Abstract
This study aims to evaluate the variations in image quality of CCTA conducted at different time intervals and their clinical implications. A retrospective analysis of 641 patients who underwent CCTA between July 2023 and June 2024 was performed. The examination times were divided into morning group(8:00–12:00, 316 cases), and afternoon group༈14:00–18:00, 325 cases) for comparison. For patients with a heart rate ≥ 60 bpm, 25 mg of metoprolol was given orally to control heart rate, along with 0.5 mg of sublingual nitroglycerin before the CCTA examination. Image quality, initial heart rate, post-medication heart rate, heart rate differences (pre- and post-medication), percentage heart rate changes, radiation dose, age, and sex were compared between the two groups. Statistical analyses, including the Mann-Whitney U test, Spearman correlation coefficients, and logistic multivariate regression, were used to assess factors influencing image quality. Finally, receiver operating characteristic (ROC) curves were used to analyse the predictive value of examination timing on image quality. The image quality excellence rates for the morning group and the afternoon group were 87.9% and 74.1%, respectively, with no undiagnosable cases in either group. Significant differences (P < 0.05) were observed between the two groups in subjective image scores, post-medication heart rates, heart rate differences (pre- and post-medication), percentage heart rate changes, and age. However, no significant differences were found in initial heart rate, radiation dose, or sex (P > 0.05). Logistic multivariate regression analysis indicated a statistically significant association between image quality and both examination timing and age (P < 0.05). However, no significant associations were found with initial heart rate, heart rate differences (pre- and post-medication), percentage heart rate changes, radiation dose, or sex (P > 0.05). The regression equation was determined as Y = 11.386 + 0.873 × 1 + 0.023 × 2, where Y represents image quality, X1 represents the examination timing, and X2 represents age. For the morning group, the ROC curve area under the curve (AUC) for initial heart rate and post-medication heart rate were 0.598 and 0.890, with optimal thresholds of 79 bpm and 71 bpm, respectively. For the afternoon group, the AUC values were 0.596 and 0.812, with optimal thresholds of 75 bpm and 68 bpm, respectively. CCTA performed in the morning (8:00–12:00) yields superior image quality compared to the afternoon (14:00–18:00). Moreover, morning CCTA scans tolerated higher initial heart rates (up to 79 bpm) without affecting image quality, in contrast to the lower threshold of 75 bpm in the afternoon. These findings offer robust data to guide the timing of clinical CCTA procedures and heart rate management, indicating that morning CCTA scans may facilitate higher-quality imaging, especially for patients with elevated heart rates.
Similar content being viewed by others
Introduction
Coronary computed tomography angiography (CCTA), a non-invasive imaging technique, has served as a critical tool for diagnosing coronary artery disease (CAD) since its introduction in the 1990s1. 。Over the past two decades, technological advancements have positioned CCTA as a cornerstone in clinical diagnostics and decision-making, enabling comprehensive evaluation of coronary artery lesions and facilitating treatment planning2. 。However, despite its increasing clinical relevance, the image quality of CCTA is still constrained by factors such as level of heart rate, arrhythmias, cardiac motion, and respiratory activity3,4.
In response to these limitations, recent years have witnessed notable advancements in CCTA technology. Advances such as faster gantry rotation, the introduction of dual-source scanners, and the use of motion correction algorithms have considerably improved the temporal resolution of CCTA5. 。Additionally, wide-detector technology has extended the utility of CCTA to scenarios involving high heart rates or complex arrhythmias6. These technological innovations have not only improved image quality but also broadened the clinical applications of CCTA. Nevertheless, external factors such as patient heart rate and respiratory control remain critical determinants of image quality, constrained by the inherent limits of current hardware7. Research indicates that β-blockers to reduce heart rate and nitroglycerin to dilate coronary arteries can markedly enhance the quality of CCTA imaging7. However, heart rate variability is also modulated by external factors, including circadian rhythms8. Studies have demonstrated that heart rates are generally lower and more stable in the early morning, offering a promising direction for optimising CCTA procedures.
Against this backdrop, this study aims to explore how the timing of CCTA examinations influences heart rate thresholds and image quality. By examining the differences in heart rate and their corresponding effects on image quality between morning and afternoon sessions, this study seeks to offer theoretical insights and practical recommendations for optimising CCTA protocols.
