Abstract
Lowering mutant huntingtin (HTT) gene products is a promising approach for slowing the progression of Huntington’s disease (HD), a monogenic neurodegenerative disease caused by an expansion mutation in the HTT gene (NCBI Gene ID: 3064). Branaplam, an orally available HTT messenger RNA splicing modulator, reduces HTT protein levels in vitro and in animal models, and is the first splicing modulator to be evaluated in individuals with HD. Here we present the design and results of VIBRANT-HD, a randomized phase 2b study of branaplam in HD, along with preclinical findings in nonhuman primates. VIBRANT-HD utilized an innovative study design informed by our preclinical data, including targeted safety monitoring measures (for example, neurofilament light chain measurements in blood, nerve conduction studies), and staggered cohorts to capture potential neurotoxic effects early. Of the 21 participants in the initial cohort receiving branaplam 56 mg weekly, 18 (85.7%) showed at least one sign or symptom of peripheral neuropathy. This safety signal, along with dose-modeling results triggered the early termination of VIBRANT-HD. The primary outcome, a decrease in cerebrospinal fluid mutant HTT levels versus placebo, was summarized descriptively, making branaplam the first splicing modulator to lower mutant HTT levels in the cerebrospinal fluid of individuals with HD. Increased neurofilament light chain levels observed in most participants reversed after treatment discontinuation. ClinicalTrials.gov identifier: NCT05111249
Similar content being viewed by others
Main
Huntington’s disease (HD) is an autosomal dominant, life-limiting neurodegenerative disease caused by a mutation in the gene encoding HTT, a protein involved in cellular processes including neuronal development and function1,2,3,4. The mutation involves an expansion in the number of trinucleotide (CAG) repeats, leading to the transcription of expanded messenger RNA species and the production of abnormally long versions of HTT (mutant huntingtin (mHTT))5. mHTT may form aggregates in neurons, possibly disrupting cellular processes and causing neurodegeneration, with symptoms and signs including motor dysfunction, cognitive decline and psychiatric disturbances6,7. Recent evidence has shown that the mutant mRNA transcripts may additionally contribute to cellular dysfunction in HD8.
While existing therapies for HD are limited to symptomatic treatment, strategies that aim to suppress the formation of the mHTT products, either the mRNA transcripts or mHTT, have the potential to halt or slow disease progression9. One particularly attractive therapeutic strategy involves the use of orally bioavailable, brain-penetrant small molecules that modulate splicing, leading to lower levels of HTT mRNA and protein.
Branaplam was originally developed as a treatment for spinal muscular atrophy (SMA), in which it increases the amount of functional survival motor neuron protein produced by the SMN2 gene by modifying its mRNA splicing10,11.
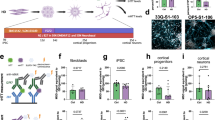
Branaplam was also shown to modify the splicing of HTT mRNA and became the first oral splicing modulator evaluated in people with HD12,13,14. Full-length HTT mRNA includes 67 exons, which are all typically spliced together during transcription, with intervening introns spliced out. Branaplam disrupts this process by promoting the inclusion of a pseudoexon with premature stop codons (Fig. 1). These stop codons lead to degradation of the HTT mRNA before it can be translated into protein, resulting in decreased production of both normal HTT and mHTT. Branaplam had been shown to lower mHTT levels in neuroblastoma cells of individuals with HD and in an HD mouse model (BacHD)13. Before being explored in people with HD, oral branaplam was also shown to lower blood HTT mRNA expression in children with type I SMA (NCT02268552)13.
HTT gene transcription and branaplam mode of action. Branaplam modifies the splicing of HTT mRNA, resulting in the inclusion of a pseudoexon which introduces premature stop codons and leads to HTT mRNA decay.
Based on animal studies and human genetics, a 30%–50% reduction in mHTT and normal HTT in the brain may slow disease progression while preserving the function of normal HTT15,16. Lowering the expression of total or mutant HTT in the brain is associated with a corresponding decrease in HTT levels in the cerebrospinal fluid (CSF)17, and a reduction of up to 40% in CSF mHTT has been shown to be safe and well tolerated in humans18.
Modulation of mRNA splicing nevertheless carries risks associated with off-target effects19. Safety studies of branaplam in dogs identified a potential risk of neurotoxicity, as evidenced by axonal degeneration of peripheral nerves and spinal cord20, and preliminary studies in nonhuman primates (NHPs) were indicative of a neuropathic effect (‘Results’). However, studies in juvenile mice, rats and dogs demonstrated that branaplam has no impact on neurogenesis in juvenile animals21. Moreover, careful monitoring of young children who received branaplam for up to 7 years in the SMA trial did not reveal any risk of axonal degeneration13 (S. Jevtic et al., manuscript in preparation) suggesting that safety signals observed in some preclinical animal models may not occur in humans. The broad distribution of branaplam throughout the brain and periphery, including the cortex and striatum (key brain regions in the neuropathology of HD), and its lowering effect on HTT and/or mRNA levels in cells of people with HD, BacHD mice and people with SMA13, combined with the ability to monitor for potential safety risks, provided a strong foundation for investigating the benefit–risk ratio of branaplam in people with HD13.
In the first part of this paper, we report the results of two studies carried out in NHPs to evaluate the safety profile of branaplam and to support the use of neurofilament light chain (NfL) levels as a prodromal biomarker for peripheral neurotoxicity. In the second part, we present results from the phase 2b dose-range finding and proof-of-concept VIBRANT-HD study (NCT05111249), which evaluated the safety, tolerability and pharmacodynamic (PD) effects of branaplam in participants with early manifest HD. This study aimed to identify a safe and well-tolerated oral dose of branaplam administered weekly that would lower CSF mHTT levels sufficiently to expect a clinical benefit. An innovative study design, encompassing a staggered cohort gating approach and a comprehensive and new safety monitoring plan that included the use of NfL as an exploratory safety signal, was put in place to identify early signs and symptoms of peripheral neurotoxicity. Here, we report the results of safety, PD and pharmacokinetic (PK) analyses from the VIBRANT-HD study along with modeling data that ultimately led to termination of the development of branaplam for HD.
Results
Preclinical—nonhuman primates
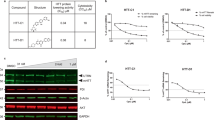
Nonclinical safety studies in rats, dogs and NHPs were conducted to support the clinical development of branaplam. While initially dog was chosen as the nonrodent toxicology species20, additional studies of 6 and 39 weeks’ duration were conducted in NHPs because their metabolic pattern is more comparable with that of humans. In particular, a major human metabolite of branaplam (UFB112) was identified that is not produced in rat or dog at appreciable levels, but is produced in NHPs, prompting further toxicology studies in this species22.
We previously reported that induction of peripheral neurotoxicity with branaplam in dogs was accompanied by increased NfL levels in serum and CSF, which correlated with neurodegeneration observed histologically20. Similarly, a dose-related increase in NfL levels was observed in the NHP studies described here. The results of the initial NHP study, including cynomolgus monkeys (n = 12; all males) dosed with branaplam 0, 0.6, 3.0 or 6.0 mg kg−1 twice a week for a total of 6 weeks, demonstrated increased serum and CSF NfL levels at the end of treatment. Although NfL levels in CSF were generally higher than those in serum, these levels showed a good correlation across the two biofluids (Fig. 2a).
