.
In vivo antitumour efficacy of MnO2/Co-DA@BiTE/HPT
To investigate whether MnO2/Co-DA@BiTE/HPT nanobombs have significant antitumour effects. The subcutaneous tumor model of CT26 was established (Fig. 3a). The tumor-bearing mice were divided into six groups to be treated with different formulations. The temperature of the MnO2/Co-DA group rose to 40 °C, while the tumor temperature was 52.3 °C in MnO2/Co-DA@BiTE/HPT group (Supplementary Fig. 39). As shown in Fig. 3b and Supplementary Fig. 40, CT26-bearing mice treated with BiTE and MnO2/Co-DA displayed a slight inhibition of tumor growth. However, the mice receiving MnO2/Co-DA@BiTE/HPT+L treatment presented stronger tumor growth inhibition owing to the effective activation of the adaptive and innate immune systems. On the 18th day, the tumors were collected, weighed, and photographed (Fig. 3c). A similar antitumour trend was observed after treatment with different formulations in Fig. 3d. The weight of tumor-bearing mice did not significantly change after treatment with different formulations (Fig. 3e). Subsequently, H&E, Ki67, and TUNEL staining were carried out (Fig. 3f). Mice treated with MnO2/Co-DA@BiTE/HPT+L showed the most marked tumor necrosis, proliferation inhibition, and cell apoptosis.
In vivo antitumour investigation by MnO2/Co-DA@BiTE/HPT nanobombs. a The schematic diagram illustrates tumor implantation and treatment. b Tumor growth inhibition curves upon various treatments (n = 5). c Photographs of the tumors and d tumor weight after different treatments (n = 3). e The body weight changes upon various treatments (n = 3). f H&E, TUNEL, and Ki67 staining of the tumor tissue. g Representative flow cytometry plots and quantitative analysis of T cells (gated on CD3+ T cells) in tumors after different treatments (n = 3). h Immunofluorescence images of CD4+, CD8+ T cells, and IFN-γ within the tumors after treatments. j Flow cytometry analysis of tumor-infiltrating DCs (CD80+CD86+ in CD11c+ cells) after various treatments (n = 3). Quantitative analysis of i FOXP3 (FOXP3+CD4+CD25+ in CD3+ cells), k Mature DCs (CD80+CD86+ in CD11c+ cells), and l Tem (CD62L-CD44+ in CD8+ T cells) (n = 3). m The cytokine levels of IFN-β, TNF-α, IFN-γ, and IL-6 in serum after different treatments (n = 3). All data were presented as mean ± SD. I: NS, II: BiTE, III: MnO2/Co-DA, IV: MnO2/Co-DA+L, V: MnO2/Co-DA@BiTE/HPT, VI: MnO2/Co-DA@BiTE/HPT+L
To explore the immune response after treatment with different formulations, the tumors were collected to analyze the immune cells by flow cytometry (Supplementary Fig. 41). CD8+ T cells in MnO2/Co-DA@BiTE/HPT+L tumors were threefold higher than those in NS mice (Fig. 3g). Similarly, the immunofluorescence staining images further indicated that MnO2/Co-DA@BiTE/HPT+L improved more tumor infiltration of CD4+ and CD8+ T cells compared with the other groups (Fig. 3h). Moreover, the mice treated with MnO2/Co-DA@BiTE/HPT+L exhibited enhanced expression of IFN-γ. Treg cells in the tumor microenvironment could promote the immune escape of tumor cells. Therefore, we analyzed Treg cells after treatment with different formulations. As shown in Fig. 3i and Supplementary Fig. 42, the proportion of Treg cells decreased after treatment. Compared with that in the NS group, the proportion of Treg cells decreased to 9.52% in the MnO2/Co-DA@BiTE/HPT+L group. The maturation of DCs infiltrated in tumors has important significance for the strength of the T-cell immune response and the prognosis of tumor patients. Activation of the STING pathway improves the maturation of DCs. Thus, the DCs in tumors were analyzed. MnO2/Co-DA@BiTE/HPT increased the frequency of mature DCs to 38.41%, compared with 17.17% in the NS group. The DC maturation ratio of the MnO2/Co-DA@BiTE/HPT group was markedly increased to 50.10% upon laser irradiation (Fig. 3j). Additionally, to assess the systemic immune response, we further examined the proportion of mature DCs in tumor-draining lymph nodes and Tems in the spleen. MnO2/Co-DA@BiTE/HPT+L effectively enhanced DC maturation in the tumor-draining lymph nodes of mice (Supplementary Fig. 43 and Fig. 3k). The proportion of Tem increased from 10.11% to 33.51% (Supplementary Fig. 44 and Fig. 3l). Moreover, the mice treated with MnO2/Co-DA@BiTE/HPT+L showed improved levels of the cytokines IFN-β, TNF-α, IL-6, and IFN-γ (Fig. 3m). The results indicated that the MnO2/Co-DA@BiTE/HPT nanobombs could effectively stimulate the systemic immune response for immunotherapy.
Subsequently, we explored the biological mechanisms of MnO2/Co-DA@BiTE/HPT+L on tumors by RNA sequencing. The Venn diagram suggested that there were significant discrepancies among primary transcripts between the NS and MnO2/Co-DA@BiTE/HPT+L groups (Fig. 4a). Compared with the NS group, 866 upregulated genes and 525 downregulated genes were observed in the tumors treated with MnO2/Co-DA@BiTE/HPT+L (Fig. 4b). To further understand the potential targeting pathway of MnO2/Co-DA@BiTE/HPT+L, KEGG analysis showed that some cGAS-STING related pathways were significantly upregulated compared with those in NS mice, including chemokine signaling, the IL-17 signaling pathway, cytokine and cytokine receptor interaction, TNF signaling, and the cytoplasmic DNA sensing pathway, which could induce a systemic immune response (Fig. 4c). Additionally, Fig. 4d shows that most pathways in tumors were upregulated after MnO2/Co-DA@BiTE/HPT+L treatment because the number of upregulated enriched genes in each pathway was higher than that of downregulated genes. Studies have shown that Mn2+ can enhance IFN-I, proinflammatory cytokines, and chemokines by activating the cGAS-STING pathway. Co2+ and dsDNA could synergistically amplify the activation of the STING pathway. Subsequently, gene set enrichment analysis (GSEA) was applied to determine the impact of MnO2/Co-DA@BiTE/HPT+L on the corresponding signaling pathways at immunotherapy (Fig. 4e). The results showed positive enrichment of inflammatory, TNFA, and IFN-γ in MnO2/Co-DA@BiTE/HPT+L-treated tumors (Fig. 4f–h).