Materials and methods
General data
This study included 641 patients who underwent CCTA examinations at The First Affiliated Hospital of Naval Medical University between July 2023 and June 2024. Exclusion criteria were: allergy to iodinated contrast agents, pregnancy, hyperthyroidism, renal insufficiency, coronary artery bypass grafting, and bradycardia (heart rate < 60 bpm). Clinical data of the patients are detailed in Table 1. The study was approved by the Ethics Committee of Shanghai Changhai Hospital and strictly adhered to the Declaration of Helsinki. Written informed consent was obtained from all patients prior to examination.
Instruments and methods
All patients underwent CCTA examinations using a 320-slice multi-detector CT scanner (uCT 960+, United Imaging Healthcare, Shanghai, China). For patients with a heart rate ≥ 60 bpm, oral tartrate metoprolol (25 mg, AstraZeneca Pharmaceuticals, China) was administered 1 h before the examination to control heart rate, with a standardised dosage of 25 mg for all. This is because when the heart rate is less than 60 bpm, there is no need to take.
oral tartrate metoprolol. Since this study is based on the administration of 25 mg oral tartrate metoprolol as the experimental foundation, excluding individuals with bradycardia helps to eliminate the potential bias caused by differences in drug dosage.Unless contraindicated, patients were also given sublingual nitroglycerin tablets (0.5 mg, Harbin Pharmaceutical Group, China) 5 min before the scan. All patients received standardised breathing training.
The scanning range extended from 10 mm below the carina to the diaphragmatic surface of the heart, ensuring complete coverage of coronary artery anatomy. An automatic trigger scanning technique was used, with the monitoring slice placed at the level of the descending aorta at the carina. The trigger threshold was set at 120 HU, and scanning commenced after a 6-second delay. Non-ionic iodinated contrast medium (iopamidol, 370 mgI/ml, Bracco, China) was administered via an Ulrich dual-barrel high-pressure injector with individualised dosing. The injection protocol consisted of 23 mgI/kg/s over 11 s, followed by 40 ml of saline flush.
A prospective ECG-gated axial scanning mode was utilised with parameters including 100 kV tube voltage, 100–200 mAs tube current, 0.25 s/r rotation speed, 12–16 cm collimator width, a field of view of 300 mm × 300 mm, and a matrix of 512 × 512. Optimal phase images were reconstructed using ePhase software (United Imaging Healthcare, Shanghai, China). Data were subsequently uploaded to the United Imaging workstation (uWS-CT, United Imaging Healthcare, Shanghai, China) for post-processing. Post-processing techniques included volume rendering (VR), maximum intensity projection (MIP), multiplanar reconstruction (MPR), and curved planar reconstruction (CPR). Patients were categorised into a morning group (8:00–12:00) and an afternoon group (14:00–18:00) based on the examination time. All patients were further divided into seven groups in 5 bpm increments to study the relationship between different heart rates and the optimal heart rate.
Image quality assessment
Two experienced radiologists scored all the images. Axial images, which have the least distortion and post-processing errors [9], were primarily used for scoring, supplemented by other processed images. The American Heart Association’s 15-segment model was used to classify image quality of coronary artery segments. The coronary arteries were divided into the right coronary artery (RCA) (1–3), left main coronary artery (LM), left anterior descending artery (LAD) (6–8), and left circumflex artery (LCX) (11–13). The quality of RCA, LAD, and LCX branches was evaluated using a 5-point grading system: 5 points (Excellent): No motion artifacts, smooth and clear vascular contours. 4 points (Good): Minor artifacts with slight segment blurring. 3 points (Adequate): Presence of some artifacts and moderate blurring, but no structural discontinuity. 2 points (Poor): Severe artifacts, doubling or discontinuity in the segments. 1 point (Non-diagnostic): Image cannot be evaluated, and vascular structures are indistinguishable.Vessel segments with a diameter of less than 1.5 mm were excluded from the assessment9.Image quality scores of 5 and 4 were classified as high-quality images, while scores of 3 and 2 were considered adequate images. A score of 1 was deemed an unacceptable image. Figure 1 illustrates the distribution of image quality among patients.
