Abstract
Coronary artery disease poses a significant public health threat, and coronary computed tomography angiography is the preferred imaging modality for diagnosis and risk assessment of coronary artery disease through plaque evaluation. However, understandings of how atherosclerotic characteristics vary by age and sex remains limited due to challenges in manual quantitative plaque assessment. Here, we conducted a retrospective, consecutive, multi-center Chinese cohort study of 16,300 patients undergoing clinically indicated coronary computed tomography angiography that revealed multi-level quantitative patterns of atherosclerosis stratified by age and sex. We found that females experienced a delayed atherosclerosis onset by approximately 20 years compared to males, with plaque burden increasing nonlinearly with age and accelerating more evidently after menopause. The built coronary atlas identified plaque clusters, primarily within proximal segments of major coronary arteries, slightly upstream side branch bifurcations. Our findings provide deeper insights into coronary atherosclerosis in the Chinese population, supporting more tailored prevention strategies.
Similar content being viewed by others
Introduction
Coronary artery disease (CAD), as a leading cause of ischemic heart disease, represents a significant public health threat and imposes considerable challenges on healthcare systems, particularly in developing countries1. The prevalence of CAD in China in 2020 was 10.2‰, with a mortality rate of 131.395 per 100,000, and it is expected to continue rising2. It is known that major adverse cardiovascular events (MACE), such as sudden cardiac death and acute myocardial infarction, are often associated with the rupture of atherosclerotic plaques, which are typically characterized by a high plaque burden and unfavorable characteristics like thin-cap fibroatheroma3,4,5,6. In accordance with current guidelines, coronary computed tomography angiography (CCTA) has established itself as the preferred diagnostic modality for evaluating suspected CAD, facilitating risk stratification through detailed characterization and quantification of atherosclerotic plaques7,8,9,10,11.
Population strategy has demonstrated general efficacy in preventing CAD and reducing associated mortality12,13. However, disparities in risk awareness, clinical manifestation and treatment response still exist across sex14,15,16,17,18, age19,20,21, and geographic regions22, which are influenced by complex sociodemographic factors. For example, men exhibit a higher incidence and severity of CAD than women across all age groups, attributed to the elevated cardiovascular risk factors and influence of sex hormones23. On the other hand, women are reported to experience longer patient and system delays, resulting in worse clinical outcomes compared to men following acute coronary syndrome24. This disparity is related to the absence of sex-specific thresholds in clinical guidelines and lower awareness for CAD risk in women, with this underestimation potentially more pronounced among older females25.
These studies indicated the underlying differences in the pathophysiology of CAD among diverse population groups, underscoring the need for ongoing research in this area. A few recent investigations utilized CCTA to characterize the profile of coronary atherosclerotic plaques across a broad population. In a study by Bergström et al.26, researchers examined the prevalence and severity of coronary atherosclerosis and its correlation with coronary artery calcification scores (CACS) in a general Swedish population without established disease. Meanwhile, Tzimas et al.27 developed age- and sex-specific nomograms for atherosclerotic plaque measures from a large North American cohort undergoing clinically indicated CCTA. These studies provide invaluable insights into the range of atherosclerotic plaque phenotypes across diverse population groups; however, they either rely on manual interpretation of CCTA images, which lacks quantitative assessments26, or focus solely on measuring plaque volume and stenosis severity with the analysis of plaque distribution constrained to the main branch level27. In the last decade, artificial intelligence (AI)-powered technologies have advanced rapidly in the field of cardiovascular imaging, demonstrating successful applications in enhancing the accuracy and efficiency of atherosclerotic plaque assess- ment while reducing inter-observer variability in CCTA imaging28. Deep learning-based methods are widely applied to solve various problems, including coronary tree extraction29,30,31,32,33, plaque detection and segmentation32,34,35,36,37,38,39, stenosis severity assessment32,34,38,40, and high-risk plaque characterization35,37,41.
In this study, we sought to employ an automated plaque analysis system using machine-learning algorithms (PLASMA) to perform all the aforementioned functions of plaque quantification and characterization. With this system, we conducted a comprehensive analysis of the atherosclerotic plaque phenotypes across different age- and sex-specific population groups in a large Chinese cohort comprising 16,300 subjects, as depicted in Fig. 1a. Furthermore, we built an average shape model of coronary artery centerlines from this cohort and mapped each subject’s plaques onto this model, resulting in a three-dimensional (3D) coronary atlas with a statistical representation of plaque distribution along the centerlines. Unlike previous studies26,27 that were confined to the main and side branches, our approach provides a continuous point-level statistical analysis of plaques along the coronary centerlines, capturing plaque characteristics with greater spatial precision. Our findings illuminate the substantial impact of age and sex on plaque characteristics within clinical populations, while also addressing potential regional and ethnic disparities in plaque progression. These insights offer important knowledge for enhancing prevention strategies and optimizing the precision of CAD diagnosis and treatment.
a Study approach. A large multi-center CCTA dataset was collected as input to the PLASMA for extracting coronary artery- and plaque-related information. Then, characteristics that are significant for clinical diagnosis were calculated, and the plaque distribution atlas was built, based on system outputs. Finally, we conducted analysis at the per-subject and per-segment level, and in the continuous space stratified by age and sex. b Demographic distribution of the study cohort. The multi-layered donut chart illustrates characteristics of the cohort (N = 16,300), stratified by sex (innermost), age (middle), and geographic (outermost) region. c PLASMA-based plaque characterization. Anatomical structures and lesion information were automatically extracted by PLASMA and used to calculate plaque characteristics, including position, burden, and morphology. d Main results and clinical applications.
Results
Population
A total of 20,089 patients who underwent clinically indicated CCTA between June 2023 and August 2023 were initially enrolled from 42 medical centers across China. After excluding 1674 patients with a history of percutaneous coronary intervention (PCI) or coronary artery bypass grafting (CABG), 1237 patients due to insufficient image quality, 812 patients for missing age and sex demographic data, and 66 patients under the age of 25, a final cohort of 16,300 individuals was included in the study for analysis, as shown in Fig. 2a. CCTA images were acquired using CT scanners from a variety of manufacturers, including GE Healthcare, Siemens, Philips, Toshiba, and United Imaging, as detailed in Fig. 2b. The mean age of the included 16,300 individuals was 61.49 ± 11.68 years, with 6780 (41.6%) being women. Figure 1b illustrates the distribution of males and females across various age groups, as well as the geographic distribution of the total population. The cohort included participants from seven major geographical regions in China, with sample sizes as follows: East (n = 3333), North (n = 2680), Northeast (n = 2979), Northwest (n = 1120), Southwest (n = 2100), Central (n = 2696), and South (n = 1392), as detailed in Supplementary Table 5. In addition, the cohort comprised 14,923 participants from more-developed urban areas and 1377 participants from less-developed rural areas, as summarized in Supplementary Table 4. Of 16,300 individuals, PLASMA detected atherosclerotic plaques in the CCTA images of 12,287 subjects (75.4%).
a Cohort selection workflow. Our study included 16,300 subjects from 42 centers in mainland China. b CT scanner vendor distribution in our study.
Age-related trends in plaque burden and composition
In this study, atherosclerotic plaque burden was mainly evaluated as the percentage of total plaque volume relative to the entire coronary artery volume (Methods), namely percent atheroma volume (PAV, %), to account for variations in vessel sizes across patients of different sexes and geographic regions. In addition to the total plaque, the analysis considered its four components: calcified, fibrous, fibro-fatty, and lipid, with the latter three collectively referred to as non-calcified plaques. As illustrated in Fig. 3a, total plaque burden increases with age, with the average PAV at 2.9% in patients under 45 years old rising to 10.4% in those over 75 years old. The burden of all four plaque components also increases with age, with calcified plaques showing the most rapid growth (an increase of 0.93% in average PAV per decade), followed by fibrous (0.66%), fibro-fatty (0.26%), and lipid (0.03%) components. In particular, the burdens of fibro-fatty and lipid plaques tend to stabilize in individuals over 75 years old. Analyzing the relative percentages of four components within total plaque PAV, we observed a rapid increase in the proportion of calcified plaque with advancing age, as shown in Fig. 3b. Among the non-calcified components, only fibrous plaque shows a slight increase in percentage with age, while fibro-fatty and lipid plaques exhibit a significant percentage decline.
a Plaque PAV distributions across age groups in the overall cohort (n = 16,300). (The 1st and 2nd rows) Box plots of plaque PAV distributions for individual subjects within the indicated age group, with PAV-age trajectories of mean (solid line), 10% and 90% centiles (dotted lines) estimated by cubic B-spline. Boxes show interquartile ranges (25th–75th percentiles), whiskers extend to 1.5 × IQR, solid lines mark means, and dashed lines mark medians. (The 3rd row) Rates of PAV change over the lifespan, derived from PAV-age trajectories. b Relative percentages of four components across age groups, shown in green, blue, orange and pink. c Calcified (green) and non-calcified (pink) proportion changes in the Chinese cohort compared with the North American population27, where dashed lines and square points denote the North American data.
