Abstract
Stimulants are the first-line pharmacological treatment for ADHD and generally effective, yet 35–61% of individuals discontinue treatment within a year. We investigated the contribution of common and rare genetic variants to early stimulant discontinuation using data from 18,362 individuals with ADHD (31% female) initiating stimulants in iPSYCH, a Danish population-based case-cohort linked to national registers. Discontinuation was defined as a ≥ 180-day gap between dispensations within one year of initiation. We examined genetic differences by age groups, estimated SNP-heritability (h2SNP), conducted genome-wide association studies (GWAS), polygenic score (PGS) analyses, and assessed associations with protein truncating variants (PTV). Within one year, 7102 individuals (39%) had discontinued stimulants. Age-stratified analyses (cut-off: age 16) revealed low genetic correlation (r₉ = 0.23, 95% CI: –0.37, 0.83) between children and adolescents/adults. The h²snp for discontinuation was 0.06 (95% CI: 0.02, 0.11) overall, 0.08 (95% CI: 0.02, 0.14) in children, and 0.14 (95% CI: 0.02, 0.27) in adolescents/adults. No genome-wide significant loci were identified overall or in adolescents/adults; however, one locus (SLC5A12, chromosome 11) reached genome-wide significance in children. Ten of 36 PGSs were associated with discontinuation, with higher psychiatric risk PGSs predicting increased discontinuation, while educational attainment and BMI PGSs showed divergent effects by age. Reduced burden of dopamine-related PTVs was nominally associated with discontinuation, particularly in adolescents/adults. These findings suggest modest contributions of both common and rare variants to stimulant discontinuation in ADHD and point to potential developmental differences in genetic architecture.
Similar content being viewed by others
Introduction
Attention-deficit hyperactivity disorder (ADHD) is a common neurodevelopmental condition affecting 5–7% of children, with prevalence declining to 1% in older adults [1]. Stimulant medications are first-line pharmacological treatment and found effective in reducing core symptoms in randomized controlled trial [2]. Observational studies also report positive effects on real-world outcomes, including injury rates, educational attainment, and substance misuse [3]. However, 20–40% of individuals have suboptimal response to stimulants, and while generally well tolerated, side effects such as headaches, appetite loss, sleep disturbances, and elevated blood pressure or heart rate are common, particularly during initiation [1, 2, 4]. Adverse effects and poor response are along with dosing inconvenience, stigma, and patient attitudes common reported reason for medication discontinuation in ADHD [5, 6]. A recent multi-national study found that 35–61% of individuals with ADHD discontinued medication within one year of starting, with higher rates among adolescents and adults compared to children [7]. U.S. studies further show that more than half of children [8] and adults [9] with ADHD do not refill their first prescription, suggesting that many disengage during the titration phase—a crucial period for identifying optimal treatment [1]. Early discontinuation can represent a major challenge, resulting in potential symptom exacerbation, functional impairment, and elevated risk of adverse outcomes [1,2,3]. Understanding why some individuals discontinue treatment early is therefore essential to improve long-term management of ADHD.
It is increasingly recognized that variability in treatment response and tolerability to psychotropic medication is influenced by genetics. Yet large-scale studies aimed at discovering genetic factors affecting pharmacotherapeutic outcomes in psychiatry in general, and ADHD in particular, are sparse [10]. Identifying genetic markers associated with stimulant discontinuation could offer new insights into the biological mechanisms underlying treatment response, tolerability, as well as behaviors related to medication persistence. This may inform more tailored treatment approaches, including risk stratification at medication initiation, prediction of tolerability profiles, or alternative treatment strategies for those at higher risk of discontinuation. To date, pharmacogenomic ADHD research has been dominated by candidate gene studies focused on methylphenidate (MPH). Replicated associations are reported for variants in DAT, DRD4, ADRA2A, COMT, and NET genes, though individual effect sizes are modest [11, 12]. Only three small genome-wide association studies (GWAS; N < 200) have examined MPH response [13, 14] or adverse effects [15], with no genome-wide significant loci identified. We recently reported suggestive evidence that common genetic variants contribute to stimulant discontinuation [16] defined by prescriptions from 7427 individuals with ADHD [17, 18]. SNP-heritability (h2SNP) was estimated to be 0·13 (SE 0·08) and higher polygenic scores (PGSs) for bipolar disorder and schizophrenia were associated with increased rates of discontinuation. However, broader genetic liabilities, including traits related to cognition, physical comorbidity (e.g., obesity, blood pressure, cardiometabolic risk), and side-effects [2,3,4, 19] may also influence discontinuation. Additionally, individuals with ADHD show an elevated burden of protein-truncating variants (PTVs) in highly constrained genes [20, 21] and rare variants are proposed to influence medication metabolism, response and tolerability [22]. Yet, no studies have investigated the role of rare variants in genes potentially relevant for stimulant pharmacodynamics. Finally, no studies have examined genetic contributions to age-related differences in discontinuation, despite known age-related variation in discontinuation rates, comorbidity profiles, and ADHD h2SNP [5, 7, 21]. To address these knowledge gaps, we aimed to comprehensively characterize the contributions of common and rare genetic variants to stimulant discontinuation in individuals with ADHD. We specifically focus on early medication discontinuation, based on the hypothesis that individuals who experience strong side effects or lack of therapeutic response are more likely to discontinue treatment early than individuals for whom the medication is working well, but might discontinue later due to less biological factors. Consequently, our design may increase the likelihood of capturing the genetic and biological components of treatment discontinuation.
