Abstract
Neonatal Encephalopathy (NE) is a clinical syndrome presenting as neurological dysfunction. Persistent dysregulated Inflammation is associated with NE and miRNA biomarkers may correlate with developmental outcomes. We investigated miR-20a, miR-20b, miR-93 and miR-532 expression at birth and childhood following Neonatal Encephalopathy (NE) as potential biomarkers of inflammation, brain development, and long-term outcomes. Blood samples were collected from neonates with NE (week 1 of life) and children post-NE (2–5 years of age) and compared to age-matched controls (Neonatal and paediatric). Whole blood was stimulated ex-vivo with lipopolysaccharide, and total RNA was extracted from serum. MiR-20a, miR-20b, miR-93 and miR-532 were identified by TaqMan® Advanced miRNA Assays. Forty-five children were recruited (n = 11–12 in each group). MiR-20b, miR-93 and miR-532 significantly increased in neonates with NE compared to neonatal controls. MiR-20b expression decreased in children with NE compared to neonates with NE, to childhood control levels. MiR-93 increased in control children compared to control neonatal. MiR-20b significantly decreased with lipopolysaccharide in children with NE compared to their paired neonatal NE sample. MiR-20b, miR-93, and miR-532-5p are linked to neuron development and cellular stress responses. Their dysregulated expression might indicate altered immune responses and have potential as a biomarker.
Similar content being viewed by others
Introduction
Neonatal encephalopathy (NE) is a “clinical syndrome of disturbed neurologic function in the earliest days after birth in an infant born at or beyond 35 weeks of gestation, manifest by a subnormal level of consciousness or seizures, often accompanied by difficulty with initiating and maintaining respiration, and depression of tone and reflexes”1. In addition to supportive multiorgan intensive care, Therapeutic Hypothermia (TH) remains the only new therapy introduced in the last 20 years. TH is initiated within six hours of birth to ensure optimal neuroprotection2,3. Due to this short window of opportunity, it is necessary to identify further adjuvant therapies. NE is a risk factor for neurodevelopmental conditions and can lead to disability such as cerebral palsy (CP) and neurodevelopmental delay4.
Persistent systemic inflammation has been associated with brain injury in animal models, and several reports indicate it is also an important factor in neonates with NE. Altered expression of pro- and anti-inflammatory cytokines has been shown to correlate with abnormal neuroimaging or death when assessed over the first week of life in the serum of neonates with NE5. Our group has previously described a correlation between persistent inflammation and a more severe grade of NE in neonates6. In later childhood, immune dysfunction persists long after the initial NE insult, manifesting as higher monocyte, Tumour Necrosis Factor alpha (TNF-α) and Toll-like receptor (TLR)-4 expression, and changes in nucleotide-binding oligomerisation domain-like receptors (NLR) family pyrin domain containing 3 (NLRP3) inflammasome7.
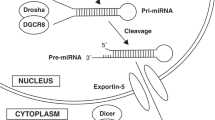
MicroRNAs, small non-coding RNAs (miRNAs; 22–24 nucleotides), are key regulators in post-transcriptional gene regulation8. MiRNAs have an important role in brain development and have been associated with neurodegenerative diseases9. This role is mainly associated with the regulation of essential cellular processes such as oxidative stress, inflammation, apoptosis and angiogenesis, as well as brain-specific mechanisms like blood-brain barrier protection and neurogenesis10. MiRNAs are both diagnostic markers and potential therapeutic targets in injuries of the central nervous system (CNS) like stroke, traumatic brain injury (TBI) and spinal cord injury (SCI)10. Dysregulation of miRNA expression has been linked to persistent inflammation, epilepsy, and seizures11,12,13and they have been linked to long-term outcomes after neonatal hypoxia in pre-clinical models14.
We evaluated the expression of four key microRNAs in inflammation and brain development in the serum of neonates and children with NE and compared the expression to control neonates and children. miR-20a, miR-20b, miR-93 and miR-532 have been previously linked to hypoxic ischemic encephalopathy in preclinical models and human samples15,16,17,18. Gao et al. (2022) described an anti-apoptotic role of miR-20a, which mitigates hypoxic-ischemic brain damage in neonatal mice16. miR-93 delivered by cell-derived extracellular vesicles was shown to prevent oxygen-glucose deprivation hippocampal neuron apoptosis and inflammation in a similar model17. Meanwhile, miR-532 was seen to be decreased in clinical samples of adults with acute ischemic stroke18. Interestingly, the 4 miRNAs have also been associated with signalling pathways involved in NE, such as inflammation, brain development and brain injury10,19,20,21,22,23. Recent studies also highlight their involvement in brain disorders such as cerebral ischemic stroke, epilepsy, traumatic injury, autism spectrum disorders and neurodegenerative diseases like Alzheimer’s disease, Parkinson’s disease and multiple sclerosis9,24,25,26,27. Expression of miRNAs was also assessed following the LPS challenge ex-vivo to determine the capacity of response to an inflammatory stimulus. MicroRNAs can be an overlooked biological target involved in the immunopathology of NE, and diagnostic tools for long-term outcomes after NE. Therefore, identifying pathways and analysing target genes can help us gain a better understanding of NE and potentially identify theranostic targets or biomarkers to predict outcomes.
Results
Demographics
Forty-five children were recruited for the study (Table 1), including neonates with NE (n = 10), neonatal controls (n = 12), children (2–5 years of age) following NE (n = 11) and age-matched child controls (n = 12). Neonates with NE had a median (IQR) gestational age of 39 (2.7) weeks and a weight of 3.5 (0.9) kg (Table 2). Apgar scores at 1, 5 and 10 min were a median (IQR) range of 4 (1.5), 5.5 (2.8) and 7 (2), respectively. Five neonates with NE were scored as Sarnat Grade 2, 2 as Grade 1 and 3 as Grade 3, with 9 of them receiving Therapeutic hypothermia, 6 had seizures, and 4 presented with abnormal brain MRI results (Table 2).
