Abstract
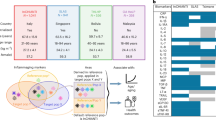
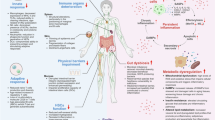
Inflammaging describes a chronic, systemic, low-grade inflammatory state that is recognized as a major risk factor for age-related diseases (ARDs) and a pivotal convergence point of multiple biological mechanisms involved in aging. Here, we discuss the heterogeneity of inflammaging, proposing that it emerges as a consequence of each individual’s lifelong exposures to inflammatory stimuli, shaped by a unique combination of genetics, lifestyle, socioeconomic conditions and environmental factors such as infections and pollution. Through this lens, we then discuss measuring inflammaging, describing the development of inflammatory clocks that quantify inflammatory age and show strong associations with ARD incidence as well as how other aging clocks intersect with inflammaging. Finally, we consider interventions that may counteract inflammaging, including nutritional interventions, physical activity and gerotherapies such as senolytics. We propose that deepening our knowledge of the individual nature of inflammaging stands to enhance our understanding of personalized aging trajectories and inform precision interventions.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Franceschi, C. et al. Inflamm‐aging: an evolutionary perspective on immunosenescence. Ann. N. Y. Acad. Sci. 908, 244–254 (2000).
Franceschi, C., Garagnani, P., Parini, P., Giuliani, C. & Santoro, A. Inflammaging: a new immune–metabolic viewpoint for age-related diseases. Nat. Rev. Endocrinol. 14, 576–590 (2018).
Fulop, T. et al. Immunology of aging: the birth of inflammaging. Clin. Rev. Allergy Immunol. 64, 109–122 (2021).
Santoro, A., Bientinesi, E. & Monti, D. Immunosenescence and inflammaging in the aging process: age-related diseases or longevity? Ageing Res. Rev. 71, 101422 (2021).
Franceschi, C. et al. The network and the remodeling theories of aging: historical background and new perspectives. Exp. Gerontol. 35, 879–896 (2000).
Fulop, T., Witkowski, J. M., Olivieri, F. & Larbi, A. The integration of inflammaging in age-related diseases. Semin. Immunol. 40, 17–35 (2018).
Kerepesi, C., Zhang, B., Lee, S.-G., Trapp, A. & Gladyshev, V. N. Epigenetic clocks reveal a rejuvenation event during embryogenesis followed by aging. Sci. Adv. 7, eabg6082 (2021).
Franceschi, C., Ostan, R. & Santoro, A. Nutrition and inflammation: are centenarians similar to individuals on calorie-restricted diets? Annu. Rev. Nutr. 38, 329–356 (2018).
Fulop, T. et al. Immunosenescence and inflamm-aging as two sides of the same coin: friends or foes? Front. Immunol. 8, 1960 (2018).
Remondini, D. et al. Identification of a T cell gene expression clock obtained by exploiting a MZ twin design. Sci. Rep. 7, 6005 (2017).
Franceschi, C. et al. Immunobiography and the heterogeneity of immune responses in the elderly: a focus on inflammaging and trained immunity. Front. Immunol. 8, 982 (2017).
Audi, R The Cambridge Dictionary of Philosophy (Cambridge Univ. Press, 1999).
Brodin, P. & Davis, M. M. Human immune system variation. Nat. Rev. Immunol. 17, 21–29 (2017).
Brodin, P. et al. Variation in the human immune system is largely driven by non-heritable influences. Cell 160, 37–47 (2015).
Lyons, C. E. et al. Chronic social stress induces p16-mediated senescent cell accumulation in mice. Nat. Aging 5, 48–64 (2024).
Marfella, R. et al. Microplastics and nanoplastics in atheromas and cardiovascular events. N. Engl. J. Med. 390, 900–910 (2024).
Kwiatkowska, K. M. et al. Heterogeneity of cellular senescence: cell type-specific and senescence stimulus-dependent epigenetic alterations. Cells 12, 927 (2023).
Muscatell, K. A., Brosso, S. N. & Humphreys, K. L. Socioeconomic status and inflammation: a meta-analysis. Mol. Psychiatry 25, 2189–2199 (2020).
Hamilton, O. S. & Steptoe, A. Socioeconomic determinants of inflammation and neuroendocrine activity: a longitudinal analysis of compositional and contextual effects. Brain Behav. Immun. 107, 276–285 (2023).