Evaluation of the MnO2/Co-DA@BiTE/HPT-mediated antitumour immunotherapy mechanism. a Venn diagram of CT26 tumors treated with NS and MnO2/Co-DA@BiTE/HPT+L. b Volcano plot showing the upregulated, not significantly changed, or downregulated genes when comparing MnO2/Co-DA@BiTE/HPT+L-treated mice with the NS-treated group. c KEGG analysis of differentially expressed genes between NS- and MnO2/Co-DA@BiTE/HPT+L-treated tumors. d Circular graph enrichment analysis of differentially expressed genes between NS and MnO2/Co-DA@BiTE/HPT+L treated tumors. e Subnetworks of the notable enrichment maps via GSEA. f–h Strong enrichment in inflammatory, TNF, and IFN-γ pathways in MnO2/Co-DA@BiTE/HPT+L-treated tumors via gene set enrichment analysis. i The expression of STING pathway-related genes in tumors after different drug treatments via qPCR. j Western blot assays of p-IRF3 and p-STING in tumors after different treatments. All data were presented as mean ± SD. I: NS, II: BiTE, III: MnO2/Co-DA, IV: MnO2/Co-DA+L, V: MnO2/Co-DA@BiTE/HPT, VI: MnO2/Co-DA@BiTE/HPT+L
Additionally, to elucidate the antitumour mechanism of MnO2/Co-DA@BiTE/HPT+L, we first studied the RNA and protein levels of the STING pathway in tumor tissues. The expression levels of IFNa4, IFIt1, IFNb, Isg15, and IFN-β were significantly increased (Fig. 4i). Moreover, WB analysis revealed that the protein levels of p-IRF3 and p-STING were robustly upregulated in MnO2/Co-DA@BiTE/HPT+L mice (Fig. 4j and Supplementary Fig. 45).
MnO2/Co-DA@BiTE/HPT boosted antitumour immunotherapy
A CT26 bilateral tumor model was used to evaluate the antitumour effect of MnO2/Co-DA@BiTE/HPT (Fig. 5a). As shown in Fig. 5b, MnO2/Co-DA@BiTE/HPT, synergizing with PTT, displayed an obvious inhibitory effect on distal tumors. On the 12th day, the tumors were collected, weighed, and photographed (Fig. 5c). As shown in Fig. 5d, tumor volumes and weights were reduced after treatment with different formulations, especially in the MnO2/Co-DA@BiTE/HPT+L group. Moreover, the MnO2/Co-DA@BiTE/HPT+L group inhibited tumor proliferation and induced more tumor necrosis and cell apoptosis (Supplementary Fig. 46). And the body weight of the mice during the treatment process showed no obvious change (Fig. 5e). Next, cytotoxic T lymphocytes from distant tumors were analyzed (Fig. 5f). The highest frequency of CD8+ T cells was observed in the MnO2/Co-DA@BiTE/HPT+L group (33.99% in distant tumors). The immunofluorescence staining of CD4+ and CD8+ T cells in tumors displayed the same trend (Fig. 5g). Similarly, a significant increase (39.31% in distant tumors) in tumor-infiltrating mature DCs (CD80+CD86+) was detected in the MnO2/Co-DA@BiTE/HPT+L group relative to that in the NS group (Fig. 5h and Supplementary Fig. 47). Additionally, after treatment with MnO2/Co-DA@BiTE/HPT+L, the lowest frequency of Treg cells was observed in distant tumors (Fig. 5i and Supplementary Fig. 48). Next, the spleen and lymph nodes were collected to detect the maturation of DCs (Fig. 5j). Compared with the NS group, the MnO2/Co-DA@BiTE/HPT+L group exhibited higher maturation of DCs. The spleens were collected to investigate the induction of Tem cells (Fig. 5k). Indeed, the number of Tems gated on CD3+CD8+ T cells only increased slightly after treatment with BiTE and MnO2/Co-DA. Compared with the BiTE and MnO2/Co-DA groups, the MnO2/Co-DA@BiTE/HPT group displayed a much higher level of Tem, confirming that the combination of BiTE and MnO2/Co-DA could induce immunological memory. Moreover, high secretion levels of proinflammatory cytokines in serum supported that MnO2/Co-DA@BiTE/HPT+L induced a robust systemic immune response (Supplementary Fig. 49).
Antitumour effect of MnO2/Co-DA@BiTE/HPT nanobombs on mice with a CT26 bilateral tumor model. a Diagram illustrating the bilateral tumor implantation and treatment schedule. b Distal tumor growth curves of CT26 tumor-bearing mice after various treatments (n = 5). c Representative photos of the sacrificed distal tumor. d The sacrificed primary tumor weights (n = 5). e The body weight of the mice during the treatment process (n = 5). f Flow cytometry plots and quantification of CD3+CD8+ and CD3+CD4+ T cells in tumor tissues (n = 3). g Representative immunofluorescence images of CD4+ and CD8+ infiltration in tumor tissues after treatment. Quantitative analysis of FOXP3 (h) and mature DCs (i) in tumor tissues (n = 3). j Flow cytometry plots and quantification of mature DCs in the spleen and lymph nodes (n = 3). k Flow cytometry plots and quantification of Tem in the spleen (n = 3). All data were presented as mean ± SD. I: NS, II: BiTE, III: MnO2/Co-DA, IV: MnO2/Co-DA+L, V: MnO2/Co-DA@BiTE/HPT, VI: MnO2/Co-DA@BiTE/HPT+L
Antitumour efficacy in rechallenged and metastatic tumours
Inspired by the significant tumor therapy and immunostimulation efficacy of the synergistic treatment, the immune memory effect induced by MnO2/Co-DA@BiTE/HPT was next investigated. We rechallenged the secondary CT26 tumors 11 days after resection of the primary CT26 tumors (Fig. 6a). The NS, BiTE, and MnO2/Co-DA groups failed to avoid tumor recurrence due to weak immune memory effects. The progression of the secondary tumors was obviously suppressed in the MnO2/Co-DA@BiTE/HPT+L group (Fig. 6b, c). The spleens and lymph nodes were collected to analyze Tem (Fig. 6d). After treatment with MnO2/Co-DA@BiTE/HPT+L, the proportion of Tem cells in the spleen and lymph nodes was significantly increased, indicating the activation of the systemic immune response. In conclusion, the systemic antitumour immunity mediated by MnO2/Co-DA@BiTE/HP+L could not only inhibit the growth of primary tumors, but also prevent tumor recurrence after surgery, which had significant therapeutic and preventive effects.
