Abstract
Cathepsin C (CatC) is an enzyme which regulates the maturation of neutrophil serine proteases (NSPs) essential for neutrophil activation. Activated neutrophils are key players in the innate immune system, and are also implicated in the etiology of various inflammatory diseases. This study aims to demonstrate a therapeutic potential for CatC inhibitors against disorders in which activated neutrophil-derived neutrophil extracellular traps (NETs) play a significant role. We demonstrate that a CatC inhibitor, MOD06051, dose-dependently suppresses the cellular activity of NSPs, including neutrophil elastase (NE), in vitro. Neutrophils derived from MOD06051-administered rats exhibit significantly lower NE activity and NET-forming ability than controls. Furthermore, MOD06051 dose-dependently ameliorates vasculitis and significantly decreases NETs when administered to a rat model of myeloperoxidase (MPO)-antineutrophil cytoplasmic antibody-associated vasculitis (AAV). These findings suggest that CatC inhibition is a promising strategy to reduce neutrophil activation and improve activated neutrophil-mediated diseases such as MPO-AAV.
Similar content being viewed by others
Introduction
Neutrophils are the most abundant leukocytes in human peripheral blood and are activated in response to a variety of conditions. Activated neutrophils play key roles in many physiological and pathological events, including the innate immune response, wound healing, and inflammation1. Neutrophil serine proteases (NSPs) such as neutrophil elastase (NE) and proteinase 3 (PR3) are granule-associated proteases primarily known for their role in the intracellular killing of pathogens2. NSPs are also involved in neutrophil activation and regulate inflammatory responses through interactions with diverse molecules, including cytokines, chemokines, and growth factors. Cathepsin C (CatC) functions as a key enzyme in the maturation of NSPs and converts the inactive forms to the active forms by digesting dipeptides at the N-terminus during neutrophil differentiation in bone marrow3.
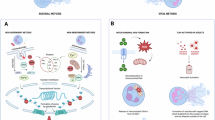
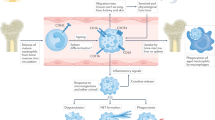
To accomplish these diverse physiological and pathological missions, activated neutrophils release biologically active substances, including NSPs, cytokines, chemokines, reactive oxygen species (ROS), and neutrophil extracellular traps (NETs). Among these, NETs have attracted recent attention due to their conflicting host defense and pathogenic properties4. NETs are a mixture of DNA and bactericidal proteins, such as myeloperoxidase (MPO) and NE, and are secreted into the extracellular space in response to infection with certain types of pathogens. NETs have been recognized as another antimicrobial weapon that neutrophils employ, in addition to the engulfment and digestion of pathogens in the phagosome5. Although NETs can trap and eliminate pathogens, excess formation of NETs has adverse aspects, including cytotoxicity6, autoantigenicity7, and thrombogenicity8.
The NET formation depends on the production of ROS during the activation of NADPH oxidase via the protein kinase C (PKC) and Raf-MEK-ERK signaling pathways9. ROS translocates peptidylarginine deiminase 4 (PAD4) from the cytoplasm to the nucleus10. In the nucleus, PAD4 citrullinates the arginine residue of histone H3 and alters its molecular conformation, resulting in the detachment of DNA that coils around histones11,12. In addition, azurophilic granules release MPO and NSPs, including NE, into the cytoplasm, which are then moved to the nucleus in a ROS-dependent manner13. In the nucleus, NE synergizes with MPO and cleaves histones to promote DNA unraveling14. Eventually, the unraveled DNA breaks through the nuclear membrane, followed by mixing with cytoplasmic antimicrobial substances. NE also cleaves gasdermin D to generate its active form, making pores in the plasma membrane15. Finally, the unraveled DNA fiber intertwined with antimicrobial substances emerges from the plasma membrane into the extracellular space16.
The excess formation of NETs has been implicated in a wide variety of human disease conditions; the pathogenesis of sepsis, autoinflammatory diseases such as gout, metabolic diseases such as diabetes, and autoimmune diseases such as systemic lupus erythematosus (SLE), rheumatoid arthritis (RA), and antineutrophil cytoplasmic antibody (ANCA)-associated vasculitis (AAV)4. Suppressing NET formation is expected to decrease the severity of these and other NET-associated diseases thus, could be a promising strategy to ameliorate many different types of human disorders.
Several strategies to suppress in vivo NET formation have been considered. The mitochondrial ROS scavenger MitoTEMPO suppresses NET formation and decreases disease severity in lupus-prone mice17. PAD inhibitors such as Cl-amidine also reduce NET formation and suppress the development of murine lupus18 or the production of MPO-ANCA in propylthiouracil-administered mice19. Because NSPs, especially NE, are critically involved in the pathway leading to NET formation, and neutrophils derived from Papillon-Lefevre syndrome (PLS) patients who have null CatC activity cannot release NETs20, targeting CatC to prevent the maturation and activation of NE could be an effective way to suppress NET formation.
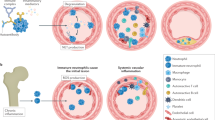
AAV is a systemic small-vessel vasculitis characterized by the development of necrotizing and crescentic glomerulonephritis (NCGN)21, with a subtype, MPO-AAV, developing pulmonary hemorrhage due to alveolar septal capillaritis. Activated neutrophils and NETs are critically involved in AAV pathogenesis22,23. ANCA is a pathogenic autoantibody that can activate neutrophils, which have expressed ANCA antigens on the plasma membrane upon priming24. Although the pathway whereby ANCA activates neutrophils has not been completely elucidated, common molecules, such as ROS and PAD4, are involved in the formation of PKC activator phorbol 12-myristate 13-acetate (PMA)- and ANCA-induced NETs25. It has also been demonstrated that NETs are induced by ANCA via receptor-interacting protein kinase (RIPK) 1/3- and mixed-lineage kinase domain-like (MLKL)-dependent necroptosis22.
Pharmacological inhibition of RIPK1 suppressed NET formation, resulting in improvement of AAV pathology in mice22. More recently, it has been shown that neutrophils derived from PLS patients failed to be activated by ANCA and did not injure vascular endothelial cells, and that pharmacologic CatC inhibition reduced NSPs, ANCA-induced neutrophil activation, and NSP-dependent vascular endothelial damage in cell culture26. Therefore, CatC inhibition could be a potential therapeutic option for AAV.
Here, we show that pharmaceutical inhibition of CatC can reduce the activity of NSPs, including NE and inhibit excess NET formation, thereby decreasing the severity of vasculitis in MPO-AAV, a representative activated neutrophil-mediated disease (Supplementary Fig. 1). Although the concept is based on the evidence obtained in the preceding basic studies, the results of this study demonstrate through in vivo studies the possibility of treating activated neutrophil-mediated diseases with CatC inhibitors, bringing this treatment option one step closer to clinical application.
Results
Inhibition specificity and efficacy of CatC inhibitor MOD06051
Enzymatic activities of cathepsins B, C, D, E, H, K, L, L2, S, and Z were determined using recombinant human enzymes and fluorescent substrates in an appropriate buffer (Supplementary Table 1). MOD06051 inhibited the enzymatic activity of CatC with an IC50 value of 1.5 nM, but not of other cathepsins even at 10 μM, indicating the high specificity of MOD06051 to CatC among cathepsin family enzymes (Table 1). The direct inhibitory effect of MOD06051 on NE was also assessed using recombinant human enzyme and fluorescent substrate (Supplementary Table 1). The results showed no direct inhibitory effect of MOD06051 on NE up to 30 μM. The inhibition of cellular CatC activity by MOD06051 was also confirmed (Supplementary Fig. 2).
