Abstract
Regenerative heart valve prostheses are essential for treating valvular heart disease, which requested interactive materials that can adapt to the tissue remodeling process. Such materials typically involves intricate designs with multiple active components, limiting their translational potential. This study introduces a facile method to engineer interactive materials for heart valve regeneration using 1,1’-thiocarbonyldiimidazole (TCDI) chemistry. TCDI crosslinking forms cleavable thiourea and thiocarbamate linkages which could gradually release H2S during degradation, therefore regulates the immune microenvironment and accelerates tissue remodeling. By employing this approach, a double network hydrogel was formed on decellularized heart valves (DHVs), showcasing robust anti-calcification and anti-thrombosis properties post fatigue testing. Post-implantation, the DHVs could adaptively degrade during recellularization, releasing H2S to further support tissue regeneration. Therefore, the comprehensive endothelial cell coverage and notable extracellular matrix remodeling could be clearly observed. This accessible and integrated strategy effectively overcomes various limitations of bioprosthetic valves, showing promise as an attractive approach for immune modulation of biomaterials.
Similar content being viewed by others
Introduction
Valvular heart disease (VHD) is a prevalent cause of cardiovascular morbidity and mortality, affecting over 74 million individuals worldwide1. Currently, there are no medications available to halt the progression of valve deterioration, leading to valve replacement surgery as the most effective treatment option. Mechanical valves are durable heart valve prostheses, which unfortunately requesting lifelong anticoagulation therapy for the patients1,2. Although the bioprosthetic valve does not require long-term anticoagulant therapy, the service life is only 10–15 years. As a compromised solution, particularly for infants and young children, the ROSS procedure involves autograft transplantation of the patient’s own pulmonary valve into the aortic position was often implemented in clinical practice. However, complicated risks are associated with this product, such as late autograft failure and the reintervention of both neocortical valves and the reconstructed right ventricular outflow tract (RVOT). In response to these challenges, decellularized heart valves (DHVs) have emerged as a promising class of new-type valves due to their reduced immunogenicity and preservation of the 3D structure and bioactive compositions that mimic natural heart valves3. Ideally, DHVs can serve as building blocks for tissue remodeling, facilitating the development of regenerative valvular tissue in vivo4. Unfortunately, the decellularization process often compromises the integrity of the extracellular matrix (ECM) and the biomechanical properties of the valves5. Consequently, clinical and preclinical trials using various naked DHV products (e.g., CryoValve SG from CryoLife Inc, Kennesaw, Ga) have demonstrated rapid degradation in vivo and a lack of remodeling or cellularization3. To improve the durability of DHVs, glutaraldehyde crosslinking has been widely adopted in clinical practice6. However, the presence of exposed aldehyde groups in crosslinked DHVs results in severe toxicity and hinders the endothelialization process. This, in turn, induces calcification, thrombosis and chronic inflammation, ultimately accelerating valve dysfunction7.
Given these clinical challenges, it is crucial to further advance DHV modification methods that can improve mechanical properties while simultaneously promoting the tissue remodeling process. Mechanistic studies have identified the reversal of the pro-inflammatory immune microenvironment and the acceleration of endothelialization as critical factors in improving the tissue remodeling of bioprosthetic heart valves8,9. The proinflammatory immune response can cause significant damage to the ECM components in DHVs10,11. The inflammatory M1 Macrophages can produce calcium-binding proteins and secrete extracellular vesicles that induce mineralization, increasing the risk of DHV calcification12,13. Moreover, local inflammation triggers the activation of the fibrinolytic system, resulting in platelet adsorption and the formation of thrombi around the implant14,15. These processes can limit the movement of the valve leaflet, causing leaflet stenosis and valve dysfunction16,17. Similarly, endothelial cells, as key components of innate and adaptive immunity barriers, secrete multiple bioactive molecules that modulate inflammation and the coagulation process. An intact endothelium can reduce valve thrombus formation and the exposure of heterogeneous ECM, thereby decreasing the incidence of pathological intimal neogenesis, endocarditis, and early valve calcification18. Therefore, developing an effective DHV modification strategy to regulate the immune environment after implantation and accelerate the early-stage endothelialization process is highly desirable.
In light of these mechanistic understandings, various methods have been developed for DHV modifications. For example, numerous studies have investigated new valve crosslinking agents, such as riboflavin19, epoxide6, and free radical polymerization crosslinker20. While these agents have shown significant improvements in the mechanical performance of DHVs, most of them lack bioactive functions and result in non-degradable covalent crosslinking that is not conducive to tissue remodeling (Supplementary Table 1). As an alternative approach, hydrogel coating has been extensively investigated. Hydrogels have the ability to enhance the mechanical strength of heart valves, reduce calcification and thrombosis, and serve as a matrix for incorporating functional molecules such as RGD peptides21, SDF-1α22, VEGF23, and other factors that promote endothelial cell adhesion and proliferation23,24,25,26. Nevertheless, several challenges still persist, including the rapid release of active molecules that hinder long-term microenvironment regulation, non-degradable covalent hydrogels that are unable to adapt to the tissue remodeling process, and the loss of protective effects under cyclic stress and high shear stress caused by blood circulation27,28. Consequently, achieving DHVs that meet comprehensive clinical requirements, including appropriate mechanical strength, long-term durability, and the ability to induce and adapt to tissue remodeling, remains an exceedingly challenging task.
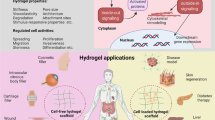
Herein, we introduce a one-step multi-functional crosslinking strategy using 1,1’-thiocarbonyldiimidazole (TCDI) chemistry. This easy accessible approach not only enhances the mechanical strength of DHVs but also effectively regulates macrophage polarization to reverse the proinflammatory immune environments as well as accelerates endothelialization after implantation (Fig. 1). TCDI efficiently crosslinks the collagens of DHVs by reacting with amino and hydroxyl groups. The resulting thiourea and thiocarbamate linkers gradually degrade upon encountering free thiol groups like cysteine or glutathione, releasing H2S. As a gasotransmitter, H2S exerts anti-inflammatory effects by promoting the polarization of M2 macrophages and upregulating the gene expressions of antioxidant enzymes, such as heme oxygenase (HO-1)29,30. H2S also promotes the proliferation and migration of epidermal/endothelial cells by activating the expression of p-ERK1/2 and p-p38 and stimulates angiogenesis by upregulating the expression of angiopoietin-131,32. The easy and efficient one-step TCDI crosslinking readily offers multiple functions to fulfill clinical requirements for DHVs. Applying TCDI chemistry, we further fabricated an interactive polyethylene glycol/poly(sulfobetaine methacrylate) (PEG/PSBMA) double network hydrogel coating on DHVs (Fig. 1B). The PEG network was formed by TCDI crosslinking with DHV and 4-arm PEG-NH2, providing a degradable polymer coating with abundant thiourea linkers that adapt to the recellularization process. The PSBMA network offers anti-fouling, resilience, and self-healing properties to ensure anti-fatigue performance27,33,34. The resulting PEG/PSBMA-DHV exhibits promising anti-calcification and anti-thrombotic properties, even after repeated stretching (Fig. 1B). Both in vitro and in vivo experiments have demonstrated enhanced M2 macrophage infiltration and rapid endothelialization along with the material degradation. In an in vivo abdominal aorta model, PEG/PSBMA-DHV facilitate complete endothelialization of the valve, significantly promotes tissue regeneration, and regulates the local immune microenvironment (Fig. 1C). As a result, these double network hydrogel-coated DHVs overcome several clinical challenges without the need for complicated additives. Particularly, the unique TCDI crosslinking chemistry could also offer a general strategy for fabricating immune regulation materials for a wide range of tissue engineering applications.
A The challenge of bioprosthetic valves (created with BioRender.com). B A schematic overview of the fabrication process and structure of PEG/PSBMA-DHV (Partial material created with BioRender.com). C A schematic overview of the function of PEG/PSBMA-DHV.
Results
Construction of the TCDI crosslinked DHV (T-DHV) and the mechanism of H2S release
TCDI is a versatile reagent and building block in organic synthesis. It is an efficient and widely used thiocarbonylating agent that enables the introduction of thiocarbonyl functionality into various organic molecules35. TCDI readily reacts with a variety of nucleophiles, such as amino36, alcohols37,38, and thiols39, to form thiocarbamate, thioester, and thioether derivatives, respectively40. These reactions proceed under mild conditions at room temperature with fast kinetics and high yields40.
In the context of DHV crosslinking, utilizing TCDI offers several advantages. First, its ability to crosslink collagen by reacting with amino and hydroxyl groups makes it an ideal candidate for enhancing the mechanical strength of DHVs. Second, the resulting thiocarbonyl groups left after crosslinking can serve as a source for the release of the gasotransmitter H2S (Fig. 2A)41,42,43, which has potential benefits for immune modulation. Even though TCDI as a crosslinking reagent for tissue engineering has never been investigated.
A A schematic overview presenting the fabrication process and the mechanism of H2S release of T-DHV (DHV created with BioRender.com). B The content of free amino group on samples’ surface determined by ninhydrin staining (n = 4). C The content of free hydroxyl group on samples’ surface determined by dansyl chloride staining (n = 5). D, E Mechanical properties of DHV with different crosslinking degrees: C Strain-stress curves; D Young’s modulus (n = 4); E Ultimate tensile strength (n = 4). F H2S release equations of DETU and MECT with cysteine. G The release kinetics of DETU and MECT (n = 3). H H2S release mechanism of DETU. Int.1: MS (ESI) for C6H11N2O2S2-, [M-]: calcd.: 207.03; found: 207.07. Int.2: MS (ESI) for C4H4NO2S2-, [M-]: calcd.: 161.97; found: 161.99. Int.3: MS (ESI) for C8H10N2O6S42-, [M]2-: calcd.: 89.48; found: 89.02. I) The H2S release kinetics of DHV, GV, and T-DHV with 16 mM cysteine (n = 3). J) The H2S release kinetics of T-DHV with different concentration cysteine (n = 3). Data were expressed as mean ± SD, *P < 0.05, **P < 0.01, ***P < 0.001, and ****P < 0.0001. n means the number of independent experiments. For box plots, the lower edge denotes the first quartile (Q1, or the 25th percentile) of the data, the central line within the box signifies the median (Q2, or the 50th percentile), while the upper edge of the box corresponds to the third quartile (Q3, or the 75th percentile). The lower whisker extends to the minimum value, indicating its range of variation, and the upper whisker reaches the maximum value, demonstrating its variability. One-way ANOVA was used for analyzing the data.
