Abstract
We aimed at investigating the impact of coronavirus disease 2019 (COVID-19) on the time required to complete a 1000-m run and vital capacity (VC) among healthy male students at three universities in Wuhan, China, followed for four years covering the prepandemic (2019), early/late pandemic (2020/2021), and post-pandemic (2022) periods. Demographic information including age, body height/weight, and body mass index (BMI) were also collected. After dividing the participants into four groups based on BMI (i.e., underweight: BMI < 18.5; normal: 18.5 ≤ BMI < 25; overweight: 25 ≤ BMI < 30; obese: BMI ≥ 30), the associations of 1000-m run performance with changes in BMI and VC between different groups and within each group in different periods were analyzed. A 4-year follow-up on 10,037 participants demonstrated a progressive deterioration of 1000-m performance (p < 0.001) except the obese group. All participants showed a drop in VC in the post-pandemic period (all p < 0.001) compatible with their impaired 1000-m run performance. The underweight/normal BMI groups also exhibited an annual increase in BMI (all p < 0.001). Impairment in 1000-m performance was most conspicuous during the early pandemic period and as the pandemic subsided. Our findings showed deterioration in physical endurance and VC among university students during the pandemic, highlighting the need for cardiopulmonary exercise reinforcement during a pandemic.
Similar content being viewed by others
Introduction
The coronavirus disease 2019 (COVID-19) pandemic was a global public health issue that imposed a long-lasting negative impact on the physical, cognitive, and mental health domains following the initial infection1. It is noteworthy that not only did the pandemic take a heavy mental and physical toll on those infected2, but it also had indirect acute effects on uninfected individuals3,4. Nevertheless, only a few reports focused on the objective measurements of physical performance of those who were not infected5,6,7,8.
A prior study reported particular vulnerability to impaired physical fitness among those who received high-intensity training before the lockdown5. In contrast, another investigation reported that elite athletes showed more favorable levels of physical activity during the COVID-19 pandemic than their fellow non-athletes9. Therefore, the impact of lockdown-associated inactivity on physical performance remained controversial. In respect of the overall influence of lockdown during the pandemic on a large population, a previous study on primary school children demonstrated impairment in physical fitness as well as an increase in the obese and underweight populations after the pandemic6. Reduced physical activities were also reported among university students during the pandemic10. In the early stages of the pandemic, implementation of online physical training programs was found to be beneficial to university students’ physical health7,8. A pairwise comparison of the physical fitness of university students between 2019 and 2021 in one study7 as well as between 2019 and 2020 in another8 both reported a significant increase in vital capacity among their participants. However, the lockdown policy that only allowed home-based exercises appeared to contradict such a finding. More importantly, changes in their physical performance after the pandemic lockdown remained unclear.
Through comparing the changes in performance of 1000-m run and pulmonary vital capacity among male students from three universities at ground zero (i.e., Wuhan) before, during, and after the pandemic, the current study aimed at investigating its differential impacts on the physical endurance of this population at various stages. The fluctuations in body mass index, which may affect physical performance11, were also analyzed.
Materials and methods
Study protocol and subjects
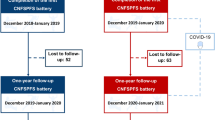
The present retrospective cohort study was based on data from the annual physical fitness assessment program, China, which is a mandatory national policy for all university students. It is a 1-day event including the gathering of baseline demographic information, body mass index (BMI), and the evaluation of athletic capacity. Only those diagnosed with physical disabilities were exempted from the program. To ensure an uninterrupted follow-up on changes in physical status, data on demography, 1000-m run performance, pulmonary vital capacity, and BMI of first-year male university students from three universities in Wuhan, China, namely Wuhan Textile University, Huazhong University of Science and Technology, and Huazhong Agricultural University registered in the year 2019 were collected annually for 4 years to cover the prepandemic (2019), early and late pandemic (2020 and 2021, respectively), and post-pandemic (2022) periods. To avoid the confounding environmental factors, the event is held in October every year. Therefore, the annual assessment was not affected by the COVID-19 lockdown period of the city, which was from January 23 to April 8, 2020.