Sex disparities in atherosclerosis onset and plaque progression
The mean total plaque burden, measured by PAV, is 6.60% ± 8.42% in our population. As expected, male individuals have a higher average PAV (8.11% ± 9.14%) compared to female individuals (4.47% ± 6.74%) (p < 0.0001). Likewise, the average burdens of all four plaque components are greater in men than in women, as shown in Supplementary Table 3. The average PAV of total plaque and its four components across different age groups are compared between men and women in Fig. 4a. Male participants consistently showed greater total plaque burden than females across all age groups. This trend also applies to total plaque growth rate, except in the age groups over 65–75, where the growth rate in females begins to surpass that of the males. Unlike men, who display an approximately linear increase in total plaque burden with an almost constant growth rate (an increase of 2.25% in average PAV per decade), women experience a nonlinear progression, with a continuously accelerating growth rate starting near zero for those under 45 rising to approximately 3.22% increase per decade for those over 75 years old. Considering the role of menopause in female CAD development42, we further applied a refined 5-year age stratification. This finer analysis revealed a notable increase in total plaque burden in women after age 45–50, with a modest 0.2% rise from <45 to 45–50, followed by a sharper 0.6% increase from 45–50 to 50–55, and sustained elevated increases thereafter. The estimated growth rate of plaque burden increased from 0.78% to 1.33% between the 45–50 and 50–55 age groups (see more details in Supplementary Fig. 2. Correspondingly, the PAV of calcified and fibrous components does not increase notably in women until after ages of 45–55, whereas these components always show accelerating or steady increases in men across all age groups, as illustrated in the second and third columns in Fig. 4a.
a Sex differences in plaque burden characteristics (n = 16,300). (The 1st row) Scatter plots and kernel density estimates of ‘raw’ plaque PAV values for total plaque, calcified, fibrous, fibro-fatty, and lipid plaques. (The 2nd row) Box plots of plaque PAV distributions by age group. Solid lines mark means, dashed lines mark medians, boxes show interquartile ranges (25th–75th percentiles), and whiskers extend to 1.5 × IQR. (The 3rd row) Mean PAV-age trajectories (solid lines) and 10% and 90% centiles (dotted lines). (The 4th row) Rates of PAV change over the lifespan, derived from PAV-age trajectories. All plots are stratified by sex (female, red; male, blue). b Sex differences in plaque morphologies. Violin plots with means for maximum stenosis ratio, eccentricity index, and remodeling index, and prevalence of obstructive stenosis and high-risk plaque, which are calculated as the number of positive subjects divided by the group size. c Disparities in atherosclerosis severity between sexes. The delayed onset of CCTA-detected atherosclerosis in women was modeled by shifting the x-axis relative to men in 1-year interval and identifying the minimum of the sum of squared differences in annualized atherosclerosis prevalence between sexes. (Left) Yearly trajectories of mean total plaque PAV (solid lines) and prevalence of obstructive stenosis (dashed lines with circular markers); (right) sum of squared differences in atherosclerosis severity between women and men across different age shifts.
In this study, four high-risk plaque features are considered: positive remodeling (PR), low attenuation plaque (LAP), napkin ring sign (NRS), and spotty calcification (SC) following the definitions in Abdelrahman et al.43. Plaques presenting two or more of these characteristics are classified as high-risk. Figure 4b shows the prevalence of individuals with high-risk plaques and obstructive stenosis (stenosis ≥50%) across different age and sex population groups. In both men and women, the prevalence of these conditions increases with age. Notably, women exhibit a nonlinear, accelerating rise in the prevalence of obstructive stenosis with age, mirroring the trend observed for plaque burden.
The observations clearly indicate that females experience a significant delay in the progression of atherosclerosis. To quantify temporal difference in CAD progression between men and women, we calculated the year gap that minimizes the sum of squared errors (MSE) between two sexes in terms of annual average PAV and prevalence of obstructive stenosis, as depicted in Fig. 4c. This analysis revealed a 20-year delay in plaque burden accumulation and an 18-year delay in the onset of obstructive stenosis in Chinese women.
Comparison of plaque burden and calcification progression between Chinese and North American populations
The quantitative plaque burden results from our research were compared with those reported previously by Tzimas et al., which involved a cohort of 11,080 patients from Canada and the United States27. Both studies were conducted on patients undergoing clinically indicated CCTA. As shown in Table 1, the average total plaque volume in the Chinese population (age: 61.5 ± 11.7 years; male: 58.4%; plaque volume: 296.2 ± 420.6 mm3) is significantly lower than that of the North American population (age: 62.7 ± 12.2 years; male: 54.1%; plaque volume: 413.5 ± 515.0 mm3), despite comparable age and sex distributions in two cohorts. Moreover, PAV, which accounts for variations in coronary artery size, is also notably lower in the Chinese population (6.6 ± 8.4%) compared to the North American population (14.0 ± 14.7%), shown in Supplementary Table 3. The atherosclerotic plaque progresses to calcification much faster in the Chinese population, with the proportion of calcified plaque increasing from 11.7% in individuals under 45 years old to 36.0% in those over 75 years old. In contrast, the North American population shows a more gradual increase in calcification, rising from 15.1% only to 24.6% over the same age range, as illustrated in Fig. 3c. Supplementary Fig. 1 shows sex-specific changes in calcified and non-calcified plaque proportions with age.
Spatiotemporal distribution and evolution of coronary artery plaque characteristics
In this study, a three-dimensional atlas of 18-segment coronary artery centerlines was built by averaging reconstructed coronary arteries across the enrolled population, following the Society of Cardiovascular Computed Tomography (SCCT) reporting guidelines44,45. Plaques identified from individual CCTA images were then mapped onto this atlas to analyze their statistical spatial distribution across different coronary segments, as illustrated in Fig. 5b. Figure 5a and Table 2 rank the 18 coronary vessel segments based on PAV, average plaque volume, prevalence of detected plaque, and the presence of plaque with obstructive stenosis detected. Overall, the plaque PAV was highest in proximal left anterior descending (pLAD), followed by middle LAD (mLAD), proximal right coronary artery (pRCA), and middle RCA (mRCA), with progressively descending order in subsequent vessel segments as shown in Fig. 5a, culminating in the posterior-lateral branch from left circumflex artery (L-PLB) with the lowest plaque PAV.
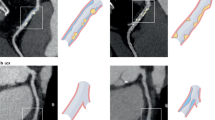
a Plaque PAV ranks among AHA-18 segments. Violin plots and lines display the distributions and means of segment-level plaque PAV values, stratified by sex (all, gray; female, red; male, blue). b Spatial distribution of plaque prevalence in the Chinese population. The probability of plaque occurrence at each location on the 3D coronary atlas is shown for all, male, and female groups. The difference map is calculated by subtracting the male probability from the female probability at each position. Segment names are labeled in gray text. For clarity, specific segments are indicated with their AHA-18 numbers: D1 (9), D2 (10), OM1 (12), OM2 (14), L-PDA (15), RAMUS (17), and L-PLB (18). Other coronary artery segments are labeled with their standard abbreviations. c Spatial distribution of plaque, high-risk plaque, and obstructive stenosis prevalence on four main branches (flatten view). Prevalence values are displayed for all (the 1st row) and different age groups (the 2nd row). The x-axis represents relative positions on the atlas segment (0–1), and the y axis represents prevalence (%), with a uniform range of 0–72 across subplots. d Spatiotemporal distribution of plaque prevalence by sex and age groups.
The coronary atlas further revealed that atherosclerotic plaques are not uniformly distributed within each vessel segment, as shown in Fig. 5b, c, and clustered regions on coronary artery segments were identified. On the LAD, plaques cluster around 10% of the vessel’s total length from its origin, showing a peak occurrence frequency of 45.58% in the total population. Notably, this location is close to, and slightly upstream of, the first diagonal branch (D1) bifurcation point of the atlas model, which occurs at 12% of the vessel’s total length. A comparable clustering pattern is seen on the left circumflex artery (LCx) at 21% of its length, with a peak frequency of 14.84%, similarly near and just proximal to the first obtuse marginal (OM1) bifurcation point at 25% of the vessel’s length. For the RCA, two clusters were identified: one at 19% of its length in the proximal segment (26.98% frequency) and another at 92% in the distal segment (16.14% frequency). Unlike the three main vessels, plaques on the side branches consistently cluster around the initial bifurcation locations from which they branch off from the main vessels.
