Abstract
Background
Intrapancreatic fat deposition (IPFD) has been linked to impaired β cell function and development of type 2 diabetes (T2D). It remains unclear whether IPFD is associated with incident T2D independent of visceral adiposity. Sex differences in the associations of IPFD with T2D are also unclear. We aimed to investigate the sex-specific associations of IPFD with risk of incident T2D, and whether the associations are independent of hepatic fat and visceral fat.
Methods
This is a cohort study using data from the UK Biobank cohort. 22,703 participants with available magnetic resonance imaging (MRI)- derived adiposity measures and without diabetes at the imaging visit were included. The main exposure was MRI-measured IPFD. The main outcome was incident T2D.
Results
Here we show that IPFD is associated with risk of T2D in both men (HR 1.35, 95% CI 1.17–1.55) and women (HR 1.53, 95% CI 1.32–1.78). After adjusting for BMI or hepatic fat, IPFD remains significantly associated with incident T2D in both sexes. The association between IPFD and incident T2D remains significant in men adjusted for visceral fat (HR 1.22, CI 1.05–1.43). IPFD is no longer significantly associated with T2D adjusted for visceral fat in women (HR 1.19, CI 0.99–1.44).
Conclusions
In this large-scale cohort study, IPFD is associated with incident T2D independent of BMI, hepatic fat and visceral fat in men and independent of BMI and hepatic fat in women. The results suggest that IPFD is of additional predictive value for future T2D.
Plain language summary
Intrapancreatic fat deposition is the result of excess fat present in the pancreas. The condition often goes underrecognized without symptoms. Evidence suggests that intrapancreatic fat deposition may lead to problems with hormone regulation and can be associated with diabetes. Here we utilized data from a large-scale cohort in the UK to examine the link between level of intrapancreatic fat deposition and future type 2 diabetes in a sex-specific manner. We show that intrapancreatic fat deposition affects risk of diabetes differently in men and women. In men, intrapancreatic fat deposition has a unique effect on risk of diabetes when taking into account other types of body fat.
Similar content being viewed by others
Introduction
Type 2 diabetes (T2D) is a complex, multifactorial disease and remains one of the leading causes of mortality and morbidities globally1. The onset of T2D is closely linked to excess calorie intake and obesity. Recent magnetic resonance imaging (MRI)-based studies have led to the twin cycle hypothesis of the pathogenesis of T2D, which postulated that muscle and liver insulin resistance leads to deranged lipid metabolism and then consequently β cell dysfunction through intrapancreatic fat deposition (IPFD)2. The link between IPFD and impaired β cell dysfunction has been supported by animal studies where exposure to fatty acids caused islet cell damage3. In humans, cross-sectional studies have reported higher prevalence of fatty pancreas disease (FPD) in T2D patients and the presence of FPD determined by sonography was found to be associated with increased risk of T2D4,5,6.
Despite growing evidence linking IPFD to diabetes, the contribution of IPFD to the development of T2D remains not fully understood. A few longitudinal studies have investigated the associations between IPFD and incident diabetes but with conflicting results7,8,9. Furthermore, it remains unclear whether the association between IPFD and incident T2D was confounded by increased visceral adiposity, since mounting evidence now suggests that visceral adiposity better predicts obesity related comorbidities than general obesity10.
It is well established that the threat adiposity poses differs between the sexes11. Men are at a higher risk of developing T2D compared with pre-menopausal women, which is believed to be at least partially explained by differences in adipose tissue characteristics between the sexes12. The sex differences of the associations of IPFD with incident T2D remain unclear. In this study, we aimed to assess the sex-specific associations between IPFD and incident T2D and to investigate whether the associations were independent of hepatic fat and visceral fat content using the UK Biobank cohort.
We find that IPFD is associated with incident T2D independent of BMI, hepatic fat and visceral fat in men and that IPFD is associated with incident T2D independent of BMI and hepatic fat in women. Additionally, significant interaction is found between age group and IPFD in men, with a greater increase of risk of T2D associated with increase of IPFD found in younger men.