MnO2/Co-DA@BiTE/HPT nanobombs transformed cold tumors into hot tumors and achieved long-term immune memory. a Schematic diagram illustrating the primary and re-challenged tumor implantation and treatment process. b The average and c individual growth curves of tumors in rechallenge tumor models (n = 5). d Flow cytometry plots and quantification of Tem in the spleen and lymph nodes (n = 3). e Diagram illustrating the lung metastasis model implantation and treatment schedule. f Average tumor growth curves of CT26 lung metastasis models after treatments (n = 5). g Average number of lung metastatic foci of CT26 tumors (n = 3). h Photos and i representative H&E staining of lung tissues after treatment with various nanobombs. All data were presented as mean ± SD. I: NS, II: BiTE, III: MnO2/Co-DA, IV: MnO2/Co-DA + L, V: MnO2/Co-DA@BiTE/HPT, VI: MnO2/Co-DA@BiTE/HPT + L
Finally, given the high immune memory of MnO2/Co-DA@BiTE/HPT nanobombs, as demonstrated in the rechallenged model, we further evaluated the antimetastatic effect of MnO2/Co-DA@BiTE/HPT in the lungs (Fig. 6e). Consistent with previous results of tumor volume, MnO2/Co-DA@BiTE/HPT synergizing with PTT exerted a much greater antimetastatic effect (Fig. 6f). As shown in Fig. 6g, h, widespread metastatic nodules could be observed in the lung in the NS group, and the mice treated with BiTE and MnO2/Co-DA exhibited lung metastatic nodules to some extent. Conversely, treatment with MnO2/Co-DA@BiTE/HPT and MnO2/Co-DA@BiTE/HPT+L efficiently inhibited the development of metastatic nodules in lung tissues. Moreover, H&E staining of lung sections further confirmed the antimetastatic effect of MnO2/Co-DA@BiTE/HPT+L (Fig. 6i). MnO2/Co-DA@BiTE/HPT+L not only increased the number of mature DCs in spleens and lymph nodes, but also significantly increased the amount of Tem. Such outstanding therapeutic benefits were likely attributed to a remarkable systemic immune response by the STING pathway, BiTE, and PTT therapy to prevent tumor metastasis.
Antitumor effect of MnO2/Co-DA@BiTE/HPT nanobobms on mice with B16-F10 tumor model. a Tumor volume curves of B16-F10 tumor-bearing mice after various treatments (n = 5). b Representative photos of the scarified tumors and c tumor weight after various treatments (n = 5). d H&E, TUNEL, and Ki67 staining of the tumor tissue. e Representative flow cytometry plots and quantitative analysis of T cells (gated on CD3+ T cells) in tumors after various treatments (n = 3). f Representative flow cytometry plots and quantitative analysis of tumor-infiltrating DCs (CD80+CD86+ in CD11c+ cells) after various treatments (n = 3). All data were presented as mean ± SD. I: NS, II: BiTE, III: MnO2/Co-DA, IV: MnO2/Co-DA+L, V: MnO2/Co-DA@BiTE/HPT, VI: MnO2/Co-DA@BiTE/HPT+L
Antitumor efficacy in the melanoma model
The therapeutic effects of MnO2/Co-DA@BiTE/HPT were further evaluated in a melanoma model. Similarly, after treatment with MnO2/Co-DA@BiTE/HPT+L, the mice displayed significant tumor growth inhibition (Fig. 7a–c). As shown in Fig. 7d, the mice treated with MnO2/Co-DA@BiTE/HPT+L had the most marked tumor necrosis, cell apoptosis, and proliferation inhibition compared to the other groups. Subsequently, the immune cells (T cells and DCs) in tumor tissues were analyzed using flow cytometry. The percentages of both CD8+ T cells (Fig. 7e) and DCs maturation (Fig. 7f) were markedly greater in MnO2/Co-DA@BiTE/HPT+L group than in the other treatment groups, suggesting that MnO2/Co-DA@BiTE/HPT+L effectively activated the immune response, resulting in enhanced antitumor activity.
Biosafety evaluation
The biosafety of nanobombs is crucial in clinical applications. Thus, the body weight of the mice was monitored. As shown in Fig. 3e, the weight of tumor-bearing mice did not significantly change after treatment with different formulations. In addition, H&E staining was performed on the major organs (Supplementary Fig. 50). Compared with the NS group, no pathological changes were observed in the organs after treatment. The results showed that the nanobombs have great biological safety. The blood biochemical index is an important index to judge whether the body is healthy (Supplementary Fig. 51). The indices of liver and kidney function of tumor-bearing mice after administration were investigated. After treatment, there was no obvious difference in several indices compared with the NS group, indicating that the nanobombs would not destroy liver and kidney function at the experimental dose.
Hemolysis assay was used to evaluate the blood compatibility of MnO2/Co-DA@BiTE/HPT nanobomb (Supplementary Fig. 52). The concentrations of MnO2/Co-DA in MnO2/Co-DA@BiTE/HPT nanobomb ranged from 25 to 200 μg/mL, while the hemolysis rates were below the safety standard of 5%, suggesting that MnO2/Co-DA@BiTE/HPT exhibited excellent hemocompatibility.
