Abstract
This study investigates the effect of epiretinal membrane (ERM) removal in the combined hamartomas of the retina and retinal pigment epithelium (CHRRPE) patients. In this retrospective, comparative case series, 15 CHRRPE patients were included. Six patients received ERM surgery (operation group) and 9 patients were observed (observation group). The differences of age at diagnosis and the severity of ERM were not statistically significant for the operation and observation group at initial diagnosis. The change in central macular thickness (CMT), foveo-papillary distance (FPD) and best corrected visual acuity (BCVA) were analyzed for both groups at initial and final follow-up visits. In the operation group, CMT significantly decreased (initial 480 ± 151 μm VS final 365 ± 59 μm; P = 0.036), while FPD significantly increased (P = 0.031). BCVA significantly improved at the final follow-up in operation group (P = 0.031). In the observation group, FPD decreased significantly (P = 0.012) and BCVA did not change significantly (P = 0.438). Removal of ERM may be beneficial in normalizing macular anatomy and may be effective in preventing visual deterioration in patients with ERM associated with CHRRPE.
Similar content being viewed by others
Introduction
Combined hamartomas of the retina and retinal pigment epithelium (CHRRPE) is a rare intraocular tumor first described by Gass in 1973 as elevated, charcoal grey mass involving the retinal pigment epithelium (RPE), retina, and overlying vitreous1. Extending in a fanlike projection toward the periphery, CHRRPE is covered by thickened grey-white retinal and preretinal tissue, showing contraction of the inner surface with an absence of retinal detachment, hemorrhage, exudation, and vitreous inflammation2. However, due to its rarity, not much is known about this clinical entity. With the development of optical coherence tomography (OCT), some typical characteristics of CHRRPE have been revealed. In a case series by Shields et al., epiretinal membrane (ERM) was found in all 11 patients, while posterior vitreous detachment (PVD) was absent in all the cases3. In 2017, Chawla et al. showed that the hamartoma primarily involved the inner retinal layers limited externally by the outer plexiform layer in 93.7% of the eyes4. Moreover, a recent multicenter study has shown that older aged patients had more alterations at the ellipsoid zone and RPE than younger patients5.
Since ERM is present in almost all CHRRPE patients, there has been a constant debate concerning ERM removal and its visual outcomes. In 1985, McDonald et al. described two patients with CHRRPE (ages 44 and 26 years) in whom surgical removal of epiretinal membrane was performed, and visual acuity did not improve in either case6. The authors suggested that these older patients with a presumed congenital tumor had irreversible visual loss. Subsequently, Mason and Kleiner reported a case of visual improvement following surgical removal of ERM in younger patients with CHRRPE7. A report published in 2010 showed that ERM removal improved anatomical outcomes, such as central macular thickness (CMT), while little improvement in visual acuity was seen in patients aged 6 to 21 years.8 In a recent multicenter study, Ozdek et al. reported that surgical removal of ERM may have more favorable visual and anatomical outcomes than in observation group in pediatric CHRRPE patients (average age 7.7 ± 4.7 years)9.
Herein, we retrospectively investigate the effect of surgical removal of ERM in CHRRPE patients on the macular structure and visual acuity. Toward this end, we analyzed the OCT images and clinical features in CHRRPE patients of diverse ages that underwent or did not go through ERM surgery (operation group and observation group, respectively).
Methods
Study participants
This retrospective, comparative case series adhered to the tenets of the Declaration of Helsinki and all experimental protocols were approved by the institutional review board of Gangnam Severance Hospital. Ethical approval and informed consent was waived by institutional review board of Gangnam Severance Hospital due to retrospective design.
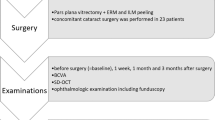
We used the U-Severance electronic medical records program to screen patients diagnosed with CHRRPE at Severance Hospital between January 2006 and July 2022. Multimodal imaging of all potential patients with CHRRPE was primarily reviewed by two retinal specialists (CHL. and MK). Patients were excluded if they had a history of ocular trauma, inflammatory disease, severe cataract, or a follow-up of less than 6 months. Patients were divided into two groups based on whether they had conservative management (observation group) or pars plana vitrectomy and ERM removal (operation group). The final diagnosis and inclusion of CHRRPE cases in the study were confirmed by two senior experienced retinal specialists (JL and MK) in consensus.