NfL levels in NHPs dosed with branaplam twice a week in the 6- and 39-week studies. a, CSF and serum NfL levels at 6 weeks. Bar charts represent mean ± s.e. b, Plasma NfL levels over time up to 39 weeks. Error bars represent s.e. aMeasures were performed at weeks 13, 30 and recovery week 17 in females, and at weeks 17, 31 and recovery week 16 in males.
Because NfL levels in peripheral blood proved to be a robust marker and blood samples are easier to obtain than CSF samples, only plasma NfL levels were determined in the subsequent NHP study, in which cynomolgus monkeys were dosed with branaplam 0.6, 3.0 or 6.0 mg kg−1twice a week for up to 39 weeks (n = 40; 50% males). The mid- and high-dose levels were not well tolerated, and after 30–31 weeks of dosing, dosing suspension or early euthanasia was required for some animals as per the study protocol. Doses of ≥3 mg kg−1 branaplam twice a week induced increased plasma NfL levels as early as day 29 (week 4) in some animals, with most showing increased NfL levels by day 92 or 120 (week 13 or 17) (Fig. 2b). In addition, a subgroup of animals from the control (4 of 12) and high-dose (6 mg kg−1; 4 of 12) groups were kept for a treatment-free period of up to 16–17 weeks to assess plasma NfL levels after cessation of dosing. In these animals, plasma NfL levels decreased, and returned to pre-dose values after 16–17 weeks of recovery (Fig. 2b).
Histopathology
A histopathological assessment of nervous tissues was performed in both NHP studies. In the 6-week study, no histopathological change indicative of a neuropathic effect was observed. This discrepancy, when compared with the previous dog study, is most likely due to the early observation timepoint (6 weeks post-dose) at which histological changes were not yet manifest. In the 39-week study, at all dose levels there were findings in the peripheral and/or central nervous systems that were suggestive of a sensory peripheral neuropathy. Microscopic findings indicative of peripheral neuropathy were observed in the spinal cord (dying-back axonopathy), cervical, thoracic and/or lumbar; lumbar and/or cervical dorsal root ganglion (including dorsal spinal roots); and/or the fibular, medial plantar, radial, sciatic (left and/or right), sural, tibial and/or ulnar nerves of unscheduled and terminal necropsy animals that received ≥3 mg kg−1 twice a week. Microscopic findings indicative of sensory neuropathy were also observed in the peripheral nerves (sciatic, tibial, ulnar and/or fibular) of animals that received ≥0.6 mg kg−1 twice a week. A trend towards partial and/or full resolution of branaplam-related sensory peripheral neuropathy was observed after treatment cessation (see Supplementary Tables 1 and 2 for more details on microscopic findings observed in each treatment arm and after the recovery phase, respectively). The histology findings were comparable to those observed in dogs20. Altogether, these results demonstrated the utility of NfL as an early, predictive biomarker of safety, supporting our decision to use it as an exploratory safety signal in the VIBRANT-HD study.
No changes in body weight, qualitative food consumption, physical examination, ophthalmic observations, neurobehavioral observations, vital signs, echocardiogram (ECG) findings, coagulation, urinalysis, organ weights or macroscopic observations were attributable to branaplam.
Clinical—VIBRANT-HD
Study population and early termination
VIBRANT-HD, which started on 8 December 2021, planned to include 75 participants. However, after cohort 1 was fully recruited, the study treatment was temporarily suspended on 5 August 2022 because of safety concerns related to signs and signals of potential peripheral neuropathy. Four months later, following careful monitoring of the study participants and a review of unblinded data by the VIBRANT-HD cohort gating assessment team, it was determined that the benefit–risk ratio was not favorable. The decision was then made to permanently discontinue the study treatment and halt the development of branaplam as a potential treatment for people with HD. This decision was endorsed by the independent Data Monitoring Committee as well as the VIBRANT-HD Steering Committee. The Data Monitoring Committee and Steering Committee agreed with the study team’s recommendation for participants in the active arm to be followed up for 1 year after treatment discontinuation to monitor safety.
Overall, only 61 participants were screened, of whom 26 completed screening (Extended Data Fig. 1a) and were randomized to cohort 1 (with first participants enrolled on 10 January 2022 and the last on 4 July 2022). Because only these 26 participants were included in the data analysis (all in cohort 1), the original planned analyses of primary, secondary and exploratory endpoints to demonstrate efficacy and dose-range finding were no longer applicable.
The randomized participants were treated for a variable amount of time (treatment exposure ranging from 5 to 22 weeks) before treatment discontinuation. As requested, those in the active arm were followed up for 1 year (up to week 69) (Extended Data Fig. 1b). A total of 21 participants received branaplam 56 mg weekly, including 15 who remained in the study until week 69 and 6 who terminated early. Five participants received placebo; they were all part of the study until week 33.
Despite a low number of participants and a resulting gender imbalance in the placebo group, all baseline disease characteristics were similar between the two arms (Extended Data Table 1).
Safety findings
Safety findings leading to treatment discontinuation
Safety signals suggestive of potential peripheral neuropathy were captured very early in some individuals of cohort 1, which prompted a temporary suspension of study treatment and a review of unblinded data up to 11 weeks following the last dose. The results of this review demonstrated that 85.7% of the participants receiving branaplam 56 mg weekly had one or more signs or symptoms potentially indicative of peripheral neuropathy (including changes in the neurological examination or in nerve conduction and symptom reports) and 71.4% showed an increase in NfL levels after 9 weeks of treatment. Magnetic resonance imaging (MRI) findings also suggested an increase in lateral ventricle volume in most participants receiving branaplam. Although MRI data were preliminary and no clinical symptoms were attributed to this particular finding, altogether these results led to the decision to permanently stop treatment with the 56 mg dose and to not initiate any additional cohorts. The 1-year follow-up of participants in the active arm was particularly aimed at further assessing signs and symptoms of peripheral neuropathy and collecting additional MRI data.
Modeling data leading to study termination
In parallel, a translational PK–PD model created using data from the BacHD mouse model and adapted to humans was retrospectively utilized to determine whether lower or less-frequent doses could still demonstrate a sufficient mHTT-lowering effect with a potentially better safety profile; that is, whether any doses and/or dose regimens were anticipated to lead to at least 30% lowering of CSF mHTT with a smaller branaplam exposure than the 56 mg weekly regimen23.
The translational PK–PD model, which was able to predict the preliminary observed reduction in mHTT in the CSF of participants with HD, was further used to simulate the decrease in mutant protein levels at steady state (maximum reduction in mHTT levels) with a range of doses and dosing regimens.
The modeling and simulation work showed that, while some regimens could lead to less branaplam exposure than 56 mg once weekly, potentially with a better safety profile (Fig. 3a), none of those regimens would lead to at least 30% lowering of CSF mHTT (Fig. 3b). The 56 mg dose administered once weekly achieved the minimum reduction in mHTT levels that is expected to offer clinical benefits. These conclusions were key arguments in the decision to terminate the development of branaplam in HD.
Predicted branaplam PK and PD between weeks 49 and 53 for different dosing regimens. a, Branaplam AUC. Boxes show the median and interquartile range (IQR), the whiskers extend to 1.5× IQR and the dots represent the values beyond the whiskers. The dashed horizontal line represents the median AUC between weeks 49 and 53 for the 56 mg once a 1 week treatment. Simulations performed assuming 1,000 participants per treatment group, all with the same body weight (70 kg). b, Simulated median CSF mHTT percentage ratio to baseline. The solid horizontal line shows the target decrease of 30%, the dashed horizontal line represents the mHTT 100% ratio to baseline values. Q1W, once every 1 week; Q2W, once every 2 weeks; Q4W, once every 4 weeks.
