Abstract
Pathogenic intracellular bacteria pose a significant threat to global public health due to the barriers presented by host cells hindering the timely detection of hidden bacteria and the effective delivery of therapeutic agents. To address these challenges, we propose a tandem diagnosis-guided treatment paradigm. A supramolecular sensor array is developed for simple, rapid, accurate, and high-throughput identification of intracellular bacteria. This diagnostic approach executes the significant guiding missions of screening a customized host-guest drug delivery system by disclosing the rationale behind the discrimination. We design eight azocalix[4]arenes with differential active targeting, cellular internalization, and hypoxia responsiveness to penetrate cells and interact with bacteria. Loaded with fluorescent indicators, these azocalix[4]arenes form a sensor array capable of discriminating eight intracellular bacterial species without cell lysis or separation. By fingerprinting specimens collected from bacteria-infected mice, the facilitated accurate diagnosis offers valuable guidance for selecting appropriate antibiotics. Moreover, mannose-modified azocalix[4]arene (ManAC4A) is screened as a drug carrier efficiently taken up by macrophages. Doxycycline loaded with ManAC4A exhibits improved efficacy against methicillin-resistant Staphylococcus aureus-infected peritonitis. This study introduces an emerging paradigm to intracellular bacterial diagnosis and treatment, offering broad potential in combating bacterial infectious diseases.
Similar content being viewed by others
Introduction
Bacterial infections have become the second leading cause of death globally, claiming 7.7 million lives in 2019, which pose a grave threat to public health1,2. The cunning bacteria that reside inside cells pose an even greater challenge for humans, proving to be an exceptionally stubborn nuisance. Some infectious bacteria, such as Staphylococcus aureus (SA), Listeria monocytogenes (LM), and Salmonella typhimurium (ST), exhibit a remarkable ability to evade the impact of antibiotics and the killing by immunes cells. They hide within mammalian cells, including the macrophages tasked with eradicating bacteria3,4,5. In this case, macrophages not only fail to eliminate bacteria but also become a source of bacterial multiplication, enabling the spread of bacteria from the initial site of infection and invasion into various non-phagocytic cell types in tissues. Intracellular bacteria are associated with various severe diseases, including sepsis, osteomyelitis, and cancer metastasis6,7,8. Unfortunately, treatment failure and relapse are common9. There are two critical reasons for the poor efficacy of clinical treatments against intracellular bacteria: (1) the inability to quickly and accurately identify the specific type of bacteria hinders timely and precise symptomatic treatment10,11,12, and (2) host cells act as protective sanctuaries for bacteria due to their cell membrane barrier, which lead to poor intracellular accumulation of antibiotics3,9,13. Therefore, these facts may potentially lead to inappropriate and/or excessive antibiotic use, which in turn exacerbates antibiotic resistance of bacteria14. Accurately identifying the type of intracellular bacteria and achieving the diagnosis-guided treatment emerges to be a tandem pathway highly on demand, but still faces formidable challenges.
Hereinto, diagnosis is the prerequisite for ensuring effective treatment. Currently, the conventional methods, including microbial culture15, transmission electron microscopy16, polymerase chain reactions17, immunofluorescence staining18, and matrix-assisted laser desorption ionization time-of-flight mass spectrometry19 are used for detecting intracellular bacteria. Most of them involve lysing the host cells and then detecting the pathogens inside. The status of intracellular bacterial diagnosis is still facing the problems of expensive equipment, complicated operation, reliance on experience, skilled techniques, and time consumption, which cannot satisfy clinical needs for timely and reliable diagnosis of bacterial infections for a large number of patients and may delay the treatment20. In recent years, researchers have been dedicated to developing novel fluorescent probes that can directly visualize intracellular bacteria without the need for cell lysis21,22,23,24,25. For instance, some designed probes can respond to the overexpressed caspase-1 in infected cells, leading to the activation of fluorescence14,26. A nanoprobe modified with dual recognition units for SA, including an aptamer and teicoplanin, has been utilized for the specific detection of intracellular SA24. However, these probes cannot differentiate between bacterial species inside cells and instead focus mainly on determining the presence of an infection. Note: During the peer review process of this manuscript, Rotello et al. reported a sensor array for the discrimination of intracellular bacteria (see ref. 25). Consequently, there is an urgent need to develop a simple, rapid, accurate, and high-throughput approach for identifying intracellular bacterial species.
After gaining a clear understanding of the bacterial species, symptomatic treatment can be administered that guides the selection of antibiotics. However, compared to killing extracellular bacteria, the host cell barrier presents another challenge for antibiotics to reach the pathogen-containing compartments, limiting their efficacy in treating intracellular bacterial infections. The use of drug delivery systems (DDS) holds great potential in overcoming drug transport barriers and enhancing the accumulation of antibiotics, leading to more effective treatment of intracellular bacterial infections27,28,29,30. For instance, through the modification of host cell-targeting ligands (e.g., carbohydrates and hyaluronic acid)31,32,33,34,35, and the introduction of moieties capable of responding to microenvironmental stimuli (e.g., pH, enzymes, and reactive oxygen species)36,37,38, some cleverly designed DDSs have been developed. However, these existing studies on anti-intracellular bacterial DDS are based on the premise that the type of infected bacteria is known, neglecting the potentially valuable information provided by the crucial diagnostic step. With regard to diagnosis-guided treatment, the other significant mission for diagnosis is to guide the screening of a customized DDS, in addition to guiding the screening of antibiotics.
To achieve the above-mentioned goals of diagnosis-guided therapy, differential sensing appears to be a promising approach. Sensor arrays, also known as the chemical nose, characterized by their cross-reactivity, encompass multiple non-specific receptors that interact with the analytes. They generate pattern fingerprints for each analyte, which are then classified using mathematical algorithms. This distinctive feature makes them well-suited for rapid analysis of complex systems, even for distinguishing analytes or analyte mixtures that have not been exhaustively characterized39. Supramolecular system offers a powerful avenue for constructing the sensor array. Its inherently dynamic and reversible nature enables easy construction of sensor units that can generate information-rich patterns, thereby enhancing discriminative capabilities40,41.
In this work, we propose a tandem pathway to combat against intracellular bacteria by establishing a supramolecular sensor array for discriminating intracellular bacteria, which in turn provides valuable guidance for screening a host-guest DDS to carry the assigned antibiotic (Fig. 1). Three classes of azocalix[4]arenes with different upper rim modifications incorporating carbohydrate, amino acid, and negatively charged groups, are designed to differentially interact with infected cells and respond to the hypoxic microenvironment induced by bacterial infection. These azocalix[4]arenes encapsulate the fluorescent indicator to form the supramolecular sensor array, which perceives the phenotypic changes in infected cells through a series of mechanisms including thermodynamic and kinetic factors, enabling the accurate discrimination of intracellular bacteria simply and rapidly. The successful identification of blind intracellular bacteria guides the selection of antibiotics. Moreover, by disclosing the rationale behind the discrimination, we screen a host-guest DDS, mannose-modified azocalix[4]arene (ManAC4A), that achieves the precise delivery of the employed antibiotic, doxycycline (Dox). The active targeting of the mannose group to macrophages and the hypoxia-responsiveness of the azo group enhance the antibacterial efficacy of this DDS against methicillin-resistant SA (MRSA)-infected peritonitis. This supramolecular sensor array and host-guest DDS hold great promise in combating intracellular bacterial infections under the guidance of accurate diagnosis.
Initially, a supramolecular sensor array based on azocalix[4]arene receptors is employed for discriminating intracellular bacteria. Subsequently, the sensor array diagnoses peritoneal fluid samples from mice as MRSA infection, guiding the selection of the antibiotic Dox. By analyzing the sensing rationale, ManAC4A is chosen as the drug carrier due to its optimal cellular uptake. The active targeting system Dox@ManAC4A is then used for the treatment of MRSA-infected peritonitis. The azo groups respond quickly under hypoxic conditions, which leads to the controlled release of Dox for bacterial infections.