Children with NE during the neonatal period had a median (IQR) gestational age of 40.3 (1.5) weeks and a weight of 3.4 (0.65) kg. Apgar scores at 1, 5 and 10 min were a median (IQR) range of 2 (1.5), 6 (3.5) and 7 (4.2), respectively. Eight of them were scored as Sarnat Grade 2, 1 as Grade 1 and 2 as Grade 3, with 10 receiving Therapeutic hypothermia, 5 having seizures and 5 presenting with abnormal brain MRI results (Table 2). When comparing the clinical assessment in the children’s groups, the median age in months (IQR) was 49.5 (22) in healthy children and 44 (19) in children with NE. Children with NE were more likely to present with abnormal clinical development assessment as reported by the parents compared to the healthy controls, with 2 children (18%) presenting with difficulties in Gross motor, 1 (9%) in vision and fine motor, 3 (27%) in Hearing, speech and language and 2 (18%) in Social, emotional and behavioural assessments. Scaling and scoring of the Pediatric Quality of Life Inventory™ (PedsQL) measure health-related quality of life (HRQOL)28. Higher scores indicate better HRQOL. Median (IQR) PedsQL score was 85.1 (6.3) and 88.1 (14.29) in healthy children and children with NE, respectively.
miR-20b, miR-93 and miR-532 are increased in neonates with NE
Alterations in miRNAs in NE during neonatal age can have an impact on neurodevelopmental conditions later in childhood. Little is known about their expression and role in brain injury post-NE. We examined the expression of miR-20a, miR-20b, miR-93 and miR-532 in neonates and children with NE compared to control neonates and children (Fig. 1a to d). miR-20b (p = 0.0009), miR-93 (p = 0.0002) and miR-532 (p = 0.0002) were significantly increased in neonates with NE when compared to neonatal controls. miR-20b expression decreased in children with NE compared to neonates with NE (p = 0.0456), to similar levels to childhood controls. Meanwhile, miR-93 increased in childhood controls compared to neonatal controls (p = 0.0008). The opposite trend is observed in NE, where miR-93 is decreased in children with NE compared to neonates with NE; however, this difference does not reach statistical significance. No significant differences were observed in the expression of miR-20a when comparing healthy to NE or neonates to children.
MicroRNA expression in NE and controls comparing neonatal age to follow-up in children aged 2–6 years old. (a-d) Graphs show relative (ΔCT) expression of miR-20a (a), miR-20b (b), miR-93 (c) and miR-532 (d) in the serum of Neonates controls (n = 12), Child controls (n = 7–10), Neonate NE (n = 8–10) and Child NE (n = 6–11). Comparisons were done between four independent cohorts using Kruskal-Wallis test and expressed as ΔCT expression with median and interquartile range (IQR). *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001. Neonate control (yellow), Children control (blue), Neonates NE (orange) and children NE (purple).
Endotoxin challenge decreases miR-20b in children with NE
We evaluated the effect of an LPS challenge on the expression of the miRNAs, as a measurement of the capacity of response to an inflammatory stimulus. Expression of miR-20a, miR-20b, miR-93 and miR-532 was analysed in the serum of neonates and children with NE compared to control children (Fig. 2a to d). The volume of blood was restricted for neonatal controls, therefore, LPS treated samples could not be included for this analysis. miR-20b decreased in neonates with NE following an LPS challenge; however, the difference was not statistically significant. miR-20b was significantly decreased in LPS-treated samples of children with NE compared to the neonate with NE (p = 0.0045, respectively). miR-20a, miR-93, and miR-532 did not change significantly after LPS treatment compared to their corresponding basal samples within the group or when comparing control children to either neonates or children with NE. miR-93 and miR-532 are higher in neonates with NE compared to healthy children and children with NE, although this represents a non-significant trend. The expression of miR-20b, miR-93 and miR-532 is similar in children with NE compared to healthy controls.
Changes in microRNA expression in response to LPS treatment in NE and controls. (a-d) Graphs show relative (ΔCT) expression of miR-20a (a), miR-20b (b), miR-93 (c) and miR-532 (d) in the serum of child control (n = 7–11), Neonate NE (n = 9–10) and Child NE (n = 6–11). Whole blood from both groups was stimulated with Lipopolysaccharides (LPS, 10 ng/mL) for 1 h at 37 °C, and serum separated at 900 g for 10 min. “veh” refers to unstimulated (PBS) and it is represented in light colours. Dark colour samples are the corresponding LPS-treated samples. Comparisons were done between three independent cohorts using Kruskal-Wallis test and expressed as ΔCT expression with median and interquartile range (IQR). *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001. Children control (blue), Neonates NE (orange) and children NE (purple).
Further, a comparison of microRNA levels between vehicle and LPS-treated showed that miR-20b (p = 0.0322) was lower in LPS-treated samples in children affected by NE at birth, however, levels of miR-20b were similar in the control group (Fig. 3). miR-20a (p = 0.0273) and miR-93 (p = 0.0137) were significantly decreased in LPS-treated samples compared to vehicle samples in control children but not in NE neonates or NE Children (Supp. Figure 1a-f). Levels of miR-532 were similar in the vehicle and LPS-treated samples, independent of the cohort group (Supp. Figure 1g-i).
Changes in miR-20b expression between vehicle and LPS-treated samples. (a-c) Graphs show relative (ΔCT) expression of miR-20b in the vehicle and LPS-treated samples in control children (a, n = 10), NE neonates (b, n = 8) and NE children (c, n = 11). Wilcoxon signed-rank tests were done between three independent cohorts. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001. Children control (blue), Neonates NE (orange) and children NE (purple).
Statistical performance of MiRNAs miR-20b, miR-93 and miR-532 as plausible biomarkers for NE
Receiver operating characteristic (ROC) analysis was performed to evaluate the performance of miR-20b, miR-93 and miR-532 to discriminate between NE and control children (Fig. 4a to g). The closer the value of the area under the curve (AUC) to 1, the better the sensitivity and specificity of the microRNA to discriminate between groups. The best performance of the individual microRNAs was miR-93 with an AUC of 0.715 (Fig. 4b). Combination analysis was also performed to evaluate discrimination between NE and control neonates. The combination of miR-93 and miR-532 has an AUC of 0.857 (Fig. 4f), and this was higher than the single analysis of three of the microRNAs.
Predictive value of microRNAs in NE status of child vehicle samples. (a-g) Graphs show ROC curves of relative (ΔCT) expression of miR-20b (a), miR-93 (b), miR-532 (c), miR-20b and miR-93 (d), miR-20b and miR-532 (e), miR-93 and miR-532 (f) and miR-20b, miR-93 and miR-532 (g) in the serum of child NE (n = 6–11) and child control (n = 6–11).