Inhibition of cellular NE activity by MOD06051 in vitro and in vivo
Human CD34+ Bone Marrow Stem/Progenitor Cells were cultured in a conditioned medium to differentiate into neutrophils in the presence of 0–10 µM MOD06051. NE activity in in vitro-differentiated neutrophils was suppressed by MOD06051 with an IC50 value of 18 nM (Fig. 1a). To determine the NE inhibitory potential of MOD06051 in vivo, normal rats were administered with MOD06051 (0, 0.3, 1, 3, and 10 mg/kg) orally bis in die (bid) daily for two weeks (n = 5/group). NE activity in polymorphonuclear cells (PMNs) derived from the bone marrow of these rats was suppressed by MOD06051 administration in a dose-dependent manner with an ED50 value of around 0.3 mg/kg bid, and with 3 mg/kg bid reaching trough level (Fig. 1b). Furthermore, NE activity in rat peripheral blood neutrophils was significantly reduced by MOD06051 administration (3 mg/kg bid for two weeks) compared with vehicle controls (Supplementary Fig. 3, p = 0.0322). Since MOD06051 does not possess a direct inhibitory effect against NE, these inhibitions were considered to be caused by disruption of the CatC-mediated NE maturation that occurs during differentiation from bone marrow stem/progenitor cells to neutrophils. To support this hypothesis, we tested CatC activity in rat whole blood, and MOD06051 administration at 0.3 and 3 mg/kg showed 68% and 93% inhibition of CatC activity at two hours post-dosing, respectively (Fig. 1c).
a Human CD34+ Bone Marrow Stem/Progenitor Cells were differentiated into neutrophils in the presence of 0–10 µM MOD06051. NE activity in in vitro-differentiated neutrophils was determined. NE activity was inhibited by MOD06051 with an IC50 value of 18 nM, which was calculated based on repeated biological experiments (N1 and N2). Each experiment was conducted in duplicate. To estimate all NE activity in samples, an excess dose (200 µM) of sivelestat (sv) was used. b Normal rats were administered with MOD06051 (0, 0.3, 1, 3, and 10 mg/kg) orally bid daily (n = 5/group). Two weeks later, NE activity in PMNs derived from the bone marrow was assessed. Results showed an ED50 dose around 0.3 mg/kg bid and that the administration of 3 mg/kg bid reached the trough level. To estimate all specific NE activity in samples, the maximum dose (10 mg/kg) of AZD7986 was used for reference. Values are displayed as the mean with standard error of the mean (SEM), and p-values were calculated using One-way ANOVA followed by Dunnett’s analysis. c Normal rats were administered with MOD06051 (0, 0.3, and 3 mg/kg) orally (n = 5/group). Two hours later, CatC activity in whole blood was assessed using a membrane-permeable CatC-specific fluorescent substrate. Values are displayed as the mean with SEM and p-values were calculated using One-way ANOVA followed by Dunnett’s analysis. d Human CD34+ Bone Marrow Stem/Progenitor Cells were differentiated into neutrophils in the presence of 0–10 µM MOD06051. PR3 activity in in vitro-differentiated neutrophils was determined. PR3 activity was inhibited by MOD06051 with an IC50 value of 29 nM, which was calculated based on repeated biological experiments (N1 and N2). Each experiment was conducted in duplicate. To estimate all NE activity in samples, an excess dose (200 µM) of sivelestat (sv) was used. Cell surface expression of PR3 on in vitro-differentiated neutrophils treated with and without MOD06051 was assessed by FCM. Representative histograms (e) and dose-dependent shift of mean fluorescence intensity (MFI; f) based on four independent experiments are shown. *p < 0.05, **p < 0.01, ****p < 0.0001. Source data are provided as a Source Data file.
Inhibition of cellular PR3 activity and reduction in cell surface expression of PR3 by MOD06051
PR3 activity in neutrophils differentiated from Human CD34+ Bone Marrow Stem/Progenitor Cells was also suppressed by MOD06051 with an IC50 value of 29 nM (Fig. 1d). In addition, surface expression of PR3 on these neutrophils was reduced by MOD06051 in a dose-dependent manner (Fig. 1e, f). These findings reflect the fact that PR3 is translocated from the cytoplasm to the plasma membrane as a result of the CatC-mediated conversion to the active form27 and suggest that MOD06051 could suppress NSPs through a multifaceted mechanism.
Reduced NET formation in neutrophils derived from MOD06051-administered normal rats
To determine whether CatC inhibition would reduce NET formation, normal rats were administered orally bid with MOD06051 (3 mg/kg) or vehicle (0.5% methylcellulose) daily for two weeks (n = 3/group), after which whole blood samples were obtained and neutrophils were extracted for further studies. NET formation was induced in these neutrophils by reacting with immune complexes (IC) formed with MPO and anti-MPO antibody (MPO-ANCA), and the pro-inflammatory cytokine TNF-α or anaphylatoxin C5a was used to prime neutrophils according to a previous report demonstrating that priming of neutrophils enhanced Fcγ receptor-mediated signals28. Extracellular DNA, which is positive with 4’,6-diamidino-2-phenylindole (DAPI), was observed around neutrophils isolated from vehicle-administered rats, after priming with TNF-α or C5a, followed by stimulation with MPO-ANCA-IC (Supplementary Fig. 4a, b, upper). These data were reproduced in neutrophils derived from a non-treated normal rat, and colocalization of citrullinated histone H3 (Cit-H3) and extracellular DNA confirmed that these cells underwent NETosis (Supplementary Fig. 4a, b, lower).
To quantify the level of NET formation objectively, neutrophils stimulated with MPO-ANCA-IC in the chamber after priming were collected by pipetting, and then NET-forming neutrophils were detected by flow cytometry (FCM) using a plasma membrane impermeable DNA-binding dye Sytox Green (Fig. 2a) with slight modification of our previous report29. Compared to vehicle controls, MPO-ANCA-IC-induced NET-forming neutrophils were significantly decreased in both TNF-α-primed and C5a-primed neutrophils derived from MOD06051-administered rats (Fig. 2b, p = 0.0420 in TNF-α-primed neutrophils and p = 0.0084 in C5a-primed neutrophils). As a reference, neutrophils isolated from a non-treated normal rat were stimulated and harvested similarly. Sytox Green histograms in Fig. 2c demonstrated that NET-forming neutrophils were increased by MPO-ANCA-IC stimulation after priming. Although a few cells were Sytox Green-positive in the neutrophils without stimulation and in those primed but without MPO-ANCA-IC stimulation, this may be background staining because MPO-DNA complexes were not detected in the supernatants. MPO-ANCA-IC-induced NET formation in primed neutrophils was confirmed by Cit-H3 labeling results and MPO-DNA complex levels in the supernatants.
Normal rats were administered orally bid with MOD06051 (3 mg/kg) or vehicle (0.5% methylcellulose) daily (n = 3/group). Two weeks later, neutrophils were separated from the blood using Polymorphprep and treated with 100 ng/ml rat TNF-α or 100 ng/ml mouse C5a for 15 min at 37 °C. Thereafter, these cells were incubated in MPO-ANCA-IC-immobilized 4-well slide chambers for 3 h at 37 °C. Cells were collected by pipetting in chambers and resuspended in EDTA-PBS were allowed to react with Sytox Green, and then submitted for FCM to detect Sytox Green+ NET-forming neutrophils. a The representative FCM profiles that reproduced in each group. b Comparison of NET-forming rate in TNF-α-primed neutrophils and C5a-primed neutrophils between MOD06051-administered rats and vehicle controls. Values are displayed as the mean with SEM, and p-values were calculated using a one-sided Student’s t test. c Neutrophils isolated from a non-treated normal rat were stimulated and harvested similarly and then subjected to fluorescent immunostaining for Cit-H3 and FCM using Sytox Green. Moreover, MPO-DNA complexes in supernatants were quantified by ELISA. *p < 0.05, **p < 0.01. Bar, 50 µm. Source data are provided as a Source Data file.
