Abstract
Eosinophils are a part of the human immune system and have traditionally been thought to be associated with allergic reactions. Recent research has revealed their potentially important role in cardiovascular disease. We retrospectively collected data on 1155 patients who were diagnosed with carotid artery stenosis at our center from January 2016 to June 2021. These data included demographic information, laboratory measurements, and carotid ultrasounds. We constructed predictive models through binary logistic regression. A total of 1,155 patients were ultimately included in this study, among whom 157 experienced major adverse cardiovascular and cerebrovascular events (MACCE) within a three-year follow-up period. Multifactorial adjustment showed that previous operation history (OR 1.66[1.14–2.41], P = 0.008), previous history of stroke (OR 1.59[1.10–2.31], P = 0.014), total proteins (OR 0.97[0.95–0.99], P = 0.02), erythrocyte sedimentation rate(OR 1.01[1.01–1.02], P = 0.031), eosinophil counts(OR 4.62[1.60–13.35], P = 0.005) and treated with calcium channel blockers(CCBs) + β-blockers(BBs) (OR 3.08[2.04–4.63], P < 0.001) were independently associated with 3-year MACCE. Based on these key factors, the prediction model we constructed demonstrated satisfactory prediction performance, with an initial value of 0.739 for the area under the curve, which was stabilised at 0.721 after adjustment. After a dichotomous analysis of eosinophils based on cut-off values, we assessed their role in different outcomes. The results of the analysis showed that eosinophil counts was a significant risk factor for all the outcomes considered. Patients with carotid artery stenosis exhibiting a baseline eosinophil counts of 0.185*109/L had a higher incidence of MACCE. Furthermore, a previous 3-year operation history, previous history of stroke, total proteins, erythrocyte sedimentation rate and treated with a combination of CCBs and BBs were also significantly associated with the occurrence of MACCE.
Similar content being viewed by others
Introduction
Atherosclerotic cardiovascular disease (ASCVD) is the most prevalent disease worldwide, and its complications remain the leading cause of death globally1,2. The carotid artery is the main blood vessel supplying blood to the human brain, and major adverse cardiovascular events such as stroke caused by carotid artery lesions have become a serious public health concern3,4. The primary cause of carotid artery stenosis is the formation and progressive enlargement of atherosclerotic plaques, leading to luminal narrowing. With advancing age, both the incidence and severity of carotid artery stenosis increase significantly, thereby markedly elevating the risk of major cardiovascular events5. Aging, diabetes, hyperlipidemia, and hypertension are traditional risk factors for atherosclerosis. They contribute to the initiation and progression of atherosclerosis through mechanisms such as promoting lipid deposition, inducing low-grade chronic inflammation, triggering oxidative stress, and impairing endothelial function6,7,8,9,10. However, traditional ASCVD risk factors may not be reliable enough due to variations in problematic vessels, individual differences, and lifestyle factors. Therefore, it has become a trend to explore novel biomarkers for complete cardiovascular risk stratification to guide clinical prognostic interventions.
Eosinophils (EO) were first discovered by Paul Ehrlich11 in 1879. Eosinophils are members of the innate immune system. After maturation in the bone marrow, eosinophils enter the peripheral blood circulation, where they participate in the immune response. In the blood of healthy individuals, eosinophils make up 1–5% of the total number of leukocytes12. Although they are well known for their role in allergic reactions, eosinophils also regulate the immune balance by secreting a variety of inflammatory mediators and chemokines, which also play a crucial role in the prevention and treatment of non-allergic diseases12,13,14. More and more studies have clarified that it is significantly related to the occurrence and development of cardiovascular diseases15,16,17. Research has demonstrated that eosinophils can post-myocardial infarction preserve cardiac function and delay the development of an AngII-induced abdominal aortic aneurysm18,19. However, in atherosclerosis, eosinophils contribute to atherosclerosis by infiltrating into the vessel wall through the release of eosinophil cationic proteins (ECP) and by interacting with platelets16,20. In a large-scale clinical study from the UK Biobank, a significant association was found between eosinophil counts and cardiovascular disease and its mortality21. However, another study found lower eosinophil counts in patients with ST-segment elevation myocardial infarction(STEMI) who experienced major adverse cardiovascular events(MACE)22. In response to this seemingly contrary discovery, Norbert Gerdes23 shared his discovery that a high eosinophil counts in patients with stable cardiovascular diseases (CVD) predicted risk for MACE in the future. In contrast, acute injury may recruit eosinophils from the circulation due to injured tissue, which would result in a decrease in the number of eosinophils in the blood23. This hypothesis highlights that eosinophils may play different roles at different stages of the disease, thereby affecting their number in the circulation. However, the evidence is limited in regard to the occurrence of major adverse cardiac and cerebrovascular events (MACCE) after carotid stenosis. Therefore, the objective of this study was to determine whether the levels of eosinophil counts at admission could indicate the long-term prognosis of patients with carotid stenosis.