Target and pathways regulated by miR-20b, miR-93 and miR-532
Finally, we examined the targets of the three microRNAs, as this provides additional mechanistic evidence for novel theranostic tools. We hypothesized that the three microRNAs may regulate pathways involved in neuroinflammation. There are several experimentally validated mRNA targets in common (Fig. 5a) between the miRNAs. 7 mRNAs have been validated with strong low throughput evidence as targets of both miR-20b and miR-93, while miR-20b and miR-532 share one target. Furthermore, Reactome pathway analysis reveals that many biological pathways are significantly enriched by high-confidence targets of both miR-20b and miR-93 (Fig. 5b) including multiple inflammation pathways, and cellular senescence and circadian clock-associated pathways. In contrast, miR-532 shares only one commonly enriched pathway with the other miR-20b and miR-93, intracellular signalling by second messengers.
Pathway analysis of microRNAs. (a) Circos plot showing experimentally validated targets in common among miR-20b, miR-93 and miR-532. The width of the connecting lines corresponds to the MirDIP predicted interaction score. (b) Significantly enriched Reactome pathways for the high confidence mRNA targets of miR-20b, miR-93 and miR-532. Adjusted p-values (Benjamini-Hochberg) < 0.05 were considered significant. Pathways significantly enriched in targets of 2 or more of the miRNAs are shown and are sorted by the number of targeting miRNAs and descending sum of p-values. Dot size indicates the number of mRNA in the pathway targeted by each miRNA. Related subpathways are grouped into their Reactome parent pathways.
Discussion
In the present study, we found significantly increased expression of miR-20b, miR-93 and miR-532 in neonates with NE compared to control neonates. Increased levels of these miRNAs in this group could be evidence of brain injury during this early stage of life or activation of mechanisms to promote recovery of injured regions of the brain. miR-20a/miR-20b and miR-93 belong to the miR-17 ~ 92 family, which has previously been associated with neuronal differentiation19,29. miR-20b has been linked to neuron development and proliferation20,21,22. Dysregulation of miR-20b in different brain regions of Alzheimer’s disease patients affects calcium homeostasis and neurite outgrowth in neuronal cells21. High levels of miR-20b are also present in proneural glioblastoma30. Multiple studies describe the role of miR-20b in the inflammatory response during cerebral ischemia by promoting the activation of the NLRP3 signalling pathway, leading to increased levels of pro-inflammatory markers such as IL-1β, IL-18 and reactive oxygen species (ROS), and by targeting Thioredoxin-interacting protein (TXNIP), an important factor in apoptosis22,31. In this study, we demonstrated a strong correlation between our set of microRNAs and the regulation of inflammation-related pathways, particularly the TLR cascade and interleukin signalling. This includes the involvement of extracellular signal-regulated kinases (ERK)/Mitogen-Activated Protein Kinases (MAPK), Myeloid Differentiation Primary Response 88 (MyD88), and Nuclear Factor Kappa B (NF-кB) pathways. Interestingly, miR-20b may also be a therapeutic strategy for cerebral ischemic stroke22,31. Our study is the first to report increased expression of miR-20b in neonates with NE, which may reflect an effort to promote neuroregeneration in the injured brain. This alights with the findings of Wang et al. (2023), who demonstrated that microglial exosomes containing miR-20b promote neurite outgrowth and synapse recovery in injured neurons following mild hypothermia treatment after traumatic brain injury (TBI) in an in vivo model20. This is considering most of the patients in the neonates with NE group (90%) received therapeutic hypothermia. It could also constitute systemic evidence of brain injury happening during that stage. However, additional mechanistic studies are required to determine if the role of miR-20 in neonates with NE is pro-inflammatory or pro-regeneration in their brain. It is important to note that the levels of miR-20b in children with NE are similar to those of healthy control children.
Our results indicate that miR-93 and miR-532 were significantly increased in neonates with NE compared to control neonates. miR-93 and miR-532-5p are associated with homeostasis mechanisms protecting cells under stress conditions, such as autophagy, apoptosis and cell viability17,18,29,31,32,33. The role of miR-93 is also explored in various neurological conditions. Qiu et al. (2023) found that miR-93 downregulation is associated with impaired learning and memory in mice through a mechanism that regulates neuroinflammation and apoptosis34. Regulation of signal transducer and activator of transcription 3 (STAT3) expression by miR-93, an important factor in neuroinflammation, is also described in Parkinson’s disease32. Lower brain Neuronal-Enriched Extracellular Vesicles (NEEVs) miR-93 expression is associated with increased markers of inflammation in serum (such as interleukin (IL)-1 receptor antagonist (IL-1RA), IL-6, tumour necrosis factor (TNF), and leptin), a potential neuroendocrine dysregulation associated with major depressive disorder (MDD)35. While miR-93 delivered by bone marrow-derived mesenchymal stem cell extracellular vesicles (BMSC-EVs) in hypoxic-ischemic brain injury (HIBD) was described to inhibit apoptosis in hippocampal neurons and alleviate HIBD17. miR-532 is also implicated in various aspects of brain function and neurodegenerative diseases. In the context of axon development, miR-532 was detected in axons and growth cones of cortical neurons, indicating a potential role in local mRNA regulation during axon extension and pathfinding36. miR-532 levels were found to be reduced in rats displaying vulnerability to chronic stress, suggesting its potential as a biomarker for stress resilience in the context of psychiatric disorders such as post-traumatic stress disorder (PTSD) and depression37. miR-532 has been described to play an important role as a mechanistic protector and potential biomarker for cerebral ischemia/reperfusion injury in both in vivo and in vitro models by reducing neurological dysfunction, infarct area, neuronal apoptosis, and activating the PI3K/Akt signalling pathway18,33. miR-532 also promotes the clearance of brain amyloid-β in Alzheimer’s disease, improving the blood-brain barrier function, and indicating a potential therapeutic role38. Our findings of increased miR-93 and miR-532 in neonates with NE are consistent with the literature, highlighting their roles in neuroprotection, neuroinflammation, and apoptosis, as their increase indicates an effort to recover the injured brain tissue.
There were no significant differences in the expression of miR-20a in our study when comparing neonatal controls to NE neonates, control children or NE children. miRNA-20a regulates inflammatory pathways via NLRP3 signalling39. It has also been described to have an important role in neurodegenerative diseases. miR-20a is among the deregulated miRNAs associated with Alzheimer’s disease, impacting key molecular players such as amyloid precursor protein (APP), tau protein, and α-synuclein19. miR-20a regulates neurogenic differentiation and influences the miR-20a/NeuroD1 signalling pathway in ischemic brain injury, and it has emerged as a potential therapeutic agent in stroke, with its upregulation in astrocytes showing neuroprotective effects40. Altered miR-20a expression was also identified in autism spectrum disorders and epileptogenesis24,25. The lack of significant differences in miR-20a expression in our study contrasts with literature linking miR-20a to neuroinflammation, neurodegeneration, and brain injury, suggesting its role in NE may be limited or context-dependent.
