Abstract
Obesity concurrent with gestational diabetes mellitus (GDM) markedly increases the risk of adverse pregnancy outcomes, wherein placental dysfunction acts as a key mediating factor, however, the underlying mechanisms involved remain elusive. This pilot study was designed to focus on the role of mitochondria-endoplasmic reticulum contacts (MERCs) in obesity with GDM-induced placental dysfunction. Term placental tissues from pregnant women with obesity and GDM or healthy control were analyzed. Reduced cell count of placental trophoblasts, disorganized cell arrangement, and higher apoptosis rate were observed in placental tissue from women with obesity and GDM. In addition, oxidative stress levels and protein expression levels of endoplasmic reticulum (ER) stress markers phosphorylated inositol-requiring enzyme 1 (pIRE1α) and CCAAT/enhancer-binding protein homologous protein (CHOP) were both markedly upregulated compared to the healthy controls. Of note, proximity ligation assay (PLA) revealed increased formation of MERCs core complexes mitofusin 1 (MFN1)-mitofusin 2 (MFN2) and inositol 1,4,5-trisphosphate receptor type 1 (IP3R1)-glucose-regulated protein 75 (GRP75)-voltage-dependent anion channel 1 (VDAC1) in obesity and GDM group. These findings suggest that obesity comorbid with GDM may induce MERCs restructuring via oxidative stress and ER stress, thereby triggering trophoblast apoptosis and subsequent placental dysfunction. Our study sheds light on the underlying mechanisms driving placental pathology in women with obesity and GDM.
Similar content being viewed by others
Introduction
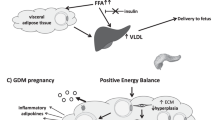
As society progresses and living standards undergo substantial enhancement, obesity has evolved into a critical issue of global health significance. It is estimated that up to 50% of women of reproductive age are overweight or obese, and obesity increases the risk of comorbidities during the perinatal period for both mothers and their offspring1. Compared with women of normal weight, obese women exhibit a three-fold increase in the risk of developing gestational diabetes mellitus (GDM)2. Moreover, obesity with GDM further elevates the risk of adverse offspring outcomes, including macrosomia, neonatal hypoglycemia, and metabolic or organ developmental abnormalities3,4,5. Maternal obesity combined with GDM is typically characterized by hyperglycemia and hyperlipidemia, wherein hyperinsulinemia induced by hyperglycemia and elevated free fatty acids resulting from lipolysis collectively impair placental function6.The placenta is a critical organ for material exchange between the fetus and mother, and aberrations in its function may mediate the occurrence of adverse birth outcomes. It is noteworthy that GDM pregnancies are characterized by a state of chronic low-grade inflammation and endothelial dysfunction, which are recognized as key contributors to placental pathology7,8. Research also demonstrates that maternal obesity and GDM can induce oxidative stress, endoplasmic reticulum (ER) stress, and mitochondrial dysfunction in placental trophoblasts, compromising placental function9,10,11,12.