Figure 5d presents the coronary atlas displaying the statistical spatial distribution of plaques across different age groups in men and women, providing a visual representation of how plaque develops and progresses over time. The figures indicate that plaques tend to form initially in specific, isolated locations and gradually spread more diffusely with age, following a similar growth pathway in both men and women. The spatiotemporal distributions of high-risk plaques and the plaques with obstructive stenosis are further illustrated in Supplementary Fig. 4, while the Supplementary Movie 1 presents dynamic spatiotemporal maps of plaque characteristics in the whole, female and male populations.
Performance evaluation of PLASMA
PLASMA serves as the core analytical tool in this study. As shown in Fig. 1c, it enables fully automated interpretation of CCTA images, encompassing cardiac and coronary artery structure analysis, plaque detection and quantification, stenosis grading, and high-risk feature classification. Eight trained technicians reviewed the PLASMA-generated segmentations and applied manual corrections when necessary to ensure accuracy. From these outputs, we derived a comprehensive set of plaque characteristics—including spatial, burden-related, and morphological features—that support the large-scale population analyses presented in this study. The accuracy and efficiency of PLASMA, together with expert supervision, enabled standardized and reproducible measurements across a large, diverse cohort, which is essential to the validity of our findings. The computational efficiency of PLASMA, including computation time and memory usage across five different GPU configurations, is presented in Supplementary Table 2. In this section, we present detailed evaluations of PLASMA’s performance to demonstrate its reliability and practical applicability in large-scale clinical research.
Regarding coronary segmentation and labeling, on the internal validation dataset comprising 1968 patients, the coronary segmentation model demonstrated an average Dice coefficient of 0.897. Subgroup analyses further confirmed the model’s robustness across various vascular conditions. The Dice scores for specific subgroups were 0.898 for native vessels (n = 1641), 0.901 for stents (n = 185), 0.855 for bypass grafts (n = 81), 0.903 for origin anomalies (n = 61), 0.890 for CTO patients (n = 208), and 0.897 for non-CTO patients (n = 1754), indicating consistent performance regardless of anatomical complexity. External validation focuses specifically on complex clinical scenarios. Among 211 patients with 240 CTO lesions identified on CCTA, the model achieved successful automated segmentation and reconstruction for 95% (n = 228) of all lesions without requiring any manual editing, compared to 48% (n = 116) of all lesions segmented using a conventional manual protocol (p < 0.001)30. Another external validation cohort of 812 patients (mean age, 64.0 ± 11.6 years), including 100 with origin anomalies, 152 with stents, and 105 with bypass grafts, was also analyzed. The success rates for automatic reconstruction were 100% (455/455) for patients with native vessels, 97% (97/100) for those with origin anomalies, 100% (152/152) for those with stents, and 76.2% (80/105) for those with bypass grafts. The image quality scores of the model’s reconstructions were significantly higher than those obtained using conventional manual approaches across all subgroups31.
For plaque detection and stenosis grading, the internal validation (n = 1008) showed that the model achieved an overall sensitivity of 92.7% (95% CI: 0.919, 0.934), with an average of 0.32 false positives per volume, resulting in a detection precision of 93.1% (95% CI: 0.923, 0.938) at the lesion level. The sensitivity for different plaque types was 94.7% for calcified plaques (95% CI: 0.937, 0.956), 96.5% for mixed plaques (95% CI: 0.954, 0.973), and 84.3% (95% CI: 0.821, 0.863) for non-calcified plaques. The model reached an overall stenosis grading accuracy of 81.0%. The majority of errors involved a one-grade discrepancy, likely due to cases where the stenosis degree was near the borderline between two adjacent grade scales. The discrepancies of two or more grades accounted for only 2.3%. We conducted a multi-center, multi-case study (n = 374) to serve as the external validation of the developed plaque detection and stenosis grading model32. The model achieved a vessel-level sensitivity of 83.2% (95% CI: 78.7%, 87.1%) and specificity of 80.0% (95% CI: 77.6%, 82.2%), with an AUC of 0.82 (95% CI: 0.79, 0.84). When interpreting independently, the 12 radiologists achieved a sensitivity of 65.8% (95% CI: 64.3%, 67.3%), specificity of 91.2% (95% CI: 90.8%, 91.7%), and AUC of 0.78 (95% CI: 0.78, 0.79). With AI assistance, their sensitivity improved to 73.1% (95% CI: 71.7%, 74.5%), specificity to 89.3% (95% CI: 88.8%, 89.8%), and AUC to 0.81 (95% CI: 0.80, 0.82).
For plaque segmentation, the five-fold cross-validation (n = 1560) showed that the automated plaque segmentation model achieved excellent agreement with manual annotations. For total plaque volume, the average ICC was 0.92 (95% CI: 0.90–0.94) and Pearson’s r was 0.93 (95% CI: 0.91–0.95). Calcified plaque volume showed near-perfect agreement with an ICC of 0.99 (95% CI: 0.98–0.99) and Pearson’s r of 1.00 (95% CI: 0.99–1.00). Non-calcified plaque volume yielded an ICC of 0.88 (95% CI: 0.85–0.91) and Pearson’s r of 0.90 (95% CI: 0.87–0.91). Detailed fold-wise results are provided in Supplementary Table 1. External validation on an independent dataset (n = 439) from three medical centers further confirmed the robustness of the plaque segmentation module. Total plaque volume had an ICC of 0.93 (95% CI: 0.91–0.94) and Pearson’s r of 0.94 (95% CI: 0.93–0.95). Calcified volume showed an ICC of 0.92 (95% CI: 0.90–0.93) and Pearson’s r of 0.94 (95% CI: 0.92–0.95). For non-calcified volume, ICC was 0.90 (95% CI: 0.88–0.92) and Pearson’s r was 0.92 (95% CI: 0.90–0.93). The Bland-Altman analysis for external validation also showed good agreement between automatic segmentation and manual annotations, as shown in Supplementary Fig. 6.
Finally, regarding the classification of high-risk plaque characteristics, a random subset (n = 241) of the internal validation dataset was annotated to evaluate the performance of the high-risk plaque characteristics classification. This subset comprised a total of 1320 plaques, including 274 plaques with PR, 383 with LAP, 52 with NRS, and 98 with SC. As shown in Supplementary Fig. 7, the model achieved comparable performance in detecting PR and LAP, each with an AUC of 0.87 (95% CI: 0.85, 0.89). For SC, it attained a lower AUC of 0.81 (95% CI: 0.79, 0.83), and it demonstrated higher accuracy in detecting the NRS, with an AUC of 0.93 (95% CI: 0.92, 0.94).
Discussion
In recent years, the incidence and mortality rates of atherosclerotic cardiovascular disease have been reported to decline in Western countries, largely benefiting from population-based prevention strategies13. However, in China, both the incident and mortality rates of cardiovascular disease remain high and continue to rise2. This trend is likely linked to lower levels of awareness, treatment, and control of major risk factors such as hypertension, dyslipidemia, and diabetes—compared with those of developed countries46,47. Given the differences in the epidemiology of cardiovascular disease between the Chinese and Western populations, the prevention guidelines on cardiovascular disease established by the European Society of Cardiology (ESC)48 and the American College of Cardiology/American Heart Association (ACC/AHA)49 may not be entirely applicable to the Chinese population. The more recent Chinese primary prevention guidelines50 have adapted risk assessment models and prevention strategies to better suit the Chinese population. For instance, they account for the lower tolerance for high-dose statins among Chinese individuals. Nevertheless, these guidelines still rely on the Western standards for certain quantitative indicators, such as the CACS thresholds used in risk modifiers, due to absence of large-scale quantitative studies in Chinese cohorts.
Furthermore, previous research has indicated that, in addition to CACS51,52,53, the volume and characteristics of atherosclerotic plaques identified through CCTA—such as plaque morphology9,54,55,56, burden3,57, and position58,59—have gained increasing importance in assessing CAD risk and predicting the occurrence of myocardial infarction. These factors hold the potential to improve prognostic accuracy for cardiovascular disease when combined with traditional risk factors58. However, despite the widespread inclusion of CACS as a risk enhancer in primary prevention guidelines globally, other plaque characteristics have yet to be integrated into risk assessment processes. It is largely due to traditional dependence on manual tools and the absence of reference values for various plaque measurements.