Several studies have explored the roles of miRNAs in neonatal hypoxic-ischemic encephalopathy (HIE) pathogenesis, one of the main clinical forms of NE. miRNA profiling has allowed for the identification of miR-323a-3p, miR-30e-5p, hsa-mir-145-5p, and others, highlighting their potential as diagnostic and prognostic tools41,42. miR-384 has also been identified as a diagnostic biomarker, inversely correlating with HIE severity and mitigating neuroinflammation43. miR-214-3p, miR-19b-3p, miR-363-3p and miR-210 have been shown to protect against neuronal apoptosis and reduce neuronal injury in animal and cellular models of HIE44,45,46,47. These findings underscore the promise of miRNAs in improving NE management through early detection and targeted therapy. Based on our results, miR-20b, miR-93 and miR-532 have an important role in NE during the neonatal stage. These changes may evidence the neuroprotective effect of the miRNAs during the injury period and the consequent neurodevelopmental outcomes that will become evident later in the developmental stages.
When stimulated with LPS, the expression of miR-20b decreased in children and neonates with NE when compared to their corresponding untreated samples. This might indicate an impaired systemic response to endotoxin and a consequence of the injury sustained by neonates and children with NE. In non-classical monocytes, LPS stimulation results in a distinctive epigenetic profile characterised by down-regulated miRNAs, including miRNA-20a, which translates into elevated Tripartite motif containing 8 (TRIM8) expression in pro-inflammatory gene expression48. NE is a complex condition that affects a critical moment of development. MicroRNAs are multi-targeting molecules that regulate the expression of thousands of genes. In this study, we evaluated the main pathways affected by these 3 microRNAs, and interestingly inflammation-regulated pathways were among the most highly regulated, including ERK/MAPK, MyD88, NF-кB, and Tumor necrosis factor receptor-associated factor 6 (TRAF6). Nevertheless, at this developmental time window, activation of pathological inflammation may affect neuronal pruning via microglia regulation.
The study explores the role of four key miRNAs (miR-20a, miR-20b, miR-93, and miR-532) as regulators of inflammation and brain development after neonatal encephalopathy (NE). We aimed to identify pathways of immunopathology in NE and explore the potential of these 4 miRNAs as theranostic targets or biomarkers to predict outcomes. We assessed potential correlations between the 4 miRNAs and outcomes such as clinical assessment (Gross motor, fine motor, Hearing, speech and language, and Social, emotional and behavioural assessments), Bayleys Score, PedQL and MRI, but no correlation was established. The study’s limitations include the age of healthy term controls (with samples taken within a week rather than within 72 h of NE diagnosis), the low volume of blood collected (precluding LPS samples for healthy term neonates), the small sample size, the male-to-female ratio and the heterogeneity among NE patients. All of these limits statistical power and restricts the interpretation of results. Therefore, the results must be considered within the context of the study’s specific limitations. We described a significant increase in miR-20b, miR-93, and miR-532 expression in NE neonates, suggesting a possible stress resilience response to brain injury during this stage. Analysis of specific target genes may help to identify pathological pathways and could be of therapeutic value. We observed that the higher therapeutic potential is for miR-20b or miR-93 combined with miR-532. miR-20b and miR-93 shared many of the target genes, and no additive value was observed when combined.
Methods
Ethical approval and study participants
The Ethics committees of Rotunda Hospital (REC-2020-005, REC-2016-028), Coombe Hospital (2–2020 – FIREFLY; 12–2016 – NIMBUS; 11-2017-GENIE), the National Maternity Hospital in Dublin (EC 14 2019; EC 14 2016; EC11 2017), and Tallaght University Hospital (Project ID: 0147) granted ethical committee approval for this study. All experiments were performed following relevant guidelines and regulations. Families received verbal and written information on the research, and informed consent was obtained from all subjects and/or their legal guardian(s).
Patient groups
The participants were recruited from four separate cohorts. Whole blood samples were obtained from Neonate with NE, healthy term babies (Neonates controls), Children who had NE and control children:
-
1.
Neonates control group: The neonatal control cohort was enrolled in the ‘Gender and Neonatal Inflammation in Preterm Outcomes’ (GENIE) study funded by the National Children’s Research Centre (NCRC; NCHF-2017-002)49. Healthy neonatal controls were born following a full-term normal delivery with normal Apgar scores, neurological examination and postnatal course and no underlying co-morbidities. Peripheral blood was collected in healthy term controls recruited in the Coombe Hospital within the first week after delivery. Term controls were eligible for participation if they were having routine phlebotomy performed on the postnatal ward and did not have any clinical or laboratory evidence of infection or serious congenital abnormalities (genetic, metabolic, cardiac).
-
2.
Child control group: Healthy child controls were enrolled in the ‘Follow-up of Inflammatory Responses and Multiorgan Outcomes Following Neonatal Brain Injury’ (FIREFLY) study, funded by the Health Research Board (HRB; ILP-POR-2019-086`; ClinicalTrial.Gov Registration: NCT04816331, study type: Observational, Patient Registry). The controls include age-matched children with no acute infections undergoing routine phlebotomy in the Tallaght University Hospital as part of a day case procedure. Inclusion criteria: (i) Healthy children born at full term, with no problems at birth and in the neonatal period ii) have no underlying co-morbidities. Following informed parental consent, children were recruited to the study as controls and a clinical assessment was performed. Parents reported development assessment as normal or abnormal in the areas of Gross motor, vision and fine motor, hearing, speech and language, and Social, emotional and behavioural assessments during clinical evaluation.
-
3.
