Abstract
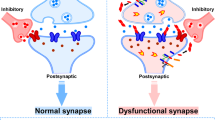
Alzheimer’s disease (AD) is characterized by synaptic dysfunction and proteostatic imbalance, partly driven by amyloid-beta oligomers (Aβo). This study focuses on the effects of low-concentration Aβo exposure on synaptic architecture and de novo protein synthesis in primary cortical neurons, and assesses the neuroprotective potential of the MAP kinase interacting kinase (MNK) inhibitor, eFT508. Using expansion microscopy, we observed that 5-day exposure of low concentrations of Aβo significantly increased synapse density, particularly single synaptic boutons (SSBs) and multi-innervated spines (MIS). This finding indicates that we modelled increases in synapses characteristic of mild cognitive impairment (MCI), a transition to AD. The clinically approved MNK inhibitor eFT508 partially suppressed these synaptic alterations, restoring synapse density to control levels. While total de novo protein synthesis remained unchanged under Aβo exposure using bioorthogonal non-canonical amino acid tagging (BONCAT), subsequent proteomic profiling identified selective changes in de novo protein synthesis that are involved in synaptic function, cytoskeletal regulation, mitochondrial activity, autophagy, and the ubiquitin-proteasome system, and part of these dysregulations could be inhibited by eFT508. These findings indicate that Aβo exposure in an in vitro model of AD leads to synaptogenesis and dysregulation in de novo protein synthesis and they identify eFT508 as a compound that can counteract some of these Aβo-induced dysfunctions.
Similar content being viewed by others
Introduction
Alzheimer’s disease (AD) is the most prevalent form of dementia. The two major histological hallmarks of AD are extracellular accumulation of amyloid-β (Aβ) peptides, as oligomers and plaques, and intracellular aggregation of hyper-phosphorylated tau proteins forming neurofibrillary tangles [1]. Among the earliest and most critical symptoms of AD is memory loss, which correlates with synapse loss [2, 3]. However, mild cognitive impairment (MCI), a transitional state to AD, is associated with an increase in synapses [4, 5]. Interestingly, in Aβ-generating transgenic mouse models of AD, presynaptic terminals undergo dynamic changes throughout the pathological progression: boutons associated with cholinergic, glutamatergic, and GABAergic synapses initially exhibit an increase but progressively decline as the phenotype advances [6]. It is unclear whether the increase in synapses in MCI is a compensatory mechanism for cognition, or whether it is detrimental due to excitotoxicity or due to abnormal multi-synapse formation preventing memory retrieval [2].
Early synaptic change in AD is thought to result from the effects of Aβ oligomers (Aβo), which are produced due to abnormal processing of amyloid precursor protein (APP) at synapses [3, 7, 8]. Furthermore, the translation of APP mRNA has been shown to increase in primary neurons when exposed to Aβo [9]. This has led to the hypothesis that Aβ induces a cascade of amyloid production by increasing the local synthesis of APP protein and other fragile X mental retardation protein (FMRP)-regulated proteins at amyloid-exposed synapses [10].
Emerging evidence suggests that deregulated protein synthesis is one of the early events driving synaptic dysfunction in AD [11]. In models of the early stages of AD, an up-regulation of de novo protein synthesis has been observed, whilst models of later AD stages appear to be associated with a down-regulation of de novo protein synthesis [12,13,14,15,16,17,18,19]. Additionally, recent evidence indicates that Aβo increases protein synthesis via MAP kinase interacting kinase (MNK), which phosphorylates the eukaryotic translation initiation factor 4E (eIF4E), a key regulator of protein synthesis [16]. Additionally, MNK activates mechanistic target of rapamycin(mTOR) signalling, another key signalling regulator of protein synthesis [20, 21]. Notably, eFT508 is a very potent and selective inhibitor of MNK, which has been used in clinical trials to treat cancer patients [22, 23].
The synaptic alterations that underlie cognitive decline during MCI remain poorly understood. Elucidating these early synaptic changes is crucial for identifying therapeutic targets and developing interventions to slow or prevent disease progression. Therefore, we investigated how low concentration Aβo exposure affects synapse density and structure. We also studied the de novo proteome in primary cortical neurons and assessed whether eFT508 co-treatment could mitigate these effects. We employed expansion microscopy, a novel approach that significantly enhances spatial resolution and allows for detailed visualization of synaptic subtypes [24] and bioorthogonal non-canonical amino acid tagging (BONCAT) to detect changes in newly synthesized proteins [25]. By integrating immunofluorescence imaging, proteomic analyses, and functional pathway assessments, this work uncovered molecular mechanisms underlying Aβo-induced synaptic changes, offering new insights into very early AD pathogenesis and potential therapeutic interventions.
Materials and methods
Preparation of synthetic Aβ oligomers
Rat amyloid-β oligomers were prepared as described [16]. Briefly, a stock solution of Aβ1-42 (Sigma-Aldrich) was prepared at a concentration of 100 μM in 200 mM HEPES buffer (pH 8.5). The solution was gently agitated at room temperature for 30 min, aliquoted, and stored at −80 °C. Aliquots were thawed once for experimental treatments and were not subjected to repeated freeze-thaw cycles to maintain their oligomeric form.
To confirm the composition of the prepared Aβ1-42, the NativePAGE™ system was employed. The presence of oligomers was validated by treating Aβ1-42 peptides with 5 M guanidine hydrochloride (1:1 ratio), which disrupts oligomeric structures. Detection of oligomers was performed using clone 4G8 (Biolegend, diluted 1:1000).
Primary neuronal culture
Primary cortical neuronal cultures were established using embryonic day 18 (E18) Sprague-Dawley rat embryos. Neurons were seeded into culture plates pre-coated with poly-D-lysine. The cells were maintained in neurobasal medium supplemented with 2% B27, 0.5 mM L-glutamine, and 1% penicillin/streptomycin. To support long-term culture and mitigate excitotoxicity-induced cell death, 200 μM D,L-amino-phosphonovalerate (D,L-APV, Abcam), an N-methyl-D-aspartate (NMDA) receptor antagonist, was added to the media at four days in vitro (DIV). Thereafter, 50% of the culture medium was replaced weekly to sustain cell viability and functionality. Neuronal cultures were maintained until they reached maturity, typically after DIV 21. These cells were daily treated with Aβo at a low concentration of 100 nM for 5 days. For experiments involving eFT508 (provided by eFFECTOR Therapeutics, USA), the compound was added to the culture medium at a final concentration of 2 nM, 30 min prior to Aβo exposure. The selected eFT508 concentration was determined based on its well-documented potency [26, 27] and on our finding that 2 nM eFT508 reversed Aβo-induced increase in BONCAT-measured de novo protein synthesis after 1-day exposure (S. Lee and K.P. Giese, unpublished data). Cells were used either for expansion microscopy or de novo protein expression analysis.