Results
The design of the supramolecular sensor array
Differential sensing requires multiple sensor units that exhibit variable responses to the target analytes, in this case, intracellular bacteria. To design and construct the effective sensor array, several processes may be taken into consideration, including the interactions between the recognition receptors and the cells or bacteria, the uptake of the sensor units by the cells or bacteria, as well as the transduction of the response into the monitorable signal. Due to their broad-spectrum encapsulation feature, macrocyclic receptors are remarkably adaptable for differential sensing based on pattern recognition39,42. Calixarenes, as a family of highly modifiable macrocyclic receptors, offer a wide range of chemical design spaces, enabling the construction of diverse cross-reactive sensor units41,43. Moreover, the unique property of complexation-induced quenching of fluorescent indicators exhibited by calixarenes empowers the sensor array to generate a prominent fluorescent turn-on signal in response to intracellular bacteria. Our group has synthesized a series of azocalix[n]arenes in recent years44,45. The azo-coupling reaction on calixarenes provides a powerful and facile approach for synthesizing azocalix[n]arenes. These azocalix[n]arenes with deepened cavities exhibit much-improved recognition ability than conventional calixarenes and may be able to recognize a greater variety of guest molecules in this complex system45,46. In addition, the azo groups can be reduced by azoreductase under the intracellular bacterial infection-induced hypoxic microenvironment, converting them into aminocalixarenes47,48. The decrease in binding affinities of indicators before and after the reduction leads to indicator release, which is expected to add another pathway to the transduction of output signals. Therefore, three classes of azocalix[4]arenes with different upper edge modifications are tailored specifically for the discrimination of intracellular bacteria (Fig. 2a). The first type is carbohydrate-modified azocalix[4]arenes. The mannose receptor, galactose receptor, and β-glucan receptor expressed by macrophages49,50,51,52, along with lectins, toxins, and adhesins present on bacteria53,54, can recognize carbohydrates. The second type is amino acid-modified azocalix[4]arenes. Macrophages coordinate the expression of amino acid transporters after being infected with bacteria, which in turn affects their uptake of amino acids55. The third type is carboxyl- and sulfonate-modified azocalix[4]arenes, which do not carry active targeting groups but may provide additional information for array-based sensing complementary to the first two types. Thus, these azocalix[4]arenes are chosen as recognition receptors, because they approach macrophages and bacteria to different extents, which lays the foundation for differential sensing.
a Chemical structures of the employed azocalix[4]arenes and fluorescent indicator. b Fluorescence response patterns of the sensor array against various intracellular bacteria and the blank macrophage. Data are presented as mean ± SD, n = 5 biological replicates. c Canonical score plot for the two factors of simplified fluorescence response patterns obtained from LDA with 90% confidence ellipses, n = 5 biological replicates. d Canonical score plot for the mixtures of intracellular SA and LM with 90% confidence ellipses, n = 5 biological replicates. e Canonical score plot for intracellular bacteria from peritoneal fluid samples with 90% confidence ellipses, n = 5 biological replicates. Source data are provided as a Source Data file.
Six azocalix[4]arenes, including ManAC4A (1), LacAC4A (2), GalAC4A (3), GluAC4A (4), CAC4A (5), and SAC4A (6), were synthesized and purified according to the literature procedures (Supplementary Figs. 1−12)44,56,57,58,59. The other two new macrocyclic compounds, LysAC4A (7) and SerAC4A (8), were prepared for providing probably differential signal outputs (Supplementary Figs. 13−20). Taking the synthesis of LysAC4A as an example, CAC4A was activated by 1-(3-dimethylaminopropyl)-3-ethylcarbodiimide hydrochloride and n-hydroxysuccinimide (NHS) to form an unstable active intermediate CAC4A-NHS, which was further condensed with n-epsilon-boc-lysine to obtain amino-protected lysine modified azocalix[4]arenes (Boc-LysAC4A). Finally, LysAC4A was obtained by deprotection of the t-butyloxy carbonyl group. Similar synthetic routes produce SerAC4A, as shown in the Methods section. Among them, ManAC4A58, LacAC4A56, GalAC4A56, GluAC4A59, LysAC4A, SerAC4A, and CAC4A spontaneously self-assemble into nanoparticles with diameters ranging from 25 to 131 nm (Supplementary Fig. 21), while SAC4A does not60. Indicator displacement assay (IDA) responses were demonstrated to occur in both single molecules and assemblies (Supplementary Fig. 22). For signal transduction, azocalix[4]arenes complex with the indicator, 1,1′,3,3,3′,3′-hexamethylindodicarbocyanine (CY5), and quench its fluorescence (Supplementary Fig. 23). The dynamic light scattering (DLS) results indicate that the original assembly structure of azocalix[4]arenes was not disrupted after complexation with the indicator CY5 (Supplementary Fig. 24). The formed host-guest sensor units may undergo fluorescence recovery through competitive complexation with the analytes. Besides, the azo bond reduction under hypoxic environments also leads to the release of CY5, resulting in fluorescence turn-on to varying degrees.
The discrimination of intracellular bacteria for model samples
Eight bacteria, including SA, MRSA, LM, ST, Escherichia coli (EC), Pseudomonas aeruginosa (PA), Klebsiella pneumoniae (KP), and Streptococcus mutans (SM), were selected as target intracellular pathogens for proof of concept. Among them, SA, MRSA, LM, ST, EC, PA, and KP have been known to possess the ability to invade and reside inside host cells61,62,63,64,65,66,67. SM was included as the analyte to mimic bacterial phagocytosis by macrophages68. Eight reporter pairs consisting of azocalix[4]arenes with the indicator CY5 were co-incubated with infected and blank macrophages. The fluorescence intensity was measured using a microplate reader accessory attached to a fluorescence spectrometer (Supplementary Table 1). As depicted in Fig. 2b, each sensor unit exhibited distinct levels of fluorescence intensity corresponding to specific intracellular bacteria present. This demonstrates the possibility of the sensor array for identifying different types of intracellular bacteria. To test the capabilities of the constructed sensor array, the fluorescence response patterns of intracellular bacteria generated by the sensor array were analyzed using linear discriminant analysis (LDA), a powerful statistical method widely used for pattern recognition69. The eight bacteria-infected macrophages and macrophages alone are well clustered into nine groups that are fully distinguished from each other (Fig. 2c). Cross-validation by the leave-one-out method in LDA achieved and demonstrated 100% discrimination accuracy, proving that our constructed sensor array is very effective in identifying both the presence and species of intracellular bacteria (Supplementary Table 2).
Clinical diagnosis is often faced with mixed pathogen samples70,71. Therefore, we conducted additional discrimination experiments using a mixture of SA- and LM-infected macrophages, both of which can be transmitted to humans through food, causing severe intracellular bacterial infections72. Mixtures of different proportions were well classified on the LDA plot (Fig. 2d and Supplementary Table 3). We also explored the feasibility of the supramolecular sensor array for the quantitative analysis of intracellular bacteria. The results indicate that different concentrations of SA and LM (OD600 = 1.0, 0.5, 0.2, and 0.1) are effectively separated in their LDA score plots (Supplementary Table 4 and Supplementary Fig. 25a and b). Furthermore, as shown in Supplementary Fig. 25c and d, the two major categories covering different concentrations of SA and LM could also be distinguished through both LDA and principal component analysis (PCA).
We challenged the azocalix[4]arene-based sensor array for discriminating intracellular bacteria with peritoneal fluid samples from mice. MRSA, EC, and PA were injected intraperitoneally into mice to cause infection. The macrophages in the peritoneal cavity were extracted by injecting phosphate-buffered saline (PBS) the next day. The proposed sensor array was applied to the extracted infected cell samples (Supplementary Table 5). The LDA patterns of three kinds of bacteria-infected cells and the cells from healthy mice were obtained as shown in Fig. 2e. These clusters representing different analytes were significantly distinguished. After establishing a standard profile of intracellular bacteria for peritoneal fluid samples from mice, further validation of the practical application capability of this array in diagnosing intracellular bacterial infections was conducted through blind tests. As Supplementary Table 6 illustrates, three blind intracellular bacteria samples from mice were tested and correctly identified as MRSA. This preliminarily proves the potential of the supramolecular sensor array for practical diagnostic applications.
The analysis of the rationale behind the discrimination
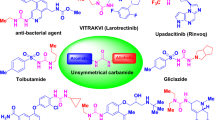
While the sensor array functions as a black box, our objective is to unravel the underlying rationale behind its successful differentiation, aiming to offer valuable insights and guidance for future sensor array design and construction. We speculate that the following three processes are involved in generating differential signals. (1) The quenched fluorescence of CY5@azocalix[4]arene reporter pairs can be illuminated by competing guests on the cell surface through IDA43,73. (2) Bacteria-infected macrophages exhibit varying capacities to uptake azocalix[4]arenes with different modified groups. (3) The azo bonds of azocalix[4]arenes can be reduced under a hypoxic microenvironment caused by intracellular bacteria, resulting in the release of the indicator to varying degrees (Fig. 3a). Through these steps, the sensor array composed of multiple units can convert the inherent differences between target analytes into activated fluorescent signals. During LDA, the magnitude of the standardized coefficients indicates the degree of contribution made by each variable to the discrimination. Larger absolute values of the standardized coefficients signify a greater contribution of the corresponding predictor variable to the discriminant function74,75,76. As shown in Supplementary Table 7, ManAC4A, LysAC4A, SerAC4A, and CAC4A provided the largest discriminant contribution at the most important factor 1 dimension. Therefore, these four azocalix[4]arenes and six common intracellular bacteria (SA, MRSA, LM, EC, PA, and ST) were employed to validate the proposed hypothesis.
a Illustration of signal transduction of intracellular bacteria by azocalix[4]arene-based fluorescent sensor array. b Uptake capacity of ManAC4A, LysAC4A, SerAC4A, and CAC4A by macrophages infected with SA, MRSA, LM, ST, EC, and PA. The concentration of azocalix[4]arene was measured using UV − Vis spectroscopy. Data are presented as mean ± SD, n = 3 biological replicates. c The reduction kinetics fitting of ManAC4A, LysAC4A, SerAC4A, and CAC4A. Absorbance (red) at 420 nm of azocalix[4]arene (10.0 μM) as a function of time following the addition of SDT (2.3 mM) and the corresponding curve (blue) was fitted according to a quasi-first order reaction decay model. d Absorbance at 420 nm as a function of varying time of ManAC4A, LysAC4A, SerAC4A, and CAC4A (10.0 μM) in the presence of varying concentrations of rat liver microsomes (0, 15, 30, and 40 μg/mL) and 40.0 μM NADPH in PBS under hypoxic conditions. Source data are provided as a Source Data file.
