Abstract
Interleukin-17 receptor A (IL17RA) is a critical mediator of pro-inflammatory cytokine signaling and a key immune checkpoint in autoimmune diseases. While monoclonal antibodies targeting IL17RA have demonstrated clinical efficacy, their high costs, complexity in production, and lack of oral bioavailability present significant limitations. In response to these challenges, we developed AL-8(0), a novel peptide specifically designed to inhibit the IL17A-IL17RA signaling pathway. AL-8(0) was synthesized with high purity and systematically evaluated for its binding affinity and anti-inflammatory activity. Biophysical and cellular assays confirmed the peptide’s strong affinity for IL17RA and its ability to inhibit inflammatory cytokine production in IL17RA-expressing monocyte-macrophages and keratinocytes. Moreover, its anti-inflammatory effects were com-parable to IL17RA-targeting monoclonal antibodies and were dependent on IL17RA expression, as demonstrated by experiments using IL17RA-deficient cells. These results underscore AL-8(0)’s potential as a targeted therapeutic for autoimmune diseases, offering a peptide-based alternative with lower antigenicity, improved scalability, and potential for oral administration. This study lays the groundwork for further development of AL-8(0) and similar peptides as innovative treatments for inflammatory disorders driven by the IL17A-IL17RA pathway.
Similar content being viewed by others
Introduction
Interleukin-17 (IL17) is the first identified member of the IL17 cytokine family, which comprises six subunits: IL17A to IL17F. These subunits play essential roles in immune system function and are produced by a variety of immune cell types1,2. IL17 is secreted by adaptive immune cells, such as helper T 17 (Th17) cells and CD8 + T cells, as well as innate immune cells, including γδ T cells, natural killer T (NKT) cells, and innate lymphoid cells. The diverse cellular sources of IL17 highlight its pivotal role in immune responses, particularly in bridging innate and adaptive immunity, underscoring its biological importance3.
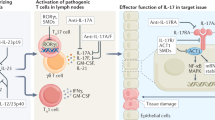
The IL17 receptor is a dimeric structure composed of two of the five subunits: IL17RA, IL17RB, IL17RC, IL17RD, and IL17RE. Each subunit contains a SEFIR domain in its cytoplasmic region, which is critical for initiating signal transduction4,5. IL17A, a homodimer, binds specifically to a heterodimeric receptor formed by IL17RA and IL17RC, triggering downstream signaling pathways. Upon receptor binding, the IL17A-IL17RA pathway activates IL17RA-expressing cells to produce a variety of pro-inflammatory mediators, including cytokines (e.g., IL1β, IL6, TNFα), chemokines (e.g., CXCL1, CXCL8/IL8, CXCL5, CCL20), matrix metalloproteinases (MMPs), and antimicrobial proteins (AMPs)6,7. These mediators act as chemotactic agents, recruiting immune cells such as neutrophils, lymphocytes, and monocytes to sites of inflammation or infection. The IL17 receptor complex plays a pivotal role in IL17A-mediated signaling, driving robust pro-inflammatory responses, immune cell recruitment, and contributing to inflammatory regulation and host defense mechanisms8,9.
The IL17-IL17R signaling pathway initiates signal transduction by recruiting Act1 via the SEFIR domain of the IL17 receptor. Act1, an E3 ubiquitin ligase, facilitates the ubiquitination of TRAF6, thereby activating the NF-κB and MAPK signaling pathways and promoting the transcription of inflammation-related genes. Additionally, this cascade activates transcription factors such as C/EBPβ and C/EBPδ, driving the expression of specific target genes. Beyond transcriptional regulation, the IL17 signaling pathway employs post-transcriptional mechanisms mediated by RNA-binding proteins like Regnase-1/ZC3H12A, which modulate the stability and expression of IL17 target gene mRNAs10,11,12. This dual regulation not only controls the production of inflammatory mediators but also influences keratinocyte proliferation, a key pathological feature in autoimmune diseases such as rheumatoid arthritis and psoriasis. Overall, the IL17-IL17R signaling pathway integrates transcriptional and post-transcriptional regulatory mechanisms, playing a central role in inflammatory responses and keratinocyte regulation. Its involvement in these processes highlights its critical role in the pathogenesis of various autoimmune diseases13,14.
IL17 plays a pivotal role in the pathogenesis of various autoimmune diseases. Dysregulated Th17 cells and elevated IL17 levels stimulate IL17RA-expressing cells to secrete high levels of pro-inflammatory cytokines (e.g., IL1β, TNFα, IL6) and chemokines (e.g., IL8, CXCL1, CCL20), triggering localized inflammation and driving lesion formation15,16. The chronic IL17A-mediated response is a key factor in the development of autoimmune diseases such as psoriasis and rheumatoid arthritis. Clinically validated blockade therapies targeting IL17 have demonstrated significant efficacy with minimal side effects17,18. Since 2016, three neutralizing antibodies have received clinical approval: Secukinumab and Ixekizumab, which inhibit IL17A, and Brodalumab, which targets IL17RA. These therapies effectively reduce inflammation in conditions like psoriasis and rheumatoid arthritis, improving patient outcomes and offering precise, targeted treatments. In summary, IL17 dysregulation is a critical driver of autoimmune disease pathogenesis, and neutralizing antibodies against IL17 or its receptor provide a highly effective therapeutic approach for managing these conditions19,20.