Materials and methods
Patient selection
This study followed the Declaration of Helsinki, was approved by the Institutional Ethics Committee of the Second Hospital of Shanxi Medical University, and the informed consent form were obtained. (No. 2023126) We retrospectively recruited 1892 patients who underwent carotid ultrasound between January 2016 and June 2021, of whom 1660 were diagnosed with carotid stenosis. Carotid stenosis was considered to be more than 30% stenosis according to the criteria of the North American Symptomatic Carotid Endarterectomy Trial (NASCET) group24. According to the Carotid artery stenosis: gray-scale and Doppler US diagnosis—Society of Radiologists in Ultrasound Consensus Conference, carotid occlusion was considered to be either no blood flow in the lumen or failure to detect lumen25. Symptomatic patients presented with transient ischemic attack, transient blackout, or minor nondisabling stroke within 180 days prior. Conversely, asymptomatic patients26.
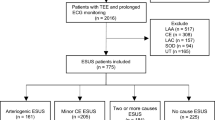
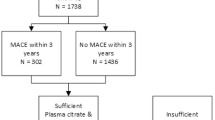
Patients with acute infections, severe renal disease (serum creatinine > 1.4 mg/dL), severe hepatic disease (hepatic function parameters > 3 × upper limit of normal), hematologic disorders, autoimmune disorders, malignant neoplasms, or incomplete critical medical records were excluded. In addition, preexisting events that could have influenced the determination of the endpoint outcome of the present study, such as: within the past 30 days myocardial infarction or severe stroke, were also excluded as confounders. A total of 1291 patients were enrolled in this study. Three investigators without prior knowledge of the patients’ clinical data followed up all patients by telephone to determine whether MACCE had occurred. Ultimately, we successfully followed up on 1155 individuals (Fig. 1).
Flow diagram of patient selection.
Data collection
All data were collected from medical electronic records by clinicians who were unaware of the purpose of the study. This included patients’ demographic characteristics [Age, Gender, Height, Weight, and body mass index (BMI)], cardiovascular risk factors [Smoke, Drunk, Hypertension, Diabetes, history of stroke], laboratory parameters [Fibrinogen, Activated partial thromboplastin time, ALT, AST, Bilirubin, Creatinine, Urea nitrogen, Homocysteine, Lipids, Red blood cells, Leukocytes, Platelets, Hemoglobin, etc.], surgical history [CEA\CAS and surgery], medication [antiplatelet agents, hypoglycemic, beta-blockers, angiotensin-converting enzyme inhibitors (ACEIs)/angiotensin receptor blockers (ARBs), calcium channel blockers, etc.], and carotid ultrasound [carotid artery branch plaques, carotid branch of the largest plaque, maximum plaque length, maximum plaque width, maximum plaque area, etc.] Peripheral blood samples were collected after overnight fasting and blood biochemistry levels were determined in a central laboratory.
Carotid ultrasound
Carotid ultrasound was performed by senior sonographers, who were not informed of the participants’ basic information and laboratory indicators in advance. All procedures are performed according to diagnostic criteria established by the American College of Radiology in 200325. Participants were placed in a supine position and examined using an iU22 ultrasound system (Philips Healthcare) and a 6–10 array mhz linear array transducer. Bilateral common carotid artery (CCAs), internal carotid artery (ICAs), external carotid artery (ECAs), subclavian artery and vertebral artery diameter and stenosis rate were recorded accurately.
Endpoints
The primary endpoint outcome of this study was the occurrence of MACCE, defined as a composite of transient ischemic attack(TIA), ischemic stroke, acute myocardial infarction(AMI), or all-cause death27. Deaths from clear causes of non-cardiovascular disease were excluded. Secondary endpoints included TIA\ischemic stroke, AMI. The outcome diseases were diagnosed by senior specialists or supported by examination reports.
Missing value
Variables with missing values > 30% were excluded, and the remaining missing values were imputed through the ‘mice’ package in R. The imputation dataset was 20 times, and the with and pool function selected the imputation set that was most consistent with the original dataset.