Neonates with NE group: All neonatal NE participants were enrolled in the Neonatal Encephalopathy PhD training network, and Neonatal Encephalopathy multidisciplinary PhD program (NEPTUNE; www.nbci.ie) study funded by the HRB (HRB-CDA-2018-008). The neonatal NE group blood samples were obtained during the first week of life from neonates with a clinical diagnosis of NE and a gestational age (GA) of > 35 weeks. Neonates with NE were given therapeutic hypothermia if they fulfilled the national guideline criteria and were only diagnosed with Hypoxic–Ischaemic-Encephalopathy (HIE) if they fulfilled the ACOG/AAP definition50. Neonates with congenital abnormalities, GA < 35 weeks, birth weight < 2 kg, confirmed sepsis or evidence of maternal substance abuse were excluded. Neonates were consider at risk of perinatal asphyxia (PA) if they had three of the following diagnostic criteria: (1) Intrapartum distress indicated by fetal bradycardia (heart rate less than 100), late decelerations, or absence of heart rate variability, (2) thick meconium stained amniotic fluid, (3) an Apgar score of 6 or less at 5 min, (4) the requirement for resuscitation for more than one minute with positive pressure ventilation and oxygen immediately after delivery, or (5) an arterial pH of less than 7.3 or a base deficit of at least 14 within the first hour of life51. Modified Sarnat staging was used to grade the severity of NE: grade I – mild encephalopathy, grade II – moderate encephalopathy, and grade III – severe encephalopathy. Most of the details on the mode of delivery, Apgar scores, clinical or electrographic seizures, cord Ph (arterial), initial lactate and Magnetic resonance imaging (MRI) scans were collected (Table 2).
-
4.
Children with NE group: The childhood NE cohort was recruited at follow-up from the neonatal group in ‘Neonatal Inflammation and Multiorgan Dysfunction and Brain Injury Research’ (NIMBUS) funded by HRB (HRA-POR-2015-2507)52 and NEPTUNE studies, when children reached 2 and 5 years of age, in the FIREFLY study. Ninety per cent of the children in the NE group received TH in the neonatal period following the TOBY (total body hypothermia for neonatal encephalopathy) criteria for 72 hours53. These neonates were categorised as mild (Sarnat grade 0/I), moderate (Sarnat Grade II) and Severe (Sarnat Grade III) encephalopathy at birth. Details on the mode of delivery, Apgar scores, clinical or electrographic seizures, cord Ph (arterial), initial lactate and Magnetic resonance imaging (MRI) scans at the neonatal stage were also compiled (Table 2). Parents reported development assessment as normal or abnormal in the areas of Gross motor, vision and fine motor, hearing, speech and language, and Social, emotional and behavioural assessments during clinical evaluation.
Pediatric quality of life inventory™ (PedsQL)
Scaling and scoring of the Pediatric Quality of Life Inventory™ (PedsQL) measure health-related quality of life (HRQOL) was also performed during recruitment28. The PedsQL assesses physical, emotional, social and school (when age-relevant) functioning domains. The age-appropriate PedsQL was completed by the parents of children in the control group and children with NE during the clinical evaluation and any parental concerns were addressed. The age of the children was in the range of 2–5 years.
Blood sampling
Whole-blood sampling was performed following informed parental consent. Samples were taken at times of routine patient phlebotomy using an aseptic technique via central, peripheral arterial or venous lines. The blood (1-3mL) was collected in sodium citrate tubes and processed for Serum collection within 2 h after phlebotomy.
Serum collection
Whole blood was incubated ex-vivo in the presence or absence of lipopolysaccharide (LPS) at a final concentration of 10 ng/mL (Sigma Life Science, Dublin, Ireland) at 37 °C for 1 h. Stimulation with LPS was done within 2 h of blood collection in fresh samples. Basal levels are defined as the concentration of miRNAs without LPS stimulation. Phosphate-buffered saline (PBS) was used in unstimulated samples (defined as “vehicle”) at an equal volume to LPS. The volume of blood for neonatal controls was restricted, therefore, only vehicle samples were included for that group. After incubation, the serum was separated by centrifugation at 900 g for 10 min at room temperature (RT). The serum was removed and stored at − 80 °C for batch processing.
MiRNA isolation and cDNA template preparation
Total RNA was extracted using the miRNeasy Serum/Plasma Kit (Qiagen, West Sussex, UK). Fifty microliters of serum were diluted up to 200 µl in water. Briefly, RNA was isolated by Qiazol/chloroform phase separation, then small RNA was further isolated by serum/plasma small RNA kit (Qiagen, West Sussex, UK) and diluted in RNase-free water. 2 µl of total RNA was processed by reverse transcriptase and pre-amplification steps following the manufacturer’s protocol for single-tube TaqMan® Advanced miRNA Assays (Applied Biosystems, Massachusetts, United States). Briefly, cDNA templates were prepared following 4 steps/reactions: poly(A) tailing reaction, adaptor ligation reaction, reverse transcription (RT) reaction and miR-Amp reaction. Each step is accompanied by a manufacturer-tailored master mix and its corresponding thermal cycler protocol.
Real-Time PCR (RT-PCR) analysis of MiRNAs
A 1:10 dilution of the cDNA template was prepared. 5 µl of the dilution was added to 15 µl of PCR Reaction Mix (TaqMan™ Fast Advanced Master Mix, Thermo Fisher, Cat n: 4444557) following the manufacturer’s protocol. Pre-designed primers for the primary sequence of miR-20a-5p, miR-20b-5p, miR-93-5p, miR-532-5p and the housekeeping gene miR-16 were purchased from Thermo Fisher (TaqMan® Advanced miRNA Assay, sequences as per table below). miR-16 was used as a housekeeping gene, as its levels have been shown to be stable in human samples54. QuantStudio 5 (appliedbiosystems by Thermo Fisher Scientific) was used, and relative quantification (RQ) values were calculated using the ΔCT method. The relative quantification of each target miRNA was expressed as delta cycle threshold (ΔCT). ΔCT was calculated as follows: CT of the target miR – CT of the housekeeping gene (miR-16). A lower ΔCT value indicates higher gene expression, and higher ΔCT values indicate reduced gene expression.
Mature miRNA Sequence (TaqMan™ Advanced miRNA Assay, Cat# A25576): hsa-miR-20a-5p: UAAAGUGCUUAUAGUGCAGGUAG (Assay ID: 478586_mir); hsa-miR-20b-5p: CAAAGUGCUCAUAGUGCAGGUAG (Assay ID: 477804_mir); hsa-miR-93-5p: CAAAGUGCUGUUCGUGCAGGUAG (Assay ID: 478210_mir); hsa-miR-532-5p: CAUGCCUUGAGUGUAGGACCGU (Assay ID: 478151_mir); hsa-miR-16-5p: UAGCAGCACGUAAAUAUUGGCG (Assay ID: 477860_mir).
ROC analysis methods
Receiver operating characteristic (ROC) curve analysis was generated using the pROC package in R55. This was done using the ΔCT values of a single miRNA and/or combination of miRNAs in both the vehicle-treated samples. Logistic regression analysis was carried out using relative miRNA expression (ΔCT) as the independent variable and NE status as the dependent variable.