Subjects and methods
Study population and genomic data
iPSYCH is a population-based case-cohort identified from all singletons born in Denmark 1 May 1981 until 31 December 2008, linked to national registries using the personal identification number assigned to all Danish residents [17, 18]. iPSYCH includes 50,615 randomly selected population-based controls and 79,336 individuals with at least one diagnosis of ADHD (F90.0), schizophrenia spectrum disorders (SCZ;F20-F29), affective disorders (F30–F39), or autism (ASD;F84.0,F84.1,F84.5,F84.8,F84.9) in the Danish Psychiatric Central Research Register (DPCRR) between 1 January 1994 and 31 December 2015 [23]. The DPCCR contains data on all in-patient admissions since 1969 and outpatient since 1995. Diagnoses are recorded according the International Classification of Diseases, 10th revision, Diagnostic Criteria for Research from 1994 [23]. We selected all iPSYCH individuals diagnosed with ADHD and with >1 dispensation of a stimulant ADHD medication (methylphenidate [N06BA04], dexamfetamine [N06BA02], lisdexamfetamine [N06BA12]) between 1 January 1996 and 31 December 2018 in the Danish National Prescription Register (DNPR) [24]. DNPR includes all redeemed prescriptions in Denmark since 1995 classified by Anatomical Therapeutic Chemical (ATC) codes. Information on sex assigned at birth, date of birth, emigration and death were obtained from the Danish Civil Registration System and the Cause of Death Register. Individuals who died, emigrated, or with missing information during follow-up were excluded.
DNA from all individuals in iPSYCH was extracted from dried bloodspots obtained from the Danish Neonatal Screening Biobank. iPSYCH individuals were genotyped in two waves (iPSYCH2012 and iPSYCH2015i), using Illumina´s PsychChip and Global Screening array, and subsequently merged. Detailed descriptions of the sample, DNA extraction [17, 18], imputation, and quality control (QC) [19] are provided elsewhere. For current analyses, best guess genotypes from the combined, imputed and QC´ed iPSYCH sample (nSNPs = 8785,478; nsample = 134,628) were extracted. We excluded variants with imputation info score <0.8, minor allele frequencies (MAF) < 0.01, missing call rates >0.02, and with Hardy-Weinberg equilibrium exact test p-value < 1×10−8, as well as samples with missing call rates >0.05, leaving 7,124,623 SNPs from 22 autosome chromosomes. Filtering was done using the bigsnpr R package [25] and PLINK1.9 [26]. After phenotypic and genomic filtering, 18,362 individuals were retained for analyses (Fig. 1).
Individuals diagnosed with ADHD, affective disorders, schizophrenia spectrum disorder, and/or autism from the iPSYCH cohort was the initial sample before filtering. Individuals who died, emigrated, has missing information in the civil registration system or only redeemed one stimulant prescription during follow-up were excluded from analyses. After the filtering steps, 18,362 individuals diagnosed with ADHD and > 1 stimulant medication dispensation were retained for analyses.
Stimulant discontinuation
DNPR does not contain information about prescription length or cause of discontinuation. Therefore and in line with prior research [7, 16], we defined stimulant discontinuation by a gap ≥180 days between dispensations. The ≥180 days cut-off was selected to capture clinically meaningful medication gaps rather than shorter breaks. We focused on discontinuation within one year of initiation (i.e. first stimulant dispensation in the DNPR) as this may be more likely to reflect discontinuation due to poor response or tolerability, which may in turn be more influenced by genetics, compared to discontinuation after longer-term treatment. Individuals with a gap ≥180 days between consecutive stimulant dispensations were defined as discontinuers if the last dispensation followed by the gap occurred within the first year of initiation (Figure S1).
Statistical analyses
h2 SNP and GWAS
To evaluate the variance in stimulant discontinuation explained by the included SNPs, h2SNP was estimated using genome-based restricted maximum likelihood (GREML) implemented in GCTA [27]. We report h2SNP on the observed scale due to the variability prevalence estimates of discontinuation in the ADHD population. To explore age-related genetic differences, we split the sample by age at initiation using a genetically informed cut-off, moving the cut-off one year at a time. At each cut-off, h2SNP and genetic correlation (rg) between “child” and “adolescent/adult” groups were estimated to identify the cut-off with the largest genetic difference (lowest rg) between groups, while maintaining adequate sample sizes. GWAS was then performed using logistic regression in PLINK1.9 for all individuals, the child group, and the adolescent/adult group. Analyses were corrected for sex assigned at birth, genotyping wave, age at initiation, and the first 10 ancestral principal components (PCs). See Supplement for details.
