Abstract
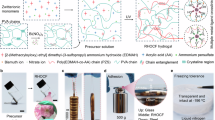
Over 30-40% of 1.5 million annual hand flexor tendon injuries in the United States result in peritendinous adhesions which limit range of motion (ROM) and severely impact quality of life. Currently, no widespread solution exists for adhesion prevention in the delicate space of the digit while allowing full ROM quickly following surgery. Here, we develop dynamically crosslinked, bioresorbable supramolecular hydrogels as easy-to-apply peritendinous adhesion barriers. These hydrogels exhibit long-term stability, injectability, and thermally stable viscoelastic properties that enable simple storage and application. Interactions at the interface of hydrogel and human tissues demonstrate maintenance of a lubricious hydrogel barrier between tissues. Ex vivo studies show cadaveric tendon biomechanics are unimpaired. Application in preclinical rat tendon injury reveals prolonged hydrogel retention and improved functional recovery, including ROM and maximal dorsiflexion. These hydrogels are safe, do not impair tendon healing, and present a scalable intervention to limit peritendinous adhesions with translational potential.
Similar content being viewed by others
Data availability
All source data generated are provided with this paper in the Source Data file. Source data are provided with this paper.
Code availability
All code supporting the findings of this study was deposited into a public GitHub repository (https://github.com/cmw290/preventing-peritendinous-adhesions, release tag 1.0, https://doi.org/10.5281/zenodo.18636339).
References
Legrand, A., Kaufman, Y., Long, C. & Fox, P. M. Molecular biology of flexor tendon healing in relation to reduction of tendon adhesions. J. Hand Surg. 42, 722–726 (2017).
Fenwick, S. A., Hazleman, B. L. & Riley, G. P. The vasculature and its role in the damaged and healing tendon. Arthritis Res. 4, 252–260 (2002).
Daley, B. J., Cecil, W., Clarke, C. P., Cofer, J. B. & Guillamondegui, O. D. How slow is too slow? Correlation of operative time to complications: an analysis from the Tennessee Surgical Quality Collaborative. J. Am. Coll. Surg. 220, 550 (2015).
Sikirica, V. et al. The inpatient burden of abdominal and gynecological adhesiolysis in the US. BMC Surg. 11, 13 (2011).
Docheva, D., Müller, S. A., Majewski, M. & Evans, C. H. Biologics for tendon repair. Adv. Drug Deliv. Rev. 84, 222–239 (2015).
Strickland, J. W. Flexor tendon injuries: I. Foundations of treatment. J. Am. Acad. Orthop. Surg. 3, 44 (1995).
Titan, A. L., Foster, D. S., Chang, J. & Longaker, M. T. Flexor tendon: development, healing, adhesion formation, and contributing growth factors. Plast. Reconstr. Surg. 144, 639e–647e (2019).
Chinchalkar, S. J., Larocerie-Salgado, J. & Suh, N. Pathomechanics and management of secondary complications associated with tendon adhesions following flexor tendon repair in zone II. J. Hand Microsurg. 8, 70–79 (2016).
Zhang, Q., Yang, Y., Yildirimer, L., Xu, T. & Zhao, X. Advanced technology-driven therapeutic interventions for prevention of tendon adhesion: design, intrinsic and extrinsic factor considerations. Acta Biomater. 124, 15–32 (2021).
Hohendorff, B. et al. Tenolysis of extensor and flexor tendons of the hand. Orthopäde. 49, 771–783 (2020).
Feldscher, S. B. & Schneider, L. H. Flexor tenolysis. Hand Surg. https://doi.org/10.1142/S0218810402000819 (2011).
Seppi, S., Vecchi, S., Raccagni, I., Novelli, C. & Pajardi, G. E. Pre- and post-treatment in flexor tendon tenolysis: an observational study. J. Hand Ther. https://doi.org/10.1016/j.jht.2023.10.004 (2024).
