Abstract
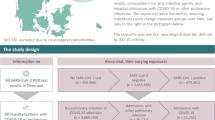
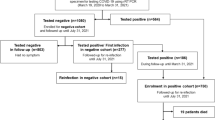
Nationwide follow-up studies of long-term post-acute COVID-19 sequelae compared with sequelae of other infections have been lacking. Using nationwide registers, we analyzed all SARS-CoV-2 PCR test results, prescriptions for anti-infective agents, and hospitalizations with COVID-19 or other infections in Denmark from March 2020 to June 2023, including up to 40-month follow-up. We used Cox proportional hazards models with time-varying exposures to estimate the rates of first-time mental disorders (n = 5,306,132) and general medical conditions (n = 3,517,630). Here we show that positive SARS-CoV-2 PCR tests alone were not associated with clinically relevant increased rates of mental disorders or general medical conditions when compared with negative SARS-CoV-2 PCR tests, nor when compared to individuals with anti-infective prescriptions. Rates of general medical conditions after a positive compared with a negative SARS-CoV-2 PCR test were only elevated for virus types preceding Omicron and for individuals with less than 3 vaccination doses. Compared with the general population, the rates of mental disorders or general medical conditions were elevated among hospitalized COVID-19 patients, and particularly when ICU treatment was required. However, when comparing patients hospitalized with COVID-19 to patients hospitalized with non-COVID-19 pulmonary infections or other infections, the rates of mental disorders or general medical conditions were increased to the same extent. In conclusion, severe COVID-19 post-infection sequelae are comparable to sequelae observed after other infections of similar severity.
Similar content being viewed by others
Data availability
We used the following registers: the Microbiology Database, the Danish National Patient Register, the Danish Psychiatric Central Research Register, the Population Education Register, the Income Statistics Register, and the Danish National Prescription Register. The data are available from Statistics Denmark, https://www.dst.dk/en/TilSalg/Forskningsservice/Dataadgang. To access health data in Denmark, applications must be submitted to the Danish Data Protection Agency, the Danish National Board of Health, and Statistics Denmark. For more information, see https://www.itgovernance.eu/da-dk/eu-gdpr-compliance-dk, https://sundhedsdatastyrelsen.dk/da/english, and https://dst.dk/en. Source data are provided with this paper.
Code availability
Code available at: https://github.com/Biological-and-Precision-Psychiatry/COVID-19-post-infection-sequelae63. The managing of data, analyses, and illustrations were made in R version 4.4.1. Analyses using the Cox proportional hazards model were performed with the coxph function from the survival package version 3.7-0. Additional packages used (version): data.table (1.16.2), dplyr (1.1.4), lubridate (1.9.3), foreach (1.5.2), doParallel (1.0.17), and emmeans (1.10.2).
References
World Health Organization. Coronavirus Disease (COVID-19). https://www.who.int/news-room/fact-sheets/detail/coronavirus-disease-(covid-19) (2023).
Lancet, T. Long COVID: 3 years in. Lancet 401, 795 (2023).
Ballering, A. V., van Zon, S. K. R., Olde Hartman, T. C. & Rosmalen, J. G. M. Persistence of somatic symptoms after COVID-19 in the Netherlands: an observational cohort study. Lancet 400, 452–461 (2022).
Daugherty, S. E. et al. Risk of clinical sequelae after the acute phase of SARS-CoV-2 infection: retrospective cohort study. BMJ 373, n1098 (2021).
Cohen, K. et al. Risk of persistent and new clinical sequelae among adults aged 65 years and older during the post-acute phase of SARS-CoV-2 infection: retrospective cohort study. BMJ 376, e068414 (2022).
Bowe, B., Xie, Y. & Al-Aly, Z. Postacute sequelae of COVID-19 at 2 years. Nat. Med. 29, 2347–2357 (2023).