Kivimäki, M. et al. Social disadvantage accelerates aging. Nat. Med. 31, 1635–1643 (2025).
Natale, B. N. et al. Systemic inflammation contributes to the association between childhood socioeconomic disadvantage and midlife cardiometabolic risk. Ann. Behav. Med. 57, 26–37 (2023).
Gireesh, A., Sacker, A., McMunn, A. & Cadar, D. Role of inflammation in the socioeconomic inequalities of neurocognitive disorders. Brain Behav. Immun. 113, 203–211 (2023).
Noppert, G. A., Stebbins, R. C., Dowd, J. B. & Aiello, A. E. Socioeconomic and race/ethnic differences in immunosenescence: evidence from the Health and Retirement Study. Brain Behav. Immun. 107, 361–368 (2023).
Ye, X. et al. Associations of socioeconomic status with infectious diseases mediated by lifestyle, environmental pollution and chronic comorbidities: a comprehensive evaluation based on UK Biobank. Infect. Dis. Poverty 12, 5 (2023).
Tang, B., Li, Z., Hu, S. & Xiong, J. Economic implications of health care burden for elderly population. Inquiry 59, 469580221121511 (2022).
Solovev, I. et al. Aging and physiological barriers: mechanisms of barrier integrity changes and implications for age-related diseases. Mol. Biol. Rep. 51, 917 (2024).
Franceschi, C., Garagnani, P., Vitale, G., Capri, M. & Salvioli, S. Inflammaging and ‘garb-aging’. Trends Endocrinol. Metab. 28, 199–212 (2017).
Franceschi, C. et al. Inflammaging and anti-inflammaging: a systemic perspective on aging and longevity emerged from studies in humans. Mech. Ageing Dev. 128, 92–105 (2007).
Olivieri, F., Prattichizzo, F., Lattanzio, F., Bonfigli, A. R. & Spazzafumo, L. Antifragility and antiinflammaging: can they play a role for a healthy longevity? Ageing Res. Rev. 84, 101836 (2023).
Furman, D. et al. Chronic inflammation in the etiology of disease across the life span. Nat. Med. 25, 1822–1832 (2019).
Santoro, A. et al. Inflammaging, hormesis and the rationale for anti-aging strategies. Ageing Res. Rev. 64, 101142 (2020).
Storci, G. et al. Genomic stability, anti-inflammatory phenotype, and up-regulation of the RNAseH2 in cells from centenarians. Cell Death Differ. 26, 1845–1858 (2019).
Sayed, N. et al. An inflammatory aging clock (iAge) based on deep learning tracks multimorbidity, immunosenescence, frailty and cardiovascular aging. Nat. Aging 1, 598–615 (2021).
Baker, C., Kim, M. & Benayoun, B. A. A researcher’s guide to studying sex differences in immune aging. Trends Mol. Med. https://doi.org/10.1016/j.molmed.2025.01.005 (2025).
Márquez, E. J. et al. Sexual-dimorphism in human immune system aging. Nat. Commun. 11, 751 (2020).
Martínez de Toda, I. et al. Sex differences in markers of oxidation and inflammation. Implications for ageing. Mech. Ageing Dev. 211, 111797 (2023).
Ostan, R. et al. Gender, aging and longevity in humans: an update of an intriguing/neglected scenario paving the way to a gender-specific medicine. Clin. Sci. 130, 1711–1725 (2016).
de Assunção Cortez Corrêa, L. C., Raffin, J., Vellas, B., Guerra, R. O. & de Souto Barreto, P. Sex-specific associations of neurodegeneration and inflammatory biomarkers with intrinsic capacity in older adults: findings from the 4-year longitudinal Multidomain Alzheimer’s Prevention Trial (MAPT). Maturitas 193, 108191 (2025).
Bronikowski, A. M. et al. Sex‐specific aging in animals: perspective and future directions. Aging Cell 21, e13542 (2022).
Ungvari, A. et al. Sex-specific mechanisms in vascular aging: exploring cellular and molecular pathways in the pathogenesis of age-related cardiovascular and cerebrovascular diseases. Geroscience 47, 301–337 (2025).
Barbieri, M. et al. Is it time to revise the fighting strategy toward type 2 diabetes? Sex and pollution as new risk factors. Ageing Res. Rev. 99, 102405 (2024).
