Abstract
Wearable sweat rate and electrolyte sensors offer real-time assessment of hydration status. Current epidermal microfluidic devices represent the widely adopted approach; however, their limitation for microliter-scale sweat collection often results in response latency and compromised detection accuracy. A rapid sweat-absorbing material (RSAM) filled in the collection chamber between the microfluidic device and the skin has been demonstrated as an effective solution. This work proposes a polyvinyl alcohol@polyurethane microfiber composite hydrogel (PVA@PU MH) with unidirectional sweat-transport capability in the inlet chamber of a microfluidic. The optimized PVA@PU MH exhibits a sweat collection efficiency that is 49.76 ± 6.75% higher than traditional methods. With anisotropic microchannels, PVA@PU MH leverages capillary action to confine sweat laterally and drive vertical transport directionally. Additionally, the integration of conductivity-sensing components within the microfluidic system enables the detection of both sweat rate and electrolyte concentration. A low-power unit was developed to process and wirelessly transmit real-time sweat data to mobile devices for continuous monitoring. The PVA@PU MH facilitated both faster sweat uptake and more physiologically representative analyte readings, as evidenced by a strong correlation with whole-body measurements. The proposed strategy rapidly acquires microliter sweat samples, substantially expanding wearable monitoring capabilities.
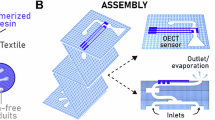
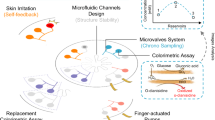
Similar content being viewed by others
Introduction
Sweating is a critical physiological process for human water-electrolyte balance1,2,3. Monitoring sweat rate and electrolyte concentration can provide insights into hydration status, enabling timely fluid replenishment and timely adjustment of exercise intensity4,5,6,7,8. However, traditional absorbent patch weighing methods are inconvenient, labor-intensive, and seriously hysteretic, which makes real-time sweat analysis impractical9,10. The emergence of flexible electronic wearables for in situ sweat monitoring is driving the need for personalized hydration strategies11,12,13,14,15.
Flexible electronics are now integrated with photometric, temperature, conductivity, and electrochemical sensing technologies. This integration enables the continuous and simultaneous measurement of both sweat rate and electrolyte concentrations. Consequently, it facilitates comprehensive hydration assessment16,17,18,19,20,21. In comparison, conductivity detection utilizing epidermal microfluidics offers a distinct advantage for decoupling sweat rate from electrolyte concentration5,22. Nevertheless, this configuration has a limitation that strong sweat-skin adhesion and prolonged microfluidic channel filling time cause response delays (>10 min), particularly for low sweat rate (<0.4 μL/(min cm2))20. Thus, rapid sweat transport methods are required to deliver trace epidermal sweat to microfluidic channels.
Rapid sweat-absorbing materials (RSAMs) with superior hydrophilicity to skin filled in the sweat collection chamber between the microfluidic and skin promote the ability to gather microliter-scale sweat23. Hydrophilic absorbent fibers are commonly used for collecting sweat at low secretion rates, and Janus membranes also demonstrate high sweat collection efficiency (>1 μL/(min cm²)). However, the intrinsic hydrophilic surface increases the flow resistance for sweat entering the microchannels24,25,26. Hydrogels exhibit exceptional sweat uptake capacity, enabling micro-sampling from fingertips at rates as low as 2 nL/min27,28,29,30. But the fabrication of reusable thin hydrogel films remains highly challenging, which significantly hinders their practical integration into wearable devices. Wedgy microstructures with directional liquid transport capability show promise (>0.2 μL), yet face fabrication and integration challenges31,32,33. Therefore, developing directional sweat transport structures with low flow resistance remains crucial.
Herein, a wearable device is presented for monitoring sweat rate and electrolyte concentration, integrating polyvinyl alcohol@polyurethane microfiber composite hydrogel (PVA@PU MH)-filled microfluidic, conductivity sensors, and signal processing circuitry. The PVA leads to the formation of anisotropic microchannels within the fibrous network while simultaneously decreasing porosity to 68.56%. The PVA@PU MH at the skin–microfluidic interface achieves directional permeation with a breakthrough pressure of only 0.176 kPa, significantly lower than that of conventional RSAMs (0.495–0.972 kPa). This enables highly efficient microliter-scale sweat collection. The PVA@PU MH was fabricated via mixed electrospinning, with optimized mass ratios of 25% PU and 3% PVA. The integrated microchannel with interdigitated electrodes enables dual-parameter detection. Integrated with low-power conductivity sensing and wireless transmission, the system monitored dynamic sweat metrics during exercise, achieving a 310-s faster response than the unfilled system. In summary, the design presented in this work offers advantages such as high sweat collection efficiency and simple fabrication (Table S1), making it promising for application in wearable sweat-sensing devices.