Although IL17-blocking antibody therapies have shown remarkable efficacy in treating autoimmune diseases, they have limitations and cannot meet al.l clinical needs. Immunogenicity remains a significant challenge, as some patients develop anti-drug antibodies (ADAs), leading to reduced therapeutic efficacy. Long-term studies show that Secukinumab has a low ADA incidence rate (< 1%), while Ixekizumab exhibits variable immunogenicity, with some patients experiencing a marked decline in efficacy. Brodalumab’s ADA incidence ranges from 1.8 to 11%, further illustrating the complexity of this issue21,22,23. Additionally, IL17 blockade therapies are not universally effective, with a notable proportion of patients failing to respond, resulting in suboptimal outcomes. While biologics are generally safe, they can cause mild adverse effects, including an increased susceptibility to infections, particularly Candida infections. These challenges underscore that, despite significant advances in treating inflammatory and autoimmune diseases, issues such as immunogenicity, non-responsiveness, and mild adverse effects persist. Therefore, developing improved therapies or alternative treatment strategies is essential to address unmet clinical needs and optimize disease management24,25,26,27.
Developing oral drugs targeting the IL17 pathway is a significant advancement, offering a more convenient therapeutic option compared to injectable biologics. Oral medications provide key advantages such as ease of use, painlessness, and lower production costs, making them more accessible to a broader patient population28,29. In addition, small molecule antagonists have the potential to reduce side effects more effectively than biologics, while being cost-efficient and easily scalable for production. These features make them a promising alternative for treating autoimmune diseases30,31. Numerous studies have identified small molecule compounds targeting the IL17 pathway, demonstrating promising pharmacological potential and forming a foundation for the development of novel oral drugs. However, despite encouraging preclinical findings, none of these compounds have advanced to clinical trials32,33. Overall, oral small molecule antagonists targeting the IL17 pathway represent a highly promising research direction, offering affordable, user-friendly, and potentially safer therapeutic options. Nonetheless, further research and clinical validation are essential to fully realize their potential, particularly in terms of efficacy and safety, which require more in-depth investigation34,35.
Developing novel ligands targeting the IL17A-IL17RA signaling pathway represents a promising strategy for advancing small-molecule therapies to treat autoimmune diseases. Given the pivotal role of the IL17A-IL17RA pathway in the pathogenesis of autoimmune disorders, it is a key target for drug development. Research on ligands targeting this pathway could enable the creation of efficient and convenient small-molecule treatments for conditions such as psoriasis and rheumatoid arthritis. In this study, we designed a novel peptide, AL-8(0), capable of binding to IL17RA and blocking the IL17A-IL17RA signaling pathway. Monocyte-derived macrophages, fibroblasts and keratinocytes were selected as model systems to evaluate ligand efficacy, as these cell types are integral to early-stage drug discovery and pharmacodynamic studies for autoimmune diseases.
This study aims to identify novel immunopharmacological ligands targeting the pro-inflammatory IL17A-IL17RA signaling pathway to develop innovative therapeutic solutions for inflammatory diseases. To achieve this, a combination of biophysical and cellular assays was employed to systematically identify and evaluate the efficacy of potential ligands. By integrating these methodologies, the study seeks to advance drug development for autoimmune diseases such as psoriasis and rheumatoid arthritis, with the goal of achieving new therapeutic breakthroughs.
Methods
Synthesis and detection of AL-8(0)
Peptides were synthesized using the Focus XC system (AAPPTec, USA) via solid-phase synthesis. During coupling, 1-hydroxybenzotriazole (HOBt) and N, N′-diisopropylcarbodiimide (DIC) were used as coupling agents, while piperidine (PIP) served as the deprotection agent. Following synthesis, peptides were cleaved using 90% trifluoroacetic acid (TFA) and precipitated with ether to yield the crude product. The crude peptides were then purified by HPLC, with purity and molecular weight confirmed using HPLC and ESI-MS, respectively. Additionally, the FITC-AL-8(0) peptide was prepared by coupling Fluorescein Isothiocyanate (FITC) to AL-8(0) through the Acp active group. The resulting product was purified and analyzed using the same processes.
Cell culture
The HaCaT human keratinocyte cell line, NIH3T3 murine fibroblast cell line, THP-1 human monocyte macrophage cell line and RAW264.7 murine monocyte macrophage cell line were purchased from the Cell Bank of the Chinese Academy of Sciences (Shanghai, China). HaCaT and NIH3T3 cells were cultured in DMEM medium (Gibco, USA) supplemented with 100 µg/ml streptomycin, 50 µg/ml penicillin, 2200 µg/ml NaHCO3, and 10% (v/v) fetal bovine serum (FBS) (Gibco, USA). THP-1 and RAW264.7 cells were cultured in RPMI1640 medium (containing 0.05 mM β-mercaptoethanol) (Gibco, USA) with the same supplements. All cells were maintained in a humidified incubator at 37 °C with 5% CO2.
