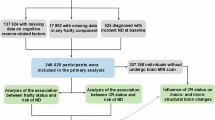
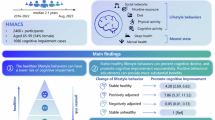
Abstract
Cognitive reserve, a component of resilience, may be conceptualized as the ability to overcome accumulating neuropathology and maintain healthy aging and function. However, research measuring and evaluating it in American Indians is needed. We recruited American Indians from 3 regional centers for longitudinal examinations (2010-13, n = 818; 2017-19, n = 403) including MRI, cognitive, clinical, and questionnaire data. We defined cognitive reserve by measuring the residual from individual regressions of cognitive tests over imaged brain volumes, adjusted for age and sex. Analyses examined three different metrics of cognitive reserve against sociodemographic, clinical, and longitudinal cognitive data in causal mediation models. Better cognitive reserve was significantly associated with more education, higher income, lower prevalence of depression, lower prevalence of diabetes, and lower prevalence of kidney disease, but we found no statistically significant evidence for an association with plasma biomarkers for Alzheimer’s disease and related dementias, APOE e4 carrier status, alcohol use, body mass, or hypertension. Better cognitive reserve was associated with better cognitive function over mean 6.7 years follow-up (range 4-9 years); and the association for education with cognition over time was mediated in part (15-24%) by cognitive reserve. Cognitive reserve, although challenging to measure, appears important for understanding the range of cognitive aging in American Indians.
Similar content being viewed by others
Introduction
Cognitive resilience may be conceptualized using three different facets: as cognitive reserve, or resilience in cognition despite advancing pathological status; as brain reserve, or resilience in brain functionality despite advancing pathological status; or as brain maintenance, or resilience to change in neuropathologic status despite substantive risk factors such as advancing age1. Cognitive reserve is challenging to study—first because direct measures are not available, so operationalization using proxy and latent variables is still needed. Furthermore, in vivo measures of neuronal pathology are not widely available, further distancing available measures from reflecting true status. When neither the injury nor the mediating construct can be directly measured, conceptual frameworks can be difficult to construct and interpret.
Nevertheless, cognitive reserve, may be conceptualized as the ability to overcome the influence of accumulating brain pathology, in order to maintain cognition and functioning2,3. Thus, those with more cognitive reserve may be better equipped—perhaps via enhanced cortical thickness and/or connectivity—in compensating for accumulating disease burden, and thus preventing or delaying the emergence of clinical symptoms4,5,6,7. Such an abstract concept may be quantified in multiple ways: one option is to declare intact cognitive status, despite substantive accumulated pathology or advanced age. However, dichotomizing cognitive state as intact versus impaired may be overly reductionistic, arbitrary, and may introduce bias and measurement error in contexts where neuropsychological tests are not validated and normative data do not yet exist8,9.
A more ideal approach utilizes continuous estimation, thus also enabling adjustment for confounding by premorbid function10. In such an approach, cognitive reserve is represented as a continuous measure of association between selected measures of cognition and neuropathology, and could theoretically reflect those with abnormally positive aging, negative aging, or both9. Continuous estimation of cognitive reserve by regressing cognitive test scores against measures of imaged brain volumes, adjusting for confounders such as age and sex, and predicting the expected residual values from each regression provides an intraindividual metric of observed-over-expected performance10. As an estimate of continuous, comparative cognitive reserve, regressed residual metrics have unknown specificity to the chosen cognitive domain and pathologic marker9.
The selection of specific measures to define the metric of cognitive reserve can influence the patterns of association for that metric. For example, a metric using a measure of processing speed over general brain volume might be demonstrative of global pathologies1,10, whereas a metric of phonemic fluency over white matter hyperintensities (WMH) might be more sensitive to vascular pathologies11, and a metric of memory over hippocampal loss might be more reflective of neurodegenerative pathologies12.
Despite increasing interest in resilient aging and cognitive reserve, research is still needed to examine both risk and protective features in American Indians. Note that we use the term “American Indian” per specific direction from our partner Tribal communities and Community Advisory Board. American Indians convey many features associated with strength-based aging13, including psychological resilience14,15,16, community, and social support17. However, this population is also at particularly high risk for vascular disease, Alzheimer’s disease (AD), and related dementias18,19, in part due to the high burden of modifiable, clinical risk factors—although not all conventional AD risk factors appear generalizable in effect20. Thus, estimation of cognitive reserve in this unique population may help elucidate some of the observed, potentially modifiable effects from factors such as diabetes and depression21,22,23, as well as some of the observed variance in mediating factors such as education. In previous research, we detected the strongest associations of brain, WMH, and hippocampal volumes with cognitive test performance24, and thus structured candidate metrics using these imaging features, in combination with corresponding test scores for processing speed, fluency and executive function, and memory, respectively.
This study aimed to develop understanding of these metrics in this population facing unique challenges, with the ultimate goal to identify social determinants across the life-course that have the potential to promote healthier aging trajectories for American Indian older adults and their communities.
