Abstract
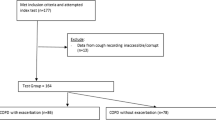
Early COPD diagnosis is vital for effective management, yet conventional tools such as professional spirometers are often inaccessible in resource-limited settings. We present Cough Search, a smartphone-based deep learning algorithm that uses voluntary cough sounds to detect COPD, offering a cost-efficient and accessible diagnostic approach. The presented COPD detection algorithm (Cough Search) employs a transformer-based neural network model. It was trained on a training cohort (406 COPD and 1631 non-COPD) with hyperparameters tuned on the balanced internal validation cohort (151 COPD and 225 non-COPD participants). The algorithm was finally validated on the external validation cohort (105 COPD and 617 non-COPD participants from four hospitals). Participants were classified as COPD or non-COPD based on spirometry and clinical diagnoses. Cough Search achieved an area under the receiver operating characteristic curve (AUC) of 0.92 and 0.94 in the internal and external validation cohorts, respectively. In the external validation cohort study, the model demonstrated high sensitivity (92%) and specificity (86%) in distinguishing COPD from non-COPD cases. Performance remained robust across all COPD stages, with a sensitivity exceeding 93% for severe stages (GOLD 3–4) and above 91% for moderate stages (GOLD 1–2). The algorithm maintained its accuracy across non-COPD respiratory conditions and smartphone models. Cough Search shows promise as a scalable, accessible tool for COPD detection, particularly in underserved areas, potentially transforming early COPD diagnosis and management. Trial registration: ClinicalTrials.gov Identifier: NCT06082791.
Similar content being viewed by others
Data Availability
No datasets were generated or analysed during the current study.
References
Chen, S. et al. The global economic burden of chronic obstructive pulmonary disease for 204 countries and territories in 2020–50: a health-augmented macroeconomic modelling study. Lancet Glob Health 11, e1183–e1193 (2023).
Fang, Liwen et al. Chronic obstructive pulmonary disease in China: a nationwide prevalence study. Lancet Respir. Med. 6, 421-430.
Diab, N. et al. Underdiagnosis and Overdiagnosis of Chronic Obstructive Pulmonary Disease. Am J Respir Crit Care Med American Thoracic Society - AJRCCM 198, 1130–1139 (2018).
Chen, Q. et al. Cost-effectiveness of population-based screening for chronic obstructive pulmonary disease in China: a simulation modeling study. Lancet Reg Health West Pac 46, 101065 (2024).
Patel, N. An update on COPD prevention, diagnosis, and management: The 2024 GOLD Report. Nurse Pract 49, 29–36, https://doi.org/10.1097/01.NPR.0000000000000180 (2024).
Graham, B. L. et al. Standardization of spirometry 2019 update. an official American thoracic society and european respiratory society technical statement. Am J Respir Crit Care Med American Thoracic Society - AJRCCM 200, e70–e88 (2019).
Arne, M. et al. How often is diagnosis of COPD confirmed with spirometry?. Respir Med 104, 550–556 (2010).
Zhou, J. et al. Accuracy of six chronic obstructive pulmonary disease screening questionnaires in the chinese population. Int J Chron Obstruct Pulmon Dis 17, 317–327 (2022).
Yang, X. et al. Comparative study on chronic obstructive pulmonary disease screening tools in primary healthcare institutions in Beijing, China. COPD Dove Press 18, 1773–1781 (2023).
Infante, C. et al. Use of cough sounds for diagnosis and screening of pulmonary disease. IEEE Global Humanitarian Technology Conference (GHTC). 20171–10IEEE: San Jose, CA, 2017.
Chen, Z. et al. Exploring explainable AI features in the vocal biomarkers of lung disease. Computers in Biology and Medicine Pergamon 179, 108844 (2024).
Widdicombe, J. & Fontana, G. Cough: what’s in a name?. European Respiratory Journal European Respiratory Society 28, 10–15 (2006).
Porter, P. et al. Diagnosing chronic obstructive airway disease on a smartphone using patient-reported symptoms and cough analysis: diagnostic accuracy study. JMIR Formative Research 4, e24587 (2020).