Safety findings during the study treatment and at the end of the 1-year follow-up are presented in the following three sections.
Neurofilament light chain
Most of the branaplam-treated participants from cohort 1 (who received 56 mg weekly) showed elevations in NfL levels that typically began at week 9. According to one of our two preset definitions of elevation (Methods), 76.2% and 61.9% of the participants in the active arm had an increase in serum NfL and CSF NfL levels, respectively, compared with no participants in the placebo arm (Fig. 4a and Supplementary Table 3). At the end of the study, all participants with follow-up data showed reversal of the increase in serum NfL levels (no follow-up data for CSF NfL).
Safety findings related to neurotoxicity (safety analysis set). a, Individual serum and CSF levels of NfL over time. The upper limit for the range of the serum NfL assay is 500 pg ml−1. Values above 500 mg ml−1 are imputed to 501 pg ml−1 for the purpose of analysis. Assessment is defined as ‘on treatment’ if the assessment date is within 2 weeks after the last dose. b, Neuropathy-related findings and resolution. A neurological examination finding is defined by two or more consecutive decreased or absent deep tendon reflexes and/or sensory findings. AEs (preferred terms) indicative of neurotoxicity or peripheral neuropathy included axonal and demyelinating polyneuropathy, axonal neuropathy, coordination abnormal, electric shock sensation, hypogeusia, hyporeflexia, loss of proprioception, neuralgia, neuropathy peripheral, paresthesia, peripheral sensory neuropathy, polyneuropathy and oral discomfort (Supplementary Table 6).
Neuropathy
In line with the results of the interim review leading to study termination, 18 of 21 (85.7%) participants who received branaplam 56 mg weekly had at least one sign or symptom potentially indicative of peripheral neuropathy, as demonstrated by nerve conduction studies (NCS), neurological examination or reported in the neuropathy questionnaire or as an adverse event (AE) (Fig. 4b and Supplementary Table 4). These were either resolved or downgraded in severity at the end of the 1-year follow-up period (Fig. 4b and Supplementary Tables 4 and 5). Details on all neuropathy findings are provided in Supplementary Tables 4–6).
Based on the NCS results, 11 of 21 (52.4%) participants in the branaplam 56 mg weekly arm had a ≥50% reduction in sural sensory nerve action potential (SNAP) amplitude and 3 (14.3%) participants in tibial compound motor action potential (CMAP) amplitude. By contrast, only one (20%) participant in the placebo arm showed a ≥50% reduction in one of the NCS measures (tibial CMAP). Sural SNAP returned to baseline at the final visit (week 69) in four (36.4%) participants and in all three participants with tibial CMAP (Supplementary Table 5A).
Neurological examinations with new findings of reduced motor function (weakness), reduced or absent deep tendon reflexes or decreased or absent sensory function at two consecutive visits were reported in 13 (61.9%) participants in the branaplam 56 mg arm. Among these 13 participants, 8 recovered partially and 2 recovered fully after the 1-year follow-up period. No participants in the placebo arm had any abnormal findings noted in their neurological examinations (Supplementary Tables 4 and 5B).
Neuropathy symptoms were confirmed using a neuropathy questionnaire in six (28.6%) participants in the branaplam 56 mg arm compared with one (20.0%) in the placebo arm. Five (83.3%) participants in the branaplam 56 mg arm recovered partially and one (16.7%) recovered fully (Supplementary Tables 4 and 5C).
Neuropathy was reported as an AE in 13 (61.9%) participants (Fig. 4b and Supplementary Table 4) in the branaplam arm versus 1 (paresthesia) in the placebo arm. Three (23.1%) participants with branaplam-related AEs fully recovered. The details of neuropathy-related AEs are provided in Supplementary Table 6.
Lateral ventricle measurements using MRI
At week 17, the mean percentage change in lateral ventricle volume was higher in branaplam-treated participants than in those on placebo, with results from the subgroup analysis excluding participants with subdural hematoma consistent with the primary analysis (Fig. 5a and Supplementary Table 7, respectively). The rate of change in ventricular volume in the subsequent weeks appeared to be similar to that observed initially in the placebo arm, and the difference between the two groups decreased.
Percentage change from baseline in volumetric MRI (safety analysis set). a, Lateral ventricle. b, Whole brain. c, Caudate. The results exclude participants with subdural hematoma. Numbers are means and data points are means (s.e.). The red diamond represents a single data point from one placebo participant who had an MRI at Week 53. TRACK-HD, observational TRACK-HD study used as external control arm24.
Clinical and pharmacodynamic assessments
Measured mHTT protein levels
Branaplam at a dose of 56 mg weekly for 5–22 weeks lowered mHTT levels in the CSF. Mean percentage (s.e.) change from baseline to week 9 in CSF mHTT was −22.3% (3.34; 17 participants) with branaplam 56 mg compared with −6.4% (15.05; 5 participants) with placebo at week 9, and −26.6% (7.45; 9 participants) with branaplam 56 mg compared with −1.4% (10.26; 4 participants) with placebo at week 17 (Fig. 6). At week 17, the difference in mean percentage (s.e.) change (branaplam 56 mg to placebo) was −25.2% (−2.81), indicating a 25.2% placebo-corrected lowering of mHTT levels in the CSF. Spaghetti plots are presented in Supplementary Fig. 1.
Percentage change from baseline in CSF mHTT levels over time (safety analysis set). Data show mean percent change from baseline over time in mHTT protein levels in CSF. Error bars represent standard errors.
These findings are in line with the predicted mHTT lowering based on translational PK–PD modeling data (‘Modeling data leading to study termination’). Branaplam 56 mg weekly interacted with the target, leading to a decrease in HTT mRNA and an increase in HTT pseudoexon (PS50A) inclusion in blood (Supplementary Fig. 2).
Unified Huntington’s Disease Rating Scale
There were no treatment-induced changes in secondary clinical measures, including the Unified Huntington’s Disease Rating Scale (UHDRS) Total Functional Capacity (TFC), UHDRS Total Motor Score (TMS), UHDRS Independence Scale (IS), the composite UHDRS (cUHDRS) (Extended Data Fig. 2) and UHDRS-Functional Assessment Scale (FAS) (not shown). Changes in these measures in the branaplam 56 mg arm from baseline to week 69 were consistent with those typically observed for the annual rate of decline for participants at this disease stage.
Volumetric MRI
Volumetric MRI of the whole brain, caudate and lateral ventricles was originally intended for measuring the effect of branaplam 56 mg on slowing disease progression over a longer period. Volumetric MRI of the lateral ventricles was also used as a safety biomarker considering reports of increased ventricular volume following treatment with other HTT-lowering agents (‘Safety findings’)24.
There were no meaningful differences in mean percentage change in whole-brain volume and caudal volume (left and right) from baseline between the placebo and branaplam 56 mg treatment arms (Fig. 5b,c). An increase in lateral ventricle volume was observed with branaplam compared with placebo, as described in the ‘Safety findings’ section (Fig. 5a). The results for all volumetric MRI measures reported in Fig. 5 exclude participants with subdural hematoma; they were consistent with the analysis based on the full analysis set (Supplementary Table 7). Volumetric MRI measures in branaplam-treated participants were also compared with those of a matched cohort from the observational TRACK-HD study used as external control arm24 (Methods). Figure 5a suggests that the rate of increase in lateral ventricular volume after discontinuation from branaplam is similar to the expected rate observed in the matched observational, natural history TRACK-HD cohort.
