Abstract
Rare skeletal disorders (RSDs) cause disability, pain, and reduced quality of life (QoL), with limited access to effective rehabilitation. This pilot study evaluated the feasibility, safety, and preliminary effects of a sailing-based rehabilitation program for adolescents with RSDs, integrating wearable inertial sensors and validated patient-reported outcomes. Eight adolescents (12–18 years) with RSDs participated in a five-day sailing intervention focused on physical activity, social interaction, and psychological reflection. Feasibility (recruitment, retention, adherence, acceptability) and safety (adverse events) were primary outcomes. Secondary measures included QoL (EuroQol 5-Dimension), psychological well-being (Pediatric Outcomes Data Collection Instrument, Rosenberg Self-Esteem Scale, Young Persons-Clinical Outcomes in Routine Evaluation, Tampa Scale of Kinesiophobia), and physical function assessed using inertial measurement units. All feasibility criteria met or exceeded: 100% retention and adherence, and high acceptability (mean score 3,75, SD = 0,46). No serious adverse events occurred. Significant benefits were found in proprioception (p = 0.01), postural control (p = 0.01), gait quality (p = 0.04), and upper limb function (p = 0.02). Trends toward improved QoL (EuroQol 5-Dimension Visual Analogue Scale, p = 0.10), happiness (Pediatric Outcomes Data Collection Instrument, p = 0.06), and reduced kinesiophobia (Tampa Scale of Kinesiophobia, p = 0.03) were observed. Some effects declined at follow-up. Sailing-based rehabilitation appears feasible, safe, and potentially effective for improving physical and psychological outcomes in RSDs. These findings support the development of larger controlled trials.
Trial registration: ClinicalTrials.gov NCT06397443; release date: May 2, 2024.
Introduction
Rare diseases consist of a heterogeneous group of disorders involving approximately 263–446 million people worldwide, with a deep impact on individuals’ lives1. Among these, rare skeletal disorders (RSDs) represent a group of conditions characterized by significant skeletal deformities, chronic pain, disability, and reduced quality of life2. Despite their extreme impact, effective rehabilitation options for RSD patients remain severely limited 3. This unmet need exacerbates psychological distress and social isolation, with patients often reporting frustration, loss of independence, and difficulty navigating fragmented healthcare systems4,5. The lack of adapted rehabilitation services not only delays physical recovery but also contributes to a diminished overall quality of life6.
Addressing these needs requires innovative and multidisciplinary approaches that integrate physical rehabilitation with psychological support, all within the framework of the International Classification of Functioning, Disability, and Health7. Sailing-based programs have emerged as an encouraging intervention with the potential to address the multifaceted needs of RSD patients. These programs leverage nature-based activities and group collaboration to foster physical and psychological health. Previous studies indicate that sailing interventions can reduce distress and enhance well-being in various populations, including cancer survivors and individuals with chronic conditions8,9,10. Furthermore, sailing-based programs provide an engaging environment that combines physical activity with social interaction, essential factors for improving participation and quality of life in individuals facing complex physical and emotional challenges11.
Prior research on sailing-based rehabilitation have primarily examined psychosocial and quality of life outcomes in different clinical populations. Carta et al. (2014) reported improved well-being in individuals with severe mental disorders after a structured sailing program8, while Mirandola et al. (2020) observed reduced distress and better quality of life in breast cancer survivors following a tailored sailing intervention9.
Evidence from neurological and motor disorders also indicates rehabilitative benefits. Recio et al. (2013) showed that sailing supports social integration12, and Aprile et al. (2016) reported neuromotor improvements13. Interventions combining virtual reality with sailing simulators in children with motor and balance impairments, including spinal cord injury, cerebral palsy, diplegia, apraxia, and dyspraxia, have been shown to produce significant improvements in postural control. These benefits arise from the integration of exteroceptive and proprioceptive stimuli, reinforcing the broader therapeutic value of sports engagement for individuals with disabilities in improving quality of life and participation 13.
More recently, Boarini et al. (2024) reported short-term health-related quality-of-life improvements after a five-day sailing program in individuals with RSDs10. The present study builds on and extends this body of work by focusing on adolescents with RSDs, integrating synchronized wearable sensor and pressure platform measurements to objectively assess proprioception, postural stability, gait, and upper-limb motor function, and prospectively evaluating feasibility and safety in conjunction with multidomain outcomes and a three-month follow-up period.
Advanced technologies like Inertial Measurement Units (IMUs) are increasingly utilized in rehabilitation research. IMUs provide reliable tools for quantifying complex movement patterns, such as mobility and posture, while carefully monitoring rehabilitation progress14,15. For individuals with RSDs, these systems permit precise evaluation of balance, gait, and upper limb function, domains often compromised by their condition. By integrating objective data from IMUs with validated Patient-Reported Outcomes (PROs), well suited to evaluate populations with musculoskeletal conditions, such as EuroQol 5-Dimension (EQ-5D), Pediatric Outcomes Data Collection Instrument (PODCI), Rosenberg Self-Esteem Scale (RSES), Young Persons-Clinical Outcomes in Routine Evaluation (YP-CORE), and Tampa Scale of Kinesiophobia (TSK), this study adopts a multidimensional approach to evaluating both the physical and psychological effects of rehabilitation16,17,18,19.
This research addresses a central public health issue: the urgent need for effective rehabilitation strategies for individuals with RSDs20. By systematically evaluating the feasibility and safety of a structured sailing-based intervention, this study contributes to advancing medical knowledge and practice in rehabilitative care while exploring the integration of cutting-edge motion tracking technologies and psychological well-being. Furthermore, this study sets itself within the broader context of emerging trends in rehabilitation research that point up combining advanced technologies with supportive social environments. Such approaches have demonstrated promising results in improving outcomes for patients with rare diseases and other chronic conditions21,22,23.
The primary aim of the present study is to evaluate the feasibility and safety of a sailing-based rehabilitation intervention for individuals with RSDs. A secondary aim is to explore potential changes in sensor-derived measures of proprioception, posture, gait, and upper limb function, as well as PROs. Our findings may inform scalable, patient-centered rehabilitation strategies customized to the unique needs of individuals with RSDs, contributing to improved outcomes and guiding future therapeutic approaches for this neglected population24.
Methods
Study design
This single-center, non-randomized, longitudinal feasibility study was conducted from May 16th to September 13th, 2024, to evaluate feasibility, safety, and describe trends in potential efficacy of a sailing-based rehabilitative intervention for individuals with RSDs.