Polygenic score analyses
We selected 36 polygenic scores (PGSs) for phenotypes relevant to ADHD and ADHD medication outcomes from a catalog of 943 PGSs generated in the iPSYCH cohort using LDpred2 [28] and GWAS summary statistics without iPSYCH data, which has been described in details [29] (see also Supplement). PGSs for ADHD, major depressive disorder (MDD), SCZ, bipolar [BP] and autism were generated using meta-PRS described in Ref. 28, which combine internal individual-level data and external GWAS summary statistics for polygenic prediction, and has proven more precise when large individual-level data are available. PGSs represented domains including psychiatric disorders, education and cognition, cardiometabolic traits, and potential adverse effects of ADHD medication or self-medication (Table S1). Associations with stimulant discontinuation were estimated using logistic regression in the full sample and by age group, adjusting for age at first dispensation, sex, genotyping batch, and the first 10 principal components. Results are reported as odds ratios (ORs) with 95% confidence intervals (CI) per standard deviation increase in PGS. The Benjamini–Hochberg False discovery rate (FDR) correction was applied in the full sample and each age-group, adjusting for 36 tests. For PGSs with associations surviving FDR correction, we estimated the odds of discontinuation across quintiles relative to the lowest. Variance explained by the PGS was estimated as the difference in Pseudo-R² between a model with covariates only and covariates plus PGS. We tested for replication of associated PGSs in an independent sample of 829 individuals with ADHD who had initiated stimulant treatment from the Child and Adolescent Twin Study in Sweden (CATSS) [30]. We used generalized estimating equations with a logit link and cluster-robust standard errors to account for twin relatedness. Analyses were conducted in R and adjusted for the same covariates as the main analyses. We report nominally significant associations (p < 0.05) and FDR-corrected p-values. Details in Supplement.
Rare variant analyses
We investigated the role of protein-truncating variants (PTVs) in discontinuation using exome sequencing data from a subsample of 5999 individuals in iPSYCH (2280 discontinuers and 3719 continuers). Although PTVs with strong deleterious effects are typically rare due to negative selection, stimulant discontinuation is unlikely to have been under such evolutionary pressure. Therefore, we included both rare and low-frequency PTVs (minor allele frequency ≤0.01). We analyzed three gene sets (Tables S2–S4), selected for their hypothesized involvement in stimulant and/or dopamine response, as stimulant medications act by increasing extracellular dopamine levels [2]. These were: (1) pLI genes, including 2991 loss-of-function-intolerant genes (pLI > 0.9) based on gnomAD v2.1.1; (2) dopamine response genes, including 82 genes involved in cellular or organismal responses to dopamine, identified in MSigDB; and (3) stimulant medication genes, including 44 genes identified via DGIdb v5.0 using the term “methylphenidate+hydrochloride”. We focused on genes interacting with methylphenidate, as around 80% of individuals with ADHD in Denmark initiate treatment with methylphenidate [7]. The remaining patients are treated primarily with non-stimulants and initiating treatment with other stimulants is very rare [7]. As a negative control, we also evaluated the burden of synonymous variants in each gene set, as these are not expected to affect protein function or medication response. Details are in Supplement.
Sensitivity analyses
We conducted two sensitivity analyses. First, we re-estimated h2SNP further adjusting for co-occurring iPSYCH-ascertained disorders (SCZ, ASD and affective disorders). Second, we re-estimated h2SNP, and performed GWAS and PGS analyses after excluding 3257 individuals who discontinued within three months of treatment initiation, as this may reflect limited treatment engagement [8, 9] which is potentially less influenced by genetics.
Results
Among 18,362 individuals with ADHD who started stimulant treatment (31·0% female), the median age at initiation was 12 years (IQR 8–18). Within one year, 7102 (39·0%) had discontinued. Discontinuers had a higher median age at initiation than continuers (15 years [IQR 10–20] vs 10 years [IQR 8–15]) and more often at least one co-occuring iPSYCH diagnosis (32·0% of discontinuers vs 28·0% of continuers [Table 1]).
SNP-heritability and GWAS
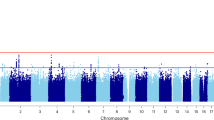
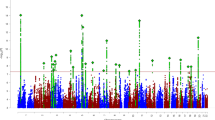
In the full sample, the h2SNP of discontinuation was 0.06 (95% CI 0.02–0.11) and significantly different from zero (p < 0·001), indicating a small common variant contribution. Table S5 shows the h2SNP, rg and associated test statistics from age-stratified analyses. The lowest rg, between children and adolescents/adults was observed when splitting at age 16 (rg = 0·23, 95%CI 0·37–0·83), which was significantly different from 1 (p < 0·012). The h2SNP of discontinuation was 0·08 (95% CI 0·02–0·14) in children <16 years and 0·14 (95% CI 0·02–0·27) in adolescents/adults ≥16 years. Henceforth, the full sample is referred to as DISCALL (n = 18,362; 7102 discontinuers), the child group as DISCbelow16 (n = 12,229; 3598 discontinuers), and the adolescents/adult group as DISCabove16 (n = 6133; 3504 discontinuers). Adjusting for co-occurring iPSYCH ascertained disorders did not affect h2SNP estimates (Table S6) and were therefore not included as covariates in subsequent analyses. No genome wide significant loci were identified for DISCALL or DISCabove16 (Figure S2 and S4). One locus on chromosome 11 reached genome wide significance in DISCbelow16 (index variant rs73438427, OR 0·65, p = 1·54 × 10⁻⁸; Figure S3), located in the protein-coding gene SLC5A12 (Figure S5). Table S7 presents the top 10 SNPs associated with DISCbelow16 and their corresponding associations in DISCALL and DISCabove16. Genomic inflation factors (λ) were <1·02 across GWASs and visual inspection of QQ plots (Figures S6–S8) showed no strong evidence of residual confounding.