Expansion microscopy
Cell fixation and anchoring
We used a total of eighteen samples: 6 controls, 6Aβo-treated, and 6 Aβo + eFT508-treated samples. Cells (treated or untreated) were rinsed with ice-cold phosphate-buffered saline (PBS) and fixed at room temperature (RT) for 10 min, using 4% paraformaldehyde (PFA) in PBS. Following fixation, cells were washed twice with PBS for 5 min each. Subsequently, cells were incubated in an anchoring solution (dissolving 0.2% methacrylic acid N-hydroxy succinimide ester in dimethyl sulfoxide and diluting the stock solution 1:100 in 1xPBS) for 2–3 h at RT. After incubation, cells were washed twice with PBS for 15 min per wash.
Preparation of gelation chambers and gelation of cells
During the anchoring step, gelation chambers were prepared, using gelation solution (15% 2-acrylamido-2-methyl-1-propanesulfonic (AMPS) acid sodium, 10% acrylamide, 0.1% N,N’-methylene-bis-acrylamide, 0.1% ammonium persulfate, and 0.05% N,N,N´,N´-tetra-methyl-ethylene-diamine). Cells were incubated on ice for 5 min in the gelation solution. Coverslips containing cells were placed upside down on a microscope slide, and the gap between the slide and coverslip was filled with additional gelation solution to press the coverslip to eliminate air bubbles gently. Samples were then incubated at 37 °C for 1 h to allow gelation.
Denaturation
After gelation, coverslips were carefully removed from the microscope slide and discarded, and the edges of the gel were trimmed. Samples were then incubated in a denaturation solution (0.6% Tris base, 1.2% sodium chloride, and 5.8% sodium dodecyl sulphate) at 60 °C for 1 h, then allowed to cool to RT, and subsequently washed twice with PBS for 15 mins each.
Blocking and antibody staining
Prior to staining, samples were blocked in 5% normal goat serum (NGS, Sigma Aldrich) with 1% Triton X-100 in PBS at RT for 1 h. Primary antibodies (MAP2, Antibodies, 1:500; PSD95, synapsin1, Abcam 1:100), diluted in blocking solution, were applied, and samples were incubated with gentle shaking overnight at 4 °C. The following day, primary antibodies were removed, and samples were washed four times for 5 min each with PBS containing 0.1% Triton X-100. Secondary antibodies (Alexa Fluor 488, Alexa Fluor 568, Alexa Fluor 647, Thermo Fisher Scientific, 1:200) were added, and samples were incubated at RT for 4 h under light-blocking conditions. After secondary antibody incubation, samples were washed four times with 0.1% Triton X-100 in PBS for 5 min each. Samples were stored in fresh PBS at 4 °C until imaging.
Sample mounting and imaging
Before imaging, samples were incubated in Milli-Q water while 2% low melting point agarose was prepared at 70 °C. Samples were mounted on coverslips, and Milli-Q water was added to the gel to prevent drying. Approximately 200 µl of 2% low melting point agarose gel solution. Samples were then covered with a coverslip and placed on ice for 10 mins for gel solidification. Once solidified, samples were ready for imaging by confocal high-resolution microscopy. 3D reconstruction, and analysis of whole neurons was performed with Imaris software (version 10.0.2, Oxford, UK). We evaluated Aβ-induced synaptic pathology across dendritic compartments, with primary dendrites representing initial synaptic inputs and secondary dendrites reflecting downstream effects, thus thoroughly assessing cellular responses. So, both primary and secondary dendrites were analyzed, as indicated in the figure legends (e.g., Fig. 1d and Fig. 2 for primary dendrites, and Fig. S1 for secondary dendrites). For each biological group, we selected two neurons and analysed at least 200 synapses per image. We measured the total dendritic length and manually categorized the synaptic types.
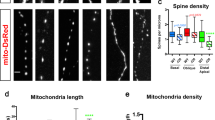
(a) The strategy for revealing synaptic changes with expansion microscopy between the three experimental groups. At DIV 21, primary cortical neurons were daily treated for five days with Aβo (100 nM), or Aβo with eFT508 (2 nM); control cells were not treated. At DIV 26, the neurons were fixed and anchored, followed by embedding in a hydrogel matrix. The embedded cells were denatured at 60 °C, blocked, and labelled with specific antibodies for immunostaining. Confocal microscopy was used to image the expanded cells, and image analysis was performed. This figure panel was created using BioRender. (b) Representative images of control (Ctrl) neurons, and neurons treated with Aβo with or without eFT508. For immunostaining synapsin1 (Syn1, green) served as pre-synaptic marker, PSD95 (white) as post-synaptic marker, MAP2 (magenta) as marker of the neuronal structure. Scale bar: 70 µm. (c) Representative comparison of primary cortical neurons visualized before expansion (left), after expansion (middle), and in the 3D analysis model (right). For a chosen dendritic region single synapse bouton (SSBs), multi-innervated spines (MIS), multi-spine boutons (MSBs) including complex MSBs (cMSBs) containing more than 2 spines are indicated. Red arrow (upper left): SSB; yellow arrow (bottom left): MSB; green arrow (upper right): complex MSB; blue arrow (bottom right): MIS. Scale bar: 70 µm. (d) Aβo significantly increased synapse density compared to the control group and eFT508 suppressed this effect (F2, 33 = 7.513, p = 0.002; Ctrl vs. Aβo: q = 5.482, p = 0.0014). Data represent mean ± SEM, n = 6 biological replicates and analysis of 2 dendritic segments per biological replicate. **p < 0.01, ns = not significant.
Quantification of synapse types obtained from the experiments described in Fig. 1. (a) Aβo significantly increased SSB density and eFT508 suppressed this effect (F2, 33 = 10.23, p < 0.0001, Ctrl vs. Aβo: q = 6.076, p < 0.001; Aβo vs. Aβo + eFT508: q = 4.772, p < 0.01). No significant differences were observed in the ratios of SSBs to total synaptic boutons across the experimental groups. (b) Aβo results in an increased on the MIS density (F2, 33 = 3.464, p < 0.05, Ctrl vs. Aβo: q = 3.677, p < 0.05) and did not alter the ratio of MIS to total spines across the experimental groups. (c) No significant differences were observed in MSB density and ratios of MSBs to total synaptic boutons and in the density of cMSBs across the experimental groups. Data represent mean ± SEM, n = 6 biological replicates and analysis of 2 dendritic segments per biological replicate. *p < 0.05, **p < 0.01,***p < 0.001, ns = not significant.
BONCAT
Non-canonical amino acid treatment
Twenty hours after the last Aβo or control treatment, neurons were subjected to non-canonical amino acid labelling with 1 mM azidohomoalanine (AHA) dissolved in Dulbecco’s modified Eagle’s medium (DMEM) for 4 h. Then cells were lysed in lysis buffer (20 mM Tris pH 7.4, 150 mM NaCl, 1% Triton X-100, 5 mM EDTA pH 8) supplemented with protease and phosphatase inhibitor cocktails (Sigma). Protein concentrations in the lysates were determined using the bicinchoninic acid assay (Thermo Fisher Scientific).