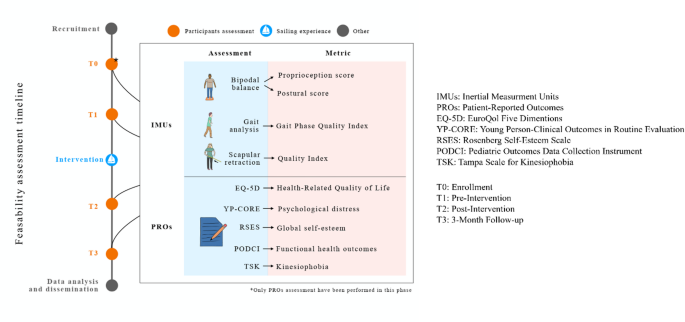
The study design was chosen to prioritize analysis of feasibility metrics while addressing the challenges of conducting research with small, and heterogeneous populations affected by RSDs. The intervention and assessments followed the CONSORT guidelines for feasibility trials (Appendix A)25. A visual summary of the study’s timeline and participants assessment is provided in Fig. 1.
Feasibility study timeline and participants assessment from recruitment to three-month follow-up.
All data were managed using the REDCap electronic data storage tool hosted at Yale University. REDCap’s real-time data validation, automated audit trails, and centralized management features ensured data integrity across multiple time points, particularly given the complexity of managing repeated measures in a longitudinal study26.
Ethical approval was obtained from the Local Ethical Committee, Comitato Etico Area Vasta Emilia Centro (CE-AVEC), under protocol number 115/2024/Sper/IOR. The study was registered on ClinicalTrials.gov (NCT06397443) and conducted in accordance with the 1964 Declaration of Helsinki and its subsequent amendments.
Setting
The study was conducted across three sites: enrollment (at T0) and three-month follow-up assessment (T3) were performed at IRCCS Istituto Ortopedico Rizzoli (IOR), national referral centre for RSDs, based in Bologna, Italy; sailing sessions were held at the port of Marina di Ravenna, Italy; and ‘Palazzo Manzoni’ in San Zaccaria (Ravenna, Italy) served as the accommodation site, hosting the pre- and post-intervention (T1 and T2) evaluations.
Participants’ recruitment
Participants were recruited and screened from April 10th to May 10th, 2024, using a combined approach, including direct engagement during outpatient visits at the Department of Rare Skeletal Disorders at IOR and through outreach to the national rare disease community, with social media initiatives and patient advocacy networks, in collaboration with UNIAMO-Federazione Italiana Malattie Rare (UNIAMO-FIMR), the Italian umbrella patients advocacy organization, who played an essential role in the study’s conceptualization, planning, execution, and dissemination.
Eligibility criteria included: (a) age of 12 years or older; (b) a confirmed diagnosis of a rare skeletal disorder; (c) the ability to engage in physical activities with adaptations; and (d) no surgical interventions within the six months before enrollment. These criteria were selected to ensure a balance between homogeneity for meaningful analyses and practical inclusivity given the rarity of the conditions.
Exclusion criteria included: (a) ongoing evaluation for a differential diagnosis; (b) recent surgical interventions (< 6 months); (c) fractures or musculoskeletal injuries (< 12 months); (d) conditions contraindicating marine environments or sailing activities; (e) absence of a rare skeletal disorder (i.e., healthy individuals); or (f) refused to provide informed consent.
Written informed consent was obtained from participants aged 18 years or older, and parental/guardian consent was secured for minors.
Sample size
Consistent with FDA Rare Disease Guidance (2023), a sample size of eight participants was selected to prioritize feasibility outcomes (e.g., 85% power to detect adherence rates > 75% at α = 0.10)27. This approach aligns with recommendations for pilot studies in rare populations. Small cohorts are necessary in early-phase studies due to limited recruitment capacity and patient heterogeneity; as noted by Mitani et al. (2020) and Videnovic et al. (2023), small sample sizes are scientifically and ethically justified, providing reliable feasibility data to inform later for larger, confirmatory studies28,29.
Intervention
The sailing-based intervention (Fig. 2) was conducted through a collaboration between IOR research team, Euleria srl Società Benefit, and Marinando Ravenna ODV, a charitable organization based in Marina di Ravenna. This organization advocates sailing and navigation as effective means of promoting social integration, emphasizing the values of perseverance, discipline, respect for others, inclusivity, and active participation. The sailing sessions took place at the ‘Marinara’ port in Marina di Ravenna, with each session lasting approximately five hours. Sessions were scheduled from the morning to the afternoon, starting with a brief overview of the daily activities, followed by the division of participants into two groups of equal sizes.
Timeline and activities of the sailing-based rehabilitative intervention. The timeline and structure of the sailing-based rehabilitation intervention are summarized in this figure. The program covered five days, starting with an orientation session and a pre-intervention assessment (T1) on Day 1. Over the next three days (Days 2–4), participants engaged in daily sailing sessions, which included morning briefings to set objectives, practical sailing activities, and debriefing sessions to reflect on the experiences. On the final day (Day 5), a feedback session and post-intervention assessment (T2) were conducted to gather participants’ perspectives and to evaluate both physical and psychological outcomes. A follow-up at three months was also planned to assess the sustainability of the intervention’s effects.
Over a five-day period, participants engaged in three sailing sessions, each lasting five hours. The first and last days were dedicated to physical and psychological data collection, while the intermediate days included sailing activities combined with structured debriefing meetings. Participants were accommodated at the ‘Palazzo Manzoni’, which served as the site for daily debriefing activities, and hosted the full program on the first and last day. On the first day (May 27th, 2024), participants attended an explanatory session, where they were introduced to the Marinando skippers and volunteers, received basic sailing instruction, and were briefed on safety procedures. On the final day (May 31st, 2024), participants took part in an extended debriefing discussion, offering detailed feedback on their emotional, cognitive, and experiential responses to the intervention. This session lasted approximately two hours.
Two 10-meter sloop-rigged sailing yachts (Oasis 33s model), “Gaia” and “Rolling Black”, adapted to accommodate individuals with disabilities and special needs, were used for the sailing sessions (Fig. S1). These boats were skippered by Marinando-certified instructors. Volunteers from Marinando Ravenna ODV supported the participants throughout the activities. Participants actively rotated through various roles on the boat (such as steering, adjusting sails, and assisting with navigation), under the guidance of the skipper. The final session included a friendly race between the two boats. Each sailing session concluded with a one-hour debriefing session conducted by clinical psychologist research assistant, allowing participants to reflect on their experiences, discuss challenges faced, and provide feedback.
In case of adverse weather conditions, contingency plans were implemented to ensure both the safety and engagement of participants. Activities were either rescheduled or adapted while maintaining the treatment aims of the program.