Methods
Setting
The Strong Heart Study (SHS) is a longitudinal study of American Indians from the Northern Plains, Southern Plains, and Southwest, recruited for multiple examinations between 1989–199925. Using the SHS as a sampling frame, the ancillary Cerebrovascular Disease and its Consequences in American Indians study (CDCAI) conducted two neurological examinations in 818 consenting study survivors in 2010–2013 (Visit 1) and in 403 of the 818 in 2017–2019 (Visit 2), as previously reported26.
Ethics and inclusion
Institutional, Indian Health Service, and Tribal research review boards approved all procedures. All participants provided written, informed consent, and were compensated for their participation in this study. This study analysis was pre-proposed to the Strong Heart Study Publication & Presentations committee (Proposal 846, Approved 2024-06-13); a list of approved publications is available at https://strongheartstudy.org/Research/Papers-and-Abstracts/Approved-Papers-Dissertation. There was no additional preregistration for this study. All partnering Tribes and communities approved all written dissemination materials. Of note, the term “American Indian” is used herein, per specific direction from our study partner Tribal communities and Community Advisory Board, who have the final say in the representation of their identity. Terminology preferences vary substantively by Tribe, community, and individual, but this term is generally considered acceptable in the United States; is commonly the preferred term when individual Tribe or Tribal nations cannot be directly named; and is also the preferred term based on guidance from nationally-representative, self-governing, Indigenous-led organizations such as the National Congress of American Indians.
Cognitive testing
The Weschler Adult Intelligence Scale 4th edition digit symbol coding subtest (WAIS-DSST, processing speed or visuomotor speed)27 Controlled Oral Word Association FAS (COWA FAS, verbal fluency, executive function)28, California Verbal Learning Test II Short Form (CVLT II-SF, verbal learning and memory)29, were administered at both CDCAI Visit 1 and Visit 2. Modified Mini-Mental Status Examination (3MSE, general multidomain cognitive screening)30, was also administered at both Visit 1 and Visit 2; other tests added at CDCAI Visit 2 included the National Alzheimer’s Coordinating Center Uniform Data Set version 3.0 form C2 battery31, with Montreal Cognitive Assessment (MoCA, multidomain general screening)32, Number Span Test forward and backward (attention and working memory), Benson Complex Figure copy and recall (visuospatial skills and memory)32,33, animal and vegetable naming tests (semantic fluency), Craft Story immediate and delayed recall (contextual verbal memory)34, Trail Making Test A and B (processing speed, simple and divided attention)35, and Multilingual Naming Test (MINT, semantic memory and naming)36. Of note, lower cognitive scores correspond with poorer cognition for all measures except the Trail Making timed tests wherein more time (seconds) needed to complete the activity corresponds to poorer performance. Internal consistency-reliability for cognitive tests in this population appear to follow a pattern of excellent fit and performance for overall or summary scores (omega coefficients >0.9), but poor metrics of fit and performance for individual domain, subcomponent, or tasks (omega <0.8;)37,38,39. Composite, multidomain cognitive test performance was also defined as the average of Z-scored cognitive tests.
MRI
At both CDCAI Visit 1 and Visit 2, participants underwent 1.5T MRI scans with six sequences including sagittal T1-weighted localizer, co-registered 5 mm axial-T1, 5 mm axial-T2, 5 mm axial-T2* susceptibility-weighted images in the anterior commissure/posterior commissure plane, 3 mm axial fluid-attenuated inversion recovery (FLAIR) images, and 1.5 mm sagittal T1-weighted volumetric gradient echo. Additional details regarding repetition time, echo time, inversion time, slice thickness, slice spacing, acquisition matrix, number excitations, echo train, flip angle, and field of view have been provided in prior reports. MRI were processed for structural volumetrics, including total gray and white tissue for the whole brain, white matter hyperintensities (on FLAIR) or hypointensities (on T1), and hippocampus volume using version 5.3 of the FreeSurfer image analysis suite23, with motion correction and visual checks at intermediate points in the process for gross misregistrations and other processing failures. Such problems were corrected manually. Only images that exceeded the field of view were censored, although these did not usually pass quality control. Skull stripping using cortical reconstruction by voxel-based parcellation of T1 images, skull stripping using cortical reconstruction, removal of non-brain tissue using a hybrid watershed-surface deformation procedure, automated Talairach transformation, segmentation of subcortical white matter and deep gray matter volumetric structures, intensity normalization, tessellation of the gray matter-white matter boundary, automated topology correction, and surface deformation following intensity gradients to place optimally the gray matter-white matter and gray matter-CSF borders at the location where the greatest shift in intensity defines the transition to the other tissue class. Overall, the results of these procedures include brain and cranial volumetric estimates that include cerebellum but not ventricles, CSF, and dura. All features were estimated in millimeters cubed, and then standardized to intracranial volume to account for interindividual variations in head size.