Purification and analysis
To quantify de novo protein synthesis, 10 µg of each sample was labelled using the Click-iT™ Protein Reaction Buffer Kit (Thermo Fisher Scientific) with biotin-alkyne (Lumiprobe) according to the manufacturer’s instructions. Equal volumes of the labelled proteins were boiled at 95 °C for 5 min, separated on 4–12% Criterion™ TGX™ precast gels, and subsequently transferred onto methanol-activated 0.2 µm polyvinylidene fluoride membranes. After transfer, the membranes were air-dried, rehydrated with ultrapure water, and stained with Revert 700 Total Protein Stain (LI-COR) for 5 min. Excess stain was removed using Revert 700 Wash Solution (LI-COR), followed by rinsing with ultrapure water. The stained membranes were imaged using an Odyssey Imaging System in the 700 nm channel. Following imaging, the membranes were blocked with blocking buffer (5%BSA in TBST), incubated with streptavidin in blocking buffer (Abcam, 1:10,000) overnight, and protein detection was performed using a Chemidoc Imaging System. The results were normalized to the total protein level of each sample accordingly.
For BONCAT- mass spectrometry (MS) analysis, 100 µg of each sample was labelled as described above. Samples were incubated with 100 µM DIBO-biotin (Lumiprobe) at RT for 30 min. Biotinylated proteins were purified using 40 µg of streptavidin coated Dynabeads (Thermo Fisher Scientific). The beads were washed multiple times with wash buffer (0.1% BSA in PBS), and bound proteins were eluted by adding 0.1 mL of a solution containing 0.2% trifluoroacetic acid (TFA), 0.1% formic acid, and 80% acetonitrile in water [28]. Beads were centrifuged at 1000 x g, and the first elution of biotinylated peptides was collected. To ensure maximum elution release, a second elution was performed by boiling the beads in the same solution for 5 min.
Liquid chromatography-tandem mass spectrometry (LC-MS/MS) analysis
Mass spectrometry was performed to measure the differential amounts of de novo proteins from primary cortical neurons with different treatments. Seventeen samples (6 controls, 5 Aβo-treated neurons, and 6 Aβo + eFT508-treated neurons; numbers refer to biological replicates) were biotinylated and immunoprecipitated to isolate de novo synthesized proteins. Proteins (20 μg/sample) were reduced with 50 mM tris (2-carboxyethyl) phosphine hydrochloride, (TCEP) in 0.2 M EPPS (pH 8.5) and incubated at RT for 30 min. They were alkylated with 20 mM iodoacetamide (IAM) in a 4:1 ratio to TCEP for 30 min in the dark, followed by quenching with 10 μl of 50 mM DTT. Proteins were precipitated using ice-cold acetone at -20 °C overnight, centrifuged, dried, and resuspended in 0.2 M EPPS. Enzymatic digestion was performed using a trypsin/LysC mix at a 1:100 enzyme-to-substrate ratio and incubated at 37 °C overnight. Peptides were labeled using TMTpro reagents. The pH of samples was adjusted to 8.5, and 6 μl of TMT reagent was added per sample. After 1-hour incubation at RT, samples were pooled and analyzed by LC-MS/MS for label efficiency. The remaining samples were stored at -80 °C.
TMT-labeled peptides were fractionated using high-pH reversed-phase chromatography using high capacity C18 desalting spin columns (Thermo Fisher Scientific) and eluted into nine fractions. Labeled peptides were separated using a U3000 UHPLC NanoLC system (Thermo Fisher Scientific). Peptides were resolved by reversed-phase chromatography on a 75 μm C18 Pepmap column (50 cm length, ES903; Thermo Fisher Scientific) using a linear gradient of 80% acetonitrile in 0.1% formic acid at a flow rate of 250 nl/min over 120 min and ionized by electrospray ionization using an Orbitrap Fusion Lumos (Thermo Fisher Scientific) operating under Xcalibur v4.4.16. Peptides were detected using a Synchronous Precursor Selection (SPS) MS3 HCD fragmentation method with Real-Time Search (RTS) set to 120k Orbitrap resolution with scan range m/z 350-1500 and AGC 100% (MS1), quadrupole isolation with ion trap CID fragmentation (35% normalized collision energy) set to rapid (MS2) and top 10 precursors ions selected for Orbitrap HCD fragmentation at 60k resolution, 200% AGC with scan range m/z 100-500 (MS3). Raw data were processed in Proteome Discoverer v2.5, with protein identifications performed at a 1% false discovery rate (FDR) against the rat taxonomy database downloaded from UniProt (10,232 entries; March 2024). Consensus data was exported and uploaded into Perseus software (v2.0.1) [29] for statistical protein quantification analysis. In order to depict the function clustering of the differentially expressed proteins described, the STRING database was used. This online resource contains both known and predicted protein-protein interactions. STRING enrichment was conducted against the rat genome.
Statistical analysis
Statistical analyses for expansion microscopy and BONCAT experiments were conducted using GraphPad Prism 10.0 software. Data were tested for normality with a Shapiro–Wilk test. One-way analysis of variance (ANOVA) with Tukey’s multiple comparison test was applied for data analysis. Results are expressed as mean ± standard error of the mean (SEM). Statistical significance thresholds were defined as follows: *P < 0.05, **P < 0.01, ***P < 0.001, and ****P < 0.0001.
Results
Low concentrations of Aβo increase synapse density in primary cortical neurons and the changes are reversed by the MNK inhibitor eFT508
In order to model a very early stage of AD, we exposed mature (DIV 21), primary cortical neurons from rat with low concentrations of Aβo (100 nM) over 5 days. In this study, rat Aβo was used to model physiological processes in the rodent neurons. Further, we used cortical neurons as amyloid pathology in AD commences in cortex [30]. One experimental group was treated with Aβo and eFT508, a specific MNK inhibitor, as our earlier work indicated that MNK inhibition could mitigate some Aβo-induced changes in de novo protein synthesis [16]. To study the impact on synaptic changes, we utilized expansion microscopy, a novel technique that allows high-magnification immunofluorescent staining of synapses, using confocal microscopy [31] (Fig. 1a). Following treatment, the cells were stained with antibodies against Syn1, PSD95, and MAP2 to assess pre-, post-synaptic and neuronal structure in detail (Fig. 1b). Expansion microscopy magnified the samples by 5–6 times. The combination with 3D structural analysis allowed for the detections of specific synaptic types, such as single synaptic boutons (SSBs), multi-innervated spines (MIS), multi-spine boutons (MSBs), and complex MSBs (cMSBs) having more than two dendritic spines (Fig. 1c). We found that Aβo exposure resulted in a significant increase in overall synapse density and eFT508 treatment prevented this increase, as there were no significant changes in the synapse density in primary and secondary dendrites between the Aβo and eFT508 group compared to control (Fig. 1d, Fig. S1a). Further, we conducted a detailed analysis of synapse types to obtain insights into how Aβo alters distinct synaptic populations and how eFT508 modulates these changes. Aβo exposure resulted in a significant increase in SSB density. Treatment with eFT508 effectively suppressed this increase (Fig. 2a, Fig. S1b), indicating a potential role of eFT508 in preventing SSB increases. We also found that the Aβo-induced increases in SSB density did not affect the observed ratio of SSBs to total synaptic boutons, indicating that SSB increases were not at the expense of MSB decreases. Further, MIS was a minor synaptic subtype, comprising only 1–2% of total synapses, and Aβo exposure led to an increase in MIS density in secondary (Fig. 2b), but not in primary dendrites (Fig. S1c). The increase in MIS density in secondary dendrites was not at the expense of spine loss as the ratio of MIS to total spines was not altered (Fig. 2b). Furthermore, MSB density in the secondary dendrites of the Aβo group and Aβo with eFT508 group did not significantly differ from control levels (Fig. 2c), while the MSB density in primary dendrites was significantly increased by Aβo treatment and suppressed by eFT508 (Fig. S1d). Ratios of MSBs to total synaptic boutons and cMSBs showed no significant changes across the experimental groups. Furthermore, no significant changes were observed in the ratio of MSBs to total synaptic boutons or in the density of cMSBs across the experimental groups (Fig. 2c, Fig. S1d). Taken together, our findings reveal that Aβo induces distinct synaptic alterations, characterized by a consistent increase in SSB density, while MIS and MSB densities exhibit variability depending on dendritic order. Notably, eFT508 shows considerable potential to counteract these effects.
