Abstract
Iron metabolism disorder has been identified as a contributor to the pathogenesis and progression of multiple cognitive dysfunction-related diseases, including postoperative delirium. However, the association between preoperative iron reserves and postoperative delirium risk remains elusive. This retrospective cohort study aimed to explore the impact of preoperative serum ferritin levels on the risk of postoperative delirium in elderly patients undergoing non-neurosurgical and non-cardiac procedures. Conducted at the Chinese PLA General Hospital between January 2014 and December 2021, the study finally included 12,841 patients aged 65 years and above. Preoperative serum ferritin levels were assessed within 30 days before surgery, and postoperative delirium occurrence within the first seven days after surgery was determined through medical chart review. The analyses revealed that both low and high levels of serum ferritin were associated with an increased risk of postoperative delirium. Patients in the lowest quintile of serum ferritin exhibited an 81% increased risk, while those in the highest quintile faced a 91% increased risk compared to those in the second quintile. Furthermore, mediation analyses indicated that the direct effect of preoperative serum ferritin on postoperative delirium contradicted its indirect effect mediated by hemoglobin levels. These findings suggest that maintaining serum ferritin within moderate range preoperatively could be beneficial for managing postoperative delirium risk among elderly patients.
Similar content being viewed by others
Introduction
Postoperative delirium (POD) is an acute neuropsychiatric syndrome characterized by fluctuating changes in cognition, attention, and consciousness after surgery, especially common in a rapidly growing aging population [1, 2]. This condition is associated with increased morbidity, impaired long-term cognitive function [3], and higher rates of hospital readmissions and mortality [4]. Despite these significant clinical implications, the underlying mechanisms driving POD are not fully understood, underscoring the need for more targeted biomarkers to elucidate its pathophysiology.
There are several theories regarding the pathophysiology of POD, predominantly derived from findings in animal models [5]. These theories encompass a spectrum of mechanisms, including neuroinflammation, disturbances in neurotransmitter balance, subclinical cerebral vascular events, and breaches in the blood-brain barrier integrity. Among these, oxidative stress and cellular damage mechanisms, such as ferroptosis—a form of regulated cell death dependent on iron—have been increasingly recognized as critical contributors to the pathogenesis of POD [6,7,8,9,10]. Iron, a central element in various cellular processes, becomes a double-edged sword when in excess, leading to the generation of reactive oxygen species (ROS) and subsequent oxidative damage cascading by means of Fenton reaction, where ferrous iron reacts with hydrogen peroxide to produce highly reactive hydroxyl radicals that can cause significant damage to cellular components, including lipids, proteins, and DNA and ultimately lead to ferroptosis [11, 12]. Despite the insights gained from animal models, the translation of these findings to human populations has been constrained by the limited availability of robust human study data.
Emerging researches have indicated that central iron deposits may stem from dysregulated peripheral iron homeostasis, leading to abnormal iron accumulation in the bloodstream [13,14,15]. Recent studies have highlighted the role of peripheral iron status in cognitive disorders, where dysregulated iron metabolism and oxidative stress are implicated in neuronal injury and cognitive deficits [15, 16]. However, a systematic report about the association between peripheral iron status and POD is not found in our literature research.
The current study hypothesizes that iron redundancy may push the elderly patients to more susceptible conditions. Therefore, serum ferritin (SF) levels, traditionally recognized as the most accurate indicator of total body iron reserves, may serve as a critical biomarker in the context of POD [17]. Consequently, this research aims to investigate the predictive effect of SF levels on POD risk among elderly patients aged 65 and above undergoing non-neurosurgical and non-cardiac procedures in depth utilizing a large clinical database from China.
Materials and methods
Data source
This retrospective, observational cohort study was in accordance with the Declaration of Helsinki and was authorized by the Ethics Committee of Chinese PLA General Hospital (No.S2023-788-02). The present cohort study was analyzed and hereby reported in compliance with the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines [18]. All methods used in this study were performed in accordance with relevant guidelines and regulations.
Study population
Patients in Chinese PLA General Hospital from January 2014 to December 2021 meeting the following criteria were included: (1) age ≥ 65 years, (2) undergoing non-neurosurgical and non-cardiac procedures, and (3) with measurements of preoperative SF and identification of POD events. Patients meeting the following criteria were excluded: (1) preoperative use of antipsychotics, or (2) diagnosis or history description of preoperative cognitive disorders including dementia and Parkinson’s diseases.