Other data
Participants self-reported age (years), sex (male; female), years of formal education, annual household income, and typical use of alcohol (drinks per day). Participants underwent clinical and anthropometric examinations, including basic blood and urine laboratory testing, medical history, and transcription of medications. Diabetes mellitus was defined as fasting blood glucose ≥126 mg/dL, prior physician diagnosis, or use of antihyperglycemic medications or insulin. Body mass index (BMI) was defined as weight in kilograms divided by height in meters squared, and categorized using standard criteria (normal BMI <25 kg/m2; overweight BMI 25 to 29.9; obese BMI 30+). Hypertension was defined as averaged, seated systolic blood pressure ≥130 mmHg, diastolic ≥90, or the use of antihypertensive medications. Chronic kidney disease was defined as an estimated glomerular filtration rate <60 mL/min. Participants self-reported emotional and mental health using the 20-item Centers for Epidemiologic Studies Depression (CESD) symptoms scale, and depression was dichotomized using a cutoff ≥16. Plasma biomarkers related to Alzheimer’s disease were measured (using samples from Visit 2) on the Quanterix platform including phosphorylated tau (pTau181), amyloid beta 42 and 40 (AB42/40 ratio), glial fibrillary acidic protein (GFAP), and neurofilament light chain (NfL). Apolipoprotein E epsilon 4 carrier status was assessed using standard genotyping.
Cognitive reserve metrics
Cognitive reserve was operationalized as observed-over-expected cognitive performance, by regression of cognitive test score (WAIS-DSST score, COWA FAS overall score, or CVLT long delay free recall score) over a continuous estimate of brain pathology (total brain volume, WMH volume, or hippocampus volume, respectively; all standardized to IC volume); adjusted for age and sex, resulting in three metrics: WAIS-Brain, COWA-WMH, and CVLT-Hipp. Predicted values for each individual participant according to the regression line were subtracted from their observed values, producing a “residual”, or estimated degree of positive or negative cognition-beyond-pathology. In this paradigm, these residuals represent a continuous estimate for the latent variable of cognitive reserve, with positive values indicating higher reserve and negative values lower reserve. Residuals were then analyzed continuously, as well as in tertiles of low, middle, and high-reserve groups. This method was similar to those used by other groups, and the specific pairings (WAIS-Brain, COWA-WMH, CVLT-Hipp) were defined on the basis of theoretical associations of changes in cognition with associated affected region or pathology10.
Statistical analyses
Analyses were conducted as complete analysis, with exclusion only on the basis of missing data; for transparency, numbers included in each analysis figure and table were reported separately. Descriptive analyses estimated mean and standard deviation or count and percent, by examination visit, for participant characteristics, including the three metrics of cognitive reserve (WAIS-Brain, COWA-WMH, CVLT-Hipp). Graphical representations included histogram, scatterplot, linear fit, boxplot with whiskers, and heatmap. Heatmap colorations were based on pairwise correlation coefficients (Pearson) and P values. Statistical tests for association included one-way ANOVA (F-test) for between-group differences, T-tests for equivalence in distributions, or regression. Causal mediation analysis estimated direct and indirect effects as well as the proportion of effect mediated for models with education, depression, or diabetes as exposure, composite cognitive test score as outcome, and metric of cognitive reserve as mediator. Evaluation of assumptions included assessment of normality in residuals, residual association with age and sex after adjustment, and heteroscedasticity. All analyses were done using Stata v17-18 (College Station, Texas) or R v4 (Vienna, Austria).
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Results
At Visit 1 (2010–13), this population-based cohort of American Indians had a mean age of 73, was majority female, and had about half with at least some college (Table 1). Depression symptom (CESD) scores were high at both Visit 1 and Visit 2. Diabetes was detected in about half of the cohort at both visits. As noted in prior reports, income was relatively low, overweight and obesity, hypertension, and kidney disease were relatively common, and alcohol use was generally uncommon.
Metrics of cognitive reserve, defined as residuals of cognitive test scores over brain imaging features as % IC volume and adjusted for age and sex, included WAIS DSST over brain volume (WAIS-Brain), COWA fas over WMH volume (COWA-WMH), and CVLT LF over hippocampus volume (CVLT-Hipp). WAIS-Brain residuals were not significantly different comparing Visit 1 to Visit 2, over age, and were normally distributed (Fig. 1). COWA-WMH residuals were somewhat lower from Visit 1 to Visit 2 (mean residual difference 2.6 (95% CI: 1.5, 3.7; t-test P < 0.0001), significantly associated with age (beta -0.6; 95% CI: -0.5, -0.8; P < 0.0001), and were normally distributed. CVLT-Hipp residuals were not significantly different comparing Visit 1 and Visit 2, or by age, and were somewhat normally distributed but with a mild left skew.
