Abstract
This study aimed to explore the diagnostic value of the two cytology techniques, including liquid-based cytology of mammary ductal lavage fluid and nipple discharge smear cytology, in the intraductal lesions in patients with pathological nipple discharge (PND). This retrospective analysis included 119 patients with PND who underwent surgical treatment. At the same time, they all underwent fiberoptic ductoscopy (FDS), nipple discharge smear cytology and liquid-based cytology of ductal lavage fluid before surgery. With postoperative pathological diagnosis as the gold standard, we compared the clinical diagnostic efficacy of the two cytology techniques applied independently and combined with FDS to evaluate their diagnostic value in intraductal lesions. Finally, the receiver operating characteristic (ROC) curves and the area under the curve (AUC) were used to evaluate the diagnostic value of each examination method. There were 22 breast malignant tumors, 75 intraductal papillomas and 22 non-tumorous lesions among the 119 PND patients. The cell types of liquid-based cytology of ductal lavage fluid was significantly more abundant than that of smear cytology, and the detection rate of tumor cells, atypia cells and atypical hyperplasia cells was significantly increased. The diagnostic accuracy and sensitivity of liquid-based cytology of ductal lavage fluid were significantly higher than that of smear cytology (P < 0.05). At the same time, the accuracy of liquid-based cytology was superior to that of smear cytology when combined with FDS (P < 0.05), and the diagnostic efficiency was excellent. FDS combined with liquid-based cytology of ductal lavage fluid was more effective than the other methods (AUC = 0.8182). When diagnosing the intraductal space-occupying lesions in PND patients, liquid-based cytology of ductal lavage fluid can obtain more abundant intraductal shed cells. This advantage can compensate for the limitation of FDS for diagnosing terminal ductal unit lesions and significantly improve the early diagnosis rate of intraductal lesions, especially intraductal malignant tumors.
Similar content being viewed by others
Introduction
Pathological nipple discharge (PND) usually refers to spontaneous nipple discharge, which occurs in a non-lactation, non-pregnancy period. It can manifest as serous, bloody, and other characteristics. Clinically, PND is the most common clinical manifestation of breast disease except breast pain and lumps1,2. The most common causes of PND mainly include ductal dilatation, intraductal papilloma (IDP), atypical ductal epithelial hyperplasia, etc. IDP is the most common reason. In addition, about 5–10% of patients with PND are diagnosed as breast malignant tumors3. At the same time, IDP also has a certain risk of developing cancer. Therefore, the early clinical screening of intraductal lesions for the patients with PND as the main manifestation is of great clinical significance.
In the past, the most commonly used cytology detection for patients with PND was nipple discharge smear cytology. However, due to the small sample size of nipple discharge, the false negative rate of smear cytology was high. At present, ductoscopy technology has matured and widely used in patients with PND. The ductal lavage fluid in ductoscopy can reach the distal duct and acinar. Collecting the lavage fluid for cytological examination can be a powerful aid and supplement for ductoscopy. It can significantly improve the diagnostic rate of intraductal lesions in PND patients, especially terminal ductal lesions, and is of great value for early diagnosis of intraductal lesions4.
Recent studies have shown that the cell samples in the ductal lavage fluid were fresh and sufficient, which provides a more reliable basis for the accuracy of cytological detection in diagnosing mammary intraductal lesions5,6. However, there are only small samples of clinical comparative data in the literature before, and there is insufficient clinical evidence for the clinical application of ductal lavage fluid in diagnosing intraductal lesions. Therefore, 119 patients with PND were retrospectively included in this study, which is the largest sample size of relevant studies as we have retrevied in the literature. The diagnostic value of smear cytology and liquid-based cytology of ductal lavage fluid in clinical diagnosis of intraductal lesions was evaluated by comparing the two methods with postoperative pathology to improve the early diagnosis rate of PND patients and their prognosis.