The inclusion criteria were first-year male university students enrolled in one of the three universities in 2019 whose data were available over four consecutive years. Individuals (1) aged under 18 at the time of enrollment, (2) who were diagnosed with COVID-19 anytime within the study period, (3) had a history of acute (e.g., stroke, myocardial infarction) or chronic (e.g., diabetes mellitus, malignancy) medical conditions, or (4) failed to provide 4 years of complete data for reasons other than above (e.g., dropout) were excluded. The protocol of the study was reviewed and approved by the Institutional Review Board (IRB) of Tongji Hospital, Tongji Medical College, Huazhong University of Science and Technology (IRB no. [2023] IEC (S172), approval date: November 29, 2023), which waived informed consents from the study subjects due to the retrospective observational nature of the present investigation. All procedures were performed in accordance with relevant guidelines and regulations.
Definitions
To elucidate the correlation between BMI and physical performance, all subjects were divided into four groups according to their BMI (Underweight: BMI < 18.5; Normal: 18.5 ≤ BMI < 25; Overweight: 25 ≤ BMI < 30; Obese: BMI ≥ 30)12 according to their baseline data acquired in 2019. Once an individual was assigned to a BMI group, he stayed in the same group throughout the whole study to enable a pairwise comparison of their changes in BMI, 1000-m run performance, and vital capacity between different years.
Procedures
The annual assessment program is conducted in university gymnasia. Outdoor physical performance (e.g., 1000-m run) is evaluated on university soccer fields. Body height and body weight were electronically measured with the subject standing barefoot and erect on a device (Catalog code: CSTF-ST, Tongfang Health Technology Co., Ltd., Beijing, China), while the time taken to complete a 1000-m run was precisely measured with another electronic instrument (Catalog code: CSTF-ZC, Tongfang Health Technology Co., Ltd., Beijing, China). Measurement of the vital capacity of the lungs was conducted with a spirometer (Catalog code: CSTF-FH, Tongfang Health Technology Co., Ltd., Beijing, China) in accordance with the procedure previously described13. The same measurement devices were used nationwide to ensure comparability of the findings. All participants of a 1000-m run used a standing start. Mask-wearing was not required during exercises.
Statistical analysis
We used descriptive statistics for the baseline characteristics (i.e., year 2019) of the participants and checked the normality of data distribution with the Kolmogorov-Smirnov test. Average values of non-normally distributed data are expressed as medians and interquartile ranges (IQR). To elucidate the causes of the changes in 1000-m run performance during the pandemic, Kendall rank correlation coefficient was used to assess the significance of correlations of the time required to complete a 1000-m run with the physical characteristics of the participants, namely body height, body weight, BMI, and vital capacity based on the prepandemic data (i.e., year 2019). For non-normally distributed data, Kruskal-Wallis one-way analysis of variance (ANOVA) was adopted to appraise the significance of overall annual difference between the four BMI groups before the conduction of Dunn’s multiple pairwise comparisons. Moreover, we used Friedman’s two-way analysis of variance test to assess the variation of a BMI group in the 4-year time course. A finding of a significant difference was subjected to further scrutiny through the conduction of Dunn’s multiple comparison tests. Adjustments of the significance values for multiple tests were performed using Bonferroni correction to minimize Type I error (α) probability14. We used SPSS 25 for Mac (IBM Corp., Armonk, NY, USA) for all statistical analyses. A probability value (p) less than 0.05 was considered statistically significant.
Results
Demographic characteristics of participants
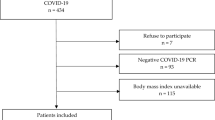
Of the 12,052 male university students initially recruited, 2015 were excluded due to different reasons (Fig. 1), resulting in a total of 10,037 eligible participants for the current study. Their median age at the time of university admission (i.e., year 2019) was 19.0 (IQR: 18.0–19.0) (Table 1). The majority of subjects had a normal BMI (69.4%). The participants in the four BMI groups showed no significant difference in age. In respect of body height, the overweight group was significantly taller than the normal BMI group, while the obese group was taller than the other three groups. The variation in body weight was consistent with that of BMI with significant differences noted between the four groups. The distribution of BMI of all the participants is shown in Fig. 2.
Flow diagram of participant enrollment.
Distribution of body mass index among male university students at baseline (N = 10037, year 2019).