Olivieri, F. et al. Sex/gender-related differences in inflammaging. Mech. Ageing Dev. 211, 111792 (2023).
Tylutka, A., Walas, Ł. & Zembron-Lacny, A. Level of IL-6, TNF, and IL-1β and age-related diseases: a systematic review and meta-analysis. Front. Immunol. 15, 1330386 (2024).
Kalyakulina, A. et al. Inflammaging markers in the extremely cold climate: a case study of Yakutian population. Int. J. Mol. Sci. 25, 13741 (2024).
Alpert, A. et al. A clinically meaningful metric of immune age derived from high-dimensional longitudinal monitoring. Nat. Med. 25, 487–495 (2019).
Yusipov, I. et al. Accelerated epigenetic aging and inflammatory/immunological profile (ipAGE) in patients with chronic kidney disease. Geroscience 44, 817–834 (2022).
Kalyakulina, A., Yusipov, I., Moskalev, A., Franceschi, C. & Ivanchenko, M. Explainable artificial intelligence (XAI) in aging clock models. Ageing Res. Rev. 93, 102144 (2024).
Markov, N. T. et al. Age-related brain atrophy is not a homogenous process: different functional brain networks associate differentially with aging and blood factors. Proc. Natl Acad. Sci. USA 119, e2207181119 (2022).
Widjaja, A. A. et al. Inhibition of IL-11 signalling extends mammalian healthspan and lifespan. Nature 632, 157–165 (2024).
Lehallier, B. et al. Undulating changes in human plasma proteome profiles across the lifespan. Nat. Med. 25, 1843–1850 (2019).
Lehallier, B., Shokhirev, M. N., Wyss‐Coray, T. & Johnson, A. A. Data mining of human plasma proteins generates a multitude of highly predictive aging clocks that reflect different aspects of aging. Aging Cell 19, e13256 (2020).
Argentieri, M. A. et al. Proteomic aging clock predicts mortality and risk of common age-related diseases in diverse populations. Nat. Med. 30, 2450–2460 (2024).
Hällqvist, J. et al. Plasma proteomics identify biomarkers predicting Parkinson’s disease up to 7 years before symptom onset. Nat. Commun. 15, 4759 (2024).
Horvath, S. & Raj, K. DNA methylation-based biomarkers and the epigenetic clock theory of ageing. Nat. Rev. Genet. 19, 371–384 (2018).
Crimmins, E. M., Klopack, E. T. & Kim, J. K. Generations of epigenetic clocks and their links to socioeconomic status in the Health and Retirement Study. Epigenomics 16, 1031–1042 (2024).
Yusipov, I., Kalyakulina, A., Trukhanov, A., Franceschi, C. & Ivanchenko, M. Map of epigenetic age acceleration: a worldwide analysis. Ageing Res. Rev. 100, 102418 (2024).
Zaghlool, S. B. et al. Epigenetics meets proteomics in an epigenome-wide association study with circulating blood plasma protein traits. Nat. Commun. 11, 15 (2020).
Stevenson, A. J. et al. Characterisation of an inflammation-related epigenetic score and its association with cognitive ability. Clin. Epigenetics 12, 113 (2020).
Stevenson, A. J. et al. Creating and validating a DNA methylation-based proxy for interleukin-6. J. Gerontol. A Biol. Sci. Med. Sci. 76, 2284–2292 (2021).
Gadd, D. A. et al. Correction: Epigenetic scores for the circulating proteome as tools for disease prediction. eLife 12, e94481 (2023).
Bernabeu, E. et al. Refining epigenetic prediction of chronological and biological age. Genome Med. 15, 12 (2023).
Kalyakulina, A. et al. EpInflammAge: epigenetic-inflammatory clock for disease-associated biological aging based on deeplearning. Int. J. Mol. Sci. 26, 6284 (2025).
Ahadi, S. et al. Personal aging markers and ageotypes revealed by deep longitudinal profiling. Nat. Med. 26, 83–90 (2020).
Prattichizzo, F. et al. Organ-specific biological clocks: ageotyping for personalized anti-aging medicine. Ageing Res. Rev. 96, 102253 (2024).
Jung, A. M. et al. Associations between epigenetic age acceleration and microRNA expression among U.S. firefighters. Epigenet. Insights 16, 25168657231206301 (2023).