Polygenic score analyses
Table S8-S10 show all PGS associations. Ten of the 36 selected PGSs were statistically significantly associated with stimulant discontinuation in at least one of three groups (DISCALL, DISCbelow16 or DISCabove16) after FDR correction (Table 2). These included PGSs for five psychiatric (psychopathology [P]-factor, SCZ, MDD, BP obssesive compulsive disorder [OCD]), two cognitive (educational attainment [EA], intelligence quotient [IQ]), and three phenotypes related to adverse effects or self-medication (cannabis use [CU], body mass index [BMI], and migraine). No cardio-metabolic PGSs were significantly associated with discontinuation. In DISCALL, the strongest associations were with the P-factor-PGS, derived from a factor analysis of GWAS of SCZ and MDD, (OR 1·11, 95% CI 1·08–1·14) and SCZ-PGS (OR 1·10, 95% CI 1·06–1·13). In DISCbelow16 the strongesG associations were with the P-factor-PGS (OR 1·12, 95% CI 1·08–1·17) and the BMI-PGS (OR 0·90, 95% CI 0·86–0·94). In DISCabove16, the strongest associations were with SCZ-PGS (OR 1·09, 95% CI 1·03–1·14) and IQ-PGS (OR 0·91, 95% CI 0·87–0·96). Notably, the EA-PGS showed opposite directions of association in DISCbelow16 (OR 1·06, 95%CI 1·02–1·11) and DISCabove16 (OR 0·93, 95%CI 0·88–0·97). Each PGS explained from 0.01–0·23% of the variance in discontinuation (Tables S8–S10). ORs by PGS quintiles for the 10 associated PGSs are shown in Fig. 2 and Table S11.
Odds ratio (OR) and 95% confidence intervals (CI) for stimulant discontinuation among individuals with ADHD who initiated stimulant treatment, by their polygenic score (PGS) quintiles (on the x-axis) for the following phenotypes: psychopathology (P) factor, schizophrenia, major depressive disorder, bipolar disorder, obsessive compulsive disorder, body mass index, IQ, educational attainment, migraine, and cannabis use. First quintile is used as reference. Results are shown for DISCALL (in orange), DISCbelow16 (purple), and DISCabove16 (green) and vertical bars indicate 95% confidence intervals.
Testing for replication in an independent sample (n = 829; 39% discontinuers; Table S12), only the BMI- and IQ-PGSs were nominally associated with discontinuation in the full sample, showing consistent direction of effects as in iPSYCH. In DISCbelow16 (n = 592, 33% discontinuers), MDD-PGS and SCZ-PGS were nominally associated with increased odds of discontinuation, while in DISCabove16 (n = 237, 56% discontinuers) BMI-PGS again showed a nominal negative association. No associations survived FDR correction. PGSs for the P-factor, OCD, and cannabis use disorders could not be generated due to data linkage constraints.
Rare variant analyses
Neither PTVs in the pLI gene set (OR 1·01, 95% CI 0·98–1·05) nor in the stimulant medication gene set (OR 0·96, 95% CI 0·75–1·23) were associated with discontinuation (Table S13). PTVs in dopamine response genes showed a nominally significant (p < 0.05) association in DISCALL (OR 0·81, 95% CI 0·66–0·99), indicating a lower PTV burden in discontinuers compared to continuers. A similar, though non-significant, effect was observed in DISCbelow16 (OR 0·89, 95% CI 0·69–1·15), while a somewhat stronger and nominally significant association was seen in DISCabove16 (OR 0·64, 95% CI 0·45–0·91; p < 0·02) (Fig. 3).
Boxplot of odds ratios (OR) and 95% confidence intervals (CI) from logistic regression of the effect of protein truncating variants (PTVs) in the “dopamine response” gene set on stimulant discontinuation. ORs are shown as a solid vertical line and upper and lower 95%CI as the upper and lower boundaries of the boxes for DISCALL, DISCbelow16 and DISCabove16. Results are shown for PTVs in red, and for comparison the load of synonymous variants in green.
Sensitivity analyses
In sensitivity analyses excluding individuals who discontinued stimulants within the first three months, 15,105 were retained of whom 25% discontinued within 1 year (n discontinuers=3845 [eDISCall]). The age split yielding the lowest rg between children and adolescents/adults was 14 years (rg 0·12, 95% CI –0·47–0·71). h2SNP was 0·07 (95% CI 0·01–0·12) for eDISCALL, 0·09 (0·01–0·17) for eDISCbelow14, and 0·18 (0·05–0·31) for eDISCabove14 (table S14). No genome-wide significant loci were identified (Figure S9-S14). PGSs for the P-factor, SCZ and BMI (figures S15–17; table S15) were significantly associated with discontinuation in the eDISC samples, with consistent directions of effect as in the main analyses.
Discussion
We found evidence of a small contribution of common genetic variants to stimulant discontinuation, with h²snp estimates indicating slightly higher heritability in adolescents and adults than in children. The age cut-off between children and adults at 16 years was determined by genetics analyses, but grouping of adolescents together with young adults are in line with findings from a large epidemiological study that identified differences in treatment discontinuation in children (7–11 years) compared to adolescents (12–17) and young adults (18 – 25 years), with lower discontinuation in the childhood group compared to the other two groups [7]. The GWAS identified one significantly associated locus in children below 16 at initiation, located in the gene SLC5A12. PGSs for mainly adult-onset psychiatric disorders, cognitive, side-effect and body weight related phenotypes were associated with discontinuation, with the strongest signals seen for the P-factor, schizophrenia, educational attainment and BMI PGSs. Several of these associations showed age-specific patterns. Rare variant analyses showed no associations with protein-truncating variants (PTVs) in broad constraint- or medication-related gene sets, but nominal evidence of reduced PTV burden in dopamine response genes among discontinuers. Together, these findings suggest that both common and rare genetic variants can influence stimulant discontinuation, albeit with small effects, and that genetic contributions may be partially distinct across age groups.