Methods
Study population
The UK Biobank study recruited 502,682 participants aged 40–69 from the general population between 2006 and 201013. Participants underwent touchscreen questionnaire, verbal interview and physical measures. A sub-sample of the original participants attended the imaging study since 2014. Over 60,000 participants underwent scanning by 2023. Participants were scanned with a Siemens 1.5 Tesla MAGNETOM Aera scanner (Siemens Healthineers, Erlangen, Germany) in supine position for body MRI scans, according to previous publications14. We included participants that completed body MRI scans in this study. Participants with missing values of IPFD, liver proton density fat fraction (PDFF) or visceral fat derived from MRI or with diabetes of any form (ICD-10 code E10-E14) (Table S2) at the imaging visit based on primary care data, hospital inpatient data and self-reported medical conditions were excluded.
Assessment of ectopic fat by MRI
The subjects were scanned using a 6-minute dual-echo Dixon Vibe protocol and an additional multiecho Dixon acquisition at the imaging visit. The assembled Dixon data were then used for automatic image segmentation as described before15,16. Visceral adipose tissue (VAT), defined as the adipose tissue within abdominal cavity, was measured using AMRA Profiler Research (AMRA Medical AB, Linköping, Sweden). MRI-derived PDFF, a measure that reflects the concentration of triglycerides within tissues was used for quantification of hepatic fat and IPFD17. Liver and pancreas PDFF were estimated from the single-slice multi-echo data using the PRESCO (Phase Regularized Estimation using Smoothing and Constrained Optimization) algorithm18,19.
Assessment of outcome
The outcome of this study was incident T2D. Diagnosis of T2D was ascertained from hospital inpatient records, primary care data, death register records and self-reported medical conditions linked to the UK Biobank. T2D was defined by International Classification of Diseases, Tenth Revision (ICD-10) code E11. Deaths were ascertained from linkage to national death registries. Data fields used for defining outcome are listed at Table S1. Subjects were censored at death or 31 October 2022, whichever occurred first.
Covariates
Age at the imaging visit was calculated using date of birth and date of the visit. Sex of participant was acquired from NHS registry at recruitment. Ethnicity information was self-reported at recruitment. Townsend deprivation index (TDI), a measure of material deprivation, was calculated according to location postcode prior to recruitment based on national census20. Average total household income before tax (<18,000, 18,000–30,999, 31,000–51,999, 52,000–100,000 and >100,000 £) and education level (college or university degree and others) were self-reported at the imaging visit. Alcohol intake (never, previous and current drinker) and smoking status (never, previous and current smoker) were self-reported by touchscreen at the imaging visit. Physical activity level, categorized into low, moderate and high, was obtained by touchscreen at the imaging visit based on the International Physical Activity Questionnaire (IPAQ) scoring protocol21. Healthy diet score (0 to 5) was calculated based on self-reported frequency of food intake at the imaging visit. Scoring criteria included vegetable intake (≥4 tablespoons/day), fruit intake (≥3 pieces/day), fish intake (≥2 times/week), unprocessed red meat intake (≤2 times/week), and processed meat intake (≤2 times/week) as previously reported22. Blood pressure and anthropometry measures were obtained at the imaging visit by trained staff. BMI was calculated by weight (kg) divided by square of height (m). Selected biochemistry markers including hemoglobin A1C (HbA1c), cholesterol, low-density lipoprotein (LDL), triglycerides and high-density lipoprotein (HDL) were measured with blood samples collected at recruitment. The UK Biobank standard polygenic risk scores (sPRS) for T2D were generated using a Bayesian approach based on trait-specific meta-analyses of external GWAS sources, as previously described23,24. Data fields used for defining covariates are listed at Table S3.