Salignon, J. et al. Age prediction from human blood plasma using proteomic and small RNA data: a comparative analysis. Aging 15, 5240–5265 (2023).
Roig-Genoves, J. V., García-Giménez, J. L. & Mena-Molla, S. A miRNA-based epigenetic molecular clock for biological skin-age prediction. Arch. Dermatol. Res. 316, 326 (2024).
Martucci, M. et al. Mediterranean diet and inflammaging within the hormesis paradigm. Nutr. Rev. 75, 442–455 (2017).
Izquierdo, M. et al. International Exercise Recommendations in Older Adults (ICFSR): expert consensus guidelines. J. Nutr. Health Aging 25, 824–853 (2021).
Gensous, N. et al. One-year Mediterranean diet promotes epigenetic rejuvenation with country- and sex-specific effects: a pilot study from the NU-AGE project. Geroscience 42, 687–701 (2020).
Gialluisi, A. et al. Epidemiological and genetic overlap among biological aging clocks: new challenges in biogerontology. Ageing Res. Rev. 72, 101502 (2021).
Ghosh, T. S. et al. Mediterranean diet intervention alters the gut microbiome in older people reducing frailty and improving health status: the NU-AGE 1-year dietary intervention across five European countries. Gut 69, 1218–1228 (2020).
Moskalev, A. et al. Targeting aging mechanisms: pharmacological perspectives. Trends Endocrinol. Metab. 33, 266–280 (2022).
Di Giosia, P. et al. The role of nutrition in inflammaging. Ageing Res. Rev. 77, 101596 (2022).
Casas, R. et al. The effects of the Mediterranean diet on biomarkers of vascular wall inflammation and plaque vulnerability in subjects with high risk for cardiovascular disease. A randomized trial. PLoS ONE 9, e100084 (2014).
Firth, J. et al. The effects of dietary improvement on symptoms of depression and anxiety: a meta-analysis of randomized controlled trials. Psychosom. Med. 81, 265–280 (2019).
Longo, V. D. et al. Interventions to slow aging in humans: are we ready? Aging Cell 14, 497–510 (2015).
de Cabo, R. & Mattson, M. P. Effects of intermittent fasting on health, aging, and disease. N. Engl. J. Med. 381, 2541–2551 (2019).
Mercken, E. M. et al. Calorie restriction in humans inhibits the PI3K/AKT pathway and induces a younger transcription profile. Aging Cell 12, 645–651 (2013).
Kittana, M., Apostolopoulos, V. & Stojanovska, L. in Biochemistry and Cell Biology of Ageing: Part V, Anti-Ageing Interventions (eds Korolchuk, V. I. & Harris, J. R.) 173–181 (Springer, 2024).
Trichopoulou, A. et al. Definitions and potential health benefits of the Mediterranean diet: views from experts around the world. BMC Med. 12, 112 (2014).
Fadnes, L. T., Økland, J.-M., Haaland, Ø. A. & Johansson, K. A. Estimating impact of food choices on life expectancy: a modeling study. PLoS Med. 19, e1003889 (2022).
Kahleova, H., Levin, S. & Barnard, N. Cardio-metabolic benefits of plant-based diets. Nutrients 9, 848 (2017).
Casas, R. et al. Long-term immunomodulatory effects of a Mediterranean diet in adults at high risk of cardiovascular disease in the Prevención con Dieta Mediterránea (PREDIMED) randomized controlled trial. J. Nutr. 146, 1684–1693 (2016).
Margină, D. et al. Chronic inflammation in the context of everyday life: dietary changes as mitigating factors. Int. J. Environ. Res. Public Health 17, 4135 (2020).
Berendsen, A. et al. A parallel randomized trial on the effect of a healthful diet on inflammageing and its consequences in European elderly people: design of the NU-AGE dietary intervention study. Mech. Ageing Dev. 134, 523–530 (2013).
Santoro, A. et al. Combating inflammaging through a Mediterranean whole diet approach: the NU-AGE project’s conceptual framework and design. Mech. Ageing Dev. 136–137, 3–13 (2014).
Ostan, R. et al. Cross-sectional analysis of the correlation between daily nutrient intake assessed by 7-day food records and biomarkers of dietary intake among participants of the NU-AGE study. Front. Physiol. 9, 1359 (2018).