Data collection and definitions
Demographic information, preexisting comorbidities, baseline laboratory examination, and operation related materials were retrospectively retrieved and extracted from Electronic Medical Record (EMR) systems, including the patient record integrated management system (PRIDE 2.1.2.193, Heren Health, China) and the anesthesia information management system (DoCare 3.1.0 build 153, MEDICALSYSTEM, China) using the SQL Server (Microsoft, USA). The International Classification of Diseases version 10 (ICD-10) was used as the criterion for identifying illnesses. Demographic data included age, sex, weight, and height. Preexisting comorbidities data including preoperative use of antipsychotics, diagnosis or history of preoperative cognitive disorders, renal insufficiency, diabetes mellitus, cancer, and anemia were identified. The baseline laboratory examination values including hemoglobin (Hb) levels, plasma neutrophil and lymphocyte counts, total bilirubin (TBil), and alanine aminotransferase (ALT) were adopted based on the latest records within 30 days before surgery from EMR. Neutrophil-to-lymphocyte ratio (NLR) was calculated using the following formula: neutrophil (109/L)/lymphocyte (109/L). Body mass index (BMI) was calculated by dividing weight (kg) by the square of height (m). Considering that there are no recognized diagnostic criteria for dystrophy to date, BMI was used as one quantifiable surrogate of nutritional status, defining a BMI of less than 18.5 kg/m2 as dystrophy. Stress and systemic inflammation were effectively assessed by NLR, with an NLR of more than three defined as indicative of inflammation status [19]. Hepatic function was assessed using a combination of ALT and TBil, which indicates the extent of hepatic damage, hepatic secretory and excretory function, respectively. Surgery related data included the surgery type, specialty, and duration.
Exposure and outcome identification
Preoperative SF is routinely detected as an indicator commonly for cancer and anemia in preoperative biochemical examination package. In this study, preoperative SF was also obtained from the EMR using the most recent data within 30 days before surgery.
The outcome was the occurrence of POD within the first seven days following surgery. Since this study was conducted retrospectively, the utilization of the Confusion Assessment Method (CAM) scale for assessing delirium was not feasible. Medical chart review, a method that has been validated in medical and critical care unit patients and used to identify delirium in a range of medical and surgical patients with 74% sensitivity and 83% specificity, and overall agreement was 82% in older adults, was used for POD determination in this study [20,21,22]. The defining criteria were as follows: (1) delirium-related terms (“mental status change”, “confusion”, “disorientation”, “agitation”, “delirium”, “inappropriate behavior”, “inattention”, “hallucinations”, “combative behavior”, “drowsy”, “slept poorly”) included in postoperative medical records or (2) postoperative record of delirium or psychotropic drugs treatment, specifically quetiapine, olanzapine, fluphenazine, haloperidol, or risperidone. Patients that fit at least one of the above criteria were first screened by computer from the whole database, and then these preliminarily defined delirium cases were adjudicated by trained neurologists, who were blind to the design, based on the Diagnostic and Statistical Manual of Mental Disorders, Fourth edition (DSM-IV) criteria [23] and the CAM scale [24] to establish the final delirium population [25, 26].
Statistical analysis
Continuous variables with a normal distribution were described as mean with standard deviation (SD), while skewed data were described as median (interquartile range, IQR). Categorical variables were summarized as frequency with percentage. Comparison of continuous and categorical variables among different groups was analyzed by analysis of variance (ANOVA) or the rank sum test and Chi-square test or Fisher’s exact test, as appropriate. Multiple imputation was used for the treatment of missing data. The sample size of this study was confirmed using the 10 Events Per Variable (10 EPV) concept [27], a widely accepted empirical rule for ensuring that each predictive parameter that ends up in the regression equation corresponds to at least ten endpoint events.
Due to the lack of a common set of normal values for SF in elderly population and the difference in normal reference value for men and women, associations between SF levels or predefined SF categories and POD risk were examined. In light of previous pertinent literature [28], five equally distributed categories of SF were defined by the 20th, 40th, 60th, and 80th centiles, and the reference category for these analyses was designated as the SF group with the lowest incidence and risk of POD. Multivariable logistic regression analyses were applied to identify the corresponding odds ratios (ORs) after adjustment for confounding factors. The optimal set for adjustment comprises covariates that, when adjusted for, minimize confounding bias in estimating the association between exposure and outcome. It was identified by constructing a directed acyclic graph (DAG) using DAGitty software [29], which represents a causal one-way network, grounded on theoretical causal relationships. Trend tests for ORs were conducted by using the median value of each quintile of SF as a continuous variable.
For the balance between best fit and overfitting, restricted cubic spline (RCS) analyses with five knots, at the 5th, 27.5th, 50th, 72.5th, and 95th centiles of the log10 SF, were then performed to flexibly model and visualize the association between log10 SF and POD risk. The reference value (OR = 1) was set at median. In the RCS models, we also adjusted for other factors as mentioned above and tested for potential non-linearity. Moreover, as the associations between log10 SF and POD were approximately linear below and above the median, we additionally used a linear model to calculate OR per SD increase in log10 SF.
To evaluate the potential effect modification, we then conducted subgroup analyses according to cancer (present or absent), sex (male or female), age (<75 or ≥75 years), and diabetes mellitus (present or absent) and exhibited as the forest plots. For each factor, we generated a multiplicative term by multiplying the exposure by dichotomous variables used in the multivariable model, assessing multiplicative interactions with a likelihood ratio test.
Moreover, considering that the additional bias may be introduced after controlling for the potential mediator, preoperative Hb was appropriately accounted for by being additionally adjusted. Structural equation modeling was used for simple mediation analysis to estimate whether the association between SF levels and POD risk was mediated by Hb levels. Direct and indirect mediation effects with their 95% confidence interval (CI) were estimated. The significance of the mediation effects was assessed based on 1,000 bootstrap iterations.