To evaluate long-term safety, the mice were intravenously injected with normal saline and MnO2/Co-DA@BiTE/HPT for 2 months (Supplementary Fig. 53a). The blood, kidneys, livers, lungs, hearts, and spleens of the mice were collected for assessment. Supplementary Fig. 53b shows the body weight drop for the treated mice in the early days after injection of MnO2/Co-DA@BiTE/HPT, and the mice regained their body weights later. And the hematological tests and serum biochemical assays did not show toxicity of MnO2/Co-DA@BiTE/HPT on blood cells and the function of the kidney, liver, and heart (Supplementary Fig. 53c–e). The HE-staining showed that MnO2/Co-DA@BiTE/HPT did not harm the histological structure of the main organs (Supplementary Fig. 53f). Additionally, no significant change of cytokine levels, including IFN-γ, IL-6, IL-2, IL-10, and TNF-α, was observed (Supplementary Fig. 54). These results showed the long-term safety of MnO2/Co-DA@BiTE/HPT.
Discussion
CRC is the third most common cancer after lung cancer and the second most deadly.44 With the continuous progress of medical treatment, the methods for patients with CRC are more diverse. In addition to traditional radiotherapy and chemotherapy, targeted therapy and immunotherapy have ushered in increasingly better treatment options for CRC patients.45 As an important part of immunotherapy, bispecific antibodies are only four types on the global market, and no bispecific antibodies against CRC have been approved. BiTE enhances the cytotoxicity of T cells by targeting CD3 and tumor-specific antigens.46 However, the number of T cells in the TME is limited, and tumor cells can activate a variety of mechanisms to escape T-cell killing. The expression of some TAAs is universal, which may result in the “on-target off-tumor” effect of BiTE in practical applications and produce toxic reactions such as cytokine storms and tissue damage.10 Additionally, the immunosuppressive TME and the loss of target antigens may cause tumor immune tolerance to BiTE.8 Combination therapy has been extensively studied to reverse the microenvironment, break immune tolerance, and improve the efficacy of BiTE immunotherapy.8,12
The cGAS-STING pathway can sense not only exogenous danger signals from viruses and bacteria, but also endogenous signals from damaged mitochondria and endocytosis fragments of dead cells.14,16 Activation of the STING pathway in APCs may produce IFN-I to recruit and cross-activate effector T cells, thereby overcoming the “cold” tumor barrier.19,20 To date, most of the Mn-based nanoparticles, such as MnO2, MnSe2, Mn3O4, Mn-MOF, and Mn-phenolic, have been reported and applied in STING-related immunotherapy.47,48,49,50 However, the immunotherapy that relies on the activation of the STING pathway by Mn2+ cannot effectively inhibit tumor growth. In our study, the biometallic nanobombs were synthesized based on MnO2 and metal-phenolic (Co-DA), which could activate the STING pathway by Mn2+/Co2+ and the damaged dsDNA of PTT. Aptamers, known as chemical antibodies, are structured oligonucleotide sequences that can mimic antibodies by folding into unique 3D structures to selectively bind to targets. To enhance the active targeting of STING agonist and BiTE, a PD-L1 aptamer was introduced in our work.
Herein, we prepared biometallic nanobombs (MnO2/Co-DA@BiTE/HPT), which were based on the rational combination of STING activator, BiTE therapy, and PTT to significantly augment antitumour immunotherapy. The MnO2/Co-DA nanobombs rapidly depolymerized under acidic conditions, releasing Co2+ and Mn2+. In addition to activating the STING pathway, MnO2/Co-DA nanobombs had PTT functions under 808 nm laser irradiation. The triple-killing of MnO2/Co-DA@BiTE/HPT nanobombs induced CT26 cell death to release damaged dsDNA, which could cooperate with bimetallic ions (Mn2+ and Co2+) to amplify the signals of the STING pathway, induce the maturation of BMDCs, and release IFN-β. Additionally, MnO2/Co-DA@BiTE/HPT could induce initial T-cell proliferation and activation to enhance the antitumour effect. STING activator and BiTE were synchronously and accurately delivered to the tumor tissues with the targeting of HPT. There are limitations to our study. One of the major translational barriers is the scalability and reproducibility of our nanobombs. The current preparation process of MnO2/Co-DA@BiTE/HPT is complex and time-consuming. Achieving consistent quality and yield on a large scale is a significant challenge. Variations in reaction conditions, such as temperature, pH, and reagent concentrations, can lead to differences in the properties of the final product, affecting its efficacy and safety. Another critical issue is the safety profile of our nanobombs in clinical applications. Although our preclinical studies have shown no obvious signs of severe toxicity, the long-term effects and potential side effects in humans are still unknown. The Mn2+/Co2+ and BiTE may trigger unexpected immune responses or interact with other drugs or medical conditions in patients. Extensive clinical trials and long-term follow-up studies are required to fully assess the safety and tolerability of our approach. Furthermore, the animal models in our study did not fully recapitulate the genetic, immunological, and microenvironmental heterogeneity observed in human colorectal malignancies. This limitation inherently restricts the generalizability of the efficacy data and might result in an overestimation of clinical translatability.
Bimetallic ions (Mn2+ and Co2+) activate the STING pathway with the assistance of PTT, transforming “cold” tumors into “hot” tumors, thereby overcoming the resistance of “cold” tumors to BiTE. Specifically, the activation of DCs induced by Mn2+/Co2+ and released dsDNA produced type I interferons and pro-inflammatory cytokines, which assessed and promoted T-cell proliferation, differentiation, and activation.25 Activated DCs upregulated the expression of co-stimulatory molecules (such as CD80 and CD86), providing a second signal for T cell activation, thereby enhancing the cytotoxicity of BiTE-mediated T cells.51,52 Furthermore, BiTE-mediated cytotoxicity of T cells led to the lysis and death of target cells, thereby releasing more tumor antigens that can be taken up and processed by DCs, further activating the STING signaling pathway, generating more type I interferons and pro-inflammatory cytokines, forming a positive feedback loop, and enhancing the anti-tumor immune response.
This study combined the triple-kill pathways of the STING pathway, BiTE therapy, and PTT for the first time in colorectal cancer immunotherapy, initiating both natural immunity and adaptive immunity, improving the immune microenvironment, producing long-term immune memory, inhibiting tumor growth, and preventing tumor recurrence and metastasis. This study is expected to provide a new idea for the treatment of colorectal cancer.