Pathway analysis methods
Predicted and experimentally validated mRNA targets of hsa-miR-20b-5p, hsa-miR-93-5p and hsa-miR-532-5p were identified using miRDIP 5.256, miRTarBase 9.057, miRTargetLink 2.058. Circos plots of validated target genes by Western blot, PCR or reporter assay were generated using the circlize package in R59. The Reactome pathway enrichment analysis on high-confidence mRNA targets was generated using the packages ReactomePA and clusterProfiler60 in R, with an adjusted Benjamini-Hochberg p-value of 0.05 considered significant. The grouped significantly enriched pathways were manually allocated to their respective parent Reactome pathways.
Statistical methods
All results are presented as ΔCT expression with standard error of the mean (SEM). Statistical analysis was performed on GraphPad PRISM version 9. Data on Figs. 1 and 2 were not normally distributed as indicated by the Shapiro-Wilk normality test and were analysed using non-parametric and unpaired (unmatched) Kruskal-Wallis test to compare median results between three and four independent cohorts. Dunn’s test allowed for the adjustment of p-values to account for multiple comparisons following Kruskal-Wallis. Figure 3, non-parametric Wilcoxon signed-rank tests were performed to compare vehicle and LPS results between three independent cohorts. Non-normal distribution was assumed. Significance was accepted as P < 0.05. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001.
Data availability
Raw data were generated at The Children´s Research Laboratory, Discipline of Paediatric Medicine, Trinity College Dublin, the University of Dublin. The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Executive summary. Neonatal encephalopathy and neurologic outcome, second edition. Report of the American College of Obstetricians and Gynecologists’ Task Force on Neonatal Encephalopathy. Obstet Gynecol 123, 896–901, (2014). https://doi.org/10.1097/01.AOG.0000445580.65983.d2
Sabir, H., Bonifacio, S. L., Gunn, A. J., Thoresen, M. & Chalak, L. F. Unanswered questions regarding therapeutic hypothermia for neonates with neonatal encephalopathy. Semin Fetal Neonatal Med. 26, 101257. https://doi.org/10.1016/j.siny.2021.101257 (2021).
Wassink, G., Harrison, S., Dhillon, S., Bennet, L. & Gunn, A. J. Prognostic neurobiomarkers in neonatal encephalopathy. Dev. Neurosci. 44, 331–343. https://doi.org/10.1159/000522617 (2022).
Murray, D. M., O’Connor, C. M., Ryan, C. A., Korotchikova, I. & Boylan, G. B. Early EEG grade and outcome at 5 years after mild neonatal hypoxic ischemic encephalopathy. Pediatrics 138 https://doi.org/10.1542/peds.2016-0659 (2016).
O’Hare, F. M. et al. Serial cytokine alterations and abnormal neuroimaging in newborn infants with encephalopathy. Acta Paediatr. 106, 561–567. https://doi.org/10.1111/apa.13745 (2017).
O’Hare, F. M. et al. Persistent systemic monocyte and neutrophil activation in neonatal encephalopathy. J. Matern Fetal Neonatal Med. 29, 582–589. https://doi.org/10.3109/14767058.2015.1012060 (2016).
Kelly, L. A. et al. Altered inflammasome activation in neonatal encephalopathy persists in childhood. Clin. Exp. Immunol. 205, 89–97. https://doi.org/10.1111/cei.13598 (2021).
Dexheimer, P. J., Cochella, L. & MicroRNAs From mechanism to organism. Front. Cell. Dev. Biol. 8, 409. https://doi.org/10.3389/fcell.2020.00409 (2020).
Quinlan, S., Kenny, A., Medina, M., Engel, T. & Jimenez-Mateos, E. M. MicroRNAs in neurodegenerative diseases. Int. Rev. Cell. Mol. Biol. 334, 309–343. https://doi.org/10.1016/bs.ircmb.2017.04.002 (2017).
Sun, P., Liu, D. Z., Jickling, G. C., Sharp, F. R. & Yin, K. J. MicroRNA-based therapeutics in central nervous system injuries. J. Cereb. Blood Flow. Metab. 38, 1125–1148. https://doi.org/10.1177/0271678x18773871 (2018).
Xie, G. et al. The dysregulation of MiRNAs in epilepsy and their regulatory role in inflammation and apoptosis. Funct. Integr. Genomics. 23, 287. https://doi.org/10.1007/s10142-023-01220-y (2023).
Brennan, G. P. & Henshall, D. C. MicroRNAs as regulators of brain function and targets for treatment of epilepsy. Nat. Rev. Neurol. 16, 506–519. https://doi.org/10.1038/s41582-020-0369-8 (2020).
Leavy, A. & Jimenez Mateos, E. M. Perinatal brain injury and inflammation: lessons from experimental murine models. Cells 9 https://doi.org/10.3390/cells9122640 (2020).
Leavy, A., Brennan, G. P. & Jimenez-Mateos, E. M. MicroRNA Profiling Shows a Time-Dependent Regulation within the First 2 Months Post-Birth and after Mild Neonatal Hypoxia in the Hippocampus from Mice. Biomedicines 10, (2022). https://doi.org/10.3390/biomedicines10112740
Truettner, J. S., Katyshev, V., Esen-Bilgin, N., Dietrich, W. D. & Dore-Duffy, P. Hypoxia alters MicroRNA expression in rat cortical pericytes. Microrna 2, 32–44. https://doi.org/10.2174/2211536611302010005 (2013).
Gao, H. et al. Long Non-coding RNA Peg13 alleviates Hypoxic-Ischemic brain damage in neonatal mice via miR-20a-5p/XIAP axis. Neurochem Res. 47, 656–666. https://doi.org/10.1007/s11064-021-03474-z (2022).
Luo, H. et al. microRNA-93 packaged in extracellular vesicles from mesenchymal stem cells reduce neonatal hypoxic-ischemic brain injury. Brain Res. 1794, 148042. https://doi.org/10.1016/j.brainres.2022.148042 (2022).
Wang, J. et al. MicroRNA-532-5p upregulation protects neurological deficits after ischemic stroke through Inhibition of BTB and CNC homology 1. Int. Immunopharmacol. 100, 108003. https://doi.org/10.1016/j.intimp.2021.108003 (2021).
Rezaee, D. et al. The role of MicroRNAs in the pathophysiology of human central nervous system: A focus on neurodegenerative diseases. Ageing Res. Rev. 92, 102090. https://doi.org/10.1016/j.arr.2023.102090 (2023).