Statistical analysis
A retrospective cohort study was conducted, and statistical analysis was performed using R (version 4.2.2). Quantitative variables are expressed as the mean ± standard deviation (mean ± SD), while categorical variables are expressed as percentages (%). The Kolmogorov‒Smirnov test was used to check for a normal distribution. Student’s t test or X2 test was deployed to compare the variables of interest between the MACCE outcome groups. Receiver operating characteristic (ROC) curve analysis was carried out on significant continuous variables to determine the cutoff value with the highest sum of sensitivity and specificity in the predicted event. In light of the scientific objectives of this study, the statistical properties of the predictors, and the nature of the dataset, logistic regression was employed to systematically investigate the associations between risk factors and the outcome variable. Factors with significant univariate relationships with MACCE (p < 0.05) were included in the binary logistic multiple regression model. The reliability of the model was assessed using ROC curves, and the consistency of the model was confirmed using calibration curves.
Results
A total of 1155 participants (68.37% male) were included. Traditional cardiovascular disease risk factors, including diabetes (28.21%), hypertension (61.03%), operation history (37.13%) and previous stroke history (30.92%), exhibited a high prevalence in this study population. It is noteworthy that 29.03% of the patients had symptomatic carotid artery stenosis (Table 1). The use of multiple imputation for missing variables did not significantly affect the results (Supplementary Table 1).
MACCE occurred in 157 patients within 3 years after the diagnosis of carotid stenosis (total events 13.59%, TIA or stroke 8.57%, AMI 3.29%, and mortality 3.46%). Compared with the control group, the MACCE group had a significantly higher proportion of patients with a history of drinking alcohol, previous 3-year operation history, and previous history of stroke. In addition, this group had higher mean maximum plaque width and eosinophil counts(EO), and a higher proportion of patients were on hypoglycemic and antihypertensive medications. At the same time, their total protein levels(TP), blood calcium concentrations(Ca), homocysteine levels(HCY), and low-density lipoprotein cholesterol (LDL.C) levels were relatively low. Notably, the largest plaques in patients who developed MACCE were more commonly found on the left side of the body. Baseline data showed no significant difference between the two groups in the prevalence rates of hyperglycemia and hypertension. However, patients who experienced MACCE required medication more frequently, reflecting the possibility that they may have poorer control of their diseases and thus be an important risk factor for the development of MACCE. In contrast to previous studies28, however, LDL.C levels were lower in the MACCE group, a difference that may be related to the smaller sample size in our study (Table 1).
The univariate logistic regression results showed that a history of drinking alcohol (OR 1.55 [1.11–2.18], p = 0.011), previous 3-year operation history (OR 2.12 [1.51–2.98], p < 0.001), previous history of stroke (OR 1.64[1.16–2.32], p = 0.005), history of carotid artery stenting (OR 2.14 [1.12–4.11], p = 0.021), the largest plaque was located on the right side (OR 0.69 [0.49–0.96], p = 0.029), maximum plaque width (OR 6.04 [1.54–23.71], p = 0.01), total proteins (TP) (OR 0.98 [0.95–1.00], p = 0.025), LDL.C(OR 0.76 [0.61–0.96], p = 0.019), erythrocyte sedimentation rate(ESR)(OR 1.01 [1.00–1.02], p = 0.025), EO(OR 4.03 [1.65–9.84], p = 0.002), treated with metformin and Acarbose (OR 2.18 [1.43–3.33], p < 0.001), treated with CCBs and BBs(OR 4.01 [2.78–5.77], p < 0.001), and treated with nifedipine (OR 0.58 [0.38–0.87], p = 0.008) were significantly associated with the occurrence of MACCE (Table 2). After multifactorial adjustment, previous 3-year operation history (OR 1.66[1.14 ~ 2.41], p = 0.008), previous history of stroke (OR 1.59 [1.10 ~ 2.31], p = 0.014), TP(OR 0.97 (0.95 ~ 0.99), p = 0.02), ESR(OR 1.01[1.00–1.02], p = 0.031), EO(OR 4.62 (1.60 ~ 13.35), p = 0.005) and treated with CCBs and BBs (OR 3.08 [2.04 ~ 4.63], P < 0.001) were identified as independent risk factors for long-term prognosis in patients with carotid artery stenosis(Fig. 2).
Factors associated with 3-year MACCE. Adjusted odds ratios for 3-year MACCE in the presence of associated factors during baseline Age, Gender, BMI, SBP, Smoke, Drunk, Diabetes, Hypertension.