Recent research has revealed profound structural and functional interplay between the ER and mitochondria, with their contact sites fundamentally regulating cellular homeostasis13.The ER and mitochondria are closely interconnected, and this connection extensively participates in regulating numerous critical physiological processes, including lipid metabolism regulation, calcium homeostasis maintenance, proper mitochondrial functioning, response to ER stress, and orderly execution of autophagy14. Vesicle-associated membrane protein-associated protein-B (VAPB) interacts with protein tyrosine phosphatase-interacting protein−51 (PTPIP51) in the gap between the ER and mitochondrial membranes, exerting a tethering function that facilitates calcium transport into mitochondria. Inositol 1,4,5-trisphosphate receptor (IP3R), voltage-dependent anion channel (VDAC), and glucose-regulated protein 75 (GRP75) collectively form a complex composed of channel proteins and tethering proteins, which mediates the transfer of calcium from the ER to mitochondria. Mitofusin 2 (MFN2) in the ER membrane forms both homotypic and heterotypic interactions with MFN1/2 in the mitochondrial membrane. Sigma−1 receptor interacts with IP3R on the ER membrane side and regulates multiple aspects of mitochondria-endoplasmic reticulum contacts (MERCs) function14,15.Previous study demonstrated that obesity can induce remodeling of mitochondria-associated endoplasmic reticulum membranes (MAMs), leading to calcium overload in hepatic cell mitochondria and impairing their oxidative phosphorylation capacity16. Pyruvate dehydrogenase kinase 4 (PDK4) can mediate obesity-induced increase in skeletal muscle MERCs and the development of insulin resistance17. During the decidualization process of endometrial stromal cells, the contact between mitochondria and ER increases, thereby enhancing the oxidative phosphorylation capacity of decidualized cells18. Currently, although no studies have reported the role of MERCs in placental tissues of pregnant women with obesity combined with gestational diabetes mellitus, since obesity or gestational diabetes can affect the function of the ER and mitochondria in trophoblasts, we hypothesize that MERCs may play a mediating role in placental dysfunction induced by obesity combined with GDM. This pilot study aims to identify potential molecular targets, providing a basis for developing novel drugs and therapeutic measures.
Materials and methods
General information
A total of 12 pregnant women with obesity combined with GDM and 12 healthy pregnant women who underwent regular antenatal examinations and delivered at term in the Obstetrics Medical Center, Weifang People’s Hospital from June 2024 to June 2025 were selected as the pilot study subjects, aged 20–39 years. The inclusion criteria includes: (1) Single-fetus pregnant women; (2) The pregnant woman continued to carry the fetus until full-term delivery (37 weeks of gestation ≤ gestation age<42 weeks of gestation)༛(3) The group with obesity and GDM: The pregnant woman was diagnosed with obesity before pregnancy and with GDM during pregnancy༛(4) Pregnant women and their families signed the informed consent form. (5) The diagnosis of GDM should comply with the diagnostic criteria recommended by the National Diabetes Data Group (NDDG), and the obesity criteria should adhere to the classification standard established by the China Obesity Working Group in 2001 (obesity defined as BMI ≥ 28 kg/m², normal weight as BMI 18.5–23.9 kg/m²). The exclusion criteria includes: (1) Premature birth or post-term birth༛(2) Has received assisted reproductive technology༛(3) Twins or multiple pregnancies༛(4) During pregnancy, there are concurrent conditions such as hepatitis, thyroid disorders, diabetes, and infectious diseases༛(5) Pregnancy complicated with hypertensive disorders, cholestasis syndrome, placenta previa, placental abruption, and others༛This study was approved by the Ethics Committee of our hospital (Weifang People’s Hospital). All participants provided written informed consent. All experiments were performed in accordance with relevant guidelines and regulations.
Collection and processing of specimens
Within 15 min after placental delivery, three pieces of placental tissue (each measuring 2 cm × 1 cm × 1 cm) were collected from the maternal surface at approximately 2 cm from the umbilical cord insertion site. Each piece of tissue was divided into two portions and rinsed with sterile saline. Subsequently, three pieces were fully fixed in 10% formalin, while the remaining three pieces were rapidly frozen in liquid nitrogen for approximately 5 min, then transferred to−80 °C for long-term storage.
Hematoxylin-eosin (H&E) staining
Placental tissues were fixed for 24 h before sampling, followed by routine dehydration, clearing, paraffin impregnation, embedding, and sectioning at a thickness of 5 μm. Sections were sequentially dewaxed in xylene, rehydrated through graded ethanol series, stained in hematoxylin solution(G1125, Solarbio, China) for 10 min, differentiated in acid-alcohol, blued in tap water, counterstained with eosin for 30 s, dehydrated via graded ethanol series, cleared in xylene, and mounted with neutral balsam. Histopathological alterations were then observed under a microscope.