Starr, H. M., Snoddy, M., Hammond, K. E. & Seiler, J. G. Flexor tendon repair rehabilitation protocols: a systematic review. J. Hand Surg. 38, 1712–1717.e1714 (2013).
Lister, G. D., Kleinert, H. E., Kutz, J. E. & Atasoy, E. Primary flexor tendon repair followed by immediate controlled mobilization. J. Hand Surg. 2, 441–451 (1977).
Zhang, P. et al. Antiadhesion biomaterials in tendon repair: application status and future prospect. Tissue Eng. Part B: Rev. 31, 20–30 (2024).
Xu, P. J. et al. Advanced biomimetic materials in the prevention of tendon adhesions: design, preparation, and application of hydrogel and electrospun fiber membranes. Small 21, 2411913 (2025).
Zhou, H. & Lu, H. Advances in the development of anti-adhesive biomaterials for tendon repair treatment. Tissue Eng. Regen. Med. 18, 1–14 (2021).
Bassetto, F. et al. Efficacy and safety of dynavisc® gel in prevention of scar adhesions recurrence after flexor tendons tenolysis in zone 2. Multicenter retrospective cohort study. Ann. Ital. Chir. 94, 529–536 (2023).
von Kieseritzky, J., Rosengren, J. & Arner, M. Dynavisc as an adhesion barrier in finger phalangeal plate fixation—a prospective case series of 8 patients. J. Hand Surg. Glob. Online 2, 109–112 (2020).
Ishiyama, N. et al. The prevention of peritendinous adhesions by a phospholipid polymer hydrogel formed in situ by spontaneous intermolecular interactions. Biomaterials 31, 4009–4016 (2010).
Wang, K., Chen, D., Wang, Z., Yang, J. & Liu, W. An injectable and antifouling supramolecular polymer hydrogel with microenvironment-regulatory function to prevent peritendinous adhesion and promote tendon repair. Macromol. Biosci. 23, 2300142 (2023).
Chou, P.-Y. et al. Thermo-responsive in-situ forming hydrogels as barriers to prevent post-operative peritendinous adhesion. Acta Biomater. 63, 85–95 (2017).
Barzegar, P. E. F. et al. Graphene-MoS2 polyfunctional hybrid hydrogels for the healing of transected Achilles tendon. Biomater. Adv. 137, 212820 (2022).
Wu, R. et al. Injectable pH-responsive CI1040 delayed-release hydrogel for the treatment of tendon adhesion. Adv. Funct. Mater. 34, 2314731 (2024).
Luo, R. et al. Piezoelectric injectable anti-adhesive hydrogel to promote endogenous healing of tendon injuries. Adv. Mater. 37, 2501306 (2025).
Marchesini, A. et al. Effectiveness of hyaluronan autocross-linked-based gel in the prevention of peritendinous adherence following tenolysis. Appl. Sci. 11, 7613 (2021).
Tan, L. et al. Mechanically-adaptive Janus hydrogel enhances scarless tendon healing with tissue-adhesion prevention. Acta Biomater. 202, 170–192 (2025).
Freedman, B. R. et al. Enhanced tendon healing by a tough hydrogel with an adhesive side and high drug-loading capacity. Nat. Biomed. Eng. 6, 1167–1179 (2022).
Pascual-Antón, L. et al. Sprayable extracellular matrix hydrogel reduces postoperative adhesion formation and protects healing tissues in preclinical models. Sci. Transl. Med. 17, eadn3179 (2025).
Vinitpairot, C., Yik, J. H. N., Haudenschild, D. R., Szabo, R. M. & Bayne, C. O. Current trends in the prevention of adhesions after zone 2 flexor tendon repair. J. Orthop. Res. https://doi.org/10.1002/jor.25874 (2024).
Concha, V. O. C. et al. Harnessing electrospinning for improvement of polymeric drug delivery systems. Polym. Bull. 82, 5909–5943 (2025).