Graphical representation of three metrics of cognitive reserve, with (top) residuals of Weschler Adult Intelligence Scale Digit Symbol Coding Test (WAIS DSST) over brain volume as percent intracranial volume (WAIS-Brain), (middle) residuals of Controlled Oral Word Association f/a/s test (COWA) over white matter hypointensities volume (MRI T1 sequence) as percent intracranial volume (COWA-WMH), and (bottom) residuals of California Verbal Learning Test version II short form long delay free recall test (CVLT LF) over hippocampus volume as percent intracranial volume (CVLT-Hipp). Metrics of cognitive reserve defined by regression of cognitive test score over brain imaging feature, adjusted for age and sex. Left: scatterplots of cognitive test scores (Y-axis) by brain imaging features (X-axis). The coloration of scatter points with fit lines by tertile of metric for cognitive reserve, with the highest reserve in green, middle in blue, and lowest in red. Note: COWA-WMH scatterplot shown with X-axis on a log scale, and CVLT-Hipp plot with point-jitter for visibility purposes. Left-middle: Boxplots (mean, 25th, and 75th percentiles), with scatter overlay, and whisker bars (10th and 90th percentiles) for tertiles of (A, B, C) metrics of cognitive reserve. Right-middle: histograms for distribution of each metric with normal tracing. Right: scatterplots of metrics over age, with polynomial fit line and 95% confidence interval. Numbers included in the analysis: WAIS-Brain Visit 1 n = 765, COWA-WMH Visit 1 n = 765, CVLT-Hipp Visit 1 n = 744.
Separating all three metrics of cognitive reserve into tertiles enabled comparison of low, middle, and high categories of cognitive reserve, independent of age and sex (Fig. 1). Graphically represented in boxplots by tertile or in scatterplots of each metric’s cognitive test score (WAIS DSST, COWA fas, or CVLT LF, respectively) over brain imaged volumetric feature (overall volume, WMH volume, or hippocampus volume as % intracranial volumes, respectively), with low tertile colored red, middle in blue, and high in green, tertiles had clear separation and consistent linear associations for the WAIS-Brain metric, less clear separation but consistent linear associations for the CVLT-Hipp metric, and somewhat clear separation and inconsistent linear associations for the COWA-WMH metric.
Comparing in a heatmap these three metrics of cognitive reserve with sociodemographic, clinical, and psychological features (Fig. 2), better cognitive reserve (higher residual values) was significantly associated with more years of formal education (WAIS-Brain ρ = 0.45; 95% CI: 0.40, 0.51; P < 0.001and COWA-WMH ρ = 0.48; 95% CI: 0.42, 0.53; P < 0.001), and not significant for CVLT-Hipp (ρ = 0.08; 95% CI: 0.01, 0.15; P = 0.06). Higher income was also significantly associated with the three metrics of cognitive reserve (WAIS-Brain ρ = 0.3, P < 0.001, COWA-WMH ρ = 0.3, P < 0.001, CVLT-Hipp ρ = 0.1, P < 0.001). Diabetes (WAIS-Brain ρ = −0.1 P = 0.001, COWA-WMH ρ = −0.1, P = 0.001) and depression (WAIS-Brain ρ = −0.1, P < 0.001, COWA-WMH ρ = −0.1, P < 0.001, CVLT-Hipp ρ = −0.1, P = 0.02) were significantly associated with lower cognitive reserve, although diabetes was not associated with CVLT-Hipp (ρ = 0.0, P = 0.5). APOEe4 allele status, field center, overweight/obesity, hypertension, chronic kidney disease (CKD), and alcohol use were not statistically associated with the three metrics of cognitive reserve. Boxplots with scatter overlay (Fig. 3) display the distribution of each of the three metrics of cognitive reserve, over four categories of education graphically suggested dose-dependent associations for WAIS-Brain and COWA-WMH metrics of cognitive reserve.
Heatmap with coloration from red (strongest negative association) to green (strongest positive association), with yellow as intermediary values), and overlaid rho Pearson correlation coefficients and P values for associations of three metrics for cognitive reserve: residuals of Weschler Adult Intelligence Scale Digit Symbol Coding Test (WAIS DSST) over brain volume as percent intracranial volume (WAIS-Brain), residuals of Controlled Oral Word Association f/a/s test (COWA) over white matter hypointensities volume (MRI T1 sequence) as percent intracranial volume (COWA-WMH), and residuals of California Verbal Learning Test version II short form long delay free recall test (CVLT LF) over hippocampus volume as percent intracranial volume (CVLT-Hipp) with each other and with sociodemographic & clinical features. All metrics of cognitive reserve defined by regression of cognitive test score over brain imaging feature, adjusted for age and sex. Numbers included in the analysis: WAIS-Brain Visit 1 n = 765, COWA-WMH Visit 1 n = 765, CVLT-Hipp Visit 1 n = 744.