Al-Aly, Z., Bowe, B. & Xie, Y. Long COVID after breakthrough SARS-CoV-2 infection. Nat. Med. 28, 1461–1467 (2022).
Rahmati, M. et al. New-onset neurodegenerative diseases as long-term sequelae of SARS-CoV-2 infection: a systematic review and meta-analysis. J. Med. Virol. 95, e28909 (2023).
Shrestha, A. B. et al. Long COVID syndrome and cardiovascular manifestations: a systematic review and meta-analysis. Diagnostics 13, 491 (2023).
Zuin, M. et al. Increased risk of acute myocardial infarction after COVID-19 recovery: a systematic review and meta-analysis. Int. J. Cardiol. 372, 138–143 (2023).
Zuin, M., Rigatelli, G., Bilato, C., Pasquetto, G. & Mazza, A. Risk of incident new-onset arterial hypertension after COVID-19 recovery: a systematic review and meta-analysis. High. Blood Press. Cardiovasc. Prev. 30, 227–233 (2023).
Zuin, M. et al. One-year risk of myocarditis after COVID-19 infection: a systematic review and meta-analysis. Can. J. Cardiol. 39, 839–844 (2023).
Pan, B. et al. Risk of kidney and liver diseases after COVID-19 infection: a systematic review and meta-analysis. Rev. Med. Virol. 34, e2523 (2024).
Zhang, T. et al. Risk for newly diagnosed diabetes after COVID-19: a systematic review and meta-analysis. BMC Med. 20, 444 (2022).
Lund, L. C. et al. Post-acute effects of SARS-CoV-2 infection in individuals not requiring hospital admission: a Danish population-based cohort study. Lancet Infect. Dis. 21, 1373–1382 (2021).
Nersesjan, V., Christensen, R. H. B., Kondziella, D. & Benros, M. E. COVID-19 and risk for mental disorders among adults in Denmark. JAMA Psychiatry 80, 778–786 (2023).
Clift, A. K. et al. Neuropsychiatric ramifications of severe COVID-19 and other severe acute respiratory infections. JAMA Psychiatry 79, 690 (2022).
Grønkjær, C. S., Christensen, R. H. B., Kondziella, D. & Benros, M. E. Long-term neurological outcome after COVID-19 using all SARS-CoV-2 test results and hospitalisations in Denmark with 22-month follow-up. Nat. Commun. 14, 4235 (2023).
Taquet, M. et al. Neurological and psychiatric risk trajectories after SARS-CoV-2 infection: an analysis of 2-year retrospective cohort studies including 1 284 437 patients. Lancet Psychiatry 9, 815–827 (2022).
Lai, Y.-J. et al. Biomarkers in long COVID-19: a systematic review. Front. Med. 10, 1085988 (2023).
Espín, E. et al. Cellular and molecular biomarkers of long COVID: a scoping review. EBioMedicine 91, 104552 (2023).
Ellingjord-Dale, M., Brunvoll, S. H. & Søraas, A. Prospective memory assessment before and after Covid-19. N. Engl. J. Med. 390, 863–865 (2024).
Ellingjord-Dale, M. et al. Temporal trajectories of long-COVID symptoms in adults with 22 months follow-up in a prospective cohort study in Norway. Int. J. Infect. Dis. 149, 107263 (2024).
Spudich, S. & Nath, A. Nervous system consequences of COVID-19. Science 375, 267–269 (2022).
Yong, S. J. Long COVID or post-COVID-19 syndrome: putative pathophysiology, risk factors, and treatments. Infect. Dis. 53, 737–754 (2021).
State Serum Institute. Timeline for COVID-19 (in Danish). https://www.ssi.dk/-/media/arkiv/subsites/covid19/presse/tidslinje-over-covid-19/covid-19-tidslinje-lang-for-2020-2022-version-2---december-2022.pdf (2022).
Pottegård, A. et al. Existing data sources in clinical epidemiology: the Danish COVID-19 cohort. Clin. Epidemiol. 12, 875–881 (2020).
