Abstract
Background
Pancreatic ductal adenocarcinoma (PDAC) presents an urgent challenge that necessitates improved early risk identification. We investigated the association between predictors of PDAC present at least two years before diagnosis and PDAC occurence.
Methods
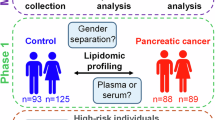
This case-control study used electronic health records from The Health Improvement Network Database (UK). Cases (10,575) were matched with controls (105,750) in a 1:10 ratio by gender, age, follow-up duration, and year of inclusion in the database. Variables included clinical features, comorbidities and blood result abnormalities, reported at least 2 years before PDAC diagnosis or equivalent timeframe for controls. Conditional logistic regression model with backward estimated odds ratios (OR) and 95% confidence interval (CI).
Results
Electronic health records of cases reported higher prevalence of alcohol intake, cigarette smoking, dyslipidemia, increased blood pressure, and diabetes of more than four years’ duration. Independent risk factors included pancreatic cysts (OR = 4.39), pancreatitis (OR = 2.16), dyslipidemia (OR = 1.50), smoking (OR = 1.09), and alcohol intake (OR = 1.09). Laboratory markers associated with higher risk included elevated alkaline phosphatase (OR = 3.21), bilirubin (OR = 2.48), alanine aminotransferase (OR = 1.76), erythrocyte sedimentation rate (OR = 1.27), and decreased albumin (OR = 1.54).
Conclusions
Primary care electronic records can identify individuals at medium-term increased risk of PDAC, thus raises the opportunity to develop early detection models and address modifiable factors.
Similar content being viewed by others
Introduction
Pancreatic ductal adenocarcinoma (PDAC) ranks among the deadliest cancers mainly due to its late diagnosis and chemoresistance [1]. In 2022, PDAC accounted for 510,566 new cases and 467,005 cancer-related deaths worldwide [2]. The burden of PDAC has increased considerably over the past decades mainly because of the aging structure of the population together with the increased prevalence of established risk factors [3, 4]. Around 80% of patients with PDAC are diagnosed with locally advanced or metastatic stages that are not amenable to curative surgery [5]. The remaining 20% present with surgically resectable disease that may be cured by combining surgery and chemotherapy [6,7,8,9]. Nevertheless and despite extended survivals with multimodal regimens, 50–75% of these patients will relapse within 2 years and ultimately die of their disease [6,7,8, 10, 11]. Thus, a better understanding of its risk factors and the identification of patients at increased risk of PDAC have become a pressing clinical need [12].
Epidemiological studies on risk prediction models of PDAC have mainly focused on specific high-risk individuals and well established risk factors for PDAC [13,14,15,16,17,18,19,20]. So far, the efforts toward screening for PDAC in the general population were disappointing and did not improve survival outcomes [21]. Subsequently, the latest guidelines restricted screening of PDAC to individuals at high risk of PDAC due to family history or rare inherited pathogenic variants or cystic lesions and did not recommend it in the asymptomatic general population [21,22,23,24]. Electronic health records (EHRs) present an interesting analytic opportunity to study risk factors that may be overlooked in traditional studies and to follow the trajectories of these risk factors over many year [25, 26]. To address the challenge of identifying individuals at increased risk of PDAC in the medium term in the general population, we sought to evaluate the comorbidities, clinical data and blood test results before PDAC diagnosis of patients consulting in primary care setting. For this purpose, we analysed a large nested case-control studies drawn from The Health Improvement Network database in the United Kingdom (THIN® UK) to describe the risk factors associated with an increased risk of PDAC at least two years before the PDAC diagnosis.
Materials and methods
Data source
The study used data extracted from THIN® Database (A Cegedim Proprietary Database) in UK, which includes various information covering basic demographic characteristics, medical history, medical diagnoses coded according to the International Classification of Disease, 10th Revision (ICD-10), laboratory values, and medication prescriptions (including date, dosage, and duration). THIN® UK was created in 1994 and covers 19 million patients in 2023. Several epidemiologic studies have explored this database to examine patterns of prescription and medical diagnosis [27,28,29,30,31,32,33,34,35].