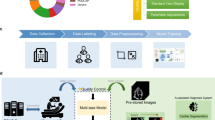
Flow chart of post-processing of patient data in this study.
Radiation dose assessment
Radiation dose was evaluated using the effective dose (ED), where ED = DLP × K. The dose-length product (DLP) is expressed in mGy·cm, and the constant K is 0.014 mSv·(mGy·cm)^(-1)10.
Statistical analysis
Statistical analysis was performed using SPSS 25.0 software. Quantitative variables were expressed as means ± standard deviation or medians (interquartile range), and categorical variables were presented as frequencies or percentages. For intergroup comparisons, non-normally distributed data were analysed using the Mann-Whitney U test, and paired samples were analysed using the Wilcoxon signed-rank test. A p-value of < 0.05 was considered statistically significant. The consistency between two radiologists in scoring the same images was evaluated using the Kappa consistency test. A Kappa value of ≥ 0.75 indicated good consistency, 0.4 ≤ Kappa < 0.75 indicated moderate consistency, and Kappa < 0.4 indicated poor consistency. Correlation analysis was conducted using the Spearman correlation coefficient to examine the relationship between image quality and variables such as patient heart rate, radiation dose, scanning mode, and technical parameters. The correlation strength is categorized as follows: |r| = 0.8 to 1.0 indicates a very strong correlation, |r| = 0.6 to 0.8 indicates a strong correlation, |r| = 0.4 to 0.6 indicates a moderate correlation, |r| = 0.2 to 0.4 indicates a weak correlation, and |r| = 0.0 to 0.2 indicates no or very weak correlation. A logistic regression model was employed in the multivariate analysis, incorporating variables such as patient age, gender, heart rate, BMI, radiation dose, and scanning mode. Stepwise regression was used to identify significant predictors for the development of the model. Receiver operating characteristic (ROC) analysis was used to assess the diagnostic performance of the image quality prediction model, and the area under the curve (AUC) was used to measure predictive ability. An AUC > 0.9 indicates excellent predictive ability, 0.7 ≤ AUC ≤ 0.9 indicates good predictive ability, and 0.5 ≤ AUC < 0.7 indicates moderate predictive ability.
Results
Study population characteristics
A total of 641 patients underwent CCTA. In the morning cohort, the mean initial heart rate (HR) was 78.33 ± 6.06 bpm (range: 65–100 bpm), while the post-medication HR was 63.61 ± 9.82 bpm (range: 40–96 bpm). This group included 172 males and 144 females, with a mean age of 63.11 ± 11.24 years (age range: 27–88 years). In the afternoon cohort, the mean initial heart rate was 78.57 ± 5.47 bpm (range: 66–96 bpm), and the post-medication HR was 62.20 ± 10.03 bpm (range: 36–117 bpm). This group included 177 males and 148 females, with a mean age of 60.60 ± 11.51 years (age range: 22–87 years). There were no significant differences between the two groups in terms of gender distribution, age, baseline heart rate, or radiation dose (all P values < 0.05). A significant difference was observed in post-medication heart rate (t = -3.823, P < 0.001).
Subjective image quality
Consistency assessment
Two observers independently rated the coronary artery images of 641 patients, yielding a Kappa coefficient of 0.873, which indicates a high degree of agreement between the observers’ subjective assessments. The clarity of the scoring criteria, along with the observers’ extensive experience, may have contributed to this high level of consistency. The overall median subjective score was 4 [4–5], with scores progressively decreasing as heart rate increased, further confirming the difference in image quality between the afternoon and morning groups(see Table 2).
Comparison of image scores and quality rates
As shown in Fig. 2, subjective scoring results demonstrated typical images with scores ranging from 2 to 5 points (Figs. 2 A–2D). The morning group exhibited a significantly higher excellent image quality rate of 87.9% compared to 74.1% in the afternoon group (Z = -4.453, P < 0.001). Table 3 presents the excellent image quality rates for both groups across different heart rate intervals. For instance, at HR ≤ 60 bpm, the morning group had an excellent rate of 98.4% (124/126) versus 95.7% (90/94) in the afternoon group. In the 60 < HR ≤ 65 bpm interval, the morning group maintained an excellent rate of 97.5% (77/79), while the afternoon group decreased to 83.4% (57/66). The difference in excellent rates significantly increased when HR > 75 bpm. The Wilcoxon Signed-Rank Test revealed statistically significant differences between the morning and afternoon groups across various HR ranges before and after medication.