Finally, we performed sensitivity analyses to test the robustness of our findings including computing the E-value [30] defined as the minimum strength of association on the OR scale that an unmeasured confounder must have with both SF levels and POD to completely negate the observed association, conditional on the measured covariates.
A two-sided p-value < 0.05 was defined as the statistical threshold. Statistical analyses were performed using R software (version 4.2.2, R Foundation for Statistical Computing, Vienna, Austria).
Results
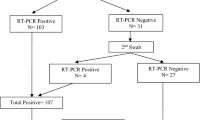
Of the 12,984 elderly patients undergoing non-neurosurgical and non-cardiac procedures, 12,841 were finally enrolled in our study (Fig. 1), 445 (3.5%) of whom developed POD after surgery. At baseline, the median (IQR) SF was 142.10 (65.63-266.40) μg/L, while the mean (SD) Hb was 126.00 (19.26) g/L. The median (IQR) age was 70 (67–75) years. Of the 12,841 patients, 7903 (61.5%) were male, 7659 (59.6%) were diagnosed with cancer, 299 (2.3%) with renal insufficiency, 3152 (24.5%) with diabetes mellitus, and 3265 (25.4%) with anemia. The patients were separated into five groups based on quintiles of SF levels. Further analyses revealed statistically significant variances across the five groups in terms of demographic characteristics, preexisting comorbidities, baseline laboratory examination values, and operation related materials collected in this study. Specifically, the highest proportion of male patients and the highest level of NLR were observed in quintile 5. Additionally, quintile 1 exhibited a higher prevalence of cancer compared to quintile 5. The Hb levels in quintile 1 were significantly lower than those in the other groups. The incidence of renal insufficiency in quintile 5 was markedly higher than in any other group. Furthermore, both TBil and ALT levels in quintile 5 were significantly elevated compared to those in quintile 1. Normality assumptions were checked, and a logarithmic transformation of SF was used for parametric analyses (Supplementary Fig. 1). The distribution of baseline characteristics across SF quintiles is elaborated in Table 1, while Supplementary Table 1 delineates the differences in characteristics between male and female patients. Interestingly, this study observed a higher prevalence of anemia and cancer among males.
Flowchart of study population.
The minimally sufficient adjustment set selected in this study comprises age, sex, dystrophy, inflammation, cancer, hepatic or renal insufficiency, and diabetes mellitus (Supplementary Fig. 2). Given the revealed non-linear trend shown in our exploratory study (Supplementary Table 2) and previous similar studies [28], we selected the continuous and quintile results as our primary outcomes to identify the median SF level group, which is critical for understanding the optimal range of SF levels for POD prevention. Results from logistic regression analyses showed that the multivariable-adjusted OR of log10 SF as a continuous variable was 1.06 (0.87–1.30, p = 0.560). However, after dividing SF levels into quintiles, a critical observation was that in comparison with subjects in quintile 2, the adjusted OR for POD was 1.81 (1.31–2.53, p < 0.001) for subjects in quintile 1, 1.47 (1.04–2.09, p = 0.029) for subjects in quintile 4, and 1.91 (1.37–2.69, p < 0.001) for subjects in quintile 5 (Table 2). These findings revealed a phenomenon of a non-linear link between SF levels and POD risk.
Further, RCS analyses confirmed that there were strong U-shaped associations of SF levels with POD risk even after adjustment for other confounding factors (all p-values for non-linearity < 0.001; Fig. 2A, B). The value of the log10 SF corresponding to an OR equal to 1 was really close to the median level of log10 SF which is 2.15 (corresponding to SF of 158.49 μg/L) in the general population. The graph demonstrated a significant decrease in POD risk at lower levels of preoperative log10 SF, with the nadir of risk occurring at a log10 SF value of around 2.15, beyond which the risk began to escalate. Below this log10 SF threshold of 2.15, the OR per SD increase in predicted POD was 0.69 (0.57–0.83), indicating a protective effect. Conversely, above a log10 SF of 2.15, the OR for each SD increase in predicted POD escalated to 1.67 (1.31–2.12), suggesting an increased risk.
A Unadjusted model. B Multivariable model adjusted for age, sex, BMI, NLR, TBil, ALT, cancer, diabetes mellitus, and renal insufficiency. C Multivariable model additionally adjusted for Hb levels as a potential mediator. ORs are indicated by red solid lines and 95% CIs by dark gray dotted lines. Reference lines for no association are indicated by the gray dotted lines at an OR of 1.0. Density plots are presented by gray shadow area to show the fraction of the population with different levels of log10 SF. The log10 SF level corresponding to the OR equal to 1 (reference value) is shown by dark spot. SF, serum ferritin; POD, postoperative delirium; BMI, body mass index; NLR, neutrophil-to-lymphocyte ratio; TBil, total bilirubin; ALT, alanine aminotransferase; Hb, hemoglobin; OR, odds ratio; CI, confidence interval; SD, standard deviation.