Cognition
No treatment-induced changes were observed in any of the exploratory cognitive measures including Stroop Word Reading Test (SWRT), Montreal Cognitive Assessment (MoCA) and Symbol Digit Modalities Test (SDMT) (Supplementary Fig. 3).
Adverse events
Overall, AEs were experienced by 76.9% (20 of 26) of the participants from cohort 1, 40.0% (2 of 5) in the placebo arm and 85.7% (18 of 21) in the branaplam 56 mg arm, with 20.0% (1 of 5) and 66.7% (14 of 21), respectively, considered treatment related. Most AEs were mild or moderate in severity. All 19.0% (4 of 21) serious AEs (SAEs) were reported in the branaplam 56 mg arm and 14.3% (3 of 21) were considered treatment related. Treatment-related SAEs were subdural hematoma (two participants) and vestibular neuronitis (one participant). The percentage of participants with AEs leading to study drug discontinuation was 7.7% in cohort 1, all (9.5%; 2 of 21) in the branaplam 56 mg arm. None of the participants had fatal SAEs (Supplementary Table 8).
Pharmacokinetics
The median time to reach the maximum concentration (Tmax), the maximum concentration (Cmax), the area under the curve (AUC) from time zero to 168 h (7 days) after the last dose (AUC0–168h) and the total drug exposure across time are given in Supplementary Table 9. Following single and repeated oral administration of branaplam 56 mg, branaplam concentrations increased slowly, with Tmax values of approximately 7.0 h and 4.2 h at weeks 1 and 17, respectively. At week 1, mean Cmax was 26.1 ng ml−1 and AUC0–168h was 1,880 h ng ml−1, whereas at week 17, mean Cmax increased to 45.3 ng ml−1 and AUC0–168h to 3,190 h ng ml−1. The drug’s accumulation, as measured by comparing the Cmax and AUC0–168h values between weeks 17 and 1, showed a 1.49-fold increase in exposure for both parameters. The variability in mean Cmax and AUC0–168h values ranged from 14.3% to 30.6%, indicating low to moderate variability between individuals.
The trough concentration (Ctrough) values of branaplam 56 mg weekly, which were determined from weeks 2 to 17, indicated that a steady state of branaplam 56 mg exposure was achieved from week 5 onwards, with the Ctrough ratio (compared with week 2) reaching a maximum of 2.20 at week 5 (data not shown).
Discussion
Here we present the results of a randomized, double-blind, placebo-controlled trial of an oral HTT-lowering agent in people with HD. The initiation of VIBRANT-HD, a phase 2b dose-range finding and proof-of-concept study of the splicing modulator branaplam, was motivated by the demonstration of a HTT-lowering effect in both preclinical HD models and in children with type 1 SMA13, as well as the encouraging safety findings in children with SMA treated with branaplam for 7 years (S. Jetvic et al., manuscript in preparation). To mitigate the potential risk of neurotoxicity, as identified by preclinical animal studies in dogs20 and preliminary results in NHPs, we developed an innovative protocol including a staggered cohort approach along with multimodal monitoring for neurotoxicity (NfL, NCS, neurological examination and neuropathy questionnaire). The staggered cohort approach allowed for assessment of the safety and tolerability of lower doses of branaplam before randomizing participants to higher doses. This study design proved effective by enabling the detection of safety signals in the initial phase of the study, which prompted its early termination. Additional data in NHPs were gathered in parallel to the clinical trial, providing deeper insights into the potential outcomes and underlying mechanisms.
The initial safety signal was observed at the 56 mg once weekly dose, the lowest of the planned dose regimens, typically as an increase in serum NfL levels. Our preclinical data in NHPs, which showed an increase in NfL levels before any histological change, supported such use of NfL as an early exploratory clinical trial safety biomarker. This early signal was followed by measured or reported signs or symptoms indicative of peripheral neuropathy in most, but not all participants, which ultimately led to the decision to stop treatment in the 56 mg arm and not to proceed with any of the higher dose arms. Unfortunately, the modeling simulations indicated that a lower dose was unlikely to lower mHTT levels sufficiently to expect any clinical benefits, culminating in the final decision to stop the development of branaplam for HD.
Importantly, the signs and symptoms suggestive of neuropathy were either partially or fully reversed after treatment discontinuation in both VIBRANT-HD participants and our preclinical studies in NHPs, as demonstrated by follow-up safety monitoring measures including NfL levels, NCS and neurological examination.
Lateral ventricle volume appeared to transiently increase in participants receiving branaplam compared with those who received placebo at week 17. However, there was some recovery by week 33, after which progression occurred at a similar rate to that of an external matched control group from the TRACK-HD study24. It is not known whether the observed volume increase is due to changes in CSF flow dynamics as a consequence of lowering wild-type HTT levels or whether this is due to a neurotoxic effect related to branaplam. The rapid onset and reversibility of the effect, the lack of detectable loss of brain tissue, as indicated by other volumetric MRI measures, and the absence of any associated symptoms (for example, cognitive decline, confusion, gait problems) argue in favor of this being a consequence of lowering the wild-type HTT levels, an important modulator of cilia genesis25,26. Interestingly, a similar observation was reported for another HTT-lowering investigational therapy—an intrathecally administered antisense oligonucleotide27—suggesting that this phenomenon may be shared across routes of administration and therapeutic modalities.
As expected, weekly oral doses of branaplam 56 mg lowered the levels of mHTT in CSF (by 25% compared with placebo at week 17). This shows that an oral drug is capable of reducing CSF mHTT levels in people with HD. The extent of mHTT lowering is consistent with that predicted by our translational PK–PD modeling data, and this finding is in line with previous evidence showing that branaplam exhibits dose-dependent effects in lowering total and mutant HTT levels in BacHD mice, fibroblasts and induced pluripotent stem cell-derived cortical neurons of controls and people with HD13. The increase in HTT mRNA pseudoexon usage observed in our trial is also consistent with the expected mechanism of action of branaplam.
The mechanisms by which branaplam may cause peripheral neuropathy are not yet clear and would require further investigation. Based on in vitro data, nuclear stress and subsequent p53 activation have been postulated as a mode of action28,29. However, comprehensive gene expression data from in vivo studies in dogs do not support this hypothesis20. The hypothesis is also not supported by our in vitro and NHP study results, which are due to be published separately. In any case, neuropathy-related signals are unlikely to be due to the lowering of HTT levels because branaplam does not modulate HTT mRNA splicing in dogs or NHPs. Therefore, the observed peripheral neuropathy in these species is most likely a consequence of off-target splicing modulation yet to be identified. These data underscore the importance of comprehensive safety explorations of investigational therapies in multiple species including organ systems beyond the intended targeted organ.
Interestingly, branaplam treatment did not induce cellular toxicity in patients with HD12, consistent with the absence of neurotoxicity indicators in infants enrolled in the SMA trial (S. Jevtic et al., manuscript in preparation). Proposed mechanisms are only speculative because the data available so far are insufficient to draw a definite conclusion.
As a limitation, following the early termination of the VIBRANT-HD trial, the number of participants in the placebo arm was one-quarter of that in the branaplam arm, and these participants were followed up for up to 33 weeks, versus 69 weeks for the branaplam arm, which makes the comparison between treatment arms more difficult. This imbalance was partly addressed by the post hoc inclusion of an external control arm based on historical data from the TRACK-HD study. It should also be noted that follow-up of NfL levels in the branaplam arm was conducted only in serum, with no CSF NfL measurements performed after treatment discontinuation.