Low concentrations of Aβo do not alter total de novo protein synthesis in primary neurons
Previous research [16] and unpublished data conducted in our laboratory have demonstrated that a 24-h Aβo exposure upregulates de novo protein synthesis in primary cortical neurons. Here, we investigated the effects of 5-day low concentration Aβo exposure on de novo protein synthesis and the impact of the MNK inhibitor, eFT508. We substituted methionine in culture medium with AHA, a non-canonical methionine analogue, which is incorporated into newly synthesized proteins during a four-hour window (Fig. 3a). Proteins were labelled, using click chemistry, and analysed via western blot and LC-MS/MS for quantification and identification of newly synthesized proteins (Fig. 3b). Quantitative analysis of total de novo protein synthesis indicated no statistically significant differences between the control, Aβo-treated, and Aβo + eFT508-treated groups after normalization to protein levels (Fig. 3c). Even though 5-day Aβo exposure did not alter total de novo protein synthesis, the nature of the de novo protein synthesis could have been changed by Aβo and eFT508 treatment. To address this, de novo proteomics was performed.
(a). The strategy for revealing changes in de novo protein synthesis, using the BONCAT method. At DIV 21, primary cortical neurons were daily treated for five days with Aβo (100 nM), or Aβo with eFT508 (2 nM); control cells were not treated. Newly synthesized proteins were labelled by incubation in a methionine-depleted medium containing 1 mM AHA for 4 h prior to harvest. Azide-bearing proteins were subsequently labelled using click chemistry with biotin-alkyne, followed by western blots or proteomic analysis after purification. This figure panel was created using BioRender. (b). Representative BONCAT-Western Blot image showing AHA-labelled newly synthesized proteins across the experimental groups and corresponding total protein levels as revealed by Revert labelling. (c). Quantitative analysis of the results, normalized to total protein levels and presented as bar graphs, indicates no significant changes in the total amount of de novo protein synthesis across the experimental groups. Data represent mean ± SEM, n = 5 or 6 biological replicates. ns = not significant.
De novo proteomic dysregulation in the primary cortical neurons after low concentrations of Aβo and impact of eFT508 treatment
To assess the impact of low-concentration Aβo exposure on the de novo proteome, LC-MS analyses were performed to identify and quantify newly synthesized proteins. Across all experimental conditions, a total of 1067 de novo synthesized proteins were identified in primary cortical neurons. Among these, 49 proteins displayed significant differential expression in Aβo-treated neurons relative to control, 95 proteins were differentially expressed in Aβo + eFT508-treated neurons compared to control, and 29 proteins showed significant differences between Aβo-treated and Aβo + eFT508-treated groups (Table S1, Fig. 4). Most dysregulated proteins in both Aβo (76%) and Aβo + eFT508 (71%) groups were downregulated (Fig. 5a, c). An overlap analysis of dysregulated proteins identified one commonly affected protein across all groups, with 15 shared between Aβo vs. Ctrl and Aβo + eFT508 vs. Ctrl, 27 unique to the Aβo-treated group, and 74 unique to the Aβo + eFT508-treated group (Fig. 5b). The heatmap displays all 145 significantly altered proteins among three different comparisons (Fig. 5b), offering clear insights into the effects of Aβ treatment and eFT508 intervention in our cellular model (Fig. 4, asterisks indicating proteins with statistically significant changes). To gain mechanistic insights, STRING network analysis reviewed functional interactions among dysregulated proteins. As shown in Fig. 6, Aβo treatment prominently affected proteins involved in post- and pre-synaptic processes and translation. Co-treatment with eFT508 appeared to engage in different pathways, including an effect on ribosomes, as indicated by the STRING analysis in Fig. S2a. The 33 proteins shown in Fig. 7 represent a significant subset of the 145 differentially expressed proteins identified in our proteomics analysis, selected for their strong association with the highlighted pathways and their response to Aβo treatment and eFT508 intervention. Pathway-specific analysis of dysregulated de novo proteins indicated that Aβo exposure primarily disrupted processes associated with synaptic function, cytoskeletal organization, mitochondrial activity, autophagy, and the ubiquitin-proteasome system (UPS). These pathways were not the only ones dysregulated but were chosen as they represent the most significantly altered processes. Among the 33 proteins analyzed, all exhibit significant alterations in expression due to Aβo exposure. Notably, 24 of these proteins (representing over 70%) are normalized following eFT508 treatment, where such a substantial degree of normalization indicates the promising therapeutic potential of eFT508. For instance, synapse-associated proteins, such as APP, bassoon (Bsn), and synapsin 2 (Syn2) were significantly upregulated in Aβo-treated neurons but remained unaltered in Aβo + eFT508-treated neurons relative to controls. Interestingly, downregulation of some synaptic signaling proteins, such as secreted frizzled-related protein 1 (Sfrp1) and neuronal calcium sensor 1 (Ncs1) in Aβo-treated neurons also remained unaltered in Aβo + eFT508-treated neurons relative to controls. The attenuation of significant changes in these proteins upon eFT508 treatment suggests its potential protective effects, as it may partially restore protein expression to baseline levels. These data suggest that low concentrations of Aβo disrupts key neuronal processes, while eFT508 co-treatment mitigates these effects by restoring protein expression and preserving cellular function, highlighting its neuroprotective potential.
The heatmap shows differentially expressed proteins in the de novo proteome among different groups (asterisks indicating proteins with statistically significant changes). A-C: Aβo vs. Ctrl, E-C: Aβo + eFT508 vs.Ctrl E-A: Aβo + eFT508 vs. Aβo.
(a) Volcano plot of all the proteins in the de novo proteome. The abscissas represent the fold change in log2, and the ordinates are p-values of t-tests between two groups in −log10 Red dots represent upregulated proteins, blue dots are downregulated proteins, and black dots illustrate unchanged proteins. Dot sizes are related to the fold change of each protein. (b) Venn diagram illustrating the total number of significantly altered de novo proteins under different treatment groups, highlighting both shared and unique changes.