Induction THP-1 and RAW264.7 cells to M1 macrophages
THP-1 cells were differentiated into M1 macrophages by incubating them in medium supplemented with 100 ng/ml phorbol 12-myristate 13-acetate (PMA) (MedChemExpress, USA) for 120 h, followed by replacement with fresh medium containing 1 µg/ml lipopolysaccharide (LPS) and 20 ng/ml IFNγ (MedChemExpress, USA) for an additional 24 h. RAW264.7 cells were polarized into M1 macrophages by incubating them in medium supplemented with 1 µg/ml LPS and 20 ng/ml IFNγ for 24 h. The THP-1 and RAW264.7 cells used in the subsequent experiments were all M1 macrophages36.
Generation of IL17RA-deficient cells
IL17RA-deficient cells (1 × 10⁶ cells/ml) were generated using small interfering RNA (siRNA) transfection. The cells were seeded in 12-well plates at 40% density the day before transfection, and the medium was replaced with 800 µl Opti-MEM (Gibco, USA) 4 hours prior to transfection. For each well, 200 µl Opti-MEM (Invitrogen, USA) was mixed with 2 µl Lipofectamine™ 2000 (Invitrogen, USA) and 5 µl siRNA, which was designed and synthesized by Invitrogen according to the manufacturer’s instructions. The transfection mixture was incubated at room temperature for 20 minutes before being added to the cells. Six hours after transfection, the medium was replaced with fresh medium, and cells were harvested 48 hours post-transfection for analysis. The siRNA sequences were as follows: IL17RA: sense 5’-CCUA CGUU GUUU GCUA CUU-3’ and antisense 5’-AAGU AGCA AACA ACGU AGG-3’. Control siRNA was purchased from GenePharma (Shanghai, China).
Real-time qPCR
Total RNA was extracted using Trizol (Invitrogen, USA) and reverse-transcribed into cDNA with the PrimeScript RT reagent kit (Invitrogen, USA), following the manufacturer’s protocol. The mRNA expression levels of target genes were quantified using SYBR Green Master Mix (Takara Biotechnology, Japan) on a QuantStudio® Flex Real-Time PCR System (Life Technologies, Singapore). The primer sequences used were as follows: IL17RA: Forward 5’- CCAT CAGC GAGC TAAT GTCA-3’ and Reverse 5’- AATG GCGA TGAG TGTG ATGA-3’.
Peptide binding and functional assay
Human IL17RA protein was purchased from KactusBio (Waltham, USA), along with biotin-labeled proteins for assay use. Microscale thermophoresis (MST) experiments were conducted using the Monolith NT.115 system (NanoTemper, Germany)37,38. Enzyme-linked immunosorbent assays (ELISA) were performed following standard sandwich, indirect, and competitive ELISA protocols37,38. Color changes in each well were measured at 450 nm using a Multiskan plate reader (Thermo Scientific, USA). Surface plasmon resonance (SPR) assays were performed on a Biacore T200 system (Cytiva, USA), with data analyzed using Biacore Evaluation Software.
Flow cytometry analysis
Flow cytometry was used to evaluate the binding of AL-8(0) to IL17RA-expressing and IL17RA-deficient cells. Briefly, cells were detached using 0.25% trypsin (Gibco, USA) and adjusted to a concentration of 3 × 10⁶ cells/ml. A 100 µl aliquot of the cell suspension was incubated with either FITC-AL-8(0) or FITC-IL17RA mAb (BioLegend, W15177A/S19010F, USA) for 1 h in a humidified environment (5% CO₂, 37 °C, in the dark). Following two washes with PBS, the cells were analyzed using a CytoFLEX flow cytometer (Beckman Coulter, USA). Data were processed using FlowJo 10.0 software.
Immunofluorescence analysis
For immunofluorescence analysis, cells (1 × 10⁵ cells/ml) were incubated with 5 µM FITC-AL-8(0) at 37 °C for 1 h, followed by washing with PBS. The cells were then incubated with Dil plasma membrane stain (Invitrogen, USA) for 20 min at 4 °C. After three additional washes with PBS, the cells were fixed with 4% paraformaldehyde (PFA). Finally, the cells were mounted using mounting medium (DAKO, CA) and observed under an IX53 fluorescence microscope (OLYMPUS, Japan).
Cytotoxicity analysis
IL17RA-expressing and IL17RA-deficient cells(1 × 10⁴ cells/ml) were separately seeded into 96-well plates. AL-8(0) was added to the culture medium at different concentrations (100 µl/well). After 24 h, 10 µl of Cell Counting Kit-8 reagent (Beyotime, Shanghai, China) was added to each well and incubated for 4 h. Absorbance was measured at 450 nm using a Multiskan plate reader (Thermo Scientific, USA).