Daily transportation between ‘Palazzo Manzoni’ and the ‘Marinara’ port was thoughtfully arranged by the ‘Pubblica Assistenza Paolina’ of Imola (Bologna, Italy), a public assistance service, ensuring continuous logistical support and participant safety throughout the program.
The intervention adhered to the Template for Intervention Description and Replication (TIDieR, Appendix B), ensuring detailed documentation for replicability30.
Measures
Demographic and clinical characteristics
Baseline demographic and clinical characteristics, including age, gender, educational level, participation in sports, disease type, anthropometric measurements (height, weight, and BMI), physical impairments, and mobility status, were collected during the enrollment visit at IOR (T0). All assessments were conducted by the physical medicine and rehabilitation team specializing in RSDs, using a study-specific Research Report Form (Appendix C).
Primary outcomes: feasibility and safety
Feasibility was evaluated following Bowen et al. (2009), which fits to this study’s context31. Five core parameters were assessed: recruitment, retention, compliance, adherence, and acceptability, with thresholds based on existing literature27,32.
Recruitment was the proportion of eligible participants approached and who consented, with a threshold of ≥ 80%. Retention reflected participants completing the intervention and assessments, targeting ≥ 75%. Compliance was measured by attendance, with satisfactory compliance set at ≥ 75% of sessions. Adherence was defined as total sailing hours completed relative to the planned program, with ≥ 75% completion deemed satisfactory. Acceptability was assessed post-intervention (T2) using a 5-point Likert scale evaluating agreement with the statement, “I have been happy with the things I have done,” from 0 (“Not at all”) to 4 (“Most or all the time”), with a mean score ≥ 3 indicating acceptability.
Safety was monitored after each sailing session using a checklist documenting adverse events, duration, premature discontinuation, and medications. A standardized approach tracked symptom progression and new adverse effects.
This multidimensional assessment comprehensively evaluated the study’s feasibility across key metrics.
Secondary outcomes: health-related quality of life (HRQoL), psychological well-being, and physical functioning
HRQoL and psychological well-being were assessed at all time points (T0 to T3) using validated Italian versions of standardized instruments33,34,35,36,37. A clinical psychology research assistant specializing in RSDs and affiliated with IOR conducted the assessments with paper-based forms.
The EQ-5D is a standardized generic instrument for assessing HRQoL. This study employed the EQ-5D-5 L version for adults (≥ 16 years), following EuroQol guidelines, which allow use from age 1238. The questionnaire evaluates five dimensions: mobility, self-care, usual activities, pain/discomfort, and anxiety/depression, each rated on five severity levels. A summary Index Value (IV) was assigned using the Italian EQ-5D-5 L value set40. Health profiles range from the best (11111) to the worst (55555), with IV scores from 1 (perfect health) to 0 (death-equivalent), and negative values for “worse than death.” Participants also rated their health on a visual analog scale (VAS) from 0 to 100, with higher scores indicating better overall health status.
The PODCI assesses functional health outcomes in pediatric and adolescent musculoskeletal conditions41. It includes 86-item across six scales: Upper Extremity, Transfer and Basic Mobility, Sports and Physical Function, Pain/Comfort, Happiness, and Global Function. Scores range from 0 to 100, with higher values indicating better function. It provides a comprehensive measure of physical ability, pain, and psychosocial satisfaction.
The RSES measures global self-esteem in individuals aged ≥ 12 years42. It includes 10 items rated on a 4-point Likert scale, assessing positive (e.g., “I feel I am a person of worth”) and negative self-esteem (e.g., “At times, I think I am no good at all”). Scores range from 10 to 40, with higher values indicating greater self-esteem.
The YP-CORE assesses psychological distress and well-being in youth16. It consists of 10 items rated on a 5-point Likert scale (0–4), covering emotional well-being, interpersonal functioning, and coping. Scores range from 0 to 40, with higher values indicating greater distress.
The TSK evaluates fear of movement or re-injury due to pain43. The 13-item Italian version, rated on a 4-point Likert scale (1–4), measures harm and activity avoidance. Scores range from 13 to 52, with higher values indicating greater kinesiophobia. It is validated for musculoskeletal and chronic pain populations37.
Physical functioning was assessed from T1 to T3 using objective measures developed in collaboration with biomedical engineers and bioinformatician specializing in RSDs, affiliated with IOR and Euleria Health, a Benefit Company specializing in digital rehabilitation solutions. All assessments were supervised by the physical medicine and rehabilitation team and conducted according to a standardized physical functioning exercises protocol (Appendix D).
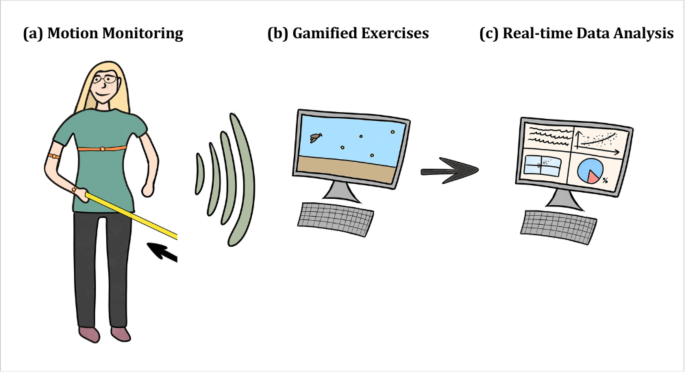
The IMUs are wearable, non-invasive devices that provide objective data on movement patterns, including mobility, proprioception, and posture44. They offer quantitative measurements that, along with self-reported outcomes, enable a comprehensive assessment of physical improvement. In this study, five IMUs and a pressure board were integrated with dedicated software (Euleria Lab, Euleria srl, Rovereto, Italy). Both systems communicated with the software via Bluetooth Low Energy (BLE), and operated at a 60 Hz sampling frequency, enabling synchronized data acquisition and real-time visualization (Fig. 3). The IMU system has an angular resolution of 0.1° and a dynamic accuracy within ± 2°, thereby meeting the threshold recommended for clinically relevant motion analysis, particularly in monitoring upper-limb movements45,46. The IMUs were positioned on specific anatomical landmarks with adjustable elastic bands, as detailed below. Calibration was performed before each assessment, requiring participants to stand still for three seconds while wearing the IMUs, and, when specified, standing on the pressure platform.
Three primary assessments evaluated mobility using IMUs:
-
(a)
Bipodal balance: a single IMU at the sternum level was used to estimate postural stability and the Center of Mass (COM), while the Centre of Pressure (COP) trajectory was derived from the pressure board data as participants stood for 30 s. The test was conducted with both eyes open and closed to assess proprioception, with the eyes-closed condition evaluating reliance on vestibular, and somatosensory inputs in the absence of visual feedback.