Wan, R. et al. 109. Comparing the postoperative adhesion prevention effectiveness of collagen-glycosaminoglycan (GAG), hyaluronic acid (HA), and pentamidine using a turkey in vivo model. Plast. Reconstr. Surg. Glob. Open 11, 68 (2023).
Turner, J. B., Corazzini, R. L., Butler, T. J., Garlick, D. S. & Rinker, B. D. Evaluating adhesion reduction efficacy of type I/III collagen membrane and collagen-GAG resorbable matrix in primary flexor tendon repair in a chicken model. HAND 10, 482–488 (2014).
McDermott, E. R., Bowers, Z. & Nuelle, J. A. The application of hyaluronic acid/alginate sheet to flexor pollicis longus tendon repair to prevent adhesion formation: a second look. Cureus 14, e33147 (2022).
McCahon, J. A. S., Bridges, T. N. & Parekh, S. G. Application of hyaluronic acid/alginate sheet to Achilles tendon injuries to prevent peritendinous adhesions. Tech. Foot Ankle Surg. 23, 184–187 (2024).
Wan, R. et al. Evaluating the effectiveness of commercially available antiadhesion tendon protector sheets in tendon repair surgery versus tendon repair surgery alone: a preclinical model study. J. Hand Surg. 50, 1009.e1001–1009.e1010 (2025).
Adu, Y. et al. Evaluating the effect of VersaWrap tendon protector on functional outcomes in operative tendon repairs. Front. Surg. https://doi.org/10.3389/fsurg.2024.1447515 (2024).
Bridges, T. N., McCahon, J. A. & Parekh, S. G. Surgical arthroscopy with intra-articular hyaluronic acid/alginate adjunct in the treatment of ankle osteoarthritis. Tech. Foot Ankle Surg. 23, 204 (2024).
Research, S. A Single-Center, Prospective, Clinical Study of VersaWrap Utilization in the Hand. Report No. NCT05598801 (clinicaltrials.gov, 2025).
University of, F. Prospective Randomized Blinded Trial of VersaWrap Tendon Protector for Zone 2 Flexor Tendon Injuries. Report No. NCT04322370 (clinicaltrials.gov, 2025).
University of Colorado, D. Quantitative and Clinical Assessment of Flexor Tendon Gliding Following Application of a Bioresorbable Hydrogel: A Prospective, Randomized Study in Patients Undergoing Distal Radius Fracture Repair. Report No. NCT04976335 (clinicaltrials.gov, 2024).
Bindra, R. & McCoy, N. A First-in human study evaluating the safety and efficacy of TYBR Health B3 GEL in Flexor or Extensor Tendon Tenolysis. anzctr.org.au Registration Number: ACTRN12625000522415. Updated May 26, 2025. Accessed December 17, 2025. https://anzctr.org.au/Trial/Registration/TrialReview.aspx?id=389346.
Voleti, P. B., Buckley, M. R. & Soslowsky, L. J. Tendon healing: repair and regeneration. Annu. Rev. Biomed. Eng. 14, 47–71 (2012).
Appel, E. A. et al. Self-assembled hydrogels utilizing polymer–nanoparticle interactions. Nat. Commun. 6, 6295 (2015).
Stapleton, L. M. et al. Use of a supramolecular polymeric hydrogel as an effective post-operative pericardial adhesion barrier. Nat. Biomed. Eng. 3, 611–620 (2019).
Stapleton, L. M. et al. Dynamic hydrogels for prevention of post-operative peritoneal adhesions. Adv. Therap. 4, 2000242 (2021).
Song, Y. E. et al. Highly extensible physically crosslinked hydrogels for high-speed 3D bioprinting. Adv. Healthcare Mater. 14, 2404988 (2025).
Eckman, N. & Appel, E. A. Crosslink dynamics control injection force and flow profiles of non-covalent gels. Macromolecules 58, 6350–6358 (2025).