Results
Design of the wearable sweat detection system
Figure 1a presents the exploded view of the sweat sensor integrated with electrolyte concentration and perspiration rate monitoring, which consists of a multilayered architecture designed for sweat collection, detection, and signal transmission. The incorporation of the PVA@PU composite effectively mitigates the resistance encountered during sweat transport from the skin into the microfluidic channels (Fig. S1), thereby enhancing epidermal sweat uptake efficiency. This structural optimization significantly reduces the lag time (LT) required for sweat migration from the skin surface to the detection area, leading to an earlier onset of the effective time (ET), as demonstrated in Fig. 1b, c. During the effective time, whenever sweat traverses a designated trigger point, the equivalent circuit behaves as an additional activated parallel circuit, resulting in a stepwise increase in the overall conductance. The electrolyte concentration is derived from the amplitude analysis of the conductance signal, while the perspiration rate is determined by evaluating the temporal variation in conductance, as illustrated in Fig. S2.
a Exploded view of sweat sensor. b, c The PVA@PU MH enhances sweat collection rate and reduces the hysteresis time. d Top view of PVA@PU MH SEM. e Side view of PVA@PU MH SEM. f Schematic illustration of the force distribution of sweat in PVA@PU MH.
Figure 1d, e demonstrate detailed morphology of the PVA@PU MH, which reveals that PVA uniformly coats the PU fibers and reconstructs them into an interconnected network. Notably, vertically aligned PVA channels are formed within this hybrid structure. In conventional absorbent materials (e.g., fibrous substrates and hydrogel) and vertical-transport sweat collection structure (e.g., Janus membrane and Droplet self-driving structure), absorbed sweat tends to undergo isotropic diffusion driven by capillary forces, and microfluidic channel infiltration occurs only after full saturation of the absorbent matrix, which necessitates a high breakthrough pressure (Fig. S3). The Janus membrane typically comprises a skin-facing hydrophobic layer and an overlying hydrophilic layer (Fig. S4a, b). The Laplace pressure difference at the hydrophilic-hydrophobic interface generates the driving force for sweat transport. However, the presence of the hydrophobic layer often requires a relatively large liquid volume to break through, consequently leading to sweat accumulation and thereby prolonging the detection time. Droplet self-driving structures, also known as asymmetric structures, utilize engineered asymmetry to generate a Laplace pressure difference for fluid transport (Fig. S4c). Common structures include conical and wedge-shaped geometries. However, it remains challenging to fabricate highly ordered arrays of such conical micropores within thin films. In contrast, the PVA-reinforced network in PU fibers creates anisotropic microchannels that restrict lateral sweat diffusion, as shown in Fig. 1f. Under the synergistic effects of surface tension and capillary action, sweat is preferentially driven upward along the vertical channels, enabling directional liquid transport. Moreover, the partial pore-filling by PVA reduces the overall porosity, contributing to a significantly lower breakthrough pressure compared to traditional materials.
Preparation and performance enhancement of PVA@PU MH
Figure 2a illustrates the fabrication procedure of PVA@PU MH. Initially, a PU fibrous scaffold was prepared via electrospinning technology. Subsequently, the PVA solution was spin-coated onto the PU fibrous membrane. Through a multi-cyclic freeze-thaw process, the growth of ice crystals induced partial crystallization of PVA molecular chains along with the formation of intermolecular hydrogen bonds, thereby establishing a physically crosslinked network34. According to Fick’s law, the water permeation rate of PU films prepared with varying PU concentrations was systematically measured, leading to the identification of the 25 wt% PU film as the optimal scaffold, as illustrated in Fig. S5. Subsequently, the concentration of PVA was systematically varied. Figure 2b presents the microscopic images of PVA@PU MH with different PVA loadings. The 1 wt% PVA@PU MH shows minimal PVA deposition on PU fibers, while 2 wt% yields only sparse coating. At 3 wt%, a distinct “spider-web-like” PVA network forms on the PU scaffold, with hydrogel contraction during crosslinking creating vertically aligned macropores. In contrast, the 4 wt% composite displays densely packed, longitudinally oriented pores with significantly reduced diameters. PVA@PU MH membrane exhibits exceptional mechanical properties and remarkable flexibility, demonstrating significant performance enhancement compared to PVA hydrogel films (Figs. 2c, S6 and S7). Figures 2d and S8 display the Raman spectrum of the PVA@PU MH, which can be deconvoluted into four Gaussian components corresponding to hydrogen bonds in free, bound, and intermediate states. Thermogravimetric analysis revealed a bound-to-free water ratio of 1:335. To ensure experimental consistency, both in vitro and on-body tests were conducted using MH in their free water-depleted state, as excessive free water content could potentially interfere with subsequent electrolyte concentration measurements.
a Schematic illustration of the PVA@PU MH preparation process. b SEM of PVA@PU MH at different PVA concentration. c Optical images demonstrating the mechanical properties of PVA@PU MH. d Characterization of water states in PVA@PU MH. e Pore size diameter distribution of PVA@PU MH at different concentrations. f Hydrostatic pressure bearing capability of PVA@PU MH at different concentrations. g Filling rate of PVA@PU MH at different concentrations.