Statistics and reproducibility
For descriptive analyses, continuous variables were expressed as means ± standard deviations (SDs), and categorical variables were represented by frequency and percentage. The distribution of liver PDFF was found to be right-skewed and log transformation was performed for downstream analysis. IPFD, log-transformed liver PDFF and VAT were treated as continuous variables and z-score normalization was performed for each sex separately. Sex-specific multivariable Cox proportional hazards models were used to test the associations of IPFD with incident T2D. Hazard ratios (HRs) were calculated per 1-SD increase of IPFD for each sex separately. The main model (model 1) was adjusted for multiple covariates. We then further adjusted for BMI, liver PDFF and VAT separately to test whether IPFD is independently associated with T2D. Missing values for covariates were imputed using the missing indicator approach and sex-specific mean values for categorical and continuous covariates, respectively. We further employed restricted cubic spline regressions to assess nonlinear associations of adiposity measures with incident T2D, with knots fixed at 5th, 35th, 65th, and 95th percentiles. To assess effect modification, we then performed subgroup analysis by the following factors: age (≥60 or <60 years), BMI (≥30 or <30 kg/m2) and sPRS (bottom 20%, median 60% or top 20%). Interaction effect was tested using the likelihood ratio test. Several sensitivity analyses were conducted to test the robustness of our results: Firstly, multiple imputations with chained equations were employed for handling missing values of covariates using the ‘mice’ package of R, version 3.16.0. Secondly, we repeated analysis where adjusted covariates were restricted to age, ethnicity, HbA1c, TG, HDL, smoking and drinking status, physical activity, TDI and standard PRS for T2D and individuals with missing data of covariates were excluded. Thirdly, participants with serious conditions like cardiovascular disease (CVD) or cancer at baseline were excluded. Fourthly, participants with HbA1c levels >48 mmol/mol (6.5%) at baseline were removed. Fifthly, we used genetic ethnic grouping data instead of self-reported ethnicity in the analysis. All analyses were performed with R (version 4.3.0).
Ethical approval
The UK Biobank study was approved by the North West Multi-Center Research Ethics Committee. All participants provided written informed consent. We applied and were approved to access the UK biobank data (application ID 96582).
Results
Population characteristics
The study population was restricted to participants without diabetes at the imaging visit with available data of IPFD, liver PDFF and VAT (Fig. 1). IPFD, liver PDFF and VAT data were available for 29,464, 30,357 and 56,016 participants, respectively.
Study participant flow.
The final cohort comprised 22,703 participants, of whom 11,895 (52.4%) were females. During a median follow-up of 4.2 years, 262 cases of incident T2D (1.15%) were documented.
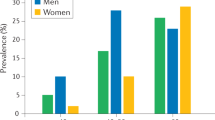
Baseline characteristics of the participants are shown in Table 1. Mean age of female participants was 63 years (SD 7), and 11579 (98%) were from a white ethnic background. Mean age of male participants was 65 years (SD 8), and 10,480 (97%) were of white ethnic background. Male participants had a higher level of IPFD compared with female participants, with a mean IPFD (%) of 13 (SD 9) in men and 8 (SD 7) in women. IPFD was positively associated with BMI, liver PDFF and VAT. Spearman correlation coefficients between adiposity measures were calculated for each sex. In women, Spearman correlation coefficients were 0.675 (p < 0.001) between VAT and IPFD, 0.416 (p < 0.001) between liver PDFF and IPFD, and 0.525 (p < 0.001) between BMI and IPFD (Table S4). In men, Spearman correlation coefficients were 0.578 (p < 0.001) between VAT and IPFD, 0.320 (p < 0.001) between liver PDFF and IPFD, and 0.433 (p < 0.001) between BMI and IPFD (Table S4).