Figure 3 illustrates the proportion of images with subjective scores ≥ 4 points in the morning and afternoon groups at different heart rates. When the initial heart rate was ≤ 70 bpm, the morning group’s excellent image rate was above 92.9%, while the afternoon group’s rate decreased from 95.7% (HR ≤ 60 bpm) to 76.1% (65 < HR ≤ 70 bpm). When the initial heart rate exceeded 70 bpm, the morning group’s excellent image rate declined gradually with increasing heart rate, whereas the afternoon group exhibited a more pronounced decline.
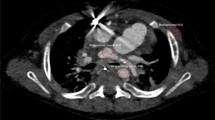
CCTA examination showed different types of artefacts and scoring results. Patient 1 (1 A, 1B, 1 C, 1D) – 1 A shows the axial image at the position marked by the arrow in 1B (RCA curved CPR reconstruction). 1 C is the CCTA axial image, where the contour of the RCA segment is unclear, with a comet-tail blur at the arrow position. 1D (VR image) shows the overall continuity of the CCTA with no layering or motion artefacts, indicating that only the RCA segment exhibits artefacts, with a score of 4. Patient 2 (2 A, 2B, 2 C, 2D, 2E, 2 F) – 2 A and 2 C correspond to 2B (RCA curved CPR reconstruction) and 2D (LCX curved CPR reconstruction) at the marked positions in the axial images. 2E is the CCTA axial image, where the contours of both the RCA and LCX vessels are unclear, with comet-tail blur present. 2 F (VR image) demonstrates the overall continuity of the CCTA with no layering or motion artefacts, indicating artefacts in both the RCA and LCX segments, resulting in a score of 3.
The impact of different examination time periods on coronary CTA image quality under varying heart rate conditions. The x-axis represents the heart rate of patients after medication during the CCTA examination, while the y-axis shows the proportion of CCTA images with excellent quality (subjective score ≥ 4).
Correlation of image quality and regression analysis
Spearman correlation analysis was performed to assess the relationship between image quality and various factors. The correlation coefficients between image quality and age, gender(female), initial heart rate, post-medication heart rate, heart rate difference before and after medication, percentage change in heart rate after medication, radiation dose, and examination time(14:00–18:00) periods were 0.175, -0.050, -0.154, -0.675, 0.545, 0.585, 0.364, and − 0.251, respectively (Table 4). A strong negative correlation was observed between post-medication heart rate and image quality (ρ = -0.675, p < 0.001). Conversely, the heart rate difference before and after medication (ρ = 0.545, p < 0.001) and the percentage change in heart rate after medication (ρ = 0.585, p < 0.001) exhibited moderate positive correlations with image quality. Correlations between other variables and image quality were weak or non-significant (p > 0.05).
Given the multicollinearity between the difference in heart rate before and after medication and the percentage change in heart rate after medication (ρ = 0.872, p < 0.001), the percentage change in heart rate was excluded from subsequent regression analysis to avoid multicollinearity bias. A multivariable logistic regression analysis was conducted to examine the independent associations between image quality and other variables. The model included age, gender, initial heart rate, post-medication heart rate, heart rate difference before and after medication, radiation dose, and examination time intervals. Results showed that age significantly impacted coronary CTA image quality (OR = 1.023, 95% CI 1.002–1.045, P = 0.032). Examination time intervals also had a significant effect on image quality (OR = 2.395, 95% CI 1.451–3.954, P = 0.001). However, initial heart rate, post-medication heart rate, heart rate difference, radiation dose, and gender did not significantly affect coronary CTA image quality (p > 0.05; see Table 5 for details).
The regression equation is as follows:
Y denotes image quality, X1 indicates different examination time intervals, and X2 represents age.
Age and different examination time periods are independent factors influencing image quality, with the morning group showing significantly better image quality than the afternoon group (OR = 2.395, p < 0.001). Although the heart rate after medication is significantly negatively correlated with image quality, it did not show independent statistical significance in the regression model.