Umberson, D. & Montez, J. K. Social relationships and health: a flashpoint for health policy. J. Health Soc. Behav. 51, S54–S66 (2010).
Schmidt, M. et al. The Danish National Patient Registry: a review of content, data quality, and research potential. Clin. Epidemiol. 7, 449–490 (2015).
Wildenschild, C. et al. Registration of acute stroke: validity in the Danish Stroke Registry and the Danish National Registry of Patients. Clin. Epidemiol. 6, 27–36 (2014).
Johnsen, S. P., Ingeman, A., Hundborg, H. H., Schaarup, S. Z. & Gyllenborg, J. The Danish stroke registry. Clin. Epidemiol. 8, 697–702 (2016).
Christensen, J., Vestergaard, M., Olsen, J. & Sidenius, P. Validation of epilepsy diagnoses in the Danish National Hospital Register. Epilepsy Res. 75, 162–170 (2007).
Jensen, V. M. & Rasmussen, A. W. Danish education registers. Scand. J. Public Health 39, 91–94 (2011).
Phung, T. K. T. et al. Validity of dementia diagnoses in the Danish hospital registers. Dement. Geriatr. Cogn. Disord. 24, 220–228 (2007).
Koch-Henriksen, N., Rasmussen, S., Stenager, E. & Madsen, M. The Danish multiple sclerosis registry. History, data collection and validity. Dan. Med. Bull. 48, 91–94 (2001).
Brønnum-Hansen, H., Koch-Henriksen, N. & Stenager, E. The Danish multiple sclerosis registry. Scand. J. Public Health 39, 62–64 (2011).
Wermuth, L., Lassen, C. F., Himmerslev, L., Olsen, J. & Ritz, B. Validation of hospital register-based diagnosis of Parkinson’s disease. Dan. Med. J. 59, A4391 (2012).
Mors, O., Perto, G. P. & Mortensen, P. B. The Danish psychiatric central research register. Scand. J. Public Health 39, 54–57 (2011).
State Serum Institute. COVID-19 - monitoring [in Danish]. https://www.ssi.dk/sygdomme-beredskab-og-forskning/sygdomsovervaagning/c/covid19-overvaagning (2023). Date accessed: 25. februar 2026.
Davis, H. E., McCorkell, L., Vogel, J. M. & Topol, E. J. Long COVID: major findings, mechanisms and recommendations. Nat. Rev. Microbiol. https://doi.org/10.1038/s41579-022-00846-2 (2023).
Kucirka, L. M., Lauer, S. A., Laeyendecker, O., Boon, D. & Lessler, J. Variation in false-negative rate of reverse transcriptase polymerase chain reaction-based SARS-CoV-2 tests by time since exposure. Ann. Intern. Med. 173, 262–268 (2020).
Pedersen, C. B. The Danish civil registration system. Scand. J. Public Health 39, 22–25 (2011).
Voldstedlund, M., Haarh, M. & Mølbak, K. The Danish microbiology database (MIBA) 2010 to 2013. Eurosurveillance 19, 20667 (2014).
Lynge, E., Sandegaard, J. L. & Rebolj, M. The Danish national patient register. Scand. J. Public Health 39, 30–33 (2011).
Lam, I. C. H. et al. Long-term post-acute sequelae of COVID-19 infection: a retrospective, multi-database cohort study in Hong Kong and the UK. EClinicalMedicine 60, 102000 (2023).
Wan, E. Y. F. et al. Association of COVID-19 with short- and long-term risk of cardiovascular disease and mortality: a prospective cohort in UK Biobank. Cardiovasc. Res. 119, 1718–1727 (2023).
Xu, E., Xie, Y. & Al-Aly, Z. Long-term gastrointestinal outcomes of COVID-19. Nat. Commun. 14, 983 (2023).
Xie, Y., Xu, E., Bowe, B. & Al-Aly, Z. Long-term cardiovascular outcomes of COVID-19. Nat. Med. 28, 583–590 (2022).