Materials and methods
Clinical data
A total of 119 patients with PND who were hospitalized in the Galactophore department of Beijing Hospital of Traditional Chinese Medicine, Capital Medical University, from May 2022 to December 2023, were retrospectively selected, and all of them received surgical treatment.
The inclusion criteria included: (1) female patients with pathological nipple discharge; (2) the patients underwent FDS examination, nipple discharge smear cytology and liquid-based cytology of ductal lavage fluid before surgery and obtained complete examination reports; (3) the patients underwent surgical treatment to remove the lesion mammary duct and obtained a complete pathological report.
The exclusion criteria included: the patients with incomplete clinical information.
Methods
(1) Nipple discharge smear cytology.
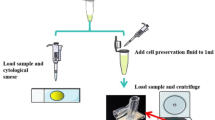
The patient’s affected nipple was cleaned and disinfected before ductscopy examination. Then the clinician gently squeezed the nipple along the direction of the mammary duct to collect the overflow into a sterile EP tube. After mixing the fluid in the tube upside down gently, a few drops were placed onto a clean, dry microscope slide and evenly spread using another slide. Then, the samples were numbered, stained, rinsed, and dried. The cell morphology was observed by HE staining (Leica AutoStainer XL (ST 5010) - Automatic staining machine, Germany). Cytological diagnoses were performed by professional cytopathologists in the pathology department, who subsequently issued a smear cytological examination report.
(2) Fiberoptic ductoscopy examination.
A electronic breast duct endoscope (Model: SZ-DS, Jiangsu Suzhong Pharmaceutical Group Medical Equipment Co., Ltd, China) was used for all FDS examinations. The patients were positioned supine, and the breast on the affected side was disinfected routinely. The root of the nipple was gently squeezed to identify the nipple foramen from which discharge was emanating. A flat lacrimal probe was then precisely inserted into the duct opening on the nipple. Following adequate local anesthesia, the mammary duct was dilated using different size of probes. Subsequently, the ductoscope was carefully inserted after successful duct dilation. During the examination, 0.9% normal saline was infused to flush the duct and maintain a clear view under the ductoscopy. The ductoscope images were captured, and diagnoses were made according to the lesions observed during the examination. After the examination, the professional breast surgeon should diagnose the ductoscope findings and generate an report7.
(3) Liquid-based cytology of ductal lavage fluid.
During ductoscopy examination, the mammary duct was flushed with normal saline, and the lavage fluid was collected into a liquid-based cytological storage bottle. The storage bottle was processed using liquid-based cell preparation equipment, which included HE staining and slide preparation, followed by microscopic examination (The instrument and method were consistent with those mentioned in Nipple discharge smear cytology.). The cytological diagnosis results were obtained by two professional cytopathologists, who then issued the examination report.
Patients were divided into three groups based on postoperative pathological diagnosis: non-tumor lesion group (NTL), intraductal papilloma group (IDP) and breast cancer group (BC). We analyzed the diagnostic accuracy, sensitivity, and specificity of the two cytology tests, both individually and in conjunction with FDS, to comprehensively evaluate their overall clinical diagnostic value.
The International Academy of Cytology Yokohama System for Reporting Breast Fine Needle Aspiration Biopsy Cytopathology was adopted as the cytological diagnostic standard (including insufficient/inadequate, benign, atypical, suspicious of malignancy and malignant). In the statistical analysis, we considered the first two types of pathological diagnosis as negative cytological diagnosis, and the latter three types as positive diagnosis. Specifically, tumor cells, atypic cells and ductal epithelial atypical hyperplasia were diagnosed as positive; other normal cell types such as acellular, ductal epithelial, lymphocytes, neutrophils, and an insufficient number of cells were diagnosed as negative.
Diagnostic efficacy evaluation:
Sensitivity = true positive / (true positive + false negative) × 100%;
Specificity = true negative / (true negative + false positive) × 100%;
Accuracy = (true positive + true negative) / (total cases examined by surgical pathology) × 100%.