Suppression of NET formation by pharmaceutical inhibition of NE
We hypothesized that the reduction in NET formation in the neutrophils derived from MOD06051-treated rats could be the result of decreased NE activity due to CatC inhibition. To verify this hypothesis, human peripheral blood neutrophils were treated with sivelestat, a NE inhibitor. Neutrophils treated with sivelestat (0, 50, and 500 µM) were primed with TNF-α, followed by stimulation with MPO-ANCA-IC. When TNF-α-primed neutrophils were stimulated with MPO-ANCA-IC, NET formation was verified by colocalization of CD15 (neutrophil marker), Cit-H3 (NETs marker), and extracellular DAPI-positive substances (DNA) (Fig. 3a). DAPI-positive DNA area per neutrophil was reduced by sivelestat dose-dependently and significantly.
Neutrophils were separated from the peripheral blood of healthy volunteers (n = 3) using Polymorphprep and treated with sivelestat (0, 50, and 500 µM) for 15 min, followed by 5 ng/ml TNF-α (a and b) for 15 min at 37 °C. Thereafter, these cells were incubated in MPO-ANCA-IC-immobilized 4-well slide chambers for 3–4 h at 37 °C. After the removal of supernatants and chambers, cells were fixed on the slide by paraformaldehyde and then stained for CD15 (neutrophil marker), Cit-H3 (NETs marker), and DNA (using DAPI) (a). Three microphotographs were taken in a randomized manner per well, and the DAPI-positive DNA area per neutrophil was calculated using ImageJ 1.50i. Alternatively, cells were collected by pipetting in chambers and resuspended in EDTA-PBS, and then analyzed by FCM to examine FSC/SSC profiles (b). In this analysis, swollen neutrophils [R1 gate (whole neutrophils) - R5 gate (normal size neutrophils)] were focused on. Furthermore, the cells were subjected to Cit-H3 immunofluorescent staining, and ELISA was used to quantify MPO-DNA complexes in supernatants. Values are displayed as the mean with SEM, and p-values were calculated using One-way ANOVA followed by Dunnett’s analysis for (a)and (b). Yellow bar, 25 µm; White bar, 50 µm. *p < 0.05, **p < 0.01, ***p < 0.001. Source data are provided as a Source Data file.
To quantify the level of NET formation more objectively, neutrophils primed and subsequently stimulated with MPO-ANCA-IC in the chamber were collected by pipetting and then subjected to FCM. Since neutrophil swelling has been shown to occur prior to NET formation30, we monitored neutrophil size by FCM. MPO-ANCA-IC induced swelling of TNF-α-primed neutrophils, as detected in the forward scatter (FSC)/side scatter (SSC) plot and these cells were also labeled with Cit-H3 (Fig. 3b), thus indicating that the swollen neutrophils were in a state of early NET formation prior to the expulsion of DNA. MPO-ANCA-IC-induced swelling was significantly suppressed by 500 µM sivelestat (p = 0.0359). Sivelestat dose-dependent inhibition of NET formation was also confirmed by the Cit-H3 intensity of neutrophils and the quantification of MPO-DNA complexes in supernatants.
Similar results were obtained when C5a was used as a priming factor instead of TNF-α (Fig. 4a, b). These findings were consistent with the results of the experiments using neutrophils derived from MOD06051-administered rats. Interestingly, avacopan, a C5a receptor (C5aR) antagonist, suppressed MPO-ANCA-IC-induced NET formation only in C5a-primed neutrophils but not in TNF-α-primed neutrophils (Supplementary Fig. 5). These results suggest that avacopan specifically inhibits C5aR-mediated stimulation.
Neutrophils were separated from the peripheral blood of healthy volunteers (n = 3) using Polymorphprep and treated with sivelestat (0, 50, and 500 µM) for 15 min, followed by 100 ng/ml C5a (a and b) for 15 min at 37 °C. Thereafter, these cells were incubated in MPO-ANCA-IC-immobilized 4-well slide chambers for 3–4 h at 37 °C. After the removal of supernatants and chambers, cells were fixed on the slide by paraformaldehyde and then stained for CD15 (neutrophil marker), Cit-H3 (NETs marker), and DNA (using DAPI) (a). Three microphotographs were taken in a randomized manner per well, and the DAPI-positive DNA area per neutrophil was calculated using ImageJ 1.50i. Alternatively, cells were collected by pipetting in chambers and resuspended in EDTA-PBS, and then analyzed by FCM to examine FSC/SSC profiles (b). In this analysis, swollen neutrophils [R1 gate (whole neutrophils) - R5 gate (normal size neutrophils)] were focused on. Furthermore, the cells were subjected to Cit-H3 immunofluorescent staining, and ELISA was used to quantify MPO-DNA complexes in supernatants. Values are displayed as the mean with SEM, and p-values were calculated using One-way ANOVA followed by Dunnett’s analysis for (a) and (b). Yellow bar, 25 µm; White bar, 50 µm. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001. Source data are provided as a Source Data file.
MOD06051 did not affect MPO-ANCA titers
To determine the efficacy of MOD06051 on NET-associated diseases in vivo, we conducted experiments in a rat model of MPO-ANCA-associated vasculitis (MPO-AAV). MPO-AAV was induced in Wistar Kyoto (WKY) rats (4-week-old, male) by subcutaneous immunization of human native MPO according to Little’s protocol31 (Supplementary Fig. 6). These rats were divided into three groups (n = 8/group), and MOD06051 (0.3 or 3 mg/kg) or vehicle (0.5% methylcellulose) was administered orally bid daily for 42 days (Fig. 5a). There was no difference in body weight gain and food intake among the groups throughout the experimental period (Supplementary Fig. 7a, b). Serum MPO-ANCA titer at day 42 was determined by enzyme-linked immunosorbent assay (ELISA). The titer of ANCA in the MPO-AAV rats was significantly higher than that of normal rats (p = 0.0015), and was not decreased by MOD06051 administration (Fig. 5b). This result indicates that MOD06051 does not affect the acquired, at least humoral, immune response in vivo.
a MPO-AAV rats were divided into three groups (n = 8/group), and MOD06051 (0.3 or 3 mg/kg) or vehicle (0.5% methylcellulose) was administered orally bid daily for 42 days. b Serum MPO-ANCA titer at day 42 was determined by ELISA. Normal rats (n = 8) were used as controls. Urine was collected on day 40, and hematuria (c) and proteinuria (d) were detected using dipsticks. Macroscopic foci of pulmonary hemorrhage (e) on the surface of the lungs were counted at necropsy. Microscopic foci of pulmonary hemorrhage (f) with clear regional bleeding were counted in the maximal section of the lung under a low-power field of view. Glomeruli exhibiting NCGN were counted, and the glomerular lesion rate was calculated (g): total glomerular lesion, (h): necrotic glomerular lesion, and (i): crescentic glomerular lesion). The arrowhead in (h) (periodic acid-Schiff (PAS) staining) indicates a necrotic lesion, and the dotted line in (i) (PAS staining) indicates a crescent. Tubular erythrocyte casts in the renal cortex (j), which represented glomerular bleeding, were also counted. Urinary NGAL (k) was measured with the ELISA kit on day 40. Values are displayed as the mean with SEM. P-values were calculated using One-way ANOVA followed by Dunnett’s analysis for (e, f, i, and j)and Kruskal-Wallis followed by Dunn’s analysis for (b–d, g, h, and k). Pathology: vehicle control; Low dose: 0.3 mg/kg, bid; High dose: 3 mg/kg, bid. *p < 0.05, **p < 0.01, ***p < 0.001. Bar, 50 µm. Source data are provided as a Source Data file.