THIN® EHR extracts are transmitted by a network of voluntary physicians in compliance with current regulations, including European general data protection regulations. THIN® UK database was granted ethical approval by the NHS South-East Multicentre Research Ethics Committee in 2003 (reference 03/01/073) and was further updated in 2020 by the NHS South Central, Oxford C Research Ethics Committee (reference 20/SC/0011). This retrospective study used secondary deidentified data extract only without mentioning of personal information and as such the legislation did not require additional ethical approval, thus the requirement for obtaining informed consent was waived. This study was examined and approved by THIN® Scientific Review Committee (protocol number 20 002 R1).
Patient selection and study design
The target population enclosed all patients aged 18 years or older who were enroled in the THIN® UK database between 1994 and 2021. EHRs were eligible for inclusion if the corresponding patient had been enroled in the database for at least one year and had continuous follow-up with the same General Practitioner (GP) for at least one year. This criterion helped ensure consistency in medical records and minimise the risk of missing relevant health information. Importantly, the patients included in this analysis were unlikely to have had an unreported PDAC, as their regular consultations with the same GP allowed for continuous monitoring of their health status. We excluded patient records with inconsistent dates of birth or death, PDAC diagnosis before their inclusion in the database and those with non-adenocarcinoma pancreatic tumours.
Cases were identified from EHRs with a reported diagnosis of PDAC at any point during follow-up. To identify patient records with PDAC, we used the following THIN® UK specific codes instead of the ICD10 codes because they were more granular and specific regarding the pathology of the pancreatic tumour, as reported by the GP (Supplementary Table).
To create a control group, we randomly selected EHRs from the THIN® UK database without a reported cancer diagnosis at their last follow-up. Controls had to have at least one year of follow-up in the THIN® UK; this ensured that they consulted the same GP regularly, reducing the likelihood of having an unreported PDAC case among the control group. To ensure comparability between cases and controls and minimise potential confounding factors, we matched each case to 10 controls based on gender, age, follow-up duration, and year of inclusion, with the choice of 10 controls per case accounting for the prevalence of PDAC and in accordance with previous studies (Supplementary Fig.) [36, 37]. The follow-up period was defined as the time from inclusion in THIN® UK to either pancreatic cancer diagnosis (for cases) or the last follow-up visit (for controls).
Candidate risk factors
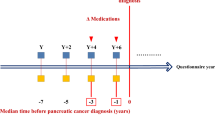
For each patient consultation, the medical history, diagnosis for each visit, clinical data, blood test results, and prescriptions made by the primary care physicians were available. Based on a literature review and clinical relevance, we defined a comprehensive list of PDAC risk factors, including age, cigarette smoking, alcohol intake, medical comorbidities, clinical data, and laboratory test results [4, 19, 38, 39]. Relevant information was collected from the most recent medical record at least two years before the PDAC diagnosis for the cases, and at the last consultation for the controls (Supplementary Fig.). In the THIN® UK database, family history of PDAC was not systematically reported and was therefore excluded from our analysis.
Comorbidities
The personal history of lung, head and neck, bladder cancers, melanoma as well as pancreatic diseases (including intraductal papillary mucinous neoplasm, acute and chronic pancreatitis, and pancreatic cysts), dyslipidemia, increased blood pressure, diabetes mellitus, cholecystitis, and Helicobacter pylori infection were collected from the EHRs. Missing variables were imputed as negative based on the assumption that patients who had consulted the same GP for more than one year were unlikely to present outdated records. Information on diabetes mellitus, changes of antidiabetic medication, dyslipidemia and increase blood pressure was verified through medical reimbursement records.
Information regarding alcohol intake and cigarette smoking were also obtained. Alcohol intake was either reported directly by the primary care physicians or imputed in patients with alcohol-related complications such as alcohol-induced cirrhosis. Given that the estimation of alcohol intake was not possible, it was defined as any alcohol use and alcohol use disorder including those with alcohol-related complications. Similarly, cigarette smoking was either mentioned in the medical record or assumed from the prescription of nicotine substitutes; it was classified as never or ever smoking.
Clinical data
The anthropometric measures were collected directly from the EHRs at the last consultation with available corresponding data. Weight loss was defined as a decrease of 5% or more in body weight. Data on fatigue and abdominal pain were obtained whenever reported by the primary care physicians. These variables were collected from the most recent available time point at least two years before diagnosis among patient records with PDAC.
