Abstract
Innovation literacy is a critical competency for medical students, yet existing research lacks precise measurement tools. This study aimed to develop a scientific, practical indicator system for evaluating Chinese medical students’ innovation literacy and assess their current level. Using the Delphi expert consultation method, we established an indicator system comprising 3 primary indicators, 6 secondary indicators, and 19 specific items, with weights calculated via the Analytic Hierarchy Process (AHP). A stratified sampling on-site survey was conducted among 584 medical students in Yantai, with data analyzed through descriptive analysis, t-tests, ANOVA, and multiple linear regression. The overall innovation literacy score was 3.16±0.79, significantly influenced by age, grade, and professional category (P < 0.05): older and higher-grade students performed better, while those majoring in medicine and medical engineering outperformed peers in medical management. The indicator system demonstrates scientific weighting and credible results, providing a solid basis for evaluating medical students’ innovation literacy. It highlights the role of innovative thinking andoffers practical guidance for curriculum reform, resource allocation, and faculty development, with policy relevance and replicability across higher education contexts.
Similar content being viewed by others
Introduction
Innovation literacy has become an essential competence for college students in the knowledge economy, serving as a driver of both personal development and societal progress (Cortright et al., 2005). Within medical education, innovation literacy is particularly critical: rapid advances in medical science and the increasing complexity of healthcare demand professionals who can think creatively, solve problems, and adapt to emerging challenges. Medical schools, therefore, play a vital role in equipping future healthcare practitioners with the necessary innovation literacy.
There are several issues in the research on college students’ innovation literacy. Most existing studies focus primarily on educational models (Sun, 2020), teaching methods (Shirazi M, 2020), or the factors influencing innovation literacy (F. Liu et al., 2023), but they often overlook the specific context of specialized schools, such as medical schools. Moreover, there is a lack of comprehensive studies that integrate indicator systems with questionnaire data analysis. As a result, current research often fails to provide accurate insights into the innovation literacy status of medical students (Thys et al., 2014).
This gap has also been highlighted in broader policy discussions. International initiatives such as the OECD’s Learning Framework 2030 have emphasized innovation as a core educational priority (Sklar, 2019). In response, China has undertaken reforms in medical education, including policy initiatives and curriculum improvements to enhance innovation training (Dai et al., 2019; Fu et al., 2022). Despite these efforts, challenges persist, including uneven development of innovation-related competencies, limited institutional resources, and the absence of a standardized evaluation system (Cai et al., 2022; Lucas et al., 2017). These constraints hinder medical schools from accurately diagnosing gaps in students’ innovation literacy and from designing effective interventions.
Therefore, this study aims to develop a scientific innovation literacy indicator system for medical college students and apply it through a cross-sectional observation in China. This approach facilitates the assessment of their current level of innovation literacy, thereby providing a foundation for future curriculum reform and policy development.
Methods
Conceptual model
To evaluate the innovation literacy of medical college students, we adopted the Object-Strategy-Measure (OSM) model as the framework (Keinänen et al., 2018; van Broekhoven et al., 2020; Van Melle et al., 2019; Wang, 2023). This model consists of three core elements: Object, Strategy, and Measure, allowing for a systematic assessment by defining objectives, formulating targeted strategies, and employing precise metrics to measure the achievement of objectives. For the Object, this study was to assess the innovation literacy of medical college students. Based on the European Commission’s Innovation Competence Framework (EU Commission, 2018) and its three-dimensional ‘knowledge-attitudes-skills’ model, we operationalize medical students’ innovation competence through three distinct yet interrelated dimensions: “innovation cognition,” “innovation thinking,” and “innovation ability” (Berkhout et al., 2018; Duval et al., 2023; Ojo and Volkova, 2023). These indicators clearly and effectively represent the study’s objectives.
Delphi expert consultation method
The Delphi expert consultation questionnaire comprises three sections: (a) The questionnaire description. (b) The expert background information. (c) The main body presents the evaluation indicators. Additionally, it includes columns for “comments for deletion” and “suggestions for new indicators.”
This study engaged 16 experts in the field of medical college student innovation and entrepreneurship through correspondence. All participants signed informed consent forms, committing to actively participate in the study and complete two rounds of questionnaires.