Immumohistochemical staining
After dewaxing the placental tissue sections, the slices were placed in antigen retrieval solution (AR0024, Boster Biological Technology, China) and microwaved at medium power for 8 min. Subsequently, 3% hydrogen peroxide was applied for a 10-minute incubation at room temperature to block endogenous peroxidase activity. The sections were then blocked with 10% normal goat serum (AR0009, Boster Biological Technology) for 30 min, followed by the addition of primary antibody༈CHOP, AF6277, Affinity Biosciences, US; p-IRE1α, AF7150, Affinity Biosciences) and overnight incubation at 4 °C. The next day, the sections were rinsed with PBS༈AR0032, Boster Biological Technology), incubated with secondary antibody at room temperature for 30 min, and rinsed again with PBS. Finally, DAB (AFIHC004, AiFang biological, China) chromogenic reaction was performed, counterstained with hematoxylin (SH8390, Solarbio), dehydrated, cleared, mounted with neutral balsam, and observed under a microscope for positive expression.
Oxidative stress detection
After dewaxing and rehydration of placental tissue sections, dihydroethidium (DHE) (S0064S, Beyotime, China) solution was diluted with PBS at a 1:1000 ratio. The diluted DHE solution was applied and incubated at 37 °C for 1 h under light-protected conditions, followed by PBS rinsing. Sections were then mounted with antifade mounting medium containing DAPI (S2110, Solarbio) and observed under a confocal laser scanning microscope.
Proximity ligation assay (PLA)
After dewaxing and rehydration of placental tissue sections, the slices were placed in antigen retrieval solution and microwaved at medium power for 8 min. Subsequently, 0.5% Triton−100 was applied for a 10-minute incubation at room temperature for permeabilization. Using the PLA kit (DUO92101, Sigma-Aldrich, Germany) blocking, primary antibody incubation, ligation, and amplification were performed. Finally, sections were washed with Tris-NaCl, mounted with antifade mounting medium containing DAPI, and observed under a confocal laser scanning microscope.
TUNEL assay
Tissue sections underwent dewaxing and rehydration, followed by the addition of diluted proteinase K for a 30-minute incubation at 37 °C to achieve permeabilization. After PBS rinsing, the TUNEL reaction mixture (T6013S, Uelandy, China) was applied to the samples and incubated at 37 °C under light-protected conditions for 1 h. The reaction mixture was then discarded, and sections were rinsed with PBS, followed by a wash with 0.1% Triton−100. Finally, sections were mounted with antifade mounting medium containing DAPI and observed under a confocal laser scanning microscope.
Western blotting
Placental tissues were weighed and mixed with RIPA lysis buffer (P0013K, Beyotime) and protease inhibitor cocktail (HY-K0010, MedChemExpress, US) homogenized using a tissue grinder, then lysed on ice for 30 min. After centrifugation at 4 °C and 10,000 × g for 10 min, total proteins were extracted. Protein concentrations were determined using BCA working reagent (AR1189, Boster Biological Technology), followed by protein denaturation, electrophoresis, and membrane transfer. Membranes were blocked for 1.5 h, incubated with primary antibodies against p-IRE1α (AF7150, Affinity Biosciences, 1:2000) and CHOP (AF6277, Affinity Biosciences, 1:2000) at 4 °C overnight, then incubated with secondary antibody (AB_2839429, Affinity Biosciences, 1:3000)) for 1 h. After washing, ECL chemiluminescent substrate (AR1191, Boster Biological Technology) was prepared for signal detection.
Statistical methods
Statistical analysis was performed using GraphPad Prism 10.0 software. Image J software was employed to analyze pathological and immunohistochemical staining results. The normality of the data distribution was confirmed using the Shapiro-Wilk test. Next, Student’s t-test was applied to compare the difference between the control group and the Obesity with GDM group. P < 0.05 was considered statistically significant..