The logistic regression model, which incorporated previous operation history, previous history of stroke, TP, ESR, EO and treated with CCBs and BBs and traditional risk factors exhibited good performance in identifying the occurrence of MACCE in patients diagnosed with carotid stenosis, with an ROC of 0.739 [95% CI 0.6977–0.7805], a sensitivity of 64.3%, and a specificity of 72.4% (Fig. 3). The calibration curve results showed a high degree of overlap between the corrected curve and the ideal curve, which implied that the model prediction results were consistent with the actual occurrence of the events in patients (Fig. 4). For the internal validation of the model, the strengthen Boostrap method was used to resample the full dataset cohort 1000 times to calculate the high estimate of the logistic regression model. The results showed a high estimate of 0.0185 for the ROC and − 0.0013 for the Brier score. After imputing the final model performance correction, the real model performed well with an ROC of 0.721 and a Brier score of 0.0539 (Table 3).
AUROC of the regression model based on Operation history, previous history of stroke, TP, ESR, EO and treated with CCBs and BBs in the full dataset.
Calibration curve of regression model based on Operation history, previous history of stroke, TP, ESR, EO and treated with CCBs and BBs in the full dataset.
Using the receiver operating characteristic (ROC) curve, we determined the optimal cutoff value for each significant univariate continuous variable with the Youden index (Supplementary Table 2). In our model analysis, the EO had the highest OR value of 4.62. To explore in depth the potential of the EO in predicting MACCE, we categorized the EO into two groups on the basis of its optimal cutoff value, and thus assessed its efficacy in predicting the primary and secondary outcomes. After adjustment for traditional risk factors such as age, sex, BMI, SBP, smoking, drinking, diabetes, and hypertension, our results showed that EO was a significant risk factor in predicting both primary and secondary outcomes of our concerns. Although no statistically significant differences were observed between the two groups for acute myocardial infarction(AMI), this may be related to the low incidence of these events (Table 4). Next, we performed a dichotomous analysis of other potential risk factors to see their effect in predicting primary and secondary outcomes. The results of the study showed that patients treated with CCBs and BBs exhibited a significant increased risk for all outcomes. (Supplementary Table 3-7).
Discussion
The severity of ASCVD in public health has been extensively studied and recognized29. The inflammatory response of the arterial wall tissue characterized by chronic progressive inflammation and the formation of sclerotic plaques plays a crucial role in pathogenesis30. The complications associated with atherosclerosis are even more critical in the carotid artery, which is the primary blood supply vessel to the brain, and its impact on cerebral perfusion provides the opportunity for stroke, myocardial infarction, and peripheral arterial disease. To explore the key factors affecting the prognosis of patients with carotid stenosis, multidimensional data, including demographic characteristics, serum laboratory measurements, and imaging features, were fully utilized. Previous studies have shown that multiple factors differ regarding their effect on the prognosis of patients with carotid stenosis. However, eosinophils, as a terminally differentiated leukocyte in the body, has not been studied thoroughly in the prognosis of carotid stenosis.
Atherosclerosis is a chronic inflammatory response whose progression is closely linked to endothelial dysfunction as well as oxidative stress31. As part of the innate immune system, eosinophils have been shown to be involved in the development of atherosclerosis and have been recognized as a promising biomarker32,33. In addition, the high expression levels of eosinophil chemokines in atherosclerotic lesions further support this finding34. Despite the fact that eosinophils contain cytokines with anti-inflammatory effects such as IL4 and IL13, the experimental results of Meng et al.20 showed that the knockout of the IL4 and IL13 genes was not sufficient to accelerate atherosclerosis development. Instead, their study revealed the important role of ECP in promoting smooth muscle cell (SMC) calcification as well as atherosclerotic progression20.
The role of eosinophils in cardiovascular disease has garnered widespread attention35, Studies have demonstrated that elevated eosinophil levels can release various cationic proteins and generate extracellular traps, thereby promoting the initiation and propagation of inflammatory responses35,36. Surfactant protein-D (SP-D), secreted by airway epithelial cells, can inhibit the formation of eosinophil extracellular traps. However, SP-D is inherently susceptible to oxidation, and once oxidized, its ability to suppress extracellular trap formation is markedly diminished37. Moreover, genetic markers associated with eosinophilia may also contribute to the pathogenesis of cardiovascular diseases. Several microRNAs, such as miR-10a, miR-125, miR-21, and miR-233, not only play regulatory roles in eosinophil-related inflammatory diseases38,39,40, but also participate in multiple key processes of atherosclerosis, including the expression of endothelial adhesion molecules, foam cell formation, macrophage polarization, and ventricular remodeling following myocardial infarction41,42. These findings suggest that eosinophil-mediated immune regulatory mechanisms may be involved in the development and progression of carotid and coronary atherosclerosis through multiple pathways, warranting further in-depth investigation. Thrombosis, a serious complication of atherosclerosis, has attracted a great deal of attention from researchers, and a study by Stefan Uderhardt et al.43 points out that eosinophils play a key role in promoting thrombosis. Studies have shown that in atherosclerosis complicated by thrombosis, eosinophils are activated by being attracted to the edge of the thrombus and interacting with platelets. This activation process leads to the production of eosinophil extracellular traps (EETs), which exacerbates the inflammatory response and thus promotes the deterioration of atherosclerosis. Also, EETs further activate platelets and exacerbate thrombus formation. These findings point to the fact that eosinophils may be a potential target for future treatment of atherosclerosis and its thrombotic complications16.