Banasiewicz, T. et al. Preliminary study with SprayShield™ adhesion barrier system in the prevention of abdominal adhesions. Wideochir. Inne Tech. Maloinwazyjne 8, 301–309 (2013).
Aldawsari, H. et al. Combined use of cyclodextrins and hydroxypropylmethylcellulose stearoxy ether (Sangelose®) for the preparation of orally disintegrating tablets of type-2 antidiabetes agent glimepiride. J. Incl. Phenom. Macrocycl. Chem. 80, 61–67 (2014).
Liang, Y.-K., Cheng, W.-T., Chen, L.-C., Sheu, M.-T. & Lin, H.-L. Development of a swellable and floating gastroretentive drug delivery system (sfGRDDS) of ciprofloxacin hydrochloride. Pharmaceutics 15, 1428 (2023).
Griffin, M., Hindocha, S., Jordan, D., Saleh, M. & Khan, W. Management of extensor tendon injuries. Open Orthop. J. https://doi.org/10.2174/1874325001206010036 (2012).
Pearce, O., Brown, M. T., Fraser, K. & Lancerotto, L. Flexor tendon injuries: repair & rehabilitation. Injury 52, 2053–2067 (2021).
Grimaldo Ruiz, O. et al. Finite element analysis of the flexor digitorum profundus tendon during a passive rehabilitation protocol. Rev. Fac. Ing. Univ. Antioq. https://doi.org/10.17533/udea.redin.20210528 (2021).
Ugbolue, U. C., Hsu, W.-H., Goitz, R. J. & Li, Z.-M. Tendon and nerve displacement at the wrist during finger movements. Clin. Biomech. 20, 50–56 (2005).
Sapienza, A., Yoon, H. K., Karia, R. & Lee, S. K. Flexor tendon excursion and load during passive and active simulated motion: a cadaver study. J. Hand Surg. 38, 964–971 (2013).
Napoleone, C. P. et al. An observational study of CoSeal® for the prevention of adhesions in pediatric cardiac surgery☆☆☆. Interact. Cardiovasc. Thorac. Surg. 9, 978–982 (2009).
Zhang, Q., Li, X. & Jasti, B. R. Role of physicochemical properties of some grades of hydroxypropyl methylcellulose on in vitro mucoadhesion. Int. J. Pharm. 609, 121218 (2021).
Jons, C. K. et al. Yield-stress and creep control depot formation and persistence of injectable hydrogels following subcutaneous administration. Adv. Funct. Mater. 32, 2203402 (2022).
Ryan, G. B., Grobéty, J. & Majno, G. Postoperative peritoneal adhesions. A study of the mechanisms. Am. J. Pathol. 65, 117–148 (1971).
Luotonen, O. I. V. et al. Benchmarking supramolecular adhesive behavior of nanocelluloses, cellulose derivatives and proteins. Carbohydr. Polym. 292, 119681 (2022).
Tudoroiu, E.-E. et al. An overview of cellulose derivatives-based dressings for wound-healing management. Pharmaceuticals 14, 1215 (2021).
Fox, P. M. et al. Decellularized human tendon-bone grafts for composite flexor tendon reconstruction: a cadaveric model of initial mechanical properties. J. Hand Surg. Am. 38, 2323–2328 (2013).
Stevens, K. A., Caruso, J. C., Fallahi, A.-K. M. & Patiño, J. M. Flexor Tendon Lacerations. StatPearls (ed. Patiño, J. M.) (StatPearls Publishing, 2023).
McCarthy, D. M., Boardman, N. D., Tramaglini, D. M., Sotereanos, D. G. & Herndon, J. H. Clinical management of partially lacerated digital flexor tendons: a surgery of hand surgeons. J. Hand Surg. 20, 273–275 (1995).
Varejão, A. S. P. et al. Motion of the foot and ankle during the stance phase in rats. Muscle Nerve 26, 630–635 (2002).
Chamberlain, C. S. et al. Temporal healing in rat Achilles tendon: ultrasound correlations. Ann. Biomed. Eng. 41, 477–487 (2013).