Subgroup analyses verified that the association adopted a more pronounced U-shaped pattern among elderly patients without a cancer diagnosis [OR (95% CI) = 3.71 (1.79–8.43) in quintile 1, 3.65 (1.83–8.10) in quintile 4, 5.37 (2.75–11.76) in quintile 5, and quintile 2 as reference; p for interaction < 0.001]. Moreover, in the male subgroup, an elevated risk of POD was more markedly observed at lower SF levels than in the female subgroup, whereas in females, the risk increase was more pronounced at higher SF levels (p for interaction = 0.028). Across other subgroups, the differences in associations between SF quintiles and POD risk were of no statistical significance, showing no significant interaction effects, as detailed in Fig. 3 and Supplementary Table 3.
Forest plots showed associations in the overall population (A, B) and subgroups (C, D, E, and F). Subgroup analyses were adjusted as in model 2. *p < 0.05, **p < 0.01, ***p < 0.001. SF serum ferritin; POD postoperative delirium; OR odds ratio; CI confidence interval.
Given the robust clinical correlation observed between Hb levels and both SF levels and POD outcomes, an adjustment for Hb levels was further implemented to elucidate its prominent role. Upon comparing the outcomes, it was evident that even after adjusting for Hb levels, a heightened risk of POD associated with elevated SF levels persisted, albeit to a lesser extent at lower SF concentrations within the general population, suggesting a potential mediating role for Hb. To be specific, the additionally Hb-adjusted OR of log10 SF as a continuous variable for POD was 1.27 (1.04–1.55, p = 0.018) with statistical significance. And the additionally Hb-adjusted OR of SF as a categorical variable was 1.44 (1.03–2.04, p = 0.037) for subjects in quintile 1, 1.54 (1.09–2.18, p = 0.015) for subjects in quintile 4, 1.86 (1.33–2.61, p < 0.001) for subjects in quintile 5, and quintile 2 as reference (Table 2). The Hb-adjusted OR per SD increase in predicted POD was 0.79 (0.63–0.99) in the overall population when log10 SF was below 2.15, and 1.50 (1.17–1.91) when log10 SF exceeded 2.15 as shown in RCS analysis (p for non-linearity = 0.003; Fig. 2C).
To elucidate the potential underlying causes of the U-shaped association, mediation analyses were conducted to assess the role of variability in Hb levels. These analyses controlled for the same confounders as identified in the initial association study. The results revealed the direct effect of SF on POD (c’ = 0.788, 95% CI = 0.063 to 0.901, p = 0.002), which was in contrast to its indirect effect mediated through Hb levels (ab = −0.753, 95% CI = −0.802 to −0.066, p = 0.002). The total effect was not statistically significant (c = 0.035, 95% CI = −0.063 to 0.139, p = 0.493), with the proportion of effect suppressed being calculated as 95.56% (|ab/c’|) across the entire study population. The discrepancy in the mediation effect among different subgroups are provided in Fig. 4 and Supplementary Table 4.
Mediation analyses in the overall population (A, B) and subgroups (C, D, E, and F). Subgroup analyses were adjusted as in model 2. a = the effects of log10 SF on Hb; b = the effects of Hb on POD risk. ab: the indirect effect; c: the total effect; c’: the direct effect. *p < 0.05, **p < 0.01, ***p < 0.001. SF serum ferritin; Hb hemoglobin; POD postoperative delirium.
The sensitivity analyses did not significantly modify the results after excluding patients who underwent emergency surgery or had a history of certain comorbidities, changing the method of processing missing values, or adding major intraoperative factors to the multivariable model, among other things (Supplementary Table 5). Additionally, the E-value was counted to be 3.23 for quintile 5 suggesting that, to explain away the observed OR of 1.91, an unmeasured confounder would need to be associated with both SF levels and POD risk with an OR of at least 3.23 each, above and beyond the measured confounders, 3.02 for quintile 1, and 2.3 for quintile 4 (Supplementary Fig. 3).
Discussion
Two key findings were highlighted in this study: (1) The U-shaped association between preoperative SF levels and POD risk was identified. The optimal SF concentration for the lowest POD risk closely aligns with the median log10 SF level of 2.15, equivalent to SF level of 158.49 μg/L, and (2) Hb partially mediates the association between preoperative SF levels and POD risk. This mediation may explain the observed U-shaped association.
The limited iron excretion mechanism in the human body makes individuals susceptible to iron overload, which can result in various health issues. Unfortunately, there is a common focus on “iron deficiency” rather than “iron overload”, even among healthcare professionals. Studies have indicated that iron accumulation in the brain increases with age, contributing markedly to the pathogenesis of neurodegenerative diseases including Alzheimer’s disease [9], Parkinson’s disease [31], and POD [10]. Iron chelation therapy has shown promise in corresponding animal models, yet the exploration of iron’s impact on cognitive function in human clinical studies is still emerging and remains a subject of debate. While certain investigations presented negative conclusions about the association between dietary iron intake and cerebral iron deposition [32], alternative studies propose that iron supplementation could potentially elevate brain iron concentrations, subsequently precipitating cognitive deterioration in humans [16, 33, 34].
Iron overload can be detected clinically through methods like serum biochemistry, cardiac biopsy, liver biopsy, and magnetic resonance imaging. Among these, SF testing is preferred as an accurate indicator of systemic iron stores due to its simplicity, cost-effectiveness, and repeatability. Recent discourse has emphasized the need for research into the association between SF levels and clinical outcomes, particularly in regard to cognitive function. Despite the positive correlation between SF levels and neocortical amyloid-β accumulation according to Goozee et al. [35], a recent study has unveiled a divergent positive relationship between SF levels and executive function [36]. Therefore, this study set out to investigate the correlation between levels of SF and risk of POD among elderly patients, a demographic notably susceptible to both iron overload and cognitive decline, to provide further evidence on this issue.
