Abstract
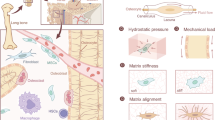
Bone’s ability to adapt to mechanical demands is governed by mechanoregulation, the process by which cells sense and respond to mechanical stimuli to maintain skeletal integrity. In osteoporosis, increased bone resorption activity leads to structural deterioration and elevated fracture risk. While existing pharmacological therapies aim to restore bone mass to reduce fracture risk, it is unclear how they modulate mechanoregulation, especially when combined with physical interventions. Here, we investigate the joint effects of load-bearing physical and pharmacological treatment in a female mouse model of osteoporosis using longitudinal in vivo micro-computed tomography and computational mechanics. We demonstrate that mechanical loading additively and synergistically enhanced predicted strength, bone volume, and mechanoregulation parameters when combined with anabolic therapies (parathyroid hormone and sclerostin antibody) but not with anti-catabolic treatments (bisphosphonates). Increases in predicted strength are associated with reductions in bone resorption rates, shifts in the (re)modeling thresholds as anticipated by Frost in the mechanostat theory, and the modeling capacity of anabolic pharmacological treatments. These findings underscore the therapeutic potential of combining anabolic pharmacological therapies with load-bearing physical activity, particularly in early treatment phases, to optimize bone adaptation and fracture prevention in osteoporosis management.
Similar content being viewed by others
Data availability
The primary data supporting the findings of this study are available within the paper. The raw data generated during the study are available in a Zenodo repository (see link below). Source data are provided with this paper.
Code availability
All data and code are available in a Zenodo repository: https://doi.org/10.5281/zenodo.17256047.
References
Kanis, J. A. et al. A reference standard for the description of osteoporosis. Bone 42, 467–475 (2008).
Schumm, A. K. et al. Does adding exercise or physical activity to pharmacological osteoporosis therapy in patients with increased fracture risk improve bone mineral density and lower fracture risk? A systematic review and meta-analysis. Osteoporos. Int 34, 1867–1880 (2023).
Kim, S. W. et al. Sclerostin antibody administration converts bone lining cells into active osteoblasts. J. Bone Miner. Res. 32, 892–901 (2017).
Duan, P. & Bonewald, L. F. The role of the wnt/beta-catenin signaling pathway in formation and maintenance of bone and teeth. Int J. Biochem. Cell Biol. 77, 23–29 (2016).
Kim J. M., Lin C., Stavre Z., Greenblatt M. B., Shim J. H. Osteoblast-osteoclast communication and bone homeostasis. Cells 9, 2073 (2020).
Schulte, F. A. et al. Local mechanical stimuli regulate bone formation and resorption in mice at the tissue level. PLoS One 8, e62172 (2013).
Dell, R. M. et al. Incidence of atypical nontraumatic diaphyseal fractures of the femur. J. Bone Min. Res 27, 2544–2550 (2012).
Kulkarni, N. H. et al. Effects of parathyroid hormone on WNT signaling pathway in bone. J. Cell Biochem 95, 1178–1190 (2005).
Sugiyama, T. et al. Mechanical loading enhances the anabolic effects of intermittent parathyroid hormone (1-34) on trabecular and cortical bone in mice. Bone 43, 238–248 (2008).
Rooney, A. M., McNeill, T. J., Ross, F. P., Bostrom, M. P. G. & van der Meulen, M. C. H. PTH treatment increases cortical bone mass more in response to compression than tension in mice. J. Bone Miner. Res. 38, 59–69 (2023).
Baron, R. & Kneissel, M. WNT signaling in bone homeostasis and disease: from human mutations to treatments. Nat. Med. 19, 179–192 (2013).
Ominsky, M. S., Boyce, R. W., Li, X. & Ke, H. Z. Effects of sclerostin antibodies in animal models of osteoporosis. Bone 96, 63–75 (2017).
Robling, A. G. et al. Mechanical stimulation of bone in vivo reduces osteocyte expression of Sost/sclerostin. J. Biol. Chem. 283, 5866–5875 (2008).
Rauner M., Taipaleenmaki H., Tsourdi E., Winter E. M. Osteoporosis treatment with anti-sclerostin antibodies-mechanisms of action and clinical application. J. Clin. Med. 10, 787 (2021).
Frost, H. M. The mechanostat: a proposed pathogenic mechanism of osteoporoses and the bone mass effects of mechanical and nonmechanical agents. Bone Min. 2, 73–85 (1987).
Frost, H. M. Bone “mass” and the “mechanostat”: a proposal. Anat. Rec. 219, 1–9 (1987).