We identified one genome-wide significant locus for stimulant discontinuation in children, located on chromosome 11 within SLC5A12, a gene encoding a sodium-coupled monocarboxylate transporter involved in lactate and pyruvate transport. The gene is primarily expressed in peripheral tissues with limited expression in the brain and has not been previously been implicated in ADHD, neurodevelopment, or drug metabolism. Thus, the relevance of this finding for stimulant pharmacokinetics remains unclear and would need to be replicated in independent cohorts. This is the largest GWAS of stimulant-treatment related outcomes to date, yet we did not identify genome-wide significant associations beyond this single locus. This underscores the challenge to detect common variants with small to moderate effects influencing multifactorial traits like medication discontinuation, even in relatively large pharmacogenomic samples. Replication and meta-analysis with other cohorts is needed to increase power and validate findings, yet this remains challenging due to the limited availability of pharmacogenomic ADHD samples. Further, our findings of modest SNP-heritability and the lack of strong genome-wide significant signals suggest that biological influences likely only explain a small part of stimulant discontinuation. Genetic associations may be more readily detectable for measures of stimulant response and tolerability, as found in recent pharmacogenomics studies of symptom change following antidepressant treatment [31].
Among the 36 polygenic scores examined, psychiatric PGSs showed the clearest pattern of association with stimulant discontinuation, particularly for the general psychopathology (P-factor) and schizophrenia. These associations were largely consistent across age, suggesting that higher genetic burden for mood and psychotic disorder increases the likelihood of discontinuation. Effects of psychiatric PGSs were somewhat stronger in children, yet the overall pattern supports a link between broad psychiatric vulnerability and reduced treatment persistence across ages. This aligns with clinical observations and some prior research, suggesting that psychiatric comorbidities can complicate ADHD treatment [2, 5]. Our findings highlight the potential value of genetic predisposition as an early indicator of treatment challenges, providing insights that precede, and may be independent of, the later emergence of psychiatric disorders. Interestingly, the ADHD-PGS was not associated with discontinuation, suggesting distinct genetic influences on ADHD diagnosis and stimulant persistence. This is also partly supported by inconsistent findings, where some studies have linked more severe ADHD symptoms to better treatment response and others the opposite patterns [32].
Similarly, no association was observed for alcohol use disorder PGS, despite prior evidence linking substance misuse to treatment complications and drop-out [2, 5, 16]. Polygenic load for cognitive traits showed diverging effects by age. In adolescents/adults, higher IQ- and educational attainment (EA)-PGSs were associated with reduced odds of discontinuation, consistent with studies linking higher education to better treatment adherence [6]. In contrast, in children, higher EA-PGS was associated with increased odds of discontinuation, potentially reflecting less severe ADHD symptoms or greater access to alternative strategies for managing ADHD in families with higher EA. BMI and migraine were associated with reduced discontinuation in children. Higher genetic propensity for higher BMI may offset stimulant-related appetite suppression, which is a common cause of discontinuation for children with a standard-range BMI [2]. The Migraine-PGS was also inversely associated with discontinuation in children, potentially due to a hypothesized beneficial effect of stimulants on dopamine-linked migraine symptoms [33]. Cardiometabolic PGSs showed no association with discontinuation, consistent with emerging evidence that stimulants does not confer significant cardiovascular risk when considering short-term treatment [34]. While our PGS findings highlight biologically plausible mechanisms and potential age-specific effects underlying stimulant discontinuation, PGSs explained only a small proportion of variance (0.003–0.23%), limiting clinical utility of current PGSs.
Rare variant analyses suggested that individuals who discontinued stimulants had a lower burden of protein-truncating variants (PTVs) in dopamine response genes, particularly among adolescents and adults. This may reflect less disruption of dopamine pathways and potentially less severe ADHD, indicating a reduced biological need for stimulant treatment. In contrast, individuals with a higher PTV burden may have more impaired dopamine signaling and therefore benefit more from stimulants, leading to continued use. While this points to a possible link between rare variant load and treatment efficacy or necessity, the lack of association of the ADHD-PGS, which is linked to ADHD symptom severity [35], complicates this interpretation. Given the modest effect sizes and nominal significance, findings should be interpreted cautiously but highlight need for further research into how rare genetic variation may shape treatment response in ADHD.
In summary, we observed age-related differences in the genetic underpinnings of discontinuation. Among adolescents and adults 16 or older, stronger genetic associations in common and rare variant signals could suggest that discontinuation in this group more often reflects individual biological responses, such as perceived efficacy or side-effects. In contrast, discontinuation among children may be more influenced by external factors, including clinicians and parental preferences. These age-related patterns, though modest, point to developmental and contextual influences on how genetic liability shapes treatment discontinuation in ADHD.