Associations of IPFD with Incident T2D
Increased IPFD was associated with elevated risk of incident T2D for both sexes adjusted for multiple covariates (Fig. 2). Per 1-SD increase of IPFD was associated with a 35% higher risk of T2D in men (HR 1.35, CI 1.17–1.55, p < 0.001) and a 53% higher risk of T2D in women (HR 1.53, CI 1.32–1.78, p < 0.001). The associations were consistent when BMI was added as a covariate, with per 1-SD increase of IPFD associated with a 25% higher risk of T2D in men (HR 1.25, CI 1.08–1.44, p < 0.01) and a 33% higher risk in women (HR 1.33, CI 1.12–1.57, p < 0.01). Increase of IPFD remained to be significantly associated with increased risk of T2D after adjustment for liver PDFF in both men (HR 1.23, CI 1.07–1.42, p < 0.01) and women (HR 1.41, CI 1.21–1.65, p < 0.001). However, when adjusted for VAT, the magnitude of association between IPFD and T2D attenuated substantially only in women (HR 1.19, CI 0.99–1.44, p = 0.07) while the association between IPFD and T2D remained in men (HR 1.22, CI 1.05–1.43, p = 0.011).
Sex-specific associations between IPFD and T2D (N = 22703). A Cox proportional hazards models showing associations between IPFD and T2D in women. IPFD is significantly associated with incident T2D adjusted for BMI (p = 0.001) or liver PDFF (p < 0.001). B Cox proportional hazards models showing associations between IPFD and T2D in men. IPFD is significantly associated with incident T2D adjusted for BMI (p = 0.003), liver PDFF (p = 0.004) or VAT (p = 0.011). Data is presented as a hazard ratio (HR) with 95% confidence intervals (CI). P values (two-sided) were calculated with Wald test derived from the Cox proportional hazards models. Model 1 was adjusted for age, ethnicity, Townsend deprivation index, household income, education level, drinking status, smoking status, physical activity, healthy diet score, systolic blood pressure, HbA1c, LDL, HDL, total cholesterol, triglycerides and standard polygenic risk scores for T2D. Abbreviations: HR hazard ratio, CI confidence interval, BMI body mass index, VAT visceral adipose tissue, PDFF proton density fat fraction. Center for the error bars indicate hazard ratios estimated by maximizing the Cox partial likelihood derived from the Cox proportional hazards models; the error bars indicate 95% confidence intervals. N indicates number of participants included in analysis.
Adjusted restricted cubic splines were plotted for visualization of the dose-effect relationship between adiposity measures and risk of T2D. Results of the restricted cubic spline analyses adjusted for multiple covariates showed a nonlinear relationship between IPFD and T2D risk in women (P for nonlinearity <0.05) while risk of T2D increased linearly with increased IPFD in men (P for nonlinearity >0.05) (Fig. S1). However, the nonlinear relationship between IPFD and T2D in women disappeared after further adjustment for BMI (P for nonlinearity > 0.05).
Subgroup analysis
Interaction effect between IPFD and age, BMI and genetic risk scores was evaluated for men and women separately (Fig. 3). No interaction effect was observed between IPFD and BMI or genetic risk group for both sexes. Statistically significant interaction was found between IPFD and age group for men (p for interaction 0.003). A more pronounced increase in HR associated with per 1-SD increase of IPFD was found in men <60 years old (HR 2.18, CI 1.59–2.99) compared with men ≥60 years old (HR 1.24, CI 1.07–1.44) after multivariable adjustment. The interaction effect between IPFD and age group in men persisted even after further adjustment for BMI, liver PDFF or VAT (Table S5). No interaction between IPFD and age group was found in women.
Sex-specific associations between IPFD and T2D stratified by age, BMI and genetic risk (N = 22703). A Stratified analysis of associations between IPFD and T2D in women. B Stratified analysis of associations between IPFD and T2D in men. Significant interaction was identified between IPFD and age group in men (p for interaction 0.003). Data is presented as a hazard ratio (HR) with 95% confidence intervals (CI). P for interaction (two-sided) was calculated with likelihood ratio test. Results were adjusted for age, ethnicity, Townsend deprivation index, household income, education level, drinking status, smoking status, physical activity, healthy diet score, systolic blood pressure, HbA1c, LDL, HDL, total cholesterol, triglycerides and standard polygenic risk scores for T2D. Abbreviations: HR hazard ratio, CI confidence interval, BMI body mass index. Center for the error bars indicate hazard ratios estimated by maximizing the Cox partial likelihood derived from the Cox proportional hazards models; the error bars indicate 95% confidence intervals. N indicates number of participants included in analysis.