To conclude, the results of the VIBRANT-HD clinical trial demonstrate that an oral HTT mRNA splice modulator can lower mHTT levels in the CSF of people with HD. The results also demonstrate the utility of a robust and data-driven safety monitoring plan and clinical trial design to allow for the safe therapeutic assessment of an experimental treatment with detected preclinical safety signals. Such a design enabled us to promptly reach the decision to pause and subsequently terminate dosing upon detecting the earliest signals of potential peripheral neurotoxicity. Finally, the preclinical and clinical findings presented here highlight the importance of exploratory biomarkers such as NfL to serve as early safety signals and support further evaluation of more selective HTT mRNA splicing modulators.
Methods
NHP studies
Study designs
All procedures in the 6-week and 39-week studies were in compliance with the Animal Welfare Act, the Guide for the Care and Use of Laboratory Animals, the Office of Laboratory Animal Welfare, and fully commensurate with international standards of Good Laboratory Practices and approved by the local Institutional Animal Care and Use Committee.
The 6-week NHP study was designed as a dose-range finding study conducted in male cynomolgus monkeys (Macaca fascicularis) obtained from Envigo Global Services Inc. At dosing initiation, the monkeys were approximately 31–38 months of age and weighed 2.1–3.0 kg. Doses of branaplam 0.6, 3 and 6 mg kg−1 were administered twice a week as a suspension or solution through oral gavage to three groups (three animals per group) of monkeys twice weekly for 6 weeks. In an additional group, animals (n = 3) received vehicle control article at an equivalent dosing volume of 5 ml kg−1, serving as controls.
The 39-week toxicology study was conducted in male (n = 20) and female (n = 20) cynomolgus monkeys. The animals were obtained from Envigo Global Services Inc. (2 males) and Worldwide Primates Inc. (20 males and 22 females; including 2 spare animals). At dosing initiation, animals were approximately 29–61 months old and weighed 2.0–4.9 kg for males and 2.1–4.5 kg for females.
Branaplam was administered twice weekly for up to 39 weeks to three groups of cynomolgus monkeys (groups 2–4; four or six animals per sex per group), each receiving a different branaplam dose (Extended Data Table 2). Another group of cynomolgus monkeys (group 1; six animals per sex) received the vehicle and served as controls.
The reversibility of the effects was assessed during an extended (16 weeks for males and 17 weeks for females) recovery phase for a subset of animals receiving the highest dose or the vehicle control (see details in Extended Data Table 2).
Assessments
Clinical observations (daily), body weight (once pre-dose and weekly throughout the dosing phase), food consumption determinations (daily), ophthalmology, clinical pathology (hematology, coagulation and clinical chemistry) evaluations, ECG, physical examination, vital signs and neurobehavioral observations were performed. Necropsies were also performed, with a recording of macroscopic abnormalities for all animals and tissues. Microscopic examinations were conducted on a standard list of organs and tissues of all animals.
Blood samples were collected for serum (6-week study) or plasma (39-week study) NfL biomarker analysis. In the 6-week study, CSF (at necropsy) samples were also collected for NfL analysis. Blood samples were collected on days 1 and 36 pre-dose and at 0.5, 2, 4, 7, 12, 24 and 96 h post-dose, and on day 41 before euthanasia for toxicokinetic analyses. Whole-blood samples were collected for serum (pre-dose day 1; days 8, 15, 29 and 40; and day 41).
In the 39-week study, blood samples were collected twice during the pre-dose phase; at 2 h post-dose on days 29, 120, 176 and 253; and once on the day before the scheduled euthanasia. Because of the early termination of dosing for group 3 and 4 animals, blood samples were collected 2 h post-dose on days 215 (males) and 208 (females) of the dosing phase.
NfL sample preparation and analysis
Blood samples were collected into tubes containing potassium (K2) EDTA as the anticoagulant and maintained on chilled cryoracks before and after centrifugation. Samples were centrifuged within 30 min of collection for approximately 10 min in a refrigerated centrifuge (set to maintain 4 °C) at approximately 1,100–1,300g. Following harvesting, samples were stored on dry ice until placed in a freezer, set to maintain at −60 °C to −80 °C, until shipped to Novartis Institutes for BioMedical Research, Inc.
For the determination of serum, plasma and CSF NfL levels, samples were thawed and analyzed at 4-fold, 5-fold and 100-fold dilution, respectively, using a qualified single-molecule array immunoassay according to the manufacturer’s instructions (Simoa NF-light Advantage Kit for SR-X; cat. no. 103400, Quanterix), read on a Quanterix Simoa SRX analyzer, and data were analyzed using SoftMax Pro v.5.4.1 (Molecular Devices).
Histopathology
Tissues from all animals at the terminal necropsy and from all animals euthanized at an unscheduled interval were embedded in paraffin, sectioned at a nominal 5-µm thickness, and slides were prepared and stained with hematoxylin and eosin based on best practice guidelines recommended by the Society of Toxicologic Pathology30 and test facility standard operating procedures. Following completion of the primary microscopic evaluation, an independent peer review evaluation was performed by the sponsor. The pathologic evaluation of individual animals represents the consensus of the principal investigator for anatomic pathology and the reviewing pathologist.
VIBRANT-HD
Study design
The VIBRANT-HD study was conducted according to ICH E6 Guidelines for Good Clinical Practice that have their origin in the Declaration of Helsinki. The study protocol was reviewed and approved by institutional review boards and ethics committees at each participating site, including: Comité de Protection des Personnes Sud-Ouest et Outre-Mer II (Toulouse, France); Ethikkommission der Universität Ulm (Ulm, Germany); SZTE Klinikai Központ Regionális IKEB (Szeged, Hungary); Semmelweis Egyetem Regionális Intézményi Tudományos és Kutatásetikai Bizottsága (RKEB) (Budapest, Hungary); CEIm Fundació de Gestió Sanitària Hospital de la Santa Creu i Sant Pau (Barcelona, Spain); and Comité d’éthique de la recherche du Centre Hospitalier de l’Université de Montréal (CER CHUM) (Montreal, Canada).
VIBRANT-HD was designed as a randomized, double-blind, placebo-controlled study including a core part with a variable duration (consisting of a 17-week dose-range finding portion followed by a blinded extension for up to approximately 53 weeks) and a 1-year open-label extension in approximately 75 participants with early-stage manifest HD (Extended Data Fig. 3).
The innovative study design included a staggered cohort approach, starting with branaplam 56 mg oral solution or matching placebo once weekly (cohort 1), which would allow the assessment of the safety and tolerability of lower doses before randomizing participants to higher doses. As planned, the core period consisted of three treatment arms; each of which would enroll approximately 25 participants. Sex or gender was not stratified because of the small number of participants planned for each dose cohort.
More details on treatment, randomization and blinding are provided in the Supplementary Methods.
Participants
This study was conducted at 12 HD Centers of Excellence in Canada, France, Germany, Spain and Hungary. The study population included male and female participants aged >25 years with confirmed stage 1 or 2 HD (based on the Shoulson and Fahn staging system)31, ≥40 CAG repeats in the huntingtin gene and a UHDRS-TFC score of >8. An age cap of 75 years was used to avoid age-related comorbidities (see Supplementary Information for full inclusion and exclusion criteria).
The study design was informed by input from a patient advisory meeting held before protocol finalization. Informed consent was obtained from each participant in writing before screening and before any study-specific procedure was performed. No financial compensation was provided; only study-related expenses were reimbursed.