This study has several limitations. First, the sample was underpowered to conduct sex-stratified or subgroup analyses based on specific medication patterns. Second, discontinuation was defined using dispensation data, without information on adherence or reasons for stopping treatment. Genetic influences may differ by discontinuation cause (e.g., adverse effects vs poor response), but we could not disentangle these. Furthermore, our sensitivity analysis did not suggest that inclusion of individuals who discontinued within three months had a strong impact on the results. Nevertheless, it should be noted that we did not have information on the cause of discontinuation and therefore cannot separate discontinuation due to side effects or poor response from low treatment engagement, which in particular could affect those with early discontinuation, where the former likely has a larger biological component. Third, registry coverage for ADHD diagnoses were available from 1994 and prescription data from 1996, resulting in possible misclassification of treatment initiation. However, ADHD diagnosis and medication use were rare in Denmark prior to mid-2000s, suggesting this is unlikely to substantially impact findings. Finally, we only investigated the genetic architecture underlying early stimulant discontinuation which might differ from the genetic underpinnings of longe-term treatment patters, and the sample was limited to individuals of European ancestry and findings may therefore not generalize to other populations.
We found that common and rare genetic variants modestly contribute to stimulant discontinuation in ADHD, without identifying strong effects from individual genes. Our findings tentatively support genetic contributions to age-related differences in discontinuation and suggest that genetic liability for broad psychiatry vulnerability, BMI and cognition, but not ADHD itself, impacts treatment discontinuation. Future large-scale studies are needed to clarify the relevance of our findings for stimulant discontinuation, response and tolerability and in developing personalized ADHD treatment strategies.
Data availability
iPSYCH data can be accessed after approval by the iPSYCH Data Access Committee and can only be accessed on the secured Danish server (GenomeDK [https://genome.au.dk]) as the data are protected by Danish legislation. For data access and correspondence contact: Ditte Demontis (ditte@biomed.au.dk).
References
Faraone SV, Bellgrove MA, Brikell I, Cortese S, Hartman CA, Hollis C, et al. Attention-deficit/hyperactivity disorder. Nat Rev Dis Primers. 2024;10:11. https://doi.org/10.1038/s41572-024-00495-0.
Cortese S. Pharmacologic treatment of attention deficit–hyperactivity disorder. N Engl J Med. 2020;383:1050–6. https://doi.org/10.1056/NEJMra1917069.
Chang Z, Ghirardi L, Quinn PD, Asherson P, D’Onofrio BM, Larsson H. Risks and benefits of attention-deficit/hyperactivity disorder medication on behavioral and neuropsychiatric outcomes: a qualitative review of pharmacoepidemiology studies using linked prescription databases. Biol Psychiatry. 2019;86:335–43. https://doi.org/10.1016/j.biopsych.2019.04.009.
Farhat LC, Lannes A, Del Giovane C, Parlatini V, Garcia-Argibay M, Ostinelli EG, et al. Comparative cardiovascular safety of medications for attention-deficit hyperactivity disorder in children, adolescents, and adults: a systematic review and network meta-analysis. Lancet Psychiatry. 2025;12:355–65. https://doi.org/10.1016/S2215-0366(25)00062-8.
Gajria K, Lu M, Sikirica V, Greven P, Zhong Y, Qin P, et al. Adherence, persistence, and medication discontinuation in patients with attention-deficit/hyperactivity disorder - a systematic literature review. Neuropsychiatric Dis Treat. 2014;10:1543–69. https://doi.org/10.2147/NDT.S65721.
Khan MU, Aslani P. A review of factors influencing the three phases of medication adherence in people with attention-deficit/hyperactivity disorder. J Child Adolesc Psychopharmacol. 2019;29:398–418. https://doi.org/10.1089/cap.2018.0153.
Brikell I, Yao H, Li L, Astrup A, Gao L, Gillies MB, et al. ADHD medication discontinuation and persistence across the lifespan: a retrospective observational study using population-based databases. Lancet Psychiatry. 2024;11:16–26. https://doi.org/10.1016/s2215-0366(23)00332-2.
Biederman J, Fried R, DiSalvo M, Storch B, Pulli A, Woodworth KY, et al. Evidence of low adherence to stimulant medication among children and youths with adhd: an electronic health records study. Psychiatr Services, appips. 2019;70:874–80. https://doi.org/10.1176/appi.ps.201800515.
Biederman J, Fried R, DiSalvo M, Woodworth KY, Biederman I, Driscoll H, et al. Further evidence of low adherence to stimulant treatment in adult ADHD: an electronic medical record study examining timely renewal of a stimulant prescription. Psychopharmacology. 2020;237:2835–43. https://doi.org/10.1007/s00213-020-05576-y.
Koch E, Pardiñas AF, O’Connell KS, Selvaggi P, Camacho Collados J, Babic A, et al. How real-world data can facilitate the development of precision medicine treatment in psychiatry. Biol Psychiatry. 2024;96:543–51. https://doi.org/10.1016/j.biopsych.2024.01.001.
Myer NM, Boland JR, Faraone SV. Pharmacogenetics predictors of methylphenidate efficacy in childhood ADHD. Mol Psychiatry. 2018;23:1–8. https://doi.org/10.1038/mp.2017.234.
Yuan D, Zhang M, Huang Y, Wang X, Jiao J, Huang Y. Noradrenergic genes polymorphisms and response to methylphenidate in children with ADHD: a systematic review and meta-analysis. Medicine. 2021;100:e27858. https://doi.org/10.1097/md.0000000000027858.
Mick E, Neale B, Middleton FA, McGough JJ, Faraone SV. Genome-wide association study of response to methylphenidate in 187 children with attention-deficit/hyperactivity disorder. Am J Med Genet B Neuropsychiatr Genet. 2008;147:1412–8. https://doi.org/10.1002/ajmg.b.30865.