Statistical analysis
Microsoft Excel 2019 was used to establish the database, and statistical software SPSS 27.0 was used for statistical analysis. Quantitative data were presente as mean ± standard deviation (Mean ± SD), and the counting data were expressed as frequency (percentage) [n(%)]. The chi-square test was employed to compare the distribution differences between groups with a P value < 0.05 considered statistically significant. Additionally, R software was used to generate the receiver operating characteristic (ROC) curves for intraductal papilloma and intraductal malignancy in the clinical diagnosis of PND patients. This analysis included a comparison of their areas under the curve (AUC) to thoroughly assess their clinical diagnostic utility.
Results
The age of the 119 female patients with PND ranged from 26 to 75 years, with the duration of symptoms varying from seven days to over ten years. Both the age and duration of symptoms in the IDP and BC groups were significantly higher than those in the NTL group (P < 0.05). Additionally, the BC group exhibited significantly older ages and longer symptom durations compared to the IDP group (P < 0.05). In the patients, 34 experienced bilateral nipple discharge, while 85 had discharge from one breast only. Moreover, when it comes to the number of duct opening with nipple discharge, 107 patients was unitary opening and just 12 patients was multiple. There was no significant statistical difference among the three groups (P > 0.05) (Table 1; Fig. 1).
Comparison of age (A), course of disease (B) among the three groups.
Postoperative histopathological results of the patients
The final postoperative histopathological examination results showed that among 119 patients with PND, 22 cases (18.49%) were non-tumor lesions (including duct epithelial hyperplasia in 12 cases, breast adenosis in 6 cases, duct dilatation in 3 cases, and papillary adenoma in 1 case), 75 cases (63.03%) were intraductal papilloma and 22 cases (18.49%) were breast malignancies (including 17 ductal carcinoma in situ and five invasive carcinoma) (Table 2).
Comparison of nipple discharge characteristics and histopathological results
When comparing the characteristics of nipple discharge among the three groups, the predominant types of discharge were serous and bloody. In NTL group, the discharge was mostly watery or serous. Serous discharge was most common in patients with IDP, followed by bloody discharge. Conversely, patients with breast malignant tumors predominantly presented with bloody discharge, although serous or watery discharges were also observed. The discharge characteristics in IDP and BC groups were significantly different from those in NTL group (P < 0.05 for both comparisons) (Table 3).
Comparison of cell abundance between two cytological examinations
In the non-tumour lesion group, the cytological findings were mainly epithelial cells, with occasional neutrophils, foam cells, and red blood cells. In the intraductal papilloma group, smear cytology primarily revealed epithelial cells and lymphocytes. In contrast, liquid-based cytology of ductal lavage fluid manifested a broader array of cells, including epithelial cells, histiocytes, lymphocytes, foam cells and other cells. Despite detecting a wider variety of cell types, liquid-based cytology did not demonstrate significant diagnostic specificity. Finally, for the breast cancer group, the microscopic observation of smear cytology was still dominated by duct epithelial cells and histiocytes, and the detection rate of tumour cells was low. However, the liquid-based cytology of ductal lavage fluid results showed a significant increase in the detection rate of atypical proliferative epithelial cells, atypical cells and tumor cells. This enhanced detection is crucial for the early diagnosis of intraductal malignant tumors, underscoring the diagnostic value of liquid-based cytology in identifying malignancies at an early stage (Table 4; Fig. 2) .
Microscope images of smear cytology and liquid-based cytology (HE staining, 200X).
Comparison of diagnostic accuracy of two cytological examinations
For intraductal papilloma patients, the diagnostic accuracy of smear cytology was 41.33%, while liquid-based cytology of ductal lavage fluid achieved a higher accuracy rate of 58.67% (P < 0.05). In the diagnosis of intraductal malignant tumors, the accuracy of smear cytology was only 22.73%, significantly lower than the 68.18% accuracy achieved with liquid-based cytology of ductal lavage fluid (P < 0.05). These results indicate that liquid-based cytology of ductal lavage fluid offers superior diagnostic accuracy to the smear cytology when assessing space-occupying lesions in the duct. Moreover, the enhanced detection rate of tumour cells in liquid-based cytology of ductal lavage fluid is particularly advantageous for the clinical diagnosis of intraductal malignant tumours (Table 5).