Subsequently, the PVA concentration was optimized based on comprehensive evaluations of porosity and water permeability characteristics. With the increase of PVA concentration, the PVA@PU MH exhibited a progressive decline in porosity, which correlated well with the microstructural evolution observed by SEM (Figs. 2e, S9). The hydrostatic pressure of the PVA@PU MH exhibited an increasing trend, showing relatively moderate enhancement at concentrations below 3 wt%, while a pronounced pressure elevation was observed when increasing from 3 to 4 wt%. Comparative evaluation with both PVA hydrogel and plasma-treated PU films demonstrated superior water permeation performance (Figs. 2f, S10). Finally, MH with identical thickness but varying PVA concentrations (1, 2, 3, and 4 wt%) were loaded into the sampling chamber for conductivity measurements to determine response times, as shown in Fig. 2g. The experimental results demonstrate that the PVA@PU MH filling does not interfere with the generation of step signals. Notably, the response time of the filled PVA@PU MH exhibits a non-monotonic concentration dependence, initially decreasing and subsequently increasing with higher spin-coated PVA concentrations. The optimal response time was achieved at 3 wt% concentration, whereas the 4 wt% sample exhibited the slowest response, even exceeding the latency observed with an empty chamber. The superior performance exhibited by the 3 wt% concentration can be attributed to its optimal porosity (68.56%) and relatively low hydrostatic pressure. The moderate porosity reduces the required sweat-filling volume, while the diminished hydrostatic pressure facilitates rapid sweat permeation through the PVA@PU MH, thereby preventing accumulation within the chamber. Consequently, the 3 wt% PVA@PU MH was identified as the optimal filling layer material in microfluidic. Owing to the PU fiber skeleton, PVA@PU MH exhibits excellent anti-swelling properties, ensuring stable performance during subsequent usage (Fig. S11).
To comparatively assess the water permeability of 3 wt% PVA@PU MH against conventional liquid-absorbing materials (airlaid, filter paper, and hydrophilic PU) as shown in Fig. 3a–c, two parallel experiments involving an eccentric injection method (Fig. 3d) and a liquid transmittance measurement (Fig. 3g) were designed. The detailed experimental procedures are provided in the “Methods” section. Upon eccentric ink injection, conventional absorbent materials exhibited complete lateral saturation before liquid entered the microchannel (Fig. 3e, f). In contrast, the PVA@PU MH enabled directional flow, initiating microfluidic penetration at only 75.53 ± 2.184% surface coverage, significantly reducing liquid infusion time. The liquid transmittance was quantified by measuring the diffusion distance on absorbent filter paper strips placed beneath the materials after depositing 10 μL of ink. Notably, the 3 wt% PVA@PU MH demonstrated the longest diffusion distance (1.05 ± 0.228 cm), significantly outperforming conventional absorbents (Fig. 3h, i). This advantage can be attributed to the directional liquid transport capability of the PVA@PU MH, whereas the isotropic diffusion characteristics of conventional materials lead to predominant in-plane spreading with limited longitudinal liquid conduction.
a Optical and SEM images of airlaid paper. b Optical and SEM images of filter paper. c Optical and SEM images of 25% PU. d Eccentric perfusion method, in contrast to directional penetration. e, f Comparative analysis of filling rates among different diffusion materials. g Comparative study of liquid permeation capacity. h, i Comparative analysis of liquid permeability in different diffusion materials.