MOD06051 ameliorated MPO-AAV in the model rats
To assess the severity of AAV in the model rats, multiple biomarker and histopathological analyses were performed. Hematuria grade was significantly decreased by high-dose (3 mg/kg, bid) MOD06051 administration compared with vehicle controls (p = 0.0392), with similar trends observed in the low-dose (0.3 mg/kg, bid) group (Fig. 5c). Proteinuria was not prominent in the model used in this study and no clear differences between the groups were observed (Fig. 5d). In vehicle controls, bleeding foci were identified macroscopically on the surface of the lungs and micro-bleeding was observed under the microscope in order to count alveolar hemorrhagic lesions. These lesions showed a dose-dependent decreasing trend with MOD06051 administration, and a significant decrease in microscopic lesions was observed in the high-dose (3 mg/kg) group (Fig. 5e, p = 0.0657 and 5f, p = 0.0305). MOD06051 administration significantly decreased the percentage of affected glomeruli exhibiting NCGN, characterized by tuft necrosis and crescent formation in a dose-dependent manner (Fig. 5g–i and Supplementary Fig. 8a, c, e). Furthermore, tubular erythrocyte cast counts in the renal cortex, which represented glomerular bleeding, and urinary neutrophil gelatinase-associated lipocalin (NGAL), an established biomarker of tubular injury32, were significantly decreased in MPO-AAV rats administered with high-dose (3 mg/kg, bid) MOD06051 compared with vehicle controls (Fig. 5j, p = 0.0028 and Fig. 5k, p = 0.0305), with similar trends observed in the low-dose (0.3 mg/kg, bid) group (Supplementary Fig. 8b, d, f).
MOD06051 reduced NET-forming neutrophils in the peripheral blood and NET deposition in tissues in MPO-AAV rats
NET-forming neutrophils were detected in peripheral blood by FCM using Sytox Green at day 42. The level of NET-forming neutrophils significantly increased in MPO-AAV rats compared with normal controls, but were suppressed to normal levels upon MOD06051 administration (Fig. 6a). NET-forming neutrophils were detected as MPO/Cit-H3/DAPI triple positive substances33 in glomeruli of MPO-AAV rats (Fig. 6b). The rate of NET-forming neutrophils in neutrophils infiltrating into glomeruli was significantly decreased by MOD06051 administration even in the low-dose group (Fig. 6c, p = 0.0001). Parallel findings were obtained concerning NET deposition in renal tubules in the cortex (Supplementary Fig. 9). In contrast, glomerular infiltration of neutrophils was significantly reduced by MOD06051 administration in the high-dose group but not in the low-dose group, although a tendency toward reduction appeared in the low dose group (Fig. 6d). A similar MOD06051 dose-dependent decrease in macrophage infiltration into and around glomeruli was also observed (Fig. 6e).
a NET-forming neutrophils in the blood at day 42 were detected by FCM using Sytox Green (n = 8/group). Normal rats (n = 8) were used as controls. b NET-forming neutrophils were detected as MPO+ Cit-H3+ DAPI+ substances (arrowhead) in glomeruli of MPO-AAV rats. c The rate of NET-forming neutrophils (arrowhead) in neutrophils infiltrating into glomeruli (%) was calculated. d The number of MPO+ neutrophils (arrowheads) infiltrated into 10 glomeruli were counted, and neutrophils per glomerulus (dotted circle) were calculated. e The number of CD68+ macrophages infiltrated into and around glomeruli were counted. Arrowheads indicate macrophages infiltrated into the glomerulus. Extraglomerular macrophage infiltration was scored as follows; 0: none, 1: 1–10, 2: 11–25, 3: 26–50, 4: > 50 macrophages infiltrated around the glomerulus. Values are displayed as the mean with SEM. P-values were calculated using One-way ANOVA followed by Dunnett’s analysis for (c) and Kruskal-Wallis followed by Dunn’s analysis for (a, d, and e). *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001. Bar, 50 µm. Source data are provided as a Source Data file.
Discussion
This study demonstrated that MOD06051, a proprietary CatC inhibitor, showed potent and specific suppression of CatC activity followed by the functional inhibition of downstream NSPs, including NE and PR3, and NET formation both in in vitro experiments using rat and human neutrophils and in vivo experiments using rats.
The formation of excess NETs has been implicated in the pathogenesis of a variety of human diseases, including sepsis, gout, diabetes, SLE, RA, and AAV. Upon disease-initiating stimuli, including exposure to infectious agents and causative environmental factors, neutrophils are primed by pro-inflammatory cytokines such as TNF-α and/or C5a, which are produced by activation of the complement alternative pathway. Primed neutrophils express ANCA antigens on the plasma membrane, to which ANCA binds, resulting in IC formation on the cellular surface. Consequently, neutrophils are excessively activated and produce ROS, followed by the release of NETs. Several research groups have demonstrated efficacy in suppressing NET formation in vivo disease models17,18,19,22, and these strategies, including ROS elimination and PAD inhibition, are considered as promising clinical therapies for NET-associated diseases4. However, as seen in chronic granulomatous disease, a genetic condition resulting in congenital immunodeficiency whereby neutrophils cannot produce ROS34, ROS inhibition could potentially induce immunosuppression. Furthermore, PAD4-deficient mice are more susceptible to bacterial infection than wild-type mice due to their inability to form NETs12. Another approach is therefore necessary to avoid these serious complications.
PLS is a human CatC deficiency35. Although PLS patients showed almost no CatC activity in their tissues and cells, including neutrophils, neutrophils isolated from these patients demonstrated no obvious dysfunction other than reduced NSP activity35. In addition, PLS does not result in an increased incidence of serious infectious diseases, with periodontitis being the main concern for these patients. In CatC-deficient mice, the effector function of NK cells and CD8+ cytotoxic T cells is equivalent to that of wild-type mice36. Thus, the specific inhibition of CatC could be a safer treatment option for NET-associated diseases, avoiding severe immunosuppression while suppressing excess NET formation.
In the present study, MPO-ANCA-IC-induced NET formation was significantly suppressed in neutrophils derived from MOD06051-administered rats regardless of priming stimuli. Similar findings were observed with the NE inhibitor sivelestat when human peripheral blood neutrophils were stimulated by MPO-ANCA-IC. These collective findings suggest that CatC inhibition, which blocks NE maturation and activation, can suppress NET formation as well as NE inhibition. Interestingly, peripheral blood neutrophils derived from patients with PLS have been shown to fail to generate NETs upon stimulation by PMA, another NETs inducer20, further supporting our observation.
The results of this study showed that the specific CatC inhibitor MOD06051 could successfully ameliorate MPO-AAV in a rat model. Since activation and maturation of NSPs occur during neutrophil maturation in the bone marrow, a process that takes weeks, CatC inhibitors would need to be continuously dosed for several weeks to show significant suppression of downstream NSPs and thus efficacy in peripheral neutrophils. This study dosed animals before MPO-AAV symptoms were exhibited; thus, this protocol may be interpreted as prophylactic rather than therapeutic. However, sufficient MPO-ANCA was produced by day 14 in this disease model31, induced tissue injury, and compound treatment resulted in less tissue damage. Therefore, CatC inhibition may be efficacious even after the onset of MPO-AAV. Furthermore, MPO-AAV is a recurring disorder with progressive worsening due to constant microinjuries. Treatment is necessary not only during the exacerbation stage but maintenance therapies are also considered during remission periods. Therefore, the efficacy of MOD06051 in prophylactic treatment in rat MPO-AAV model can still be clinically meaningful. Treatment with CatC inhibitors may stop the continuous cycle, even in the presence of MPO-ANCA. Thus, MOD06051 could be a therapeutic candidate for the treatment of MPO-AAV in humans.