Correlations of 1000-m run performance with demographic characteristics
The time to complete a 1000-m run demonstrated a weak but significant negative correlation with the body height of the participants (Fig. 3A), while it was positively associated with their body weight (Fig. 3B) and BMI (Fig. 3C) (all p < 0.001). Besides, the finishing time weakly but negatively correlated with their vital capacity (Fig. 3D) (p < 0.001). Kendall rank correlation coefficient analysis further revealed weak but significant positive correlations of vital capacity with body height (r = 0.264), body weight (r = 0.285), and BMI (r = 0.187) (all p < 0.001).
Correlations of the time for a 1000 m run with (A) body height, (B) body weight, (C) body mass index, and (D) vital capacity among 10,037 male university students in prepandemic period (i.e., year 2019). Significance determined by Kendall rank correlation coefficient.
Performance of 1000-m run
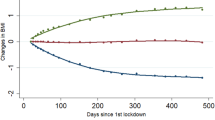
Following the initial outbreak of the pandemic in 2020, the underweight, normal BMI, and overweight groups demonstrated a significant increase in the time required to complete a 1000-m run (all p < 0.001) except the obese group that showed no notable change (Fig. 4A). On entering the late phase of the pandemic in 2021, only the normal BMI group exhibited a significant impairment in performance (p = 0.029), while no remarkable difference was noted in the other three groups compared to their status during the early pandemic periods (i.e., 2020). Nevertheless, the performance of all groups in the late pandemic period (i.e., 2021) was significantly worse than that in the prepandemic period (i.e., 2019). Interestingly, further substantial plummeting of performance was noted in the underweight, normal BMI, and overweight groups when the pandemic subsided in 2022 (all p < 0.001) compared with their performance in the late pandemic phase (i.e., 2021), while the obese group showed no significant difference between the two periods. Overall, compared with the prepandemic stage (i.e., 2019), the underweight, normal BMI, and overweight groups demonstrated a highly significant deterioration as the pandemic subsided. On the other hand, the performance of the obese group after the pandemic was comparable to their prepandemic status.
(A) Performance of 1000 m run in male university students (n = 10037) categorized into four groups based on body mass index (BMI) before (2019), during (early: 2020; late: 2021), and after (2022) the COVID-19 pandemic; (B) comparison of 1000 m run performance between the four BMI groups during each period; (C) changes in pulmonary vital capacity in male university students categorized into four groups based on body mass index (BMI) before, during, and after the COVID-19 pandemic; (D) comparison of vital capacity between the four BMI groups in each period; (E) Changes in body mass index (BMI) of male university students categorized into four groups according to BMI before, during, and after the COVID-19 pandemic; (F) comparison of BMI between the four BMI groups during each period. *p < 0.05, **p < 0.001 based on Dunn’s multiple comparison test. Underweight: body mass index (BMI) < 18.5; normal: 18.5 ≤ BMI < 25; overweight: 25 ≤ BMI < 30; obese: BMI ≥ 30.
Regarding the performance of the four groups at each time point, the time to complete a 1000-m run was similar between the underweight and normal BMI groups throughout the 4-year period (Fig. 4B). On the other hand, the performance was negatively associated with the BMI of the participants in the years 2019, 2020, and 2021 (all p < 0.001). After the pandemic (i.e., 2022), the performance became comparable between the overweight and obese groups.
Changes in vital capacity during the pandemic
Regardless of their BMI, all participants showed a unanimous substantial drop in vital capacity after the pandemic (i.e., 2022) compared with that in the prepandemic (i.e., 2019) phase (all p < 0.001) (Fig. 4C). Moreover, all four BMI groups exhibited a notable drop when the pandemic shifted from the late (i.e., 2021) to the post-pandemic (i.e., 2022) phase (p < 0.001). On the other hand, the pattern of decrease was slightly different between the four BMI groups. Among those who were underweight or overweight, the initial decrease after the pandemic outbreak (p = 0.008) was followed by no significant change in the late phase of the pandemic until it subsided when a more remarkable reduction was noted (p < 0.001). In contrast, the normal BMI group demonstrated a significant increase in vital capacity as the pandemic shifted from the early (i.e., 2020) to late (i.e., 2021) phase before the substantial drop as the pandemic subsided (both p < 0.001). The obese group was unique in that it showed no significant change in vital capacity until the pandemic subsided when a drastic plummeting occurred compared with its performance at other stages of the pandemic (all p < 0.001).