Comparison of the diagnostic efficiency of two cytological methods: independent diagnosis or combined with FDS diagnosis
FDS is an important method for the diagnosis of PND patients. It can visually observe the morphology of different types of intraductal lesions (Fig. 3). After comparing the clinical diagnostic efficacy of intraductal lesions, we found that the accuracy and sensitivity of liquid-based cytology of ductal lavage fluid were higher than that of smear cytology when applied independently for intraductal lesions (P < 0.05). However, there was no significant difference in diagnostic specificity between the two tests (P > 0.05) (Table 6). When both cytology tests combined with FDS, there was a significant improvement in accuracy, sensitivity, and specificity for diagnosing intraductal lesions. Moreover, the diagnostic accuracy of FDS combined with liquid-based cytology of ductal lavage fluid significantly surpassed that of FDS combined with smear cytology (P < 0.05) (Table 7; Fig. 4).
FDS images of patients in three groups.
Comparison of clinical diagnostic efficacy of each test method.
Additionally, we plotted the Receiver Operating Characteristic (ROC) curves to determine the area under the curve (AUC) values for each test in diagnosing intraductal lesions. The results indicated that FDS combined with liquid-based cytology of ductal lavage fluid was more effective than the other three methods (AUC = 0.8182) when diagnosing intraductal papilloma and intraductal malignant tumors of patients with PND. (Fig. 5)
The receiver operating characteristic curves of each examination method (Figure a shows the diagnosis of intraductal papilloma. Figure b shows the diagnosis of intraductal malignancy.) (A, smear cytology; B,liquid-based cytology; C, FDS + smear cytology; D, FDS + liquid-based cytology).
Discussion
This study revealed that the onset age of PND patients ranged from 26 to 75 years, with an average age of about 47. The distribution of onset ages was irregular. Additionally, the wide range in the duration of symptoms, from 7 days to 10 years, is attributed to the occult nature of intraductal lesions. Most patients with PND have difficulty with timely self-examination, potentially leading to the long-term accumulation of secretions in the breast ducts, particularly in the terminal ducts, which brings significant challenges for clinical diagnosis. According to the histopathological results, the most common PND patients included in this study were intraductal papilloma (63.03%), followed by breast cancer and non-tumor lesion, both accounting for 18.49%. These findings align with prior literature1. Regarding the characteristics of nipple discharge, bloody discharge was the most common in breast malignant tumor and intraductal papilloma patient. A retrospective study found that patients with bloody discharge had a 9% risk of breast cancer, significantly higher than that of the non-bloody discharge group (2%)8. In addition, the probability of mammary malignant tumor diagnosis by nipple discharge smear cytology is 37.5%9. Patients with bloody or clear discharge are more likely to develop breast cancer, while this risk does not increase with age10. Since 85% of PND patients showed no significant abnormalities on radiological evaluation, making it challenging to diagnose based on clinical presentation and imaging alone. Due to the diagnosis rate of malignant tumors in patients with PND is low, and clinical manifestations generally lack specificity. Therefore, it is urgent for clinicians to improve the early diagnosis rate of this disease. As a common clinical manifestation of breast diseases, nipple discharge is of great significance and value for early diagnosis and screening of intraductal lesions. At present, there are many specific detection methods for pathological nipple discharge1, including mammography, magnetic resonance imaging, mammary duct angiography, tumor markers of nipple discharge, etc. However, these methods often face limitations in balancing sensitivity and specificity, which restricts their clinical application. Currently, FDS is the preferred examination method for patients with PND. Due to the advantages of convenient operation, minimal trauma, and direct vision in the duct, FDS has become a major diagnostic and adjuvant treatment tool for intraductal lesions of the breast7. According to literature reports, the diagnostic sensitivity, accuracy and negative predictive value of ductoscopy for PND patients are higher than ultrasound11, and it has excellent sensitivity and specificity for detecting intraductal malignant tumors12. Previous network meta-analysis of clinical diagnostic methods for PND patients showed that ductoscopy had the highest diagnostic accuracy (88%), followed by cytology (82%) and MRI (77%)1. Despite its strengths, ductoscopy does have limitations, particularly in the diagnosis of terminal duct lobular units (TDLUs) lesions in the breast. In this case, liquid-based cytology of ductal lavage fluid offers additional diagnostic potential, facilitating the early detection of intraductal lesions in patients with PND.