Sensitivity analysis
The associations between IPFD and T2D risk remained in sensitivity analyses. The main results persist when multiple imputation with chained equations was applied for imputing missing values of covariates (Table S6) and when individuals with missing covariates were removed from analysis with fewer covariates in the model (Table S7). When excluding participants with baseline CVD or cancer, IPFD remained associated with higher risk of T2D for both men (HR 1.32, CI 1.16–1.51, p < 0.001) and women (HR 1.40, CI 1.21–1.62, p < 0.001) after adjusting for confounders (Table S8). To account for potential undiagnosed diabetes at baseline, an additional sensitivity analysis where participants with HbA1c levels >48 mmol/mol at recruitment were removed was conducted and IPFD remained significantly associated with increased risk of incident T2D in men (HR 1.27, CI 1.09–1.47, p < 0.005) and in women (HR 1.512, CI 1.27–1.80, p < 0.001) (Table S9). When genetic ethnic grouping data were used instead of self-reported ethnicity in the analysis, IPFD was also significantly associated with T2D in men (HR 1.34, CI 1.17–1.53, p < 0.001) and women (HR 1.46, CI 1.26–1.69, p < 0.001) (Table S10). In consistence with the primary analysis, IPFD was significantly associated with T2D risk controlling for BMI, liver PDFF or VAT in men and was significantly associated with T2D risk controlling for BMI or liver PDFF in women in all sensitivity analyses.
Discussion
In this longitudinal study using the UK Biobank cohort, we examined the sex-specific associations between MRI measured IPFD and risk of T2D. Our findings indicated that IPFD was associated with T2D independent of BMI and hepatic fat in both men and women. IPFD remained significantly associated with incident T2D after adjustment for VAT in men. However, the association between IPFD and T2D was no longer statistically significant when VAT was added as a covariate for women.
Previous studies have reported controversial results regarding the associations between IPFD and T2D. One Japanese study of 1478 participants found that fatty pancreas determined by CT was associated with T2D in lean populations only adjusted for BMI and liver attenuation8. Another longitudinal study of 631 middle-aged, healthy subjects in Hong Kong showed that IPFD but not BMI, central obesity or fatty liver was independently associated with T2D9. In contrast, one study of a Japanese cohort of 813 participants showed that the association between IPFD measured by CT and T2D disappeared after adjusting for BMI and liver attenuation7. The disparities of results may be explained by the heterogeneity nature of T2D and the limited sample sizes of previous imaging studies. In this large-scale UK Biobank cohort study, we showed that IPFD was independently associated with risk of T2D regardless of BMI groups or genetic risk levels. Additionally, ethnic differences in IPFD have been previously characterized, which may partially explain the disparities of results between the current study and previous studies on Asian populations25.
Increased IPFD has been shown to contribute to risk of T2D through both increased insulin resistance and impaired β cell functions. A few studies found that in patients with impaired fasting glucose (IFG) or impaired glucose tolerance (IGT), elevated IPFD was associated with insulin resistance26. More evidence suggests that IPFD leads to β cell dysfunction. Increased pancreatic fat content in patients with prediabetes or obesity was found to be associated with impaired insulin secretion6. Another study found that IPFD was associated with impaired insulin secretion only in genetically predisposed populations27. In the current study, we found that IPFD was associated with incident T2D independent of general and other ectopic adiposity measures in men and independent of general adiposity and hepatic fat in women, highlighting the additional predictive value of IPFD to future T2D. These findings thus support the notion that IPFD plays a unique role in the development of T2D through localized effect of fat depots, most likely due to impaired β cell functions.
Sex dimorphism of obesity-related complications is well characterized and strengths of associations between adiposity measures and cardiometabolic diseases vary between men and women12,28,29. The sex difference of the association between IPFD and T2D is unclear. In this analysis, a similar strength of association between IPFD and incident T2D was found in men and women adjusted for multiple confounders. However, adjustment of VAT led to a marked decrease of HR in women only. Previous studies have found greater associations between VAT and cardiometabolic risk factors in women than in men30. Another study of the Framingham Heart Study cohort found that VAT had a markedly stronger association with risk of CVDs compared with BMI in women only31. Our findings indicated that the association between IPFD and T2D in women at least partially reflected the effect of elevated VAT associated with increased pancreatic fat content.