Frost, H. M. Bone’s mechanostat: a 2003 update. Anat. Rec. A Discov. Mol. Cell Evol. Biol. 275, 1081–1101 (2003).
Lambers, F. M., Schulte, F. A., Kuhn, G., Webster, D. J. & Müller, R. Mouse tail vertebrae adapt to cyclic mechanical loading by increasing bone formation rate and decreasing bone resorption rate as shown by time-lapsed in vivo imaging of dynamic bone morphometry. Bone 49, 1340–1350 (2011).
Marques F. C. et al. Mechanostat parameters estimated from time-lapsed micro-computed tomography data of mechanically driven bone adaptation are logarithmically dependent on loading frequency. Front Bioeng Biotech 11, 1140673 (2023).
Christen, P. et al. Bone remodelling in humans is load-driven but not lazy. Nat. Commun. 5, 4855 (2014).
Griesbach, J. K., Schulte, F. A., Schadli, G. N., Rubert, M. & Müller, R. Mechanoregulation analysis of bone formation in tissue engineered constructs requires a volumetric method using time-lapsed micro-computed tomography. Acta Biomater 179, 149–163 (2024).
Taylor, S. et al. Time-dependent cellular and transcriptional changes in the osteoblast lineage associated with sclerostin antibody treatment in ovariectomized rats. Bone 84, 148–159 (2016).
Ominsky, M. S. et al. Romosozumab improves bone mass and strength while maintaining bone quality in ovariectomized cynomolgus monkeys. J. Bone Miner. Res. 32, 788–801 (2017).
Morse, A. et al. Sclerostin antibody augments the anabolic bone formation response in a mouse model of mechanical tibial loading. J. Bone Min. Res. 33, 486–498 (2018).
Morse, A. et al. Mechanical load increases in bone formation via a sclerostin-independent pathway. J. Bone Min. Res. 29, 2456–2467 (2014).
Witcher P. C. et al. Sclerostin neutralization unleashes the osteoanabolic effects of Dkk1 inhibition. JCI Insight 3, e98673 (2018).
Morse, A. et al. KO mice treated with sclerostin antibody have additional increases in bone volume. Calcif. Tissue Int. 103, 298–310 (2018).
Florio M. et al. A bispecific antibody targeting sclerostin and DKK-1 promotes bone mass accrual and fracture repair. Nat. Commun. 7, 11505 (2016).
Ryder, K. D. & Duncan, R. L. Parathyroid hormone modulates the response of osteoblast-like cells to mechanical stimulation. Calcif. Tissue Int 67, 241–246 (2000).
Hagino, H., Okano, T., Akhter, M. P., Enokida, M. & Teshima, R. Effect of parathyroid hormone on cortical bone response to in vivo external loading of the rat tibia. J. Bone Min. Metab. 19, 244–250 (2001).
Robinson, S. T., Shyu, P. T. & Guo, X. E. Mechanical loading and parathyroid hormone effects and synergism in bone vary by site and modeling/remodeling regime. Bone 153, 116171 (2021).
Uusi-Rasi, K. et al. Effect of alendronate and exercise on bone and physical performance of postmenopausal women: a randomized controlled trial. Bone 33, 132–143 (2003).
Kistler-Fischbacher, M., Yong, J. S., Weeks, B. K. & Beck, B. R. A comparison of bone-targeted exercise with and without antiresorptive bone medication to reduce indices of fracture risk in postmenopausal women with low bone mass: the MEDEX-OP randomized controlled trial. J. Bone Min. Res 36, 1680–1693 (2021).
Sims, N. A. & Martin, T. J. Osteoclasts provide coupling signals to osteoblast lineage cells through multiple mechanisms. Annu. Rev. Physiol. 82, 507–529 (2020).
Birkhold, A. I. et al. Mineralizing surface is the main target of mechanical stimulation independent of age: 3D dynamic in vivo morphometry. Bone 66, 15–25 (2014).
Schulte, F. A., Lambers, F. M., Kuhn, G. & Müller, R. In vivo micro-computed tomography allows direct three-dimensional quantification of both bone formation and bone resorption parameters using time-lapsed imaging. Bone 48, 433–442 (2011).
Birkhold, A. I. et al. Monitoring in vivo (re)modeling: a computational approach using 4D microCT data to quantify bone surface movements. Bone 75, 210–221 (2015).
Acevedo, C., Stadelmann, V. A., Pioletti, D. P., Alliston, T. & Ritchie, R. O. Fatigue as the missing link between bone fragility and fracture. Nat. Biomed. Eng. 2, 62–71 (2018).