In vitro anti-inflammatory analysis
IL17RA-expressing and IL17RA-deficient cells were seeded at a density of 1 × 10⁵ cells/well in 6-well plates. After 24 h, the cells were incubated with 100 nM AL-8(0) or 100 nM anti-IL17RA functional antibody (R&D Systems, MAB177 /MAB4481, USA) at 37 °C for 30 min. Subsequently, IL17RA-expressing or IL17RA-deficient cells were co-cultured with 100 nM recombinant IL17A protein (Sigma-Aldrich, H7791, USA) at 37 °C for 24 h. The concentrations of tumor necrosis factor (TNF)-α, IL-1β, IL-6, IL-8, and C-C motif chemokine ligand 20 (CCL20) in the supernatants were measured at 6, 12, 18, and 24 h. At the 24-hour time point, the expression levels of pNF-κB p65 and p-IκBα in the cell lysates were quantified and expressed as pNF-κB p65/NF-κB p65 (%) and p-IκBα/IκBα (%), respectively. All measurements were performed using corresponding enzyme-linked immunosorbent assay (ELISA) kits (Beyotime, Shanghai, China). Experimental procedures were conducted according to the manufacturer’s instructions.
Statistical analysis
Statistical analysis was performed using GraphPad Prism 8.0 (GraphPad Software, CA). Values are expressed as the mean ± SEM from at least three independent experiments conducted in biological duplicates or triplicates. Differences between groups were analyzed using one-way analysis of variance (ANOVA), followed by pairwise comparisons with the Student’s t-test (*P < 0.05; **P < 0.01; ns, not significantly different).
Results
Structure and synthesis of peptides of AL-8(0)
Studies have demonstrated that the aberrant activation of the IL17A-IL17RA signaling pathway is driven and regulated by the IL17A molecule. This study, therefore, focused on the IL17A-IL17RA binding site to design a peptide molecule. The resulting peptide, designated AL-8(0), has the sequence ASPVIYHL-NH2, and its structure is shown in Fig. 1A. AL-8(0) was synthesized using solid-phase synthesis, and its purity was assessed by high-performance liquid chromatography (HPLC). The molecular weight of AL-8(0) was determined through electrospray ionization mass spectrometry (ESI-MS), as shown in Fig. 1C. Figure 1B confirms that the molecular weight of AL-8(0) is 899, and its other physicochemical properties are consistent with expected values. The synthesized peptide achieved a purity of 96.3%, meeting the requirements for subsequent experiments.
Structure and synthesis of peptides. (A) Chemical structure of peptide AL-8(0). (B) Physicochemical properties of the peptides. (C) Analysis of peptide AL-8(0) by high-performance liquid chromatography (HPLC, up) and electrospray ionization mass spectrometry (ESI-MS, down).
AL-8(0)-target binding affinity
The binding assay results showed that the peptide fusion protein specifically binds to its targets. Microscale thermophoresis (MST) analysis demonstrated that AL-8(0) binds to IL17RA with an affinity of 89 nM (Fig. 2A and F). Similarly, surface plasmon resonance (SPR) analysis confirmed an affinity of 83 nM between AL-8(0) and IL17RA (Table. S1 and Fig. 2F). In addition, ELISA results provided key evidence of the specific binding affinity of AL-8(0) for the IL17RA target (Fig. 2B). The half-maximal effective concentration (EC₅₀) for AL-8(0) binding to IL17RA was determined to be 92.64 ng/ml (Fig. 2F), while no measurable EC₅₀ values were observed for IL17RC (Fig. 2C), IL17A (Fig. 2D) or IL17F (Fig. 2E). These findings further emphasize the specific binding capability of the AL-8(0) peptide within the IL17A-IL17RA signaling pathway.
AL-8(0)-target binding and functional assay. (A) Analysis of the data from the MST of AL-8(0) and IL17RA (left: sample uniformity, right: MST analysis of the interaction between). (B-E) ELISA assays of AL-8(0) targeting IL17RA (B), IL17RC (C), IL17A (D), IL17F(E). (F) AL-8(0)-target binding assay summary results.
IL17RA-deficient cells generation
IL17RA is highly expressed on the surface of immune cells and fibroblast s/keratinocytes3. To investigate its role, we selected the HaCaT human keratinocyte cell line, NIH3T3 murine fibroblast cell line, THP-1 human monocyte macrophage cell line and RAW264.7 murine monocyte macrophage cell line as research models. The high surface expression of IL17RA on these cells was confirmed using RT-qPCR and flow cytometry (Fig. 3A-D and Fig. S1). To generate IL17RA-deficient cells, siRNA was used to knock down IL17RA expression in four cell types. RT-qPCR and flow cytometry further validated a significant reduction in IL17RA expression in the target cells (Fig. 3A-D and Fig. S1), creating IL17RA-deficient models for subsequent studies.