Xie, Y., Xu, E. & Al-Aly, Z. Risks of mental health outcomes in people with COVID-19: cohort study. BMJ 376, e068993 (2022).
Xu, E., Xie, Y. & Al-Aly, Z. Long-term neurologic outcomes of COVID-19. Nat. Med. 28, 2406–2415 (2022).
Xie, Y., Bowe, B. & Al-Aly, Z. Burdens of post-acute sequelae of COVID-19 by severity of acute infection, demographics and health status. Nat. Commun. 12, 6571 (2021).
Yang, X. et al. Two-year health outcomes in hospitalized COVID-19 survivors in China. JAMA Netw. Open 5, e2231790 (2022).
Huang, L. et al. Health outcomes in people 2 years after surviving hospitalisation with COVID-19: a longitudinal cohort study. Lancet Respir. Med. 10, 863–876 (2022).
Fernández-de-Las-Peñas, C. et al. Post-COVID-19 symptoms 2 years after SARS-CoV-2 infection among hospitalized vs nonhospitalized patients. JAMA Netw. Open 5, e2242106 (2022).
Momen, N. C. et al. Association between mental disorders and subsequent medical conditions. N. Engl. J. Med. 382, 1721–1731 (2020).
Osler, M. et al. Hearing loss, cognitive ability, and dementia in men age 19–78 years. Eur. J. Epidemiol. 34, 125–130 (2019).
Islamoska, S. et al. Mid- to late-life migraine diagnoses and risk of dementia: a national register-based follow-up study. J. Headache Pain. 21, 98 (2020).
Baadsgaard, M. & Quitzau, J. Danish registers on personal income and transfer payments. Scand. J. Public Health 39, 103–105 (2011).
Charlson, M. E., Pompei, P., Ales, K. L. & MacKenzie, C. R. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J. Chronic Dis. 40, 373–383 (1987).
Arendt, J. F. H. et al. Existing data sources in clinical epidemiology: laboratory information system databases in Denmark. Clin. Epidemiol. 12, 469–475 (2020).
Wallach Kildemoes, H., Toft Sørensen, H. & Hallas, J. The Danish national prescription registry. Scand. J. Public Health 39, 38–41 (2011).
Grove Krause, T., Jakobsen, S., Haarh, M. & Mølbak, K. The Danish vaccination register. Euro Surveill. 17, 20155 (2012).
Christensen, R. H. B. & Grønkjær, C. S. Post-infection sequelae of COVID-19 and other infectious diseases—a nationwide Danish study with 40-month follow-up. Biological-and-precision-psychiatry/COVID-19-post-infection-sequelae: first release (v1.0.0). Zenodo. https://doi.org/10.5281/zenodo.18486856 (2026).
Acknowledgements
We thank Elisabeth Anne Wreford Andersen for invaluable input for the pre-registration of this study and the data analysis. The research was funded by an unrestricted grant from the Novo Nordisk Foundation (grant number NNF21OC0067769) (M.E.B. and D.K.) and the Lundbeck Foundation (grant number 349-2020-658) (M.E.B. and D.K.). The funding sources had no role in the design, data, analysis, interpretation, writing of the article, or decision to publish the findings.
Author information
Authors and Affiliations
Contributions
M.E.B. and D.K. received funding for the study. All authors participated in the design of the study. C.S.G. and R.H.B.C. verified the underlying data. C.S.G. conducted the statistical analysis, wrote the first draft of the manuscript, and all authors contributed to editing and approving the final version.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Anders Koch, Merete Ellingjord-Dale and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Grønkjær, C.S., Christensen, R.H.B., Kondziella, D. et al. Post-infection sequelae of COVID-19 and other infectious diseases—a nationwide Danish study with 40-month follow-up. Nat Commun (2026). https://doi.org/10.1038/s41467-026-70351-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-026-70351-0