Demographic and clinical data, including age, sex, presenting symptoms, and best-corrected visual acuity (BCVA), of all patients were collected. We reviewed their medical histories, blood work-up results, and laboratory test results to check for a history of inflammatory and infectious disease.
Surgical technique
Surgeries were performed by surgeons with more than 10 years of experience. After the placement of trocars at pars plana, core vitrectomy was performed. After PVD induction, ERM was gently removed using forceps. Internal limiting membrane (ILM) peeling was also performed with the assistance of indocyanine green dye staining. All patients aged 50 years or less underwent lens saving vitrectomy. Patients over the age of 50 years received phacoemulsification and intraocular lens implantation combined with vitrectomy.
Fundus photography
All included eyes were evaluated using color fundus photography with the Optos ultra-widefield fundus camera (Optos PLC, Dunfermline, United Kingdom) and KOWA VX-20 retinal fundus camera (Kowa Company Ltd., Tokyo, Japan). Descriptive fundus findings included presence of exudates, retinal hemorrhage, pigmentation, and tumor location (peripapillary, macular, or peripheral). As quantitative measurement, the tumor basal dimensions were measured. Having used two different fundus camera systems, we calibrated the quantitative measurements by assuming that the horizontal diameter of the optic disc was 1.77 mm10,11. No cases of an unusually small or large disc that could affect the calibration were present.
Optical coherence tomography
Spectral-domain optical coherence tomography (OCT) was performed using Spectralis OCT (Heidelberg Engineering GmbH; Heidelberg, Germany). Images captured at both the CHRRPE lesion and the macula center were analyzed. Descriptive findings included the presence of subretinal fluid (SRF), PVD, and ERM. For quantitative measurements, the images captured at the macula center were used. These included 1) central macular thickness (CMT) defined by the average thickness within 1.0 mm central circle of the Early Treatment Diabetic Retinopathy Study (ETDRS) grid, 2) average retinal thickness of 3.0 mm inner subfields of ETDRS grid: nasal, temporal, superior, and inferior, and 3) foveo-papillary distance (FPD). For the operation group, these quantitative measurements were assessed preoperatively as well as at final postoperative follow-up visit. For the observation group, the initial values at first visit and the values at final follow-up visit were recorded and compared. FPD is defined as the distance between the macular center and a designated vessel at the optic disc margin and is calculated using the caliper tool on the near-infrared (NIR) image provided by Spectralis OCT software12,13,14. The difference of FPD between two different time points (∆FPD) quantifies the degree of dragging of foveal center with respect to the optic disc, with negative values representing nasal dragging and positive values representing temporal dragging (nasal dragging: ∆FPD < 0, temporal dragging: ∆FPD > 0). FPD was useful in quantifying changes at foveal center in previous studies that investigated the dragging of macula after macular hole surgery13,14. FPD at initial and final follow-up visits were measured and compared to show the change of the position of the foveal center with respect to the optic disc in CHRRPE patients. The designation of the vessel at the optic disc margin and macular center was done by two senior experienced retinal specialists (JL and MK) by consensus. The measurement of FPD was done by two masked graders (JHJ and EYC). Representative photos and measurements of a CHRRPE patient are shown in Fig. 1.
Multimodal imaging of a combined hamartomas of the retina and retinal pigment epithelium (CHRRPE) patient A 7-years-old female patient visited our clinic with complaints of gradual decrease in visual acuity of the left eye. Her best corrected visual acuity was 0.397 logMAR. (A) Fundus photography and (B) ultra-widefield fundus photography show a 6.64 mm × 5.50 mm sized elevated mass at peripapillary area. No intraretinal hemorrhage, intraretinal exudation, or pigmentation were noted. (C) On autofluorescence photography, mild hypoautofluorescence was observed at the intraocular mass. (D) On near infrared (NIR) imaging, the mass was isoreflective. The optical coherence tomography (OCT) shows typical elevation and proliferation of retinal layers and the retinal pigment epithelium at the peripapillary area. Posterior vitreous detachment (PVD) is not present. Mild epiretinal membrane (ERM) is noted at nasal to fovea. (E) On B-scan ultrasonography, a slightly hypoechoic mass with height of 1.24 mm was observed at peripapillary location. (F) The foveo-papillary distance (FPD) was calculated from the foveal center to a vessel located at inferior disc margin (red circle). The foveal center was slightly nasally shifted (red asterisk). (G) The central macular thickness (CMT) at 1.0 mm center of the Early Treatment Diabetic Retinopathy Study (ETDRS) grid was 506 μm. The average retinal thicknesses of 3.0 mm inner subfields of ETDRS grid were 786 μm, 394 μm, 513 μm, and 523 μm at nasal, temporal, superior, and inferior, respectively.