To address these limitations, we employed an automated AI-based plaque analysis system and obtained age- and sex-specific benchmark values for plaque quantification using CCTA datasets from a large, multi-center Chinese cohort. In addition, for the first time we created a 3D atlas of the coronary arteries with mapped plaque features, providing a detailed statistical view of the temporal and spatial patterns of plaque development and progression, extending beyond the conventional vessel- or segment-level analysis.
Our study observed a general increase in total plaque burden with advancing age. Notably, the younger individuals primarily exhibited non-calcified plaque. In both males and females, the proportion of calcified plaque within the total plaque volume showed the most rapid increase with age, followed by a slight increase in fibrous plaque, a decrease in fibro-fatty, and the most pronounced decrease in lipid plaques. These results are consistent with the previous research on the North American population27, reflecting the possible natural progression of coronary atherosclerotic plaque development.
Significant differences in atherosclerotic progression were revealed between men and women. Specifically, we confirmed an approximate 20-year delay in the onset of atherosclerosis in Chinese female patients, which is markedly greater than the 10-year delay previously reported in the Swedish general population26. Notably, this sex-specific delayed gap was also preserved across rural and urban populations (see Supplementary Fig. 3), indicating that the sex difference in atherosclerotic progression is robust regardless of economic development level. This delayed pattern was consistently present across the seven major geographic regions of China, with most regions showing an approximate 20-year delay. Regions with more pronounced deviations included the Southwest (24 years) and South (25 years), as shown in Supplementary Table 5. These regional differences may result from variations in lifestyle, dietary habits, genetic background, or healthcare access, which could influence cardiovascular risk and the pace of atherosclerotic progression. Additionally, women demonstrated a nonlinear pattern of plaque progression, with an accelerating growth rate as they age. In particular, the increase of total plaque burden is not apparent in women until ages 50–55, which is nearly beyond the mean age at natural menopause (ANM) in Chinese women (48.7 years old). Moreover, a recent study reported an inverted V-shaped trend in lipid level changes among Chinese women, with the highest lipid levels occurring at ages 40–4960. Given the correlation between lipid levels and plaque manifestation, these findings provide additional support that plaque formation in females tends to lag behind the hormonal and metabolic changes associated with menopause. These observations also indicate the potential impact of menopause on lipid profiles in women, which, in turn, exacerbates plaque development, thereby elevating the risk of MACE.
It is recommended that future prevention guidelines recognize menopause as a critical factor for women, emphasizing lipid control and enhanced cardiovascular monitoring during and after the menopausal transition. In comparison, men exhibited a consistent, linear increase in plaque accumulation across all age groups, with both plaque burden and growth rate generally surpassing those observed in women of corresponding ages. However, as they approached age 75 or beyond, men’s growth rate began to fall behind that of women. Given that plaque accumulation in men seemed to start earlier, it is important to implement preventive measures at a younger age. Additional research is required to characterize the atherosclerosis development in young adult males, potentially informing the ideal age for initiating preventive interventions.
Next, we compared regional disparities in plaque progression between the Chinese population and the North American population as previously reported27. The findings indicate that both the total plaque volume and PAV in Chinese patients are significantly lower than in North American patients, alongside a notably faster progression of plaque calcification over time, irrespective of sex and age range. This observation was consistently supported by our rural–urban subgroup analysis and the seven major regional subgroup analysis (see the Supplementary Table 4 and 5), in which all subgroups exhibited lower average plaque volume compared to the North American cohort. Apart from the distinct algorithm models used for automatic segmentation of the coronary artery and plaques in the two studies, this difference may also be attributed to regional variations in risk factors. Specifically, risk factors such as hypertension, dyslipidemia, obesity, and inflammation tend to be at more favorable levels in China compared to the USA47.
In this study, the 3D atlas of coronary centerlines we constructed, for the first time, provides fine-grained spatial distribution of plaques with a variety of their features averaged over the collected cohort. The order of plaque prevalence among the four main coronary branches follows the sequence of LAD, RCA, LCx, and left main (LM), consistent with findings from previous studies26,27. Furthermore, the atlas pinpointed specific segments and sites where plaques, high-risk plaques, and plaques with obstructive stenosis are most likely to form. Prominent plaque clustering was noted in the proximal segments of the LAD, LCx, and RCA, near and slightly upstream of bifurcation points of side branches such as D1 and OM1, with an additional cluster found in the distal RCA segment. Consistent with previous studies, which indicate that high-risk plaques and culprit lesions of ST-segment elevated myocardial infarction frequently localize near side branches61,62, our findings support this pattern. Prior research has suggested that low or oscillatory wall shear stress in these areas can promote inflammatory activation63 and increase the likelihood of high-risk plaque phenotype formation64. Consequently, clustering of plaques in LAD and LCx may be driven by blood flow dynamics shaped by coronary anatomical features in these regions, such as the presence of diagonal or obtuse marginal branches. Tensile stress may be a possible cause of the clustering observed in the pRCA. In this region, the vessel is more closely anchored to the surface of the heart by side and deep branches, potentially creating a compliance mismatch between the ostium and the proximal segment of the RCA, which leads to tensile stress concentrations65. Such mechanical stress, in combination with hemodynamic factors, could exacerbate endothelial dysfunction and promote localized plaque development. Moreover, the clustering in the dRCA could be related to slower blood flow in this region, potentially facilitating the retention of atherogenic lipoproteins, or its proximity to the bifurcation sites of the posterior descending artery from RCA (R-PDA) and posterior-lateral branch from RCA (R-PLB), where oscillatory shear stress might contribute. These hypotheses remain speculative and require further investigation in future studies.
For further analysis, a series of 3D atlas models were constructed by averaging plaque characteristics across varying age and sex groups, revealing a similar spatiotemporal pattern of plaque development in both men and women. Plaque formation typically begins in distinct, localized regions and progressively extends more broadly with advancing age. Besides the potential to improve the capacity of CCTA for effective age- and sex-specific risk stratification, the 3D atlas models can also be used to provide prior plaque distribution for improving the robustness of machine-learning based algorithms against small training data size.
When interpreting our findings, several key limitations should be acknowledged. Rather than community-based population screening, our cohort comprised randomly selected cross-sections of symptomatic individuals, introducing a degree of selection bias toward symptomatic or at-risk individuals. However, this practical design reflects the current diagnostic landscape in China, where CCTA is predominantly used in such populations. Interpreted within this clinical context, our results offer valuable insights into sex- and age-specific atherosclerotic patterns and supports integration into routine clinical practice, which are relevant for clinical risk stratification and decision-making. Additionally, because this study involved a real-world, consecutively recruited clinical cohort across diverse clinical centers, it mitigated the selection biases typical of registry-based studies, providing a more representative view of the general population undergoing clinically indicated CCTA. Our study also lacks comprehensive information on clinical outcomes and detailed patient characteristics, including cardiovascular risk factors, symptom status, prior CAD diagnoses, and medication use. Future research is necessary to explore these relationships with patient profiles or subsequent clinical outcomes and assess whether quantitative plaque analysis can enhance clinical decision-making and improve outcomes beyond traditional visual assessments. Potential algorithm errors and model biases may be present, even though they have been validated with expert annotations on CCTA images. Future studies are needed to compare the automatically derived plaque volumes and high-risk features with reference standards like intravascular ultrasound.
The strengths of our study include providing a multi-level analysis—at the patient, segment and point levels—of comprehensive atherosclerotic characteristics in a symptomatic Chinese population, leveraging a large-scale, multi-center dataset. Moreover, our study is the first to develop a series of spatiotemporal atlases detailing plaque characteristics across different patient age and sex subgroups. This approach enables the identification of fine-grained spatial distributions of plaque with their attributes, potentially providing valuable insights for optimizing CAD prevention and diagnostic workflows. The use of a fully automated and validated AI-CCTA system—PLASMA—enhanced the study’s effectiveness and minimized observer variability. Finally, we present invaluable insights into the differences and similarities in plaque characteristics, spatial distribution, and progression patterns between sexes, paving the way for future age- and sex-aware studies in prevention, diagnosis, and treatment of suspected CAD individuals in China.
In conclusion, we revealed age- and sex-specific distribution charts for atherosclerotic plaque characteristics in a large Chinese cohort undergoing clinically indicated CCTA, assisted with a fully automated AI coronary plaque analysis system. We confirmed that sex and age have significant influence on the plaque development and progression, with age having a particularly pronounced impact on women around menopause. Moreover, we uncovered notable differences in plaque burden and calcification progression rates across populations from different geographic regions, highlighting the importance of developing region-specific CAD prevention and treatment strategies. Finally, we constructed a series of age- and sex-stratified atlases of coronary centerlines providing spatially continuous distributions of plaques, which demonstrated that the plaques tend to cluster around bifurcation points of side branches. These atlases will serve as valuable resources for future studies on CCTA interpretation and risk stratification, and we hope our research encourages a re-evaluation and refinement of patient treatment approaches.