The relationship between heart rate and image quality at different examination times
ROC analysis was used to evaluate the relationship between heart rate before and after medication and image quality at different time intervals. For the morning group, the area under the ROC curve (AUC) for heart rate before and after medication were 0.598 and 0.890, respectively, both significantly greater than 0.5 based on the DeLong test (p < 0.001). the corresponding Youden indices (J) were 0.632 and 0.816, with optimal cut-off points of 79 bpm and 71 bpm, respectively (Fig. 4). The study suggests that by controlling the initial heart rate to below 79 bpm before the examination and administering 25 mg of metoprolol, the heart rate can be adjusted to an optimal range, thereby enhancing image quality. Furthermore, a heart rate below 71 bpm during the examination is considered an appropriate range to ensure image quality. For the afternoon group, the area under the ROC curve (AUC) for heart rate before and after medication were 0.596 and 0.812, respectively, both significantly greater than 0.5 according to the DeLong test (p < 0.001).The corresponding Youden indices (J) were 0.798 and 0.917, with optimal cut-off points of 75 bpm and 68 bpm, respectively (Fig. 5). The results indicate that by controlling the initial heart rate to below 75 bpm before the examination and administering 25 mg metoprolol, the heart rate range can be significantly optimised to achieve superior image quality. During the examination, a heart rate below 68 bpm is regarded as an acceptable range for ensuring image quality.
The relationship between heart rate and image quality in the morning cohort was analysed using the ROC method. The area under the ROC curve (AUC) for the initial heart rate in the morning group was 0.598 (p < 0.001), with a Youden’s Index (J) of 0.632 and an optimal cut-off value of 79 bpm. The area under the ROC curve (AUC) for the heart rate post-medication was 0.890 (p < 0.001), with a Youden’s Index of 0.816 and an optimal cut-off value of 71 bpm.
The relationship between heart rate and image quality in the afternoon group was analysed using the ROC method. The area under the ROC curve (AUC) for the initial heart rate in the afternoon group was 0.596 (p < 0.001), with a Youden’s Index of 0.798 and an optimal cut-off value of 75 bpm. The area under the ROC curve for the heart rate after medication was 0.812 (p < 0.001), with a Youden’s Index of 0.917 and an optimal cut-off value of 68 bpm.
Discussion
The main finding of this study is that coronary computed tomography angiography (CCTA) conducted between 08:00 and 12:00 resulted in superior image quality compared to that performed between 14:00 and 18:00. Specifically, the image high-quality rate in the morning group was 87.9%, significantly higher than the 74.1% in the afternoon group. Furthermore, we observed that the optimal cut-off values for initial heart rate were 79 bpm in the morning group and 75 bpm in the afternoon group, while after medication, the optimal cut-off values were 71 bpm and 68 bpm, respectively. These data confirm that morning examinations exhibit greater tolerance for higher heart rates, making them more suitable for higher heart rates and ensuring superior image quality.
This finding aligns with our hypothesis that circadian rhythm variations affect heart rate control, thereby influencing CCTA image quality11.The lower heart rate observed in the morning may be linked to the regulation of the body’s internal biological clock, where lower stress levels and a more balanced autonomic nervous system contribute to greater stability and relatively lower heart rates8. This finding supports the results of Bonnemeier et al.12 who observed that heart rate variability (HRV) is at its lowest during the day, which facilitates better heart rate control and consequently enhances CCTA image quality. Our study found a positive linear relationship between image quality and age, as revealed by both correlation and regression analyses, although this effect was not statistically significant. This finding is consistent with the research of Trifiro, G et al.13 who found that, at the same concentration of β-blockers, elderly individuals exhibited more significant blood pressure reduction and heart rate decrease compared to younger individuals. In our experiment, the fixed dose of 25 mg may have been insufficient to achieve optimal heart rate control in younger patients, whereas elderly patients showed a better response. Heart rate variability (HRV) decreases with age14,15,16, and the study by Bonnemeier et al.12 emonstrated that the decline in HRV is most pronounced between the ages of 31–40 and 41–50. Opthof T’s study17 further supports this hypothesis, showing that normal ageing results in a decrease in diastolic repolarisation and a reduction in the duration of respiratory sinus arrhythmia, which in turn leads to a lower intrinsic heart rate. This could explain the positive correlation between image quality and age. Our findings thus emphasise the potential influence of age on CCTA image quality and uncover the relationship between heart rate control and age, offering new avenues for future research. This is especially relevant when exploring how different age groups respond to CCTA and how to optimise examination protocols for various patient populations. These findings have significant implications for clinical practice and future research in the field of radiology, contributing to improved CCTA image quality and diagnostic accuracy.