Results
Maternal baseline characteristics
To characterize maternal baseline characteristics, we compared gestational age, maternal age, gravidity, parity, pre-pregnancy weight, and pre-pregnancy BMI between the healthy control group and the obesity with GDM group, respectively. No statistically significant differences were observed in gestational age, maternal age, gravidity, or parity between the two groups. The control group exhibited significantly lower pre-pregnancy weight and BMI compared to the obesity with GDM group (P < 0.001). Data are shown in Table 1.
Placental pathological alterations and cell apoptosis
To investigate the cause of disturbed placental function in the obesity with GDM group, HE staining was performed on placental tissues from both groups. Results showed that placental villi were uniformly sized with abundant syncytiotrophoblasts and cytotrophoblasts in healthy mothers while it exhibited reduced numbers and irregular size in obesity with GDM group, suggesting that hyperglycemia and hyperlipidemia may impact maternal placental tissue (Fig. 1). Consistently, the TUNEL method revealed significantly higher cell apoptosis rates in obesity with GDM group compared to the control group (Fig. 2), suggesting that hyperglycemia and hyperlipidemia may promote cell apoptosis in the placenta.
The pathological changes in the placenta induced by obesity with GDM. Hematoxylin-eosin staining was performed to examine pathological changes in the placenta. Representative images indicate that placental villi exhibited reduced numbers and irregular size in Obesity with GDM group while it was uniformly sized with abundant syncytiotrophoblasts and cytotrophoblasts in healthy mothers. Scale bar, 200 μm.
The assessment of cell apoptosis in the placenta. The TUNEL assay was conducted to evaluate the cell apoptosis rate of syncytiotrophoblasts and cytotrophoblasts. Green dots indicate the presence of apoptotic cells. The quantification data were shown in the bar graph (n = 12). Scale bar, 50 μm. Student’s t-test were used to compare the control group with the Obesity with GDM group. *P<0.05.
Obesity with GDM induces oxidative stress in the placenta
Oxidative stress results from excessive ROS production or insufficient clearance, reflecting an imbalance between oxidation and antioxidant systems. To analyze the oxidative stress level in the obesity with GDM condition, we employed the DHE staining in the current study. Red fluorescence will be observed when superoxide is detected. We found that red fluorescence intensity was increased significantly in the obesity with GDM group compared with healthy control, suggesting obesity with GDM may induce oxidative stress in the placenta (Fig. 3).
Obesity with GDM induces oxidative stress in the placenta. Dihydroethidium (DHE) staining was applied to detect the superoxide level in placental tissues. The red fluorescent intensity was analyzed as the quantification data (n = 12). Scale bar, 50 μm. Student’s t-test were used to compare the control group with the Obesity with GDM group. ***P<0.001.
Obesity with GDM induces ER stress in the placenta
To investigate the effect of ER stress on placental function in obese women with GDM, we detected the expression levels of CHOP and p-IRE1α by western blotting and immunohistochemical staining. Our results showed that the expression levels of CHOP and p-IRE1α were significantly elevated in the obesity with GDM group compared with the control group (Fig. 4). In addition, we observed that CHOP and p-IRE1α were expressed in both syncytiotrophoblasts and cytotrophoblasts in the placenta.
Obesity with GDM induces ER stress in the placenta. (A) The ER stress marker CHOP was detected by Immunohistochemistry in the placenta and the quantitative data was shown (n = 12). (B) The ER stress marker pIRE1α was detected by Immunohistochemistry in the placenta and the quantitative data was shown(n = 12). (C) The CHOP protein level was determined by western blotting and the quantitative data was shown (n = 12). (D) The pIRE1α protein level was determined by western blotting and the quantitative data was shown (n = 12). Ctrl: control group. O + G: Obesity with GDM group. Scale bar, 200 μm. Student’s t-test were used to compare the control group with the Obesity with GDM group. ***P<0.001, ****P<0.0001.