Cytological examination of nipple discharge is a simple, non-invasive, relatively economical and practical method which has been highly accepted by patients and can complement other diagnostic techniques such as ductoscopy. It provides valuable cytological information for the diagnosis of potential intraductal lesions, especially intraductal malignant tumors13. Previous research has pointed out that the shed cells and secretions in the mammary duct provide abundant cell types and biomarkers that may help clinical assessment of the short-term breast cancer risk and the benefit of early intervention14. At present, this kind of cytology tests mainly includes routine smear cytology and liquid-based cytology of ductal lavage fluid. Smear cytology can be qualitatively diagnosed by directly observing the shed cells visible in the discharge, which can clearly detect tumor cells, thus clarifying the nature of intraductal lesions and guiding subsequent treatment. However, the biggest bottleneck in clinical application is the generally low detection rate8. The overall positive rate of cytological examination of nipple discharge has been about 50%, and the low detection rate is the main reason restricts its broader clinical use15. At the same time, the variability in nipple discharge characteristics among patients with PND and the intricate structure of mammary ducts, clinical sample acquisition is limited, resulting in a high false-positive rate and false-negative rate during smear cytology.
Liquid-based cytology technology was developed in the 1990s, and its application in cervical cancer was first reported by Hutchinson in 199116. Then it widely used in cervical cytology detectionto significantly improve the detection rate of cervical cancer17. Liquid-based cytology is one of the best techniques for examining shed cells currently, which can enhancing the detection rates of malignant tumors through lavage fluid examinations and observations. In recent years, the liquid-based cytology technique has been used for the cytological detection of intraductal shed cells. Sakakibara reported that liquid-based cytology could improve the detection rate of early breast lesions, its diagnostic sensitivity and specificity for mammary malignant tumors are superior to a conventional cytological smear18. Yamamoto highlighted its clinical utility, both positive and negative predictive values of 89.7%, a sensitivity of 50%, and a specificity of 94.3%, thus supporting its wider clinical application19.
In this study, when comparing the cell abundance of the two cytological examinations, it was observed that the variety and number of cells detected in the liquid-based cytology were significantly greater than that in the conventional smear cytology. Similarly, reports suggest that the number of cells in mammary ductal lavage fluid is 100 times greater than in nipple discharge20. In addition, the lavage fluid can comprehensively collect the shed cells in all level of ducts, thus greatly reducing the false negative rate of diagnosis. Beyond the increased cell count, ductal lavage fluid also collects a more diverse range of cell types, including ductal epithelial cells, atypical hyperplasia cells, atypia cells and tumor cells, whereas smear cytology primarily consists of lymphocytes and histiocytes. This discrepancy may be due to the small sample of cytological fluid in conventional smears, which limits the number of cells. Therefore, liquid-based cytology of ductal lavage fluid has obvious advantages over conventional smear cytology in diagnosing intraductal papilloma and breast malignancy. It can significantly improve the detection rate of positive cells and greatly reduce the rate of missed diagnoses. In diagnosing non-tumor lesions of the breast, neither method showed significant advantages.