Study endpoints and assessments
This study had two primary endpoints:
-
(1)
The efficacy primary endpoint was the percentage change from baseline in mHTT concentration in CSF at week 17, calculated as \(\frac{(\text{mHTT at week 17}\mbox{--}\text{mHTT at baseline})}{\text{mHTT at baseline}}\times 100\). Because the early termination of the trial (‘Results’) led to a small sample size, the primary endpoint of mHTT in CSF was summarized descriptively based on the safety analysis set. The average percentage change over time (at actual weeks) from baseline was provided for each treatment group, along with error bars. In addition, a spaghetti plot was used to display the percentage change for each participant in each group. The protein assay used to measure mHTT is described in the Supplementary Information.
-
(2)
Safety and tolerability parameters and assessments included, but were not limited to, neurological examination, NCS, laboratory assessments, vital signs, cardiac function and routine safety monitoring of AEs and SAEs. To monitor for potential risks of neurotoxicity, the neurological examination (deep tendon reflexes, sensory and motor function components) was comprehensive, and a neuropathy questionnaire was completed. The NCS included CMAP and SNAP, which were performed at the screening visit to serve as a baseline and were repeated if, in the opinion of the investigator, there was a potential peripheral neuropathy based on participant self-reporting through the neuropathy questionnaire and/or abnormal findings on neurological examination. Based on the recommendation of the study neurophysiologist expert, a reduction in SNAP, CMAP or nerve conduction velocity values >50% was considered clinically relevant. Lastly, although typically used as an exploratory efficacy biomarker, NfL in serum and CSF was also used to monitor for potential neurotoxicity signal.
Secondary and exploratory endpoints included in this study were as follows.
UHDRS
The UHDRS is a research tool developed by the Huntington Study Group, which has undergone extensive reliability and validity testing to provide a uniform assessment of the clinical features and course of HD32. For this study, the UHDRS components collected were UHDRS-TFC, UHDRS-TMS, UHDRS-IS and UHDRS-FAS, which were summarized descriptively by visit and treatment group. These components are clinician-guided assessments based on participant interview, physical examination and observation during motor activities. The cUHDRS, combining motor (TMS), cognitive (SDMT and SWRT) and global functional (TFC) clinical outcome measures, was also assessed33. For more information, please refer to the Supplementary Information.
NfL in serum and CSF
NfL was an exploratory safety measure. Because serum NfL was monitored throughout the study as an early signal for potential neurotoxicity, two preset cutoffs were established that would trigger either repeat NfL testing or further neurological assessment: >100 pg ml−1 or more than 2× baseline sNfL. CSF NfL was not used to monitor for safety, but the cutoffs were established during the analysis of safety data: >10,000 pg ml−1 or CSF NfL >2× baseline CSF NfL or CSF NfL >2× CSF NfL of the previous assessment.
Volumetric MRI
Changes in volumetric MRI, including ventricular, caudate and whole-brain volume, were measured in regions of interest. Imaging data were collected, checked for quality and read centrally as specified in the Imaging Review Charter by an imaging vendor (IXICO) designated by Novartis. Lateral ventricular volume was assessed and monitored for early detection of any changes during the course of the study.
Cognitive measures
Efficacy assessments also included cognitive measures (SWRT, SDMT and MoCA). SWRT is a measure of processing and psychomotor speed34, with scores based on the number of color names read correctly. SDMT is used to assess attention, working memory, psychomotor speed and visual perceptual processing35, with scores based on the number of correctly paired items using a translation key. MoCA is a screening test that assesses several cognitive domains shown to be sensitive in HD, with lower scores representing increased cognitive impairment36.
The full details on the original endpoints and details on the clinical (HD and cognitive) and volumetric MRI assessments are presented in the Supplementary Methods.
PK and biomarkers
PK parameters (for example, AUC, Cmax, Tmax, Ctrough) in plasma as well as CSF concentrations of branaplam and its metabolite, UFB112, were determined across the study duration by validated liquid chromatography with tandem mass spectrometry. The anticipated lower limit of quantification was 0.500 ng ml−1. Concentrations were expressed in mass per volume units and referred to the free base. Concentrations below the lower limit of quantification were reported as ‘zero’, and missing data were labeled as such in the Bioanalytical Data Report.
Droplet digital polymerase chain reaction was utilized to measure the treatment-induced increase in the expression level of pseudoexon-including HTT mRNA, demonstrating the mechanism of action of branaplam as an HTT mRNA splice modulator.
In line with the decision to permanently discontinue the study treatment, blood samples for PK and biomarker analyses (including mHTT) and PAXgene samples for gene expression analyses were collected in all randomized participants up to 6 weeks after the last dose of the study drug (details on the methodology and assays are given in Supplementary Methods).
PK–PD modeling and translation from BacHD mice to humans
PK and mHTT protein kinetics data in mice were pooled from rich and sparse sampling studies, including PK, toxicokinetic and PK–PD studies conducted by Novartis in which mice were administered branaplam (10–50 mg kg−1 orally) at three doses per week for 3 weeks. Branaplam PK in mice was well described by a two-compartment model with first-order absorption, a lag time and linear elimination, using Monolix (v.2018r1, Lixoft). Population PK parameters were fixed, and PD parameters were subsequently estimated. mHTT protein kinetics were described using a turnover model incorporating inhibition of mHTT synthesis, accounting for the observed time delay (PK Tmax ~3–6 h; mHTT nadir ~72 h post-dose). PK–PD modeling was performed using mHTT reduction data from both mouse striatum (135 samples) and mouse cortex (204 samples) to predict mHTT changes in human CSF.
The PK part of the human model was built using data from a phase 1 single-dose study in 24 healthy subjects (doses ranging from 35 to 420 mg). Branaplam PK was best described with a sequential zero- and first-order absorption with a lag time, a two-compartment distribution and a linear elimination. Participants’ body weight was found to be a covariate impacting branaplam clearance and central volume of distribution. PD parameters were scaled by assuming that half-maximal inhibitory concentration (IC50) values in humans are threefold lower than those estimated in mice (reflecting a three times better penetration into the human brain compared to monkeys) and that mHTT turnover (kout) can be scaled by allometry. The PK–PD model was validated using data from participants in the VIBRANT-HD study. For each participant, branaplam plasma and mHTT CSF concentrations were simulated 100 times. The individual simulations were summarized using the median and 90% prediction interval. These values were plotted against the observed values, demonstrating that the model adequately described both branaplam PK and CSF mHTT changes in participants with HD. The validated model was then used for dose simulations with a range of doses and dosing regimens.
Statistical analysis
Sample size was determined by feasibility and was evaluated using the primary endpoint, namely mHTT reduction in CSF from baseline to week 17. n = 75 for three dose arms (three active treatment groups with n = 20 in each arm and a placebo group with n = 15) was sufficient to reach more than 80% power on average for detecting a dose–response signal using multiple comparison procedures-modeling (MCP-Mod) methodology (under the MCP step) with a one-sided significance level of 5%. The calculations were based on the assumption of 35% mHTT lowering in the CSF (for the highest dose) and 0% mHTT lowering for placebo. The assumptions on standard deviation were based on ref. 15 An inflation factor of 50% was applied to the s.d. of both the active groups (s.d. = 0.195) and the placebo group (s.d. = 0.471) to be conservative, leading to an overall treatment effect size of approximately 1. Sample size calculation was performed in RStudio v.3.6.1 using package ‘DoseFinding’. Because of the early study termination, only one cohort was initiated and only 26 participants were enrolled.