There are conflicting views in the field of clinical research on eosinophils and MACCE. Meng et al.20 reported a strong connection between eosinophil counts and levels of eosinophil cationic protein and coronary artery calcification in a randomized, controlled clinical screening experiment that included 5864 individuals with coronary artery disease. Furthermore, the results of two earlier extensive clinical studies were in agreement44,45. However, some researchers have reached contradictory conclusions, and their findings suggest that eosinophils actually play a protective role in cardiovascular disease. Gao et al.46 recruited 5,287 patients who received coronary angiograms and measured their biochemical markers in a study. The results of the study showed that the percentage of eosinophils in leukocytes showed a significant negative correlation with the degree of coronary artery stenosis and the occurrence of acute myocardial infarction. Similarly, a study by Guner et al.22 found that those patients with a low eosinophil ratio on admission were more likely to experience MACE during hospitalization. In the current controversy over the role of eosinophils in CVD, Norbert Gerdes makes the point that in stable CVD, higher levels of eosinophils may predict the risk of future adverse events; and in the case of acute injury, diseased tissue may reduce the number of blood cells detectable by recruiting eosinophils. In our study, after adjusting for traditional risk factors, those patients who experienced MACCE showed a significant increase in the number of eosinophils in the peripheral blood compared to those who did not. (OR 1.72 [1.20–2.46], p = 0.003). This is consistent with Norbert Gerdes’s point.
In addition to eosinophils, previous 3-year operation history, history of stroke, TP, ESR, treated with CCBs and BBs was also significantly associated with MACCE events at 3 years. By applying multifactor logistic regression analysis, we constructed a model for the prediction of MACCE over a 3-year period. The model had a ROC curve area value of 0.739, 0.721 after adjustment, indicating a high predictive accuracy. Notably, although not shown to be statistically significant in AMI, EO was recognised as a risk factor after dichotomisation according to the cut-off values, both in the primary and secondary outcomes.
This study has several limitations. First, it is a single-center retrospective study with a relatively small sample size, which may introduce selection bias and limit the generalizability of the findings to other populations or countries. Second, due to the retrospective nature of the study, we were only able to identify an association between eosinophil levels and the occurrence of MACCE within 3 years, without establishing a causal relationship. Prospective, multi-center studies with larger cohorts are needed to further validate the reliability and robustness of our findings. Third, the follow-up period was limited to three years, and data regarding long-term outcomes were not available, which restricts our ability to predict long-term prognosis. Fourth, the study did not include the assessment of other potential risk factors such as genetic markers, lipidomic profiles and Socio-economic levels, which may have influenced the results. Despite these limitations, our findings demonstrate that eosinophil count is an independent risk factor for MACCE within three years in patients with carotid artery stenosis, providing important support for further investigations into the role of eosinophils in the pathogenesis of atherosclerosis.
Conclusion
Eosinophil counts (> 0.185*109/L) were independently associated with the occurrence of MACCE within 3 years in patients hospitalized for carotid stenosis, but there was no significant difference in proportion of eosinophils between the two groups. In addition, previous operation history, previous history of stroke, lower TP (< 59.95 g/L), higher ESR (> 15.5 mm/h) and treated with CCBs and BBs were also strongly associated with the occurrence of MACCE.
Data availability
The data and analytical methods are available from the corresponding authors on reasonable request. Supplementary Material has been uploaded separately on submission and would be available online.