The interaction network shows the functional enrichment of differences in de novo proteins after low concentrations of Aβo exposure (only interactions with p < 0.05 are shown). Node colours are linearly related to biological processes or pathways.
Aβo induced primarily changes in de novo protein synthesis regarding the synapse, cytoskeleton, mitochondria, autophagy, and UPS. Many of these changes were prevented or reduced by eFT508 treatment, as indicated by the loss of significance when comparing control vs Aβo + eFT508. For simplicity the error bars are not indicated. n = 5-6 per group, * = significantly different in a t-test comparison, ns = not significant.
We found that Aβo treatment prominently affected de novo synthesis of proteins involved in pre-and post-synaptic processes and translation (Fig. 6). While eFT508 treatment attenuated more than 70% of the Aβo-induced changes in de novo protein synthesis (Fig. 7), eFT508 also engaged in other pathways, most notably in ribosomal protein functionality (Fig. 6 and Fig. S2). This suggests that eFT508 operates through a compensatory mechanism, likely enhancing translational efficiency or protein homeostasis, rather than directly reversing the same protein interactions disrupted by Aβo. The correction of over 70% of Aβo-dysregulated proteins by eFT508 indicates that, despite targeting different initial networks, eFT508’s downstream effects converge on the same proteins affected by Aβo. For instance, regulated ribosomal functionality could stabilize protein synthesis or turnover, indirectly restoring the levels of Aβo-dysregulated proteins. This convergence highlights a therapeutic effect where eFT508 mitigates the functional consequences of Aβo-induced dysregulation through an alternative pathway, rather than directly overlapping with Aβo’s interaction network.
The de novo proteomic analysis revealed important alterations in the expression of specific proteins across the experimental conditions. These findings suggest that while total de novo protein synthesis remains unchanged, low concentrations of Aβo may lead to selective changes in the synthesis of individual proteins, which could have implications for neuronal function and synaptic regulation. Many significantly changed protein expressions in Aβo-treated samples are consistent with findings from AD pathology (Table S2). Several proteins associated with various biological pathways exhibited altered expression levels, with eFT508 effectively reversing some of these changes. Notably, gamma-enolase (Eno2/NSE) and bassoon (Bsn), which have been previously implicated in AD pathology, showed dysregulation that was successfully mitigated by eFT508 treatment. Also, proteomic analysis revealed a significant downregulation of visinin-like protein 1 (Vsnl1/ Vilip-1) and neurofilament light polypeptide (Nefl/Nfl) following Aβo treatment.
Discussion
Synapse loss is thought to be the best correlate of cognitive impairment in AD [2, 3]. However, in some brain regions, synapse loss does not seem to precede neuronal loss in AD [2], and MCI, the transition to AD, is associated with an increase in synapse density [4,5,6]. Here, we show that low concentrations of Aβo increase synapse density in primary cortical neurons and thereby effectively mimic synapse increases occurring in MCI. Our findings indicate that Aβo increases distinct synaptic subtypes, such as SSBs and MIS in secondary dendrites. We also show that eFT508, a specific MNK inhibitor, mitigates Aβo-induced increases in synapse density, suggesting that this clinically accepted compound could be useful for preventing cognitive impairment associated with MCI and progression into AD. Further, proteomic analyses revealed that Aβo-induced dysregulation of pathways that are associated with synaptic vesicle dynamics, cytoskeletal organization, mitochondrial function, autophagy, and the ubiquitin-proteasome system (UPS), mechanisms previously implicated in early AD pathogenesis.
We treated rat primary cortical neurons with rat Aβo to model the early cortical stages of AD. Although rodent Aβ₁₋₄₂ can undergo aggregation, it does so less efficiently than the human peptide due to three amino acid substitutions within its sequence [32]. Our results show that low concentrations of rat Aβo increase synapse numbers, particularly elevating the density of SSBs and MIS (Fig. 2, Fig. S1). Using a higher concentration of rat Aβo (500 nM) decreased PSD-95 levels already at an earlier time point, indicating synaptotoxicity (Fig. S3). Consistently, when primary neurons with mature synapses are treated with 500 nM human Aβo for 24 h the synapse number decreases to 59% of control levels [33]. In contrast, low concentrations of human Aβ correlate with synaptogenesis in human iPS cell-derived neurons with APP knock-in mutations [34]. Moreover, in young human Aβo-producing transgenic mice presynaptic bouton density increases before synapse loss occurs at an older age [6]. Thus, taken together, at low concentrations Aβo promote synaptogenesis, whereas high concentrations of Aβo are synaptotoxic. As an increase in glutamatergic bouton density in MCI has been observed [4, 5], we suggest that in the early and prodromal stages of AD, Aβo is synaptogenic and in the later stages of AD, Aβo is synaptotoxic.
It has been debated whether the increased synapse density in MCI is compensation for other neurodegenerative processes or whether it is part of the disease contributing to the cognitive impairment [4, 6, 8]. Since we have observed an Aβo-induced increase in synapse density, and the environment in cultured neurons lacks complex regulatory mechanisms of the brain [35], we suggest that the increased synapse number in MCI is a pathological response rather than a compensation. The increased synapse number could reflect a maladaptive response to early neurodegenerative processes, such as the accumulation of Aβo, which disrupts synaptic homeostasis. This disruption may trigger an aberrant overproduction of synapses as an attempt to maintain connectivity, rather than a beneficial compensatory adaptation. As it has been shown in Aβ-generating transgenic mouse models of AD, presynaptic terminals undergo dynamic changes throughout the pathological progression: boutons associated with cholinergic, glutamatergic, and GABAergic synapses initially exhibit an increase but progressively decline as the phenotype advances [6]. An additional mechanism that may contribute to the observed effects is the synaptic model proposed by Westmark [9]. In this model, Aβo binds to metabotropic glutamate receptors (mGluRs), triggering local protein synthesis at synapses. One of the proteins locally synthesized is APP. This process establishes a feedforward loop wherein Aβo binding enhances APP production, leading to increased generation of abnormally cleaved Aβ peptides. This self-amplifying cycle may exacerbate Aβo-mediated toxicity, contributing to synaptic dysfunction and disease progression. The increased synapse density is likely detrimental as dysregulated synaptic remodelling disrupts normal network activity, impairing synaptic plasticity and neuronal communication, key processes required for cognition and memory [36]. Moreover, an increase in synapse density may result in excitotoxicity [5]. Finally, our analysis suggests that not only SSB density is increased, but that also multi-synapses, such as MIS, are elevated. MIS generation has been suggested to underlie memory in old age [37], and therefore abnormal MIS generation may impair memory. Follow-up studies are needed to assess multi-synapses in MCI brain, using either 3D electron microscopy or expansion microscopy.