First, IDA experiments were conducted by analyzing the fluorescence changes of different bacteria-infected macrophages added individually to the host-guest complexes. An increase in fluorescent intensity indicates the displacement of CY5 due to competitive binding (Supplementary Fig. 26a−c). Moreover, the extent of fluorescence changes varied, suggesting different interactions between azocalix[4]arenes and the analytes. It is worth noting that a contrasting phenomenon was observed when infected cells were added to the CY5@ManAC4A complex, leading to a further decrease in the fluorescence intensity (Supplementary Fig. 26d). This may be ascribed to the cooperative binding between CY5@ManAC4A and the cell analytes, but not the competitive binding. However, this is advantageous for differential sensing as it promotes more cross-reactivity. In a word, azocalix[4]arenes exhibit different supramolecular interactions with the same kind of infected macrophage, and the interaction between a specific azocalix[4]arene and macrophages infected with different types of bacteria also varies. This could be attributed to differences in the expression or quantity of receptors on the cell membrane following infection by different bacteria.
Next, we tested the ability of bacteria-infected macrophages to uptake these azocalix[4]arenes. The concentration of internalized azocalix[4]arenes was quantified by examining their UV−Vis spectra in culture medium before and after co-incubation with bacteria-infected macrophages. As illustrated in Fig. 3b, variations were observed in the uptake of different azocalix[4]arenes by each type of bacteria-infected macrophages. Among them, the uptake of ManAC4A was found to be higher compared to the amino acid- and carboxyl-modified azocalix[4]arenes. This can be attributed to the well-known binding of mannose to CD206, a mannose receptor that is abundantly expressed on the surfaces of macrophages77,78. Furthermore, the uptake of the same azocalix[4]arene exhibited variations among different intracellular bacteria. As mentioned in the literature, bacterial infection in macrophages can lead to coordinated expression of transport proteins55,79. The expression and functional levels of transporters may influence the rate and efficiency of endocytosis, thereby affecting the uptake amount of azocalix[4]arenes. Therefore, at the cellular uptake aspect, the good cross-reactivity of the sensor units has been validated, which is crucial for the response of the sensor unit towards analytes.
Finally, we examined the reduction kinetics of azocalix[4]arenes to hypoxic conditions. Sodium dithionite (SDT), an azo reductase mimic, was introduced into the solutions of azocalix[4]arenes. The intensity attenuation curves for the azo bond were well-fitted to a quasi-first-order reaction decay model. The obtained rate constants for ManAC4A, LysAC4A, SerAC4A, and CAC4A were 0.28, 2.05, 1.63, and 3.57 min−1, respectively (Fig. 3c). The corresponding half-lives were calculated to be 2.48, 0.34, 0.43, and 0.19 min. This indicates that the reduction kinetics of these four macrocycles with different modifying groups were distinct. Subsequently, enzyme-linked immunosorbent assay (ELISA) confirmed that the accumulation of hypoxia inducible factor-1 (HIF-1α) varied in infected macrophages depending on the bacterial species (Supplementary Fig. 27). Stimulation of bacterial infection leads to an upregulation of HIF-1α expression in macrophages, indicating cellular hypoxia80,81,82,83. To simulate the reduction response of each azocalix[4]arene to intracellular bacteria with varying degrees of hypoxia, the azocalix[4]arenes were treated with rat liver microsomes, which contain a wide range of redox enzymes84. The reduction rates of azocalix[4]arenes depended on the enzyme concentrations, corresponding to the differences in fluorescence signals generated in individual microenvironments (Fig. 3d).
Therefore, our meticulously designed sensor units facilitate the discrimination of intracellular bacteria through various processes, including but not limited to the interactions between the sensor units and bacteria-infected macrophages, cellular uptake, and hypoxia response. Among them, there are both thermodynamic factors, such as intermolecular interactions, chemical potential differences, transcription of specific genes, and significant kinetic factors, such as the rate of cellular uptake and reduction of azocalix[4]arenes. Currently, thermodynamic factors are often utilized to construct sensor arrays. Our disclosure of the rationale motivates great attention to kinetic information when designing sensor arrays, which can provide additional assistance for differential sensing based on cross-reactivity. Furthermore, it was observed that ManAC4A exhibited the highest cellular uptake by the tested macrophages infected with bacteria, significantly outperforming LysAC4A, SerAC4A, and CAC4A (Fig. 3b). Compared to the precursor CAC4A, the uptake capacity of ManAC4A increased by approximately 4 to 24 times. These findings highlight the considerable potential of ManAC4A as a drug delivery carrier for anti-intracellular bacterial infection.
In vitro anti-intracellular bacterial activity of the host-guest DDS
Hypoxia-responsive azocalix[4]arenes not only possess the ability to recognize intracellular bacteria through multiple pathways that integrate signal changes, but also demonstrate their potential in drug delivery for treating bacterial infection. To validate the conceptual treatment of intracellular bacterial infection, we utilized blind samples of MRSA identified by the sensor array as an example. ManAC4A, which exhibited the highest uptake capacity during the rational disclosure process, functions as a hypoxia-responsive drug delivery carrier. The hydrophilic mannose group modification at the upper rim of the azocalix[4]arene forms an amphiphilic ManAC4A, which self-assembles into nanoparticles with a hydrated diameter of approximately 80 nm at 20 μM (Supplementary Fig. 21d). The size of ManAC4A nanoparticles varies with concentration, reaching around 120 nm at 0.5–1.0 mM58. The morphologic structure was further confirmed by utilizing static light scattering (SLS) and DLS, in which the value of Rg/Rh was calculated to be 1.06, representing the vesicular morphology (Supplementary Fig. 28)85. This structure facilitates multivalent interactions with mannose receptors on the surface of macrophages and bacteria due to its amphiphilic assembly. The deep cavity of the azocalix[4]arene significantly enhances the antibiotic binding capacity, and the azocalix[4]arene is sensitive to bacterial intracellular azoreductase. Therefore, ManAC4A integrates loading, targeting, and controlled release, holding great potential in combating intracellular bacterial infections. CAC4A, devoid of the mannose group, was employed as the control compound.
To assess the role of ManAC4A as a carrier in facilitating antibiotic internalization into MRSA, the co-localization of ManAC4A and MRSA was initially observed using confocal laser scanning microscopy (CLSM). CY5, which can form complexes with ManAC4A and CAC4A resulting in significant fluorescence quenching, was utilized to track the localization of azocalix[4]arenes. The complexation between CY5 and ManAC4A or CAC4A was further validated by 1H NMR spectroscopy (Supplementary Figs. 29 and 30). In the presence of representative azocalix[4]arene ManAC4A or CAC4A, CY5 protons exhibited upfield shifts caused by the ring current effect of the aromatic nuclei of azocalix[4]arenes, indicating the encapsulation within the cavity of the azocalix[4]arenes. Under hypoxic conditions, the fluorescein isothiocyanate (FITC)-labeled MRSA (green fluorescence) was co-incubated with CY5@ManAC4A (red fluorescence in response), followed by CLSM observation (Supplementary Fig. 31). The results demonstrated substantial overlap between the green and red signals, indicating that the carrier facilitates antibiotic delivery into bacteria. Compared to bacteria treated with CAC4A, it has been confirmed that mannose modification enhances binding ability towards bacteria. In the free CY5 group, a minimal presence of CY5 within bacteria was observed; similarly, under normoxic conditions, there was a scant observable presence of CY5 in bacterial cells. This suggests that azocalix[4]arene not only aids small molecule penetration through bacterial membranes but also responds to release under hypoxic environments, potentially enhancing the bactericidal effect of the drug.