The ongoing advancement of CT technology, especially with upgrades in both hardware and software, has led to significant changes in the scope and workflow of CT examinations, particularly in coronary CT angiography (CCTA) imaging18。The enhancement in time resolution due to technological advances has enabled higher heart rate thresholds for CCTA imaging, which is crucial for effective heart rate control. The improvement in time resolution involves multiple aspects, including the reduction in gantry rotation time, an increase in the number of x-ray tubes and detectors, and upgrades to motion compensation algorithms and detector width6。From the first-generation dual-source MSCT used by S. Achenbach et al. to the third-generation dual-source MSCT, we have observed a continuous increase in the upper limit for heart rate control4,19,20。The use of motion calibration algorithms (e.g.MAC) has further improved the machine’s time resolution, enabling higher diagnostic heart rate limits even at lower gantry rotation speeds21。Moreover, this study effectively tackled CCTA imaging challenges in patients with irregular heart rates or those unable to hold their breath by employing 16 cm wide detector technology in combination with ultra-high rotation speeds (0.25s/r). This approach mitigated the impact of arrhythmias and poor breath-holding on image quality, demonstrating that the acceptable heart rate threshold for image quality is higher during the morning compared to the afternoon.
Heart rate control is essential for obtaining high-quality images and minimising radiation exposure in coronary computed tomography angiography (CCTA). Research (Neefjes LA et al.22 ) suggests that an increase in heart rate leads to a decline in image quality and an increase in radiation dose. A heart rate of 65 bpm is considered the threshold beyond which image quality deteriorates significantly. A study by Ondrejkovic M et al.23 demonstrated that at a gantry rotation speed of 0.25 r/s, image motion artefacts are minimal when the heart rate is below 75 bpm, with pulsation artefacts less than 1 mm. When the heart rate is between 80 and 90 bpm, vascular and pulsation artefacts increase, with pulsation artefacts exceeding 1 mm. Image quality is significantly better when the heart rate is below 75 bpm compared to heart rates above 80 bpm, further confirming the importance of heart rate control. Ondrejkovic M et al.23 demonstrated that with a 16 cm wide detector and a gantry rotation speed of 0.28 s/r, the excellent image quality rate is 76% when the heart rate is below 70 bpm, whereas it drops to 50% when the heart rate exceeds 70 bpm. In this study, when the heart rate was ≤ 70 bpm, the rate of excellent image quality was 92.4% (97.2% in the morning group, 87.2% in the afternoon group). However, when the heart rate exceeded 70 bpm, the excellent image quality rate dropped to 48.5% (55.1% in the morning group and 43.9% in the afternoon group). The image quality in our study was superior to the results reported by Ondrejkovic M et al., yet the radiation dose did not increase. This may be attributed to the coronary motion correction algorithm employed in our study24, which enhances tolerance to variations in heart rate and optimises image quality. Therefore, although new CT devices improve image quality through various methods, heart rate control remains a key factor in improving image quality and reducing radiation dose in CCTA examinations, with significant clinical implications.
This study has several limitations. Firstly, our scoring system is based entirely on subjective evaluation, lacking an objective, quantifiable method, which could introduce potential bias in the assessment. Secondly, the study included only two examination time points, restricting a comprehensive analysis of how different time intervals may impact image quality. Future studies should explore additional time points to enhance the generalisability of the findings. Furthermore, as this study was not validated using CT scanners from different manufacturers, we cannot confirm whether the findings are consistent across various devices. This will require further investigation in subsequent studies. Finally, the study administered a standard dose of 25 mg of β-blockers, and it remains uncertain whether doubling the dose for patients with high heart rates affects structural changes. This will be investigated in future studies.