Therapeutically, eFT508 is a highly specific MNK inhibitor, which has been used in clinical trials with cancer patients [22, 23]. We found that eFT508 mitigates Aβo-induced increases in synapse density. Considering the similarity with increased synapse density in MCI, we suggest that inhibiting MNK signalling may be suitable to treat synapse density and cognitive dysfunction in MCI. Follow-up studies will need to address whether the MNK inhibition is effective via preventing phosphorylation of eIF4E at serine 209 [16, 38], or via blocking mTOR signalling [20, 21], as both signalling routes impact on de novo protein synthesis.
The observed synaptic changes prompted further exploration to better understand the underlying functions and pathways involved. Our findings indicate that 5-day exposure of low concentrations of Aβo to primary cortical neurons does not result in significant changes in total de novo protein synthesis (Fig. 3). However, data from our lab demonstrate that 1-day exposure to low concentration of Aβo induces upregulation of de novo protein synthesis [16]. These observations suggest that Aβo may dynamically regulate protein synthesis in the primary neuron model, with an initial increase in total de novo protein synthesis potentially followed by a subsequent decrease. This biphasic dynamic pattern may explain the lack of significant changes observed during prolonged exposure. Such fluctuations in protein synthesis may reflect an early adaptive response that transitions into dysregulation over time.
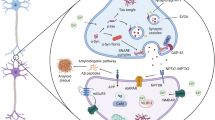
Although total de novo protein synthesis did not markedly differ across the experimental conditions, our proteomic data highlight selective dysregulation of proteins critical for synapse, cytoskeletal organization, autophagy, and UPS - processes also implicated in AD and other neurodegenerative disorders [39,40,41,42]. The proteomic findings provide some insights into the molecular underpinnings of the Aβo-induced increase in synapse density. We found that de novo synthesis of APP is elevated with Aβo exposure. This is consistent with the earlier observation that in primary neurons translation of APP mRNA increases after exposure to Aβo [9]. Accordingly, we have found that eFT508 treatment significantly attenuates the Aβo-induced increase in APP synthesis, reducing the fold change from 1.86 to 1.54. But note that the 1.54-fold increase by Aβo + eFT508 was not significantly different from control (Table S1). APP is known to promote synaptogenesis [43]. And the APP-Swedish mutation in human neurons leads to increased synapse numbers and synaptic transmission. Interestingly, the deletion of the APP gene results in fewer synapses and reduced synaptic transmission [34]. Therefore, we suggest that Aβo increases synapses density via promoting the synthesis of APP. Thus, our findings may link to the previously described feedback loop at Aβo-exposed synapses, suggesting that Aβo activates mGluR5 signalling, leading to MNK signalling increasing translation of APP mRNA through FMRP [44, 45], thereby providing additional substrates for β- and γ-secretase cleavage, which in turn producing more Aβo [10].
Synaptic structure is closely associated with changes in synaptic strength, with atypical synapses often exhibiting multiple inputs or outputs. Among these, MSBs feature one input and multiple outputs, connecting a presynaptic terminal to several dendritic spines, while MIS has multiple inputs but only one output. Changes in the number and complexity of MSBs and MIS are believed to influence brain connectivity and play a crucial role in memory processes [46]. We observed an increase in MIS density within secondary dendrites and a significant increase in MSB density in primary dendrites. However, the underlying mechanisms for these variations in distribution remain unclear. MIS generation occurs by the addition of a novel presynaptic input onto an existing 1:1 synapse, and it was shown to be a memory mechanism in old mice when LTP is impaired [37]. It is conceivable that the Aβo-induced APP de novo synthesis causes MIS generation. Additionally, our de novo proteomics detected the downregulation of Sfrp1, an inhibitor of Wnt signalling, that may also impact this process, as Wnt signalling promotes nitric oxide synthesis which is critical for MIS generation [47]. In addition to increases in MIS density, we also observed an increase in MSBs (in primary dendrites), which have been implicated in memory formation [48]. Based on this, we suggest that Aβo can hijack memory mechanisms (MIS and MSB generation) and thereby cause cognitive impairment.
The restoration of bouton density in neurons co-treated with eFT508 suggests that eFT508 may preserve key synaptic constituents’ mechanisms that are otherwise dysregulated in Aβo-exposed neurons. While the precise cascade by which eFT508 exerts this effect remains to be fully elucidated, our data support the hypothesis that a targeted intervention at the level of translational initiation may protect synaptic structure, consistent with the study linking translational control to long-lasting synaptic plasticity and memory [49]. We show that eFT508 modulates some of these Aβo-induced synaptic changes, particularly by mitigating alterations in SSB density. The de novo proteomics suggests that eFT508 treatment modulates many of these same dysregulated proteins, implicating an ability to adjust the neuronal proteome under pathological conditions. Although eFT508 appears protective in mitigating Aβo-induced increases in synapses, we question whether its effects are sufficient to prevent AD progression. Notably, we observed consistent upregulation of mitogen-activated protein kinase 10 or c-Jun kinase 3 expression with both Aβo treatment alone and Aβo combined with eFT508. Mapk10 is specifically expressed in the brain and is elevated in human AD cases, as well as in familial AD mouse models [50]. Importantly, Mapk10 phosphorylates APP, which is crucial in the process of amyloid-beta formation and central to AD pathology [51]. In our study, eFT508 did not inhibit the upregulation of Mapk10. We believe that the effect of eFT508 when used alone is limited and may require a combination with other drugs to target a broader range of pathways. Further investigation, including in vivo confirmation and mechanistic studies of eFT508’s precise role and side effects in mRNA-specific translation, will be essential to validate its therapeutic value.
The analysis of cerebrospinal fluid (CSF) and blood-based biomarkers, which serve as indicators of key pathophysiological processes in the central nervous system, has emerged as a valuable approach for the early and precise clinical diagnosis of AD. These biomarkers not only facilitate early detection but also offer insights into disease progression and potential therapeutic targets. Interestingly, some of our findings exhibit discrepancies with prior studies. While we observed a downregulation of visinin-like protein 1 (Vsnl1/Vilip-1) and neurofilament light polypeptide (Nefl), previous reports have documented their elevation in the CSF or plasma of AD patients [52, 53]. This divergence may be attributed to differences in disease stage, sample origin (CSF vs. blood), or methodological variations across studies. Given that both Vsnl1 and Nefl are linked to neurodegeneration and synaptic dysfunction, future investigations should explore the underlying mechanisms driving these alterations and assess their potential as reliable biomarkers for AD.
Several limitations should be acknowledged in this study. First, it remains unclear whether the newly generated synapses are functionally active. Second, our molecular analyses were conducted using an in vitro model, which may not fully recapitulate the complexity of the in vivo neural environment. Therefore, future studies should prioritize validating these findings in in vivo models and further elucidating the molecular mechanisms underlying synaptic alterations. Such investigations will refine our understanding of early-stage synaptic dysfunction in AD. At this stage, we have not been able to perform these experiments and thus could not determine which specific pathway is involved. We plan to address this in future studies to better elucidate the drug’s mechanism of action. Lastly, we used rat synthetic Aβ oligomers to match our rodent neuron model, ensuring physiological compatibility and protocol consistency. While rodent Aβ1-42 aggregates less efficiently than human Aβ, it suited our in vitro study. Nonetheless, human-derived Aβ oligomers better mimic human AD pathology, so they will need to be used in follow-up studies.