-
(b)
Gait analysis: five sensors placed on the feet, tibias, and trunk measured the gait cycle during straight walking. Gait phases were compared to standard references to detect asymmetrical or anomalies.
-
(c)
Arm exercises: participants performed bilateral and unilateral scapular retraction (isometric and repetitive) and overhead lateral shifts while wearing five IMUs on the trunk, wrists, and humeri. These controlled the Euleria Lab exergame and collected kinematic data.
Performance was quantified using:
-
I.
In-game score: The “Arm Quality Index” (AQI), calculated within Euleria Lab software, measured adherence to optimal movement trajectories.
-
II.
Raw and derived scores: Additional metrics included the Gait Phase Quality Index (GPQI), Proprioception Scores, and Postural Scores.
Workflow for IMU-based motion monitoring, gamification, and data analysis. This figure presents a sensor-based telerehabilitation workflow designed to enhance rehabilitation outcomes. The system incorporates three key components: (a) motion monitoring, where wearable sensors capture real-time motion data during patient movements; (b) gamified exercises, employing interactive tasks to promote patient adherence and motivation; and (c) real-time data analysis, delivering immediate feedback and generating clinically relevant insights to support data-driven decision-making for personalized rehabilitation interventions.
Statistical analysis
Descriptive statistics, including median, minimum and maximum, mean, standard deviations, and frequencies, were used to illustrate the study population and summarize feasibility, and safety outcomes.
HRQoL and psychological well-being outcomes were calculated according to the developers’ guidelines.
Physical functioning outcomes were assessed using specific quantitative metrics designed to evaluate proprioception, postural control, gait and arm quality, which are critical for understanding the impact of the intervention.
The Proprioception Score quantifies proprioceptive control by integrating trunk and COP variability. Trunk position was recorded using a sternum IMU, while COP position was measured via a pressure board. Both signals were synchronized at 60 Hz using Euleria Lab software (Euleria srl, Rovereto, Italy).
The score was calculated as:
where σt and σCOP represent the standard deviations of the distribution of the trunk and COP positions, respectively. Lower variability of trunk and COP indicates higher proprioceptive control, reflected by a higher Proprioception Score47,48.
The Posture Score assesses posture control by evaluating the alignment between trunk and COP. Trunk position was recorded via the sternum IMU, and COP via the pressure board, with both signals synchronized at 60 Hz.
The score was calculated as:
where \(\:{\overline{D}}_{\left(t-COP\right)}\:\)is the average Euclidean distance between trunk and COP positions. Smaller distances indicate closer trunk-COP alignment, corresponding to higher posture control and a higher Posture Score47,48.
The AQI quantifies the performance of the patient during the gaming experience, and it expressed as a percentage.
The GPQI total was calculated using the formula:
where P represents the observed proportion of time spent in each phase for both the right (R) and left (L) foot and the reference value r for each ith phase of the gait cycle. The reference values (r) correspond to normative gait timing in healthy subjects: heel strike 7%, full stance 39%, heel-off 16%, and swing 38%. The squared differences between the observed and reference values are summed across the four phases for both feet. The square root of this sum yields the GPQI, which reflects how the individual’s gait deviates from the normal pattern across all phases of the gait cycle. Higher GPQI values indicate greater deviation from normal gait, capturing both inter-limb asymmetries and overall phase timing differences.
Changes over time were analyzed using the Wilcoxon signed-rank test, selected for its robustness with small sample sizes and non-normal data distributions. Statistical significance was set at p < 0.05 and p < 0.10, recognizing the exploratory nature of this feasibility study and the inherent limitations of statistical power in small sample sizes. In addition, a significance of 0.10 < p < 0.15 was applied to highlight potential trends warranting further investigation. Data analysis was performed using R software version 3.6.3 (The R Foundation for Statistical Computing, Wien).
Results
Participant demographics and clinical presentation
A total of eight participants were enrolled in the study (Fig. S2). The cohort was equally distributed by gender (50% male, 50% female), with a mean age of 14 years (SD = 2), ranging from 12 to 18 years. Five out of eight participants (62,5%) had completed middle school, and 87,5% were active in sports. Diagnoses included Multiple Osteochondromas (50%), Ollier Disease (25%), and Osteogenesis Imperfecta (25%). Clinical assessment indicated that 62,5% of participants had physical impairments, including skeletal deformities, functional limitations, or both. Notably, all participants were independent in mobility, as clinically verified.
Table 1 provides a summary of the participants’ characteristics.
Feasibility and safety
The feasibility of the study was evaluated across five parameters: recruitment, retention, compliance, adherence, and acceptability (Table S1).
Recruitment reached 80% of the eligible individuals approached (8/10), meeting the ≥ 80% threshold (Fig. 3). Retention was 100% (8/8), exceeding the ≥ 75% threshold. Compliance and adherence were 100% (8/8), surpassing the ≥ 75% threshold for each. Acceptability was assessed post-intervention using a study-specific 5-point Likert scale, with an average score of 3,75 (SD = 0,46), exceeding the threshold of ≥ 3.
The high scores across all domains indicate that the study was highly feasible, with all predefined criteria met or exceeded.
No serious adverse effects were reported. Among the nine predefined categories of mild adverse effects monitored during the sailing-based intervention, only two were reported. Nausea/dizziness occurred in four out of eight participants (50%), predominantly after the second sailing session, whereas muscle soreness was reported by one out of eight participants (12,5%) after each of the three sessions. All adverse events were mild, transient, and self-limiting, requiring neither medication nor medical evaluation, and no participant discontinued the study due to adverse effects. No other categories of adverse events (muscle cramps, thermal discomfort, general fatigue, post-activity drowsiness, bruising/abrasions, temporary joint stiffness, or lower back/neck discomfort) were observed (Fig. 4). Complete results are available in Table S2.
Mild adverse effects reported by participants across the sailing-based intervention (N = 8). The figure illustrates the incidence of mild adverse effects across the three sailing sessions during the sailing-based rehabilitation intervention. The most frequently reported adverse effect was nausea or dizziness, occurring in approximately 50% of participants during the second sailing session. Muscle soreness was reported by a smaller proportion of participants across all sessions, with no reports of muscle cramps, thermal discomfort, general fatigue, post-activity drowsiness, bruising or abrasions, temporary joint stiffness, or lower back or neck discomfort.
Exploratory impact on HRQoL, psychological well-being, and physical functioning
HRQoL and psychological well-being
The sailing intervention was associated with positive benefits in HRQoL and psychological well-being (Table 2).