Materials and methods
Materials
Hyaluronic acid (HA, Mw~10 kDa) was obtained from Bloomage Freda Biopharm, Co. Ltd. The PD-L1 aptamer was obtained from Tsingke Biotechnology. KMnO4, CoCl2•6H2O, NaCl, CaCl2•2H2O, MnCl2•2H2O, and CeCl3•7H2O were purchased from Aladdin. The calcein-AM/PI kit, JC-1 kit, DAPI, RIPA lysis buffer, and BCA kit were purchased from Beyotime Biotechnology. The γ-H2AX antibody was purchased from Abcam. HMGB1, CRT, and p-IRF3 antibodies were obtained from Huabio. p-TBK1 and p-STING antibodies obtained from CST. Picogreen dsDNA quantitation reagent and goldband 3-color regular range protein marker (10–180 kDa) were purchased from Yeasen. IL2, IL15, GM-CSF, IL4, CD3/CD28, and flow antibodies purchased from Biolegend (Table S1). Endo-free Plasmid Mini Kit was obtained from Omega. The IFN-β and IFN-γ ELISA kit was obtained from RuixinBio (Quanzhou, China). PD-L1/CD3 BiTE was obtained from Aiping Tong group. Serum was purchased from NEWZERUM (FBS-UP500). RPMI 1640 (L210KJ) and penicillin-streptomycin combination (S110JV) were obtained from BasalMedia.
Preparation and characterization of MnO2/Co-DA@BiTE/HPT nanobombs
Then, 2 mL KMnO4 (3.2 mg/mL) was added to a silene bottle to stir for 15 min. Then, 200 μL polyacrylamide hydrochloride (PAH) (37.4 mg/mL) was added and stirred at room temperature for 2 h to obtain MnO2 nanoparticles.
The MnO2 nanoparticles obtained above were added to the silene bottle after suspension, and 100 μL CeCl3•6H2O, CaCl2•2H2O, NaCl, and CoCl2•6H2O (20 mM) were added to the stirring for 15 min. Then, 20 μL DA (2 mg/mL) was added to the above solutions with stirring for 30 min to obtain MnO2/Na-DA, MnO2/Ca-DA, MnO2/Ce-DA, and MnO2/Co-DA.
MnO2/Co-DA nanoparticles were suspended in saline, and the BiTE antibody was added and incubated at 4 °C for 24 h. Next, the material HPT was added to stir for 2 h in an ice bath. Finally, MnO2/Co-DA@BiTE/HPT nanobombs were obtained by centrifugation.
In vitro release behavior of BiTE
To detect the drug loading of BiTE in MnO2/Co-DA@BiTE/HPT nanobombs, an ultrafiltration tube (300 kDa) was used to remove the unloaded BiTE. Hyaluronidase (HAase) (500 μ/mL) was coincubated with MnO2/Co-DA@BiTE/HPT to release the BiTE antibody. A PD-L1 ELISA kit was applied to detect the content of loaded BiTE.
MnO2/Co-DA@BiTE/HPT nanobombs were transferred into a dialysis bag (MWCO: 300 kDa), which was immersed in PBS media containing 0 μ/mL, 200 μ/mL, and 500 μ/mL HAse. The released media were removed at different time points, and the same volume of fresh buffer was added. The cumulative release of BiTE was detected by a PD-L1 ELISA kit.
The function of the BiTE assay
T-cell/CT26 cells (4:1) were seeded in a 24-well plate overnight and cultured with IgG, BiTE, and MnO2/Co-DA@BiTE/HPT (after culture with hyaluronidase) for 24 h. Next, the cells were blocked with 2% BSA buffer for 15 min and stained with anti-CD3, anti-CD8, anti-CD25, and anti-CD69 antibodies for 30 min for flow cytometry analysis (ACEA, Novocyte). The cell supernatant was analyzed with an IFN-γ ELISA kit.
Additionally, to investigate the effect of the 808 nm laser on BiTE biological activity, after laser irradiation, the binding affinity of PD-L1 in MnO2/Co-DA@BiTE/HPT nanobombs was examined. First, the MnO2/Co-DA@BiTE/HPT nanobombs were treated with 0.75 W cm−2 and 1.5 W cm−2 808 nm lasers for 5 min. Next, the MnO2/Co-DA@BiTE/HPT nanobombs were treated with hyaluronidase to release BiTE. Finally, the binding affinity of BiTE was evaluated via a PD-L1 ELISA kit.
In vitro ICD induction
CT26 cells were seeded in a 24-well plate coated with a cover glass and cultured overnight. The cells were incubated with PBS, BiTE, MnO2/Co-DA, MnO2/Co-DA+L, MnO2/Co-DA@BiTE/HPT, and MnO2/Co-DA@BiTE/HPT+L for 4 h and then irradiated with 808 nm laser (0.75 W cm−2, 5 min). After culturing for another 8 h, CRT exposure and HMGB1 release were analyzed through immunofluorescence staining. The cells were fixed with 4% PFA for 15 min and blocked with 2% BSA for 1.5 h. Next, the cells were incubated with anti-CRT and anti-HMGB1 (1:200, Huabio) overnight. Finally, the cells were stained with Alexa Fluor 594-labelled goat-anti-mouse antibody (1:200, Huabio) for 2 h and DAPI for 5 min for observation with CLSM (Zeiss, LSM880).
Analysis of BMDC-stimulated maturation
CT26 cells were seeded in 24-well plates for 24 h and incubated with PBS, BiTE, MnO2/Co-DA, MnO2/Co-DA+L, MnO2/Co-DA@BiTE/HPT, and MnO2/Co-DA@BiTE/HPT+L. The cells were incubated with MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT nanobombs for 4 h under an 808 nm laser at 0.75 W cm−2 for 5 min. Next, the cells were cultured for 24 h and stained with anti-CD11c, anti-CD80, and anti-CD86 antibodies for flow cytometry analysis. The cell supernatant was collected for the IFN-β assay. For the transwell experiment, CT26 cells were seeded on the transwell upper chamber for 24 h. The cells were incubated with PBS, BiTE, MnO2/Co-DA, MnO2/Co-DA+L, MnO2/Co-DA@BiTE/HPT, and MnO2/Co-DA@BiTE/HPT+L. The cells were incubated with MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT nanobombs for 4 h, under 808 nm laser at 0.75 W cm−2 for 5 min. Then, BMDC cells were inoculated in the lower chamber for 24 h. Finally, the BMDCs were stained with anti-CD11c, anti-CD80, and anti-CD86 antibodies for flow cytometry analysis. The cell supernatant was collected for the IFN-β assay.