Ultrasonography
We performed ultrasonography (Eye Cubed; Ellex; Adelaide, Australia) and analyzed the thickness of the CHRRPE lesions.
Statistical analysis
The mean, median, and standard deviation values of the evaluated variables are reported using descriptive statistics. We conducted Mann–Whitney test and Wilcoxon matched pairs test for unpaired parameters and longitudinal analysis, respectively. Qualitative and quantitative measurements were performed by two masked graders (JHJ and EYC). The intra-class correlation coefficient (ICC) was calculated for quantitative measurements to verify the agreement between the masked graders. Cohen’s kappa coefficient was calculated for inter-rater agreement for qualitative assessments. If the two masked graders disagreed on the qualitative assessment, adjudication was conducted by senior experienced retinal specialists (JL and MK) to settle the argument. Statistical analysis was performed by CHL and MK. All quantitative data are presented as mean ± standard deviation unless otherwise indicated.
Results
Clinical findings of CHRRPE patients at initial presentation
A total of 15 patients were included in the study. All patients were ethnically homogenous (Korean, 100%). Six patients underwent ERM surgery and nine patients were observed without treatment. The mean ± standard deviation value of the age at diagnosis was 38 ± 22 years for the operation group and 38 ± 20 years for the observation group (Mann–Whitney test, P > 0.999). The total follow-up periods for the operation and observation groups were 2.18 ± 1.79 years and 3.56 ± 2.9 years, respectively (P = 0.528). All patients in the operation group had a peripapillary location of CHRRPE (n = 6, 100.0%). In the observation group, one patient had CHRRPE at the macula (n = 1, 11.1%), while all other patients had CHRRPE at the peripapillary location (n = 8, 88.9%). The tumor dimensions were 5.79 ± 1.64 mm and 4.64 ± 1.83 mm for the operation and observation groups, respectively (Mann–Whitney test, P = 0.328). Tumor thicknesses on ultrasonography were 1.42 ± 0.41 mm and 1.21 ± 0.30 mm for the operation and observation groups, respectively (P = 0.284). PVD was not present in any of the patients in both groups; however, ERM was present in all patients in both the groups. None of the patients had intraretinal hemorrhage. Exudation was present in two patients from the operation group (33.3%) and one patient from the observation group (11.1%). SRF was absent in the operation group, and one patient had SRF in the observation group (11.1%). Pigmentation was present in five (83.3%) and six (66.7%) patients in the operation and observation groups, respectively. The CMT was 480 ± 151 μm in the operation group, while it was 413 ± 166 μm in the observation group (P = 0.456). The retinal thicknesses at 3.0 mm inner subfield of ETDRS grid for the operation and observation groups, respectively, were as follows: nasal 605 ± 214 μm and 520 ± 207 μm, temporal 374 ± 99 μm and 396 ± 98 μm (P = 0.689), superior 493 ± 237 μm and 451 ± 170 μm (P = 0.864), inferior 409 ± 142 μm and 389 ± 72 μm (P = 0.999). The BCVA at presentation was worse in the operation group (0.48 ± 0.21 logMAR) than in the observation group (0.16 ± 0.17 logMAR) (P = 0.02). The clinical findings at the initial visit to our institution are summarized in Tables 1 and 2.
Main outcomes at the final follow-up
In the operation group, mean postoperative CMT at final follow-up was significantly lower compared to that at initial presentation (initial 480 ± 151 μm VS final 365 ± 59 μm; Wilcoxon matched pairs test, P = 0.036). All patients in the operation group exhibited a decrease in CMT after surgery (-115 ± 131 μm; range: -2 ~ -332 μm). In contrast, mean CMT did not change significantly in the observation group (initial 412 ± 166 μm, final 441 ± 178 μm; P = 0.313). Out of the nine observation group patients, CMT remained unchanged in one, decreased in three (range: -4 ~ -61), increased in five (range: + 8 ~ + 178) patients (Fig. 2A).