Notably, the overall health status (EQ-5D VAS) improved post-intervention (p = 0.04), suggesting a better perception of quality of life. Positive changes were observed in happiness (PODCI-Happiness scale, p = 0.06), and psychological distress showed a positive trend (YP-CORE, p = 0.15), indicating a potential short-term benefit in emotional well-being. However, most improvements were not sustained at three-month follow-up, with most scores showing a decline compared to post-intervention levels.
A sustained reduction in fear of movement (T2 vs. T3, p = 0.10) was observed at three months, with the Harm subscale showing a decrease over time (T0 vs. T3, p = 0.03). These results suggest that the intervention improved participants’ confidence in engaging in physical activities, a critical outcome for long-term behavioral changes. Additionally, trends toward positive changes were observed in the Global Functioning and Pain/Comfort scales (PODCI) post-intervention (p = 0.15 for both), although these effects diminished over time. These results highlight the transient nature of most intervention-related improvements, while pointing up the importance for ongoing support to maintain long-term benefits.
Complete results are available in Table S3.
Physical functioning
Proprioception and posture
In the Eyes Open exercise, marginal improvements in proprioception were observed immediately by post-intervention, becoming statistically significant at the three-month follow-up (T1 vs. T3, p = 0.01) (Fig. 5a, left panel). Postural stability improvements were significant across all conditions (Fig. 5a, right panel). Participants exhibited immediate benefits following the intervention, with sustained effects at the three-month follow-up (T1 vs. T2, p = 0.01; T1 vs. T3, p = 0.01, respectively). Heatmap analysis of balance metrics (Fig. 5b) revealed a slight and progressive reduction in COP displacement particularly in the mediolateral direction and trunk sway in the anteroposterior direction, indicating improved postural control.
Evaluation of proprioception, posture, and balance over time (eyes open) (N = 8). (a) Box plots of proprioception (left) and posture (right) scores measured at three time points: T1 (pre-intervention), T2 (post- intervention), and T3 (three-month follow-up). (b) Heatmaps represent the balance metrics in the anteroposterior (y-axis) and mediolateral (x-axis) directions for all eight participants: COP (top) and trunk sensor (bottom) coordinates during a 30-second static balance test at T1, T2, and T3.
Similar patterns emerged in the Eyes Closed exercise, where proprioception reaching statistical significance at the three-month follow-up (T1 vs. T3, p = 0.01) (Fig. 6a, left panel). Postural scores demonstrated a positive trend post-intervention that was maintained at T3 (T1 vs. T3, p = 0.02) (Fig. 6a, right panel). Heatmap analyses (Fig. 6b) highlighted consistent reductions in COP sway and trunk displacement across both anteroposterior and mediolateral directions during static balance tests, underscoring improved sensorimotor integration and postural stability in the absence of visual input. These findings suggest that the intervention effectively enhances proprioceptive function and balance control independently of visual compensation, with sustained benefits evident at follow-up.
Evaluation of proprioception, posture, and balance over time (eyes closed) (N = 8). (a) Box plots of proprioception (left) and posture (right) scores measured at three time points: T1 (pre-intervention), T2 (post- intervention), and T3 (three-month follow-up). (b) Heatmaps represent the balance metrics in the anteroposterior (y-axis) and mediolateral (x-axis) directions for all eight participants: COP (top) and trunk sensor (bottom) coordinates during a 30-second static balance test at T1, T2, and T3.
Gait phase quality index and arm quality index
No significant difference in total GPQI was observed between the pre- and post-intervention assessments (T1 vs. T2, p = 0.38). However, a significant decrease in total GPQI was detected over time (T1 vs. T3, p = 0.04) (Fig. 7a).
The intervention significantly improved upper limb function, particularly in repetitive and isometric movements involving the scapular region. For repeated bi-scapular retractions, increased AQI was noted post-intervention (T1 vs. T2, p = 0.02) (Fig. 7b). In isometric bi-scapular retraction, a positive trend of AQI was observed between pre- and post- intervention, although not significant (0.10 < p < 0.15) (Fig. 7c).
Detailed results of GPQI, and AQI scores over time can be found in Fig. S3.
Evaluation of Gait Phase Quality Index (GPQI), and Arm Quality Index (AQI) over time (N = 8). Box plots of GPQI total scores (a), AQI in repeated bi-scapular retraction (b), and AQI in isometric bi-scapular retraction (c) measured at three time points: T1 (pre-intervention), T2 (post- intervention), and T3 (three-month follow-up).
Discussion
RSDs represent a significant challenge in rehabilitation medicine, given their overwhelming impact on physical function, psychological well-being, and overall quality of life. Despite progresses in genetic diagnosis and therapeutic approaches, effective rehabilitation strategies for these conditions remain scarce, intensifying the burden of disease for patients and their families1,2. This study addresses these unmet needs by evaluating the feasibility and safety of a sailing-based rehabilitative intervention while exploring its potential to improve both physical and psychological outcomes through an innovative, multidisciplinary approach.
Our findings demonstrate that a sailing-based intervention is feasible and safe for adolescents with RSDs. High recruitment, retention, compliance, and adherence rates indicate strong participant engagement and acceptability. Moreover, mild and transient adverse effects underline the safety of this intervention. Notably, participants experienced positive benefits in physical functioning, psychological well-being, as well as HRQoL. These results align with prior evidence suggesting that sailing-based interventions could effectively address the multifaceted needs of individuals with chronic conditions by combining physical activity with social interaction in an engaging environment8,9,10,11,12,13.
The observed benefits may be attributed to several mechanisms. The intense and repetitive physical activities of sailing likely contributed to improved proprioception and postural stability, as evidenced by positive trends in sensory-motor integration and adaptive balance mechanisms. Additionally, mastering sailing skills may have enhanced participants’ confidence in managing their condition and daily activities, thereby fostering self-efficacy. The collaborative nature of sailing promoted social relationships among participants, potentially reducing feelings of isolation that are common among RSD patients.
Furthermore, overcoming challenges in an unconventional environment with others may have contributed to the participants’ promotion of psychological well-being, such as happiness and better perception of overall health status, consistent with research on nature-based therapies49,50,51. These psychological aspects are particularly relevant for patients with RSDs, who often navigate fragmented healthcare systems and limited opportunities for social engagement4,5.
Objective assessments using IMUs integrated with a pressure board revealed positive improvements in proprioception, postural stability, and neuromotor coordination. These findings are consistent with evidence supporting balance-challenging interventions aimed at improving sensory-motor integration14,52. In addition, improvements in gait quality and upper limb function suggest that sailing-based activities may act as a comprehensive rehabilitative tool targeting multiple domains affected by RSDs. However, the observed decline in outcomes at the three-month follow-up highlights the need for sustained interventions to maintain these benefits over time. This aligns with studies advocating longitudinal strategies to promote lasting functional benefits in chronic musculoskeletal populations53,54.
