Abstract
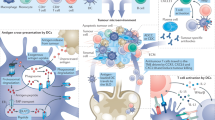
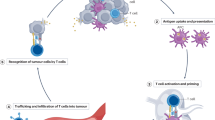
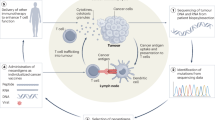
The development of prophylactic cancer vaccines typically involves the selection of combinations of tumour-associated antigens, tumour-specific antigens and neoantigens. Here we show that membranes from induced pluripotent stem cells can serve as a tumour-antigen pool, and that a nanoparticle vaccine consisting of self-assembled commercial adjuvants wrapped by such membranes robustly stimulated innate immunity, evaded antigen-specific tolerance and activated B-cell and T-cell responses, which were mediated by epitopes from the abundant number of antigens shared between the membranes of tumour cells and pluripotent stem cells. In mice, the vaccine elicited systemic antitumour memory T-cell and B-cell responses as well as tumour-specific immune responses after a tumour challenge, and inhibited the progression of melanoma, colon cancer, breast cancer and post-operative lung metastases. Harnessing antigens shared by pluripotent stem cell membranes and tumour membranes may facilitate the development of universal cancer vaccines.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
The RNA-seq data are available from the NCBI database under accession code GSE279478. The mass spectrometry proteomics data are available from the ProteomeXchange Consortium via the PRIDE partner repository with the dataset identifier PXD056678. The raw and analysed datasets generated during the study are available for research purposes from the corresponding authors on reasonable request. Source data are provided with this paper.
References
Bray, F., Jemal, A., Torre, L. A., Forman, D. & Vineis, P. Long-term realism and cost-effectiveness: primary prevention in combatting cancer and associated inequalities worldwide. J. Natl Cancer Inst. 107, djv273 (2015).
Enokida, T., Moreira, A. & Bhardwaj, N. Vaccines for immunoprevention of cancer. J. Clin. Invest. 131, e146956 (2021).
Finn, O. J. The dawn of vaccines for cancer prevention. Nat. Rev. Immunol. 18, 183–194 (2018).
Markowitz, L. E. et al. Human papillomavirus vaccine introduction—the first five years. Vaccine 30, F139–F148 (2012).
Hu, Y. & Yu, H. Prevention strategies of mother-to-child transmission of hepatitis B virus (HBV) infection. Pedia. Invest. 4, 133–137 (2020).
Van Zyl, D. G., Mautner, J. & Delecluse, H. J. Progress in EBV vaccines. Front. Oncol. 9, 104 (2019).
Alam, S. et al. Predicting and designing epitope ensemble vaccines against HTLV-1. J. Integr. Bioinform. 16, 20180051 (2020).
Cheever, M. A. et al. The prioritization of cancer antigens: a National Cancer Institute pilot project for the acceleration of translational research. Clin. Cancer Res. 15, 5323–5337 (2009).
Bayo, C., Jung, G., Espanol-Rego, M., Balaguer, F. & Benitez-Ribas, D. Vaccines for non-viral cancer prevention. Int. J. Mol. Sci. 22, 10900 (2021).
Czerniecki, B. J. et al. Targeting HER-2/neu in early breast cancer development using dendritic cells with staged interleukin-12 burst secretion. Cancer Res. 67, 1842–1852 (2007).
Carlos, C. A. et al. Human tumor antigen MUC1 is chemotactic for immature dendritic cells and elicits maturation but does not promote Th1 type immunity. J. Immunol. 175, 1628–1635 (2005).
Finn, O. J. & Beatty, P. L. Cancer immunoprevention. Curr. Opin. Immunol. 39, 52–58 (2016).
Ishihara, M. et al. First-in-human phase I clinical trial of the NY-ESO-1 protein cancer vaccine with NOD2 and TLR9 stimulants in patients with NY-ESO-1-expressing refractory solid tumors. Cancer Immunol. Immunother. 69, 663–675 (2020).
Roudko, V. et al. Shared immunogenic poly-epitope frameshift mutations in microsatellite unstable tumors. Cell 183, 1634–1649 (2020).
Gabitzsch, E. S. et al. The generation and analyses of a novel combination of recombinant adenovirus vaccines targeting three tumor antigens as an immunotherapeutic. Oncotarget 6, 31344–31359 (2015).
Hanahan, D. Hallmarks of cancer: new dimensions. Cancer Discov. 12, 31–46 (2022).
Jassim, A., Rahrmann, E. P., Simons, B. D. & Gilbertson, R. J. Cancers make their own luck: theories of cancer origins. Nat. Rev. Cancer 23, 710–724 (2023).
