Abstract
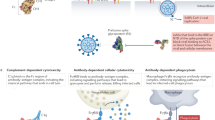
Respiratory viral infections, such as influenza and COVID-19, pose significant global health challenges. For patients with invasive pulmonary aspergillosis, a subsequent viral infection can lead to markedly worse clinical outcomes. Although amphotericin B (AmB) remains a cornerstone antifungal therapy, our investigation demonstrates that it paradoxically enhances the entry of influenza A virus and SARS-CoV-2. Mechanistically, AmB directly binds to and activates glucocerebrosidase, leading to ceramide accumulation and RAB7 upregulation in the late endosomes, thereby enhancing late endosomal maturation and fusion with viruses. In animal models, AmB treatment enhances viral infection in both influenza A virus–infected mice and SARS-CoV-2–challenged hamsters, resulting in accelerated weight loss, higher viral loads, and aggravated tissue damage. Consistently, in our propensity score-matched cohort of patients with culture-confirmed invasive pulmonary aspergillosis (2016–2025, n = 1,072), systemic use of AmB is associated with a significantly higher incidence of subsequent viral infection compared to other antifungals (21.55% vs. 7.76%, P = 0.003), which is further supported by multivariable analysis confirming AmB as an independent risk factor (adjusted OR = 3.45, 95% CI 2.20–5.41, P = 7.174 × 10-8). In summary, our findings provide crucial clinical evidence to guide antifungal therapy and reveal glucocerebrosidase as a potential target for developing novel antiviral strategies.
Similar content being viewed by others
Data availability
The mass spectrometry proteomics data generated in this study have been deposited in the ProteomeXchange Consortium under accession codes PXD064601 and PXD064637. The targeted lipidomics data are provided in Supplementary Data 1. Raw lipidomics instrument files are unavailable due to third-party intellectual property restrictions associated with the service provider (LipidALL Technologies), but the provided quantitative dataset is sufficient to interpret and validate the reported findings. Patient clinical data are not publicly available to strictly comply with data privacy laws and ethical regulations protecting patient confidentiality. However, de-identified clinical data will be made available to researchers upon reasonable request. Access requests should be submitted to the corresponding author and must include a research proposal and a signed Data Use Agreement. The corresponding author will review requests in accordance with the ethics committee’s requirements and respond within 4 weeks. All other data supporting the findings of this study are available within the article, its Supplementary Information, or the Source Data file. Source data are provided with this paper.
References
World Health Organization. The burden of influenza. Available at: https://www.who.int/news-room/feature-stories/detail/the-burden-of-influenza. (Accessed: 2025).
World Health Organization. WHO COVID-19 dashboard. Available at: https://data.who.int/dashboards/covid19. (Accessed: 2025).
Schauwvlieghe, A. et al. Invasive aspergillosis in patients admitted to the intensive care unit with severe influenza: a retrospective cohort study. Lancet Respir. Med. 6, 782–792 (2018).
Gangneux, J. P. et al. Fungal infections in mechanically ventilated patients with COVID-19 during the first wave: the French multicentre MYCOVID study. Lancet Respir. Med. 10, 180–190 (2022).
Prattes, J. et al. Risk factors and outcome of pulmonary aspergillosis in critically ill coronavirus disease 2019 patients-a multinational observational study by the European Confederation of Medical Mycology. Clin. Microbiol. Infect. 28, 580–587 (2022).
Janssen, N. A. F. et al. Multinational observational cohort study of COVID-19-associated pulmonary aspergillosis(1). Emerg. Infect. Dis. 27, 2892–2898 (2021).
Feys, S. et al. A visual and comprehensive review on COVID-19-associated pulmonary Aspergillosis (CAPA). J. Fungi 7 https://doi.org/10.3390/jof7121067 (2021).
Patel, A. et al. Multicenter epidemiologic study of coronavirus disease-associated mucormycosis, India. Emerg. Infect. Dis. 27, 2349–2359 (2021).
Xie, M. et al. SARS-CoV-2 coinfection in patients with invasive pulmonary aspergillosis: clinical characteristics and prognosis. Ann. Clin. Microbiol. Antimicrob. 24, 38 (2025).
Muthu, V. et al. Definition, diagnosis, and management of COVID-19-associated pulmonary mucormycosis: Delphi consensus statement from the Fungal Infection Study Forum and Academy of Pulmonary Sciences, India. Lancet Infect. Dis. 22, e240–e253 (2022).
Feys, S. et al. Influenza-associated and COVID-19-associated pulmonary aspergillosis in critically ill patients. Lancet Respir. Med. 12, 728–742 (2024).
Umegawa, Y. et al. Amphotericin B assembles into seven-molecule ion channels: An NMR and molecular dynamics study. Sci. Adv. 8, eabo2658 (2022).
Sawaya, B. P., Briggs, J. P. & Schnermann, J. Amphotericin B nephrotoxicity: the adverse consequences of altered membrane properties. J. Am. Soc. Nephrol. 6, 154–164 (1995).
Xu, F. et al. Amphotericin B inhibits enterovirus 71 replication by impeding viral entry. Sci. Rep. 6, 33150 (2016).