Comprehensive analysis indicated that the accuracy of liquid-based cytology was higher than that of conventional smear cytology, and the sensitivity was significantly increased. This improvement effectively compensates for the limitation of the difficulty in diagnosing the terminal duct lobular unit lesions by ductoscopy. When compared the two cytology test methods combined with FDS, we found that FDS combined with liquid-based cytology can significantly improve the diagnostic accuracy, sensitivity, and specificity of intraductal lesions, it has high application value in clinical diagnosis. A prospective study demonstrated that the results of ductoscopy, liquid-based cytology of ductal lavage fluid and imaging are complementary, which can enhancing the guidance provided for clinical diagnosis21. In addition, a meta-analysis of the literature has shown that the traditional examination of shed cells is relatively limited in the early diagnosis and differential diagnosis of intraductal disease with a less sensitive2,22. In this case, duct perfusion increases cellshedding within the duct, thereby increasing the sensitivity of cytological detection and reducing heterogeneity. Moreover, ductal lavage fluid is always performed in combination with ductoscopy or mammography23, with the ductoscopy or a contrast agent is directly inserted into the discharge duct. Consequently, we could obtained a sufficient number of cell samples. All of these studies showed significant advantages of liquid-based cytology compared with smear cytology, and they were in deep agreement with our findings. Therefore, it can be asserted that there are abundant cells in the duct lavage fluid samples for cytological examination and diagnosis, and repeated tests can be conducted to verify the diagnosis so that the diagnostic accuracy is significantly improved24,25.
To sum up, for the early diagnosis of intraductal lesions in patients with PND, liquid-based cytology has a significant advantage when compared with conventional smear cytology. Particularly noteworthy is the combined application of ductoscopy with liquid-based cytology for diagnosing intraductal malignant tumors, which demonstrates excellent clinical diagnostic value and and can be widely applied. In addition, in view of the correlation between the abnormal cytological examination of duct lavage fluid and the increased risk of breast cancer26, the local cell and secretions of the ductal system obtained by duct lavage fluid can be considered as the microenvironment for tumor development27,28. Therefore, the analysis of possible biomarkers in ductal lavage fluid has significant clinical significance for evaluating asymptomatic and high-risk patients, and it represents a promising area for future research in breast cancer screening.
However, there are still some limitations in this study. First, in this study, we paid more attention to the diagnostic value of cytology and its combination with ductoscopy in the diagnosis of intraductal space occupying lesions, especially intraductal malignancies. The diagnostic value of cytological examination in the non-space occupying lesions of the catheter can be further explored. In addition, our study was a single-center retrospective study with a relatively limited sample size, especially the number of cases of intraductal malignancies. Finally, our study has limitations in the statistical analysis of clinical features of PND patients. For example, regarding the classification of nipple discharge traits, the literature also mentions sero-sanginous and other types. We hope to refine it in follow-up studies.
Conclusion
In summary, for patients with PND, more and fresher mammary ductal cells can be obtained by collecting the diseased duct lavage fluid through ductoscopic lavage. The positive diagnosis rate of intraductal lesions, especially intraductal malignant tumors, can be significantly improved by using liquid-based cytology to prepare and analyze these samples. Liquid-based cytology technique offers higher sensitivity and specificity compared to conventional smear cytology. It can capture a greater number and variety of exfoliated cells within the duct. This technique provides significant clinical value in diagnosing intraductal lesions in PND patients. Additionally, ductoscopy combined with liquid-based cytology can significantly reduce the false positive rate of ductoscopy alone. This combination compensates for the limitation of ductoscopy in reaching terminal duct lobular units and significantly improve the accuracy of clinical diagnosis of intraductal lesions in PND patients.
Data availability
The data that support the findings of this study are available from the corresponding author on reasonable request. The data are not publicly available due to privacy or ethical restrictions.
References
Filipe, M. D. et al. Network Meta-analysis for the Diagnostic Approach to Pathologic Nipple Discharge. Clin. Breast Cancer. 20 (6), e723–e748. https://doi.org/10.1016/j.clbc.2020.05.015 (2020).