Laboratory test results
Laboratory test results performed at least two years before the diagnosis PDAC for cases and censoring for controls were retrieved and considered as normal, abnormal (elevated or decreased) or missing. Only biologically plausible laboratory test results were included, specifically those related to liver function (alanine aminotransferase, aspartate aminotransferase, alkaline phosphatase, gamma-glutamyl transferase, bilirubin), pancreatic function (lipase, amylase), inflammatory state (complete blood count, erythrocyte sedimentation rate, C-reactive protein, lactate dehydrogenase), and cachexia (albumin, total cholesterol, glycated haemoglobin A1c).
Statistical analysis
Patient characteristics, comorbidities and blood results were described using frequencies and proportions for categorical variables. We evaluated the association of various health conditions and test results with PDAC using conditional logistic regression. For the multivariable analysis, we employed backward selection with a significance threshold of p < 0.05 to identify the most relevant variables, computing odds ratios (OR) and their corresponding 95% confidence intervals (95% CI). All statistical analyses were performed using R 4.3.1 with the 'survival' package.
Results
Our eligible matched cohort included 10,575 EHRs with PDAC and 105,750 controls (Fig. 1). The patient characteristics and comorbidities of cases and their matched controls are presented in Table 1. Males comprised 51.5% of the cohort and age over 70 years represented 52.2% of eligible EHR. Alcohol intake was more prevalent among cases (64.9%) compared to controls (62.1%). Additionally, a higher percentage of cases had an alcohol use disorder (5.6%) relative to controls (4.5%). Cigarette smoking was also more common in cases, with 56.6% having a history of smoking compared to 50.0% in controls.
PDAC: pancreatic ductal adenocarcinoma.
Regarding comorbidities, dyslipidemia (48.3 vs. 39.8%) and increased blood pressure (41.1 vs. 37.6%) were more frequent in cases than in controls. Cases also had a slightly higher incidence of other conditions like pancreatitis (1.6 vs. 0.6%) and cholecystitis (1.5 vs. 1.1%). A notable difference was observed in the prevalence of diabetes; diabetes diagnosed for more than 4 years was recorded in 10.9% of cases versus 9.2% of controls, while diabetes diagnosed within 4 years was also more frequent among cases (5.6 vs. 4.9%).
We evaluated the association between the collected candidate risk factors and the occurrence of PDAC (Table 2). Univariable analyses suggested that pancreatic cysts (OR = 6.34, 95% CI 3.45–11.64), pancreatitis (OR = 2.58, 95% CI 2.18–3.05), dyslipidemia (OR = 1.53, 95% CI 1.46–1.60), cholecystitis (OR = 1.39, 95% CI 1.17–1.64), and increased blood pressure (OR = 1.18, 95% CI 1.13–1.23) were the clinical variables associated with an increased risk of PDAC. Elevated levels of total bilirubin (OR = 2.91, 95% CI 2.70–3.14), alanine aminotransferase (OR = 2.07, 95% CI 1.95–2.19), C-reactive protein (OR = 2.00, 95% CI 1.82–2.18), glycated haemoglobin A1c (OR = 1.57, 95% CI 1.43–1.72) and decreased levels of albumin (OR = 1.72, 95% CI 1.64–1.82) compared to normal values were the blood test abnormalities with the higher association with PDAC. Conversely, some markers and conditions with missing values were associated with lower odds of PDAC diagnosis.
Multivariable analysis showed that pancreatic cysts (OR = 4.39, 95% CI 2.28–8.45) and elevated alkaline phosphatase (OR = 3.21, 95% CI 3.03–3.39) were the strongest independent variables associated with PDAC. Clinical risk factors independently associated with an increased risk of PDAC included pancreatitis (OR = 2.16, 95% CI 1.81–2.58), dyslipidemia (OR = 1.50, 95% CI 1.43–1.57), cigarette smoking (OR = 1.19, 95% CI 1.13–1.24), alcohol intake (OR = 1.09, 95% CI 1.02–1.17), and introduction or changes of antidiabetic medication over the last four years (OR = 1.19, 95% CI 1.11–1.28). Laboratory markers linked to higher PDAC risk included elevated alanine aminotransferase (OR = 1.76, 95% CI 1.66–1.87), total bilirubin (OR = 2.48, 95% CI 2.29–2.68), and erythrocyte sedimentation rate (OR = 1.27, 95% CI 1.18–1.37), as well as decreased albumin (OR = 1.54, 95% CI 1.46–1.62).