Obesity with GDM increases MERCs in the placenta
Mitochondria and ER interacts closely via several tethering proteins. Here we conducted PLA to detect the protein tethering between IP3R and VDAC, and MFN1 and MFN2, to reflect the MERCs level. Our data indicated that the tethering levels of MFN1 and MFN2 or IP3R1 and VDAC1 in Obesity with GDM condition are both increased significantly, suggesting the elevated level of MERCs (Figs. 5 and 6).
Obesity with GDM increases MERCs in the placenta. Proximity ligation assay (PLA) was performed to detect the MERCs level in the placenta. Green dots indicate the protein tethering of MFN1 with MFN2. The bar graph was the quantification data in Green PLA dots per area (n = 12).Scale bar, 50 μm. Student’s t-test were used to compare the control group with the Obesity with GDM group. *P<0.05, **P<0.01.
Obesity with GDM increases MERCs in the placenta. PLA was performed to detect the MERCs level in the placenta.The green dots indicate the protein tethering of IP3R with VDAC1. The bar graph shows the quantitative data in Green PLA dots per area (n = 12). Scale bar, 50 μm. Student’s t-test were used to compare the control group with the Obesity with GDM group. *P<0.05, **P<0.01.
Discussion
Obesity during pregnancy poses both short-term and long-term health risks to the mother and her offspring, and can cause a series of obstetric complications, including GDM and preeclampsia19,20. It also affects pregnancy outcomes, increasing the risks of preterm birth, stillbirth, fetal malformations, and growth disturbances21,22. GDM is one of the most common metabolic disorders during pregnancy and can similarly cause multiple adverse birth outcomes23. Currently, the mechanisms by which obesity and GDM lead to adverse birth outcomes remain unclear, and aberrant changes in placental function may play a mediating role. In the current study, we observed increased fibrinoid deposits within and around placental villi, elevated calcification and infarction outside villi, and intravillous vascular edema in placental tissues of obese women with GDM. These pathological changes were associated with significantly elevated oxidative stress levels, consistent with previous research findings24,25. This indicates that oxidative stress may be the upstream trigger leading to abnormal placental morphology and function.
Previous studies have demonstrated that obesity and GDM can also induce ER stress in placental trophoblast cells9,26. IRE1α and CHOP are core signaling molecules of ER stress. IRE1α acts as a sensor for ER stress, primarily initiating adaptive responses to restore homeostasis. Under excessive stress, activated IRE1α leads to X-box binding protein−1 (XBP1) splicing and apoptosis signal-regulating kinase 1 (ASK1)-c-Jun N-terminal kinase 1/2 (JNK1/2) signaling pathway, leading to cell apoptosis27. CHOP serves as the apoptosis executor of ER stress, which is induced when stress cannot be alleviated. It regulates the apoptotic protein Bcl−2 and activates the BAX-caspase 3 cascade reaction, ultimately leading to placental cell apoptosis9. Together, they constitute the adaptation-apoptosis molecular switch in ER stress, maintaining cellular homeostasis or eliminating damaged cells28,29. In this study we found the expression levels of pIRE1α and CHOP were significantly elevated in placental tissues from obese women with GDM, as well as increased placental cell apoptosis. This suggests that the hyperglycemic and hyperlipidemic environment may induce ER stress in placental cells via ER stress, ultimately leading to cellular apoptosis.