The integration of advanced technologies such as IMUs represents methodological advancement in rehabilitation research. These tools provide precise, objective measures of movement patterns that complement PROs, offering a multidimensional approach to evaluating intervention15,19. For instance, combining IMU data with validated PROs such as EQ-5D or PODCI enables a comprehensive assessment of both physical and psychological domains. This approach aligns with current trends in evidence-based medicine that emphasize integrating objective data with patient-centered measures to inform clinical practice25,30.
While these findings are promising, several limitations must be acknowledged. The small sample size limits statistical significance and generalizability. Additionally, the absence of a control group precludes definitive conclusions regarding the efficacy of this intervention compared to standard treatments. The brief follow-up period limits our ability to assess the long-term sustainability of benefits. Future studies should address these limitations by adopting randomized controlled designs with larger sample sizes and extended follow-up periods, while also exploring complementary approaches such as virtual reality-based sailing simulations to enhance accessibility for patients unable to participate in physical activities55. Such studies would provide more robust evidence on the effectiveness of sailing-based rehabilitation while allowing for a deeper understanding of its mechanisms of action.
Conclusion
In conclusion, this study contributes valuable evidence supporting the feasibility and safety of sailing-based rehabilitation for individuals with RSDs. By addressing both physical impairments and psychosocial challenges within a holistic framework, this intervention aligns with the principles of evidence-based medicine by offering an innovative solution to a pressing public health issue. Future research should build on these findings by leveraging advanced technologies and multidisciplinary approaches to develop scalable, patient-centered rehabilitation strategies adapted to the unique needs of individuals with RSDs and beyond.
Data availability
The data supporting the conclusions of this manuscript will be made available by the corresponding author on a reasonable request. The data is not publicly available due to national privacy regulations.
References
Nguengang Wakap, S. et al. Estimating cumulative point prevalence of rare diseases: analysis of the Orphanet database. Eur. J. Hum. Genet. 28 (2), 165–173. https://doi.org/10.1038/s41431-019-0508-0 (2020).
Shore, E. M. & Pacifici, M. JBMRPlus: Special issue on rare bone diseases 2019. JBMR Plus. 3 (8), e10218. https://doi.org/10.1002/jbm4.10218 (2019).
Gutenbrunner, C., Schiller, J., Goedecke, V., Lemhoefer, C. & Boekel, A. Screening of patient impairments in an outpatient clinic for suspected rare Diseases-A Cross-Sectional study. Int. J. Environ. Res. Public. Health. 19 (14), 8874. https://doi.org/10.3390/ijerph19148874 (2022).
von der Lippe, C., Diesen, P. S. & Feragen, K. B. Living with a rare disorder: a systematic review of the qualitative literature. Mol. Genet. Genomic Med. 5 (6), 758–773. https://doi.org/10.1002/mgg3.315 (2017).
Benito-Lozano, J. et al. Psychosocial impact at the time of a rare disease diagnosis. PLoS One. 18 (7), e0288875. https://doi.org/10.1371/journal.pone.0288875 (2023).
Sequeira, A. R., Mentzakis, E., Archangelidi, O. & Paolucci, F. The economic and health impact of rare diseases: A meta-analysis. Health Policy Technol. 10 (1), 32–44. https://doi.org/10.1016/J.HLPT.2021.02.002 (2021).
World Health Organization. The International Classification of Functioning, Disability and Health: ICF (WHO, 2001). https://www.who.int/standards/classifications/international-classification-of-functioning-disability-and-health. Accessed 3 Feb 2025.
Carta, M. G. et al. Sailing can improve quality of life of people with severe mental disorders: results of a cross over randomized controlled trial. Clin. Pract. Epidemiol. Ment Health. 10, 80–86. https://doi.org/10.2174/1745017901410010080 (2014).
Mirandola, D. et al. Tailored sailing experience to reduce psychological distress and improve the quality of life of breast cancer survivors: A Survey-Based pilot study. Int. J. Environ. Res. Public. Health. 17 (12), 4406. https://doi.org/10.3390/ijerph17124406 (2020).
Boarini, M. et al. Nature-based interventions for individuals with rare skeletal disorders: evaluation of a 5-day sailing program on health-related quality of life. Sci. Rep. 14 (1), 26339. https://doi.org/10.1038/s41598-024-77934-1 (2024).
Gillison, F. B., Skevington, S. M., Sato, A., Standage, M. & Evangelidou, S. The effects of exercise interventions on quality of life in clinical and healthy populations; a meta-analysis. Soc. Sci. Med. 68 (9), 1700–1710. https://doi.org/10.1016/j.socscimed.2009.02.028 (2009).
Recio, A. C. et al. Use of a virtual reality physical ride-on sailing simulator as a rehabilitation tool for recreational sports and community reintegration: a pilot study. Am. J. Phys. Med. Rehabil. 92 (12), 1104–1109. https://doi.org/10.1097/PHM.0000000000000012 (2013).
Aprile, I. et al. Use of a Virtual-Technological sailing program to prepare children with disabilities for a real sailing course: effects on balance and quality of life. J. Child. Neurol. 31 (8), 1074–1080. https://doi.org/10.1177/0883073816638756 (2016).
Tulipani, L. et al. Validation of an inertial sensor system for physical therapists to quantify movement coordination during functional tasks. J. Appl. Biomech. 34 (1), 23–30. https://doi.org/10.1123/jab.2016-0139 (2018).
Demeco, A. et al. Gait alteration in individual with limb loss: the role of inertial sensors. Sens. (Basel). 23 (4), 1880. https://doi.org/10.3390/s23041880 (2023).
Twigg, E. et al. The young person’s CORE: development of a brief outcome measure for young people. Counselling Psychother. Res. 9 (3), 160–168. https://doi.org/10.1080/14733140902979722 (2009).
do Monte, F. A. et al. Validation of the Brazilian version of the pediatric outcomes data collection instrument: a cross-sectional evaluation in children and adolescents with juvenile idiopathic arthritis. BMC Pediatr. 13, 177. https://doi.org/10.1186/1471-2431-13-177 (2013).
Luque-Suarez, A., Martinez-Calderon, J. & Falla, D. Role of kinesiophobia on pain, disability and quality of life in people suffering from chronic musculoskeletal pain: a systematic review. Br. J. Sports Med. 53 (9), 554–559. https://doi.org/10.1136/bjsports-2017-098673 (2019).