Sweat rate measurement
A flexible microfluidic device integrated with conductivity detection to simultaneously monitor sweat rate and total electrolyte concentration was developed, as illustrated in Fig. 4a. The device was fabricated following the manufacturing protocol detailed in Fig. S12. The microchannel features a width of 500 μm, while the integrated electrodes are designed with an 80 μm width and a 6 mm inter-electrode spacing. For electrolyte concentration measurement, a compact electrode pair with 80 μm width and 250 μm spacing was implemented. As illustrated in Fig. S4, the variation in liquid coverage over the interdigitated electrodes significantly alters the overall equivalent circuit impedance. Figure 4b demonstrates that the impedance magnitude when the electrodes are fully submerged is substantially lower than when only half of the electrodes are covered by the liquid. The equivalent circuit impedance exhibited a progressive decrease with increasing electrolyte concentration, while distinct impedance models emerged between low and moderate-to-high concentration regimes (Figs. 4c, d and S13)36.
a Structural schematic of a sweat detection microfluidic chip. b Impedance spectra of interdigitated electrodes with varying sweat infiltration indices. c Impedance spectra of interdigitated electrodes in low-concentration NaCl solution. d Impedance spectra of interdigitated electrodes in high-concentration NaCl solution. e Conductivity response to varying sweat rate. f Derivative of the electrical conductivity response at different sweat rate. g Fitted curves of sweat rate versus inter-electrode transit time. h Conductivity response to varying electrolyte concentrations. i Calibration model development for conductivity detection. j Comparative plots of conductivity versus electrolyte concentration before and after infusion.
The flexible microfluidic sweat sensor was continuously perfused with NaCl solution at fixed concentrations using a syringe pump and perspiration simulation platform, while different sweat rates were simulated through precise regulation of the injection flow rate. The experimental results presented in Fig. 4e demonstrate a characteristic step function in the conductivity signal, where the step width exhibits a clear correlation with sweat rate. Specifically, higher sweat rates correspond to narrower step widths, indicative of reduced transit time between adjacent electrodes, whereas lower sweat rates result in broader step widths due to prolonged electrolyte passage through the electrode array. The step function was subsequently differentiated, as shown in Fig. 4f, with each conductivity transition generating a distinct peak. Quantitative analysis of the interpeak time intervals enabled precise determination of flow velocity variations corresponding to different sweat rates. Based on these results, a quantitative relationship model was established between the sweat rate and step width (corresponding to the transit time of sweat between adjacent electrodes), as shown in Fig. 4g. Through repeated natural evaporation and comprehensive in vitro testing across the full operational range, the sweat sensor filled with PVA@PU MH consistently maintained identical response time intervals at the beginning, middle, and end of each usage cycle, while demonstrating insensitivity to flow rate variations. These results confirm the reusability and indicate that prolonged sweat exposure does not compromise the sweat-transport performance of PVA@PU MH (Figs. S14 and S15). Subsequently, the conductivity response to electrolyte solutions of varying concentrations was systematically characterized. As demonstrated in Fig. 4h, i, a strong linear correlation was observed between the electrolyte concentration and the measured conductivity values. To further investigate the influence of filler materials on sensor performance, a comparative study was conducted between the unfilled configuration and the PVA@PU MH-filled system. Systematic measurements of conductivity values corresponding to varying NaCl concentrations (Figs. 4j, S16) revealed negligible differences between filled and unfilled states, confirming that the dry PVA@PU MH matrix does not interfere with concentration detection. Afterwards, the feasibility of sweat rate detection was experimentally validated through continuous modulation of infusion rates during in vitro testing. By incorporating the geometric parameters of the collection chamber, successful conversion from conductivity profiles to sweat rate was achieved. Comparative analysis demonstrated excellent agreement between the sensor-derived sweat rate and the preset syringe flow rate (Fig. S17).
The sweat rate and electrolyte concentration sensor presented in this work can be flexibly worn on any location of the epidermis, enabling real-time monitoring of physiological parameters during physical exercise, as illustrated in Fig. 5a. Subsequently, a low-power conductivity detection and signal transmission module for sweat signal acquisition and real-time data transmission to personal terminals was developed (Figs. 5b–d, S18). The integration of a dedicated filtering circuit and an applied bias voltage enables the sensor to achieve a high SNR of 39.679, along with reliable long-term operation in saline environments (Figs. S19 and S20). This enabled the establishment of a real-time monitoring system for sweat rate and electrolyte concentration, which successfully tracked relevant sweat parameters in human trials. The module consisted of signal conditioning, signal transduction, and data processing parts, which established a stable electrical connection with the sweat sensor through physical contact interfaces.
a The subject wore the sweat detection system while performing cycling exercise. b Optical image of the sweat detection system, which comprises a microfluidic and an electrical conductivity signal processing module. c Schematic diagram of the conductivity signal detection and transmission module. d Mobile terminal interface display. e The process of sweat flow into microfluidic channels during exercise. f Performance comparison of sweat rate monitoring in PVA@PU MH-embedded versus empty microfluidic systems. g The relationship between the detected local sweat rate and whole-body average sweat rate for male subjects.