In this study, the DHVs were obtained by decellularizing the leaflets of procine aortic valves, which contain collagens as the main component44,45. The sufficient decellularization was confirmed by histological staining and DNA content detection as shown in Supplementary Fig. 1. When incubating DHVs with the increasing concentration of TCDI, the amino and hydroxyl groups on collagen gradually decreases, indicating successful crosslinking (Figs. 2B, C). The mechanical properties of the resulting TCDI-crosslinked DHVs (T-DHVs), such as Young’s modulus and ultimate tensile strength, exhibit an increase with higher TCDI concentration (Figs. 2D & E). For example, when the TCDI concentration was 18 mg/mL, Young’s modulus and ultimate tensile strength reached values of 20.95 ± 1.15 MPa and 11.79 ± 0.48 MPa, respectively (Figs. 2D & E). These mechanical strengths are comparable to those of commercially available glutaraldehyde-crosslinked bioprosthetic valves (GV)27. These results confirm that TCDI can serve as a fast crosslinking reagent as efficient as glutaraldehyde.
Based on the reactivity of TCDI, T-DHV would contain thiourea (1) and thiocarbamate (2) linkages (Fig. 2A) after the crosslinking reaction with amino and hydroxyl groups of collagens. Thiocarbamate is well-known to slowly release H2S by hydrolysis, which would be accelerated if exposed to thiol-containing compounds such as cysteine and glutathione43. On the other hand, release of H2S using thiourea as donors is much slower and requires the presence of cysteine, and its reaction kinetics has not been studied (Fig. 2F)27,42. We investigated the release kinetics of thiourea and thiocarbamate using model compounds, N, N-diethyl thiourea (DETU) and O-(1-Methylethyl) N-ethylcarbamothioate (MECT). These studies revealed that cysteine can catalyze the degradation of thiourea and thiocarbamate, thereby accelerating release of H2S (Supplementary Figs. 3A and B, Fig. 2G). Since the cysteine-catalyzed cleavage of thiourea has not been well discussed in the literature, we have conducted a meticulous investigation into its release mechanism. Analysis of reaction mixture by mass spectroscopy suggested formation of carbamodithioate Int.2 and thiazolidine-2-thione Int.3. The latter was also evidenced in 1H nuclear magnetic resonance (NMR) spectra (Supplementary Fig. 3). Based on the experimental results, a plausible reaction pathway is proposed to account for the cysteine-catalyzed release of H2S from thioureas using the model compound DETU (Fig. 2H). The process begins with the nucleophilic addition of cysteine thiol to the thiocarbonyl group of DETU, forming thiolate Int.1, followed by elimination of ethylamine, leading to the formation of carbamodithioate Int.2. This intermediate undergoes an intramolecular ring-closing cyclization to generate thiazolidine-2-thione Int.3, accompanied by the release of a second ethylamine. The ring opening occurs through the nucleophilic addition of a basic hydroxide. The resulting thiocarboxycysteine Int.4 decomposes to produce carbonyl sulfide (COS) and regenerate cysteine46. COS is then hydrolyzed to produce H2S and CO247.
The release of H2S was also observed in T-DHV. In the presence of 16 mM cysteine, significant H2S release was observed in the T-DHV samples, while the raw DHV and the clinically used glutaraldehyde-crosslinked heart valve (GV) exhibited negligible H2S release (Fig. 2I). The rate of H2S release is dependent on the concentration of cysteine. When no cysteine was added, T-DHV showed a slow release of H2S in PBS buffer. However, as the cysteine concentration increased, the rate of H2S release accelerated (Fig. 2J). Overall, these results demonstrate that TCDI efficiently crosslinks DHVs, improves their mechanical properties, and facilitates the continuous release of H2S, most likely due to the formation of thiocarbamate and thiourea linkers.
Construction of double network hydrogel coated DHV (PEG/PSBMA-DHV)
When the naked DHV is implanted, a cascade of coagulation reactions occurs immediately after contact with the bloodstream and absorption of circulating proteins, leading to thrombosis48. In addition, naked DHV forms a large amount of calcium and phosphorus salt deposits on the valve surface due to a large number of groups in the ECM that can bind to Ca2+ in the blood49,50. Therefore, it is necessary to construct a hydrogel coating that could provide anti-coagulation and anti-calcification functions immediately after implantation. Traditional covalent crosslinked hydrogels cannot adapt to the tissue remodeling process and are susceptible to breaking and losing of their protective effect under high shear stress in circulating blood7,28. The tiny cracks formed by hydrogel rupture may lead to more serious calcium and phosphorus salt deposition7,51.
For this purpose, TCDI chemistry was further applied to construct a degradable double network hydrogel coating with anti-fatigue property on DHV. In brief, the DHV and 4-arm-PEG-NH2 (Mw = 2 kDa) were crosslinked by TCDI to immobilize the first PEG hydrogel network on DHV (PEG-DHV). Then, the second hydrogel network was constructed by soaking PEG-DHV in SBMA solution containing free radical initiator, resulting to a PEG/PSBMA dual-network hydrogel-modified DHV (PEG/PSBMA-DHV) (Fig. 3A). The PEG hydrogel alone exhibited brittleness and weak mechanical strength. The incorporation of PSBMA as the second network led to improved anti-fatigue properties (Supplementary Fig. 4A). The homogeneous PSBMA hydrogel displayed a self-recovery rate of 50% after 20 cycles of continuous stretching stimulation, demonstrating excellent self-recovery and anti-fatigue characteristics (Supplementary Figs. 4B & C). When the PSBMA hydrogel was combined with the PEG hydrogel, the performance of the PEG hydrogel was significantly enhanced, with a self-recovery rate of about 70% (Supplementary Figs. 4D & E). The fatigue resistance of the hydrogel coating is attributed to the formation of hydrogen bonds between the sulfur element and the secondary amine group in the first hydrogel network, as well as the ionic bonds formed between the SO3− and N+ groups in the second hydrogel network34,52. The presence of numerous reversible non-covalent bonds between the hydrogel networks imparts strong fatigue resistance to the hydrogel.
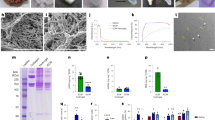
A A schematic overview presenting the fabrication process and structure of PEG/PSBMA-DHV. B General picture of different DHVs. C Surface and cross-section structure of the scaffolds observed by SEM and S element detected by EDS showing that TCDI achieves the cross-linking of DHV and the successful modification of SBMA. D Analysis of S element content by elemental analysis (n = 4). E, F Mechanical properties of DHV with different crosslinking degrees: (E) Ultimate tensile strength (n = 4); (F) Young’s modulus (n = 4). G Pictures of water droplet contacting scaffolds. H) Water contact angle (WCA) showing increased hydrophilicity after modification (n = 5). I The release kinetics of DHV, GV, T-DHV, PEG-DHV and PEG/PSBMA-DHV with 16 mM cysteine by WSP-1 probe (n = 4). J The thermal shrinkage temperature of scaffolds. K) Relative weight loss of DHVs after collagenase digestion (n = 5). Data were expressed as mean ± SD, *P < 0.05, **P < 0.01, ***P < 0.001, and ****P < 0.0001. n means the number of independent experiments. For box plots, the lower edge denotes the first quartile (Q1, or the 25th percentile) of the data, the central line within the box signifies the median (Q2, or the 50th percentile), while the upper edge of the box corresponds to the third quartile (Q3, or the 75th percentile). The lower whisker extends to the minimum value, indicating its range of variation, and the upper whisker reaches the maximum value, demonstrating its variability. One-way ANOVA was used for analyzing the data.
From the general pictures, T-DHV and GV appear similar yellow, but gradually turn white with the modified PEG hydrogel and PEG/PSBMA hydrogel (Fig. 3B). Observations using scanning electron microscopy (SEM) revealed that the T-DHV, PEG-DHV, and PEG/PSBMA-DHV samples had smooth and flat surfaces compared to the rough surface formed by GV. Additionally, the glutaraldehyde crosslinking process led to the loss of the porous structure, whereas T-DHV, PEG-DHV, and PEG/PSBMA-DHV maintained cross-sectional structures similar to DHV (Fig. 3C). Energy-dispersive spectrum (EDS) mapping scans showed a significant increase in the sulfur element signal in T-DHV, PEG-DHV, and PEG/PSBMA-DHV compared to DHV and GV, particularly in the PEG/PSBMA-DHV. This confirmed the successful modification and crosslinking, as well as the even distribution of SBMA (Fig. 3C).
Elemental analysis (EA) and Fourier-transform infrared spectrophotometer (FTIR) were used to analyze the elemental content and composition of the samples. EA results showed that the sulfur element content in T-DHV (1.50 ± 0.42%) and PEG-DHV (4.13 ± 1.24%) was higher than that in DHV (0.30 ± 0.05%) and GV (0.27 ± 0.07%) due to the TCDI crosslinking. The sulfur element content in PEG/PSBMA-DHV reached 6.61 ± 0.82% due to the further modification of PSBMA on the surface of DHV (Fig. 3D). A comparison of the FTIR spectra between PEG-DHV and PEG/PSBMA-DHV revealed an additional absorption peak at 1038 cm−1 in the latter, which can be attributed to the S = O symmetric stretching in SBMA chains. This further confirms the successful construction of the PEG/PSBMA double-network hydrogel-modified DHV (Supplementary Fig. 5A).
The PEG/PSBMA-DHV exhibited a similar Young’s modulus and ultimate tensile strength to T-DHV and PEG-DHV (Supplementary Figs. 5B, Figs. 3E, F), all of which were comparable to the clinically used GV and significantly higher than unmodified DHV27. However, the hydrophilicity of the DHV was significantly improved after the application of the hydrogel coating. The water contact angle (WCA) of PEG/PSBMA-DHV decreased to 44.0 ± 9.9°, indicating a much more hydrophilic surface compared to the uncoated DHV (WCA = 80.7 ± 8.8°) and T-DHV (64.8 ± 5.2°) (Figs. 3G, H). These characterizations indicate the PEG/PSBMA-DHV could provide favorable mechanical strength and hydrophilic surface property.
Furthermore, the PEG/PSBMA-DHV also exhibited a gradual release of H2S, albeit at a slower initial rate compared to T-DHV (Fig. 3I). This can be attributed to the release of H2S from the thiourea groups in the PEG hydrogel, which has slower kinetic comparing to the cleavage of thiocarbamates in T-DHV. Notably, after long-term incubation, both the PEG-DHV and PEG/PSBMA-DHV were capable of releasing more H2S than T-DHV due to the additional TCDI crosslinking sites (Fig. 3I). The presence of the PSBMA network further contributed to the slowing down of H2S release compared to PEG-DHV, resulting in less H2S release from PEG/PSBMA-DHV within the observation period. However, it is conceivable that prolonged time may lead to a further increase in H2S release from PEG/PSBMA-DHV. This observation underscores another advantage of the PEG/PSBMA hydrogel coating, which offers the potential for a continuous, slow release of H2S to regulate the immune microenvironment for an extended period.