Takahashi, K. & Yamanaka, S. Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell 126, 663–676 (2006).
Zhai, Y. W. et al. A splenic-targeted versatile antigen courier: iPSC wrapped in coalescent erythrocyte-liposome as tumor nanovaccine. Sci. Adv. 7, 6326 (2021).
Kooreman, N. G. et al. Autologous iPSC-based vaccines elicit anti-tumor responses in vivo. Cell Stem Cell 22, 501–513 (2018).
Shin, B. K. et al. Global profiling of the cell surface proteome of cancer cells uncovers an abundance of proteins with chaperone function. J. Biol. Chem. 278, 7607–7616 (2003).
Hu, Z. et al. The Cancer Surfaceome Atlas integrates genomic, functional and drug response data to identify actionable targets. Nat. Cancer 2, 1406–1422 (2021).
Ferguson, I. D. et al. The surfaceome of multiple myeloma cells suggests potential immunotherapeutic strategies and protein markers of drug resistance. Nat. Commun. 13, 4121 (2022).
Chen, L. et al. Bacterial cytoplasmic membranes synergistically enhance the antitumor activity of autologous cancer vaccines. Sci. Transl. Med. 13, 601 (2021).
Gonzalez, H., Hagerling, C. & Werb, Z. Roles of the immune system in cancer: from tumor initiation to metastatic progression. Genes Dev. 32, 1267–1284 (2018).
Ong, J. Y. & Torres, J. Z. Phase separation in cell division. Mol. Cell 80, 9–20 (2020).
Ananya, A. et al. ‘Just right’ combinations of adjuvants with nanoscale carriers activate aged dendritic cells without overt inflammation. Immun. Ageing 20, 10 (2023).
Mata-Haro, V. et al. The vaccine adjuvant monophosphoryl lipid A as a TRIF-biased agonist of TLR4. Science 316, 1628–1632 (2007).
Li, M. et al. Engineering multifunctional DNA hybrid nanospheres through coordination-driven self-assembly. Angew. Chem. Int. Ed. 58, 1350–1354 (2019).
Cheng, R. et al. Recombination monophosphoryl lipid A-derived vacosome for the development of preventive cancer vaccines. ACS Appl. Mater. Interfaces 12, 44554–44562 (2020).
Duan, T., Du, Y., Xing, C., Wang, H. Y. & Wang, R. F. Toll-like receptor signaling and its role in cell-mediated immunity. Front. Immunol. 13, 812774 (2022).
World Health Organization Guidelines on Nonclinical Evaluation of Vaccines (WHO Technical Report Series, 927, 2005).
Gilchrist, R. B., Ritter, L. J. & Armstrong, D. T. Mouse oocyte mitogenic activity is developmentally coordinated throughout folliculogenesis and meiotic maturation. Dev. Biol. 240, 289–298 (2001).
Perez, D. et al. Predictive autoimmunity using autoantibodies: screening for anti-nuclear antibodies. Clin. Chem. Lab. Med. 56, 1771–1777 (2018).
Satoh, M., Ceribelli, A., Hasegawa, T. & Tanaka, S. Clinical significance of antinucleolar antibodies: biomarkers for autoimmune diseases, malignancies, and others. Clin. Rev. Allergy Immunol. 63, 210–239 (2022).
Ying, Y., Liu, S., Wu, Y., Li, S. & Huang, Q. Anticentromere antibody induced by immunization with centromere protein a and Freund’s complete adjuvant may interfere with mouse oocyte meiosis. Reprod. Biol. Endocrinol. 19, 50 (2021).
Ben Lamine, Z. et al. Anti-gp210 and anti-Sp100 antibodies in primary biliary cholangitis. Arab J. Gastroenterol. 22, 316–320 (2021).
Zhang, W., Wang, D., Yuan, W. & Yao, S. Combined detection of ACL and beta2-GP1 in diagnosis of adverse pregnancy. Am. J. Transl. Res. 13, 5653–5658 (2021).
Kruger, J. A. et al. Characterization of stem cell-like cancer cells in immune-competent mice. Blood 108, 3906–3912 (2006).
Charafe-Jauffret, E. et al. Breast cancer cell lines contain functional cancer stem cells with metastatic capacity and a distinct molecular signature. Cancer Res. 69, 1302–1313 (2009).
Muehlberg, F. L. et al. Tissue-resident stem cells promote breast cancer growth and metastasis. Carcinogenesis 30, 589–597 (2009).