In summary, we demonstrate that low concentrations of Aβo induce distinct synaptic and proteomic alterations associated with early-stage neurodegeneration. The Aβo causes an increase in synapse density similar to what has been observed in MCI. Thus, our work suggests that low concentrations of Aβo recapitulate synaptic changes in MCI, including disruption of synaptic protein homeostasis and alterations in synaptic density. Furthermore, the ability of eFT508, a specific MNK inhibitor, mitigates some of these changes in our in vitro model. Follow-up in vivo studies will need to assess whether eFT508 is a suitable therapeutic candidate for treatment of MCI and early AD. Further investigations into the molecular mechanisms underlying eFT508’s effects are essential to elucidate its role in modulating synaptic function, thereby advancing its development as a potential therapeutic intervention.
Data availability
The datasets generated and/or analyzed during the current study were not deposited in a public repository but are available from the corresponding author upon reasonable request.
References
Lane CA, Hardy J, Schott JM. Alzheimer’s disease. Eur J Neurol. 2018;25:59–70.
Martínez-Serra R, Alonso-Nanclares L, Cho K, Giese KP. Emerging insights into synapse dysregulation in Alzheimer’s disease. Brain Commun. 2022;4:fcac083.
Selkoe DJ, Hardy J. The amyloid hypothesis of Alzheimer’s disease at 25 years. EMBO Mol Med. 2016;8:595–608.
Bell KF, Bennett DA, Cuello AC. Paradoxical upregulation of glutamatergic presynaptic boutons during mild cognitive impairment. J Neurosci. 2007;27:10810–7.
Merlo S, Spampinato SF, Sortino MA. Early compensatory responses against neuronal injury: A new therapeutic window of opportunity for Alzheimer’s Disease?. CNS Neurosci Ther. 2019;25:5–13.
Bell KF, Claudio Cuello A. Altered synaptic function in Alzheimer’s disease. Eur J Pharmacol. 2006;545:11–21.
Bjorklund NL, Reese LC, Sadagoparamanujam VM, Ghirardi V, Woltjer RL, Taglialatela G. Absence of amyloid β oligomers at the postsynapse and regulated synaptic Zn2+ in cognitively intact aged individuals with Alzheimer’s disease neuropathology. Mol Neurodegener. 2012;7:23.
Spires-Jones TL, Hyman BT. The intersection of amyloid beta and tau at synapses in Alzheimer’s disease. Neuron. 2014;82:756–71.
Westmark CJ, Westmark PR, O’Riordan KJ, Ray BC, Hervey CM, Salamat MS, et al. Reversal of fragile X phenotypes by manipulation of AβPP/Aβ levels in Fmr1KO mice. PLoS One. 2011;6:e26549.
Westmark CJ. What’s hAPPening at synapses? The role of amyloid β-protein precursor and β-amyloid in neurological disorders. Mol Psychiatry. 2013;18:425–34.
Cozachenco D, Ribeiro FC, Ferreira ST. Defective proteostasis in Alzheimer’s disease. Ageing Res Rev. 2023;85:101862.
Borreca A, Valeri F, De Luca M, Ernst L, Russo A, Nobili A, et al. Transient upregulation of translational efficiency in prodromal and early symptomatic Tg2576 mice contributes to Aβ pathology. Neurobiol Dis. 2020;139:104787.
Baleriola J, Walker CA, Jean YY, Crary JF, Troy CM, Nagy PL, et al. Axonally synthesized ATF4 transmits a neurodegenerative signal across brain regions. Cell. 2014;158:1159–72.
Li C, Götz J. Tau-based therapies in neurodegeneration: opportunities and challenges. Nat Rev Drug Discov. 2017;16:863–83.
Cefaliello C, Penna E, Barbato C, Di Ruberto G, Mollica MP, Trinchese G, et al. Deregulated local protein synthesis in the brain synaptosomes of a mouse model for Alzheimer’s disease. Mol Neurobiol. 2020;57:1529–41.
Ghosh A, Mizuno K, Tiwari SS, Proitsi P, Gomez Perez-Nievas B, Glennon E, et al. Alzheimer’s disease-related dysregulation of mRNA translation causes key pathological features with ageing. Transl Psychiatry. 2020;10:192.
Elder MK, Erdjument-Bromage H, Oliveira MM, Mamcarz M, Neubert TA, Klann E. Age-dependent shift in the de novo proteome accompanies pathogenesis in an Alzheimer’s disease mouse model. Commun Biol. 2021;4:823.
Ma Y, McClatchy DB, Barkallah S, Wood WW, Yates JR III. HILAQ: A novel strategy for newly synthesized protein quantification. J Proteome Res. 2017;16:2213–20.
Wang X, Zhou X, Lee J, Furdui CM, Ma T. In-depth proteomic analysis of de novo proteome in a mouse model of Alzheimer’s disease. J Alzheimers Dis. 2023;91:1471–82.
Brown MC, Gromeier M. MNK Controls mTORC1: Substrate association through regulation of TELO2 binding with mTORC1. Cell Rep. 2017;18:1444–57.
Chalkiadaki K, Hooshmandi M, Lach G, Statoulla E, Simbriger K, Amorim IS, et al. Mnk1/2 kinases regulate memory and autism-related behaviours via Syngap1. Brain. 2023;146:2175–90.
Huang B, Jin P, Yi K, Duan J. MAPK-interacting kinases inhibition by eFT508 overcomes chemoresistance in preclinical model of osteosarcoma. Hum Exp Toxicol. 2023;42:9603271231158047.
Jin X, Yu R, Wang X, Proud CG, Jiang T. Progress in developing MNK inhibitors. Eur J Med Chem. 2021;219:113420.
Chen F, Tillberg PW, Boyden ES. Optical imaging. Expansion microscopy. Science. 2015;347:543–8.
Ngo JT, Tirrell DA. Noncanonical amino acids in the interrogation of cellular protein synthesis. Acc Chem Res. 2011;44:677–85.
Webster KR, Goel VK, Hung IN, Parker GS, Staunton J, Neal M, et al. eFT508, a potent and selective mitogen-activated protein kinase interacting kinase (MNK) 1 and 2 inhibitor, is efficacious in preclinical models of diffuse large B-cell lymphoma (DLBCL). Blood. 2015;126:1554.
Dreas A, Mikulski M, Milik M, Fabritius CH, Brzózka K, Rzymski T. Mitogen-activated protein kinase (MAPK) interacting kinases 1 and 2 (MNK1 and MNK2) as targets for cancer therapy: Recent progress in the development of MNK inhibitors. Curr Med Chem. 2017;24:3025–53.
Shah SH, Schiapparelli LM, Yokota S, Ma Y, Xia X, Shankar S, et al. Quantitative BONCAT allows identification of newly synthesized proteins after optic nerve injury. J Neurosci. 2022;42:4042–52.
Tyanova S, Temu T, Sinitcyn P, Carlson A, Hein MY, Geiger T, et al. The Perseus computational platform for comprehensive analysis of (prote)omics data. Nat Methods. 2016;13:731–40.