Dox has been reported as an effective treatment option against MRSA, while ciprofloxacin (Cip), a broad-spectrum antibiotic, has demonstrated limited efficacy86,87,88,89. A study involving over 2400 MRSA isolates obtained from patients with community-onset and nosocomial infections across various regions of the United States revealed that 89% of all isolates exhibited resistance to Cip90. We compared the bactericidal effect of Dox with Cip on MRSA (Supplementary Fig. 32a and b). Even at micromolar concentrations, Dox significantly inhibited MRSA growth, whereas Cip required concentrations hundreds of times higher for a similar effect. Furthermore, at equivalent drug concentrations, the DDS displayed a distinct difference in its killing effect on MRSA; the Dox group successfully eradicated most bacteria, while the Cip group only exerted a partial inhibitory effect on bacterial growth (Supplementary Fig. 32c). These findings underscore the importance of accurately identifying bacteria to guide appropriate antibiotic selection.
We then evaluated the loading capacity of azocalix[4]arenes for antibiotics. Due to the displacement of the dye Rhodamine B (RhB) from the cavity of CAC4A by Dox, Dox is considered to be loaded into the cavity of the azocalix[4]arene assemblies (Supplementary Figs. 33 and 34). The drug-loaded CAC4A and ManAC4A were prepared following established procedures in the literature (Supplementary Figs. 34 and 35)91. The complexation of Dox with azocalix[4]arenes was studied by 1H NMR spectroscopy (Supplementary Figs. 36 and 37). The results indicate that the protons of the benzene ring moiety of Dox underwent upfield shifts upon the addition of ManAC4A and CAC4A, suggesting that the benzene ring moiety has entered the deep cavities of ManAC4A and CAC4A. The DLS results indicate that the assembly sizes of CAC4A and ManAC4A complexes with Dox remain almost unchanged, suggesting that the original assembly structures were not disrupted (Supplementary Fig. 24). To obtain insight into the guest binding behaviors, geometry optimizations of Dox@ManAC4A and CY5@ManAC4A complexes were performed using B3LYP-D3/6-31 G(d, p)/SMD (water) method. We calculated and mapped the molecular electrostatic potential (MEP) on the molecular van der Waals surfaces of ManAC4A and these two guests (Dox and CY5, Supplementary Fig. 38a). In MEP maps, red indicates regions of positive electrostatic potential (electron-deficient), while blue indicates regions of negative electrostatic potential (electron-rich). The optimized binding geometry is reasonable since molecules tend to approach each other in a complementary manner based on the MEP. The green areas in the isosurfaces indicate that there are certain moderate interactions, such as van der Waals forces, between ManAC4A and the two guest molecules. For Dox, its amide moiety is likely to interact with the amide moiety of ManAC4A, which is reasonable according to the MEP. Its aromatic ring is poised to penetrate the azocalix[4]arene cavity (Supplementary Fig. 38b). In the case of CY5, π−π stacking interactions between the aromatic rings of CY5 and ManAC4A may contribute to complex formation (Supplementary Fig. 38b).
Next, the antibacterial activity of ManAC4A as a carrier for Dox delivery was investigated using the plate counting method (Fig. 4a). Treatment with Dox@ManAC4A significantly reduced MRSA viability compared to the PBS, Dox, and ManAC4A groups under hypoxic conditions (Fig. 4b). While CAC4A alone exhibited strong bactericidal ability, its efficacy as a carrier was inferior to that of ManAC4A in enhancing antibiotic-mediated bactericidal effects. In contrast to hypoxic conditions, the normoxic group treated with Dox@ManAC4A did not demonstrate such pronounced bactericidal performance. These results highlight the potential of ManAC4A as an effective carrier for the targeted delivery of Dox to bacteria by facilitating internalization and improving antimicrobial capacity through hypoxia-specific release. Living and dead bacteria were stained with acridine orange (AO, green fluorescence) and ethidium bromide (EB, red fluorescence), respectively, followed by visualized CLSM. As shown in Fig. 4c, bacteria in the control group exhibited green fluorescence indicating their viability; however, most bacteria displayed red fluorescence in the Dox@ManAC4A group signifying efficient damage inflicted on MRSA by released Dox from the carrier—a finding consistent with the plate counting method results.
a The images of remaining MRSA after being treated with PBS, Dox, CAC4A, ManAC4A, Dox@CAC4A, and Dox@ManAC4A under hypoxic and normoxic conditions, respectively. b The quantification of remaining MRSA after various treatments under hypoxic and normoxic conditions, respectively. Data are presented as mean ± SD, n = 3 biological replicates, *p < 0.05, **p < 0.01 and ***p < 0.001, two-tailed Student’s t-test. c Representative CLSM images of MRSA after different treatments under hypoxic and normoxic conditions. Scale bar: 25 μm. Data from 3 replicates. Source data are provided as a Source Data file.
To evaluate the capacity of ManAC4A in recognizing intracellular bacteria, a three-channel CLSM was employed to observe MRSA-infected macrophages (Fig. 5a). Macrophages (4’,6-diamidino-2-phenylindole (DAPI)-labeled, blue fluorescence) infected with MRSA (FITC-labeled, green fluorescence) were treated with azocalix[4]arenes (Cy5-complexed, red fluorescence). The distribution of ManAC4A exhibited significant overlap with that of MRSA and resulted in bright yellow fluorescence after superposition. In contrast, CAC4A lacking the targeting group produced weaker red fluorescence than ManAC4A, indicating the crucial role played by mannose motifs in intracellular bacterial targeting and internalization.
a Representative CLSM images of intracellular FITC-labeled MRSA after incubation with CY5@ManAC4A, CY5@CAC4A, and free CY5 under hypoxic conditions. Blue represented DAPI, green represented FITC, and red represented CY5. Scale bar: 25 μm. Data from 3 replicates. b The images of remaining intracellular MRSA after being treated with PBS, Dox, ManAC4A, and Dox@ManAC4A under hypoxic conditions. c The quantification of remaining intracellular MRSA after various treatments. Data are presented as mean ± SD, n = 3 biological replicates, *p < 0.05, **p < 0.01 and ***p < 0.001, two-tailed Student’s t-test. d The expression difference of IL-6 and TNF-α in MRSA-infected RAW 264.7 cells after different treatments determined by ELISA. Data are presented as mean ± SD, n = 3 biological replicates, *p < 0.05, **p < 0.01 and ***p < 0.001, two-tailed Student’s t-test. e Representative CLSM observation of MRSA-infected RAW 264.7 cells with the different treatments. Scale bar: 10 μm. Data from 3 replicates. Due to the cytotoxicity of CAC4A (Supplementary Fig. 39) and its inherent antibacterial activity (Fig. 4b), this control compound was excluded in subsequent experiments. Source data are provided as a Source Data file.
After confirming the targeting capability of ManAC4A to intracellular bacteria, we further investigated the efficacy of Dox@ManAC4A in eradicating intracellular bacteria. MRSA-infected RAW 264.7 macrophages were treated with PBS, Dox, ManAC4A, and Dox@ManAC4A followed by lysis and analysis of intracellular MRSA quantity using plate colony counting (Fig. 5b and c). Treatment with Dox resulted in inhibition of intracellular MRSA compared to the PBS group. The use of Dox@ManAC4A demonstrated enhanced inhibitory capacity over free Dox due to improved internalization mediated by mannose receptor-mediated endocytosis into macrophages facilitated by ManAC4A as a carrier. Moreover, treatment with Dox@ManAC4A led to decreased macrophage expression levels of TNF-α and IL-6, representative pro-inflammatory cytokines, indicating stronger inflammation alleviation abilities (Fig. 5d). Additionally, CLSM was employed to observe anti-intracellular accumulation of MRSA in infected RAW 264.7 cells (Fig. 5e). The results exhibited a significant decrease in the number of intracellular bacteria within the Dox@ManAC4A treatment group consistent with findings obtained through plate counting.
Evaluation of biocompatibility and in vivo antibacterial efficacy
The biosafety assessment of ManAC4A is imperative before its utilization as a drug delivery system for in vivo therapeutic applications. RAW 264.7 macrophages were employed to evaluate the cytotoxicity of ManAC4A. Remarkably, even after incubation with various concentrations of ManAC4A ranging from 0 to 500 μM for 24 h (Supplementary Fig. 39), the impact on cell viability was negligible, with cell viability consistently remaining above 90%. Furthermore, to assess the potential in vivo toxicity of ManAC4A, a mouse model was utilized and subjected to intraperitoneal injection once daily for three consecutive days. Encouragingly, no mortality or weight loss was observed across all treatment groups. Additionally, histomorphological examination through hematoxylin and eosin (H&E) staining revealed the tissue architecture without any significant pathological abnormalities in major organs including heart, liver, spleen, lung, and kidney (Supplementary Fig. 40), thereby indicating biocompatibility of ManAC4A.