Following the termination of the study, the originally planned analyses of primary, secondary and exploratory endpoints, designed to demonstrate efficacy and identify dose ranges, were no longer applicable. Instead, descriptive summary statistics were provided, including clinical endpoints (for example, UHDRS and its subscales), volumetric MRI data by region, and biomarker endpoints (HTT, mHTT and NfL in serum and/or CSF). Standard safety endpoints were also summarized, encompassing AEs, laboratory findings, vital signs, ECG results and related measures. Neurotoxicity and recovery were assessed based on neurological examinations, NCS, and increases in NfL, among other factors. For continuous variables, descriptive statistics—including mean, median, s.d. and range—were reported. For categorical variables, frequencies and relative percentages were summarized.
All analyses were performed on the safety analysis set of the first cohort, which consists of all participants who received at least one dose of study drug over the core period. SAS v.9.4 (SPSS) and higher was used for the analyses.
External control arm
To address the imbalance in sample size and follow-up duration between the placebo and branaplam arms following early termination of the study, a post hoc analysis was conducted using propensity score–matched patients from the prospective observational TRACK-HD study24 as controls (1:1 matching with a total of 26 patients).
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
Protocol and SAP are available on ClinicaltTrials.gov at https://cdn.clinicaltrials.gov/large-docs/49/NCT05111249/Prot_000.pdf and https://cdn.clinicaltrials.gov/large-docs/49/NCT05111249/SAP_001.pdf, respectively. The reader is able to request the raw data (anonymized) and related documents (for example, clinical study report) of the clinical study by connecting to CSDR (https://www.clinicalstudydatarequest.com) and signing a Data Sharing Agreement with Novartis. The data will be made available to researchers, with requests reviewed and approved by an independent review panel of CSDR
References
Ross, C. A. et al. Huntington disease: natural history, biomarkers and prospects for therapeutics. Nat. Rev. Neurol. 10, 204–216 (2014).
Walker, F. O. Huntington’s disease. Lancet 369, 218–228 (2007).
Seefelder, M., Klein, F. A. C., Landwehrmeyer, B., Fernández-Busnadiego, R. & Kochanek, S. Huntingtin and its partner Huntingtin-Associated Protein 40: structural and functional considerations in health and disease. J. Huntingtons Dis. 11, 227–242 (2022).
Saudou, F. & Humbert, S. The biology of huntingtin. Neuron 89, 910–926 (2016).
MacDonald, M. E. et al. A novel gene containing a trinucleotide repeat that is expanded and unstable on Huntington’s disease chromosomes. Cell 72, 971–983 (1993).
Shao, J. & Diamond, M. I. Polyglutamine diseases: emerging concepts in pathogenesis and therapy. Hum. Mol. Cell 16, R115–R123 (2007).
Ross, C. A. & Tabrizi, S. J. Huntington’s disease: from molecular pathogenesis to clinical treatment. Lancet Neurol. 10, 83–98 (2011).
Heinz, A., Nabariya, D. K. & Krauss, S. Huntingtin and its role in mechanisms of RNA-mediated toxicity. Toxins (Basel) 13, 487 (2021).
Caron, N. S., Dorsey, E. R. & Hayden, M. R. Therapeutic approaches to Huntington disease: from the bench to the clinic. Nat. Rev. Drug Discov. 17, 729–750 (2018).
Childs-Disney, J. L. et al. Targeting RNA structures with small molecules. Nat. Rev. Drug Discov. 21, 736–762 (2022).
Palacino, J. et al. SMN2 splice modulators enhance U1–pre-mRNA association and rescue SMA mice. Nat. Chem. Biol. 11, 511–517 (2015).
Krach, F. et al. An alternative splicing modulator decreases mutant HTT and improves the molecular fingerprint in Huntington’s disease patient neurons. Nat. Commun. 13, 6797 (2022).
Keller, C. G. et al. An orally available, brain penetrant, small molecule lowers huntingtin levels by enhancing pseudoexon inclusion. Nat. Commun. 13, 1150 (2022).
Dash, D. & Mestre, T. A. Therapeutic update on Huntington’s disease: symptomatic treatments and emerging disease-modifying therapies. Neurotherapeutics 17, 1645–1659 (2020).
Tabrizi, S. J., Ghosh, R. & Leavitt, B. R. Huntingtin lowering strategies for disease modification in Huntington’s disease. Neuron 101, 801–819 (2019).
Leavitt, B. R., Kordasiewicz, H. B. & Schobel, S. A. Huntingtin-lowering therapies for Huntington disease: a review of the evidence of potential benefits and risks. JAMA Neurol. 77, 764–772 (2020).
Southwell, A. L. et al. Ultrasensitive measurement of huntingtin protein in cerebrospinal fluid demonstrates increase with Huntington disease stage and decrease following brain huntingtin suppression. Sci. Rep. 5, 12166 (2015).
Tabrizi, S. J. et al. Targeting huntingtin expression in patients with Huntington’s disease. N. Engl. J. Med. 380, 2307–2316 (2019).
Ottesen, E. W. et al. Diverse targets of SMN2-directed splicing-modulating small molecule therapeutics for spinal muscular atrophy. Nucleic Acids Res. 51, 5948–5980 (2023).
Theil, D. et al. Neurofilament light chain: a translational safety biomarker for drug-induced peripheral neurotoxicity. Toxicol. Pathol. 51, 135–147 (2023).
Theil, D. et al. Orally administered branaplam does not impact neurogenesis in juvenile mice, rats, and dogs. Biol. Open 10, bio058551 (2021).
Lozac’h, F, et al. Insights into the human pharmacokinetics and metabolism of branaplam, a splicing modulator of a survival motor neuron-2 (SMN2) and huntingtin (HTT) pre-MRNAs, in infants and adults. Drug Metab. Dispos. (in the press).
Faller, D. O., Faller, T., Caputo, A., Borowsky, B. & Laisney, M. Branaplam translational PK/PD model supported key decision making in Huntington’s disease. In Development Innovation Conference (2023).
Tabrizi, S. J. et al. Predictors of phenotypic progression and disease onset in premanifest and early-stage Huntington’s disease in the TRACK-HD study: analysis of 36-month observational data. Lancet Neurol. 12, 637–649 (2013).
Kaliszewski, M., Knott, A. B. & Bossy-Wetzel, E. Primary cilia and autophagic dysfunction in Huntington’s disease. Cell Death Differ. 22, 1413–1424 (2015).
Karam, A. et al. A novel function of huntingtin in the cilium and retinal ciliopathy in Huntington’s disease mice. Neurobiol. Dis. 80, 15–28 (2015).
McColgan, P. et al. Tominersen in adults with manifest Huntington’s disease. N. Engl. J. Med. 389, 2203–2205 (2023).
Börstler, T. et al. I010 RNA splicing modulator for Huntington’s disease treatment induces 1 peripheral neuropathy. J. Neurol. Neurosurg. Psychiatry 95, A145 (2024).
Krach, F. et al. RNA splicing modulator for Huntington's disease treatment induces peripheral neuropathy. iScience 28, 112380 (2025).
Bolon, B. et al. STP position paper: recommended practices for sampling and processing the nervous system (brain, spinalcord, nerve, and eye) during nonclinical general toxicity studies. Toxicol. Pathol. 41, 1028–1048 (2013).
Shoulson, I. & Fahn, S. Huntington disease: clinical care and evaluation. Neurology 29, 1–3 (1979).
Huntington Study Group Unified Huntington’s Disease Rating Scale: reliability and consistency. Mov. Disord. 11, 136–142 (1996).