Mitochondria and the endoplasmic reticulum are two critical organelles within cells. They form close physical connections through MERCs, rather than direct fusion of membrane structures. This contact is non-random and highly dynamic, with its quantity and function altering in response to cellular states such as nutritional levels and stress conditions14,30. Mfn2 is primarily located on the mitochondrial membrane. Mfn1/2 can simultaneously exist on the ER membrane. Mitochondrial Mfn2 binds to ER Mfn1, directly connecting the two organelle membranes, serving as one of the bridge molecules maintaining MERCs structure. IP3R-VDAC-GRP75 complex serves as another bridge between mitochondria and ER, which is essential for activating the mitochondrial respiratory chain and cellular energy supply. It’s abnormalities may cause calcium overload, inducing mitochondrial damage and cellular apoptosis15,31. High glucose induces the expression of p66Shc and its translocation to mitochondria, which promotes the formation of MAMs and stimulates PINK1-PRKN-mediated mitophagy32. During high glucose-induced neuronal amyloidosis, MERCs levels and tissue-type transglutaminase 2 (TGM2) are significantly elevated. Silencing TGM2 suppresses the interaction between IP3R1 and VDAC1, blocking high glucose-induced mitochondrial calcium influx and mitochondrial reactive oxygen species accumulation33. Obesity enhances MERCs levels in hepatic cells and alters the morphology of the ER and mitochondria16. In the current study, we found that the tethering between MFN1 and MFN2 or IP3R1 and VDAC1was increased remarked in obesity with GDM condition compared with the control, revealing that the dysregulated MERCs levels might play a role in the placental dysfunction.
Conclusion
We speculated that hyperglycemic and hyperlipidemic microenvironment in the placenta of obese women with GDM may produce excessive ROS, inducing ER stress and enhanced MERCs levels, and then promoting placental cells. Therefore, we suggest that MERCs might play a mediating role in placental dysfunction induced by obesity with GDM. However, there are several limitations in the current study. This is a pilot study, and the sample size is relatively small, only 12 pregnant women with obesity plus GDM and 12 healthy controls were recruited. One of the significant limitations of our study is the lack of separate analysis on the impact of obesity or GDM alone on placental function. Given that obesity and GDM often coexist in pregnant women, and both have been shown to independently impair placental function, future studies should consider including a group with obesity and a separate group with GDM alone. The placental tissue used in this study primarily comprises decidual tissue and villous tissue, a limitation that prevents it from representing the pathological and physiological profiles of all placental tissue types. The connection among oxidative, ER stress, MERCs, and apoptosis was not revealed and further studies are still needed to further elucidate the underlying regulating relationship.
Data availability
All data generated or analysed during this study are included in this published article.
Abbreviations
- DHE:
-
dihydroethidium
- ER:
-
endoplasmic reticulum
- GDM:
-
gestational diabetes mellitus
- H&E:
-
hematoxylin-eosin
- IP3R1:
-
inositol 1,4,5-trisphosphate receptor type 1
- MAMs:
-
mitochondria-associated endoplasmic reticulum membranes
- MERCs:
-
mitochondria-endoplasmic reticulum contacts
- MFN1/2:
-
mitofusin 1/2
- PDK4:
-
pyruvate dehydrogenase kinase 4
- PLA:
-
proximity ligation assay
- ROS:
-
reactive oxygen species
- VDAC:
-
voltage-dependent anion channel
References
Kanagalingam, M. G., Forouhi, N. G., Greer, I. A. & Sattar, N. Changes in booking body mass index over a decade: retrospective analysis from a Glasgow Maternity Hospital. Bjog 112, 1431–1433. https://doi.org/10.1111/j.1471-0528.2005.00685.x (2005).
Leddy, M. A., Power, M. L. & Schulkin, J. The impact of maternal obesity on maternal and fetal health. Rev. Obstet. Gynecol. 1, 170–178 (2008).
Kc, K., Shakya, S. & Zhang, H. Gestational diabetes mellitus and macrosomia: a literature review. Ann. Nutr. Metab. 66 (Suppl 2), 14–20. https://doi.org/10.1159/000371628 (2015).
Paredes, C., Hsu, R. C., Tong, A. & Johnson, J. R. Obesity and pregnancy. NeoReviews 22, e78–e87. https://doi.org/10.1542/neo.22-2-e78 (2021).
Harrison, R. K., Saravanan, V., Davitt, C., Cruz, M. & Palatnik, A. Antenatal maternal hypoglycemia in women with gestational diabetes mellitus and neonatal outcomes. J. Perinatology: Official J. Calif. Perinat. Association. 42, 1091–1096. https://doi.org/10.1038/s41372-022-01350-4 (2022).