PEG/PSBMA-DHV increased thermal stability and enzymatic degradation resistance
The introduction of the PEG/PSBMA double network hydrogel coating is expected to enhance the thermal stability of DHV and prevent enzymatic degradation. Therefore, the thermal shrinkage temperature of the samples was determined using DSC (Differential Scanning Calorimetry). The results, as shown in Fig. 3J, indicated that the thermal shrinkage temperatures of T-DHV and PEG-DHV were similar to those of clinically used GV and significantly higher than those of the raw DHV. This finding further supports the effective crosslinking achieved with TCDI. The incorporation of the second PSBMA network further improved the thermal stability of DHV. The thermal shrinkage temperature of PEG/PSBMA-DHV increased to 100.6 °C (Fig. 3J). Furthermore, the enzymatic degradation resistance of the samples was evaluated using collagenase treatment. As shown in Fig. 3K, GV barely degraded within seven days ( < 6.5 ± 2.1% weight loss), due to the non-degradable glutaraldehyde crosslinking. In contrast, DHV without modification degraded rapidly 31.1 ± 3.5% weight loss was already observed on the first day and almost complete degradation was revealed on day 7. All TCDI crosslinked samples showed improved stability comparing to DHV. T-DHV could retain half mass on the day 7, whereas PEG-DHV and PEG/PSBMA-DHV revealed even slower degradation rate (31.9 ± 6.6% and 23.1 ± 2.8% weight loss respectively on day 7). These results suggested that the TCDI crosslinking and hydrogel coating enhanced the thermal stability of DHVs and prevented the fast enzymatic degradation. The PEG/PSBMA-DHV could be relatively stable just after implantation and adaptively degrade over a longer regenerative period.
The durable anti-calcification and anti-fouling property of PEG/PSBMA-DHV
Heart valves require anti-calcification and anti-fouling properties to maintain their functionality and longevity. Calcification can stiffen the valve leaflets, leading to valve stenosis and obstruction50,53. Therefore, anti-calcification properties are essential to preserve the flexibility of heart valves, prevent blockages, and enhance durability49. Similarly, the absorption of blood proteins also hinders valve movement and promotes thrombus formation and inflammation49. Hence, anti-fouling properties is also requested to ensure proper valve function, reduce the risk of clot formation, and minimize inflammatory responses. Particularly, heart valves undergo continuous, cyclic mechanical stimulation due to the rhythmic contractions and relaxations of the heart muscle. Consequently, it is highly demanded to investigate the anti-calcification and anti-fouling properties even after intensive repetitive motion.
For this purpose, we investigate the anti-calcification and anti-fouling property of PEG/PSBMA-DHV before and after fatigue test. The sample strips (length of 10 mm and width of 5 mm) were cut from the thickest central area of the valve belly (Fig. 4A). The thickness of the samples was measured by vernier caliper before the cyclic tensile tests to ensure the consistency among different samples. To simulate the calcification conditions, the samples, both before and after undergoing 500 fatigue tests, were immersed in a solution of CaCl2 for 24 h, followed by a dropwise addition of Na2HPO4 solution (Figs. 4A, B). The calcium deposition on the DHV’s ventricular layer was characterized using SEM and Atomic Absorption Spectrometry (AAS). PEG/PSBMA-DHV exhibited the lowest level of calcification (2.1 ± 0.6 ug/mg), confirming the desired function of the double network hydrogel coating. Remarkably, T-DHV also exhibited reduced calcification (5.2 ± 1.0 ug/mg) compared to commercially used GV (7.4 ± 1.5 ug/mg), further demonstrating the superiority of TCDI crosslinking over glutaraldehyde crosslinking. Importantly, when DHV samples underwent continuous mechanical cyclic stimulation, the degree of calcification for DHV (7.2 ± 1.1 ug/mg), GV (12.4 ± 0.7 ug/mg), T-DHV (11.2 ± 1.3 ug/mg), and PEG-DHV (7.9 ± 1.4 ug/mg) significantly increased by 1–3 times after 500 stretching cycles. However, there was no significant difference in the degree of calcification observed for PEG/PSBMA-DHV (2.3 ± 0.9 ug/mg) after the fatigue test (Fig. 4D). SEM images exhibited a similar trend (Fig. 4B). These results indicate that the hydrophilic hydrogel modification can significantly reduce calcium deposition on the valve surface, and the anti-fatigue property provided by PSBMA facilitate long-term protection even after cyclic mechanical stimulation.
A Schematic diagram of fatigue test (created with BioRender.com). B SEM observed calcium deposition on sample surface before and after fatigue test. C Laser confocal microscopy observed sample surface protein (BSA-TXO) deposition before and after fatigue test, and the TXO group can be excited by 405 nm to emit blue fluorescence. D Quantitative analysis of calcium content in samples before and after fatigue test by atomic absorption spectrometer (n = 3). E Quantitative analysis of BSA content in samples before and after fatigue test by BCA method (n = 3). Data were expressed as mean ± SD, *P < 0.05, **P < 0.01, ***P < 0.001, and ****P < 0.0001. n means the number of independent experiments.
The in vitro protein adhesion test was performed by incubating bovine serum albumin (BSA) with DHV for 12 h at 37 °C. The amount of protein absorbed on DHV was quantified by determining the BSA concentration in the solution before and after incubation with DHV samples by bicinchoninic acid (BCA) method (Fig. 4E). For visualization, the BSA was further labeled with thioxanthone (TXO) and imaged using a confocal laser scanning microscope (Fig. 4C). The results indicated that raw DHV exhibited significant protein adhesion, particularly after the fatigue test. Although the crosslinking by both glutaraldehyde and TCDI did not initially reduce protein adhesion, the amount of absorbed protein after the fatigue test was remarkably reduced due to increased mechanical stability. PEG/PSBMA-DHV showed the lowest protein adhesion both before and after the fatigue test (500 time stretching), indicating a durable anti-fouling effect after coating with double network hydrogel.
In vitro hemocompatibility and biocompatibility of PEG/PSBMA-DHV
Excellent blood compatibility is the most important criteria for blood-contacting devices such as heart valves. Cell damage, protein adhesion, platelet activation and other phenomena caused by blood-contacting devices can lead to serious consequences such as inflammation and thrombosis54. Thus, superior hemocompatibility is highly demanded for ideal DHV materials. As an endogenous gas signaling molecule, H2S can inhibit platelet aggregation and activation, thus inhibiting thrombus formation55. When combined with the efficient anti-fouling ability of PEG/PSBMA, the coated DHV should further improve its anti-thrombotic ability and achieve excellent blood compatibility. Therefore, the hemocompatibility of PEG/PSBMA-DHV was evaluated from three perspectives: hemolysis, platelet adhesion and thrombosis (Fig. 5A).
A Schematic diagram of hemocompatibility tests (created with BioRender.com). ACD: Acetate citrate diethylene, which is a commonly used blood anticoagulant reagent. B Platelets (false color from yellow) adhered on the scaffolds observed by SEM. C LDH assay quantified number of platelets adhered to the scaffolds (n = 6). D Quantification of the thrombus (OD540nm) by spectrophotometric method (n = 6). E Hemolysis rates of the samples (OD450nm) by spectrophotometric method (n = 3). F General picture of hemolysis experiments at different time points and thrombogenesis of the scaffolds after incubating with whole blood. *: From left to right are DHV, GV, T-DHV, PEG-DHV, and PEG/PSBMA-DHV. G Cytotoxicity of HUVECs by MTT, indicating good cytocompatibility of all scaffolds except GV group (n = 6). H) Cytotoxicity of BMSCs by MTT (n = 5). I BMSC cultured on different samples and stained by calcein to visualize the live cells. Data were expressed as mean ± SD, *P < 0.05, **P < 0.01, ***P < 0.001, and ****P < 0.0001. n means the number of independent experiments. For box plots, the lower edge denotes the first quartile (Q1, or the 25th percentile) of the data, the central line within the box signifies the median (Q2, or the 50th percentile), while the upper edge of the box corresponds to the third quartile (Q3, or the 75th percentile). The lower whisker extends to the minimum value, indicating its range of variation, and the upper whisker reaches the maximum value, demonstrating its variability. One-way ANOVA was used for analyzing the data.
The platelet-rich plasma was incubated with the samples at 37 °C for 1 h, and platelet adhesion and activation were visualized using SEM and quantified through LDH (lactic dehydrogenase) analysis. Among the samples, DHV exhibited the highest number of adherent platelets (0.34 ± 0.02 OD). In contrast, T-DHV, PEG-DHV, and PEG/PSBMA-DHV showed minimal platelet adhesion, similar to GV (0.12 ± 0.01 OD) (Fig. 5C). SEM also confirmed this trend in platelet adhesion, with DHV showing a large number of pseudopodia formation indicating platelet activation. In contrast, a small number of platelets were observed on T-DHV’s surface which remained inactive (Fig. 5B). The hydrogel coating clearly reduced platelets adhesion as shown by both PEG-DHV and PEG/PSBMA-DHV.
The in vitro thrombosis test was conducted by incubating the samples with recalcified whole blood at 37 °C for 30 min. The anti-thrombotic ability was analyzed using general photographs and spectrophotometry. DHV’s surface was prone to significant thrombus formation, while GV, which is clinically used with glutaraldehyde cross-linking, exhibited less thrombus formation due to its cytotoxicity (Figs. 5D, F). T-DHV had slightly higher thrombus formation than GV but significantly lower than DHV. Thrombus formation was significantly inhibited after hydrogel coating. Both PEG-DHV and PEG/PSBMA-DHV showed lower levels of thrombosis compared to clinically used GV (Figs. 5D, F).
Hemolytic properties were also analyzed quantitatively using spectrophotometry and visualized through general photographs. The hemolytic rate was determined by measuring the absorbance of hemoglobin released from erythrocytes. The hemolysis rates of DHV, GV, T-DHV, PEG-DHV, and PEG/PSBMA-DHV were found to be below 2% after 1 h with no significant difference (Fig. 5E), which is consistent with the observations in general photographs (Fig. 5F).
Glutaraldehyde cross-linked bioprosthetic valves have a limited lifespan due to the presence of toxic aldehyde groups that hinder cellularization. Therefore, tissue-engineered valves need to exhibit excellent biocompatibility to facilitate recellularization and accelerate endothelialization. HUVECs (Human umbilical cord blood endothelial cells) and BMSCs (Bone marrow mesenchyml stem cell) were used to evaluate the cytotoxicity of PEG/PSBMA-DHV. As depicted in Fig. 5G & H, the cell viability of HUVECs and BMSCs co-cultured with T-DHV, PEG-DHV, and PEG/PSBMA-DHV exceeded 90%, with no significant differences observed among the samples. This suggests that TCDI cross-linking and PSBMA copolymerization in DHV do not induce cytotoxicity. In contrast, GV resulted in the death of nearly half of the cells, exhibiting cell viability below 60%. Furthermore, the staining of the live cells after 48 h of co-culture indicated that all samples, except GV, maintained good cell morphology of BMSCs (Fig. 5I). These results indicate that TCDI and SBMA copolymerization cross-linked DHV demonstrated better biocompatibility compared to GV.