During the first round of expert consultation, the consultation questionnaire was distributed to experts either offline or online. After collecting the responses, the indicator items were analyzed based on the experts’ feedback. Adjustments or deletions shall be made based on the inclusion criteria for indicators and expert opinions All modifications were summarized and explained, and the revised evaluation indicator system was used to prepare the second-round consultation questionnaire. One month later, the second round of Delphi consultation was conducted. In this round, experts reached a consensus, confirming that all indicator items met the selection criteria. The evaluation indicator system was finalized.
Expert reliability is assessed based on two factors: expert motivation and expert authority (Nie and Wang, 2024). Kendall’s W test was applied to test the overall consistency of expert opinions. The degree of concentration of expert opinion is analysed by the importance value.
For the specific operational procedures of the Delphi expert consultation method, please refer to the Appendix.
Analytic hierarchy process
To evaluate the relative importance of each indicator, the study utilized the AHP to construct an expert judgment matrix. Experts conducted pairwise comparisons of the indicators to determine their relative significance. The judgment matrix was based on Saaty’s 1–9 scale (Lucas et al., 2017) (see Appendix for detailed scale definitions).
Hierarchical analysis was used to calculate the weights of each indicator, and a consistency test was conducted on the experts’ ratings. The consistency ratio (CR) was calculated, with a CR value of less than 0.10 indicating good consistency (Nie and Wang, 2024). Finally, the experts who passed the consistency test were selected to calculate the average weight of each indicator.
Questionnaire survey for students
We selected a sample of students from two medical colleges in Yantai City, China for the survey. These two institutions were selected because they represent both undergraduate and college, and they are also the largest medical schools in the region. They recruit students nationwide, maintain high enrollment numbers, and thus provide a representative sample. The investigators were trained before the survey to unify the survey terminology. All surveyed students met the following criteria: (a) full-time enrollment; (b) enrollment in medical-related majors; and (c) provision of informed consent and voluntary participation in the survey.
The student survey questionnaire comprises three sections: (a) basic student information, (b) innovation literacy indicator system, and (c) understanding and participation in innovation activities. Specific details on the innovation literacy indicator system are presented in the Results section (Table 3).
This study mainly uses stratified sampling method to carry out the survey, a total of 600 questionnaires were distributed, 584 valid questionnaires, the effective recovery rate is 97.3%. The standardized Cronbach’s Alpha value of the questionnaire in this study is 0.945, and the KMO value of the questionnaire is greater than 0.6, indicating that the questionnaire has good reliability and validity, and is suitable to be used as a measurement tool for the survey and research of medical college students’ innovation literacy.
Data analysis
Statistical analysis was performed using SPSS 26.0. Descriptive statistics were performed on the basic information of the surveyed medical college students, and t-test, ANOVA, and multiple linear regression analyses were used to analyse the influencing factors of medical college students’ innovation literacy. P < 0.05 was taken to mean that the difference was statistically significant.
All students participating in the study sign an informed consent form before data collection to ensure the ethical compliance of the study. Students’ personal information is strictly confidential, and only anonymous data is used in research reports. All data storage and processing comply with relevant data protection regulations.
Results
Indicator of innovation literacy of medical college students
Two rounds of expert consultation were used in this study. The return rate of the questionnaires for both rounds of consultation was 100%, which attests to the high level of motivation of the experts. Eight (50%) and four (25%) experts provided suggestions for changes in the first and second rounds, respectively.
The coefficient of judgement of authority of experts in the first round (Ca=0.875), the coefficient of familiarity (Cs=0.888) and the coefficient of authority (Cr=0.881). The judgement coefficient of the second round (Ca=0.950), familiarity coefficient (Cs=0.981), and authority coefficient (Cr=0.966) can be considered as a high level of authority of the experts who participated in this study.
The coordination degree between the two rounds of expert opinions is very high,as indicated by Kendall’s W values across the hierarchical levels (Table 1). All values were statistically significant (p < 0.05).
The degree of concentration of expert opinions was analyzed using three indices: importance value, full-score rate, and coefficient of variation. Higher importance values and full-score rates, together with lower coefficients of variation, indicate stronger consensus among experts. As shown in Table 2, the concentration of expert opinions improved from the first to the second round of consultation. Specifically, the importance values and full-score rates increased across all indicator levels, while the coefficients of variation decreased, reflecting greater stability and agreement among the experts after iterative feedback.