Huegel, J. et al. Quantitative comparison of three rat models of Achilles tendon injury: a multidisciplinary approach. J. Biomech. 88, 194–200 (2019).
Khayyeri, H. et al. Achilles tendon compositional and structural properties are altered after unloading by Botox. Sci. Rep. 7, 13067 (2017).
de Oliveira, R. R. et al. Mechanical properties of Achilles tendon in rats induced to experimental diabetes. Ann. Biomed. Eng. 39, 1528–1534 (2011).
Murrell, G. A. C., Jang, D., Deng, X.-H., Hannafin, J. A. & Warren, R. F. Effects of exercise on Achilles tendon healing in a rat model. Foot Ankle Int. 19, 598–603 (1998).
Eliasson, P., Andersson, T. & Aspenberg, P. Rat Achilles tendon healing: mechanical loading and gene expression. J. Appl. Physiol. 107, 399–407 (2009).
Szewczyk, P. K. & Stachewicz, U. The impact of relative humidity on electrospun polymer fibers: from structural changes to fiber morphology. Adv. Colloid Interface Sci. 286, 102315 (2020).
Nezarati, R. M., Eifert, M. B. & Cosgriff-Hernandez, E. Effects of humidity and solution viscosity on electrospun fiber morphology. Tissue Eng. Part C. Methods 19, 810–819 (2013).
Jiang, Y., Zhu, C., Ma, X. & Fan, D. Smart hydrogel-based trends in future tendon injury repair: a review. Int. J. Biol. Macromol. 282, 137092 (2024).
Foster, D. S. et al. Postoperative adhesions are abrogated by a sustained-release anti-JUN therapeutic in preclinical models. Sci. Transl. Med. 17, eadp9957 (2025).
Chang, J., Thunder, R., Most, D., Longaker, M. T. & Lineaweaver, W. C. Studies in flexor tendon wound healing: neutralizing antibody to TGF-β1 increases postoperative range of motion. Plast. Reconstr. Surg. 105, 148 (2000).
De Wilde, R. L. et al. The future of adhesion prophylaxis trials in abdominal surgery: an expert global consensus. J. Clin. Med. 11, 1476 (2022).
Potenza, A. D. Tendon healing within the flexor digital sheath in the dog: an experimental study. JBJS 44, 49 (1962).
Boz, M. et al. Does methylene blue reduce adhesion during the healing process after tendon repair? Jt. Dis. Relat. Surg. 31, 246–254 (2020).
Zhao, C. et al. Effects of a lubricin-containing compound on the results of flexor tendon repair in a canine model in vivo. JBJS 92, 1453 (2010).
Karakurum, G., Buyukbebeci, O., Kalender, M. & Gulec, A. Seprafilm® interposition for preventing adhesion formation after tenolysis: an experimental study on the chicken flexor tendons. J. Surg. Res. 113, 195–200 (2003).
Liang, J.-I. et al. Video-based gait analysis for functional evaluation of healing Achilles tendon in rats. Ann. Biomed. Eng. 40, 2532–2540 (2012).
Nakajima, T. et al. Grafting of iPS cell-derived tenocytes promotes motor function recovery after Achilles tendon rupture. Nat. Commun. 12, 5012 (2021).
Correa, S., Grosskopf, A. K., Klich, J. H., Hernandez, H. L. & Appel, E. A. Injectable liposome-based supramolecular hydrogels for the programmable release of multiple protein drugs. Matter 5, 1816–1838 (2022).
Meany, E. L. et al. Injectable polymer-nanoparticle hydrogel for the sustained intravitreal delivery of bimatoprost. Adv. Therap. 6, 2200207 (2023).
Ou, B. S. et al. Broad and durable humoral responses following single hydrogel immunization of SARS-CoV-2 subunit vaccine. Adv. Healthc. Mater. 12, 2301495 (2023).