Boxplots (mean, 25th and 75th percentiles), with scatter overlay, and whisker bars (10th and 90th percentiles) for three metrics of cognitive reserve, over categories of education (less than high school, <HS; high school graduate, HS; any college; college graduate degree and beyond, BA/BS). Cognitive reserve metrics include (top) residuals of Weschler Adult Intelligence Scale Digit Symbol Coding Test (WAIS DSST) over brain volume as percent intracranial volume (WAIS-Brain), (middle) residuals of Controlled Oral Word Association f/a/s test (COWA) over white matter hypointensities volume (MRI T1 sequence) as percent intracranial volume (COWA-WMH), and (bottom) residuals of California Verbal Learning Test version II short form long delay free recall test (CVLT LF) over hippocampus volume as percent intracranial volume (CVLT-Hipp). All metrics of cognitive reserve defined by regression of cognitive test score over brain imaging feature, adjusted for age and sex. Numbers included in the analysis: WAIS-Brain Visit 1 n = 765, COWA-WMH Visit 1 n = 765, CVLT-Hipp Visit 1 n = 744.
Using ANOVA to examine associations of tertiles of the three metrics of cognitive reserve—defined at Visit 1, with plasma biomarkers for Alzheimer’s disease and related dementias—defined at Visit 2 (Table 2), only NfL had a significant association with COWA-WMH (tertile 1 to tertile 3 residual mean difference 10.2, P = 0.006). Of note, several of the comparisons showed significant departure from equal variance (i.e., significant Bartlett chi2 test) across tertiles (categories) of cognitive reserve: WAIS-Brain metric with all four of the plasma biomarkers, COWA-WMH and CVLT-Hipp metrics with pTau and amyloid beta, and CVLT-Hipp with NfL.
Longitudinal regression analyses for tertiles of the 3 metrics of cognitive reserve—defined at Visit 1, with cognitive test scores—collected at Visit 2 (Table 3) detected generally consistent, significant associations of earlier cognitive reserve with later cognitive test performance. General cognition (3MSE; MoCA), processing speed (WAIS DSST) verbal fluency (COWA fas), semantic fluency (animal naming, vegetable naming, MINT), contextual memory (Craft story immediate and delayed recall), and executive function or attention (number span forward and backward, Trail Making Test A and B) were all significantly associated with cognitive reserve measured a mean of 6.7 years earlier (range: 4–9 years). Analysis of visual processing and memory (Benson figure copy and recall) and verbal learning and memory (CVLT LF) scores were statistically associated with COWA-WMH and CVLT-Hipp metrics, but did not have statistical evidence of association with the WAIS-Brain metric.
Given positive associations of cognitive reserve with education, depression, and diabetes, as well as with cognitive test scores, causal mediation analysis examined the proportion of mediated effect for models with education, depression, or diabetes as exposure, metric of cognitive reserve—WAIS-Brain, COWA-WMH, or CVLT-Hipp—as mediator, and composite cognitive test score performance (Z-scale) as outcome, with adjustment for age and sex and robust standard errors estimation (Table 4). Of the three exposures considered, only education had a significant mediation (indirect) effect: accounting for an estimated 24% (95% CI: 5-44%, P = 0.014) of the WAIS-Brain metric association with later overall cognitive test performance, and accounting for estimated 15% (95% CI: 0–29%, P = 0.045) of the COWA-WMH metric association with later overall cognitive test performance.
Discussion
Overall, these findings suggest that cognitive reserve—conceptualized as observed-over-expected cognitive performance and defined using three separate metrics—is positively associated with sociodemographic, clinical, psychological, and cognitive features of aging in American Indian older adults. This examination of cognitive reserve in American Indians compared cognitive reserve using 3 separate metrics: WAIS-Brain, a general metric reflecting processing speed and overall volumetric change; COWA-WMH, a vascular-sensitive metric reflecting changes in phonemic fluency with small vessel disease; and CVLT-Hipp, a memory-sensitive metric attuned to changes in a region targeted preferentially by Alzheimer’s disease.
Income and depression were strongly and consistently associated with all three metrics of cognitive reserve (WAIS-Brain; COWA-WMH; CVLT-Hipp); education and diabetes are consistently associated with 2 of the metrics (WAIS-Brain, COWA-WMH). Kidney disease was associated only with COWA-WMH metric, as was the NfL plasma biomarker. In longitudinal analyses, all three metrics (WAIS-Brain; COWA-WMH; CVLT-Hipp) were also strongly related to cognitive test performance over time, in all cognitive domains except memory. Finally, causal analysis of education with cognitive test performance showed significant mediation (direct effect estimation) by WAIS-Brain (24%) and COWA-WMH (15%) metrics of cognitive reserve. Overall, these findings suggest that some metrics of cognitive reserve may be more informative than others, with patterns of association specific to their definition, but overall such metrics are generally consistent in associations with key social and clinical determinants, thus representing potentially modifiable protective processes in aging.
Our findings of strong and consistent associations for observed-over-expected performance with education, independent of age, are consistent with theoretical models that cognitive reserve is built over a lifetime, developed in early childhood through educational development in cognitive plasticity40,41. Such a model suggests that cognitive reserve, once built, may also be deconstructed through exposure to especial challenges such as socioeconomic deprivation42 or chronic stress43, also consistent with our findings of negative associations with depression. Aside from the processing speed-overall volume (WAIS-Brain) associations, the strongest associations were for executive function and phonemic fluency and small vessel injury (COWA-WMH), especially with income and depression; associations for the metric related to memory (CVLT-Hipp) were not as strong or consistent as for the other two metrics.