Overall, the results presented above support the significantly improved biocompatibility provided by TCDI crosslinking compared to the clinically used glutaraldehyde crosslinking. Additionally, T-DHV demonstrated the ability to reduce platelet activation and thrombus formation compared to raw DHV, which is a favorable outcome. Moreover, the PEG/PSBMA hydrogel coating further reduced platelet adhesion and prevented thrombosis. These findings, along with the low hemolysis rate and excellent biocompatibility with HUVECs and BMSCs, highlight the superior hemocompatibility and biocompatibility of both T-DHV and PEG/PSBMA-DHV, indicating their significant potential for clinic applications.
Evaluation of immunomodulatory capacity of PEG/PSBMA-DHV
Macrophages, particularly the M2 phenotype, have emerged as a key focus in tissue regeneration research due to their extensive interactions with stem cells and crucial involvement in all stages of tissue repair56. In cardiovascular diseases (CVDs), the macrophage phenotype plays a pivotal role, with a predominance of pro-inflammatory M1 macrophages observed at the lesion site11,57,58. The resultant pro-inflammatory cytokines and oxidative stress generated by M1 macrophages can induce osteoblast-like differentiation of valve interstitial cells and subsequently lead to valve calcification11,57,59. However, monocytes/macrophages possess the ability to alter their phenotype in response to environmental changes, thereby modulating their function. H2S has been found to exert anti-inflammatory effects by promoting M2 macrophage polarization. It not only inhibits various inflammatory pathways, including NF-κB, JNK, and ERK signaling, through protein S-sulphydration but also functions as a potent cell redox regulator, regulating macrophage epigenetics and promoting mitochondrial biogenesis9. Furthermore, M2 macrophages secrete transforming growth factor-beta (TGF-β), vascular endothelial growth factor (VEGF), and fibroblast growth factor (FGF), which play critical roles in recruiting fibroblasts and endothelial cells, facilitating angiogenesis, collagen deposition, and wound contraction29,60,61. Therefore, it is expected that TCDI crosslinked DHVs, endowed by their H2S release ability, could promote macrophage M2 phenotypic polarization and subsequently accelerates valve endothelialization. In this section, flow cytometry and cell migration assays were used to evaluate the immunoregulatory capacity of PEG/PSBMA-DHV and its effect on cell migration (Fig. 6A).
A Schematic diagram of immunomodulatory capacity tests (created with BioRender.com). CM: Conditional medium. B Phenotypic analysis of RAW264.7 by flow cytometry (n = 6). C Statistics of the proportion of CD206 positive cells (n = 6). D-E) mRNA expression of anti-inflammatory factors was analyzed by RT-qPCR: (D) Arg 1 (n = 3); (E) IL-10 (n = 3). F TGF-β1 content was detected by ELLSA method (n = 3). G Scratch migration experiment of HUVECs (n = 6). H HUVECs mobility statistics (n = 6). Data were expressed as mean ± SD, *P < 0.05, **P < 0.01, ***P < 0.001, and ****P < 0.0001. n means the number of independent experiments. For box plots, the lower edge denotes the first quartile (Q1, or the 25th percentile) of the data, the central line within the box signifies the median (Q2, or the 50th percentile), while the upper edge of the box corresponds to the third quartile (Q3, or the 75th percentile). The lower whisker extends to the minimum value, indicating its range of variation, and the upper whisker reaches the maximum value, demonstrating its variability. One-way ANOVA was used for analyzing the data.
To investigate the immunomodulatory function of the DHVs, we characterized the cell phenotype of RAW264.7 macrophages co-cultured with the samples for 48 h using flow cytometry (Fig. 6A). As depicted in Figs. 6B, C, the CD206 positivity of RAW264.7 cells co-cultured with T-DHV (37.05 ± 3.85%), PEG-DHV (32.19 ± 2.05%), and PEG/PSBMA-DHV (27.05 ± 1.71%) was significantly higher compared to DHV (3.86 ± 0.60%) and GV (4.85 ± 0.32%). Furthermore, we assessed the secretion of cytokines by RAW264.7 cells using enzyme-linked immunosorbent assay (ELISA) and quantitative reverse transcription PCR (RT-qPCR). TGF-β1, Arg1, and IL-10 are characteristic cytokines secreted by M2 macrophages, known for their crucial role in anti-inflammatory responses62. The relative mRNA levels of Arg1 and IL-10 were markedly upregulated in macrophages treated with these three samples, compared to DHV and GV (Fig. 6D & E). Additionally, ELISA results showed a significant promotion of TGF-β1 expression by T-DHV, PEG-DHV, and PEG/PSBMA-DHV (Fig. 6F). These findings provide evidence that T-DHV, PEG-DHV, and PEG/PSBMA-DHV effectively induce macrophage polarization toward the M2 phenotype. These observations align with the H2S release rate discussed in Fig. 2, further supporting the notion that the immunomodulatory ability is attributed to the H2S release facilitated by TCDI crosslinking. To further validate the immunomodulatory capacity independent of the modifiers, we treated RAW264.7 cells separately with 4-arm-PEG-NH2 and SBMA monomers, which resulted in no significant change in the macrophage phenotype. The CD206 positive ratios were measured as 3.73 ± 0.22% and 3.475 ± 1.00%, respectively (Supplementary Figs. 6A and C). Furthermore, no H2S production was detected from the DMEM medium with 4-arm-PEG-NH2 and SBMA monomers (Supplementary Fig. 6B). These additional experiments further confirm that the regulation of macrophage phenotype in this system is achieved through H2S release enabled by TCDI crosslinking.
Furthermore, to enhance the H2S release, we added 0.8 M cysteine to the RAW264.7 cells co-cultured with 4-arm-PEG-NH2 monomer, SBMA monomer, DHV, GV, T-DHV, PEG-DHV, and PEG/PSBMA-DHV, respectively. Flow cytometry results revealed that the DHVs with TCDI crosslinking (T-DHV, PEG-DHV, and PEG/PSBMA-DHV) promoted enhanced macrophage polarization towards the M2 phenotype. In contrast, the rate of CD206-positive macrophages in the remaining samples did not change significantly (Supplementary Fig. 7A and B). These findings suggest that free cysteine in blood stream could possibly enhance the immune regulation ability due to the accelerated H2S release.
In addition to evaluating the macrophage phenotype, we also investigated the recruitment and migration capabilities of differentiated macrophages towards HUVECs and BMSCs. We co-cultured the DHVs with macrophages for 48 h, and the resulting conditioned media were used to stimulate HUVECs and BMSCs. As shown in Figs. 6G, H, the conditioned media derived from T-DHV, PEG-DHV, and PEG/PSBMA-DHV significantly promoted HUVECs migration, with respective mobilities of 67.23 ± 15.03%, 61.67 ± 8.57%, and 58.43 ± 11.81% after 48 h of culture (Fig. 6H). Additionally, transwell-based cell invasion experiments also demonstrated that TCDI cross-linked DHVs promoted BMSCs recruitment (Supplementary Fig. 8). Overall, our findings indicate that the TCDI cross-linked DHVs induce macrophage polarization towards the M2 phenotype, resulting in cytokine secretion that can effectively recruit stem cells from peripheral blood and promote the migration of endothelial cells from peripheral blood vessels. These advantages are highly desirable for accelerating valve endothelialization and tissue regeneration after implantation.
In vivo degradation and immunomodulatory ability of the DHVs after subcutaneous implantation
A rat subdermal implantation model was established to assess the in vivo histocompatibility of the DHVs (Fig. 7A). The histological staining results are presented in Fig. 7B, and ImageJ was used to make statistics on the section area occupied by residual collagen in different sections, which was used to reflect the situation of collagen. The DHV was predominantly occupied by cells, with minimal residual collagen observed in most areas, indicating the highest degradation ratio of 69.12 ± 4.07% (Figs. 7B and D). In comparison, the collagen degradation ratios of T-DHV, PEG-DHV, and PEG/PSBMA-DHV were 29.61 ± 5.24%, 29.84 ± 7.92%, and 32.91 ± 3.72%, respectively, which demonstrated a significant deceleration in degradation compared to DHV (Fig. 7D). Notably, there was no statistical difference in degradation rate between these three samples and the GV group (24.72 ± 2.93%). Furthermore, von Kossa staining revealed the absence of calcification in all samples except the GV group, where an abundance of calcium nodules was observed throughout the entire layers.
A Schematic diagram of subcutaneous implantation (created with BioRender.com). B After 28 days of subcutaneous embedding, sections were stained with HE, Masson, EVG and von Kossa. HE for cell and ECM, Masson stain for collagen, EVG stain for elastin, and von Kossa stain for calcification. * indicates the position of the heart valve (n = 3). C Samples were taken at day 7, day 14 and day 28, and CD163 (green) / iNOS (red) /DAPI (blue) staining was performed on the sections to evaluate the immunomodulatory capacity of the sample (n = 3). D The degradation rate of sample was calculated by calculating the percentage of collagen in the Masson stain (n = 6). E The ratio of CD163/DAPI double-positive cells to DAPI-positive cells was calculated by Image J, representing the proportion of M2 phenotype macrophages in the sample (n = 6). Data were expressed as mean ± SD, *P < 0.05, **P < 0.01, ***P < 0.001, and ****P < 0.0001. n means the number of biologically independent samples. For box plots, the lower edge denotes the first quartile (Q1, or the 25th percentile) of the data, the central line within the box signifies the median (Q2, or the 50th percentile), while the upper edge of the box corresponds to the third quartile (Q3, or the 75th percentile). The lower whisker extends to the minimum value, indicating its range of variation, and the upper whisker reaches the maximum value, demonstrating its variability. One-way ANOVA was used for analyzing the data.
We also investigated the immunomodulatory capacity of the samples in vivo, as shown in Fig. 7C. In the GV group, no significant cell infiltration was observed at any time point due to the cytotoxicity of glutaraldehyde. In the DHV group, only a small number of M2 phenotype macrophages were present over the observation period. Encouragingly, T-DHV, PEG-DHV, and PEG/PSBMA-DHV exhibited a substantial presence of M2 phenotype macrophages after 28 days. Particularly, T-DHV demonstrated 34.05 ± 3.31% M2 macrophages 7 days after implantation, and the prevalence of M2 macrophages gradually increased over time due to the rapid H2S release facilitated by the thiocarbamate groups on the surface of T-DHV. In contrast, PEG-DHV and PEG/PSBMA-DHV initially showed low amount of M2 macrophages at day 7, but the amount of M2 macrophages were increased to the comparable level with T-DHV after 28 days. This phenomenon is consistent with the in vitro DHV degradation tests (Fig. 3K). The PEG-DHV and PEG/PSBMA-DHV exhibited slower degradation rate comparing to T-DHV due to the additional hydrogel layer and the slower cleavage kinetic of the predominant thiourea linkage. This slow gradation prevented cell infiltration, but is beneficial to provide sufficient anti-calcification and anti-thrombotic function at the initial stage after implantation. As the implantation time extended, the gradual degradation facilitated continuous release of H2S and resulted in similar level of M2 macrophages infiltration comparing to DHV after 4 weeks.