Jiwa, N. et al. Diagnostic accuracy of Nipple Discharge Fluid Cytology: a Meta-analysis and systematic review of the literature. Ann. Surg. Oncol. 29 (3), 1774–1786. https://doi.org/10.1245/s10434-021-11070-2 (2022).
Vavolizza, R. D. & Dengel, L. T. Management of Nipple Discharge. Surg Clin North Am. 102(6), 1077–1087https://doi.org/10.1016/j.suc.2022.06.006 (2022).
Bahl, M. et al. Evaluation of pathologic nipple discharge: what is the added diagnostic value of MRI? Ann. Surg. Oncol. 22 (Suppl 3), S435–S441. https://doi.org/10.1245/s10434-015-4792-9 (2015).
Li, Z. et al. Application value of fiberoptic ductoscopy in the treatment of pathologic nipple discharge[J]. China Med. Herald. 19 (04), 99–102 (2022).
Lili Wang, H. et al. Pathological comparative analysis of liquid-based cytology of mammary ductoscopy lavage fluid and exfoliative cytology[J]. China Practical Med. 16(12), 208–210 (2021).
Zhang, D. et al. Expert consensus on the clinical diagnosis and treatment of ductoscopy (2022) [J]. China Medical Herald. 20(11), 4–8. https://doi.org/10.20047/j.issn1673-7210.2023.11.01 (2023).
Dolan, R. T., Butler, J. S., Kell, M. R., Gorey, T. F. & Stokes, M. A. Nipple discharge and the efficacy of duct cytology in evaluating breast cancer risk. Surgeon 8 (5), 252–258. https://doi.org/10.1016/j.surge.2010.03.005 (2010).
Al Nemer, A. & Kussaibi, H. The accuracy of nipple discharge cytology in detecting breast cancer. Diagnosis (Berl). 8(2), 269–273. https://doi.org/10.1515/dx-2020-0026 (2020).
Montroni, I. et al. Nipple discharge: is its significance as a risk factor for breast cancer fully understood? Observational study including 915 consecutive patients who underwent selective duct excision. Breast Cancer Res. Treat. 123 (3), 895–900. https://doi.org/10.1007/s10549-010-0815-1 (2010).
Hongjv, Y. et al. Diagnostic value of ultrasound and fiberoptic ductoscopy in patients with pathological nipple discharge[J]. Chin. J. Med. Ultrasound(Electronic Edition). 18 (08), 800–805 (2021).
Liu, G. Y. et al. Fiberoptic ductoscopy combined with cytology testing in the patients of spontaneous nipple discharge. Breast Cancer Res. Treat. 108, 271–277. https://doi.org/10.1007/s10549-007-9598-4 (2008).
Wang, B. et al. A Nomogram to predict the probability of breast intraductal tumors in patients with nipple discharge: a real-world study based on our 13-Year clinical experience. Cancer Manag Res. 12, 11191–11201. https://doi.org/10.2147/CMAR.S273728 (2020).
Masood, S. Development of a novel approach for breast cancer prediction and early detection using minimally invasive procedures and molecular analysis: how cytomorphology became a breast cancer risk predictor. Breast J. 2015 Jan-Feb. 21(1), 82–96. https://doi.org/10.1111/tbj.12362.
Wang, H. X. et al. Diagnosis of breast intraductaltumor by fiberoptic ductoscopy [J]. Modem Oncol. 22 (4), 847–850 (2014).
Hutchinson, M. L., Cassin, C. M. & Ball, H. G. 3rd The efficacy of an automated preparation device for cervical cytology. Am J Clin Pathol. 96(3), 300–305. https://doi.org/10.1093/ajcp/96.3.300 (1991).
Wenjie Lian, X. Screening effect of positive liquid based cytology tests on cervical lesions[J]. Chronic Pathematology J. 24 (01), 65–67. https://doi.org/10.16440/J.CNKI (2023).