Discussion
This large comprehensive nested case-control study provides insights into the risk factors associated with PDAC in the general population of UK as reported in the THIN® UK database. It stands out from many previous investigations by addressing the potential risk factors present at least two years before PDAC diagnosis as it highlights a potential window of opportunity for early intervention before the disease becomes clinically apparent. This study provides evidence that a more comprehensive and multifactorial approach to risk assessment may outperform traditional high-risk screening criteria, which primarily emphasise family history or genetic predisposition. By analysing comorbidities, clinical data, and blood test results at least two years before PDAC diagnosis, this study offers an interesting perspective of clinical significance with the early identification of individuals at increased risk of PDAC [4, 40].
This study showed a strong association between alcohol intake and increased PDAC risk, especially in cases involving alcohol use disorder. The higher prevalence of alcohol use and alcohol use disorders among cases aligns with prior research demonstrating a dose-dependent relationship between alcohol consumption and PDAC risk [41]. Cigarette smoking and alcohol intake are well-established risk factors for PDAC, the relatively modest association observed in this study suggests that other risk factors may play a more significant role in certain populations [42, 43]. However, reducing smoking and alcohol consumption remains a relevant preventive strategy due to their modifiable nature. The independent association between dyslipidemia and PDAC adds to the growing body of literature linking metabolic disorders and PDAC [19]. The underlying mechanisms may involve chronic inflammation, insulin resistance, and alterations in the tumour microenvironment [44, 45].
Another finding of this study is the strong association between liver function abnormalities and PDAC risk, even two years before diagnosis. Elevated alkaline phosphatase and bilirubin levels emerged as the strongest independent risk factors of PDAC in the multivariable analysis. This aligns with recent research suggesting that subtle changes in liver function may precede clinically apparent PDAC by several years [46, 47]. On the other hand, missing bilirubin data was associated with lower odds of PDAC, reflecting the potential for diagnostic gaps in patients without available blood test results. The study also observed a significant relationship between elevated erythrocyte sedimentation rate and PDAC risk. Although erythrocyte sedimentation rate is a non-specific marker of inflammation, its elevation may reflect underlying chronic inflammatory states that promote pancreatic carcinogenesis [45]. This finding suggests that integrating inflammatory markers into risk prediction models for PDAC could enhance early detection.
The study’s results regarding diabetes mellitus favour the bidirectional relationship between diabetes and PDAC, which was substantiated by the higher prevalence of long-standing and recent-onset diabetes among records of cases [48]. While long-standing diabetes is a known risk factor for PDAC, recent-onset diabetes may, in some cases, be an early manifestation of the disease itself [49]. This highlights the importance of careful monitoring of new-onset diabetes in older adults, particularly when accompanied by other risk factors identified in this study. Last, the observed associations between PDAC and other pancreatic comorbidities, such as pancreatic cysts and pancreatitis are consistent with previous research [50, 51]. These conditions may create a pro-inflammatory environment in the pancreas that promotes carcinogenesis. However, the relatively low prevalence of these conditions in the study population suggests that they may have limited utility as standalone risk factors for population-wide screening. Interestingly, obesity was not associated with an increased risk in the medium term although it has long been described as a major risk factor for pancreatic cancer. This could be due to a lack of medium term effect, or to the effect of certain drugs these patients may receive, including GLP1 inhibitors [52, 53].
The main strength of this study is its use of EHR with a long longitudinal follow-up to capture a wide range of potential risk factors, including laboratory parameters that may not be routinely included in traditional epidemiological studies [54]. It provides valuable insights but several limitations should be acknowledged. First, the retrospective nature of the analysis and reliance on EHR may introduce bias due to incomplete or inconsistent data recording. It also highlights the challenges of missing data in real-world clinical settings, as evidenced by the association between missing laboratory results and PDAC risk. Second, the study’s focus on a UK population may limit generalisability to other populations with different genetic backgrounds, lifestyle factors or healthcare systems. Third, while the study identifies several potentially modifiable risk factors, such as alcohol intake and dyslipidemia, the impact of interventions targeting these factors on PDAC risk reduction remains to be determined.