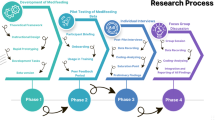
Figure 1 illustrates the Delphi consultation process. In the first round, the team revised three tertiary indicators, deleted six and added one, based on expert opinion. In round 2, the consulting experts only revised some of the wording. Thus, the evaluation system of innovation literacy indicators for medical college students in medical schools was determined, including 3 first-level indicators, 6 second-level indicators and 19 third-level indicators.
Flow diagram of the Delphi process.
Indicator system weight distribution
The innovation literacy indicator system for medical college students, developed through expert consultation and demonstration, consists of three first-level indicators: innovation cognition, innovation thinking, and innovation ability. In terms of comprehensive weight, innovation cognition accounts for 27.6%, innovation thinking for 48.7%, and innovation ability for 23.7%. Finally, the combined weights for the indicators across all levels of the innovation literacy indicator system are determined through comprehensive calculation (Table 3).
Status of the questionnaire
A total of 584 valid questionnaires were collected, as shown in Table 4. The sample demonstrated a balanced gender distribution (54.1% female) and encompassed diverse age groups, type of school undergraduate, and grade level. Participants included students from medical, medical engineering, and medical management programs, with varying achievement ranking and from both rural and urban backgrounds. This diversity strengthens the representativeness of the findings. The survey also investigated the number of student participation in innovation activities, teachers guidance, and understanding of scientific research.
Factors influencing innovation literacy among medical college students
The results of the questionnaire survey were weighted according to the weights of the indicators of medical college students’ innovation literacy, and it was found that the overall score of medical college students’ innovation literacy was 3.16 ± 0.79, and the scores of the three first-level indicators were innovation cognition (0.88 ± 0.24), innovation thinking (1.52 ± 0.45) and innovation ability (0.76 ± 0.22), all of which satisfy normality (Table 5)
After t-test and ANOVA, Table 6 shows that the p-value of the three influencing factors of medical college students’ age, grade level, and professional category is less than 0.05, which can be considered to have an impact on medical college students’ innovation literacy.
Multiple linear regression analyses were conducted using medical college students’ innovation literacy scores as the dependent variable, with age, grade level, and professional category—identified through univariate analysis—as independent variables. The results indicated that age, grade level, and professional category significantly influenced the innovation literacy of medical college students (P < 0.05). Innovation literacy was higher among older students and those in higher grade levels. Additionally, students majoring in medicine and medical engineering exhibited greater innovation literacy compared to those majoring in medical management. (Table 7).
Discussion
This study developed a scientifically grounded indicator system to evaluate innovation literacy among medical college students and applied it in a cross-sectional survey. The system, constructed through Delphi consultation and weighted using the AHP, demonstrated high expert consensus and methodological reliability(Hasson F, 2000; Keeney S, 2006). A questionnaire survey of 584 medical students was conducted to explore their overall level of innovation literacy and its influencing factors. This study not only provides reliable evidence for the assessment of medical students’ innovation literacy but also lays a solid foundation for the subsequent application of this indicator system in medical student groups.
This study successfully established a systematic framework for evaluating innovation literacy among medical college students, filling a gap in existing research where standardized and discipline-specific tools have been lacking. The indicator system comprises three first-level indicators—innovation cognition, innovation thinking, and innovation ability—together with six secondary and 19 tertiary indicators. Among these, innovation thinking received the highest weight (0.487), emphasizing its pivotal role in enabling students to approach problems from multiple perspectives and to translate abstract concepts into practical solutions(Chan, 2013; Ness, 2011). Innovation cognition (0.276) reflects the significance of mastering multidisciplinary knowledge and research tools as a foundation for creativity (Runco, 2004), while innovation ability (0.237) highlights the value of traits such as curiosity, initiative, and persistence in sustaining innovative engagement.(Dai et al., 2019). Compared with prior frameworks that often focused narrowly on creativity or teaching effectiveness(Jin, 2022; Liu et al., 2021), the present system integrates three dimensions, providing a more comprehensive measure of innovation literacy. This approach not only confirms previous evidence regarding the centrality of innovative thinking in higher education(Roberta B. Ness, 2015) but also advances the field by providing a weighted framework tailored to medical education, thereby supporting more accurate evaluation and targeted interventions.