Abbreviations
- CCBs:
-
Calcium channel blockers
- BBs:
-
β-Blockers
- MACCE:
-
Major adverse cardiac and cerebrovascular event
- MACE:
-
Major adverse cardiovascular event
- ASCVD:
-
Atherosclerotic cardiovascular disease
- TIA:
-
Transient ischemic attack
- AMI:
-
Acute myocardial infarction
- ROC:
-
Receiver operating characteristic
- EO:
-
Eosinophil counts
- ECP:
-
Eosinophil cationic proteins
- STEMI:
-
ST-segment elevation myocardial infarction
- LDL.C:
-
Low-density lipoprotein cholesterol
- TP:
-
Total proteins
- Ca:
-
Calcium
- HCY:
-
Homocysteine
- ESR:
-
Erythrocyte sedimentation rate
- SMC:
-
Smooth muscle cell
- EETs:
-
Eosinophil extracellular traps
- NASCET:
-
North American symptomatic carotid endarterectomy trial
- BMI:
-
Body mass index
- CEA:
-
Carotid endarterectomy
- CAS:
-
Carotid artery stenting
- ACEI:
-
Angiotensin converting enzyme inhibitor
- ARB:
-
Angiotensin receptor blocker
- CCA:
-
Common carotid artery
- ICA:
-
Internal carotid artery
- ECA:
-
External carotid artery
References
Tsao, C. W. et al. Heart disease and stroke statistics-2023 Update: A report from the American heart association. Circulation 147(8), e93–e621. https://doi.org/10.1161/cir.0000000000001123 (2023).
Cesaro, A., Acerbo, V., Indolfi, C., Filardi, P. P. & Calabrò, P. The clinical relevance of the reversal of coronary atherosclerotic plaque. Eur. J. Int. Med. https://doi.org/10.1016/j.ejim.2024.08.010 (2024).
Roth, G. A. et al. Global, regional, and national burden of cardiovascular diseases for 10 causes, 1990 to 2015. J. Am. Coll Cardiol. 70(1), 1–25. https://doi.org/10.1016/j.jacc.2017.04.052 (2017).
Costa, D. et al. Omics science and social aspects in detecting biomarkers for diagnosis, risk prediction, and outcomes of carotid stenosis. Biomolecules 14(8), 972. https://doi.org/10.3390/biom14080972 (2024).
Piechocki, M. et al. A non-coronary, peripheral arterial atherosclerotic disease (Carotid, Renal, Lower Limb) in elderly patients-a review: Part I-epidemiology, risk factors, and atherosclerosis-related diversities in elderly patients. J. Clin. Med. 13(5), 1471. https://doi.org/10.3390/jcm13051471 (2024).
Abdellatif, M., Schmid, S. T., Fuerlinger, A. & Kroemer, G. Anti-ageing interventions for the treatment of cardiovascular disease. Cardiovasc. Res. https://doi.org/10.1093/cvr/cvae177 (2024).
Selvin, E. et al. Glycaemia (haemoglobin A1c) and incident ischaemic stroke: The Atherosclerosis Risk in Communities (ARIC) Study. Lancet Neurol. 4(12), 821–826. https://doi.org/10.1016/s1474-4422(05)70227-1 (2005).
Leenen, F. H. Blood pressure lowering, not vascular mechanism of action, is the primary determinant of clinical outcome. Can. J. Cardiol. 20(Suppl B), 77b–82b (2004).
Soppert, J., Lehrke, M., Marx, N., Jankowski, J. & Noels, H. Lipoproteins and lipids in cardiovascular disease: From mechanistic insights to therapeutic targeting. Adv. Drug. Deliv Rev. 159, 4–33. https://doi.org/10.1016/j.addr.2020.07.019 (2020).
Jannat, T., Sheikh, R., Tamanna, S. & Islam, L. N. Oxidative stress and inflammatory leukocyte markers in people with type 2 diabetes: A single center, cross-sectional study. Clin. Diabetol. 12(3), 156–163. https://doi.org/10.5603/DK.a2023.0017 (2023).
Kay, A. B. The early history of the eosinophil. Clin. Exp. Allergy 45(3), 575–582. https://doi.org/10.1111/cea.12480 (2015).
Lombardi, C., Berti, A. & Cottini, M. The emerging roles of eosinophils: Implications for the targeted treatment of eosinophilic-associated inflammatory conditions. Curr. Res. Immunol. 3, 42–53. https://doi.org/10.1016/j.crimmu.2022.03.002 (2022).
Aoki, A., Hirahara, K., Kiuchi, M. & Nakayama, T. Eosinophils: Cells known for over 140 years with broad and new functions. Allergol. Int. 70(1), 3–8. https://doi.org/10.1016/j.alit.2020.09.002 (2021).
Yang, Y. et al. Novel IL-4/HB-EGF-dependent crosstalk between eosinophils and macrophages controls liver regeneration after ischaemia and reperfusion injury. Gut 73(9), 1543–1553. https://doi.org/10.1136/gutjnl-2024-332033 (2024).
Siedlinski, M. et al. White blood cells and blood pressure: A Mendelian randomization study. Circulation 141(16), 1307–1317. https://doi.org/10.1161/circulationaha.119.045102 (2020).
Marx, C. et al. Eosinophil-platelet interactions promote atherosclerosis and stabilize thrombosis with eosinophil extracellular traps. Blood 134(21), 1859–1872. https://doi.org/10.1182/blood.2019000518 (2019).