Pagerols M, Richarte V, Sánchez-Mora C, Rovira P, Soler Artigas M, Garcia-Martínez I, et al. Integrative genomic analysis of methylphenidate response in attention-deficit/hyperactivity disorder. Sci Rep. 2018;8:1881. https://doi.org/10.1038/s41598-018-20194-7.
Mick E, McGough JJ, Middleton FA, Neale B, Faraone SV. Genome-wide association study of blood pressure response to methylphenidate treatment of attention-deficit/hyperactivity disorder. Prog Neuro-psychopharmacol Biol Psychiatry. 2011;35:466–72. https://doi.org/10.1016/j.pnpbp.2010.11.037.
Brikell I, Wimberley T, Albinana C, Pedersen EM, Vilhjalmsson BJ, Agerbo E, et al. Genetic, clinical, and sociodemographic factors associated with stimulant treatment outcomes in ADHD. Am J psychiatry. 2021;178:854–64. https://doi.org/10.1176/appi.ajp.2020.20121686.
Bybjerg-Grauholm J, Pedersen CB, Bækvad-Hansen M, Pedersen MG, Adamsen D, Hansen CS et al. The iPSYCH2015 Case-Cohort sample: updated directions for unravelling genetic and environmental architectures of severe mental disorders. medRxiv 2020.2011.2030.20237768 [Preprint]. 2020. Available from: https://www.medrxiv.org/content/10.1101/2020.11.30.20237768v1.
Pedersen CB, Bybjerg-Grauholm J, Pedersen MG, Grove J, Agerbo E, Bækvad-Hansen M, et al. The iPSYCH2012 case–cohort sample: new directions for unravelling genetic and environmental architectures of severe mental disorders. Mol Psychiatry. 2018;23:6–14. https://doi.org/10.1038/mp.2017.196.
Demontis D, Walters GB, Athanasiadis G, Walters R, Therrien K, Nielsen TT, et al. Genome-wide analyses of ADHD identify 27 risk loci, refine the genetic architecture and implicate several cognitive domains. Nat Genet. 2023;55:198–208. https://doi.org/10.1038/s41588-022-01285-8.
Satterstrom FK, Walters RK, Singh T, Wigdor EM, Lescai F, Demontis D, et al. Autism spectrum disorder and attention deficit hyperactivity disorder have a similar burden of rare protein-truncating variants. Nat Neurosci. 2019;22:1961–5. https://doi.org/10.1038/s41593-019-0527-8.
Rajagopal VM, Duan J, Vilar-Ribó L, Grove J, Zayats T, Ramos-Quiroga JA, et al. Differences in the genetic architecture of common and rare variants in childhood, persistent and late-diagnosed attention-deficit hyperactivity disorder. Nat Genet. 2022;54:1117–24. https://doi.org/10.1038/s41588-022-01143-7.
Zhou Y, Arribas GH, Turku A, Jürgenson T, Mkrtchian S, Krebs K, et al. Rare genetic variability in human drug target genes modulates drug response and can guide precision medicine. Sci Adv. 2021;7:eabi6856. https://doi.org/10.1126/sciadv.abi6856.
Mors O, Perto GP, Mortensen PB. The danish psychiatric central research register. Scand J public health. 2011;39:54–57. https://doi.org/10.1177/1403494810395825.
Pottegård A, Schmidt SAJ, Wallach-Kildemoes H, Sørensen HT, Hallas J, Schmidt M. Data resource profile: the danish national prescription registry. Int J Epidemiol. 2017;46:798–798f.
Privé F, Aschard H, Ziyatdinov A, Blum MGB. Efficient analysis of large-scale genome-wide data with two R packages: bigstatsr and bigsnpr. Bioinformatics. 2018;34:2781–7. https://doi.org/10.1093/bioinformatics/bty185.
Chang CC, Chow CC, Tellier LC, Vattikuti S, Purcell SM, Lee JJ. Second-generation PLINK: rising to the challenge of larger and richer datasets. Gigascience. 2015;4:7. https://doi.org/10.1186/s13742-015-0047-8.
Yang J, Lee SH, Goddard ME, Visscher PM. GCTA: a tool for genome-wide complex trait analysis. Am J Hum Genet. 2011;88:76–82. https://doi.org/10.1016/j.ajhg.2010.11.011.
Albiñana C, Grove J, McGrath JJ, Agerbo E, Wray NR, Bulik CM, et al. Leveraging both individual-level genetic data and GWAS summary statistics increases polygenic prediction. Am J Hum Genet. 2021;108:1001–11. https://doi.org/10.1016/j.ajhg.2021.04.014.
Albiñana C, Zhu Z, Schork AJ, Ingason A, Aschard H, Brikell I, et al. Multi-PGS enhances polygenic prediction by combining 937 polygenic scores. Nat Commun. 2023;14:4702. https://doi.org/10.1038/s41467-023-40330-w.
Anckarsater H, Lundstrom S, Kollberg L, Kerekes N, Palm C, Carlstrom E, et al. The Child and Adolescent Twin Study in Sweden (CATSS). Twin Res Hum Genet. 2011;14:495–508.
Li QS, Tian C, Hinds D, Agee M, Alipanahi B, Auton A, et al. Genome-wide association studies of antidepressant class response and treatment-resistant depression. Transl Psychiatry. 2020;10:360. https://doi.org/10.1038/s41398-020-01035-6.