AL-8(0)-Target interaction at the membrane. (A) Identification of IL17RA expressing/deficient HaCaT cells by RT-qPCR. (B) Identification of IL17RA expressing/deficient HaCaT cells by representative flow cytometry (left: HaCaT expression detected with IL17RA antibody, right: Median Flourescence intensity). (C) Identification of IL17RA expressing/deficient RAW264.7 cells by RT-qPCR. (D) Identification of IL17RA expressing/deficient RAW264.7 cells by representative flow cytometry (left: RAW264.7 expression detected with IL17RA antibody, right: Median Flourescence intensity). (E-F) Immunofluorescence analysis depicting the binding of AL-8(0) to expressing/deficient HaCaT cell. (G-H) Flow cytometry analysis depicting the binding of AL-8(0) to expressing/deficient RAW264.7 cell. (I) Median Flourescence intensity to IL17RA expressing (Normal) vs. deficient (IL17RA-) RAW264.7 cell. Student’s t-test applied to IL17RA siRNA vs. Normal. The data are presented as the mean ± SEM. p-values for the indicated compounds are **p < 0.01 (ANOVA).
AL-8(0) interactions with IL17RA expressing/deficient cells
To confirm the specific binding of AL-8(0) to IL17RA at the cellular level, we used previously generated IL17RA-deficient cells. Immunofluorescence analysis revealed that the FITC-conjugated AL-8(0) peptide binds specifically to normal HaCaT cells, with binding localized to the cell surface (marked by Dil dye). In contrast, no binding was observed in IL17RA-deficient HaCaT cells (Fig. 3E-F). Similarly, flow cytometry analysis demonstrated that the FITC-conjugated AL-8(0) peptide specifically binds to normal RAW264.7 cells but fails to bind to IL17RA-deficient RAW264.7 cells (Fig. 3G-I). Combined with previous experimental results, these findings further validate the binding specificity of the AL-8(0) peptide to IL17RA.
AL-8(0) cytotoxicity
This experiment aimed to determine whether the AL-8(0) peptide exhibits direct cytotoxicity toward target cells, independent of IL-17RA expression. IL-17RA-expressing and IL-17RA-deficient cells were co-cultured with varying concentrations of AL-8(0), and cell viability was assessed using the Cell Counting Kit-8 (CCK-8) assay. The results indicated that AL-8(0) did not induce cytotoxicity at any tested concentration in all four cell types, demonstrating its excellent safety profile (Fig. 4A-D). These findings confirm that AL-8(0) is non-toxic to target cells, laying a strong foundation for its application in future functional studies.
Assessment of AL-8(0) Cytotoxicity Using the CCK-8 Assay. The cytotoxicity assay showed that AL-8(0) was not directly cytotoxic to RAW264.7 (A), THP-1 (B), HaCaT (C), or NIH3T3 (D) cells. Normal cells are shown on the left, and IL17RA-deficient cells on the right. Data are presented as mean ± SEM. p-values for the indicated compounds were not significant (ns) based on ANOVA.
AL-8(0) anti-inflammatory in vitro
IL17A regulates immune responses via the IL17A-IL17RA signaling pathway by stimulating fibroblasts (e.g., NIH3T3) and keratinocytes (e.g., HaCaT) to produce pro-inflammatory cytokines such as TNFα, IL6, IL8, and CCL20. Additionally, it induces monocyte-derived macrophages (e.g., THP-1, RAW264.7) to secrete inflammatory mediators, including TNFα, IL1β, and IL6. This signaling activity plays a critical role in the pathogenesis of inflammatory diseases6,7,8,9.
Here, we examined the inhibitory effects of the AL-8(0) peptide on the IL17A-IL17RA signaling pathway. THP-1, RAW264.7, HaCaT, and NIH3T3 cells, either IL17RA-expressing or IL17RA-deficient, were treated with an IL17RA neutralizing antibody or AL-8(0) peptide, followed by IL17A stimulation for a defined period. Cytokine levels in the cell supernatants at key time points were quantified via ELISA to assess the inhibitory effects of AL-8(0) on IL17A-IL17RA signaling.
In addition, at the 24-hour time point, cell lysates were collected to assess the phosphorylation levels of NF-κB p65 and IκBα. Phosphorylation of NF-κB p65 protein indicates the activation of the NF-κB signaling pathway, while phosphorylation of IκBα represents the degradation of the NF-κB inhibitor, IκBα, which allows NF-κB to translocate to the nucleus. This further evaluates the activity of key mediators in the IL17A-IL17RA-driven inflammatory response pathway39. The results showed that AL-8(0) effectively inhibited IL17A–IL17RA signaling in wild-type THP-1 and RAW264.7 cells. In these cells, AL-8(0) consistently suppressed TNFα, IL-1β, and IL-6 expression at all tested time points (Fig. 5A-F). In contrast, AL-8(0) had no significant effect on IL-17RA-deficient THP-1 and RAW264.7 cells (Fig. S2), further confirming that its anti-inflammatory activity is IL17RA-dependent.
Coculture of IL17RA mAb (100nM) or AL-8(0) (100nM) with IL17RA-expressing mononuclear macrophages by IL17A (100nM) 24 h Stimulation. (A-C) Identification of TNFα(A), IL1β(B), IL6(C) expressing in THP-1 cells by ELISA. (D-F) Identification of TNFα(D), IL1β(E), IL6(F) expressing in RAW264.7 cells by ELISA. The data are presented as the mean ± SEM. p-values for the indicated compounds are **p < 0.01 (ANOVA).