The questionnaire results indicated that the average score for medical students’ innovation literacy was 3.16, reflecting a relatively high level, consistent with previous studies reporting similar findings (Haojie, 2022; Lu et al., 2023; Zhang et al., 2023). A large proportion of respondents (86.2%) reported participation in innovation competitions such as the “Internet + ” and “Challenge Cup,” which are widely recognized as influential platforms in promoting innovation among university students (Wang et al., 2022; Wang, 2025; Yang, 2020). Furthermore, the questionnaire survey indicates that 79.3% of medical students have received guidance on innovation projects from at least one teacher, while 66% reported awareness of scientific research. These results align with earlier evidence highlighting the growing role of institutional support and the increasing visibility of innovation-related activities within medical education (Hua et al., 2022). These situations reflect the influence of China’s national policies, particularly the National Innovation-Driven Development Strategy and the Ministry of Education’s emphasis on integrating “innovation and entrepreneurship education” into higher education curricula. Initiatives such as the “Double First-Class” construction plan and the Education Modernization 2035 roadmap have enhanced student innovation literacy.
Statistical analyses revealed significant associations between innovation literacy and age, grade level, and professional category. Older students and those in higher academic years obtained higher scores, which is consistent with previous studies suggesting that increasing maturity, cognitive development, and accumulated learning experiences are linked to higher levels of innovation competence (Burdett and Ronfard, 2023; Chen, 2025; Hua et al., 2022). Among professional categories, students majoring in medicine and medical engineering achieved significantly higher scores compared with those in medical management. This pattern echoes earlier findings that disciplines at the forefront of addressing pressing societal challenges, such as medicine, tend to emphasize creativity and forward-thinking skills in their training objectives (Lechler, 2017; Stage EK, 2013). In contrast, medical management students’ relatively lower scores may reflect curricula that focus more heavily on theoretical knowledge, with comparatively less emphasis on practical or innovative skill development (Martins et al., 2019).
Suggestions
Our study has several suggestions. From a governmental perspective, it is essential to deepen the reform of innovation education in higher education institutions. The reform should focus on fully exploring the innovation potential of medical students, stimulating their interest in innovation, enhancing their innovation literacy, and closely integrating innovation education with values education and professional training, with an emphasis on cultivating innovative thinking. Higher education institutions, in turn, should prioritize the development of a comprehensive innovation training system, strengthen faculty capabilities, and pay particular attention to the innovation cultivation of lower-grade and medical management students. Student performance evaluations should emphasize innovation literacy and provide appropriate incentives to encourage student enthusiasm. For medical students, it is crucial to master extensive professional knowledge, strengthen their knowledge system, and cultivate independent thinking to develop innovation literacy. Actively participating in innovation competitions and practical projects can help students integrate theory with practice, further enhancing their innovation literacy.
Advantages
This study has several advantages. Firstly, as far as we know, this is the first article to establish a comprehensive indicator system specifically designed to assess medical students’ innovation literacy and to analyze its current status. While previous research has primarily focused on teaching quality or evaluations of individual abilities—often overlooking innovation literacy—our study addresses this gap by proposing a scientifically grounded and content-rich indicator system tailored for medical students. (Dai et al., 2019; Nie and Wang, 2024; J. Wu et al., 2023; Z. Wu et al., 2023), Secondly, unlike earlier studies that tend to emphasize either the construction of innovation indicators or the assessment of innovation status in isolation (F. Liu et al., 2023; J. Liu et al., 2023; Shen et al., 2019), our research integrates both dimensions, thereby offering a more holistic perspective.
Limitations
Our study has several limitations. Firstly, due to constraints research time, we selected only 16 experts from two medical schools in Yantai, China, to participate in the Delphi survey. The Delphi method and AHP were used to construct the innovation literacy indicator system for medical college students. However, these methods rely on the subjective judgment of experts and lack face-to-face interaction, which may result in the omission of alternative perspectives. Consequently, the research findings may be biased. Secondly, due to financial constraints, the questionnaire survey and data analysis were limited to students from two medical colleges in Yantai, China. While this provided valuable insights, the small sample size and the institutional characteristics of these universities—such as their emphasis on innovation training, available resources, and local educational policies—may have influenced the results. Consequently, the findings may not fully reflect the situation in other types of institutions or regions.