Stimulation of the STING pathway assay
CT26 cells were planted in culture overnight and treated with PBS, BiTE, MnO2/Co-DA, MnO2/Co-DA+L, MnO2/Co-DA@BiTE/HPT, and MnO2/Co-DA@BiTE/HPT+L. The cells were incubated with MnO2/Co-DA and MnO2/Co-DA@BiTE/HPT nanobombs for 4 h under an 808 nm laser at 0.75 W cm−2 for 5 min. After that, the cell supernatant was collected for the following experiment. Next, DC2.4 and RAW264.7 cells were plated in culture dishes overnight. After adding the collected supernatant, the DC2.4 and RAW264.7 cells were cultured for 24 h, and the cells were collected for western blot assays.
In vitro antitumour immune system assay
T cells/BMDCs/CT26 (20:10:1) cells were seeded in 12-well plates overnight. And CT26 cells were labelled with CFSE. The supernatant of CT26 cells treated with different formulations was added to the coculture system for 24 h. Finally, the cells were collected for the CFSE+CT26 assay by flow cytometry.
In vivo antitumour effect assay
To investigate the in vivo antitumour effect of MnO2/Co-DA@BiTE/HPT nanobombs, subcutaneous CT26 tumor-bearing BALB/c mice were established. When the tumor volume reached 200 mm3, the mice were randomly assigned to six groups and received different treatments on days 1 and 3, including Control (NS), BiTE (0.5 mg/kg), MnO2/Co-DA (2 mg/kg), MnO2/Co-DA+L, MnO2/Co-DA@BiTE/HPT (MnO2/Co-DA: 2 mg/kg, BiTE: 0.5 mg/kg), and MnO2/Co-DA@BiTE/HPT+L. Two groups received 808 nm laser irradiation (0.75 W cm−2, 5 min) at 12 h postinjection. The tumor volume and body weights were monitored every 2 days. On day 18, the mice were sacrificed. The tumors and the major organs were collected for H&E and immunofluorescence staining.
A CT26 bilateral-tumor model was established by inoculating 1 × 106 and 5 × 105 cells into the right and left flanks, respectively. When the tumor volume reached 200 mm3, the mice were treated as described above. The tumor volume was monitored.
To evaluate the effectiveness of MnO2/Co-DA@BiTE/HPT nanobombs against lung metastasis, CT26 cells (1 × 105) were intravenously injected after establishing primary tumors on day 7, and the treatments were performed according to the same method described above. When the mice died in the NS group, all mice were sacrificed, and the lungs were collected, and the number of nodules was recorded. In addition, H&E staining was performed.
To verify the prevention of postoperative recurrence, a CT26 tumor-bearing mouse model was first established. When the tumor volume reached 100 mm3, the mice were randomly divided into six groups and treated with different formulations. On day 10, the tumor was surgically removed. On day 21, CT26 cells (1 × 106) were inoculated in the left flank. The tumor volume of the mice was recorded.
Evaluation of antitumour immune response
To analyze T-cell infiltration, CT26 tumor tissues were collected and then digested with collagenase (1 mg/mL)/hyaluronidase (100 μg/mL)/DNAse I (100 μg/mL) to obtain single-cell suspensions. The single-cell suspensions were blocked with 2% BSA and stained with Zombie Red™ Fixable Viability Kit, anti-CD45, anti-CD3, anti-CD4, and anti-CD8 antibodies for 30 min. Next, the cells were fixed with 4% PFA for 15 min to be analyzed with flow cytometry. To analyze the Treg cells, after blocking, the single-cell suspensions were stained with the Zombie Red™ Fixable Viability Kit, anti-CD45, anti-CD3, anti-CD4, and anti-CD25 antibodies for 30 min. Next, the cells were immobilized and permeated. Finally, the cells were stained with anti-FOXP3 antibodies for 30 min for analysis by flow cytometry. Additionally, the single-cell suspensions were stained with Zombie Red™ Fixable Viability Kit, anti-CD45, anti-CD11c, anti-CD80, and anti-CD86 antibodies for 30 min. Finally, the cells were fixed with 4% PFA to analyze the mature DCs by flow cytometry.
To analyze effector T cells (Tem) in the spleen, spleen and lymph node single-cell suspensions were obtained and stained with anti-CD3, anti-CD8, anti-CD44, and anti-CD62L antibodies for flow cytometry assays (CD3+CD8+CD44+CD62L−).
To analyze mature DCs in lymph nodes, the lymph nodes were collected to obtain single-cell suspensions. Then, the single-cell suspensions were stained with anti-CD11c, anti-CD80, and anti-CD86 antibodies for flow cytometry assays (CD11c+CD80+CD86+).
The antitumor efficacy in melanoma model
The therapeutic effects of MnO2/Co-DA@BiTE/HPT were further evaluated by a subcutaneous B16-F10 (5 × 105 cells) tumor-bearing model. When the tumor volume reached 100 mm3, the mice were randomly assigned to six groups and received different treatments on days 1 and 3, including Control (NS), BiTE (0.5 mg/kg), MnO2/Co-DA (2 mg/kg), MnO2/Co-DA+L, MnO2/Co-DA@BiTE/HPT (MnO2/Co-DA: 2 mg/kg, BiTE: 0.5 mg/kg), and MnO2/Co-DA@BiTE/HPT+L. Two groups received 808 nm laser irradiation (0.75 W cm−2, 5 min) at 12 h postinjection. The tumor volume and body weights were monitored every 2 days. On day 8, the mice were sacrificed. The tumors were collected for H&E, TUNEL, and Ki67 staining. Additionally, a portion of the tumors was used for flow cytometry analysis.