Similarly, AL-8(0) exhibited comparable anti-inflammatory activity in keratinocytes and fibroblasts. It inhibited the ability of HaCaT cells to produce TNFα, IL-8, and CCL20 through the IL17A-IL17RA signaling pathway (Fig. 6A-C) and also suppressed the production of TNFα, IL-6, and CCL20 in NIH3T3 cells via the same pathway (Fig. 6D-F). Moreover, this inhibitory effect on inflammation was not observed in IL-17RA-deficient HaCaT (Fig. S3A-C) and NIH3T3 (Fig. S3D-F) cells.
Coculture of IL17RA mAb (100nM) or AL-8(0) (100nM) with IL17RA-expressing Keratinocyte-fibroblasts by IL17A (100nM) 24 h Stimulation. (A-C) Identification of TNFα(A), IL8(B), CCL20(C) expressing in HaCaT cells by ELISA. (D-F) Identification of TNFα(D), IL6(E), CCL20(F) expressing in NIH3T3 cells by ELISA. The data are presented as the mean ± SEM. p-values for the indicated compounds are **p < 0.01 (ANOVA).
Finally, analysis of lysates from wild-type cells co-cultured with IL17A for 24 h revealed that AL-8(0) effectively inhibited IL17A–IL17RA-induced activation of the NF-κB signaling pathway by reducing phosphorylation of NF-κB p65 (Fig. 7A-D) and IκBα (Fig. 7E-H). However, AL-8(0) had no significant effect on NF-κB signaling in IL17RA-deficient cells (Fig. S4). These findings underscore the anti-inflammatory potential of AL-8(0) and support its further development as a candidate drug for autoimmune disease treatment.
Evaluation of IL17RA mAb or AL-8(0)-Mediated Inhibition of the NF-κB Pathway in IL-17RA-Expressing Cells After 24 h of IL-17 A Stimulation. (A-D) Expression Levels of Phosphorylated NF-κB p65 Protein (p-NFκB p65) in THP-1(A), RAW264.7(B), HaCaT(C), and NIH3T3(D). (E-H) Expression Levels of Phosphorylated IκBα p65 Protein (p-IκBα) in THP-1(E), RAW264.7(F), HaCaT(G), and NIH3T3(H). The data are presented as the mean ± SEM. p-values for the indicated compounds are **p < 0.01 (ANOVA).
Discussion
In this study, we demonstrated that the designed small-molecule peptide drug, AL-8(0), effectively inhibits IL17A-mediated inflammatory activity in keratinocytes and monocytes, offering a promising therapeutic strategy. This conclusion is supported by the clinical success of IL17A and IL17RA-neutralizing antibodies in treating psoriasis and rheumatoid arthritis, underscoring the critical importance of regulating inflammatory cytokine signaling pathways. In patients with psoriasis, skin inflammation is characterized by the overexpression of pro-inflammatory factors and an imbalance in anti-inflammatory factors21,22. Inhibiting the IL17A-IL17RA signaling pathway effectively restores this balance, thereby alleviating the disease. However, antibody therapies face several limitations, including high manufacturing costs, complex production processes, potential immunogenicity that can lead to the formation of anti-drug antibodies (ADAs), and reduced efficacy over time. Moreover, these therapies lack oral bioavailability. For patients with chronic diseases, oral administration is more suitable to meet treatment needs and improve patient compliance.
Developing novel ligands with anti-IL17RA activity could address these unmet clinical needs in autoimmune diseases. In this study, we developed a novel peptide, AL-8(0), using a combination of biophysical and cellular validation methods. Synthesized via solid-phase peptide synthesis, AL-8(0) achieved a high purity of 96.3% and demonstrated significant potential for specific binding to IL17RA across a series of experiments. Multiple affinity assays, including MST, SPR, and ELISA, confirmed that AL-8(0) exhibits high affinity and specificity for IL17RA. Cellular experiments using IL17RA-deficient cells further validated AL-8(0)’s ability to specifically bind IL17RA-expressing cells.
In vitro anti-inflammatory experiments demonstrated that AL-8(0) exhibits anti-inflammatory efficacy comparable to IL17RA-neutralizing antibodies, significantly inhibiting inflammatory responses mediated by the IL17A-IL17RA signaling pathway. Furthermore, neither AL-8(0) nor IL17RA antibodies exhibited therapeutic effects in IL17RA-deficient cells, clearly indicating that their anti-inflammatory mechanisms depend on the presence of IL17RA. These findings highlight the high specificity of AL-8(0) for the IL17A-IL17RA signaling pathway, providing a robust foundation for its development as a targeted anti-inflammatory therapeutic.
The IL17A-IL17RA signaling pathway is a critical driver of inflammatory responses in cells with high IL17RA expression, making it an optimal therapeutic target for drug development in autoimmune diseases. Inhibiting this pathway directly suppresses the initiation and progression of excessive immune responses. This study provides proof-of-concept evidence that IL17RA antagonists can effectively block the interaction between the IL17A cytokine and IL17RA on the surface of inflammatory cells. This blockade inhibited the secretion of inflammation-related cytokines by inflammatory cells in vitro, confirming the anti-inflammatory activity of AL-8(0). Furthermore, inhibitors of the IL17A-IL17RA pathway can be combined with other signaling inhibitors to achieve synergistic anti-inflammatory effects. For example, combining anti-IL17RA antibodies with colchicine has demonstrated superior anti-inflammatory effects in psoriasis treatment compared to either drug alone20.