Berendsen, A. A. M. et al. Changes in dietary intake and adherence to the NU-AGE diet following a one-year dietary intervention among European older adults—results of the NU-AGE randomized trial. Nutrients 10, 1905 (2018).
Marseglia, A. et al. Effect of the NU-AGE diet on cognitive functioning in older adults: a randomized controlled trial. Front. Physiol. 9, 349 (2018).
Jennings, A. et al. A Mediterranean-like dietary pattern with vitamin D3 (10 µg/d) supplements reduced the rate of bone loss in older Europeans with osteoporosis at baseline: results of a 1-y randomized controlled trial. Am. J. Clin. Nutr. 108, 633–640 (2018).
Maijo, M. et al. One-year consumption of a Mediterranean-like dietary pattern with vitamin D3 supplements induced small scale but extensive changes of immune cell phenotype, co-receptor expression and innate immune responses in healthy elderly subjects: results from the United Kingdom arm of the NU-AGE trial. Front. Physiol. 9, 997 (2018).
van Soest, A. P. M. et al. Associations between pro- and anti-inflammatory gastro-intestinal microbiota, diet, and cognitive functioning in Dutch healthy older adults: the NU-AGE study. Nutrients 12, 3471 (2020).
Biagi, E. et al. Through ageing, and beyond: gut microbiota and inflammatory status in seniors and centenarians. PLoS ONE 5, e10667 (2010).
Golshany, H. et al. The gut microbiome across the lifespan: how diet modulates our microbial ecosystem from infancy to the elderly. Int. J. Food Sci. Nutr. 76, 95–121 (2024).
Lazou-Ahrén, I. et al. Probiotic-reduced inflammaging in older adults: a randomized, double-blind, placebo-controlled trial. Probiotics Antimicrob. Proteins https://doi.org/10.1007/s12602-024-10310-7 (2024).
Roberts, J. L. et al. Bifidobacterium longum supplementation improves age‐related delays in fracture repair. Aging Cell 22, e13786 (2023).
Wang, X., Wang, T., Zhang, Q., Xu, L. & Xiao, X. Dietary supplementation with inulin modulates the gut microbiota and improves insulin sensitivity in prediabetes. Int. J. Endocrinol. 2021, 5579369 (2021).
Claesson, M. J. et al. Gut microbiota composition correlates with diet and health in the elderly. Nature 488, 178–184 (2012).
Liu, T. et al. Hesperidin and fecal microbiota transplantation modulate the composition of the gut microbiota and reduce obesity in high fat diet mice. Diabetes Metab. Syndr. Obes. 17, 3643–3656 (2024).
Novelle, M. G., Naranjo-Martínez, B., López-Cánovas, J. L. & Díaz-Ruiz, A. Fecal microbiota transplantation, a tool to transfer healthy longevity. Ageing Res. Rev. 103, 102585 (2025).
Santoro, A. et al. A cross-sectional analysis of body composition among healthy elderly from the European NU-AGE study: sex and country specific features. Front. Physiol. 9, 1693 (2018).
Santoro, A. et al. Gender-specific association of body composition with inflammatory and adipose-related markers in healthy elderly Europeans from the NU-AGE study. Eur. Radiol. 29, 4968–4979 (2019).
Ribeiro, I. S. et al. Regular physical activity reduces the effects of inflammaging in diabetic and hypertensive men. Exp. Gerontol. 155, 111558 (2021).
Antuña, E. et al. Inflammaging: implications in sarcopenia. Int. J. Mol. Sci. 23, 15039 (2022).
Izquierdo, M. et al. Global consensus on optimal exercise recommendations for enhancing healthy longevity in older adults (ICFSR). J. Nutr. Health Aging 29, 100401 (2025).
Duggal, N. A., Pollock, R. D., Lazarus, N. R., Harridge, S. & Lord, J. M. Major features of immunesenescence, including reduced thymic output, are ameliorated by high levels of physical activity in adulthood. Aging Cell 17, e12750 (2018).
Moradell, A., Casajús, J. A., Moreno, L. A. & Vicente-Rodríguez, G. Perspectives on diet and exercise interaction for healthy aging: opportunities to reduce malnutrition risk and optimize fitness. Nutrients 17, 596 (2025).