Changes in optical coherence tomography (OCT) parameters and best corrected visual acuity (BCVA) in operation group and observation group of combined hamartomas of the retina and retinal pigment epithelium (CHRRPE) patients (A) The central macular thickness (CMT) significantly decreased after the operation at the final follow-up (initial 480 ± 151 μm VS final 365 ± 59 μm; Wilcoxon matched pairs test, P = 0.036). All patients of the operation group had decreased CMT (-115 ± 131 μm; range: -2 ~ -332 μm) after surgery. In the observation group, the CMT did not change significantly (initial 412 ± 166 μm, final 441 ± 178 μm; P = 0.313). Unchanged CMT: 1 patient, decreased CMT: 3 patients (range: -4 ~ -61), and increased CMT: 5 patients (range: + 8 ~ + 178). (B-D) The retinal thickness of 3.0 mm inner subfield of Early Treatment Diabetic Retinopathy Study (ETDRS) grid did not change significantly for all the four sides (nasal, temporal, superior, inferior) (B) Nasal: initial 605 ± 213 μm, final 504 ± 201 μm; P = 0.313, operation group and initial 519 ± 207 μm, final 558 ± 213 μm; P = 0.496, observation group (C) Temporal: initial 374 ± 99 μm, final 319 ± 39 μm; P = 0.218, operation group and initial 396 ± 98 μm, final 385 ± 64 μm; P = 0.910, observation group. (D) Superior: initial 494 ± 142 μm, final 374 ± 81 μm; P = 0.062, operation group and initial 451 ± 170 μm, final 461 ± 137 μm; P = 0.496, observation group. (E) Inferior: initial 409 ± 142 μm, final 347 ± 49 μm; P = 0.438, operation group and initial 389 ± 72 μm, final 426 ± 115 μm; P = 0.097, observation group. (F) Foveo-papillary distance (FPD) significantly increased in operation group (initial 2844 ± 568 μm VS final 3077 ± 474 μm, P = 0.031), while it decreased significantly at the final follow-up in observation group (initial 3261 ± 663 μm VS final 3012 ± 738 μm, P = 0.012). Note an increase in FPD in all the patients of the operation group (+ 233 ± 169 μm; range: + 70 ~ + 490 μm) and a decrease in FPD of all the observation group patients (-293 ± 174 μm; range: -69 ~ -613 μm). (G) Best corrected visual acuity (BCVA) significantly improved at final postoperative follow-up (initial 0.48 ± 0.21 logMAR VS final 0.22 ± 0.15 logMAR, P = 0.031), but no significant change at the final follow-up was observed in the observation group (initial 0.15 ± 0.17 logMAR VS final 0.27 ± 0.28 logMAR, P = 0.438). * P < 0.05.
Similarly, the retinal thickness of 3.0 mm inner subfield of ETDRS grid also did not show any significant change, for any of the four sides, in both the groups. Nasal side: initial 605 ± 213 μm, final 504 ± 201 μm; P = 0.313 for operation group and initial 519 ± 207 μm, final 558 ± 213 μm; P = 0.496 for observation group (Fig. 2B). Temporal side: initial 374 ± 99 μm, final 319 ± 39 μm; P = 0.217 for operation group & initial 396 ± 98 μm, final 385 ± 64 μm; P = 0.910 for observation group (Fig. 2C). Similarly, for superior side: initial 494 ± 142 μm, final 374 ± 81 μm; P = 0.062 in operation group and initial 451 ± 170 μm, final 461 ± 137 μm; P = 0.496 in observation group (Fig. 2D). The retinal thickness of inferior side in operation group was 409 ± 142 μm at initial visit and 347 ± 49 μm at final visit (P = 0.438), while for the observation group, the values were: initial 389 ± 72 μm, final 426 ± 115 μm; P = 0.097 (Fig. 2E).