More importantly, due to time constraints, we were unable to perform in vivo studies on the anti-inflammatory effects of AL-8(0) in rheumatoid arthritis and psoriasis models, representing a notable limitation. Future studies should prioritize evaluating the in vivo anti-inflammatory activity of AL-8(0), including its therapeutic efficacy in animal models of psoriasis and rheumatoid arthritis, to further assess its potential as a treatment for autoimmune diseases. Additionally, structural modifications of AL-8(0) should be explored to enhance its stability and bioavailability in vivo.
Data availability
The data generated and analysed during the current study are available from the corresponding author on reasonable request.
References
Misra, D. P. & Agarwal, V. Th17.1 lymphocytes: emerging players in the orchestra of immune-mediated inflammatory diseases. Clin. Rheumatol. 41 (8), 2297–2308 (2022).
Johansen, C. et al. Characterization of the interleukin-17 isoforms and receptors in lesional psoriatic skin. Br. J. Dermatol. 160 (2), 319–324 (2009).
Chung, S. H., Ye, X. Q. & Iwakura, Y. Interleukin-17 family members in health and disease. Int. Immunol. 33 (12), 723–729 (2021).
Bastid, J., Dejou, C., Docquier, A. & Bonnefoy, N. The emerging role of the IL-17B/IL-17RB pathway in Cancer. Front. Immunol. 11, 718 (2020).
Nies, J. F. & Panzer, U. IL-17 C/IL-17RE: emergence of a unique axis in Th17 biology. Front. Immunol. 11, 341 (2020).
Majumder, S. & McGeachy, M. J. IL-17 in the pathogenesis of disease: good intentions gone awry. Annu. Rev. Immunol. 39, 537–556 (2021).
Iwakura, Y., Nakae, S., Saijo, S. & Ishigame, H. The roles of IL-17A in inflammatory immune responses and host defense against pathogens. Immunol. Rev. 226, 57–79 (2008).
Bisoendial, R. & Lubberts, E. A Mechanistic Insight into the pathogenic role of interleukin 17A in systemic autoimmune diseases. Mediators Inflamm. 6600264 (2022). (2022).
Raucci, F. et al. IL-17A neutralizing antibody regulates monosodium urate crystal-induced gouty inflammation. Pharmacol. Res. 147, 104351 (2019).
Saviano, A. et al. Anti-inflammatory and Immunomodulatory activity of Mangifera indica L. reveals the modulation of COX-2/mPGES-1 axis and Th17/Treg ratio. Pharmacol. Res. 182, 106283 (2022).
Fletcher, J. M., Moran, B., Petrasca, A. & Smith, C. M. IL-17 in inflammatory skin diseases psoriasis and hidradenitis suppurativa. Clin. Exp. Immunol. 201 (2), 121–134 (2020).
Zhang, C. et al. IL-17A-neutralizing antibody ameliorates inflammation and fibrosis in rosacea by antagonizing the CXCL5/CXCR2 axis. FASEB J. 38(19), e70096 (2024).
Xie, X. J. et al. Indirubin ameliorates imiquimod-induced psoriasis-like skin lesions in mice by inhibiting inflammatory responses mediated by IL-17A-producing Γδ T cells. Mol. Immunol. 101, 386–395 (2018).
Di, T. T. et al. Astilbin inhibits Th17 cell differentiation and ameliorates imiquimod-induced psoriasis-like skin lesions in BALB/c mice via Jak3/Stat3 signaling pathway. Int. Immunopharmacol. 32, 32–38 (2016).
Jia, Q. et al. Malassezia globosa induces differentiation of pathogenic Th17 cells by inducing IL-23 secretion by keratinocytes. Mycopathologia 189 (5), 85 (2024).
Liu, H. et al. IL-17 signaling pathway: A potential therapeutic target for reducing skeletal muscle inflammation. Cytokine 181, 156691 (2024).
Yu, C. et al. A novel mechanism for regulating lung immune homeostasis: Zukamu granules alleviated acute lung injury in mice by inhibiting NLRP3 inflammasome activation and regulating Th17/Treg cytokine balance. J. Ethnopharmacol. 324, 117831 (2024).
Song, S. et al. Alteration of gut Microbiome and correlated amino acid metabolism contribute to hyperuricemia and Th17-Driven inflammation in Uox-KO mice. Front. Immunol. 13, 804306 (2022).
Pawlik, A. et al. IL17A and IL17F gene polymorphisms in patients with rheumatoid arthritis. BMC Musculoskelet. Disord. 17, 208 (2016).
Krzysiek, J. et al. The role of heterodimer IL-17-A/F in atopic dermatitis. Postepy Dermatol. Alergol. 39 (6), 1093–1100 (2022).