According to clinically recognized knowledge [37], a decrease in SF levels could be detected in conditions including iron-deficiency anemia and dystrophy. Conversely, an increase in SF levels could occur in cases of primary hyperferritinemia (elevated SF with iron overload) and reactive hyperferritinemia (elevated SF without iron overload). Given that primary hyperferritinemia, with its etiology encompassing preoperative blood product administration and iron supplementation [38], is the focus of our investigation, these factors were not included for adjustment as confounding variables. Instead, the factors that lead to reactive hyperferritinemia including cancer, inflammatory conditions, impaired hepatic and renal function, and diabetes mellitus, were taken into consideration for adjustment. Therefore, the hypotheses of this study are presented in the form of a DAG to select covariates a priori as potential confounders to exclude the impact of confounding factors. Additionally, supplementary analyses were conducted on patients without dystrophy, cancer, inflammatory conditions, or hepatic or renal impairment to accurately assess the iron load in the body.
In this study, 12,841 elderly patients undergoing non-neurosurgical and non-cardiac procedures were finally enrolled. Our study presents a novel and comprehensive examination of the association between preoperative SF levels and the risk of POD in elderly patients. The findings indicate that preoperative SF serves as a bidirectional biomarker for predicting delirium risk in this population, characterized by a U-shaped association, revealing that intermediate levels may confer a protective effect. This finding is significant as it integrates the disparate findings from previous literature, which has separately linked low SF levels to cognitive impairment due to iron deficiency, and high SF levels to cognitive decline secondary to iron overload and oxidative stress [14, 16, 39, 40]. To our knowledge, this is the first study to simultaneously investigate the bidirectional effects of SF on cognitive impairment within the perioperative context. The unique contribution of our research lies in its ability to elucidate the complex interplay between SF levels and cognitive outcome in a surgical population. This has direct implications for perioperative care, suggesting that clinicians should be vigilant in monitoring SF levels and considering interventions that can stabilize these levels to reduce the risk of POD. This relationship may be underpinned by several mechanisms as follows. Primarily, prolonged excessive iron accumulation could heighten the risk of iron-induced oxidative stress, predisposing elderly individuals to neuroinflammation, which is a contributing factor to the pathogenesis of POD. Additionally, iron is critical for Hb synthesis, and its deficiency may disrupt hematopoiesis, potentially leading to iron deficiency anemia [41]. This condition, coupled with poor nutritional status and reduced Hb levels, has been associated with diminished cognitive function [42], suggesting a complex interplay between preoperative iron levels and POD risk. Moreover, iron is integral to numerous vital neurobiological processes, and its scarcity could impair these functions. It is noteworthy, however, that while iron deficiency is known to negatively impact cognition during critical developmental periods in youth [40], the relationship between brain iron levels and cognitive function in the elderly appears to be inverse: elevated brain iron is correlated with neurodegeneration and cognitive impairment, as highlighted in the research by Ghadery et al. [43] and Zucca et al. [44].
Delving deeper into our analysis, we observed that the relationship between low SF levels and the increased risk of POD was pronounced in the multivariate model. However, this association weakened significantly, with the 95% CIs encompassing an OR of 1.0, upon further adjustment for Hb levels, as evidenced in RCS analyses. Conversely, the correlation between elevated SF levels and POD risk remained relatively stable across all three analytical models. Importantly, the mediation analysis revealed that the direct effect of SF on POD is positive, indicating that higher SF levels are associated with an increased risk of POD. However, this direct effect is counterbalanced by an indirect effect mediated through Hb levels, a phenomenon often characterized as a “suppression effect” in the literature, a term widely recognized from the work of Shrout and Bolger [45]. The contrasting nature of the direct and indirect effects results in a total effect of SF on POD that is not statistically significant. This finding is particularly intriguing when considering the additional adjustment for Hb in our multivariate analysis, which suggests that the inverse indirect effect is more pronounced in the low SF range. This observation may provide a key to understanding the underlying mechanism of the non-linear, U-shaped relationship observed between preoperative SF and POD in our study, especially in patients with lower SF levels.
Subgroup analyses in this study have illuminated several insights. Notably, the diminished impact of SF within the cancer patient subgroup may arise from an epiphenomenon whereby various cancer cells prolifically secrete SF, rendering SF levels in cancer patients an unreliable marker of actual iron reserves. Furthermore, the investigation uncovered that the U-shaped association between SF levels and POD risk did not exhibit uniform curvature across different sexes. Specifically, in elderly male patients, the correlation between low SF levels and heightened POD risk was more pronounced compared to their female counterparts. This variance could be attributed to sex differences in the mediating effects of Hb, as evidenced by subgroup mediation analyses. An underlying mechanism for this observation may be the higher prevalence of anemia and stronger correlation between SF and Hb levels in the male cohort of the study aligning with previous findings that anemia is more prevalent among elderly males. This discrepancy is potentially due to lower testosterone levels and diminished erythropoietin production in this demographic [46]. Contrary to females, elderly males did not display a markedly increased risk of POD at elevated SF levels, possibly reflecting the higher cancer incidence observed in males within this study, corroborating earlier research that indicates a significantly higher cancer prevalence among men over 60 compared to women [47].