The results highlighted the ability of TDCI crosslinked valves to prevent rapid degradation of the collagen component and induce polarization of macrophages towards the M2 phenotype., showcasing promising biocompatibility and the potential to promote in situ regeneration of heart valves. Moreover, considering the superior anti-calcification and anti-fouling effect particularly after fatigue test as discussed in Fig. 4, PEG/PSBMA-DHV would be more attractive for in vivo application under mechanical challenges.
Overall performance of PEG/PSBMA-DHV under hemodynamic environment
Traditional animal models, such as subdermal implantation or abdominal wall repair models, have limitations in simulating the in vivo environment of heart valves. These models often do not involve direct blood contact, making it difficult to assess the recellularization capability of the valves. In this study, we addressed these challenges by sewing heart valves into hollow tubes and transplanting them into the abdominal aorta of rats, partially simulating the hemodynamics of heart valves (Fig. 8A). This animal model allowed us to evaluate not only inflammation and tissue remodeling but also blood compatibility and endothelialization of the valves. While this model does not completely replicate the microenvironment of the valve in vivo, it represents a significant improvement over traditional small animal experimental models and holds great promise in evaluating the performance of tissue-engineered heart valves48.
A Schematic diagram of abdominal aorta transplantation (created with BioRender.com). B General views and doppler ultrasound images of the scaffolds implanted in the rat abdominal aorta. The model was established successfully, and DHV scaffold dilated significantly like aneurysm while the other two remained tubular structure (n = 3). C Immunofluorescence staining of endothelial cells (CD31 + , green) and all the infiltrated cells (DAPI, blue) after 7 days, 14 days and 28 days showing the endothelialization process of the scaffolds. The * represents the position of blood flow. PEG/PSBMA-DHV scaffold presented the fastest speed and highest degree of endothelialization among groups (n = 3).
The performance of double network hydrogel coated PEG/PSBMA-DHV under the hemodynamic environment was evaluated in rat abdominal aorta implantation model, and compared with raw DHV and clinical used GV. Figure 8B presents photographic images of the valves after being implanted for 4 weeks. Due to the rapid degradation of DHV in vivo, the naked DHV exhibited significant dilation resembling an aneurysm, while the other samples maintained their tubular structure. Doppler ultrasound examination confirmed that all valves remained unobstructed during the study period (Fig. 8B). To assess the endothelialization capacity of the materials, we collected samples at 7 days, 14 days, and 28 days and performed CD31 fluorescence staining (green). Similar to the results in subcutaneous embedding models (Fig. 7C), no significant signs of cell infiltration were observed for PEG/PSBMA-DHV after 7 days implantation (Fig. 8C), due to the slow degradation of the thiourea based hydrogel coating. However, extensive endothelial cell coverage (approximately 50%) could be already observed after 14 days associated with the hydrogel degradation. Remarkably, at 28 days, complete endothelial cell coverage was found on the surface in contact with the blood. In contrast, the raw DHV and GV showed no signs of endothelialization at any of the observation time points, with minimal cell infiltration observed throughout the GV due to toxicity. These results indicate that the PEG/PSBMA-DHV possesses excellent blood compatibility while effectively accelerating valve endothelialization.
We also investigated the degradation, calcification, immunomodulatory, and recellularization capabilities of the materials under a hemodynamic environment. As shown in Fig. 9 the histological results of sample degradation, remodeling, and calcification after 4 weeks were consistent with the outcomes of the subcutaneous implantation model mentioned above. PEG/PSBMA-DHV showed certain degradation and cell infiltration capacity, but the rate was much slower than DHV. Compared with GV, PEG/PSBMA-DHV does not have calcification and supports cell infiltration. Inflammation was further visualized using immunofluorescence imaging, focusing on the macrophage phenotype. After 28 days of implantation, DHV showed almost no macrophages, while the GV still had a significant number of M1 phenotype macrophages with a pro-inflammatory phenotype (Fig. 9). Furthermore, due to the non-degradability of the GV causing a foreign body reaction, the macrophages were present in the thick fibrous tissue surrounding the sample rather than infiltrating into the valve. In contrast to the DHV and GV, PEG/PSBMA-DHV, with its cysteine-responsive H2S release ability, exhibited a large number of M2 subtype macrophages with tissue regeneration capabilities in both the valve and surrounding tissue. Additionally, due to the controlled degradation of the covalent bonds formed by TCDI cross-linking, macrophages were found infiltrated into the valve matrix (Fig. 9).
Masson staining displayed ECM collagen fiber; von Kossa staining displayed calcification of the scaffolds; Immunofluorescence staining of iNOS (for M1 subtype, green) and CD163 (for M2 subtype, red) showed inflammatory infiltration of the scaffolds; Immunofluorescence staining of CD31 (for endothelial cells, green) and vimentin (for interstitial cells, purple) showed cellularization of the samples; Collagen type I (Col-I) was stained by immunohistochemistry to reflect ECM remodeling. All the samples exhibited different degrees of cellularization, degradation and remodeling except the GV group (n = 3). The * represents the position of blood flow.
To verify the relationship between M2 phenotypic macrophages and tissue remodeling, we performed CD31 and vimentin (VIM) fluorescence staining on valve endothelial cells and valve stromal cells, respectively. The results shown in Fig. 9 revealed no cell infiltration or evident CD31+ and VIM+ cells in the GV. In the DHV, there was no complete endothelial cell layer coverage on the blood contact side, and VIM+ cells were observed within the valve tissue. However, PEG/PSBMA-DHV exhibited complete coverage of endothelial cell layers and the presence of VIM+ cells, indicating successful regeneration of valve endothelial cells and valve interstitial cells within 28 days. Collagen type I, the main component of the valve ECM, was also found regenerated, as observed through immunohistochemical staining (Fig. 9). The newly deposited collagen further demonstrated the ECM remodeling process of the materials. These results revealed that PEG/PSBMA-DHV underwent degradation and showed promising tissue remodeling, while the GV did not exhibit cellularization and DHV only permitted cell infiltration but lacked endothelialization.
Overall, the degree of recellularization and tissue regeneration correlated with the content of M2 phenotype macrophages in the heart valve. PEG/PSBMA-DHV effectively induced macrophage polarization towards an anti-inflammatory and pro-tissue regeneration phenotype, while also displaying good anti-calcification and anti-thrombotic properties. Therefore, it presented favorable endothelialization, recellularization and tissue remodeling capability, which is highly challenging for heart valve development. Moreover, the bio-controllable degradation and immunoregulatory properties of the TCDI crosslinker distinguish it from traditional covalent crosslinkers, which is essential for the remarkable cell infiltration and tissue remodeling observed in vivo. It resolves the issues of unstable crosslinking and poor mechanical strength encountered with non-covalent crosslinkers, while overcoming the problems associated with non-degradable covalent crosslinkers that impede cell infiltration and hinder tissue regeneration.
Discussion
In this study, we successfully constructed bioprosthetic heart valves with regenerative capacity by creating the PEG/PSBMA dual network hydrogel coating on the DHV via a multifunctional TCDI crosslinking strategy. The key findings of this study can be summarized as follows: I) the TCDI chemistry was explored in heart valve engineering, demonstrating the ability to crosslink DHVs and enhance the mechanical properties significantly. The cleavable thiourea and thiocarbamate linkages generated by TCDI crosslinking facilitate the slow release of H2S during degradation. This imparts the DHVs with remarkable ability to induce macrophage polarization towards the M2 phenotype, thereby accelerating endothelialization and tissue regeneration. II) Benefit from the TCDI chemistry, a degradable PEG/PSBMA double network hydrogel was created on DHVs to provide enhanced anti-fatigue properties. Even after undergoing 500 cycles fatigue tests, the modified DHVs exhibits excellent anti-calcification and anti-protein adhesion characteristics. The overall design revealed complete endothelial cells coverage, adaptive ECM remodeling, and tissue regeneration in both subdermal and hemodynamic abdominal aorta implantation models.
Among the various DHV crosslinking methods, covalent crosslinking agents (e.g. glutaraldehyde and 1-Ethyl-3-(3-dimethylaminopropyl)carbodiimide/N-Hydroxysuccinimide) offer high stability to the resulting DHVs7,63. However, their drawback lies in the limited biological activities that impede valve regeneration. On the other hand, non-covalent crosslinking using bioactive substances such as polyphenols often lacks adequate protection for DHVs, leading to significant collagen degradation within just 24 h of exposure to collagenase (Supplementary Table 1)64,65,66. Remarkably, TCDI crosslinking presents promising biocompatibility and enhanced mechanical strength comparable to other covalent crosslinking, providing improved stability to DHVs post-implantation. The thiourea and thiocarbamate linkages formed by TCDI crosslinking gradually degrade upon encountering internal thiol-containing molecules like cysteine and glutathione, releasing H2S for immune modulation. This unique property offers a facile approach to developing interactive materials that can adapt to tissue remodeling processes. Following implantation, the intact hydrogel layer offers anti-calcification and anti-thrombosis characteristics for DHVs in the early stages. In vivo findings demonstrate that this protection can persist for over 7 days without observed cell infiltration. Over a span of two to three weeks, the gradual degradation of crosslinking points leads to continuous H2S release, stimulating the repolarization of macrophages and promoting endothelial cell proliferation and migration. Subsequently, hydrogel degradation coupled with re-endothelialization on the DHV surface and infiltration of M2 macrophages and interstitial cells into the DHV can be clearly observed after 28 days of implantation. This comprehensive and multifunctional crosslinking strategy not only shows promise for bioprosthetic heart valves but also holds potential for a range of tissue engineering applications.
Overall, the remarkable features of the engineered DHVs showcased in this study provide significant advantages over traditional prosthetic valves. Particularly noteworthy is that these comprehensive benefits are achieved solely through innovative material design, eliminating the need for the supplementary of bioactive components. Therefore, it holds great potential for clinical applications.
Methods
Ethical Statement
Our research complies with all relevant ethical regulations of Huazhong University of Science and Technology. Animal experiments were approved by the Institutional Animal Care and Use Committee of Huazhong University of Science and Technology, in accordance with all relevant ethical codes (IACUC Number 3649). Abdominal aortic transplantation and subcutaneous embedding in rats approved by animal research and ethics committees have always followed humane endpoints.