APOEe4, ADRD plasma biomarkers, hypertension, body mass, field center (region), or alcohol use did not have detectable statistical evidence of association with metrics of cognitive reserve in these analyses. Other ways to conceptualize cognitive reserve may yield different results. Also, some of these results may reflect from lack of variance in the measures, such as for alcohol; with few users and low use among users, associations due to variability in alcohol use may be difficult to detect. However, education and income, depression, and diabetes—and to a lesser extent kidney disease—have consistently had strong associations with cognitive function, brain imaging and neuropathological findings, and other measures of ADRD in this population20,23,26,44,45, which is consistent with these findings. It is possible that these are key variables to risk and resilience in this population. Future research should examine whether these association patterns are consistent for other Tribes and regions, other populations, and whether addressing the much higher prevalence of vascular disease and dementia may influence the balance of these associations for future generations18,19.
Prior, cross-sectional research in non-Hispanic white Americans identified associations for a similarly-defined measure of cognitive reserve with cognitive test scores, with non-Alzheimer’s disease pathology, and with APOEe4 genotype10. We found associations with education, depression, diabetes, and with other socioeconomic and clinical conditions. In longitudinal analyses, later cognition was associated with earlier cognitive reserve, independent of age, sex, baseline cognition, and time between examinations. Future research should examine associations with other neurological conditions.
Limitations
Although causal sequence and temporality is not directly observable in cross-sectional associations, formative and environmental features such as education are likely to represent precursors to cognitive reserve, both directly and indirectly. On the other hand, differential cognitive reserve may be either a contributor or an effect of disease comorbidities such as diabetes and depression. In our longitudinal analyses, cognitive reserve was a significant mediator of only the associations for education. However, two timepoints may not be adequate for answering causal longitudinal questions, and future research may benefit from evaluation of younger populations, more timepoints, and additional measures of cognitive reserve.
Our population included American Indian participants from multiple Tribes and communities in the United States Southwest, Southern Plains, and Northern Plains, but these findings may not generalize to other Tribal groups, regions, or generational cohorts. Cognitive tests may have differential validity across cultural groups, which can affect the generalizability of findings, although preliminary psychometrics in our study population (with more forthcoming) suggest similar test score interpretability as in other populations37,38, with the exception that scores must be interpreted according to education and bilingual experience. Discriminant properties of cognitive test score cutoffs, in particular, require adjustment and validation for appropriate diagnostics—both for impaired, as well as for evaluation of “super-agers”, or those who maintain healthy cognition despite advanced age and irrespective of pathology status. Also, due to the selection structure of this longitudinal cohort, our findings may be subject to an increased likelihood of Type II error if the outcome (e.g., cognitive resilience) is unduly influenced by the likelihood of survival to participation over Visits, although the metrics evaluated appear similar between the two visits. Finally, other types of resilience, such as psychological or community resilience have yet to be explored in this context. Ongoing research in these communities aims to provide insights into this area in the future.
Conclusion
In summary, this description of cognitive reserve in American Indians suggests that cognitive reserve is strongly associated with education, other socioeconomic factors, depression, diabetes and other clinical factors, and later cognitive changes. This work also suggests that some metrics of cognitive reserve (e.g., residuals of processing speed over total brain volume or residuals of verbal fluency over white matter lesion burden) may be better markers or determinants of overall cognitive reserve than others (e.g., residuals of memory over hippocampal volume), although each metric has unique and specific association patterns. This work has the potential to inform understanding of risk and prevention for Alzheimer’s disease and related dementias.
Data availability
Data from the Strong Heart Study and its ancillary studies cannot be made publicly available, but can be accessed—per study and Tribal policies—as described on the Strong Heart Study website: https://strongheartstudy.org.
Code availability
Statistical code for these analyses is available at https://github.com/astridsd/CommPsychol2025.
References
Stern, Y. et al. A framework for concepts of reserve and resilience in aging. Neurobiol. Aging 124, 100–103 (2023).
Stern, Y., Barnes, C. A., Grady, C., Jones, R. N. & Raz, N. Brain reserve, cognitive reserve, compensation, and maintenance: operationalization, validity, and mechanisms of cognitive resilience. Neurobiol. Aging 83, 124–129 (2019).
Joshi, M. S. & Galvin, J. E. Cognitive resilience in brain health and dementia research. J. Alzheimers Dis. 90, 461–473 (2022).
Franzmeier, N. et al. Left frontal cortex connectivity underlies cognitive reserve in prodromal Alzheimer disease. Neurology 88, 1054–1061 (2017).
Zahodne, L. B., Stern, Y. & Manly, J. J. Differing effects of education on cognitive decline in diverse elders with low versus high educational attainment. Neuropsychology 29, 649–657 (2015).