Wang, C. et al. Increased level of Exosomal miR-20b-5p derived from hypothermia-treated microglia promotes neurite outgrowth and synapse recovery after traumatic brain injury. Neurobiol. Dis. 179, 106042. https://doi.org/10.1016/j.nbd.2023.106042 (2023).
Wang, R. et al. Human MicroRNA (miR-20b-5p) modulates alzheimer’s disease pathways and neuronal function, and a specific polymorphism close to the MIR20B gene influences alzheimer’s biomarkers. Mol. Psychiatry. 27, 1256–1273. https://doi.org/10.1038/s41380-021-01351-3 (2022).
Zhao, J., Wang, H., Dong, L., Sun, S. & Li, L. miRNA-20b inhibits cerebral ischemia-induced inflammation through targeting NLRP3. Int. J. Mol. Med. 43, 1167–1178. https://doi.org/10.3892/ijmm.2018.4043 (2019).
Arzhanov, I., Sintakova, K. & Romanyuk, N. The Role of miR-20 in Health and Disease of the Central Nervous System. Cells 11, (2022). https://doi.org/10.3390/cells11091525
Huang, Z. X., Chen, Y., Guo, H. R. & Chen, G. F. Systematic review and bioinformatic analysis of MicroRNA expression in autism spectrum disorder identifies pathways associated with cancer, metabolism, cell signaling, and cell adhesion. Front. Psychiatry. 12, 630876. https://doi.org/10.3389/fpsyt.2021.630876 (2021).
Feng, Y., Duan, C., Luo, Z., Xiao, W. & Tian, F. Silencing miR-20a-5p inhibits axonal growth and neuronal branching and prevents epileptogenesis through RGMa-RhoA-mediated synaptic plasticity. J. Cell. Mol. Med. 24, 10573–10588. https://doi.org/10.1111/jcmm.15677 (2020).
Viswambharan, V., Thanseem, I., Vasu, M. M., Poovathinal, S. A. & Anitha, A. MiRNAs as biomarkers of neurodegenerative disorders. Biomark. Med. 11, 151–167. https://doi.org/10.2217/bmm-2016-0242 (2017).
Grasso, M., Piscopo, P., Confaloni, A. & Denti, M. A. Circulating MiRNAs as biomarkers for neurodegenerative disorders. Molecules 19, 6891–6910. https://doi.org/10.3390/molecules19056891 (2014).
Varni, J. W., Seid, M. & Kurtin, P. S. PedsQL 4.0: reliability and validity of the pediatric quality of life inventory version 4.0 generic core scales in healthy and patient populations. Med. Care. 39, 800–812. https://doi.org/10.1097/00005650-200108000-00006 (2001).
Sun, K. T. et al. MicroRNA-20a regulates autophagy related protein-ATG16L1 in hypoxia-induced osteoclast differentiation. Bone 73, 145–153. https://doi.org/10.1016/j.bone.2014.11.026 (2015).
Huang, T. et al. A regulatory circuit of miR-125b/miR-20b and Wnt signalling controls glioblastoma phenotypes through FZD6-modulated pathways. Nat. Commun. 7, 12885. https://doi.org/10.1038/ncomms12885 (2016).
Yang, D. et al. Upregulation of miR-20b protects against cerebral ischemic stroke by targeting thioredoxin interacting protein (TXNIP). Exp. Neurobiol. 30, 170–182. https://doi.org/10.5607/en20046 (2021).
Wang, X., Liu, Z. & Wang, F. MicroRNA-93 blocks signal transducers and activator of transcription 3 to reduce neuronal damage in parkinson’s disease. Neurochem Res. 46, 1859–1868. https://doi.org/10.1007/s11064-021-03333-x (2021).
Mu, J., Cheng, X., Zhong, S., Chen, X. & Zhao, C. Neuroprotective effects of miR-532-5p against ischemic stroke. Metab. Brain Dis. 35, 753–763. https://doi.org/10.1007/s11011-020-00544-z (2020).
Qiu, F. et al. MiR-93 alleviates DEHP plasticizer-induced neurotoxicity by negatively regulating TNFAIP1 and inhibiting ubiquitin-mediated degradation of CK2β. Food Chem. Toxicol. 178, 113888. https://doi.org/10.1016/j.fct.2023.113888 (2023).
Burrows, K. et al. Exploring the role of neuronal-enriched extracellular vesicle miR-93 and interoception in major depressive disorder. Res. Sq. https://doi.org/10.21203/rs.3.rs-2813878/v1 (2023).
Sasaki, Y., Gross, C., Xing, L., Goshima, Y. & Bassell, G. J. Identification of axon-enriched MicroRNAs localized to growth cones of cortical neurons. Dev. Neurobiol. 74, 397–406. https://doi.org/10.1002/dneu.22113 (2014).
Chen, R. J. et al. MicroRNAs as biomarkers of resilience or vulnerability to stress. Neuroscience 305, 36–48. https://doi.org/10.1016/j.neuroscience.2015.07.045 (2015).
Liang, X. et al. Exosomal miR-532-5p induced by long-term exercise rescues blood-brain barrier function in 5XFAD mice via downregulation of EPHA4. Aging Cell. 22, e13748. https://doi.org/10.1111/acel.13748 (2023).
Jin, S. et al. Protectin DX restores Treg/T(h)17 cell balance in rheumatoid arthritis by inhibiting NLRP3 inflammasome via miR-20a. Cell. Death Dis. 12, 280. https://doi.org/10.1038/s41419-021-03562-6 (2021).
Branyan, T. E. et al. Functional assessment of Stroke-Induced regulation of miR-20a-3p and its role as a neuroprotectant. Transl Stroke Res. 13, 432–448. https://doi.org/10.1007/s12975-021-00945-x (2022).
Dakroub, F. et al. MicroRNAs as biomarkers of brain injury in neonatal encephalopathy: an observational cohort study. Sci. Rep. 14, 6645. https://doi.org/10.1038/s41598-024-57166-z (2024).
Winkler, I. et al. MicroRNA expression profiles as diagnostic and prognostic biomarkers of perinatal asphyxia and Hypoxic-Ischaemic encephalopathy. Neonatology 119, 204–213. https://doi.org/10.1159/000521356 (2022).
Zhang, L. et al. Epigenetics in non-classical monocytes support their pro-inflammatory gene expression. Immunobiology 225, 151958. https://doi.org/10.1016/j.imbio.2020.151958 (2020).