Notably, IPFD was found to have a stronger effect on risk of T2D in younger men in this study. Previous studies have also reported that central adiposity poses less risk in older men32. Another study using the UK Biobank cohort showed that the effect of elevated visceral fat deposition on increased mortality decreased with age, with the highest HR found in men <50 years old33. Genetic evidence also showed that BMI was causally related to worsened cardiovascular risk factors especially in the <55-year stratum34. It remains not fully understood why the effect of adiposity decreases with age. Like other adiposity measures, aging is one of the major risk factors for increased IPFD35. The decreased effect of IPFD on T2D in older men could potentially be explained by physiological changes in the aging process or survival bias. However, in this study, the risk of T2D associated with increased IPFD in older women was similar to that of younger women. It is likely that the menopause transition, associated with changes of body composition and lipid metabolism in women, adds to the complexity of the association between IPFD and T2D in older women36.
Recently, the Counterpoint, Counterbalance and the Diabetes Remission Clinical Trial (DiRECT) and other studies have shown that T2D is potentially reversible and normalization of IPFD was found to accompany disease remission37,38,39. There is now growing interest in reducing IPFD as a potential therapeutic target for reversal of T2D. Our findings support that IPFD could be included as a marker for risk stratification of T2D especially in younger men and that reducing IPFD may potentially be beneficial for disease prevention and treatment. Further causal research and mechanistic studies are required to elucidate the causal effect of IPFD on T2D.
This study has several strengths. Firstly, this is a study of the UK Biobank, which is a large-scale cohort with detailed demographic and lifestyle information. Secondly, in this study, IPFD was quantified using MRI derived PDFF, which has been confirmed to have excellent correlations with histological findings40. Moreover, our analysis in the current study was adjusted for more extensive potential confounders compared to previous studies and we uniquely included VAT in the analysis to investigate the independent associations between IPFD and T2D. Also, we included genetic risk level for T2D in this analysis both as potential confounder and effect modifier.
The study also has several limitations. Firstly, causal inference should be treated with caution given the nature of the observational study. Further investigation is required for establishment of the causal link between IPFD and subsequent diabetes. Secondly, this study cohort was comprised mainly of older adults, which may affect the generalizability of the results. Additionally, since the participants of the UK Biobank are mostly of white ethnicity, the results should be further validated in more ethnic groups.
Conclusion
In conclusion, IPFD is associated with incident T2D independent of BMI, hepatic fat and visceral fat in men and independent of BMI and hepatic fat in female in this cohort study. Our findings highlight the significance of IPFD in the development of T2D and have implications that IPFD may be an important marker for risk stratification and target for prevention of T2D.
Data availability
Data from the UK biobank cohort were used for this analysis. The UK Biobank data are available for approved researchers. Access to raw data of the UK biobank cohort can be obtained by applying at https://www.ukbiobank.ac.uk/enable-your-research/apply-for-access. Source data for figures are provided with the article. The source data for Fig. 2 is in Supplementary Data 2 and the source data for Fig. 3 is in Supplementary Data 3.
References
Ong, K. L. et al. Global, regional, and national burden of diabetes from 1990 to 2021, with projections of prevalence to 2050: a systematic analysis for the Global Burden of Disease Study 2021. Lancet 402, 203–234 (2023).
Taylor, R. Pathogenesis of type 2 diabetes: tracing the reverse route from cure to cause. Diabetologia 51, 1781–1789 (2008).
Pinnick, K., Neville, M., Clark, A. & Fielding, B. Reversibility of metabolic and morphological changes associated with chronic exposure of pancreatic islet β-cells to fatty acids. J. Cell. Biochem. 109, 683–692 (2010).