Peritonitis, considered a serious threat, is a representative model of intracellular bacterial infection that necessitates a rapid response from macrophages to eliminate the infection (Fig. 6a)33,92. In this study, we assessed the antimicrobial efficacy of Dox@ManAC4A in peritonitis caused by MRSA infection. Female Balb/C mice (aged 6−7 weeks) were intraperitoneally injected with MRSA to establish an infection model and randomly divided into five groups. Following infection, the mice received treatment every 12 h for a total of two times, with the four groups consisting of (1) PBS, (2) Dox, (3) ManAC4A, and (4) Dox@ManAC4A. At 48 h post-infection, the mice were sacrificed, peritoneal fluid was collected, and intracellular, extracellular, and total MRSA CFUs in the peritoneal fluid were quantified using plate colony counting methods (Fig. 6b). The results demonstrated that Dox@ManAC4A effectively cleared extracellular MRSA bacteria and outperformed free Dox treatment, consistent with in vitro antibacterial evaluations. Moreover, Dox@ManAC4A exhibited enhanced in vivo antimicrobial activity against intracellular MRSA due to its excellent cellular and bacterial targeting capabilities mediated by the ManAC4A carrier. The overall bactericidal effect was consistent with the trend observed for intracellular and extracellular compartments (Fig. 6c and Supplementary Fig. 41). Thus, our findings highlight the superior therapeutic efficacy of the Dox@ManAC4A complex.
(a) Schematic diagram of the mouse intraperitoneal infection model. b Photographs in the total, intracellular, and extracellular fractions and (c) CFUs in the intracellular fraction determined after the different treatments. Data are presented as mean ± SD, n = 5 biological replicates, *p < 0.05, **p < 0.01 and ***p < 0.001, two-tailed Student’s t-test. d The expression difference of IL-6, TNF-α, and IL-10 after different treatments, determined by ELISA. Data are presented as mean ± SD, n = 3 biological replicates, *p < 0.05, **p < 0.01 and ***p < 0.001, two-tailed Student’s t-test. e Representative H&E staining images of the main tissues obtained from various treatment groups. Scale bar: 100 μm. Data from 3 replicates. Source data are provided as a Source Data file.
Pro-inflammatory and anti-inflammatory cytokine assays demonstrated that Dox@ManAC4A regulated the inflammatory phase (Fig. 6d). The expression levels of proinflammatory factors IL-6 and TNF-α were reduced by treatment with Dox@ManAC4A, while the levels of the anti-inflammatory factor IL-10 increased. These results suggest that Dox@ManAC4A effectively attenuated inflammation and promoted tissue reconstruction and recovery. The results of H&E analysis revealed liver and lung tissue damage in PBS-treated mice, including sinusoidal dilatation in the liver and significant heterogeneous widening of the alveolar ducts in the lung (Fig. 6e). In contrast, treatment with Dox@ManAC4A significantly mitigated or even eradicated these tissue damages, yielding histological analysis results comparable to those of the healthy group. The results of routine blood examination are presented in Supplementary Fig. 42. Compared to pre-treatment values, white blood cell count decreased most significantly after treatment in the Dox@ManAC4A group along with a decrease in neutrophil proportion, reflecting a reduction in systemic inflammation level. These findings demonstrate the remarkable efficacy of Dox@ManAC4A for intracellular infection treatment in vivo due to its active targeting capability and controlled release ability conferred by ManAC4A.
Discussion
In this study, we present a tandem diagnosis-guided treatment paradigm comprising a supramolecular sensor array and host-guest DDS for precise and personalized treatment of intracellular bacterial infections. The supramolecular sensor array enables rapid and accurate discrimination of tested intracellular bacteria, even infected cellular samples obtained from mice, without the need for cell lysis. By uncovering the rationale underlying discrimination, effective cross-reactivity originates from both thermodynamic and kinetic considerations throughout the entire sensing process, involving intermolecular interactions, cellular uptake, and hypoxia-controlled indicator release. These microevents are finally reflected in the fluorescence response signals. Such generated unique fluorescent fingerprint for each intracellular bacterial analyte allows for the differentiation of samples based on the response pattern. The diagnostic approach not only enables personalized antibiotic administration against identified bacteria but also, through rationale investigations, facilitates the screening of customized host-guest DDS that exhibit enhanced efficacy in combating intracellular MRSA infection in a peritonitis model. This work demonstrates the advantages of diagnosis-guided personalized and precise treatment of intracellular bacteria, providing an emerging paradigm in the field of therapy for bacterial infectious diseases.
Methods
Materials
All the reagents and solvents were commercially available and used as received unless otherwise specified purification. N,N-diisopropylethyl-amine (DIPEA), (7-azabenzotriazol-1-yl)-N,N,N’,N’-tetramethyluronium hexafluorophosphate (HATU), propargylamine, copper sulfate pentahydrate (CuSO4·5H2O), sodium ascorbate and sodium methanolate (MeONa) were purchased from TCI. 1,1′,3,3,3′,3′-Hexamethylindodicarbocyanine (CY5) was obtained OKeanos Tech. Co., Ltd. Rhodamine B (RhB) was purchased from Aladdin. Sodium dithionite (SDT) and acridine orange (AO) were purchased from J&K Chemical. Ethidium bromide (EB) was purchased from Saen Chemical Technology Company. Male rat liver microsomes were purchased from Meilunbio Tech. Co., Ltd. Dihydronicotinamide adenine dinucleotide phosphate tetrasodium salt (NADPH) was purchased from Ark. Doxycycline hydrochloride (Dox) was purchased from Shanghai Macklin Biochemical Co., Ltd. Ciprofloxacin (Cip) and lysostaphin were purchased from YuanYe Bio-Technology Co., Ltd. Fetal bovine serum (FBS) and Dulbecco’s modified eagle medium (DMEM) were purchased from Thermo Fisher Scientific. Hanks buffered saline solution (HBSS), phosphate-buffered saline (PBS, 10.0 mM, pH = 7.4), cell counting kit-8 (CCK-8), and 4’,6-diamino-2-phenylindole (DAPI) were purchased from Beijing Solarbio Science & Technology Co., Ltd. Mouse total HIF-1α ELISA kit, mouse TNF-a ELISA kit and mouse IL-6 ELISA kit were purchased from Multisciences (Lianke) Biotech Co., Ltd. Fluorescein isothiocyanate (FITC) was purchased from Heowns Biochem Technologies. The mouse mononuclear macrophage leukemia cell line (RAW 264.7 cells) was purchased from Procell Life Science&Technology Co., Ltd. Staphylococcus aureus (SA), multidrug-resistant Staphylococcus aureus (MRSA), Listeria monocytogenes (LM), Salmonella typhimurium (ST), Escherichia coli (EC), Pseudomonas aeruginosa (PA), Streptococcus mutans (SM) and Klebsiella pneumoniae (KP) were provided by Microbial Resource Platform, College of Life Sciences, Nankai University.
Apparatus
1H and 13C NMR data were recorded on a Bruker AV400 spectrometer. Mass spectra were performed on Fourier transform ion cyclotron resonance mass spectrometry (Varian 7.0 T FTMS, MALDI) and Agilent 6520 Q-TOF LC/MS (ESI). Fluorescence measurements for model samples were recorded in a black 96-well plate on an Agilent Cary Eclipse spectrometer equipped with a Cary Eclipse microplate reader accessory. Fluorescence measurements for clinical samples were recorded on a SpectraMax i3x microplate reader. UV−Vis spectra were recorded in a quartz cell (light path 10 mm) on a Cary 100 UV−Vis spectrophotometer equipped with a Cary dual-cell Peltier accessory. High-performance liquid chromatography (HPLC) system (Waters, Milford, MA, USA) was employed to perform chromatographic analysis. Fluorescence microscopy images were observed by a Leica TCS SP8 confocal laser scanning microscope (CLSM). Angle-dependent dynamic light scattering (DLS) and static light scattering (SLS) measurements were examined on a laser light scattering spectrometer (BI-200SM) equipped with a digital correlator (TurboCorr) at 636 nm. The other DLS sample solutions were examined on a laser light scattering spectrometer (NanoBrook 173plus) equipped with a digital correlator at 659 nm, at a scattering angle of 90°.
Synthesis of l-lysine-modified azocalix[4]arene (LysAC4A)
CAC4A (200 mg, 0.20 mmol), EDC (310 mg, 2 mmol) and NHS (230 mg, 2 mmol) were dissolved in DMF (20 mL). The solution was stirred at room temperature for 2 h and precipitated with excess water. The precipitate was dissolved in DMF (40 mL) and added to a round-bottomed flask pre-mixed with N-epsilon-Boc-l-lysine (394 mg, 1.6 mmol), Na2CO3 (212 mg, 2.0 mmol), DMF (10 mL) and water (10 mL). The mixture was stirred at room temperature for 24 h and precipitated with 300 mL of dilute HCl. The precipitate was stirred in 50 mL trifluoroacetic acid for 24 h, and the liquid was evaporated. The obtained solid was recrystallized with methanol and water to afford 272 mg brick-red LysAC4A with a yield of 90%.