Schobel, S. A. et al. Motor, cognitive, and functional declines contribute to a single progressive factor in early HD. Neurology 89, 2495–2502 (2017).
Golden, C. J. Identification of brain disorders by the Stroop Color and Word Test. J. Clin. Psychol. 32, 654–658 (1976).
Smith, A. Symbol Digit Modalities Test (Western Psychological Services, 1973).
Nasreddine, Z. S. et al. The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J. Am. Geriatr. Soc. 53, 695–699 (2005).
Acknowledgements
We thank M.-C. Mousseau (from Novartis Ireland Ltd, Dublin, Ireland) for writing the first draft of this manuscript, coordinating reviews and incorporating comments from authors. We also thank D. Papanicolaou, P. C. Arratia, S. Jevtic and F. O’Riain for their contribution to the planning and execution of the VIBRANT-HD study. In addition, we extend our gratitude to all the participants and investigators who were involved in the study as well as the branaplam/LMI070 Program Steering Committee and the branaplam/LMI070 program Data Monitoring Committee members (Supplementary Table 10). The study was funded by Novartis. Novartis participated in study design, data interpretation and drafting of the manuscript, and was responsible for manufacturing the investigational product and matching placebo as well as data collection, monitoring and data analysis.
Author information
Authors and Affiliations
Contributions
B.B., H.R., A.C., T.F., T.P., Y.S., F.L., M.M., A.K., K.S.M., S.J.T., G.B.L. and B.R.L. contributed to VIBRANT-HD study design and study conduction. B.B., H.R., A.C., T.F., T.P., A.K., Y.S., F.L. and M.M. contributed to the data analysis of VIBRANT-HD. O.J.D. and M.L. contributed to data modeling. A.H. contributed to the NHP study design, data analysis and interpretation. All contributed to data interpretation, critically reviewed the draft and provided their final approval.
Corresponding author
Ethics declarations
Competing interests
K.S.M. received funding of grants from Parkinson’s Foundation for acting as a Steering Committee Member, receives funding of grants from NIH, MJFF, CHDI, HSG, HDSA, Prilenia, Novartis, Roche and Springer, and receives consulting fees from Novartis and funding for leadership on the Enroll HD Oversight Committee (CHDI) and HSG Steering Committee. S.J.T. received research grant funding from the Wellcome Trust (grant no. 223082/Z/21/Z), and the UK Dementia Research Institute that receives its funding from DRI Ltd, funded by the UK MRC, Alzheimer’s Society and Alzheimer’s Research UK, and from the CHDI Foundation and the UK Medical Research Council. Through the offices of UCL Consultants Ltd, a wholly owned subsidiary of University College London, S.J.T. has undertaken consultancy services for Alnylam Pharmaceuticals, Annexon, Ascidian Therapeutics, Arrowhead Pharmaceuticals, Atalanta Therapeutics, Design Therapeutics, F. Hoffman-La Roche, Iris Medicine, Latus Bio, Life Edit, Novartis Pharma, Pfizer, Prilenia Neurotherapeutics, PTC Therapeutics, Rgenta Therapeutics, Takeda Pharmaceuticals, UniQure Biopharma and Vertex Pharmaceuticals. In the past 12 months, University College London Hospitals NHS Foundation Trust, Professor Tabrizi’s host clinical institution, received funding to run clinical trials for F. Hoffman-La Roche, Novartis Pharma, PTC Therapeutics and UniQure Biopharma. G.B.L. has provided consulting services, advisory board functions, clinical trial services and/or lectures for Acadia Pharmaceuticals, AFFiRiS, Allergan, Alnylam, Amarin, AOP Orphan Pharmaceuticals AG, Bayer Pharma AG, Boehringer Ingelheim, CHDI Foundation, Deutsche Huntington-Hilfe, Desitin, Genentech, Genzyme, GlaxoSmithKline, F. Hoffmann-La Roche, Ipsen, ISIS Pharma (IONIS), Eli Lilly, Lundbeck, Medesis, Medivation, Medtronic, NeuraMetrix, Neurosearch Inc., Novartis, Pfizer, Prana Biotechnology, Prilenia, PTC Therapeutics, Raptor, Remix Therapeutics, Rhône-Poulenc Rorer, Roche Pharma AG Deutschland, Sage Therapeutics, Sanofi-Aventis, Sangamo/Shire, Siena Biotech, Takeda, Temmler Pharma GmbH, Teva, Triplet Therapeutics, Trophos, UniQure and Wave Life Sciences. B.L. was a member of the scientific advisory board and Steering Committee for the VIBRANT-HD study. He reports paid scientific consultancies with Alnylam, GLG, Teva, Roche/Genentech, Takeda, Triplet, Ionis, Novartis, Spark, Sintetica, Life Edit, Design, Remix Therapeutics, 3RD Rock and PTC Therapeutics and sRNAlytics (now GateHouse Bio). Dr Leavitt’s Laboratory has obtained research grants from CIHR, HSC, NMIN, CHDI, Teva, ProMIS and uniQure. He is a co-founder and the current CEO of Incisive Genetics Inc. B.B., H.R., A.C., T.F., T.P., Y.S., F.L., M.M., O.J.D., M.L. and A.K. are employees and shareholders of Novartis. A.H. was an employee of Novartis at the time of the study and is now retired.
Peer review
Peer review information
Nature Medicine thanks Andrew McGarry and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Peer reviewer reports are available. Primary Handling Editor: Jerome Staal in collaboration with the Nature Medicine team.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Participant disposition: a) CONSORT diagram; b) Individual treatment exposure and follow-up timeline.
*One participant from the placebo arm discontinued early but still completed week 33; 2 of the 8 participants from the branaplam 56 mg weekly arm who discontinued early still completed week 69. n, number of participants in each category; N, number of participants in the safety analysis set.
Extended Data Fig. 2 Change from baseline in Huntington clinical measures (safety analysis set).
Error bars represent s.e. cUHDRS = (TFC − 10.4)/1.9 − (TMS − 29.7)/14.9 + (SDMT − 28.4)/11.3 + (SWRT − 66.1)/20.1 + 10. Mean (s.d.) change from baseline at week 17 for placebo and branaplam 56 mg, respectively, were: −1.0 (2.35) and −0.8 (2.39) for UHDRS TFC; 6.0 (11.29) and 5.1 (9.14) for UHDRS TMS; −1.0 (11.40) and −1.8 (9.16) for UHDRS IS; −1.18 (1.813) and −1.09 (1.783) for cUHDRS; and −1.4 (3.21) and −1.1 (2.82) for UHDRS-FAS. cUHDRS, composite unified Huntington’s disease rating scale; IS, independence scale; s.d., standard deviation; SE, standard error; TFC, total functional capacity; TMS, total motor score.
Extended Data Fig. 3 Study design*.
All eligible participants were randomized via Interactive Response Technology to one of the treatment arms. *After cohort 1 was fully enrolled, safety concerns led to the decision not to initiate additional cohorts and to monitor participants who received active treatment (branaplam) for an additional year (see Results).
Supplementary information
Supplementary Information (download PDF )
Supplementary Tables 1–10, Figs. 1–3 and Methods.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Borowsky, B., Ramos, H., Caputo, A. et al. Oral splicing modulator branaplam in Huntington’s disease: a phase 2 randomized controlled trial. Nat Med 32, 103–112 (2026). https://doi.org/10.1038/s41591-025-04117-4
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41591-025-04117-4