Yadav, M. et al. Predicting immunogenic tumour mutations by combining mass spectrometry and exome sequencing. Nature 515, 572–576 (2014).
Jurtz, V. et al. NetMHCpan-4.0: improved peptide-MHC class I interaction predictions integrating eluted ligand and peptide binding affinity data. J. Immunol. 199, 3360–3368 (2017).
O’Hagan, D. T., Ott, G. S., De Gregorio, E. & Seubert, A. The mechanism of action of MF59—an innately attractive adjuvant formulation. Vaccine 30, 4341–4348 (2012).
Chevaleyre, C. et al. The tumor antigen cyclin B1 hosts multiple CD4 T cell epitopes differently recognized by pre-existing naive and memory cells in both healthy and cancer donors. J. Immunol. 195, 1891–1901 (2015).
Imaoka, H. et al. RacGAP1 expression, increasing tumor malignant potential, as a predictive biomarker for lymph node metastasis and poor prognosis in colorectal cancer. Carcinogenesis 36, 346–354 (2015).
Tang, Q. et al. MELK is an oncogenic kinase essential for metastasis, mitotic progression, and programmed death in lung carcinoma. Signal Transduct. Target. Ther. 5, 279 (2020).
Guerrera, I. C. & Kleiner, O. Application of mass spectrometry in proteomics. Biosci. Rep. 25, 71–93 (2005).
Haen, S. P., Loffler, M. W., Rammensee, H. G. & Brossart, P. Towards new horizons: characterization, classification and implications of the tumour antigenic repertoire. Nat. Rev. Clin. Oncol. 17, 595–610 (2020).
Zhao, T. et al. Vaccine adjuvants: mechanisms and platforms. Signal Transduct. Target. Ther. 8, 283 (2023).
Meyskens, F. L. et al. Cancer prevention: obstacles, challenges and the road ahead. J. Natl Cancer Inst. 108, djv309 (2016).
De Miguel, M. P. et al. Immunosuppressive properties of mesenchymal stem cells: advances and applications. Curr. Mol. Med. 12, 574–591 (2012).
Shi, Y. et al. Immunoregulatory mechanisms of mesenchymal stem and stromal cells in inflammatory diseases. Nat. Rev. Nephrol. 14, 493–507 (2018).
Kim, J. Y. et al. MHC expression in a human adult stem cell line and its down-regulation by hCMV US gene transfection. Int. J. Biochem. Cell Biol. 37, 69–78 (2005).
Weetman, A. P. The immunology of pregnancy. Thyroid 9, 643–646 (1999).
Kimura, T. et al. MUC1 vaccine for individuals with advanced adenoma of the colon: a cancer immunoprevention feasibility study. Cancer Prev. Res. 6, 18–26 (2013).
Gilbert, S. C. T-cell-inducing vaccines—what’s the future. Immunology 135, 19–26 (2012).
Wang, Y. S. et al. mRNA-based vaccines and therapeutics: an in-depth survey of current and upcoming clinical applications. J. Biomed. Sci. 30, 84 (2023).
Rabinovich, G. A., Gabrilovich, D. & Sotomayor, E. M. Immunosuppressive strategies that are mediated by tumor cells. Annu. Rev. Immunol. 25, 267–296 (2007).
Pearl, J. I., Kean, L. S., Davis, M. M. & Wu, J. C. Pluripotent stem cells: immune to the immune system? Sci. Transl. Med. 4, 164 (2012).
Finn, O. J. Human tumor antigens yesterday, today, and tomorrow. Cancer Immunol. Res. 5, 347–354 (2017).
Zhu, F. et al. Cell‐reprogramming‐inspired dynamically responsive hydrogel boosts the induction of pluripotency via phase‐separated biomolecular condensates. Adv. Mater. 36, 22 (2023).
Yu, G., Wang, L. G., Han, Y. & He, Q. Y. clusterProfiler: an R package for comparing biological themes among gene clusters. OMICS 16, 284–287 (2012).
Acknowledgements
We thank the bioinstrumentation platform of the National Center for Nanoscience and Technology for technical support. We also thank W. Qiu, G. Zheng, K. Luo and J. Cui for kind help with the tumour therapy experiments, J. Liang and Y. Wang for detection of the specific T-cell responses in human PBMC samples and A. Sheftel for critical reading of the paper. G.N. discloses support for the research described in this study from the Fundamental Research Center Project of National Natural Science Foundation of China (grant number T2288102) and the Strategic Priority Research Program of the Chinese Academy of Sciences (grant number XDB36000000). R.Z. discloses support for the publication of this study from the National Key Research and Development Program of China (grant number 2023YFC2508500), CAS Project for Young Scientists in Basic Research (grant number YSBR-041) and the Beijing Nova Program (grant number 202304584382). H.Q. discloses support for the publication of this study from the National Natural Science Foundation of China (grant number 32301202). B.H. discloses support for the publication of this study from the National Natural Science Foundation of China (grant number 52473120). H.G. discloses support for the publication of this study from CAMS Innovation Fund for Medical Sciences (grant number CIFMS 2022-I2M-1-009).