Zhou, T. et al. Health-Related quality of life in patients with different diseases measured with the EQ-5D-5L: A systematic review. Front. Public. Health. 9, 675523. https://doi.org/10.3389/fpubh.2021.675523 (2021).
UN General Assembly (76th Sess. –2022) Addressing the challenges of persons living with a rare disease and their families: resolution/adopted by the General Assembly. 2022 Jan 5 [cited 2025 Mar 12]; (2021). Available from: https://digitallibrary.un.org/record/3953765
Broadbent, F. J. & Swalwell, J. M. I can do more than I thought I could: exploring the online blogs from the sailing sclerosis oceans of hope journey. Disabil. Rehabil. 42 (6), 880–886. https://doi.org/10.1080/09638288.2018.1510046 (2020).
Høegmark, S., Andersen, T. E., Grahn, P., Mejldal, A. & Roessler, K. K. The wildman Programme-Rehabilitation and reconnection with nature for men with mental or physical health Problems-A Matched-Control study. Int. J. Environ. Res. Public. Health. 18 (21), 11465. https://doi.org/10.3390/ijerph182111465 (2021).
Manzanares, A., Camblor, Á., Romero-Arenas, S., Segado, F. & Gil-Arias, A. Adapted sailing teaching methodology using vsail-trainer simulator as rehabilitation therapy. A feasibility study. J. Spinal Cord Med. 47 (6), 960–967. https://doi.org/10.1080/10790268.2023.2228585 (2024).
Moy, N. et al. Interventions for improving clinical outcomes and health-related quality-of-life for people living with skeletal dysplasias: an evidence gap map. Qual. Life Res. 32 (10), 2751–2762. https://doi.org/10.1007/s11136-023-03431-z (2023).
Eldridge, S. M. et al. CONSORT 2010 statement: extension to randomised pilot and feasibility trials. BMJ 355, i5239. https://doi.org/10.1136/bmj.i5239 (2016).
Harris, P. A. et al. The REDCap consortium: Building an international community of software platform partners. J. Biomed. Inf. 95, 103208. https://doi.org/10.1016/j.jbi.2019.103208 (2019).
Center for Drug Evaluation and Research. Rare Diseases: Considerations for the Development of Drugs and Biological Products [Internet]. (FDA, 2024). https://www.fda.gov/regulatory-information/search-fda-guidance-documents/rare-diseases-considerations-development-drugs-and-biological-products. Accessed 12 Mar 2025.
Mitani, A. A. & Haneuse, S. Small data challenges of studying rare diseases. JAMA Netw. Open. 3(3), e201965. https://doi.org/10.1001/jamanetworkopen.2020.1965 (2020).
Videnovic, A. et al. Study design challenges and strategies in clinical trials for rare diseases: lessons learned from pantothenate kinase-associated neurodegeneration. Front. Neurol. 14, 1098454. https://doi.org/10.3389/fneur.2023.1098454 (2023).
Hoffmann, T. C. et al. Better reporting of interventions: template for intervention description and replication (TIDieR) checklist and guide. BMJ 348, g1687. https://doi.org/10.1136/bmj.g1687 (2014).
Bowen, D. J. et al. How we design feasibility studies. Am. J. Prev. Med. 36 (5), 452–457. https://doi.org/10.1016/j.amepre.2009.02.002 (2009).
Teresi, J. A., Yu, X., Stewart, A. L. & Hays, R. D. Guidelines for designing and evaluating feasibility pilot studies. Med. Care. 60 (1), 95. https://doi.org/10.1097/MLR.0000000000001664 (2022).
Savoia, E., Fantini, M. P., Pandolfi, P. P., Dallolio, L. & Collina, N. Assessing the construct validity of the Italian version of the EQ-5D: preliminary results from a cross-sectional study in North Italy. Health Qual. Life Outcomes. 4, 47. https://doi.org/10.1186/1477-7525-4-47 (2006).
Trisolino, G. et al. Translation and Cross-Cultural adaptation of the pediatric outcomes data collection instrument into the Italian Language. Children 9 (6), 853. https://doi.org/10.3390/children9060853 (2022).
Prezza, M., Trombaccia, F. R. & Armento, L. La scala dell’autostima Di rosenberg: traduzione e Validazione Italiana. [The Rosenberg Self-Esteem scale: Italian translation and validation]. Giunti Organizzazioni Speciali. 223, 35–44 (1997).
Di Biase, R. et al. Exploration of psychometric properties of the Italian version of the core young person’s clinical outcomes in routine evaluation (YP-CORE). Res. Psychotherapy: Psychopathol. Process. Outcome. 24 (2), 554. https://doi.org/10.4081/ripppo.2021.554 (2021).
Monticone, M. et al. Development of the Italian version of the Tampa scale of kinesiophobia (TSK-I): Cross-Cultural Adaptation, factor Analysis, Reliability, and validity. Spine 35 (12), 1241. https://doi.org/10.1097/BRS.0b013e3181bfcbf6 (2010).
EuroQol Group. EuroQol–a new facility for the measurement of health-related quality of life. Health Policy. 16 (3), 199–208. https://doi.org/10.1016/0168-8510(90)90421-9 (1990).
User Guides [Internet]. EuroQol. https://euroqol.org/information-and-support/documentation/user-guides/. Accessed 20 Jan 2025.
Finch, A. P., Meregaglia, M., Ciani, O., Roudijk, B. & Jommi, C. An EQ-5D-5L value set for Italy using videoconferencing interviews and feasibility of a new mode of administration. Soc. Sci. Med. 292, 114519. https://doi.org/10.1016/j.socscimed.2021.114519 (2022).
Daltroy, L. H., Liang, M. H., Fossel, A. H., Goldberg, M. J. & Group, T. P. O. I. D. The POSNA pediatric musculoskeletal functional health questionnaire: report on Reliability, Validity, and sensitivity to change. J. Pediatr. Orthop. 18 (5), 561. https://doi.org/10.1097/00004694-199809000-00001 (1998).
Rosenberg, M. The measurment of self-esteem. In Society and the Adolescent Self-Image [Internet]. 16–36 (Princeton University Press, 1965). http://www.jstor.org/stable/j.ctt183pjjh.5Accessed 24 Jan 2025.
Miller, R. P., Kori, S. H. & Todd, D. D. The Tampa scale: a measure of kinisophobia. Clin. J. Pain. 7 (1), 51 (1991).
Cutti, A. G., Paolini, G., Troncossi, M., Cappello, A. & Davalli, A. Soft tissue artefact assessment in humeral axial rotation. Gait Posture. 21 (3), 341–349. https://doi.org/10.1016/j.gaitpost.2004.04.001 (2005).