Decellularization
DHV was prepared as previously described67. Briefly, leaflets of porcine aortic valves were harvested from a local slaughterhouse and transported to the laboratory immediately. After washing away blood, valves were immersed in M3 solution prepared by dissolving 3-((3cholamidopropyl) dimethylammonio)-1-propanesulfonate (CHAPS, 2% w/v) and tributylphosphine (TnBP, 2 mM) in Tris·HCl buffer (40 mM, pH 7.8) for 24 h (37 °C, 110 rpm), followed by M4 solution prepared by dissolving CHAPS (2% w/v), amidosulfobetaine-14 (1% w/v), sulfobetaine 3−10 (2% w/v) and TnBP (2 mM) in Tris·HCl buffer (40 mM, pH 7.8) for another 24 h. After thorough rinsing with phosphate buffer saline (PBS), the valves were then treated with Benzonase® Nuclease (100 unit/mL), MgCl2 (1 mM) and NaCl (1 mM) in Tris·HCl buffer (40 mM, pH 7.8). Ultimately, DHVs were obtained and stored at 4 °C in a PBS solution with 1% penicillin-streptomycin.
Preparation of T-DHV
TCDI stock solution (0.36 g/mL) was prepared in DMF. Proper amount of the TCDI stock solutions were added to ultrapure water to achieve final concentration of 4.5 mg/mL, 9 mg/mL, 18 mg/mL, and 36 mg/mL respectively. Thereafter, the crosslinking reaction was performed by immersing DHV in these solutions at 37 °C for 24 hr.
Exploration of H2S release mechanism of diethyl thiourea (DETU)
DETU (16 mM), cysteine (16 mM) and NaOH (1 M) stock solutions were prepared in deuterated water (D2O). Then, 0.5 mL of DETU and cysteine stock solutions were mixed with 1 μl NaOH solution, and nuclear magnetic resonance spectrometry (1H NMR; AscendTM 600 MHz, Bruker, Switzerland) was performed immediately. The reaction mixture was then placed in a 37 °C water bath and heated for 2 d. Thereafter, the reaction intermediates and products were analyzed by 1H NMR and high resolution liquid chromatography-ion trap mass spectrometry (LC-MS; Orbitrap LC/MS, Thermo Fisher, Germany).
Free amino and hydroxyl content test
Free amino and hydroxyl content of all samples were evaluated by ninhydrin test and dansyl chloride test respectively as previously reported27. The samples were rinsed with deionized water and punched into 0.5 cm*0.5 cm square. Thereafter, for amino content test, ninhydrin (40 mg/mL) stock solution was prepared in 2-ethoxyethanol. The sodium citrate stock solution (20 mM) was prepared in deionized water with 1.6 mg/mL stannous chloride, which was further adjusted to pH = 5 with 10 M NaOH solution. And then, 1 ml ninhydrin working solution was prepared by mixing 0.5 ml ninhydrin with sodium citrate stock solution, which was added to each sample. The samples were incubated at 100 °C for 20 min and then cooled to room temperature. 250 μl 50% (w/v) isopropanol aqueous solution was added to each sample to terminate the reaction. The absorbance (A) of the supernatant at 570 nm was measured by a microplate reader and the background was corrected by blank ninhydrin working solution. After the test, the samples were rinsed by ultrasonic cleaning with deionized water and freeze-dried to constant weight (W). The relative free amine content was calculated as follows.
Where Asample and ADHV represent the absorbance of samples treated with different concentration of TCDI and the untreated DHV respectively, and Wsample and WDHV represent the dry weight of TCDI crosslinked samples and original DHV respectively.
For hydroxyl content test68,69, the samples were immersed in 1 mL dansyl chloride working solution (2 mg/mL dansyl chloride and 1.17 mg/mL diisopropylethylamine in diethylether) for 3 h. To remove free dansyl chloride, the samples were washed with ethanol three times (changing every hour), and left overnight for the fourth time. Finally, the fluorescence intensity (F) of the samples was analyzed with a fluorescence spectrophotometer (Ex=350 nm, Em=467 nm). After the test, the samples were rinsed by ultrasonic cleaning with deionized water and freeze-dried to constant weight (W) as mentioned above. The relative free hydroxyl content on the valve surface is calculated by the following formula:
Where, Fsample represents the fluorescence intensity of the samples treated with different concentrations of TCDI. FDHV indicates the fluorescence intensity of DHV.
Preparation of PEG-DHV and PEG/PSBMA-DHV
The DHV was immersed in the 1st reaction solution (10 wt.% 4-arm-PEG-NH2 and 8 wt.% TCDI) for 30 minutes in ice bath to rinse the DHV uniformly before reaction. Then, this solution was plated in water bath under 37 °C for 24 h to obtain the PEG-DHV. The PEG-DHV was further immersed in the 2nd reaction solution (60 wt.% SBMA, 0.3 wt.% AIBA and 0.015 wt.% MBA), and further reacted at 37 °C with stirring to obtain the PEG/PSBMA-DHV. To remove the free reactants, PEG-DHV and PEG/PSBMA-DHV were washed with sterile water three times (changing every day) and eventually immersed in sterile water for storage at 4 °C.
Mechanical test
The tensile tests were performed on a universal tester (Instron, USA) equipped with a 50 N load cell at 18 mm/min speed. For tensile test27, samples were cut into long strip with a gauge length of 10 mm, width of 5 mm, and sandpaper was placed at both ends of the sample to prevent slipping. The samples were stretched until rupture, which occurred between the upper and lower fixtures. The ultimate tensile strength was measured, and the Young’s modulus was determined by the slope of the initial region (0–5%) in the stress-strain curves. For cyclic loading-unloading tensile tests70,71, the tensile rate was set at 18 mm/min and the strain was set at 10%. After 500 cycles, the DHV, GV, T-DHV, PEG-DHV and PEG/PSBMA-DHV were used for subsequent in vitro calcification tests, and anti-protein adhesion tests. As for the PSBMA hydrogel and PEG/PSBMA hydrogel, the fatigue test was carried out with 100 % strain at a rate of 18 mm/min and then unloaded to the strain of 0 % at the same rate for 20 cycles. The energy dissipation could be obtained by calculating the area of the hysteresis loop, which was denoted as S. And the self-recovery rate was calculated as follows.
Where St and S1 represent the energy dissipation of the tnd cycle stretching and the first cycle stretching of the sample, respectively.
In vitro calcification experiment
Calcification experiment in vitro was performed as previously reported with little modifications72,73. DHV, GV, T-DHV, PEG-DHV, and PEG/PSBMA-DHV were rinsed by CaCl2 buffer (2.0 mM CaCl2, pH 7.5) and immersed in the same buffer under 37 °C for 24 h in incubator at 300 rpm. Next, Na2HPO4 buffer (2.0 mM Na2HPO4, pH 7.5) was added slowly to the solution in the tube, while pH was kept at 7.5 by dropwise addition of 0.01 M NaOH solution. The concentration of final Ca2+ was kept at 1.0 mM. The samples were then shaken at 300 rpm in incubator under 37 °C for 24 h. Finally, all the samples were rinsed 5 times with ultrapure water, and freeze-dried for further characterization.
The calcium deposition was further observed by SEM (GeminiSEM300, Carl Zeiss, Germany). For calcium quantification, fresh samples were freeze-dried and weighed, and the calcium was then dissolved by 0.2 M HCl at 60 °C. The calcium concentration was measured by atomic absorption spectroscopy (AAS; Thermo Fisher Scientific, USA).
Protein adhesion test
Protein adhesion test in vitro was performed as previously reported with little modifications73. Samples (25 mm2) were immersed in 500 μl of 0.5 mg/mL BSA solution at 37 °C for 12 h. Then, the remaining BSA concentration in the solution was measured by bicinchoninic acid (BCA) assay.
For visualization, the samples were incubated with 4 mg/mL BSA-TXO (a fluorescence labeled protein prepared according to literature74) at 37 °C overnight. After rinsed with PBS three times, the samples were observed using a confocal microscopy (CLSM; FV3000, Olympus, Janpan).
Collagenase degradation test
Collagenase degradation test in vitro was performed as previously reported with little modifications27. The samples were punched into 1 cm×1 cm square and rinsed with deionized water thoroughly, then the samples were freeze-dried and weighed (W0). Each sample was placed into 1 ml PBS buffer (pH = 7.4) containing collagenase (125 unit/mL) respectively and incubated at 37 °C for 1 d, 4 d, and 7 d. The resulted samples were rinsed with deionized water for three times, then freeze-dried to a constant weight and weighed again (Wt). The weight loss ratio of the samples was calculated according to the following formula.
In Vitro Hemocompatibility of the DHVs
The whole blood was collected from Sprague-Dawley (SD) rat and citrated with acid citrate dextrose solution immediately.
Platelet adhesion assay2. The citrated blood was rested for 10 min and then centrifuged at 590 × g for 20 min to obtain platelet-rich plasma (PRP). The samples were cut into round pieces with a diameter of 8 mm from the thickest central area of the valve belly, and incubated with PRP (1 × 108 /mL, 0.5 mL) at 37 °C for 1 h. Then the samples were collected and rinsed by PBS for later use. Platelets adhered to the samples were visualized by SEM (GeminiSEM300, Carl Zeiss, Germany). The samples were further incubated with Triton X-100 (0.5 wt.%, 1 mL) to lyse adhered platelets, and the supernatant were collected by centrifuging at 590 × g for 15 min. LDH assay (Beyotime, China) was used to quantify the number of adhered platelets on the samples in accordance with the instructions.
Thrombogenesis assay2. The DHV samples were incubated with citrated whole blood (0.5 ml) reconstituted by CaCl2 (100 mM) and MgCl2 (75 mM) mix solution (70 µL for 1 mL citrated blood) at 37 °C for 30 min, washed by PBS and photographed. Subsequently, Triton X-100 (0.5 wt.%, 1 mL) were used to perforate red blood cells (RBCs) membrane and the supernatant was measured at 540 nm to quantify formed thrombus.
Hemolysis assay2. Citrated blood was diluted 10 times by normal saline and RBCs were washed by centrifuging at 1520 x g for 10 min until the supernatant was transparent. RBCs (200 µL) was added into normal saline (1 mL) and incubated with DHV samples for 1 h at 37 °C. Normal saline and distilled water were used as negative and positive control respectively. The supernatant was collected and the absorbance was measured at 540 nm. Hemolysis rate was calculated as:
Cell culture
Human cord blood endothelial cell line cell line (HUVEC, Cell Culture Center of the Chinese Academy of Medical Sciences, Shanghai, China) was cultured in Roswell Park Memorial Institute (RPMI) 1640 medium with 10% fetal bovine serum (Gibco, USA), 100 unit/mL penicillin and 100 μg/mL streptomycin (Biosharp, China) at 37 °C in a humidified incubator containing 5% CO2. Besides, Dulbecco’s Modified Eagle Medium (DMEM, high glucose, Hyclone, USA), which contains 10% fetal bovine serum, 100 unit/mL penicillin and 100 μg/mL streptomycin was used to culture the Rat bone marrow mesenchymal stem cells (BMSCs, Sanop, Wuhan, Hubei, China) and RAW264.7 cell line (Cell Culture Center of the Chinese Academy of Medical Sciences, Shanghai, China) at 37 °C in a humidified incubator containing 5% CO2.