Pagnier M. Predicting the response of children and adolescents with ADHD to methylphenidate: a systematic review. J Atten Disord. 2023;27:1377–92. https://doi.org/10.1177/10870547231177234.
Robbins, L & Maides, J Efficacy of stimulants in migraineurs with comorbidities. Practical Pain Manag 2009;9.
Zhang L, Yao H, Li L, Du Rietz E, Andell P, Garcia-Argibay M, et al. Risk of cardiovascular diseases associated with medications used in attention-deficit/hyperactivity disorder: a systematic review and meta-analysis. JAMA Netw Open. 2022;5:e2243597–e2243597. https://doi.org/10.1001/jamanetworkopen.2022.43597.
Green A, Baroud E, DiSalvo M, Faraone SV, Biederman J. Examining the impact of ADHD polygenic risk scores on ADHD and associated outcomes: a systematic review and meta-analysis. J Psychiatr Res. 2022;155:49–67. https://doi.org/10.1016/j.jpsychires.2022.07.032.
Acknowledgements
This project has received funding from the European Union’s Horizon 2020 research and innovation program under grant agreement No 965381 (TIMESPAN). This research reflects only the authors’ view, and the European Commission is not responsible for any use that may be made of the information it contains. Ditte Demontis was supported by the Novo Nordisk Foundation (NNF20OC0065561, NNF21SA0072102, NNF23OC0083657), the Lundbeck Foundation (R344-2020-1060). The iPSYCH team was supported by grants from the ISCIII Lundbeck Foundation (R102-A9118, R155-2014-1724, and co-funded R248-2017-2003), NIH/NIMH (1R01MH124851-01 to Anders D. Børglum), and the Universities and University Hospitals of Aarhus and Copenhagen. The Danish National Biobank resource was supported by the Novo Nordisk Foundation. High-performance computer capacity for handling and statistical analysis of iPSYCH data on the GenomeDK HPC facility was provided by the Center for Genomics and Personalized Medicine and the Centre for Integrative Sequencing, iSEQ, Aarhus University, Denmark (grant to Anders D. Børglum). Søren Dalsgaard was supported by Sawmill-owner Jeppe Juhl’s and wife Ovita Juhl’s Fund, The Capital Region (grant No 22042850), and Greater Copenhagen Health Science Partners (CAG Precision Psychiatry, A7763). Marta Soler Artigas acknowledges a Miguel Servet contract (CP22/00128) awarded by the Instituto de Salud Carlos III and co-funded by the European Union Found: Fondo Social Europeo Plus, FSE + . We acknowledge The Swedish Twin Registry for access to data. The Swedish Twin Registry is managed by Karolinska Institutet and receives funding through the Swedish Research Council under the grant no 2021-00180.
Funding
ADB, DD. Critical revisions of the manuscript and final approval of the version to be published: all authors.
Author information
Authors and Affiliations
Contributions
Conception and study design: DD, IB. Statistical analysis: JPT, IB, JD. Data collection, acquisition and interpretation: JPT, DD, IB, MR, MSA, CA, SD, SVF, TW, JBG, EA, HY, ZC. Manuscript draft: JPT, IB, DD.
Corresponding author
Ethics declarations
Competing interests
Ditte Demontis has received speaker fee from Medice Nordic and Takeda. Anders D. Børglum has received speaker fee from Lundbeck. Zheng Chang has received speaker fees from Takeda Pharmaceuticals. In the past year, Stephen Faraone received income, potential income, travel expenses continuing education support and/or research support from Aardvark, Aardwolf, Otsuka, Collegium, Corium, Supernus, and Mentavi. With his institution, he has US patent US20130217707 A1 for the use of sodium-hydrogen exchange inhibitors in the treatment of ADHD. He receives royalties from books published by Guilford Press: Straight Talk about Your Child’s Mental Health, Oxford University Press: Schizophrenia: The Facts and Elsevier: ADHD: Non-Pharmacologic Interventions. All other authors report no biomedical financial interests or potential conflicts of interest.
Ethics approval
iPSYCH was approved by the Danish Scientific Ethics Committee, the Danish Health Data Authority, the Danish Data Protection Agency, and Danish Newborn Screening Biobank Steering Committee. In accordance with Danish legislation, the Danish Scientific Ethics Committee has waived the need for informed consent in biomedical research based on existing biobanks. All data were de-identified and not recognizable at an individual level. This study did not involve lived experience. iPSYCH was approved by the Ethics Committee initially in 2012, with subsequent amendments in 2013, 2015, and 2018. More details can be found at URL: https://ipsych.dk/en/data-security/health-research-and-ethical-approval. New Danish legislation (effective from January 2024) introduces the possibility for participants to opt out of studies that are exempt from active informed consent. After consulting with the Ethics Committees and patient organizations, iPSYCH contacted all participants in the iPSYCH cohort in June 2025 and offered the possibility to opt out of new genetic studies initiated henceforth. Overall, 1.8% of the iPSYCH participants chose to opt out, and their data will be deleted from the active research database. Data included in finalized and ongoing studies will not be removed.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Thirstrup, J.P., Duan, J., Ribases Haro, M. et al. Common and rare variant contributions to discontinuation of stimulant treatment in ADHD. Transl Psychiatry 16, 144 (2026). https://doi.org/10.1038/s41398-026-03925-7
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41398-026-03925-7