Petersen, A. M. W. & Pedersen, B. K. The anti-inflammatory effect of exercise. J. Appl. Physiol. 98, 1154–1162 (2005).
Docherty, S. et al. The effect of exercise on cytokines: implications for musculoskeletal health: a narrative review. BMC Sports Sci. Med. Rehabil. 14, 5 (2022).
Farley, M. J. et al. Interleukin‐15 and high‐intensity exercise: relationship with inflammation, body composition and fitness in cancer survivors. J. Physiol. 602, 5203–5215 (2024).
Ringleb, M. et al. Beyond muscles: investigating immunoregulatory myokines in acute resistance exercise — a systematic review and meta‐analysis. FASEB J. 38, e23596 (2024).
Forcina, L., Franceschi, C. & Musarò, A. The hormetic and hermetic role of IL-6. Ageing Res. Rev. 80, 101697 (2022).
Nilsson, M. I. et al. Lifelong aerobic exercise protects against inflammaging and cancer. PLoS ONE 14, e0210863 (2019).
Hayes, L. D., Herbert, P., Sculthorpe, N. F. & Grace, F. M. Short-term and lifelong exercise training lowers inflammatory mediators in older men. Front. Physiol. 12, 702248 (2021).
Ferreira, R. Z. et al. Effects of strength training with free weights and elastic resistance in older adults: a randomised clinical study. J. Bodyw. Mov. Ther. 41, 48–55 (2025).
Sallam, N. & Laher, I. Exercise modulates oxidative stress and inflammation in aging and cardiovascular diseases. Oxid. Med. Cell. Longev. 2016, 7239639 (2016).
Kolnes, K. J., Petersen, M. H., Lien-Iversen, T., Højlund, K. & Jensen, J. Effect of exercise training on fat loss—energetic perspectives and the role of improved adipose tissue function and body fat distribution. Front. Physiol. 12, 737709 (2021).
Couvert, A. et al. Effects of a cycling versus running HIIT program on fat mass loss and gut microbiota composition in men with overweight/obesity. Med. Sci. Sports Exerc. 56, 839–850 (2024).
Lavin, K. M. et al. Effects of aging and lifelong aerobic exercise on basal and exercise-induced inflammation in women. J. Appl. Physiol. 129, 1493–1504 (2020).
Perkins, R. K. et al. Effects of aging and lifelong aerobic exercise on expression of innate immune components in skeletal muscle of women. J. Appl. Physiol. 136, 482–491 (2024).
Saponaro, F. et al. Myokines and microbiota: new perspectives in the endocrine muscle–gut axis. Nutrients 16, 4032 (2024).
Tavella, T. et al. Elevated gut microbiome abundance of Christensenellaceae, Porphyromonadaceae and Rikenellaceae is associated with reduced visceral adipose tissue and healthier metabolic profile in Italian elderly. Gut Microbes 13, 1–19 (2021).
Nejati Bervanlou, R., Hlaváčová, N., Figueiredo, V. C., Attarzadeh Hosseini, S. R. & Motahari Rad, M. The impact of exercise and protein intake on inflammaging: a meta-analysis and systematic review of randomized controlled trials. Nutr. Rev. 83, e1458–e1471 (2024).
Mantzorou, M. et al. Mediterranean diet adherence is associated with favorable health-related quality of life, physical activity, and sleep quality in a community-dwelling Greek older population. Antioxidants 12, 983 (2023).
Piber, D. et al. Sleep disturbance and activation of cellular and transcriptional mechanisms of inflammation in older adults. Brain Behav. Immun. 106, 67–75 (2022).
Singh, K. K. et al. Sleep and immune system crosstalk: implications for inflammatory homeostasis and disease pathogenesis. Ann. Neurosci. 32, 196–206 (2024).
Rim, C., You, M.-J., Nahm, M. & Kwon, M.-S. Emerging role of senescent microglia in brain aging-related neurodegenerative diseases. Transl. Neurodegener. 13, 10 (2024).
Gudkov, S. V. et al. An emerging role of astrocytes in aging/neuroinflammation and gut–brain axis with consequences on sleep and sleep disorders. Ageing Res. Rev. 83, 101775 (2023).
Xiong, Y. et al. Advances in the study of the glymphatic system and aging. CNS Neurosci. Ther. 30, e14803 (2024).