Han, G.-D. et al. Potent anti-adhesion agent using a drug-eluting visible-light curable hyaluronic acid derivative. J. Ind. Eng. Chem. 70, 204–210 (2019).
Kulick, M. I., Brazlow, R., Smith, S. & Hentz, V. R. Injectable ibuprofen: preliminary evaluation of its ability to decrease peritendinous adhesions. Ann. Plast. Surg. 13, 459 (1984).
Liu, S. et al. Prevention of peritendinous adhesions with electrospun ibuprofen-loaded poly(l-Lactic Acid)-polyethylene glycol fibrous membranes. Tissue Eng. Part A 19, 529–537 (2013).
Branford, O. A., Klass, B. R., Grobbelaar, A. O. & Rolfe, K. J. The growth factors involved in flexor tendon repair and adhesion formation. J. Hand Surg. 39, 60–70 (2014).
Mao, W. F. et al. Modulation of digital flexor tendon healing by vascular endothelial growth factor gene transfection in a chicken model. Gene Ther. 24, 234–240 (2017).
Meany, E. L. et al. Generation of an inflammatory niche in a hydrogel depot through recruitment of key immune cells improves efficacy of mRNA vaccines. Sci. Adv. 11, eadr2631 (2025).
Williams, C. M., Meany, E. L. & Appel, E. A. Preventing-peritendinous-adhesions. Zenodo https://doi.org/10.5281/zenodo.18636339 (2026).
Fryhofer, G. W. et al. Postinjury biomechanics of Achilles tendon vary by sex and hormone status. J. Appl. Physiol. 121, 1106–1114 (2016).
Charles River Laboratories. C57BL/6 mouse model information sheet. https://www.criver.com/resources/c57bl6-mouse-model-information-sheet (2019).
Acknowledgements
E.L.M. was supported by the NIH Biotechnology Training Program (T32-GM008412). C.M.W., C.K.J., and S.C.W. were supported by the National Science Foundation Graduate Research Fellowship (Award Number DGE-2146755). S.C.W. was supported by the Sarafan ChEM-H Chemistry/Biology Interface training program. The authors would like to thank every member of the Appel Lab, former and current, for their on-going support, technical expertise, and scientific discussion. In particular, the authors thank Noah Eckman and Samya Sen for their contributions to theorizing calculations, and Noah Eckman for assistance socializing animals. The authors would also like to thank Prof. Dauskardt and lab members for training on and use of their MTS instrument. Histological analysis was performed by Dr. José Vilches-Moure, DVM, PhD, with Stanford’s Veterinary Service Center Comparative Pathology services. Part of this work was performed at nano@stanford (RRID:SCR_026695).
Author information
Authors and Affiliations
Contributions
E.L.M., C.M.W., P.M.F., and E.A.A. conceptualized and designed the research; P.M.F. and E.A.A. supervised all work; E.L.M., C.M.W., Y.E.S., and P.M.F. contributed to methodology; E.L.M., C.M.W.,. V.M.D., A.A., S.J.B., S.C.W., C.K.J., and P.M.F. conducted experiments and C.M.W. coded software; E.L.M. and C.M.W. produced figures, data visualization, and wrote the manuscript with review and edits from S.J.B., S.C.W., P.M.F., and E.A.A.
Corresponding authors
Ethics declarations
Competing interests
E.A.A, Y.E.S., E.L.M., and C.M.W. are listed as inventors on a patent application describing the dynamic hydrogel technology reported in this manuscript (patent PCT/US2023/079149). E.A.A. is a co-founder equity holder, and advisor for Appel Sauce Studios LLC, which holds a global exclusive license to the technology reported in this manuscript. The remaining authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Cunyi Fan, who co-reviewed with Lingchi Kong, and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Meany, E.L., Williams, C.M., Song, Y.E. et al. Preventing peritendinous adhesions using lubricious supramolecular hydrogels. Nat Commun (2026). https://doi.org/10.1038/s41467-026-71244-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-026-71244-y