To evaluate the sensing performance, comparative in vivo tests were conducted with and without PVA@PU MH filling material. Figure 5d displays the corresponding real-time data visualization on the personal terminal, while Fig. 5e demonstrates sweat collection at different time points. Due to the strategic placement of the concentration electrode upstream of the interdigitated electrodes, sweat entering the microfluidic channel first contacts the concentration sensor before flowing through two adjacent interdigitated electrodes for sweat rate measurement.
Moreover, the monitoring system incorporating PVA@PU MH demonstrated a significantly reduced response time, achieving a 311-s advancement, which highlights its superior performance characteristics. And across multiple experiments, PVA@PU MH demonstrated a 49.76% ± 6.75% increase in sweat collection. Subsequently, we systematically investigated the correlation between exercise intensity modulation and corresponding physiological responses by comparing the temporal profiles of heart rate and perspiration parameters (Fig. S21). Heart rate maintained immediate responsiveness to exercise intensity variations, while perspiration metrics exhibited pronounced hysteresis. Finally, we systematically evaluated the correlation between whole-body sweat rate (determined by timed body weight measurements before and after exercise) and anterior chest perspiration rate (measured by our sensor system) for male and female subjects. As illustrated in Figs. 5g and S22, the results demonstrated excellent agreement, with the anterior chest sweat rate being 1.206 times that of the whole-body sweat rate for male (mean sweating rate, 0.5289 ± 0.1574 μL/(min cm²)) and 0.34 times for female (mean sweating rate, 0.6399 ± 0.0637 μL/(min cm²)), which is consistent with previously reported medical statistical values37,38. The day-to-day reproducibility was performed in a controlled environment. As demonstrated in Tables S2 and S3, the sweat rate and electrolyte concentration were not different between different days. Furthermore, in this study with a limited sample size, the inter-individual variation in sweat rate was observed to be less than that in electrolyte concentration.
Discussion
In conclusion, a novel fully integrated wearable sensing platform incorporating PVA@PU MH as an RSAM has been developed for simultaneous monitoring of sweat rate and electrolyte concentration. PVA@PU MH features an anisotropic network structure and low breakthrough pressure, enabling efficient collection and transport of trace amounts of sweat from the skin surface into the microfluidic channel. The PVA@PU MH composite is fabricated through a combined process of electrospinning and cyclic freeze-thaw treatment. Systematic evaluation of water permeability and porosity characteristics identifies 25 wt% PU and 3 wt% PVA concentration as the optimal formulation. On this research foundation, the PVA@PU MH material was incorporated into a microfluidic platform with conductivity-sensing capability. This platform, combined with a low-power detection and signal transmission module, enables wearable real-time monitoring of both sweat rate and electrolyte concentration. On body testing demonstrated the exceptional sweat collection efficiency of the PVA@PU MH-filled sweat detection system. Moreover, a comparison was made between localized and whole-body sweat rates, which demonstrates the potential of this sensor for monitoring systemic dehydration. This manuscript provides crucial technical support for personalized hydration strategies while also facilitating rapid detection of other biomarkers in microliter-scale sweat.
Methods
Materials
Sodium chloride (NaCl) was purchased from Sigma-Aldrich (Shanghai) Trading Co., Ltd. Polyethylene terephthalate (PET) films and PET films with double-sided tape were provided by Suzhou Leanstar Electronic Technology Co., Ltd. PU (product no. A85P4394, Mw = 70,000, density = 1.12 g/cm3) was purchased from Shanghai Huntsman Polyurethanes Specialties Co., Ltd. Polyvinyl alcohol was obtained from Aladdin (China). N,N-dimethylformamide (DMF, ≥99.5%) was obtained from Sinopharm Group Chemical Reagent Co., Ltd., China. All other chemicals were commercially available and of analytical reagent grade. All reagents were used as received. The aqueous solutions were prepared freshly with deionized water (1 μS/cm).
Preparation of PVA@PU MH
PU was dissolved in DMF at a mass ratio of 25 wt% to prepare the electrospinning precursor solution. The electrospinning precursor solution was fed into a 5 mL syringe equipped with 22 G stainless steel needle in an electrospinning machine. The distance from the needle to the cylindrical collector was 8 cm, and an applied voltage of 12 kV was used. The feed rate was 0.08 mm/min, and the rotational speed of the collector was 300 rpm. The electrospinning environment was conducted at 25 °C and 45% relative humidity (RH). After electrospinning, the fiber membranes were put into a vacuum drying at 70 °C for 12 h to completely remove residual solvent.
PVA solutions with varying concentrations were prepared by complete dissolution in an aqueous medium through 2-h heating at 90 °C in a water bath with constant agitation. The viscosities corresponding to PVA solutions at different concentrations are shown in Fig. S23. The PVA solution was then spin-coated onto O2-plasma-treated PU fibrous membranes. Spin-coating was performed at a low speed of 300 rpm for 10 s, followed by a high-speed step at 2000 rpm for 20 s. Finally, followed by 8 cyclic freeze-thaw (−20 °C for 20 min and room temperature for 20 min) processing to fabricate the PVA@PU MH.