In contrast to retinal thickness, FPD exhibited a significant postoperative increase in the operation group (initial 2844 ± 568 μm VS final 3077 ± 474 μm, P = 0.031). All patients in the operation group had increased postoperative FPD (+ 233 ± 169 μm; range: + 70 ~ + 490 μm). However, in the observation group, the FPD significantly decreased at the final follow-up (initial 3261 ± 663 μm VS final 3012 ± 738 μm, P = 0.012), and all the observation group patients had decreased FPD (-293 ± 174 μm; range: -69 ~ -613 μm) at the final follow-up (Fig. 2F).
In the operation group, the BCVA significantly improved (initial 0.48 ± 0.21 logMAR VS final 0.22 ± 0.15 logMAR, P = 0.031). However, the observation group did not show any significant change in the BCVA at the final follow-up (initial 0.15 ± 0.17 logMAR VS final 0.27 ± 0.28 logMAR, P = 0.438) (Fig. 2G). Representative patients of the operation and observation groups are presented in Fig. 3.
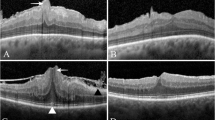
Representative patient of the operation group and a patient in the observation group of combined hamartomas of the retina and retinal pigment epithelium (CHRRPE) (A) Preoperative fundus findings of a seven-year old female combined hamartoma of the retina and retinal pigment epithelium (CHRRPE) patient shows 6.64 mm × 5.50 mm sized elevated peripapillary mass without pigmentation in her left eye. The foveo-papillary distance (FPD) was 3097 μm. The foveal center was shifted nasally (red asterisk). The central macular thickness (CMT) was 506 μm. The thicknesses of nasal, temporal, superior, and inferior 3.0 mm subfield of the Early Treatment Diabetic Retinopathy Study (ETDRS) grid were 786 μm, 394 μm, 513 μm, and 523 μm, respectively. The preoperative best corrected visual acuity (BCVA) was 0.397 logMAR. The patient underwent lens-saving trans pars plana vitrectomy and epiretinal membrane (ERM) removal due to amblyopia. (B) At postoperative 1-year follow-up, the size of the CHRRPE had not changed. However, the FPD increased to 4431 μm. The foveal center had moved temporally towards normal location (yellow asterisk). The CMT decreased to 442 μm. The thicknesses of nasal, temporal, superior, and inferior 3.0 mm subfield of the ETDRS grid decreased to 440 μm, 386 μm, 406 μm, and 360 μm, respectively. The BCVA increased to 0.155 logMAR. (C) A 34-year-old female CHRRPE patient visited the clinic with a complaint of gradual decrease in visual acuity of her right eye. Fundus examination shows 6.0 mm × 4.5 mm sized elevated peripapillary mass with mild pigmentation. The FPD was 2958 μm. The foveal center was shifted nasally (red asterisk). The CMT was 751 μm. The thicknesses of nasal, temporal, superior, and inferior 3.0 mm subfield of the ETDRS grid were 899 μm, 549 μm, 676 μm, and 592 μm, respectively. The BCVA was 0.301 logMAR. The patient was observed without treatment for 5 years. (D) The size of the CHRRPE did not change. However, the FPD decreased to 2345 μm. The foveal center moved more nasally towards the optic nerve (yellow asterisk). The CMT increased to 988 μm. The thicknesses of nasal, temporal, superior, and inferior 3.0 mm subfield of the ETDRS grid increased to 1018 μm, 635 μm, 843 μm, and 804 μm, respectively. The BCVA worsened to 0.824 logMAR.