Stern, Y. Cognitive reserve. Neuropsychologia 47, 2015–2028 (2009).
Valenzuela, M. J. & Sachdev, P. Brain reserve and dementia: a systematic review. Psychol. Med. 36, 441–454 (2006).
Verney, S. P. et al. The associations among sociocultural factors and neuropsychological functioning in older American Indians: the Strong Heart Study. Neuropsychology https://doi.org/10.1037/neu0000574 (2019).
Jones, R. N. et al. Conceptual and measurement challenges in research on cognitive reserve. J. Int. Neuropsychol. Soc. 17, 593–601 (2011).
Yao, T., Sweeney, E., Nagorski, J., Shulman, J. M. & Allen, G. I. Quantifying cognitive resilience in Alzheimer’s Disease: the Alzheimer’s disease cognitive resilience score. PLoS ONE 15, e0241707 (2020).
Guo, W. & Shi, J. White matter hyperintensities volume and cognition: a meta-analysis. Front. Aging Neurosci. 14, 949763 (2022).
Nelson, P. T. & Jicha, G. A. Early hippocampal atrophy is an important signal for clinicians but not necessarily a harbinger of Alzheimer disease. Neurology 101, 1087–1088 (2023).
Kelley, A. & Small, C. Establishing the reliability and validity of the sources of strength in one American Indian community. Am. Indian Alsk Native Ment. Health Res. 23, 84–92 (2016).
Kahn, C. B. et al. American Indian Elders’ resilience: sources of strength for building a healthy future for youth. Am. Indian Alsk. Native Ment. Health Res. 23, 117–133 (2016).
Ore, C. E., Teufel-Shone, N. I. & Chico-Jarillo, T. M. American Indian and Alaska native resilience along the life course and across generations: a literature review. Am. Indian Alsk. Native Ment. Health Res. 23, 134–157 (2016).
Nikolaus, C. J., Sinclair, K., Buchwald, D. & Suchy-Dicey, A. M. Association of stress and resilience with cardiometabolic health among American Indian and Alaska Native adults. Prev. Med. Rep. 24, 101517 (2021).
Suchy-Dicey, A. et al. Psychological and social support associations with mortality and cardiovascular disease in middle-aged American Indians: the Strong Heart Study. Soc. Psychiatry Psychiatr. Epidemiol. 57, 1421–1433 (2022).
Suchy-Dicey, A. M. et al. Epidemiology and prevalence of dementia and Alzheimer’s disease in American Indians: data from the Strong Heart Study. Alzheimers Dement. 20, 4174–4184 (2024).
Suchy-Dicey, A. M. et al. Plasma biomarkers of Alzheimer’s disease and related dementias in American Indians: the strong Heart Study. Alzheimers Dement. 20, 2072–2079 (2024).
Suchy-Dicey, A., Howard, B., Longstreth, W. T. Jr., Reiman, E. M. & Buchwald, D. APOE genotype, hippocampus, and cognitive markers of Alzheimer’s disease in American Indians: data from the Strong Heart Study. Alzheimers Dement. 18, 2518–2526 (2022).
Shibata, D. et al. Vascular risk factors and findings on brain MRI of elderly adult American Indians: the strong Heart Study. Neuroepidemiology 52, 173–180 (2019).
Cholerton, B. et al. Type 2 diabetes and later cognitive function in older American Indians: the Strong Heart Study. Int. J. Geriatr. Psychiatry 34, 1050–1057 (2019).
Suchy-Dicey, A., Su, Y., Buchwald, D. S., Manson, S. M. & Reiman, E. M. Volume atrophy in medial temporal cortex and verbal memory scores in American Indians: data from the Strong Heart Study. Alzheimers Dement. https://doi.org/10.1002/alz.12889 (2022).
Suchy-Dicey, A. et al. Cognitive correlates of MRI-defined cerebral vascular injury and atrophy in elderly American Indians: the strong Heart Study. J. Int. Neuropsychol. Soc. 26, 263–275 (2020).
Lee, E. T. et al. The strong Heart Study. a study of cardiovascular disease in American Indians: design and methods. Am. J. Epidemiol. 132, 1141–1155 (1990).
Suchy-Dicey, A. M. et al. Educational and clinical associations with longitudinal cognitive function and brain imaging in American Indians: the Strong Heart Study. Neurology 99, e2637–e2647 (2022).
Wechsler, D. Wechsler Adult Intelligence Scale—Fourth Edition Administration and Scoring Manual. (Pearson, San Antonio, TX, 2008a).
Benton, A. L. & Hansher, K. Multilingual Aphasia Examination 2nd edn. (AJA Associates, 1976).
Delis, D. C., Kramer, J. H., Kaplan, E. & Ober, B. A. California Verbal Learning Test (CVLT-II) 2nd edn. (The Psychological Corporation, 2000).
Teng, E. L. & Chang Chui, H. The modified mini-mental (3MS) examination. J. Clin. Psychiatry 48, 314–318 (1987).