Deodhar, A. et al. Long-term safety of Secukinumab in patients with moderate-to-severe plaque psoriasis, psoriatic arthritis, and ankylosing spondylitis: integrated pooled clinical trial and post-marketing surveillance data. Arthritis Res. Ther. 21 (1), 111 (2019).
Norden, A. et al. Anti-drug antibodies of IL-17 inhibitors for psoriasis: a systematic review. J. Dermatolog Treat. 33 (8), 3080–3085 (2022).
Reich, K. et al. Secukinumab, a fully human anti-interleukin-17A monoclonal antibody, exhibits low immunogenicity in psoriasis patients treated up to 5 years. J. Eur. Acad. Dermatol. Venereol. 33 (9), 1733–1741 (2019).
Wolfe, C., Kennard, B., Bewley, A. & Mehrtens, S. A retrospective review of pregnancies in our psoriasis biologic cohort. Clin. Exp. Dermatol. 49 (9), 1080–1082 (2024).
Asmani, A. Z. A. et al. Immunogenicity of monoclonal antibody: causes, consequences, and control strategies. Pathol. Res. Pract. 263, 155627 (2024).
Pizano-Martinez, O. et al. Anti-Drug antibodies in the biological therapy of autoimmune rheumatic diseases. J. Clin. Med. 12 (9), 3271 (2023).
Bray-French, K. et al. Managing the impact of immunogenicity in an era of immunotherapy: from bench to bedside. J. Pharm. Sci. 110 (7), 2575–2584 (2021).
Liu, S. et al. Inhibiting complex IL-17A and IL-17RA interactions with a linear peptide. Sci. Rep. 6, 26071 (2016).
Shaw, D. J. et al. Modulation of IL-17 backbone dynamics reduces receptor affinity and reveals a new inhibitory mechanism. Chem. Sci. 14 (27), 7524–7536 (2023).
Liu, S. Structural insights into the Interleukin-17 family cytokines and their receptors. Adv. Exp. Med. Biol. 1172, 97–117 (2019).
Hlavničková, M. et al. ABD-Derived protein blockers of human IL-17 receptor a as non-IgG alternatives for modulation of IL-17-dependent pro-inflammatory axis. Int. J. Mol. Sci. 19 (10), 3089 (2018).
Koštrun, S. et al. Macrolide inspired macrocycles as modulators of the IL-17A/IL-17RA interaction. J. Med. Chem. 64 (12), 8354–8383 (2021).
Álvarez-C, E. et al. Discovery of novel immunepharmacological ligands targeting the IL-17 inflammatory pathway. Int. Immunopharmacol. 89 (Pt A), 107026 (2020).
Berry, S. P. D. et al. The role of IL-17 and anti-IL-17 agents in the Immunopathogenesis and management of autoimmune and inflammatory diseases. Int. Immunopharmacol. 102, 108402 (2022).
Koh, C. H., Kim, B. S., Kang, C. Y., Chung, Y. & Seo, H. IL-17 and IL-21: their immunobiology and therapeutic potentials. Immune Netw. 24(1), e2 (2024).
Kuwada, K. et al. The epithelial-to-mesenchymal transition induced by tumor-associated macrophages confers chemoresistance in peritoneally disseminated pancreatic cancer. J. Exp. Clin. Cancer Res. 37, 307 (2018).
Torres, O. B. et al. A rapid solution-based method for determining the affinity of heroin hapten-induced antibodies to heroin, its metabolites, and other opioids. Anal. Bioanal Chem. 410 (16), 3885–3903 (2018).
Syedbasha, M. et al. An ELISA based binding and competition method to rapidly determine Ligand-receptor interactions. J. Vis. Exp. 2016, 53575 (2016).
Jardin, F. NFkB pathway and hodgkin lymphoma. Biomedicines 10 (9), 2153 (2022).
Acknowledgements
We acknowledge funding from the National Natural Science Foundation of China (82460323 to Xinmin Wang), the Natural Science Foundation of Inner Mongolia (2023QN08018 to Xinmin Wang), and the Fundamental Research Funds for Inner Mongolia University of Science & Technology (2023QNJS149 to Xinmin Wang).
Author information
Authors and Affiliations
Contributions
Conceptualization, Xinmin Wang; Data curation, Hang Bao, Yuya Wang, Yalu Wang, Cheng Guo, Yanning Wu and Yongbin Xu; Formal analysis, Xinmin Wang; Funding acquisition, Xinmin Wang and Yali Li; Investigation, Xinmin Wang and Hang Bao; Methodology, Xinmin Wang; Project administration, Yali Li; Resources, Xinmin Wang; Software, Xinmin Wang; Supervision, Yali Li; Validation, Xinmin Wang, Hang Bao, Cheng Guo, Yanning Wu and Yongbin Xu; Visu-alization, Yali Li; Writing – original draft, Xinmin Wang; Writing – review & editing, Yali Li. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Wang, X., Bao, H., Wang, Y. et al. Innovative peptide therapeutics targeting IL17RA to regulate inflammatory responses. Sci Rep 15, 8542 (2025). https://doi.org/10.1038/s41598-025-92915-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-92915-8