Methods
Ethics approval
The retrospective collection of CCTA data was conducted under the umbrella ethical approval of Shanghai General Hospital Institutional Review Board (IRB 2023-049), with additional approvals obtained from several participating hospitals, including Ruijin Hospital (IRB 2020-117), Peking University People’s Hospital (IRB 2021PHA022-002), Shanghai East Hospital (IRB 2021-015), The Second Affiliated Hospital of Nanchang University (IRB AF/SG-03/2.0), and The Affiliated Hospital of Hebei University (IRB HDFY-LL-2021-083). Patient informed consent was waived by all participating IRBs because the study was retrospective, used anonymized data, and had no impact on patient treatment or management.
Cohort
We conducted a multi-center cohort study across 42 clinical sites in mainland China to investigate patients who underwent clinically indicated CCTA scans between June and August 2023. CCTA scans were collected retrospectively, anonymized and exported in Digital Imaging and Communications in Medicine (DICOM) format. Eligible subjects were included based on the availability of age and sex demographics, along with the requirement that CCTA images were of sufficient quality for quantitative plaque assessment. Specifically, image quality of original axial images was visually assessed by certified CT analysts using a 4-point scale—excellent (absence of artifacts, score 3), good (presence of mild artifact, score 2), sufficient (presence of moderate artifact, but still diagnostic, score 1), and poor (presence of severe artifact, non-diagnostic, score 0)—following established criteria66. Cases with scores of 0 or 1 were excluded to ensure adequate image quality, and all four proximal coronary segments (RCA, LM, LAD, and LCx) were required to be readable for plaque evaluation. Exclusions were made for patients under 25 years of age and those who had previously undergone PCI or CABG. Prior cardiac procedures were identified using a task-specific AI model that automatically detected the presence of stents or grafts in the CCTA images, with all findings subsequently confirmed through manual review. After applying these criteria to our initial cohort of 20,089 subjects, a total of 16,300 subjects were included in the final analysis (see Fig. 2a), of which 12,287 subjects were detected with plaques, and 9520 were males and 6780 were females. The mean age was 61.49 years with a standard deviation of 11.6 years, ranging from 25 to 97 years old. The distributions by sex in each age group and geographic regions are represented in Fig. 1b.
AI models: PLASMA
The PLASMA in this study comprises of three primary AI modules: coronary segmentation and labeling models, models for plaque detection, segmentation, and stenosis grading, and models for classifying the presence of high-risk plaque features.
Regarding the coronary segmentation and labeling, the advanced progressive learning-based framework for coronary segmentation integrates two primary networks29: (a) the spatial anatomical dependency (SAD) module and (b) the hierarchical topology learning (HTL) module. The SAD module was designed to perform an initial segmentation of both the heart chambers and coronary arteries. These segmentation masks then facilitated the creation of distance field maps, effectively capturing spatial relationship between the arteries and the heart. The HTL module further refined this initial segmentation by employing multi-task learning to represent coronary topology at three distinct levels: key points, centerlines, and neighboring cube-connectivity. The combined functionality of these modules greatly enhanced the accuracy and robustness of coronary segmentation, accommodating the diverse shapes, sizes, and spatial variations of coronary arteries across individuals. The detailed demonstration of the framework can refer to the article29.
We initially pre-trained two Residual U-Net67 models to perform coarse segmentation on the heart chambers and coronary arteries separately. For the coronary artery, we generated an over-segmented mask, termed a “dilated label”, by expanding the ground truth using a 5 × 5 × 5 kernel to guide the coarse segmentation of the arteries. These preliminary segmentation outputs were then utilized to localize coronary vessels and exclude background elements, thereby supporting the subsequent, more detailed segmentation. Using the coarse segmentations of vessels and heart chambers, we extracted two sets of points: one from the coronary arteries and another from the surfaces of each heart chamber (including the left and right ventricles, left and right atria, and the aorta). By calculating the shortest distance between each coronary artery point and the points on the surface of these five cardiac substructures, we derived distance field maps. These maps encapsulated the spatial relationship between arteries and heart structures, serving as input for the next module to enhance the precision of the coronary segmentation.
To accommodate the structural diversity of coronary artery trees, a hierarchical topology learning (HTL) module was developed to concurrently capture topological features of vascular trees at three levels: detecting key points, regressing centerline heatmaps, and predicting cube connectivity. These three learning tasks share a common encoder, which optimizes learning efficiency by pooling information and applying regularization across all tasks. Bifurcation points and endpoints of each coronary branch are essential structural references in vascular trees, making their accurate detection critical. To achieve this, we designed a key-point filter unit (KFU) that generates heatmaps with a small standard deviation (σ = 3 voxels) centering around each key point. These heatmaps served as ground truth for training a model to detect key points in the coronary vascular trees. The skeletal structure defines the topology of tubular and curvilinear shapes, so a centerline regression model was created to maintain the topological integrity of coronary vessels. Similar to the KFU, we applied a 3D adaptive Gaussian filter, referred to as the centerline filter unit (CFU), to generate heatmaps along the centerline. The filter’s kernel size adjusted to match the local lumen diameter, and these heatmaps provided the ground truth for training the coronary centerline regression model. Cube connectivity refers to relationships between each vessel voxel and its 26 neighboring voxels in a 3 × 3 × 3 cube. This connectivity forms a 26-channel vector, with each element being marked as one if both the voxel and its neighboring voxel belong to a coronary vessel and zero otherwise. These 26-channel vectors represent the pairwise connectivity of adjacent points29,68. The connectivity model was trained to output these vectors, which were then processed to form the final binary vessel segmentation mask through an inverse connectivity construction process.
For model development, a separate cohort of consecutive patients undergoing clinically indicated CCTA were retrospectively included from three tertiary hospitals between January, 2010 and December, 2018. In order to generalize the model applicability to CCTA post-processing in various clinical settings, we enrolled all patients with a history of coronary bypass grafting, stenting, and diagnosis of origin anomaly during that time span to train the model. The exclusion criterion was significantly-impaired image quality of CCTA, defined as the presence of severe artifacts leading to non-diagnostic image quality. This led to a final inclusion of 8031 patients, who were then randomly split into a training set (n = 6063) and an internal validation set (n = 1968) in an approximate 3:1 ratio.
All segmentation networks and experimental procedures were implemented using PyTorch 2.0 and deployed on two NVIDIA Tesla V100S GPUs with 40 GB memory each. The network was trained over 600 epochs on mini-batches containing four cropped CTA images, employing the Adam optimizer with an initial learning rate of 10−4. For model training, the mean squared error (MSE) loss was applied to both the key point detection and centerline regression models, while the cube-connectivity prediction model used the average Dice similarity coefficient as its loss function. Model performance was evaluated on validation data, with the optimal training epoch selected based on the lowest observed validation loss.
To evaluate coronary artery segmentation accuracy, the Dice coefficient was reported. The internal validation was conducted on a dataset of 1968 patients, which were manually segmented by a team of two experienced technicians supervised by a senior radiologist as the standard. To further evaluate the robustness of the segmentation model against variations caused by vascular abnormalities and pathologies, the internal validation cohort was stratified into subgroups: patients with native vessels (n = 1641), stents (n = 185), bypass grafts (n = 81), and origin anomalies (n = 61). Additionally, patients were divided into those with chronic total occlusion (CTO) (n = 208) and those without CTO (n = 1754).
Beyond internal validation, two retrospective, multi-center studies were performed to assess the model performance using external validation datasets, focusing specifically on patients with chronic total occlusion (CTO)30, and other complex clinical scenarios including stents, bypass grafts and origin anomalies31. The first study involved 211 patients with 240 CTO lesions identified on CCTA, while the second external validation cohort consisted of 812 patients (mean age, 64.0 ± 11.6 years), including 100 patients with origin anomalies, 152 with stents, and 105 with bypass grafts. The detailed validation results are presented in the Results section.
The whole flowchart of automated plaque detection and segmentation, stenosis grading, as well as the plaque composition classification is shown in Supplementary Fig. 5. After segmenting the coronary arteries from the CCTA images, the centerlines of the vessels, represented by an ordered sequence of points in three-dimensional space, were extracted. The vessels were then processed using straightened curved planar reconstruction (SCPR) to facilitate subsequent plaque detection and stenosis grading. A series of cropped image patches, each sized 32 voxels³ with an isotropic resolution of 0.3 mm per voxel, were extracted as a sliding window along the straightened vessel centerline at a sampling interval of 0.3 mm. The fixed-sized cropped image patch was processed through a residual classification network, ResNet69, to determine the presence of any plaques around the center point. The consecutive centerline points with classification probabilities exceeding the threshold were grouped together, identifying a detected plaque. Once a plaque was located, a tightly cropped image patch enclosing it was extracted along the straightened vessels and input into two separate networks for plaque segmentation and stenosis grading, respectively. The segmented plaque voxels were subsequently categorized into calcified, fibrous, fibro-fatty, and lipid compositions according to hounsfield unit (HU) density thresholds of 350 HU, 130 HU, and 30 HU, respectively, following the expert consensus on coronary CT imaging of atherosclerotic plaque44.