Cytotoxicity test
The cytotoxicity of DHVs was evaluated by co-incubation method75,76,77. The DHV samples were punched into 0.5 cm2 square, sterilized with 0.25% (v/v) peracetic acid (PAA) solution at room temperature for 3 h, followed by thorough rinsing with sterile PBS solution. HUVECs and BMSCs were cultured in 96-well plates at the density of 10,000 cells/well overnight. Then the samples were added into the 96-well plates to co-incubate for 48 h. Cell viability was determined by an MTT (Beyotime, China) method according to the supplier’s instructions, and calcein AM (Beyotime, China) was used to observe cell morphology and viability under a confocal microscope (Olympus, Japan).
Detection of macrophage phenotype
Raw264.7 macrophages were cultured in 12-well plates overnight. The DHV samples were treated similar as for cytotoxicity assay and subsequently added to the macrophages to co-culture for 48 h. M2-polarized macrophages were labeled with FITC-anti-mouse CD206 (Abcam, UK, Lot number: B381906) according to the supplier’s instructions, and the proportion of M2-phenotype macrophage polarization was detected by flow cytometry (CytoFLEX, BD Biosciences, Oxford, UK). Cell-secreted factors (TGF-β1) associated with M2 macrophages were detected using the TGF-β1 ELISA kit according to the supplier’s instructions. The mRNA expression of IL-10 and Arg 1 was detected by RT-qPCR. The sequence of primers was listed in Supplementary Table 2. The gating strategy of flow cytometry was shown in Supplementary Fig. 9.
In vivo degradation and tissue remodeling test by rat subdermal implantation model
Animal experiments were approved by the Institutional Animal Care and Use Committee of Huazhong University of Science and Technology (IACUC Number 3649). The experimental animals were provided by Hubei Bainte Biotechnology Co., LTD. Rat subdermal implantation model was established to evaluate in vivo histocompatibility of the DHVs as previously reported2. All samples were cut into 1 cm2 and were sterilized with 0.25% (v/v) peracetic acid (PAA) solution. SD rats (male, 180–200 g) were anesthetized by intraperitoneal injection with 0.01–0.02 mL/g of 0.3% pentobarbital sodium. Five samples were fixed on the back of each rat as shown in Fig. 7A.
Samples were removed and characterized by HE, Masson, EVG, and Von Kossa staining to show ECM change and calcification at day 7, 14 and 28. Collagen percentage (D) of heart valve section area in Masson staining was used to reflect the degradation rate of sample. The relative degradation rate was calculated as:
The immunomodulatory ability of the samples in vivo was further evaluated, and CD163/iNOS/DAPI staining was performed on sections at each time to detect the phenotype of macrophages. To further calculate the proportion of M2 phenotypic macrophages, we randomly select 6 fields of view for each slice at a 200x magnification. Then, we counted the number of cells (N0) according to DAPI fluorescence staining and the number of M2 phenotype macrophages (N1) according to CD163 fluorescence staining. The phenotype proportion of M2 macrophages was calculated by the following formula78,79:
In vivo endothelialization evaluated by rat abdominal aorta implantation model
A rat abdominal aorta implantation model was established to evaluate the performance of the DHVs under the hemodynamic environment as previously reported2. Details of operation procedures has been shown in Fig. 8A. In brief, the sample was cut into 4 × 5 mm2 pieces and sewed into tubes with an 8–0 surgical suture needle (Lingqiao, China) (the ventricular layer was used as the inner wall of the tube). And then, SD rats (male, 180–200 g) were anesthetized by intraperitoneal injection with 0.01–0.02 mL/g of 0.3% pentobarbital sodium. The tubes were transplanted into the rat’s abdominal aorta as shown in Fig. 8A. After 4 weeks, all rats were checked by Doppler ultrasound and then the samples were subjected to HE, Masson and Von Kossa staining to show ECM structure and calcification. Macrophage marker (iNOS, and CD163), ECs marker (CD31), interstitial cells marker (vimentin), and collagen type I was stained to evaluate inflammation, cellularization and remodeling of the implanted DHVs respectively. To evaluate endothelialization, immunofluorescence staining of CD31 and DAPI was also performed at day 7 and 14.
Statistics and reproducibility
Statistical analysis was performed using GraphPad Prism 8.0. Each experiment was repeated independently at least three times and with similar results. All measurements were expressed as mean ± SD, the differences were considered significant at P < 0.05 (**P < 0.01, ***P < 0.001, ****P < 0.0001). T-test was used for comparison between the two groups, and one-way ANOVA was used for comparison more than two groups. The correlation was analyzed using a Pearson correlation test.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
All data are presented in the main text and the supplementary files. Source data are provided with this paper.
References
Coffey, S. et al. Global epidemiology of valvular heart disease. Nat. Rev. Cardiol. 18, 853–864 (2021).
Zhou, Y. et al. Nitric oxide generation and endothelial progenitor cells recruitment for improving hemocompatibility and accelerating endothelialization of tissue engineering heart valve. Adv. Funct. Mater. 33, 2211267 (2022).
Lisy, M. et al. Allograft heart valves: current aspects and future applications. Biopreserv. Biobank. 15, 148–157 (2017).
Dai, J. et al. Modifying decellularized aortic valve scaffolds with stromal cell-derived factor-1α loaded proteolytically degradable hydrogel for recellularization and remodeling. Acta Biomater. 88, 280–292 (2019).
Li, B. et al. Comprehensive analyses and prioritization of various swim bladder-derived extracellular matrix in the application of heart valve prosthesis. Smart Mater. Med. 2, 209–218 (2021).
Sun, Z. et al. Epoxy chitosan-crosslinked acellular bovine pericardium with improved anti-calcification and biological properties. ACS Appl. Bio Mater. 3, 2275–2283 (2020).
Cheng, S. et al. Double‐network hydrogel armored decellularized porcine pericardium as durable bioprosthetic heart valves. Adv. Healthc. Mater. 11, 2102059 (2022).
Fioretta, E. S. et al. Next-generation tissue-engineered heart valves with repair, remodelling and regeneration capacity. Nat. Rev. Cardiol. 18, 92–116 (2020).
Chen, J. et al. H2S-releasing versatile hydrogel dressing with potent antimicrobial, anti-inflammatory, epithelialization and angiogenic capabilities for diabetic wound healing. Chem. Eng. J. 469, 143985 (2023).
Kim, A. J., Xu, N. & Yutzey, K. E. Macrophage lineages in heart valve development and disease. Cardiovasc. Res. 117, 663–673 (2021).
Hénaut et al. New insights into the roles of monocytes/macrophages in cardiovascular calcification associated with chronic kidney disease. Toxins 11, 529 (2019).
Yaker, L. et al. Extracellular vesicles from lps-treated macrophages aggravate smooth muscle cell calcification by propagating inflammation and oxidative stress. Front. Cell Dev. Biol. 10, 823450 (2022).
Turner, M. E., Bartoli‐Leonard, F. & Aikawa, E. Small particles with large impact: Insights into the unresolved roles of innate immunity in extracellular vesicle‐mediated cardiovascular calcification. Immunol. Rev. 312, 20–37 (2022).
Labarrere, C. A., Dabiri, A. E. & Kassab, G. S. Thrombogenic and inflammatory reactions to biomaterials in medical devices. Front. Bioeng. Biotechnol. 8, 123 (2020).
Aksu, K., Donmez, A. & Keser, G. Inflammation-induced thrombosis: management. Curr. Pharm. Des. 18, 1478–1493 (2012).
Chen, J.-H., Simmons, C. A. & Towler, D. A. Cell–matrix interactions in the pathobiology of calcific aortic valve disease. Circ. Res. 108, 1510–1524 (2011).
Ben-Dor, I. et al. Correlates and causes of death in patients with severe symptomatic aortic stenosis who are not eligible to participate in a clinical trial of transcatheter aortic valve implantation. Circulation 122, 38–42 (2010).
Chester, A. H. & Grande-Allen, K. J. Which biological properties of heart valves are relevant to tissue engineering? Front Cardiovasc Med. 7, 63 (2020).
Lei, Y., Guo, G., Jin, W., Liu, M. & Wang, Y. Riboflavin photo‐cross‐linking method for improving elastin stability and reducing calcification in bioprosthetic heart valves. Xenotransplantation 26, e12481 (2019).
Jin, L., Guo, G., Jin, W., Lei, Y. & Wang, Y. Cross-linking methacrylated porcine pericardium by radical polymerization confers enhanced extracellular matrix stability, reduced calcification, and mitigated immune response to bioprosthetic heart valves. ACS Biomater. Sci. Eng. 5, 1822–1832 (2019).
Hersel, U., Dahmen, C. & Kessler, H. RGD modified polymers: biomaterials for stimulated cell adhesion and beyond. Biomaterials 24, 4385–4415 (2003).
Tang, J.-M. et al. VEGF/SDF-1 promotes cardiac stem cell mobilization and myocardial repair in the infarcted heart. Cardiovasc. Res. 91, 402–411 (2011).
Marinval, N. et al. Fucoidan/VEGF-based surface modification of decellularized pulmonary heart valve improves the antithrombotic and re-endothelialization potential of bioprostheses. Biomaterials 172, 14–29 (2018).
Lei, Y. et al. Hybrid pericardium with vegf‐loaded hyaluronic acid hydrogel coating to improve the biological properties of bioprosthetic heart valves. Macromol. Biosci. 19, 1800390 (2019).
Naito, H., Iba, T. & Takakura, N. Mechanisms of new blood-vessel formation and proliferative heterogeneity of endothelial cells. Int. Immunol. 32, 295–305 (2020).
Fang, J. et al. Orthogonally functionalizable polyurethane with subsequent modification with heparin and endothelium-inducing peptide aiming for vascular reconstruction. ACS Appl. Mater. Interfaces 8, 14442–14452 (2016).
Yang, F. et al. Polyzwitterion-crosslinked hybrid tissue with antithrombogenicity, endothelialization, anticalcification properties. Chem. Eng. J. 410, 128244 (2021).
Wang, Z. et al. Mechanically enhanced nested-network hydrogels as a coating material for biomedical devices. Acta Biomater. 70, 98–109 (2018).
Liang, X., Hu, C. & Wang, Y. Biomimetic-modified bioprosthetic heart valves with controlled release of glycyrrhizin acid mediated by the inflammatory microenvironment for anti-thrombotic, anti-inflammatory, and anti-calcification. Chem. Eng. J. 472, 128244 (2023).
Sun, F. et al. The role of hydrogen sulphide signalling in macrophage activation. Immunology 162, 3–10 (2020).