Characterization
A RM2000 Raman spectrometer from Renishaw plc. was used to characterize the water composition of PVA@PU MH. A SEM from HITACHI was used to observe the surface morphology of the membranes. The porosity was measured by an AutoPore IV 9500 mercury porosimeter. The mechanical property of PVA@PU MH was tested by the Instron 3365 compression and tensile strength tester.
Measurements
The Ex vivo tests of sweat rate and electrolyte concentration were evaluated using an injection pump (KD Scientific LEGATOTM 100) coupled with an artificial perspiration platform. A 100 mmol/L NaCl solution was loaded into the syringe, with flow rates adjusted from 0.44 to 3.54 μL/(min cm2) through precise injection pump control (equivalent to epidermal perspiration rates, where Rs = V/S; Rs represents simulated perspiration rate, V denotes pump flow rate, and S indicates collection area). Real-time conductance signals were acquired by the sensor during testing. The system delivered NaCl solutions at varying concentrations (25–200 mmol/L) at a constant flow rate (2 μL/min) while the sensor recorded corresponding conductivity changes.
The detailed eccentric perfusion method is that circular absorbent materials of identical area were positioned at the microfluidic channel inlets, followed by ink injection at a fixed offset distance from the center using a syringe pump. The time required for ink penetration through the absorbent matrix and subsequent 1 cm flow within the microchannel was systematically recorded.
An experiment was conducted to study the liquid permeability. A 3D model similar to running tracks was fabricated using 3D printing for comparing the performance of water-absorbing papers, as shown in the Fig. S24. One end of a narrow paper strip was fixed at the center of the circular cavity. The material to be tested was cut into a circular sample with a radius of 5 mm, matching the cavity dimensions, and placed inside, ensuring its position directly above the paper strip. A fixed volume (10 μL) of black ink was subsequently dropped into the center of the cavity. The ink penetrated vertically through the circular sample and subsequently diffused along the paper strip. The liquid transport capacity of the material in the vertical direction was quantitatively characterized by comparing the diffusion distance along the paper strip.
The comparative study of breakthrough pressure was set through the following method. The fiber membrane, cut into a fixed shape (a circle with a radius of 15 mm), was clamped between two bottomless measuring cylinders. The rhodamine solution was then dispensed onto one side of the membrane using a syringe pump (KD Scientific LEGATO™ 100) with 10 μL/min. The hydrostatic pressure P was calculated based on the volume of solution dispensed with P = ρgh when three consecutive droplets permeated through the opposite side of the membrane under increasing hydrostatic pressure, where ρ is the density of rhodamine solution, g represents the gravitational acceleration, and h is defined as the height of the rhodamine solution column maintained in the upper bottomless measuring cylinder. The average value for each membrane type was determined from three independent measurements. The small error bars of the data indicate good test repeatability.
On body test
The designated skin areas were thoroughly cleaned using ethanol and deionized water, followed by drying with lint-free wipes. The flexible patch containing the sensor module was firmly applied to the prepared sites. Subjects performed graded-intensity exercise on a stationary bicycle (Keep K0102C) under controlled ambient conditions (22–27 °C, 20–30% RH). Real-time heart rate monitoring was achieved using a smart sports watch (HUAIWEI WATCH GT4), while exercise intensity was modulated through simultaneous adjustment of bicycle resistance and pedaling frequency. Perspiration data (sweat rate and electrolyte concentration) were transmitted wirelessly via Bluetooth to a mobile device for real-time monitoring. On-body tests using the sweat sensor followed relevant instructions approved by the Institutional Review Board of Suzhou Institute of Nano-Tech and Nano-Bionics (SINANO/EC/2025-036). Eight healthy subjects (five males and three females) understood the guidelines of the test and offered written informed consent. First, the subjects removed their clothing, and their body weight was recorded. They then immediately wore the sweat sensors. No water or food intake was allowed during the test. The subjects performed approximately 20–60 min of indoor cycling. After the test, the sweat sensors were not removed immediately, as residual sweat remained on the volunteers. Instead, a second weight measurement was conducted after a 10-min delay to allow for the evaporation of sensible sweat. Given that the predominant pathway of water loss during this period was through sweating, the influence of other factors on systematic error is considered negligible39.