Synthesis of l-serine-modified azocalix[4]arene (SerAC4A)
CAC4A (200 mg, 0.20 mmol), EDC (310 mg, 2 mmol) and NHS (230 mg, 2 mmol) were dissolved in DMF (20 mL). The solution was stirred at room temperature for 2 h and precipitated with excess water. The precipitate was dissolved in DMF (40 mL) and added to a round-bottomed flask pre-mixed with l-serine (168 mg, 1.6 mmol), Na2CO3 (212 mg, 2.0 mmol), DMF (10 mL), and water (10 mL). The mixture was stirred at room temperature for 24 h and precipitated with 300 mL of dilute HCl. The precipitate was recrystallized with methanol and water to afford 235 mg brick-red SerAC4A with a yield of 88%.
Discrimination of intracellular bacteria
RAW 264.7 cells were seeded in 6-well plates at a density of 5 × 105 cells/well and allowed to adhere overnight with 5% CO2/95% air. Then the cells were infected with various bacteria (OD600 = 2.0, 100 μL) at 37 °C to allow for phagocytosis, respectively. After 1 h of infection, the media were removed. The bacteria-infected cells were incubated with CY5@azocalix[4]arenes (20/20 μM) for 1 h. Subsequently, the cells were washed with PBS and the fluorescence intensity of the cell suspension was measured at an excitation wavelength of 630 nm. The obtained fluorescence intensities at 650 nm of CY5@azocalix[4]arenes were used as the response signals for array-based sensing analysis. Finally, the raw data matrix was handled using linear discriminant analysis (LDA) and principal component analysis (PCA).
Cellular uptake activity of azocalix[4]arenes
RAW 264.7 cells were seeded in 6-well plates at a density of 5 × 105 cells/well and allowed to adhere overnight. Then the cells were infected with various bacteria (SA, MRSA, LM, ST, EC, PA, OD600 = 2.0, 100 μL) at 37 °C to allow for phagocytosis, respectively. After 1 h of infection, the media were removed. The bacteria-infected cells were incubated with ManAC4A, LysAC4A, SerAC4A, and CAC4A (80 μM) at 37 °C for 1 h. The concentrations of azocalix[4]arenes taken up by the infected cells were obtained by quantifying the residual azocalix[4]arenes in the supernatant using UV − Vis.
Reduction kinetics of azocalix[4]arenes
The reduction kinetics of ManAC4A, LysAC4A, SerAC4A, and CAC4A were monitored using UV − Vis spectroscopy. Excess SDT (2.3 mM) was injected into 2.5 mL of azocalix[4]arene solutions (10.0 μM) to monitor the time-dependent absorbance of azocalix[4]arenes at 420 nm at 37 °C. Besides SDT, the time-dependent absorbance of ManAC4A, LysAC4A, SerAC4A, and CAC4A was measured in PBS containing varying concentrations of rat liver microsomes (15, 30 and 40 μg/mL) and NADPH (40.0 μM) at 37 °C. Argon gas was bubbled into the solution for 40 min to create a hypoxic environment.
In vitro antibacterial activity against intracellular bacteria
RAW 264.7 cells were seeded in 6-well plates at a density of 5 × 105 cells/well and allowed to adhere overnight. Then the cells were infected with MRSA (OD600 = 2.0, 100 μL) at 37 °C to allow for phagocytosis. After 1 h of infection, the media were removed, and the cells were further treated with lysostaphin (at a final concentration of 15 μg/mL) to obliterate extracellular bacteria. MRSA-infected RAW 264.7 cells were incubated with PBS, Dox (1.5 μM), ManAC4A (200 μM), and Dox@ManAC4A (1.5/200 μM) for 2 h under hypoxic conditions. After that, the cells were rinsed with sterile PBS and lysed with HBSS containing 1% Triton X-100. Samples were diluted and plated onto LB agar plates to determine the number of bacteria. The concentrations of IL-6 and TNF-α in cell culture supernatant were determined with ELISA kits. CLSM was performed by infecting RAW 264.7 cells with FITC-stained MRSA, followed by various treatments, and subsequent staining of the cell nuclei with DAPI.
In vivo antibacterial activity
Female Balb/c mice (aged 6 − 7 weeks) were purchased from Tianjin Huafukang Biotechnology Co., Ltd. MRSA-infected peritonitis model was used to test the antibacterial effect in vivo. The mice were randomly divided into 5 groups (n = 5 mice). Mice in the healthy group were intraperitoneally injected with PBS, and mice in other groups were intraperitoneally injected with MRSA solution (OD600 = 1.0, 50 μL). The criteria for successful modeling of peritonitis in mice were poor mental state, crouching immobility, anorexia, messy hair, and eye congestion. Subsequently, the mice were intraperitoneally injected with 100 μL of PBS, free Dox (2.25 mM, 6.0 mg/kg), ManAC4A (2.25 mM, 27.0 mg/kg), and Dox@ManAC4A (2.25/2.25 mM, 6.0/27.0 mg/kg) at 12 h and 24 h, respectively. After 24 h of treatment, the mice in each group were anesthetized, and their eyeball blood was collected for routine blood examination. Additionally, serum levels of pro-inflammatory cytokines, including IL-6 and TNF-α, as well as the anti-inflammatory cytokine IL-10, were measured. Then, the mice were sacrificed and intraperitoneally injected with 2 mL cold HBSS. The peritoneal fluid was collected to determine the total, extracellular, and intracellular CFUs by being distributed onto LB agar plates and cultured in a bacterial incubator overnight for colony counting. 1/3 peritoneal fluid was used to quantify the total CFUs. 1/3 peritoneal fluid was centrifuged and the supernatant was collected to quantify extracellular CFUs. 1/3 peritoneal fluid was incubated with lysostaphin (15 μg/mL) to kill the extracellular MRSA and lysed with HBSS containing 1% Triton X-100 to quantify intracellular CFUs. At last, the collected main organs including the heart, liver, spleen, lungs, and kidneys were collected and stained with H&E for histopathologic analysis. This study did not consider sex as a factor because the experimental model does not involve sex-specific variables or outcomes.
Statistics and reproducibility
Data are presented as mean ± SD. The number of statistical samples and experimental repeats were indicated in the figure legends. Experimental data were plotted and analyzed using either Microsoft Excel, Origin, or GraphPad Prism, and statistical significance was determined by Student’s t-test analysis (two-tailed) for two groups. A value of p < 0.05 was considered to indicate a significant difference.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
All data supporting the findings of this study are available within the main text, Supplementary Information, and source data file. Source data are provided with this paper.
References
Vos, T. et al. Global burden of 369 diseases and injuries in 204 countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 396, 1204–1222 (2020).
Ikuta et al. Global mortality associated with 33 bacterial pathogens in 2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 400, 2221–2248 (2022).
Kamaruzzaman, N. F., Kendall, S. & Good, L. Targeting the hard to reach: challenges and novel strategies in the treatment of intracellular bacterial infections. Br. J. Pharmacol. 174, 2225–2236 (2017).
Lehar, S. M. et al. Novel antibody-antibiotic conjugate eliminates intracellular S. aureus. Nature 527, 323–328 (2015).
de Souza Santos, M. & Orth, K. Subversion of the cytoskeleton by intracellular bacteria: lessons from Listeria, Salmonella and Vibrio. Cell Microbiol. 17, 164–173 (2015).
Ercoli, G. et al. Intracellular replication of Streptococcus pneumoniae inside splenic macrophages serves as a reservoir for septicaemia. Nat. Microbiol. 3, 600–610 (2018).
Masters, E. A. et al. Skeletal infections: microbial pathogenesis, immunity and clinical management. Nat. Rev. Microbiol. 20, 385–400 (2022).
Fu, A. et al. Tumor-resident intracellular microbiota promotes metastatic colonization in breast cancer. Cell 185, 1356–1372 (2022).
Liu, X., Liu, F., Ding, S., Shen, J. & Zhu, K. Sublethal levels of antibiotics promote bacterial persistence in epithelial cells. Adv. Sci. 7, 1900840 (2020).
Baré, M. et al. Importance of appropriateness of empiric antibiotic therapy on clinical outcomes in intra-abdominal infections. Int. J. Technol. Assess. Health Care 22, 242–248 (2006).
Yang, C.-Y. et al. Differential effects of inappropriate empirical antibiotic therapy in adults with community-onset gram-positive and gram-negative aerobe bacteremia. J. Infect. Chemother. 26, 222–229 (2020).
Kang, C.-I. et al. Bloodstream infections caused by antibiotic-resistant gram-negative bacilli: risk factors for mortality and impact of inappropriate initial antimicrobial therapy on outcome. Antimicrob. Agents Chemother. 49, 760–766 (2005).
Tulkens, P. M. Intracellular distribution and activity of antibiotics. Eur. J. Clin. Microbiol. Infect. Dis. 10, 100–106 (1991).