Conclusions
In this study, we developed and validated an innovation literacy indicator system tailored for medical college students and applied it to assess their current levels of innovation literacy. The findings highlight the central role of innovation thinking, alongside the contributions of innovation cognition and innovation ability, in shaping students’ overall literacy. These results carry several important implications. For policymakers and university administrators, the indicator system provides a practical framework for evaluating and monitoring the effectiveness of innovation education initiatives, thereby offering evidence to guide curriculum reform, resource allocation, and faculty development. For educators, the system can serve as a diagnostic tool to identify gaps in students’ innovation literacy and to design targeted interventions, particularly for junior students and those in medical management programs. Beyond the immediate context, the framework has the potential to be adapted and replicated in other higher education settings, both within and beyond China, thereby contributing to broader comparative research on innovation literacy.
Data availability
All data generated or analysed during this study are included in this article. Further enquiries can be directed to the corresponding author.
References
Berkhout JJ, Helmich E, Teunissen PW, van der Vleuten CPM, Jaarsma ADC (2018) Context matters when striving to promote active and lifelong learning in medical education. Med Educ 52(1):34–44. https://doi.org/10.1111/medu.13463
Burdett ERR, Ronfard S (2023) Tinkering to innovation: how children refine tools over multiple attempts. Dev Psychol 59(6):1006–1016. https://doi.org/10.1037/dev0001512
Cai Q, Cheng Y, Ke Y (2022) Construction of evaluation index system for training quality of high-level tennis team. Front Psychol 13:902516. https://doi.org/10.3389/fpsyg.2022.902516
Chan ZCY (2013) A systematic review of creative thinking/creativity in nursing education. Nurse Educ Today 33(11):1382–1387. https://doi.org/10.1016/j.nedt.2012.09.005
Chen P, Liu H, Ma Y, Jiang F (2025) Executives’ postgraduate education and corporate ambidextrous innovation evidence from China’s listed companies. Humanit Soc Sci Commun 12:211. https://doi.org/10.1057/s41599-025-04426-6
Cortright RN, Collins HL, DiCarlo SE (2005) Peer instruction enhanced meaningful learning: ability to solve novel problems. Adv Physiol Educ 29(2):107–111. https://doi.org/10.1152/advan.00060.2004
Dai F, Wei K, Chen Y, Ju M (2019) Construction of an index system for qualitative evaluation of undergraduate nursing students innovative ability: a Delphi study. J Clin Nurs 28(23-24):4379–4388. https://doi.org/10.1111/jocn.15020
Duval PE, Fornari E, Décaillet M, Ledoux JB, Beaty RE, Denervaud S (2023) Creative thinking and brain network development in schoolchildren. Dev Sci 26(6):e13389. https://doi.org/10.1111/desc.13389
Fu X, Wu X, Liu D, Zhang C, Xie H, Wang Y, Xiao L (2022) Practice and exploration of the “student-centered” multielement fusion teaching mode in human anatomy. Surg Radiologic Anat 44(1):15–23. https://doi.org/10.1007/s00276-021-02866-8
Haojie G (2022) Innovation and entrepreneurship strategies of teachers and students in financial colleges and universities under the direction of food security. Front Psychol 13:848554. https://doi.org/10.3389/fpsyg.2022.848554
Hasson F, Keeney S, McKenna H (2000) Research guidelines for the Delphi survey technique. J Adv Nurs 32(4):1008–1015
Hua J, Zheng K, Fan S (2022) The impact of entrepreneurial activities and college students’ entrepreneurial abilities in higher education—A meta-analytic path. Front Psychol 13:843978. https://doi.org/10.3389/fpsyg.2022.843978
Jin Y (2022) Analysis of college students’ entrepreneurship education and entrepreneurial psychological quality from the perspective of ideological and political education. Front Psychol 13:739353. https://doi.org/10.3389/fpsyg.2022.739353
Keeney S, Hasson F, McKenna H (2006) Consulting the oracle: ten lessons from using the Delphi technique in nursing research. J Adv Nurs 53(2):205–212