The crux of addressing delirium, especially among high-risk elderly individuals, lies in its prevention. To our knowledge, this study represents the first, most comprehensive, and extensive exploration into the association between preoperative systemic iron stores and POD in the elderly demographic. We have meticulously examined the nonlinear dynamics between preoperative SF levels and POD occurrences, identifying a U-shaped relationship in this population, with Hb levels playing a mediating role for the first time. These findings contribute valuable scientific insights and furnish an evidence-based foundation for understanding POD pathogenesis, potentially leading to the development of novel therapeutic strategies. Clinicians could use preoperative SF as a biomarker to identify elderly patients at increased risk for POD. This could lead to more targeted preoperative assessments and interventions, potentially including nutritional support or iron supplementation for those with low SF levels, and comprehensive monitoring and refined management of iron overload for those with high SF levels. This could involve dietary interventions, pharmacological treatments, or other strategies aimed at normalizing SF levels preoperatively. Moreover, the findings from our study open up avenues for future research, including randomized controlled trials to evaluate the efficacy of interventions aimed at modulating SF levels in reducing the incidence of POD. These contributions serve as an essential reference for healthcare practitioners engaged in the care of this vulnerable group.
However, several limitations should be noted. Firstly, given the retrospective design of this study, a chart-based approach was utilized, which is particularly adept at identifying delirium in severe cases or hyperactive delirium compared with the CAM method. Nevertheless, in clinical practice, it is usually the severe cases of delirium that always need urgent intervention due to their poor prognosis, and the hyperactive delirium that leads to severe events such as falling out of bed or pulling out tubes. Therefore, despite the limitations, the findings of this study remain valuable for predicting and warning against severe or hyperactive cases of delirium in clinical practice [48]. Moreover, the necessity for a large sample size, especially before delirium evaluation became a standard postoperative procedure, justified the use of a retrospective database. Secondly, with a focus on a single site from China, the findings may not extend well to broader populations or contexts. Therefore, caution is advised when extrapolating conclusions from this study. Additionally, despite comprehensive adjustments for numerous covariates to minimize confounding effects based on DAG, unmeasured and residual confounders that are not available in the dataset, such as socio-economic status and education level, remain. However, the likelihood of an unmeasured confounder having a more substantial association with SF levels and POD risk than those documented in existing literature appears slim [49], as suggested by the calculated E-values. In summary, these findings warrant a cautious interpretation and highlight the need for further research to elucidate the causal pathways and the clinical implications of these relationships.
Conclusion
Taken together, both low and high levels of preoperative SF are associated with elevated POD risk in elderly patients after non-neurosurgical and non-cardiac procedures. Keeping SF at moderate levels may help reduce POD risk in this vulnerable population. This study will not only enhance our understanding of the complex interplay between iron metabolism and cognitive health but also potentially guide the development of targeted interventions to reduce POD risk.
Data availability
Upon reasonable request, the corresponding author can provide access to the data supporting the findings of this study.
Code availability
Upon reasonable request, the corresponding author can provide access to the code supporting the findings of this study.
References
Inouye SK, Westendorp RGJ, Saczynski JS. Delirium in elderly people. Lancet. 2014;383:911–22.
Oh ES, Fong TG, Hshieh TT, Inouye SK. Delirium in older persons: advances in diagnosis and treatment. JAMA. 2017;318:1161–74.
Austin CA, O’Gorman T, Stern E, Emmett D, Stürmer T, Carson S, et al. Association between postoperative delirium and long-term cognitive function after major nonemergent surgery. JAMA Surg. 2019;154:328–34.
Li T, Li J, Yuan L, Wu J, Jiang C, Daniels J, et al. Effect of regional vs general anesthesia on incidence of postoperative delirium in older patients undergoing hip fracture surgery: The RAGA randomized trial. JAMA. 2022;327:50–8.
Jin Z, Hu J, Ma D. Postoperative delirium: perioperative assessment, risk reduction, and management. Br J Anaesth. 2020;125:492–504.
Zhang X, Cao J, Zhang L, Li Y, Mi W. Deferoxamine attenuates lipopolysaccharide-induced neuroinflammation and memory impairment in mice. J Neuroinflammation. 2015;12:20.
Li Y, Sun M, Cao F, Chen Y, Zhang L, Li H, et al. The ferroptosis inhibitor liproxstatin-1 ameliorates LPs-induced cognitive impairment in mice. Nutrients. 2022;14:4599.
Sun M, Li Y, Liu M, Li Q, Shi L, Ruan X, et al. Insulin alleviates lipopolysaccharide-induced cognitive impairment via inhibiting neuroinflammation and ferroptosis. Eur J Pharmacol. 2023;955:175929.
Jakaria M, Belaidi AA, Bush AI, Ayton S. Ferroptosis as a mechanism of neurodegeneration in Alzheimer’s disease. J Neurochem. 2021;159:804–25.