Conclusion
The key finding of this study is that coronary CT angiography (CCTA) conducted in the morning (08:00–12:00) provided superior image quality compared to examinations carried out in the afternoon (14:00–18:00). Specifically, the heart rate thresholds before and after medication in the morning group (79 bpm and 71 bpm, respectively) were higher than those in the afternoon group (75 bpm and 68 bpm, respectively). This result suggests that CCTA performed in the morning can accommodate higher heart rates while maintaining image quality. Compared to the afternoon period, this finding raised the heart rate threshold from 68 bpm to 71 bpm. These data provide strong support for the scheduling of CCTA examinations and heart rate management in clinical practice.
Data availability
Data availability statement: Data will be made available on request from the corresponding author, Yin Wei, on reasonable request.
Abbreviations
- CCTA:
-
Coronary computed tomography angiography
- HR:
-
Heart rate
- bpm:
-
Beats per minute
- ROC:
-
receiver operating characteristic
- AUC:
-
Area under the curve
- CAD:
-
Coronary artery disease
- VR:
-
Volume rendering
- MIP:
-
Maximum intensity projection
- MPR:
-
Multiplanar reconstruction
- CPR:
-
Curved planar reconstruction
- RCA:
-
Right coronary artery
- LM:
-
Left main coronary artery
- LAD:
-
Left anterior descending artery
- LCX:
-
Left circumflex artery
- ED:
-
Effective dose
- DLP:
-
Dose-length product
- HRV:
-
Heart rate variability
References
Serruys, P. W. et al. Coronary computed tomographic angiography for complete assessment of coronary artery disease: JACC State-of-the-Art Review[J]. J. Am. Coll. Cardiol. 78 (7), 713–736. https://doi.org/10.1016/j.jacc.2021.06.019 (2021).
Collet, C. et al. Coronary computed tomography angiography for heart team decision-making in multivessel coronary artery disease[J]. Eur. Heart J. 39 (41), 3689–3698. https://doi.org/10.1093/eurheartj/ehy581 (2018).
Abbara, S. et al. SCCT guidelines for the performance and acquisition of coronary computed tomographic angiography: A report of the society of cardiovascular computed tomography guidelines committee: endorsed by the North American society for cardiovascular imaging (NASCI)[J]. J. Cardiovasc. Comput. Tomogr. 10 (6), 435–449. https://doi.org/10.1016/j.jcct.2016.10.002 (2016).
Morsbach, F. et al. Performance of turbo high-pitch dual-source CT for coronary CT angiography: first ex vivo and patient experience[J]. Eur. Radiol. 24 (8), 1889–1895. https://doi.org/10.1007/s00330-014-3209-7 (2014).
Shuai, T. et al. Free-breathing coronary CT angiography using 16-cm wide-detector for challenging patients: comparison with invasive coronary angiography[J]. Clin. Radiol. 73 (11), 981–986. https://doi.org/10.1016/j.crad.2018.06.023 (2018).
FitzGerald, P. et al. Quest for the ultimate cardiac CT scanner[J]. Med. Phys. 44 (9), 4506–4524. https://doi.org/10.1002/mp.12397 (2017).
Rovere, G. et al. Practical instructions for using drugs in CT and MR cardiac imaging[J]. Radiol. Med. 126 (3), 356–364. https://doi.org/10.1007/s11547-020-01261-4 (2021).
Waterhouse, J., Fukuda, Y. & Morita, T. Daily rhythms of the sleep-wake cycle[J]. J. Physiol. Anthropol. 31 (1), 5. https://doi.org/10.1186/1880-6805-31-5 (2012).
Jia, X. et al. Individualized protocol for radiation and contrast medium dose reduction in one-stop assessment for kidney transplantation patients[J]. Eur. J. Radiol. 140, 109757. https://doi.org/10.1016/j.ejrad.2021.109757 (2021).
Einstein, A. J. et al. Radiation dose from single-heartbeat coronary CT angiography performed with a 320-detector row volume scanner[J]. Radiology 254 (3), 698–706. https://doi.org/10.1148/radiol.09090779 (2010).
Achenbach, S. et al. Influence of heart rate and phase of the cardiac cycle on the occurrence of motion artifact in dual-source CT angiography of the coronary arteries[J]. J. Cardiovasc. Comput. Tomogr. 6 (2), 91–98. https://doi.org/10.1016/j.jcct.2011.11.006 (2012).