The response performance of identical sweat flow rate sensors, with and without PVA@PU MH filling, was compared. Sensors with and without the functional membrane were affixed adjacently on the left side of the chest, and sweat accumulation in both sensors was simultaneously recorded during physical exercise. Timing was initiated at the onset of exercise (t = 0), and the reported reduction in system response time was calculated relative to this baseline. Owing to the operational principle of the interdigital electrodes, the signal onset was defined as the moment when the first current step was detected. The enhancement efficiency E was calculated as:
Where, Tempty represents the response time of the sweat rate sensor without PVA@PU MH, and TMH is the response time of the sweat rate sensor with PVA@PU MH.
Furthermore, the statistical analysis of the on-body test results was performed using Matlab.
Data availability
Data will be made available on request.
References
Bariya, M., Nyein, H. Y. Y. & Javey, A. Wearable sweat sensors. Nat. Electron. 1, 160–171 (2018).
Brasier, N. et al. The potential of wearable sweat sensors in heart failure management. Nat. Electron. 7, 182–184 (2024).
Yang, D. S., Ghaffari, R. & Rogers, J. A. Sweat as a diagnostic biofluid. Science 379, 760–761 (2023).
Cinca-Morros, S., Garcia-Rey, S., Álvarez-Herms, J., Basabe-Desmonts, L. & Benito-Lopez, F. A physiological perspective of the relevance of sweat biomarkers and their detection by wearable microfluidic technology: a review. Anal. Chim. Acta 1327, 342988 (2024).
Liu, M. et al. Adaptively resettable microfluidic patch for sweat rate and electrolytes detection. Biosens. Bioelectron. 257, 116299 (2024).
Liu, M. et al. Perspiration permeable, textile embeddable microfluidic sweat sensor. Biosens. Bioelectron. 237, 115504 (2023).
Wang, S. et al. An unconventional vertical fluidic-controlled wearable platform for synchronously detecting sweat rate and electrolyte concentration. Biosens. Bioelectron. 210, 114351 (2022).
Clausen, D. et al. Wearable continuous diffusion-based skin gas analysis. Nat. Commun. 16, 4343 (2025).
Liu, C., Xu, T., Wang, D. & Zhang, X. The role of sampling in wearable sweat sensors. Talanta 212, 120801 (2020).
Brasier, N. et al. The molecular signature of heat stress in sweat reveals non-invasive biomarker candidates for health monitoring. Commun. Biol. 8, 650 (2025).
Zhang, T., Kabandana, G. K. M., Terrell, J. A., Chen, H. & Chen, C. Recent advances in wearable sweat sensor development. Wiley Interdiscip. Rev. Nanomed. Nanobiotechnol. 17, e70006 (2025).
Kim, S. R. et al. Electrodermal activity as a proxy for sweat rate monitoring during physical and mental activities. Nat. Electron. 8, 353–361 (2025).
Kim, J. et al. A skin-interfaced, miniaturized microfluidic analysis and delivery system for colorimetric measurements of nutrients in sweat and supply of vitamins through the skin. Adv. Sci. 9, 2103331 (2022).
Tu, J. et al. A wireless patch for the monitoring of C-reactive protein in sweat. Nat. Biomed. Eng. 7, 1293–1306 (2023).
Choi, J. et al. Skin-Interfaced microfluidic systems that combine hard and soft materials for demanding applications in sweat capture and analysis. Adv. Healthc. Mater. 10, 200722 (2021).
Bandodkar, A. J. et al. Battery-free, skin-interfaced microfluidic/electronic systems for simultaneous electrochemical, colorimetric, and volumetric analysis of sweat. Sci. Adv. 5, eaav3294 (2019).
Yang, Y. et al. Wearable microfluidics: fabric-based digital droplet flowmetry for perspiration analysis. Lab Chip 17, 926–935 (2017).
Kwon, K. et al. An on-skin platform for wireless monitoring of flow rate, cumulative loss and temperature of sweat in real time. Nat. Electron. 4, 302–312 (2021).
Dautta, M. et al. Tape-Free, digital wearable band for exercise sweat rate monitoring. Adv. Mater. Technol. 8, 2201187 (2023).
Baker, L. B. et al. Skin-Interfaced microfluidic system with personalized sweating rate and sweat chloride analytics for sports science applications. Sci. Adv. 6, eabe3929 (2020).
Nelson, R. S. et al. Remote analysis and management of sweat biomarkers using a wearable microfluidic sticker in adult cystic fibrosis patients. Proc. Natl. Acad. Sci. USA 122, e2506137122 (2025).
Bariya, M. et al. Resettable microfluidics for broad-range and prolonged sweat rate sensing. ACS Sens. 7, 1156–1164 (2022).
Ding, H., Yang, H. & Tsujimura, S. Nature-Inspired superhydrophilic biosponge as structural beneficial platform for sweating analysis patch. Adv. Sci. 11, e2401947 (2024).