Natarajan, S. K. et al. Saturated free fatty acids induce placental trophoblast lipoapoptosis. PLoS One. 16, e0249907. https://doi.org/10.1371/journal.pone.0249907 (2021).
Cristodoro, M. et al. First trimester placental biomarkers for pregnancy outcomes. Int. J. Mol. Sci. 25 https://doi.org/10.3390/ijms25116136 (2024).
Tossetta, G. et al. HtrA1 in gestational diabetes mellitus: A possible biomarker? Diagnostics (Basel). 12 https://doi.org/10.3390/diagnostics12112705 (2022).
Shen, W. B. et al. Obesity impacts placental function through activation of p-IRE1a-XBP1s signaling. Front. Cell. Dev. Biol. 11, 1023327. https://doi.org/10.3389/fcell.2023.1023327 (2023).
Jantape, T. et al. Maternal obesity alters placental and umbilical cord plasma oxidative Stress, a Cross-Sectional study. Int. J. Mol. Sci. 25 https://doi.org/10.3390/ijms251910866 (2024).
Etchegaray-Armijo, K. et al. Biomarkers of oxidative stress in maternal plasma, umbilical cord and placenta of patients with gestational diabetes: a systematic review and meta-analysis. Free Radic. Biol. Med. 237, 650–665. https://doi.org/10.1016/j.freeradbiomed.2025.06.007 (2025).
Lu, M. & Sferruzzi-Perri A. N. Placental mitochondrial function in response to gestational exposures. Placenta 104, 124–137. https://doi.org/10.1016/j.placenta.2020.11.012 (2021).
Obara, C. J. et al. Motion of VAPB molecules reveals ER-mitochondria contact site subdomains. Nature 626, 169–176. https://doi.org/10.1038/s41586-023-06956-y (2024).
Serangeli, I., Diamanti, T., De Jaco, A. & Miranda, E. Role of mitochondria-endoplasmic reticulum contacts in neurodegenerative, neurodevelopmental and neuropsychiatric conditions. Eur. J. Neurosci. 60, 5040–5068. https://doi.org/10.1111/ejn.16485 (2024).
Mao, H., Chen, W., Chen, L. & Li, L. Potential role of mitochondria-associated Endoplasmic reticulum membrane proteins in diseases. Biochem. Pharmacol. 199, 115011. https://doi.org/10.1016/j.bcp.2022.115011 (2022).
Arruda, A. P. et al. Chronic enrichment of hepatic Endoplasmic reticulum-mitochondria contact leads to mitochondrial dysfunction in obesity. Nat. Med. 20, 1427–1435. https://doi.org/10.1038/nm.3735 (2014).
Thoudam, T. et al. PDK4 augments ER-Mitochondria contact to dampen skeletal muscle insulin signaling during obesity. Diabetes 68, 571–586. https://doi.org/10.2337/db18-0363 (2019).
Dalla Torre, M. et al. Mitochondria remodeling during endometrial stromal cell decidualization. Life Sci. Alliance. 7 https://doi.org/10.26508/lsa.202402627 (2024).
Yogev, Y., Langer, O., Xenakis, E. M. & Rosenn, B. The association between glucose challenge test, obesity and pregnancy outcome in 6390 non-diabetic women. J. Matern Fetal Neonatal Med. 17, 29–34. https://doi.org/10.1080/14767050400028766 (2005).
Mission, J. F., Marshall, N. E. & Caughey, A. B. Obesity in pregnancy: a big problem and getting bigger. Obstet. Gynecol. Surv. 68, 389–399. https://doi.org/10.1097/OGX.0b013e31828738ce (2013).
Syböck, K., Hartmann, B. & Kirchengast, S. Maternal prepregnancy obesity affects foetal Growth, birth Outcome, mode of Delivery, and miscarriage rate in Austrian women. Int. J. Environ. Res. Public Health. 20 https://doi.org/10.3390/ijerph20054139 (2023).