Jucker M, Walker LC. Pathogenic protein seeding in Alzheimer disease and other neurodegenerative disorders. Ann Neurol. 2011;70:532–40.
Chen F, Tillberg PW, Boyden ES. Expansion microscopy. Science. 2015;347:543–8.
Xu G, Ran Y, Fromholt SE, Fu C, Yachnis AT, Golde TE, et al. Murine Aβ over-production produces diffuse and compact Alzheimer-type amyloid deposits. Acta Neuropathol Commun. 2015;3:72.
Rönicke R, Mikhaylova M, Rönicke S, Meinhardt J, Schröder UH, Fändrich M, et al. Early neuronal dysfunction by amyloid β oligomers depends on activation of NR2B-containing NMDA receptors. Neurobiology of Aging. 2011;32:2219–28.
Zhou B, Lu JG, Siddu A, Wernig M, Südhof TC. Synaptogenic effect of APP-Swedish mutation in familial Alzheimer’s disease. Sci Transl Med. 2022;14:eabn9380.
Lee K, Park TI, Heppner P, Schweder P, Mee EW, Dragunow M, et al. Human in vitro systems for examining synaptic function and plasticity in the brain. J Neurophysiol. 2020;123:945–65.
Yan Z, Rein B. Mechanisms of synaptic transmission dysregulation in the prefrontal cortex: pathophysiological implications. Mol Psychiatry. 2022;27:445–65.
Aziz W, Kraev I, Mizuno K, Kirby A, Fang T, Rupawala H, et al. Multi-input synapses, but not LTP-strengthened synapses, correlate with hippocampal memory storage in aged mice. Curr Biol. 2019;29:3600–.e3604.
Waskiewicz AJ, Johnson JC, Penn B, Mahalingam M, Kimball SR, Cooper JA. Phosphorylation of the Cap-binding protein eukaryotic translation initiation factor 4E by protein kinase Mnk1 in vivo. Mol Cell Biol. 1999;19:1871–80.
Oddo S, Caccamo A, Shepherd JD, Murphy MP, Golde TE, Kayed R, et al. Triple-transgenic model of Alzheimer’s disease with plaques and tangles: intracellular Abeta and synaptic dysfunction. Neuron. 2003;39:409–21.
Wurz AI, Schulz AM, O’Bryant CT, Sharp JF, Hughes RM. Cytoskeletal dysregulation and neurodegenerative disease: Formation, monitoring, and inhibition of cofilin-actin rods. Front Cell Neurosci. 2022;16:982074.
Palmer JE, Wilson N, Son SM, Obrocki P, Wrobel L, Rob M, et al. Autophagy, aging, and age-related neurodegeneration. Neuron. 2025;113:29–48.
Ciechanover A, Kwon YT. Degradation of misfolded proteins in neurodegenerative diseases: therapeutic targets and strategies. Exp Mol Med. 2015;47:e147.
Wang Z, Yang L, Zheng H. Role of APP and Aβ in synaptic physiology. Curr Alzheimer Res. 2012;9:217–26.
Renner M, Lacor PN, Velasco PT, Xu J, Contractor A, Klein WL, et al. Deleterious effects of amyloid beta oligomers acting as an extracellular scaffold for mGluR5. Neuron. 2010;66:739–54.
Westmark CJ, Malter JS. FMRP mediates mGluR5-dependent translation of amyloid precursor protein. PLoS Biol. 2007;5:e52.
Borczyk M, Radwanska K, Giese KP. The importance of ultrastructural analysis of memory. Brain Res Bull. 2021;173:28–36.
McLeod F, Boyle K, Marzo A, Martin-Flores N, Moe TZ, Palomer E, et al. Wnt Signaling through nitric oxide synthase promotes the formation of multi-innervated spines. Front Synaptic Neurosci. 2020;12:575863.
Geinisman Y, Berry RW, Disterhoft JF, Power JM, Van der Zee EA. Associative learning elicits the formation of multiple-synapse boutons. J Neurosci. 2001;21:5568–73.
Costa-Mattioli M, Sossin WS, Klann E, Sonenberg N. Translational control of long-lasting synaptic plasticity and memory. Neuron. 2009;61:10–26.
Yoon SO, Park DJ, Ryu JC, Ozer HG, Tep C, Shin YJ, et al. JNK3 perpetuates metabolic stress induced by Aβ peptides. Neuron. 2012;75:824–37.
Bruckner SR, Tammariello SP, Kuan CY, Flavell RA, Rakic P, Estus S. JNK3 contributes to c-Jun activation and apoptosis but not oxidative stress in nerve growth factor-deprived sympathetic neurons. J Neurochem. 2001;78:298–303.
Halbgebauer S, Steinacker P, Riedel D, Oeckl P, Anderl-Straub S, Lombardi J, et al. Visinin-like protein 1 levels in blood and CSF as emerging markers for Alzheimer’s and other neurodegenerative diseases. Alzheimer’s Res Ther. 2022;14:175.
Lewczuk P, Ermann N, Andreasson U, Schultheis C, Podhorna J, Spitzer P, et al. Plasma neurofilament light as a potential biomarker of neurodegeneration in Alzheimer’s disease. Alzheimer’s Res Ther. 2018;10:71.
Acknowledgements
We are grateful to eFFECTOR Therapeutics, USA for eFT508 and Dr. Michiko Sumiya for advice on eFT508 concentration. We thank Drs. Xingjian Wang and Sam Barnes (Imperial College London, UK) for advice on expansion microscopy, Dr. Jürgen Götz (University of Sydney, Australia) for advice on BONCAT experiments, and Dr. Alessio Delogu for helpful comments on an earlier draft of this manuscript. This work was supported by the King’s-China Scholarship Council PhD Scholarship Program (to K.W.), a King’s-Korean Brain Research Institute PhD studentship (to S.L.), an MRC PhD studentship (MR/N013700/1 to R.M.-S.), and an Alzheimer’s Society grant (AS-PG-21-008) awarded to K.P.G. The use of the Nikon AX Inverted Confocal Microscope was made possible through support from the Wohl Cellular Imaging Centre (WCIC).
Author information
Authors and Affiliations
Contributions
K.W. and K.P.G. designed the project and wrote the manuscript. K.W. performed most of the experiments and analysed the data. Suji L. provided and treated a portion of the primary neurons used, and optimized BONCAT protocol and IP in this study. R.M.-S. developed the protocol for Expansion Microscopy. L.Z. contributed to figure preparation related to proteomics data. Steven L. conducted the mass spectrometry analysis. All authors discussed the results and commented on the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The killing of time-mated rats was according to the UK Animals (Scientific Procedures) Act 1986 and approval by the animal welfare and ethical reviewing body at King’s College London, UK.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wu, K., Lee, S., Martinez-Serra, R. et al. Low concentrations of amyloid-beta oligomers induce synaptogenesis characteristic for mild cognitive impairment and alter the de novo proteome. Transl Psychiatry 16, 132 (2026). https://doi.org/10.1038/s41398-026-03905-x
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41398-026-03905-x