Zhao, Y. et al. Comprehensive macro and micro views on immune cells in ischemic heart disease. Cell Prolif. 57, 13725. https://doi.org/10.1111/cpr.13725 (2024).
Liu, J. et al. Eosinophils improve cardiac function after myocardial infarction. Nat. Commun. 11(1), 6396. https://doi.org/10.1038/s41467-020-19297-5 (2020).
Liu, C. L. et al. Eosinophils protect mice from angiotensin-II perfusion-induced abdominal aortic aneurysm. Circ. Res. 128(2), 188–202. https://doi.org/10.1161/circresaha.120.318182 (2021).
Meng, Z. et al. Cationic proteins from eosinophils bind bone morphogenetic protein receptors promoting vascular calcification and atherogenesis. Eur. Heart J. 44(29), 2763–2783. https://doi.org/10.1093/eurheartj/ehad262 (2023).
Welsh, C. et al. Association of total and differential leukocyte counts with cardiovascular disease and mortality in the UK biobank. Arterioscler. Thromb. Vasc. Biol. 38(6), 1415–1423. https://doi.org/10.1161/atvbaha.118.310945 (2018).
Güner, A. et al. Eosinophil percentage as a new prognostic marker in patients with ST-segment elevation myocardial infarction undergoing primary percutaneous coronary intervention. Interv. Med. Appl. Sci. 11(3), 146–153. https://doi.org/10.1556/1646.11.2019.17 (2020).
Gerdes, N. Eosinophils promote vascular calcification and atherosclerosis: Adding another layer of complexity on the path to clarity?. Eur. Heart J. 44(29), 2784–2786. https://doi.org/10.1093/eurheartj/ehad323 (2023).
Eliasziw, M., Rankin, R. N., Fox, A. J., Haynes, R. B. & Barnett, H. J. Accuracy and prognostic consequences of ultrasonography in identifying severe carotid artery stenosis. North American Symptomatic Carotid Endarterectomy Trial (NASCET) Group. Stroke 26(10), 1747–1752. https://doi.org/10.1161/01.str.26.10.1747 (1995).
Grant, E. G. et al. Carotid artery stenosis: Gray-scale and Doppler US diagnosis–Society of radiologists in ultrasound consensus conference. Radiology 229(2), 340–346. https://doi.org/10.1148/radiol.2292030516 (2003).
Brott, T. G. et al. Stenting versus endarterectomy for treatment of carotid-artery stenosis. N. Engl. J. Med. 363(1), 11–23. https://doi.org/10.1056/NEJMoa0912321 (2010).
Smilowitz, N. R. et al. Perioperative major adverse cardiovascular and cerebrovascular events associated with noncardiac surgery. JAMA Cardiol. 2(2), 181–187. https://doi.org/10.1001/jamacardio.2016.4792 (2017).
Ference, B. A., Braunwald, E. & Catapano, A. L. The LDL cumulative exposure hypothesis: Evidence and practical applications. Nat. Rev. Cardiol. https://doi.org/10.1038/s41569-024-01039-5 (2024).
Zheng, W. C., Chan, W., Dart, A. & Shaw, J. A. Novel therapeutic targets and emerging treatments for atherosclerotic cardiovascular disease. Eur. Heart J. Cardiovasc. Pharmacother. 10(1), 53–67. https://doi.org/10.1093/ehjcvp/pvad074 (2024).
Björkegren, J. L. M. & Lusis, A. J. Atherosclerosis: Recent developments. Cell 185(10), 1630–1645. https://doi.org/10.1016/j.cell.2022.04.004 (2022).
Botts, S. R., Fish, J. E. & Howe, K. L. Dysfunctional vascular endothelium as a driver of atherosclerosis: Emerging insights into pathogenesis and treatment. Front. Pharmacol. 12, 787541. https://doi.org/10.3389/fphar.2021.787541 (2021).
Kita, H. Eosinophils: Multifaceted biological properties and roles in health and disease. Immunol. Rev. 242(1), 161–177. https://doi.org/10.1111/j.1600-065X.2011.01026.x (2011).
Niccoli, G. et al. Eosinophil cationic protein: A new biomarker of coronary atherosclerosis. Atherosclerosis 211(2), 606–611. https://doi.org/10.1016/j.atherosclerosis.2010.02.038 (2010).
Haley, K. J. et al. Overexpression of eotaxin and the CCR3 receptor in human atherosclerosis: Using genomic technology to identify a potential novel pathway of vascular inflammation. Circulation 102(18), 2185–2189. https://doi.org/10.1161/01.cir.102.18.2185 (2000).