Statistical analysis
The experimental data are shown as the mean ± standard deviation (SD). The differences between multiple groups were performed using one-way analysis of variance (ANOVA) with Tukey’s test. The student’s test was used to analyze the significant differences between the two groups. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001.
Data availability
All data generated or analyzed during this study have been included either in this article or in the supplementary information files. The data reported in this paper have been deposited in the OMlX, China National Center for Bioinformation/Belling instituteof Genomics, Chinese Academy of Sciences (https:/ingdc.cncb.ac.cn/omix: accession no. OMIX013900).
References
Kruse, B. et al. CD4+ T cell-induced inflammatory cell death controls immune-evasive tumours. Nature 618, 1033–1040 (2023).
Chu, Y. et al. Pan-cancer T cell atlas links a cellular stress response state to immunotherapy resistance. Nat. Med. 29, 1550–1562 (2023).
Humby, F., Kirkham, B. & Taams, L. BiTE therapy for rheumatoid arthritis. Nat. Med. 30, 1533–1534 (2024).
Seckinger, A. et al. Target expression, generation, preclinical activity, and pharmacokinetics of the BCMA-T cell bispecific antibody EM801 for multiple myeloma treatment. Cancer Cell 31, 396–410 (2017).
Klein, C., Brinkmann, U., Reichert, J. M. & Kontermann, R. E. The present and future of bispecific antibodies for cancer therapy. Nat. Rev. Drug Discov. 23, 301–319 (2024).
Goebeler, M. E. et al. Bispecific T-cell engager (BiTE) antibody construct blinatumomab for the treatment of patients with relapsed/refractory non-Hodgkin lymphoma: final results from a phase I study. J. Clin. Oncol. 34, 1104–1111 (2016).
Ishiguro, T. et al. An anti–glypican 3/CD3 bispecific T cell–redirecting antibody for treatment of solid tumors. Sci. Transl. Med. 9, eaal4291 (2017).
Belmontes, B. et al. Immunotherapy combinations overcome resistance to bispecific T cell engager treatment in T cell-cold solid tumors. Sci. Transl. Med. 13, eabd1524 (2021).
Goebeler, M. E. & Bargou, R. C. T cell-engaging therapies - BiTEs and beyond. Nat. Rev. Clin. Oncol. 17, 418–434 (2020).
Gong, N. et al. Small-molecule-mediated control of the anti-tumour activity and off-tumour toxicity of a supramolecular bispecific T cell engager. Nat. Biomed. Eng. 8, 513–528 (2024).
Liu, D. et al. Microenvironment-responsive anti-PD-L1 x CD3 bispecific T-cell engager for solid tumor immunotherapy. J. Control. Release 354, 606–614 (2023).
Fan, R. et al. Engineering MMP-2 activated nanoparticles carrying B7-H3 bispecific antibodies for ferroptosis-enhanced glioblastoma immunotherapy. ACS Nano 17, 9126–9139 (2023).
Cheng, W. J. et al. Bispecific T-cell engagers non-covalently decorated drug-loaded PEGylated nanocarriers for cancer immunochemotherapy. J. Control. Release 344, 235–248 (2022).
Maxwell, M. B. et al. ARID1A suppresses R-loop-mediated STING-type I interferon pathway activation of anti-tumor immunity. Cell 187, 3390–3408.e19 (2024).
Wu, J. X. et al. Cyclic GMP-AMP is an endogenous second messenger in innate immune signaling by cytosolic DNA. Science 339, 826–830 (2013).
Ding, B. et al. A novel platinum(IV) prodrug, gramine-Pt(IV) enhances chemoimmunotherapy by activating cGAS-STING and modulating TGF-β-MHC-I axis. Drug Resist. Update 81, 101252 (2025).
Lanng, K. R. B., Lauridsen, E. L. & Jakobsen, M. R. The balance of STING signaling orchestrates immunity in cancer. Nat. Immun. 25, 1144–1157 (2024).
Yang, H., Yang, S., Guo, Q., Sheng, J. & Mao, Z. ATP-responsive manganese-based bacterial materials synergistically activate the cGAS-STING pathway for tumor immunotherapy. Adv. Mater. 36, e2310189 (2024).
Chen, B. et al. Boosting peroxidase-mimetic activity of FeMn-NCeDual-atom radiosensitizing nanozymes for augmented radiodynamic immunotherapy. ACS Nano 19, 10147–10161 (2025).
Wang, Y. et al. Universal STING mimic boosts antitumour immunity via preferential activation of tumour control signalling pathways. Nat. Nanotechnol. 19, 1235 (2024).
Tang, Y. et al. Condensate nanovaccine adjuvants augment CD8+ T-Cell-dependent antitumor immunity through mtDNA leakage-triggered cGAS-STING axis activation. Signal Transduct. Target. Ther. 10, 149 (2025).
Wang, C. et al. Manganese increases the sensitivity of the cGAS-STING pathway for double-stranded DNA and is required for the host defense against DNA viruses. Immunity 48, 675–687.e7 (2018).
Du, M. & Chen, Z. J. DNA-induced liquid phase condensation of cGAS activates innate immune signaling. Science 361, 704–709 (2018).
Wang, C. et al. Maintaining manganese in tumor to activate cGAS-STING pathway evokes a robust abscopal anti-tumor effect. J. Control. Release 331, 480–490 (2021).
Sun, X. et al. Amplifying STING activation by cyclic dinucleotide-manganese particles for local and systemic cancer metalloimmunotherapy. Nat. Nanotechnol. 21, 1260–1270 (2021).
Li, K. et al. Overcome the challenge for intratumoral injection of STING agonist for pancreatic cancer by systemic administration. J. Hematol. Oncol. 17, 62 (2024).
Yang, L. et al. Self-assembled aptamer-grafted hyperbranched polymer nanocarrier for targeted and photoresponsive drug delivery. Angew. Chem. Int. Ed. 57, 17048–17052 (2018).
Zhu, W. et al. Modulation of hypoxia in solid tumor microenvironment with MnO2nanoparticles to enhance photodynamic therapy. Adv. Funct. Mater 26, 5490–5498 (2016).