Author information
Authors and Affiliations
Contributions
N.L., B.H., G.N. and R.Z. conceived the project. N.L., H.Q. and F.Z. designed and performed most of the experiments, analysed the data and wrote the paper. Y.C. and Yixuan Lin assisted in tumour therapy experiments. T.M. and Y. Lv assisted in obtaining tissue samples and detecting immune responses. H.D., R.D. and C.X. assisted in the data analysis. R.L. and Y.W. assisted in liposome synthesis. J.S. and H.C. provided suggestions on data presentation. G.Z., H.G., M.L. and Yongfang Lin bred the k-Ras muted mice and provided related advice. R.Z. provided suggestions on experiment design and data analysis. B.H., G.N., Y.Z. and R.Z. supervised all experiments. N.L., G.N. and R.Z. wrote and revised the paper.
Corresponding authors
Ethics declarations
Competing interests
The authors G.N., R.Z. and N.L. are inventors on a filed provisional application for China patent no. CN2024103159244 (An immune composition and its application) and no. CN2024113741833 (Tumour-shared surface antigen epitope peptide and its screening method), submitted by the National Center for Nanoscience and Technology, covering the potential application of tumour prevention of iPM nanovax. The authors declare no other competing interests.
Peer review
Peer review information
Nature Biomedical Engineering thanks Siwen Li, Zhuang Liu and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Peer reviewer reports are available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Serum antibodies produced by iPM nanovax vaccination against iPSCs and multiple cancer cells.
C57BL6N mice were injected by the indicated groups for totally 4 weeks, once a week. A month later, serum from the indicated groups was incubated with iPSCs (a), MC38 cells (b), or B16F0 cells (c) for 45 min and then stained with anti-IgG, followed by flow cytometry. The data are presented as the mean ± s.d. (n = 6 biological replicates). P values in a–c were calculated using one-way ANOVA with Tukey’s comparison test; ns, no significant difference.
Extended Data Fig. 2 Increased memory immune responses elicited by iPM nanovax.
The healthy C57BL6N mice received four rounds of iPM nanovax vaccination. Two months later, flow cytometry analysis was performed to determine the percentage of memory B cells and T cells in mice. The frequency of plasma cells (CD3−CD19−CD138−IgM+) in peripheral blood (a) was detected. The percentage of plasma cells (CD3−CD19−CD138−IgM+) and plasmablast cells (CD3−CD19+CD138+IgM+) in bone marrow (b) were detected. The frequency of memory B cells (CD3−CD19+CD138−PDL2+IgM+) in bone marrow (c), central memory T cells (CD44highCD62LhighCD8+ and CD44highCD62LhighCD4+) in peripheral blood (d) and spleen (e) were detected. The data are presented as the mean ± s.d. (n = 6 biological replicates). P values in a–e were calculated using an unpaired t-test.
Extended Data Fig. 3 Schematic illustration of epitope prediction and validation to examine the epitope basis of the effectiveness of iPM nanovax.
(a) Differentially shared membrane proteins identification. (b) Screening of immune epitopes for shared proteins. (c) The shared epitope-specific responses evoked by iPM nanovax. (d) Detecting the epitopes-specific responses in human PBMCs.
Supplementary information
Supplementary Information (download PDF )
Supplementary figures and tables.
Supplementary data (download XLSX )
Source data for the supplementary figures.
Source data
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, N., Qin, H., Zhu, F. et al. Potent prophylactic cancer vaccines harnessing surface antigens shared by tumour cells and induced pluripotent stem cells. Nat. Biomed. Eng 9, 215–233 (2025). https://doi.org/10.1038/s41551-024-01309-0
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41551-024-01309-0
This article is cited by
-
Cell reprogramming: methods, mechanisms and applications
Cell Regeneration (2025)
-
Identification of plasma extracellular vesicle protein biomarkers in diabetic retinopathy progression
Scientific Reports (2025)
-
Leveraging T cells for cancer immunotherapy
Immunity & Inflammation (2025)
-
Sharing antigens from stem cell membranes
Nature Biomedical Engineering (2024)