Reed, J., Case, S. & Rijhsinghani, A. Maternal obesity: perinatal implications. SAGE open. Med. 11, 20503121231176128. https://doi.org/10.1177/20503121231176128 (2023).
Ye, W. et al. Gestational diabetes mellitus and adverse pregnancy outcomes: systematic review and meta-analysis. BMJ (Clinical Res. ed.). 377, e067946. https://doi.org/10.1136/bmj-2021-067946 (2022).
Hu, C., Yan, Y., Ji, F. & Zhou, H. Maternal obesity increases oxidative stress in placenta and it is associated with intestinal microbiota. Front. Cell. Infect. Microbiol. 11, 671347. https://doi.org/10.3389/fcimb.2021.671347 (2021).
Hoch, D., Gauster, M., Hauguel-de Mouzon, S. & Desoye, G. Diabesity-associated oxidative and inflammatory stress signalling in the early human placenta. Mol. Aspects Med. 66, 21–30 (2019).
Yung, H. W. et al. Placental Endoplasmic reticulum stress in gestational diabetes: the potential for therapeutic intervention with chemical chaperones and antioxidants. Diabetologia 59, 2240–2250. https://doi.org/10.1007/s00125-016-4040-2 (2016).
Yang, P., Reece, E. A., Wang, F. & Gabbay-Benziv, R. Decoding the oxidative stress hypothesis in diabetic embryopathy through proapoptotic kinase signaling. Am. J. Obstet. Gynecol. 212, 569–579. https://doi.org/10.1016/j.ajog.2014.11.036 (2015).
Sano, R. & Reed, J. C. ER stress-induced cell death mechanisms. Biochim. Biophys. Acta. 1833, 3460–3470. https://doi.org/10.1016/j.bbamcr.2013.06.028 (2013).
Ekundayo, B. E. et al. Oxidative stress, Endoplasmic reticulum stress and apoptosis in the pathology of alzheimer’s disease. Cell Biochem. Biophys. 82, 457–477. https://doi.org/10.1007/s12013-024-01248-2 (2024).
Wang, Y. et al. Endoplasmic Reticulum-Mitochondria contacts: A potential therapy target for cardiovascular Remodeling-Associated diseases. Front. cell. Dev. Biology. 9, 774989. https://doi.org/10.3389/fcell.2021.774989 (2021).
Rowland, A. A. & Voeltz, G. K. Endoplasmic reticulum-mitochondria contacts: function of the junction. Nat. Rev. Mol. Cell. Biol. 13, 607–625. https://doi.org/10.1038/nrm3440 (2012).
Ji, L. et al. High glucose-induced p66Shc mitochondrial translocation regulates autophagy initiation and autophagosome formation in syncytiotrophoblast and extravillous trophoblast. Cell. Communication Signaling: CCS. 22, 234. https://doi.org/10.1186/s12964-024-01621-x (2024).
Lee, H. J. et al. Urolithin A suppresses high glucose-induced neuronal amyloidogenesis by modulating TGM2-dependent ER-mitochondria contacts and calcium homeostasis. Cell Death Differ. 28, 184–202. https://doi.org/10.1038/s41418-020-0593-1 (2021).
Funding
This work was supported by Scientific Research Development Fund of the Affiliated Hospital of Shandong Second Medical University (2024FYM033).
Author information
Authors and Affiliations
Contributions
RW, JL, QL, and XY conducted the experiments. HJ, GW, NL, and YZ conceived the study design. RW analyzed the data. RW, YZ, and GW were major contributors in writing the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Wang, R., Liu, J., Li, Q. et al. Obesity concurrent with gestational diabetes mellitus dysregulates mitochondria-endoplasmic reticulum contacts in human placenta. Sci Rep 16, 1686 (2026). https://doi.org/10.1038/s41598-025-31193-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-31193-w