Keinänen M, Ursin J, Nissinen K (2018) How to measure students’ innovation competences in higher education: Evaluation of an assessment tool in authentic learning environments. Stud Educ Eval 58:30–36. https://doi.org/10.1016/j.stueduc.2018.05.007
Lechler R (2017) Diversity, creativity, and flexibility will be needed from the next generation of medical scientists. Lancet 389:S1. https://doi.org/10.1016/s0140-6736(17)30199-x
Liu F, Qu S, Fan Y, Chen F, He B (2023) Scientific creativity and innovation ability and its determinants among medical postgraduate students in Fujian province of China: a cross sectional study. BMC Med Educ 23(1):444. https://doi.org/10.1186/s12909-023-04408-9
Liu J, Qiu H, Zhang X, He F (2023) Construction of a competency index system for shift nurses in China: a Delphi study. Nurs Open 10(8):5638–5648. https://doi.org/10.1002/nop2.1809
Liu T, Yu X, Liu M, Wang M, Zhu X, Yang X (2021) A mixed method evaluation of an integrated course in improving critical thinking and creative self-efficacy among nursing students. Nurse Educ Today 106:105067. https://doi.org/10.1016/j.nedt.2021.105067
Lu Q, Chai Y, Ren L, Ren P, Zhou J, Lin C (2023) Research on quality evaluation of innovation and entrepreneurship education for college students based on random forest algorithm and logistic regression model. PeerJ Computer Sci 9:e1329. https://doi.org/10.7717/peerj-cs.1329
Lucas RI, Promentilla MA, Ubando A, Tan RG, Aviso K, Yu KD (2017) An AHP-based evaluation method for teacher training workshop on information and communication technology. Eval Program Plan 63:93–100. https://doi.org/10.1016/j.evalprogplan.2017.04.002
Martins JM, Isouard G, Freshman B (2019) Human dimension of health service management. Aust Health Rev 43(1):103–110. https://doi.org/10.1071/ah17063
Ness RB (2011) Commentary: teaching creativity and innovative thinking in medicine and the health sciences. Acad Med 86(10):1201–1203. https://doi.org/10.1097/ACM.0b013e31822bbb9f
Nie S, Wang L (2024) Constructing an evaluation index system for clinical nursing practice teaching quality using a Delphi method and analytic hierarchy process-based approach. BMC Med Educ 24(1):772. https://doi.org/10.1186/s12909-024-05770-y
Ojo KS, Volkova NV (2023) Modelling Innovation competence profiles: the empowering roles of self-monitoring and resilience. BMC Psychol 11(1):293. https://doi.org/10.1186/s40359-023-01340-x
Ness RB (2015) Promoting innovative thinking. Am J Public Health 105(S1):S114–S118. https://doi.org/10.2105/AJPH.2014.302365
Runco MA (2004) Creativity. Annu Rev Psychol 55(1):657–687. https://doi.org/10.1146/annurev.psych.55.090902.141502
Shen L, Yang J, Jin X, Hou L, Shang S, Zhang Y (2019) Based on Delphi method and analytic hierarchy process to construct the Evaluation Index system of nursing simulation teaching quality. Nurse Educ Today 79:67–73. https://doi.org/10.1016/j.nedt.2018.09.021
Shirazi M, Shariati MM, Hosseini M, Dehshiri AS (2020) Technical simulation using goldfish bowl method: a medical teaching method for increasing student’s creativity. Arch Iran Med 23(1):37–43
Sklar DP (2019) Looking ahead: futures planning for medical education. Acad Med 94(10):1401–1403. https://doi.org/10.1097/acm.0000000000002861
Stage EK, Asturias H, Cheuk T, Daro PA, Hampton SB (2013) Science education. Opportunities and challenges in next generation standards. Science 340(6130):276–277. https://doi.org/10.1126/science.1234011
Sun X (2020) Exploration and Practice of “Internet + Maker Education” University Innovative entrepreneurship education model from the perspective of positive psychology. Front Psychol 11:891. https://doi.org/10.3389/fpsyg.2020.00891
Thys E, Sabbe B, De Hert M (2014) The assessment of creativity in creativity/psychopathology research – a systematic review. Cogn Neuropsychiatry 19(4):359–377. https://doi.org/10.1080/13546805.2013.877384
van Broekhoven K, Cropley D, Seegers P (2020) Differences in creativity across Art and STEM students: We are more alike than unalike. Think Skills Creativity 38:784225. https://doi.org/10.1016/j.tsc.2020.100707