Focusing on the differences in vital capacity between the four groups at various stages of the pandemic (Fig. 4D), our results showed a consistent positive correlation of vital capacity with BMI of the participants (all p < 0.001) with the exception of a lack of difference in vital capacity between the overweight and obese groups in all phases of the pandemic.
Body mass index at different stages of the pandemic
The underweight and normal BMI groups showed highly significant annual increases in BMI during the 4-year period (both p < 0.001) (Fig. 4E). On the other hand, the overweight and obese groups both exhibited a non-significant increase in BMI during the initial pandemic outbreak but demonstrated a significant reduction after the pandemic subsided.
The four groups maintained an overall significant distinction between each other at different stages of the pandemic despite their progressive widening in BMI distribution (Fig. 4F). Nevertheless, the difference in BMI between the overweight and obese groups became non-significant following relief of the pandemic.
Discussion
Main findings and significance
To our best knowledge, the present study was the first large-scale investigation into the effects of different stages of the COVID-19 pandemic on the physical endurance of university students at ground zero by following their performance for four successive years. The results revealed an overall progressive deterioration in 1000-m run performance, a reduction in vital capacity, and an increase in BMI in the majority of participants. Besides, our novel findings included the identification of two time periods in which impairments of 1000-m performance and vital capacity were most notable, namely the early phase after the pandemic outbreak and the recovery phase when the pandemic subsided.
Although previous studies focused on the cardiopulmonary function of individuals who recovered from COVID-1915,16,17, it was soon realized that the pandemic is a global public health issue that also affected those who were not infected2,3. The lockdown measure and the policy of social distancing imposed on the general population are known to negatively affect both their mental and physical health10, which have been found to be interrelated regardless of age18,19,20. The findings highlighted the importance of physical fitness maintenance during such a critical period. Prior investigations have shown that online physical training courses may have a positive impact on the exercise performance of university students during the lockdown period7,8. To address this issue, the current study first identified the significant factors including BMI and pulmonary vital capacity that influenced the time required to finish a 1000-m run, followed by the elucidation of the effects of these factors on long run performance in four BMI groups during a 4-year period. Our results underscored the need for reinforcing cardiopulmonary exercise tolerance among university students not only following the lockdown measure but also after the lockdown was lifted.
Comparison with other studies
The global lockdown and social distancing policy triggered by the COVID-19 pandemic posed an unprecedented threat to both the mental and physical health of the world population1,3. Our findings were comparable to those of prior investigations from different countries that reported an increase in BMI associated with the COVID-19 pandemic probably attributable to increased sedentary behavior, low physical activity, as well as high psychological distress and daily emotional eating21,22,23,24,25. On the other hand, our results of an overall reduction in vital capacity during and after the pandemic were inconsistent with those of previous large-scale studies focusing on the early stages of the pandemic that showed an increase in vital capacity among university students after the lockdown measure7,8. The discrepancy in findings may be attributed to a longer duration of follow-up in the current study than that in previous investigations7,8.
Interpretation and policy implication
Notwithstanding the reported negative influences of the pandemic on physical health, prior studies have shown a positive impact of implementing online physical exercise programs on the maintenance of physical flexibility (e.g., sit-and-reach), muscle strength (e.g., 50-m sprint, pull-up), and explosiveness (e.g., standing long jump)7,8. The national online physical education program implemented by the Ministry of Education, China26, included a weekly 90-min course with an emphasis being placed on aerobic exercises, stretching, and muscle strength training in a domestic setting. Nevertheless, the merits of such home-based programs appeared to have limited benefits regarding physical performance in outdoor exercises such as long runs7,8. Accordingly, our results demonstrated impaired physical endurance as the pandemic proceeded, which was reflected by an increased time required to complete a 1000-m run, in most participants except for the obese group whose performance was comparable to their prepandemic level. Taking into account the results of our correlation study that revealed a negative effect of BMI and a positive impact of vital capacity on 1000-m run performance, the impairment in physical endurance in the majority of participants may be at least partly explained by the progressive increase in BMI coupled with a decrease in vital capacity as the pandemic progressed. Following the same line of argument, a notable reduction in BMI in the obese group after the pandemic subsided may contribute to their ability to maintain a prepandemic status of physical performance. Such an apparently paradoxical drop in BMI may be attributed to a self-awareness of being overweight as previously reported among adolescents27, although the exact causes remain to be investigated.