Gordleeva, S., Kanakov, O., Ivanchenko, M., Zaikin, A. & Franceschi, C. Brain aging and garbage cleaning. Semin. Immunopathol. 42, 647–665 (2020).
Krivonosov, M. I. et al. Correction to: A new cognitive clock matching phenotypic and epigenetic ages. Transl. Psychiatry 12, 452 (2022).
Brewster, G. S., Riegel, B. & Gehrman, P. R. Insomnia in the older adult. Sleep Med. Clin. 17, 233–239 (2022).
Barone, M. et al. Towards a personalized prediction, prevention and therapy of insomnia: gut microbiota profile can discriminate between paradoxical and objective insomnia in post-menopausal women. EPMA J. 15, 471–489 (2024).
Ratiner, K., Ciocan, D., Abdeen, S. K. & Elinav, E. Utilization of the microbiome in personalized medicine. Nat. Rev. Microbiol. 22, 291–308 (2024).
Moskalev, A. et al. Developing criteria for evaluation of geroprotectors as a key stage toward translation to the clinic. Aging Cell 15, 407–415 (2016).
He, C. et al. Enhanced longevity by ibuprofen, conserved in multiple species, occurs in yeast through inhibition of tryptophan import. PLoS Genet. 10, e1004860 (2014).
Danilov, A. et al. Influence of non-steroidal anti-inflammatory drugs on Drosophila melanogaster longevity. Oncotarget 6, 19428–19444 (2015).
Rivero-Segura, N. A. et al. Exploring the geroprotective potential of nutraceuticals. Nutrients 16, 2835 (2024).
Proshkina, E. et al. Polyphenols as potential geroprotectors. Antioxid. Redox Signal. 40, 564–593 (2024).
Proshkina, E. et al. Terpenoids as potential geroprotectors. Antioxidants 9, 529 (2020).
Landsberger, T., Amit, I. & Alon, U. Geroprotective interventions converge on gene expression programs of reduced inflammation and restored fatty acid metabolism. Geroscience 46, 1627–1639 (2023).
Justice, J. N. et al. A framework for selection of blood-based biomarkers for geroscience-guided clinical trials: report from the TAME Biomarkers Workgroup. Geroscience 40, 419–436 (2018).
Wang, J. et al. Effects of metformin treatment on serum levels of C-reactive protein and interleukin-6 in women with polycystic ovary syndrome. Medicine 96, e8183 (2017).
Moskalev, A. A. & Shaposhnikov, M. V. Pharmacological inhibition of phosphoinositide 3 and TOR kinases improves survival of Drosophila melanogaster. Rejuvenation Res. 13, 246–247 (2010).
Harrison, D. E. et al. Rapamycin fed late in life extends lifespan in genetically heterogeneous mice. Nature 460, 392–395 (2009).
Konopka, A. R. et al. Blazing a trail for the clinical use of rapamycin as a geroprotecTOR. Geroscience 45, 2769–2783 (2023).
Mandrioli, J. et al. Randomized, double-blind, placebo-controlled trial of rapamycin in amyotrophic lateral sclerosis. Nat. Commun. 14, 4970 (2023).
Niechcial, A. et al. Spermidine ameliorates colitis via induction of anti-inflammatory macrophages and prevention of intestinal dysbiosis. J. Crohns Colitis 17, 1489–1503 (2023).
Ji, S. et al. Cellular rejuvenation: molecular mechanisms and potential therapeutic interventions for diseases. Signal Transduct. Target. Ther. 8, 116 (2023).
Ma, S. et al. Heterochronic parabiosis induces stem cell revitalization and systemic rejuvenation across aged tissues. Cell Stem Cell 29, 990–1005 (2022).
Robbins, P. D. et al. Senolytic drugs: reducing senescent cell viability to extend health span. Annu. Rev. Pharmacol. Toxicol. 61, 779–803 (2021).
Krzystyniak, A. et al. Combination of dasatinib and quercetin improves cognitive abilities in aged male Wistar rats, alleviates inflammation and changes hippocampal synaptic plasticity and histone H3 methylation profile. Aging 14, 572–595 (2022).
Farheen, S. et al. Patho-physiology of aging and immune-senescence: possible correlates with comorbidity and mortality in middle-aged and old COVID-19 patients. Front. Aging 2, 748591 (2021).