Zhang, W. et al. Cobalt-directed assembly of antibodies onto metal-phenolic networks for enhanced particle targeting. Nano Lett. 20, 2660–2666 (2020).
Sun, Q. et al. Phototherapy and anti-GITR antibody-based therapy synergistically reinvigorate immunogenic cell death and reject established cancers. Biomaterials 269, 120648 (2021).
Zhao, S. et al. Immunochromatographic assay based on polydopamine-decorated iridium oxide nanoparticles for the rapid detection of salbutamol in food samples. ACS Appl. Mater. Inter. 13, 28899–28907 (2021).
Zhang, J. et al. PD-L1 aptamer-functionalized metal-organic framework nanoparticles for robust photo-immunotherapy against cancer with enhanced safety. Angew. Chem. Int. Ed. 62, e202214750 (2023).
Mu, M. et al. Augmented the sensitivity of photothermal-ferroptosis therapy in triple-negative breast cancer through mitochondria-targeted nanoreactor. J. Control. Release 375, 733–744 (2024).
Sang, W. et al. A triple-kill strategy for tumor eradication reinforced by metal-phenolic network nanopumps. Adv. Funct. Mater. 21, 2113168 (2022).
Zhang, M. et al. MnO2-based nanoplatform serves as drug vehicle and MRI contrast agent for cancer theranostics. ACS Appl. Mater. Inter. 9, 11337–11344 (2017).
Zhu, Y. et al. Oxygen self-supply engineering-ferritin for the relief of hypoxia in tumors and the enhancement of photodynamic therapy efficacy. Small 18, e2200116 (2022).
Wang, Y. et al. Oxygen-deficient molybdenum oxide nanosensitizers for ultrasound-enhanced cancer metalloimmunotherapy. Angew. Chem. Int. Ed. 9, e202215467 (2023).
Prasad, R. et al. A biodegradable fluorescent nanohybrid for photo-driven tumor diagnosis and tumor growth inhibition. Nanoscale 10, 19082–19091 (2018).
Zhao, Z. et al. Reactive oxygen species–activatable liposomes regulating hypoxic tumor microenvironment for synergistic photo/chemodynamic therapies. Adv. Funct. Mater. 29, 1905013 (2019).
Tian, H. et al. Metal-phenolic nanomaterial with organelle-level precision primes antitumor immunity via mtDNA-dependent cGAS-STING activation. Angew. Chem. Int. Ed. 63, e202411498 (2024).
Prasad, R. et al. Liposomal nanotheranostics for multimode targeted in vivo bioimaging and near-infrared light mediated cancer therapy. Commun. Biol. 3, 284 (2020).
Yan, J. et al. Engineering radiosensitizer-based metal-phenolic networks potentiate STING pathway activation for advanced radiotherapy. Adv. Mater. 34, e2105783 (2021).
Worbs, T., Hammerschmidt, S. I. & Forster, R. Dendritic cell migration in health and disease. Nat. Rev. Immunol. 17, 30–48 (2017).
Bando, H., Ohtsu, A. & Yoshino, T. Therapeutic landscape and future direction of metastatic colorectal cancer. Nat. Rev. Gastroenterol. Hepatol. 20, 306–322 (2023).
Riley, R. S., June, C. H., Langer, R. & Mitchell, M. J. Delivery technologies for cancer immunotherapy. Nat. Rev. Drug. Discov. 18, 175–196 (2019).
Ye, Q.-N. et al. Orchestrating NK and T cells via tri-specific nano-antibodies for synergistic antitumor immunity. Nat. Commun. 15, 6211 (2024).
Yi, L. et al. A hybrid nanoadjuvant simultaneously depresses PD-L1/TGF-β1 and activates cGAS-STING pathway to overcome radio-immunotherapy resistance. Adv. Mater. 36, e2304328 (2024).
Sun, W. et al. Metal-phenolic vehicles potentiate cycle-cascade activation of pyroptosis and cGAS-STING pathway for tumor immunotherapy. ACS Nano 18, 23727–23740 (2024).
Li, X. et al. Octadecyl gallate and lipid-modified MnSe2 nanoparticles enhance radiosensitivity in esophageal squamous cell carcinoma and promote radioprotection in normal tissues. Adv. Mater. 36, e2311291 (2024).
Qiao, W. et al. A single-atom manganese nanozyme Mn-N/C promotes anti-tumor immune response via eliciting type I interferon signaling. Adv. Sci 211, e2305979 (2024).
Li, W. et al. cGAS-STING–mediated DNA sensing maintains CD8+ T cell stemness and promotes antitumor T cell therapy. Sci. Transl. Med. 12, eaay9013 (2020).
Shae, D. et al. Endosomolytic polymersomes increase the activity of cyclic dinucleotide STING agonists to enhance cancer immunotherapy. Nat. Nanotechnol. 14, 269–278 (2019).
Acknowledgements
This work was financially supported by the National Natural Sciences Foundation of China (31971308, 81960769, and U1903211), National S&T Major Project (2019ZX09301-147), Noncommunicable Chronic Diseases-National Science and Technology Major Project (2023ZD050610X/2023ZD0506100), China Postdoctoral Science Foundation (2024M762225), and Sichuan Science and Technology Program (2022YFS0007 & 22GJHZ0015).
Author information
Authors and Affiliations
Contributions
M.M. designed and performed the experiments, analyzed the data, and prepared the manuscript. H.L. collected the data. B.C. performed characterization of the nanobombs. R.F. and G.W. provided suggestions and technical support. K.Z. provided the plasmid. H.L., B.C., and C.F. assisted in the in vivo experiments. G.G. conceptualized, supervised, and supported the whole project. A.T. edited manuscript and supervised the study. N.C. supervised and supported the study. B.Z. conceptualized, supervised, and supported the whole project. All the authors have read and approved the article.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Mu, M., Li, H., Chen, B. et al. Unleashing the potential of bimetallic nanobomb-mediated STING pathway to enhance bispecific T-cell engager against colorectal cancer photo-immunotherapy. Sig Transduct Target Ther 11, 80 (2026). https://doi.org/10.1038/s41392-026-02596-6
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41392-026-02596-6