Al-Khikani, F. H. O. Amphotericin B as antiviral drug: possible efficacy against COVID-19. Ann. Thorac. Med. 15, 118–124 (2020).
Xing, Y. et al. Multifaceted functions of host cell caveolae/caveolin-1 in virus infections. Viruses 12 https://doi.org/10.3390/v12050487 (2020).
Pleskoff, O., Seman, M. & Alizon, M. Amphotericin B derivative blocks human immunodeficiency virus type 1 entry after CD4 binding: effect on virus-cell fusion but not on cell-cell fusion. J. Virol. 69, 570–574 (1995).
Lin, T. Y. et al. Amphotericin B increases influenza A virus infection by preventing IFITM3-mediated restriction. Cell Rep. 5, 895–908 (2013).
Zheng, M. et al. Bat SARS-Like WIV1 coronavirus uses the ACE2 of multiple animal species as receptor and evades IFITM3 restriction via TMPRSS2 activation of membrane fusion. Emerg. Microbes Infect. 9, 1567–1579 (2020).
Nguyen, D. et al. SARS-CoV-2 infection enhancement by amphotericin B: implications for disease management. J. Virol. 99, e0051925 (2025).
Virág, E. et al. Repurposed nystatin to inhibit SARS-CoV-2 and mutants in the GI tract. bioRxiv, 2021.2010.2019.464931 https://doi.org/10.1101/2021.10.19.464931 (2021).
Jiménez-Munguía, I., Beaven, A. H., Blank, P. S., Sodt, A. J. & Zimmerberg, J. Interferon-induced transmembrane protein 3 (IFITM3) and its antiviral activity. Curr. Opin. Struct. Biol. 77, 102467 (2022).
Rust, M. J., Lakadamyali, M., Zhang, F. & Zhuang, X. Assembly of endocytic machinery around individual influenza viruses during viral entry. Nat. Struct. Mol. Biol. 11, 567–573 (2004).
de Vries, E. et al. Dissection of the influenza A virus endocytic routes reveals macropinocytosis as an alternative entry pathway. PLoS Pathog. 7, e1001329 (2011).
Mercer, J., Schelhaas, M. & Helenius, A. Virus entry by endocytosis. Annu Rev. Biochem 79, 803–833 (2010).
White, J. M. & Whittaker, G. R. Fusion of Enveloped Viruses in Endosomes. Traffic 17, 593–614 (2016).
Sakai, T. et al. Dual wavelength imaging allows analysis of membrane fusion of influenza virus inside cells. J. Virol. 80, 2013–2018 (2006).
Sun, X. et al. Constitutively expressed IFITM3 protein in human endothelial cells poses an early infection block to human influenza viruses. J. Virol. 90, 11157–11167 (2016).
Kagan, S. et al. Toxicity mechanisms of amphotericin B and its neutralization by conjugation with arabinogalactan. Antimicrob. Agents Chemother. 56, 5603–5611 (2012).
Jackson, C. B., Farzan, M., Chen, B. & Choe, H. Mechanisms of SARS-CoV-2 entry into cells. Nat. Rev. Mol. Cell Biol. 23, 3–20 (2022).
Yang, B. et al. SNX27 suppresses SARS-CoV-2 infection by inhibiting viral lysosome/late endosome entry. Proc. Natl. Acad. Sci. USA 119 https://doi.org/10.1073/pnas.2117576119 (2022).
Thankamani, K. et al. Middle East respiratory syndrome coronavirus (MERS-CoV) internalization does not rely on DPP4 cytoplasmic tail signaling. Npj Viruses 2, 67 (2024).
Vertut-Doï, A., Ohnishi, S. I. & Bolard, J. The endocytic process in CHO cells, a toxic pathway of the polyene antibiotic amphotericin B. Antimicrob. Agents Chemother. 38, 2373–2379 (1994).
Boer, D. E. C., van Smeden, J., Bouwstra, J. A. & Aerts, J. Glucocerebrosidase: functions in and beyond the lysosome. J. Clin. Med. 9 https://doi.org/10.3390/jcm9030736 (2020).
Lauwers, E., Goodchild, R. & Verstreken, P. Membrane lipids in presynaptic function and disease. Neuron 90, 11–25 (2016).
Mulligan, R. J. & Winckler, B. Regulation of endosomal trafficking by Rab7 and its effectors in neurons: clues from Charcot-Marie-Tooth 2B Disease. Biomolecules 13 https://doi.org/10.3390/biom13091399 (2023).
Drews, K. et al. Glucosylceramidase maintains influenza virus infection by regulating endocytosis. J. Virol. 93 https://doi.org/10.1128/jvi.00017-19 (2019).
Drews, K. et al. Glucosylceramide synthase maintains influenza virus entry and infection. PLoS One 15, e0228735 (2020).
Finnegan, C. M. & Blumenthal, R. Fenretinide inhibits HIV infection by promoting viral endocytosis. Antivir. Res 69, 116–123 (2006).