Li Y, Pan K, Chen L, Ning J-L, Li X, Yang T, et al. Deferoxamine regulates neuroinflammation and iron homeostasis in a mouse model of postoperative cognitive dysfunction. J Neuroinflammation. 2016;13:268.
Ganz T. Systemic iron homeostasis. Physiol Rev. 2013;93:1721–41.
Jiang X, Stockwell BR, Conrad M. Ferroptosis: mechanisms, biology and role in disease. Nat Rev Mol Cell Biol. 2021;22:266–82.
Berggren KL, Chen J, Fox J, Miller J, Dodds L, Dugas B, et al. Neonatal iron supplementation potentiates oxidative stress, energetic dysfunction and neurodegeneration in the R6/2 mouse model of Huntington’s disease. Redox Biol. 2015;4:363–74.
Topiwala A, Wang C, Ebmeier KP, Burgess S, Bell S, Levey DF, et al. Associations between moderate alcohol consumption, brain iron, and cognition in UK Biobank participants: observational and Mendelian randomization analyses. PLoS Med. 2022;19:e1004039.
Yang X, Wang M, Liu W, Hou M, Zhao J, Huang X, et al. Quantitative susceptibility mapping in rats with minimal hepatic encephalopathy: does iron overload aggravate cognitive impairment by promoting neuroinflammation? NeuroImage. 2023;283:120418.
Shi Z, Li M, Wang Y, Liu J, El-Obeid T. High iron intake is associated with poor cognition among Chinese old adults and varied by weight status-a 15-y longitudinal study in 4852 adults. Am J Clin Nutr. 2019;109:109–16.
Daru J, Colman K, Stanworth SJ, De La Salle B, Wood EM, Pasricha S-R. Serum ferritin as an indicator of iron status: what do we need to know? Am J Clin Nutr. 2017;106:1634S–9S.
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370:1453–7.
Gong P, Liu Y, Gong Y, Chen G, Zhang X, Wang S, et al. The association of neutrophil to lymphocyte ratio, platelet to lymphocyte ratio, and lymphocyte to monocyte ratio with post-thrombolysis early neurological outcomes in patients with acute ischemic stroke. J Neuroinflammation. 2021;18:51.
Zhang LM, Hornor MA, Robinson T, Rosenthal RA, Ko CY, Russell MM. Evaluation of postoperative functional health status decline among older adults. JAMA Surg. 2020;155:950–8.
Kim EM, Li G, Kim M. Development of a risk score to predict postoperative delirium in patients with hip fracture. Anesthesia Analgesia. 2020;130:79–86.
Saczynski JS, Kosar CM, Xu G, Puelle MR, Schmitt E, Jones RN, et al. A tale of two methods: chart and interview methods for identifying delirium. J Am Geriatrics Soc. 2014;62:518–24.
Porcerelli JH, Cogan R, Markova T, Miller K, Mickens L. The diagnostic and statistical manual of mental disorders, fourth edition defensive functioning scale: a validity study. Compr Psychiatry. 2011;52:225–30.
Oberhaus J, Wang W, Mickle AM, Becker J, Tedeschi C, Maybrier HR, et al. Evaluation of the 3-minute diagnostic confusion assessment method for identification of postoperative delirium in older patients. JAMA Netw Open. 2021;4:e2137267.
Goudzwaard JA, de Ronde-Tillmans MJAG, de Jager TAJ, Lenzen MJ, Nuis R-J, van Mieghem NM, et al. Incidence, determinants and consequences of delirium in older patients after transcatheter aortic valve implantation. Age Ageing. 2020;49:389–94.
Song Y, Zhang D, Wang Q, Liu Y, Chen K, Sun J, et al. Prediction models for postoperative delirium in elderly patients with machine-learning algorithms and SHapley additive exPlanations. Transl Psychiatry. 2024;14:57.
Peduzzi P, Concato J, Kemper E, Holford TR, Feinstein AR. A simulation study of the number of events per variable in logistic regression analysis. J Clin Epidemiol. 1996;49:1373–9.
Yang J, Zheng Y, Li C, Gao J, Meng X, Zhang K, et al. The impact of the stress hyperglycemia ratio on short-term and long-term poor prognosis in patients with acute coronary syndrome: insight from a large cohort study in Asia. Diab Care. 2022;45:947–56.
Textor J, van der Zander B, Gilthorpe MS, Liskiewicz M, Ellison GT. Robust causal inference using directed acyclic graphs: the R package ‘dagitty’. Int J Epidemiol. 2016;45:1887–94.
Haneuse S, VanderWeele TJ, Arterburn D. Using the e-value to assess the potential effect of unmeasured confounding in observational studies. JAMA. 2019;321:602–3.
Wypijewska A, Galazka-Friedman J, Bauminger ER, Wszolek ZK, Schweitzer KJ, Dickson DW, et al. Iron and reactive oxygen species activity in parkinsonian substantia nigra. Parkinsonism Relat Disord. 2010;16:329–33.
Hernández MdCV, Allan J, Glatz A, Corley J, Kyle J, Brett CE, et al. Exploratory analysis of dietary intake and brain iron accumulation detected using magnetic resonance imaging in older individuals: the Lothian Birth Cohort 1936. J Nutr, Health Aging. 2015;19:64–9.