Regarding the clinical implications of our findings, the prepandemic data showed worst 1000-m run performance in the obese group compared with the others, while the obese and overweight groups exhibited significantly higher vital capacities than the other two groups. The findings suggested that BMI outweighed vital capacity as a negative impact on 1000-m performance in obese individuals. This may also explain the improved performance of the obese group as the pandemic subsided when they experienced a notable reduction in BMI, despite a concomitant decrease in vital capacity that may be detrimental to their performance. Our finding of a positive correlation between body height and vital capacity (Table 1) has long been reported28. Besides body height, a large-scale study aiming at providing a normal reference range for forced vital capacity based on data acquired from more than 25 thousand younger men in China indicated a highly significant correlation between geographical factors and vital capacity29, showing a lack of universally applicable range of vital capacity for defining healthy individuals. Therefore, in spite of the significant drop in vital capacity at the end of the pandemic, it was likely a subclinical condition. Likewise, although we showed statistically significant changes in 1000-m run performance in our participants, the clinical significance of those changes remain unclear because of a lack of consensus on the acceptable performance of a healthy individual in this particular sport.
In addition to elucidating the overall influence of the pandemic on the physical endurance of university students, the current study attempted to pinpoint the specific periods during which the impairment occurred. Our results revealed that two periods, namely the period just after pandemic outbreak (i.e., from 2019 to 2020) and that from the late stage of the pandemic to the time when it subsided (i.e., from 2021 to 2022), were associated with significant impairment in both physical endurance and vital capacity in the majority of participants. Although the initial deterioration in physical performance may be attributed to the unexpected outbreak and the lockdown measures, the subsequent impairment as the pandemic subsided appeared paradoxical and may be partly attributed to a resumption of unhealthy lifestyles30.
Our ANOVA and Dunn’s multiple pairwise comparison (Fig. 3D) as well as Kendall rank correlation coefficient all showed a positive association between vital capacity and BMI among the participants, which was supported by the result of a previous study that focused on medical students13. Nevertheless, our results demonstrated an overall decrease in vital capacity at the end of the pandemic despite the annual increases in BMI among the underweight and normal BMI groups after the pandemic outbreak. One explanation may be our finding of a positive correlation between vital capacity and body height taking into account the fact that individuals in the overweight and obese groups were significantly taller than those in the other groups in the present study. The other possibility may be that the increase in BMI was insufficient to achieve significant elevations in vital capacity, which was further hampered by a lack of cardiopulmonary exercise in a domestic setting. Overall, the results of the current study highlighted the need for enhancing cardiopulmonary exercise capacity among university students during and following the lockdown period of a pandemic, considering the potential three-fold increase in the probability of encountering extreme epidemics in the coming decades31.
Strengths and limitations
Despite being the first large-scale study focusing on the changes in physical endurance of healthy male university students over four consecutive years covering different stages of the COVID-19 pandemic at ground zero (i.e., Wuhan) that was the earliest city in the world to implement the lockdown measure to enable a maximal study period for comparison, the current investigation had its limitations. First, because healthy behaviors and willingness to participate in physical activities depend on multiple factors including socioeconomic as well as physical and mental health status32,33, variations in these factors may introduce heterogeneity that obscured the significance of our findings. Second, the size of the obese group was relatively small, although the population still showed consistent findings. Third, data on changes in lifestyles after the pandemic were unavailable to pinpoint the causes of the subsequent decline in physical endurance and vital capacity. Fourth, as discussed above, the clinical significance of our finding of a statistically significant reduction in vital capacity and 1000-m run performance in most of our participants warrants further elucidation. Finally, to avoid heterogeneity of our study population, we only targeted healthy individuals who could provide uninterrupted data for 4 years without recruiting those infected with COVID-19 due to their variations in disease onset (i.e., year of their university study) and severity (i.e., minor symptoms vs. life-threatening conditions) as well as sequelae (i.e., complete recovery vs. life-long functional impairment) that not only would introduce heterogeneity into our findings but also preclude an accurate subgroup analysis.