Cai, Q. et al. Chemotaxis-instructed intracellular Staphylococcus aureus infection detection by a targeting and self-assembly signal-enhanced photoacoustic probe. Nano. Lett. 18, 6229–6236 (2018).
Reisner, B. S. & Woods, G. L. Times to detection of bacteria and yeasts in BACTEC 9240 blood culture bottles. J. Clin. Microbiol. 37, 2024–2026 (1999).
Hamza, T. & Li, B. Differential responses of osteoblasts and macrophages upon Staphylococcus aureus infection. BMC Microbiol. 14, 207 (2014).
Wang, J. et al. A novel, universal and sensitive lateral-flow based method for the detection of multiple bacterial contamination in platelet concentrations. Anal. Sci. 28, 237–241 (2012).
Heesemann, J. & Laufs, R. Double immunofluorescence microscopic technique for accurate differentiation of extracellularly and intracellularly located bacteria in cell culture. J. Clin. Micobiol. 22, 168–175 (1985).
Romero-Gómez, M.-P., Gómez-Gil, R., Paño-Pardo, J. R. & Mingorance, J. Identification and susceptibility testing of microorganism by direct inoculation from positive blood culture bottles by combining MALDI-TOF and Vitek-2 Compact is rapid and effective. J. Infection 65, 513–520 (2012).
Sfeir, M. M. Diagnosis of multidrug-resistant pathogens of Pneumonia. Diagnostics 11, 2287 (2021).
Lee, M. M. S. et al. Highly efficient phototheranostics of macrophage-engulfed gram-positive bacteria using a NIR luminogen with aggregation-induced emission characteristics. Biomaterials 261, 120340 (2020).
Hu, R. et al. Specific discrimination of gram-positive bacteria and direct visualization of its infection towards mammalian cells by a DPAN-based AIEgen. Biomaterials 187, 47–54 (2018).
Dai, T. et al. An AIEgen as an intrinsic antibacterial agent for light-up detection and inactivation of intracellular gram-positive bacteria. Adv. Healthcare Mater. 10, 2100885 (2021).
Fu, F. et al. Intracellular pathogen detection based on dual-recognition units constructed fluorescence resonance energy transfer nanoprobe. Anal. Chem. 92, 11462–11468 (2020).
Chattopadhyay, A. N. et al. Nanosensor-enabled detection and identification of intracellular bacterial infections in macrophages. Biosensors 14, 360 (2024)
Qi, G. et al. An AIEgen-peptide conjugate as a phototheranostic agent for phagosome-entrapped bacteria. Angew. Chem. Int. Ed. 58, 16229–16235 (2019).
Qu, S. & Zhu, K. Endocytosis-mediated redistribution of antibiotics targets intracellular bacteria. Nanoscale 15, 4781–4794 (2023).
Ladavière, C. & Gref, R. Toward an optimized treatment of intracellular bacterial infections: input of nanoparticulate drug delivery systems. Nanomedicine 10, 3033–3055 (2015).
Feng, W., Chittò, M., Moriarty, T. F., Li, G. & Wang, X. Targeted drug delivery systems for eliminating intracellular bacteria. Macromol. Biosci. 23, 2200311 (2022).
Zhan, W. et al. Tandem guest-host-receptor recognitions precisely guide ciprofloxacin to eliminate intracellular Staphylococcus aureus. Angew. Chem. Int. Ed. 62, e202306427 (2023).
Xiong, M.-H. et al. Bacteria-responsive multifunctional nanogel for targeted antibiotic delivery. Adv. Mater. 24, 6175–6180 (2012).
Chen, Q. et al. Biodegradable nanoparticles decorated with different carbohydrates for efficient macrophage-targeted gene therapy. J. Control. Release 323, 179–190 (2020).
Feng, W. et al. Cascade-targeting poly(amino acid) nanoparticles eliminate intracellular bacteria via on-site antibiotic delivery. Adv. Mater. 34, e2109789 (2022).
Qiu, Y. et al. Synergistic clearance of intracellular pathogens by hyaluronan-streptomycin micelles encapsulated with rapamycin. Carbohydr. Polym. 210, 364–371 (2019).
Zhang, X. et al. The highly efficient elimination of intracellular bacteria via a metal organic framework (MOF)-based three-in-one delivery system. Nanoscale 11, 9468–9477 (2019).
Lunn, A. M., Unnikrishnan, M. & Perrier, S. Dual pH-responsive macrophage-targeted isoniazid glycoparticles for intracellular tuberculosis therapy. Biomacromolecules 22, 3756–3768 (2021).
Xiong, M. H. et al. Lipase-sensitive polymeric triple-layered nanogel for “on-demand” drug delivery. J. Am. Chem. Soc. 134, 4355–4362 (2012).
Ye, M. et al. A dual-responsive antibiotic-loaded nanoparticle specifically binds pathogens and overcomes antimicrobial-resistant Infections. Adv. Mater. 33, 2006772 (2021).
You, L., Zha, D. & Anslyn, E. V. Recent advances in supramolecular analytical chemistry using optical sensing. Chem. Rev. 115, 7840–7892 (2015).
Sasaki, Y., Kubota, R. & Minami, T. Molecular self-assembled chemosensors and their arrays. Coordin. Chem. Rev. 429, 213607 (2021).
Tian, J.-H. et al. A facile way to construct sensor array library via supramolecular chemistry for discriminating complex systems. Nat. Commun. 13, 4293 (2022).
Lavigne, J. J. & Anslyn, E. V. Sensing a paradigm shift in the field of molecular recognition: from selective to differential receptors. Angew. Chem. Int. Ed. 40, 3118–3130 (2001).
Hu, X.-Y. et al. A heteromultivalent host-guest sensor array for cell recognition and discrimination. Chem. Commun. 58, 13198–13201 (2022).
Geng, W.-C. et al. A noncovalent fluorescence turn-on strategy for hypoxia imaging. Angew. Chem. Int. Ed. 58, 2377–2381 (2019).
Hu, X.-Y., Fu, R. & Guo, D.-S. Hypoxia-responsive host-guest drug delivery system. Acc. Mater. Res. 4, 925–938 (2023).
Chen, F.-Y., Geng, W.-C., Cai, K. & Guo, D.-S. Molecular recognition of cyclophanes in water. Chin. Chem. Lett. 35, 109161 (2023).
Ryan, A. Azoreductases in drug metabolism. Br. J. Pharmacol. 174, 2161–2173 (2017).
Ryan, A., Wang, C. J., Laurieri, N., Westwood, I. & Sim, E. Reaction mechanism of azoreductases suggests convergent evolution with quinone oxidoreductases. Protein Cell 1, 780–790 (2010).
Nielsen, M. C. et al. The macrophage-related biomarkers sCD163 and sCD206 are released by different shedding mechanisms. J. Leukoc. Biol. 106, 1129–1138 (2019).
Lasky, C. E., Olson, R. M. & Brown, C. R. Macrophage polarization during murine Lyme Borreliosis. Infect. Immun. 83, 2627–2635 (2015).
Marino, K. V., Cagnoni, A. J., Croci, D. O. & Rabinovich, G. A. Targeting galectin-driven regulatory circuits in cancer and fibrosis. Nat. Rev. Drug. Discov. 22, 295–316 (2023).
Palma, A. S. et al. Ligands for the beta-glucan receptor, Dectin-1, assigned using “designer” microarrays of oligosaccharide probes (neoglycolipids) generated from glucan polysaccharides. J. Biol. Chem. 281, 5771–5779 (2006).
Imberty, A. & Varrot, A. Microbial recognition of human cell surface glycoconjugates. Curr. Opin. Struct. Biol. 18, 567–576 (2008).
Novoa, A. et al. A LecA ligand identified from a galactoside-conjugate array inhibits host cell invasion by Pseudomonas aeruginosa. Angew. Chem. Int. Ed. 53, 8885–8889 (2014).
Jiang, Q. & Shi, L. Coordination of the uptake and metabolism of amino acids in Mycobacterium tuberculosis-infected macrophages. Front. Immunol. 12, 711462 (2021).
Li, J.-J. et al. Lactose azocalixarene drug delivery system for the treatment of multidrug-resistant pseudomonas aeruginosa infected diabetic ulcer. Nat. Commun. 13, 6279 (2022).
Zhang, T.-X. et al. A hypoxia-responsive supramolecular formulation for imaging-guided photothermal therapy. Theranostics 12, 396–409 (2022).
Li, S. et al. Supramolecular integration of multifunctional nanomaterial by mannose-decorated azocalixarene with ginsenoside Rb1 for synergistic therapy of rheumatoid arthritis. ACS Nano 17, 25468–25482 (2023).
Geng, Y.-Q. et al. Alleviating recombinant tissue plasminogen activator-induced hemorrhagic transformation in ischemic stroke via targeted delivery of a ferroptosis inhibitor. Adv. Sci. 2309517 (2024).