Ou, H.-Y., Wang, C.-Y., Yang, Y.-C., Chen, M.-F. & Chang, C.-J. The association between nonalcoholic fatty pancreas disease and diabetes. PLoS ONE 8, e62561 (2013).
Wang, C., Ou, H., Chen, M., Chang, T. & Chang, C. Enigmatic ectopic fat: prevalence of nonalcoholic fatty pancreas disease and its associated factors in a Chinese population. J. Am. Heart Assoc. 3, e000297 (2014).
Heni, M. et al. Pancreatic fat is negatively associated with insulin secretion in individuals with impaired fasting glucose and/or impaired glucose tolerance: a nuclear magnetic resonance study. Diab. Metab. Res. Rev. 26, 200–205 (2010).
Yamazaki, H. et al. Lack of independent association between fatty pancreas and incidence of type 2 Diabetes: 5-Year Japanese Cohort Study. Diab. Care 39, 1677–1683 (2016).
Yamazaki, H. et al. Longitudinal association of fatty pancreas with the incidence of type-2 diabetes in lean individuals: a 6-year computed tomography-based cohort study. J. Gastroenterol. 55, 712–721 (2020).
Chan, T. T. et al. Fatty pancreas is independently associated with subsequent diabetes mellitus development: a 10-year prospective cohort study. Clin. Gastroenterol. Hepatol. 20, 2014–2022.e4 (2022).
Goossens, G. H. The metabolic phenotype in obesity: fat mass, body fat distribution, and adipose tissue function. Obes. Facts 10, 207–215 (2017).
Kautzky-Willer, A., Harreiter, J. & Pacini, G. Sex and gender differences in risk, pathophysiology and complications of type 2 diabetes mellitus. Endocr. Rev. 37, 278–316 (2016).
Delaney, K. Z. & Santosa, S. Sex differences in regional adipose tissue depots pose different threats for the development of Type 2 diabetes in males and females. Obes. Rev. 23, e13393 (2022).
Sudlow, C. et al. UK biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLOS Med. 12, e1001779 (2015).
Littlejohns, T. J. et al. The UK Biobank imaging enhancement of 100,000 participants: rationale, data collection, management and future directions. Nat. Commun. 11, 2624 (2020).
Linge, J. et al. Body composition profiling in the UK biobank imaging study. Obesity 26, 1785–1795 (2018).
West, J. et al. Feasibility of MR-based body composition analysis in large scale population studies. PLOS ONE 11, e0163332 (2016).
Tamaki, N. Non-invasive methods for imaging hepatic steatosis and their clinical importance in NAFLD. Nat Rev Endocrinol. 18, 55–66 (2022).
Liu, Y. et al. Genetic architecture of 11 organ traits derived from abdominal MRI using deep learning. eLife 10, e65554 (2021).
GitHub - marcsous/pdff: Proton density fat fraction calculation for MRI. https://github.com/marcsous/pdff.
Townsend, P. Deprivation. J. Soc. Policy 16, 125–146 (1987).
CRAIG, C. L. et al. International physical activity questionnaire: 12-Country reliability and validity. Med. Sci. Sports Exerc. 35, 1381–1395 (2003).
Wang, M. et al. Baseline Vitamin D Status, Sleep Patterns, and the Risk of Incident Type 2 Diabetes in Data From the UK Biobank Study. Diabetes Care 43, 2776–2784 (2020).
Collister, J. A., Liu, X. & Clifton, L. Calculating Polygenic Risk Scores (PRS) in UK Biobank: a practical guide for epidemiologists. Front. Genet. 13, 818574 (2022).
Thompson, D. J. et al. A systematic evaluation of the performance and properties of the UK Biobank Polygenic Risk Score (PRS) Release. PLOS ONE 19, e0307270 (2024).
Szczepaniak, L. S. et al. Pancreatic steatosis and its relationship to β-Cell dysfunction in humans. Diabetes Care 35, 2377–2383 (2012).
Lee, J. S. et al. Clinical implications of fatty pancreas: correlations between fatty pancreas and metabolic syndrome. World J. Gastroenterol. 15, 1869 (2009).