Standard interventions for MPO-AAV include glucocorticoids (GCs) and immunosuppressive drugs such as cyclophosphamide and rituximab37,38,39. The most critical problem with these drugs is secondary immunodeficiency-based opportunistic infections40. In contrast, CatC inhibition suppresses the maturation of NSPs but does not affect other antibacterial proteins such as MPO. In addition, there is no effect on acquired immunity. In fact, even in MPO-AAV rats, the amount of MPO-ANCA produced by human MPO immunization was not reduced by MOD06051. Therefore, CatC inhibition appears to have no significant effect on the humoral immune response in vivo.
Recent studies have demonstrated that avacopan, which inhibits the binding of C5a with C5aR and the resulting priming of neutrophils, is a promising drug for MPO-AAV treatment41,42,43. In this study, avacopan suppressed MPO-ANCA-IC stimulation only in C5a-primed neutrophils but not in TNF-α-primed ones. This finding contrasts with the results demonstrating that MPO-ANCA-IC-induced neutrophil activation was significantly suppressed by MOD06051 regardless of priming stimuli. As a selective antagonist to C5aR, avacopan acts relatively upstream of neutrophil activation in MPO-AAV pathogenesis23, whereas MOD06051 interferes with the activation of NE and acts further downstream compared with avacopan. Therefore, MOD06051 is expected to be effective against diverse priming factors, including TNF-α and C5a, and is considered to possess high versatility for NET suppression. In addition, because the points of action are different, a combination with avacopan could potentially be considered as an MPO-AAV treatment option in the future.
In this study, we demonstrated that the number of NET-forming neutrophils in peripheral blood was quantifiable and correlated with the presence of NET-forming neutrophils in affected glomeruli in MPO-AAV rats. These findings may allow us to use NETs, especially in peripheral blood, as a biomarker to monitor the disease state of NET-related diseases such as MPO-AAV. Further discussion is needed to determine whether decreased NET-forming neutrophils in glomeruli in MOD06051-administered rats are a result of decreased neutrophil infiltration into the kidneys. MPO-AAV rats administered with low-dose MOD06051 showed some level of glomerular neutrophil infiltration, while the rate of NET-forming cells in neutrophils infiltrating into glomeruli was quite low. Since neutrophils derived from PLS patients, who have almost no CatC activity, showed no change or only a faint decrease in various readouts for chemotaxis44, it is not likely that pharmacological CatC inhibitor significantly suppresses chemotaxis of neutrophils in vivo. Although we believe that MOD06051 principally suppresses NET formation and inhibition of neutrophil recruitment was a secondary effect, comprehensive and chronological analyses of inflammatory cells in the kidneys should be conducted in future studies to address this question.
One limitation of this study was the lack of NET induction experiments using in vitro-differentiated neutrophils from CD34+ Bone Marrow Stem/Progenitor Cells. We unsuccessfully attempted to induce NETs in neutrophils differentiated from CD34+ Bone Marrow Stem/Progenitor Cells. Kuhikar et al. reported that NETs can be induced in neutrophils differentiated from CD34+ stem cells in peripheral blood and umbilical cord blood45. Because their neutrophil differentiation protocol is nearly identical to ours, the difference may be attributed to the source of cells; namely, bone marrow or peripheral blood. Further studies are needed to clarify this issue.
Another limitation was the lack of comparison of in vivo efficacy between MOD06051 and other compounds with a different mechanism of action. In particular, a comparison with NE inhibitors would be useful, considering the role of NE in NET formation. While NE inhibitors suppress mature NE activity, specifically in peripheral blood neutrophils, CatC inhibitors inhibit the maturation of not only NE but also other NSPs, such as PR3, in the bone marrow. Interestingly, MOD06051 suppressed enzymatic activity and surface expression of PR3 in neutrophils differentiated from bone marrow stem/progenitor cells. Because cell surface PR3 on dead neutrophils interferes with phagocytosis by macrophages and is involved in the persistence of inflammation46, MOD06051 might suppress disease development in MPO-AAV rats through the increase in macrophage-mediated clearance of dead neutrophils in addition to the suppression of NSPs activity and NET formation.
Other limitations include the low-level destruction of glomeruli and proteinuria in MPO-AAV rats used here, the use of a single animal model, and the small number of rats used. Although we have demonstrated that some neutrophils infiltrating into glomeruli underwent NETosis in MPO-AAV rats, the amount was not very large compared with the findings previously shown in patients with MPO-AAV47,48. Glomerular lesion rate in MPO-AAV rats was up to 16% in this study, and this is consistent with the original paper demonstrating that less than 20% of glomeruli showed glomerulonephritis on average31. We have demonstrated that a few neutrophils underwent NETosis in the glomerulus in MPO-AAV rats, which is equivalent to the MPO-ANCA transfer mouse model22. In this mouse model, approximately 20% of glomeruli showed crescent formation, and few or no neutrophils were positive for phosphorylated MLKL, one of the markers of ANCA-induced NETosis22, in the glomerulus. Although the exact reason why the extent of NET deposition in glomeruli is smaller in murine models than in humans remains unknown, one possible explanation is the difference in the activity of DNase I in serum, which digests NETs49. It has been demonstrated that serum DNase I activity was significantly decreased in patients with MPO-AAV compared with healthy individuals50. In contrast, there is no such evidence in rats and mice. Therefore, the amount of NET deposition in murine MPO-AAV models might be underestimated because NETs could be digested by DNase I in vivo. In this study, proteinuria was checked using dipsticks developed for human urine. Further investigation; e.g., rat albumin quantification, is needed to evaluate proteinuria precisely. In addition, further, larger studies should aim to demonstrate the efficacy of MOD06051 using other NET-associated disease models.
In conclusion, MOD06051 inhibited CatC-mediated NSP activation in rat and human neutrophils, and NE-mediated NET formation and ameliorated MPO-AAV in rats. This suggests that CatC inhibition is a promising therapeutic strategy for many different kinds of activated neutrophil-mediated disorders, including NET-associated diseases.
Methods
Ethics approval
Experiments using rats were permitted by the Animal Experiments Committee of Hokkaido University (permission no. 20-0032) and performed in accordance with the Guidelines for the Care and Use of Laboratory Animals at Hokkaido University. Experiments using human materials were permitted by the Ethics Committee of the Faculty of Health Sciences, Hokkaido University (permission no. 20–40) and performed in accordance with the Declaration of Helsinki. After the acquisition of written informed consent, peripheral blood (10 ml) was drawn from healthy volunteers.
Compound and drugs
Alivexis, Inc. (Tokyo, Japan) developed a CatC inhibitor, MOD06051. It also synthesized and supplied BI-1750, a membrane-permeable CatC-specific substrate. Sivelestat, an NE inhibitor, avacopan, a C5aR inhibitor, and AZD7986, a clinical-stage CatC inhibitor, were purchased from Cayman Chemical (Ann Arbor, MI, USA), Selleck Chemicals (Houston, TX, USA), and Angene International (Nanjing, China), respectively.
Inhibition specificity of MOD06051
Enzymatic activities of cathepsins B, C, D, E, H, K, L, L2, S, Z, and NE were determined using recombinant human enzymes and each fluorescent substrate in an appropriate buffer (Supplementary Table 1). The inhibitory activity of MOD06051 against these enzymes was determined in vitro.