Van Melle E, Frank JR, Holmboe ES, Dagnone D, Stockley D, Sherbino J (2019) A core components framework for evaluating implementation of competency-based medical education programs. Acad Med 94(7):1002–1009. https://doi.org/10.1097/acm.0000000000002743
Wang J, Guo Y, Zhang M, Li N, Li K, Li P, Huang Y (2022) The impact of entrepreneurship competitions on entrepreneurial competence of Chinese College Students. Front Psychol 13:784225. https://doi.org/10.3389/fpsyg.2022.784225
Wang J, Wang H (2025) Cultivation of innovative thinking and career development in design education. Humanit Soc Sci Commun 12:1390. https://doi.org/10.1057/s41599-025-05754-3
Wang, R (2023). Research on WBS-RBS Oriented Security Risk Assessment Index System for Space Domain Private Network. J Phys Conf Ser, 2489(1). https://doi.org/10.1088/1742-6596/2489/1/012021
Wu J, Wang F, Wang J, Yuan R, Lv Y, Tao D, Hu L (2023) Construction of an index system of core competence assessment for otolaryngology nurse specialists in China: a Delphi study. Nurse Educ Today 131:105956. https://doi.org/10.1016/j.nedt.2023.105956
Wu Z, Huang W, Ding Y, Jiang L, Zhao Y, Zhu X, Huang J (2023) Construction of an evaluation index system of core competencies for critical care blood purification nurses in China: a Delphi study. Nurse Educ Pract 72: 103751. https://doi.org/10.1016/j.nepr.2023.103751
Yang Y (2020) Exploration and practice of maker education mode in innovation and entrepreneurship education. Front Psychol 11:1626. https://doi.org/10.3389/fpsyg.2020.01626
Zhang H, Zhang D, Jin Y (2023) Does expansion of college education benefit urban entrepreneurship and innovation in China?. Heliyon 9(11):e21813. https://doi.org/10.1016/j.heliyon.2023.e21813
Acknowledgements
Shandong Provincial Education Science Planning Special Project on Innovation Literacy: Research on Establishing a Collaborative College Student Innovation Literacy Cultivation System Among Multiple Stakeholders in Medical Institutions in the Big Data Era (2022CYB267).
Author information
Authors and Affiliations
Contributions
Ronghang Liu, Xiuqing Li, Chuyun Liu, Surong Zhao, contributed to the development of the study and analysis of the data and the writing, Meijing Yang, Xiaoqian Shao, Wanru Zhao, Yitong Jiang, Haozheng Wang contributed to the participation in the Delphi method expert survey and questionnaire. Chunlei Han, Zhang Cao, Guangcheng Wang contributed to the conception and design of the study and critically revised all versions of the manuscript. All authors have read and approved the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
All study procedures were approved by Binzhou Medical University Hospital Ethics Committee, approved number KYLL-127, approved time September 2022. The scope of approval covers the entire research process. All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
In November 2022, prior to the commencement of the survey, the investigator provided participants with a written informed consent form. All participants were required to review and sign the informed consent form. The consent form outlined the study’s purpose (e.g., understanding the current level of student innovation literacy), the use of the collected data (i.e., solely for scientific research and publication purposes with no personally identifiable information retained), the assurance of participant anonymity, the confidentiality of private information, participant rights (including the right of withdrawal at any time without punishment), and no potential risk of this survey. All participants were fully informed and had signed the informed consent form before the formal survey was initiated.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Liu, R., Li, X., Liu, C. et al. Construction of innovation literacy indicator system for medical college students and analysis of current situation based on a cross-sectional observation in China. Humanit Soc Sci Commun 13, 55 (2026). https://doi.org/10.1057/s41599-025-06352-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1057/s41599-025-06352-z