Bonnemeier, H. et al. Circadian profile of cardiac autonomic nervous modulation in healthy subjects: differing effects of aging and gender on heart rate variability[J]. J. Cardiovasc. Electrophysiol. 14 (8), 791–799. https://doi.org/10.1046/j.1540-8167.2003.03078.x (2003).
Trifirò, G. & Spina, E. Age-related changes in pharmacodynamics: focus on drugs acting on central nervous and cardiovascular systems[J]. Curr. Drug Metab. 12 (7), 611–620. https://doi.org/10.2174/138920011796504473 (2011).
Shaffer, F. & Ginsberg, J. P. An overview of heart rate variability metrics and Norms[J]. Front. Public. Health. 5, 258. https://doi.org/10.3389/fpubh.2017.00258 (2017).
Abhishekh, H. A. et al. Influence of age and gender on autonomic regulation of heart[J]. J. Clin. Monit. Comput. 27 (3), 259–264. https://doi.org/10.1007/s10877-012-9424-3 (2013).
Nunan, D., Sandercock, G. R. & Brodie, D. A. A quantitative systematic review of normal values for short-term heart rate variability in healthy adults[J]. Pacing Clin. Electrophysiol. 33 (11), 1407–1417. https://doi.org/10.1111/j.1540-8159.2010.02841.x (2010).
Opthof, T. The normal range and determinants of the intrinsic heart rate in man[J]. Cardiovasc. Res. 45 (1), 177–184. https://doi.org/10.1016/s0008-6363(99)00322-3 (2000).
Yan, C. et al. Automatic vs manual coronary CT angiography reconstruction for whole-heart coverage CT scanner: a comparison study in general patient population[J]. J. Xray Sci. Technol. 30 (2), 389–398. https://doi.org/10.3233/XST-211048 (2022).
Achenbach, S. et al. High-pitch spiral acquisition: a new scan mode for coronary CT angiography[J]. J. Cardiovasc. Comput. Tomogr. 3 (2), 117–121. https://doi.org/10.1016/j.jcct.2009.02.008 (2009).
Achenbach, S. et al. Detection of coronary artery stenoses by low-dose, prospectively ECG-triggered, high-pitch spiral coronary CT angiography[J]. JACC Cardiovasc. Imaging. 4 (4), 328–337. https://doi.org/10.1016/j.jcmg.2011.01.012 (2011).
Machida, H. et al. Influence of the motion correction algorithm on the quality and interpretability of images of single-source 64-detector coronary CT angiography among patients grouped by heart rate[J]. Jpn J. Radiol. 33 (2), 84–93. https://doi.org/10.1007/s11604-014-0382-1 (2015).
Neefjes, L. A. et al. Diagnostic accuracy of 128-slice dual-source CT coronary angiography: a randomized comparison of different acquisition protocols[J]. Eur. Radiol. 23 (3), 614–622. https://doi.org/10.1007/s00330-012-2663-3 (2013).
Ondrejkovic, M. et al. Radiation dose and image quality of CT coronary angiography in patients with high heart rate or irregular heart rhythm using a 16-cm wide detector CT scanner[J]. Med. (Baltim). (37), 101. https://doi.org/10.1097/MD.0000000000030583 (2022).
Yin, W. et al. Influence of a new motion correction algorithm (CardioCapture) on the correlation between heart rate and optimal reconstruction phase[J]. Heliyon 9 (10), e20588. https://doi.org/10.1016/j.heliyon.2023.e20588 (2023).
Acknowledgements
This study was financially supported by The National Key Research and Development Program of China(No.2016YFC0104610). The sponsoring organization had no involvement in the conduct, writing or submission of the research results.
The appropriate ethics committee research registration number:CHE2020-164
Author information
Authors and Affiliations
Contributions
ZqK and JkY made measurement and analysis of CT data, and drafted the article. ZqK, BhZ and XL contributed to statistical analysis and manuscript revision. WY and XzL contributed to the conception and design of this research, analysis of data and manuscript revision. All authors approved the final version and made agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Kang, Z., Yang, J., Ling, X. et al. Optimising the workflow of coronary computed tomography angiography through effective timing and heart rate management. Sci Rep 15, 38302 (2025). https://doi.org/10.1038/s41598-025-22178-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-22178-w