Hernández-Silva, D. et al. Senescence-independent anti-inflammatory activity of the senolytic drugs dasatinib, navitoclax, and venetoclax in zebrafish models of chronic inflammation. Int. J. Mol. Sci. 23, 10468 (2022).
Kirkland, J. L. & Tchkonia, T. Senolytic drugs: from discovery to translation. J. Intern. Med. 288, 518–536 (2020).
Hickson, L. J. et al. Corrigendum to ‘Senolytics decrease senescent cells in humans: preliminary report from a clinical trial of dasatinib plus quercetin in individuals with diabetic kidney disease’ EBioMedicine 47 (2019) 446–456. EBioMedicine 52, 102595 (2020).
Carpenter, V. J., Saleh, T. & Gewirtz, D. A. Senolytics for cancer therapy: is all that glitters really gold? Cancers 13, 723 (2021).
Batista, M. A. et al. Inflammaging in endemic areas for infectious diseases. Front. Immunol. 11, 579972 (2020).
Franck, M. et al. Nonuniversality of inflammaging across human populations. Nat. Aging. https://doi.org/10.1038/s43587-025-00888-0 (2025).
Nie, C. et al. Distinct biological ages of organs and systems identified from a multi-omics study. Cell Rep. 38, 110459 (2022).
Bracken, O. V., De Maeyer, R. P. H. & Akbar, A. N. Enhancing immunity during ageing by targeting interactions within the tissue environment. Nat. Rev. Drug Discov. 24, 300–315 (2025).
Andonian, B. J. et al. Inflammation and aging-related disease: a transdisciplinary inflammaging framework. Geroscience 47, 515–542 (2024).
Capri, M. et al. Long-term human spaceflight and inflammaging: does it promote aging? Ageing Res. Rev. 87, 101909 (2023).
Mohammadian, A. et al. The effect of acarbose on inflammatory cytokines and adipokines in adults: a systematic review and meta-analysis of randomized clinical trials. Inflammopharmacology 32, 355–376 (2024).
Islam, M. T. et al. Senolytic drugs, dasatinib and quercetin, attenuate adipose tissue inflammation, and ameliorate metabolic function in old age. Aging Cell 22, e13767 (2023).
Kalyakulina, A. et al. Small immunological clocks identified by deep learning and gradient boosting. Front. Immunol. 14, 1177611 (2023).
Nauta, M. et al. From anecdotal evidence to quantitative evaluation methods: a systematic review on evaluating explainable AI. ACM Comput. Surv. 55, 1–42 (2023).
Acknowledgements
This work was supported by funding from the Italian Ministry of Health ‘Ricerca Corrente’ to IRCCS INRCA and by Next Generation EU, in the context of the National Recovery and Resilience Plan, Investment PE8, Project Age-It: ‘Ageing Well in an Ageing Society’ to F.O. The views and opinions expressed are only those of the authors and do not necessarily reflect those of the European Union or the European Commission. Neither the European Union nor the European Commission can be held responsible for them. This work was also supported by the Ministry of Economic Development of the Russian Federation (grant no. 139-15-2025-004 dated 17 April 2025, agreement identifier 000000С313925P3X0002) to M.I. We thank M. Marzio (IRCCS INRCA, Ancona, Italy) for drawing Figs. 1, 3 and 4; I. Yusipov and A. Kalyakulina (Lobachevsky University, Nizhny Novgorod, Russia) for preparing Fig. 2 and L.S. Jurado-Medina (University of Bologna, Bologna, Italy) for checking the text and preparing the reference list.
Author information
Authors and Affiliations
Contributions
C.F. and A.S. conceived the Review and wrote the first draft of the manuscript. F.O., A.M. and M.I. provided constructive input and wrote additional sections in subsequent revisions of the manuscript. All authors approved the final version of the Review and its tables, box and figures.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Aging thanks Niharika Duggal and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Franceschi, C., Olivieri, F., Moskalev, A. et al. Toward precision interventions and metrics of inflammaging. Nat Aging 5, 1441–1454 (2025). https://doi.org/10.1038/s43587-025-00938-7
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s43587-025-00938-7
This article is cited by
-
A paradigm shift: from precision medicine to precision health in neurodegenerative conditions and aging
Journal of Precision Health (2026)
-
Potential dietary geroprotectors and their impact on key mechanisms of aging
Biogerontology (2026)