Conclusion
This comprehensive analysis of risk factors for PDAC in the general population showed that primary care EHR can identify individuals at medium-term increased risk of PDAC using widely accessible data in daily practice, which is particularly important for clinical translation. The identified risk factors can eventually provide practical guidance to increase the vigilance of physicians in patients where multiple risk indicators converge. They can be insightful for developing PDAC screening and early detection strategies, mainly in regards to the identification of subtle changes in biomarkers that may precede clinical diagnosis of PDAC by several years. Current guidelines, which restrict screening to high-risk individuals based on family history and rare genetic variants, may be missing opportunities for early detection in the general population [23]. The constellation of risk factors identified in this study suggests that a more nuanced approach to risk stratification could improve the yield of screening efforts and lays the groundwork for developing prediction models. However, translating these findings into clinical practice will require careful consideration. The relatively low incidence of PDAC in the general population means that even with improved risk prediction models, the positive predictive value of any screening approach is likely to be limited. This underscores the need for specific screening modalities to minimise false positives and increase the prediction accuracy.
Data availability
THIN® Database (A Cegedim Proprietary Database) analysed for this paper is the private property of CEGEDIM. Access to the data can be granted upon reasonable written request and approval by the THIN® Scientific Review Committee.
References
Kleeff J, Korc M, Apte M, La Vecchia C, Johnson CD, Biankin AV, et al. Pancreatic cancer. Nat Rev Dis Prim. 2016;2:1–22.
Bray F, Laversanne M, Sung H, Ferlay J, Siegel RL, Soerjomataram I, et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2024;74:229–63.
Pourshams A, Sepanlou SG, Ikuta KS, Bisignano C, Safiri S, Roshandel G, et al. The global, regional, and national burden of pancreatic cancer and its attributable risk factors in 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet Gastroenterol Hepatol. 2019;4:934–47.
Klein AP. Pancreatic cancer epidemiology: understanding the role of lifestyle and inherited risk factors. Nat Rev Gastroenterol Hepatol. 2021;18:493–502.
Ducreux M, Cuhna ASA, Caramella C, Hollebecque A, Burtin P, Goéré D, et al. Cancer of the pancreas: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up†. Ann Oncol. 2015;26:v56–68.
Neoptolemos JP, Stocken DD, Friess H, Bassi C, Dunn JA, Hickey H, et al. A randomized trial of chemoradiotherapy and chemotherapy after resection of pancreatic cancer. N Engl J Med. 2004;350:1200–10.
Oettle H, Neuhaus P, Hochhaus A, Hartmann JT, Gellert K, Ridwelski K, et al. Adjuvant chemotherapy with gemcitabine and long-term outcomes among patients with resected pancreatic cancer: the CONKO-001 randomized trial. JAMA. 2013;310:1473–81.
Conroy T, Hammel P, Hebbar M, Ben Abdelghani M, Wei AC, Raoul JL, et al. FOLFIRINOX or gemcitabine as adjuvant therapy for pancreatic cancer. N Engl J Med. 2018;379:2395–406.
Conroy T, Castan F, Lopez A, Turpin A, Ben Abdelghani M, Wei AC, et al. Five-year outcomes of FOLFIRINOX vs gemcitabine as adjuvant therapy for pancreatic cancer: a randomized clinical trial. JAMA Oncol [Internet]. 2022 [cited 16 Nov 2022] https://doi.org/10.1001/jamaoncol.2022.3829
Oettle H, Post S, Neuhaus P, Gellert K, Langrehr J, Ridwelski K, et al. Adjuvant chemotherapy with gemcitabine vs observation in patients undergoing curative-intent resection of pancreatic cancera randomized controlled trial. JAMA 2007;297:267–77.
Neoptolemos JP, Stocken DD, Bassi C, Ghaneh P, Cunningham D, Goldstein D, et al. Adjuvant chemotherapy with fluorouracil plus folinic acid vs gemcitabine following pancreatic cancer resection: a randomized controlled trial. JAMA. 2010;304:1073–81.
Rahib L, Smith BD, Aizenberg R, Rosenzweig AB, Fleshman JM, Matrisian LM. Projecting cancer incidence and deaths to 2030: the unexpected burden of thyroid, liver, and pancreas cancers in the United States. Cancer Res. 2014;74:2913–21.