Discussion
To the best of our knowledge, this is the first study that has compared the changes in OCT macular structure in detail, including CMT, retinal thickness of 3.0 mm inner subfields of ETDRS grid, and FPD, between CHRRPE patients who underwent (operation group) or did not undergo (observation group) surgical removal of ERM. The operation group exhibited a significant decrease in CMT and increase in FPD and improvement of BCVA at final follow-up. The observation group, however, showed significant decrease in FPD, while no significant change in either CMT or BCVA was observed. The decrease of CMT and improvement of BCVA after ERM operation in CHRRPE patients have been documented in several previous studies9,15,16,17. Results favoring operation of ERM in symptomatic CHRRPE patients with decreased visual acuity have been published recently. Furthermore, since many of these patients present with amblyopia at an early age, early ERM removal may be beneficial for development of visual function and prevention of amblyopia. However, all these studies were published recently, and a longer study period and follow-up to confirm the benefits of early ERM surgery in CHRRPE patients were needed. Our study has relatively longer follow-up (2.18 ± 1.79 years / range : 1.00 ~ 5.74 years) than previous studies, that shows favorable results of stable visual improvement in the operation group. Although the mean age of the patients in the operation group of our study was relatively higher than that in previous studies (38 ± 22, range: 7 ~ 58), visual acuity improved significantly. Although younger patients had more drastic improvement of visual acuity, our study suggests that the removal of ERM in symptomatic CHRRPE patients may be beneficial even in older patients. Similar results in a study with older population have been reported by Brue et al.17, supporting results of our study.
Complete PVD is present in most idiopathic ERMs; however, most patients do not have PVD in ERM associated with CHRRPE. Moreover, since complete PVD is not present, the tractional force towards the optic disc may become very strong, resulting in nasal dragging of the foveal center. This nasal dragging may progress in some cases if the traction is not relieved surgically. After relieving the tractional forces via pars plana vitrectomy and ERM removal, the FPD increased in all patients in the operation group. Meanwhile, the FPD in the observation group decreased for all patients. ∆FPD quantifies the degree of dragging of foveal center with respect to the optic nerve, with negative values representing nasal dragging and positive values representing temporal dragging (nasal dragging: ∆FPD < 0, temporal dragging: ∆FPD > 0)13,14. We believe that by relieving the traction and nasal foveal displacement, the anatomical macular structure may be slowly normalized. On the other hand, FPD decreased in patients observed without surgery. In some patients, visual acuity at final follow-up deteriorated significantly (n = 3, 33.3%). Although the relationship between anatomical normalization and functional benefits is debatable, our study shows that operation of ERM in CHRRPE patients results in some normalization of fovea anatomy, while in the absence of a surgical intervention, the fovea may continue to be dragged towards the disc. This is a novel finding that has not been analyzed or published previously.
As a limitation of this study, since this is a retrospective study, it has been difficult to analyze the intentions for why some patients have undergone surgery and some haven’t. Some surgeons may have considered the effects of amblyopia and may not have performed the surgery because they considered that surgery would not benefit the patients if they were amblyopic. The age is the main factor that would determine amblyopia, and since the age between the operation and observation group had no significant difference, we believe that amblyopia may not have been a confounding factor for the comparison of the two groups.
In conclusion, this detailed comparison and analysis of macular structure of CHRRPE patients with and without ERM operation has shown that ERM operation may be beneficial in normalizing the macular anatomy. Although further study is needed with longer follow-up, we believe that early ERM removal of symptomatic CHRRPE patients may be beneficial in preventing amblyopia and functional deterioration of the macula by relieving tractional forces resulting in decreased CMT and normalization of foveal position with respect to the optic disc.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Gass, J. D. An unusual hamartoma of the pigment epithelium and retina simulating choroidal melanoma and retinoblastoma. Trans. Am. Ophthalmol. Soc. 71, 171–183 (1973).
Schachat, A. P. et al. Combined hamartomas of the retina and retinal pigment epithelium. Ophthalmology 91(12), 1609–1615. https://doi.org/10.1016/s0161-6420(84)34094-5 (1984).
Shields, C. L., Mashayekhi, A., Dai, V. V., Materin, M. A. & Shields, J. A. Optical coherence tomographic findings of combined hamartoma of the retina and retinal pigment epithelium in 11 patients. Arch. Ophthalmol. 123(12), 1746–1750. https://doi.org/10.1001/archopht.123.12.1746 (2005).
Chawla, R. et al. Combined hamartoma of the retina and retinal pigment epithelium: An optical coherence tomography-based reappraisal. Am. J. Ophthalmol. 181, 88–96. https://doi.org/10.1016/j.ajo.2017.06.020 (2017).
Ledesma-Gil, G. et al. Presumed natural history of combined hamartoma of the retina and retinal pigment epithelium. Ophthalmol Retina. 5(11), 1156–1163. https://doi.org/10.1016/j.oret.2021.01.011 (2021).