Inhibition of cellular NE activity by MOD06051
Human CD34+ Bone Marrow Stem/Progenitor Cells (Hemacare, Northridge, CA, USA) were cultured in Stem Span SFEM II (Stemcell Technologies, Vancouver, Canada) supplemented with 100 ng/ml SCF (PeproTech, Cranbury, NJ, USA), 10 ng/ml IL-3 (R&D Systems, Minneapolis, MN, USA), and Stemspan CD34+ expansion media (Stemcell Technologies) for the first two weeks with regular medium change every four days. On day 15, cells were centrifuged at 400 × g for 5 min at room temperature (RT) and resuspended in the medium containing 10 ng/ml G-CSF (R&D Systems) and 0–10 µM MOD06051 (2 × 105 cells/well of 96-well plate). Half of the medium was freshly replaced every day. One week later, the cells were transferred onto a 96-well V-bottom plate. After centrifugation of the plate at 540 × g for 5 min at RT, the supernatants were carefully removed. Fifty µl of cold NE lysis buffer was added, and the samples were analyzed by NE activity assay using the NE substrate (MeOSuc-AAPV-AFC; Abcam, Cambridge, UK). To estimate all NE activity in samples, an excess dose (200 µM) of sivelestat was used. For the in vivo study, normal rats were administered MOD06051 (0, 0.3, 1, 3, and 10 mg/kg) orally bid every day (n = 5/group). Two weeks later, PMNs in the bone marrow were recovered and their NE activity was assessed. The 100% of NE activity in the lysed samples was set as the mean activity of vehicle-treated rats, and 0% of activity in the samples was set as the mean activity of 10 mg/kg of AZD7986-treated rats. For the in vivo CatC activity measurement, normal rats were administered MOD06051 (0, 0.3, and 3 mg/kg) orally (n = 5/group). Two hours later, whole blood was collected, and CatC activity was assessed using BI-1750, which is a specific and membrane-permeable substrate for CatC. Collected rat blood was incubated with 4.0 µM of BI-1750 at 25 °C. The 100% CatC activity in the samples was set as the mean activity of vehicle-treated rats, and 0% CatC activity in the samples was determined by adding AZD7986 (final concentration, 30 µM).
Inhibition of cellular PR3 activity and cell surface expression of PR3 by MOD06051
Human CD34+ Bone Marrow Stem/Progenitor Cells were differentiated into neutrophils in the presence of 0–10 µM MOD06051, as aforementioned. One week later, PR3 activity was assessed similarly to NE activity using the PR3 substrate (Abz-Val-Ala-Asp-Nva-Arg-Asp-Arg-Gln-EDDn; Cayman Chemical) instead. To estimate all PR3 activity in samples, an excess dose (200 µM) of sivelestat was used. Although sivelestat is an NE inhibitor, it has been shown to inhibit PR3 activity at a high-dose51. Cell surface expression of PR3 on the in vitro-differentiated neutrophils was detected with FCM using an anti-PR3 antibody (10 µg/ml, clone MCPR3-2; Sigma-Aldrich, St. Louis, MO, USA) and isotype mouse IgG1 (BioLegend, San Diego, CA, USA).
Immobilization of MPO-ANCA-IC on chamber slides
Human native MPO solution (50 µg/ml; Elastin Products, Owensville, MO, USA) was incubated in 4-well slide chambers overnight at 4 °C to immobilize MPO on the slides. After washing with PBS containing 0.05% Tween 20 (PBS-T), the slides were allowed to react with rat anti-human MPO IgG (6.25 µg/ml) or rabbit anti-human MPO antibody (1 µg/ml, ab9535; Abcam) for 1 h at RT. The former was in-house IgG eluted from the serum of rats immunized with human MPO, using a protein G column, and applied to assays with rat neutrophils. The latter was applied to assays with human neutrophils. PBS-T-washed chamber slides were used as MPO-ANCA-IC-immobilized slides.
NET formation inhibitory ability of MOD06051
To determine whether CatC inhibition would reduce NET formation, normal rats were administered orally bid with MOD06051 (3 mg/kg) or vehicle (0.5% methylcellulose) daily (n = 3/group). Two weeks later, neutrophils were separated from the blood using Polymorphprep (Progen, Heidelberg, Germany) and treated with 100 ng/ml rat TNF-α (R&D systems) or 100 ng/ml mouse C5a (R&D systems) for 15 min at 37 °C. Thereafter, these cells were incubated in MPO-ANCA-IC-immobilized 4-well slide chambers (5 × 105/well) at 37 °C. Three hours later, vehicle-administered rat neutrophils were fixed with 4% paraformaldehyde (PFA) for 15 min at RT and mounted with a DAPI-containing mounting solution (Vector Laboratories, Newark, CA, USA). Alternatively, neutrophils isolated from a non-treated normal rat were stimulated similarly and then subjected to fluorescent immunostaining for Cit-H3 using an anti-Cit-H3 antibody (1:100, ab5103; Abcam) after cells were fixed and permeabilized with 0.1% NP-40. Next, vehicle- and MOD06051-administered rat neutrophils, which had been primed with TNF-α or C5a and stimulated with MPO-ANCA-IC, were analyzed by FCM using a plasma membrane impermeable DNA-binding dye Sytox Green (Thermo Fisher Scientific, Waltham, MA, USA). As a reference, neutrophils isolated from a non-treated normal rat were stimulated and harvested similarly and then subjected to FCM using Sytox Green and fluorescent immunostaining for Cit-H3. Moreover, MPO-DNA complexes in supernatants were quantified by ELISA47.
Suppression of MPO-ANCA-IC-induced NET formation by sivelestat and avacopan
Neutrophils were separated from peripheral blood of healthy volunteers (n = 3) using Polymorphprep and treated with the NE inhibitor sivelestat (0, 50, and 500 µM) or the C5aR inhibitor avacopan (0, 0.1, and 1 µM) for 15 min, followed by 5 ng/ml TNF-α (Merck, Darmstadt, Germany) or 100 ng/ml C5a (Merck) for 15 min at 37 °C. Thereafter, these cells were incubated in MPO-ANCA-IC-immobilized 4-well slide chambers (5 × 105/well) for 3–4 h at 37 °C. After removal of supernatants and chambers, cells were fixed on the slide by PFA for 15 min at RT and then stained for CD15 (neutrophil marker) using anti-CD15 antibody (1:100, clone W6D3, BD Biosciences, Franklin Lakes, NJ, USA), Cit-H3 (NETs marker), and DNA (using DAPI). Three microphotographs were taken in a randomized manner per well, and DAPI-positive DNA area per neutrophil was calculated using ImageJ 1.50i (https://imagej.nih.gov/ij/; National Institutes of Health, Bethesda, MD, USA). Alternatively, cells were collected by pipetting in chambers, resuspended in EDTA-PBS, and then analyzed by FCM to examine FSC/SSC profiles. In this analysis, swollen neutrophils [R1 gate (whole neutrophils) - R5 gate (normal size neutrophils)] were focused on. Furthermore, the cells were subjected to Cit-H3 immunofluorescent staining. Cit-H3 intensity per neutrophil was assessed using ImageJ 1.50i. Moreover, MPO-DNA complexes in supernatants were quantified by ELISA.
MPO-AAV rat model
WKY rats (4-week-old, male) were immunized with human native MPO according to Little’s protocol31. In brief, human native MPO (1600 µg/kg) was injected subcutaneously with Freund’s complete adjuvant on day 0, and 800 ng pertussis toxin was injected intraperitoneally on days 0 and 2. The rats were divided into three groups (n = 8/group), and MOD06051 (0.3 or 3 mg/kg) or vehicle (0.5% methylcellulose) was administered orally bid daily for 42 days (from day 0 to day 41). Body weight and food intake were measured every week, and blood was collected by tail cut every 2 weeks. The collected blood was heparinized, and the separated plasma was stored at − 20 °C until analysis. Urine was collected on day 40, and qualitative evaluation of hematuria and proteinuria was performed using a dipstick (Siemens Healthineers, Erlangen, Germany). All rats were euthanized at the end of the study for serological and histological evaluations.
NGAL
Urinary NGAL is a biomarker of acute renal injury32. NGAL was quantified using fresh urine samples and an ELISA kit (Abcam).
MPO-ANCA titer
Serum MPO-ANCA titer was determined using the human MPO-immobilized ELISA plate (Abnova, Taipei, Taiwan) and horseradish peroxidase-conjugated goat anti-rat IgG antibody (Bethyl Laboratories, Montgomery, TX, USA).