The complete internal training dataset (n = 6063) for coronary segmentation model development was likewise employed to train the lesion detection and stenosis grading models. However, due to the extensive annotation efforts required for lesion segmentation, a random subset of this dataset (n = 1560) was employed for five-fold cross-validation. Manual lesion annotation and delineation, along with stenosis measurement, were all performed on the SCPR of the vessels by an experienced team of technicians under the supervision of a senior radiologist. To enhance model generalization, data augmentation was applied during training, including random elastic deformation in the cropped image patches (0 to 2 mm), slight random scaling (0.9 to 1.1), and minor random rotation (−5° to +5°) around the longitudinal directions of the vessels. Focal loss, Dice loss and L2 loss functions were adopted for the plaque detection, plaque segmentation and stenosis regression model, respectively. The Adam optimizer (initial learning rate = 10−4, β1 = 0.9, β2 = 0.999) was chosen to minimize the loss functions. The optimal training epoch for each model was selected based on the minimum loss on the validation data. The framework was implemented in PyTorch using an NVIDIA Tesla V100 GPU.
From the overall internal validation dataset (n = 1968) for the coronary segmentation model, a subset (n = 1008) was randomly selected to validate the plaque detection and stenosis grading models. This subset included a total of 4673 plaques, consisting of 2165 calcified plaques, 1386 mixed plaques, and 1122 non-calcified plaques. The stenosis severity of these plaques was manually measured and annotated according to the SCCT grading scales, with 1000 plaques showing no visible or minimal stenosis (0–24%), 2305 classified as having mild stenosis (25–49%), 955 as moderate stenosis (50–69%), and 413 as severe stenosis or complete occlusion (70–100%).
A retrospective, multi-reader, multi-case study was recently published to further assess the diagnostic performance of the developed lesion detection and stenosis grading models32. This study included 374 patients from five medical institutions across Northern and Eastern China. It involved 12 radiologists, each reading every CT scan twice—once with AI assistance and once without, with a one-month washout period between readings. For statistical analysis at the vessel level, four vessels along with their branches, namely the LM, LAD, LCx, and RCA, were included for each patient, leading to a total of 1495 vessels. With invasive coronary angiography used to establish the reference standard, any vessel with at least one obstructive coronary stenosis is considered a positive case.
For plaque segmentation, we conducted a five-fold cross-validation (n = 1560) on the internal dataset and an external validation (n = 439) to evaluate the performance of automated segmentation against manual annotations. This assessment was conducted using the intraclass correlation coefficient (ICC), Pearson’s correlation coefficient and Bland-Altman analysis across total plaque volume, calcified plaque volume, non-calcified plaque volume, and lipid plaque volume. Results of external validation demonstrated excellent agreement and strong correlation for total plaque volume, calcified plaque volume and good agreement on non-calcified volume, as detailed in the Results section.
Finally, regarding the classification of high-risk plaque characteristics, each cropped image patch containing a detected plaque was simultaneously input into a classification network trained to identify the presence of four high-risk plaque features, i.e., PR, LAP, NRS, and SC.
Three junior radiologists, each with under five years of experience, independently labeled the four high-risk plaque features following the criteria outlined in Abdelrahman et al.43. The initial annotations were then reviewed by two senior radiologists with over ten years of experience, who relabeled plaques as needed. In cases where the senior radiologists disagreed, an arbitration expert with 15 years of experience in cardiovascular imaging made the final decision, which served as the reference standard.
The classification network employs the same ResNet architecture as the stenosis grading network, with the loss function replaced with binary cross-entropy. The four features share the same weights of the network backbone, differing only in their classification heads. A random subset (n = 2160) of the entire internal training dataset was designated for model development and parameter tuning, while a separate random subset (n = 241) of the internal validation dataset was annotated and reserved for performance evaluation. The model was trained on an NVIDIA A40 GPU with 48 GB memory, employing the same data augmentation strategy and hyperparameters as those applied to the plaque segmentation and stenosis grading models.
Spatiotemporal map construction
To construct the 3D coronary atlas, we began by calculating the average length of each coronary artery segment across the cohort of 16,300 subjects enrolled in this study (LAD: 145.14 mm; LCx: 76.35 mm; RCA: 109.27 mm; LM: 11.78 mm). With a sampling interval of 0.3 mm, we determined the number of centerline points Ns for each vessel segment s based on its average length, and then resampled the centerline of segment s for each subject to Ns equidistant and ordered points. After performing Procrustes analysis, the mean shape of each vessel segment was obtained by averaging the 3D coordinates of the resampled centerline points. Given the anatomical variations that result in the occasional absence of certain branch vessels, such as D1 or the second diagonal branch (D2), we calculated the average bifurcation position of these branches in terms of their normalized distance from the origin of the main vessel from which they branch off. In the atlas, the mean centerlines of these branch vessels were positioned starting from their corresponding averaged bifurcation points. After constructing the coronary centerline atlas, each automatically detected plaque, along with its features—such as the stenosis, composition, and high-risk characteristics—was mapped onto the atlas. This mapping was based on each plaque’s normalized position and range within its respective vessel segment, allowing for spatially aligned statistical analysis across patient subgroups by age and sex.
Statistical analysis
In this study, continuous variables are generally presented as mean ± standard deviation and percentiles, while categorical variables are reported as counts or percentages. We employed t test to assess the significance of age and sex on plaque burden-related features. In the per-subject analysis, boxplots were used to visualize the distribution of values, including the mean, median, and interquartile range (IQR). We plotted age-related trajectories for continuous variables, showing the mean as well as the 10th and 90th percentiles. These trajectories were modeled using cubic B-spline interpolation based on data from five age groups (<45, 45–55, 56–65, 66–75, and ≥75 years) across males, females, and the entire population. The corresponding growth rate trajectories were calculated as the first-order derivatives of the mean trajectories. Here, the growth rate is expressed per decade, reflecting the unit used in our fitting model, where each step corresponds to a 10-year age interval. If absolute age values (e.g., 40, 50, 60, 70, 80) were used instead—implying a 1-year interval—the slope magnitude would be numerically smaller by a factor of 10, while the overall trend remains unchanged. The delayed onset of CCTA-detected atherosclerosis in women was modeled by shifting the x-axis relative to men in a 1-year interval and identifying the minimum of the sum of squared differences in annualized atherosclerosis prevalence between sexes. In the per-segment analysis, we computed plaque burden-related features averaged across various age subgroups. Given the variations in coronary anatomy and the occasional absence of specific vessel segments, these features were averaged only among patients with the relevant segments present. In the spatiotemporal analysis, the spatial distribution of plaque prevalence was similarly determined by dividing the number of patients with plaques detected at specific atlas-aligned locations over the total number of patients in the group with the corresponding segment. All positions along the segments of the atlas represent relative locations within a range of [0, 1], indicating the distance from the segment’s origin as a proportion of the segment’s total length.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
A sample dataset and an interactive demo of PLASMA, which features automated coronary artery reconstruction and plaque analysis, are available at https://aidemo.united-imaging.com/ (username: demo; password: Uai@434254!). Statistical atlases of plaque characteristics derived from the cohort are shared in GitHub (https://github.com/MEI243/PS-CTA-Plaque-Atlas) and archived on Zenodo (https://zenodo.org/records/16741227)70. All shared data is fully anonymized to protect patient privacy in accordance with relevant legal requirements. Due to restrictions imposed by institutional review boards, the raw datasets used in this study are not publicly accessible. However, requests for access to aggregated data and supporting clinical documentation will be evaluated by an independent review panel based on the scientific merit of the request. For data access inquiries related to this study, please contact the corresponding author, Dinggang Shen (dinggang.shen@gmail.com). Requests will be reviewed and responded to within two months. Source data are provided with this paper.