Xu, J. et al. Differential roles of eosinophils in cardiovascular disease. Nat. Rev. Cardiol. 22(3), 165–182. https://doi.org/10.1038/s41569-024-01071-5 (2025).
Mackman, N. Eosinophils, atherosclerosis, and thrombosis. Blood 134(21), 1781–1782. https://doi.org/10.1182/blood.2019003027 (2019).
Yousefi, S. et al. Oxidative damage of SP-D abolishes control of eosinophil extracellular DNA trap formation. J. Leukoc. Biol. 104(1), 205–214. https://doi.org/10.1002/jlb.3ab1117-455r (2018).
Tarallo, A. et al. MiR-21–5p and miR-223–3p as treatment response biomarkers in pediatric eosinophilic esophagitis. Int. J. Mol. Sci. 26(7), 3111. https://doi.org/10.3390/ijms26073111 (2025).
Gil-Martínez, M. et al. Obese asthma phenotype is associated with hsa-miR-26a-1–3p and hsa-miR-376a-3p modulating the IGF axis. Int. J. Mol. Sci. 24(14), 11620. https://doi.org/10.3390/ijms241411620 (2023).
Grueso-Navarro, E. et al. MicroRNAs in plasma-derived extracellular vesicles as non-invasive biomarkers for eosinophilic esophagitis. Int. J. Mol. Sci. 26(2), 639. https://doi.org/10.3390/ijms26020639 (2025).
Kabłak-Ziembicka, A., Badacz, R. & Przewłocki, T. Clinical application of serum microRNAs in atherosclerotic coronary artery disease. J. Clin. Med. 11(22), 6849. https://doi.org/10.3390/jcm11226849 (2022).
Badacz, R., Przewłocki, T., Legutko, J., Żmudka, K. & Kabłak-Ziembicka, A. microRNAs associated with carotid plaque development and vulnerability: The clinician’s perspective. Int. J. Mol. Sci. 23(24), 15645. https://doi.org/10.3390/ijms232415645 (2022).
Uderhardt, S. et al. Enzymatic lipid oxidation by eosinophils propagates coagulation, hemostasis, and thrombotic disease. J. Exp. Med. 214(7), 2121–2138. https://doi.org/10.1084/jem.20161070 (2017).
Hou, L. et al. White blood cell count in young adulthood and coronary artery calcification in early middle age: Coronary artery risk development in young adults (CARDIA) study. Eur. J. Epidemiol. 28(9), 735–742. https://doi.org/10.1007/s10654-013-9842-7 (2013).
Tanaka, M. et al. Eosinophil count is positively correlated with coronary artery calcification. Hypertens Res. 35(3), 325–328. https://doi.org/10.1038/hr.2011.191 (2012).
Gao, S. et al. Eosinophils count in peripheral circulation is associated with coronary artery disease. Atherosclerosis 286, 128–134. https://doi.org/10.1016/j.atherosclerosis.2019.05.027 (2019).
Acknowledgements
We thank Dr. Tian Yao for his assistance in data analysis and acquisition.
Funding
This work was supported by the Central Guidance Local Science and Technology Development Fund Project of Shanxi Provincial Department of Science and Technology (YDZJSX2021C026), Leading talent team building Project in Shanxi Province (202204051002010) and the Shanxi Province Graduate Education Innovation Program (2024SJ169).
Author information
Authors and Affiliations
Contributions
Honglin Dong: Presentation of the study concept. Ruijing Zhang, Xiaotong Qi, Jie Hu and Runze Chang: Study design. Xiaotong Qi, Runze Chang and Lin Zheng: Data analysis. Xing Cheng, Maolin Qiao, Siqi Gao, Yaling Li and Jinshan Chen completed the clinical information collection and follow-up of the patients. Xiaotong Qi and Runze Chang: manuscript drafting. Xiaotong Qi, Runze Chang, Ruijing Zhang, Xing Cheng, Lin Zheng, Jie Hu, and Honglin Dong critically revised the manuscript. All authors contributed to the article and approved the submitted version.
Corresponding author
Ethics declarations
Competing interest
The authors declare no competing interests.
Ethics approval
This retrospective study involving human participants was in accordance with the Helsinki Declaration and approved by the Ethics Committee of Second hospital of Shanxi Medical University (No. 2023126).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, R., Chang, R., Qi, X. et al. Eosinophil counts predict 3-year risk of major adverse cardiovascular and cerebrovascular events in carotid artery stenosis patients. Sci Rep 15, 20939 (2025). https://doi.org/10.1038/s41598-025-06350-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-06350-w