Pathological findings
Macroscopic foci of pulmonary hemorrhage on the surface of the lungs were counted at necropsy. Formalin-fixed systemic organs were embedded in paraffin. Four-µm sections of the formalin-fixed and paraffin-embedded (FFPE) tissues were subjected to hematoxylin and eosin staining and periodic acid-Schiff (PAS) staining. Microscopic foci of pulmonary hemorrhage with clear regional bleeding were counted in the maximal section of the lung under a low-power field of view. Glomeruli exhibiting necrotizing and crescentic glomerulonephritis were counted, and the glomerular lesion rate (affected glomeruli/total glomeruli) was calculated. Tubular erythrocyte casts in the renal cortex, which represented glomerular bleeding, were also counted.
NET-forming neutrophils in rat blood
Rat blood collected on day 42 was hemolyzed, and Sytox Green was added. Thereafter, Sytox Green+ NET-forming neutrophils per 2 × 104 cells in the neutrophil gate were calculated by FCM.
Immunofluorescent staining
Frozen or FFPE sections of kidneys were subjected to immunofluorescent staining for NETs. FFPE sections were heated at 121 °C for 20 min with Tris-EDTA (pH 9.0) buffer for antigen retrieval. After masking with Protein Block Serum-free solution (Agilent, Santa Clara, CA, USA), sections were allowed to react with rabbit anti-Cit-H3 antibody (10 μg/ml, ab5103; Abcam) for 60 min at RT. Thereafter, the sections were incubated with Alexa Flour 594-labeled donkey anti-rabbit IgG antibody (4 μg/ml; Abcam) and fluorescein isothiocyanate-conjugated mouse anti-MPO antibody (2 μg/ml, LS-C140180; LSBio, Seattle, WA, USA) for 60 min at RT in the dark. Alternatively, FFPE kidney sections were heated at 121 °C for 20 min with Tris-EDTA (pH 9.0) buffer for antigen retrieval. The sections were masked with Protein Block Serum-free solution and then allowed to react with goat anti-human MPO antibody (2 μg/ml, AF3667; R&D systems) overnight at 4 °C. Thereafter, the sections were incubated with Alexa Flour 488-labeled donkey anti-goat IgG antibody (4 μg/ml; Abcam) for 60 min at RT in the dark. Autofluorescence was suppressed with Vector TrueVIEW (Vector Laboratories). After mounting with a DAPI-containing mounting solution, the sections were observed under a fluorescence microscope. To calculate the percentage of Cit-H3-positive NET-forming cells in neutrophils infiltrating into glomeruli, more than 30 MPO-positive cells infiltrating into glomeruli were counted independently by two investigators, and the mean values were adopted.
Immunohistochemistry
FFPE kidney sections were autoclaved at 121 °C for 20 min with citrate buffer (pH 6.0) to retrieve antigens and exposed to methanol supplemented with 3% H2O2 for 5 min to consume endogenous peroxidase in tissues. After the nonspecific binding of antibodies was blocked by 10% goat serum, the sections were incubated with mouse anti-rat CD68 antibody (1:200, clone ED1; Bio-Rad Laboratories, Tokyo, Japan) for 60 min at RT. After removal of unbound antibodies with PBS, the sections were incubated with horseradish peroxidase (HRP)-conjugated goat anti-mouse IgG antibody (1:100; Seracare, Milford, MA, USA) for 60 min at RT. After the removal of unbound antibodies with PBS, HRP activity was developed with diaminobenzidine.
Statistics
All statistical analysis was performed using GraphPad Prism 10.2 (GraphPad Software, California, USA). One-way ANOVA or Kruskal-Wallis analysis was applied to parametric or non-parametric multiple comparisons among groups. Student’s t test was applied to parametric comparison between two groups. P < 0.05 was considered statistically significant for all statistical analyses.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
All data generated in this study are provided in the Supplementary Information. Source data are provided with this paper.
References
Nemeth, T., Sperandio, M. & Mocsai, A. Neutrophils as emerging therapeutic targets. Nat. Rev. Drug Discov. 19, 253–275 (2020).
Pham, C. T. Neutrophil serine proteases fine-tune the inflammatory response. Int. J. Biochem. Cell Biol. 40, 1317–1333 (2008).
Korkmaz, B. et al. Therapeutic targeting of cathepsin C: from pathophysiology to treatment. Pharm. Ther. 190, 202–236 (2018).
Mutua, V. & Gershwin, L. J. A review of neutrophil extracellular traps (NETs) in disease: potential anti-NETs therapeutics. Clin. Rev. Allergy Immunol. 61, 194–211 (2021).
Brinkmann, V. et al. Neutrophil extracellular traps kill bacteria. Science 303, 1532–1535 (2004).
Kaplan, M. J. & Radic, M. Neutrophil extracellular traps: double-edged swords of innate immunity. J. Immunol. 189, 2689–2695 (2012).
Nakazawa, D. et al. Abnormal conformation and impaired degradation of propylthiouracil-induced neutrophil extracellular traps: implications of disordered neutrophil extracellular traps in a rat model of myeloperoxidase antineutrophil cytoplasmic antibody-associated vasculitis. Arthritis Rheum. 64, 3779–3787 (2012).
Kimball, A. S., Obi, A. T., Diaz, J. A. & Henke, P. K. The emerging role of NETs in venous thrombosis and immunothrombosis. Front. Immunol. 7, 236 (2016).
Hakkim, A. et al. Activation of the Raf-MEK-ERK pathway is required for neutrophil extracellular trap formation. Nat. Chem. Biol. 7, 75–77 (2011).
Castanheira, F. V. S. & Kubes, P. Neutrophils and NETs in modulating acute and chronic inflammation. Blood 133, 2178–2185 (2019).
Wang, Y. et al. Histone hypercitrullination mediates chromatin decondensation and neutrophil extracellular trap formation. J. Cell Biol. 184, 205–213 (2009).
Li, P. et al. PAD4 is essential for antibacterial innate immunity mediated by neutrophil extracellular traps. J. Exp. Med. 207, 1853–1862 (2010).
Metzler, K. D., Goosmann, C., Lubojemska, A., Zychlinsky, A. & Papayannopoulos, V. A myeloperoxidase-containing complex regulates neutrophil elastase release and actin dynamics during NETosis. Cell Rep. 8, 883–896 (2014).
Papayannopoulos, V., Metzler, K. D., Hakkim, A. & Zychlinsky, A. Neutrophil elastase and myeloperoxidase regulate the formation of neutrophil extracellular traps. J. Cell Biol. 191, 677–691 (2010).
Kambara, H. et al. Gasdermin D exerts anti-inflammatory effects by promoting neutrophil death. Cell Rep. 22, 2924–2936 (2018).
Sollberger, G. et al. Gasdermin D plays a vital role in the generation of neutrophil extracellular traps. Sci. Immunol. 3, eaar6689 (2018).
Lood, C. et al. Neutrophil extracellular traps enriched in oxidized mitochondrial DNA are interferogenic and contribute to lupus-like disease. Nat. Med. 22, 146–153 (2016).
Knight, J. S. et al. Peptidylarginine deiminase inhibition disrupts NET formation and protects against kidney, skin and vascular disease in lupus-prone MRL/lpr mice. Ann. Rheum. Dis. 74, 2199–2206 (2015).
Kusunoki, Y. et al. Peptidylarginine deiminase inhibitor suppresses neutrophil extracellular trap formation and MPO-ANCA production. Front. Immunol. 7, 227 (2016).
Sorensen, O. E. et al. Papillon-Lefevre syndrome patient reveals species-dependent requirements for neutrophil defenses. J. Clin. Invest. 124, 4539–4548 (2014).
Jennette, J. C. et al. 2012 revised international chapel hill consensus conference nomenclature of vasculitides. Arthritis Rheum. 65, 1–11 (2013).