Code availability
The implementation of PLASMA relies on proprietary internal tools and infrastructure and is covered by patents (application numbers: CN111815599B71, CN113902693A72), which prevent public release of the code. Nevertheless, a demo for plaque atlas calculation, along with example data, is openly available on GitHub (https://github.com/MEI243/PS-CTA-Plaque-Atlas) and archived on Zenodo (https://zenodo.org/records/16741227)70. Detailed descriptions of all experiments and implementation procedures are provided in the Methods section, enabling replication using freely available libraries. Additionally, core components relevant to our work can be accessed through open-source platforms, such as PyTorch (https://pytorch.org/) and ResNet (https://github.com/pytorch/vision/blob/main/torchvision/models/resnet.py).
References
Nowbar, A. N., Gitto, M., Howard, J. P., Francis, D. P. & Al-Lamee, R. Mortality from ischemic heart disease: analysis of data from the world health organization and coronary artery disease risk factors from ncd risk factor collaboration. Circ. Cardiovasc. Qual. Outcomes 12, e005375 (2019).
Wang, Z. et al. Summary of the 2022 report on cardiovascular health and diseases in china. Chin. Med. J. 136, 2899–2908 (2023).
Mortensen, M. B. et al. Impact of plaque burden versus stenosis on ischemic events in patients with coronary atherosclerosis. J. Am. Coll. Cardiol. 76, 2803–2813 (2020).
Stone, G. W. et al. A prospective natural-history study of coronary atherosclerosis. N. Engl. J. Med. 364, 226–235 (2011).
Gallone, G. et al. Coronary plaque characteristics associated with major adverse cardiovascular events in atherosclerotic patients and lesions: a systematic review and meta-analysis. JACC Cardiovasc. Imaging 16, 1584–1604 (2023).
Burke, A. P. et al. Coronary risk factors and plaque morphology in men with coronary disease who died suddenly. N. Engl. J. Med. 336, 1276–1282 (1997).
Baeßler, B. et al. Artificial intelligence in coronary computed tomography angiography: demands and solutions from a clinical perspective. Front. Cardiovasc. Med. 10, 1120361 (2023).
Knuuti, J. et al. 2019 esc guidelines for the diagnosis and management of chronic coronary syndromes: the task force for the diagnosis and management of chronic coronary syndromes of the european society of cardiology (esc). Eur. Hear. J. 41, 407–477 (2020).
Cury, R. C. et al. Cad-rads™ 2.0–2022 coronary artery disease-reporting and data system: an expert consensus document of the society of cardiovascular computed tomography (scct), the american college of cardiology (acc), the american college of radiology (acr), and the north america society of cardiovascular imaging (nasci). JACC Cardiovasc. Imaging 15, 1974–2001 (2022).
Maroules, C. D. et al. Coronary artery disease reporting and data system (cad-radstm): inter-observer agreement for assessment categories and modifiers. J. Cardiovasc. Comput. Tomogr. 12, 125–130 (2018).
Usami, K. et al. Impact of coronary plaque characteristics on periprocedural myocardial injury in elective percutaneous coronary intervention. Eur. Radiol. 33, 3020–3028 (2023).
Mufarreh, A., Shah, A. J., Vaccarino, V. & Kulshreshtha, A. Trends in provision of medications and lifestyle counseling in ambulatory settings by gender and race for patients with atherosclerotic cardiovascular disease, 2006-2016. JAMA Netw. Open 6, e2251156–e2251156 (2023).
Björck, L., Rosengren, A., Bennett, K., Lappas, G. & Capewell, S. Modelling the decreasing coronary heart disease mortality in sweden between 1986 and 2002. Eur. Hear. J. 30, 1046–1056 (2009).
Regitz-Zagrosek, V. & Gebhard, C. Gender medicine: effects of sex and gender on cardiovascular disease manifestation and outcomes. Nat. Rev. Cardiol. 20, 236–247 (2023).
Mosca, L., Barrett-Connor, E. & Kass Wenger, N. Sex/gender differences in cardiovascular disease prevention: what a difference a decade makes. Circulation 124, 2145–2154 (2011).
Du, X. et al. Treatment and outcomes of acute coronary syndromes in women: an analysis of a multicenter quality improvement chinese study. Int. J. Cardiol. 241, 19–24 (2017).
Mohamed, M. O. et al. Sex disparities in the choice of cardiac resynchronization therapy device: an analysis of trends, predictors, and outcomes. Can. J. Cardiol. 37, 86–93 (2021).
Mehilli, J. & Presbitero, P. Coronary artery disease and acute coronary syndrome in women. Heart 106, 487–492 (2020).
Thalmann, I., Preiss, D., Schlackow, I., Gray, A. & Mihaylova, B. Population-wide cohort study of statin use for the secondary cardiovascular disease prevention in Scotland in 2009–2017. Heart 109, 388–395 (2023).
Madhavan, M. V., Gersh, B. J., Alexander, K. P., Granger, C. B. & Stone, G. W. Coronary artery disease in patients 80 years of age. J. Am. Coll. Cardiol. 71, 2015–2040 (2018).
Kim, M. et al. Impact of age on coronary artery plaque progression and clinical outcome: a paradigm substudy. J. Cardiovasc. Comput. Tomogr. 15, 232–239 (2021).
Mendis, S. et al. Global atlas on cardiovascular disease prevention and control (World Health Organization, 2011).
McDonagh, T. A. et al. 2021 esc guidelines for the diagnosis and treatment of acute and chronic heart failure: Developed by the task force for the diagnosis and treatment of acute and chronic heart failure of the european society of cardiology (esc) with the special contribution of the heart failure association (hfa) of the esc. Eur. Heart J. 42, 3599–3726 (2021).
Haider, A. et al. Sex and gender in cardiovascular medicine: presentation and outcomes of acute coronary syndrome. Eur. Heart J. 41, 1328–1336 (2020).
Oertelt-Prigione, S. et al. Cardiovascular risk factor distribution and subjective risk estimation in urban women–the befri study: a randomized cross-sectional study. BMC Med. 13, 1–9 (2015).
Bergström, G. et al. Prevalence of subclinical coronary artery atherosclerosis in the general population. Circulation 144, 916–929 (2021).
Tzimas, G. et al. Age-and sex-specific nomographic CT quantitative plaque data from a large international cohort. JACC Cardiovasc. Imaging 17, 165–175 (2024).
Föllmer, B. et al. Roadmap on the use of artificial intelligence for imaging of vulnerable atherosclerotic plaque in coronary arteries. Nat. Rev. Cardiol. 21, 51–64 (2024).
Zhang, X. et al. An anatomy-and topology-preserving framework for coronary artery segmentation. IEEE Trans. Med. Imaging 43, 723–733 (2023).
Li, M. et al. Deep learning segmentation and reconstruction for CT of chronic total coronary occlusion. Radiology 306, e221393 (2022).
Yu, L. et al. Deep learning reconstruction for coronary CT angiography in patients with origin anomaly, stent or bypass graft. Radiol. Med. 129, 1173–1183 (2024).
Yang, W. et al. Diagnostic performance of deep learning-based vessel extraction and stenosis detection on coronary computed tomography angiography for coronary artery disease: a multi-reader multi-case study. Radiol. Med. 128, 307–315 (2023).
Jia, D. & Zhuang, X. Learning-based algorithms for vessel tracking: a review. Comput. Med. Imaging Graph. 89, 101840 (2021).
Lin, A. et al. Deep learning-enabled coronary CT angiography for plaque and stenosis quantification and cardiac risk prediction: an international multicentre study. Lancet Digit. Health 4, e256–e265 (2022).
Kim, D. Deep learning-based quantitative image analysis for detecting coronary artery stenosis, calcification, and vulnerable plaque in coronary computed tomography angiography. Eur. Heart J. 44, ehad655–145 (2023).
Jávorszky, N. et al. Deep learning–based atherosclerotic coronary plaque segmentation on coronary CT angiography. Eur. Radiol. 32, 7217–7226 (2022).
Al’Aref, S. J. et al. A boosted ensemble algorithm for determination of plaque stability in high-risk patients on coronary cta. JACC Cardiovasc. Imaging 13, 2162–2173 (2020).
Zreik, M. et al. A recurrent CNN for automatic detection and classification of coronary artery plaque and stenosis in coronary CT angiography. IEEE Trans. Med. Imaging 38, 1588–1598 (2018).
Ramasamy, A. et al. Novel near-infrared spectroscopy–intravascular ultrasound-based deep-learning methodology for accurate coronary computed tomography plaque quantification and characterization. Eur. Hear. J. Open 3, oead090 (2023).
Ma, X., Luo, G., Wang, W. & Wang, K. Transformer network for significant stenosis detection in CTA of coronary arteries. In Medical Image Computing and Computer-Assisted Intervention – MICCAI 2021 of Lecture Notes in Computer Science, 12906: 516–525 (Springer, Strasbourg, France, 2021).