Audi, A., Soudani, N., Dbaibo, G. & Zaraket, H. Depletion of host and viral sphingomyelin impairs influenza virus infection. Front Microbiol 11, 612 (2020).
Schloer, S. et al. The clinically licensed antifungal drug itraconazole inhibits influenza virus in vitro and in vivo. Emerg. Microbes Infect. 8, 80–93 (2019).
Van Damme, E. et al. In vitro activity of itraconazole against SARS-CoV-2. J. Med Virol. 93, 4454–4460 (2021).
Wang, P. G., Tang, D. J., Hua, Z., Wang, Z. & An, J. Sunitinib reduces the infection of SARS-CoV, MERS-CoV and SARS-CoV-2 partially by inhibiting AP2M1 phosphorylation. Cell Discov. 6, 71 (2020).
Celestino, I. et al. Differential redox state contributes to sex disparities in the response to influenza virus infection in male and female mice. Front Immunol. 9, 1747 (2018).
Dhakal, S. et al. Sex differences in lung imaging and SARS-CoV-2 antibody responses in a COVID-19 golden syrian hamster model. mBio 12, e0097421 (2021).
Wang, H. et al. NF-κB and FosB mediate inflammation and oxidative stress in the blast lung injury of rats exposed to shock waves. Acta Biochim. Biophys. Sin. 53, 283–293 (2021).
Wang, Z. et al. ACE2 can act as the secondary receptor in the FcγR-dependent ADE of SARS-CoV-2 infection. iScience 25, 103720 (2022).
Matlin, K. S., Reggio, H., Helenius, A. & Simons, K. Infectious entry pathway of influenza virus in a canine kidney cell line. J. Cell Biol. 91, 601–613 (1981).
Kumar, N. et al. Identification of diphenylurea derivatives as novel endocytosis inhibitors that demonstrate broad-spectrum activity against SARS-CoV-2 and influenza A virus both in vitro and in vivo. PLoS Pathog. 19, e1011358 (2023).
Banerjee, I. et al. Influenza A virus uses the aggresome processing machinery for host cell entry. Science 346, 473–477 (2014).
Ma, L., Ouyang, Q., Werthmann, G. C., Thompson, H. M. & Morrow, E. M. Live-cell Microscopy and Fluorescence-based Measurement of Luminal pH in Intracellular Organelles. Front Cell Dev. Biol. 5, 71 (2017).
de Araùjo, M. E., Huber, L. A. & Stasyk, T. Isolation of endocitic organelles by density gradient centrifugation. Methods Mol. Biol. 424, 317–331 (2008).
Song, J. W. et al. Omics-driven systems interrogation of metabolic dysregulation in COVID-19 pathogenesis. Cell Metab. 32, 188–202.e185 (2020).
Acknowledgements
We thank Dr. Linqi Zhang and Dr. Xuanling Shi from Tsinghua University for providing the plasmids CMV/R‑HA and CMV/R‑N1NA; Dr. Ning Jiao and Dr. Xiaodong Dou from Peking University for their discussions on the experimental framework; Dr. Hui Wang from Peking University People’s Hospital for her comments on the manuscript; Dr. Xiaoying Gu and Dr. Rongling Zhang from China-Japan Friendship Hospital for their suggestions on statistical analysis; Dr. Fei Zhu from Xiangya Hospital for assistance with chemical structures; and Wenqing He from China Medical University for help with figure preparation and data verification. The work was supported by the National Natural Science Foundation of China (Nos. 82241056 and 82530002 to B.C., Nos. 82170015 and 82570008 to Z.W., No. 824B2001 to W.Z.), the Chinese Academy of Medical Sciences (CAMS) Innovation Fund for Medical Sciences (Nos. CIFMS 2021-I2M-1-048 and 2024-I2M-ZD-011 to B.C.), the Excellence & Innovation Initiative of China-Japan Friendship Hospital (No. ZRZC2025-KCB03 to Z.W.), the New Cornerstone Science Foundation (to B.C.), and the Fundamental Research Funds for the Central Universities (No. APL24200210010302003 to W.Z.).
Author information
Authors and Affiliations
Contributions
B.C., Z.W., and P.W. conceived and supervised the study. Z.W. and M.L. designed the experimental framework. D.H., W.Z., Y.H., Y.Y., W.W., and Y.L. carried out the in vitro cellular experiments. H.L., Q.F., X.L., and Yun Z. performed the molecular biology assays. Z.X., W.T., and Ying Z. executed the animal infection studies. D.H., J.Z., X.Z., and D.P. collected and analyzed the clinical coinfection data. D.H. and W.Z. conducted data analysis and drafted the manuscript. B.C., Z.W., and W.Z. obtained funding for the study. All authors contributed to the manuscript preparation and approved the final version.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Indranil Banerjee and the other anonymous reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
He, D., Zuo, W., Xiang, Z. et al. Amphotericin B promotes respiratory viral entry by enhancing late endosomal maturation and fusion via glucocerebrosidase-mediated ceramide remodeling. Nat Commun (2026). https://doi.org/10.1038/s41467-026-70095-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-026-70095-x