Liu, J., Xu, Z., Wang, H., Zhao, Y. & Lin, T. Directional liquid transport in thin fibrous matrices: Enhancement of advanced applications. ACS Nano 19, 5913–5937 (2025).
Li, D. et al. Janus textile: advancing wearable technology for autonomous sweat management and beyond. Small 21, 2409730 (2025).
Zhang, S., Tan, R., Xu, X., Iqbal, S. & Hu, J. Fibers/textiles-based flexible sweat sensors: a review. ACS Mater. Lett. 5, 1420–1440 (2023).
Lin, P. H., Sheu, S. C., Chen, C. W., Huang, S. C. & Li, B. R. Wearable hydrogel patch with noninvasive, electrochemical glucose sensor for natural sweat detection. Talanta 241, 123187 (2022).
Lu, L. et al. Sweat-Sensing patches with integrated hydrogel interface for resting sweat collection and multi-information detection. Biosensors 15, 342 (2025).
Lin, S. et al. Natural perspiration sampling and in situ electrochemical analysis with hydrogel micropatches for user-identifiable and wireless chemo/biosensing. ACS Sens. 5, 93–102 (2020).
Nyein, H. Y. Y. et al. A wearable patch for continuous analysis of thermoregulatory sweat at rest. Nat. Commun. 12, 1823 (2021).
Shen, H. et al. Multi-Bioinspired droplet self-actuated sweat transport platform for continuous wearable biochemical monitoring. Adv. Mater. Technol. 9, 2301803 (2024).
Son, J. et al. Cactus-Spine-Inspired sweat-collecting patch for fast and continuous monitoring of sweat. Adv. Mat. 33, 2102740 (2021).
Shin, S. et al. A bioinspired microfluidic wearable sensor for multiday sweat sampling, transport, and metabolic analysis. Sci. Adv. 11, eadw9024 (2025).
Gao, Q. et al. Biological tissue-inspired ultrasoft, ultrathin, and mechanically enhanced microfiber composite hydrogel for flexible bioelectronics. Nanomicro. Lett. 15, 139 (2023).
Liang, J. et al. Bioinspired mechanically robust and recyclable hydrogel microfibers based on hydrogen-bond nanoclusters. Adv. Sci. 11, 2401278 (2024).
Lazanas, A. C. & Prodromidis, M. I. Electrochemical impedance spectroscopy─a tutorial. ACS Meas. Sci. Au 3, 162–193 (2023).
Smith, C. J. & Havenith, G. Body mapping of sweating patterns in male athletes in mild exercise-induced hyperthermia. Eur. J. Appl. Physiol. 111, 1391–1404 (2011).
Smith, C. J. & Havenith, G. Body mapping of sweating patterns in athletes: a sex comparison. Med. Sci. Sports Exerc. 44, 2350–2361 (2012).
Yamada, Y. et al. Variation in human water turnover associated with environmental and lifestyle factors. Science 378, 909–915 (2022).
Acknowledgements
The authors acknowledge the funding support from the National Natural Science Foundation of China (Grant No. 62125112, 62271479, U24A20228, 62471465, 62401562, 62301554, 62501590), the Strategic Priority Research Program of the Chinese Academy of Science (Grant No. XDB0520301). Funded by Jiangsu Funding Program for Excellent Postdoctoral Talent (Grant No. 2025ZB251), Basic Research Program of Jiangsu (BK20243004), the Natural Science Foundation of Jiangsu Province (Grant No. BK20240476). The China Postdoctoral Science Foundation (Grant No. 2024M753441, 2024M762320). The authors also thank to Suzhou Leanstar Electronic Technology Co., Ltd., for their assistance in the production of sweat sensors.
Author information
Authors and Affiliations
Contributions
**H. S.** and **S. L.** contributed equally to this work. **H. S.** wrote the main manuscript text and prepared Figures 1-5. **S. L.** assisted in the preparation of the manuscript and all figures. **M. L**., **M. W.**, **Y. W. and Q. G.** participated in the experiment presented in Figure 5. **Y. L.** and **F. W.** assisted in the preparation of Figures 1-2. **L. L.** participated in the revision of this manuscript. **D. Z. and Z. X.** participated in the fabrication of the sweat sensors. **S. W.** reviewed and edited the manuscript and acquired funding. **T. Z.** reviewed and edited this manuscript, supervised the project, and acquired funding.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Shen, H., Liu, S., Liu, M. et al. Directional permeation-driven microfiber composite hydrogel towards rapid sweat uptaking and hydration monitoring. npj Flex Electron 10, 33 (2026). https://doi.org/10.1038/s41528-026-00535-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41528-026-00535-7