Klein AP, Lindström S, Mendelsohn JB, Steplowski E, Arslan AA, Bueno-de-Mesquita HB, et al. An absolute risk model to identify individuals at elevated risk for pancreatic cancer in the general population. PLOS ONE. 2013;8:e72311.
Boursi B, Finkelman B, Giantonio BJ, Haynes K, Rustgi AK, Rhim AD, et al. A clinical prediction model to assess risk for pancreatic cancer among patients with new-onset diabetes. Gastroenterology. 2017;152:840–50.e3.
Hsieh MH, Sun LM, Lin CL, Hsieh MJ, Hsu CY, Kao CH. Development of a prediction model for pancreatic cancer in patients with type 2 diabetes using logistic regression and artificial neural network models. Cancer Manag Res 2018;10:6317–24.
Sharma A, Kandlakunta H, Nagpal SJS, Feng Z, Hoos W, Petersen GM, et al. Model to determine risk of pancreatic cancer in patients with new-onset diabetes. Gastroenterology. 2018;155:730–9.e3.
Muhammad W, Hart GR, Nartowt B, Farrell JJ, Johung K, Liang Y, et al. Pancreatic cancer prediction through an artificial neural network. Front Artif Intell. 2019;2.
Baecker A, Kim S, Risch HA, Nuckols TK, Wu BU, Hendifar AE, et al. Do changes in health reveal the possibility of undiagnosed pancreatic cancer? Development of a risk-prediction model based on healthcare claims data. PLOS ONE. 2019;14:e0218580.
Yuan C, Babic A, Khalaf N, Nowak JA, Brais LK, Rubinson DA, et al. Diabetes, weight change, and pancreatic cancer risk. JAMA Oncol. 2020;6:e202948.
Appelbaum L, Cambronero JP, Stevens JP, Horng S, Pollick K, Silva G, et al. Development and validation of a pancreatic cancer risk model for the general population using electronic health records: an observational study. Eur J Cancer Oxf Engl 1990. 2021;143:19–30.
US Preventive Services Task Force, Owens DK, Davidson KW, Krist AH, Barry MJ, Cabana M, et al. Screening for pancreatic cancer: US Preventive Services Task Force Reaffirmation Recommendation Statement. JAMA 2019;322:438–44.
Yang J, Xu R, Wang C, Qiu J, Ren B, You L. Early screening and diagnosis strategies of pancreatic cancer: a comprehensive review. Cancer Commun. 2021;41:1257–74.
Henrikson NB, Aiello Bowles EJ, Blasi PR, Morrison CC, Nguyen M, Pillarisetty VG, et al. Screening for pancreatic cancer: updated evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2019;322:445–54.
Goggins M, Overbeek KA, Brand R, Syngal S, Del Chiaro M, Bartsch DK, et al. Management of patients with increased risk for familial pancreatic cancer: updated recommendations from the International Cancer of the Pancreas Screening (CAPS) Consortium. Gut. 2020;69:7–17.
Goldstein BA, Navar AM, Pencina MJ, Ioannidis JPA. Opportunities and challenges in developing risk prediction models with electronic health records data: a systematic review. J Am Med Inf Assoc. 2017;24:198–208.
Gianfrancesco MA, Goldstein ND. A narrative review on the validity of electronic health record-based research in epidemiology. BMC Med Res Methodol. 2021;21:234.
Nedelec T, Couvy-Duchesne B, Monnet F, Daly T, Ansart M, Gantzer L, et al. Identifying health conditions associated with Alzheimer’s disease up to 15 years before diagnosis: an agnostic study of French and British health records. Lancet Digit Health. 2022;4:e169–78.
Rassy E, Bardet A, Bougacha O, Gantzer L, Lekens B, Delaloge S, et al. Association of adherence to endocrine therapy among patients with breast cancer and potential drug-drug interactions. JAMA Netw Open. 2022;5:e2244849.
Hurst JR, Dilleen M, Morris K, Hills S, Emir B, Jones R. Factors influencing treatment escalation from long-acting muscarinic antagonist monotherapy to triple therapy in patients with COPD: a retrospective THIN-database analysis. Int J Chron Obstruct Pulmon Dis. 2018;13:781–92.