Lapresa, M. et al. Validation of Magneto-Inertial measurement units for Upper-Limb motion analysis through an anthropomorphic robot. IEEE Sens. J. 22 (17), 16920–16928. https://doi.org/10.1109/JSEN.2022.3193313 (2022).
Villa, G. et al. Validation of a commercially available IMU-Based system against an optoelectronic system for Full-Body motor tasks. Sensors 25 (12), 3736. https://doi.org/10.3390/s25123736 (2025).
Ruhe, A., Fejer, R. & Walker, B. Center of pressure excursion as a measure of balance performance in patients with non-specific low back pain compared to healthy controls: a systematic review of the literature. Eur. Spine J. 20 (3), 358–368. https://doi.org/10.1007/s00586-010-1543-2 (2011).
Prieto, T. E., Myklebust, J. B., Hoffmann, R. G., Lovett, E. G. & Myklebust, B. M. Measures of postural steadiness: differences between healthy young and elderly adults. IEEE Trans. Biomed. Eng. 43 (9), 956–966. https://doi.org/10.1109/10.532130 (1996).
Hartig, T., Mitchell, R., de Vries, S. & Frumkin, H. Nature and health. Annu. Rev. Public Health. 35 (35, 2014), 207–228. https://doi.org/10.1146/annurev-publhealth-032013-182443 (2014).
Coventry, P. A. et al. Nature-based outdoor activities for mental and physical health: systematic review and meta-analysis. SSM - Popul. Health. 16, 100934. https://doi.org/10.1016/j.ssmph.2021.100934 (2021).
Twohig-Bennett, C. & Jones, A. The health benefits of the great outdoors: A systematic review and meta-analysis of greenspace exposure and health outcomes. Environ. Res. 166, 628–637. https://doi.org/10.1016/j.envres.2018.06.030 (2018).
Peterka, R. J. Sensory integration for human balance control. Handb. Clin. Neurol. 159, 27–42. https://doi.org/10.1016/B978-0-444-63916-5.00002-1 (2018).
Giggins, O. M., Persson, U. M. & Caulfield, B. Biofeedback in rehabilitation. J. Neuroeng. Rehabil. 10 (1), 60. https://doi.org/10.1186/1743-0003-10-60 (2013).
Bennell, K. L., Dobson, F. & Hinman, R. S. Exercise in osteoarthritis: moving from prescription to adherence. Best Pract. Res. Clin. Rheumatol. 28 (1), 93–117. https://doi.org/10.1016/j.berh.2014.01.009 (2014).
Asadzadeh, A., Samad-Soltani, T., Salahzadeh, Z. & Rezaei-Hachesu, P. Effectiveness of virtual reality-based exercise therapy in rehabilitation: A scoping review. Inf. Med. Unlocked. 24, 100562. https://doi.org/10.1016/j.imu.2021.100562 (2021).
Acknowledgements
We are deeply grateful to all participants and their families for their invaluable contributions, which were at the heart of this project. We are profoundly thankful to Marinando Ravenna ODV, Sante Ghirardi, and all the charitable organization’s volunteers for their outstanding professionalism, expertise, and dedication, without which none of this would have been possible. Our sincere appreciation extends to ‘Palazzo Manzoni’, Massimo Bottura, and its staff for creating a warm and supportive environment where participants can reflect on and make sense of their experiences. We are also profoundly thankful to the “Pubblica Assistenza Paolina” of Imola, Dr. Alessandro Di Silverio, and its team, whose presence ensured safety for all participants throughout the intervention. A special thanks to the residents in physical and rehabilitation medicine, and PhD students of the IOR, whose enthusiasm and support during the assessment days were invaluable. We are deeply grateful to the patient associations UNIAMO-FIMR, ACAR Aps, AsItOI, and Aismme Aps for their constant commitment and essential support, particularly for their pivotal role in disseminating the study and recruiting participants, which has made a meaningful difference to the success of this initiative.Several authors are members of the ERN BOND - the European Reference Network for rare BONe Diseases (https://ernbond.eu/). The study was funded by the generous contribution of Catalent Inc. via the King Baudouin Foundation United States (Fund ID: #1050/Grant #8558).
Funding
The study was funded by the contribution of Catalent Inc. via the King Baudouin Foundation United States (Fund ID: #1050/Grant #8558). The funder had no role in the collection, analysis, and interpretation of data; in the writing of the report; and in the decision to submit the paper for publication.
Author information
Authors and Affiliations
Contributions
MB: Conceptualization; Data curation; Formal analysis; Investigation; Methodology; Project administration; Supervision; Validation; Visualization; Writing – original draft; Writing – review & editing. FB: Formal analysis; Methodology; Validation; Writing – review & editing. DS: Data curation; Formal analysis; Methodology; Validation; Visualization; Writing – original draft; Writing – review & editing. GMF: Conceptualization; Data curation; Investigation; Methodology; Validation; Writing – original draft; Writing – review & editing. GR: Data curation; Investigation; Methodology; Validation; Visualization; Writing – original draft; Writing – review & editing. EDS, and GV: Investigation; Methodology; Software; Validation; Writing – review & editing. DP, LB, AL, and SS: Conceptualization; Investigation; Methodology; Writing – review & editing. SF, AS: Conceptualization; Methodology; Writing – review & editing. ML: Investigation; Writing - review & editing. LS: Conceptualization; Funding acquisition; Investigation; Methodology; Resources; Supervision; Validation; Visualization; Writing – original draft; Writing – review & editing. All authors participated in the reading, critical review, and approval of the final manuscript. Multiple authors directly accessed and verified the underlying data reported in the study. All authors had full access to the study data and assumed responsibility for the decision to submit the manuscript for publication. Written informed consent for the publication of identifiable images and/or video recordings of participants was obtained from all adult participants involved in the study. For participants under the age of 18, written informed consent for publication was obtained from their parents/guardians.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical statement and informed consent
The study was approved by the Local Ethical Committee, Comitato Etico Area Vasta Emilia Centro (CE-AVEC), under protocol number: 115/2024/Sper/IOR, and conducted in accordance with the 1964 Declaration of Helsinki. Written informed consent was obtained from all participants aged ≥ 18 years and from parents/guardians of those participants aged < 18 years.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Boarini, M., Banchelli, F., Fittipaldi, S. et al. Feasibility and safety of sailing based rehabilitation for rare skeletal disorders using wearable sensors and patient reported outcomes. Sci Rep 15, 37153 (2025). https://doi.org/10.1038/s41598-025-22231-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-22231-8