McDonald, H. R., Abrams, G. W., Burke, J. M. & Neuwirth, J. Clinicopathologic results of vitreous surgery for epiretinal membranes in patients with combined retinal and retinal pigment epithelial hamartomas. Am. J. Ophthalmol. 100(6), 806–813. https://doi.org/10.1016/s0002-9394(14)73372-0 (1985).
Mason, J. O. 3rd. & Kleiner, R. Combined hamartoma of the retina and retinal pigment epithelium associated with epiretinal membrane and macular hole. Retina 17(2), 160–162 (1997).
Zhang, X., Dong, F., Dai, R. & Yu, W. Surgical management of epiretinal membrane in combined hamartomas of the retina and retinal pigment epithelium. Retina 30(2), 305–309 (2010).
Ozdek, S. et al. Combined hamartoma of the retina and retinal pigment epithelium at pediatric age: Surgical versus conservative approach. Retina https://doi.org/10.1097/IAE.0000000000003652 (2022).
Quigley, H. A., Brown, A. E., Morrison, J. D. & Drance, S. M. The size and shape of the optic disc in normal human eyes. Arch. Ophthalmol. 108(1), 51–57. https://doi.org/10.1001/archopht.1990.01070030057028 (1990).
Sagong, M., van Hemert, J., Olmos de Koo, L. C., Barnett, C. & Sadda, S. R. Assessment of accuracy and precision of quantification of ultra-widefield images. Ophthalmology 122(4), 864–866. https://doi.org/10.1016/j.ophtha.2014.11.016 (2015).
Nair, U., Mohan, A., Sheera, K. R., Indurkar, A. & Soman, M. Macular morphometrics in foveal displacement following full thickness macular hole surgery. Indian J. Ophthalmol. 68(7), 1436–1440. https://doi.org/10.4103/ijo.IJO_1845_19 (2020).
Kawano, K. et al. Displacement of foveal area toward optic disc after macular hole surgery with internal limiting membrane peeling. Eye (Lond). 27(7), 871–877. https://doi.org/10.1038/eye.2013.99 (2013).
Ishida, M. et al. Retinal displacement toward optic disc after internal limiting membrane peeling for idiopathic macular hole. Am. J. Ophthalmol. 157(5), 971–977. https://doi.org/10.1016/j.ajo.2014.01.026 (2014).
Sun, L. S., Raouf, S., Rhee, D. & Ferrone, P. J. Surgical outcomes of epiretinal membrane removal due to combined hamartoma of the retina and RPE. Ophthalmic Surg. Lasers Imaging Retina. 51(10), 546–554. https://doi.org/10.3928/23258160-20201005-02 (2020).
Konstantinidis, L., Chamot, L., Zografos, L. & Wolfensberger, T. J. Pars Plana vitrectomy and epiretinal membrane peeling for vitreoretinal traction associated with combined hamartoma of the retina and retinal pigment epithelium (CHRRPE). Klin Monbl Augenheilkd. 224(4), 356–359. https://doi.org/10.1055/s-2007-962840 (2007).
Brue, C., Saitta, A., Nicolai, M., Mariotti, C. & Giovannini, A. Epiretinal membrane surgery for combined hamartoma of the retina and retinal pigment epithelium: Role of multimodal analysis. Clin. Ophthalmol. 7, 179–184. https://doi.org/10.2147/OPTH.S39909 (2013).
Acknowledgements
Approval : All experimental protocols were approved by Gangnam Severance Hospital.Informed consent: Due to the retrospective nature of the study, the need to obtain the informed consent was waived by Gangnam Severance Hospital IRB.
Author information
Authors and Affiliations
Contributions
Chul Hee Lee and Min Kim wrote the main manuscript text. Chul Hee Lee and Kang Hyun Kim prepared Figs. 1, 2 and 3. Chul Hee Lee and Young Jae Choi prepared Tables 1, and 2. Jee Myung Yang, Seung Min Lee, Eun Young Choi, and Junwon Lee revised and reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Lee, C.H., Kim, K.H., Choi, Y.J. et al. Changes in macular structure after removal of epiretinal membrane in combined hamartomas of the retina and retinal pigment epithelium. Sci Rep 16, 9462 (2026). https://doi.org/10.1038/s41598-026-39124-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-39124-z