Yang, L. et al. Abnormal expression and role of MicroRNA-214-3p/SLC8A1 in neonatal Hypoxic-Ischaemic encephalopathy. Int. J. Exp. Pathol. 104, 199–208. https://doi.org/10.1111/iep.12475 (2023).
Zeng, H. & Chen, Y. X. MiR-19b-3p inhibits Hypoxia-Ischemia encephalopathy by inhibiting SOX6 expression via activating Wnt/β-catenin pathway. Neurochem Res. 48, 874–884. https://doi.org/10.1007/s11064-022-03812-9 (2023).
Jia, Y. et al. MiR-363-3p attenuates neonatal hypoxic-ischemia encephalopathy by targeting DUSP5. Neurosci. Res. 171, 103–113. https://doi.org/10.1016/j.neures.2021.03.003 (2021).
Li, B., Dasgupta, C., Huang, L., Meng, X. & Zhang, L. MiRNA-210 induces microglial activation and regulates microglia-mediated neuroinflammation in neonatal hypoxic-ischemic encephalopathy. Cell. Mol. Immunol. 17, 976–991. https://doi.org/10.1038/s41423-019-0257-6 (2020).
Zhang, L. et al. miRNA-20a suppressed lipopolysaccharide-induced HK-2 cells injury via NFκB and ERK1/2 signaling by targeting CXCL12. Mol. Immunol. 118, 117–123. https://doi.org/10.1016/j.molimm.2019.12.009 (2020).
McGovern, M. et al. Gender and sex hormone effects on neonatal innate immune function. J. Matern Fetal Neonatal Med. 37, 2334850. https://doi.org/10.1080/14767058.2024.2334850 (2024).
Branagan, A., Molloy, E. J., Badawi, N. & Nelson, K. B. Causes and terminology in neonatal encephalopathy: what is in a name?? neonatal encephalopathy, Hypoxic-ischemic encephalopathy or perinatal asphyxia. Clin. Perinatol. 51, 521–534. https://doi.org/10.1016/j.clp.2024.04.015 (2024).
Huang, C. C., Wang, S. T., Chang, Y. C., Lin, K. P. & Wu, P. L. Measurement of the urinary lactate:creatinine ratio for the early identification of newborn infants at risk for hypoxic-ischemic encephalopathy. N Engl. J. Med. 341, 328–335. https://doi.org/10.1056/nejm199907293410504 (1999).
O’Dea, M. I. et al. Dysregulated monocyte and neutrophil functional phenotype in infants with neonatal encephalopathy requiring therapeutic hypothermia. Front. Pediatr. 8, 598724. https://doi.org/10.3389/fped.2020.598724 (2020).
Azzopardi, D. et al. The TOBY study. Whole body hypothermia for the treatment of perinatal asphyxial encephalopathy: a randomised controlled trial. BMC Pediatr. 8, 17. https://doi.org/10.1186/1471-2431-8-17 (2008).
Sandau, U. S. et al. Analysis of the longitudinal stability of human plasma MiRNAs and implications for disease biomarkers. Sci. Rep. 14, 2148. https://doi.org/10.1038/s41598-024-52681-5 (2024).
Robin, X. et al. pROC: an open-source package for R and S + to analyze and compare ROC curves. BMC Bioinform. 12, 77. https://doi.org/10.1186/1471-2105-12-77 (2011).
Hauschild, A. C. et al. MirDIP 5.2: tissue context annotation and novel MicroRNA curation. Nucleic Acids Res. 51, D217–d225. https://doi.org/10.1093/nar/gkac1070 (2023).
Huang, H. Y. et al. MiRTarBase update 2022: an informative resource for experimentally validated miRNA-target interactions. Nucleic Acids Res. 50, D222–d230. https://doi.org/10.1093/nar/gkab1079 (2022).
Kern, F. et al. MiRTargetLink 2.0-interactive MiRNA target gene and target pathway networks. Nucleic Acids Res. 49, W409–w416. https://doi.org/10.1093/nar/gkab297 (2021).
Gu, Z., Gu, L., Eils, R., Schlesner, M. & Brors, B. Circlize implements and enhances circular visualization in R. Bioinformatics 30, 2811–2812. https://doi.org/10.1093/bioinformatics/btu393 (2014).
Yu, G., Wang, L. G., Han, Y. & He, Q. Y. ClusterProfiler: an R package for comparing biological themes among gene clusters. Omics 16, 284–287. https://doi.org/10.1089/omi.2011.0118 (2012).
Acknowledgements
We extend our gratitude to the parents, families and children who participated in this study whose support and willingness to be a part of this research was invaluable. We also express our deep appreciation to our collaborators at Rotunda Hospital, Coombe Hospital, the National Maternity Hospital in Dublin, and Tallaght University Hospital whose dedication and partnership made this study possible. We would like to acknowledge the support of the Health Research Board (HRB) for funding this research. Their commitment to advancing healthcare through research has been instrumental in making this study possible.
Author information
Authors and Affiliations
Contributions
J.I.C. ran the miRNA experiments on both children cohorts and performed the corresponding data analysis, prepared Figs. 1 and 2, and Tables 1 and 2, wrote the main manuscript text, coordinated the collection of clinical data and is the corresponding (submitting) author. E.I. recruited children’s cohorts (healthy control and follow-up patients with NE), took blood and separated serums. R.M. prepared Figs. 3, 4 and 5, and a supplementary figure, and wrote parts of the methodology and results of the manuscript about statistical performance and targeted pathway analysis. T.H. recruited neonatal patients with NE, took blood, separated serums and ran miRNA experiments. M.MG. recruited neonatal healthy controls, took blood and separated serums. M.OR., S.T. and G.K. collected clinical data in three neonatal hospitals. M.OD. and L.K. recruitment of the children with NE cohort when they were neonates, collected neonatal clinical data of this cohort. M.D. contributed to the conception and design of the study. J.M., C.V., and J.K. coordinated the recruitment of patients in three hospitals. E.J.M. conceived and designed the study, ran miRNA experiments, interpreted data, wrote parts of the manuscript, substantively revised it, and is a corresponding author. E.M. conceived and designed the study, interpreted data, wrote parts of the manuscript, substantively revised it, and is a corresponding author. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of interest
The author(s) declare no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Isaza-Correa, J.M., Isweisi, E., Murphy, R. et al. Childhood resolution of early abnormal miRNA following neonatal encephalopathy. Sci Rep 15, 30489 (2025). https://doi.org/10.1038/s41598-025-13776-9
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-13776-9