Chen, Q. et al. A coronary ct angiography radiomics model to identify vulnerable plaque and predict cardiovascular events. Radiology 307, e221693 (2023).
WangM. Factors related to age at natural menopause in China: results from the China Kadoorie Biobank. Menopause 28, 1130–1142 (2021).
Abdelrahman, K. M. et al. Coronary computed tomography angiography from clinical uses to emerging technologies: Jacc state-of-the-art review. J. Am. Coll. Cardiol. 76, 1226–1243 (2020).
Shaw, L. J. et al. Society of cardiovascular computed tomography/north american society of cardiovascular imaging–expert consensus document on coronary ct imaging of atherosclerotic plaque. J. Cardiovasc. Comput. Tomogr. 15, 93–109 (2021).
Leipsic, J. et al. Scct guidelines for the interpretation and reporting of coronary ct angiography: a report of the society of cardiovascular computed tomography guidelines committee. Eur. Hear. J. 8, 342–358 (2014).
Zhang, M. et al. Prevalence, awareness, treatment, and control of hypertension in china, 2004-18: findings from six rounds of a national survey. BMJ 380, e071952 (2023).
Lu, Y. et al. Comparison of prevalence, awareness, treatment, and control of cardiovascular risk factors in china and the united states. J. Am. Hear. Assoc. 7, e007462 (2018).
Parums, D. V. The 2021 european society of cardiology (esc) guidelines on the real-world prevention of atherosclerotic cardiovascular disease (ascvd). Med. Sci. Monit. Int. Med. J. Exp. Clin. Res. 27, e935172–1 (2021).
Arnett, D. K. et al. 2019 acc/aha guideline on the primary prevention of cardiovascular disease: a report of the american college of cardiology/american heart association task force on clinical practice guidelines. Circulation 140, e596–e646 (2019).
Prevention, C. D., Prevention, T., of Cardiology of Chinese Medical Association, C. S., of Chinese Medical Doctor Associ- ation, T. C. et al. Chinese guideline on the primary prevention of cardiovascular diseases. Zhonghua Xin Xue Guan Bing. Za Zhi 48, 1000–1038 (2020).
Budoff, M. J. et al. Ten-year association of coronary artery calcium with atherosclerotic cardiovascular disease (ascvd) events: the multi-ethnic study of atherosclerosis (mesa). Eur. Heart J. 39, 2401–2408 (2018).
Mahabadi, A. A. et al. Cac score improves coronary and cv risk assessment above statin indication by esc and aha/acc primary prevention guidelines. JACC Cardiovasc. Imaging 10, 143–153 (2017).
McClelland, R. L. et al. 10-year coronary heart disease risk prediction using coronary artery calcium and traditional risk factors: derivation in the mesa (multi-ethnic study of atherosclerosis) with validation in the hnr (heinz nixdorf recall) study and the dhs (dallas heart study). J. Am. Coll. Cardiol. 66, 1643–1653 (2015).
Puchner, S. B. et al. High-risk plaque detected on coronary ct angiography predicts acute coronary syndromes independent of significant stenosis in acute chest pain: results from the romicat-ii trial. J. Am. Coll. Cardiol. 64, 684–692 (2014).
Williams, M. C. et al. Low-attenuation noncalcified plaque on coronary computed tomography angiography predicts myocardial infarction: results from the multicenter scot-heart trial (scottish computed tomography of the heart). Circulation 141, 1452–1462 (2020).
Otsuka, K. et al. Napkin-ring sign on coronary ct angiography for the prediction of acute coronary syndrome. JACC Cardiovasc. Imaging 6, 448–457 (2013).
Driessen, R. S. et al. Effect of plaque burden and morphology on myocardial blood flow and fractional flow reserve. J. Am. Coll. Cardiol. 71, 499–509 (2018).
Han, D. et al. Association of plaque location and vessel geometry determined by coronary computed tomographic angiography with future acute coronary syndrome–causing culprit lesions. JAMA Cardiol. 7, 309–319 (2022).
Han, D. et al. Prognostic significance of plaque location in non-obstructive coronary artery disease: from the confirm registry. Eur. Heart J. Cardiovasc. Imaging 23, 1240–1247 (2022).
Li, J. et al. Age and genetic risk score and rates of blood lipid changes in China. JAMA Netw. Open 6, e235565–e235565 (2023).
Katritsis, D. G. et al. Ruptured versus stable plaques in human coronary arteries. Coron. Artery Dis. 22, 345–351 (2011).
Bourantas, C. V. et al. Clinical and angiographic characteristics of patients likely to have vulnerable plaques: analysis from the prospect study. JACC Cardiovasc. Imaging 6, 1263–1272 (2013).
Björkegren, J. L. & Lusis, A. J. Atherosclerosis: recent developments. Cell 185, 1630–1645 (2022).
Yamamoto, E. et al. Low endothelial shear stress predicts evolution to high-risk coronary plaque phenotype in the future: a serial optical coherence tomography and computational fluid dynamics study. Circ. Cardiovasc. Interv. 10, e005455 (2017).
Ojha, M., Leask, R. L., Butany, J. & Johnston, K. W. Distribution of intimal and medial thickening in the human right coronary artery: a study of 17 rcas. Atherosclerosis 158, 147–153 (2001).
Dai, X. et al. Image quality and diagnostic accuracy of coronary ct angiography derived from low-dose dynamic ct myocardial perfusion: a feasibility study with comparison to invasive coronary angiography. Eur. Radiol. 29, 4349–4356 (2018).
Kerfoot, E. et al. Left-ventricle quantification using residual u-net. In Statistical Atlases and Computational Models of the Heart. Atrial Segmentation and LV Quantification Challenges. STACOM 2018 of Lecture Notes in Computer Science, 11395: 371–380 (Springer, Granada, Spain, 2019).
Qin, Y. et al. Airwaynet: a voxel-connectivity aware approach for accurate airway segmentation using convolutional neural networks. In Medical Image Computing and Computer-Assisted Intervention – MICCAI 2019 of Lecture Notes in Computer Science, 11769; 212–220 (Springer, Shenzhen, China, 2019).
He, K., Zhang, X., Ren, S. & Sun, J. Deep residual learning for image recognition. In Proceedings of the IEEE Conference on Computer Vision and Pattern Recognition (CVPR), 770–778 (IEEE, Las Vegas, Nevada, USA, 2016).
Yang, X. et al. Deciphering age- and sex-specific patterns of coronary artery atherosclerosis from a large chinese cohort. PS-CTA-Plaque-Atlas https://doi.org/10.5281/zenodo.16741227 (2025).
Rui Li, D. W. & Bingzhen L. Image processing method, device, equipment and storage medium. China Patent CN111815599B. Available at: https://patents.google.com/patent/CN111815599B/en?oq=CN111815599B. (2023).
Jiahao Li, D. W. F. Y. B. L., P Dong. Image segmentation method and computer-readable storage medium. China Patent CN113902693A. Available at: https://patents.google.com/patent/CN113902693A/en?oq=CN113902693A. (2022).
Acknowledgements
We gratefully acknowledge the support of Beijing Natural Science Foundation (No. Z210013) (Y.W., D.W.), National Key Research and Development Program of China (No. 2022YFE0209800) (D.W.), National Natural Science Foundation of China (Nos. U23A20295 (D.S.), 82441023 (D.S.), 62131015 (D.S.), 22322816 (Y.D.), 82471982 (J.Z.), 62471418 (Q.H.)), the InnoHK initiative of the Innovation and Technology Commission of the Hong Kong Special Administrative Region Government, Shanghai Municipal Central Guided Local Science and Technology Development Fund (No. YDZX20233100001001) (D.S.), Key Project of Shanghai Municipal Education Commission (No. 2024AIZD017) (J.Z.), City University of Hong Kong Project (No. 9610640) (Y.D.), and HPC Platform of ShanghaiTech University (D.S.).
Author information
Authors and Affiliations
Contributions
D.S. conceived the idea. X.Y., Y.S., Y.W., D.W. and D.S. designed the study. J.Z., Y.S. and D.W. collected and curated the data. X.Y. and Y.S. implemented and performed the experiments. X.Y., J.Z., Y.S., D.J., Q.H., Y.Z., X.S.Z., Y.D. and D.W. analyzed the data and interpreted the results. X.Y. and D.W. wrote the paper. All the authors reviewed, edited and approved the paper.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks the anonymous reviewers for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Yang, X., Zhang, J., Song, Y. et al. Deciphering age- and sex-specific patterns of coronary artery atherosclerosis from a large Chinese cohort. Nat Commun 16, 10616 (2025). https://doi.org/10.1038/s41467-025-64940-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-025-64940-8