Deslee G, Fabry-Vendrand C, Poccardi N, Thabut G, Eteve Pitsaer C, Coriat A, et al. Use and persistence of single and multiple inhaler triple therapy prescribed for patients with COPD in France: a retrospective study on THIN database (OPTI study). BMJ Open Respir Res. 2023;10:e001585.
Lewis JD, Schinnar R, Bilker WB, Wang X, Strom BL. Validation studies of the health improvement network (THIN) database for pharmacoepidemiology research. Pharmacoepidemiol Drug Saf. 2007;16:393–401.
Cooper C, Steinbuch M, Stevenson R, Miday R, Watts NB. The epidemiology of osteonecrosis: findings from the GPRD and THIN databases in the UK. Osteoporos Int. 2010;21:569–77.
Finnikin S, Ryan R, Marshall T. Statin initiations and QRISK2 scoring in UK general practice: a THIN database study. Br J Gen Pract. 2017;67:e881–7.
Osborn DP, Petersen I, Beckley N, Walters K, Nazareth I, Hayes J. Weight change over two years in people prescribed olanzapine, quetiapine and risperidone in UK primary care: Cohort study in THIN, a UK primary care database. J Psychopharmacol. 2018;32:1098–103.
Zhou X, Murugesan S, Bhullar H, Liu Q, Cai B, Wentworth C, et al. An evaluation of the THIN database in the OMOP common data model for active drug safety surveillance. Drug Saf. 2013;36:119–34.
Fritsche LG, Patil S, Beesley LJ, VandeHaar P, Salvatore M, Ma Y, et al. Cancer PRSweb: an online repository with polygenic risk scores for major cancer traits and their evaluation in two independent biobanks. Am J Hum Genet. 2020;107:815–36.
Sharma S, Tapper WJ, Collins A, Hamady ZZR. Predicting pancreatic cancer in the UK biobank cohort using polygenic risk scores and diabetes mellitus. Gastroenterology. 2022;162:1665–74.e2.
Boursi B, Finkelman B, Giantonio BJ, Haynes K, Rustgi AK, Rhim AD, et al. A clinical prediction model to assess risk for pancreatic cancer among patients with prediabetes. Eur J Gastroenterol Hepatol. 2022;34:33–8.
Santos R, Coleman HG, Cairnduff V, Kunzmann AT. Clinical prediction models for pancreatic cancer in general and at-risk populations: a systematic review. Am J Gastroenterol. 2022;118, 26–40.
Maisonneuve P, Lowenfels AB. Risk factors for pancreatic cancer: a summary review of meta-analytical studies. Int J Epidemiol. 2015;44:186–98.
Wang YT, Gou YW, Jin WW, Xiao M, Fang HY. Association between alcohol intake and the risk of pancreatic cancer: a dose-response meta-analysis of cohort studies. BMC Cancer. 2016;16:212.
Maisonneuve P, Lowenfels AB. Variation of the age at onset of pancreatic cancer according to tobacco smoking and family history. Int J Epidemiol. 2018;47:1357.
Lugo A, Peveri G, Bosetti C, Bagnardi V, Crippa A, Orsini N, et al. Strong excess risk of pancreatic cancer for low frequency and duration of cigarette smoking: a comprehensive review and meta-analysis. Eur J Cancer Oxf Engl 1990. 2018;104:117–26.
Incio J, Liu H, Suboj P, Chin SM, Chen IX, Pinter M, et al. Obesity-induced inflammation and desmoplasia promote pancreatic cancer progression and resistance to chemotherapy. Cancer Discov. 2016;6:852–69.
Greer JB, Whitcomb DC. Inflammation and pancreatic cancer: an evidence-based review. Curr Opin Pharm. 2009;9:411–8.
Berrington de Gonzalez A, Yun JE, Lee SY, Klein AP, Jee SH. Pancreatic cancer and factors associated with the insulin resistance syndrome in the Korean cancer prevention study. Cancer Epidemiol Biomark Prev. 2008;17:359–64.
Park JH, Hong JY, Han K, Kang W, Park JK. Increased risk of pancreatic cancer in individuals with non-alcoholic fatty liver disease. Sci Rep. 2022;12:10681.
Andersen DK, Korc M, Petersen GM, Eibl G, Li D, Rickels MR, et al. Diabetes, pancreatogenic diabetes, and pancreatic cancer. Diabetes. 2017;66:1103–10.