Morris, J. C. et al. The uniform data set (UDS): clinical and cognitive variables and descriptive data from Alzheimer Disease Centers. Alzheimer Dis. Assoc. Disord. 20, 210–216 (2006).
Nasreddine, Z. S. et al. The Montreal Cognitive assessment, MoCA: a brief screening tool for mild cognitive impairment. J. Am. Geriatr. Soc. 53, 695–699 (2005).
Possin, K. L., Laluz, V. R., Alcantar, O. Z., Miller, B. L. & Kramer, J. H. Distinct neuroanatomical substrates and cognitive mechanisms of figure copy performance in Alzheimer’s disease and behavioral variant frontotemporal dementia. Neuropsychologia 49, 43–48 (2011).
Liew, T. M. Developing a brief neuropsychological battery for early diagnosis of cognitive impairment. J. Am. Med. Dir. Assoc. 20, 1054.e1011–1054.e1020 (2019).
Llinas-Regla, J. et al. The trail making test. Assessment 24, 183–196 (2017).
Ivanova, I., Salmon, D. P. & Gollan, T. H. The multilingual naming test in Alzheimer’s disease: clues to the origin of naming impairments. J. Int. Neuropsychol. Soc. 19, 272–283 (2013).
Suchy-Dicey, A. M. et al. Psychometric reliability, validity, and generalizability of 3MSE scores among American Indian adults: the Strong Heart Study. J. Int. Neuropsychol. Soc. 30, 454–463 (2024).
Suchy-Dicey, A. M. et al. Psychometric properties of controlled oral word association (COWA) test and associations with education and bilingualism in American Indian adults: the Strong Heart Study. Assessment 31, 745–757 (2024).
Suchy-Dicey, A. M. et al. Psychometric reliability, validity, and generalizability of MoCA in American Indian adults: the Strong Heart Study. Assessment https://doi.org/10.1177/10731911241261436 (2024).
Lovden, M., Backman, L., Lindenberger, U., Schaefer, S. & Schmiedek, F. A theoretical framework for the study of adult cognitive plasticity. Psychol. Bull. 136, 659–676 (2010).
2024 Alzheimer’s disease facts and figures. Alzheimers Dement. 20, 3708–3821 (2024).
Johnson, N. F., Kim, C. & Gold, B. T. Socioeconomic status is positively correlated with frontal white matter integrity in aging. Age 35, 2045–2056 (2013).
McEwen, B. S. The brain on stress: toward an integrative approach to brain, body, and behavior. Perspect. Psychol. Sci. 8, 673–675 (2013).
Suchy-Dicey, A. et al. Depression symptoms and cognitive test performance in older American indians: the Strong Heart Study. J. Am. Geriatr. Soc. 68, 1739–1747 (2020).
Suchy-Dicey, A. M. et al. Findings of vascular brain injury and structural loss from cranial magnetic resonance imaging in elderly American Indians: the Strong Heart Study. Neuroepidemiology 48, 39–47 (2017).
Acknowledgements
The authors wish to thank all Strong Heart Study staff, participants, and communities. This study has been funded in whole or in part with federal funds from the National Institutes of Health, including K01AG057821, P50AG005136, R01HL093086, and R01AG070822. The Strong Heart Study has been funded in whole or in part with federal funds from the National Heart, Lung, and Blood Institute under contract numbers 75N92019D00027, 75N92019D00028, 75N92019D00029, and 75N92019D00030. The study was previously supported by research grants: R01HL109315, R01HL109301, R01HL109284, R01HL109282, and R01HL109319 and by cooperative agreements: U01HL41642, U01HL41652, U01HL41654, U01HL65520, and U01HL65521. The funders had no role in study design, data collection and analysis, the decision to publish, or the preparation of the manuscript. The opinions expressed in this paper are solely the responsibility of the author(s) and do not necessarily reflect the official views of the Indian Health Service or the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
All authors (A.M.S.-D., T.J.G., W.T.L., K.R., D.S.B.) contributed to data colleciton; A.M.S.-D. and T.J.G. conceptualized hypotheses; A.M.S.-D., W.T.L., and K.R. finalized analytic models; A.M.S.-D. conducted analyses; A.M.S.-D. wrote the manuscript; all authors (A.M.S.-D., T.J.G., W.T.L., K.R., and D.S.B.) contributed to manuscript editing and results interpretation.
Corresponding author
Ethics declarations
Competing interests
The authors (A.M.S.-D., T.J.G., W.T.L., K.R., and D.S.B.) declare no competing interests.
Peer review
Peer review information
Communications Psychology thanks Patrick Pflanz, Antoine Trammell and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Primary Handling Editors: Claudia von Bastian and Jennifer Bellingtier. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Suchy-Dicey, A.M., Longstreth, W.T., Buchwald, D.S. et al. Cognitive reserve is associated with education, social determinants, and cognitive outcomes among older American Indians in the Strong Heart Study. Commun Psychol 3, 14 (2025). https://doi.org/10.1038/s44271-025-00198-6
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s44271-025-00198-6