Coletta, C. et al. Hydrogen sulfide and nitric oxide are mutually dependent in the regulation of angiogenesis and endothelium-dependent vasorelaxation. P NATL A SCI INDIA B 109, 9161–9166 (2012).
Lin, W.-C. et al. In situ depot comprising phase-change materials that can sustainably release a gasotransmitter H2S to treat diabetic wounds. Biomaterials 145, 1–8 (2017).
Tseng, H. et al. Anisotropic poly(ethylene glycol)/polycaprolactone hydrogel–fiber composites for heart valve tissue engineering. Tissue Eng. Part A. 20, 2634–2645 (2014).
Bai, T. et al. Zwitterionic fusion in hydrogels and spontaneous and time-independent self-healing under physiological conditions. Biomaterials 35, 3926–3933 (2014).
Ooi, T., Kameda, M., Taniguchi, M. & Maruoka, K. Development of highly diastereo- and enantioselective direct asymmetric aldol reaction of a glycinate schiff base with aldehydes catalyzed by chiral quaternary ammonium salts. J. Am. Chem. Soc. 126, 9468–9874 (2004).
Wu, Wen-Lian et al. Dopamine D1/D5 receptor antagonists with improved pharmacokinetics: design, synthesis, and biological evaluation of phenol bioisosteric analogues of benzazepine D1/D5 antagonists. J. Med. Chem. 48, 680–693 (2005).
White, J. D., Wang, G. & Quaranta, L. Studies on the synthesis of gymnodimine. stereocontrolled construction of the tetrahydrofuran subunit. Org. Lett. 5, 4109–4112 (2003).
Munro, T. A., Rizzacasa, M. A., Roth, B. L., Toth, B. A. & Yan, F. Studies toward the pharmacophore of salvinorin A, a potent K opioid receptor agonist. J. Med. Chem. 2, 345–348 (2005).
Toyo’oka, T. Recent advances in separation and detection methods for thiol compounds in biological samples. J. CHROMATOGR B 877, 3318–3330 (2009).
Nudelman, A., Marcovici-Mizrahi, D., Nudelman, A., Flint, D. & Wittenbach, V. Inhibitors of biotin biosynthesis as potential herbicides. Tetrahedron 60, 1731–1748 (2004).
Song, Z. L. et al. Progress and perspective on hydrogen sulfide donors and their biomedical applications. Med. Res. Rev. 42, 1930–1977 (2022).
Zaorska, E. et al. Evaluation of thioamides, thiolactams and thioureas as hydrogen sulfide (H2S) donors for lowering blood pressure. Bioorg. Chem. 88, 102941 (2019).
Cerda, M. M., Zhao, Y. & Pluth, M. D. Thionoesters: a native chemical ligation-inspired approach to cysteine-triggered H2S donors. J. Am. Chem. Soc. 140, 12574–12579 (2018).
Namiri, M. et al. Engineering natural heart valves: possibilities and challenges. J. Tissue Eng. Regen. Med. 11, 1675–1683 (2017).
Bejleri, D. & Davis, M. E. Decellularized extracellular matrix materials for cardiac repair and regeneration. Adv. Healthc. Mater. 8, 1801217 (2019).
Zhao, Y., Henthorn, H. A. & Pluth, M. D. Kinetic insights into hydrogen sulfide delivery from caged-carbonyl sulfide isomeric donor platforms. J. Am. Chem. Soc. 139, 16365–16376 (2017).
Guo, H. et al. The hydrolysis mechanism and kinetic analysis for COS hydrolysis: a DFT study. Russ. J. Phys. Chem. B. 10, 427–434 (2016).
Ground, M., Waqanivavalagi, S., Walker, R., Milsom, P. & Cornish, J. Models of immunogenicity in preclinical assessment of tissue engineered heart valves. Acta Biomater. 133, 102–113 (2021).
Badria, A. F., Koutsoukos, P. G. & Mavrilas, D. Decellularized tissue-engineered heart valves calcification: what do animal and clinical studies tell us? J. MATER SCI-MATER M 31, 1–21 (2020).
VeDepo, M., Buse, E., Paul, A., Hopkins, R. & Converse, G. Comparison of candidate cell populations for the recellularization of decellularized heart valves. Cell. Mol. Bioeng. 11, 197–209 (2018).
Cai, C. et al. Self‐healing hydrogel embodied with macrophage‐regulation and responsive‐gene‐silencing properties for synergistic prevention of peritendinous adhesion. Adv. Mater. 34, 2106564 (2021).
Zheng, S. Y. et al. Molecularly engineered zwitterionic hydrogels with high toughness and self-healing capacity for soft electronics applications. Chem. Mater. 33, 8418–8429 (2021).
Demer, L. L. & Tintut, Y. Heart valve calcification. In: Principles of Heart Valve Engineering (Academic Press, 2019).
Manivasagam, V. K., Sabino, R. M., Kantam, P. & Popat, K. C. Surface modification strategies to improve titanium hemocompatibility: a comprehensive review. Mater. Adv. 2, 5824–5842 (2021).
Zagli, G. et al. Hydrogen sulfide inhibits human platelet aggregation. Eur. J. Pharmacol. 559, 65–68 (2007).
Yu, W. P. et al. Titanium dioxide nanotubes promote M2 polarization by inhibiting macrophage glycolysis and ultimately accelerate endothelialization. Immun., Inflamm. Dis. 9, 746–757 (2021).
Raddatz, M. A. et al. Macrophages promote aortic valve cell calcification and alter STAT3 splicing. Arterioscler., Thromb., Vasc. Biol. 40, 153–165 (2020).
Nasser, M. I. et al. Macrophages: first guards in the prevention of cardiovascular diseases. Life Sci. 250, 117559 (2020).
Grim, J. C. et al. Secreted factors from proinflammatory macrophages promote an osteoblast-like phenotype in valvular interstitial cells. Arterioscler., Thromb., Vasc. Biol. 40, 296–308 (2020).
Naito, Y., Takagi, T. & Higashimura, Y. Heme oxygenase-1 and anti-inflammatory M2 macrophages. Arch. Biochem. Biophys. 564, 83–88 (2014).
Zhao, Y. et al. Regulation of endothelial functionality through direct and immunomodulatory effects by Ni-Ti-O nanospindles on NiTi alloy. Mat. Sci. Eng. C.-MATER 123, 112007 (2021).
Chen, X. et al. Dental follicle stem cells ameliorate lipopolysaccharide-induced inflammation by secreting TGF-β3 and TSP-1 to elicit macrophage M2 polarization. Cell. Physiol. Biochem. 51, 2290–2308 (2018).
Luo, Y., Huang, S. & Ma, L. A novel detergent-based decellularization combined with carbodiimide crosslinking for improving anti-calcification of bioprosthetic heart valve. Biomed. Mater. 16, 045022 (2021).
Lim, H. G., Kim, S. H., Choi, S. Y. & Kim, Y. J. Anticalcification effects of decellularization, solvent, and detoxification treatment for genipin and glutaraldehyde fixation of bovine pericardium. EUR J. CARDIO-THORAC 41, 383–390 (2011).
Wang, X., Ma, B. & Chang, J. Preparation of decellularized vascular matrix by co-crosslinking of procyanidins and glutaraldehyde. Bio-Med. Mater. Eng. 26, 19–30 (2015).
Liu, J. et al. Curcumin-crosslinked acellular bovine pericardium for the application of calcification inhibition heart valves. Biomed. Mater. 15, 045002 (2020).
Song, C. et al. Generation of individualized immunocompatible endothelial cells from HLA-I-matched human pluripotent stem cells. Stem Cell Res. Ther. 13, 2211267 (2022).
Ivanov, V. B., Behnisch, J., Holländer, A., Mehdorn, F. & Zimmermann, H. Determination of functional groups on polymer surfaces using fluorescence labelling. Surf. Interface Anal. 24, 257–262 (1996).
Seifert, B. et al. Polyetherimide: a new membrane‐forming polymer for biomedical applications. Artif. Organs 26, 189–199 (2008).
Lu, Y. et al. Self-Recovery, fatigue-resistant, and multifunctional sensor assembled by a nanocellulose/carbon nanotube nanocomplex-mediated hydrogel. ACS Appl. Mater. Interfaces 13, 50281–50297 (2021).
Zhang, M. et al. Toughening double‐network hydrogels by polyelectrolytes. Adv. Mater. 35, 2301551 (2023).
Liu, X. et al. DNA framework-encoded mineralization of calcium phosphate. Chem 6, 472–485 (2020).
Guo, F. et al. Artificial heart valves with balanced charged networks exhibiting anti-calcification properties. ACS Appl. Bio Mater. 3, 838–847 (2019).
Fu, Y. et al. A recyclable supramolecular photocatalyst for the chemoselective [2 + 2] photocycloaddition of chalcones in water. ACS Sustain. Chem. Eng. 11, 17752–17759 (2023).
Wu, C. et al. Double-crosslinked nanocomposite hydrogels for temporal control of drug dosing in combination therapy. Acta Biomater. 106, 278–288 (2020).
Yu, J. et al. In situ covalently cross-linked PEG hydrogel for ocular drug delivery applications. Int. J. Pharm. 470, 151–157 (2014).
Shen, S. et al. Copper-induced injectable hydrogel with nitric oxide for enhanced immunotherapy by amplifying immunogenic cell death and regulating cancer associated fibroblasts. Biomater. Res. 27, 1–22 (2023).
Yuan, A. et al. Opposite effects of M1 and M2 macrophage subtypes on lung cancer progression. Sci. Rep. 5, 1–12 (2015).
Yu, T. et al. Enhanced activity of the macrophage M1/M2 phenotypes and phenotypic switch to M1 in periodontal infection. J. Periodontol. 87, 1092–1102 (2016).
Acknowledgements
We thank the National Natural Science Foundation of China (No. 81930052, 82270381) for financial support. We thank the Analytical and Testing Center of HUST, Analytical and Testing Centre of School of Chemistry and Chemical Engineering (HUST), and Research Core Facilities for Life Science (HUST) for instrument support.
Author information
Authors and Affiliations
Contributions
Y.W. conceived and supervised the project. J.L. performed the experiments and interpreted the data. W.Q. assisted with the experiments and revised the the article. Y.L., H.L., and Z.Y. assisted the animal experiment. S.W. and Y.X. assisted the cell experiment. Y.Z., S.W., and W.W. assisted the blood compatibility experiment. J.S. and N.D. supervised the design of animal experiments. Y. W. supervised the design of materials and wrote the manuscript with input from all of the authors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Ali Akpek, David Centurion, and Arn Mignon for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Li, J., Qiao, W., Liu, Y. et al. Facile engineering of interactive double network hydrogels for heart valve regeneration. Nat Commun 15, 7462 (2024). https://doi.org/10.1038/s41467-024-51773-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-024-51773-0
This article is cited by
-
Synthetic strategies for the preparation of hydrogels using star-shaped polymers
Polymer Bulletin (2025)