Sakakibara, E. et al. An aspiration materialpreparation system; application of a new liquid-based cytologytechnique for fine-needle aspiration of the breast. Acta Cytol. 55 (1), 92–99 (2011).
Yamamoto, D., Senzaki, H. & Nakagawa, H. Detection of chromosomal aneusomy by fluorescence in situ hybridization for patients with nipple discharge[J]. Cancer. 97(3), 690–694 (2003).
Shen, K. W. et al. Fiberoptic ductoscopy for breastcancer patients with nipple discharge[J]. Surg. Endose. 15 (11), 1340–1345 (2001).
Sauter, E. R., Klein-Szanto, A., Macgibbon, B. & Ehya, H. Nipple aspirate fluid and ductoscopy to detect breast cancer. Diagn. Cytopathol. 38 (4), 244–251. https://doi.org/10.1002/dc.21177 (2010).
Li, X. Q., Xu, F., Lei, C. Q., Li, J. & Jiang, H. C. Accuracy for cytological evaluation in the detection of breast cancer among patients with pathologic nipple discharge: a PRISMA-compliant meta-analysis. Chin. Med. J. (Engl). 133 (4), 435–443. https://doi.org/10.1097/CM9.0000000000000643 (2020).
Denewer, A., El-Etribi, K., Nada, N. & El-Metwally, M. The role and limitations of mammary ductoscope in management of pathologic nipple discharge. Breast J. 14, 442–449. https://doi.org/10.1111/j.1524-4741.2008.00620.x (2008).
Jiwa, N. et al. Diagnostic accuracy of Nipple Aspirate Fluid Cytology in Asymptomatic patients: a Meta-analysis and systematic review of the literature. Ann. Surg. Oncol. 28 (7), 3751–3760. https://doi.org/10.1245/s10434-020-09313-9 (2021).
Mannello, F. New horizon for breast cancer biomarker discoveries: what might the liquid biopsy of nipple aspirate fluid hold? Proteonomics Clin. Appl 11, 9–10 (2017).
Shaheed, S. U. et al. Nipple aspirate fluid-A liquid biopsy for diagnosing breast health. Proteom. Clin. Appl. 11 (9–10), 1700015. https://doi.org/10.1002/prca.201700015 (2017).
Hornberger, J., Chen, S. C., Li, Q., Kakad, P. & Quay, S. C. Proliferative epithelial disease identified in nipple aspirate fluid and risk of developing breast cancer: a systematic review. Curr. Med. Res. Opin. 31 (2), 253–262 (2015).
Jiwa, N. et al. Nipple aspirate fluid and its use for the early detection of breast cancer. Ann. Med. Surg. (Lond). 77, 103625. https://doi.org/10.1016/j.amsu.2022.103625 (2022).
Funding
This study was supported by a Special Project on Traditional Chinese Medicine (TCM) heritage of ancient books, literature, and distinctive techniques (GZY-KJS-2022-035), Young doctor scholar project (2022), Capital research and transformation of clinical diagnosis and treatment technology (Z211100002921020), Research project on education and teaching reform at Capital Medical University (2023JYY326).
Author information
Authors and Affiliations
Contributions
Y.Z. and D.Z. wrote the main manuscript text. J.L. and N.F. carried out data organization. Y.Z. and Y.G. provided clinical information. M.L. and H.Z. provided guidance on cytopathology for this study. N.F. and J.C. revised and embellished the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Statement of Ethics
This study has been reviewed by the Ethics Committee of Beijing Hospital of Traditional Chinese Medicine, Capital Medical University (No: 2023BL02-112-01). We have confirmed that all methods were carried out in accordance with relevant guidelines and regulations and all experimental protocols were approved by the Ethics Committee. The informed consents have been obtained from all subjects and/or their legal guardian(s).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zeng, Y., Li, J., Zhang, D. et al. The diagnostic value of cytology in the mammary intraductal lesions of patients with pathological nipple discharge. Sci Rep 15, 3243 (2025). https://doi.org/10.1038/s41598-025-86533-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-86533-7