Conclusion
The current retrospective analysis of 4-year data acquired from male university students covering different stages of the pandemic at ground zero showed an overall plummeting of physical endurance and vital capacity in combination with a progressive increase in BMI in most recruited subjects. The deterioration in physical endurance was most notable during the initial outbreak and after the pandemic subsided, underscoring the importance of reinforcing cardiopulmonary physical training during and after the lockdown period. It is noteworthy that pandemic-related inactivity or sedentary behavior caused by lockdown or social distancing policies, rather than the pandemic alone, may have led to our results.
Data availability
All data are available on reasonable request made to the corresponding authors (YL or CKS).
References
The Lancet Respiratory & Long, M. Confronting a growing public health crisis. Lancet Respir. Med. 11, 663. https://doi.org/10.1016/s2213-2600(23)00268-0 (2023).
Evans, R. A. et al. Physical, cognitive, and mental health impacts of COVID-19 after hospitalisation (PHOSP-COVID): A UK multicentre, prospective cohort study. Lancet Respir. Med. 9, 1275–1287 (2021).
Mansfield, K. E. et al. Indirect acute effects of the COVID-19 pandemic on physical and mental health in the UK: A population-based study. Lancet Digit. Health. 3, e217–e230 (2021).
Taheri, M. et al. Effects of home confinement on physical activity, nutrition, and sleep quality during the COVID-19 outbreak in amateur and elite athletes. Front. Nutr. 10, 1143340 (2023).
Zieschang, T. et al. The impact of pandemic-related social distancing regulations on exercise performance—Objective data and training recommendations to mitigate losses in physical fitness. Front. Public. Health. 11, 1099392 (2023).
Yip, K. et al. Physical fitness and body mass index status of Hong Kong primary schoolchildren across the COVID-19 pandemic, before and after school closure. J. Pediatr. 264, 113729 (2024).
Sun, J. et al. Comparative research on the development of college students’ physical fitness based on online physical education during the COVID-19 pandemic. BMC Public. Health. 23, 742 (2023).
Xia, W. et al. The physical fitness level of college students before and after web-based physical education during the COVID-19 pandemic. Front. Pead. 9, 726712 (2021).
Shokri, F., Taheri, M., Irandoust, K. & Mirmoezzi, M. Effects of the COVID-19 pandemic on physical activity, mood status, and eating patterns of Iranian elite athletes and non-athletes. Zahedan J. Res. Med. Sci. 24, 1–7 (2022).
Zhang, B. et al. Changes in health behaviors and conditions during COVID-19 pandemic strict campus lockdown among Chinese university students. Front. Psychol. 13, 1022966 (2022).
Chen, G., Chen, J., Liu, J., Hu, Y. & Liu, Y. Relationship between body mass index and physical fitness of children and adolescents in Xinjiang, China: A cross-sectional study. BMC Public. Health. 22, 1680 (2022).
Lindeman, K. et al. Physical activity changes from before to during the first wave of the COVID-19 pandemic among community-dwelling older adults in Finland. J. Aging Phys. Act. 1, 1–9 (2023).
Song, L. et al. Body mass index is associated with blood pressure and vital capacity in medical students. Lipids Health Dis. 22, 174 (2023).
Bland, J. M. & Altman, D. G. Multiple significance tests: The bonferroni method. Bmj 310, 170 (1995).
O’Sullivan, O. et al. Cardiopulmonary, functional, cognitive and mental health outcomes post-COVID-19, across the range of severity of acute illness, in a physically active, working-age population. Sports Med.-Open. 9, 7 (2023).
Chamley, R. R. et al. Exercise capacity following SARS-CoV-2 infection is related to changes in cardiovascular and lung function in military personnel. Int. J. Cardiol. 395, 131594 (2024).
Singh, I. & Joseph, P. Vol. 61 (Eur Respiratory Soc, 2023).
Veliz, P. & Mutumba, M. Assessing the role of sports participation on depression, suicide ideation, and suicide behaviors among adolescents before and during COVID-19. J. Phys. Activity Health. 1, 1–12 (2023).