Hagemeier J, Tong O, Dwyer MG, Schweser F, Ramanathan M, Zivadinov R. Effects of diet on brain iron levels among healthy individuals: an MRI pilot study. Neurobiol Aging. 2015;36:1678–85.
Agrawal S, Berggren KL, Marks E, Fox JH. Impact of high iron intake on cognition and neurodegeneration in humans and in animal models: a systematic review. Nutr Rev. 2017;75:456–70.
Goozee K, Chatterjee P, James I, Shen K, Sohrabi HR, Asih PR, et al. Elevated plasma ferritin in elderly individuals with high neocortical amyloid-β load. Mol Psychiatry. 2018;23:1807–12.
Rosell-Díaz M, Santos-González E, Motger-Albertí A, Ramió-Torrentà L, Garre-Olmo J, Pérez-Brocal V, et al. Gut microbiota links to serum ferritin and cognition. Gut Microbes. 2023;15:2290318.
Palmer WC, Zaver HB, Ghoz HM. How I approach patients with elevated serum ferritin. Am J Gastroenterol. 2020;115:1353–5.
Huang C, Ma W, Luo Q, Shi L, Xia Y, Lao C, et al. Iron overload resulting from the chronic oral administration of ferric citrate induces parkinsonism phenotypes in middle-aged mice. Aging. 2019;11:9846–61.
Terekeci HM, Kucukardali Y, Onem Y, Erikci AA, Kucukardali B, Sahan B, et al. Relationship between anaemia and cognitive functions in elderly people. Eur J Intern Med. 2010;21:87–90.
Larsen B, Bourque J, Moore TM, Adebimpe A, Calkins ME, Elliott MA, et al. Longitudinal development of brain iron is linked to cognition in youth. J Neurosci Off J Soc Neurosci. 2020;40:1810–8.
Camaschella C. Iron-deficiency anemia. N. Engl J Med. 2015;372:1832–43.
Roggenbach J, Klamann M, von Haken R, Bruckner T, Karck M, Hofer S. Sleep-disordered breathing is a risk factor for delirium after cardiac surgery: a prospective cohort study. Crit Care. 2014;18:477.
Ghadery C, Pirpamer L, Hofer E, Langkammer C, Petrovic K, Loitfelder M, et al. R2* mapping for brain iron: associations with cognition in normal aging. Neurobiol Aging. 2015;36:925–32.
Zucca FA, Segura-Aguilar J, Ferrari E, Muñoz P, Paris I, Sulzer D, et al. Interactions of iron, dopamine and neuromelanin pathways in brain aging and Parkinson’s disease. Prog Neurobiol. 2017;155:96–119.
Shrout PE, Bolger N. Mediation in experimental and nonexperimental studies: new procedures and recommendations. Psychol Methods. 2002;7:422–45.
Roy CN, Snyder PJ, Stephens-Shields AJ, Artz AS, Bhasin S, Cohen HJ, et al. Association of testosterone levels with anemia in older men: a controlled clinical trial. JAMA Intern Med. 2017;177:480–90.
Qiu H, Cao S, Xu R. Cancer incidence, mortality, and burden in China: a time-trend analysis and comparison with the United States and United Kingdom based on the global epidemiological data released in 2020. Cancer Commun. 2021;41:1037–48.
la Cour KN, Andersen-Ranberg NC, Weihe S, Poulsen LM, Mortensen CB, Kjer CKW, et al. Distribution of delirium motor subtypes in the intensive care unit: a systematic scoping review. Crit Care (Lond, Engl). 2022;26:53.
Janssen TL, Steyerberg EW, Faes MC, Wijsman JH, Gobardhan PD, Ho GH, et al. Risk factors for postoperative delirium after elective major abdominal surgery in elderly patients: a cohort study. Int J Surg (Lond, Engl). 2019;71:29–35.
Acknowledgements
Thanks to Tongyan Sun and Wei Wei from Hangzhou Le9 Healthcare Technology Co., Ltd for their help in the clinical data collection of this study.
Funding
This work was funded by the National Key Research and Development Program of China (Grant No. 2018YFC2001900), the National Natural Science Foundation of China (Nos. 81901097, 82171180), and the Military Medical Technology Incubation Project for Youth (20QNPY094).
Author information
Authors and Affiliations
Contributions
Conceptualization, Project administration, Supervision: X-YZ, W-DM, and Y-LM. Funding acquisition: X-YZ, and W-DM. Data collection: X-HR, YL, and M-YY. Methodology, Investigation: X-HR, YL, M-YY, HL, and J-SL. Data verification: Y-HL, J-BC, and Y-LM. Writing original draft: X-HR, and YL. Writing review & editing: X-YZ, W-DM, Y-LM, X-HR, YL, and M-YY. All authors approved the final version of the manuscript for submission.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Ruan, X., Li, Y., Yuan, M. et al. Preoperative serum ferritin as a biomarker for predicting delirium among elderly patients receiving non-cardiac surgery: a retrospective cohort study. Transl Psychiatry 14, 377 (2024). https://doi.org/10.1038/s41398-024-03090-9
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41398-024-03090-9