Schreiber, A. et al. Necroptosis controls NET generation and mediates complement activation, endothelial damage, and autoimmune vasculitis. Proc. Natl. Acad. Sci. USA 114, E9618–E9625 (2017).
Nakazawa, D., Masuda, S., Tomaru, U. & Ishizu, A. Pathogenesis and therapeutic interventions for ANCA-associated vasculitis. Nat. Rev. Rheumatol. 15, 91–101 (2019).
Kettritz, R., Jennette, J. C. & Falk, R. J. Crosslinking of ANCA-antigens stimulates superoxide release by human neutrophils. J. Am. Soc. Nephrol. 8, 386–394 (1997).
Nakazawa, D. & Kudo, T. Novel therapeutic strategy based on neutrophil subset and its function in autoimmune disease. Front. Pharm. 12, 684886 (2021).
Jerke, U. et al. Targeting cathepsin C in PR3-ANCA vasculitis. J. Am. Soc. Nephrol. 33, 936–947 (2022).
Seren, S. et al. Consequences of cathepsin C inactivation for membrane exposure of proteinase 3, the target antigen in autoimmune vasculitis. J. Biol. Chem. 293, 12415–12428 (2018).
Bournazos, S., Gupta, A. & Ravetch, J. V. The role of IgG Fc receptors in antibody-dependent enhancement. Nat. Rev. Immunol. 20, 633–643 (2020).
Masuda, S. et al. Measurement of NET formation in vitro and in vivo by flow cytometry. Cytom. A 91, 822–829 (2017).
Neubert, E. et al. Chromatin swelling drives neutrophil extracellular trap release. Nat. Commun. 9, 3767 (2018).
Little, M. A. et al. Experimental autoimmune vasculitis: an animal model of anti-neutrophil cytoplasmic autoantibody-associated systemic vasculitis. Am. J. Pathol. 174, 1212–1220 (2009).
Shang, W. & Wang, Z. The update of NGAL in acute kidney injury. Curr. Protein Pept. Sci. 18, 1211–1217 (2017).
Masuda, S. et al. Phorbol 12-myristate 13-acetate stimulation under hypoxia induces nuclear swelling with DNA outflow but not extracellular trap formation of neutrophils. Exp. Mol. Pathol. 125, 104754 (2022).
Yu, H. H., Yang, Y. H. & Chiang, B. L. Chronic granulomatous disease: a comprehensive review. Clin. Rev. Allergy Immunol. 61, 101–113 (2021).
Giannetti, L. et al. Papillon-lefevre syndrome: Oral aspects and treatment. Dermatol. Ther. 33, e13336 (2020).
Andoniou, C. E., Fleming, P., Sutton, V. R., Trapani, J. A. & Degli-Esposti, M. A. Cathepsin C limits acute viral infection independently of NK cell and CD8+ T-cell cytolytic function. Immunol. Cell Biol. 89, 540–548 (2011).
Ntatsaki, E. et al. BSR and BHPR guideline for the management of adults with ANCA-associated vasculitis. Rheumatology 53, 2306–2309 (2014).
Yates, M. et al. EULAR/ERA-EDTA recommendations for the management of ANCA-associated vasculitis. Ann. Rheum. Dis. 75, 1583–1594 (2016).
Harigai, M. et al. 2017 Clinical practice guidelines of the Japan Research Committee of the Ministry of Health, Labour, and Welfare for Intractable Vasculitis for the management of ANCA-associated vasculitis. Mod. Rheumatol. 29, 20–30 (2019).
Flossmann, O. Risks of treatments and long-term outcomes of systemic ANCA-associated vasculitis. Presse Med. 44, e251–e257 (2015).
Jayne, D. R. W. et al. Randomized trial of C5a receptor inhibitor avacopan in ANCA-associated Vasculitis. J. Am. Soc. Nephrol. 28, 2756–2767 (2017).
Jayne, D. R. W., Merkel, P. A., Schall, T. J. & Bekker, P. Avacopan for the treatment of ANCA-associated Vasculitis. N. Engl. J. Med. 384, 599–609 (2021).
Soulsby, W. D. Journal club review of “Avacopan for the treatment of ANCA-associated Vasculitis”. ACR Open Rheumatol. 4, 558–561 (2022).
Roberts, H. et al. Characterization of neutrophil function in Papillon-Lefevre syndrome. J. Leukoc. Biol. 100, 433–444 (2016).
Kuhikar, R. et al. Neutrophils generated in vitro from hematopoietic stem cells isolated from apheresis samples and umbilical cord blood form neutrophil extracellular traps. Stem. Cell Res. 50, 102150 (2021).
Kantari, C. et al. Proteinase 3, the Wegener autoantigen, is externalized during neutrophil apoptosis: evidence for a functional association with phospholipid scramblase 1 and interference with macrophage phagocytosis. Blood 110, 4086–4095 (2007).
Kessenbrock, K. et al. Netting neutrophils in autoimmune small-vessel vasculitis. Nat. Med. 15, 623–625 (2009).
O’Sullivan, K. M. et al. Renal participation of myeloperoxidase in antineutrophil cytoplasmic antibody (ANCA)-associated glomerulonephritis. Kidney Int. 88, 1030–1046 (2015).
Hakkim, A. et al. Impairment of neutrophil extracellular trap degradation is associated with lupus nephritis. Proc. Natl. Acad. Sci. USA 107, 9813–9818 (2010).
Nakazawa, D. et al. Enhanced formation and disordered regulation of NETs in myeloperoxidase-ANCA-associated microscopic polyangiitis. J. Soc. Am. Nephrol. 25, 990–997 (2014).
Hwang, T. L., Wang, W. H., Wang, T. Y., Yu, H. P. & Hsieh, P. W. Synthesis and pharmacological characterization of 2-aminobenzaldehyde oxime analogs as dual inhibitors of neutrophil elastase and proteinase 3. Bioorg. Med. Chem. 23, 1123–1134 (2015).
Acknowledgements
We are grateful to the animal facility staff, Ms. Maiko Ono, Mr. Hisato Suga, and Dr. Noriko Tosa at the Graduate School of Medicine, Hokkaido University, for supporting animal experiments and breeding. We thank R. Thakur, G. Iyappan, S. Lakkavajhala Srivalli and A. Tiwari in Syngene International Ltd. for experimental support. We also thank Ms. Stephanie C. Napier for editing the draft of this manuscript. This work was supported by the Japanese Grant-in-Aid for Scientific Research (no. 21H0295802).
Author information
Authors and Affiliations
Contributions
Y.N., S.A., M.T., I.N., H.O., S.K., Y.H., A.S., R.N., S.M., T.N., and A.I. performed experiments. Y.N., S.A., M.T., R.N., S.M., D.N., U.T., T.S., W.S., T.N., Y.T., and A.I. analyzed the data. T.N., Y.T., and A.I. designed the study. Y.N., S.M., T.N., Y.T., and A.I. wrote the manuscript. All authors read the final version of the manuscript and provided critical feedback.
Corresponding author
Ethics declarations
Competing interests
T.S., W.S., T.N., and Y.T. are employees of Alivexis, Inc. Y.N., S.M., and A.I. were given research funds from Alivexis, Inc. The remaining authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Daniel Appelgren, Kim Maree O’Sullivan, and the other anonymous, reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Nishibata, Y., Arai, S., Taniguchi, M. et al. Cathepsin C inhibition reduces neutrophil serine protease activity and improves activated neutrophil-mediated disorders. Nat Commun 15, 6519 (2024). https://doi.org/10.1038/s41467-024-50747-6
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-024-50747-6
This article is cited by
-
Platelets as drivers of immunothrombosis in rheumatic diseases
Nature Reviews Rheumatology (2025)
-
Neutrophils and NETs in kidney disease
Nature Reviews Nephrology (2025)