Wagner, R. et al. Pancreatic steatosis associates with impaired insulin secretion in genetically predisposed individuals. J. Clin. Endocrinol. Metab. 105, 3518–3525 (2020).
Cooper, A. J., Gupta, S. R., Moustafa, A. F. & Chao, A. M. Sex/gender differences in obesity prevalence, comorbidities, and treatment. Curr. Obes. Rep. 10, 458–466 (2021).
Peters, S. A. E., Bots, S. H. & Woodward, M. Sex differences in the association between measures of general and central adiposity and the risk of myocardial infarction: results from the UK Biobank. J. Am. Heart Assoc. 7, e008507 (2018).
Abraham, T. M., Pedley, A., Massaro, J. M., Hoffmann, U. & Fox, C. S. Association between visceral and subcutaneous adipose depots and incident cardiovascular disease risk factors. Circulation 132, 1639–1647 (2015).
Kammerlander, A. A. et al. Sex differences in the associations of visceral adipose tissue and cardiometabolic and cardiovascular disease risk: the framingham heart study. J. Am. Heart Assoc. 10, e019968 (2021).
Schousboe, J. T. et al. Central obesity and visceral adipose tissue are not associated with incident atherosclerotic cardiovascular disease events in older men. J. Am. Heart Assoc. 7, e009172 (2018).
Yu, B. et al. Age-specific and sex-specific associations of visceral adipose tissue mass and fat-to-muscle mass ratio with risk of mortality. J. Cachexia Sarcopenia Muscle 14, 406–417 (2023).
Fall, T. et al. Age- and Sex-specific causal effects of adiposity on cardiovascular risk factors. Diabetes 64, 1841–1852 (2015).
Wong, V. W.-S. et al. Fatty pancreas, insulin resistance, and β-cell function: a population study using fat-water magnetic resonance imaging. Am. J. Gastroenterol. 109, 589–597 (2014).
Bermingham, K. M. et al. Menopause is associated with postprandial metabolism, metabolic health and lifestyle: The ZOE PREDICT study. eBioMedicine 85, 104303 (2022).
Taylor, R. et al. Remission of Human Type 2 diabetes requires decrease in liver and pancreas fat content but is dependent upon capacity for β Cell recovery. Cell Metab. 28, 547–556.e3 (2018).
Petrov, M. S. & Taylor, R. Intra-pancreatic fat deposition: bringing hidden fat to the fore. Nat. Rev. Gastroenterol. Hepatol. 19, 153–168 (2022).
Steven, S. et al. Weight loss decreases excess pancreatic triacylglycerol specifically in type 2 diabetes. Diabetes Care 39, 158–165 (2016).
Fukui, H. et al. Evaluation of fatty pancreas by proton density fat fraction using 3-T magnetic resonance imaging and its association with pancreatic cancer. Eur. J. Radiol. 118, 25–31 (2019).
Acknowledgements
This work was supported by National High Level Hospital Clinical Research Funding (2022-PUMCH-B-015), CAMS Innovation Fund for Medical Sciences (2023-I2M-C&T-B-043), CAMS Innovation Fund for Medical Sciences (No. 2021-1-12M-002), Beijing Municipal Natural Science Foundation (No.M22014).
Author information
Authors and Affiliations
Contributions
H.Z. and Y.L. had full access to all data of the study and take responsibility for the integrity of the data and the accuracy of the data analysis. H.Z., X.W. and Y.L. planned the concept and design of this study. H.Z. and X.W. conducted data analysis. Y.Y., S.H., and Z.L. carried out data cleaning. L.X., F.P. and W.L. provided critical revisions for the manuscript. All authors reviewed and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Communications Medicine thanks Yuliya Kupriyanova and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Wang, X., Yang, Y., Han, S. et al. Sex-specific associations of intrapancreatic fat deposition with incident type 2 diabetes. Commun Med 5, 501 (2025). https://doi.org/10.1038/s43856-025-01221-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s43856-025-01221-x