Chen, M.-M. et al. Sulfonated azocalix[4]arene: a universal and effective taste-masking agent. ACS Appl. Mater. Interfaces 16, 53591–53598 (2024).
Helaine, S. et al. Internalization of Salmonella by macrophages induces formation of nonreplicating persisters. Science 343, 204–208 (2014).
Garzoni, C. & Kelley, W. L. Staphylococcus aureus: new evidence for intracellular persistence. Trends Microbiol. 17, 59–65 (2009).
Barbuddhe, S. B. & Chakraborty, T. Listeria as an enteroinvasive gastrointestinal pathogen. Curr. Top. Microbiol. Immunol. 337, 173–195 (2009).
Dikshit, N. et al. Intracellular uropathogenic E. coli exploits host Rab35 for iron acquisition and survival within urinary bladder cells. PLoS Pathog. 11, 1005083 (2015).
Angus, A. A. et al. Pseudomonas aeruginosa induces membrane blebs in epithelial cells, which are utilized as a niche for intracellular replication and motility. Infect. Immun. 76, 1992–2001 (2008).
Jiang, L. et al. Clearance of intracellular Klebsiella pneumoniae infection using gentamicin-loaded nanoparticles. J. Control. Release 279, 316–325 (2018).
Cano, V. et al. Klebsiella pneumoniae survives within macrophages by avoiding delivery to lysosomes. Cell Microbiol. 17, 1537–1560 (2015).
Chen, P.-M. et al. The two-component system ScnRK of Streptococcus mutans affects hydrogen peroxide resistance and murine macrophage killing. Microbes Infect. 10, 293–301 (2008).
Anzenbacher, P. Jr., Lubal, P., Bucek, P., Palacios, M. A. & Kozelkova, M. E. A practical approach to optical cross-reactive sensor arrays. Chem. Soc. Rev. 39, 3954–3979 (2010).
Lee, W.-C. et al. The impacts of bacterial co-infections and secondary bacterial infections on patients with severe influenza pneumonitis admitted to the intensive care units. J. Crit. Care 72, 154164 (2022).
Camus, L., Briaud, P., Vandenesch, F., Doléans-Jordheim, A. & Moreau, K. Mixed populations and co-infection: Pseudomonas aeruginosa and Staphylococcus aureus. Adv. Exp. Med. Biol. 1386, 397–424 (2022).
Tadielo, L. E. et al. Pure and mixed biofilms formation of Listeria monocytogenes and Salmonella Typhimurium on polypropylene surfaces. LWT Food Sci. Technol. 162, 113469 (2022).
Han, J. et al. A polymer/peptide complex-based sensor array that discriminates bacteria in urine. Angew. Chem. Int. Ed. 56, 15246–15251 (2017).
Zhong, Y., Qu, M. & Shen, A. H. Comparison of chemical composition and spectroscopy of purple-brownish red garnet from Zambia, Tanzania and Australia. Spectrosc. Spect. Anal. 42, 184–190 (2022).
Silva, D. et al. Prediction of long-term (5 Years) conversion to dementia using neuropsychological tests in a memory clinic setting. J. Alzheimers Dis. 34, 681–689 (2013).
UCLA: Statistical Consulting Group, Discriminant analysis, SPSS annotated output. https://stats.oarc.ucla.edu/spss/output/discriminant-analysis/.
Cummings, R. D. The mannose receptor ligands and the macrophage glycome. Curr. Opin. Struct. Biol. 75, 102394 (2022).
Martinez-Pomares, L. The mannose receptor. J. Leukoc. Biol. 92, 1177–1186 (2012).
Tsang, A. W., Oestergaard, K., Myers, J. T. & Swanson, J. A. Altered membrane trafficking in activated bone marrow-derived macrophages. J. Leukoc. Biol. 68, 487–494 (2000).
Knight, M. & Stanley, S. HIF-1α as a central mediator of cellular resistance to intracellular pathogens. Curr. Opin. Immunol. 60, 111–116 (2019).
Lee, P., Chandel, N. S. & Simon, M. C. Cellular adaptation to hypoxia through hypoxia inducible factors and beyond. Nat. Rev. Mol. Cell Biol. 21, 268–283 (2020).
Schaffer, K. & Taylor, C. T. The impact of hypoxia on bacterial infection. FEBS J. 282, 2260–2266 (2015).
Palazon, A., Goldrath, A. W., Nizet, V. & Johnson, R. S. HIF transcription factors, inflammation, and immunity. Immunity 41, 518–528 (2014).
Zhou, Y. et al. Azo-based small molecular hypoxia responsive theranostic for tumor-specific imaging and therapy. J. Control. Rel. 288, 14–22 (2018).
Patterson, J. P., Robin, M. P., Chassenieux, C., Colombani, O. & O’Reilly, R. K. The analysis of solution self-assembled polymeric nanomaterials. Chem. Soc. Rev. 43, 2412–2425 (2014).
Ruhe, J. J., Monson, T., Bradsher, R. W. & Menon, A. Use of long-acting tetracyclines for methicillin-resistant Staphylococcus aureus infections: case series and review of the literature. Clin. Infect. Dis. 40, 1429–1434 (2005).
Naimi, H. M., Rasekh, H., Noori, A. Z. & Bahaduri, M. A. Determination of antimicrobial susceptibility patterns in Staphylococcus aureus strains recovered from patients at two main health facilities in Kabul, Afghanistan. BMC Infect. Dis. 17, 737 (2017).
Tasneem, U. et al. Co-occurrence of antibiotic resistance and virulence genes in methicillin resistant Staphylococcus aureus (MRSA) isolates from Pakistan. Afr. Health Sci. 22, 486–495 (2022).
Son, N. T. et al. First report on multidrug-resistant methicillin-resistant Staphylococcus aureus isolates in children admitted to tertiary hospitals in Vietnam. J. Microbiol. Biotechnol. 29, 1460–1469 (2019).
Diekema, D. J. et al. Survey of infections due to Staphylococcus species: frequency of occurrence and antimicrobial susceptibility of isolates collected in the United States, Canada, Latin America, Europe, and the western Pacific region for the SENTRY antimicrobial surveillance program, 1997–1999. Clin. Infect. Dis. 32, S114–S132 (2001).
Zhang, T.-X. et al. A general hypoxia-responsive molecular container for tumor-targeted therapy. Adv. Mater. 32, 1908435 (2020).
Nandi, A. et al. Differential induction of inflammatory cytokines and reactive oxygen species in murine peritoneal macrophages and resident fresh bone marrow cells by acute staphylococcus aureus infection: contribution of toll-like receptor 2 (TLR2). Inflammation 38, 224–244 (2015).
Acknowledgements
The authors gratefully acknowledge financial support from NSFC (U20A20259 to D.S.G, 22101142 to X.Y.H., 21975133 to X.Z., and 22371147 to D.S.G), the Fundamental Research Funds for the Central Universities to D.S.G, the NCC Fund (grant no. NCC2020FH04 to D.S.G), and the Tianshan Innovation Team Plan of Xinjiang Uygur Autonomous Region (2023D14002 to D.S.G). The authors also acknowledge Dr. Zhihao Gong and Dr. Zhaoxi Sun for their contributions to theoretical calculations, and Shu-Xin Zhang for assistance with NMR experiments.
Author information
Authors and Affiliations
Contributions
J.H.T. and S.H. contributed equally. K.R.W., X.Y.H., X.Z., and D.S.G. conceptualized the project. J.H.T. and S.H. conducted the experimental work, analyzed the data, and drafted the manuscript. Z.H.W., J.J.L., B.S.S., Y.Y.Z., and H.Y.Z. synthesized the compounds. X.S. and Z.T.J. assisted in conducting the animal experiments. X.Y.H., X.Z., and D.S.G. supervised the work.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics
All the animal experiments were conducted in accordance with the guidelines of the Tianjin Medical Experimental Animal Care, and animal protocols were approved by the Institutional Animal Care and Use Committee of Yi Shengyuan Gene Technology (Tianjin) Co., Ltd. (Approval number: YSY-DWLL-2023371).
Peer review
Peer review information
Nature Communications thanks the anonymous, reviewers for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Tian, JH., Huang, S., Wang, ZH. et al. Supramolecular discrimination and diagnosis-guided treatment of intracellular bacteria. Nat Commun 16, 1016 (2025). https://doi.org/10.1038/s41467-025-56308-9
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-025-56308-9
This article is cited by
-
Harnessing immunopeptidomics for next-generation vaccines against intracellular bacterial pathogens
Molecular Biology Reports (2025)



![Fig. 3: Differential interactions and response signals between azocalix[4]arenes and intracellular bacteria.](http://media.springernature.com/lw685/springer-static/image/art%3A10.1038%2Fs41467-025-56308-9/MediaObjects/41467_2025_56308_Fig3_HTML.png)