Hernandez, C. J., Lambers, F. M., Widjaja, J., Chapa, C. & Rimnac, C. M. Quantitative relationships between microdamage and cancellous bone strength and stiffness. Bone 66, 205–213 (2014).
Lambers, F. M., Bouman, A. R., Rimnac, C. M. & Hernandez, C. J. Microdamage caused by fatigue loading in human cancellous bone: relationship to reductions in bone biomechanical performance. PLoS One 8, e83662 (2013).
Mathavan, N. et al. Spatial transcriptomics in bone mechanomics: exploring the mechanoregulation of fracture healing in the era of spatial omics. Sci. Adv. 11, eadp8496 (2025).
Duda, G. N. et al. The decisive early phase of bone regeneration. Nat. Rev. Rheumatol. 19, 78–95 (2023).
Lambers, F. M., Kuhn, G., Schulte, F. A., Koch, K. & Müller, R. Longitudinal assessment of in vivo bone dynamics in a mouse tail model of postmenopausal osteoporosis. Calcif. Tissue Int 90, 108–119 (2012).
Webster, D. J., Morley, P. L., van Lenthe, G. H. & Müller, R. A novel in vivo mouse model for mechanically stimulated bone adaptation-a combined experimental and computational validation study. Comput. Methods Biomech. Biomed. Engin 11, 435–441 (2008).
Scheuren, A. C. et al. Mechano-regulation of trabecular bone adaptation is controlled by the local in vivo environment and logarithmically dependent on loading frequency. Front. Bioeng. Biotechnol. 8, 566346 (2020).
Christen, P., van Rietbergen, B., Lambers, F. M., Müller, R. & Ito, K. Bone morphology allows estimation of loading history in a murine model of bone adaptation. Biomech. Model Mechanobiol. 11, 483–492 (2012).
Stadelmann, V. A., Bonnet, N. & Pioletti, D. P. Combined effects of zoledronate and mechanical stimulation on bone adaptation in an axially loaded mouse tibia. Clin. Biomech. 26, 101–105 (2011).
Alexander, J. M. et al. Human parathyroid hormone 1-34 reverses bone loss in ovariectomized mice. J. Bone Min. Res. 16, 1665–1673 (2001).
Bouxsein, M. L. et al. Guidelines for assessment of bone microstructure in rodents using micro-computed tomography. J. Bone Miner. Res. 25, 1468–1486 (2010).
Flaig, C. & Arbenz, P. A scalable memory efficient multigrid solver for micro-finite element analyses based on CT images. Parallel Comput 37, 846–854 (2011).
Pistoia, W. et al. Estimation of distal radius failure load with micro-finite element analysis models based on three-dimensional peripheral quantitative computed tomography images. Bone 30, 842–848 (2002).
Nyman, J. S. et al. Predicting mouse vertebra strength with micro-computed tomography-derived finite element analysis. Bonekey Rep. 4, 664 (2015).
R Core Team. R: a language and environment for statistical computing. In: R Foundation for Statistical Computing (Vienna, Austria, 2021).
Acknowledgements
We acknowledge Kathleen Koch for assistance and performance of animal experiments of the PTH and BIS groups, and Dr. Ulrike Kettenberger for assistance and performance of animal experiments of the PTH group. Nirujan Pasupathy and Júlia van den Nest Molina have supported the analyses of modeling and mechanoregulation mechanisms. This work was funded by the European Union grant VPHOP (FP7-ICT-2008-223865; FAS, FML, CW, GAK) and the European Research Council ERC Advanced grant (MechAGE ERC-2016-ADG-741883; FCM, GAK).
Funding
Open access funding provided by Swiss Federal Institute of Technology Zurich.
Author information
Authors and Affiliations
Contributions
RM, GAK, and PJR designed the experiment. CW, GAK, MS, and FML performed the experiments. FAS, FCM, JG, CW, MS, FML, and GAK performed image processing and analysis. MK provided pharmacological agents. RM, GAK, PJR, and CK supervised the project. FAS wrote the original draft of the manuscript. All authors contributed to data interpretation, were involved in discussions throughout the study, and participated in manuscript revision and preparation.
Corresponding author
Ethics declarations
Competing interests
MK, PJR, and CK are employees of Novartis. The other authors declare they have no competing interests.
Peer review
Peer review information
Nature Communications thanks Matthew Silva, and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Schulte, F.A., Marques, F.C., Griesbach, J.K. et al. Combined physical and pharmacological anabolic osteoporosis therapies increase bone response and mechanoregulation in female mice. Nat Commun (2026). https://doi.org/10.1038/s41467-026-70309-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-026-70309-2