Seiffer, B. et al. The association of changes in leisure-time physical activity on depressive symptoms during Covid-19 in German adults: A longitudinal study. Psychol. Sport Exerc. 70, 102562 (2024).
Zhang, Y., Wen, Z., Li, J., Shi, Y. & Meng, S. The influences of dormitory exercise on negative emotions among quarantined Chinese college students during the COVID-19 pandemic. Front. Psychiatry. 14, 1243670 (2023).
Arjmand, E. J. et al. Changes in body mass index and their associations with psychological distress, worries, and emotional eating during the COVID-19 pandemic: A Norwegian cohort study. Nutrients 15, 3834 (2023).
Ayhan Başer, D. et al. The effects of the COVID-19 pandemic on sedentary life in young adults: A cross-sectional study. Int. J. Environ. Health Res. 34, 2544–2555 (2024).
Ochi, S. et al. Impact of the COVID-19 pandemic on exercise habits and overweight status in Japan: A nation-wide panel survey. PLOS Global Public. Health. 3, e0002653 (2023).
Zaccardi, F. et al. The impact of COVID-19 lockdowns on the body mass index of people living with obesity: A UK retrospective cohort study using the UK clinical practice research datalink. Obes. Res. Clin. Pract. 17, 468–476 (2023).
Zaccagni, L. et al. Assessing the impact of COVID-19 prevention measures on adolescent growth in Italy. Healthcare 11, 2101 (2023).
Ministry of Education of the People’s Republic of China. Guidance on Online Teaching for Higher Education in Response to the Novel Coronavirus Pneumonia Epidemic. (2020). http://www.moe.gov.cn/srcsite/A08/s7056/202002/t20200205_418138.html
Lee, M. S. & Lee, H. A. Comparison of changes in health behavior, obesity, and mental health of Korean adolescents before and during the COVID-19 pandemic: Online cross-sectional study. Psychiatry Invest. 20, 1086 (2023).
Vital Capacity. Family Practice Notebook. February (2025). https://fpnotebook.com/Lung/Lab/VtlCpcty.htm (Accessed 5.
Ge, M. et al. Normal reference value of forced vital capacity of Chinese younger men and geographical factors. J. Chin. Clin. Med. 4, 1–5 (2009).
Tavolacci, M. P. et al. The impact of COVID-19 lockdown on health behaviors among students of a French university. Int. J. Environ. Res. Public Health. 18, 4346 (2021).
Marani, M., Katul, G. G., Pan, W. K. & Parolari, A. J. Intensity and frequency of extreme novel epidemics. Proceed. Natl. Acad. Sci.. 118, e2105482118 (2021).
O’Connor, S. & Bélanger-Gravel, A. & team, i. S. Social determinants of long-term reported changes in physical activity and healthy eating during the COVID-19 pandemic in Canada: Multiple cross-sectional surveys analysis from the iCARE study. Appl. Physiol. Nutr. Metab. 49, 179–189 (2023).
Adzrago, D., Sulley, S., Ormiston, C. K. & Williams, F. Socioeconomic and clinical risk factors associated with moderate intensity physical activity before and during the COVID-19 pandemic. Prev. Med. Rep. 37, 102555 (2024).
Funding
This work was funded by grants from the Fundamental Research Funds for the Central Universities (HUST: 2023WKYXQN003).
Author information
Authors and Affiliations
Contributions
L.Z. and C.L. equally contributed as first authors to this work and C.-K.S. and Y.L. who jointly supervised the current study, contributed equally as corresponding authors to this work. Conceptualization, L.Z., and Y.L.; methodology, C.L.; software, Y.L.; validation, H.F. and J.H.; formal analysis, Y.L.; investigation, C.L.; resources, C.L.; data curation, C.L.; writing—original draft preparation, C.-K.S. and L.Z.; writing—review and editing, C.-K.S. and L.Z.; visualization, C.-K.S.; supervision, L.Z. and H.F.; project administration, C.L. All authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zhang, L., Fu, H., Liu, C. et al. Effect of lockdown during COVID-19 pandemic on physical endurance among healthy male university students in Wuhan: a retrospective cohort study. Sci Rep 15, 8397 (2025). https://doi.org/10.1038/s41598-025-92534-3
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-92534-3