Sharma A, Chari ST. Pancreatic cancer and diabetes mellitus. Curr Treat Options Gastroenterol. 2018;16:466–78.
Kirkegård J, Mortensen FV, Cronin-Fenton D. Chronic pancreatitis and pancreatic cancer risk: a systematic review and meta-analysis. Am J Gastroenterol. 2017;112:1366–72.
Kirkegård J, Gaber C, Lund JL, Hinton SP, Ladekarl M, Heide-Jørgensen U, et al. Acute pancreatitis as an early marker of pancreatic cancer and cancer stage, treatment, and prognosis. Cancer Epidemiol. 2020;64:101647.
Wang L, Wang W, Kaelber DC, Xu R, Berger NA. GLP-1 receptor agonists and colorectal cancer risk in drug-naive patients with type 2 diabetes, with and without overweight/obesity. JAMA Oncol. 2024;10:256–8.
Moll H, Frey E, Gerber P, Geidl B, Kaufmann M, Braun J, et al. GLP-1 receptor agonists for weight reduction in people living with obesity but without diabetes: a living benefit–harm modelling study. EClinicalMedicine. 2024;1:73.
Mishra AK, Chong B, Arunachalam SP, Oberg AL, Majumder S. Machine learning models for pancreatic cancer risk prediction using electronic health record data—a systematic review and assessment. J Am Coll Gastroenterol ACG. 2024;119:1466.
Acknowledgements
This work uses data provided by patients and collected by the NHS as part of their care and support. YS and BL from CEGEDIM R&D Paris, coauthors of this manuscript, had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Funding
Open access funding provided by Université Paris-Saclay.
Author information
Authors and Affiliations
Contributions
ER: concept of the study and review of the literature, statistical analysis, writing of the initial draft. SD: concept of the study and review of the literature, critical revision of the manuscript and approval of the final version of this manuscript. YS: statistical analysis, critical revision of the manuscript and approval of the final version of this manuscript. TP: critical revision of the manuscript and approval of the final version of this manuscript. BL: statistical analysis, critical revision of the manuscript and approval of the final version of this manuscript. AB: critical revision of the manuscript and approval of the final version of this manuscript. SM: concept of the study and review of the literature, critical revision of the manuscript and approval of the final version of this manuscript. MK: concept of the study and review of the literature, critical revision of the manuscript and approval of the final version of this manuscript.
Corresponding author
Ethics declarations
Competing interests
ER reports grants (institutional) from Gilead and Menarini; travel, accommodations, and expenses fees from Pfizer, Roche, Mundipharma, Eli Lilly, Gilead, Novartis and Menarini; honoraria (institutional) for lectures, presentations, consultancy from Eli Lilly, Seagen, Novartis, Astrazeneca, and Menarini; all outside the scope of the submitted work. SD: Consulting or Advisory Role: AstraZeneca, Research Funding: AstraZeneca (Inst), Pfizer (Inst), Roche/Genentech (Inst), Puma (Inst), Eli Lilly (Inst), Novartis (Inst), Sanofi (Inst). Travel, Accommodations, Expenses: Pfizer, AstraZeneca, Roche. YS and BL are employees of Cegedim. TP: Travel and accommodation fees from Servier and Viatris outside the submitted work. AB: Consulting or Advisory Role, Travel, Accommodations, Expenses: Mercks, Viatris, Ipsen, Servier. SM reports personal fees from Scientific Committee Study member to Roche, Data and safety monitoring member of clinical trials: IQVIA, Kedrion, Biophytis, Servier, Yuhan, all outside the scope of the submitted work. MK: None relevant to this study.
Ethics approval and consent to participate
THIN® comprises electronic medical records compliant with the European General Data Protection Regulations (GDPR). This study was examined and approved by THIN® Scientific Review Committee (protocol number 20 002 R1).
Consent to publish
This is a retrospective data of THIN® comprises electronic medical records compliant with the European general data protection regulations (GDPR). A consent to publish this manuscript was not required.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Rassy, E., Delaloge, S., Slaouti, Y. et al. Identifying health conditions associated with an increased risk of pancreatic ductal adenocarcinoma at medium term in nationwide electronic health records of primary care physicians. Br J Cancer 133, 1317–1325 (2025). https://doi.org/10.1038/s41416-025-03172-5
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41416-025-03172-5