Claxton, S. et al. Identifying acute exacerbations of chronic obstructive pulmonary disease using patient-reported symptoms and cough feature analysis. npj Digital Medicine 4, 107 (2021).
Sharan, R. V., Qian, K. & Yamamoto, Y. Automated cough sound analysis for detecting childhood pneumonia. IEEE Journal of Biomedical and Health Informatics 28, 193–203 (2024).
Yellapu, G. D. et al. Development and clinical validation of swaasa AI platform for screening and prioritization of pulmonary TB. Scientific reports 13, 4740 (2023).
Agustí, A. et al. Global initiative for chronic obstructive lung disease 2023 report: GOLD executive summary. Am J Respir Crit Care Med. 207, (2023). https://www.atsjournals.org/doi/full/10.1164/rccm.202301-0106PP.
Wang, Q. et al. Towards reliable respiratory disease diagnosis based on cough sounds and vision transformers. arXiv http://arxiv.org/abs/2408.15667 (2024).
Dosovitskiy, A. et al. An image is worth 16x16 words: transformers for image recognition at scale. Arxiv https://openreview.net/forum?id=YicbFdNTTy (2020).
Chen, W. et al. EAT: Self-supervised pre-training with efficient audio transformer. arXiv http://arxiv.org/abs/2401.03497 (2024).
Austin, P. C. An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivariate Behav Res 46, 399–424 (2011).
Zhang, H. et al. mixup: Beyond empirical risk minimization. arXiv:1710.09412, https://arxiv.org/abs/1710.09412 (2017).
Fang, L. et al. Chronic obstructive pulmonary disease in China: a nationwide prevalence study. The Lancet Respiratory Medicine Elsevier 6, 421–430 (2018).
Tracey, B. et al. Towards interpretable speech biomarkers: exploring MFCCs. Scientific Reports 13, 22787 (2023).
Checkley, W. et al. Population-based screening for chronic obstructive pulmonary disease using the st. George’s respiratory questionnaire in resource-limited settings. Am J Respir Crit Care Med 211, 779–788 (2025).
Lee, S. et al. Screening major depressive disorder using vocal acoustic features in the elderly by sex. J Affect Disord 291, 15–23 (2021).
LoMauro, A. & Aliverti, A. Sex differences in respiratory function[J]. Breathe 14, 131–140 (2018).
Levin, K. A., Anderson, D. & Crighton, E. Prevalence of COPD by age, sex, socioeconomic position and smoking status; a cross-sectional study. Health Education 120, 275–288 (2020).
Burney, P. et al. Prevalence and population-attributable risk for chronic airflow obstruction in a large multinational study. Am J Respir Crit Care Med 203, 1353–1365 (2021).
Stockley, R. A. Bronchiectasis: a progressive phenotype of chronic obstructive pulmonary disease. Clinical Infectious Diseases 72, 411–413 (2021).
Gut-Gobert, C. et al. Women and COPD: do we need more evidence?. Eur Respir Rev 28, 180055 (2019).
Acknowledgements
This work was funded by National Key Research and Development Project (No. 2022YFC2010005); Natural Science Foundation of China under Grant (No. 82070004, 82200004); Shanghai Key Laboratory of Emergency Prevention, Diagnosis and Treatment of Respiratory Infectious Diseases (No. 20dz2261100); Cultivation Project of Shanghai Major Infectious Disease Research Base (No. 20dz2210500).
Author information
Authors and Affiliations
Contributions
Concept and design: J.Z., J.W.H., M.Z., J.M.Q.; Inclusion participants: P.W., Q.W., J.H.Y., H.F.C., L.H., J.X.M., Y.L., L.T., X.W.S., D.X.Z.; Acquisition or processing of the data: S.C., X.L.R., Y.Z.; Algorithm and data analysis: Q.W., Z.Y.B., M,Y.; Statistical analysis: W.Y.Z., E.F.; Manuscript writing and draft: J.Z., J.W.H., M.Z., X.L.R., Q.W.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zhou, J., Huang, J., Wang, Q. et al. A cough sound-based deep learning algorithm for accessible prompt detection of chronic obstructive pulmonary disease with smartphones. npj Prim. Care Respir. Med. (2026). https://doi.org/10.1038/s41533-026-00486-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41533-026-00486-6